Beruflich Dokumente
Kultur Dokumente
Meningomyelocele
Hochgeladen von
rajan kumar0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
2K Ansichten34 SeitenMyelomeningocele is the most serious central nervous system birth defect compatible with life. Described from times of hippocrates and aristotle, who even recommended infanticide for these children Progress in treatment rapid since introduction of valved Many aspects still remain undiscovered. Associated in most cases with Arnold Chiari type II malformation Possible Aetiology Cytotoxic agents - Vinblastine and cyto chalasins Calcium channel blockers Phospholipase
Originalbeschreibung:
Copyright
© Attribution Non-Commercial (BY-NC)
Verfügbare Formate
PPT, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenMyelomeningocele is the most serious central nervous system birth defect compatible with life. Described from times of hippocrates and aristotle, who even recommended infanticide for these children Progress in treatment rapid since introduction of valved Many aspects still remain undiscovered. Associated in most cases with Arnold Chiari type II malformation Possible Aetiology Cytotoxic agents - Vinblastine and cyto chalasins Calcium channel blockers Phospholipase
Copyright:
Attribution Non-Commercial (BY-NC)
Verfügbare Formate
Als PPT, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
2K Ansichten34 SeitenMeningomyelocele
Hochgeladen von
rajan kumarMyelomeningocele is the most serious central nervous system birth defect compatible with life. Described from times of hippocrates and aristotle, who even recommended infanticide for these children Progress in treatment rapid since introduction of valved Many aspects still remain undiscovered. Associated in most cases with Arnold Chiari type II malformation Possible Aetiology Cytotoxic agents - Vinblastine and cyto chalasins Calcium channel blockers Phospholipase
Copyright:
Attribution Non-Commercial (BY-NC)
Verfügbare Formate
Als PPT, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 34
Meningomyelocele
Introduction
Most serious central nervous system birth defect compatible
with life
Described from times of Hippocrates & Aristotle, who even
recommended infanticide for these children
Progress in treatment rapid since introduction of valved
shunts
Many aspects still remain undiscovered
Embryopathology
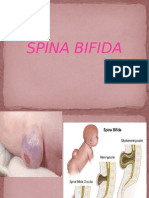
Localised failure of caudal neural tube closure causes
meningomyelocele
Two theories suggested
- Nonclosure theory
- Overdistension theory
Overdistension theory has now been discarded
Associated in most cases with Arnold Chiari type II
malformation
Possible Aetiology
Cytotoxic agents – Vinblastine & cyto chalasins
Calcium channel blockers
Phospholipase – C or concanavalin A
Retinoic acid, Hydroxyurea, Mitomycin C
Deficiency of folate
Misexpression of Pax 3 gene product causes neural
tube defects
Epidemiology
Incidence 0.7 – 0.8 per 1000 live births
Recurrence risk for parents with
1 previously affected child rises to 1-2%
2 previously affected children raises risk to as
high as 10 %
For a parent with myelomeningocele the risk of
child with the same is 3%
Prenatal diagnosis
Maternal AFP at 16 to 18 wks detects open neural
tube defects with sensitivity of 75% ( not specific)
Fetal USG has a sensitivity of nearly 100%
( Banana sign & Lemon sign)
Amniotic fluid AFP & AChE done together final
method of identification
Initial neurosurgical care
Includes
2. Stabilizing the infant, identifying associated
abnormalities, closing myelomeningocele
4. Treating associated hydrocephalus when
present
Initial clinical assessment
Spinal level & size of lesion, redundancy and quality of
surrounding skin, presence of kyphosis can affect difficulty of
repair
Sensorimotor level determined by observing movements of
lower limbs & response to sensation
Initial evaluation for hydrocephalous i.e. head circumference,
palpation of anterior fontanelle, sutural diastasis
Assessment of lower cranial nerves and brainstem function
Initial clinical assessment
Poor prognostic signs
Poor feeding/nasal regurgitation,
Weak cry, stridor, central apneoa,
Hypotonia, poor head control, weak upper
extremities
General paediatric examination to identify
associated congenital anomalies
Stabilisation & pre operative
care
Placode protected since birth by covering with
sterile saline soaked gauzes (not with povidone
iodine) since it contains partially functioning neural
tissue
Systemic antibiotics for 1st 3 post natal days to
prevent CSF / UT infections
Operative treatment
Operative treatment
Placode closed in 1st 48 – 72 hrs to avoid neurologic
deterioration & meningitis
Care taken to avoid cutting dorsal nerve roots along ventral
side of placode near its skin border
Intact filum terminale / associated anomalies causing
persistent tethering sectioned or treated simutaneously
Dural sac made capacious to prevent tethering
Operative treatment
Significant kyphosis interferes with closure,
compromises spinal stability hence kyphectomy
performed simultaneously
Skin subcutaneous tissues undermined and closed
primarily
For large skin defects transposition flaps or
musculocutaneous flaps used
Treatment of Hydrocephalous
Hydrocephalous clinically evident at birth (15%) or
develops days to weeks after closure of placode
If untreated CSF may leak from wound chances
of meningitis
USG or CT measurements of ventricular size
done
Pulsed Doppler measurements of IC bld flow &
resistive index in borderline cases
Progressive increase in RI more suggestive
Treatment of Hydrocephalous
Most common treatment is VP shunt
Isolated contralateral entrapped lateral ventricle
after shunting seen in these pts due to stenosis /
obstruction of foramen of Monro
Shunting contralateral ventricle or fenestrating
septum pellucidum treats these cases
Hydrocephalous in Older child
By 6yrs 52% children with meningomyelocele have had shunt revision &
20 % multiple revisions
Signs & symptoms of shunt malfunction in meningomyelocele
4. Headache, loss of appetite, nausea , vomiting
5. Behavioral changes
6. New onset / change in freq of seizures
7. Decline in motor performence
8. Worsening urinary function
9. Stridor / Vocal cord palsy
10. Pain in back or legs
11. Worsening scoliosis
Hydrocephalous in Older child
Fundoscopy a must in such cases
Cranial USG & CT for change in ventricular size
Shunt tap provides valuable info on shunt blockage
Traditionally malfunctions treated by shunt revision but
recently third ventriculostomy may be done in >6mths of
age
Encephalocele
Introduction
Congenital malformation where CNS structures in
communication with CSF pathways herniate
through defect in cranium
Incidence varies geographically from 1 in 3000 to
1 in 10000 live births
Classification
According to According to location
contents of
swelling Posterior
Meningocele
- occipital
Encephalocele
Anterior
Meningoencephaloce
- frontal
le
- sincipital
Hydroencephalomeni
ngocele - basal
Encephalocystocele
Pathophysiology
Primary abnormality is mesodermal defect resulting in defect in calvarium
and dura with herniation of CSF, brain tissue,meninges through defect
Failure of surface ectoderm to separate from neuroectoderm early in
embryonic development
In the calvarium, induction of bone formation may be defective, or
pressure erosion from an intracranial mass may occur
Defects at skull base may be related to faulty closure of neural tube or
failure of basilar ossification
Frontoethmoidal encephaloceles most common in Asia.
Clinical presentation
Swelling present at birth
Head size small ( larger the herniation smaller the head
size )
Frontoethmoidal – swelling over root or bridge of nose
Nasopharyngeal, sphenoethmoidal,
transsphenoidal – no obvious external swelling, CSF
rhinorrhea or nasal obstruction may be present
Orbital – proptosis
Occipital – posterior swelling
Associated Pathologies
Cleft lip, palate
Micrognathia
Spinovertebral anomalies
Renal agenesis
Retinal detachment
Cardiac anomalies
Pulmonary & renal hypoplasia
Prenatal Diagnosis
Diagnosis thought impossible before skull ossification at 10 weeks'
gestation (Earliest reported at 13 weeks' gestation)
US appearances of encephalocele variable in first trimester
Once diagnosed, search for associated anomalies, both intracranial
and extracranial (60-80%) performed
Risk of chromosomal abnormalities 13-44%; karyotyping offered to
mother
USG mainstay of fetal imaging, fetal MRI provides superior detail of
central nervous system (CNS) anomalies
Prenatal USG
3D Reconstruction of USG
Differential diagnosis
- Branchial cleft cyst
- Hemangioma
- Cystic hygroma
- Myelomeningocele
- Scalp edema
- Teratoma
- Epidermal scalp cyst
- Cloverleaf skull
Operative treatment
Consists of excision of hernial sac & repair of dural defect after
replacing brain into cranial cavity
Not an emergency except when CSF leak present
Extensive surgery better tolerated at 6-8 mths of age
VP shunt can be inserted before corrective surgery to prevent
leak
Surgery best avoided when microcephaly with extensive
neural tissue in sac present
Prognosis
Size, content and presence of hydrocephalus
influence prognosis in posterior encephalocele
In absence of hydrocephalus & meningitis
prognosis of anterior encephalocele is usually
good
Absence of brain tissue within herniated sac most
favorable prognostic feature for survival
Preop & post op anterior
encephalocele
Preop & post op posterior
encephalocele
Das könnte Ihnen auch gefallen
- Spina BifidaDokument33 SeitenSpina BifidaRegine Prongoso DagumanpanNoch keine Bewertungen
- Neural Tube Defects: Group 1Dokument28 SeitenNeural Tube Defects: Group 1imneverwrong2492100% (1)
- ACFrOgBz6SCL6SA VJUDh46tP6NUDhw3P47 NPjiCaRlywgh9trN 5PhQeKcHqMl2xUsHtUBcc7n4mL1On5SlTP2X94BYDVb HoGkGegg5erftVOvtVci7Q4s0omLCXYn6dldjBQhk2bZ6Jpfl6cDokument24 SeitenACFrOgBz6SCL6SA VJUDh46tP6NUDhw3P47 NPjiCaRlywgh9trN 5PhQeKcHqMl2xUsHtUBcc7n4mL1On5SlTP2X94BYDVb HoGkGegg5erftVOvtVci7Q4s0omLCXYn6dldjBQhk2bZ6Jpfl6cMalavika A GNoch keine Bewertungen
- Encephaloceles - An Encephalocele Is A Cranial Meningocele. These Occur Most Often in TheDokument6 SeitenEncephaloceles - An Encephalocele Is A Cranial Meningocele. These Occur Most Often in Thecriselda desistoNoch keine Bewertungen
- Neural Tube Defects: Dr.M.G.Kartheeka Fellow in Neonatology Cloudnine, OARDokument36 SeitenNeural Tube Defects: Dr.M.G.Kartheeka Fellow in Neonatology Cloudnine, OARM G KARTHEEKANoch keine Bewertungen
- Neural Tube DefectDokument8 SeitenNeural Tube DefectReema Akberali nooraniNoch keine Bewertungen
- Congenital Neurologic DisordersDokument114 SeitenCongenital Neurologic DisordersKirk08Noch keine Bewertungen
- CNS Congenital AnomaliesDokument74 SeitenCNS Congenital AnomaliesMoh DrhusseinyNoch keine Bewertungen
- Birth Injuries To The BabyDokument7 SeitenBirth Injuries To The BabyNeeraj DwivediNoch keine Bewertungen
- CNS AbnormalitiesDokument127 SeitenCNS AbnormalitiesJosselle Sempio CalientaNoch keine Bewertungen
- Trans Congenital MalformationsDokument10 SeitenTrans Congenital MalformationsRemelou Garchitorena AlfelorNoch keine Bewertungen
- Hydrocephalus: Dr. Tondi Maspian Tjili SPBS, M.KesDokument34 SeitenHydrocephalus: Dr. Tondi Maspian Tjili SPBS, M.KesLuthfianaNoch keine Bewertungen
- Birthinjuries Dr.M.maniDokument65 SeitenBirthinjuries Dr.M.manimaniNoch keine Bewertungen
- Pedia-Reviewer CompleteDokument36 SeitenPedia-Reviewer CompletePotato BroNoch keine Bewertungen
- Close During Embryonic Development Generally in The Lumbosacral RegionDokument24 SeitenClose During Embryonic Development Generally in The Lumbosacral RegionPotato BroNoch keine Bewertungen
- Hydrocephalus - Pediatrics - MSD Manual Professional EditionDokument4 SeitenHydrocephalus - Pediatrics - MSD Manual Professional EditionTONY GO AWAYNoch keine Bewertungen
- Pattern of Encephaloceles A Case SeriesDokument4 SeitenPattern of Encephaloceles A Case SeriesSayyid Hakam PerkasaNoch keine Bewertungen
- HydrocephalusDokument33 SeitenHydrocephalusrajan kumar100% (2)
- Cornell A 2003Dokument13 SeitenCornell A 2003dnazaryNoch keine Bewertungen
- No. 44. Neural Tube DefectsDokument11 SeitenNo. 44. Neural Tube DefectsenriqueNoch keine Bewertungen
- Anesthesia For Neurosurgery in Infants and Children: Barbara Van de Wiele, M.D. Los Angeles, CaliforniaDokument24 SeitenAnesthesia For Neurosurgery in Infants and Children: Barbara Van de Wiele, M.D. Los Angeles, CaliforniaKamel HadyNoch keine Bewertungen
- HydrocephalusDokument33 SeitenHydrocephalusRoselyn VelascoNoch keine Bewertungen
- Hydrocephalus AND Neural Tube DefectDokument7 SeitenHydrocephalus AND Neural Tube DefectTherese ArellanoNoch keine Bewertungen
- Hydrocephalus AND Neural Tube DefectDokument7 SeitenHydrocephalus AND Neural Tube DefectTherese ArellanoNoch keine Bewertungen
- Pedia Nursing Resource Unit - FinalDokument69 SeitenPedia Nursing Resource Unit - FinalDaryl Adrian RecaidoNoch keine Bewertungen
- HydrancephalyDokument3 SeitenHydrancephalyinammetNoch keine Bewertungen
- Choanal Atresia2Dokument40 SeitenChoanal Atresia2Mavina ReeNaNoch keine Bewertungen
- Spina Bifida Brochure 508compDokument20 SeitenSpina Bifida Brochure 508compfsaajaNoch keine Bewertungen
- EXPOSEEDokument9 SeitenEXPOSEEMind BlowerNoch keine Bewertungen
- EncehaDokument29 SeitenEncehaToko RaMy Line100% (1)
- Neural Tube DefectsDokument12 SeitenNeural Tube Defectsdaniel_1592Noch keine Bewertungen
- Hydro Cep Hal UsDokument11 SeitenHydro Cep Hal UsEmmanuel MukukaNoch keine Bewertungen
- HYDROCEPHALUSDokument63 SeitenHYDROCEPHALUSJohnsatish Rudrapogu50% (2)
- 415 1689 1 PB PDFDokument2 Seiten415 1689 1 PB PDFChandula SuriyapperumaNoch keine Bewertungen
- Cranial Ultrasound: DR Muhammad Jazib ShahidDokument43 SeitenCranial Ultrasound: DR Muhammad Jazib ShahidJazib ShahidNoch keine Bewertungen
- MyelodysplasiaDokument12 SeitenMyelodysplasiaJhon AlefeNoch keine Bewertungen
- Choanal Atresia2Dokument40 SeitenChoanal Atresia2pramod555Noch keine Bewertungen
- Bahan Ajar Iv Spina BifidaDokument7 SeitenBahan Ajar Iv Spina Bifidaanon_800290919Noch keine Bewertungen
- Neurogenic BladderDokument8 SeitenNeurogenic BladderrafendyfendyNoch keine Bewertungen
- Neural Tube Defects.Dokument34 SeitenNeural Tube Defects.ChosenNoch keine Bewertungen
- Spina BifidaDokument29 SeitenSpina Bifidaann dimcoNoch keine Bewertungen
- Musawi 29Dokument22 SeitenMusawi 29Full MarksNoch keine Bewertungen
- Journal of Diagnostic Medical Sonography 2010 Moore 286 9Dokument4 SeitenJournal of Diagnostic Medical Sonography 2010 Moore 286 9Hanarisha Putri AzkiaNoch keine Bewertungen
- PEDS Exam 2 - OutlineDokument67 SeitenPEDS Exam 2 - OutlineBonquisha OrgamiNoch keine Bewertungen
- DiscursoDokument21 SeitenDiscursoLeslye SimbañaNoch keine Bewertungen
- Congenital Malformations of The BrainDokument57 SeitenCongenital Malformations of The Brainmanisha paikarayNoch keine Bewertungen
- Hydrocephalus: Mira Octavionita Michael SalimDokument17 SeitenHydrocephalus: Mira Octavionita Michael SalimMichelle SalimNoch keine Bewertungen
- Espina Bifida 2022Dokument7 SeitenEspina Bifida 2022Edwin Fabian Paz UrbanoNoch keine Bewertungen
- DysrafismDokument44 SeitenDysrafismdeealoveadyNoch keine Bewertungen
- Hydrocephalus PresentationDokument49 SeitenHydrocephalus PresentationSourina BeraNoch keine Bewertungen
- Clinical AnophthalmosDokument46 SeitenClinical AnophthalmosYenyenAwoenDepranJuniorNoch keine Bewertungen
- 9th Week PediaDokument20 Seiten9th Week PediaaagNoch keine Bewertungen
- Fetal Ventriculomegaly: Postnatal Management: Special Annual IssueDokument3 SeitenFetal Ventriculomegaly: Postnatal Management: Special Annual IssueRendra Artha Ida BagusNoch keine Bewertungen
- 1 PBDokument7 Seiten1 PBsahrirNoch keine Bewertungen
- MedBack MyelomeningoceleDokument3 SeitenMedBack MyelomeningoceleJulia Rei Eroles IlaganNoch keine Bewertungen
- Ostrower Preauricular Cysts, Pits, and Fissures - Practice Essentials, Epidemiology, EtiologyDokument8 SeitenOstrower Preauricular Cysts, Pits, and Fissures - Practice Essentials, Epidemiology, EtiologyAndre HawkNoch keine Bewertungen
- Neuro Lo Week 1 - 1 DraftDokument15 SeitenNeuro Lo Week 1 - 1 DraftMarcellina AwingNoch keine Bewertungen
- The Myth of Autism: How a Misunderstood Epidemic Is Destroying Our ChildrenVon EverandThe Myth of Autism: How a Misunderstood Epidemic Is Destroying Our ChildrenBewertung: 2.5 von 5 Sternen2.5/5 (8)
- Disorders of the Spinal Cord in ChildrenVon EverandDisorders of the Spinal Cord in ChildrenMichael PikeNoch keine Bewertungen
- Degenerative Cervical Myelopathy: From Basic Science to Clinical PracticeVon EverandDegenerative Cervical Myelopathy: From Basic Science to Clinical PracticeMichael G. FehlingsNoch keine Bewertungen
- Anatomy and Pathophysiology of ProstrateDokument44 SeitenAnatomy and Pathophysiology of Prostraterajan kumar100% (3)
- Pathophysiology of TBI 97Dokument51 SeitenPathophysiology of TBI 97rajan kumarNoch keine Bewertungen
- Carcinoma Gall BladderDokument25 SeitenCarcinoma Gall Bladderrajan kumarNoch keine Bewertungen
- Oesophageal Atresia and Its ManagementDokument26 SeitenOesophageal Atresia and Its Managementrajan kumarNoch keine Bewertungen
- Adrenal and PheochromocytomaDokument86 SeitenAdrenal and Pheochromocytomarajan kumar100% (1)
- Current Role of Surgery in The Management of Peptic UlceDokument19 SeitenCurrent Role of Surgery in The Management of Peptic Ulcerajan kumarNoch keine Bewertungen
- HydrocephalusDokument33 SeitenHydrocephalusrajan kumar100% (2)
- Head Injury ManagementDokument11 SeitenHead Injury Managementrajan kumar100% (1)
- Prospects of Breast Reconstruction in LABCDokument22 SeitenProspects of Breast Reconstruction in LABCrajan kumarNoch keine Bewertungen
- Fluid Regulation Is Essential To HomeostasisDokument24 SeitenFluid Regulation Is Essential To Homeostasisrajan kumarNoch keine Bewertungen
- ETV PresentationDokument33 SeitenETV Presentationrajan kumarNoch keine Bewertungen
- Work Up of Gynecomastia (Slides)Dokument22 SeitenWork Up of Gynecomastia (Slides)rajan kumar67% (3)
- Abdominal Tbpresentation Diagnosis and Treatment NewDokument36 SeitenAbdominal Tbpresentation Diagnosis and Treatment Newrajan kumar100% (3)
- Management of The Hydrocephalus and OutcomeDokument24 SeitenManagement of The Hydrocephalus and Outcomerajan kumar100% (1)
- Scales of SedationDokument3 SeitenScales of Sedationrajan kumar100% (2)
- Shock N SepsisDokument98 SeitenShock N Sepsisrajan kumar100% (15)
- Ca PenisDokument25 SeitenCa Penisrajan kumar100% (2)
- Principles and Practice of GI EndosDokument101 SeitenPrinciples and Practice of GI Endosrajan kumar90% (21)
- Principles of CT Scan AbdomenDokument101 SeitenPrinciples of CT Scan Abdomenrajan kumar100% (16)
- Evaluation of Factors Influencing Morbidity and Mortality in Cases of Oesophageal Atresia And/or Tracheo-Oesophageal Fistula RepairDokument26 SeitenEvaluation of Factors Influencing Morbidity and Mortality in Cases of Oesophageal Atresia And/or Tracheo-Oesophageal Fistula Repairrajan kumarNoch keine Bewertungen
- Graves' Disease & PregnancyDokument19 SeitenGraves' Disease & Pregnancyrajan kumar100% (1)
- Abdominal Wall HerniaDokument21 SeitenAbdominal Wall Herniarajan kumar100% (1)
- Case Report of Hydatid Cyst in Thigh: - A Rare OccurrenceDokument5 SeitenCase Report of Hydatid Cyst in Thigh: - A Rare Occurrencerajan kumar100% (3)
- Unusual Case of Inter Muscular Hydatid CystDokument21 SeitenUnusual Case of Inter Muscular Hydatid Cystrajan kumar100% (3)
- NH Pressure UlcerDokument46 SeitenNH Pressure Ulcerrajan kumar100% (3)
- Approach To Thyroid NoduleDokument33 SeitenApproach To Thyroid Nodulerajan kumar100% (5)
- Mechanical Ventilation SeminarDokument82 SeitenMechanical Ventilation Seminarrajan kumar90% (21)
- Liver TransplantationDokument22 SeitenLiver Transplantationrajan kumar100% (6)
- Tracheo-Oesophageal FistulaDokument19 SeitenTracheo-Oesophageal Fistularajan kumar100% (3)
- HLR BasicsDokument13 SeitenHLR BasicsAyan Chakraborty75% (4)
- Lantus SoloStar Pen Guide PDFDokument7 SeitenLantus SoloStar Pen Guide PDFKai HarukaNoch keine Bewertungen
- A Letter To GodDokument9 SeitenA Letter To GodUjjwal ChoudharyNoch keine Bewertungen
- Two Steps From Hell Full Track ListDokument13 SeitenTwo Steps From Hell Full Track ListneijeskiNoch keine Bewertungen
- Artificial Neural NetworkDokument16 SeitenArtificial Neural NetworkSahil ChopraNoch keine Bewertungen
- Impulse: Operation ManualDokument8 SeitenImpulse: Operation ManualRonggo SukmoNoch keine Bewertungen
- Schedule Standard and Syllabus: Section A: Geomorphology and Remote SensingDokument6 SeitenSchedule Standard and Syllabus: Section A: Geomorphology and Remote SensingPankaj SharmaNoch keine Bewertungen
- The Effect of Carbon Black On The Oxidative Induction Time of Medium-Density PolyethyleneDokument8 SeitenThe Effect of Carbon Black On The Oxidative Induction Time of Medium-Density PolyethyleneMIRELLA BOERYNoch keine Bewertungen
- Cohort 2 Assignment Essay FinalDokument4 SeitenCohort 2 Assignment Essay Finalapi-652640066Noch keine Bewertungen
- A Translation Quality Assessment of Two English Translations of Nazım HikmetDokument14 SeitenA Translation Quality Assessment of Two English Translations of Nazım HikmetIntzarEltlNoch keine Bewertungen
- 2020-08-17 WITS - MECN 5005A - Systems MGMT - Lecture 2 of 8 - SharedDokument73 Seiten2020-08-17 WITS - MECN 5005A - Systems MGMT - Lecture 2 of 8 - SharedUnarine MutshinyaloNoch keine Bewertungen
- ViShNu-Virachita Rudra StotramDokument6 SeitenViShNu-Virachita Rudra StotramBhadraKaaliNoch keine Bewertungen
- Arup Kumar Mandal (New Format)Dokument2 SeitenArup Kumar Mandal (New Format)sharafat_321Noch keine Bewertungen
- Estoryang BinisayaDokument27 SeitenEstoryang BinisayaAngel GellaNoch keine Bewertungen
- Sampling TechniquesDokument96 SeitenSampling Techniquessixteen liquidoNoch keine Bewertungen
- Introduction and Assessment of The Renal - Urological SystemDokument182 SeitenIntroduction and Assessment of The Renal - Urological SystemValerie Suge-Michieka100% (1)
- THE STUDY OF THE TESTIMONIES. - No. 1. A Series Presented at The 1893 General Conference Session by ELDER J. N. LOUGHBOROUGHDokument16 SeitenTHE STUDY OF THE TESTIMONIES. - No. 1. A Series Presented at The 1893 General Conference Session by ELDER J. N. LOUGHBOROUGHKunedog1Noch keine Bewertungen
- Data ListDokument239 SeitenData Listpriyanka chithran100% (1)
- Las Grade 7Dokument16 SeitenLas Grade 7Badeth Ablao67% (3)
- Project Proposal - Hospital Management SystemDokument20 SeitenProject Proposal - Hospital Management SystemDilanka Liyanage95% (19)
- Dynamic Behavior of Closed-Loop Control Systems: 10.1 Block Diagram RepresentationDokument26 SeitenDynamic Behavior of Closed-Loop Control Systems: 10.1 Block Diagram Representationratan_nitNoch keine Bewertungen
- MultidisciplinaryDokument20 SeitenMultidisciplinaryrabiaNoch keine Bewertungen
- RCBC Capital Corporation Vs Banco de OroDokument18 SeitenRCBC Capital Corporation Vs Banco de OroLove HatredNoch keine Bewertungen
- A REPORT ON MIMO IN WIRELESS APPLICATIONS - FinalDokument11 SeitenA REPORT ON MIMO IN WIRELESS APPLICATIONS - FinalBha RathNoch keine Bewertungen
- Sandy Ishikawa DiagramDokument24 SeitenSandy Ishikawa DiagramjammusandyNoch keine Bewertungen
- Key Influence Factors For Ocean Freight Forwarders Selecting Container Shipping Lines Using The Revised Dematel ApproachDokument12 SeitenKey Influence Factors For Ocean Freight Forwarders Selecting Container Shipping Lines Using The Revised Dematel ApproachTanisha AgarwalNoch keine Bewertungen
- TaTa TeA Ad AnaLysiSDokument3 SeitenTaTa TeA Ad AnaLysiSAmiya RautNoch keine Bewertungen
- Music TherapyDokument13 SeitenMusic TherapyXavier KiranNoch keine Bewertungen
- Courtesy Begins at HomeDokument2 SeitenCourtesy Begins at Homell Snowitchy llNoch keine Bewertungen
- 6 Money SupplyDokument6 Seiten6 Money SupplySaroj LamichhaneNoch keine Bewertungen