Beruflich Dokumente
Kultur Dokumente
Lets Show Patients Their Mental Health Records
Hochgeladen von
api-251504806Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Lets Show Patients Their Mental Health Records
Hochgeladen von
api-251504806Copyright:
Verfügbare Formate
Opinion
A PIECE OF MY MIND
Michael W. Kahn, MD Department of Psychiatry, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, Massachusetts. Sigall K. Bell, MD Department of Medicine, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, Massachusetts. Jan Walker, RN, MBA Department of Medicine, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, Massachusetts. Tom Delbanco, MD Department of Medicine, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, Massachusetts.
Lets Show Patients Their Mental Health Records
Should we health professionals encourage patients with mental illness to read their medical record notes? As electronic medical records and secure online portals proliferate, patients are gaining ready access not only to laboratory findings but also to clinicians notes.1 Primary care patients report that reading their doctors notes brings many benefits including greater control over their health care, and their doctors experience surprisingly few changes in workflow. 2 While patients worry about electronic records and potential loss of privacy, they vote resoundingly for making their records more available to them and often to their families.3 As consumers urge that fully open medical records become the standard of care, policy makers, clinicians, and patients advocate also that mental illness gain far more attention and support.4 Primary care physicians and medical and surgical subspecialties have long managed many patients with mental illness, but with the exception of the Department of Veterans Affairs, most systems implementing open records continue to carve out from patients view behavioral health notes written by psychiatrists, psychologists, and social workers. We believe such exclusions are unnecessary. Inviting patients to read what clinicians write about their feelings, thoughts, and behaviors does seem different from sharing assessments of their hypertension or diabetes. Bringing transparency into mental health feels like entering a minefield, triggering clinicians worst fears about sharing notes with patients. How will a patient react to reading a diagnosis of his personality disorder? What about the patient with schizophrenia learning that her firm convictions are seen as delusional? Will outrage disrupt care as psychiatric diagnoses and terminology familiar to clinicians come across to patients as judgmental, dismissive, reductionist, or stigmatizing? Based on our experiences as psychiatric, medical specialty, and primary care clinicians, we suggest that transparency may instead yield fruitful opportunities. By writing notes useful to both patients and ourselves and then inviting them to read what we write, we may help patients address their mental health issues more actively and reduce the stigma they experience. Just as radiologists report a shadow on a chest film as a density rather than leap to diagnostic language, describing behaviors rather than labeling them could lead to less clinical prejudice, less diagnostic anchoring, and more engagement with patients. Descriptive language should not replace firm diagnoses, but rather complement the usual problem lists and medical terms to help balance and humanize notesand the patients they depict. As clinicians become accustomed to sharing notes with patients and describing clinical findings in ways that exemplify collaborative, nonjudgmental assessment, they might find their writing more efficient and to the point: Ms Jones and I continued our discussion of her tendency to use black-or-white-thinking in ways that make her relationships at work problematic. Mr Smith and I continue to agree to disagree about his conviction that his apartment is bugged. Ms Williams expressed dissatisfaction with my treatment decisions quite clearly, but preferred not to talk about that today. I encouraged her to discuss our disagreements in the future. This approachdescriptive, nonjudgmental summarizingcan help with documenting many potentially value-laden subjects. A patients addiction to Internet pornography may be deeply troubling, and his doctor or social worker would be justifiably worried about shaming him further by documenting it. This might be noted as Mr Martin and I continued our discussion of his addictive behavior and reviewed techniques for dealing with it. This principle can also be applied to a variety of sensitive topics, including psychodynamic issues. The medical record should offer a practical synopsis of a patients history and treatment, but it does not need to contain an exhaustive catalog of vulnerabilities. Caring for patients with substance abuse provides fertile ground for conflict, but here too reading the clinicians views in black and white may be helpful. Patients with addictions are often so used to being lectured that they tune out real-time discussions of harmful consequences of their behavior, no matter how tactful the clinician. Offering patients time for unpressured review of the clinicians assessment in a private setting may diminish the need for defensive maneuvers (such as evasiveness, minimization, or denial) that guard against feeling exposed and stigmatized, thereby affording the patient opportunity to get closer to acknowledging an addiction. Anecdotally, some doctors have commented that inviting their patients to see their problems in writing was far more effective in catalyzing behavior change than was discussing them. Deliberately highlighting patient strengths and achievements in notes is another strategy that may help many mental health patients. Virtually all individuals, including those with severe and persistent mental illnesses, have readily identifiable positive traits or accomplishments that can be concisely documented. While the brevity of office visits requires an efficient focus on symptoms and signs, clinicians can nevertheless document nonpathologic aspects of a patients life in a way that helps the patient profit from reading about his or her own strengthsas validated by the clinicianand gain a larger context for considering his or her illness. Ideally, the patient would see that his clinician knows theres more to me than my immediate worries. With both clinician and patient taking a more balanced and holistic perspecJAMA April 2, 2014 Volume 311, Number 13 1291
Corresponding Author: Michael W. Kahn, MD (mkahn @bidmc.harvard.edu). Section Editor: Roxanne K. Young, Associate Senior Editor. jama.com
Copyright 2014 American Medical Association. All rights reserved.
Downloaded From: http://jama.jamanetwork.com/ by a Self Regional Healthcare User on 04/02/2014
Opinion A Piece of My Mind
tive, the therapeutic alliance may be enhanced, even as the clinician addresses maladaptive behavior. Contrary to the fears of many cliniciansand perhaps mental health professionals in particularthe so-called difficult or personality-disordered patient might in fact benefit from more transparency. Many of these patients have some awareness that their behavior is troublesome, but a deep sense of shame inhibits their acknowledging it. Inviting them to read accurate and nonjudgmental notes may help diminish this shame. Even patients with severe personality disorders can be relieved to know that the turbulence and unhappiness that permeates their lives reflects suffering from a familiar clinical entity shared by others, rather than their being a bad person. A clinicians hesitation to reveal a note may largely reflect two questionable assumptions. The firstthat the note will in some way be devastating rather than comfortingoverlooks the fact that patients self-evaluations are often more negative than those of their clinicians. For example, an anxious patient may typically wonder whether he is crazy, but fears asking about it and getting an affirmative answer. In these cases, reading the note may actually reduce some worries that are fully operant but unwarranted. The second assumptionthat the patient will be unable to say I think you got something wrong and in fact be rightdiscounts the potentially enormous benefit arising from patients opportunity to factcheck their own histories. Indeed, the clinician who actively solicits
Conflict of Interest Disclosures: The authors have completed and submitted the ICMJE Form for the Disclosure of Potential Conflicts of Interest and none were reported. Funding/Support: This work is supported by a grant from the Robert Wood Johnson Foundation. Additional Contributions: Dr Kahn thanks Pamela Peck, PsyD, and Zsuzsanna Varhelyi, PhD, for helpful comments.
open and ongoing dialogue, including a patients opinion about a notes accuracy, may enhance both clinical precision and the treatment relationship. Benefits from this approach could extend to patients across the spectrum of mental disorders, including those with factitious illness, although admittedly no data are available currently to support this impression. But for some patients, reading notes may carry more risk than benefit. While HIPAA grants virtually all patients access to their records, a carefully considered decision to exclude a note from a patients view should remain an option when weighing harm and individualizing treatment. The opportunity to make such choices can also reduce clinicians anxiety as they become comfortable with a new approach to documentation. For the most part, however, our experience in primary care is that clinicians tend over time to withhold fewer and fewer notes. A psychologist colleague, initially skeptical about open records, changed her mind and developed a new perspective: When we think about our patients in a kind of language that we deem inappropriate or potentially offensive to the uninitiated, who is to say that our own attitudes toward our patients are not affected by that language? Wouldnt we be closer to our patients experience if we got into the habit of thinking about them in language they would find meaningful and useful? (Cassandra Cook, PhD, e-mail communication) We agree. Its time to offer fully transparent care to our patients with mental illness.
3. Vodicka E, Mejilla R, Leveille SG, et al. Online access to doctors notes: patient concerns about privacy. J Med Internet Res. 2013;15(9):e208. 4. Guest JA, Quincy L. Consumers gaining ground in health care. JAMA. 2013;310(18):1939-1940.
1. Walker J, Darer JD, Elmore JG, Delbanco T. The road toward fully transparent medical records. N Engl J Med. 2014;370(1):6-8. 2. Delbanco T, Walker J, Bell SK, et al. Inviting patients to read their doctors notes: a quasi-experimental study and a look ahead. Ann Intern Med. 2012;157(7):461-470.
1292
JAMA April 2, 2014 Volume 311, Number 13
jama.com
Copyright 2014 American Medical Association. All rights reserved.
Downloaded From: http://jama.jamanetwork.com/ by a Self Regional Healthcare User on 04/02/2014
Das könnte Ihnen auch gefallen
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- Toilet Train IntensiveDokument2 SeitenToilet Train IntensiveAnis KusnawatiNoch keine Bewertungen
- Bacalan DoDokument5 SeitenBacalan DoThalia Rhine AberteNoch keine Bewertungen
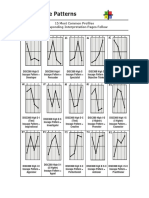
- Style Patterns: 15 Most Common Profiles Corresponding Interpretation Pages FollowDokument9 SeitenStyle Patterns: 15 Most Common Profiles Corresponding Interpretation Pages FollowantontansilNoch keine Bewertungen
- BA102 Lecture 1Dokument43 SeitenBA102 Lecture 1胡艺怀Noch keine Bewertungen
- Depression QuestionnaireDokument1 SeiteDepression QuestionnaireNurulIzzatiZainudinNoch keine Bewertungen
- Curriculum Map For Physical Education and Health 11Dokument11 SeitenCurriculum Map For Physical Education and Health 11CM Mykolot100% (1)
- Module11 130323045501 Phpapp02Dokument5 SeitenModule11 130323045501 Phpapp02jade tagabNoch keine Bewertungen
- Qualitative ResearchDokument22 SeitenQualitative ResearchTABBAL JAN PAOLONoch keine Bewertungen
- Reyes Et Al 2023Dokument21 SeitenReyes Et Al 2023Martin Radley Navarro-LunaNoch keine Bewertungen
- PETA1 TopicPoolDokument6 SeitenPETA1 TopicPoolRich BlancaflorNoch keine Bewertungen
- Ian E. Pagaran: Teacher 1Dokument11 SeitenIan E. Pagaran: Teacher 1Yanyan EducNoch keine Bewertungen
- Avolio - 2007 - Promoting More Integrative Strategies For Leadership Theory BuildingDokument9 SeitenAvolio - 2007 - Promoting More Integrative Strategies For Leadership Theory BuildingradufriteaNoch keine Bewertungen
- Stress TheoryDokument16 SeitenStress TheoryLeviNoch keine Bewertungen
- Elliot Niesta 2008 JPSPDokument16 SeitenElliot Niesta 2008 JPSPIqbal Hanun AziziNoch keine Bewertungen
- Background To The Functional Dimensions of Coping (FDC) ScaleDokument5 SeitenBackground To The Functional Dimensions of Coping (FDC) Scalejotajota10004950Noch keine Bewertungen
- Reflection On Interviews - DeseoDokument3 SeitenReflection On Interviews - DeseoRommel SarjNoch keine Bewertungen
- Everyday Optimism PP Guide Worksheets 2020Dokument22 SeitenEveryday Optimism PP Guide Worksheets 2020Nikita Jadhav100% (1)
- Addiction To PerfectionDokument4 SeitenAddiction To PerfectionBrontolina100% (1)
- Final Defense About Wearing Proper UniformDokument29 SeitenFinal Defense About Wearing Proper UniformAyessa Joy GarciaNoch keine Bewertungen
- Oct Unit Exam 2Dokument1 SeiteOct Unit Exam 2ESTHER DE FELIPENoch keine Bewertungen
- Law Wong Song (2004) JAPDokument14 SeitenLaw Wong Song (2004) JAPUmair ArshadNoch keine Bewertungen
- A Sample Format of Questionnaires On Career Planning and DevelopmentDokument2 SeitenA Sample Format of Questionnaires On Career Planning and DevelopmentSameer OmlesNoch keine Bewertungen
- Proposal Presentation DefenseDokument13 SeitenProposal Presentation DefenseElla AlabastroNoch keine Bewertungen
- Impacts of Online Games To Grade 11Dokument3 SeitenImpacts of Online Games To Grade 11Jenny Ann CerdeñaNoch keine Bewertungen
- Chapters 5 Guidance HUMANA NAJUDDokument4 SeitenChapters 5 Guidance HUMANA NAJUDTata Duero LachicaNoch keine Bewertungen
- 12 Ways To Combat Anxiety: Nix ThackrayDokument34 Seiten12 Ways To Combat Anxiety: Nix ThackrayOanaSirbuNoch keine Bewertungen
- GATTACA Student's WorksheetDokument3 SeitenGATTACA Student's WorksheetAngel Angeleri-priftis.Noch keine Bewertungen
- Week 9 Personal RelationshipDokument5 SeitenWeek 9 Personal RelationshipAbdelmar SusulanNoch keine Bewertungen
- Primal Leadership - The Hidden Driver of Great PerformanceDokument3 SeitenPrimal Leadership - The Hidden Driver of Great PerformanceRiyoHussainMNoch keine Bewertungen
- RockingtheboatassignmentDokument6 SeitenRockingtheboatassignmentapi-259701565Noch keine Bewertungen