Beruflich Dokumente
Kultur Dokumente
Pre Eclampsia Case Study
Hochgeladen von
Kaloy Kamao83%(12)83% fanden dieses Dokument nützlich (12 Abstimmungen)
11K Ansichten40 SeitenPre eclampsia case study hypertension pre hypertension drug study pathophysiology
Originaltitel
Pre Eclampsia case study
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenPre eclampsia case study hypertension pre hypertension drug study pathophysiology
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
83%(12)83% fanden dieses Dokument nützlich (12 Abstimmungen)
11K Ansichten40 SeitenPre Eclampsia Case Study
Hochgeladen von
Kaloy KamaoPre eclampsia case study hypertension pre hypertension drug study pathophysiology
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 40
Page | 1
Liceo de Cagayan University
College of Nursing
RN Pelaez Boulevard
Submitted as partial fulfillment for the requirements in
NCM102 RLE
A case study on
Chronic Hypertension with
Severe Superimposed Pre-Eclampsia
Submitted by:
Ezra Mae G. Ebisa
Anisa M. Usman
Carl Anthony Q. Parantar
Submitted to:
Mrs. Emma M. Dejarme, RN, MAN
January 8, 2014
Page | 2
CONTENTS
TABLE OF CONTENTS
I. INTRODUCTION 3
II. DATABASE AND HISTORY 6
III. NURSING SYSTEMS REVIEW CHART 7
IV. DEVELOPMENTAL DATA 18
V. MEDICAL MANAGEMENT 20
VI. PATHOPHYSIOLOGY 22
VII. DRUG STUDY 24
VIII. NURSING MANAGEMENT 27
IX. REFERRALS AND FOLLOW UP 38
X. EVALUATION AND IMPLICATIONS 38
XI. BIBLIOGRAPHY 39
Page | 3
I. INTRODUCTION
Overview of the Case
In the case of Mrs. Irene O. Cabasag, 39 years old from Tambaling 11, Bolobolo,
El Salvador, Misamis Oriental, she was admitted to Northern Mindanao Medical Center
(A2F1-OB-WARD 7 Service Ward - Bed 5) last December 6, 2013 at 7:00pm with a
chief complaint: 3 days prior to admission, patient had onset of headache associated
with dizziness and epigastric pain condition tolerated, no consult done. Her admission
diagnosis is: Pregnancy uterine, 31 5/7 weeks age of gestation, chronic hypertension
with superimposed preeclampsia severe, G2P1(1001). Her principal diagnosis is:
Pregnancy Uterine Pre Term, cephalic presentation delivered to a live premature baby
girl APGAR 9, BW 2.4kg, via Normal Spontaneous Vaginal Delivery.
What Is Chronic Hypertension?
There are 2 types of chronic hypertension: essential hypertension and secondary
hypertension. We do not know the cause of essential hypertension, but because
hypertension commonly runs in families, we know that genes are involved. A minority of
individuals has secondary hypertension, which means that the hypertension is
explained by another condition such as kidney disease, narrowing of the artery to the
kidney, and adrenal tumors. In many such cases, the hypertension will resolve after
treatment for the underlying problem. If you are undergoing evaluation for a secondary
form of hypertension, it is advisable to be treated for the underlying condition before
becoming pregnant. A third type of hypertension is called pregnancy-induced
hypertension. Some women develop new-onset hypertension in pregnancy, which can
present in the second half of pregnancy, usually in the third trimester.
What Are Some of the Complications of Chronic Hypertension During
Pregnancy?
Most women with chronic hypertension do well in pregnancy. In normal
pregnancy, blood pressure falls at the end of the first trimester and then increases to
pre-pregnancy values in the third trimester. For the majority of women with chronic
Page | 4
hypertension, blood pressure follows the same pattern. Some women, however,
experience a rise in blood pressure during pregnancy, which can increase their risk for
stroke and other complications and may therefore require more aggressive
antihypertensive treatment. A healthcare professional should monitor you to ensure that
a hypertension-related complication does not develop.
A more worrisome complication of chronic hypertension is the development of
superimposed preeclampsia. Preeclampsia is a serious condition that can affect many
organ systems and cause liver dysfunction, kidney failure, and an increase in bleeding
tendency, and at times it can progress to eclampsia seizures. Superimposed
preeclampsia is more likely to occur in women who have poorly controlled hypertension,
underlying renal disease, and diabetes mellitus. At present, there is no treatment for
preeclampsia except for delivery of the baby; therefore, babies of women who have this
condition are frequently born prematurely. Another complication of chronic hypertension
that may cause premature birth is placental abruption. An abruption is an early
separation of the placenta from the wall of the uterus, usually leading to strong
contractions, bleeding, and early delivery.
Objective
The objective of making this case study is to identify the problem of our patient and to
determine the factors that contribute to this kind of disease so that specific actions
should be done and rendered to our patient. The group has selected the patient having
this kind of disease because the primary concept that should fit our study is all about
abnormalities pertaining obstetric and gynecologic nursing. Having this kind of case
study is a privilege for us because it would be a good learning process by adding new
knowledge and concept about different kinds of diseases that may be present in some
patients. By making this case study we can identify the disease step by step, its nature
on how this disease occur, and nursing actions that would be appropriate for the patient.
Page | 5
SCOPE and LIMITATIONS of the STUDY
The study was conducted at Northern Mindanao Medical Center Delivery Room and OB
Ward, Cagayan de Oro City in which observation, analyzing and understanding the
patients condition was done. We were only given 24hours on understanding patients
problem. The study is also limited to the condition of the patient, which are chronic
hypertension with super imposed pre-eclampsia and its effect during pregnancy. The
study focuses only on obtaining the patients profile, health history and present health
condition; assessing, recording, and gathering of pertinent data about the patient.
Estimating the nursing needs and coping capacity of the patient. Finding the primary
health problems of the patient and the appropriate nursing interventions to solve the
condition of the patient. The objectives, nursing care plans, doctors order, and drug
study evaluation for the patient also done in this study.
Page | 6
II.DATA BASE AND HISTORY
Our Patient is Irene O. Cabasag, 39 years old married female form Tambaling
11, Bolobolo, El Salvador, Misamis Oriental. G2P1 with an LMP of May 28, 2013 and an
EDC of February 4, 2014. Her AOG is 31 5/7weeks and was admitted due to onset of
headache associated with dizziness and epigastric pain.
While at the Delivery Room her BP was fluctuating from 180/110 to 200/120 mmHg.
Patient Cabasag had her first child in 1997 with NSVD, few years after she developed
hypertension.
During her assessment in the labor room, her fundal height was 27cm. FHB was
taken and recorded at 160 BPM RUQ. Internal examination was done. The patient was
in active labor. In her ultrasound report, her diagnosis is:
Pregnancy Uterine, 29 weeks and 5 days by fetal biometry, singleton, live,
cephalic in presentation.
Postero-fundal placenta, grade II.
Adequate Amniotic Fluid
Estimated Fetal weight of 1651.22 grams
Her admitting diagnosis was Pregnancy uterine, 31 5/7 weeks age of gestation,
chronic hypertension with superimposed preeclampsia severe, G2P1 (1001)
She had previous NSVD delivery in 1997. Coughs and colds with few bouts were
also experienced with the date not specifically recalled. She takes OTC medications for
common ailments like biogesic for fever and alaxan for pain reliever.
Upon interview her hypertension started with her second pregnancy and upon
further investigation she had a heredo-familial history of hypertension on her mothers
side.
The physician in charge of Mrs. Cabasag is Dr. Brobo.
Page | 7
III. NURSING SYSTEM REVIEW CHART
Name of Patient: Irene O. Cabasag Date of Assessment: December 10, 2013
Body Measurements:
Weight: 67 Kg Height: 52
Vital Signs upon Assessment:
Temp: 37C PR: 106bpm RR: 24cpm BP: 160/100 mmHg
EENT
[ ] Impaired Vision [ ] Blind [ ] Pain
[ ] Reddened [ ] Drainage [ ] Gums
[ ] Impaired Hearing[ ] Deaf [ ] Burning
[X] Edema [ ] Lesions [ ] Teeth
Assess Eyes, Ears, Nose,
and throat for any abnormalities
[ ] No Problem
RESPIRATORY
[ ] Asymmetrical [X] Tachypnea[ ] Apnea
[ ] Rales [ ] Cough [ ] Barrel Chest
[ ] Bradypnea [ ] Shallow [ ] Rhonchi
[ ] Sputum [ ] Diminished[ ] Dyspnea
[ ] Orthopnea [ ] Labored [ ] Wheezing
[ ] Pain [ ] Cyanotic
Assess respiration, rate, rhythm, depth, pattern,
breath sounds, comfort
[X] No Problem
Facial Edema
Significant lower
extremities edema
BP 160/100
Proteinuria
Hyperreflexia
Epigastric Pain
Vaginal Bleeding
Tachycardia
Blurred Vision
Tachypnea
Episiotomy
Page | 8
CARDIOVASCULAR
[ ] Arrhythmia [X] Tachycardia [ ] Numbness
[ ] Diminished Pulse[ ] Edema [ ] Fatigue
[ ] Irregular [ ] Bradycardia [ ] Mur-mur
[ ] Tingling [ ] Absent Pulse [ ] Pain
Assess heart sounds, rate, rhythm, pulse, blood pressure,
circulation, fluid retention, comfort
[ ] No Problem
GASTROINTESTINAL
[ ] Obese [ ] Distension[ ] Mass
[ ] Dysphagia[ ] Rigidity [X] Pain
Assess abdomen, bowel habits, swallowing,
bowel sounds, Comfort.
[ ] No Problem
GENITO URINARY and GYNE
[X] Pain [X] Urine Color [X] Vaginal Bleeding
[ ] Hematuria [ ] Discharges [ ] Nocturia
Assess Urine frequency, control, color, odor, comfort, Gyne Bleeding,
Discharges
[ ] No Problem
NEUROLOGIC
[ ] Paralysis [ ] Stuporous [ ] Unsteady
[ ] Seizure [ ] Lethargic [ ] Comatose
[ ] Vertigo [ ] Tremors [X] Confused
[X] Vision [ ] Grip
Assess motor function, sensation, LOC, Strength, Grip, gait, coordination,
Speech
[ ] No Problem
Confused
Page | 9
MUSCULOSKELETAL and SKIN
[ ] Appliance [ ] Stiffness [ ] Itching
[ ] Petechiae [ ] Hot [ ] Drainage
[ ] Prosthesis[ ] Swelling [ ] Lesions
[ ] Poor Turgor[ ] Cool [ ] Deformity
[ ] Wound [ ] Rash [ ] Skin Color
[ ] Flushed [ ] Atrophy [ ] Pain
[ ] Echymosis [ ] Diaphoretic[ ] Moist
Assess mobility, motion gait, alignment, joint function, Skin color, texture, turgor,
integrity
[X] No Problem
Place an (X) in the area of abnormality. Comment at the space provided. Indicate the
location of the problem in the figure if appropriate, using (X).
Page | 10
NURSING ASSESSMENT II
SUBJECTIVE OBJECTIVE
COMMUNICATION:
[ ] Hearing Loss
[X] Visual Changes
[ ] Denied
Comments:
Ambot di ko ka
klaro. As
verbalized by the
client.
[ ] Glasses
[ ] Contact
Lens
[ ] Languages
[ ] Hearing Aide
[ ] Speech Difficulties
Pupil Size: R_3mm _ L _3mm__
Reaction: _PERRLA (Pupil Equally Round
& Reactive to Light Accommodation
OXYGENATION:
[ ] Dyspnea
[ ] Smoking History
__
_______________
[ ] Cough
[ ] Sputum
[X] Denied
Comments:
Dili man pud ko
gapaninigarilyo
ug di pud ko ga-
lisud bahin sa
pag-ginhawa.
As verbalized by
the client.
Respiration: [ ] Regular [X] Irregular
Describe:
Pt. has a condition of rapid
breathing (Tachypnea)
R: Symmetric to left; full chest
expansion
L: Symmetric to right; full chest
expansion
CIRCULATION:
[ ] Chest Pain
[X] Leg Pain
[X] Numbness of
__ extremities
[ ] Denied
Comments:
Gasakit dapit sa
akong tiyan og
akong tiil oi As
verbalized by
the client.
Heart Rhythm: [ ] Regular [X] Irregular
Ankle Edema: Patient has 1+ mild pitting,
slight indentation, no perceptible swelling of
the leg
Pulse Car Rad DP Fem*
Right + 106bpm + +
Left + 106bpm + +
Comments Pulses on both left and right
Page | 11
: are present and palpable
NUTRITION:
Diet: Low salt, Low fat
[ ] Dentures [X] None
Full Incomplete
With
Patient
Upper
X
Lower
X
[ ] N [ ] V
Character
_________________
[ ] Recent change in
weight, appetite
[ ] Swallowing
difficulty
[X] Denied
Comments:
dili man pud ko
kabati ug
kasukaon labi na
nuon sa
pagsuka. As
verbalized by the
client.
ELIMINATION:
Usual bowel pattern:
Thrice a day
[ ] Constipation
__ Remedy
Papaya
__ Date of last BM
Dec. 6, 2013
[ ] Diarrhea
__ Character
[ ] Urinary
Frequency
15 times/day
[ ] Urgency
[ ] Dysuria
[ ] Hematuria
[ ] Incontinence
[X] Polyuria
[ ] Foly in place
[ ] Denied
Comments:
No
abdominal
tenderness
upon
palpation.
Bowel sounds:
_normoactive 10 bowel sounds
per minute__
Abdominal Distention:
Present: [X]Yes [ ]No
Urine:
Color: Yellowish
Odor: Foully
Consistency:
MGT. OF HEALTH & ILLNESS:
[ ] Alcohol [X] Denied
__ Amount & Frequency
Dili sad koga-inom.as
verbalized by the client
SBE Last Pap
Smear:
Briefly describe the patients ability to follow
treatments (diet, meds, etc.) for chronic
problems (if present).
The patient is following the instructions that
is given to her and takes her medications
religiously.
Page | 12
LMP: May 28, 2013
SKIN INTEGRITY:
[ ] Dry
[ ] Itching
[ ] Other
[X] Denied
Comments:
ok ra man, dili
man ko gapangatol
. As verbalized by
the client.
[ ] Dry
[ ] Flushed
[ ] Moist
[X] Cold
[ ] Warm
[ ] Cyanotic
[ ] Pale
*Rashes, ulcers, decubitus (describe size,
*location, drainage):
No rashes, ulcers, or decubitus noted; striae
gravidarum & linea negra were observed.
ACTIVITY/SAFETY
:
[ ] Convulsion
[X] Dizziness
[X] Limited motion
of joints
Limitation in ability
to:
[X] Ambulate
[ ] Bathe Self
[ ] Other
[ ] Denied
Comments:
Kalipongon ko
molakaw. As
verbalized by the
client.
[ ] Level of Consciousness and Orientation
The client is awake and coherent
__ Gait: __ Walker __ Cane __ Other
__ Gait: __ Steady
__ Gait: _X_ Unsteady: _______________
[ ] Sensory and motor losses in face or
extremities:
No sensory and motor loses on face and
extremities noted.
[X] Range of Motion Limitations:
Client cannot move her legs well
[X] Facial Grimaces
[ ] Guarding
[X] Other Signs of Pain:
Page | 13
COMFORT/SLEEP/AWAKE:
Patient is complaining of epigastric
pain
[ ] Siderail release form signed (60+ years)
None (N/a)
[X] Pain
Location:
Pelvic region
Frequency:
8/10
Remedies:
Alaxan/Biogesic
[ ] Nocturia
[X] Sleep Difficulties
[ ] Denied
Comments:
Dili kayo ko
katulog tarong
sakit ako pus-on.
as verbalized by
the client.
COPING:
Occupation: Housewife
Members
of
household:
Husband and
children
Most
supportive
person:
Husband
Observe non-verbal behavior:
No eye contact during the assessment.
Patient was grouchy at the time of interview.
The person and his phone number that can
Be reached anytime:
Not on record
Page | 14
SPECIAL PATIENT INFORMATION (USE LEAD PENCIL)
Not Ordered Daily Weight Not Ordered PT/OT__________
Not Ordered BP q Shift Not Ordered Irradiation
Not Ordered Neuro VS 12/06/2013 Urine Test: Protein Trace
Not Ordered CVP/SG. Reading Not Ordered 24 hour Urine Collection
Date
ordered
Diagnostic/
Laboratory
Exams
Date Done Date
Ordered
I.V. Fluids/ Blood Date Disc.
11/06/2013 Ultrasound 11/06/2013 12/06/2013 D5LR 1L
@30gtts/min
12/07/2013
12/06/2013 Blood Chem 12/06/2013 12/07/2013 PNSS 1L + 40
mEq s KCl
@30gtts/min
12/07/13
12/06/2013 Urinalysis 12/06/2013 12/09/2013 D5LR 1L
@20gtts/min
Ongoing
12/08/2013 CBC 12/08/2013
LABORATORY TEST RESULT AND INTERPRETATION:
BLOOD COUNT RESULT:
Expected Values Unit Result Test
5.0 10.0 x10^3/uL 11.68 White Blood Cells
4.2 5.4 x10^6/uL 3.67 Red Blood Cells
12.0 16.0 g/dL 11.2 Hemoglobin
37.0 47.0 % 32.5 Hematocrit
9.0 16.0 fL 8.9 Platelet
Distribution Width
4.5 10.5 % 11.0 Monocyte
Page | 15
WHITE BLOOD CELL COUNT: is a blood test to measure the number of white blood
cells (WBCs).
- The white blood cell count of patient Cabasag was greater than the expected value
of or the normal value of white blood cell we have to our body.
- The white cell count (the number of cells in a given amount of blood) in someone
with an infection often is higher than usual because more WBCs are being produced or
are entering the bloodstream to battle the infection.
After the body has been challenged by some infections, lymphocytes "remember" how
to make the specific antibodies that will quickly attack the same germ if it enters the
body again.
RED BLOOD CELL COUNT: is a blood test that tells how many red blood cells (RBCs)
you have.
- The red blood cell count of patient Cabasag was less than the expected value of or
the normal value of red blood cell we have to our body.
- Red blood cells carry oxygen to all parts of your body. When your red blood cell (or
hemoglobin) count is low, parts of your body do not get enough oxygen to do their work.
This condition is called anemia and can make you feel very tired.
HEMOGLOBIN: is a protein in red blood cells that carries oxygen. A blood test can tell
how much hemoglobin you have in your blood.
- The hemoglobin of patient Cabasag was less than to the expected value or normal
result.
HEMATOCRIT: is a blood test that measures the percentage of the volume of whole
blood that is made up of red blood cells. This measurement depends on the number of
red blood cells and the size of red blood cells.
-The hematocrit of patient Cabasag was lesser than the expected value of a normal
result.
PDW COUNT: Platelet Distribution Width is an indication of variation in platelet size,
which can be a sign of active platelet release.
-The PDW of patient Cabasag was lesser than the expected value of a normal result.
Page | 16
MONOCYTE COUNT: This test measures the amount of monocytes in blood.
Monocytes are a type of white blood cell (WBC). This test is used to evaluate and
manage blood disorders, certain problems with the immune system, and cancers,
including monocytic leukemia. This test may also be used to evaluate for the risk of
complications after a heart attack.
-The monocyte of patient Cabasag was higher than the expected value of a normal
result.
URINALYSIS
Urine Test
A urine test checks different components of urine, a waste product made by
the kidneys. A regular urine test may be done to help find the cause of symptoms. The
test can give information about your health and problems you may have.
-The color of the urine of patient Cabasag was straw and the clarity was turbid, the
color of urine is affected to what she taking. The pH result was 6.0 it is an indication that
the body's fluids elsewhere are too acid, and it is working overtime to rid itself of an acid
medium. They have few epithelial cells, few bacteria and the calcium oxalate was rare
in her urine. If theirs bacteria, epithelial cells seen in the urine there was an infection.
The ALT(GPT) was in normal result, ASAT(SGOT) was in normal result,
Creatinine was in normal result, Blood in uric acid was in normal result. Patient
Cabasag has few bacteria in her urine it means she has an infection in her urine that will
lead to urinary tract infection.
Bacteria are common in urine specimens because of the abundant normal microbial
flora of the vagina or external urethral meatus and because of their ability to rapidly
multiply in urine standing at room temperature. Therefore, microbial organisms found in
all but the most scrupulously collected urines should be interpreted in view of clinical
symptoms.
Diagnosis of bacteriuria in a case of suspected urinary tract infection requires culture. A
colony count may also be done to see if significant numbers of bacteria are present.
Generally, more than 100,000/ml of one organism reflects significant bacteriuria.
Multiple organisms reflect contamination. However, the presence of any organism in
catheterized or suprapubic tap specimens should be considered significant.
Page | 17
ULTRA SOUND:
LMP: May 28, 2013 AOG: 23 weeks & 1 day EDC: February 4, 2014
No. of Fetuses: One
Presentation: Cephalic
FHB: 60 bpm
Amniotic Fluid Index: 13.5cm
Remarks:
Pregnancy Uterine, 29 weeks and 5 days by fetal biometry, singleton, live,
cephalic in presentation.
Postero-fundal placenta, grade II.
Adequate Amniotic Fluid
Estimated Fetal weight of 1651.22 grams
PLACENTA
Location: Postero-fundal
Grade: II
Distance from internal os
Page | 18
IV. DEVELOPMENTAL DATA
The term growth and development both refers to dynamic process. Often used
interchangeably, these terms have different meanings. Growth and development are
interdependent, interrelated process. Growth generally takes place during the first 20
years of life; development continues after that.
Growth:
1. Physical change and increase in size.
2. It can be measured quantitatively.
3. Indicators of growth include height, weight, bone size, and dentition.
4. Growth rates vary during different stages of growth and development.
5. The growth rate is rapid during the prenatal, neonatal, infancy and adolescent
stages and slows during childhood.
6. Physical growth is minimal during adulthood.
Development:
1. It is an increase in the complexity of function and skill progression.
2. It is the capacity and skill of a person to adapt to the environment.
3. Development is the behavioral aspect of growth.
Page | 19
Eriksons Stages of Psychosocial Development Theory
STAGE AGE CENTRAL
TASK
(+) RESOLUTION
(-) RESOLUTION
Young
Adulthood
18-40
y/o
Intimacy
vs.
isolation
Intimate
relationship with
another person.
Commitment to
work and
relationships.
Impersonal
relationships.
Avoidance of
relationship,
Career or lifestyle
commitments.
Intimacy vs. Isolation. Occurring in Young adulthood, we begin to share ourselves
more intimately with others. We explore relationships leading toward longer-term
commitments with someone other than a family member. Successful completion can
lead to comfortable relationships and a sense of commitment, safety, and care within a
relationship. Avoiding intimacy, fearing commitment and relationships can lead to
isolation, loneliness, and sometimes depression.
Havighursts Developmental Stage and Tasks
Adulthood - Selecting a mate
- Achieving a masculine or feminine social role
- Learning to live with a marriage partner
- Starting a family
- Rearing children
Page | 20
- Managing a home
- Getting started in an occupation
- Taking on civic responsibility
- Finding a congenial social group
It is the period of life to which they have looked forward during their adolescence and
early adulthood. And the time passes so quickly during these full and active middle
years that most people arrive at the end of middle age and the beginning of later
maturity with surprise and a sense of having finished the journey while they were still
preparing to commence it.
V. MEDICAL MANAGEMENT
December
06, 2013
7:00 PM
Admit to OB
TPR every 4 hours For further monitoring
Low salt and Low fat Diet To prevent hypertension
Laboratory Exams
Blood Chem, Urinalysis
Start IVF with D5LR 1 L @
30gtts/min
To replace lost fluids and
electrolytes
BP> 200/120 mmHg
Magnesium Sulfate 5gms deep
IM on alternate buttocks q6H x
4doses as maintenance dose
Anticonvulsant drug
RR 23cpm
FBC F14 attach, I and O q4
Hydralazine 5mg IVTT now
Methyldopa 250mg 1tab q8H
Antihypertensive drug for high blood
Treatment of sustained moderate to
severe hypertension
Page | 21
CBR with TP
Refer the BP if >160/100
Refer accordingly
December
07, 2013
7:10am Continue medication To maintain blood pressure
Monitor BP Served as baseline data
10:45am Follow-up other labs and refer For the doctor to see the result
Check vital signs every 4 hours To monitor the vital signs
FHB every 4 hours To monitor FHB
Change PNSS 1L + 40 mEq s KCl
@30gtts/min Source of water and electrolytes
3:00pm
Transport to OB-OPD clinic for
fetal heart assessment
To check for any abnormalities
Given hydralazine as prescribed Antihypertensive drug for high blood
8:00pm
May transport patient to OB-
OPD clinic for fetal heart rate
To check for any abnormalities
8:40pm FHT 152bpm Normal FHB
Hydralazine 5mg q15min
provide for DBP 110mmHg
Antihypertensive drug for high blood
December
08, 2013 Continue BP Measure for baseline information.
Continue Medication To improve patients condition.
Continue CBR with TP
December
09, 2013 Continue BP
8:00 am Continue Medication To improve patients condition.
Change IVF with D5LR 1 L @
20gtts/min
To replace lost fluids and
electrolytes
10:00 am For trans abdominal Ultrasound To diagnose pregnancy condition
especially the fetus condition
Continue monitoring V/S & FHB Monitor the V/S & FHB whether
every 4hrs. a good base line rate is present.
7:00 pm
May transport patient to Delivery
Room To prepare for delivery.
Page | 22
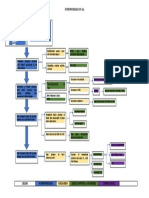
V. Pathophysiology
Predisposing
Factors:
Gender
Pregnant
Age
Heredity
Chronic Hypertension with
superimposed Preeclampsia
Precipitating Factors:
Stress
Sedentary
Lifestyle
Increase Systemic
Vascular Resistance
Increase Afterload
Decrease blood flow
to Organs
Blood Pressure
Juxtaglomerular
Cells
Renin
Angiotensin I
Angiotensinogen
Angiotensin II
Adrenal Cortex
stimulation II
Arteriolar Vasoconstriction
Increase Peripheral Resistance
Chronic Hypertension is characterized by either a BP 140/90
mmHg or greater before pregnancy or diagnosed before 20
weeks' gestation; Preeclampsia is characterized by a BP of
140/90 mm Hg or greater after 20 weeks' gestation
Increase
Aldosterone
Page | 23
Increase Blood
Pressure
After 20 weeks of
gestation
Increasing Blood
Pressure
Effects on Fetus
I. Premature Placental Aging
II. Decreased Placental Flow
and FGR
III. Fetal Hypotension and Low
Amniotic Fluid
IV. Increase Risk of Diseases
V. Placental Abruption
Page | 24
VI. DRUG STUDY
GENERIC
NAME OF
ORDERE
D DRUG
BRAN
D
NAME
DATE
ORDERE
D:
CLASSIF
ICATION
DOSE/FR
EQUENC
Y ROUTE
MECHANISM OF ACTION SPECIFIC
INDICATI
ON
CONTRAI
NDICATIO
N
SIDE
EFFECTS/TOXI
C EFFECTS
NURSING
PRECAUTION
Hydralaz
ine
Aprso
line
Decem
ber 6,
2013
antihyp
ertensiv
e
5mg
IVTT
It works by relaxing the
blood vessels so that
blood can flow more
easily through the
body. Hydralazine
apparently lowers
blood pressure by
exerting a peripheral
vasodilating effect
through a direct
relaxation of vascular
smooth muscle.
Hydralazine, by altering
cellular calcium
metabolism, interferes
with the calcium
movements within the
vascular smooth
muscle that are
responsible for
initiating or maintaining
the contractile state.
Treat-
ment of
severe
essentia
l hyper-
tension.
Patients
with
Coronar
y artery
disease;
mitral
valvular
rheumati
c heart
disease.
-flushing
(feeling of
warmth)
-headache
-upset
stomach
-vomiting
-loss of
appetite
-diarrhea
-constipation
-eye tearing
-stuffy nose
-rash
-in
pregnancy
(teratogenic)
-the nurse should
inform the patient
of possible side
effects and
advised to take
the medication
regularly and
continuously as
prescribed by the
doctor
-advised the
patient to avoid
alcohol because it
can make the
side effects from
hydralazine worse
-the nurse should
administer this
drug cautiously to
postpartum
patients with
advance renal
damage,
suspected
coronary artery
disease.
Page | 25
GENERIC
NAME OF
ORDERE
D DRUG
BRAN
D
NAME
DATE
ORDERE
D:
CLASSIF
ICATION
DOSE/FR
EQUENC
Y ROUTE
MECHANISM OF ACTION SPECIFIC
INDICATI
ON
CONTRAI
NDICATIO
N
SIDE
EFFECTS/TOXI
C EFFECTS
NURSING
PRECAUTION
Magnesi
um
Sulfate
Epso
m
Salt
Decem
ber 6,
2013
Anti-
convuls
ant
5gms
deep IM
on
alternate
buttocks
q6
4doses
as
mainten
ance
dose
Magnesium is the
second most plentiful
caution of the
intracellular fluids. It is
essential for the
activity of many
enzyme systems and
plays an important
role with regard to
neurochemical
transmission and
muscular excitability.
Magnesium sulfate
reduces striated
muscle contractions
and blocks peripheral
neuromuscular
transmission by
reducing acetylcholine
release at the
myoneural junction.
Additionally,
Indicate
d to
prevent
seizures
associat
ed with
pre-
eclamps
ia, and
for
control
of
seizures
with
eclamps
ia.
-
Patients
with
allergy
to
magnesi
um
products
; heart
block,
myocard
ial
damage;
hepatitis
-
CNS:
-Weakness,
dizziness,
fainting,
sweating
CV:
-Palpations
GI:
-Excessive
bowel
activity,
perianal
irritations
Metabolic:
-
Hypomagnes
aemia and
toxicity in
patients with
renal failure
-Reserve IV use
in eclampsia for
immediate life
threatening
situations
-Give IM route for
deep IM injection
of undiluted
(50%) solution
-Monitor serum
magnesium levels
during parenteral
therapy
-Monitor knee-jerk
reflex
-Do not give
magnesium
sulfate to patient
with abdominal
pain, nausea and
vomiting
Page | 26
Magnesium inhibits
Ca
2+
influx through
dihydropyridine-
sensitive, voltage-
dependent channels.
This accounts for
much of its relaxant
action on vascular
smooth muscle.
GENERIC
NAME OF
ORDERE
D DRUG
BRAN
D
NAME
DATE
ORDER
ED:
CLASSI
FICATI
ON
DOSE/F
REQUEN
CY
ROUTE
MECHANISM OF ACTION SPECIFI
C
INDICATI
ON
CONTRAIN
DICATION
SIDE
EFFECTS/TOXI
C EFFECTS
NURSING
PRECAUTION
Page | 27
Methyld
opa
Aldo
met
Dece
mber
6,
2013
Anti-
Hyper
tensiv
e
250mg
1tab
q8
Although the
mechanism of action
has yet to be
conclusively
demonstrated, the
antihypertensive effect
of Methyldopa probably
is due to its metabolism
to alpha-
methylnorepinephrine,
which then lowers
arterial pressure by
stimulation of central
inhibitory alpha-
adrenergic receptors,
false
neurotransmission,
and/or reduction of
plasma renin activity.
Methyldopa has been
shown to cause a net
reduction in the tissue
concentration of
serotonin, dopamine,
norepinephrine, and
epinephrine.
This
medica
tion is
used
alone
or with
other
medica
tions to
treat
high
blood
pressu
re
-
Patients
with
active
hepatic
disease
-History
of
methyld
opa-
associat
ed liver
dysfuncti
on
-
Drowsiness
-Headache
-Muscle
weakness
-Swollen
ankles or
feet
-Upset
stomach
-Vomiting
-Diarrhea
-Dry mouth
-
Tolerance may
occur, Monitor
hepatic
function,
- Discontinue
drug if fever,
abnormalities in
liver function
tests, or
jaundice occur.
- Discontinue if
edema
progresses or
signs of CHF
occur.
Page | 28
VII. NURSING MANAGEMENT
Ideal Nursing Interventions for Hypertension:
Nursing Diagnosis
Nursing Interventions
Rationale
Risk for decreased
cardiac
output related to
increased afterload,
vasoconstriction,
myocardial
ischemia, and
ventricular
hypertrophy.
1. Monitor blood
pressure, measure in
both arms/thighs three
times, use correct cuff
size and accurate
technique.
2. Note
dependent/general
edema.
3. Note presence, quality
of central and
peripheral pulses.
4. Observe skin color,
moisture, temperature,
and capillary refill time.
Comparison of pressures
provides a more
complete picture of
vascular
involvement/scope of
problem. Systolic
hypertension also is an
established risk factor for
cerebrovascular disease
and ischemic heart
disease, when diastolic
pressure is elevated.
May indicate heart
failure, renal or vascular
impairment.
Pulses in the legs/feet
may be diminished,
reflecting effects of
vasoconstriction
(increased systemic
vascular resistance
[SVR]) and venous
congestion.
Presence of pallor; cool,
moist skin; and delayed
capillary refill time may
be due to peripheral
vasoconstriction or reflect
cardiac decompensation
/ decreased output.
Page | 29
Nursing Diagnosis
Nursing Interventions
Rationale
Acute Pain
related to
increased
cerebral vascular
pressure.
1. Assess pain scale.
Determine specifics of pain,
e.g.,
location, characteristics.
2. Encourage bed rest during
acute phase.
3. Assist patient with
ambulation as needed.
4. Minimize vasoconstricting
activities that may
aggravate headache.
Helpful in evaluating
effectiveness of
therapy.
Minimizes
stimulation/promotes
relaxation.
Patient may also
experience episodes of
postural hypotension,
causing weakness
when ambulating.
Activities that increase
vasoconstriction
accentuate the
headache in the
presence of increased
cerebral vascular
pressure.
Page | 30
Nursing Diagnosis
Nursing Interventions
Rationale
Activity
Intolerance
related to
generalized
weakness,
imbalance
between
oxygen supply
and demand.
1. Instruct patient in
energy-conserving
techniques, e.g., using
chair when showering,
sitting to brush teeth or
comb hair, carrying out
activities at a slower
pace.
2. Encourage progressive
activity/self-care when
tolerated. Provide
assistance as needed.
Energy-saving techniques
reduce the energy
expenditure, thereby assisting
in equalization of oxygen
supply and demand.
Gradual activity progression
prevents a sudden increase in
cardiac workload. Providing
assistance only as needed
encourages independence in
performing activities.
Nursing
Diagnosis
Nursing Interventions
Rationale
Knowledge
deficit
related to
lack of
information
about the
disease
process
1. Define and specify the desired
blood pressure limits. Describe
hypertension and its effect on
the heart, blood vessels,
kidneys, and brain.
2. Assist patients in identifying the
risk factors that can be
modified, for example, obesity,
a diet high in sodium, saturated
fat, and cholesterol, sedentary
lifestyle, smoking, alcohol
consumption, and stress
lifestyle.
Provides a basis for
understanding blood
pressure elevation, and
describes commonly used
medical terms.
Understanding that high
blood pressure can occur
without symptoms is the
center allows patients to
continue treatment, even
when it feels good.
Risk factors that have
been shown to contribute
to hypertension and
cardiovascular and renal
disease.
Page | 31
Ideal Nursing Interventions for Preeclampsia:
Nursing Diagnosis
Nursing Interventions
Rationale
High risk of seizures in
pregnant women
related
to decreased organ
function (vasospasm
and increased blood
pressure).
1. Monitor blood
pressure every 4
hours.
2. Record the patient's
level of
consciousness.
3. Assess signs
of eclampsia (hyper
active, the patellar
reflexes,
decreased pulse and
respiration, epigastric
pain and oliguria).
4. Monitor for signs and
symptoms of labor or
uterine contractions.
5. Collaboration with the
medical team in the
provision of anti-
hypertension.
The pressure over 110
mmHg diastole and
systole 160 or more an
indication of PIH.
The decline of
consciousness as an
indication of decreased
cerebral blood flow.
The symptoms are a
manifestation of changes
in the brain, kidney, heart
and lung that precedes
seizure status.
Seizures will increase the
sensitivity of the uterus,
which will allow the
delivery.
Anti-hypertension to
lower blood pressure.
Page | 32
Nursing Diagnosis
Nursing Interventions
Rationale
High risk of fetal
distress related to
changes in the
placenta.
1. Monitor fetal heart
rate as indicated.
2. Review on fetal
growth.
3. Explain the signs of
solusio placenta
(abdominal pain,
bleeding, uterine
tension, decreased fe
tal activity).
4. Collaboration with the
medical ultrasound
and NST.
Increased fetal heart rate
as an indication of
hypoxia, premature and
solusio placenta.
Decrease in placental
function may be caused by
hypertension, causing
IUGR.
Pregnant women may
know the signs and
symptoms of solutio
placenta. Pregnant women
can learn from hypoxia in
the fetus.
Ultrasound and NST to a
known state / welfare of
the fetus.
Page | 33
Nursing Diagnosis
Nursing Interventions
Rationale
Impaired sense of
comfort (pain) related
to uterine contractions.
1. Assess the patient's
pain intensity level.
2. Explain the causes of
pain.
3. Help the pregnant
woman by rubbing /
massage on the
painful part.
The threshold of pain
everyone is different, thus
will be able to determine
appropriate action
treatment with the patient's
response to pain.
Pregnant women can
understand the causes of
pain.
To distract the patient.
Page | 34
NURSING CARE PLAN
Cues Nursing
Diagnosis
Objectives Nursing Interventions Rationale Evaluation
S: Sakit kaayo
akong tahi as
verbalized by the
patient
O: - Facial
Grimaces
- Rated Pain as
9 in a pain scale
of 1-10, 10 being
the highest
Acute Pain
related to
surgical incision
as evidenced by
facial mask of
pain
At the end of 1
hr. of nursing
care, the patient
will:
Identify and
use
appropriate
interventions
to manage
pain/discomfo
rt
Verbalize
lessening of
level of pain
Appear
relaxed, able
to sleep/rest
appropriately
Independent:
1. Reposition client,
reduce noxious
stimuli, and offer
comfort measures,
e.g. back rubs
2. Encourage use of
breathing and
relaxation techniques
and distraction
(stimulation of
cutaneous tissue)
3. Encourage adequate
rest period
4. Encourage early
ambulation
Dependent:
1. Administer
analgesics as
prescribed by the
doctor
Relaxes muscles,
and redirects
attention away
from painful
sensations
Promotes comfort,
and reduces
unpleasant
distractions,
enhancing sense
of well-being
To prevent fatigue
To prevent
pooling of blood
which prevents
blood clots
Promotes comfort,
which improves
psychological
status and
enhances mobility
After of 1 hr. of
nursing care,
the patient:
Identified and
used
appropriate
interventions
to manage
pain/discomfo
rt
Verbalized
lessening of
level of pain
Appeared
relaxed, able
to sleep/rest
appropriately
Page | 35
NURSING CARE PLAN
Cues Nursing
Diagnosis
Objectives Nursing Interventions Rationale Evaluation
S: Ga paspas
ang akong
kasing2x as
verbalized by the
patient.
O: - BP: 160/100
mmHg
- RR: 24cpm
- PR: 106bpm
- Lower
extremities
edema
Decreased
cardiac output
related to altered
heart rate
(106bpm), as
evidenced by
tachycardia and
increased blood
pressure,
patients report of
palpations; r/t
decreased
venous return as
evidenced by
lower extremities
edema, SOB
(24cpm)
At the end of 2
hr. of nursing
care, the patient
will display
hemodynamic
stability (heart
rate will
decrease from
106 bpm to 100
bpm, BP from
160/100 to
120/80)
Independent:
1. Keep client on bed
and in position of
comfort
2. Decrease stimuli;
provide quiet
environment
3. Encourage deep
breathing exercise
4. Encourage changing
positions slowly
5. Give information
about positive signs
of improvement
Dependent:
6. Administer
antihypertensive drug
as prescribed by the
doctor.
Decreases oxygen
consumption
To promote
adequate rest
To reduce anxiety
To reduce risk for
orthostatic
hypotension
To provide
encouragement
To treat
hypertension
After 2 hr. of
nursing care,
the patient was
able to display
hemodynamic
stability (heart
rate decreased
from 106 bpm
to 100 bpm, BP
from 160/100 to
(120/80)
Page | 36
NURSING CARE PLAN
Cues Nursing
Diagnosis
Objectives Nursing Interventions Rationale Evaluation
S:
O: - Post
surgical incision
Risk Factors
(Nanda)
Environmental
Factor
Decreased
tissue
perfusion
Decreased
wound healing
time
Risk for infection
related to post
surgical incision
After series of
nursing
interventions
the client
should:
Short Term
Identify the
risk factors
present in the
clients
condition
Clients partial
understanding
about infection
and its risk
factors
Long Term
Effective
prevention of
infection to the
client
Clients full
understanding
to the risk of
infection
Independent:
1. Teach patient to wash
hands often, especially
before toileting, before
meals and before and
after administering self-
care
2. Discuss to patients the
following signs of
infection -redness,
swelling, increased
pain, or purulent
drainage on the site
and fever
3. Demonstrate and allow
return demonstration of
wound care
4. Monitor vital signs
Dependent:
1. Administer antibiotics
as prescribed by the
doctor
Hand washing
reduces the risks for
infection
To impart to the
patient when the
wound become
infected and when to
sought medical care
To know if the
patient really
understand the
principle of proper
wound care
Temperature
elevation and
tachycardia may
reflect developing
sepsis
To prevent infection
After 30 min of
nursing
interventions,
client was able
to identify the
risk factors
present in her
condition, able
to gain
knowledge on
effective
prevention of
infection and
full
understanding
to the risk of
infection
Page | 37
Actual nursing management (DAR)
D
> Received Awake sitting on bed IVF of D5LR 1L
@ 900cc
level regulated @ 10 gtts/min
> BP= 160/100 FHB= 134
> 1+ mild pitting, slight indentation noted
A > Vital signs monitored and recorded
> On complete bed rest toilet privilege
> Kept on left lateral decubitus position
> Encouraged deep breathing exercise
> Advised to increase greens in diet like ampalaya
& malunggay leaves
> Encouraged to have adequate rest and sleep
> Health teachings imparted with emphasis on
a) Sodium restriction
b) Avoiding foods rich in oil and fats
c) Limiting daily activities and exercises
d) Proper nutrition
e) Compliance to medication
f) Proper hygiene
> Kept back dry
R > Able to rest well
> Endorsed with latest BP= 160/100
Page | 38
Discharge Plan:
Exercise
1. Encourage patients on deep breathing exercises.
2. Move extremities when lying.
3. Elevate the head part when sleeping, to promote increase peripheral circulation
4. Encourage overall passive and active exercises program during pregnancy to
prevent need for cesarean birth.
5. Exercises like tailor sitting, squatting, kegel exercise, pelvic rocking, and abdominal
muscle contraction will promote easy delivery.
Treatment:
1. Use of drugs
2. Catheterization
3. Obtaining labs. (CBC, platelets count, liver function, BUN and creatinine, and fibrin
degregation)
Health Teachings imparted with emphasis on:
1. Sodium restriction.
2. Avoiding foods rich in oil and fats.
3. Encourage patient to limit her daily activities and exercises.
Diet:
1. Low fats and sodium diet, restriction if possible.
2. High in protein, calcium and iron.
3. Adequate fluid intake
Sex:
1. Limit sexual activity
2. Sexual intercourse at 2nd trimester should be avoided.
Page | 39
VIII. REFERRALS AND FOLLOW-UP:
Instructed the client to come back one week after discharged for further follow-up
and evaluation of the clients health condition. This is very important so that the health
condition of the client will be evaluated if there is better improvement. The physician
should see and examine the physical appearance of the client.
IX: EVALUATION AND IMPLICATIONS:
This care study enables us to further our learning association with disease
condition of the patient. From it, we have gained knowledge in the progression of the
disease and the reaction of the body to maintain homeostasis and how eventually it
causes harm.
Through this, we actually improved our understanding and skills in the
management of the patient through the experiences weve had in implementing our
care. It also enhanced our confidence in intervening because of the input gained form
our research.
Case studies are a way of getting familiar or get acquainted not only with the
patient but also on his or her condition. It provides concrete examples of how the
theoretical knowledge learned during lectures was applied. How the concepts of the
various disease conditions were manifested through the client. It allows the opportunity
to facilitate the acquisition of knowledge through the experiences gained in
management and in caring for the patient. As a result, it is a must that case studies
should be made not just for requirement purposes but also for the pursuit of knowledge.
In general, the case study promoted learning through the research and actual
experiences and made us more knowledgeable in caring for the patient and that can
really be used in our chosen field.
Page | 40
X. Bibliography
120 Diseases (The essential Guide to more than 120 Medical Conditions,
syndromes, and diseases) by Prof. Peter Abrahams 2007 pp. 158
Essentials of pathophysiology by Carol Mattson Porth RN, MSN, PhD Pp.605-613
Manual of Nursing Practice by Lippincott 10
th
ed. Pp. 1201-1212
Maternal and child health nursing by Adele Pillitteri 5th edition; volume 1
page 426-433;page 329-332
WWW.MEDSCAPE.COM
WWW.WIKIPEDIA.ORG
http://nursingcrib.com
Das könnte Ihnen auch gefallen
- CP On Pre-EclampsiaDokument152 SeitenCP On Pre-Eclampsiakathy100% (2)
- pre-EClampsia Individual Case StudyDokument68 Seitenpre-EClampsia Individual Case Studycutekaize83% (18)
- Pregnancy Induced Hypertension Case StudyDokument77 SeitenPregnancy Induced Hypertension Case StudyJoe Anne Maniulit, MSN, RN84% (49)
- Nursing Care Management of a Client with Eclampsia: A Case StudyDokument72 SeitenNursing Care Management of a Client with Eclampsia: A Case StudyMauren Daza100% (4)
- Pre Eclampsia Case StudyDokument39 SeitenPre Eclampsia Case StudyAnton RossiniNoch keine Bewertungen
- Pre Eclampsia Case StudyDokument38 SeitenPre Eclampsia Case StudyFelmerPolancoRodaNoch keine Bewertungen
- Preeclampsia FinalDokument112 SeitenPreeclampsia FinalEarl John DayanghirangNoch keine Bewertungen
- Pre Eclampsia Nursing Care Plan by Maria Amabelles SorianoDokument39 SeitenPre Eclampsia Nursing Care Plan by Maria Amabelles SorianoLei Santillan0% (1)
- Severe PreeclampsiaDokument84 SeitenSevere PreeclampsiaJm Bernardo50% (2)
- CP Preeclampsia RevisedDokument32 SeitenCP Preeclampsia RevisedTessa Grace PugonNoch keine Bewertungen
- Nursing Management of Chronic Hypertension with Superimposed PreeclampsiaDokument40 SeitenNursing Management of Chronic Hypertension with Superimposed PreeclampsiaRaidis Pangilinan100% (2)
- Pre-eclampsia, (Pregnancy with Hypertension And Proteinuria) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandPre-eclampsia, (Pregnancy with Hypertension And Proteinuria) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Pre-Eclampsia: A Case StudyDokument49 SeitenPre-Eclampsia: A Case Studytinay85% (48)
- Case Presentation PreeclampsiaDokument41 SeitenCase Presentation PreeclampsiaJomari Zapanta50% (2)
- PreeclampsiaDokument58 SeitenPreeclampsiarhyanne100% (8)
- Case Study Pre-EclampsiaDokument51 SeitenCase Study Pre-EclampsiaRomelle Jane M. VelascoNoch keine Bewertungen
- Preeclampsia Case PresentationDokument26 SeitenPreeclampsia Case PresentationLohrhen Lheighh Cahreeniyow100% (2)
- CASESTUDY EclampsiaDokument39 SeitenCASESTUDY EclampsiayasiraNoch keine Bewertungen
- Vital Signs and Physical Exam FindingsDokument30 SeitenVital Signs and Physical Exam Findingssamangelo94Noch keine Bewertungen
- OLFU College of Nursing Case Study on Pregnancy HypertensionDokument32 SeitenOLFU College of Nursing Case Study on Pregnancy HypertensionOlivia Gianchand100% (9)
- Case Study PreEclampsiaDokument48 SeitenCase Study PreEclampsia1thea10% (2)
- PIH CASE FinalDokument35 SeitenPIH CASE FinalrJ67% (3)
- A Case Study PreeclampsiaDokument4 SeitenA Case Study PreeclampsiaJubaina DimacutaNoch keine Bewertungen
- Pregnancy Induced Hypertension: Eclampsia: Republic of The PhilippinesDokument62 SeitenPregnancy Induced Hypertension: Eclampsia: Republic of The PhilippinesKrisyll Meah Torred RamalNoch keine Bewertungen
- Angeles University Foundation Nursing Program Details Pregnancy HypertensionDokument31 SeitenAngeles University Foundation Nursing Program Details Pregnancy HypertensionMylene Angelie Bognot100% (2)
- Casestudy EclampsiaDokument40 SeitenCasestudy Eclampsiayasira100% (5)
- Case Study of Pregnancy Induced HypertensionDokument12 SeitenCase Study of Pregnancy Induced HypertensionJamaica Leslie Noveno100% (1)
- Case Study On Pre EclampsiaDokument28 SeitenCase Study On Pre EclampsiaVianca Louriele Lavarro100% (3)
- Placenta Previa Case StudyDokument59 SeitenPlacenta Previa Case Studyjuel_navarro88% (33)
- CP Placenta PreviaDokument95 SeitenCP Placenta Previakathy60% (5)
- PreeclampsiaDokument179 SeitenPreeclampsiaJohn Wilbert Birung100% (3)
- Case Study Placenta Previa This Is It 1Dokument71 SeitenCase Study Placenta Previa This Is It 1Homework Ping100% (1)
- Pih Case Study For PrintDokument17 SeitenPih Case Study For Printfoxrivergate100% (1)
- Pre EclampsiaDokument17 SeitenPre Eclampsiachristeenangela0% (1)
- Case Study (Preeclampsia)Dokument6 SeitenCase Study (Preeclampsia)Jobelle AcenaNoch keine Bewertungen
- Case Presentation On Pre-EclampsiaDokument18 SeitenCase Presentation On Pre-EclampsiaPabhat Kumar86% (7)
- Final Copy For Pre-EclampsiaDokument60 SeitenFinal Copy For Pre-EclampsiaSheena ClaireNoch keine Bewertungen
- A Case Study of Placenta PreviaDokument10 SeitenA Case Study of Placenta PreviaAdriane ComaNoch keine Bewertungen
- CaseDokument54 SeitenCaseRaja100% (4)
- Pregnancy Induced Hypertension Case StudyDokument75 SeitenPregnancy Induced Hypertension Case StudyJing CruzNoch keine Bewertungen
- In Partial Fulfillment of The Requirements in Care of Mother and Child and Adolescent 217 Related Learning ExperienceDokument28 SeitenIn Partial Fulfillment of The Requirements in Care of Mother and Child and Adolescent 217 Related Learning ExperienceAllyssa BunagNoch keine Bewertungen
- Placenta Previa Case StudyDokument7 SeitenPlacenta Previa Case StudyphearlieNoch keine Bewertungen
- Case Study (Placenta Previa)Dokument18 SeitenCase Study (Placenta Previa)Jai - Ho80% (30)
- Pre-eclampsia Case StudyDokument31 SeitenPre-eclampsia Case StudyRajaNoch keine Bewertungen
- Fluid Volume Excess Nursing Care PlanDokument1 SeiteFluid Volume Excess Nursing Care PlanMonica Cruz Dalida74% (23)
- Case Study (Aub)Dokument16 SeitenCase Study (Aub)Lucila Lugo0% (2)
- Postpartum Discharge PlanDokument3 SeitenPostpartum Discharge PlanCassey CamamaNoch keine Bewertungen
- Case StudyDokument19 SeitenCase Studywella goNoch keine Bewertungen
- Case Study On Pregnancy Induced Hypertension (PIH) : University of Northern Philippines College of NursingDokument42 SeitenCase Study On Pregnancy Induced Hypertension (PIH) : University of Northern Philippines College of Nursing3B NOVIDA, ALEYA G.Noch keine Bewertungen
- Preeclampsia, Severe, UncontrolledDokument22 SeitenPreeclampsia, Severe, UncontrolledLharra Cagulada-PostranoNoch keine Bewertungen
- Corrections INP CASE STUDYDokument59 SeitenCorrections INP CASE STUDYNoveeNoch keine Bewertungen
- Inp Case StudyDokument58 SeitenInp Case StudyNoveeNoch keine Bewertungen
- University of Northern Philippines: Republic of The Philippines Tamag, Vigan City, Ilocos SurDokument26 SeitenUniversity of Northern Philippines: Republic of The Philippines Tamag, Vigan City, Ilocos Surneo quartoNoch keine Bewertungen
- Thesis On Pregnancy Induced HypertensionDokument8 SeitenThesis On Pregnancy Induced Hypertensionalisonhallsaltlakecity100% (2)
- PREECLAMPSIADokument60 SeitenPREECLAMPSIAMary Grace MasNoch keine Bewertungen
- NSVD Case Study: Normal Spontaneous Vaginal DeliveryDokument29 SeitenNSVD Case Study: Normal Spontaneous Vaginal DeliveryKimberly Anne SP Padilla82% (11)
- Case Based Discussion KB PH, MSDokument8 SeitenCase Based Discussion KB PH, MSRaziNoch keine Bewertungen
- I Sack oDokument10 SeitenI Sack oisacksotiNoch keine Bewertungen
- Nursing Care for Abruption PlacentaDokument6 SeitenNursing Care for Abruption PlacentaKrizzia Angela BacotocNoch keine Bewertungen
- Gestational Diabetes Mellitus Induction at 40 WeeksDokument12 SeitenGestational Diabetes Mellitus Induction at 40 WeeksAiman ArifinNoch keine Bewertungen
- Health TeachingsDokument1 SeiteHealth TeachingsKaloy KamaoNoch keine Bewertungen
- ProQuestDocuments 2016-01-08Dokument7 SeitenProQuestDocuments 2016-01-08Kaloy KamaoNoch keine Bewertungen
- Nursing Care PlansDokument2 SeitenNursing Care PlansKaloy KamaoNoch keine Bewertungen
- Location and Pictures of Different Organs in The AbdomenDokument13 SeitenLocation and Pictures of Different Organs in The AbdomenKaloy KamaoNoch keine Bewertungen
- Penetrating Injuries To The Liver or Spleen - Care GuideDokument4 SeitenPenetrating Injuries To The Liver or Spleen - Care GuideKaloy KamaoNoch keine Bewertungen
- Laboratory ResultsDokument1 SeiteLaboratory ResultsKaloy KamaoNoch keine Bewertungen
- Motorcycle Rider Risk ManagementDokument3 SeitenMotorcycle Rider Risk ManagementKaloy KamaoNoch keine Bewertungen
- Pathophysiology 3Dokument10 SeitenPathophysiology 3Kaloy KamaoNoch keine Bewertungen
- IvtttDokument1 SeiteIvtttBobot Julius OropezaNoch keine Bewertungen
- Injury Severity ScoringDokument12 SeitenInjury Severity ScoringJavier del MattoNoch keine Bewertungen
- Motorcycle Rider Risk ManagementDokument3 SeitenMotorcycle Rider Risk ManagementKaloy KamaoNoch keine Bewertungen
- Nursing Care PlansDokument2 SeitenNursing Care PlansKaloy KamaoNoch keine Bewertungen
- Paramedic Care: Principles & Practice Trauma EmergenciesDokument61 SeitenParamedic Care: Principles & Practice Trauma EmergenciesKaloy KamaoNoch keine Bewertungen
- Penetrating Injuries To The Liver or Spleen - Care GuideDokument4 SeitenPenetrating Injuries To The Liver or Spleen - Care GuideKaloy KamaoNoch keine Bewertungen
- Location and Pictures of Different Organs in The AbdomenDokument13 SeitenLocation and Pictures of Different Organs in The AbdomenKaloy KamaoNoch keine Bewertungen
- Pain ManagementDokument19 SeitenPain ManagementKaloy KamaoNoch keine Bewertungen
- Health TeachingsDokument1 SeiteHealth TeachingsKaloy KamaoNoch keine Bewertungen
- Doctor's Order SheetDokument2 SeitenDoctor's Order SheetKaloy KamaoNoch keine Bewertungen
- Transverse Myelitis and Vaccines - A Multi-AnalysisDokument8 SeitenTransverse Myelitis and Vaccines - A Multi-AnalysisKaloy KamaoNoch keine Bewertungen
- Management of Hydrocephalus in Patients With Tuberculous MeningitisDokument11 SeitenManagement of Hydrocephalus in Patients With Tuberculous MeningitisKaloy KamaoNoch keine Bewertungen
- Nutrition: Your Role in Promoting ProperDokument11 SeitenNutrition: Your Role in Promoting ProperKaloy KamaoNoch keine Bewertungen
- Occupational Nursing CHN Ward ClassDokument2 SeitenOccupational Nursing CHN Ward ClassKaloy KamaoNoch keine Bewertungen
- Nursing Management in The Local Public Health SystemDokument33 SeitenNursing Management in The Local Public Health SystemKaloy KamaoNoch keine Bewertungen
- Group 2 Lesson Plan HandwashingDokument8 SeitenGroup 2 Lesson Plan HandwashingKaloy KamaoNoch keine Bewertungen
- Management of Pain - Non-Pharmacological Management - Nursing Best Practice GuidelinesDokument2 SeitenManagement of Pain - Non-Pharmacological Management - Nursing Best Practice GuidelinesKaloy KamaoNoch keine Bewertungen
- Management of Pain - Non-Pharmacological Management - Nursing Best Practice GuidelinesDokument2 SeitenManagement of Pain - Non-Pharmacological Management - Nursing Best Practice GuidelinesKaloy KamaoNoch keine Bewertungen
- Mapping The Literature of Public Health and Community NursingDokument4 SeitenMapping The Literature of Public Health and Community NursingKaloy KamaoNoch keine Bewertungen
- CHN Ward ClassDokument1 SeiteCHN Ward ClassKaloy KamaoNoch keine Bewertungen
- Prevention CHN Ward ClassDokument2 SeitenPrevention CHN Ward ClassKaloy KamaoNoch keine Bewertungen
- Transverse MyelitisDokument7 SeitenTransverse MyelitisKaloy KamaoNoch keine Bewertungen
- Interpretation of Histograms and Peripheral Smear FindingsDokument5 SeitenInterpretation of Histograms and Peripheral Smear FindingsrezqiNoch keine Bewertungen
- Filipino Widow's Medical CaseDokument30 SeitenFilipino Widow's Medical Casereginebenedicte100% (1)
- Phlebotomy Study SheetsDokument50 SeitenPhlebotomy Study SheetsJona Aure100% (4)
- Medical Terminology Blood Lymph SystemsDokument29 SeitenMedical Terminology Blood Lymph Systemsapi-268199514100% (1)
- Internship Log: Zahra Khan Learns Phlebotomy SkillsDokument2 SeitenInternship Log: Zahra Khan Learns Phlebotomy SkillsGhina YazbekNoch keine Bewertungen
- LABSSDokument5 SeitenLABSSJohn BretanaNoch keine Bewertungen
- Intervalle de Référence Hémogramme GhanaDokument13 SeitenIntervalle de Référence Hémogramme GhanaMARTELOTNoch keine Bewertungen
- Lesson Plan PatternDokument11 SeitenLesson Plan PatternFenina S. Calma100% (2)
- Hema RecallDokument11 SeitenHema Recallmkct111100% (1)
- Handling and Processing of Blood Specimens For Laboratory TestingDokument32 SeitenHandling and Processing of Blood Specimens For Laboratory TestingNajibah A. CasimNoch keine Bewertungen
- Maria 0001Dokument1 SeiteMaria 0001Irene Hail GingoyonNoch keine Bewertungen
- General Concepts and Administrative IssuesDokument52 SeitenGeneral Concepts and Administrative IssuesJOHN CARLO YADAONoch keine Bewertungen
- Oxymetholone Therapy: in Aplastic AnemiaDokument8 SeitenOxymetholone Therapy: in Aplastic AnemiaUrsus BarriosNoch keine Bewertungen
- Toxicological Safety Evaluation of Pasteurized: Akkermansia MuciniphilaDokument15 SeitenToxicological Safety Evaluation of Pasteurized: Akkermansia MuciniphilaalzennNoch keine Bewertungen
- Pathophysiology of AllDokument1 SeitePathophysiology of AllBGHMC PEDIAHONoch keine Bewertungen
- Accelerating Commercialization Cost Saving Health Technologies ReportDokument25 SeitenAccelerating Commercialization Cost Saving Health Technologies ReportBrazil offshore jobsNoch keine Bewertungen
- Typhoid Test ReportDokument4 SeitenTyphoid Test ReportDEEPAK DubeyNoch keine Bewertungen
- L34 - MR - Nilesh Yadav - Kota CC 6 RAY-99/100, Bajrang Nagar Main Road, Near Bright Land School, Kota-324001Dokument11 SeitenL34 - MR - Nilesh Yadav - Kota CC 6 RAY-99/100, Bajrang Nagar Main Road, Near Bright Land School, Kota-324001Shivam MittalNoch keine Bewertungen
- Dengue Fever Case StudyDokument15 SeitenDengue Fever Case StudyJeLai Lozano AbeciaNoch keine Bewertungen
- 01 Guidelines For Creating TPN OrdersDokument6 Seiten01 Guidelines For Creating TPN OrdersMohammedNoch keine Bewertungen
- Diagnostics Test ReportDokument5 SeitenDiagnostics Test Reportrakesh_danduNoch keine Bewertungen
- Veterinary Clinical PathologyDokument15 SeitenVeterinary Clinical Pathologypand00raNoch keine Bewertungen
- Blood Transfusion PDFDokument20 SeitenBlood Transfusion PDFalaamorsyNoch keine Bewertungen
- VETSCAN HM5 Operator - S Manual ABX 00248Dokument164 SeitenVETSCAN HM5 Operator - S Manual ABX 00248Moisés RodríguezNoch keine Bewertungen
- Introduction To Medtech NotesDokument44 SeitenIntroduction To Medtech NotesJanelle RemorozaNoch keine Bewertungen
- Urinalysis, Fecalysis, & Complete Blood Count: NCM 112 Rle Ward ClassDokument14 SeitenUrinalysis, Fecalysis, & Complete Blood Count: NCM 112 Rle Ward ClassJabber PaudacNoch keine Bewertungen
- Aldomet: (Methyldopa)Dokument6 SeitenAldomet: (Methyldopa)Riska AuliahNoch keine Bewertungen
- Technical Document Medonic M-Series M32 Hematology Analyzer: Product Name ManufacturerDokument18 SeitenTechnical Document Medonic M-Series M32 Hematology Analyzer: Product Name ManufacturerGiovanni BalderramaNoch keine Bewertungen
- Int J Lab Hematology - 2021 - Feriel - Effects of Circadian Variation Lifestyle and Environment On HematoloDokument10 SeitenInt J Lab Hematology - 2021 - Feriel - Effects of Circadian Variation Lifestyle and Environment On HematoloPaul Avelino CallupeNoch keine Bewertungen
- XS 1000i Operators Instructions PDFDokument238 SeitenXS 1000i Operators Instructions PDFmihai2007750% (2)