Beruflich Dokumente
Kultur Dokumente
Hip Dislocation Research
Hochgeladen von
api-2688390110 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
131 Ansichten8 SeitenOriginaltitel
hip dislocation research
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
131 Ansichten8 SeitenHip Dislocation Research
Hochgeladen von
api-268839011Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 8
Candace Perkins MSAT 6500
A hip dislocation can be a very painful experience and is considered a medical
emergency. The dislocation either happens anterior or posterior in the joint.
Most of these types
of injuries will happen with high impact sports or direct trauma to the area.
1
Although very
painful events, hip dislocations are not very common because the hip is a stable joint.
5
But with
right timing and right position this event can happen. Patients need to be carefully examined to
rule out other pathologies to other joints. Patient education is highly recommended when these
injuries occur due to possible surgery and rehab.
12
The hip has many structures that can be
damaged in this injury.
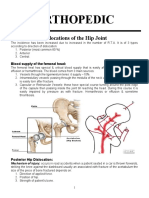
The hip joint is what is called a ball-and-socket joint because of the way the femoral head
and acetabulum articulate, the femoral head represents the ball and the acetabulum represents the
socket where the ball sits in the joint.
3
There are five ligaments that help keep the femoral head in
the acetabulum: the illiofemoral ligament, pubofemoral ligament, ischiofemoral ligament,
transverse acetabelar ligament, and the femoral head ligament. The ischiofemoral ligament is
posterior and the illiofemoral ligament is anterior. These ligaments form a capsule around this
joint. This capsule is thick due to how deep the socket is and the musculature and ligaments
surrounding it, which is a reason dislocations are uncommon.
12
The sciatic nerve and femoral
nerve also lie close to the joint.
1
A hip dislocation can be anterior or posterior.
Hip dislocations are mainly caused by axial loading and common with impact in mostly
motor-vehicle accidents.
12
A dislocation depends on the magnitude of the forces involved at
impact of the injury. In a hip dislocation, the leg affected can have a shortened appearance
compared to the opposite limb.
13
An anterior inferior hip dislocation occurs with forced
abduction, external rotation, and flexion of the femur. The femoral head then ruptures through
Candace Perkins MSAT 6500
the joint capsule. An anterior superior hip dislocation is similar to an inferior dislocation. The
superior dislocation is caused by forced abduction, external rotation, and extension of the femur.
4
Posterior hip dislocations occur when the femur is adducted and flexed during time of
event.
6
About 85-90% of dislocations are posterior.
12
Also with a posterior hip dislocation, a
femoral neck fracture can occur. This is an uncommon occurrence but this can sometimes lead
to surgical replacement or salvage of the femoral head.
7
Dislocations can also happen after a
Total Hip Replacement(THR).
After a patient goes through a THR or Total Hip Arthroplasty (THR), the patient can
experience a hip dislocation. It remains a major problem and can also have a negative effect on
the patients quality of life after this surgery.
9
THR dislocation occurs with getting out of bed,
putting socks and shoes on , and going to the restroom when sitting and standing. Activities that
have less affect on dislocation are getting into and out of a bath or shower, and twisting and
turning in a crouched position.
2
Although many studies have been done, many questions still
remain as to why this occurs. What has been shown to help with these dislocations are the use of
dual-mobility cups. Using these cups have shown promising results in stopping dislocations
from happening after THR.
9
There can be many risk factors when dealing with hip dislocations.
Risks after dislocating a hip can be drastic. Long term disability, chronic pain, and
limited use can all occur with this injury. Also, long-term gait problems occur in about 16% of
patients with a hip dislocation. An injury to the sciatic nerve can occur as well. This can happen
with the femoral head stretching or a bony landmark tearing the nerve. Another risk factor is
arthritis to the joint. Posttraumatic arthritis is a more common long-term condition following
this injury.
8
Other injuries can occur to other joints near the hip. Injuries to the patella and knee
Candace Perkins MSAT 6500
joint, ankle, and foot joints are common injury sites for a dislocated hip.
12
The epidemiology for
this injury mainly happen in high impact events.
About 70% of hip dislocations happen in motor vehicle accidents. There is very little
documentation of hip dislocations in sporting events, however, American football, rugby,
snowboarding, gymnastics, and professional basketball seem to be the sports that do have some
documentation of hip dislocations occurring.
1
During these sporting events the hip joint can enter
a vulnerable stance and can be susceptible to dislocations. Age and gender have also been
looked at with hip dislocations.
Major trauma hip dislocations are more common in the ages of 35 years or younger due
to high-energy activities. In ages 65 years or older, the main cause of hip dislocations are falls.
8
A major problem in the elderly population is a displaced femoral neck fracture, which can be a
type of hip dislocation.
11
Age for THR patients had no impact on the occurring dislocations, but it
was shown that females are less likely than males to have hip dislocations following a THR.
9
In
infants, hip dislocations can occur called hip Developmental Dysplasia of the Hip (DDH).
Opposite from THR, females are more susceptible than males to be diagnosed with DDH.
10
The
occurrence of DDH in infants is 2-4 births in every 1000 births.
Gender plays a role in a general
hip dislocation. These injuries commonly happen to males more than females also due to the
high risk activities they partake in.
8
Detection of hip dislocations should be caught early.
When trying to detect a hip dislocation the patient usually will be in some painful
discomfort and will not be able to move their lower extremity. The hip will appear to be in a
flexed position along with some internal rotation and adduction. Need to test for the sciatic and
femoral nerve at the site of dislocation; these can be damaged in this injury. Also check for
Candace Perkins MSAT 6500
femur fractures as well as some knee pathologies. X-rays are a good tool to use when
diagnosing a hip dislocation and are often used before treatment and after treatment.
12
Classification and treatment for this injury is essential.
The direction of the injury is one of the first observations a physician, athletic
trainer, therapist, etc. should take note of. The Thompson-Epstein and the Stewart-Milford
classification systems are the two systems that are commonly used. Each systems have different
types of dislocations. In the Stewart-Milford has four types. Type I is a simple dislocation with
no fracture involved, type II is a dislocation with one or more fragments but has stability after
reduction, type III is a dislocation with a fracture producing a gross deformity, and type IV is a
dislocation with a fracture of the femoral head and/or neck.
12
The Thompson-Epstein system has
an anterior system and a posterior system.
The anterior Thompson-Epstein system has many different types. Type I are superior
dislocations, type IA has no fractures included in the dislocation, type IB as a fracture included
or an impaction of the head of the femur, type IC has a fracture in the acetabullum. Type II is an
inferior dislocation, type IIA-C has the same classifications as type IA-C.
12
The Posterior Thompson-Epstein system has five types. Type I is a dislocation with no
fractures, type II has a large posterior wall fragment, type III has many posterior fragments, type
IV adds a fracture in the acetabular floor, and type V adds a fracture in the head of the
femur.
12
With these classifications, treatments can be adjusted.
Immediate reduction of the femoral head is essential in most cases of hip dislocations.
Reduction can be obtained with the patient in the supine position with in-line traction,
immediately followed by force being applied to the opposing vector on the injury. To help
Candace Perkins MSAT 6500
muscles not to spasm, the traction should be applied in a steady manner.
12
In more serious cases
with femoral neck fractures and acetabular fractures occuring, these should be treated as surgical
emergencies and need immediate open reduction should be performed.
12
Delayed start to
reduction in the combined dislocation and fracture can negatively affect the prognosis due to
degenerative arthritis or avascular necrosis. Even though hip dislocations are rare for athletics,
athletic trainers, emergency responders, and therapists should have the knowledge of treatment
and management of these injuries.
13
Rehab for these injuries should include strength exercises to
the surrounding musculature.
12
There should be short term and long term goals during the rehab
for the patient. Short term goals should include, but not limited to, hip and knee range of motion
increased and pain decreased. Long term goals should include, but are not limited to, increase
strength or return to original strength and return to normal gait. Gait training should start within
the first session of rehab. The athlete should be able to perform functional testing exceptionally
to return to play.
13
Returning to high energy activities should be held off for 6-12 weeks or until
hip strength returns to what is normal to the patient.
12
Hip dislocations are medical emergencies and should be treated as so. When the femoral
head is displaced from the socket a dislocation has occurred. Without early detection and
reduction, hip dislocations can cause problems in the joint in the future. Mechanisms include
force directly at the hip joint in certain movements. Many of these injuries will need to be
surgically repaired followed by rehab to ensure the strength of the muscles and joints is returned.
The rehab needs to be a well thought out number of sessions that includes goals and eventually
return to play and activities of daily living. All of these precautions and treatments are to help
ensure no further complications after a hip dislocation. Also, the treatments and rehab are to
help the patient make a full and successful recovery from this traumatic injury.
Candace Perkins MSAT 6500
References
1. Hip Dislocation. Available at http://emedicine.medscape.com/article/86930-
overview#showall. Accessed July 24, 2014
2. Smith T, Davies L, Ingham C, Mann C. What activities cause hip dislocation? A review of
100 total hip replacement dislocations*. Advances In Physiotherapy [serial online]. June
2012;14(2):55-60. Available from: SPORTDiscus with Full Text, Ipswich, MA. Accessed July
24, 2014.
3. Hip Joint Anatomy. Available at http://emedicine.medscape.com/article/1898964-overview.
Accessed July 24, 2014
4. Erb R, Steele J, Nance E, Edwards J. Traumatic anterior dislocation of the hip: spectrum of
plain film and CT findings. AJR. American Journal Of Roentgenology [serial online]. November
1995;165(5):1215-1219. Available from: MEDLINE, Ipswich, MA. Accessed July 24, 2014.
5. Sansone M, Ahldn M, Jnasson P, Swrd L, Eriksson T, Karlsson J. Total dislocation of the
hip joint after arthroscopy and ileopsoas tenotomy. Knee Surgery, Sports Traumatology,
Arthroscopy [serial online]. February 2013;21(2):420-423. Available from: SPORTDiscus with
Full Text, Ipswich, MA. Accessed July 24, 2014.
6. Upadhyay S, Moulton A, Burwell R. Biological factors predisposing to traumatic posterior
dislocation of the hip. A selection process in the mechanism of injury. The Journal Of Bone And
Joint Surgery. British Volume [serial online]. March 1985;67(2):232-236. Available from:
MEDLINE, Ipswich, MA. Accessed July 24, 2014.
Candace Perkins MSAT 6500
7. Henderson L, Johnston A, Mockford B, Craig B. Posterior hip dislocation and ipsilateral
isolated femoral neck fracture: A novel fixation method. Journal Of Surgical Case Reports [serial
online]. October 1, 2012;2012(10):14. Available from: MEDLINE, Ipswich, MA. Accessed July
24, 2014.
8. Hip Dislocation in Emergency Medicine. Available
http://emedicine.medscape.com/article/823471-overview#showall. Accessed July 24, 2014
9. Hailer N, Weiss R, Stark A, Krrholm J. The risk of revision due to dislocation after total hip
arthroplasty depends on surgical approach, femoral head size, sex, and primary diagnosis. Acta
Orthopaedica [serial online]. October 2012;83(5):442-448. Available from: SPORTDiscus with
Full Text, Ipswich, MA. Accessed July 24, 2014.
10. Bracken J, Tran T, Ditchfield M. Developmental dysplasia of the hip: Controversies and
current concepts. Journal Of Paediatrics & Child Health [serial online]. November
2012;48(11):963-973. Available from: Academic Search Premier, Ipswich, MA. Accessed July
25, 2014.
11. Zhao Y, Fu D, Yin X, et al. Outcome of Hemiarthroplasty and Total Hip Replacement for
Active Elderly Patients with Displaced Femoral Neck Fractures: A Meta-Analysis of 8
Randomized Clinical Trials. Plos ONE [serial online]. May 2014;9(5):1-7. Available from:
Academic Search Premier, Ipswich, MA. Accessed July 25, 2014.
12. Sanders S, Tejwani N, Egol K. Traumatic Hip Dislocation. Bulletin Of The NYU Hospital
For Joint Diseases [serial online]. April 2010;68(2):91-96. Available from: SPORTDiscus with
Full Text, Ipswich, MA. Accessed July 25, 2014.
Candace Perkins MSAT 6500
13. Hip Dislocation and Acetabular Fracture in a Collegiate Football Player. International
Journal Of Athletic Therapy & Training [serial online]. January 2013;18(1):7-11. Available
from: SPORTDiscus with Full Text, Ipswich, MA. Accessed July 25, 2014.
Das könnte Ihnen auch gefallen
- Healthy Shoulder Handbook: Second Edition: 100 Exercises for Treating Common Injuries and Ending Chronic PainVon EverandHealthy Shoulder Handbook: Second Edition: 100 Exercises for Treating Common Injuries and Ending Chronic PainNoch keine Bewertungen
- 20 Questions - Orthopedic and Extremity InjuryDokument3 Seiten20 Questions - Orthopedic and Extremity InjurymichaelsophianNoch keine Bewertungen
- Shoulder Dislocation Background: Shoulder Dislocations Traumatic InjuryDokument7 SeitenShoulder Dislocation Background: Shoulder Dislocations Traumatic Injuryanastasiaanggita_265Noch keine Bewertungen
- Traumatic Hip Dislocations in Children and Adolescents: Pitfalls and ComplicationsDokument7 SeitenTraumatic Hip Dislocations in Children and Adolescents: Pitfalls and ComplicationsFadhli Aufar KasyfiNoch keine Bewertungen
- Joint Instability: Hendradi Khumarga SPOT. FICSDokument48 SeitenJoint Instability: Hendradi Khumarga SPOT. FICSJoshua ObrienNoch keine Bewertungen
- SpondylolisthesisDokument9 SeitenSpondylolisthesiswangNoch keine Bewertungen
- Fractures of The Hip: Extraarticular Fracture Does Not Involve The Articular SurfaceDokument6 SeitenFractures of The Hip: Extraarticular Fracture Does Not Involve The Articular SurfaceBella DonnaNoch keine Bewertungen
- Dislocation Shoulder GoodDokument7 SeitenDislocation Shoulder GoodZahiera NajibNoch keine Bewertungen
- Fracture-Dislocation of The Hip-KaizarDokument69 SeitenFracture-Dislocation of The Hip-KaizarKaizar Ennis100% (1)
- Hip FractureDokument100 SeitenHip Fracturegeronimo antNoch keine Bewertungen
- ScoliosisDokument18 SeitenScoliosisMj EnofnaNoch keine Bewertungen
- Progression and Correction of Deformities in Adults With Cerebral PalsyDokument4 SeitenProgression and Correction of Deformities in Adults With Cerebral PalsyAirika PeningNoch keine Bewertungen
- Hip DislocationDokument4 SeitenHip DislocationcrunkestNoch keine Bewertungen
- Diagnostico y Tratamiento de Tendinitis y TendinosisDokument7 SeitenDiagnostico y Tratamiento de Tendinitis y TendinosisMatias ListaNoch keine Bewertungen
- Frienchzel Joy A. Asis Group 3 BSN 3-ADokument14 SeitenFrienchzel Joy A. Asis Group 3 BSN 3-AKenneth Louis GalizaNoch keine Bewertungen
- Femur Fractures 5-07Dokument12 SeitenFemur Fractures 5-07Kaine Lacsina SinforosoNoch keine Bewertungen
- Splints BracesDokument18 SeitenSplints BracesvaishnaviNoch keine Bewertungen
- Acetabulum FractureDokument32 SeitenAcetabulum FracturePhysiotherapist AliNoch keine Bewertungen
- The Fractured Femur: Directed Readings in The ClassroomDokument68 SeitenThe Fractured Femur: Directed Readings in The ClassroomEddie Wyatt100% (1)
- Back Pain BackupDokument9 SeitenBack Pain BackupArun Kumar PTNoch keine Bewertungen
- Lower Limb InjuriesDokument47 SeitenLower Limb InjuriesDaisyyhyNoch keine Bewertungen
- Hip Dislocation: Evaluation and Management: Review ArticleDokument11 SeitenHip Dislocation: Evaluation and Management: Review ArticleFadhli Aufar KasyfiNoch keine Bewertungen
- Acquired DeformitiesDokument6 SeitenAcquired DeformitiesAnonymous fVtDc9hNoch keine Bewertungen
- Traumatic Anterior Hip Dislocation in A 12-Year-Old ChildDokument3 SeitenTraumatic Anterior Hip Dislocation in A 12-Year-Old ChildMikael AngelooNoch keine Bewertungen
- Congenital DeformitiesDokument102 SeitenCongenital DeformitiesFahmi MujahidNoch keine Bewertungen
- Kimberli Case StudyDokument4 SeitenKimberli Case StudyLLLJJJ100% (3)
- Sport Injury in Children (Short)Dokument3 SeitenSport Injury in Children (Short)Ribka TheodoraNoch keine Bewertungen
- Sci 4Dokument8 SeitenSci 4anna widiaNoch keine Bewertungen
- Traumatic Hip Dislocation: A ReviewDokument6 SeitenTraumatic Hip Dislocation: A ReviewAna HurtadoNoch keine Bewertungen
- Clavicle Fracture RehabDokument7 SeitenClavicle Fracture Rehabnmmathew mathewNoch keine Bewertungen
- LL InjuriesDokument25 SeitenLL InjuriesShrutiNoch keine Bewertungen
- Shoulder Sports InjuryDokument12 SeitenShoulder Sports InjuryfriskaNoch keine Bewertungen
- The Shoulder Replacement Book: Frank Norberg, MDDokument8 SeitenThe Shoulder Replacement Book: Frank Norberg, MDRammah EmadNoch keine Bewertungen
- Shoulder DislocationDokument28 SeitenShoulder DislocationQueen SofiaNoch keine Bewertungen
- Morphopedics: Broken Neck (Hangman's Fracture)Dokument7 SeitenMorphopedics: Broken Neck (Hangman's Fracture)Sulla FelixNoch keine Bewertungen
- Orthopedic: Dislocations of The Hip JointDokument16 SeitenOrthopedic: Dislocations of The Hip JointAnmarNoch keine Bewertungen
- Distal Radius Fractures in AdultsDokument35 SeitenDistal Radius Fractures in AdultsNicolás OpazoNoch keine Bewertungen
- About:: Birth Defects Muscular Dystrophy, Cerebral Palsy Marfan's DiseaseDokument4 SeitenAbout:: Birth Defects Muscular Dystrophy, Cerebral Palsy Marfan's DiseaseAbie BeyNoch keine Bewertungen
- Tibia and Fibula Shaft Fracture in Pediatric Case (Ola)Dokument20 SeitenTibia and Fibula Shaft Fracture in Pediatric Case (Ola)Junarto Putra Tandiarrang100% (1)
- Shoulder Dislocation SubluxationDokument4 SeitenShoulder Dislocation SubluxationSisca Dwi AgustinaNoch keine Bewertungen
- Manejo de Fracturas Mediales de Cadera 2015 Femoral Neck Fractures - Current ManagementDokument9 SeitenManejo de Fracturas Mediales de Cadera 2015 Femoral Neck Fractures - Current ManagementSergio Tomas Cortés MoralesNoch keine Bewertungen
- Returntoplayfollowing Anklesprainandlateral LigamentreconstructionDokument13 SeitenReturntoplayfollowing Anklesprainandlateral LigamentreconstructionNICOLÁS ANDRÉS AYELEF PARRAGUEZNoch keine Bewertungen
- Types of ScoliosisDokument5 SeitenTypes of ScoliosisDimple Castañeto CalloNoch keine Bewertungen
- Hip Dislocation: Current Treatment Regimens: Paul Tornetta III, MD, and Hamid R. Mostafavi, MDDokument10 SeitenHip Dislocation: Current Treatment Regimens: Paul Tornetta III, MD, and Hamid R. Mostafavi, MDJaime Anaya Sierra100% (1)
- Lower Extremity Bone Fracture Lecture 3Dokument88 SeitenLower Extremity Bone Fracture Lecture 3Tselmeg TselmegNoch keine Bewertungen
- Uy 8 UyDokument62 SeitenUy 8 UyVandana SinghNoch keine Bewertungen
- Scolio SIS: Submitted ToDokument10 SeitenScolio SIS: Submitted Tojean thereseNoch keine Bewertungen
- Diaphyseal Femur FracturesDokument9 SeitenDiaphyseal Femur FracturesSoulmates1Noch keine Bewertungen
- Drop Claw FootDokument3 SeitenDrop Claw FootfmtaNoch keine Bewertungen
- Spondylosis Vs Spondylolysis Vs SpondylolisthesisDokument6 SeitenSpondylosis Vs Spondylolysis Vs Spondylolisthesisahmad saffwanNoch keine Bewertungen
- Ankle Injury EvaluationDokument7 SeitenAnkle Injury EvaluationManiDeep ReddyNoch keine Bewertungen
- Femur Injuries and Fractures 2Dokument23 SeitenFemur Injuries and Fractures 2chelle_morales26Noch keine Bewertungen
- Posterior Dislocation of The Hip JointDokument25 SeitenPosterior Dislocation of The Hip JointadibahNoch keine Bewertungen
- Complications Following An AmputationDokument10 SeitenComplications Following An AmputationPatricio Sobarzo CasanovaNoch keine Bewertungen
- Background: FrequencyDokument15 SeitenBackground: FrequencyRandi SukmanaNoch keine Bewertungen
- Fractured Neck of FemurDokument20 SeitenFractured Neck of Femurrajvikram87Noch keine Bewertungen
- S Pondy Lols Ys ThesisDokument35 SeitenS Pondy Lols Ys ThesisSal LieNoch keine Bewertungen
- Healthy Shoulder Handbook: 100 Exercises for Treating and Preventing Frozen Shoulder, Rotator Cuff and other Common InjuriesVon EverandHealthy Shoulder Handbook: 100 Exercises for Treating and Preventing Frozen Shoulder, Rotator Cuff and other Common InjuriesBewertung: 2 von 5 Sternen2/5 (1)
- (Formerly Known As Max Bupa Health Insurance Co. LTD.) : Product Name: Reassure - Product Uin: Maxhlip21060V012021Dokument47 Seiten(Formerly Known As Max Bupa Health Insurance Co. LTD.) : Product Name: Reassure - Product Uin: Maxhlip21060V012021apprenant amitNoch keine Bewertungen
- E The Real Facts Supporting Jeanne Calment As The Oldest Ever HumanDokument9 SeitenE The Real Facts Supporting Jeanne Calment As The Oldest Ever Humanliz201177Noch keine Bewertungen
- CCAC MSW City Action Plan Cebu City, PhilippinesDokument6 SeitenCCAC MSW City Action Plan Cebu City, Philippinesca1Noch keine Bewertungen
- Addis Ababa Science and Technology University (AASTU)Dokument24 SeitenAddis Ababa Science and Technology University (AASTU)Wasihun DanielNoch keine Bewertungen
- Application Form For Accreditation SPDokument4 SeitenApplication Form For Accreditation SPMyk Twentytwenty NBeyondNoch keine Bewertungen
- Shoulder Impingement GuidelinesDokument3 SeitenShoulder Impingement GuidelinesTasha MillerNoch keine Bewertungen
- Lung Collapse PDFDokument65 SeitenLung Collapse PDFRibhav GuptaNoch keine Bewertungen
- Confidential: Iom Minimum Medical Review QuestionnaireDokument3 SeitenConfidential: Iom Minimum Medical Review QuestionnairePochieNoch keine Bewertungen
- Peplu Theory ApplicationDokument7 SeitenPeplu Theory ApplicationVarsha Gurung100% (1)
- Seal of Good Local Governance For Barangay (SGLGB)Dokument2 SeitenSeal of Good Local Governance For Barangay (SGLGB)Ponciano AlveroNoch keine Bewertungen
- HSE Covid-19 Doffing CoverallDokument1 SeiteHSE Covid-19 Doffing Coveralliq_dianaNoch keine Bewertungen
- Alpha-2 Adrenergic Agonists (Dexmedetomidine) Pekka Talke MD UCSF Faculty Development Lecture Jan 2004Dokument53 SeitenAlpha-2 Adrenergic Agonists (Dexmedetomidine) Pekka Talke MD UCSF Faculty Development Lecture Jan 2004Nur NabilahNoch keine Bewertungen
- Erbacher Vita 2010Dokument5 SeitenErbacher Vita 2010HuntMNoch keine Bewertungen
- Yoga and Pregnancy Pre and Postnatal Resources PDFDrive ComDokument63 SeitenYoga and Pregnancy Pre and Postnatal Resources PDFDrive ComsilverbirddudeNoch keine Bewertungen
- Research Paper FinalDokument12 SeitenResearch Paper Finalapi-582867034Noch keine Bewertungen
- Purpose 1Dokument4 SeitenPurpose 1Rizzah MagnoNoch keine Bewertungen
- Jamie's Story 15q21.3-22.2 DeletionDokument1 SeiteJamie's Story 15q21.3-22.2 DeletionNatasha RadcliffeNoch keine Bewertungen
- Risk Management in Military AviationDokument16 SeitenRisk Management in Military AviationSp AndaNoch keine Bewertungen
- Water Pollution Is The Contamination ofDokument36 SeitenWater Pollution Is The Contamination ofsuradotNoch keine Bewertungen
- PHD Thesis On Coronary Artery DiseaseDokument5 SeitenPHD Thesis On Coronary Artery Diseasebdg9hkj6100% (1)
- InterbarkadaDokument8 SeitenInterbarkadaJay Vincent DiamanteNoch keine Bewertungen
- Response in OppositionDokument36 SeitenResponse in OppositionForeclosure FraudNoch keine Bewertungen
- Applying 5S ProceduresDokument70 SeitenApplying 5S ProceduresSanta Best100% (3)
- Journal Club: A Step Towards Evidence Based Practice: January 2011Dokument6 SeitenJournal Club: A Step Towards Evidence Based Practice: January 2011Jommy ChawalaNoch keine Bewertungen
- SP - Sindy MilaDokument2 SeitenSP - Sindy MilaSindy MelindaNoch keine Bewertungen
- Report Decentralised Planning Kerala 2009 OommenDokument296 SeitenReport Decentralised Planning Kerala 2009 OommenVaishnavi JayakumarNoch keine Bewertungen
- AnumwraDokument30 SeitenAnumwratejasNoch keine Bewertungen
- Plazma Ionizarot CP 212 Eng ManualDokument1 SeitePlazma Ionizarot CP 212 Eng ManualVladimirDulaNoch keine Bewertungen
- IntralipidDokument3 SeitenIntralipidGwyn RosalesNoch keine Bewertungen
- Lazuli ProfileDokument25 SeitenLazuli ProfileNew Seljuk EmpireNoch keine Bewertungen