Beruflich Dokumente
Kultur Dokumente
Pathophysiology of Status Epilepticus
Hochgeladen von
Kysha Ruth SevillaOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Pathophysiology of Status Epilepticus
Hochgeladen von
Kysha Ruth SevillaCopyright:
Verfügbare Formate
Legend: - Leading to * - Manifested - Signs and Symptoms Characteristic Pathophysiology of Seizure Disorder Generalized Epileptiform
Precipitating Factors: Stroke Head injury Hemorrhage Infection such as encephalitis or meningitis Flashing lights Intoxicants or adverse reactions to drugs Insufficient dosage of a medication Sudden withdrawal from a seizure medication Consumption of alcoholic beverages while on an anticonvulsant or alcohol withdrawal Starting on a new medication that reduces the effectiveness of the anticonvulsant Developing a resistance to an anticonvulsant already being used Gastroenteritis while on an anticonvulsant Metabolic disturbances Insomnia or sleep deprivation
Predisposing Factors: *Age: Less than 2 years Family history Perinatal brain injury Congenital central nervous system malformations
Excess excitation and reduced inhibition of the neurons Failure of inhibitory process Electrical signal spreads to surrounding normal brain cells
Partial Seizures Complex Partial Seizure Simple Partial Seizure
Generalized Seizures
Excess excitation of bilateral hemispheres of the brain Motor: Jerking; Stiffening of the muscles; Myoclonus Sensory: Hypersensitivi ty of the five senses (vision, hearing, smell, taste or touch
Loss of awareness
Excess excitation of temporal lobes or hippocampi
Retains awareness
Autonomic: racing heart beat, stomach upset, diarrhea, loss of bladder control
Psychological: Deja vu; Jamis vu; Fear; Euphoria; Depersonalization; Hallucinations; Anger
Absence Seizure
Atypical Absence
Tonic
Clonic
Tonic-Clonic
Atonic
Myoclonic
Blank stare
Hand motions and fluttering
Stiffening of the muscles
Repetitive, jerking movements
Unconscious ness, convulsions, muscle rigidity
General loss of muscle tone, particularly in the arms and legs
Sporadic (isolated), jerking movements
With Interventions Diagnostic tests: *Electroencephalography (EEG) Magnetic Resonance Imaging (MRI)
Without Interventions Failure of inhibitory process by the GABA Abnormal transmission of neural responses to body functions
Magnetic Resonance Spectroscopy (MRS) Positron Emission Tomography (PET) Single Photon Emission Computed Tomography (SPECT Neuropsychological Testing Wada Test Psychiatric Evaluation Laboratory Tests:v *Fecalysis *Hematology *Urinalysis
Physiologic
Psychologic Behavioral changes
Sensory disturbance Vertigo
Unpredictable seizures
Decreased function of immune system Infection
Hormonal imbalance
Metabolic imbalance Electrolyte imbalance
Risk for injury Head trauma Heart failure Respiratory failure GI upset
Medical Intervention: a. Pharmacologic Anticonvulsants: Carbamazepine Tigabine Zonisamide Lamotrigine Pregabalin Gabapentin Valproic acid Anxiolytic: *Diazepam Lorazepam Clonazepam *Phenobarbital Anti-epeleptics: Ethosuximide Hemorrhage Spread of bacteria to systemic circulation Spread of bacteria to brain Hypertrophy of brain tissue Bacterial invasion through respiratory tract
Meningeal invasion Subarachnoid space inflammation Increased CSF outflow Increased intracranial pressure
Cerebral Vasculitis
Interstitial edema
Rupture of brain tissues
Aneurism
Anti-pyretic: *Paracetamol Antibiotic: *Metronidazole *Ceftriaxone Surgery: Lobe resection Lesionectomy Corpus callostomy Functional hemispherectomy Temporal Lobe Resection Nursing interventions: 1. Monitor vital signs every 2 hours. 2. Provide sponge baths if temperature continues to rise 3. Provide safe environment by padding side rails, putting pillows on the side. 4. Do not restrain the patient during seizure. 5. Do not put anything in the patients mouth during seizure. 6. Protect the patients head during the seizure. 7. Maintain a patent airway until the patient is fully awake after a seizure. 8. Monitor for and report seizure activity and decreasing level of consciousness. 9. Keep bed in low position with side rails elevated. 10. Administer prescribed intravenous antibiotics. 11. Remind the family the importance of following medication examinations.
Sepsis
Decrease blood flow to brain Hypoxia to brain cells Brain cell death Systemic loss of body functions
DEATH
POOR PROGNOSIS
Proper management of disease Achieve optimum level of functioning GOOD PROGNOSIS
Das könnte Ihnen auch gefallen
- Pathophysiology of Urinary Tract ObstructionDokument50 SeitenPathophysiology of Urinary Tract ObstructionPryo UtamaNoch keine Bewertungen
- Pathophysiology Sickle Cell Anemia PDFDokument1 SeitePathophysiology Sickle Cell Anemia PDFTine GuibaoNoch keine Bewertungen
- Pathophysiology of Meniere FinalDokument1 SeitePathophysiology of Meniere Final1S VILLEGAS GabrielNoch keine Bewertungen
- Pathophysiology of HyperthyroidismDokument4 SeitenPathophysiology of HyperthyroidismKitty YuffieNoch keine Bewertungen
- Pathophysiology Sickle Cell AnemiaDokument1 SeitePathophysiology Sickle Cell AnemiaTine GuibaoNoch keine Bewertungen
- Acc Phu Case NCP HyperthermiaDokument1 SeiteAcc Phu Case NCP Hyperthermiamacy_bautistaNoch keine Bewertungen
- Appendicitis NCPDokument5 SeitenAppendicitis NCPEarl Joseph DezaNoch keine Bewertungen
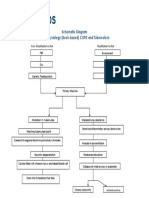
- Schematic Diagram Pathophysiology (Book-Based) COPD and TuberculosisDokument1 SeiteSchematic Diagram Pathophysiology (Book-Based) COPD and Tuberculosispragna novaNoch keine Bewertungen
- Drug Study GuideDokument2 SeitenDrug Study GuideAubrey Sunga100% (1)
- Drug StudyDokument4 SeitenDrug StudyPam RomeroNoch keine Bewertungen
- Pathophysiology of VSDDokument1 SeitePathophysiology of VSDMarlon CruzNoch keine Bewertungen
- PneumoniaDokument2 SeitenPneumoniaPia MedinaNoch keine Bewertungen
- Measles PathophysiologyDokument1 SeiteMeasles PathophysiologyAl TheóNoch keine Bewertungen
- SNU49Dokument2 SeitenSNU49Nora BacolNoch keine Bewertungen
- BPH Pathophysio 4CDokument2 SeitenBPH Pathophysio 4CPatricia Camille Ponce JonghunNoch keine Bewertungen
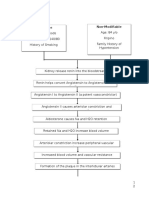
- "Acute Coronary Syndrome Non ST Elevation Myocardial Infarction, Hypertensive Cardiovascular Disease, Diabetes Mellitus Type 2, and Community Acquired Pneumonia" Client Centered PathophysiologyDokument3 Seiten"Acute Coronary Syndrome Non ST Elevation Myocardial Infarction, Hypertensive Cardiovascular Disease, Diabetes Mellitus Type 2, and Community Acquired Pneumonia" Client Centered PathophysiologyCarl Elexer Cuyugan Ano50% (2)
- (Patho) PTB COPDDokument1 Seite(Patho) PTB COPDKyle HannahNoch keine Bewertungen
- V. Pathophysiology Modifiable Non-ModifiableDokument3 SeitenV. Pathophysiology Modifiable Non-ModifiableSteffi MurielNoch keine Bewertungen
- Risk For InfectionDokument1 SeiteRisk For InfectionEuanne OrellanoNoch keine Bewertungen
- Pathophysiology of Gastroenteritis, Dehydration, and NecatoriasisDokument3 SeitenPathophysiology of Gastroenteritis, Dehydration, and NecatoriasisRalph Delos Santos100% (2)
- Pa Tho Physiology of OsteoporosisDokument2 SeitenPa Tho Physiology of Osteoporosisjcam_o9Noch keine Bewertungen
- Assesment Diagnosis Planning Interventio N Rationale EvaluationDokument2 SeitenAssesment Diagnosis Planning Interventio N Rationale EvaluationRenea Joy ArruejoNoch keine Bewertungen
- Angina Pectoris PathophysiologyDokument2 SeitenAngina Pectoris PathophysiologyALIANA KIMBERLY MALQUESTONoch keine Bewertungen
- DP Discharge Plan@@@@@@@@Dokument6 SeitenDP Discharge Plan@@@@@@@@Maemae SumalinogNoch keine Bewertungen
- NCP UreteroDokument1 SeiteNCP UreteroCerie Anne OlayNoch keine Bewertungen
- Chronic Kidney Disease: A. Pathophysiology A. Schematic DiagramDokument3 SeitenChronic Kidney Disease: A. Pathophysiology A. Schematic DiagramDaniel GeduquioNoch keine Bewertungen
- Oraa, Jamie - Drug Study Surgical WardDokument1 SeiteOraa, Jamie - Drug Study Surgical WardJamie LeeNoch keine Bewertungen
- Pathophysiology of Gastrointestinal Bleeding Secondary To Bleeding PolypsDokument1 SeitePathophysiology of Gastrointestinal Bleeding Secondary To Bleeding PolypsGinoTevesNoch keine Bewertungen
- Drug StudyDokument7 SeitenDrug StudyHerwincayeNoch keine Bewertungen
- Albendazole - Drug Information PDFDokument7 SeitenAlbendazole - Drug Information PDFjjjkkNoch keine Bewertungen
- A Case PresentationDokument50 SeitenA Case PresentationAnaleah MalayaoNoch keine Bewertungen
- Precipitating Factors Predisposing Factors Chronic Kidney DiseaseDokument3 SeitenPrecipitating Factors Predisposing Factors Chronic Kidney DiseaseGrace Jane DionaldoNoch keine Bewertungen
- NAPREXDokument2 SeitenNAPREXKarl EdemNoch keine Bewertungen
- AGE PathophysiologyDokument2 SeitenAGE Pathophysiologyjosephcanlas67% (3)
- Assessment Planning Intervention Rationale Evaluation: Mechanism of ActionDokument2 SeitenAssessment Planning Intervention Rationale Evaluation: Mechanism of ActionNicole CalpoturaNoch keine Bewertungen
- Darbepoetin AlfaDokument3 SeitenDarbepoetin Alfaapi-3797941Noch keine Bewertungen
- Pathophysiology PDFDokument3 SeitenPathophysiology PDFJenievieve MerzaNoch keine Bewertungen
- TherablocDokument3 SeitenTherablocianecunar100% (2)
- Nstemi PathoDokument2 SeitenNstemi PathoSheana TmplNoch keine Bewertungen
- Buerger's DiseaseDokument5 SeitenBuerger's Diseaseglie_e52164100% (5)
- NCP LeukemiaDokument5 SeitenNCP LeukemiaTriciaNoch keine Bewertungen
- Assessment Diagnosis Objectives of Care Intervention Rationale Evaluation Difficulty of Breathing (Rapid and Shallow)Dokument1 SeiteAssessment Diagnosis Objectives of Care Intervention Rationale Evaluation Difficulty of Breathing (Rapid and Shallow)Jamaica Leslie NovenoNoch keine Bewertungen
- Decreased Cardiac OutputDokument5 SeitenDecreased Cardiac Outputshuang81Noch keine Bewertungen
- Drug Study SARAHDokument2 SeitenDrug Study SARAHirene Joy DigaoNoch keine Bewertungen
- MannitolDokument3 SeitenMannitolAlexandra AntondyNoch keine Bewertungen
- Concept Map AsthmaDokument4 SeitenConcept Map AsthmaAstrid Moreno De LeonNoch keine Bewertungen
- Pathophysiology Diagram of Congestive Heart FailureDokument3 SeitenPathophysiology Diagram of Congestive Heart FailureLeng Royo BrionesNoch keine Bewertungen
- PHASE 2 NCP (Injury, Risk For Bleeding)Dokument3 SeitenPHASE 2 NCP (Injury, Risk For Bleeding)NE TdrNoch keine Bewertungen
- Medical Diagnosis: Chronic Kidney Disease Stage 5 Patient's NameDokument4 SeitenMedical Diagnosis: Chronic Kidney Disease Stage 5 Patient's NameHadeer Mahmoud Abuslima100% (1)
- TAHBSO ReportDokument4 SeitenTAHBSO ReportsachiiMeNoch keine Bewertungen
- COPD PathoDokument1 SeiteCOPD PathoLeah May AnchetaNoch keine Bewertungen
- ENCEPHALOPATHY Udah DibacaDokument7 SeitenENCEPHALOPATHY Udah DibacaJemmy Fandri100% (1)
- Seizure 091214081436 Phpapp01Dokument26 SeitenSeizure 091214081436 Phpapp01সোমনাথ মহাপাত্রNoch keine Bewertungen
- ENCEPHALOPATHYDokument5 SeitenENCEPHALOPATHYSepta RinaldyNoch keine Bewertungen
- Metabolic Coma DRDokument32 SeitenMetabolic Coma DRKintan UtamiNoch keine Bewertungen
- Meiti Frida Department of Neurology Andalas University PadangDokument49 SeitenMeiti Frida Department of Neurology Andalas University PadangIe Dochie100% (1)
- Meiti Frida Department of Neurology Andalas University PadangDokument49 SeitenMeiti Frida Department of Neurology Andalas University PadangelvistiaNoch keine Bewertungen
- Seizure-Case StudyDokument6 SeitenSeizure-Case StudyELaine ELena TiongsonNoch keine Bewertungen
- Chapter 14 Neurologic Disorders Study Guide Outline #2Dokument12 SeitenChapter 14 Neurologic Disorders Study Guide Outline #2Del Delgado100% (1)
- NR 325 Neuro Worksheet 2Dokument6 SeitenNR 325 Neuro Worksheet 2John Thomas100% (1)