Beruflich Dokumente
Kultur Dokumente
Anatomy of Periodontium
Hochgeladen von
Nana HindraOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Anatomy of Periodontium
Hochgeladen von
Nana HindraCopyright:
Verfügbare Formate
1
Anatomy of the periodontium
The four principal gingival fibre groups are: Dentogingival fibres Alveologingival fibres Circular fibres (shown in cross section) Transeptal fibres Gingivae Junctional epithelium enamel gingival connective tissue cement-enamel junction circular fibres
Enamel
Oral sulcular epithelium
Dentine
Alveolar bone
RI
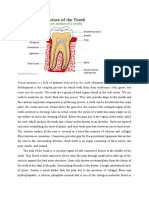
periodontal ligament fibres bone The gingiva is made up of the gingival epithelium and connective tissue. The gingival epithelium comprises oral epithelium, oral sulcular epithelium and junctional epithelium. Figure 1.1 Longitudinal section through part of a tooth showing healthy periodontal tissues.
MA
TE
Figure 1.2 Dentogingival fibres, alveolar crest fibres and circular fibres in the gingival connective tissue.
AL
Periodontal ligament
Oral epithelium
alveologingival fibres dentogingival fibres
enamel interdental papilla circular fibres transeptal fibres
PY R
IG
HT
ED
dentogingival fibres alveolar crest fibres horizontal fibres oblique fibres
bone
CO
Figure 1.3 Interdental area showing transeptal and circular fibre groups in the gingival connective tissue.
apical fibres The four periodontal ligament fibre groups are: Alveolar crest fibres Horizontal fibres Oblique fibres Apical fibres Figure 1.4 The periodontal ligament.
dehiscence Fenestration In most situations these areas of missing bone remain undetected as they are covered with soft tissue. They may be clinically significant if associated with loss of soft tissue resulting in gingival recession (Chapter 32). Figure 1.5 Bony fenestration and dehiscence.
2 Chapter 1 Anatomy of the periodontium
The periodontal tissues form the supporting structures of the teeth. The principal components of the periodontium are shown in Fig. 1.1: Gingivae (including epithelium and connective tissue). Periodontal ligament. Cementum. Alveolar bone.
lie bundles of collagen bres; these are divided into four groups based on their position (Fig. 1.4). Within the ligament are mechanoreceptors that provide sensory input for jaw reexes. Cells from the periodontal ligament are involved in the formation and remodelling of alveolar bone and cementum. The periodontal ligament acts to dissipate masticatory forces to the supporting alveolar bone and its width, height and quality determine a tooths mobility.
Gingivae
The gingivae in health are pink and rm with a knife-edge appearance, scalloped around the teeth. In certain ethnic groups the gingivae may be pigmented. In health, the gingival margin is a few millimetres coronal to the cementenamel junction. The gingival sulcus (or crevice) is a shallow groove which may be between 0.5 and 3 mm in depth around a fully erupted tooth. The gingival tissues are keratinised and appear paler pink than sites of non-keratinised oral epithelium.
Cementum
Cementum is a mineralised tissue overlying the root dentine. It does not undergo physiological remodelling but is continuously deposited throughout life. Cementum is classied into two types: Acellular. Cellular.
Acellular cementum Gingival epithelium
The gingival epithelium comprises (Fig. 1.1): Oral epithelium (OE). Oral sulcular epithelium (SE). Junctional epithelium (JE). The gingival sulcus is lined by SE and JE. Oral epithelium The OE is an orthokeratinised, stratied, squamous epithelium. Surface cells lose their nuclei and are packed with the protein keratin. It presents an impermeable physical barrier to oral bacteria. The basal layer of epithelial cells is thrown up into folds overlying the supporting connective tissue. These folds increase the surface area of contact between the epithelium and connective tissue and are known as rete ridges or rete pegs. Oral sulcular epithelium There are no rete ridges. Cells are keratinised but still have nuclei (parakeratinised). Junctional epithelium The JE forms a specialised attachment to the tooth via: a hemidesmosomal layer within the JE cells; a basal lamina produced by the epithelial cells. The JE is non-keratinised and has a very fast turnover of cells (26 days compared to 1 month for OE). The most apical part of the JE lies at the cement-enamel junction in health. The JE at its widest point is 20 30 cells thick coronally. The JE tapers until it is only one cell in width apically. The JE is permeable with wide intercellular spaces through which cells and substances can migrate (such as bacterial toxins or host defence cells). Migration of the JE from its position in health apically onto the root cementum indicates a loss of periodontal attachment and progression to the disease state of periodontitis. Acellular cementum forms on root dentine during root formation and tooth eruption. Fibres inserted from the periodontal ligament are mineralised within the cementum and are known as Sharpeys bres and are abundant in acellular cementum.
Cellular cementum
Cellular cementum lies over the acellular cementum. It contains cells called cementocytes which lie in lacunae. The cellular cementum layer is thicker in the apical region of the root where it is between 0.2 and 1 mm thick.
Alveolar bone
The walls of the sockets are lined with a layer of dense bone called compact bone, which also forms the buccal and lingual/palatal plates of the jaw bones. In between the sockets and the compact jaw bone walls lies cancellous bone that is made up of bony trabeculae. The compact bone plates of the jaws are thicker on the buccal aspect of the mandibular molars and thinnest on the labial surface of the mandibular incisors. The thickness of the compact bone layer is relevant to the choice of local analgesia techniques as the anaesthetic solution passes through bone to reach the nerve supply. The thin bone, particularly in the lower incisor region, can manifest as incomplete bony coverage in the form of fenestrations and dehiscences (Fig. 1.5). The tooth sockets are lined with compact bone within which the principal bres of the periodontal ligament are inserted. This area of bone can appear as a dense white line called the lamina dura on a radiograph.
Key points
Gingivae JE forms the specialised attachment to the tooth The most apical part of JE lies at the cementenamel junction in health Supported by connective tissue containing collagen bre bundles Periodontal ligament Forms attachment between the cementum and bone Cementum Mineralised and deposited continuously Alveolar bone Compact and cancellous bone Periodontal ligament bres inserted into compact bone lining the tooth sockets
Anatomy of the periodontium Chapter 1 3
Gingival connective tissue
The gingival connective tissue (or lamina propria) is made up of collagen bre bundles called gingival bres, around which lie ground substance, broblasts, blood and lymph vessels and neural tissues. The four bre groups are shown in Figs 1.2 and 1.3.
Periodontal ligament
The periodontal ligament forms the attachment between the cementum and alveolar bone. It is a richly vascular connective tissue within which
Das könnte Ihnen auch gefallen
- Evolution of Dental Tissues and Paleobiology in SelachiansVon EverandEvolution of Dental Tissues and Paleobiology in SelachiansNoch keine Bewertungen
- PDL Structure and FunctionsDokument45 SeitenPDL Structure and Functionsshahzeb memonNoch keine Bewertungen
- Advanced farriery knowledge: A study guide and AWCF theory course companionVon EverandAdvanced farriery knowledge: A study guide and AWCF theory course companionNoch keine Bewertungen
- Anatomy and Microstructure of PeriodontiumDokument9 SeitenAnatomy and Microstructure of PeriodontiumAnonymous k8rDEsJsU1100% (1)
- Alveolar Bone in HealthDokument87 SeitenAlveolar Bone in HealthPrathik RaiNoch keine Bewertungen
- Orthodontically Driven Corticotomy: Tissue Engineering to Enhance Orthodontic and Multidisciplinary TreatmentVon EverandOrthodontically Driven Corticotomy: Tissue Engineering to Enhance Orthodontic and Multidisciplinary TreatmentFederico BrugnamiNoch keine Bewertungen
- Literature Review: Periodontal AnatomyDokument68 SeitenLiterature Review: Periodontal AnatomyRoshna NarayanNoch keine Bewertungen
- Presentation 3Dokument15 SeitenPresentation 3Anchal RainaNoch keine Bewertungen
- Anatomy of the Periodontium: A Guide to the Tissues Surrounding and Supporting TeethDokument46 SeitenAnatomy of the Periodontium: A Guide to the Tissues Surrounding and Supporting TeethNathnael GebeyehuNoch keine Bewertungen
- Periodontal LigamentDokument38 SeitenPeriodontal LigamentyogeshNoch keine Bewertungen
- 4 - The Periodontium (Mahmoud Bakr)Dokument128 Seiten4 - The Periodontium (Mahmoud Bakr)MobarobberNoch keine Bewertungen
- Semina 2periodontal Ligament NUSDokument102 SeitenSemina 2periodontal Ligament NUSnusreenNoch keine Bewertungen
- Final PDLDokument100 SeitenFinal PDLDrRahat SaleemNoch keine Bewertungen
- Normal PeriodontiumDokument37 SeitenNormal PeriodontiumEslam KillineyNoch keine Bewertungen
- Chapter 4 - Dental Anatomy (Essentials of Dental Assisting)Dokument28 SeitenChapter 4 - Dental Anatomy (Essentials of Dental Assisting)mussanteNoch keine Bewertungen
- Alveolar BoneDokument26 SeitenAlveolar Bonelokesh_045Noch keine Bewertungen
- Perio DSL EssayDokument8 SeitenPerio DSL EssayIfzal MalookNoch keine Bewertungen
- Periodontal LigamentDokument65 SeitenPeriodontal LigamentReshmaa Rajendran100% (1)
- Endodontics FinalDokument114 SeitenEndodontics FinalContas AleatóriasNoch keine Bewertungen
- The Normal Periodontium 1-GingivaDokument34 SeitenThe Normal Periodontium 1-GingivaHeba S Radaideh100% (1)
- CementumDokument10 SeitenCementumAshish BisaneNoch keine Bewertungen
- Junctional EpitheliumDokument88 SeitenJunctional Epitheliumshashi kant chaudhary100% (3)
- Molecular & Cell Biology of GingivaDokument28 SeitenMolecular & Cell Biology of GingivaPoojan ThakoreNoch keine Bewertungen
- Alveolar BoneDokument47 SeitenAlveolar BoneShashi kiranNoch keine Bewertungen
- CementumDokument139 SeitenCementumpraveenmdasNoch keine Bewertungen
- Periodontium 1Dokument65 SeitenPeriodontium 1Hussain M A KhuwajaNoch keine Bewertungen
- Jaringan PeriodontalDokument45 SeitenJaringan PeriodontalSasmita Prima DaniNoch keine Bewertungen
- Taeb 487 Tooth StructureDokument14 SeitenTaeb 487 Tooth StructuremohammedNoch keine Bewertungen
- Oral and Dental HistologyDokument6 SeitenOral and Dental HistologyCésar HelenoNoch keine Bewertungen
- Structure and Functions of Alveolar BoneDokument30 SeitenStructure and Functions of Alveolar BonepadmineekrishnanNoch keine Bewertungen
- Oral HistologyDokument6 SeitenOral HistologyMr. Orange100% (2)
- Structures of The TeethDokument22 SeitenStructures of The TeethJonie HonradoNoch keine Bewertungen
- Structure and Support of Teeth and GingivaDokument22 SeitenStructure and Support of Teeth and GingivaharnageaNoch keine Bewertungen
- Periodontal Ligament Structure and FunctionsDokument39 SeitenPeriodontal Ligament Structure and Functionssamar yousif mohamedNoch keine Bewertungen
- Tooth Structure 9075Dokument2 SeitenTooth Structure 9075Andreea CojocariNoch keine Bewertungen
- 1 Tema 1 2 Anatomy PF PeriodontiumTD-75916Dokument56 Seiten1 Tema 1 2 Anatomy PF PeriodontiumTD-75916Salameh Abu MUSSANoch keine Bewertungen
- Sulcular Epithelium:: Periodontics Lec. 2Dokument7 SeitenSulcular Epithelium:: Periodontics Lec. 2زهرة الحبNoch keine Bewertungen
- Alveolar BoneDokument114 SeitenAlveolar BoneDent DealsNoch keine Bewertungen
- Anatomi Copy 121Dokument60 SeitenAnatomi Copy 121HAKAMNoch keine Bewertungen
- Alveolar BoneDokument59 SeitenAlveolar BoneMohammed hisham khan100% (7)
- 2 Normal Clinical Features of The GingivaDokument30 Seiten2 Normal Clinical Features of The Gingivaceudmd3d100% (3)
- Dentin Structure, Composition, Development and Types ExplainedDokument118 SeitenDentin Structure, Composition, Development and Types ExplainedKhalid Lafi100% (1)
- Periodontal LigamentDokument27 SeitenPeriodontal Ligamentsamar yousif mohamedNoch keine Bewertungen
- The Periodontium Tissues Supporting TeethDokument78 SeitenThe Periodontium Tissues Supporting TeethShuba Prasad100% (1)
- Week 9 Structure, Function and Repair of Hard and Soft TissueDokument4 SeitenWeek 9 Structure, Function and Repair of Hard and Soft TissueDelaney IslipNoch keine Bewertungen
- Parts of The ToothDokument22 SeitenParts of The Toothd389Noch keine Bewertungen
- Tooth AnatomyDokument31 SeitenTooth Anatomydhea wirantiNoch keine Bewertungen
- Alveolar BoneDokument25 SeitenAlveolar Bonesamar yousif mohamedNoch keine Bewertungen
- .Periodontal LigamentDokument33 Seiten.Periodontal Ligamentمصطفى احمدNoch keine Bewertungen
- PeriodontiumDokument86 SeitenPeriodontiumShahzeb MemonNoch keine Bewertungen
- 0 - Periodontal LigamentDokument82 Seiten0 - Periodontal LigamentSonali Sharma100% (1)
- Biology of Normal PeriodontiumDokument80 SeitenBiology of Normal PeriodontiumAmmar Hussain MemonNoch keine Bewertungen
- Alveolar Process: Dr. Kanza NawadatDokument22 SeitenAlveolar Process: Dr. Kanza NawadatSaud IqbalNoch keine Bewertungen
- Periodontal Ligament: RIC. Dental Students Batch 1Dokument42 SeitenPeriodontal Ligament: RIC. Dental Students Batch 1Tariq WalidNoch keine Bewertungen
- Width of PDL SpaceDokument50 SeitenWidth of PDL SpaceShruti Maroo - RathiNoch keine Bewertungen
- Terminology Used To Describe The Tissues of A Tooth: DR - Yad Raouf BDS, Efb, MrcsedDokument20 SeitenTerminology Used To Describe The Tissues of A Tooth: DR - Yad Raouf BDS, Efb, MrcsedRabarNoch keine Bewertungen
- Tissues Surrounding Teeth: PeriodontiumDokument33 SeitenTissues Surrounding Teeth: PeriodontiumSweet SumanNoch keine Bewertungen
- Basic Guide To Dental InstrumentsDokument7 SeitenBasic Guide To Dental Instrumentssinofrisa31Noch keine Bewertungen
- Lab.9 The Oral Cavity Cont. 2Dokument10 SeitenLab.9 The Oral Cavity Cont. 2bgj9cddvxhNoch keine Bewertungen
- Dental Alloys Used in ProsthodonticsDokument11 SeitenDental Alloys Used in ProsthodonticsShufeiNoch keine Bewertungen
- Local Anesthesia PDFDokument29 SeitenLocal Anesthesia PDFNana HindraNoch keine Bewertungen
- JHSFHJSDBF HGJSDGHFSD HJGHSDGBFSDDokument14 SeitenJHSFHJSDBF HGJSDGHFSD HJGHSDGBFSDNaresh TeresNoch keine Bewertungen
- Headgear Appliances - Columbia New - BWDokument8 SeitenHeadgear Appliances - Columbia New - BWNana HindraNoch keine Bewertungen
- Deep-Neck Spaces InfectionsDokument61 SeitenDeep-Neck Spaces InfectionsmuditanatomyNoch keine Bewertungen
- ASDA White Paper Final-NewcombDokument20 SeitenASDA White Paper Final-NewcomborthodontistinthemakingNoch keine Bewertungen
- Understanding Anchorage in Orthodontics-Review ArticlesDokument5 SeitenUnderstanding Anchorage in Orthodontics-Review ArticlesSoe San KyawNoch keine Bewertungen
- Task Bahasa Inggris: Kementerian Kesehatan R.I Politeknik Kesehatan Denpasar Jurusan Keperawatan Gigi TAHUN 2019Dokument8 SeitenTask Bahasa Inggris: Kementerian Kesehatan R.I Politeknik Kesehatan Denpasar Jurusan Keperawatan Gigi TAHUN 2019FadhilaNoch keine Bewertungen
- Currículo Profissional - Tamize InglesDokument7 SeitenCurrículo Profissional - Tamize InglesTamize SILVA GONCALVESNoch keine Bewertungen
- Prosthetic TreatmentDokument23 SeitenProsthetic Treatmenttristiarina0% (1)
- Evidence Based Caries PreventionDokument196 SeitenEvidence Based Caries PreventionJean PaulNoch keine Bewertungen
- Dental Anatomy Understanding The Structure and Function of TeethDokument4 SeitenDental Anatomy Understanding The Structure and Function of TeethSafeer SefiNoch keine Bewertungen
- Restorative DentistryDokument13 SeitenRestorative DentistryPriya Sargunan50% (2)
- Considerations For Orthognathic Surgery During Growth, Part 1 - Mandibular DeformitiesDokument7 SeitenConsiderations For Orthognathic Surgery During Growth, Part 1 - Mandibular DeformitiesLeonardo LamimNoch keine Bewertungen
- All RememberedDokument186 SeitenAll RememberedTariq KhalidNoch keine Bewertungen
- Impact of Molar Incisor Hypomineralization On Quality of Life in Children With Early Mixed Dentition: A Hierarchical ApproachDokument11 SeitenImpact of Molar Incisor Hypomineralization On Quality of Life in Children With Early Mixed Dentition: A Hierarchical ApproachfghdhmdkhNoch keine Bewertungen
- Oral PathologyDokument184 SeitenOral Pathologyyalahopa100% (1)
- Int Endodontic J - 2022 - Fransson - Tooth Survival After Endodontic TreatmentDokument14 SeitenInt Endodontic J - 2022 - Fransson - Tooth Survival After Endodontic TreatmentkecasweatNoch keine Bewertungen
- Dentapreg and Signum Maryland BridgeDokument4 SeitenDentapreg and Signum Maryland BridgeCherine SnookNoch keine Bewertungen
- THEORIES OF Tooth Eruption 1st SeminarDokument50 SeitenTHEORIES OF Tooth Eruption 1st SeminarShivani DubeyNoch keine Bewertungen
- KS3 Science 2009 Paper 1 Level 5-7Dokument28 SeitenKS3 Science 2009 Paper 1 Level 5-7Aryaveer Kumar100% (1)
- Kode Icd X (Gigi)Dokument5 SeitenKode Icd X (Gigi)Lia CitraNoch keine Bewertungen
- Integrated Science Form 4 Final ExamDokument14 SeitenIntegrated Science Form 4 Final ExamCHRISTOPHER SCALE100% (1)
- Oral Health ProgramDokument6 SeitenOral Health ProgramPoohlarica UyNoch keine Bewertungen
- Effective Exercises For A Short FrenumDokument2 SeitenEffective Exercises For A Short FrenumlblessingerNoch keine Bewertungen
- Dental InsuranceDokument4 SeitenDental InsuranceJason100% (1)
- Antenatal & Postnatal Care: 1. General InformationDokument7 SeitenAntenatal & Postnatal Care: 1. General InformationanishnithaNoch keine Bewertungen
- Secret Kitchen CuresDokument75 SeitenSecret Kitchen Curescharleswagner1231000100% (1)
- Somalia Standard Treatment Guidelines and Training ManualDokument154 SeitenSomalia Standard Treatment Guidelines and Training ManualAhmed Reda DoniaNoch keine Bewertungen
- Oral Hygiene Autis PDFDokument7 SeitenOral Hygiene Autis PDFNoviyana Idrus DgmapatoNoch keine Bewertungen
- Perio Endo LesionsDokument39 SeitenPerio Endo Lesionsthanhchon100% (17)
- Module 5 Anatomy I Splanchnology 1Dokument17 SeitenModule 5 Anatomy I Splanchnology 1neannaNoch keine Bewertungen
- Dental Hygiene and Periodontal DiseaseDokument7 SeitenDental Hygiene and Periodontal Diseaseapi-536835901Noch keine Bewertungen
- Keeping Teeth HealthyDokument2 SeitenKeeping Teeth HealthyMedstudNoch keine Bewertungen
- Root Resorption: Challenge To The Endodontist: Acta Scientific Dental SciencesDokument11 SeitenRoot Resorption: Challenge To The Endodontist: Acta Scientific Dental SciencesMuhammadDeniRahmanNoch keine Bewertungen
- Dental Terminology and Concepts ReviewDokument7 SeitenDental Terminology and Concepts Reviewmichal ben meronNoch keine Bewertungen
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionVon EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionBewertung: 4 von 5 Sternen4/5 (402)
- Why We Die: The New Science of Aging and the Quest for ImmortalityVon EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityBewertung: 3.5 von 5 Sternen3.5/5 (2)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisVon EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisBewertung: 4 von 5 Sternen4/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedVon EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedBewertung: 5 von 5 Sternen5/5 (78)
- The Age of Magical Overthinking: Notes on Modern IrrationalityVon EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityBewertung: 4 von 5 Sternen4/5 (13)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeVon EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNoch keine Bewertungen
- The Comfort of Crows: A Backyard YearVon EverandThe Comfort of Crows: A Backyard YearBewertung: 4.5 von 5 Sternen4.5/5 (23)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsVon EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsBewertung: 3.5 von 5 Sternen3.5/5 (3)
- Techniques Exercises And Tricks For Memory ImprovementVon EverandTechniques Exercises And Tricks For Memory ImprovementBewertung: 4.5 von 5 Sternen4.5/5 (40)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsVon EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsBewertung: 5 von 5 Sternen5/5 (1)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsVon EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsBewertung: 4.5 von 5 Sternen4.5/5 (169)
- The Obesity Code: Unlocking the Secrets of Weight LossVon EverandThe Obesity Code: Unlocking the Secrets of Weight LossBewertung: 5 von 5 Sternen5/5 (4)
- The Ultimate Guide To Memory Improvement TechniquesVon EverandThe Ultimate Guide To Memory Improvement TechniquesBewertung: 5 von 5 Sternen5/5 (34)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingVon EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingBewertung: 5 von 5 Sternen5/5 (4)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaVon EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsVon EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNoch keine Bewertungen
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisVon EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisBewertung: 5 von 5 Sternen5/5 (8)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingVon EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingBewertung: 3.5 von 5 Sternen3.5/5 (33)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Von EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Bewertung: 4.5 von 5 Sternen4.5/5 (110)
- Summary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisVon EverandSummary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisBewertung: 5 von 5 Sternen5/5 (3)
- The Happiness Trap: How to Stop Struggling and Start LivingVon EverandThe Happiness Trap: How to Stop Struggling and Start LivingBewertung: 4 von 5 Sternen4/5 (1)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeVon EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeBewertung: 4.5 von 5 Sternen4.5/5 (253)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsVon EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNoch keine Bewertungen
- The Tennis Partner: A Doctor's Story of Friendship and LossVon EverandThe Tennis Partner: A Doctor's Story of Friendship and LossBewertung: 4.5 von 5 Sternen4.5/5 (4)