Beruflich Dokumente
Kultur Dokumente
Glaukoma Dan Hipermetropi
Hochgeladen von
fuadaffanOriginalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Glaukoma Dan Hipermetropi
Hochgeladen von
fuadaffanCopyright:
Verfügbare Formate
Abstract Chapter I Introduction : Glaucoma is when the optic nerve is damaged by high pressure in the eye.
This can cause visual impairment. The particular type of glaucoma that a hypermetropic eye is prone to is called 'Acute Close Angle Glaucoma'. Although angle-closure glaucoma is often related to
an acute, painful crisis associated with blurred vision, more than 75% of patients do not have an acute attack,80 instead they have an asymptomatic course with progressive loss of the visual field similar to that in patients with open-angle glaucoma. Worldwide, a third of patients with primary glaucoma have angle-closure glaucoma.1 The proportionate vision loss in angle-closure glaucoma might be as much as twice as great as open-angle glaucoma, so half of patients blinded by glaucoma have angle-closure glaucoma.81 Epidemiological observations by Alsbirk82 documented a high prevalence of angleclosure glaucoma in Greenland, and confirmed that small eye size was a major risk factor. Data from later population-based studies in China,83 India,84 Europe,85 and Africa86 indicated that risk of developing angleclosure glaucoma increases exponentially with age, is more common in women, and has a greater prevalence in people of Asian and Indian ethnic origin than in those of European and African descent.87 People of African and European ethnic origin have a similar prevalence of angle-closure glaucoma. Because of the ethnic distribution and the large populations in which angle-closure glaucoma is more prevalent, many patients with this type of glaucoma live in Asia and India. Because eye size is partly genetically determined,88 the fact that data from twin studies lend support to a genetic eff ect in the disease is not surprising. No specific gene has yet been associated with angle-closure glaucoma. The aim of this study is to establish the association between acute angle- closure glaucoma and hypermetropia.
Chapter II Literatur Review Glaucoma :
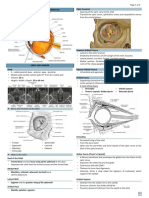
Definition : Primary acute closed-angle glaucoma is caused by the inhibition of the circulation of aqueous humour. From the cillary body, aqueous humour crosses the posterior chamber, through the pupil into the anterior chamber. The majority of fluid drains through the trabecular meshwork and Schlemm canal into the circulation through the angle of the eye. Around 10 per cent drains out via the uveo-scleral venous outflow. In closed-angle glaucoma this trabecular pathway is disrupted. The anatomy of the eye prevents the aqueous humour from passing through the pupil, inducing pupil block, which in turn leads to crowding of the anterior chamber angle, preventing any fluid from draining through the trabeculae Raised intraocular pressure (IOP) affects the optic nerve. Recent research has shown how very high IOP leads to optic disc changes in an hour.1 Factors such as a shallow anterior chamber, thin ciliary bodies, anteriorly positioned and thickened lens, a thinner iris and a hypermetropic patient increase the risk of this condition. The inadequate circulation leads to an acute rise in the IOP of the affected eye. An attack can resolve spontaneously. Patients may have experienced several previous temporary episodes. If acute glaucoma does not resolve, severe and permanent visual loss can occur. Patients with acute closed-angle glaucoma present with eye pain, nausea, vomiting, a loss of vision and haloes (rainbow coloured rings around lights). On clinical examination these patients may have a unilateral red eye, a non-reactive and oval pupd, a cloudy cornea and loss of the red reflex. They may have significant vision loss to 6/36 or worse, due to the corneal oedema. Oedema causes the hazy appearance of the cornea, which prevents visualisation of the iris and loss of the red reflex. Ischaemia of the iris prevents it from reacting to changes in avadable light. The diagnosis can be made with two symptoms out of ocular pain, nausea or vomiting, and intermittent visual blurring with haloes. As wed as three of the fodowing, raised IOP >21mmHg, corneal oedema, mid-ddated and non-reactive pupil and a shallower chamber tf there is oedema. As closed-angle glaucoma represents a significant risk to a patient's sight, there should always be a high index of suspicion in someone with a painful red eye and loss of visual acuity. Immediate treatment includes topical beta adrenaline receptor blockers and to improve outflow, intravenous acetazolomide, which suppress aqueous production. Alpha adrenaline receptor blockers are also thought to reduce IOP.2 Initiation of the inflammatory response is an important part of closed-angle glaucoma and topical steroids reduce inflammation and minimise damage to the optic nerve Pdocarpine can be used to reverse pupd block. It should be given after the initial treatment has reduced IOP, as paralysis of the iris would prevent it working if given immediately. There is a risk that pilocarpine can raise IOP as cilliary muscle contraction leads to a shallower anterior chamber. Symptomatic treatment should be given including, antiemetics (anti-sickness medication such as cyclizine) and analgesia.
Once the attack has resolved, preventative treatment involves the continuation of medication or laser iridotomy.3 Laser treatment punches a small perforation in the iris allowing aqueous humour to pass from the posterior to the anterior chamber bypassing the pupd. If the aetiology of the closed angle includes a structure behind the iris argon lasers have been used to further open the angle.4 Secondary acute open or closed-angle glaucoma can occur when an existing condition interrupts the aqueous circulation. Causes include trauma, uveitis, steroid therapy, pseudoexfoliation, pigment dispersion, lens abnormalities (including cataracts), aphakia and neovascularisation of the iris (rubeosis). Some of these conditions will have a gradual onset, it is important to exclude any existing eye disease in the history and examination. Angle-closure glaucoma Clinical features, risk factors, and pathogenesis Angle-closure glaucoma is distinguished from openangle glaucoma by the closure of the angle between the iris and cornea, obstructing outflow of aqueous humour. This obstruction often results from high resistance for aqueous movement, through the doughnut-shaped channel between the iris and lens that is 25 m in height or less in eyes with definite angle closure. Increased resistance in this iris-lens channel leads the iris to bow forward, closing off access to the trabecular meshwork and decreasing aqueous humour outflow. If present for days to weeks, this event leads to permanent adherence of the iris to the meshwork, chronically increased intraocular pressure, and eventually to glaucomatous neuropathy similar to that seen in open-angle glaucoma. The production of a hole through the iris with laser, iridotomy, removes this basic mechanism and is an initial treatment for patients with angle-closure glaucoma. Although people with angle-closure glaucoma have eyes of shorter overall length and with shallower anterior chambers than the mean in the general population, anatomic size does not explain why most people with narrow angles do not develop the disease. Additionally, small eye size alone does not explain the high prevalence of angle-closure glaucoma in Chinese people, who proportionately do not have smaller diameter eyes than do European people, but have five times the prevalence of angle-closure glaucoma.89 Abnormalities in dynamic, physiological responses seem to be indicators of which smaller eyes develop angle-closure glaucoma.7 The iris gains and loses volume with pupil constriction and dilation, presumably by exchange of aqueous humour between the iris stroma and the anterior chamber90 (figure 5). Patients with angle closure, particularly those who have an acute high intraocular pressure, do not lose enough iris volume on pupil enlargement, increasing the likelihood that the iris obstructs the angle.91 Additionally, fluid movement between the iris and lens meets greater resistance with forward movement of the lens. Individuals with angle closure seem to have expansion of the extravascular space of the choroid (between the retina and sclera), causing forward movement of the lens and intensifying the block of aqueous humour through the pupil.92 Diagnosis The definitive clinical examination to identify people at risk for angle-closure glaucoma is gonioscopy. Although several systems for gonioscopic grading exist, none has been validated in a prospective trial to measure its predictive power. Several lens types are in use, with some
allowing dynamic viewing to look for scarring (synechiae) of the iris to the meshwork-signs that permanent angle closure has begun. Present gonioscopic grading, ultrasound biomicroscopy, and optical coherence tomography evaluations cannot be used to predict with accuracy who will develop angle-closure glaucoma.93 Provocative tests for angle-closure glaucoma have been used in which the pupil is dilated, looking for an increased intraocular pressure as the outcome, but these tests have poor predictive power.94 Because the number of individuals suspected to have angle closure is greater than the number who will develop the disease, more people are treated with the initial step of iridotomy than actually need the treatment. New anterior segment optical coherence tomographic imaging measures of iris volume change and posterior segment optical coherence tomographic estimation of choroidal volume have promise as predictive tests for the development and progression of angle-closure glaucoma. Treatment In many patients with angle-closure glaucoma, the resistance at the iris-lens channel is a dominant feature, and bypassing the pupil block by making a laser hole in the peripheral iris is curative. Both eyes of patients with primary angle closure are treated with iridotomy. Even patients who have an acute angle-closure crisis with very high intraocular pressure are initially treated to make a hole in the iris. Most eyes can have successful iridotomy under topical anaesthesia produced by laser treatment. Iridotomy is well tolerated and associated with few sideeff ects,95 but better methods are needed to limit iridotomy to those suspected to have angle-closure glaucoma who are most likely to benefit.96 Although the angle appears more open after iridotomy in two-thirds of patients, the angle remains narrow after the iris hole in a third of patients; however, most of these patients who still have narrow-looking eyes do not go on to develop angle-closure glaucoma over ensuing years, even if the aff ected eye had an acute angle-closure crisis.97 Rarely, other mechanisms participate in continued angleclosure disease after iridotomy, involving direct blockade of the angle by the iris (plateau iris syndrome)98 and forward collapse of the vitreous humour (malignant glaucoma). Specific forms of laser treatment (iridoplasty) and operative surgery (vitrectomy) are used when these disorders arise, and their mechanisms and contribution to angle-closure glaucoma overall are still controversial. If angle closure has been active before iridotomy, and especially if adhesions of the iris to the meshwork have formed, glaucomatous neuropathy might have already occurred at the time of diagnosis. This advanced stage of disease necessitates the same type of treatments to lower intraocular pressure as that for open-angle glaucoma, and the same type of chronic examination schedule is used-monitoring the optic disc, nerve fibre layer, and visual field. There is controversy about the role of early lens removal in patients with angle-closure glaucoma, with some suggestions that the long-term outcome might be improved.99 Longitudinal studies are needed to establish risk factors for the occurrence and progression of angle-closure glaucoma.
Hypermetrophia Hyperopia, also known as farsightedness, longsightedness or hypermetropia, is a defect of vision caused by an imperfection in the eye (often when the eyeball is too short or the lens cannot become round enough), causing difficulty focusing on near objects, and in extreme cases causing a sufferer
to be unable to focus on objects at any distance. As an object moves toward the eye, the eye must increase its optical power to keep the image in focus on the retina. If the power of the cornea and lens is insufficient, as in hyperopia, the image will appear blurred Rays of light relected off objects in front of the eye are focused behind the retina as shown above The smaller and shorter an eye is, the more likely light from a distant object will focus beyond the retina. The focussing power of the cornea and lens are also important in causing hypermetropia
The smaller and shorter an eye is the more likely it is to develop other eye conditions. These include:
Glaucoma Squint Amblyopia
Sometimes parents and teachers notice, by the way a child acts, that their vision might be impaired. Children may have difficulty seeing text books at school. They may complain of eye strain or headache. Parents may notice that their child's eyes also occasionally squint. If parents discuss their concerns with their Family Doctor an assessment can be arranged. The family doctor may initially suggest an appointment with an optometrist. An optometrist can diagnose hypermetropia during an examination. The level of hypermetropia can be measured by shining a light through different lenses into the eye. The level of hypermetropia is measured in focussing power units called 'dioptres'. Plus units are used to describe Hypermetropia. Mild hypermetropia is between zero and plus three dioptres. Moderate hypermetropia is between plus three and ten dioptres. Severe or 'high' hypermetropia is greater than minus ten dioptres. Spectacles or contact lenses can usually sharpen vision. Sometimes the vision will not be perfect. This can be because of other problems with the eye such as microphthalmia, squint and amblyopia. Other eye conditions such as squint can be treated by operations and wearing spectacles. Laser surgery has been used successfully to treat short sight in adults and even some adults with long sight. It involves altering the shape of the cornea to focus light from objects on to the back of the eye. Because the level of hypermetropia can change during childhood and the early twenties it is never performed on children
Correlation between relationship between angle-closure glaucoma with hypermetropia associated with the power of accommodation that will narrow angle lens COA and hypertrophy of muscle siliaris. hipermetropi refraction in patients with severe abnormalities, the patient will have difficulty seeing objects which were located close to, so when they see the objects that were located near, the eye
accommodation. when the eye iris accommodation will be pushed forward and the COA will narrow angle, narrow angle COA h.aqueous causing obstructed flow. This accumulation of fluid causes increased intraocular pressure and causes the occurrence of angle closure glaucoma. moreover, when the eyes do continuous accommodation when looking at close range, causing muscle hypertrophy due to contract siliaris continuously which will lead to more narrow angle COA and exacerbate glaucoma.
Das könnte Ihnen auch gefallen
- GlaucomaDokument14 SeitenGlaucomaWilliam SumoroNoch keine Bewertungen
- Acute Closed Angle Glaucoma: AuthorsDokument6 SeitenAcute Closed Angle Glaucoma: AuthorsNgeridingNoch keine Bewertungen
- Diagnosis and Management of Malignant GlaucomaDokument3 SeitenDiagnosis and Management of Malignant GlaucomaYazmin Peñaloza RoaNoch keine Bewertungen
- Glaucoma OverviewDokument33 SeitenGlaucoma Overviewc/risaaq yuusuf ColoowNoch keine Bewertungen
- Diagnosis and Management of Pseudoexfoliation Glaucoma - American Academy of Ophthalmology PDFDokument7 SeitenDiagnosis and Management of Pseudoexfoliation Glaucoma - American Academy of Ophthalmology PDFnoviaNoch keine Bewertungen
- Study of Glaucoma in Eyes With Shallow Anterior ChamberDokument11 SeitenStudy of Glaucoma in Eyes With Shallow Anterior ChamberjincymariyamNoch keine Bewertungen
- Primary Angle Closure GlaucomaDokument17 SeitenPrimary Angle Closure Glaucomarutuparna383Noch keine Bewertungen
- Patel 2014Dokument9 SeitenPatel 2014marieNoch keine Bewertungen
- GLAUCOMADokument10 SeitenGLAUCOMAcarls burg a. resurreccionNoch keine Bewertungen
- Glaucoma Aqueous Humour DynamicsDokument25 SeitenGlaucoma Aqueous Humour Dynamicspraveen joseNoch keine Bewertungen
- GlaucomaDokument34 SeitenGlaucomabobamaryNoch keine Bewertungen
- Glaucoma and Cataract - ContentannDokument20 SeitenGlaucoma and Cataract - ContentannDR. KUMARASWAMI HEALTH CENTRE COLLEGE OF NURSING KANYAKUMARINoch keine Bewertungen
- Glaucoma Suspect: Diagnosis and Management: Risk FactorsDokument5 SeitenGlaucoma Suspect: Diagnosis and Management: Risk FactorsKrisno ParammanganNoch keine Bewertungen
- 1 SMDokument7 Seiten1 SMAriNoch keine Bewertungen
- Nursing Practice Review Ophthalmology: in This Article..Dokument7 SeitenNursing Practice Review Ophthalmology: in This Article..intan juitaNoch keine Bewertungen
- Acute Angle-Closure Glaucoma (AACG)Dokument11 SeitenAcute Angle-Closure Glaucoma (AACG)Intan AliNoch keine Bewertungen
- Angle-Closure Glaucoma - UpToDateDokument9 SeitenAngle-Closure Glaucoma - UpToDateElaine June FielNoch keine Bewertungen
- SGD LBM 3 Modul MataDokument12 SeitenSGD LBM 3 Modul MataMillatiazmi Maulida ArdianiNoch keine Bewertungen
- Vitreous HemorrhageDokument7 SeitenVitreous HemorrhageindahNoch keine Bewertungen
- Glaucoma Case ReportDokument9 SeitenGlaucoma Case Reportsuci caraswatiNoch keine Bewertungen
- Holy 3Dokument3 SeitenHoly 3Holy Fitria ArianiNoch keine Bewertungen
- Search Uptodate: Grade 1CDokument1 SeiteSearch Uptodate: Grade 1CGabriella TjondroNoch keine Bewertungen
- Congenital GlucomaDokument22 SeitenCongenital GlucomaRIYA PARVEENNoch keine Bewertungen
- Angle Closure GlaucomaDokument6 SeitenAngle Closure GlaucomaRick van DewNoch keine Bewertungen
- Glaucoma Normo TensionDokument38 SeitenGlaucoma Normo TensionRiyang Pradewa AdmawanNoch keine Bewertungen
- Showphacomrphic Glaucoma Managemnet by Surgical and Medical Management TextDokument8 SeitenShowphacomrphic Glaucoma Managemnet by Surgical and Medical Management Textdrvishalkulkarni2007Noch keine Bewertungen
- GlaucomeaDokument21 SeitenGlaucomeamalathiNoch keine Bewertungen
- Glaucoma and Ocular HypertensionDokument6 SeitenGlaucoma and Ocular HypertensionsoniasistNoch keine Bewertungen
- Aqueous Humor Outflow:: Anterior Cavity: The Lens Divides The Anterior Cavity Into Further Two ChambersDokument20 SeitenAqueous Humor Outflow:: Anterior Cavity: The Lens Divides The Anterior Cavity Into Further Two ChambersNavjot BrarNoch keine Bewertungen
- Angle Recession GlaucomaDokument1 SeiteAngle Recession GlaucomaHitesh SharmaNoch keine Bewertungen
- Methods: Risk Factors That Should Prompt Referral To An Eye Care Practitioner For Evaluation For GlaucomaDokument2 SeitenMethods: Risk Factors That Should Prompt Referral To An Eye Care Practitioner For Evaluation For GlaucomasukmaangNoch keine Bewertungen
- HHS Public Access: Role of Cataract Surgery in The Management of GlaucomaDokument13 SeitenHHS Public Access: Role of Cataract Surgery in The Management of GlaucomaayuNoch keine Bewertungen
- Surgery: BackgroundDokument22 SeitenSurgery: BackgroundJefri SandikaNoch keine Bewertungen
- American Optometric Association. Glaucoma HTTP - WWW - Aoa.org - Glaucoma - Xml.Dokument8 SeitenAmerican Optometric Association. Glaucoma HTTP - WWW - Aoa.org - Glaucoma - Xml.Adriana FallaNoch keine Bewertungen
- Chronic Closed Angle Glaucoma - StatPearls - NCBI BookshelfDokument6 SeitenChronic Closed Angle Glaucoma - StatPearls - NCBI BookshelfAngel LimNoch keine Bewertungen
- Pharmacological and Environmental Factors in Primary Angle-Closure GlaucomaDokument19 SeitenPharmacological and Environmental Factors in Primary Angle-Closure Glaucomajoydev samantaNoch keine Bewertungen
- Primary GlaucomaDokument118 SeitenPrimary GlaucomaaswanfaqihNoch keine Bewertungen
- Congenital GlaucomaDokument17 SeitenCongenital GlaucomaKevin ArielNoch keine Bewertungen
- Glaucoma Pathophysiology and DiagnosisDokument10 SeitenGlaucoma Pathophysiology and Diagnosisagus sanjayaNoch keine Bewertungen
- Ageing Eye Posterior Segment ChangesDokument6 SeitenAgeing Eye Posterior Segment ChangesirijoaNoch keine Bewertungen
- Acute Closed Angle Glaucoma: AuthorsDokument4 SeitenAcute Closed Angle Glaucoma: AuthorsRova OktavaniNoch keine Bewertungen
- Primary Open-Angle Glaucoma: SeminarDokument10 SeitenPrimary Open-Angle Glaucoma: SeminarFebry LuthunananaNoch keine Bewertungen
- Chapter 3 - Introduction To GlaucomaDokument16 SeitenChapter 3 - Introduction To Glaucoma1330658Noch keine Bewertungen
- Case Report Absolute GlaucomaDokument22 SeitenCase Report Absolute GlaucomaDewi Permatasari100% (2)
- Jurnal KoreaDokument7 SeitenJurnal KoreachindiaNoch keine Bewertungen
- Aafp Open Angle Glaucoma PDFDokument8 SeitenAafp Open Angle Glaucoma PDFdwi kartikaNoch keine Bewertungen
- New Management Strategies For Ectopia LentisDokument14 SeitenNew Management Strategies For Ectopia LentisximoNoch keine Bewertungen
- A Laser Peripheral Iridotomy Would Most Likely Relieve AngleDokument2 SeitenA Laser Peripheral Iridotomy Would Most Likely Relieve AngleGlaucoma UnhasNoch keine Bewertungen
- Glaucoma and CataractDokument30 SeitenGlaucoma and CataractJayselle ArvieNoch keine Bewertungen
- Angle Closure GlaucomaDokument10 SeitenAngle Closure GlaucomaGreselda TandudjajaNoch keine Bewertungen
- Pigmentary GlaucomaDokument9 SeitenPigmentary GlaucomaIim Syahida ZurifaNoch keine Bewertungen
- GLUACOMADokument43 SeitenGLUACOMAJoanna RachelNoch keine Bewertungen
- Eye Docs GlaucomaDokument147 SeitenEye Docs GlaucomaMuneeb ShahzadNoch keine Bewertungen
- Glaucoma Note (DR - Abeba)Dokument17 SeitenGlaucoma Note (DR - Abeba)creativejoburgNoch keine Bewertungen
- GlaucomaDokument9 SeitenGlaucomaNil NilNoch keine Bewertungen
- Glaucoma, Pseudoexfoliation: Emedicine Specialtiesophthalmologyintraocular PressureDokument9 SeitenGlaucoma, Pseudoexfoliation: Emedicine Specialtiesophthalmologyintraocular PressureChintya Dwi PutriNoch keine Bewertungen
- A. Primary GlaucomaDokument5 SeitenA. Primary GlaucomasekiannNoch keine Bewertungen
- Dr. Liesa Zulhidya, SP.M: GlaucomaDokument37 SeitenDr. Liesa Zulhidya, SP.M: GlaucomaShapira alNoch keine Bewertungen
- The Human Eye PowerpointDokument28 SeitenThe Human Eye Powerpointapi-325864985Noch keine Bewertungen
- Parts of The EarDokument5 SeitenParts of The EarThons Nacu LisingNoch keine Bewertungen
- Chronic Dacryocystitis Case PresentationDokument19 SeitenChronic Dacryocystitis Case Presentationr7ptzc5kcmNoch keine Bewertungen
- Physical AssessmentDokument19 SeitenPhysical Assessmentsilentscream0618Noch keine Bewertungen
- Glaucoma LectureDokument166 SeitenGlaucoma LectureSonali Gupta100% (1)
- Ophthalmic Dictionary and Vocabulary Builder For Eye Care ProfessionalsDokument431 SeitenOphthalmic Dictionary and Vocabulary Builder For Eye Care ProfessionalsPutri Rosalina TamzilNoch keine Bewertungen
- Bowes 2013Dokument5 SeitenBowes 2013Salmadiar RiskaNoch keine Bewertungen
- Cap 18 Raices Sist SensorialDokument2 SeitenCap 18 Raices Sist SensorialSandra OrtizNoch keine Bewertungen
- Integumentary SystemDokument4 SeitenIntegumentary SystemSonali PawarNoch keine Bewertungen
- Kurva Baku: 0.8 1 F (X) 0.08455 X 0.0402999999999999 R 0.962341067113597 Series2 Linear (Series2)Dokument9 SeitenKurva Baku: 0.8 1 F (X) 0.08455 X 0.0402999999999999 R 0.962341067113597 Series2 Linear (Series2)Yusup AhmadiNoch keine Bewertungen
- Corneal Drawing and Other StructureDokument2 SeitenCorneal Drawing and Other StructureOden Mahyudin50% (2)
- Eye Movements GuytonDokument10 SeitenEye Movements GuytonDavis KallanNoch keine Bewertungen
- Introduction To Eye Disorders-1Dokument11 SeitenIntroduction To Eye Disorders-1bhavani GNoch keine Bewertungen
- Andrews - Chapter 2 - Cutaneous Signs and DiagnosisDokument18 SeitenAndrews - Chapter 2 - Cutaneous Signs and DiagnosisAngeli Ramos-Estrella100% (1)
- What Order Should I Apply Skin Care ProductsDokument5 SeitenWhat Order Should I Apply Skin Care ProductsLenard GarxiaNoch keine Bewertungen
- Hifema: Dr. Bobi Ahmad Sahid, S.KepDokument21 SeitenHifema: Dr. Bobi Ahmad Sahid, S.Kepdr.Bobi Ahmad Sahid, S.KepNoch keine Bewertungen
- QuestionnaireDokument2 SeitenQuestionnaireLim Zi Xuan100% (1)
- Vestibular Function and Anatomy RatnaDokument36 SeitenVestibular Function and Anatomy RatnaRatna WindyaningrumNoch keine Bewertungen
- A Project On " Human Eye": Submitted To-Submitted byDokument13 SeitenA Project On " Human Eye": Submitted To-Submitted byaman1990100% (1)
- (Ophtha) 1.1 Anatomy of The EyeDokument4 Seiten(Ophtha) 1.1 Anatomy of The EyePatrick BautistaNoch keine Bewertungen
- Assessment of The Ears - StudentDokument8 SeitenAssessment of The Ears - StudentSherinne Jane CariazoNoch keine Bewertungen
- Accomodation of EyeDokument11 SeitenAccomodation of EyeThadei Mruma100% (1)
- Cataract InformationDokument25 SeitenCataract InformationDr.K.M. AbdullaNoch keine Bewertungen
- UCL Age Redefining LMSDokument36 SeitenUCL Age Redefining LMSsumitbharuka907Noch keine Bewertungen
- Daftar Pustaka: Orphanet J Rare Diseases. 2012 7:57Dokument3 SeitenDaftar Pustaka: Orphanet J Rare Diseases. 2012 7:57fidyaNoch keine Bewertungen
- Dermabrasion Chemabrasion Laser ResurfacingDokument76 SeitenDermabrasion Chemabrasion Laser Resurfacingpilyoungg1994100% (1)
- Cauliflower Ear: Cauliflower Ear Is An Irreversible Condition That Occurs When TheDokument5 SeitenCauliflower Ear: Cauliflower Ear Is An Irreversible Condition That Occurs When TheCorneliu PaschanuNoch keine Bewertungen
- Learning Material Topic 7 Eyes and Ears AssessmentDokument4 SeitenLearning Material Topic 7 Eyes and Ears AssessmentDevi NurhidayatiNoch keine Bewertungen
- Kuliah Glaukoma Dr. Nuri, SPMDokument58 SeitenKuliah Glaukoma Dr. Nuri, SPMPutri Widya LarasatiNoch keine Bewertungen
- Physiol Toric Calculator: With Abulafia-Koch Regression FormulaDokument1 SeitePhysiol Toric Calculator: With Abulafia-Koch Regression FormuladeliNoch keine Bewertungen