Beruflich Dokumente
Kultur Dokumente
Mental Health Weekly WhatsMyM3
Hochgeladen von
OTMMediaOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Mental Health Weekly WhatsMyM3
Hochgeladen von
OTMMediaCopyright:
Verfügbare Formate
Special Issue: Mental Health Innovations
Volume 22 Number 41 October 29, 2012 Print ISSN 1058-1103 Online ISSN 1556-7583
IN THIS ISSUE
Behavioral health care providers in Arizona are co-locating behavioral health and primary care services with an emphasis on caring for the whole health needs, including nutrition and exercise, of consumers with serious mental illnesses. The collaborative care model teams include peers, health navigators, case managers, psychiatrists, physicians and nurse practitioners. . . . See story, top of this page Innovative screening tool recognizes multiple MH disorders . . . See page 3 New app to help consumers with anxiety disorders and compulsions . . . See page 4 Novel instrument helps parents assess ADHD treatment goals . . . See page 6 SAMHSA no longer accepting paper applications for grants . . . See page 8
Arizona co-located care models emphasize whole health approach
The Affordable Care Act (ACA) has pointed a spotlight on the behavioral health field, with an emphasis not just on coordinated and integrated care delivery for consumers with serious mental illness who have comorbid health conditions, but with a clear focus on lifestyle changes that include the support of a collaborative care team of mental health clinicians, nurses, primary care providers (PCPs) and peers. Partners in Recovery, a community mental health center in Phoenix, Ariz., launched a Private Practice Model of Integrated Care pilot in spring 2011, with the goal to break down barriers integrating physical and mental healthcare, achieve better overall health outcomes and lower healthcare costs. The agency is one of four in Mar-
Bottom Line
Innovative healthcare delivery models call for the use of health and wellness coaches, and on-site integrated labs and pharmacies. The models are improving the efficiency of mental health and physical health information and coordination.
icopa County serving consumers with serious mental illnesses in colocated settings. The other three are the Southwest Network, Choices Network and People of Color Network. This is an opportunity to reverse the negative literary trajectory regarding the life-span reduction for consumers with serious mental illness [SMI], Christy Dye, CEO of Recovery Innovations, Inc., a commuSee ARIZONA page 2
WEBSITE
DuPont earns national accolades for basic MH awareness training
At its numerous corporate locations around the world, the science and engineering giant DuPont is seeking to shatter the image of cold, uncaring workplaces in the world of big business. DuPonts simple approach to enhancing employees awareness of mental health issues will be honored next month with a National Alliance on Mental Illness (NAMI) Seeds of Hope award at the associations annual gala. Having grown out of the economic turmoil in Greece and other European countries where DuPont has operations, the companys ICU Mental Health program will have been implemented worldwide by the end of this year. The program made its U.S. debut last January and has been rolled out in waves across the country since then, according to Paul Heck, DuPonts global manager
See DUPONT page 5
FIND US ON
Bottom Line
The ICU Mental Health initiative emphasizes simple steps that employees can take to identify and address mental health concerns they observe in a co-worker.
mhwnewsletter
2012 Wiley Periodicals,Inc. View this newsletter online at wileyonlinelibrary.com DOI: 10.1002/mhw.20351
A Wiley Periodicals, Inc. publication. wileyonlinelibrary.com
Mental Health Weekly October 29, 2012
ARIZONA from page 1
nity mental health center in Phoenix, told MHW. On average, the mortality rate for consumers with serious mental illness is 25 years, she said. In Arizona, consumers with SMI are dying 32 years earlier than the general population, said Dye. Dye added, With the national focus on healthcare reform, and expanding access/quality of treatment for chronic medical conditions among persons with SMI, our integrated health home in behavioral health settings, coupled with peerdelivered health and wellness coaching services, is a significant innovation with true potential to impact the lifespan disparity of 25-32 years. The heart of the integrated model is operating a medical clinic that is co-located with behavioral healthcare outpatient services at one of the Recovery Innovations campuses in Maricopa County, said Dye. A PCP is co-located on-site to provide medical care for patients with serious mental illness. The scope of services includes physical examinations and preventative healthcare and screening exams, including prostate exams and vaccination evaluation and administration. Typically, PCPs see about four or five patients in an hour, said Dye. In our field 30 minutes with people with a serious mental illness is not
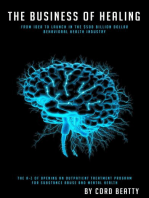
Objective lifestyle changes
(Modified lifestyle after PCP counseling)
Participates in wellness activities N=69 Stopped or decreased alcohol/drug use N=28 Stopped or decreased smoking N=102 Dietary changes N=87 Exercise initiated N=84 0% 10% 20% 30% 40% 50%
Source: Partners in Recovery, LLC and Trinity Adult Medicine, 2012
enough time, she said. The care for patients at the center is coordinated by a psychiatrist or nurse practitioner and the PCP. Staff also includes health coaches who assist program participants with healthy eating, and exercising, for example, she noted. (See graph, above.) The program includes peers as employees who are already advanced in their recovery process, said Gregory Gale, M.D., vice president of clinical services and chief medical officer at Partners in Recovery. Theyre working with program participants to help them develop their health and wellness goals, he said. Peers can also serve as role models for the participants, he said. Part of our approach is to give people the tools and skills to take
some action [regarding their healthcare] once they leave the doctors office, Gale told MHW. Consumers with mental illness can often be uncomfortable in the waiting room of PCPs, he said. Subsequently, they avoid going to the doctors office. They feel that PCPs tend to gloss over their physical symptoms and chalk it up to their behavioral health problems. Some of the disconnect between physicians and behavioral health patients can be attributed to physicians not feeling well trained in behavioral healthcare or they may have concerns about being reimbursed properly, said Gale. Many of the consumer participants who had completed health risk assessments had one thing in common: they did not feel they had any
Executive Managing Editor Karienne Stovell Managing Editor Valerie A. Canady Contributing Editor Gary Enos Editorial Assistant Elizabeth Phillips Production Editor Douglas Devaux Executive Editor Isabelle Cohen-DeAngelis Publisher Sue Lewis
Mental Health Weekly (Print ISSN 1058-1103; Online ISSN 1556-7583) is an independent newsletter meeting the information needs of all mental health professionals, providing timely reports on national trends and developments in funding, policy, prevention, treatment and research in mental health, and also covering issues on certification, reimbursement, and other news of importance to public, private nonprofit, and for-profit treatment agencies. Published every week except for the second Monday in April, the second Monday in July, the first
Monday in September, the last Monday in November and the last Monday in December. The yearly subscription rates for Mental Health Weekly are: Print only: $695 (individual, U.S./Can./Mex.), $839 (individual, rest of world), $5433 (institutional, U.S.), $5577 (institutional, Can./Mex.), $5625 (institutional, rest of world); Print & electronic: $765 (individual, U.S./Can./Mex.), $909 (individual, rest of the world), $6251 (institutional, U.S.), $6395 (institutional, Can./Mex.), $6443 (institutional, rest of the world); Electronic only: $555 (individual, worldwide), $5433 (institutional, worldwide). Mental Health Weekly accepts no advertising and is supported solely by its readers. For address changes or new subscriptions, contact Subscription Distribution US, c/o John Wiley & Sons, Inc., 111 River Street, Hoboken, NJ 07030-5774; (888) 378-2537; e-mail: subinfo@wiley.com. 2012 Wiley Periodicals, Inc., a Wiley Company. All rights reserved. Reproduction in any form without the consent of the publisher is strictly forbidden. Mental Health Weekly is indexed in: Academic Search (EBSCO), Academic Search Elite (EBSCO), Academic Search Premier (EBSCO), Current Abstracts (EBSCO), EBSCO Masterfile Elite (EBSCO), EBSCO MasterFILE Premier (EBSCO), EBSCO MasterFILE Select (EBSCO), Expanded Academic ASAP (Thomson Gale), Health Source Nursing/ Academic, InfoTrac, Student Resource Center Bronze, Student Resource Center College, Student Resource Center Gold and Student Resource Center Silver. Business and Editorial Offices: John Wiley & Sons, Inc., 111 River Street, Hoboken, NJ 07030-5774; e-mail: vcanady@wiley.com. To renew your subscription, contact Subscription Distribution US, c/o John Wiley & Sons, Inc., 111 River Street, Hoboken, NJ 07030-5774; (201) 748-6645; e-mail: subinfo@wiley.com.
It is illegal under federal copyright law to reproduce this publication or any portion of it without the publishers permission.
Mental Health Weekly DOI: 10.1002/mhw
October 29, 2012 Mental Health Weekly
medical problems when in fact they had high-risk medical problems, said Gale. They were reluctant to seek general healthcare, he said. The idea is to bring the doctor to them, added Dye. The start-up costs for the pilot program ran about $6,000, said Dye. That was the cost for the private practice doctor to be embedded in the behavioral health clinic, she said. That was unbelievably cheap, said Dye. Partners in Recovery has two more integrated care programs planned with community federally qualified health centers (FQHCs), she said. They have also hired more than 40 peer and health and wellness staff, she said. report. The pilot has since ended and the program is ongoing, said Dye. A big part of co-locating the doctor on-site is in helping consumers access care, she said. It isnt integration unless the medical professionals are talking to one another, said Dye. If theyre not sharing the information and making sure the medications dont conflict with one another, its not really integration. tegrated health home; (2) a virtual health home; and (3) a person-centered medical home in the community linked with a PCP. The care collaboration team for all three models includes health navigators and peers who work with individuals to ensure that they understand their wellness goals, said Len. The team is rounded out with a case manager, psychiatrist, nurse practitioner, community care coordinator and other family and community support, he said. The PCN has so far seen reductions in reduced hospitalization and re-hospitalization of the program participants, said Len. Were fortunate that Magellan, the RBHA, has provided funding for
People of Color Network
The People of Color Network (PCN), a nonprofit behavioral health provider organization in Phoenix is also pilot-testing three care coordination models, said Toms Len, CEO of the People of Color Net-
Program responses, lessons learned
A report of the program found that one-half of 250 participants revealed they had a PCP before the center created the co-located opportunity, she said. They switched to the PCP at Partners in Recovery because it was more convenient for them, she said. The pilot has resulted in reductions in blood pressure and in lipid profiles. Participants have overall been pleased with the convenience and the care coordinated activities, said Dye. According to the program report, it would have helped to have an integrated lab and pharmacy on the premises. The program could have been enhanced by a comprehensive health and wellness program including peer wellness coaches, according to the program
Many of the consumer participants who had completed health risk assessments had one thing in common: they did not feel they had any medical problems when in fact they had high-risk medical problems.
Gregory Gale, M.D.
work. Were taking a bidirectional approach to have direct care clinics and primary and mental health clinics serving adults with serious mental illness, Len told MHW. This is a really exciting time for health innovations. The three models are (1) an in-
provider networks to manage direct care clinics to implement care coordination models, he said. We need a variety of integrated care coordination models, he said. This is not a one size fits all. In Maricopa County, we have a large geographic [region] to cover.
Innovative screening tool recognizes multiple MH disorders
An innovative multidimensional screening tool is helping mental health and primary care clinicians with early and simultaneous identification of depression, bipolar disorder, post-traumatic stress disorder (PTSD) and anxiety in less time than single screening instruments. Research has determined that the M-3 was helpful in reviewing patients
Mental Health Weekly DOI: 10.1002/mhw
Bottom Line
Early identification of various mental health conditions can help improve treatment options and improve efficiency in healthcare delivery.
emotional health and can help lower the number of misdiagnoses. There are presently several vali-
dated self-administered instruments to detect a single disorder in health care settings for the assessment of mental illnesses, including the PHQ-9 for depression, the GAD [Generalized Anxiety Disorder]-7, the CAPS [Clinician-Administered PTSD Scale], and the MDQ [mood disorder questionnaire] for bipolar
Continues on next page
A Wiley Periodicals, Inc. publication. View this newsletter online at wileyonlinelibrary.com
Mental Health Weekly October 29, 2012
Continued from previous page
disorder. The developmental process for the screening tool started about eight or nine years ago, said Steven Daviss, M.D., co-chair of the CCHIT (Certification Commission for Health Information Technology) Behavioral Health Work Group and chair of the American Psychiatric Association (APA) Committee on Electronic Health Records. Mental health experts, physicians and researchers, including some at NIMH [National Institute of Mental Health], realized that there was no tool that was developed to screen for multiple conditions, particularly bipolar depression, Daviss told MHW. The My Mood Monitor (M-3) is considered a valid and efficient onepage tool for screening multiple common psychiatric illnesses in mental health and primary care settings said Michael Byer, president of M-3 Information, LLC in Rockville, Md. The (M-3) tool helps in the recognition and treatment of mental health by providing a score that indicates a risk of suffering from any mental health disorder, he said. It offers a specific view showing the diagnostic risk of suffering from anxiety, depression, bipolar disorder or PTSD, Byer told MHW.Clinicans can refer harder cases to a specialty provider, he said. In a collaborative care model, the screening tool allows for the whole care team to share the information before and after the referral, said Byer.
who were seeking primary care at an academic family medicine clinic between July 2007 and February 2008. They used a 2-step scoring procedure to make screening more efficient. The main outcomes measured were the sensitivity and specificity of the M-3 for major depression, bipolar disorder, any anxiety disorder, and PTSD, a specific type of anxiety disorder. Using a split sample technique, analysis proceeded from determination of optimal screening thresholds to assessment of the psychometric properties of the self-report instrument using the determined thresholds. Researchers used the Mini International Neuropsychiatric Interview
as the diagnostic standard. Feasibility was assessed with patient and physician exit questionnaires. According to the study, the M-3 checklist took less than 5 minutes to complete, and less than 1 percent of participants reported lacking sufficient time to complete it. Approximately 70 percent of participants reported talking to their clinician about mood or feelings; among those who did, 70 percent did so for at least 1 minute. Sixty-three percent of all participants reported that the M-3 helped them talk to their doctors about their mood or feelings. Among participants assigned a MINI diagnosis, 75 percent stated that the M-3 facilitated talking to their clini-
New app to help consumers with anxiety disorders and compulsions
The Mayo Clinic on Oct. 3 announced its debut of a self-help tool that assists people in reducing fears and worries ranging from extreme shyness to obsessions and compulsions. Mayo Clinic officials say the new app can also help consumers fight anxieties between sessions with their healthcare provider. The app, called Anxiety Coach, can be used on the Apple iPhone, iPad and iPod touch. The strategies used in Anxiety Coach are based on cognitive behavioral therapy, an effective psychotherapy for fear and worries, said officials. In cognitive behavioral therapy, people increase their confidence by gradually confronting situations that they have avoided out of fear. Research has demonstrated that cognitive behavioral therapy is more effective for anxiety than other approaches that rely on teaching people to relax, said officials. The app really challenges people to face their fears, as opposed to other apps that focus on relaxation strategy but dont get to the core of what is helpful in the long term, said Stephen Whiteside, Ph.D., director of the Pediatric Anxiety Disorders Program at Mayo Clinic. Features of the Mayo Clinic Anxiety Coach include: a short self-test to measure the severity of fears and worries; the ability to design a personal plan to target individual fears and worries; a library of more than 500 activities that people have found to help master a variety of fears and worries, including social anxiety, obsessions and compulsions, specific fears, separation anxiety, panic attacks, trauma-related anxiety and general worries; the ability to track anxiety while challenging fears and worries in real-life situations; the ability to record and view progress; and tools to learn about when anxiety becomes a problem and how to seek treatment. For more information, visit www.mayoclinic.org.
M-3 checklist study
Daviss said the M3 checklist was validated in a study conducted by University of North Carolina researchers and published in the March/April 2010 issue of the Annals of Family Medicine. In the study, Feasibility and Diagnostic Validity of the M-3 Checklist: A Brief, Self-Rated Screen for Depressive, Bipolar, Anxiety, and Post-Traumatic Stress Disorders in Primary Care, Researchers enrolled a sample of 647 consecutive participants ages 18 years and older
It is illegal under federal copyright law to reproduce this publication or any portion of it without the publishers permission.
Mental Health Weekly DOI: 10.1002/mhw
October 29, 2012 Mental Health Weekly
cian about mood or feelings. The study noted that the M-3 potentially can reduce missed psychiatric diagnoses and facilitate proper treatment of identified cases. The M-3 can facilitate the clinical assessment by identifying symptoms requiring fuller exploration and highlighting the patients level of impairment. Researchers said this study confirmed the validity of the M3 Checklist as a diagnostic tool, utilizing the MINI (Mini International Neuropsychiatric Interview) as a gold standard. Researchers wanted to develop a tool that can screen for multiple mental health conditions, said Daviss. The patient-reported, multidimensional M3 misses fewer cases of depression, bipolar disorder, and anxiety disorder, than the PHQ-9, MDQ and GAD-7, while maintaining a very good specificity and it only takes three minutes, he said. According to research, it takes less than 30 seconds to review, said Byer. An instrument with similar ability, the MINI mental status exam, takes 20 minutes and [requires] a person to administer. The M3 is not designed to diagnose illness on its own, said Byer. Rather, it is meant to elicit symptoms that may indicate a mood or anxiety disorder. Primary care physicians would use the M3 screen results as a basis for formulating a diagnosis and treatment. In cases where a final diagnosis is unclear, referral to a specialist may be recommended, he said. for the whole care team to share the information before and after the referral. Program officials have also developed the WhatsMyM3 application for consumers, allowing them to self-screen and track their M3 score over time, referring them to clinicians for evaluation and treatment. The WhatsMy3 app is also designed to be integrated into the doctors offices via the M3Clinician.com which interfaces with electronic medical records applications and is reimer they are 85 percent at risk for any disorder via the MINI and one out of ten are not likely to be suffering from any disorder, he said. The screening tool releases a report that provides clinicians with an overall score and then places a person on the clinical map showing diagnostic risk for one of four disorders, said Byer. The ability of the M3 to present information this way helps call focus to patients at risk. The information helps patients and their doctors recognize the need and focuses on options of care, he added. The M3 is a great tool on a number of different levels, said Mike Lardiere, vice president for HIT and strategic development for the National Council for Community Behavioral Healthcare. It can help behavioral health organizations to better manger their population. It can be integrated with electronic health records for a more seamless application, he said. Many clinicians are still trying to figure out a way to build the PHQ-9 into an EHR, said Lardiere. Behavioral health providers are encouraged to use quantitative tools that can be tracked over time, he said. Its the type of screening we all need to use more of in the future. For additional information, visit www.m3clinician.com.
Renew your subscription online at www.mentalhealthweeklynews.com
According to research, it takes less than 30 seconds to review.
Michael Byer
bursable through third party payors, said program officials. Byer added, M3 started as a consumer offering and over the last year we added the clinician side [M3Clinician] after completing our patient engagement research. The M3Clinician.com is a web-based portal for clinicians who want to use the multidimensional M3 to screen and track progress across their entire patient population, he noted. If a persons score is 33 or great-
Risk level information
Byer said M3 is considered revolutionary because it can provide clinicians with information about risk levels for major depression, PTSD, bipolar disorder, and anxiety disorders. Byer said the tool can lead to less mistreated cases and better treatment. Byer hopes the tool will help PCPs make more appropriate referrals to mental health clinicians, he said. It helps [PCPs] to refer the harder cases, he said. In a collaborative care model it allows
Mental Health Weekly DOI: 10.1002/mhw
DUPONT from page 1
of employee assistance and work/ life services. DuPonts approach to mental health awareness avoids technical detail about mental health diagnoses and symptoms, opting instead simply to encourage employees to lend a hand when they observe a coworker who appears to be in emotional distress. The pace of life today is so fast that the common niceties of life just slip by, Heck told MHW. We want
to convey to employees that its OK just to say, Are you OK?
Program origins
Heck said the idea for ICU Mental Health originated with the concerns of a DuPont employee assistance program (EAP) regional manager based in London. As economic conditions in Greece and other European countries were worsening, the manager grew increasingly worried that many DuPont employees
Continues on next page
A Wiley Periodicals, Inc. publication. View this newsletter online at wileyonlinelibrary.com
Mental Health Weekly October 29, 2012
Continued from previous page
were coming into work stressed and feeling isolated. Certainly these were not surprising reactions among residents of countries on the brink of economic collapse. The idea became one of recognizing the support role that workplace peers can play for one another. In order to nurture this, DuPont would come up with a simple approach to increasing mental health awareness, in a format easily translatable into multiple languages for its worldwide workforce. DuPont chose to work with the Harrisburg, Pa.-based strategic communications agency JPL to design the materials for the program. The major learning tool used in the initiative is an animated PowerPoint presentation with numerous voiceover options, depicting characters representing DuPont employees. The companys workers are expected each month to attend a safety meeting, Heck said, and ICU Mental Health is one of the initiatives that are rotated into these meetings. The acronym ICU has a double meaning in this programs context. Beyond the common intensive care unit reference, it also signifies the phrase I see you, pointing out the awareness of anothers distress that the program seeks to highlight. Heck emphasized that the presentation to employees does not probe deeply into the possible clinical explanations for a persons distress. The content is designed to minimize the stigma of a mental illness, he said. He added, A lot of us in the healthcare profession very quickly can get into great detail, and thats
not what most people need or want to hear. The letters in ICU refer in this program to identifying a person in distress, connecting with the person (showing a desire to help), and understanding the way forward together. In terms of the latter, the solution might be as simple as a conversation over a cup of coffee. In cases where more hands-on assistance from a professional might be necessary, employees are encouraged to make their colleagues aware of resources available through the companys EAP and medical services.
Program effects
Heck said that it is not possible to tie changes in employee service utilization rates to just one factor, but he did point out that since the rollout of ICU Mental Health in the United States at the beginning of this year, there has been a 15 to 20 percent increase in service utilization. Beyond that, The anecdotal information we hear from colleagues is that the perception of the message is so positive, Heck said. Were telling them, We want you to care, to be human. Its a warm message to open a meeting with. Heck added, Most people come to work not thinking about work as a place for this kind of emotional support. The initiative could very well take on added importance in the coming weeks, given this weeks news of significant planned layoffs at DuPont in the wake of the latest company earnings report. NAMI will present a Seeds of Hope award to DuPont at the alliances annual gala on Nov. 7 in New York City. A NAMI official did not reply to inquiries from MHW for this article, but Heck said that from what he has heard about NAMIs perspective on ICU Mental Health, It was the most innovative approach they had seen a large employer take to destigmatize mental illness in the workplace. DuPont has had a lengthy history of involvement in behavioral health issues, Heck said, having operated an alcohol counseling program in the company as far back as the early 1940s well before the nation had an addiction treatment infrastructure in place.
Most people come to work not thinking about work as a place for this kind of emotional support.
Paul Heck
The initiative does not speak to employees rank or chain-of-command issues when urging workers to reach out to others. First were humans, and then were employees and supervisors, Heck said. ICU Mental Health, according to Heck, speaks to two of the four core values in the company: safety and health, and respect for people (the other core values are highest ethical practice and environmental stewardship). The ICU program started in Europe in the winter of 2011, and materials now have been translated into six languages.
Novel instrument helps parents assess ADHD treatment goals
Researchers have developed a valid and reliable instrument to help parents measure preferences and goals for attention deficit hyperactivity disorder (ADHD), which they say can also help clinicians more easily comply with national treatment guidelines for ADHD that emphasize shared decision making (SDM), according to a new study published in the September issue of Academic Pediatrics. According to the study, Development of an Instrument to Measure Parents Preferences and Goals for the Treatment of Attention DeficitHyperactivity Disorder, SDM involves the active participation of
Mental Health Weekly DOI: 10.1002/mhw
It is illegal under federal copyright law to reproduce this publication or any portion of it without the publishers permission.
October 29, 2012 Mental Health Weekly
both clinicians and families in treatment decisions, the exchange of information, discussion of preferences and a joint determination of the treatment plan. This process helps parents and clinicians balance the risks and benefits of different options in the context of personal values, the study stated. SDM advances many of the goals of mental healthcare transformation, previously identified by the Presidents New Freedom Commission on Mental Health, the Institute of Medicine and others, according to the Substance Abuse and Mental Health Services Administration. Although ADHD has many adverse consequences, families, especially those in minority groups, are often reluctant to access effective treatments for ADHD, which include both stimulant medication and behavior therapy, alone or in combination, the study stated. Parents of children with ADHD face tough treatment decisions, Alexander G. Fiks, M.D., clinical assistant professor of research at the University of Pennsylvania School of Medicine and lead author, told MHW. SDM would enable parents to be less regretful about the choices they make. For pediatricians and clinicians, the pace of the office may not allow for an in-depth conversation about treatment goals, he said. velopment and emotional regulation, the study indicated. Ultimately, they developed a draft instrument with three separate sections: (1) medication treatment preferences; (2) behavior therapy treatment preferences; and (3) treatment goals, which included a range of indicators from not at all to definitely following such comments as My child needs to be better at staying out of trouble at school or My child needs to be more caring toward adults in our family. Researchers recruited 237 parents who had children who were between 6 and 12 years of age, enrolled in grades kindergarten or higher and had been diagnosed with ADHD within the last 18 months. The participants were recruited from four urban and four suburban primary care practices Among the goal domains and consistent with existing literature on ADHD, academic achievement was the most commonly endorsed goal, rated greatest by 52 percent of the study population. However, 46 percent of parents most wanted to address behavior problems, and 7 percent interpersonal relationships. According to the study, the analyses demonstrate that preferences for both medication and behavior therapy are multidimensional constructs. Salient barriers to treatment for individual families may be better recognized by use of the preference measures, they wrote. Fitz added further research will help determine how doctors and families can use the instrument more effectively. By measuring goals and tracking progress toward them, researchers and clinicians may also be better
Parents of children with ADHD face tough treatment decisions.
Alexander G. Fiks, M.D.
Research process
The research to develop the ADHD Preference and Goal Instrument unfolded over the last five years, said Fiks. We initially did interviews with affected families and with physicians about SDM, he said. We also engaged experts, parents, psychologists and psychiatrists. That was important. Although researchers found no instrument that directly captured ADHD treatment goals, they considered items from the Life Participation Scale for ADHD, an instrument that assesses treatment-related improvements in adaptive functioning, including quality of life, social deMental Health Weekly DOI: 10.1002/mhw
within the Childrens Hospital of Philadelphia (CHOP) Pediatric Research Consortium, a primary care practice-based research network, and the CHOP Center for Management of ADHD.
Results
The results of the study indicate that families consider goals in three broad domains: academic achievement, behavior compliance and interpersonal relationships. Highlighting the need to coordinate ADHD care, each domain spans more than one setting; academic achievement depends upon success in the classroom and homework completion, behavior compliance necessitates children following both family and school rules, and improving interpersonal relationships requires addressing interactions with teachers, peers and family.
able to assess if current treatments are helping families achieve the outcomes that they most value, researchers wrote. Such an approach may help both families and clinicians promptly identify and troubleshoot barriers to treatment success and keep families engaged in the treatment process, they said. The ADHD Preference and Goal Instrument can be used in any context for discussing treatment options with mental health professionals, school mental health program administrators, and psychiatrists and psychologists, Fiks said. Anyone involved in the care of people with ADHD will find it helpful, he said.
For more MH information, visit
www.wiley.com
A Wiley Periodicals, Inc. publication. View this newsletter online at wileyonlinelibrary.com
Mental Health Weekly October 29, 2012 BRIEFLY NOTED
SAMHSA no longer accepting paper applications for grants Beginning Fiscal Year 2013, SAMHSA discretionary grant applications, including new and continuation, must be submitted electronically through http://grants.gov. SAMHSA will not accept paper applications except when a waiver of this requirement is approved by SAMHSA. Individual applicants may request a waiver of electronic submission, for instance, if they do not have the technological means or their physical location receives poor quality or intermittent connection to the Internet. More information about a waiver and the process to apply will be forthcoming on the SAMHSA website in November and in each funding announcement. While registration takes approximately three to five business days, Grants.gov recommends that applicants allow four weeks for completion of all steps in the registration process. Information on the advance registration necessary to submit applications may be found on the portal website at http://1.usa.gov/R6vJIM. UCLA Dentistry receives grant to develop PTSD saliva test A team of researchers led by Vivek Shetty, M.D., a professor at the UCLA School of Dentistry, has received a $3.8 million research grant to develop a panel of salivary stress biomarkers that will allow early recognition of emerging mental health disorders and permit preemptive psychological care. Researchers will repeatedly conduct psychological assessments and obtain saliva samples over a six-month period among a group of 600 individuals who have recently experienced a serious physical injury or sexual assault, and then use sophisticated analytical techniques to determine the levels of the individual salivary biomarkers at different points over the six months. They will compare the bio-
Coming up
The U.S. Psychiatric and Mental Health Congress will hold its 25th Annual Conference and Exhibition 2012 November 8-11 in San Diego, Calif. For more information, visit www.psychcongress.com. ACHMA The College for Behavioral Health Leadership is hosting a policy forum, Harnessing Community Support for Health and Well-being, December 4-5 in Washington, D.C. Visit www.acmha.org for more information.
marker patterns of individuals who subsequently develop PTSD and/or depression with those who do not.
western Kentucky, but children in western Kentucky take more ADHD drugs than their counterparts in eastern Kentucky. Tennessee MH center praised for investment in Detroit facility Mich. Gov. Rick Snyder, the Detroit City Council, mental healthcare leaders and others on October 23 saluted the Nashville, Tenn.-based Behavioral Centers of America (BCA) on its selection of Detroit for a $20 million master campus investment. The move turns a formerly bankrupt eastside hospital into a comforting and healing StoneCrest Center oasisin-the-city, and helps fill the critical need for mental healthcare services in Metro Detroit and Michigan, according to StoneCrest Center officials in Detroit. BCA StoneCrest Center programs currently serve adults, adolescents, seniors and developmentally delayed patients.
Visit our website: www.mentalhealthweeklynews.com
STATE NEWS
Antipsychotic drug use rises among poor children in Kentucky The amount of powerful antipsychotic drugs distributed to poor and disabled children on Medicaid in Kentucky jumped 270 percent from 2000 to 2010, according to a new report by researchers at the University of Kentucky, the Lexington Herald-Leader reported last week. The largest growth was for minority children, who received medications for schizophrenia, bipolar disorder and depression at three times the rate of white children in 2010. The report also found unexplained geographical differences in how minority children are treated for mental illnesses; minority children in eastern Kentucky take 26 times more antipsychotic medications than minority children in
In case you havent heard
Children with mental health disorders may be more prone to bullying others, according to new research presented at the American Academy of Pediatrics National Conference and Exhibition in New Orleans on October 24, the British Psychological Society reported. The new study found these youngsters are three times more likely to victimize their peers than those who have not been diagnosed with such conditions. Children suffering from depression are at greater risk of being identified as bullies, while those found to have an oppositional defiant disorder are even more likely to behave in this way. These findings highlight the importance of providing psychological support not only to victims of bullying, but to bullies as well, said Frances Turcotte-Benedict, a masters student at Brown University and a Fellow at Hasbro Childrens Hospital in Providence, R.I.
Mental Health Weekly DOI: 10.1002/mhw
It is illegal under federal copyright law to reproduce this publication or any portion of it without the publishers permission.
Das könnte Ihnen auch gefallen
- Advocacy Is An ImportantDokument40 SeitenAdvocacy Is An ImportantPramusetya SuryandaruNoch keine Bewertungen
- Health Promotion and Mental HealthDokument417 SeitenHealth Promotion and Mental HealthPetzyMarian100% (2)
- Law On Common Carriers: Laws Regulating Transportation CompaniesDokument3 SeitenLaw On Common Carriers: Laws Regulating Transportation CompaniesLenoel Nayrb Urquia Cosmiano100% (1)
- A Call To Action: Helping Hospice Social Workers Embrace Evidence-Based Practice Improving Hospice DocumentationDokument7 SeitenA Call To Action: Helping Hospice Social Workers Embrace Evidence-Based Practice Improving Hospice DocumentationSaab AeroNoch keine Bewertungen
- Healthy Workforce: An Essential Health Promotion Sourcebook For Employers, Large and SmallDokument72 SeitenHealthy Workforce: An Essential Health Promotion Sourcebook For Employers, Large and SmallTrainer AongNoch keine Bewertungen
- United Healthcare GroupDokument18 SeitenUnited Healthcare GroupEhab elhashmyNoch keine Bewertungen
- There's an Elephant in Your Office, 2nd Edition: Practical Tips to Successfully Identify and Support Mental and Emotional Health in the WorkplaceVon EverandThere's an Elephant in Your Office, 2nd Edition: Practical Tips to Successfully Identify and Support Mental and Emotional Health in the WorkplaceNoch keine Bewertungen
- Holistic Health Solutions Business PlanDokument36 SeitenHolistic Health Solutions Business PlanRadhakrishnan SanjeeviNoch keine Bewertungen
- Health Equity Tool Kit FinalDokument25 SeitenHealth Equity Tool Kit FinalDenden Alicias100% (1)
- Helping Children and Adolescents with Chronic and Serious Medical Conditions: A Strengths-Based ApproachVon EverandHelping Children and Adolescents with Chronic and Serious Medical Conditions: A Strengths-Based ApproachNoch keine Bewertungen
- Where Did You Last Spend Your Money? What Kind of Service Did You Last Avail?Dokument52 SeitenWhere Did You Last Spend Your Money? What Kind of Service Did You Last Avail?Who Am I100% (1)
- Direct RetainerDokument186 SeitenDirect RetainerAngkita KalitaNoch keine Bewertungen
- Addressing The Opioid Epidemic On BYU Campus Through CAPS-O ProgramDokument34 SeitenAddressing The Opioid Epidemic On BYU Campus Through CAPS-O Programapi-439502865Noch keine Bewertungen
- NNTimes October 09 Issue PDFDokument72 SeitenNNTimes October 09 Issue PDFMonika Joseph0% (2)
- InvestMemo TemplateDokument6 SeitenInvestMemo TemplatealiranagNoch keine Bewertungen
- Final Care Coordination PlanDokument9 SeitenFinal Care Coordination PlanEmmanuel InyanzaNoch keine Bewertungen
- Seminar On Current Issues and Trends in Psychiatry. Mental Health Services in Kerala India and GlobalDokument34 SeitenSeminar On Current Issues and Trends in Psychiatry. Mental Health Services in Kerala India and GlobalGopika SNoch keine Bewertungen
- Christiane Nord - Text Analysis in Translation (1991) PDFDokument280 SeitenChristiane Nord - Text Analysis in Translation (1991) PDFDiana Polgar100% (2)
- Health Care Policy PaperDokument6 SeitenHealth Care Policy Paperapi-471591880Noch keine Bewertungen
- Mental Health Promotion: A Framework For ActionDokument6 SeitenMental Health Promotion: A Framework For ActionHasrat ButtarNoch keine Bewertungen
- WHO Netherlands Fajriyatul KamalDokument2 SeitenWHO Netherlands Fajriyatul KamalFajriyatul KamalNoch keine Bewertungen
- Benchmark AnalysisDokument6 SeitenBenchmark Analysisalexis delgadoNoch keine Bewertungen
- Donald J. Meyer (Ed) - The Economics of Health-W.E. Upjohn Institute For Employment Research (2016)Dokument155 SeitenDonald J. Meyer (Ed) - The Economics of Health-W.E. Upjohn Institute For Employment Research (2016)AnupaNoch keine Bewertungen
- Ethics Paper MTWDokument16 SeitenEthics Paper MTWapi-273102163Noch keine Bewertungen
- Research Paper On Mental Health in IndiaDokument4 SeitenResearch Paper On Mental Health in Indiaqzetcsuhf100% (1)
- Health CARE GRAND PROPOSALDokument15 SeitenHealth CARE GRAND PROPOSALwamburamuturi001Noch keine Bewertungen
- Module 4 2Dokument4 SeitenModule 4 2api-642701476Noch keine Bewertungen
- Hsci 6250Dokument4 SeitenHsci 6250api-642711495Noch keine Bewertungen
- Health Care Management Research Paper TopicsDokument9 SeitenHealth Care Management Research Paper Topicscapz4pp5100% (1)
- Overview of Mental IllnessDokument15 SeitenOverview of Mental IllnessbeibhydNoch keine Bewertungen
- Getting My Life Back:: Occupational Therapy Promoting Mental Health and Wellbeing in EnglandDokument20 SeitenGetting My Life Back:: Occupational Therapy Promoting Mental Health and Wellbeing in EnglandAlejandro CardonaNoch keine Bewertungen
- Health Psychology An Introduction To Behavior and Health Brannon 8th Edition Test BankDokument36 SeitenHealth Psychology An Introduction To Behavior and Health Brannon 8th Edition Test Bankexogyraquoter0f94xl100% (30)
- Disparities in Knowledge, Attitude and Practices On Mental Health Among Healthcare Workers and Community Members in Meru County, KenyaDokument22 SeitenDisparities in Knowledge, Attitude and Practices On Mental Health Among Healthcare Workers and Community Members in Meru County, KenyaMuhammad IdrisNoch keine Bewertungen
- Health Systems 2009 20aug ADokument74 SeitenHealth Systems 2009 20aug ANational Child Health Resource Centre (NCHRC)Noch keine Bewertungen
- MYM At-Work PresentationDokument23 SeitenMYM At-Work PresentationapvNoch keine Bewertungen
- Diploma in NursingDokument10 SeitenDiploma in NursinglilianNoch keine Bewertungen
- Health 10health Career Pathways FDokument26 SeitenHealth 10health Career Pathways FTsukino AzusagawaNoch keine Bewertungen
- Unit 5 WADokument8 SeitenUnit 5 WAAdanigbo MagretNoch keine Bewertungen
- Wellness DefinitionDokument29 SeitenWellness Definitionamit7907100% (1)
- Community Health Term PaperDokument7 SeitenCommunity Health Term Paperafmzmajcevielt100% (1)
- Changes in Attitudes Toward Mental Illness in Healthcare Professionals and StudentsDokument14 SeitenChanges in Attitudes Toward Mental Illness in Healthcare Professionals and StudentsleticiaNoch keine Bewertungen
- Dissertation Topics in Health PromotionDokument8 SeitenDissertation Topics in Health PromotionCollegePapersForSaleUK100% (1)
- Intro To US HealthCare Exam 1 Study GuideDokument10 SeitenIntro To US HealthCare Exam 1 Study GuideMiaLeiNoch keine Bewertungen
- Why Not Use The Term Patient?Dokument36 SeitenWhy Not Use The Term Patient?Van Errl Nicolai SantosNoch keine Bewertungen
- Health Topic Ideas For Research PapersDokument6 SeitenHealth Topic Ideas For Research Papersniisexgkf100% (1)
- Consumer Behavior To Health Care ProductsDokument63 SeitenConsumer Behavior To Health Care ProductsZohra MerchantNoch keine Bewertungen
- Running Head: Homelessness in Adolescents 1Dokument20 SeitenRunning Head: Homelessness in Adolescents 1Rachael NitzNoch keine Bewertungen
- Addressing The Opioid Epidemic On BYU Campus Through CAPS-O ProgramDokument34 SeitenAddressing The Opioid Epidemic On BYU Campus Through CAPS-O Programapi-439502865Noch keine Bewertungen
- Research Paper On Health IssuesDokument7 SeitenResearch Paper On Health Issuesrcjbhsznd100% (1)
- Role of Incentives RewardsDokument2 SeitenRole of Incentives RewardsRitesh KumarNoch keine Bewertungen
- WISH Mental Health ReportDokument52 SeitenWISH Mental Health ReportMatías ArgüelloNoch keine Bewertungen
- Advances in Integrative Medicine: EditorialDokument2 SeitenAdvances in Integrative Medicine: EditorialVictor Raul JuramaNoch keine Bewertungen
- Textbook of Urgent Care Management: Chapter 44, Integrative MedicineVon EverandTextbook of Urgent Care Management: Chapter 44, Integrative MedicineNoch keine Bewertungen
- Corporate Social Responsibility: GlobalizationDokument8 SeitenCorporate Social Responsibility: GlobalizationRaj_Padharia_7721Noch keine Bewertungen
- Alberta Post-Secondary Mental Health and Addiction FrameworkDokument35 SeitenAlberta Post-Secondary Mental Health and Addiction FrameworkBenson NinanNoch keine Bewertungen
- Trends and Innovations in Chronic Disease Prevention TreatmentDokument48 SeitenTrends and Innovations in Chronic Disease Prevention TreatmentKrisTina KhaiZer RicoNoch keine Bewertungen
- Chapter IDokument11 SeitenChapter IShoto TodorokiNoch keine Bewertungen
- Population-Health Approach: Mental Health and Addictions SectorDokument5 SeitenPopulation-Health Approach: Mental Health and Addictions SectorNilanjana ChakrabortyNoch keine Bewertungen
- Final Program Development PaperDokument54 SeitenFinal Program Development Paperapi-436257683Noch keine Bewertungen
- Pih Engage Utd April 2024 NewsletterDokument7 SeitenPih Engage Utd April 2024 Newsletterapi-739344619Noch keine Bewertungen
- DS 331Dokument9 SeitenDS 331chris fwe fweNoch keine Bewertungen
- Health Field Research Paper TopicsDokument7 SeitenHealth Field Research Paper Topicsaflbtlzaw100% (1)
- Thesis Statement On Health Care ReformDokument6 SeitenThesis Statement On Health Care Reformdwns3cx2100% (2)
- Assorti Thursday DinnerDokument3 SeitenAssorti Thursday DinnerOTMMediaNoch keine Bewertungen
- Assorti Tuesday DinnerDokument3 SeitenAssorti Tuesday DinnerOTMMediaNoch keine Bewertungen
- Assorti Sunday DinnerDokument3 SeitenAssorti Sunday DinnerOTMMediaNoch keine Bewertungen
- Assorti Saturday DinnerDokument3 SeitenAssorti Saturday DinnerOTMMediaNoch keine Bewertungen
- Assorti Monday LunchDokument2 SeitenAssorti Monday LunchOTMMediaNoch keine Bewertungen
- Assorti Monday DinnerDokument3 SeitenAssorti Monday DinnerOTMMediaNoch keine Bewertungen
- Assorti Breakfast MenuDokument1 SeiteAssorti Breakfast MenuOTMMediaNoch keine Bewertungen
- 1 Relative Maxima, Relative Minima and Saddle PointsDokument3 Seiten1 Relative Maxima, Relative Minima and Saddle PointsRoy VeseyNoch keine Bewertungen
- 1.3 Digital Communication and AnalogueDokument6 Seiten1.3 Digital Communication and AnaloguenvjnjNoch keine Bewertungen
- Worksheet For Mathematics For ManagementDokument3 SeitenWorksheet For Mathematics For Managementabel shimeles100% (1)
- Perception On The Impact of New Learning Tools in Humss StudentDokument6 SeitenPerception On The Impact of New Learning Tools in Humss StudentElyza Marielle BiasonNoch keine Bewertungen
- Kuo SzuYu 2014 PHD ThesisDokument261 SeitenKuo SzuYu 2014 PHD ThesiskatandeNoch keine Bewertungen
- PM-KISAN: Details of Eligible and Ineligible FarmersDokument2 SeitenPM-KISAN: Details of Eligible and Ineligible Farmerspoun kumarNoch keine Bewertungen
- 2013 03 01 Maurizio Di Noia PresentationDokument80 Seiten2013 03 01 Maurizio Di Noia PresentationRene KotzeNoch keine Bewertungen
- Upload Emp Photo ConfigDokument14 SeitenUpload Emp Photo Configpaulantony143Noch keine Bewertungen
- Remarkings AirportsDokument1 SeiteRemarkings AirportsJuan Jose CaleroNoch keine Bewertungen
- LESSON 6 Perfect TensesDokument4 SeitenLESSON 6 Perfect TensesAULINO JÚLIONoch keine Bewertungen
- Rousseau NotesDokument4 SeitenRousseau NotesAkhilesh IssurNoch keine Bewertungen
- Summary of All Sequences For 4MS 2021Dokument8 SeitenSummary of All Sequences For 4MS 2021rohanZorba100% (3)
- How You Are Programmed To Be POOR and THINK Small - The MAGIC of THINKING BIGDokument88 SeitenHow You Are Programmed To Be POOR and THINK Small - The MAGIC of THINKING BIGOlegario S. Sumaya IIINoch keine Bewertungen
- Aswini Expert SystemsDokument37 SeitenAswini Expert SystemsKarishma Satheesh KumarNoch keine Bewertungen
- World War I Almanac Almanacs of American WarsDokument561 SeitenWorld War I Almanac Almanacs of American WarsMatheus Benedito100% (1)
- Cambridge Latin Course Book I Vocabulary Stage 1 Stage 2Dokument3 SeitenCambridge Latin Course Book I Vocabulary Stage 1 Stage 2Aden BanksNoch keine Bewertungen
- EnglishFile4e Intermediate TG PCM Vocab RevDokument1 SeiteEnglishFile4e Intermediate TG PCM Vocab RevB Mc0% (1)
- TSH TestDokument5 SeitenTSH TestdenalynNoch keine Bewertungen
- What If The Class Is Very BigDokument2 SeitenWhat If The Class Is Very BigCamilo CarantónNoch keine Bewertungen
- English VowelDokument6 SeitenEnglish Vowelqais yasinNoch keine Bewertungen
- Mamaoui PassagesDokument21 SeitenMamaoui PassagesSennahNoch keine Bewertungen
- Lee. Building Balanced Scorecard With SWOT Analysis, and Implementing "Sun Tzu's The Art of Business Management Strategies" On QFD Methodology PDFDokument13 SeitenLee. Building Balanced Scorecard With SWOT Analysis, and Implementing "Sun Tzu's The Art of Business Management Strategies" On QFD Methodology PDFSekar Ayu ParamitaNoch keine Bewertungen
- Speakout Language BankDokument7 SeitenSpeakout Language BankСаша БулуєвNoch keine Bewertungen
- CPN Project TopicsDokument1 SeiteCPN Project TopicsvirginNoch keine Bewertungen
- Accenture 172199U SAP S4HANA Conversion Brochure US Web PDFDokument8 SeitenAccenture 172199U SAP S4HANA Conversion Brochure US Web PDFrajesh2kakkasseryNoch keine Bewertungen
- Causing v. ComelecDokument13 SeitenCausing v. ComelecChristian Edward CoronadoNoch keine Bewertungen