Beruflich Dokumente
Kultur Dokumente
Pi Is 0002934312004901
Hochgeladen von
MuliaDharmaSaputraHutapeaOriginalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Pi Is 0002934312004901
Hochgeladen von
MuliaDharmaSaputraHutapeaCopyright:
Verfügbare Formate
CLINICAL COMMUNICATION TO THE EDITOR
Tombstone ST Elevations: . . . Not Necessarily a Harbinger of Doom!
To the Editor: A 58-year-old white man with a remote spinal cord injury was admitted with bilateral lower lobe pneumonia and urinary tract infection. He had been quadriplegic for over 40 years as a result of cervical spine injury and had been experiencing autonomic dysreexia for many years. He was started on intravenous antibiotics. Respiratory status progressively worsened, requiring mechanical ventilation. On the third day of admission he complained of generalized abdominal pain, and ST-segment elevation was noted on telemetry. Oxygen saturation was 94% on room air, heart rate was 109 beats per minute, and blood pressure was 240/130 mm Hg. A 12-lead electrocardiogram (ECG) showed marked (10-mm) ST-segment elevations in inferior leads and 3-mm ST-segment depressions in V1-V3, ndings
Funding: None. Conict of Interest: None. Authorship: All authors had access to the data and a role in writing the manuscript. Requests for reprints should be addressed to Faisal Latif, MD, Department of Medicine/Cardiology, University of Oklahoma Health Sciences Center, 920 Stanton L. Young Blvd, WP# 3010, Oklahoma City, OK 73114. E-mail address: Faisal-Latif@ouhsc.edu
diagnostic of an acute inferoposterior ST-elevation myocardial infarction (Figure). Physical examination was normal except for mild diffuse abdominal tenderness but no guarding. Abdominal radiograph revealed ileus with no free air or uid levels. Laboratory values were all within normal limits, with no electrolyte abnormalities. Current ECG was remarkably different from his baseline, which showed sinus rhythm, incomplete right bundle branch block, and left anterior fascicular block. He had previously experienced similar episodes of severe hypertension, during which he was asymptomatic, and those resolved spontaneously, without accompanying ST-segment elevations. He was given aspirin 325 mg, clopidogrel 600 mg, and heparin infusion was started. Emergent cardiac catheterization revealed normal coronary arteries. There was no coronary vasospasm or slow ow either. Limited ECG during cardiac catheterization demonstrated a dynamic change to marked ST-segment depressions in inferior leads (4 mm) and 2-mm ST-segment elevation in the V lead. ST-segment changes persisted for almost 3 hours before returning to baseline. Interestingly, blood pressure normalized 2 hours before the ECG did. The ST-segment changes were not closely related to abdominal discomfort either. He continued to have occasional abdominal discomfort without recurrence of ECG changes. Transthoracic echocardiography revealed vigorous left ventricular systolic function
Figure A 12-lead electrocardiogram shows marked (10-mm) ST-segment elevations in inferior leads and 3-mm ST-segment depressions in V1-V3, ndings diagnostic of an acute inferoposterior ST-elevation myocardial infarction.
0002-9343/$ -see front matter Published by Elsevier Inc.
e2 without regional wall motion abnormalities or pericardial effusion. Interestingly, serial cardiac biomarkers remained normal (peak value of creatine kinase was 18 U/L, creatine kinase-MB was 2.3 ng/mL, and troponin I was 0.03 ng/mL). New ST-segment elevation on ECG is an alarming nding, which, if associated with chest pain and cardiac biomarker elevation, is a strong indicator of acute myocardial infarction, and urgent reperfusion therapy is the standard of care. Due to loss of supraspinal sensory input, patients with spinal cord injury may suffer asymptomatic myocardial injury.1 Therefore, clinical clues such as ECG changes, cardiac biomarkers, or atypical symptoms might indicate ongoing myocardial injury, as was the presumed case in our patient. Some patients with spinal cord injury have chronic STsegment changes, for example, ST elevation suggestive of early repolarization. These occur if the spinal cord injury is at a level that disrupts the central control of sympathetic cardiac innervation, leading to altered ventricular repolarization manifesting as ST elevations.2 However, these changes are permanent and not transient, as in our patient. Our patient most likely had autonomic dysreexia producing marked elevation of blood pressure, but additionally led to ST-segment changes typical of an acute inferoposterior myocardial infarction, a nding that has not, to our knowledge, been reported before. These ST changes are likely due to alteration in ventricular repolarization in the
The American Journal of Medicine, Vol xx, No x, Month 2012 absence of myocardial ischemia, but somehow mediated by the changes in sympathetic activity due to spinal cord injury. After a prolonged treatment with antibiotics, he was weaned off mechanical ventilation after 2 months. Then he underwent surgery for debridement of a sacral decubitus ulcer and was nally discharged home after a total of 7 months of hospitalization. Muhammad Chaudhry, MDa Zainab Omar, MDb Faisal Latif, MDc
Department of Medicine University of Oklahoma Health Sciences Center Oklahoma City b King Edward Medical College Lahore, Pakistan c Cardiovascular Section University of Oklahoma Health Sciences Center Oklahoma City
a
http://dx.doi.org/10.1016/j.amjmed.2012.05.019
References
1. Ho CP, Krassioukov AV. Autonomic dysreexia and myocardial ischemia. Spinal Cord. 2010;48(9):714-715. 2. Marcus RR, Kalisetti D, Raxwal V, et al. Early repolarization in patients with spinal cord injury: prevalence and clinical signicance. J Spinal Cord Med. 2002;25:33-38.
Das könnte Ihnen auch gefallen
- Cardiac Catheterization and Coronary Intervention (2nd Edition, 2020)Dokument353 SeitenCardiac Catheterization and Coronary Intervention (2nd Edition, 2020)John Cancel50% (2)
- Cardiology QuestionDokument63 SeitenCardiology QuestionRazi Baik100% (1)
- Final Questions 2021Dokument8 SeitenFinal Questions 2021PatrycjaSkierkaNoch keine Bewertungen
- T 20 CardiologyDokument51 SeitenT 20 Cardiologydrkhalid12100% (3)
- 3 Heart InternetNewDokument55 Seiten3 Heart InternetNewCoral Srinivasa RamaluNoch keine Bewertungen
- MCQs - CardiologyDokument16 SeitenMCQs - CardiologyZach Elzwie100% (4)
- ACN Unit3Dokument35 SeitenACN Unit3Kamran AltafNoch keine Bewertungen
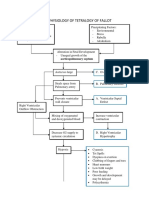
- Pathophysiology of Tetralogy of FallotDokument2 SeitenPathophysiology of Tetralogy of Fallotsubham kumar100% (3)
- Specility DepartmentDokument140 SeitenSpecility DepartmentAjay SakarayNoch keine Bewertungen
- Department of Internal Medicine Ii and Phthysiatry: - Rajkumar Subasaravanan Subgroup "12"Dokument57 SeitenDepartment of Internal Medicine Ii and Phthysiatry: - Rajkumar Subasaravanan Subgroup "12"Suba Saravanan 12Noch keine Bewertungen
- Assignment: Applied MedicineDokument15 SeitenAssignment: Applied MedicineKhadija BakhtawarNoch keine Bewertungen
- Jurnal Kedokteran Dan Kesehatan IndonesiaDokument7 SeitenJurnal Kedokteran Dan Kesehatan IndonesiaAlfix AnugrahNoch keine Bewertungen
- Massive Pulmonary Embolism Presenting As Seizures: December 2008 Vol 10 No 4Dokument4 SeitenMassive Pulmonary Embolism Presenting As Seizures: December 2008 Vol 10 No 4BelladonnaRoxNoch keine Bewertungen
- Electrocardiographic Changes and Intracranial Pathology: Geraldine Syverud, Crna, BSNDokument4 SeitenElectrocardiographic Changes and Intracranial Pathology: Geraldine Syverud, Crna, BSNchuck55Noch keine Bewertungen
- Anterolateral Papillary Muscle Rupture As A Result of Single-Vessel Coronary Artery Disease Without Myocardial InfarctionDokument3 SeitenAnterolateral Papillary Muscle Rupture As A Result of Single-Vessel Coronary Artery Disease Without Myocardial InfarctionDonatas AustysNoch keine Bewertungen
- 2017 17 4 148 150 EngDokument3 Seiten2017 17 4 148 150 Engخالد العيلNoch keine Bewertungen
- Assignment: Applied MedicineDokument13 SeitenAssignment: Applied MedicineKhadija BakhtawarNoch keine Bewertungen
- Effoe2019 Article Pseudo-WellensSyndromeAcutePanDokument6 SeitenEffoe2019 Article Pseudo-WellensSyndromeAcutePanChem Lloyd SignapanNoch keine Bewertungen
- Takotsubo Cardiomyopathy: A Case Series From A Cardiac Center in Rajasthan and Review of LiteratureDokument8 SeitenTakotsubo Cardiomyopathy: A Case Series From A Cardiac Center in Rajasthan and Review of LiteratureIJAR JOURNALNoch keine Bewertungen
- Cardio 1.5Dokument2 SeitenCardio 1.5ChibuNoch keine Bewertungen
- Case Report Sibutramine As A Cause of Sudden Cardiac DeathDokument5 SeitenCase Report Sibutramine As A Cause of Sudden Cardiac DeathAnonymous EAPbx6Noch keine Bewertungen
- Pages From Cardiology - AceQbank MCCQE1 2023 - QbankDokument10 SeitenPages From Cardiology - AceQbank MCCQE1 2023 - QbankDila KavameNoch keine Bewertungen
- Criem2020 4159526Dokument5 SeitenCriem2020 4159526m.fahimsharifiNoch keine Bewertungen
- 1 s2.0 S1878540912000473 MainDokument3 Seiten1 s2.0 S1878540912000473 MainIoana SusNoch keine Bewertungen
- Diagnosis of Acute Myocardial InfarctDokument5 SeitenDiagnosis of Acute Myocardial InfarctOscar SanNoch keine Bewertungen
- An 80 Year Old Patient Named MRDokument5 SeitenAn 80 Year Old Patient Named MRRodel Aguila SañoNoch keine Bewertungen
- Lapkas VT RevisiDokument13 SeitenLapkas VT RevisiRannyNoch keine Bewertungen
- ST-segment Depression: All Are Not Created Equal!Dokument6 SeitenST-segment Depression: All Are Not Created Equal!asclepiuspdfsNoch keine Bewertungen
- Sudden Cardiac Arrest in Takotsubo Cardiomyopathy - A Case StudyDokument5 SeitenSudden Cardiac Arrest in Takotsubo Cardiomyopathy - A Case StudyzenyxtaNoch keine Bewertungen
- Memory T-Waves, A Rare Cause of T-Wave Inversion in The Emergency Department - PMCDokument7 SeitenMemory T-Waves, A Rare Cause of T-Wave Inversion in The Emergency Department - PMCfiat.2dindaNoch keine Bewertungen
- JURNALDokument7 SeitenJURNALHarlina NurlitaNoch keine Bewertungen
- PIIS1071916416309447Dokument2 SeitenPIIS1071916416309447Made ChandraNoch keine Bewertungen
- Myocardial Infarction, Acute Case FileDokument7 SeitenMyocardial Infarction, Acute Case Filehttps://medical-phd.blogspot.comNoch keine Bewertungen
- Krunoslav Fuckar, Nenad Lakusic, Hrvoje Stipic: Case ReportDokument8 SeitenKrunoslav Fuckar, Nenad Lakusic, Hrvoje Stipic: Case ReportFariz DwikyNoch keine Bewertungen
- Cric2018 7237454Dokument4 SeitenCric2018 7237454Muhammad Nur Ardhi LahabuNoch keine Bewertungen
- Ajcdr 2 2 4Dokument5 SeitenAjcdr 2 2 4tiaraiswandaNoch keine Bewertungen
- Stress Related Takotsubo Cardiomyopathy: A Case ReportDokument6 SeitenStress Related Takotsubo Cardiomyopathy: A Case ReportSabrina JonesNoch keine Bewertungen
- PMR Poster TBI Takotsubo AAP 2010 PosterDokument1 SeitePMR Poster TBI Takotsubo AAP 2010 PosterjuanvelasquezNoch keine Bewertungen
- When Past Is Prologue: Clinical Problem-SolvingDokument7 SeitenWhen Past Is Prologue: Clinical Problem-SolvingJoni WitziNoch keine Bewertungen
- Theischemic Electrocardiogram: Daniel L. KreiderDokument16 SeitenTheischemic Electrocardiogram: Daniel L. KreiderAlejandro Peñaloza TapiaNoch keine Bewertungen
- ECG Lab FormulaeDokument35 SeitenECG Lab Formulaevivek_win95Noch keine Bewertungen
- 1 s2.0 S0735675715005483 MainDokument3 Seiten1 s2.0 S0735675715005483 Mainfebriandika gawlNoch keine Bewertungen
- Nejmcps 2116690Dokument8 SeitenNejmcps 2116690Luis MadrigalNoch keine Bewertungen
- April 2018 1522659614 97Dokument2 SeitenApril 2018 1522659614 97Rohit ThakareNoch keine Bewertungen
- Case Reports AbstractsDokument7 SeitenCase Reports AbstractsNovie AstiniNoch keine Bewertungen
- The Ischemic Electrocardiogram: Daniel L. KreiderDokument12 SeitenThe Ischemic Electrocardiogram: Daniel L. Kreidermarianagonzalezgil11Noch keine Bewertungen
- 3091 Full PDFDokument7 Seiten3091 Full PDFgeeheebNoch keine Bewertungen
- Case Study of Anterior Wall MI 48Dokument32 SeitenCase Study of Anterior Wall MI 48سوما الشمريNoch keine Bewertungen
- Andi 26-30Dokument6 SeitenAndi 26-30Andi HidayatNoch keine Bewertungen
- Reversed Rlvero-Carvallo's Sign in Right-Sided Hypertrophic Obstructive CardiomyopathyDokument3 SeitenReversed Rlvero-Carvallo's Sign in Right-Sided Hypertrophic Obstructive CardiomyopathySergio RodriguezNoch keine Bewertungen
- 1 SMDokument15 Seiten1 SMemmanuellagrace06Noch keine Bewertungen
- Journal (10 24 22)Dokument3 SeitenJournal (10 24 22)Louigen DagaydayNoch keine Bewertungen
- Acute Coronary SyndromesDokument7 SeitenAcute Coronary SyndromesAiman ArifinNoch keine Bewertungen
- Clinical Case Microcirculation. Mrs. MarieDokument2 SeitenClinical Case Microcirculation. Mrs. MarieRafael G. Garcia SanchezNoch keine Bewertungen
- Circulationaha 118 034075Dokument3 SeitenCirculationaha 118 034075Aldo Emir M. SarabiaNoch keine Bewertungen
- Allergic Acute Coronary Syndrome (Kounis Syndrome)Dokument5 SeitenAllergic Acute Coronary Syndrome (Kounis Syndrome)audiNoch keine Bewertungen
- Cardiogenic Shock and Pulmonary EdemaDokument9 SeitenCardiogenic Shock and Pulmonary EdemaFátima OlivasNoch keine Bewertungen
- Concomitant PAD and CADDokument96 SeitenConcomitant PAD and CADric_vir_014Noch keine Bewertungen
- Arab Board Exam 2 With AnswersDokument31 SeitenArab Board Exam 2 With Answersahmed.farag.ali2020Noch keine Bewertungen
- The Ischemic ElectrocardiogramDokument16 SeitenThe Ischemic ElectrocardiogramAdiel OjedaNoch keine Bewertungen
- ST Segment and T Waves:: Ischemia, Infarction, Drug & Electrolyte EffectsDokument34 SeitenST Segment and T Waves:: Ischemia, Infarction, Drug & Electrolyte EffectsHibba NasserNoch keine Bewertungen
- Mitral Valve Prolapse Syndrome With Coronary Artery Spasm: Possible Cause of Recurrent Ventricular TachyarrhythmiaDokument3 SeitenMitral Valve Prolapse Syndrome With Coronary Artery Spasm: Possible Cause of Recurrent Ventricular TachyarrhythmiaDewina Dyani RosariNoch keine Bewertungen
- Abstract For Iwoc-MetastaticDokument2 SeitenAbstract For Iwoc-MetastaticlevinaaaNoch keine Bewertungen
- WPH VMO Directory1Dokument56 SeitenWPH VMO Directory1Ragupathi MNoch keine Bewertungen
- CABG x4Dokument2 SeitenCABG x4Indranil SinhaNoch keine Bewertungen
- Linea Del Tiempo-CardioDokument7 SeitenLinea Del Tiempo-Cardioapi-560369573Noch keine Bewertungen
- Basic EP IntervalsDokument13 SeitenBasic EP IntervalsdrharoonmohdNoch keine Bewertungen
- Diastole and AnesthesiaDokument16 SeitenDiastole and AnesthesiadrsubramanianNoch keine Bewertungen
- Question Nbns2213 Hematology and Cardiology NursingDokument11 SeitenQuestion Nbns2213 Hematology and Cardiology Nursingdicky chongNoch keine Bewertungen
- Seminar On Rheumatic Heart Disease: by Zerihun GetachewDokument37 SeitenSeminar On Rheumatic Heart Disease: by Zerihun GetachewZerihun Getachew ShiferawNoch keine Bewertungen
- PUA006 Valve Disease Assessment Poster - Print ReadyDokument1 SeitePUA006 Valve Disease Assessment Poster - Print ReadyLuis Fernando Morales JuradoNoch keine Bewertungen
- Doctors OET Writing Practice TestDokument3 SeitenDoctors OET Writing Practice Testanjali hansNoch keine Bewertungen
- Acute Coronary SyndromeDokument30 SeitenAcute Coronary SyndromeEndar EszterNoch keine Bewertungen
- Fontan Ten CommandantsDokument4 SeitenFontan Ten CommandantsRuchi VatwaniNoch keine Bewertungen
- Patofisiologi AritmiaDokument27 SeitenPatofisiologi AritmiaVedora Angelia GultomNoch keine Bewertungen
- Elective Cardioversion: Critical Care Unit (CCU) The Horton General HospitalDokument8 SeitenElective Cardioversion: Critical Care Unit (CCU) The Horton General HospitalEzraGoenadiNoch keine Bewertungen
- Circuit Weight Training in Cardiac PatientsDokument5 SeitenCircuit Weight Training in Cardiac PatientsVivin YulvinaNoch keine Bewertungen
- Ekg MorphologyDokument1 SeiteEkg MorphologyTeresa MartinsNoch keine Bewertungen
- Ventricular Septal DefectDokument43 SeitenVentricular Septal DefectmalekNoch keine Bewertungen
- Mfine CardiologistsDokument7 SeitenMfine Cardiologistsmfine healthNoch keine Bewertungen
- Job Opportunities: Sr. No. Name of Hospital / Institution Post Name Specialty Name No. of PostsDokument11 SeitenJob Opportunities: Sr. No. Name of Hospital / Institution Post Name Specialty Name No. of PostsAli AwanNoch keine Bewertungen
- 02 Chain of SurvivalDokument1 Seite02 Chain of SurvivalHatem FaroukNoch keine Bewertungen
- ESC Toolkit PDFDokument164 SeitenESC Toolkit PDFHikMa AbdullahNoch keine Bewertungen
- Management of Perioperative ArrhythmiasDokument15 SeitenManagement of Perioperative Arrhythmiaszuraini_mdnoorNoch keine Bewertungen
- Lesson 20Dokument4 SeitenLesson 20Ananta KhanalNoch keine Bewertungen
- Antihypotensive Drugs: Roger Joseph Ii Ramos Jecino, RN, M.DDokument28 SeitenAntihypotensive Drugs: Roger Joseph Ii Ramos Jecino, RN, M.DFranz Earl Niño AlbesaNoch keine Bewertungen
- Aortic Root Dilatation As The Sole Cause of Atrial FibrillationDokument2 SeitenAortic Root Dilatation As The Sole Cause of Atrial FibrillationNathania HoswandiNoch keine Bewertungen
- Kuliah MITRAL STENOSISDokument19 SeitenKuliah MITRAL STENOSISAdi TrisnoNoch keine Bewertungen
- Diagnostic Services:-2D Echo, Audiometry, Bronchoscopy, CTDokument196 SeitenDiagnostic Services:-2D Echo, Audiometry, Bronchoscopy, CTLalita NaiduNoch keine Bewertungen