Beruflich Dokumente
Kultur Dokumente
Coronary Blood Flow Regulation and Determinants
Hochgeladen von
jordandenise2Originalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Coronary Blood Flow Regulation and Determinants
Hochgeladen von
jordandenise2Copyright:
Verfügbare Formate
Coronary blood flow
Tamilselvi Ramanathan FRCA Henry Skinner FRCA
The heart has the highest oxygen consumption per tissue mass of all human organs. The resting coronary blood flow is $250 ml min1 (0.8 ml min1 g1 of heart muscle); this represents 5% of cardiac output.1 Ischaemia results when oxygen demand outstrips supply. Arterial oxygen extraction is 7080%, compared with 25% for the rest of the body. Therefore, increased oxygen consumption must principally be met by an increase in coronary blood flow, which may increase fivefold during exercise. Supply usually closely matches any change in demand. However, an increase in coronary blood flow can independently increase myocardial oxygen consumption (Gregg effect).2 This may be explained by full coronary arteries splinting the heart and increasing the end-diastolic fibre length and contractility.
heart muscle and blood flow to the left ventricle is at its lowest. The force is greatest in the subendocardial layers where it approximates to intramyocardial pressure. In systole, intramyocardial blood is propelled forwards towards the coronary sinus and retrogradely into the epicardial vessels, which act as capacitors. Flow resumes during diastole when the muscle relaxes. The coronary perfusion pressure is the difference between the aortic diastolic pressure and left ventricular end-diastolic pressure (LVEDP). Phasic changes in blood flow to the right ventricle are less pronounced because of the lesser force of contraction. Central venous pressure may be a more appropriate choice for downstream pressure to calculate the right-sided coronary perfusion pressure.2
Key points Blood flow to the heart occurs mainly during diastole. Coronary blood flow is mainly determined by local oxygen demand. The vascular endothelium is the final common pathway controlling vasomotor tone. When anaesthetising patients with coronary artery disease, maintain coronary perfusion pressure and avoid tachycardia.
Downloaded from http://ceaccp.oxfordjournals.org/ at Universitatea de Medicina si Farmacie ''Carol Davila on March 11, 2013
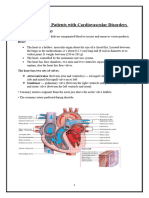
Anatomy
The two coronary ostia arise from the sinuses of Valsalva just above the aortic valve. The left coronary artery divides into the left anterior descending artery and circumflex artery. It supplies the lateral and anterior walls of the left ventricle, and the anterior two thirds of the interventricular septum. The right coronary artery supplies the right ventricle, the posterior wall of the left ventricle and posterior third of the septum. The major coronary arteries divide into epicardial arteries. Intramuscular arteries penetrate the myocardium perpendicularly to form subendocardial arterial plexuses. Most of the blood from left ventricular muscle drains into the coronary sinus. The anterior cardiac vein receives blood from the right ventricular muscle. They both open into the right atrium. Thebesian veins drain a small proportion of coronary blood directly into the cardiac chambers and account for true shunt.
Perfusion time
Any increase in heart rate impinges on diastolic time more than systolic time and reduces the perfusion time.
Vessel wall diameter
Vasomotor tone and deposits inside the vascular lumen determine the vessel wall diameter. The interplay of various mechanisms that regulate the coronary vasomotor tone usually favours vasodilatation (Fig. 1).
Factors influencing the vasomotor tone
Myocardial metabolism
Vasomotor tone is almost exclusively determined by local metabolic oxygen demand. Hypoxia causes coronary vasodilatation directly but also releases adenosine and opens ATP-sensitive potassium channels. Pre-capillary sphincters are relaxed and more capillaries recruited.
Tamilselvi Ramanathan FRCA Specialist Registrar in Anaesthesia Queens Medical Centre Nottingham NG7 2UH Fax: 01159 700739 E-mail: tamilselvir@hotmail.com (for correspondence) Henry Skinner FRCA Consultant Anaesthetist Nottingham City Hospital Nottingham NG5 1PB
Determinants of coronary blood flow
Coronary perfusion pressure
During systole, intramuscular blood vessels are compressed and twisted by the contracting
doi 10.1093/bjaceaccp/mki012
Autoregulation
Under resting conditions, coronary blood flow remains constant between mean arterial
Continuing Education in Anaesthesia, Critical Care & Pain | Volume 5 Number 2 2005 The Board of Management and Trustees of the British Journal of Anaesthesia [2005]. All rights reserved. For Permissions, please email: journals.permissions@oupjournals.org
61
Coronary blood flow
Sympathetic stimulation
Parasympathetic stimulation
Angiotensin II
M AT EDRF nitric oxide
vasoconstriction in stressed patients. The other peptides cause endothelium-mediated vasodilatation. Angiotensin II causes coronary vasoconstriction independent of sympathetic innervation. It also enhances calcium influx and releases endothelin, the strongest vasoconstrictor peptide yet identified in humans. Angiotensin-converting enzyme inactivates bradykinin, a vasodilator.
Downloaded from http://ceaccp.oxfordjournals.org/ at Universitatea de Medicina si Farmacie ''Carol Davila on March 11, 2013
Vasoconstriction
Vasodilatation
Vascular endothelium
Hypoxia K+ATP Endothelin ET Adenosine Shear forces Intraluminal pressure
Fig. 1 Factors affecting coronary vasomotor tone. a alpha receptor, b beta receptor, M muscarinic receptor, AT angiotensin receptor, ET endothelin receptor, K ATP ATP-sensitive potassium channel. Vasomotor tone is ultimately mediated by the vascular endothelium, which secretes vasodilators; endothelium derived relaxant factor (EDRF), nitric oxide and endothelin, a potent vasoconstrictor.
The vascular endothelium is the final common pathway regulating vasomotor tone. It modulates the contractile activity of the underlying smooth muscle through synthesis and secretion of vasoactive substances in response to blood flow, circulating hormones and chemical substances. Vasorelaxants are endothelium-derived relaxing factor, nitric oxide, prostacyclin and bradykinin. Vasoconstrictors include endothelin and thromboxane A2. The net response depends on the balance between the two opposing groups.2
Myocardial oxygen balance
Oxygen delivery is the product of arterial oxygen carrying capacity and myocardial blood flow. The diastolic pressure time index (DPTI) is a useful measure of coronary blood supply and is the product of the coronary perfusion pressure and diastolic time. Similarly, oxygen demand can be represented by the tension time index (TTI), the product of systolic pressure and systolic time. The ratio DPTI/TTI is the endocardial viability ratio (EVR) and represents the myocardial oxygen supply-demand balance. The EVR is normally 1 or more. A ratio <0.7 is associated with subendocardial ischaemia. Such a value may be reached in a patient with the following physiological data: Blood pressure 180/95 mm Hg Heart rate 120 min1 LVEDP 15 mm Hg DPTI 80 mm Hg (60 s/heart rate 0.2 s) 24 s mm Hg TTI 180 mm Hg 0.2 s 36 s mm Hg EVR 0.67 Note that systolic time is typically fixed at 200 ms, with diastole occupying the remaining time.
pressures of 60140 mm Hg. Beyond this range, flow becomes pressure-dependent. Probable mechanisms include the myogenic response to intraluminal pressure changes (fast) and metabolic regulation (slow). The myocardial oxygen tension and presence of vasoconstrictors or vasodilators influence the range of coronary autoregulation.
Nervous control
Autonomic influences are generally weak. It is difficult to tease out the role of neural control on coronary blood flow, as the metabolic effects of any change in blood pressure, heart rate and contractility dominate the subsequent response. The epicardial blood vessels primarily have a receptors, stimulation of which produces vasoconstriction. Intramuscular and subendocardial blood vessels predominantly have b2 receptors (vasodilatation). Sympathetic stimulation increases myocardial blood flow through an increased metabolic demand and a predominance of b receptor activation. Alpha stimulation may play a role in the distribution of blood flow within the myocardium by restricting metabolically mediated flow increase and exerting an anti-steal affect. Parasympathetic influences are minor and weakly vasodilatory. The vasodilatory effect of acetylcholine depends on an intact endothelium.
Diseases affecting the coronary blood flow
The coronary circulation functions in a state of active vasodilatation. Abnormal endothelial nitric oxide production may play a role in diabetes, atherosclerosis and hypertension.
Humoral control
Most vasoactive hormones require an intact vascular endothelium. The peptide hormones include antidiuretic hormone, atrial natriuretic peptide, vasoactive intestinal peptide, and calcitonin gene-related peptide. Antidiuretic hormone in physiological concentration has little effect on the coronary circulation but causes
Coronary artery disease
Deposits of lipids, smooth muscle proliferation and endothelial dysfunction reduce the luminal diameter. Critical stenosis occurs when coronary blood flow is unable to respond to an increase in
62
Continuing Education in Anaesthesia, Critical Care & Pain | Volume 5 Number 2 2005
Coronary blood flow
metabolic demand, usually when the diameter is reduced by 50%. Resting flow becomes affected if the diameter is reduced by 80%. With increasing stenosis, distal arterioles dilate maximally to preserve flow up to the point where the vascular bed is maximally dilated. Further stenosis leads to a drop in flow and flow becomes pressure dependent. Flow diverted into a dilated parallel bed proximal to a stenosis is called coronary steal and can aggravate ischemia. Flow in collaterals is also often pressure dependent.
coronary dilatation and lower LVEDP. The oxygen demand is lessened because of decreases in contractility and pressure load.
Drugs acting on angiotensin
Angiotensin-converting enzyme inhibitors reduce conversion of angiotensin I to angiotensin II. These drugs reduce angiotensinmediated vasoconstriction and enhance myocardial perfusion by vasodilatation without reflex tachycardia. Over time, it also regulates fibrous tissue formation after tissue injury.3 Drugs such as losartan are angiotensin receptor antagonists and enhance endothelial nitric oxide release.
Downloaded from http://ceaccp.oxfordjournals.org/ at Universitatea de Medicina si Farmacie ''Carol Davila on March 11, 2013
Hypertension
The left ventricle undergoes hypertrophy in response to raised afterload. The myofibrillar growth outstrips the capillary network, resulting in decreased capillary density. Raised intramyocardial pressure lowers the subendocardial blood flow. The pressure load increases myocardial work and oxygen demand. There is also an impaired vasomotor response to hypoxia in hypertrophied tissue that makes it susceptible to ischaemia.
Potassium channel openers
Nicorandil is a novel anti-anginal agent. Increased potassium efflux results in reduced intracellular calcium and muscle relaxation. It dilates both normal and stenotic segments of the coronary arteries.
Heart failure
Impaired ejection results in larger diastolic volumes, raised LVEDP and lower coronary perfusion pressure. Sympatheticmediated systemic vasoconstriction may help to improve the myocardial perfusion but increases pressure load and oxygen demand.
b-Blockers
Coronary blood vessels contain b2 receptors. Chronotropy and inotropy depends on b1 stimulation. Recent investigations in patients with coronary heart disease suggest that b-blockers do not depress the cardiac output as much as originally thought. The reduction in the heart rate prolongs the diastolic perfusion time and they inhibit stress-induced rises in myocardial contractility. In patients on cardioselective b1-blockers, unopposed systemic b2 stimulation reduces the afterload, improves ejection fraction, and exerts a positive inotropic effect.4
Drugs and coronary blood flow
Antiplatelet drugs, anticoagulants and lipid lowering drugs
These agents act inside the lumen to prevent further reduction in the vessel diameter. Statins inhibit HMG CoA reductase, an enzyme involved in cholesterol synthesis. Antiplatelet drugs prevent platelet aggregation, often the initial step in the formation of an occlusive thrombus. Antithrombin agents act at various sites in the coagulation cascade to inhibit thrombin formation.
Vasopressors and inotropes
These drugs restore coronary perfusion pressure in hypotensive patients and may be especially beneficial in those patients heading towards the lower end of the autoregulation range. Any increase in aortic diastolic pressure may be offset by an increase in myocardial oxygen demand related to higher workload, contractility and heart rate. In the failing heart, inotropes also reduce the LVEDP.
Nitrates
Nitrates produce vasodilatation in all vascular beds, mediated by nitric oxide release. They relieve coronary vasospasm but their main benefit is to reduce preload, afterload and to increase maximal coronary dilation. Benefits may be offset by reflex tachycardia. Regional blood flow is improved due to dilatation of collaterals and a lower LVEDP.
Anaesthesia and myocardial oxygen balance
Halogenated anaesthetic agents activate ATP-sensitive potassium channels and lower intracellular calcium. This results in negative inotropy and mimic the protective effect of discrete episodes of myocardial ischaemia before a sustained ischaemic insult, so-called ischaemic preconditioning. In addition, coronary vasodilation and reduced afterload generally results in a favourable myocardial oxygen supplydemand ratio. Isoflurane in particular causes coronary vasodilatation. Arterioles (resistance vessels) are dilated more than epicardial (conductance) vessels. Theoretically, coronary steal may occur
Calcium channel blockers
Compared to the non-dihydropyridines (verapamil and diltiazem) the dihydropyridines (nifedipine) produce more vasodilatation, less inhibition of the sinus and atrioventricular nodes, and less negative inotropy. The myocardial oxygen supply improves due to
Continuing Education in Anaesthesia, Critical Care & Pain | Volume 5 Number 2 2005
63
Coronary blood flow
in a distinct anatomical pattern of coronary artery disease but this has not been borne out in practice. Isoflurane however, can provoke ischaemia in patients with coronary artery disease if tachycardia and hypotension is permitted. Sevoflurane and halothane do not cause tachycardia or maldistribution of myocardial perfusion.5 Perioperative stress results in sympathetically mediated tachycardia, hypertension, increase in shear forces and increased myocardial oxygen demand. Central neuraxial block obtunds this potentially harmful response but any substantial fall in blood pressure will lower the coronary perfusion pressure. Thoracic epidural analgesia also blocks sympathetic outflow to the heart. Sympathetic stimulation produces coronary vasodilatation in healthy individuals but vasoconstriction in patients with coronary artery disease.6
References
1. Guyton AC, Hall JE, eds. Textbook of Medical Physiology, 9th Edn. Philadelphia: WB Saunders, 1996 2. Kaplan JA, Reich DL, Konstadt SN, eds. Cardiac Anaesthesia, 4th Edn. Philadelphia: WB Saunders, 1999 3. Schmermund A, Lerman LO, Ritman EL, Rumberger JA. Cardiac production of angiotensin II and its pharmacologic inhibition: effects on the coronary circulation. Mayo Clinic Proceedings 1999; 74: 50313
Downloaded from http://ceaccp.oxfordjournals.org/ at Universitatea de Medicina si Farmacie ''Carol Davila on March 11, 2013
4. Biccard BM. Perioperative b blockade and haemodynamic optimisation. Anaesthesia 2004; 59: 608 5. Nader-Djalal N, Knight PR. Volatile anaesthetic effects on ischemic myocardium. Curr Opin Anaesthesiol 1998; 11: 4036 6. Norbert R. Central neuroaxis blockade and coronary circulation. Curr Opin Anaesthesiol 1998; 11: 51720
See multiple choice questions 4853.
64
Continuing Education in Anaesthesia, Critical Care & Pain | Volume 5 Number 2 2005
Das könnte Ihnen auch gefallen
- Coronary Circulation PhysiologyDokument25 SeitenCoronary Circulation PhysiologyDerrick Ezra Ng100% (1)
- Mekanisme Angina - Dr. Putra Fhonna - Magang KardiologiDokument7 SeitenMekanisme Angina - Dr. Putra Fhonna - Magang KardiologiPutra FhonnaNoch keine Bewertungen
- Coronary Artery DiseaseDokument13 SeitenCoronary Artery DiseaseChristianHanjokarNoch keine Bewertungen
- AnaesDokument16 SeitenAnaessindujasaravananNoch keine Bewertungen
- Ischemic Heart DiseaseDokument43 SeitenIschemic Heart DiseasevolcanflameNoch keine Bewertungen
- Coronary Circulation & Pathologies: Arif Hussain Demonstrator Anesthesia Ipms-KmuDokument28 SeitenCoronary Circulation & Pathologies: Arif Hussain Demonstrator Anesthesia Ipms-Kmuayub khanNoch keine Bewertungen
- Leading Causes of The Global Burden of DiseaseDokument44 SeitenLeading Causes of The Global Burden of Diseasenathan asfahaNoch keine Bewertungen
- Cardiovascular Systems Factors and RegulationDokument51 SeitenCardiovascular Systems Factors and RegulationTkNoch keine Bewertungen
- Blood LossDokument6 SeitenBlood LossDungani AllanNoch keine Bewertungen
- The Normal Physiology of The Heart: Vikkineshwaran Siva SubramaniamDokument4 SeitenThe Normal Physiology of The Heart: Vikkineshwaran Siva SubramaniamSivamala MalaNoch keine Bewertungen
- CHAPTER 21 - Coronary CirculationDokument5 SeitenCHAPTER 21 - Coronary Circulationg_komolafeNoch keine Bewertungen
- 23circulation Part 1Dokument13 Seiten23circulation Part 1Jaydave PatelNoch keine Bewertungen
- The Cardiovascular System - Blood VesselsDokument39 SeitenThe Cardiovascular System - Blood VesselsMohamed YousufNoch keine Bewertungen
- Pathophysiology of Myocardial InfarctionDokument4 SeitenPathophysiology of Myocardial InfarctionYhr YhNoch keine Bewertungen
- Coronary Blood Flow Regulation and DeterminantsDokument4 SeitenCoronary Blood Flow Regulation and DeterminantsSinisa RisticNoch keine Bewertungen
- Shock PresentaionDokument30 SeitenShock PresentaionKennedy Ng'andweNoch keine Bewertungen
- Magnet Space Materijal ENGDokument40 SeitenMagnet Space Materijal ENGIvana MilosavljevicNoch keine Bewertungen
- Blood parameters and their relationship to cardiovascular and cerebrovascular healthDokument34 SeitenBlood parameters and their relationship to cardiovascular and cerebrovascular healthYupi RedNoch keine Bewertungen
- 03-07 Lecture Coronary CirculationDokument29 Seiten03-07 Lecture Coronary Circulationaspalavista50% (2)
- Cardiovascular DrugsDokument33 SeitenCardiovascular DrugsKish Gabriel100% (1)
- Fisiopatologia Del Shock Cardiogenico Por Iam PDFDokument12 SeitenFisiopatologia Del Shock Cardiogenico Por Iam PDFYESSICA CARENALGANoch keine Bewertungen
- General Internal Medicine Hour: HypertensionDokument33 SeitenGeneral Internal Medicine Hour: HypertensionRadley Jed C. PelagioNoch keine Bewertungen
- The Pharmacologic Treatment of Myocardial InfarctionDokument3 SeitenThe Pharmacologic Treatment of Myocardial InfarctiongailNoch keine Bewertungen
- Case 2 SlosDokument7 SeitenCase 2 SlosNamarNoch keine Bewertungen
- Myocardial Ischemia: Dr. Wael H. Mansy, MDDokument37 SeitenMyocardial Ischemia: Dr. Wael H. Mansy, MDHaleema SultanNoch keine Bewertungen
- Blood Pressure RegulationDokument3 SeitenBlood Pressure RegulationiMaibelle BelleNoch keine Bewertungen
- Cardiogenic ShockDokument8 SeitenCardiogenic ShockMAE RACHELLE LAMOSTENoch keine Bewertungen
- Cardiac PharmocologyDokument17 SeitenCardiac Pharmocologysuhas.kandeNoch keine Bewertungen
- Myocardial Ischemia and Coronary Artery Disease PathophysiologyDokument81 SeitenMyocardial Ischemia and Coronary Artery Disease PathophysiologyroshamaharaniNoch keine Bewertungen
- CVS Lect 6 Blood Pressure, PathophysiologyDokument13 SeitenCVS Lect 6 Blood Pressure, PathophysiologySherwan R Shal100% (5)
- Fluid Challenge Weil 1Dokument9 SeitenFluid Challenge Weil 1gamabe100% (1)
- Cardiovascular Physiology: The Autonomic Nervous SystemDokument8 SeitenCardiovascular Physiology: The Autonomic Nervous SystemRidha Surya NugrahaNoch keine Bewertungen
- Blood PressureDokument8 SeitenBlood PressureUmair RaoNoch keine Bewertungen
- Cardiovascular and Autonomic Influences On Blood Pressure: John E. Jones,, Aruna R. Natarajan,,, and Pedro A. JoseDokument23 SeitenCardiovascular and Autonomic Influences On Blood Pressure: John E. Jones,, Aruna R. Natarajan,,, and Pedro A. JoseLulu LuwiiNoch keine Bewertungen
- Med Surg 2Dokument76 SeitenMed Surg 2sham gowliNoch keine Bewertungen
- Coronary blood flow regulation and determinantsDokument4 SeitenCoronary blood flow regulation and determinantsTri RachmadijantoNoch keine Bewertungen
- Physiology of The Coronary Blood FlowDokument14 SeitenPhysiology of The Coronary Blood FlowgopscharanNoch keine Bewertungen
- Heart Guide 2022Dokument13 SeitenHeart Guide 2022AnuNoch keine Bewertungen
- Control of Blood Flow: After Reading This Chapter You Should Be Able ToDokument12 SeitenControl of Blood Flow: After Reading This Chapter You Should Be Able ToDrbee10Noch keine Bewertungen
- Hypertension and Cardiovascular DiseaseDokument99 SeitenHypertension and Cardiovascular DiseaseMiguel CuevasNoch keine Bewertungen
- Ischemic Heart DiseaseDokument6 SeitenIschemic Heart Diseaseابو الجودNoch keine Bewertungen
- Shock Is The Clinical Syndrome That Results FromDokument43 SeitenShock Is The Clinical Syndrome That Results Fromnathan asfahaNoch keine Bewertungen
- Literature ReviewDokument28 SeitenLiterature ReviewNyo LayNoch keine Bewertungen
- MF-local Circulation 2016Dokument61 SeitenMF-local Circulation 2016OnSolomonNoch keine Bewertungen
- Cardiogenic ShockDokument31 SeitenCardiogenic ShockLovelights ZamoraNoch keine Bewertungen
- Cardiovascular Pathophysiology ExplainedDokument32 SeitenCardiovascular Pathophysiology ExplainedSaif AliNoch keine Bewertungen
- Front Page: Effects of Systemic Vascular Resistance On The BodyDokument1 SeiteFront Page: Effects of Systemic Vascular Resistance On The BodyRodel Aguila SañoNoch keine Bewertungen
- Insuficiencia Cardiaca Congestiva IzquierdaDokument10 SeitenInsuficiencia Cardiaca Congestiva IzquierdaCindy Karina Carbajal MurilloNoch keine Bewertungen
- Ischemic Heart Disease and Myocardial InfarctionDokument73 SeitenIschemic Heart Disease and Myocardial InfarctionAngelEduardoVillarrealGiraldoNoch keine Bewertungen
- Circulatory Response To ExerciseDokument31 SeitenCirculatory Response To ExerciseFarhad GulNoch keine Bewertungen
- Athero 2 Dr. Raquid 2021Dokument93 SeitenAthero 2 Dr. Raquid 2021oreaNoch keine Bewertungen
- Drugs Used in Heart Failure: Pharmacology (2) PHAR 342Dokument19 SeitenDrugs Used in Heart Failure: Pharmacology (2) PHAR 342Dana HamarshehNoch keine Bewertungen
- Angina AssignmentDokument7 SeitenAngina AssignmentvictoriaNoch keine Bewertungen
- Asist. Lecturer Hasan Adnan Hashim Msc. Pharmacology and ToxicologyDokument52 SeitenAsist. Lecturer Hasan Adnan Hashim Msc. Pharmacology and Toxicologyمصطفى ابراهيم سعيدNoch keine Bewertungen
- Special Circulation - UnpriDokument44 SeitenSpecial Circulation - UnpriAnnisNoch keine Bewertungen
- LP HypertentionDokument16 SeitenLP HypertentionFitria NorkhalidaNoch keine Bewertungen
- Cathecholamine Changes in Splanchnic CirculationDokument6 SeitenCathecholamine Changes in Splanchnic Circulation037 Onpreeya LansaiNoch keine Bewertungen
- What Is Cardiogenic Shock?Dokument3 SeitenWhat Is Cardiogenic Shock?nipheyy dananNoch keine Bewertungen
- Pa Tho Physiology of Angina PectorisDokument2 SeitenPa Tho Physiology of Angina PectorisAnastasia FebianaNoch keine Bewertungen
- Beating with Precision: The Science of Cardiology: Understand the Intricacies of the Human HeartVon EverandBeating with Precision: The Science of Cardiology: Understand the Intricacies of the Human HeartNoch keine Bewertungen
- Barem Model An IIDokument1 SeiteBarem Model An IIjordandenise2Noch keine Bewertungen
- ARTICOLDokument11 SeitenARTICOLjordandenise2Noch keine Bewertungen
- Blacks Medical Dictionary Cu SemneDokument849 SeitenBlacks Medical Dictionary Cu SemneRoxana Damian100% (1)
- Ţesutul Conjunctiv: Celulele Şi Fibrele Ţesutului ConjunctivDokument17 SeitenŢesutul Conjunctiv: Celulele Şi Fibrele Ţesutului ConjunctivTeodor NeaguNoch keine Bewertungen
- Paradise Lost by John MiltonDokument191 SeitenParadise Lost by John MiltonBooks100% (5)
- Paradise Lost by John MiltonDokument191 SeitenParadise Lost by John MiltonBooks100% (5)
- TSR 9278 - DLR1 - OtherlandsDokument106 SeitenTSR 9278 - DLR1 - OtherlandsDiego RB100% (5)
- Literary Criticism ExamDokument1 SeiteLiterary Criticism ExamSusan MigueNoch keine Bewertungen
- Integrative Teaching Strategy - Module #6Dokument10 SeitenIntegrative Teaching Strategy - Module #6Joann BalmedinaNoch keine Bewertungen
- Psychological ContractDokument14 SeitenPsychological ContractvamsibuNoch keine Bewertungen
- Chapter IDokument30 SeitenChapter ILorenzoAgramon100% (2)
- MedCon Template - Melena+DOC+Septic ConditionDokument26 SeitenMedCon Template - Melena+DOC+Septic ConditionPramudia DeniNoch keine Bewertungen
- 2015 International Qualifications UCA RecognitionDokument103 Seiten2015 International Qualifications UCA RecognitionRodica Ioana BandilaNoch keine Bewertungen
- Lao Gi Vs CADokument2 SeitenLao Gi Vs CARichel DeanNoch keine Bewertungen
- Understanding First Language AcquisitionDokument4 SeitenUnderstanding First Language AcquisitionShiela Mae Saladaga TanNoch keine Bewertungen
- FREE Soroban Abacus Mental Math Learning - BasicDokument74 SeitenFREE Soroban Abacus Mental Math Learning - BasicTatyana Sukhomlinova100% (3)
- TPADokument9 SeitenTPAAli ShahNoch keine Bewertungen
- Human Resource Management and The Banking SectorDokument5 SeitenHuman Resource Management and The Banking SectorAkshay DagurNoch keine Bewertungen
- Lipid Extraction & IdentificationDokument19 SeitenLipid Extraction & IdentificationAldwin Ray Pamplona100% (2)
- Skripsi Tanpa Bab Pembahasan PDFDokument117 SeitenSkripsi Tanpa Bab Pembahasan PDFArdi Dwi PutraNoch keine Bewertungen
- Worksheets Section 1: Develop Quality Customer Service PracticesDokument3 SeitenWorksheets Section 1: Develop Quality Customer Service PracticesTender Kitchen0% (1)
- 10, Services Marketing: 6, Segmentation and Targeting of ServicesDokument9 Seiten10, Services Marketing: 6, Segmentation and Targeting of ServicesPreeti KachhawaNoch keine Bewertungen
- Task 2 AmberjordanDokument15 SeitenTask 2 Amberjordanapi-200086677100% (2)
- Dialogue CollectionDokument121 SeitenDialogue CollectionYo Yo Moyal Raj69% (13)
- CGS PPT FinalDokument14 SeitenCGS PPT FinalAbc Xyz100% (1)
- TaxGenie Introduction For Banks PDFDokument27 SeitenTaxGenie Introduction For Banks PDFsandip sawantNoch keine Bewertungen
- Part 3. Scaffolding Children's Understanding and Use of Language PDFDokument7 SeitenPart 3. Scaffolding Children's Understanding and Use of Language PDFMaksym BuchekNoch keine Bewertungen
- Sociology of Behavioral ScienceDokument164 SeitenSociology of Behavioral ScienceNAZMUSH SAKIBNoch keine Bewertungen
- Chapter 14 ECON NOTESDokument12 SeitenChapter 14 ECON NOTESMarkNoch keine Bewertungen
- MarketingDokument3 SeitenMarketingAli KhanNoch keine Bewertungen
- Ajzen - Constructing A Theory of Planned Behavior QuestionnaireDokument7 SeitenAjzen - Constructing A Theory of Planned Behavior QuestionnaireEstudanteSax100% (1)
- Critical Reading As ReasoningDokument18 SeitenCritical Reading As ReasoningKyle Velasquez100% (2)
- Data Rs910Dokument36 SeitenData Rs910Cusco PardoNoch keine Bewertungen
- Designing Organizational Structure: Specialization and CoordinationDokument30 SeitenDesigning Organizational Structure: Specialization and CoordinationUtkuNoch keine Bewertungen
- Essay 2Dokument4 SeitenEssay 2api-708904378Noch keine Bewertungen
- Moor defines computer ethics and its importanceDokument2 SeitenMoor defines computer ethics and its importanceNadia MalikNoch keine Bewertungen