Beruflich Dokumente
Kultur Dokumente
OTITIS EXTERNA Continuing Medical Education
Hochgeladen von
hanumzniiOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
OTITIS EXTERNA Continuing Medical Education
Hochgeladen von
hanumzniiCopyright:
Verfügbare Formate
Continuing Medical Education
Otitis externa
Martyn Fields FDSRCS FRCS FRACS is an otolaryngologist and head and neck surgeon.
There is little or no information on the incidence of otitis externa in New Zealand. In the USA a figure of four per 1 000 per annum is quoted, of which 1% (4 per 100 000) go on to become chronic. This gives a figure of over five million cases per annum treated by USA GPs. With New Zealands climate, extensive coastline and easy access to water, I suspect that the incidence is higher, but there is no data available at present. Ninety-seven per cent are treated by the general practitioner with no specialist ENT service involvement. Fungal: 10% (Aspergillus 80%, Candida 20%); mixed bacterial/ fungal infections common Viral: Otitis externa Haemorrhagica (bullous myringitis), Herpes Zoster and Simplex Dermatological: Eczema/seborrhoeic dermatitis/psoriasis (dont forget hypersensitivity/allergy to topical drops) Cerumen is protective being acidic and hydrophobic. In addition it contains lysozymes that inhibit bacterial growth. Too much or too little cerumen predisposes to otitis externa. Hair helps prevent entry of foreign bodies, however too much prevents migration and can add to cerumen build up, (particularly in older males where the hairs can have the effect of acting like steel rod reinforcing in concrete!).
Symptoms
Pain and/or discomfort limited to the EAM (itching through to severe pain) Deafness (conductive) Pre- and post-auricular lymph node enlargement/tenderness
Predisposing factors
Anatomical a narrow canal, excessive wax production Moisture swimming, perspiration, high humidity High environmental temperatures Mechanical removal of cerumen Trauma e.g. cotton-buds, fingernails, hearing aids, ear plugs, hair grips, paper clips etc. Chronic dermatological disease e.g. eczema, psoriasis, seborrhoeic dermatitis, acne Immuno-compromised Contaminated water (possibly)
Definition
Otitis externa is the generic term for any inflammatory condition of the external auditory meatus (EAM). It may be a local phenomenon or part of a generalised skin condition. Otitis externa can be subdivided into acute, recurrent-acute and chronic.
Signs
Erythema and swelling of the EAM skin with variable discharge/moist debris.
Anatomy/physiology of the EAM
The EAM is unique in being the only skin-lined cul-de-sac in the body. It is warm and humid and exfoliated skin provides an ideal growth medium for bacteria and fungi. The canal skin is unique in that it is continually migrating laterally carrying debris with it.
Aetiology of otitis externa
The cause is usually infective (bacterial or fungal) but non-infectious/ dermatological processes should not be forgotten. Bacterial: 80% - Staphylococcus aureus, Pseudomonas aeruginosa, Bacillus proteus
Clinical differential diagnosis of otorrhoea
The clinical appearance is rarely diagnostic but the following signs can give some clues. Culture from the
Acute fungal otitis externa
Chronic eczematous otitis externa
Chronic bacterial otitis externa
Furuncle
Chronic otitis externa with canal skin hypertrophy
Acute viral otitis externa (herpetic Ramsay Hunt Syndrome)
Photos from: A Colour Atlas of Otolaryngology. Published by Martin Dunitz.
deep part of the canal is required to confirm the diagnosis.
white conidiophores on white hyphae associated with aspergillus
Otitis externa
Acute bacterial: scanty white mucoid discharge (occasionally thick) Chronic bacterial: can be bloody often granulation tissue present Fungal: white to off-white discharge, but may be black, grey, bluish-green or yellow; black or
Otitis media with perforated tympanic membrane
Acute purulent white to yellow mucus with deep pain Serous clear mucus, especially in the presence of allergies Chronic intermittent purulent mucus without pain
Cerebrospinal fluid leak clear, thin and watery discharge Trauma bloody mucus Osteomyelitis discharge and odour
Management
Ear toilet
Most important is the removal of as much debris as possible. This is best achieved with suction (+/- microscopy)
Chronic otitis externa leading to canal stenosis
Total canal stenosis secondary to chronic otitis externa
Acute bacterial otitis externa
Volume 29 Number 2, April 2002
109
Continuing Medical Education Con
Continuing Medical Education
but dry mopping or gentle curettage with a Jobson Horn probe as an alternative. Cotton buds (other than for mopping out discharge around the meatal opening) are best avoided as they tend to push the debris further into the canal. Tissue spears tissue twisted into a point and inserted into the canal about 2cm then allowed to absorb the discharge (and repeated as required) can help clear a watery discharge and obtain deeper access when about to instil new drops. Open access to an ENT department for ear suction toilet for these patients would be the ideal and in some centres in New Zealand clinic nurses have been provided with additional training in ear suction toilet and this service is available. Funding is the major issue in other centres. One needs to visualise the tympanic membrane if possible to exclude otitis media or a tympanic membrane perforation. Syringing the ear is inadvisable if a perforation is present as it can lead to marked nausea and vertigo and damage to middle ear structures. It also often seems to make the otitis externa worse. Drying of the canals with a hair dryer if they get wet can be helpful. canal. The steroid component is important to settle the oedema. If vertigo occurs with the drops, warm the bottle in the hand for a few minutes first. Continue for three days beyond control of symptoms usually seven to ten days (up to 14 days if severe).
Analgesia
Analgesia depends on the severity of the pain. Paracetamol Codeine NSAIDs Opiates
Acute otitis externa
Sofradex Betnesol N Maxitrol eye drops Tobrex or Tobradex eye drops (for Pseudomonas check organism sensitivities first) Ciproxin HC no Phamac funding (for Pseudomonas check organism sensitivities first)
Acidification
Acidification is for maintenance/ chronic otitis externa.
Steroids
Steroids are mainly for their anti-inflammatory/oedema-reducing effects which help the itching and maintenance of canal patency.
Fungal otitis externa
Kenacomb Locorten and Vioform Daktarin 2% lotion Daktacort cream
Surgery
This is rarely required mainly as a last resort for the very narrow canal secondary to grossly hypertrophic canal skin. Swimmers osteomas can predispose to otitis externa and may require surgical removal.
Chronic eczematous otitis externa
Elocon lotion or cream 0.1% (mometasone furoate) Hydrocortisone cream 0.1% Olive oil or Almond oil (for the dry itchy canal)
Topical drop options
The standard 12 drops as directed on the bottles is totally inadequate! As a personal observation (during ventilation tube surgery), two drops rarely reaches the drum in a child, getting caught in the ear canal hairs by surface tension. A minimum of five drops was needed plus massage of the tragus and pinna to cover the canal skin. Use five to six drops, six to eight hourly. Lie on one side for five minutes after instilling drops manipulating the tragus by pumping it up and down and moving the pinna at intervals to encourage drops down the canal. If a wick is required for the very narrow canal, apply the drops three to four hourly whilst awake. Change the wick every two to five days with suction toilet depending on severity until no longer required to keep canal patent.
Maintenance
Surfers mixture Alcohol 70% Acetic acid 2% Hydrocortisone 1% Water 27% Two to five drops after swimming/ showering etc. This can be painful if the canal is already inflamed it can be diluted 50/50 with boiled water if it stings too much. Alternatively the alcohol can be left out of the formula. A homemade solution of 50% alcohol + 50% white vinegar is a further option, but does not help the itching. Vosol 3%1.2-propanediol diacetate, 2% acetic acid 0.02% benzethonium chloride in propylene glycol does not have
Culture
Culture and sensitivity is indicated if there is not a rapid response to first line topical drops. The sample should be taken from the deeper debris using a wire/cotton swab to reduce secondary bacterial contaminants. Ask the lab to look for bacteria and fungi.
Topical therapy
Antibiotic (or anti-fungal)/steroid drops. If the symptoms are worsening in spite of drops, consider an allergy/hypersensitivity to the drops. A wick is required for the very narrow or occluded canal (1/2 inch ribbon gauze or compressed foam such as a Pope wick) as it helps deliver drops to the deeper part of the
110
Volume 29 Number 2, April 2002
Continuing Medical Education
any steroid so patients often continue to complain of itching) Elocon Lotion or cream 0.1% (mometasone furoate)
Systemic treatment
Oral antibiotics
These are rarely needed; only use when otitis externa is persistent, or associated otitis media is present or when local or systemic spread has occurred beyond the EAM. Use systemic antibiotics in diabetics and the immuno-compromised. If the temperature is above 38.3C or pain is out of proportion to clinical findings suspect spread.
Prevention
Prevention of recurrence of otitis externa primarily consists of avoiding predisposing factors and treatment of underlying dermatological conditions. Swimming should be avoided for 7+ days after symptoms have settled. After bathing or swimming, options include using a hair dryer on the lowest heat setting, with the instillation of acidifying drops or surfers mixture afterwards. Avoid any manipulation of the skin of the external auditory canal (such as scratching or overzealous cleaning). This is where the topical steroids really help in reducing itching. If cerumen is difficult to remove, a ceruminolytic agent or a four per cent baking soda solution can be used to soften the cerumen first to help avoid any trauma when syringing. Ear plugs can be used for swimming but need to be kept clean to prevent re-infection. Bathing caps or neoprene ear wraps can offer better protection.
cal findings is a feature. Mortality is about 50% even with treatment urgent referral to an otolaryngologist is appropriate, treatment requires intravenous antibiotics and debridement/surgery.
Malignant change
Consider in chronic otitis externa where an area of inflammation or ulceration persists in spite of active treatment or when the pain seems excessive for the clinical findings, consider a malignancy, usually a squamous cell carcinoma of the EAM.
Complications
Furuncle
Staphylococcal abscess in the lateral third (cartilagenous part) of the ear canal from an obstructed apo-pilosebaceous gland. The lesions may be multiple and recur. The pain is severe and may require surgical drainage plus topical and systemic antibiotics.
Summary
The vast majority of cases of otitis externa respond to toilet and the application of steroid/antibiotic drops. Keep water out of the ears during treatment and for three days after the symptoms settle. If symptoms persist obtain a deep canal culture sample change drops if appropriate. Oral/systemic antibiotics if spreading or medically indicated If no improvement specialist referral/suction toilet. Maintenance/prevention with topical acidification or oil drops.
Necrotising (malignant) otitis externa
Consider the possibility in diabetics, the elderly or immuno-compromised. This is an osteomyelitis of the mastoid or temporal bone, usually caused by pseudomonas. Severe pain/headache out of proportion to the clini-
Bibliography
Blake P, Matthews R, Hornibrook J. When not to syringe an ear. NZ Med J 1998 Nov 13;111(1077):4224. Holten KB, Gick J. Management of the patient with otitis externa. J Fam Pract 2001 Apr; 50(4):35360. Rea P, Joseph T. A GP strategy for otitis externa. Practitioner 1998 Jun; 242(1587):4668, 4701.
Rowlands S, Devalia H, Smith C, Hubbard R, Dean A. Otitis externa in UK general practice: a survey using the UK General Practice Research Database. Br J Gen Pract 2001 Jul; 51(468):5338. Sander R. Otitis externa: a practical guide to treatment and prevention. Am Fam Physician 2001 Mar 1; 63(5):92736, 9412. Roland PS. Chronic external otitis Ear Nose Throat J 2001 Jun; 80 (6 Suppl):126.
Volume 29 Number 2, April 2002
111
Das könnte Ihnen auch gefallen
- Effects of Child Abuse and Neglect For Children and AdolescentsDokument15 SeitenEffects of Child Abuse and Neglect For Children and AdolescentsMaggie YungNoch keine Bewertungen
- H8SpinalAn PDFDokument8 SeitenH8SpinalAn PDFhanumzniiNoch keine Bewertungen
- Acute Scrotum 231016 PDFDokument50 SeitenAcute Scrotum 231016 PDFDany Dias100% (1)
- Lec.9 Sinonasal TumorsDokument25 SeitenLec.9 Sinonasal TumorsMariam QaisNoch keine Bewertungen
- Case Report Epilepsy (English)Dokument18 SeitenCase Report Epilepsy (English)Ressa OashttamadeaNoch keine Bewertungen
- XA6 - Emergency Provision Workbook 2020 v0 - 5 - CKDokument35 SeitenXA6 - Emergency Provision Workbook 2020 v0 - 5 - CKguyNoch keine Bewertungen
- Otic and Ohthalmic AgentsDokument46 SeitenOtic and Ohthalmic AgentsAlyssa Leonor NabutasNoch keine Bewertungen
- Craniofacial SyndromesDokument101 SeitenCraniofacial SyndromesSaranya MohanNoch keine Bewertungen
- Pediatric Blistering Diseases: MSU/Beaumont Health Dermatology Residency ProgramDokument80 SeitenPediatric Blistering Diseases: MSU/Beaumont Health Dermatology Residency ProgramGeoRNoch keine Bewertungen
- ENT Quick ReviewDokument6 SeitenENT Quick ReviewWade100% (1)
- Assessment and Initial Management Trauma PatientDokument69 SeitenAssessment and Initial Management Trauma PatientdrpagrawNoch keine Bewertungen
- Drug StudyDokument10 SeitenDrug StudybaniniycsebNoch keine Bewertungen
- Skin Ospe PDFDokument29 SeitenSkin Ospe PDFFahad2036Noch keine Bewertungen
- Ryan Martin Ko, M.DDokument54 SeitenRyan Martin Ko, M.DDhaval Makwana100% (2)
- Guideline Konjungtivitis CPG-11 PDFDokument33 SeitenGuideline Konjungtivitis CPG-11 PDFhanumzniiNoch keine Bewertungen
- Mangune v. Ermita (2016)Dokument3 SeitenMangune v. Ermita (2016)Cristelle Elaine Collera100% (1)
- Ve Siculo Bull Ous DiseasesDokument73 SeitenVe Siculo Bull Ous DiseasesAARYANoch keine Bewertungen
- Skin and Soft Tissue Injuries & InfectionsDokument221 SeitenSkin and Soft Tissue Injuries & InfectionsMario Espinosa100% (1)
- Depressed Fracture: Modul Bedah, July 2021Dokument31 SeitenDepressed Fracture: Modul Bedah, July 2021Muhammad MuhidNoch keine Bewertungen
- Survey QuestionnaireDokument2 SeitenSurvey Questionnairecyrusbatayan100% (1)
- Benign Tumors of LarynxDokument48 SeitenBenign Tumors of LarynxVilZan MominNoch keine Bewertungen
- Common Ent EmergenciesDokument65 SeitenCommon Ent EmergenciesferaNoch keine Bewertungen
- YakultDokument15 SeitenYakultMlb T. De TorresNoch keine Bewertungen
- ParecoxibDokument2 SeitenParecoxibPeetah PanNoch keine Bewertungen
- Tinea UnguiumDokument8 SeitenTinea UnguiumwirdahajaNoch keine Bewertungen
- Icd XDokument3 SeitenIcd XR Ghianesya GantinaNoch keine Bewertungen
- Otitis ExternaDokument14 SeitenOtitis ExternaRizkaGayoNoch keine Bewertungen
- Diabetic Foot: by Myrna Rita PMRDokument33 SeitenDiabetic Foot: by Myrna Rita PMRDianNurlitaAnggrainiNoch keine Bewertungen
- Hordeolum - Background, Pathophysiology, EpidemiologyDokument6 SeitenHordeolum - Background, Pathophysiology, EpidemiologyKeren SingamNoch keine Bewertungen
- Ludwig AnginaDokument7 SeitenLudwig AnginaCak BasitNoch keine Bewertungen
- Fever of Unknown OriginDokument26 SeitenFever of Unknown OriginFiona Yona Sitali100% (1)
- Frostnip & Frostbite - The BasicsDokument1 SeiteFrostnip & Frostbite - The BasicsjpackaNoch keine Bewertungen
- Komplikasi RhinosinusitisDokument54 SeitenKomplikasi RhinosinusitisWilda Kamila SungkarNoch keine Bewertungen
- Seidel's TestDokument13 SeitenSeidel's TestFahcrezaNoch keine Bewertungen
- Ocular InjuryDokument46 SeitenOcular InjurysnyNoch keine Bewertungen
- Efusi Pleura & EmpyemaDokument47 SeitenEfusi Pleura & EmpyemaArumLaksmitaDewiNoch keine Bewertungen
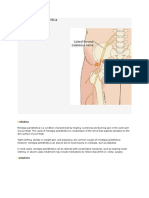
- Maralgia ParastheticaDokument8 SeitenMaralgia ParastheticaaliNoch keine Bewertungen
- Eponymous Signs in EntDokument10 SeitenEponymous Signs in Entmkct111Noch keine Bewertungen
- Jurnal Reading: Pembimbing: DR - Erna M Marbun, SPTHTDokument7 SeitenJurnal Reading: Pembimbing: DR - Erna M Marbun, SPTHTJessica LawrenceNoch keine Bewertungen
- Ear Canal Granuloma: Presentator: Anggoro Eka Raditya Moderator: Dr. Yayan MitayaniDokument76 SeitenEar Canal Granuloma: Presentator: Anggoro Eka Raditya Moderator: Dr. Yayan MitayaniAldy Bima100% (1)
- Examination of An UlcerDokument2 SeitenExamination of An UlcerHongMingNoch keine Bewertungen
- Glaucoma GuidelinesDokument28 SeitenGlaucoma GuidelinesRina RostianaNoch keine Bewertungen
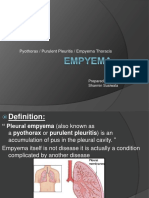
- Pyothorax / Purulent Pleuritis / Empyema Thoracis: Prepared By: Sharmin SusiwalaDokument22 SeitenPyothorax / Purulent Pleuritis / Empyema Thoracis: Prepared By: Sharmin SusiwalaAnkan Dey100% (1)
- Notes, 1/e: Acute and Chronic Inflammation of LarynxDokument23 SeitenNotes, 1/e: Acute and Chronic Inflammation of LarynxvkNoch keine Bewertungen
- Colour of UrineDokument1 SeiteColour of Urinetmunroe961Noch keine Bewertungen
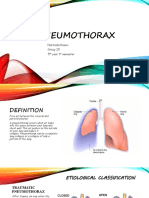
- Pneumothorax: Narmada Kasuni Group 25 5 Year 1 SemesterDokument18 SeitenPneumothorax: Narmada Kasuni Group 25 5 Year 1 SemesterNarmada PemathilakaNoch keine Bewertungen
- #Disease of External EarDokument4 Seiten#Disease of External EarameerabestNoch keine Bewertungen
- Cogan Syndrome Surger 4, AnkitDokument18 SeitenCogan Syndrome Surger 4, AnkitAnkit Tonger AnkyNoch keine Bewertungen
- Trigeminal NeuralgiaDokument2 SeitenTrigeminal NeuralgiaBryan Lloyd RayatNoch keine Bewertungen
- Acute Suppurative Otitis MediaDokument19 SeitenAcute Suppurative Otitis MediaRajesh Sharma100% (1)
- Purpura: Non-Palpable Purpura Palpable PurpuraDokument1 SeitePurpura: Non-Palpable Purpura Palpable PurpuramarishuenNoch keine Bewertungen
- Omphalocele Gastroschiasis and Umbilical HerniaDokument55 SeitenOmphalocele Gastroschiasis and Umbilical Herniamaverick boyNoch keine Bewertungen
- Pityriasis Rosea - Background, Pathophysiology, EtiologyDokument4 SeitenPityriasis Rosea - Background, Pathophysiology, EtiologysyahrulroziNoch keine Bewertungen
- Airway Management I. Airway 1. Causes of Airway ObstructionDokument1 SeiteAirway Management I. Airway 1. Causes of Airway ObstructionDelicateDogNoch keine Bewertungen
- MILIARIADokument6 SeitenMILIARIARien Anggraini RazakNoch keine Bewertungen
- Fraktur Dan Infeksi TulangDokument25 SeitenFraktur Dan Infeksi TulangAnonymous HAbhRTs2TfNoch keine Bewertungen
- 194 Surgical Cases PDFDokument160 Seiten194 Surgical Cases PDFkint100% (4)
- in Growing Toe NailDokument33 Seitenin Growing Toe NailEka CresentiaNoch keine Bewertungen
- Stevens-Johnson SyndromeDokument13 SeitenStevens-Johnson SyndromeJoyce Blancaflor LoganNoch keine Bewertungen
- 5 - Space Occupying LesionsDokument39 Seiten5 - Space Occupying LesionsAmmarNoch keine Bewertungen
- Case Presentation: by Michael ArmstrongDokument21 SeitenCase Presentation: by Michael ArmstrongWirawan Amirul BahriNoch keine Bewertungen
- Systemic Lupus Eritematus Kuliah KlerkDokument76 SeitenSystemic Lupus Eritematus Kuliah KlerkAnonymous y6NmP9NHkYNoch keine Bewertungen
- Csom (TT)Dokument24 SeitenCsom (TT)SamirNoch keine Bewertungen
- Typhoid FeverDokument2 SeitenTyphoid FeverSarah BenjaminNoch keine Bewertungen
- Tscherne Classification PDFDokument1 SeiteTscherne Classification PDFVirtues GracesNoch keine Bewertungen
- Episkleritis N Skleritis EditDokument12 SeitenEpiskleritis N Skleritis EditAnonymous HgX3mN1oNoch keine Bewertungen
- GonioskopiDokument40 SeitenGonioskopiRaissaNoch keine Bewertungen
- Clinical Manifestations and Diagnosis of Urinary Tract Obstruction and Hydroneph PDFDokument32 SeitenClinical Manifestations and Diagnosis of Urinary Tract Obstruction and Hydroneph PDFAmjad Saud0% (1)
- Dermatoscopy and Skin Cancer, updated edition: A handbook for hunters of skin cancer and melanomaVon EverandDermatoscopy and Skin Cancer, updated edition: A handbook for hunters of skin cancer and melanomaNoch keine Bewertungen
- Doctor Franke OtitisDokument6 SeitenDoctor Franke OtitisMelanie McguireNoch keine Bewertungen
- Otitis Externa: Physician. 2001 Mar 1 63 (5) :927-937Dokument11 SeitenOtitis Externa: Physician. 2001 Mar 1 63 (5) :927-937Nikita Rizky ArimamiNoch keine Bewertungen
- Tutorials: Screen Shoot ProgramsDokument4 SeitenTutorials: Screen Shoot ProgramshanumzniiNoch keine Bewertungen
- E-Hospital Assignment: Valyandra P (20121030036)Dokument2 SeitenE-Hospital Assignment: Valyandra P (20121030036)hanumzniiNoch keine Bewertungen
- Is Topical Mupirocin SaferDokument1 SeiteIs Topical Mupirocin SaferhanumzniiNoch keine Bewertungen
- The British Journal of DermatologyDokument7 SeitenThe British Journal of DermatologyhanumzniiNoch keine Bewertungen
- Bullous Pemphigoid Guidelines 2012Dokument15 SeitenBullous Pemphigoid Guidelines 2012Dzulkifli I. DotutinggiNoch keine Bewertungen
- Scottish Intercollegiate Guidelines Network .2010.management of Sore Throat and Indications ForDokument2 SeitenScottish Intercollegiate Guidelines Network .2010.management of Sore Throat and Indications ForhanumzniiNoch keine Bewertungen
- C M B C: Guidelines For Post-Dates PregnancyDokument6 SeitenC M B C: Guidelines For Post-Dates PregnancyhanumzniiNoch keine Bewertungen
- Otitis Externa A Practical Guide 2001Dokument10 SeitenOtitis Externa A Practical Guide 2001hanumzniiNoch keine Bewertungen
- Resume - EportfolioDokument3 SeitenResume - Eportfolioapi-337162374Noch keine Bewertungen
- Chapter 3 Definition - DisabilityDokument12 SeitenChapter 3 Definition - DisabilityAnimesh KumarNoch keine Bewertungen
- Form Lplpo Pustu Dan PoskesdesDokument3 SeitenForm Lplpo Pustu Dan PoskesdesristiNoch keine Bewertungen
- ProVari ManualDokument16 SeitenProVari ManualPatrickNoch keine Bewertungen
- Extended and Expanded Roles of Nurses 2Dokument1 SeiteExtended and Expanded Roles of Nurses 2Sivaprasad SNoch keine Bewertungen
- Intermittent Positive Pressure BreathingDokument12 SeitenIntermittent Positive Pressure BreathingHitesh RohitNoch keine Bewertungen
- VedicReport10 29 202211 43 48AMDokument1 SeiteVedicReport10 29 202211 43 48AMAvish DussoyeNoch keine Bewertungen
- MR Mohan LalDokument5 SeitenMR Mohan LalRajkumarNoch keine Bewertungen
- Pediatrics Rapid RevisionDokument72 SeitenPediatrics Rapid RevisionWorld MedclickzNoch keine Bewertungen
- Health Beliefs and PracticesDokument7 SeitenHealth Beliefs and Practicesapi-283426681Noch keine Bewertungen
- About The Author-James Herriot: A Triumph of Surgery Chapter - 1 Footprint Without FeetDokument4 SeitenAbout The Author-James Herriot: A Triumph of Surgery Chapter - 1 Footprint Without FeetSunil rathi100% (3)
- Food Systems For ChildrenDokument12 SeitenFood Systems For ChildrenPaulin koffiNoch keine Bewertungen
- FDA AuditDokument3 SeitenFDA AuditRazor1011Noch keine Bewertungen
- Annual Premium Statement: Bhupesh GuptaDokument1 SeiteAnnual Premium Statement: Bhupesh GuptaBhupesh GuptaNoch keine Bewertungen
- 3M Disposable Filtering Facepiece Respirator Fitting Poster English and SpanishDokument2 Seiten3M Disposable Filtering Facepiece Respirator Fitting Poster English and SpanishTrunggana AbdulNoch keine Bewertungen
- 2022 SWMS - Combined SWMSDokument8 Seiten2022 SWMS - Combined SWMSSteveNoch keine Bewertungen
- Tetanus - AnatomyDokument7 SeitenTetanus - AnatomyJoro27Noch keine Bewertungen
- Marchand 2012Dokument20 SeitenMarchand 2012Elton MatsushimaNoch keine Bewertungen
- 5AB 783651 CompleteBook R39 Jan12Dokument146 Seiten5AB 783651 CompleteBook R39 Jan12Gdb HasseneNoch keine Bewertungen
- Cot q2 w5 HEALTH (New Normal CO)Dokument4 SeitenCot q2 w5 HEALTH (New Normal CO)lizaNoch keine Bewertungen
- Nahom ShewangizawDokument38 SeitenNahom Shewangizawawel centerNoch keine Bewertungen