Beruflich Dokumente
Kultur Dokumente
Isolated Medial Collateral Ligament Injuries in The Knee
Hochgeladen von
kenthepaOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Isolated Medial Collateral Ligament Injuries in The Knee
Hochgeladen von
kenthepaCopyright:
Verfügbare Formate
Isolated Medial Collateral Ligament Injuries in the Knee
Peter A. Indelicato, MD
Abstract
The management of ligament injuries in the knee has progressed significantly over the past two decades as a result of both laboratory and clinical studies that better define the healing capacity of these supporting structures. The intracapsular ligaments (the anterior and posterior cruciate ligaments) appear to have limited potential for spontaneous healing and frequently require surgical reconstruction. The extracapsular ligaments (the medial and lateral collateral ligaments), however, appear to have a fairly robust potential for healing. As a result, the need for surgical intervention is limited to specific clinical situations. J Am Acad Orthop Surg 1995;3:9-14
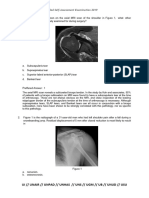
oblique ligament) as the semimembranosus corner. According to him, the semimembranosus muscle, through its various attachment sites, dynamizes this area of the knee during active contracture and provides support even with the knee in flexion. In addition, he states that surgical repair of damage to this area is essential to eliminate any valgus laxity that exists with the knee in full extension. Finally, he points out the anatomic connection between the vastus medialis muscle and the MCL and states that the MCL is also dynamized by contraction of the vastus medialis during active extension (Fig. 1, B). Grood et al,1 Warren et al,2 and Mller3 have pointed out the contribution of the MCL and the posterior oblique ligament in resisting abnormal external tibial rotation. However, the degree of external rotation that results from sectioning these two ligaments appears to be minimal and should not be confused with the more anteromedial rotatory instability that occurs with combined failure of the MCL and the anterior cruciate ligament (ACL).
The management of ligament injuries to the knee continues to evolve. Better understanding of the biomechanical function and physiologic healing process of these important structures affords the clinician a greater opportunity to secure a successful outcome when major damage to the cruciate and collateral ligaments of the knee is encountered. In this article I will review the anatomy, clinical examination, and management of isolated complete medial collateral ligament (MCL) tears in the knee.
Functional and Surgical Anatomy
The nomenclature describing the medial ligamentous structures of the knee has been somewhat confusing. In the past, the MCL has been called the superficial medial collateral ligament or the tibial collateral ligament. The MCL is attached proximally to the medial femoral condyle and distally to the metaphyseal area of the tibia, 4 or 5 cm distal to the medial joint line beneath the pes anserinus
insertion. Immediately deep to the MCL is the medial capsular ligament. Posterior to the MCL is a thickening of the capsular ligament specifically referred to as the posterior oblique ligament (Fig. 1, A). The main medial stabilizer that resists valgus loading is the MCL.1,2 Grood et al1 have shown that the MCL contributes 78% to the restraining force on the medial side of the knee. Because of its parallel collagen arrangement, only 5 to 8 mm of increased opening indicates a complete failure of the ligament. Even though this difference in laxity between the injured knee and the uninjured knee is small, significant damage has occurred to the primary restraint on the medial side of the knee, a fact not stressed enough when teaching physical examination of the knee. The midmedial portion of the medial capsular ligament, deep to the MCL, provides a firm attachment site for the medial meniscus, but does not provide significant restraint against direct valgus stress. Mller3 refers to the posteromedial aspect of the knee (posterior
Dr. Indelicato is Professor of Orthopaedics and Huizenga Professor of Sports Medicine, University of Florida, Gainesville. Reprint requests: Dr. Indelicato, University of Florida Sports Medicine Center, 200 SW 62nd Boulevard, Suite B, Gainesville, FL 32607. Copyright 1995 by the American Academy of Orthopaedic Surgeons.
Vol 3, No 1, Jan/Feb 1995
Medial Collateral Ligament Injuries
Vastus medialis Posterior oblique ligament
Connecting fibers between vastus medialis and medial collateral ligament
Semimembranosus tendon Medial capsular ligament
Medial meniscus, posterior oblique ligament, and semimembranosus unit
Pes anserinus
Medial collateral ligament
Fig. 1 A, The medial capsuloligamentous complex. B, According to Mller,3 the MCL is dynamized by the connecting fibers of the vastus medialis, and the posterior oblique ligament is dynamized by the semimembranosus.
It is critical to understand the surgical anatomy in order to appreciate the relationship the various important stabilizing structures have with the MCL. Warren and Marshall4 have defined three distinct layers, each containing important structures and landmarks. The most superficial layer (layer I) consists of the deep fascia encompassing the patellar tendon anteriorly and the popliteal fossa posteriorly and enveloping the medial hamstrings. Layer II is mainly composed of the MCL, which blends posteriorly with layer III, the posteromedial capsule (posterior oblique ligament). Layer III consists of the medial capsular ligament and blends posteriorly with layer II to form the posterior oblique ligament. There is a bursa that separates layer II, containing the MCL, from the medial capsular ligament immediately beneath it. According to Mller, this bursa
allows the MCL to glide for the required 1.5-cm anteroposterior excursion during flexion/extension of the knee.3 This bursa can be used as a familiar landmark for proper orientation when surgical repair is required.
Clinical Examination
A critical part of the history is to determine the mechanism of a potential MCL injury in the knee. The vast majority of significant MCL injuries involve a valgus force applied laterally to the lower thigh or upper leg. Although complete tears can occur from a rotational force alone, such as occurs in snow skiing, significant tears are more likely in contact sports, such as football and rugby. Since most forces are coupled (i.e., valgus and external rotation), it is not unusual to find
combined damage to both the MCL and the posterior oblique ligament. Mller stated that a pure valgus force to the lateral aspect of the knee without any rotational component will mainly damage the MCL.3 If, however, a combination of valgus and external rotational force is sustained, tears primarily to the posterior oblique ligament and possibly to the ACL can occur before the MCL is significantly damaged. When performing the physical examination, it is critical to keep in mind some basic principles. The patient must be relaxed and the contralateral knee must be used as a control to determine the presence and degree of asymmetrical medial joint opening. The key element of the physical examination is the application of a gentle valgus force with the patients knee in slight flexion (30 degrees). When examining a large patient, one should let the thigh rest
10
Journal of the American Academy of Orthopaedic Surgeons
Peter A. Indelicato, MD
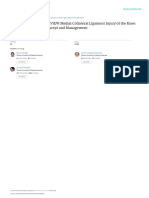
on the table and drop the lower leg off to the side while supporting the foot and ankle (Fig. 2). This gives the patient the opportunity to relax and keep the thigh musculature flaccid, a prerequisite for an accurate assessment in the presence of abnormal ligamentous laxity. For a brief period of time following the injury, a patient may be relatively pain-free even if the MCL is completely torn. Such a situation provides a golden opportunity to perform a very thorough and reliable physical examination. The degree of medial joint opening relative to the uninjured knee is a direct measure of damage to the MCL. It is worth emphasizing that a difference of only 5 to 8 mm is indicative of significant structural damage to the MCL.1 The second part of the examination, which evaluates the extent of medial soft-tissue damage, is performed with the knee in full extension. The valgus force is repeated,
Fig. 2 Placing the injured leg over the side of the table will help the patient relax while allowing the knee to flex the necessary 30 degrees.
and once again the degree of medial joint opening is compared with that in the uninjured knee. Asymmetrical opening in full extension is indicative of combined MCL and posterior oblique ligament damage and should alert the examiner to the possibility of an associated ACL or posterior cruciate ligament injury. Thus, gross medial opening in full extension strongly indicates damage to the cruciate ligaments. If the knee is stable in full extension, one can safely assume that there is no significant damage to the posterior oblique ligament. A more subtle examiner skill is the evaluation of the quality of the end point. When a complete MCL tear is present, no firm end point is encountered. In isolated complete tears of the MCL, the end point in the valgus stressed knee in slight flexion is the intact ACL. However, this end point is encountered quite beyond the normal medial opening as determined by comparison to the normal contralateral knee. Finally, it is important to distinguish between localized soft-tissue swelling and a hemarthrosis. The former is commonly seen in association with MCL damage; the latter is seen more frequently with associated ACL rupture. When combined damage to both the MCL and the ACL is present, the size of the hemarthrosis may be minimal because of the extravasation of blood outside the knee through the tear of the medial capsular ligament. Although the history and physical examination are critical to determination of the type and degree of ligamentous damage to the knee, it may be difficult to perform the appropriate examination due to pain, swelling, and muscle spasm. In this situation, it is helpful to splint the extremity and reexamine the patient a few days later when the swelling and pain have diminished. If this proves unsuccessful, magnetic resonance (MR) imaging may be
considered to highlight the location and extent of ligamentous damage present, as well as to determine whether there are coexisting meniscal abnormalities. Because of the development of MR imaging, diagnostic arthroscopy in this clinical situation is now used less frequently.
Management
Grade I and II Injuries The extent of ligamentous damage determined on clinical examination dictates treatment. Bergfeld 5 has outlined the management of incomplete tears of the MCL. During the first 48 hours, ice, compression, and elevation should be used as much as possible. In general, incomplete tears of the MCL are treated with temporary immobilization and the use of crutches for pain control. Isometric, isotonic, and eventually isokinetic progressive resistive exercises are begun within a few days of the subsidence of pain and swelling. Weight-bearing is encouraged, the rate being dictated by the level of pain. Occasionally, persistent pain over the posterior oblique ligament prevents full, pain-free extension; in this setting, the recovery can be somewhat prolonged. Derscheid and Garrick6 treated 51 incomplete tears of the MCL in a prospective study performed in college football players. A specific rehabilitation protocol, similar to that outlined above, was followed. All players with grade I injuries returned to full, unprotected participation an average of 10.6 days after injury; for players with grade II injuries, the return took 19.5 days. Although a slight amount of residual laxity remained, it proved to be of no functional significance. Grade III Injuries In 1950, ODonoghue7 advocated the immediate repair of all complete 11
Vol 3, No 1, Jan/Feb 1995
Medial Collateral Ligament Injuries
tears of the MCL whether they occurred as an isolated injury or in conjunction with other major ligament damage: The knee which demonstrates a serious or complete rupture of the medial collateral ligament, a fracture of the meniscus, or a tear in the cruciate, or any combination of these, should have early and careful repair not of one or two, but of all damaged structures. In 1983, Hughston and Barrett8 advocated primary repair of all torn medial structures, including the MCL and the posterior oblique ligament, when complete disruption is discovered on clinical examination. They believed that anterior advancement of the posterior oblique ligament was the key to restoring medial stability and advocated proper tensioning of each suture under direct visualization. Mller3 performed a primary repair of the MCL using various methods of fixation and reported good or excellent results in 86% of cases. Other authors have advocated nonoperative intervention when the MCL is completely torn. In 1974, Ellsasser et al 9 observed that severe tears of the MCL in professional football players could be treated nonoperatively with a high degree of success. In 1978, Fetto and Marshall10 reported equally satisfactory results in isolated complete tears of the MCL, irrespective of whether they were repaired primarily or treated conservatively. However, they stressed the importance of identifying any associated ligamentous damage (particularly to the ACL) and stated that the results were universally poor when combined ligamentous injuries were treated nonoperatively. More recent studies have highlighted the importance of identifying coexisting ACL damage and the deleterious effect it may have on MCL healing.11-13 For example, in 1988, Kannus14 reported poor longterm results of nonoperative treatment of complete MCL tears in 27 patients. Jones et al15 reported the results of nonoperative treatment of complete isolated MCL tears in 24 high school football players. The players were able to return to competition an average of 34 days after injury even though some had some mild residual medial laxity on physical examination. A recent study performed by Reider et al16 supports the concept of early motion and functional rehabilitation in the management of isolated MCL injuries in athletes. The data on 35 patients were reviewed (average follow-up, over 5 years). The overall results were very good. Nineteen of 34 patients estimated their time to full recovery to be under 2 months. Thirty-three patients were able to return to full participation in the preinjury sport. Sixteen of 19 football players returned to the sport within 4 weeks after the injury. My preferred method for treating isolated complete MCL tears has not changed very much since 1983. 17 Provided structural damage to either cruciate ligament has been excluded by clinical examination or MR imaging, I believe that primary repair of the MCL is not necessary, and a structured program of rehabilitation can provide predictably good results in the vast majority of cases.18 What has changed over the past few years is the rate of progression of the rehabilitation program. Compared with the original protocol published in 1983, the program has become much more aggressive and driven by patient comfort and performance rather than by any predetermined period of time. I also believe that arthroscopy is no longer indicated in every case. An accurate clinical examination with particular emphasis on the Lachman test is sufficient to evaluate the extent of damage to the ACL. During examination of the knee soon after injury, the presence of joint-line tenderness does not necessarily mean a substance tear of the medial meniscus. Occasionally, MR imaging is helpful in determining whether there is any coexisting damage to the meniscus, although it has been my experience that it is unusual to have significant damage to the body of the meniscus when there is a complete disruption of the MCL. Once it has been established that no structural damage to other ligaments has occurred, a structured supervised program is begun. If the knee is not too painful, a hinged brace is used, and quadriceps-strengthening exercises and straight leg raises are encouraged immediately. If the knee is painful, it is placed in full extension in an immobilizer without hinges. When the initial pain and swelling subside, the patient is instructed to remove the immobilizer five times daily and to perform a range-of-motion program, the limits of motion being dictated by comfort, optimally for 5 minutes each set. Usually, the patient can easily flex the knee beyond 90 degrees within 10 to 14 days, and the immobilizer can then be removed. When the patient can walk without a noticeable limp, the crutches are discontinued. No form of brace is recommended at this point. Once the knee can be flexed beyond 100 degrees, the use of a stationary bicycle is started. This encourages further motion and builds strength. It is important to note that it is unusual for an effusion to develop during the rehabilitation program. If a recurrent effusion is noted, particularly more than once, the possibility of undiagnosed associated meniscal and/or articular cartilage damage should be considered. As stated previously, a small group of patients develop posteromedial pain that prevents comfortable full extension at the beginning of
12
Journal of the American Academy of Orthopaedic Surgeons
Peter A. Indelicato, MD
their rehabilitation program. However, this is much more likely to occur in patients with incomplete tears of the posterior oblique ligament and associated vastus medialis damage than it is in patients with complete tears of the MCL not involving the posterior oblique ligament. When the patient regains 60% of his quadriceps strength, as determined on isokinetic testing, he is allowed to start a straight-ahead jogging program. Usually this takes place within the first 3 weeks of therapy. Jogging may be started sooner on a trampoline or in a pool in chestdeep water. Usually within a few more weeks the quadriceps and hamstring strength will be 80% of that on the contralateral leg. When this occurs, the patient is provided with a functional orthosis, and an agility program is begun. I prefer an off-theshelf model, the type usually recommended following ACL surgery. Return to contact sports is permitted whenever the patient can perform an agility program equivalent to that needed to play his sport. I encourage the use of a functional brace for the remainder of the season because players feel that such bracing provides additional protection. However, continued use of the brace is discouraged when the player returns the following season. Because prophylactic knee bracing remains controversial, routine use is not encouraged.
The obvious question arises: When, if ever, should primary repair of a complete MCL tear be performed? There still remains some controversy over this issue. Recently, Shelbourne and Porter 19 reported the results in 68 patients who had tears of both the MCL and the ACL. The ACL tear was treated with a primary reconstruction using autogenous patellar tendon, and the MCL tear was managed nonoperatively. They concluded that good to excellent results could be achieved without primary repair of the MCL rupture and saw no advantage to the additional surgery. My approach to combined ACLMCL damage is to decide intraoperatively whether the MCL rupture requires primary repair. After the ACL reconstruction is complete, the medial laxity is reassessed. If the knee continues to be unstable in full extension or slight flexion (grade II or III), the MCL and the posterior oblique ligament are exposed, and a primary repair is performed. Unlike Hughston and Barrett,8 however, I avoid reefing or advancement of the posterior oblique ligament during the repair in order to avoid the risk of a flexion contracture. If the degree of medial laxity has been reduced to grade I after the ACL reconstruction, primary repair of the medial ligament damage is not necessary. Regardless of whether a primary medial repair has been performed,
the knee is placed in full extension, and a range-of-motion program is started early. The rehabilitation program is focused mainly on the ACL rather than the MCL.
Summary
Clinical evaluation of patients with complete tears of the MCL will dictate the course of action necessary for a successful outcome. When associated damage to the ACL can be ruled out, primary repair is usually not necessary. Although it is important to document the mechanism of injury, the correct diagnosis is dependent on the results of the physical examination. Magnetic resonance imaging and diagnostic arthroscopy should be reserved for those situations in which the extent of damage remains questionable. There is little controversy regarding the management of incomplete tears of the MCL and the posterior oblique ligament. Although in the past some authors recommended primary repair for all complete tears of the MCL, the pendulum appears to have swung toward nonoperative management of these lesions in most cases. There still remains some controversy regarding the management of these tears when they are discovered in conjunction with tears of either cruciate ligament.
References
1. Grood ES, Noyes FR, Butler DL, et al: Ligamentous and capsular restraints preventing straight medial and lateral laxity in intact human cadaver knees. J Bone Joint Surg Am 1981;63:12571269. 2. Warren LF, Marshall JL, Girgis F: The prime static stabilizer of the medial side of the knee. J Bone Joint Surg Am 1974;56:665-674. 3. Mller W: The Knee: Form, Function, and Ligament Reconstruction. New York: Springer-Verlag, 1983. 4. Warren LF, Marshall JL: The supporting structures and layers on the medial side of the knee: An anatomical analysis. J Bone Joint Surg Am 1979;61:56-62. 5. Bergfeld J: First-, second-, and thirddegree sprains. Am J Sports Med 1979;7: 207-209. 6. Derscheid GL, Garrick JG: Medial collateral ligament injuries in football: Nonoperative management of grade I and grade II sprains. Am J Sports Med 1981;9:365-368. 7. ODonoghue DH: Surgical treatment of fresh injuries to the major ligaments of the knee. J Bone Joint Surg Am 1950;32:721-738. 8. Hughston JC, Barrett GR: Acute anteromedial rotatory instability: Long-term
Vol 3, No 1, Jan/Feb 1995
13
Medial Collateral Ligament Injuries
results of surgical repair. J Bone Joint Surg Am 1983;65:145-153. Ellsasser JC, Reynolds FC, Omohundro JR: The non-operative treatment of collateral ligament injuries of the knee in professional football players: An analysis of seventy-four injuries treated nonoperatively and twenty-four injuries treated surgically. J Bone Joint Surg Am 1974;56:1185-1190. Fetto JF, Marshall JL: Medial collateral ligament injuries of the knee: A rationale for treatment. Clin Orthop 1978;132: 206-218. Anderson DR, Weiss JA, Takai S, et al: Healing of the medial collateral ligament following a triad injury: A biomechanical and histological study of the knee in rabbits. J Orthop Res 1992;10:485-495. Inoue M, McGurk-Burleson E, Hollis JM, et al: Treatment of the medial collateral ligament injury: I. The importance of anterior cruciate ligament on the varus-valgus knee laxity. Am J Sports Med 1987;15:15-21. Woo SLY, Inoue M, McGurk-Burleson E, et el: Treatment of the medial collateral ligament injury: II. Structure and function of canine knees in response to differing treatment regimens. Am J Sports Med 1987;15:22-29. Kannus P: Long-term results of conservatively treated medial collateral ligament injuries of the knee joint. Clin Orthop 1988;226:103-112. Jones RE, Henley MB, Francis P: Nonoperative management of isolated grade III collateral ligament injury in high school football players. Clin Orthop 1986;213:137-140. Reider B, Sathy MR, Talkington J, et al: Treatment of isolated medial collateral ligament injuries in athletes with early functional rehabilitation: A five-year follow-up study. Am J Sports Med 1993;22:470-477. 17. Indelicato PA: Non-operative treatment of complete tears of the medial collateral ligament of the knee. J Bone Joint Surg Am 1983;65:323-329. 18. Indelicato PA, Hermansdorfer J, Huegel M: Nonoperative management of complete tears of the medial collateral ligament of the knee in intercollegiate football players. Clin Orthop 1990;256: 174-177. 19. Shelbourne KD, Porter DA: Anterior cruciate ligament-medial collateral ligament injury: Nonoperative management of medial collateral ligament tears with anterior cruciate ligament reconstruction: A preliminary report. Am J Sports Med 1992;20:283-286.
9.
13.
10.
14.
11.
15.
12.
16.
14
Journal of the American Academy of Orthopaedic Surgeons
Das könnte Ihnen auch gefallen
- Pediatric Primitive ReflexesDokument2 SeitenPediatric Primitive ReflexesJonathanNoch keine Bewertungen
- Anterior Cruciate Ligament-Injury & ManagementDokument101 SeitenAnterior Cruciate Ligament-Injury & ManagementYusuf Brilliant100% (1)
- Assessing Shoulder MotionDokument24 SeitenAssessing Shoulder Motionkenthepa100% (3)
- Acl Injury Surgery - Orthoinfo - AaosDokument15 SeitenAcl Injury Surgery - Orthoinfo - Aaosapi-228773845Noch keine Bewertungen
- ACL Injury: Does It Require Surgery?Dokument33 SeitenACL Injury: Does It Require Surgery?Lee Woo GuanNoch keine Bewertungen
- JAAOS - Volume 11 - Issue 04 July & August 2003Dokument70 SeitenJAAOS - Volume 11 - Issue 04 July & August 2003kenthepaNoch keine Bewertungen
- Anterior Cruciate Ligament Tear DefinitionDokument8 SeitenAnterior Cruciate Ligament Tear DefinitionEunice IquinaNoch keine Bewertungen
- Collateral Ligament Injury MRIDokument29 SeitenCollateral Ligament Injury MRILeksmana AcNoch keine Bewertungen
- ACL InjuryDokument21 SeitenACL InjuryVenkatesh Kandhaswamy RamalingamNoch keine Bewertungen
- Osteopathy Models For Diagnosis, Treatment and Practice 2nd Edition (2005) - Jon Parsons, Nicholas MarcerDokument179 SeitenOsteopathy Models For Diagnosis, Treatment and Practice 2nd Edition (2005) - Jon Parsons, Nicholas Marcerrusom88% (24)
- Internal Derangements of the Knee (IDK): Causes, Symptoms & TreatmentDokument92 SeitenInternal Derangements of the Knee (IDK): Causes, Symptoms & TreatmentAzad Roxo100% (3)
- Pediatric and Adolescent Musculoskeletal MRI PDFDokument760 SeitenPediatric and Adolescent Musculoskeletal MRI PDFJavierPiñeiroAndradeNoch keine Bewertungen
- Aaos 2019Dokument283 SeitenAaos 2019alealer2708Noch keine Bewertungen
- Exercise Plan For Bone Health - OsteoporosisDokument19 SeitenExercise Plan For Bone Health - OsteoporosisKulkasniegu100% (1)
- Free Preview: ShouldersDokument21 SeitenFree Preview: ShouldersSiva SubramanianNoch keine Bewertungen
- The Lower Limb Tendinopathies Etiology, Biology and Treatment-Springer International (2016)Dokument202 SeitenThe Lower Limb Tendinopathies Etiology, Biology and Treatment-Springer International (2016)Tony Miguel Saba Saba100% (1)
- Hip Fractures-Orthoinfo - AaosDokument9 SeitenHip Fractures-Orthoinfo - Aaosapi-228773845Noch keine Bewertungen
- Joel W. Beam - Orthopedic Taping, Wrapping, Bracing, and Padding-F. A. Davis (2021)Dokument501 SeitenJoel W. Beam - Orthopedic Taping, Wrapping, Bracing, and Padding-F. A. Davis (2021)gfdgrrgeerNoch keine Bewertungen
- Internal Derangement of Knee - 2Dokument113 SeitenInternal Derangement of Knee - 2sushil2207Noch keine Bewertungen
- Anatomy and Bio Mechanics of The KneeDokument15 SeitenAnatomy and Bio Mechanics of The KneeaimanshalpyNoch keine Bewertungen
- Surgical Techniques For Complex Proximal Tibial FracturesDokument13 SeitenSurgical Techniques For Complex Proximal Tibial FracturesHannah CoNoch keine Bewertungen
- SPINE Manual of Groin Pain 2016 PDFDokument539 SeitenSPINE Manual of Groin Pain 2016 PDF김익수100% (1)
- OrifDokument13 SeitenOrifAhmabelle Mara D. AbellaNoch keine Bewertungen
- Elbow Rehabilitation - SpringerLinkDokument35 SeitenElbow Rehabilitation - SpringerLinkasdfNoch keine Bewertungen
- Ankle and Foot InjuriesDokument42 SeitenAnkle and Foot InjuriesJulius Adams100% (1)
- Application of Proper Draping-Final DemoDokument15 SeitenApplication of Proper Draping-Final DemoMarife Hernandez Gelin80% (15)
- Medial Collateral Ligament InjuriesDokument14 SeitenMedial Collateral Ligament InjuriesJeetendra SoniNoch keine Bewertungen
- Anterior Cruciate LigamentDokument41 SeitenAnterior Cruciate Ligamentsneha ravichandranNoch keine Bewertungen
- MCL Injury PaperDokument6 SeitenMCL Injury Paperapi-268835137Noch keine Bewertungen
- Triada Terrible CCR 09lunes14Dokument15 SeitenTriada Terrible CCR 09lunes14Juan Manuel CastilloNoch keine Bewertungen
- Articular Fractures PrinciplesDokument10 SeitenArticular Fractures Principlesrmz.mariana11Noch keine Bewertungen
- Simple Elbow Dislocation: Paul M. Robinson, Emmet Griffiths and Adam C WattsDokument10 SeitenSimple Elbow Dislocation: Paul M. Robinson, Emmet Griffiths and Adam C WattsAnnisa HidayatiNoch keine Bewertungen
- Knee and Leg Injuries: Causes, Symptoms, TreatmentsDokument14 SeitenKnee and Leg Injuries: Causes, Symptoms, TreatmentsDrAyyoub AbboodNoch keine Bewertungen
- Current Concepts Review MCL - A Review On Current Concept and ManagementDokument9 SeitenCurrent Concepts Review MCL - A Review On Current Concept and Managementlite.trawler-0xNoch keine Bewertungen
- Medial Collateral Ligament Injury of The KneeDokument19 SeitenMedial Collateral Ligament Injury of The KneeAmada Angel VillanuevaNoch keine Bewertungen
- Review Article: Elbow Dislocations: A Review Ranging From Soft Tissue Injuries To Complex Elbow Fracture DislocationsDokument12 SeitenReview Article: Elbow Dislocations: A Review Ranging From Soft Tissue Injuries To Complex Elbow Fracture DislocationshermanusNoch keine Bewertungen
- Englert2013 PDFDokument12 SeitenEnglert2013 PDFMarius ChirilaNoch keine Bewertungen
- Knee Medial Collateral Ligament AugmentatDokument7 SeitenKnee Medial Collateral Ligament AugmentatHalawa205Noch keine Bewertungen
- Posterior Cruciate Ligament InjuriesDokument26 SeitenPosterior Cruciate Ligament InjuriesGopi KrishnanNoch keine Bewertungen
- Esquina Posteromedial RodillaDokument9 SeitenEsquina Posteromedial RodillaSebastian RamirezNoch keine Bewertungen
- Acl IvanDokument10 SeitenAcl IvanDINANoch keine Bewertungen
- What's in and What's Out?: Management of Anterior Cruciate Ligament InjuryDokument13 SeitenWhat's in and What's Out?: Management of Anterior Cruciate Ligament InjuryNydia OngaliaNoch keine Bewertungen
- The Relationship Between Anterior Cruciate Ligament Injury and Osteoarthritis of The KneeDokument12 SeitenThe Relationship Between Anterior Cruciate Ligament Injury and Osteoarthritis of The KneeMufidAljaruNoch keine Bewertungen
- Clinical Data Fisiotek HP2Dokument28 SeitenClinical Data Fisiotek HP2Alexandra NadinneNoch keine Bewertungen
- LisfrancDokument18 SeitenLisfrancMelissa AGNoch keine Bewertungen
- ManusDokument17 SeitenManusKhrisnanto NugrohoNoch keine Bewertungen
- 76040138-Referat-Fraktur-Pelvis EditDokument34 Seiten76040138-Referat-Fraktur-Pelvis Editsri wulanNoch keine Bewertungen
- Multiple ligament knee injuries acute managementDokument7 SeitenMultiple ligament knee injuries acute managementekyNoch keine Bewertungen
- Anterior Cruciate LigamentDokument10 SeitenAnterior Cruciate Ligamentppsc_costin_47147107Noch keine Bewertungen
- Tibial Eminence Fractures PDFDokument16 SeitenTibial Eminence Fractures PDFVidinikusumaNoch keine Bewertungen
- (II) PCL ReconstructionDokument8 Seiten(II) PCL ReconstructionRosaneLacerdaNoch keine Bewertungen
- 6 - Injuries To The Ulnar Collateral Ligament o - 2018 - Clinical Orthopaedic Re PDFDokument4 Seiten6 - Injuries To The Ulnar Collateral Ligament o - 2018 - Clinical Orthopaedic Re PDFTolo CantallopsNoch keine Bewertungen
- 2008 Article 9145-2 PDFDokument7 Seiten2008 Article 9145-2 PDFDeborah González GarcíaNoch keine Bewertungen
- Foot Ankle Clin - 2021 Jun - 26 (2) - 391-405.Dokument15 SeitenFoot Ankle Clin - 2021 Jun - 26 (2) - 391-405.Biblioteca Centro Médico De Mar del PlataNoch keine Bewertungen
- Percutaneous Osteosynthesis of The Distal Fractures of The Femur. Eladio Saura Mendoza e Eladio Saura SanchezDokument12 SeitenPercutaneous Osteosynthesis of The Distal Fractures of The Femur. Eladio Saura Mendoza e Eladio Saura SanchezNuno Craveiro LopesNoch keine Bewertungen
- Anderson and Anderson, 2011Dokument16 SeitenAnderson and Anderson, 2011Salsabila Kusuma JannatiNoch keine Bewertungen
- Fracturas de TobilloDokument23 SeitenFracturas de TobilloGregorio VillarrealNoch keine Bewertungen
- Current Perspectives On Elbow Dislocation and InstabilityDokument15 SeitenCurrent Perspectives On Elbow Dislocation and InstabilityAnonymous L9D1I7DZNoch keine Bewertungen
- Translate Apley SebagianDokument13 SeitenTranslate Apley Sebagianstudywith kyaNoch keine Bewertungen
- Magnetic Resonance Imaging of Sports Injuries of The Knee: Pictorial EssayDokument8 SeitenMagnetic Resonance Imaging of Sports Injuries of The Knee: Pictorial EssayAlvian DwiNoch keine Bewertungen
- MDCT and MRI Evaluation of Cervical Spine Trauma: Pictorial ReviewDokument9 SeitenMDCT and MRI Evaluation of Cervical Spine Trauma: Pictorial ReviewcalinmariusNoch keine Bewertungen
- Kim Technique MCL and POLDokument5 SeitenKim Technique MCL and POLManuel Vergillos LunaNoch keine Bewertungen
- Guide to Assessing and Treating Multiple Ligament Injured KneesDokument6 SeitenGuide to Assessing and Treating Multiple Ligament Injured KneesMayra BeltranNoch keine Bewertungen
- BiomechanicDokument15 SeitenBiomechanicMuhamad SdeqNoch keine Bewertungen
- Elbow Dislocation: DR Ajith John KDokument53 SeitenElbow Dislocation: DR Ajith John KPankaj VatsaNoch keine Bewertungen
- Gadline PrsentationDokument12 SeitenGadline PrsentationsumardiNoch keine Bewertungen
- The Anatomy of The ACL and Its Importance in ACL ReconstructionDokument6 SeitenThe Anatomy of The ACL and Its Importance in ACL Reconstructionlexie beatsNoch keine Bewertungen
- The Terrible Triad of The ElbowDokument5 SeitenThe Terrible Triad of The Elbowapi-250084607Noch keine Bewertungen
- Ankle Fractures in Adults - UpToDateDokument50 SeitenAnkle Fractures in Adults - UpToDateJose LuceroNoch keine Bewertungen
- Rupture of Posterior Cruciate Ligament: Diagnosis and Treatment PrinciplesDokument8 SeitenRupture of Posterior Cruciate Ligament: Diagnosis and Treatment PrinciplesSOPHIASTIA KUSBIANTI MHS 2017Noch keine Bewertungen
- 02 Current Strategies in Anesthesia and AnalgesiaDokument14 Seiten02 Current Strategies in Anesthesia and AnalgesiakenthepaNoch keine Bewertungen
- JAAOS - Volume 21 - Issue 10 October 2013 PDFDokument67 SeitenJAAOS - Volume 21 - Issue 10 October 2013 PDFkenthepaNoch keine Bewertungen
- 04 Fixation of Soft Tissue To Bone TechniquesDokument13 Seiten04 Fixation of Soft Tissue To Bone TechniqueskenthepaNoch keine Bewertungen
- JAAOS - Volume 11 - Issue 01 January & February 2003Dokument77 SeitenJAAOS - Volume 11 - Issue 01 January & February 2003kenthepaNoch keine Bewertungen
- JAAOS - Volume 11 - Issue 01 January & February 2003Dokument51 SeitenJAAOS - Volume 11 - Issue 01 January & February 2003kenthepaNoch keine Bewertungen
- 01 Tibiotalocalcaneal Fusion For Severe DeformityDokument10 Seiten01 Tibiotalocalcaneal Fusion For Severe DeformitykenthepaNoch keine Bewertungen
- JAAOS - Volume 11 - Issue 01 January & February 2003Dokument51 SeitenJAAOS - Volume 11 - Issue 01 January & February 2003kenthepaNoch keine Bewertungen
- JAAOS - Volume 09 - Issue 01 January & February 2001Dokument70 SeitenJAAOS - Volume 09 - Issue 01 January & February 2001kenthepaNoch keine Bewertungen
- JAAOS - Volume 02 - Issue 01 January 1994Dokument67 SeitenJAAOS - Volume 02 - Issue 01 January 1994kenthepaNoch keine Bewertungen
- JAAOS - Volume 11 - Issue 05 September & October 2003Dokument83 SeitenJAAOS - Volume 11 - Issue 05 September & October 2003kenthepaNoch keine Bewertungen
- JAAOS - Volume 09 - Issue 02 March & April 2001Dokument76 SeitenJAAOS - Volume 09 - Issue 02 March & April 2001kenthepaNoch keine Bewertungen
- JAAOS - Volume 02 - Issue 01 January 1994Dokument67 SeitenJAAOS - Volume 02 - Issue 01 January 1994kenthepaNoch keine Bewertungen
- JAAOS - Volume 11 - Issue 01 January & February 2003Dokument77 SeitenJAAOS - Volume 11 - Issue 01 January & February 2003kenthepaNoch keine Bewertungen
- JAAOS - Volume 03 - Issue 06 November 1995Dokument53 SeitenJAAOS - Volume 03 - Issue 06 November 1995kenthepaNoch keine Bewertungen
- Making AKO Work With Internet ExplorerDokument29 SeitenMaking AKO Work With Internet ExplorerkenthepaNoch keine Bewertungen
- JAAOS - Volume 03 - Issue 01 January 1995Dokument63 SeitenJAAOS - Volume 03 - Issue 01 January 1995kenthepaNoch keine Bewertungen
- JAOOSDokument64 SeitenJAOOSkenthepaNoch keine Bewertungen
- Hallux ValgusDokument5 SeitenHallux ValguskenthepaNoch keine Bewertungen
- Emergency Limb Injuries Guide: Critical Period ManagementDokument75 SeitenEmergency Limb Injuries Guide: Critical Period ManagementDia Inggrit PNoch keine Bewertungen
- Vaccine Information SheetDokument102 SeitenVaccine Information SheetkenthepaNoch keine Bewertungen
- Naval Special Warefare SummaryDokument11 SeitenNaval Special Warefare SummarykenthepaNoch keine Bewertungen
- Shoulder InjectionsDokument40 SeitenShoulder InjectionskenthepaNoch keine Bewertungen
- Flexor Tendon Sheath InfectionsDokument10 SeitenFlexor Tendon Sheath InfectionskenthepaNoch keine Bewertungen
- Joint Evaluation: INSTRUCTIONS: For Each Affected JointDokument2 SeitenJoint Evaluation: INSTRUCTIONS: For Each Affected JointkenthepaNoch keine Bewertungen
- Flexor Tendon Sheath InfectionsDokument10 SeitenFlexor Tendon Sheath InfectionskenthepaNoch keine Bewertungen
- Does Pad Height Affect Back Muscle Endurance in Ito TestDokument7 SeitenDoes Pad Height Affect Back Muscle Endurance in Ito TestDr. Krishna N. SharmaNoch keine Bewertungen
- Anatomy of Hip JointDokument5 SeitenAnatomy of Hip JointSneha ParveenNoch keine Bewertungen
- Anatomy Important Images: AriseDokument14 SeitenAnatomy Important Images: AriseadiNoch keine Bewertungen
- NEET PG 2013 Question Paper With SolutionsDokument2.164 SeitenNEET PG 2013 Question Paper With SolutionsSK RaulNoch keine Bewertungen
- Types of Tissue - Muscle TissueDokument3 SeitenTypes of Tissue - Muscle TissueFaye AquinoNoch keine Bewertungen
- Congenital hip dysplasia diagnosis in under 40Dokument6 SeitenCongenital hip dysplasia diagnosis in under 40Bek DiazNoch keine Bewertungen
- BursitisDokument21 SeitenBursitisJigisha ChavdaNoch keine Bewertungen
- ACCOLADE II SurgicalDokument11 SeitenACCOLADE II Surgicaltrinh thanhNoch keine Bewertungen
- Anatomic Landmarks of The Maxilla and MandibleDokument34 SeitenAnatomic Landmarks of The Maxilla and Mandiblespu123Noch keine Bewertungen
- Exercise Frozen ShoulderDokument2 SeitenExercise Frozen ShoulderAnonymous D15WroNoch keine Bewertungen
- Musculoskeletal Sports Ultrasound.1Dokument2 SeitenMusculoskeletal Sports Ultrasound.1Mateus AssisNoch keine Bewertungen
- Iliac Crest Grafting For Mandibular ReconstructionDokument10 SeitenIliac Crest Grafting For Mandibular Reconstructiontanvi vijayNoch keine Bewertungen
- Shoulder Pain Diagnosis and Management in PrimaryDokument6 SeitenShoulder Pain Diagnosis and Management in PrimaryAnonymous ckZmIgoNoch keine Bewertungen
- Amputation and RehabilitationDokument4 SeitenAmputation and RehabilitationimherestudyingNoch keine Bewertungen
- Karakteristik Morfometrik Sapi Aceh, Sapi PO Dan Sapi Bali Berdasarkan Analisis Komponen Utama (AKU)Dokument6 SeitenKarakteristik Morfometrik Sapi Aceh, Sapi PO Dan Sapi Bali Berdasarkan Analisis Komponen Utama (AKU)Fahyanti Dama31Noch keine Bewertungen
- Comparative Anatomy of The BoneDokument53 SeitenComparative Anatomy of The BoneCherry SantosNoch keine Bewertungen
- Penatalaksanaan Fisioterapi Pada Kasus Post Fraktur 1/3 Distal Radius Dextra Di RST Dr. Soejono MagelangDokument14 SeitenPenatalaksanaan Fisioterapi Pada Kasus Post Fraktur 1/3 Distal Radius Dextra Di RST Dr. Soejono MagelangAyu Nur AidaNoch keine Bewertungen
- The Assisted Nordic Hamstring Curl: Exercise TechniqueDokument4 SeitenThe Assisted Nordic Hamstring Curl: Exercise TechniqueSheilani MartinsNoch keine Bewertungen
- Deformational Plagiocephaly: A Guide To Diagnosis and TreatmentDokument16 SeitenDeformational Plagiocephaly: A Guide To Diagnosis and TreatmentManjunath VaddambalNoch keine Bewertungen
- Anatomy SBA MCQ eMRCSDokument81 SeitenAnatomy SBA MCQ eMRCSTowhid HasanNoch keine Bewertungen
- High-Energy Fractures of The Pelvis and Acetabulum in Pediatric PatientsDokument10 SeitenHigh-Energy Fractures of The Pelvis and Acetabulum in Pediatric PatientsFauzan KurniawanNoch keine Bewertungen
- AHN-II Lec2Dokument20 SeitenAHN-II Lec2Abdullah BhattiNoch keine Bewertungen
- The Skeletal SystemDokument15 SeitenThe Skeletal SystemIvan Gabriel PilienNoch keine Bewertungen