Beruflich Dokumente
Kultur Dokumente
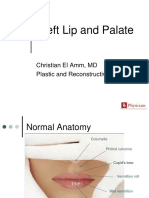
Cleft Lip and Cleft Palate
Hochgeladen von
RAJUCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Cleft Lip and Cleft Palate
Hochgeladen von
RAJUCopyright:
Verfügbare Formate
Cleft lip and Cleft palate
Introduction
Cleft lip and palate are congenital (present from before birth) abnormalities that affect the upper lip and the hard and soft palate of the mouth. That may occur separately or together. Cleft lip: It results from the failure of maxillary processes to fuse with the nose elevation on the frontal prominence. This defect varies from a notch in the lip to complete separation of the lip into a hare. The cleft lip may be unilateral or bilateral.
Unilateral Cleft lip
Bilateral Cleft lip
Cleft palate (isolated): Isolated cleft palate results from a failure of the fusion of secondary palate with each other, and with the primary palate. It can be unilateral or bilateral. Cleft lip and palate: This condition results from a combined defect of cleft lip and cleft palate.
Incidence
Cleft lip occurs in approximately 1 in 800 births. It is more common in Asians and American Indians and less common in African-Americans. Cleft palate occurs in approximately 1 in 2000 births. There are various degrees of
severity with each defect.
Etiology
Idiopathic (exact cause are unknown). Suspected causes include- mutant genes inherited from one or both parents, and teratogens (drugs, viruses, or other toxins that can cause abnormalities in a developing fetus).
Clinical manifestations
Separation of the lip alone. Separation of the palate.
Separation of the lip and palate. Varying amounts of nasal distortion. Recurrent ear infections. Failure to gain weight. Nasal regurgitations during bottle feeding. Growth retardation. Misaligned teeth. Poor speech. Feeding problems.
Investigations
Cleft lip with or without the cleft palate is easily apparent at birth. Only cleft palate may be identified when thorough assessment of the mouth is done or when the infant has difficulty with initial feeding.
Complications
Recurrent ear infections Hearing loss Dental cavities Displaced teeth Poor speech Lip deformities Nasal deformities
Management
Treatment of cleft lip and cleft palate may require joint efforts of pediatrician, plastic surgeon, nurses, orthodontist, prosthodontist, and speech therapist. Surgical Management The cleft lip is usually repaired by about 2-3 months of age and cleft palate is usually repaired by about 18-24 months of age of the baby. Closure of the cleft lip is done firstly then the closure of the cleft palate. Cleft lip is generally repaired by Z-shaped sutures, to reduce notching of the lip. After the surgery, the suture line is protected from tension by an arched metal device taped to the cheek. Cleft palate surgery is postponed later in order to wait for the changes in the palate. Orthodeontic and prosthodontic treatment may be required to correct malposition of the teeth and maxillary arch.
Children with cleft palate may have speech problem and may require speech therapy. The baby is anesthetized and asleep (general anesthesia), the tissues around the defect are trimmed and sewn together with several layers of stitches (absorbable sutures). The skin is sewn together with very small; fine stitches (sutures) to make the scar as small as possible. In cleft palate repair, tissue from the back of the mouth (pharynx) may be taken to add tissue to the deficient soft palate (this is called a pharyngeal flap). Occasionally more than one surgery is required for complete palate closure
General instructions Soon after the birth, the baby may look unattractive but the nurse should not show her reactions. The disfiguring defect may cause negative reaction and shock in the parents. The nurse should explain the positive aspects about the correction of the defect and other possible treatment. Feeding of an infant: The immediate problem faced is the feeding an infant with the cleft lip and palate, because this defect reduces the ability of the infant to suck. While feeding, the infant should be hold in upright position. A special cleft palate nipple can be used. A large and soft nipple with the large hole or a long and soft lamb's nipples are useful. When the infants have the problem to take feeds with the nipple, a syringe with the rubber tube may be used to feed.
Nursing Management
NURSING CARE PLAN
GOAL INTERVENTIONN RATIONALE
Pre-operative Care
1. Risk for Aspiration (Breast Milk or Mucus) related to anatomic defect.
The of
infant gagging
will or
Assess
respiratory
status
Allows problems.
for
early of
have no episodes aspiration.
and monitor vital signs at least every 2 hours. Position feedings. Feed needed. Burp frequently (after every 15-30 ml of fluid). Position feedings. Keep suction equipment and bulb syringe at bedside. upright for slowly and use as adaptive equipment on side after
identification
Prevents aspiration of feedings. Facilitates intake while minimizing aspiration. Helps to prevent and regurgitation aspiration. Minimizes passage of feedings through cleft. Suctioning necessary may to be remove risk of
milk or mucus.
2. Altered Nutrition: Less than Body Requirements related to the infant's inability to form an adequate seal for sucking
The
infant
will
Assess fluid and calorie intake daily. Assess weight daily (same scale, same time, with infant completely undressed).
Provides an objective measurement receiving mote of sufficient Using whether the infant is caloric intake to progrowth.
gain weight.
the
same
scale the
and when infant for
procedure weighing provides daily weights. Observe for any respiratory impairment. Any symptoms
comparability between of
respiratory compromise will interfere with the infant's ability Feedings are no to should signs suck. be of
initiated only if there respiratory distress. Facilitate breast-feeding. Breast milk is recommended as the best food for an infant. The process feeding promote between infant. Give the mother information on breast-feeding the infant with a cleft lip and/or palate such as plugging the cleft lip and eliciting a let-down reflex before nursing. If the mother is unable to breast-feed (or prefers not to), initiate bottle feeding: Hold infant in an upright or Facilitates swallowing Information specific may encourage and suggestions the of breastto and bonding mother helps
mother to persist with breast-feeding.
semisitting feeding.
position
for
and
minimizes
the
amount of fluid return from the nose. Small tire amounts the as infant do given at and as a
Feed small amounts slowly.
allow feeding do not quickly amounts larger
faster rate. They also decrease the calories used during feeding. Initiate nasogastric feedings if the infant is unable to ingest sufficient calories by mouth. Adequate must be nutrition maintained.
Use of a feeding tube allows the infant who has difficulty with oral feeding to receive adequate growth. nutrition for
Post-operative Care
3. Risk for Infection related to surgical procedure and accumulation of formula and secretions the oral cavity Assess vital signs every 2 The mucosal infection. infants tissue hours. Assess oral cavity every 2 hours or as needed for tenderness, of secretions. reddened Elevated Aids in temperature identifying
may indicate infection infection.
will heal without
areas, lesions, or presence
Cleanse normal
suture saline
line or
with sterile
Helps
decrease
the
presence of bacteria.
water if ordered. Cleanse the cleft areas by giving 5-15 ml of water after each feeding. If a crust has formed, use a cotton swab to apply a halfstrength peroxide solution. Apply antibiotic cream to suture line as ordered. Use careful hand washing and sterile technique when working with suture line Counteracts the growth of bacteria. Prevents the spread of microorganisms other sources from Prevents accumulation of which carbohydrates, encourage
bacterial growth. Helps loosen the crust, aiding in removal.
4. Ineffective Breathing Pattern related to anesthesia and increased secretions The infant will an Assess respiratory Allows problems. Enables early detection of abnormal respirations, facilitating prompt intervention. Keep suction equipment and bulb syringe at bedside. Gently suction and mist for if 2 oropharynx Provide first ordered. Reposition hours. every cool 24 Gentle suctioning will keep the airway clear. Suctioning that is too vigorous can irritate the mucosa. Moisturizes secretions to reduce pooling in lungs. Moisturizes oral cavity. Ensures expansion of all lung fields for early of
maintain effective
status and monitor vital signs at least every 2 hours. Apply a cardio respiratory monitor.
identification
breathing pattern.
nasopharynx as needed. hours
postoperatively
5. Altered Nutrition: Less Than Body Requirements related to surgery and feeding difficulties Maintain intravenous infusion as ordered. Begin with clear liquids, then give half-strength formula or breast milk as ordered. Use Asepto syringe or dropper in side of mouth. Avoids sulure line and resullant accumulation of formula in Ihat area. Do not allow pacifiers. Give high-calorie soft foods after cleft palate repair. Sucking can disrupt Provides NPO. Ensures adequate fluid when
The
infant
will
receive
adequate
nutritional intake. fluids and nutrienls.
sulure line. Rough foods, utensils, and disrupt site. slraws the could surgical
Das könnte Ihnen auch gefallen
- Cleft Lip And Palate, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandCleft Lip And Palate, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBewertung: 4.5 von 5 Sternen4.5/5 (3)
- Cleft Lip and PalateDokument18 SeitenCleft Lip and Palateicywitch100% (1)
- Cleft Lip and Cleft PalateDokument16 SeitenCleft Lip and Cleft Palatemacuka08100% (3)
- Cleft Lip and PalateDokument20 SeitenCleft Lip and Palatejapzee1988100% (1)
- Cleft Lip and Cleft PalateDokument6 SeitenCleft Lip and Cleft PalatekrishnasreeNoch keine Bewertungen
- Cleft Lip PalateDokument29 SeitenCleft Lip PalatelisalovNoch keine Bewertungen
- Cleft Lip and Palate - PPT - OrthodonticsDokument46 SeitenCleft Lip and Palate - PPT - OrthodonticsDr.Neethu Salam100% (3)
- Cleft Lip PalateDokument37 SeitenCleft Lip PalateMuhammad Hamid Muktashim100% (1)
- Case Study Cleft LipDokument55 SeitenCase Study Cleft LipJaya Prabha50% (10)
- A Case Study About Cleft Lip and Cleft PalateDokument12 SeitenA Case Study About Cleft Lip and Cleft PalateMaegan Pearl83% (6)
- Cleft Lip and Cleft PalateDokument54 SeitenCleft Lip and Cleft Palatedr parveen bathla100% (3)
- Group 11 Cleft Lip and Cleft Palate Case Study N2BDokument46 SeitenGroup 11 Cleft Lip and Cleft Palate Case Study N2BLerma PagcaliwanganNoch keine Bewertungen
- Cleft Lip and PalateDokument25 SeitenCleft Lip and PalateRahul Dhaker100% (1)
- Cleft Lip & PalateDokument43 SeitenCleft Lip & PalateKanjiMasroor100% (1)
- Cleft Lip and Palate New ApproachDokument115 SeitenCleft Lip and Palate New ApproachsoorajNoch keine Bewertungen
- Aetiology Heart Diasease in Children May Be Congenital or AcquiredDokument23 SeitenAetiology Heart Diasease in Children May Be Congenital or AcquiredkasondaNoch keine Bewertungen
- Cleft Lip and Palate Seminar Ed PDFDokument100 SeitenCleft Lip and Palate Seminar Ed PDFsaranyaazz100% (2)
- Cleft Lip and PalateDokument71 SeitenCleft Lip and PalateMegha Sahni Grover75% (4)
- Cleft Lip & PalateDokument9 SeitenCleft Lip & PalateJahzel CallinoNoch keine Bewertungen
- Anomalies of Skeletal System-1Dokument44 SeitenAnomalies of Skeletal System-1Meena Koushal100% (1)
- Ranula Cyst, (Salivary Cyst) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandRanula Cyst, (Salivary Cyst) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- OmphaloceleDokument8 SeitenOmphaloceleLily YuriNoch keine Bewertungen
- NCP Priority 1 Assessment Diagnosis Planning Intervention Rationale EvaluationDokument5 SeitenNCP Priority 1 Assessment Diagnosis Planning Intervention Rationale EvaluationDenice100% (1)
- Child - Cleft PalateDokument5 SeitenChild - Cleft PalateMelanie Anne Montecillo Aringay100% (3)
- Club Foot (Congenital Talipes Equinovarus) Club Foot (Congenital Talipes Equinovarus)Dokument24 SeitenClub Foot (Congenital Talipes Equinovarus) Club Foot (Congenital Talipes Equinovarus)jyoti kunduNoch keine Bewertungen
- Craniotomy Case StudyDokument14 SeitenCraniotomy Case StudyHoney Semafranca PlatolonNoch keine Bewertungen
- Cleft Lip and PalateDokument4 SeitenCleft Lip and PalateWithlove Anji100% (1)
- Cephalopelvic DisproportionDokument3 SeitenCephalopelvic DisproportionAira MiyaNoch keine Bewertungen
- Cleft Lip and PalateDokument50 SeitenCleft Lip and Palatesusanti bulanNoch keine Bewertungen
- Cleft Lip and PalateDokument35 SeitenCleft Lip and Palatehuma100% (1)
- TEFDokument36 SeitenTEFlumina.s100% (1)
- Acute Upper Airway Obstruction (Power Point)Dokument21 SeitenAcute Upper Airway Obstruction (Power Point)Sawsan Z. Jwaied100% (2)
- Duodenal Atresia.....Dokument13 SeitenDuodenal Atresia.....Rahul Dhaker100% (4)
- Congenital AnomaliesDokument39 SeitenCongenital Anomaliesiqiqiqiqiq100% (1)
- Modern Concept of Child CareDokument14 SeitenModern Concept of Child CareKiranNoch keine Bewertungen
- Nephrotic Syndrome Nursing Care Planning & Management - Study Guide PDFDokument18 SeitenNephrotic Syndrome Nursing Care Planning & Management - Study Guide PDFSanket Telang100% (1)
- Palatoplasty Case StudyDokument26 SeitenPalatoplasty Case StudySometwo C. Hangal100% (1)
- Care of Preterm Babies: Chinchu.MDokument59 SeitenCare of Preterm Babies: Chinchu.MChinchu MohanNoch keine Bewertungen
- Cleft Lip and Palate PDFDokument52 SeitenCleft Lip and Palate PDFSylvia Anggraeni100% (2)
- Congenital Diaphragmatic HerniaDokument21 SeitenCongenital Diaphragmatic HerniaJennifer Dixon100% (1)
- Choanal AtresiaDokument5 SeitenChoanal AtresiaPriyaNoch keine Bewertungen
- Geriatric Considerations in Nursing Anp AssignmentDokument12 SeitenGeriatric Considerations in Nursing Anp AssignmentLIDIYA MOL P V50% (2)
- Tumors of External EarDokument10 SeitenTumors of External Earsavin1996100% (2)
- Neonatal SeizuresDokument6 SeitenNeonatal SeizuresDelphy VargheseNoch keine Bewertungen
- Patient Scenario, Chapter 45, Nursing Care of A Family When A Child Has A Gastrointestinal DisorderDokument93 SeitenPatient Scenario, Chapter 45, Nursing Care of A Family When A Child Has A Gastrointestinal DisorderDay MedsNoch keine Bewertungen
- MastoidectomyDokument7 SeitenMastoidectomyFrancis Arman Cabanlit0% (1)
- TracheostomyDokument31 SeitenTracheostomyTonyScaria100% (1)
- CPDDokument45 SeitenCPDVijith.V.kumar100% (1)
- ClubfootDokument21 SeitenClubfootRoss Carolino Fernandez100% (1)
- Cleft Palate: Wan Khadijah Wan Yusoff Noor Afika Binti AzriDokument91 SeitenCleft Palate: Wan Khadijah Wan Yusoff Noor Afika Binti AzriWOne WannNoch keine Bewertungen
- Phimosis and ParaphimosisDokument9 SeitenPhimosis and ParaphimosisMuhammad Azzel Hanggara100% (3)
- Assignment On TRACHEOSTOMYDokument12 SeitenAssignment On TRACHEOSTOMYPrasann Roy100% (1)
- IUGRDokument11 SeitenIUGRAnastasiafynnNoch keine Bewertungen
- Case Study of HypospadiaDokument19 SeitenCase Study of Hypospadiagaylenice100% (10)
- 6.1 Common Neonatal ProblemsDokument40 Seiten6.1 Common Neonatal ProblemsArchanaNoch keine Bewertungen
- Case Presentation HydrocephalusDokument48 SeitenCase Presentation HydrocephalusSu Osman50% (2)
- Preparation of Child For Diagnostic ProceduresDokument22 SeitenPreparation of Child For Diagnostic ProceduresAnnie GeorgeNoch keine Bewertungen
- Nursing Care Plan Tracheoesophageal Fistula and Esophagus AtresiaDokument1 SeiteNursing Care Plan Tracheoesophageal Fistula and Esophagus Atresiagannadortch88% (17)
- Mechanism of LabourDokument28 SeitenMechanism of LabourVanitha NNoch keine Bewertungen
- Cleft Lip and PalateDokument76 SeitenCleft Lip and PalateMira Hazwani100% (1)
- Specification For Training in Obstetrics and GynaecologyDokument14 SeitenSpecification For Training in Obstetrics and GynaecologyRAJUNoch keine Bewertungen
- SociologyDokument5 SeitenSociologyRAJUNoch keine Bewertungen
- Border District Cluster StrategyDokument2 SeitenBorder District Cluster StrategyRAJU100% (1)
- Alt Shortcuts ListDokument3 SeitenAlt Shortcuts ListRAJUNoch keine Bewertungen
- Module 5 ShockDokument2 SeitenModule 5 ShockRAJUNoch keine Bewertungen
- ANC-Hb Estimation SahliDokument21 SeitenANC-Hb Estimation SahliRAJUNoch keine Bewertungen
- ANC-Hb Estimation ColorstripDokument9 SeitenANC-Hb Estimation ColorstripRAJUNoch keine Bewertungen
- 51 To 100 Beded Hospital NormsDokument11 Seiten51 To 100 Beded Hospital NormsRAJUNoch keine Bewertungen
- ANC-Malaria Rapid Diagnostic KitDokument13 SeitenANC-Malaria Rapid Diagnostic KitRAJUNoch keine Bewertungen
- Chapter 4 Basic Probability - 2 PDFDokument36 SeitenChapter 4 Basic Probability - 2 PDFRAJU100% (1)
- Facilitator Guide Section 4 Annexures PDFDokument132 SeitenFacilitator Guide Section 4 Annexures PDFRAJUNoch keine Bewertungen
- Flacc RDokument1 SeiteFlacc RRAJUNoch keine Bewertungen
- Peptic UlcerDokument2 SeitenPeptic UlcerRAJUNoch keine Bewertungen
- 100 Beded Hospital NormsDokument56 Seiten100 Beded Hospital NormsRAJU100% (1)
- 51 To 100 Beded Hospital NormsDokument85 Seiten51 To 100 Beded Hospital NormsRAJU86% (7)
- National Health ProgrammesDokument12 SeitenNational Health ProgrammesRAJU100% (2)
- Nursing TheoriesDokument14 SeitenNursing TheoriesRAJUNoch keine Bewertungen
- Increasing Teacher EffectivenessDokument171 SeitenIncreasing Teacher EffectivenessRAJUNoch keine Bewertungen
- Futuristic NursingDokument7 SeitenFuturistic NursingRAJU0% (1)
- Importance of Research in NursingDokument1 SeiteImportance of Research in NursingRAJU100% (1)
- John Dewey MainDokument7 SeitenJohn Dewey MainKirk Irvin RomasantaNoch keine Bewertungen
- JST Chang & NylundDokument18 SeitenJST Chang & Nylundab yaNoch keine Bewertungen
- Oman New Reimbursement Claim FormDokument3 SeitenOman New Reimbursement Claim Formtoalok4723Noch keine Bewertungen
- Hydrotherapy by Abdul Ghafoor Sajjad Physiotherapist AFIRMDokument4 SeitenHydrotherapy by Abdul Ghafoor Sajjad Physiotherapist AFIRMAbdul Ghafoor SajjadNoch keine Bewertungen
- Cancer (Medical Term:Malignant NeoplasmDokument7 SeitenCancer (Medical Term:Malignant NeoplasmolussojiNoch keine Bewertungen
- Case Study AnalysisDokument3 SeitenCase Study Analysisapi-241588828Noch keine Bewertungen
- Prosthetic Considerations: R Mericske-SternDokument11 SeitenProsthetic Considerations: R Mericske-SternpmodontologiaNoch keine Bewertungen
- Alpha and Beta ThalassemiaDokument6 SeitenAlpha and Beta ThalassemiaSi vis pacem...100% (1)
- Ethical Issues Clinical PsychologyDokument24 SeitenEthical Issues Clinical PsychologyRose annNoch keine Bewertungen
- First Steps in REBT - Windy DrydenDokument44 SeitenFirst Steps in REBT - Windy DrydenStefan Alexandru100% (4)
- Types of Diagnosis:: Problem-Focused Nursing Diagnoses Have Three Components: (1) Nursing DiagnosisDokument4 SeitenTypes of Diagnosis:: Problem-Focused Nursing Diagnoses Have Three Components: (1) Nursing DiagnosisDaisy MellaNoch keine Bewertungen
- Fetal EchocardiographyDokument3 SeitenFetal EchocardiographypolygoneNoch keine Bewertungen
- Action Plan For ClinicDokument2 SeitenAction Plan For ClinicMelanie Delos Santos100% (3)
- Child Psychopathology: Child Psychopathology Is The Manifestation of Psychological Disorders in Children andDokument7 SeitenChild Psychopathology: Child Psychopathology Is The Manifestation of Psychological Disorders in Children andMarvellous MunhuwaNoch keine Bewertungen
- Biochemistry of Bitterness in Bamboo Shoots: Debangana Choudhury, Jatindra K. Sahu and G. D. SharmaDokument7 SeitenBiochemistry of Bitterness in Bamboo Shoots: Debangana Choudhury, Jatindra K. Sahu and G. D. SharmaKuo SarongNoch keine Bewertungen
- Ear Infections: These Include Otitis Externa, Otitis Media, MastoiditisDokument32 SeitenEar Infections: These Include Otitis Externa, Otitis Media, Mastoiditiseugene ugayNoch keine Bewertungen
- Clinical Alert A Quick Reference To Adverse Clinical EventsDokument272 SeitenClinical Alert A Quick Reference To Adverse Clinical EventsOmasNers100% (1)
- Senior Interns GrandroundsDokument119 SeitenSenior Interns GrandroundsNicko GranadoNoch keine Bewertungen
- Junior Seau Autopsy ReportDokument16 SeitenJunior Seau Autopsy ReportDeadspin83% (6)
- Psychological ReportDokument4 SeitenPsychological ReportJoyAMC75% (4)
- Bladder Calculus Resulting From The Migration of An IntrauterineDokument8 SeitenBladder Calculus Resulting From The Migration of An IntrauterineFabrien Hein WillemNoch keine Bewertungen
- TuberculosisDokument16 SeitenTuberculosisjojolim18100% (1)
- Leptospirosis CaseDokument29 SeitenLeptospirosis CaseJp RectraNoch keine Bewertungen
- Bsn-Stem1a - M7 Post TaskDokument12 SeitenBsn-Stem1a - M7 Post TaskPhoemela Reign GregorioNoch keine Bewertungen
- Ocular Manifestations in AIDSDokument27 SeitenOcular Manifestations in AIDSAnumeha Jindal100% (1)
- Truncated Middle Turbinnate SNPDokument4 SeitenTruncated Middle Turbinnate SNPSriram RajanNoch keine Bewertungen
- 04 GTTDokument15 Seiten04 GTTAshish TuraleNoch keine Bewertungen
- Osteoporosis and Fragility Fractures Surgical PerpspectiveDokument54 SeitenOsteoporosis and Fragility Fractures Surgical PerpspectiveSonal DudaniNoch keine Bewertungen
- Blood Sugar Insulin Polyuria Polydipsia PolyphagiaDokument7 SeitenBlood Sugar Insulin Polyuria Polydipsia PolyphagiankirrNoch keine Bewertungen
- Painful Intramuscular Lipoma of The Infraspinatus Unusual Location and PresentationDokument4 SeitenPainful Intramuscular Lipoma of The Infraspinatus Unusual Location and PresentationWewik PenaNoch keine Bewertungen
- Sewage Treatment PlantDokument12 SeitenSewage Treatment Plantanuj dhavanNoch keine Bewertungen