Beruflich Dokumente
Kultur Dokumente
Nursing Care Plan
Hochgeladen von
Merfat AbubakarOriginalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Nursing Care Plan
Hochgeladen von
Merfat AbubakarCopyright:
Verfügbare Formate
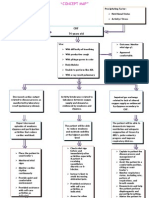
NURSING CARE PLAN
ASSESSMENT Subjective Cues: Masakit po at parang nangingilo ang legs ko, as verbalized by the patient. OBJECTIVE OF CARE At the end of 48 hours nursing intervention, the patient will be able to: NURSING INTERVENTION RATIONALE IMPLEMENTATION EVALUATION After implementing the nursing interventions: The patient have verbalized understanding of causative factors and demonstrated behaviors to resolve excess fluid volume.
Objective Cues verbalize assess patients general To determine assessed patients general - BP: 180/90 mmhg understanding of condition what approach to condition - T: 39C causative factors use in treatment - edematous leg of excess fluid - shortness of breath volume discuss the causative To give knowledge Discussed the causative - Urine Output: 500 factors of excess fluid factors of the excess fluid mL for 24 hour volume volume. period -Lab results: demonstrate monitor intake and I&O balance monitored intake and output Creatinine 6.3 adequate fluid output every 4 hours reflects fluid every 4 hours BUN 90 balance status Potassim 7.0
Nursing Diagnosis Fluid volume excess related to decrease urine out put and retention of sodium and water
weigh patient daily and compare to previous weights
Body weight is a weighed patient daily and sensitive compared to previous indicator of fluid weights balance and an increase indicates fluid volume excess
Auscultate breath When increased Auscultated breath sounds sounds q 2hr and pm for pulmonary q 2hr the presence of crackles capillary and monitor for frothy hydrostatic sputum production pressure exceeds oncotic pressure, fluid moves within the alveolar septum and is evidenced by the auscultation of crackles. Frothy, pink-tinged sputum is an indicator that the client is
developing pulmonary edema
Follow low-sodium diet Fluid restriction and/or fluid restriction may be used to decrease fluid intake, hence decreasing fluid volume excess.
Followed low-sodium diet and/or fluid restriction
Encourage or provide oral care q2
The client senses Encouraged or provide oral thirst because care q2 the body senses dehydration. Oral care can alleviate the sensation without an increase in fluid intake Inidicates fluid overload Monitored for distended neck veins and ascites
Monitor for distended neck veins and ascites
HEALTH TEACHING PLAN
SUBJECT MATTER: Acute Renal Failure TIME ALLOTMENT: 15 mins GENERAL OBJECTIVES: At the end of 15 minutes health teaching, the patient and his family will be able to acquire knowledge about acute renal failure. LEARNING OBJECTIVES At the end of health teaching, the patient should be able to: 1. Define acute renal failure The acute renal failure is an abrupt reduction in renal functions associated with oligurea (less than 400/day),fatigue,anorexia,nausea and vomiting 2 mins Explanation TIME ALLOTMENT
CONTENT
STRATEGIES
EVALUATION CRITERIA
ORAL QUESTIONING
In your own understanding, what is acute renal failure? -Ang acute renal failure po ay ang paunti-unting pagkawala ng function ng kidney natin. Can you give atleast 4 signs and symptoms? -fatigue -pagsusuka
2. Enumerate the signs and symptoms
Signs and Symptoms Oligurea (less than 400ml/day) Anuria(less than 50/day) Fatigue
4 mins
One on one discussion
3. Demonstrate understanding on the cause of acute renal failure
Anorexia Nausea Vomiting Increase creatinine and urea level in serum
-pagkonti ng dami ng ihi -walang ganang kumain
CAUSES AKI can be caused by disease, crush injury, contrast agents, some antibiotics, and more. The causes of acute kidney injury are commonly categorized into prerenal, intrinsic, and postrenal. Prerenal
6 mins
Explanation Any question about the causes of acute renal failure? -Wala po. Naiintidihan ko na isa sa mga rason kung bakit may acute renal failure ako ay dahil sa pagkakaroon ko ng diabetes.
Prerenal causes of AKI ("pre-renal azotemia") are
those that decrease effective blood flow to the kidney. These include systemic causes, such as low blood volume, low blood pressure, heart failure, and local changes to the blood vessels supplying the kidney. The latter include renal artery stenosis, or the narrowing of the renal arterywhich supplies the kidney with blood, and renal vein thrombosis, which is the formation of a blood clot in the renal vein that drains blood from the kidney. Intrinsic Sources of damage to the kidney itself are dubbed intrinsic. Intrinsic AKI can be due to damage to the glomeruli, renal tubules,
orinterstitium. Common causes of each are glomerulonephritis, acute tubular necrosis (ATN), and acute interstitial nephritis (AIN), respectively. A cause of intrinsic acute renal failure is tumor lysis syndrome.[7] Postrenal
Postrenal AKI is a consequence of urinary
tract obstruction. This may be related to benign prostatic hyperplasia, kidney stones, obstructed urinary catheter, bladder stone, bladder, ureteral or renal malignancy. It is useful to perform a bladder scan or a post void residual to rule out urinary retention.
DIET: 4. Identify the importance of diet Low sodium Diet People with acute renal failure can improve their symptoms by reducing the amount of salt (sodium) in their diet. Sodium is a mineral found in many foods. Eating too much salt causes the body to keep or retain too much water, worsening the fluid build-up associated with heart failure. 3 mins One on one discussion How will it help you? -Sa pamamagitan ng pagkain ng tama ay kahit papaano mababawasan ang aking paghihirap sa mga sintomas.
GENERIC NAME -Furosemide
INDICATION
SIDE EFFECTS
NURSING RESPONSIBILITIES Observe the 10 rights in administering medications. Assess fluid status. Notify physician or other health care professional if thirst, dry mouth, hypotension, or oliguria occurs. Monitor blood pressure and pulse before and during administration. Monitor blood glucose closely; may cause increased blood glucose level. Caution patient to change positions slowly to minimize orthostatic hypotension. Advise patient to contact health care professional immediately if muscle weakness, cramps,nausea, dizziness and numbness occurs.
CLASSIFICATION - Loop diuretics
Edema d/t heart failure, hepatic impairment or renal disease. Hypertension.
blurred vision, dizziness, head ache, vertigo
DOSAGE - 1 tablet, 200 mg
CONTRAINDICATIONS
ADVERSE EFFECTS
ROUTE -PO
Hypersensitivity; Cross-sensitivity with thiazides and sulfonamides may occur; Hepatic coma or anuria; Some liquid products may contain alcohol, avoid in patients with alcohol intolerance.
CNS blurred vision, dizziness, head ache, vertigo EENT hearing loss, tinnitus CV hypotension GI anorexia, constipation, diarrhea, dry mouth, nausea, vomiting GU excessive urination Derm photosensitivity, rash F and E dehydration
GENERIC NAME: - Norfloxacin
INDICATION
SIDE EFFECTS
NURSING RESPONSIBILITIES Observe the 10 rights in administering medications. Instuct patient to take the drug on an empty stomach. Teach patient to drink a lot of fluids. Advise patient to contact health care professional immediately if muscle weakness, cramps,nausea, dizziness and numbness occurs.
CLASSIFICATION - Antibiotic - Fluoroquinolone DOSAGE - 4oo mg
FREQUENCY: -Q12
For the treatment of adults with UTIs caused by susceptible bacteria. Prostatitis caused by E. coli
blurred vision, dizziness, head ache, vertigo
CONTRAINDICATIONS
ADVERSE EFFECTS
ROUTE -PO
Contraindicated with allergy to norfloxacin, nalidixic acid or cinoxacin; lactation; history of tendonitis or tendon rupture. Use cautiously in patients with renal impairment, seizures, pregnancy.
CNS headache, dizziness, insomnia, fatigue, somnolence, depression, blurred vision GI anorexia, constipation, diarrhea, dry mouth, nausea, vomiting
GENERIC NAME: - Amlodipine besylate
INDICATION
SIDE EFFECTS
NURSING RESPONSIBILITIES Observe the 10 rights in administering medications. Monitor patients BP carefully while adjusting drug to therapeutic doses. Administer drug without regard to meals. Instruct patient to report immediately if he will have irregular heartbeat, shortness of breath, swelling of feet or hands
CLASSIFICATION - Antianginal - Antihypertensive DOSAGE - 5 mg
FREQUENCY: -QID
Essential hypertension, alone or in combination with other antihypertensives. Also for chronic stable angina.
Nausea, vomiting and headache
CONTRAINDICATIONS
ADVERSE EFFECTS
ROUTE -PO
Contraindicated with allergy to amlodipine. Use cautiously with heart failure and pregnancy.
CNS light-headedness, dizziness, asthenia, fatigue, lethargy CV peripheral edema, arrythmias GI nausea, abdominal discomfort Dermatologic flushing, rash
GENERIC NAME: - Sodium Polystyrene Sulfonate
INDICATION
SIDE EFFECTS
NURSING RESPONSIBILITIES Observe the 10 rights in administering medications. Monitor serum electrolytes. Frequent blood tests will be needed to monitor drug effect. Report confusion, irregular heartbeats, constipation, severe GI upset.
Treatmentof hyperkalemia. CLASSIFICATION - Potassium removing resin DOSAGE - 15g
FREQUENCY: -QID
GI upset and constipation.
CONTRAINDICATIONS
ADVERSE EFFECTS
ROUTE -PO
Contraindicated with allergy to any component of the drug, obstructive bowel, severe hypertension, severe HF, marked edema.
GI constipation, fecal impacation, gastric irritation, anorexia, nausea, vomiting Hematologic Hypokalemia, electrolyte abnormalities
HEALTH PROBLEM Possible preeclampsia
FAMILY NURSING PROBLEM 1.Inability to recognize the possible complication in pregnancy due to lack of knowledge. 2.Inability to provide adequate nursing care to a pregnant member due to: a. Failure to comprehend the nature and magnitude of the condition. b.Low salience of theproblem/ condition.
GOAL OF CARE After nursing intervention, the family will be able to take the necessary measures to properly manage preeclampsia.
OBJECTIVES OF CARE After nursing intervention, thefamily will be able to:
INTERVENTIONS
IMPLEMENTATIO N
EVALUATION
1.Acquire information about the complication including the signs and symptoms.
1.Discuss with the family the causes, signs and symptoms, on complications of pre-eclampsia. RATIONALE: -To educate family about the disease condition. 2. Allow the family to verbalize doubts, questions and others which can hinder them from addressing the problem properly. RATIONALE: -To recognize thought of the family members and to provide understanding about their questions and doubts.
2. Enumerate the ways in preventing preeclampsia.
The goal of care was met since the family demonstrated > Discussed with the understanding family the causes, regarding the signs and symptoms, disease on complications of conditin and pre-eclampsia. ways to prevent it by answering all the questions > Allowed the family I asked for to verbalize doubts, each family questions and member. others which can hinder them from addressing the problem properly.
3. Name the foods that are prohibited to Mrs. Tan.
3. Discuss with the family the ways in preventing preeclampsia. RATIONALE: -To provide information about in preventing the disease. 4. Provide written information and selflearning modules for client to refer as necessary. RATIONALE: -Reinforces learning process, allows clients proceed at own pace.
> Discussed with the family the ways in preventing preeclampsia.
> Provided written information and self-learning modules for client to refer as necessary.
Das könnte Ihnen auch gefallen
- Intracranial HemorrhageDokument41 SeitenIntracranial Hemorrhagedoctormussieaberra100% (1)
- Careplan 5 MedsurgDokument8 SeitenCareplan 5 Medsurgapi-509642710Noch keine Bewertungen
- Nursing Care PlanDokument23 SeitenNursing Care PlanLorielle HernandezNoch keine Bewertungen
- Nursing Care Plan Renal FailureDokument18 SeitenNursing Care Plan Renal FailureKundan KumarNoch keine Bewertungen
- Tissue PerfusionDokument2 SeitenTissue PerfusionMichael John LeandichoNoch keine Bewertungen
- NCP For BreathingDokument17 SeitenNCP For BreathingCeleste Sin Yee100% (1)
- Nursing Care PlanDokument22 SeitenNursing Care PlanjamNoch keine Bewertungen
- Anatomy and Physiology: Circulatory SystemDokument4 SeitenAnatomy and Physiology: Circulatory SystemJordz PlaciNoch keine Bewertungen
- Urinary Tract Infection, (UTI) Is An Infection of One orDokument4 SeitenUrinary Tract Infection, (UTI) Is An Infection of One orLorebellNoch keine Bewertungen
- Actual Nursing Care Plan GT DisorderDokument3 SeitenActual Nursing Care Plan GT DisordermandzkievonnieNoch keine Bewertungen
- Nursing Care Plan: Congestive Heart Failure-Deep Vein ThrombosisDokument19 SeitenNursing Care Plan: Congestive Heart Failure-Deep Vein ThrombosisRiza Angela BarazanNoch keine Bewertungen
- Ineffective Cerebral Tissue Perfusion Related ToDokument7 SeitenIneffective Cerebral Tissue Perfusion Related TohannahNoch keine Bewertungen
- NCP BronchopneumoniaDokument8 SeitenNCP BronchopneumoniaCrisantaCasliNoch keine Bewertungen
- Student Nurses' Community: Nursing Care Plan Assessment Diagnosis Inference Planning Intervention Rationale EvaluationDokument3 SeitenStudent Nurses' Community: Nursing Care Plan Assessment Diagnosis Inference Planning Intervention Rationale Evaluationgreyciee은Noch keine Bewertungen
- 3 NCP Ineffective Tissue PerfusionDokument2 Seiten3 NCP Ineffective Tissue PerfusionSteffi MurielNoch keine Bewertungen
- Small Bowel Obstruction Concept MapDokument1 SeiteSmall Bowel Obstruction Concept MapTessa Claire JaranowskiNoch keine Bewertungen
- Case Study 2Dokument7 SeitenCase Study 2desdav100% (1)
- Rufino, Leslie Kriztel S. BSN 3-2 Group 1Dokument6 SeitenRufino, Leslie Kriztel S. BSN 3-2 Group 1Deinielle Magdangal RomeroNoch keine Bewertungen
- Case PresentationDokument5 SeitenCase PresentationJARIETTA OCHOANoch keine Bewertungen
- Decreased Cardiac Output RM 7Dokument9 SeitenDecreased Cardiac Output RM 7api-283470660Noch keine Bewertungen
- Hemophilia N C P BY BHERU LALDokument1 SeiteHemophilia N C P BY BHERU LALBheru LalNoch keine Bewertungen
- HypokalemiaDokument3 SeitenHypokalemiaSergeiNoch keine Bewertungen
- Nursing Care Plan Impaired Gas ExchangeDokument1 SeiteNursing Care Plan Impaired Gas ExchangeKarylle PetilNoch keine Bewertungen
- Concept Map SepsisDokument4 SeitenConcept Map SepsisSavanna ChambersNoch keine Bewertungen
- Health-Perception-Health-Management PatternDokument3 SeitenHealth-Perception-Health-Management PatternBela MillenaNoch keine Bewertungen
- 16 ARDS - Nursing Care ManagementDokument2 Seiten16 ARDS - Nursing Care ManagementTisha CarretteNoch keine Bewertungen
- Case Study RespiDokument3 SeitenCase Study RespiMark Jheran AlvarezNoch keine Bewertungen
- Nursing Care Plan FinalDokument16 SeitenNursing Care Plan FinalErickson OcialNoch keine Bewertungen
- Nursing Intervention For Chest PainDokument2 SeitenNursing Intervention For Chest Painjhaden100% (3)
- Aspiration PneumoniaDokument18 SeitenAspiration PneumoniaRaja Alfian IrawanNoch keine Bewertungen
- Concept Map - Abby !Dokument2 SeitenConcept Map - Abby !Abegail Abaygar100% (3)
- This Study Resource Was Shared ViaDokument4 SeitenThis Study Resource Was Shared ViaKyuSheen100% (1)
- Medication ThalassemiaDokument3 SeitenMedication ThalassemiaDivya ToppoNoch keine Bewertungen
- Nursing Care PlanDokument15 SeitenNursing Care PlanZhel Geron MercadoNoch keine Bewertungen
- 10 CaritosDokument3 Seiten10 CaritosDARREN EDMARK100% (4)
- IBSDokument1 SeiteIBSIris MambuayNoch keine Bewertungen
- Nursing Care PlanDokument5 SeitenNursing Care PlanPaola Marie VenusNoch keine Bewertungen
- ABG InterpretationDokument23 SeitenABG Interpretationprateekbatra0% (1)
- NCP Blood Glucose Imbalance 4thDokument2 SeitenNCP Blood Glucose Imbalance 4thRainier IbarretaNoch keine Bewertungen
- Multiple Sclerosis Nursing Care PlanDokument4 SeitenMultiple Sclerosis Nursing Care PlanCHRISTIE MONTANONoch keine Bewertungen
- Nursing Care PlanDokument4 SeitenNursing Care PlanDewi PurnamasariNoch keine Bewertungen
- Nursing Care PlanDokument13 SeitenNursing Care PlanCris Solis33% (3)
- NCP and DStudyDokument8 SeitenNCP and DStudyJessica Rosan Hewald ManapatNoch keine Bewertungen
- Nursing Care Plan EportfolioDokument14 SeitenNursing Care Plan Eportfolioapi-279212367Noch keine Bewertungen
- Ineffective Airway Clearance-Nursing Care Plan For COPDDokument2 SeitenIneffective Airway Clearance-Nursing Care Plan For COPDRnspeakcom100% (1)
- NCPDokument7 SeitenNCPmftaganasNoch keine Bewertungen
- FractureDokument1 SeiteFractureReechie TeasoonNoch keine Bewertungen
- Ineffective Airway Clearance: Nursing Care PlanDokument2 SeitenIneffective Airway Clearance: Nursing Care PlanJose Mari F. Esguerra0% (1)
- CC Concept MapDokument9 SeitenCC Concept Mapapi-606252228Noch keine Bewertungen
- Nursing Care PlanDokument4 SeitenNursing Care PlanKath RubioNoch keine Bewertungen
- Healthcare - Nursing Care Plan - Excess Fluid VolumeDokument4 SeitenHealthcare - Nursing Care Plan - Excess Fluid VolumeBenjamin CañalitaNoch keine Bewertungen
- CellulitisDokument12 SeitenCellulitisAlma Bertos-Agub100% (1)
- Prepu Psych Chapter 1Dokument329 SeitenPrepu Psych Chapter 1nana100% (1)
- Nursing Care Plan: Subjective DataDokument4 SeitenNursing Care Plan: Subjective DataAbdallah AlasalNoch keine Bewertungen
- Nursing Care Plans For UTIDokument2 SeitenNursing Care Plans For UTIHannah Pin67% (3)
- Clinical Log Term II PDFDokument9 SeitenClinical Log Term II PDFPriscilla S100% (1)
- Care Plan September 25 Med-SurgDokument19 SeitenCare Plan September 25 Med-Surgapi-251516913Noch keine Bewertungen
- Name of The Drug Date Ordered Classification Dose Frequency Route Mechanism of Action Specific Indication Side Effects Nursing ImplicationDokument9 SeitenName of The Drug Date Ordered Classification Dose Frequency Route Mechanism of Action Specific Indication Side Effects Nursing ImplicationFrances Oscar GaviolaNoch keine Bewertungen
- NCPsDokument13 SeitenNCPsRocel DevillesNoch keine Bewertungen
- Care of Older Adults (Prelims)Dokument12 SeitenCare of Older Adults (Prelims)Ax’l SisterNoch keine Bewertungen
- 2surgical Nursing-Chronic Illness and Older AdultsDokument6 Seiten2surgical Nursing-Chronic Illness and Older AdultsGedie RocamoraNoch keine Bewertungen
- Stress Hyperglycemia: Anand MosesDokument4 SeitenStress Hyperglycemia: Anand MosesDaeng Arya01Noch keine Bewertungen
- NCP PediaDokument2 SeitenNCP PediaAdrian John DecolongonNoch keine Bewertungen
- Nerium OleanderDokument20 SeitenNerium OleanderGeneizzel GotuatoNoch keine Bewertungen
- Paracetamol Overdose Treatment NomogramDokument1 SeiteParacetamol Overdose Treatment NomogramCoenraad van SchoorNoch keine Bewertungen
- Gonorrhea Case Study 2009Dokument4 SeitenGonorrhea Case Study 2009Garrett Batang100% (3)
- Benning Vanessa - Resume-2Dokument1 SeiteBenning Vanessa - Resume-2api-489132887Noch keine Bewertungen
- Role of Physiotherapy in Antenatal and Post-Natal Care: Dr. Venus Pagare (PT)Dokument74 SeitenRole of Physiotherapy in Antenatal and Post-Natal Care: Dr. Venus Pagare (PT)Haneen Jehad Um Malek100% (1)
- Pharmacoeconomics - Part IIIDokument29 SeitenPharmacoeconomics - Part IIISima JabbariNoch keine Bewertungen
- PAF Rev. 2.0 (FILLABLE)Dokument1 SeitePAF Rev. 2.0 (FILLABLE)Melody Joy CantosNoch keine Bewertungen
- Medication AdministrationDokument3 SeitenMedication AdministrationMonika SarmientoNoch keine Bewertungen
- Terapia Clark Referencias Cientificas OzonoDokument17 SeitenTerapia Clark Referencias Cientificas OzonoGomez Gomez100% (2)
- Activity Design For Trainings - TB - HIVDokument7 SeitenActivity Design For Trainings - TB - HIVSample BakeshopNoch keine Bewertungen
- Cardiorenal Syndrome Referat Imam (BYS & EM)Dokument27 SeitenCardiorenal Syndrome Referat Imam (BYS & EM)Afrilia IntanNoch keine Bewertungen
- Illizarov and Principle of Distraction OsteogenesisDokument7 SeitenIllizarov and Principle of Distraction OsteogenesisThiru MuruganNoch keine Bewertungen
- Arnica Montana - FayazuddinDokument13 SeitenArnica Montana - FayazuddinMohammad AtaNoch keine Bewertungen
- Flare-Ups After Endodontic Treatment: A Meta-Analysis of LiteratureDokument5 SeitenFlare-Ups After Endodontic Treatment: A Meta-Analysis of LiteratureDr.O.R.GANESAMURTHINoch keine Bewertungen
- Cycle BeadsDokument2 SeitenCycle Beadsgihan200100% (2)
- Fdar GammyDokument2 SeitenFdar GammyAndrea Sibayan SorianoNoch keine Bewertungen
- Selective Awareness TherapyDokument10 SeitenSelective Awareness TherapyHashem Al AttasNoch keine Bewertungen
- Quantum Techniques Client ManualDokument42 SeitenQuantum Techniques Client ManualVeres Beatrix100% (4)
- Remifentanil Versus Propofol/Fentanyl Combination in Procedural Sedation For Dislocated Shoulder Reduction A Clinical TrialDokument5 SeitenRemifentanil Versus Propofol/Fentanyl Combination in Procedural Sedation For Dislocated Shoulder Reduction A Clinical TrialerinNoch keine Bewertungen
- Midwifery KitDokument3 SeitenMidwifery KitRitzel CreusNoch keine Bewertungen
- Management of A Case of Ventricular Bigeminy UsingDokument2 SeitenManagement of A Case of Ventricular Bigeminy UsingAlfian AlfianNoch keine Bewertungen
- Out of Stock Items List - Till Last Week.27 JunDokument65 SeitenOut of Stock Items List - Till Last Week.27 Junmanuella ANoch keine Bewertungen
- 53 JMSCRDokument7 Seiten53 JMSCRAddinul FitryNoch keine Bewertungen
- Injectable Anesthesia and Analgesia of Birds 5-Aug PDFDokument15 SeitenInjectable Anesthesia and Analgesia of Birds 5-Aug PDFYaserAbbasiNoch keine Bewertungen
- AMA Retrospective AuditsDokument2 SeitenAMA Retrospective AuditsEma ForgacsNoch keine Bewertungen
- Formulation Design, Optimization and Evaluation of Domperidone Maleate Gastro Retentive Floating TabletsDokument10 SeitenFormulation Design, Optimization and Evaluation of Domperidone Maleate Gastro Retentive Floating TabletsDr. Raghavendra Kumar GundaNoch keine Bewertungen