Beruflich Dokumente
Kultur Dokumente
Path of Physiology
Hochgeladen von
Carla JimenezOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Path of Physiology
Hochgeladen von
Carla JimenezCopyright:
Verfügbare Formate
Pathophysiology - Pneumonia
Pneumonia inflammatory process of the lung parenchyma Classification 1. Community Acquired used to describe infections found in the community rather than the hospital/nursing home. Defined as an infection that begins outside the hospital or is diagnosed 48 hours after admission to the hospital in a person who has not resided in a long term facility for 14 days or more before admission 2. Hospital Acquired or Nosocomial is defined as a lower respiratory tract infection that was not present or incubating on admission to the hospital. Increase risk for those with mechanical ventilation, compromised immune function, chronic lung disease and airway instrumentation such as e-tube, tracheostomy, etc. Types According to Causative Agent 1. Gram Positive Bacteria Streptococcus pneumonia (pneumococcal pneumonia) most common cause of community acquired pneumonia. follows influenza I situations in which groups of people live in close contact rust colored sputum, blood tinged, purulent Staphylococcus aureus acquired thru blood or by aspiration creamy yellow sputum
2. Gram Negative Bacteria Haemophilus influenza common cause of infection in children high mortality rate greenish colored sputum Klebsiella pneumoniae (Friedlanders bacillus) most common gram negative organism acquired outside hospitals occurs in people with malignancies necrosis, abscess foration, hemoptysis and fibrotic changes occur high mortality rate red gelatinous sputum Pseudomonas aeroginosa most common gram negative organism acquired in the hospital common in the respiratory tract of hospital employees and those with cystic fibrosis greenish colored sputum Legionella pneumophilia (Legionnaires disease) most common cause of community acquired pneumonia found in warm standing water
3. ANAEROIC BACTERIAL PNEUMONIAS Commonly caused by anaerobic streptococcus History of poor dental hygiene, periodontal disease, dysphagia and altered consciousness
4. OTHER INFECTIOUS AGENTS Mycoplasma pneumoniae Fungi an organism with the characteristics of both bacteria and viruses it causes atypical/interstitial pneumonia Viral agents influenza virus, adenovirus and parainfluenza virus self-limiting may predispose to secondary bacterial infection
candidiasis, histoplasmosis, blastomycosis, cryptococcosis, aspergillosis, actinomycosis and nocardiosis follows after extended antibiotic use, immunocompromised and seriously ill people Non-infectious causes
inhalation of toxic gases, chemicals or smoke from fires and aspiration of water due to near drowning, gastric contents, vegetable/mineral oils, liquid petroleum function Pneumocystis carinii pneumonia opportunistic, often fatal form of lung infection seen in debilitated, impaired immune
RISK FACTORS Smoking Air pollution Upper Respiratory Tract Infection
Altered consciousness: alcoholism, head injury, seizure disorder, drug overdose, general anesthesia Tracheal intubation Prolonged immobility Immunosuppressive therapy: corticosteroids, chemotherapy Non-functional immune system: AIDS Severe periodontal disorders Prolonged exposure to virulent organisms Malnutrition Dehydration Chronic disease: Diabetes Mellitus, Heart disease, chronic lung disease Prolonged debilitating disorders Inhalation of noxious substances Aspiration of oral/gastric material Aspiration of foreign material
Chronically ill, elderly people who generally have poor immune systems, often residing in group living situations where there is an increase in probability of disease transmission especially through the respiratory system SIGNS AND SYMPTOMS Fever
Chills Sweats Dullness on percussion on affected area Sputum production Hemoptysis Pleuritic chest pain Dyspnea Headache Fatigue Unequal chest expansion Cough
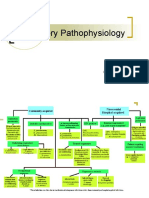
Pathophysiology Inhalation of droplet nuclei Establishes in the alveolus (usually lower lobe) Bacterial infection develops Vascular engorgement, presence of large number of bacteria Serous exudate pours into alveoli from dilated leaking vessels (engorgement first 4-12 hours) Decrease in RBC and Increase in Neutrophils and precipitation of fibrin that fills the alveoli Continuing accumulation of fibrin Consolidation of leukocytes and fibrin Exudate is lyzed and reabsorbed by macrophage DIAGNOSTIC TESTS Chest x-ray Sputum smear Blood cultures Bronchoscopy Transtracheal aspirate
MEDICAL MANAGEMENT 1. medications antimicrobial therapy, pain medication for pleuritic chest pain 2. 3. 4. oxygen therapy bed rest high-calorie diet
5.
adequate fluid intake
NURSING MANAGEMENT 1. Secure airways and ensure adequate oxygenation. 2. 3. 4. 5. 6. Administer analgesics when needed. Administer antibiotics as prescribed. Maintain adequate nutrition. Educate the patient how to cough properly and deep breathing exercises. Position the client properly so as to help clear secretions.
http://nursearchives.blogspot.com/2012/07/pathophysiology-pneumonia.html
Das könnte Ihnen auch gefallen
- PneumoniaDokument50 SeitenPneumoniaannududi378556Noch keine Bewertungen
- Pathology Slide #6+7Dokument73 SeitenPathology Slide #6+7Ibrahim MigdadyNoch keine Bewertungen
- Pneumonia CHN Case ReportDokument6 SeitenPneumonia CHN Case ReportRhaine MagtotoNoch keine Bewertungen
- Community Acquired PneumoniaDokument9 SeitenCommunity Acquired PneumoniaSuzette Rae TateNoch keine Bewertungen
- Clinical Presentation On PnemoniaDokument37 SeitenClinical Presentation On PnemoniasreekalaNoch keine Bewertungen
- Pneumonia: DefinitionDokument5 SeitenPneumonia: DefinitionhemaanandhyNoch keine Bewertungen
- Chapter 1Dokument30 SeitenChapter 1Ayro Business CenterNoch keine Bewertungen
- Community Acquired Pneumonia Nelson 400Dokument37 SeitenCommunity Acquired Pneumonia Nelson 400fatima chrystelle nuñalNoch keine Bewertungen
- Pediatric Community-Acquired Pneumonia: Nelson 20 EdDokument43 SeitenPediatric Community-Acquired Pneumonia: Nelson 20 EdRazel Kinette AzotesNoch keine Bewertungen
- PneumoniaDokument5 SeitenPneumoniasamtaynbNoch keine Bewertungen
- Lower Airway DiseasesDokument70 SeitenLower Airway DiseasesAavash PradhanNoch keine Bewertungen
- PneumoniaDokument79 SeitenPneumoniaEjiro OnoroNoch keine Bewertungen
- Pneumonia 3Dokument8 SeitenPneumonia 3janinecasilenNoch keine Bewertungen
- Pneumonia, BronchiolitisDokument65 SeitenPneumonia, BronchiolitisYemata HailuNoch keine Bewertungen
- Pneumonia: ANAND. TO, 1ST MSC Student Nursinc NsgstudentDokument11 SeitenPneumonia: ANAND. TO, 1ST MSC Student Nursinc NsgstudentArunNoch keine Bewertungen
- Respiratory Pathophysiology: B. Pimentel, M.D. University of Makati College of NursingDokument12 SeitenRespiratory Pathophysiology: B. Pimentel, M.D. University of Makati College of NursingDoc JacqueNoch keine Bewertungen
- Hospital Acquired PneumoniaDokument36 SeitenHospital Acquired Pneumoniaadamu mohammadNoch keine Bewertungen
- Clinical PresentationDokument54 SeitenClinical PresentationSêrâphîm HâdíNoch keine Bewertungen
- ncm112 FinalsDokument18 Seitenncm112 FinalsAbegail MierNoch keine Bewertungen
- Aspirasi PnemoniDokument23 SeitenAspirasi PnemoniBerto UsmanNoch keine Bewertungen
- Handout PCI 2Dokument8 SeitenHandout PCI 2Sis CrezylNoch keine Bewertungen
- Pneumonia 150514133315 Lva1 App6892Dokument34 SeitenPneumonia 150514133315 Lva1 App6892SadiaNoch keine Bewertungen
- 3 - PneumoniaDokument6 Seiten3 - PneumoniaAmmar AlnajjarNoch keine Bewertungen
- Pcap Didactics ChanDokument61 SeitenPcap Didactics ChanValerie Anne BebitaNoch keine Bewertungen
- PneumoniaDokument68 SeitenPneumoniaJelmalyn Basali100% (1)
- Week 1 TropMedDokument96 SeitenWeek 1 TropMedmyqurandiaryNoch keine Bewertungen
- Oxygen Saturation (If Available) : IagnosisDokument3 SeitenOxygen Saturation (If Available) : Iagnosisrezairfan221Noch keine Bewertungen
- Pneumonia 1Dokument17 SeitenPneumonia 1Jonathan katanaNoch keine Bewertungen
- Group 2 Community Acquired PneumoniaDokument24 SeitenGroup 2 Community Acquired PneumoniaalyanadayritNoch keine Bewertungen
- PneumoniaDokument9 SeitenPneumonianachiketpanchal8Noch keine Bewertungen
- Pneumonia WrittenDokument12 SeitenPneumonia WrittenFereli Joy SupanNoch keine Bewertungen
- Lung AbscessDokument38 SeitenLung Abscessprabad dunusingheNoch keine Bewertungen
- BPNDokument49 SeitenBPNlovelots1234100% (1)
- Pneumonia: Shervin GolbariDokument24 SeitenPneumonia: Shervin GolbarisgolbariNoch keine Bewertungen
- PneumoniaDokument3 SeitenPneumoniaKami KhanNoch keine Bewertungen
- Pediatric Community-Acquired PneumoniaDokument60 SeitenPediatric Community-Acquired PneumoniaIkea Balhon100% (1)
- Week 4 Restrictive DisordersDokument212 SeitenWeek 4 Restrictive Disordersdelrosariojm87Noch keine Bewertungen
- Communicable DiseasesDokument101 SeitenCommunicable DiseasesKira100% (4)
- Aspiration PneumoniaDokument18 SeitenAspiration PneumoniaRaja Alfian IrawanNoch keine Bewertungen
- Lect 8 Pneumonia PDFDokument68 SeitenLect 8 Pneumonia PDFRaghad AbdullaNoch keine Bewertungen
- Epidemiology of TBDokument4 SeitenEpidemiology of TByam pdNoch keine Bewertungen
- Pneumonia: Anjitha JosephDokument43 SeitenPneumonia: Anjitha JosephanjithaNoch keine Bewertungen
- Revise PneumoniaDokument7 SeitenRevise PneumoniaMelai AvilaNoch keine Bewertungen
- Pneumonia WW ReportDokument29 SeitenPneumonia WW ReportAradhanaRamchandaniNoch keine Bewertungen
- Pneumonia: Prof. Ezekiel M. WafulaDokument20 SeitenPneumonia: Prof. Ezekiel M. Wafulaokwadha simion100% (1)
- Pneumonia in ChildrenDokument22 SeitenPneumonia in ChildrenHarsha HinklesNoch keine Bewertungen
- Lung Abscess Bronchoectasis PleurisynDokument19 SeitenLung Abscess Bronchoectasis Pleurisynmarco luenaNoch keine Bewertungen
- PneumoniaDokument2 SeitenPneumoniaMargaret EricksonNoch keine Bewertungen
- Pneumonia: Heny Ekowati, PH.D., AptDokument19 SeitenPneumonia: Heny Ekowati, PH.D., Aptaryati yayaNoch keine Bewertungen
- Sistem Respirasi Sesak Napas: Problem Based LearningDokument61 SeitenSistem Respirasi Sesak Napas: Problem Based LearningAkbar IskandarNoch keine Bewertungen
- W1 L2 PneumoniaDokument57 SeitenW1 L2 PneumoniaAnas FikriNoch keine Bewertungen
- PneumoniaDokument24 SeitenPneumoniaWidhi AstutiNoch keine Bewertungen
- Care of Patient With Respiratory DisordersDokument35 SeitenCare of Patient With Respiratory Disorderskriiteeabns100% (1)
- Lec 9 Respiratory Disorders Part 2Dokument11 SeitenLec 9 Respiratory Disorders Part 2iam2117Noch keine Bewertungen
- Lung Abscess: BackgroundDokument12 SeitenLung Abscess: BackgroundTaufik TiasNoch keine Bewertungen
- Pneumonia and GastroentiritisDokument3 SeitenPneumonia and Gastroentiritismarie100% (5)
- Pneumonia: DR - Dr. Tahan P.H.,Spp.,Dtce.,Mars Fk-Uwk, 1 April 2011Dokument42 SeitenPneumonia: DR - Dr. Tahan P.H.,Spp.,Dtce.,Mars Fk-Uwk, 1 April 2011Nurfatin adilah kamarudinNoch keine Bewertungen
- The Flu: A Guide for Prevention and TreatmentVon EverandThe Flu: A Guide for Prevention and TreatmentBewertung: 5 von 5 Sternen5/5 (1)
- Hospital Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandHospital Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- 2009-10-16 Current Antiviral Recommendations For Influenza TreatmentDokument2 Seiten2009-10-16 Current Antiviral Recommendations For Influenza Treatmenttamiprior5294Noch keine Bewertungen
- MPH Comprreehensive Examination 2016 Recall Questions: RationaleDokument6 SeitenMPH Comprreehensive Examination 2016 Recall Questions: RationaleReg LagartejaNoch keine Bewertungen
- Cough, Hemoptysis, Dyspnea, WheezingDokument43 SeitenCough, Hemoptysis, Dyspnea, WheezingMelissa SalayogNoch keine Bewertungen
- 14-15 Peds Key Word Analysis NbomeDokument3 Seiten14-15 Peds Key Word Analysis NbomeChris Dubuque0% (1)
- q1121 PDFDokument8 Seitenq1121 PDFKijendran Chandra SekarNoch keine Bewertungen
- Id Resident TDDokument2 SeitenId Resident TDapi-534214500Noch keine Bewertungen
- Laboratory - Week 4 (Cytokines, in Vitro Phagocytosis)Dokument8 SeitenLaboratory - Week 4 (Cytokines, in Vitro Phagocytosis)rennel ybarolaNoch keine Bewertungen
- Tarlac National High SchoolDokument7 SeitenTarlac National High SchoolEzra SilvestreNoch keine Bewertungen
- USMLE Biostats GuideDokument45 SeitenUSMLE Biostats GuideMohammad ObaidullahNoch keine Bewertungen
- Gastroenteritis in ChildrenDokument4 SeitenGastroenteritis in ChildrenDennifer MadayagNoch keine Bewertungen
- Quick Review For OSCE, Medicine PDFDokument16 SeitenQuick Review For OSCE, Medicine PDFHengameh JavaheryNoch keine Bewertungen
- E-Newsletter - Bebelac Issue 003Dokument3 SeitenE-Newsletter - Bebelac Issue 003Anita LopokoiyitNoch keine Bewertungen
- UNICEF - 2010 - HandBook For Cold Chain ManagersDokument112 SeitenUNICEF - 2010 - HandBook For Cold Chain ManagersasmintehminaNoch keine Bewertungen
- Isolation Guidelines HealthDokument204 SeitenIsolation Guidelines HealthGrace Datu100% (1)
- Clemente V GsisDokument2 SeitenClemente V GsismischNoch keine Bewertungen
- EPI ManualDokument73 SeitenEPI ManualRich Arocena100% (1)
- Farhad Ullah Observation SheetDokument6 SeitenFarhad Ullah Observation SheetFarhad UllahNoch keine Bewertungen
- Microblot Array - 2023 - A4 - ANDokument28 SeitenMicroblot Array - 2023 - A4 - ANhazem alzed100% (1)
- Biology 9th Solving A Biological ProblemDokument5 SeitenBiology 9th Solving A Biological Problemmhussainshigri786Noch keine Bewertungen
- Autoimmune Hemolytic AnemiaDokument7 SeitenAutoimmune Hemolytic AnemiaHoopmen SilaenNoch keine Bewertungen
- Perinatal and Neonatal MortalityDokument40 SeitenPerinatal and Neonatal MortalityDuncan Jackson0% (1)
- Dengue Journal ReportDokument45 SeitenDengue Journal ReportNisvick Autriz BasulganNoch keine Bewertungen
- ScienceDokument1 SeiteScienceni putu.comsurya dianaNoch keine Bewertungen
- The Life Cycle of A Pandemic Crisis - Sars Impact On Air TravelDokument17 SeitenThe Life Cycle of A Pandemic Crisis - Sars Impact On Air TravelGabriel Charles Lim PkNoch keine Bewertungen
- Mexican Bed BugDokument10 SeitenMexican Bed BugPatrick Ross Serquiña DulayNoch keine Bewertungen
- Bodies in PathologyDokument2 SeitenBodies in PathologySreekanth KrishnamurthyNoch keine Bewertungen
- ImmunizationDokument50 SeitenImmunizationDiscover ANoch keine Bewertungen
- Pisa Science QuestionsDokument8 SeitenPisa Science QuestionsYuvi Ghaly100% (1)
- National Calendar For Vaccination: Doses Vaccine Child's AgeDokument1 SeiteNational Calendar For Vaccination: Doses Vaccine Child's AgeĐH ĐỊNH HƯỚNGNoch keine Bewertungen
- Session 1 Introduction To ParasitologyDokument33 SeitenSession 1 Introduction To Parasitologyannelle0219Noch keine Bewertungen