Beruflich Dokumente
Kultur Dokumente
The Pathology of Congestive Heart Failure
Hochgeladen von
Mar BleOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
The Pathology of Congestive Heart Failure
Hochgeladen von
Mar BleCopyright:
Verfügbare Formate
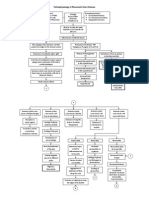
The Pathophysiology of Congestive Heart Failure
Legend: Manifested by JC Applied Intervention
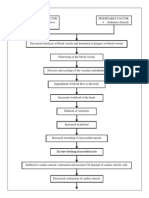
PREDISPOSING FACTORS Age (Over 65 years old) Sex (Both Sexes) Genetics
PRECIPATIONG FACTORS Hyperthyroidism Hypertension Diabetes Mellitus Dyslipidemia Obesity Cardiovascular Disease Myocardial Infarction Valvular Disease Arrhythmias
It decreases myocardial contractions and filling Myocardial Dysfunction
Systemic Heart Failure Decrease blood volume ejected from the ventricle Activation of Baroreceptors in the Aortic and Carotid Bodies
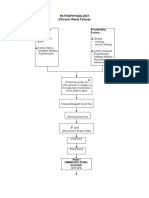
Diastolic Heart Failure
Develop as result of continuous decrease of heart workload
Ventricular Hyperthrophy and altered cellular functioning Resistance to Ventricular Filling
Sympathetic Nervous System Stimulated
Release of Epinephrine and nonEpinephrine Vasoconstriction of the Skin Vasoconstriction of Gastrointestinal Tract Vasoconstriction of the kidneys Activates Renin-angiotensinaldosterone system
Decrease ventricular filling pressures despite of a normal or reduced blood volume Less Blood in the Ventricle Low cardiac output Cause some neurohormonal response described in systolic heart failure
Renin
Angiotensin
Angiotensin converting Enzyme (Lungs) Angiotensin II
Stimulates release of Aldosterone from Adrenal Cortex
Sodium and fluid retention by the Renal Tubules Fluid Volume Overload Increase Stress on Ventricular wall
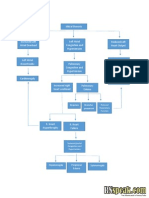
Increase Work Load of the Heart Release of counter regulatory mechanism through the release of Natriuretic Peptides (ANP) and (BNP) Heart workload Increase
Contraction of myocardial muscle fiber decreases Increase end-diastolic blood volume in the ventricle Ventricular Dilation Further increase in the stress in the ventricular wall Additional increase workload of the heart To compensate, it increases the thickness of heart muscles Ventricular Hypertrophy Proliferate abnormal myocardial cells
Ventricular Remodeling
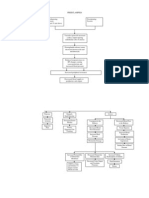
Clinical Manifestations
Left-sided Heart Failure
Right-sided Heart Failure
Increase left ventricular and diastolic blood volume
Cannot exert blood and cannot accommodate all the blood that normally returns to it from venous circulation
Increase blood flow from left atrium and left ventricle during diastole Increase blood volume and pressure on the left atrium Increase blood flow from the pulmonary vessels Congestion of the Peripheral Tissues and the Viscera Increase venous pressure
Jugular vein distention and increase hydrostatic pressure through venous system
Increase pulmonary venous blood volume and pressure
Pulmonary Congestion
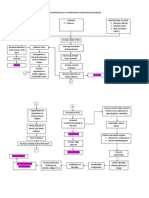
Signs and Symptoms: Dyspnea on Exertion Cough ( Dry non-productive) Pulmonary Crackles (Bibasilar) Decrease Oxygen Saturation S3 Gallop Auscultated Fatigue
Systemic Clinical Manifestations: Dependent Edema Hepatomegaly Ascites Anorexia Nausea Weight Gain
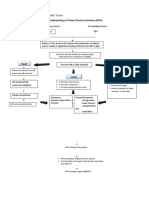
Without intervention Heart does not pump sufficient blood in the body Surgical Management: Coronary Bypass Surgery PTCA Innovative Therapies (e.g. mechanical assistive devices, Transplantation Nutritional Management Low Sodium Intake Fluid Restriction
With Intervention Early Assessment of Ventricular Functioning and Performing Diagnostic Procedures: Electrocardiogram Echocardiogram (Ejection Fraction) Exercise testing to detect CAD Laboratory Studies (Blood, Urea nitrogen, creatinine, CBC, thyroid stimulating hormone, urinalysis)
Stimulates the heart to work harder Heart cannot respond Heart failure worsen Bad Prognosis
Death
Medical Management: Ace Inhibitors (Lisinopril) (ARBs) Angiotensin II Receptor Beta Blockers (Carvedilol) Calcium Channel Blockers Diuretics (Lasix) Digitalis antihypertensive Anticoagulant (Warfarin) Antilypidemic ( Simvastatin)
Promotes vasodilation and diuresis
Reducing systemic vascular resistance
Reducing Afterload and Preload
Diminishing hearts work load Preventing exacerbation of heart failure
Good Prognosis
Das könnte Ihnen auch gefallen
- Pathophysiology of Congestive Heart Failure III With Pleural EffusionDokument3 SeitenPathophysiology of Congestive Heart Failure III With Pleural EffusionKen100% (1)
- Pathophysiology of Congestive Heart FailureDokument2 SeitenPathophysiology of Congestive Heart FailureAnonymous XvwKtnSrMR100% (10)
- Pathophysiology of CHFDokument1 SeitePathophysiology of CHFImae Mayo60% (5)
- Pathophysiology CHFDokument3 SeitenPathophysiology CHFKim Franzel M. Rabe100% (1)
- Pathophysiology Diagram of Congestive Heart FailureDokument3 SeitenPathophysiology Diagram of Congestive Heart Failurea_samiane64% (11)
- Pathophysiology of Heart FailureDokument4 SeitenPathophysiology of Heart FailureTiger Knee100% (2)
- Pathophysiology (Chronic Renal Failure)Dokument3 SeitenPathophysiology (Chronic Renal Failure)marshmalou86% (7)
- Coronary Artery Disease PathophysiologyDokument3 SeitenCoronary Artery Disease Pathophysiologynursing concept maps50% (4)
- Pathophysiology of Congestive Heart FailureDokument3 SeitenPathophysiology of Congestive Heart Failuretinayko100% (1)
- Congestive Heart Failure Schematic DiagramDokument1 SeiteCongestive Heart Failure Schematic DiagramCyrus De Asis100% (1)
- Congestive Heart FailureDokument8 SeitenCongestive Heart Failureiancel_038893% (27)
- Coronary Artery Disease PathophysiologyDokument3 SeitenCoronary Artery Disease PathophysiologyElmer Balgos Alinsog50% (4)
- Pathophysiology of Congestive Heart FailureDokument3 SeitenPathophysiology of Congestive Heart FailureMel Izhra N. MargateNoch keine Bewertungen
- Congestive Heart Failure Pathophysiology Schematic DiagramDokument3 SeitenCongestive Heart Failure Pathophysiology Schematic DiagramJacinthaVanathayahNoch keine Bewertungen
- Pathophysiology of Chronic Kidney Disease: Predisposing Factors: Precipitating FactorsDokument1 SeitePathophysiology of Chronic Kidney Disease: Predisposing Factors: Precipitating FactorsReina Samson0% (1)
- Pathophysiology of HCVD, DM2, CVD (Left Basal Ganglia)Dokument1 SeitePathophysiology of HCVD, DM2, CVD (Left Basal Ganglia)rexale ria100% (1)
- Pathophysiology CVA (Final2)Dokument10 SeitenPathophysiology CVA (Final2)Jayselle Costes FelipeNoch keine Bewertungen
- Pathophysiology of Congestive Heart Failure: Predisposing Factors Precipitating/Aggravating FactorsDokument1 SeitePathophysiology of Congestive Heart Failure: Predisposing Factors Precipitating/Aggravating Factorsguillermojerry100% (2)
- Case Study Congestive Heart Failure Patho)Dokument8 SeitenCase Study Congestive Heart Failure Patho)Mj Silva100% (3)
- Pathophysiology of CVADokument1 SeitePathophysiology of CVAChristine Joy Ilao PasnoNoch keine Bewertungen
- Pathophysiology - ESRDDokument5 SeitenPathophysiology - ESRDheiyu100% (3)
- Angina Pectoris PathophysiologyDokument2 SeitenAngina Pectoris Pathophysiologydana86% (7)
- Pathophysiology of Hypertensive Cardiovascular DiseaseDokument3 SeitenPathophysiology of Hypertensive Cardiovascular Diseasekhrizaleeh100% (10)
- Pathophysiology of Acute Renal FailureDokument2 SeitenPathophysiology of Acute Renal Failurekristel_nicole18yaho100% (3)
- Pathophysiology Hemorrhagic StrokeDokument1 SeitePathophysiology Hemorrhagic StrokeJeffrey Dela CruzNoch keine Bewertungen
- Case of A Patient Having Congestive Heart FailureDokument13 SeitenCase of A Patient Having Congestive Heart Failuresykie joy albina100% (1)
- C. Pathophysiology (Schematic Diagram) Predisposing Factors Precipitating FactorsDokument2 SeitenC. Pathophysiology (Schematic Diagram) Predisposing Factors Precipitating FactorsMarynette MapaNoch keine Bewertungen
- Pathophysiology of Rheumatic Heart DiseaseDokument3 SeitenPathophysiology of Rheumatic Heart DiseaseLouie Kem Anthony Babaran50% (8)
- Pathophysiology of Congestive Heart FailureDokument2 SeitenPathophysiology of Congestive Heart FailureTrixia Almendral100% (2)
- Pathophysiology CVADokument1 SeitePathophysiology CVANenette Aquino100% (2)
- Hypertension PathophysiologyDokument2 SeitenHypertension PathophysiologyJems60% (5)
- Stroke PathophysiologyDokument2 SeitenStroke PathophysiologyJaessa Feliciano100% (2)
- Pathophysiology of Patent Ductus Arteroisus (PDA)Dokument2 SeitenPathophysiology of Patent Ductus Arteroisus (PDA)Rodel Yacas100% (1)
- Pathophysiology of Heart FailureDokument1 SeitePathophysiology of Heart FailureabbeeyyNoch keine Bewertungen
- Myocardial Infarction: Nonmodifiable Factors: Modifiable FactorsDokument4 SeitenMyocardial Infarction: Nonmodifiable Factors: Modifiable FactorsHearty ArriolaNoch keine Bewertungen
- Pathophysiology of Cerebrovascular Disease: Predisposing Factors Etiology Precipitating FactorsDokument4 SeitenPathophysiology of Cerebrovascular Disease: Predisposing Factors Etiology Precipitating FactorsLilot Antonio Rodriguez Vinarao100% (5)
- HCVD Cad Cva InfarctionDokument2 SeitenHCVD Cad Cva InfarctionMiguel Carlos Tacderan100% (1)
- Pathophysiology of Acute Kidney InjuryDokument4 SeitenPathophysiology of Acute Kidney Injurymariaclaramutya100% (1)
- Pathophysiology of HCVDDokument5 SeitenPathophysiology of HCVDNicolne Lorraine100% (1)
- Acs Nstemi Vs Ua - PathoDokument2 SeitenAcs Nstemi Vs Ua - PathoJerom YamatNoch keine Bewertungen
- PathophysiologyDokument4 SeitenPathophysiologyCee SanchezNoch keine Bewertungen
- Case Study-Congestive Heart FailureDokument71 SeitenCase Study-Congestive Heart FailureKentTangcalagan92% (13)
- Heart FaliureDokument59 SeitenHeart FaliureMahesh RathnayakeNoch keine Bewertungen
- Heart FailureDokument39 SeitenHeart FailureMuhammad AsifNoch keine Bewertungen
- Congestive Cardiac FailureDokument38 SeitenCongestive Cardiac FailureSalman KhanNoch keine Bewertungen
- Effects of Cardiac Problems On Individuals Functions of The Cardiac SystemDokument9 SeitenEffects of Cardiac Problems On Individuals Functions of The Cardiac SystemJulie Nix FrazierNoch keine Bewertungen
- Shock: Ibrahim Ali & Winfred C. ParnellDokument30 SeitenShock: Ibrahim Ali & Winfred C. ParnellsgolbariNoch keine Bewertungen
- Circulation: Ms. Jonalyn P. SantosDokument18 SeitenCirculation: Ms. Jonalyn P. SantosHoward John M. RamiterreNoch keine Bewertungen
- Assessment of The Cardiovascular SystemDokument48 SeitenAssessment of The Cardiovascular Systemkimberlyrwarren8817Noch keine Bewertungen
- ShockDokument34 SeitenShockeman shNoch keine Bewertungen
- Heart FailureDokument10 SeitenHeart Failureurmila prajapatiNoch keine Bewertungen
- Right Sided Heart FailureDokument33 SeitenRight Sided Heart FailurePaulNoch keine Bewertungen
- CHFSP 2005Dokument36 SeitenCHFSP 2005Andy F MonroeNoch keine Bewertungen
- GewaldDokument2 SeitenGewaldGerald Sevilla CascoNoch keine Bewertungen
- Bimbingan Dokter Muda Heart FailureDokument57 SeitenBimbingan Dokter Muda Heart FailurerachmaniabudiatiNoch keine Bewertungen
- Shock: Shock Can Refer To A Range of Related Medical Conditions in Which The Victim's Heart, Lungs andDokument16 SeitenShock: Shock Can Refer To A Range of Related Medical Conditions in Which The Victim's Heart, Lungs andLucreatia RynjahNoch keine Bewertungen
- Dr. Az Rifki, Span - Kic Departemen Anestesiologi Dan Reanimasi Rsi Siti Rahmah/Fk-Fkg Universitas Baiturrahmah PadangDokument62 SeitenDr. Az Rifki, Span - Kic Departemen Anestesiologi Dan Reanimasi Rsi Siti Rahmah/Fk-Fkg Universitas Baiturrahmah PadangKamelia MarcshendaNoch keine Bewertungen
- CHF Left SidedDokument21 SeitenCHF Left SidedSandie Daniel GabalunosNoch keine Bewertungen
- Cardiogenic ShockDokument29 SeitenCardiogenic ShockagnescheruseryNoch keine Bewertungen
- Multi-Organ Dysfunction Syndrome Lesson Description - Mitch TaylorDokument34 SeitenMulti-Organ Dysfunction Syndrome Lesson Description - Mitch TaylorMuthu RajathiNoch keine Bewertungen
- Annex A-Flowchart of ProceduresDokument1 SeiteAnnex A-Flowchart of ProceduresMar BleNoch keine Bewertungen
- Set A: Nursing Practice BDokument9 SeitenSet A: Nursing Practice BMar BleNoch keine Bewertungen
- Set A: Nursing Practice 3CDokument9 SeitenSet A: Nursing Practice 3CMar BleNoch keine Bewertungen
- 100 Item Exam On Fundamentals of NursingDokument14 Seiten100 Item Exam On Fundamentals of NursingMar Ble100% (1)
- Nursing Practice I Set ADokument60 SeitenNursing Practice I Set AMar BleNoch keine Bewertungen
- 100 Item Exam On Fundamentals of Nursing KeysDokument14 Seiten100 Item Exam On Fundamentals of Nursing KeysMar BleNoch keine Bewertungen
- Nursing Thesis ExampleDokument10 SeitenNursing Thesis ExampleLyka Milo AvilaNoch keine Bewertungen
- Answer NCP 5Dokument9 SeitenAnswer NCP 5Mar Ble100% (1)
- Answer NCP 2Dokument9 SeitenAnswer NCP 2Mar BleNoch keine Bewertungen
- Answer NCP 1Dokument8 SeitenAnswer NCP 1Mar BleNoch keine Bewertungen
- Super FerryDokument1 SeiteSuper FerryMar BleNoch keine Bewertungen
- DVT NotesDokument3 SeitenDVT NotesTodd EvansNoch keine Bewertungen
- Genetic Factors Associated With Periodontal DiseasesDokument50 SeitenGenetic Factors Associated With Periodontal DiseasesDrKrishna DasNoch keine Bewertungen
- Studiu EumastosDokument8 SeitenStudiu EumastosIoana VztNoch keine Bewertungen
- Fur TierDokument22 SeitenFur Tierhodijat2009Noch keine Bewertungen
- Chronic Venous InsufficiencyDokument42 SeitenChronic Venous InsufficiencyMeor FahmiNoch keine Bewertungen
- Sem Osteoporosis (Edit)Dokument31 SeitenSem Osteoporosis (Edit)Rhomizal MazaliNoch keine Bewertungen
- Icterus NeonatarumDokument64 SeitenIcterus NeonatarumDeepti KukretiNoch keine Bewertungen
- Science - 2010 01 15Dokument147 SeitenScience - 2010 01 15Mi LaNoch keine Bewertungen
- Osmosis Endocrine, Pathology - Tumors - Endocrine Tumors PDFDokument7 SeitenOsmosis Endocrine, Pathology - Tumors - Endocrine Tumors PDFYusril Marhaen0% (1)
- My Assignment On NeurotransmitterDokument8 SeitenMy Assignment On NeurotransmitterSiti Fairuz HassanNoch keine Bewertungen
- IFA Sports Nutrition Certification Test Answer Form: Tester: Date: NameDokument8 SeitenIFA Sports Nutrition Certification Test Answer Form: Tester: Date: NameSimbarashe MabambeNoch keine Bewertungen
- ANP 202 Principles of Animal Production PDFDokument207 SeitenANP 202 Principles of Animal Production PDFBELKYSNoch keine Bewertungen
- 200 Important Points of General Pathology by DR Ejaz Waris-1Dokument14 Seiten200 Important Points of General Pathology by DR Ejaz Waris-1Arslan AhmedNoch keine Bewertungen
- Vectors For Gene DeliveryDokument6 SeitenVectors For Gene DeliveryMuhammad Ikram RabbaniNoch keine Bewertungen
- Biokemistri Volume 32, Number 2Dokument75 SeitenBiokemistri Volume 32, Number 2Clement BewajiNoch keine Bewertungen
- What Causes Cancer by Webster KehrDokument6 SeitenWhat Causes Cancer by Webster Kehrhhelp12255Noch keine Bewertungen
- A Sonographic Approach To The Prenatal Diagnosis of Skeletal DysplasiasDokument19 SeitenA Sonographic Approach To The Prenatal Diagnosis of Skeletal DysplasiasminhhaiNoch keine Bewertungen
- Abbas Basic Immunology 3eDokument7 SeitenAbbas Basic Immunology 3evudka100% (1)
- Environmental Health SciencesDokument2 SeitenEnvironmental Health SciencesindraandikapNoch keine Bewertungen
- GmosDokument5 SeitenGmosapi-297206777100% (1)
- Reproduction Pathology ReviewDokument9 SeitenReproduction Pathology ReviewkishorechandraNoch keine Bewertungen
- Immunity Mark SchemeDokument6 SeitenImmunity Mark SchemeDNoch keine Bewertungen
- Enzyme EngineeringDokument33 SeitenEnzyme EngineeringMoses DesaiNoch keine Bewertungen
- Indole 3 CarbinolDokument2 SeitenIndole 3 CarbinolEnrico S. RosalesNoch keine Bewertungen
- KianDokument4 SeitenKianMisha KhorramshahiNoch keine Bewertungen
- Lec 7proteus SPPDokument22 SeitenLec 7proteus SPPbujalkanNoch keine Bewertungen
- Released Items: Biology 30Dokument49 SeitenReleased Items: Biology 30zahwa ciprutNoch keine Bewertungen
- Protein Synthesis Notes and DiagramDokument34 SeitenProtein Synthesis Notes and Diagramapi-267117865100% (1)
- Darre Poultry Biology 2019Dokument20 SeitenDarre Poultry Biology 2019Saidatul Nur KholifahNoch keine Bewertungen
- 2022 Book TheEBMTEHACAR-TCellHandbookDokument221 Seiten2022 Book TheEBMTEHACAR-TCellHandbookInchirah Narimane MgdNoch keine Bewertungen