Beruflich Dokumente
Kultur Dokumente
Pathology Exam II Study Guide
Hochgeladen von
epsilon21210 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
122 Ansichten12 SeitenStudy Guide For General Pathology: Congenital Diseases, Immunologic Diseases, and Vitamin Deficiencies and Toxicity
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenStudy Guide For General Pathology: Congenital Diseases, Immunologic Diseases, and Vitamin Deficiencies and Toxicity
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
122 Ansichten12 SeitenPathology Exam II Study Guide
Hochgeladen von
epsilon2121Study Guide For General Pathology: Congenital Diseases, Immunologic Diseases, and Vitamin Deficiencies and Toxicity
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 12
Pathology Exam II Study Guide
Genetic and Congenital Disorders
4 Main Stages in Prenatal Development: Pre-implantation, Germ Layer
Formation, Early Organogenesis, Definite Organogenesis
Genetic Diseases = 20% of causes of all congenital Diseases, 75% unknown
Exogenous Teratogens:
Physical: X-rays, Radiation, Chemical: Drugs, Alcohol Microbial: Viruses, Bacteria
Thalidomide = flipper arms
Fetal Alcohol Syndrome (FAS): Small Size, Small Eye openings, Poor Coordination,
Hyperactive, Mental Retardation, poor reasoning and judgment skills
T: Toxoplasma Ca
2+
of basal gang. & dilation of lat. Ventricles (hydrocephalus)
O: Others
R: Rubella microcephaly, Heart defects
C: Cytomegalovirus (CMV)
H: Herpes virus CNS Defects, Skin Lesion
ES: Syphilis
Aneuploidy Loss or Gain of Chromosomes
TRISOMIES
Downs Syndrome Trisomy 21 HD (septum primum), intestinal defects,
abnormal hands and toes MOST COMMON Life Expectancy = 45 - 50
Edwards Syndrome Trisomy 18 HD, micrognathia, low-set ears,
clenched hands, Life Expectacncy = <1 Year
Patau Syndrome Trisomy 13 HD, Microopthalmia, microcephaly, cleft
lip/palate, Polydactyl Life Expectancy = <1 year
SEX CHROMOSOME ABNORMALITIES
Turner Syndrome XO - think Tina Turner HD, short stature, heart
shaped face, low posterior hairline,
Klinefelter Syndrome XXY - tall, long arms and legs, lack of beard, body
hair, and pubic hair, gynecomastia, infertile
AUTOSOMAL DOMINANT DISEASES
CONNECTIVE TISSUE AND BONES
Marfans Syndrome think MARTIAN, Mutation in glycoprotein fribrillin-1
(FBN) gene Connective tissue anomalies, elongated head, arachnodactyly,
kyphoscoliosis, pectus excavatum, and genu recurvatum, heart defects
aortic incompetence and dissecting aortic aneurysms, floppy mitral valve,
SUBLUXATION OF LENSES (Dislocated),
Achondroplastic Dwarfism Mutation: Fibroblast GrthFctr (FGF) r/c 3
Short limbed dwarfism, bulky forehead, Lumbar lordosis
Osteogenesis Imperfecta Collagen disorder Fragile bones
4 TYPES I & IV autosomal dominant; II & III autosomal recessive
TYPE I AD - mildest form, blue sclerae, musculoskeletal pain to jts.
TYPE II AR Neonatal form, MOST LETHAL, blue sclerae, skull is soft
TYPE III AR MOST SEVERE non-lethal, short stature, recurrent fractures
TYPE IV AD intermed. severity, bones fragile @ Childhood, no blue sclerae
Blue Sclerae characteristic of heritable disorders of connective tissue
CARDIOVASCULAR SYSTEM
Familial Hypercholesterolemia Hyperlipidemia type IIA, Elevated LDL
owing to defective or absent LDL r/c, Chol: Heterozygote = 300, Homozygote
= 700, severe atherosclerotic disease early in life. r/c mutations are 1/5
heterogeneous classes: Synthesis, Transport, Binding, Clustering, and
Recycling TREATMENT: Nicotinic Acid, High Dietary Fiber, Statin Drugs
KIDNEY
Polycystic Kidney Disease (PKD) Mutation of PKD1 gene in chrom 16
Represents 5-10% of end-stage renal failure pat., recessive = rare and causes
Renal failure during childhood Berry Aneurisms. By Age 75: 50 75% req.
renal transplant or dialysis. TRMT: BP control, protein intake restriction
ALWAYS BILATERAL!!!!
HEMATOPOIETIC SYSTEM
Spherocytosis RBC membrane disorder, anemia, jaundice, splenomegaly,
RBC osmotic fragility, negative direct antiglobulin test. Cell membrane
surface area decreased disproportionately to the intracellular content
Intrasplenic hemolysis. TRMT = Splenectomy
Coombs test distinguishes btwn (-)HS and (+)AIHA
NERVOUS SYSTEM
Huntingtons Disease Gene mutation on Chrom 4 CAG sequence =
repeats of Glutamine = huntingin. Signs: Chorea and Progressive cognitive
deterioration. Effects both sexes equally. Caudate Nuc. Atrophies, medium
spiny neurons in corpus striatum degenerate. Neurotransmitters GABA and
Sub. P decrease. Death 13 to 15 yrs post symptoms. The more CAG repeats
there are, the earlier the symptoms start. Death preceeded by dementia
coupled with abnormal movements(monoclinic jerks, etc.)
TRINUCLEOTIDE REPEAT EXPANSION DISEASES
Huntington disease
Myotonic dystrophy
Friedreichs ataxia
Fragile X syndrome
Genetic Anticipation = in each successive generation the disease severity increases
and age of onset decreases
AUTOSOMAL RECESSIVE DISORDERS
25% of offspring from 2 carrier parents are affected
Can be due to enzyme deficiency
Usually seen in only one generation
Commonly more severe than dominant disorders
Cystic Fibrosis Most common lethal genetic disease of Caucasians , defect
in CFTR Gene on Chrom 7 (Deletion of Phe 508), CFTR channel secretes and
resorbs cl
-
, infertility among males (no vas deferens), fat-soluble vitamin
deficiencies (A,D,E,K). Cl
-
channel secretions are thick mucus plugs lungs,
pancreas and liver. Recurrent pulmonary infections.
Sickle Cell Anemia In Hb S, Valine is substituted for glutamic acid in the 6
th
amino acid of the chain(Point Mutation). This substitution causes Hb to be
less soluble when oxygenated, forming a gel, which causes the RBC
deformity. This deformity causes inflexibility causing the RBCs to adhere to
vascular BV infarction. Chronic compensatory marrow hyperactivity
deforms the bones. RBCs appear faint on microscope due to hypochromium
Lysosomal Storage Diseases
1.) Sphingolipidoses
Fabrys Disease - XR
Gauchers Disease - AR
Niemann-Pick Disease - AR
Tay-Sachs Disease - AR
Krabbes Disease -AR
Metachromatic Leukodystrophy AR
2.) Mucopolysaccharidoses
Hurlers syndrome - AR
Hunters Syndrome XR
Tay Sachs Disease Swollen and Vacuolated neural system d/t Inc. of lipid
rich lysosomes. Four-base insertion in the hexosaminidase A gene =
Frameshift mutation. Common among Jews.
Niemann-Pick Disease Hepatocytes and Kupffer cells both foamy and
vacuolated, lipid deposits
Phenylketonuria (PKU) most common among caucasians. Excess dietary
phenylalanine is no longer converted to tyrosine by phenylalanine
hydroxylase. Loss of enzyme creates phenylalanine accumulation, BRAIN is
mainly affected. Some of phenylalanine is metabolized to phenylketones
which are secreted in urine Phenylketonuria.
--PhenylalanineTyrosineDopaDopamineNEEpi
Clincal symptoms is mental retardation, fair skin, eczema, and musty BO
Diagnosis by high phenylalanine or low tyrosine
Phenylketones = phenylacetate, phenyllactate, and phenylpyruvate
DISORDER OF AROMATIC AMINO ACID
Glycogen Storage Diseases
Type I Von Gierkes Disease fasting hypoglycemia, inc. glycogen in liver,
inc. blood lactate, hepatomegaly
Type II Pompes Disease Cardiomegaly and systemic findings leading to
early death (heart, liver, and muscle)
Type III Coris Disease Milder form of Type I, no lactate issues
Type V McArdle Disease Inc. Glycogen in muscle, but cannot break it
down, leading to muscle cramps, myoglobinuria with strenuous
exercise.
X-LINKED RECESSIVE DISORDERS
Sons of heterozygous mothers have 50% chance of being affected
No male to male transmission
Brutons agammaglobulinemia (Congenital Immunodeficiency)
Wiskott-Alderich syndrome
Immunodeficiency (X-SCID)
Fragile X
Lymphoproliferative disorders (Duncans Syndrome)
G6PD Deficiency
Ocular albinism
Lesch-Nyhan Syndrome
Dystrophies
-Duchennes Muscular dystrophy
-Beckers Muscular Dystrophy
Hemophilia A and B
Fabrys Disease
Hunters Syndrome
Be Wise, FooLs GOLD Heeds False Hope
Fragile X Syndrome Defect affecting methylation and expression of FMR1
gene. 2
nd
most common cause of mental retardation to down syndrome.
Mostly males. Fragility of X-Chromosome.
Glucose-6-phosphate dehydrogenase deficiency Prevalent in blacks.
Malarial resistance. Since G6PD is rate limiting in HMP rxn dec.
NADPHmore oxidized glutathione more free radicalshemolytic
anemia. Heinz bodies: altered hemoglobin precipitates w/in RBCs.
Bite cells result from the phagocytic removal of Heinz bodies.
SCID - Bubble boy Both B cell and T cell divisions of the adaptive immune
system are non functional due to one of several gene defects. X-SCID = most
common, Adenosine deaminase deficiency 2
nd
most common. Defective gene
for IL2 r/c (IL2RG) promotes lymphocyte growth and differentiation.
Candidiasis: fungal infection, skin, mouth etc.
Lesch-Nyhan Syndrome Purine salvage deficiency, due to absent HGPRT,
which converts hypoxanthine to IMP and Guanine to GMP excess uric acid
prod. Findings = metnal retardation, self-mutilation, aggression,
hyperuricemia.
Adenosine deaminase deficiency NOT X-Linked SCID form Excess ATP
and dATP imbalances nucleotide pool via feedback inhibition of
ribonucleotide reductaseprevents DNA Synth. dec. lymphocyte count
Duchennes (DMD) and Beckers (BMD) Muscular deficiency Result
from mutation on dystrophin gene, DMD has no functional dystrophin at all
therefore a more sever version of MD. Low dystrophin = instable structure of
muscle cell membrane and accelerates breakdown
MUTIFACTORAL INHERITANCE
Diabetes Type 2 (NIDDM) 50% of affected persons have relatives who
also have diabetes. High incidence w/ high rate of intermarriage, and
monozygotic twins.
X-LINKED DOMINANT:
Transmitted through both parents. Either male or female of affected mother
may be affected, while ALL FEMALE offspring of affected FATHER are
diseased. E.G.: Factor VIII and Factor IX (Hemophilia A or B)
PRENATAL DIAGNOSIS:
Causes of prematurity Etoh, smoking, congenital abnormalities, location
of placenta and viability
Neonatal Respiratory Distress Syndrome Surfactant deficiency due to
immature type II pneumocyte. Atelectasis, alveolar and endothelial injury of
lungs. Hypoxia - hyaline membranes around alveoli. Complications: Cerebral
intraventricular hemorrhage, hemorrhagic intestinal necrosis
Birth injury Mechanical trauma, skull fractures intracranial hemorrhage,
peripheral nerve damage and fracture of long bones of extremities.
SIDS Cause not known, Maternal, infant/fetal risk factors, most common
cause of death in infants beyond the immediate neonatal period.
DISORDERS OF THE IMMUNE SYSTEM
Immunity: -exemption from duty - persons with immunity exempt from the
suffering inflicted by infectious disease
Immune Response forms:
Natural Immunity defense mechs protective proteins: complement,
properdin plasma proteins activates alt compl. p/way, lysozyme low
molecular weight proteins aka tears, nasal secretions / intestinal secretions
Acquired Immunity concept of self vs. non-self, Immunocompetence
ability to mount a response
Lines of Defense:
1
st
:Mechanical Barriers, Chemical Barriers
2
nd
:Inflammatory Response, Phagocytosis
3
rd
:Specific immune response
Cells of the Immune system Lymphocytes: T-Lymphoctyes (T Helper (CD4+), T
Supressor/cytotoxic (CD8+), Natural Killer (NK)), B Lymphocytes, Plasma
cells, Macrophages. T,B, and NK Cells all have lymphoid cell lineage. BM cells
premyeloid & Lymphocytic
Basophil Mast Cell, Monocyte Macrophage, B Lymphocyte Plasma Cells
B-Lymphocyte cytoplasm is scant and contains few organelles
Plasma cell well developed cytoplasm w/ RERprod. of Igs
ANTIBODIES five classes
Basic Structure light (always &) and heavy chains (variable, specific to
each Ig), Disulfide bond = cysteine
IgM Largest Ig, Fx. Neutralize microorganisms, avid complement activator
has 5 complement binding sites. 1
st
to appear on initial immune response,
natural ab against ABO blood group ag
IgG smallest Mw, most copious, few at 1
st
ramps up, amts boosted on
re-exposure to antigen. Fc r/cs on: Macrophages, PMNs, Lymphocytes,
Eosinophils, and Placenta, acts as opsonin, only one to pass placenta
IgA Mainly mucosal secretions (tears, nasal, breast milk, int. trct)
Fx. Protective Ig
IgE Secreted by sensitized plasma cells in tissue, locally attached to mast
cells. Fx. Mediates allergic rxns in tissues, also protects against parasites
IgD Cell membrane-bound Ig found only on B Cells. Fx. Participates in
antigenic activation of B cells, not released into serum of body fluids
Major Histocompatibility Complex (MHC) Essential for presentation of antigens
to T-Cells, human leukocyte antigen, immunologic finger print. Responsible
for transplant rejections, typically on macrophages, T-Cells can ONLY react
with membrane-bound antigen no APCno T cell rxn
MHC Type I found on ALL nucleated cells of the body, r/cs for CD8 (T
suppressor and/or cytotoxic T lymphocytes)
MHC Type II r/cs for CD4 (Helper T), serve for presentation of exogenous
antigens that are 1
st
internalized and processed
HLA Subtypes
A3 Hemochromatosis, Myasthenia gravis, multiple sclerosis
B27- Psoriasis, Ankylosing spondylitis, IBS, Reiters Syndrome
B8- Graves Disease, celiac sprue
DR2- MS, Hay fever, SLE, Goodpatures
DR3- DM1
DR4- RA, DM1
DR5- Pernicious anemia B-12 Deficiency, Hashimotos Thyroiditis
DR7- Steroid-responsive nephrotic syndrome
Antigen-Antibody Reaction
Epitope antigenic site, can be many on antigen
Antibodies to soluble antigen form soluble complexes that may be found
in circulation
Antibodies bound to fixed antigen on cell coat the cell surface
Antigen-antibody complexes bind and activate complement (which is the
effector system) lysis of cells, agglutination, or inflammation
Hypersensitivity Reactions
Type I Hypersensitivity ANAPHYLACTIC IgE
Mediated by IgE and mast cells or basophils
Late-phase response = 4-6hrs later SRS-As
Hayfever Allergic rhinitis, seasonal, d/t foreign sub., Tx: antihistamines,
Vit. C, Desensitization
Asthma Rxn @ bronchi, d/t inhaled antigens, mediated by SRS-As, S/SX =
constriction of bronchi and overproduction of mucus. Mg relaxes airway
Atopic Dermatitis eczema, 50% of people have fam hist., allergen inhaled,
ingested, or direct contact w/ skin. the itch that blisters
Anaphylactic Shock Severe systemic response to allergen, body has been
previously sensitized (prior exposure), MASSIVE release of HISTAMINE,
S/SX: Choking 2
o
to laryngeal edema, wheezing and SOB 2
o
to bronchial
spasm. TX = Epinephrine STAT, high flow O
2
Type II Hypersensitivity CYTOTOXIC ANTIBODY MEDIATED IgG or IgM
Cytotoxic ab reacts to ag in cells or tissue components
Antigen can be intrinsic or extrinsic autoimmune diseases
Binding is ab to ag on cell surf Activation of compliment cell lysis
Antibody Dependent Cellular Cytotoxic (ADCC) rxn involves effector killer
cell, which destroy target cell coated with ab
Hemolytic anemia Several forms Systemic autoimmune disorder
(systemic lupus erthyematosus(SLE)) or Foreign Chemicals (drug rxn,
attachment to RBC as haptens, triggers hemolysis)
Goodpasture Syndrome Autoimmunity to component of collagen type IV
that has become autoallergenic. S/SX: Hemoptysis, Hematuria, Dyspnea,
cough, fatigue, fever, weight loss are common
Graves Disease Caused by autoantibody against the thyroid r/c for TSH
causes continuous secretion of T4 and T3. Infiltrative opthalmopathy
(exophthalmos) d/t inflammation orbital fibroblasts and accumulation of
glycosaminoglycans. Goiter also a sign
Myasthenia Gravis Episodic muscle weakness and easy fatigue d/t
autoantibody and cell mediated destruction of Ach r/cs. S/Sx: ptosis,
diplopia, and m. weakness after use of affected m. Dx: Via ab test for Ach r/c
Ocular mm. initially only affected in 40% of people, eventually 85%.
Milkmaids grip. Prox. Limb weakness, sensation and DTR OK.
Type III Hypersensitivity IMMUNE COMPLEX MEDIATED
Rxns cause acute inflammation in response to circulating ag-ab
complexes deposited in vessels or tissue
The complexes activate complement systemrelease of inflammatory
mediators.
Relative to [ag-ab] complexes
Can cause systemic inflammation
Poststreptococcal Glomerulonephritis Typically follows upper
respiratory tract infection by a nephritogenic streptococcal strain. Ag
planted onto GBM during filtration from plasma. Complement inflammation
evoked.
Arthus Reaction Reaction that occurs after multiple injections of foreign
serum, shows edema at 1
st
and then serum is absorbed, further injections led
to gangrene. Involves the deposition of antigen/antibody complexes mainly
in the vascular walls, serosa and glomeruli. These types of reactions can
occur post tetanus toxoid and diphtheria toxoid containing vaccines.
Polyarteritis Nodosa unknown ag, chronic HBV, Early stages = focal
fibrinoid necrosis and acute inflammation, Chronic Stages = Wall destruction,
microaneurysms, thrombosis, occlusion/infarct. Fibrous nodules along the
medium-sized arteries that are affected
SLE Glomerulonephritis deposition of complement-activation immune
complexes IgG
Type IV Hypersensitivity - CELL MEDIATED _ DELAYED TYPE
T cell-mediated
These cells are sensitized after contact with a specific antigen
Activated by re-exposure to the antigen
They damage via direct toxic effects or through release of cytokines
activate eosinophils, monocytes, and macrophages, neutrophils, and NK
Caseating Granuloma Epithelioid macrophages, Giant cells and
lymphocytes form barrier around antigen
Most common type IV rxn is contact dermatitis
Type 1 DM theorized as a virally triggered autoimmune response, infected
cells attacked + beta cells. Virtually no surviving insulin producing cells.
Transplantation Autograft = self, Isograft or syngenic graft = identical
twin or clone, Homograft/allograft = within species, Xenograft = pig heart
valve
Transplant Rejection Hyperacute rxn = during op, wrong blood type
Acute rxn = usually w/in 1
st
few weeks, Chronic transplant rejection = month
to years, obliteration of arterial lumen (endarteritis)
Types of Transplants: Kidney, liver, heart, lung, skin, pancreas, BM
Graft vs. Host Reaction Mediated by T lymphocytes, most often a
complication of bone marrow transplant. Organs most affected = skin
(dermatitis), intestine (malabsorption and liver (laundice)
Blood Transfusion when anti A or B hemagglutinins bind with
respective anti A or B antibody coagulation
Gives to Gets From
A A, AB A, O
B B, AB B, O
AB AB A, B, AB, O
O A,B,AB,O O
Rh Factor Incompatibility 1
st
Pregnancy: (Rh-) mom + (Rh+) Baby = OK
2
nd
Pregnancy: (Rh-) mom + (Rh+) Baby = moms immune system attacks
baby via (anti-Rh) mom was sensitized to (Rh+) fetus, DAD is (Rh+)
Clinical features: Hydrops Fetalis, Erthroblastosis Fetalis, and Icterus gravis
neonatorum aka Kernicterus, jaundice of basil ganglia (all of these have the
same mech.
Autoimmune Diseases
abnormal response to self antigens
look for Autoantibodies, hypersensitivities, disease is of immune nature
(aka steroids help)
Incidence based on genetic predisposition, HLA-haplotypes, sex
differences, more common in women
Systemic Lupus Erythematosus (SLE) All SLE patients have ANA, 75%
have KD involvement, Butterfly rash
Rheumatic Fever Group A Streptococcus (GAS) infection is etiological
precursor of Acute Rheumatic Fever (ARF), ARF occurs b/t 5 and 15 y/o and
is uncommon b/t 3 and 21 y/o. GAS M proteins share epitope with proteins
found in synovium, heart m. and heart valve mimicry contributes to
symptoms. Bad living condition inc. contraction rate. Skin, heart, joints and
CNS most commonly affected with this disease.
Rheumatoid Arthritis Usually in peripheral jts. SYMMETRICALLY
Inflamed destruction of articular surfaces, accompanied by systemic
symptoms. Women affected 2 to 3 times more than men. Age 35 50. I
mmune complexes produced by synovial lining and inflamed BVs. Plasma
cells produce ab (RF) that contribute to these complexes. Invaders of
synovial tissue = CD4+ T Cells. Affected people start the morning stiff,
afternoon = onset of other symptoms (fatigue, anorexia) Tx = alkaline diet or
rustox
Immunodeficiency Diseases
1
o
Immunodeficiency Diseases = Congenital
1.) Severe combined immunodeficiency - defect of lymphoid stem cells
preB , Pre-T cells
2.) Isolated deficiency of IgA The most common 1:700, often asymptomatic
3.) DiGeorges Syndrome T- Cell deficiency related to aplasia of thymus,
assoc. w/ aplasia of parathyroid glands
2
o
Immunodeficiency Diseases = Acquired
AIDS RNA retrovirus infects T Helper Cells CD4+, stored in macrophages
and related phagocytic cells. Shows itself via acute illness,
asymptomatic infection, persistent generalized lymphadenopathy
Opportunistic infections common: Lung (pneumonias), CNS
(Toxoplasma gondii). Tumors: Lymphoma of lymph nodes, GI tract,
CNS, Kaposis Sarcoma
Basic properties of Immune Deficiencies
1.) Decrease production of:
B cells Brutons agammaglobulinemia X-Linked Recessive
defect in tyrosine kinase gene assoc. w/ low levels of all classes of
immunoglobulins. Dec # of B cells d/t bacterial infections after 6
months old when mom [IgG] dec. occurs in Boys
T-Cells - Thymic aplasia (DeGeorges Syndrome) Presents with
tetany owing to hypcalcemia, recurrent viral and bacterial infections
due to T-Cell deficiency
2.) Decrease Activation of:
T-Cells IL2 r/c Deficiency
B-Cells Hyper-IgM syndrome - Defect on CD4 T Cells, inability to
class switch
B-Cells - Wiskott-Alderich Syndrome cant mount IgM response to
capsular polysaccharides of bacteria inc IgA, Triad of symptoms =
Infections, Pupura and Eczema
Macrophages Jobs Syndrome - Failure of IFN-gamma production
3.) Phagocytic Cell Deficiency:
Leukoctye adhesion deficiency syndrome defect in LFA-1
Integrin Proteins on phagocytes dec. pus formation
Chediak-Higashi Disease Defect in microtubular fx, and lysosomal
emptying of phagocytic cells
Chronic Granulomatous disease defect in phagocytosis of
neutrophils owing to a lack of NADPH oxidase activity
4.) Idiopathic Dysfunction of:
T Cells Chronic mucocutaneous Candidiasis
B Cells Selective Immunoglobulin Deficiency defect in isotope
switching
B Cells Ataxia Telangiectasia defect in DNA repair, assoc IgA def.
B Cells Common Variable Immunodeficiency dec. plasma cells,
defects in b-cell maturation
Amyloid Inert extracellular material, biochemically can be AA amyloid, AL
Amyloid and many other forms, Derived from serum Amyloid A (SAA),
Systemic amyloidosis caused by deposition of AA or AL amyloid in various organs.
Can be localized, Alzheimers for example in the brain.
VITAMINS
Fat Soluble Vitamins = ADEK
Absorption dependent on gut and pancreas, toxicity here is more common
due to their fat accumulating nature. Malabsorption issues can cause havoc
here when they mess with the fat content. Steatorrhea
Water Soluble Vitamin = Vit C, the Bs, Folate, ; all wash out easily from body
except B12 and folate as they are stored in the liver
Vitamin A Retinol aids in formation of rhodopsin, integrity of epithelia,
lysosomal stability, glocoprotein synth. DEFICIENCY = NIGHT BLINDNESS,
dry skin, perifollicular hyperkeratosis, xerophthalmia, keratomalacia, inc.
morbidity and mortality in kids. TOXICITY: Headache, Fatigue, skin changes,
peeling, sore throat, alopecia
FOUND IN: Fish oil, liver, egg yolks, butter
Vitamin D Cholecalciferol = D3, ergocalciferol = D2 Sources = Direct uv B
Irradiation of the skin(D3), fortified dairy products D2 (main source), Fish
liver oils, fatty fish, liver. FX: Ca and P absorption, mineralization and bone
repair, insulin and thyroid fx, improves immune system. Deficiency =
RICKETS Toxicity = Hypercalcemia, anorexia, renal failure, metastic
calcifications. Excess seen in Sarcoidosis
Vitamin E Group alpha-tocopherol, and other tocopherols and tocotrienols
Source = Veg. oils, nuts and legumes, Fx= intracellular antioxidant, scavenger
of free radicals in membranes. DEFICIENCY = RBC Hemolysis, neurologic
defects. Toxicity = tendency to bleed
Vitamin K Group Phylloquinone, menaquinone
Source = Green leafy veg., soy beans, veg. oils, bact. In GI Tract post Neonatal
period
Fx = Formation of prothrombin, other coagulants and bone proteins
Deficiency = bleeding due to deficiency of prothrombin etc., can occur after a
long duration of broad spectrum antibiotics. Kids givin vit K at birth since
gut cannot produce it.
Vitamin B1 Thiamin
Fx: carb, fat, aa, glucose and etoh metabolism
Deficiency = Dry Beriberi Polyneuritis, symmetrical m. wasting
Wet Beriberi High Output cardiac failure, edema
Wernicke-Korsakoff Ataxia and dec memory
Vitamin B2 Riboflavin
Fx: FAD and FMN derived from it, mucous membrane integrity
Def: Cheilosis (inflamm of lips), corneal vascularization
Vitamin B3 Niacin
Fx: NADP+ (redox rxns) and NAD+(carb met)
Def: Pellagra 4Ds =Dermatitis, Diarrhea, Dementia, Death, thickening of
tongue
Tox: Flushing
NOTES: made from tryptophan, synth reqs B6
Vitamin B5 Pantothenate, dexpanthenol
Fx: Constituent of CoA, Component of Fatty Acid Synthase
Def: Dermatitis, enteritis, alopecia, adrenal insufficiency
Vitamin B6 Pyridoxine
Fx: Nitrogen Metabolism, tryptophan conversion to Niacin, glycogen
phosphorylase
Def: Seizures, anemia, neuropathies
Tox: Peripheral Neuropathy (numbness in hands and feet)
Vitamin B12 Cobalamines
Fx: Maturation of RBCs, neural fx, DNA synth, myelination synth and repair
Def: Megaloblastic anemia, neurologic deficits
NOTES: Found only in animal products, stored in liver, very large reserves,
Def usually caused by malabsorption. SCHILLING TEST detects deficiency.
Abnormal myelin seen in def
Vitamin B9 Folate, Folic Acid
Fx: maturation of RBCs, synth of purines, pyrimidines, and methionine,
development of fetal nervous system
Def: Megaloblastic anemia, neural tube defects, mental confusion
NOTE: most common vit deficiency in US, not stored long
Vitamin C Ascorbic Acid
Fx: Collagn formation, bone and BV health
Def: Scurvy, weak vasculature, poor wound healing
NOTE: Dr. James Lind Discovers lime prevent scurvy
Vitamin B7 Biotin
Fx: cofactor for carboxylations
Def: Dermatitis, enteritis, caused by antibiotic use, AVID in egg whites
Zinc
Fx: immune fx, metalloproteinase, BPH prevention
Def: Delayed wound healing, hypogonadism, dec. adult hair
Ca/P 2:1
Mb and Se = Detox
Kwashiorkor Protein malnutrition resulting in skin lesions and liver malfunction
Malnutrition, Edema Anemia Liver(Fatty) ACITES
Marasmus Energy malnutrition resulting in wasting
Das könnte Ihnen auch gefallen
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Tetracycline Antibiotics: Medical UsesDokument2 SeitenTetracycline Antibiotics: Medical UsesHanumant SuryawanshiNoch keine Bewertungen
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Jurnal 4Dokument5 SeitenJurnal 4Nindita RahmaNoch keine Bewertungen
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Veterinary Reproductive UltrasonographyDokument255 SeitenVeterinary Reproductive Ultrasonographylenn chand100% (4)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- BODY TISSUES Reviewer 3Dokument3 SeitenBODY TISSUES Reviewer 3Jaira EmmarinaNoch keine Bewertungen
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
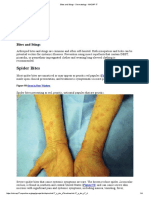
- Bites and Stings - Dermatology - MKSAP 17Dokument4 SeitenBites and Stings - Dermatology - MKSAP 17Ciara Marjorie HannaNoch keine Bewertungen
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- Spinal Cord and Spinal NervesDokument46 SeitenSpinal Cord and Spinal Nerveskombat13_708353334Noch keine Bewertungen
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Noble Conflict by Malorie Blackman (Extract)Dokument13 SeitenNoble Conflict by Malorie Blackman (Extract)RandomHouse ChildrensPublishers0% (1)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Practicing Adverb Clauses AnswersDokument9 SeitenPracticing Adverb Clauses Answersasvas100% (1)
- Cory Ne BacteriumDokument25 SeitenCory Ne BacteriumSona SandiNoch keine Bewertungen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Clinical Study: Overjet and Overbite Influence On Cyclic Masticatory Movements: A CT StudyDokument7 SeitenClinical Study: Overjet and Overbite Influence On Cyclic Masticatory Movements: A CT Studyarya091193Noch keine Bewertungen
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Bubbles HeDokument39 SeitenBubbles HePerrilyn PereyNoch keine Bewertungen
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Sensitive Gut Harvard HealthDokument57 SeitenThe Sensitive Gut Harvard HealthDayhanna Guzman100% (7)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- 15-10-2019, Mr. Jamal, 50 Yo, V.Laceratum Cruris Dextra + Skin Loss + Fraktur Os Fibula, Dr. Moh. Rizal Alizi, M.Kes, Sp. OT-1Dokument15 Seiten15-10-2019, Mr. Jamal, 50 Yo, V.Laceratum Cruris Dextra + Skin Loss + Fraktur Os Fibula, Dr. Moh. Rizal Alizi, M.Kes, Sp. OT-1anon_893244902Noch keine Bewertungen
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- Skema Pemarkahan: Tingkatan 5 Bahasa Inggeris 1119 Kertas 1 Dan 2Dokument12 SeitenSkema Pemarkahan: Tingkatan 5 Bahasa Inggeris 1119 Kertas 1 Dan 2nurmalajamaludinNoch keine Bewertungen
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Diagnostic Test in Science 4: San Carlos Elementary SchoolDokument4 SeitenDiagnostic Test in Science 4: San Carlos Elementary SchoolJohn Nomel B. Dominguez100% (1)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Biology PPT 11Dokument11 SeitenBiology PPT 11agarwalabhinav050Noch keine Bewertungen
- The Shiba Inu BreedDokument19 SeitenThe Shiba Inu BreedpsykosomatikNoch keine Bewertungen
- Appendicitis PathophysiologyDokument4 SeitenAppendicitis PathophysiologyAngelica Cassandra VillenaNoch keine Bewertungen
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- Case Study Pleural EffusionDokument32 SeitenCase Study Pleural Effusionwguino100% (1)
- Biology Terms Grade 9 ReviewerDokument3 SeitenBiology Terms Grade 9 ReviewerGreta Uy Sevilla100% (1)
- Autonomic NsDokument32 SeitenAutonomic NsErmias TewoldeNoch keine Bewertungen
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- First Aid - Ready ReckonerDokument2 SeitenFirst Aid - Ready ReckonerDr VJ GeorgeNoch keine Bewertungen
- Microsoft Word Document جديدDokument3 SeitenMicrosoft Word Document جديدHisham EssamNoch keine Bewertungen
- Diagnosis Dengue Melalui Deteksi Antibodi Imunoglobulin G Spesifik Dalam Sampel Urine Dengan Teknik ELISADokument8 SeitenDiagnosis Dengue Melalui Deteksi Antibodi Imunoglobulin G Spesifik Dalam Sampel Urine Dengan Teknik ELISANOVI WULANDARINoch keine Bewertungen
- K15 - Infeksi Sistem Saraf PusatDokument65 SeitenK15 - Infeksi Sistem Saraf PusatZikri Putra Lan LubisNoch keine Bewertungen
- Metodo, Entrenamiento y Principios Del ADVIA 120Dokument64 SeitenMetodo, Entrenamiento y Principios Del ADVIA 120Jaime Elias100% (3)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Zoology MCQDokument15 SeitenZoology MCQeesha iqbal67% (3)
- Sanum Therapy Book Helios PDFDokument314 SeitenSanum Therapy Book Helios PDFOscarNoch keine Bewertungen
- Girls and Puberty BookletDokument9 SeitenGirls and Puberty Bookletఫణీంద్ర నర్సెట్టి100% (1)
- The 5 Hidden: Libido KillersDokument6 SeitenThe 5 Hidden: Libido KillersscribduserNoch keine Bewertungen
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)