Beruflich Dokumente
Kultur Dokumente
Chronic Kidney Disease Case Presentation
Hochgeladen von
nnaesor_109150%(2)50% fanden dieses Dokument nützlich (2 Abstimmungen)
2K Ansichten14 SeitenChronic Kidney Disease Case Presentation
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenChronic Kidney Disease Case Presentation
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
50%(2)50% fanden dieses Dokument nützlich (2 Abstimmungen)
2K Ansichten14 SeitenChronic Kidney Disease Case Presentation
Hochgeladen von
nnaesor_1091Chronic Kidney Disease Case Presentation
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 14
Dr. Eutiquio Ll.
Atanacio Memorial Hospital Incorporation
San Nicolas Concepcion, Tarlac
2014
A Case Presentation
CHRONIC RENAL FAILURE
Prepared by:
Rose Ann A. Salunga RN
June 25, 2014
I. INTRODUCTION
A. Brief Description of the Disease Condition
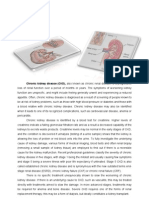
Chronic kidney disease (CKD), also known as chronic renal disease, is a
progressive loss of renal function over a period of months or years in which the bodys
ability to maintain metabolic and fluid and electrolyte balance fails, resulting in uremia or
azotemia. In this condition, the GFR falls below 10% of the normal rate.
Chronic Kidney Disease (CKD) affects 26 million Americans. Early detection
can help to prevent progression of the disease which ultimately can lead to kidney
failure and death. However, early detection can be difficult because the signs
and symptoms of kidney disease, and even acute kidney failure, are often
overlooked.
The prevalence of CKD has steadily increased over the past two decades, and
was reported to affect over 13% of the U.S. population in 2004. In 2009, more than
570,000 people in the United States were classified as having end-stage renal disease
(ESRD), including nearly 400,000 dialysis patients and over 17,000 transplant
recipients. A patient is determined to have ESRD when he or she requires replacement
therapy, including dialysis or kidney transplantation. The rise in incidence of CKD is
attributed to an aging populace and increases in hypertension (HTN), diabetes, and
obesity within the U.S. population. CKD is associated with a host of complications
including electrolyte imbalances, mineral and bone disorders, anemia, dyslipidemia, and
HTN. It is well known that CKD is a risk factor for cardiovascular disease (CVD), and
that a reduced GFR and albuminuria are independently associated with an increase in
cardiovascular and all-cause mortality.
Local Statistics:
MORTALITY: TEN LEADING (10) LEADING CAUSES
Number and rate/100,000 Population Philippines
5-Year Average (2000-2004) & 2005
Cause
5 Year Average
(2000-2004)
2005*
Number Rate No. Rate
1. Diseases of the Heart 66,412 83.3 77,060 90.4
2. Diseases of the Vascular system 50,886 63.9 54,372 63.8
3. Malignant Neoplasm 38,578 48.4 41,697 48.9
4. Pneumonia 32,989 41.4 36,510 42.8
5. Accidents 33,455 42.0 33,327 39.1
6. Tuberculosis, all forms 27,211 34.2 26,588 31.2
7. Chronic lower respiratory diseases 18,015 22.6 20,951 24.6
8.Diabetes Mellitus 13,584 17.0 18,441 21.6
9. Certain conditions originating in the
perinatal period
14,477 18.2 12,368 14.5
10. Nephritis, nephrotic syndrome and
nephrosis
9.166 11.5 11,056 3.6
Note: Excludes ill-defined and unknown causes of mortality
(R00-R99) n=23,235
* reference year
** External Causes of Mortality
Last Update: September 29, 2011
TEN LEADING (10) CAUSES OF MORTALITY AMONG MALES
Number and Rate/100,000 Population
Philippines, 2005
Cause No. Rate
1. Diseases of the Heart 43,809 102.1
2. Diseases of the Vascular system 30,531 71.2
3. Accidents 27,281 63.6
4. Malignant Neoplasms 21,993 51.3
5. Tuberculosis, all forms 18,229 42.5
6. Pneumonia 18,145 42.3
7. Chronic lower respiratory diseases 14,450 33.7
8. Diabetes Mellitus 8,912 20.8
9. Certain conditions originating in the perinatal period 7,385 17.2
10. Nephritis, nephrotic syndrome and nephrosis
6,548 15.3
Last Update: September 28, 2011
TEN LEADING (10) CAUSES OF MORTALITY AMONG FEMALES
Number and Rate/100,000 Population
Philippines, 2005
Cause No. Rate
1. Diseases of the Heart 33,251 78.5
2. Diseases of the Vascular system 23,841 56.3
3. Malignant Neoplasms 19,704 46.5
4. Pneumonia 18,365 43.3
5. Diabetes Mellitus 9,529 22.5
6. Tuberculosis, All Forms 8,359 19.7
7. Chronic lower respiratory diseases 6,501 15.3
8. Accidents 6,046 14.3
9. Certain conditions originating in the perinatal period 4,983 11.8
10. Nephritis, nephrotic syndrome and nephrosis 4,508 10.6
Note: Excludes ill-defined and unknown causes of mortality (R00-R99) for males
(n=11,840)
and females n=11,395
** External Causes of Mortality
Last Update: September 28, 2011
(http://www.doh.gov.ph/node/198)
The tables show that diseases of the vascular system are second to the highest
cause of morbidity and mortality in the Philippines in both male and female. It can also
be seen that males have higher rates than female. It is a must that people would
cautiously monitor their health and practice healthy living to avoid diseases that could
lead to death. And people should prioritize their health more than anything else.
B. GENERAL OBJECTIVES:
The general objective of the case study is to gain the comprehensive knowledge
about the disease to gain the practical exercise about the Adult Health Problem and
also to gain Practical experience working with a patient having chronic kidney disease
and to give holistic patient care according to their need.
II. ANATOMY AND PHYSIOLOGY
Function of the Urinary System
The major functions of the urinary systems are performed by the kidneys and the
kidneys plays the following essentials roles in controlling the composition and volume of
body fluids:
1. Excretion. The kidneys are the major excretory organs of the body. They remove
waste products, many of which are toxic, from the blood. Most waste products are
metabolic by- products of cells and substances absorbed from the intestine. The
skin, liver, lungs, and intestines eliminate some of these waste products, but they
cannot compensate if the kidneys fail to function.
2. Blood volume control. The kidneys play an essential role in controlling blood
volume by regulating the volume of water removed from the blood to produce urine.
3. Ion concentration regulation. The kidneys help regulate the concentration of the
major ions in the body fluids.
4. pH regulation. The kidneys help regulate the pH of the body fluids. Buffers in the
blood and the respiratory system also play important roles in the regulation of pH
5. Red blood cell concentration. The kidneys participate in the regulation of red
blood cell production and therefore, in controlling the concentration of red blood cells
in the blood.
6. Vitamin D synthesis. The kidneys. Along with the skin and the liver, participate in
the synthesis of vitamin D.
Kidneys
The kidneys balance the urinary excretion of substances against the
accumulation within the body through ingestion or production. Consequently, they are
major controller of fluid and electrolyte homeostasis. The kidneys also have several
non-excretory metabolic and endocrine functions, including blood pressure regulation,
erythropoietin production, insulin degradation, prostaglandin synthesis, calcium and
phosphorus regulation and Vitamin D metabolism.
The kidneys are located retroperitoneally, in the posterior aspect of the abdomen.
On either side of the ventral column. They lie between the 12
th
thoracic and third lumbar
vertebrae. The left kidney is usually positioned slightly higher than the right. Adult
kidneys are average approximately 11 cm in length, 5 to 7.5 cm in width, and 2.5 cm in
thickness. The kidney has a characteristic curved shape, with a convex distal edge and
a concave medial boundary.
Ureters, Urinary Bladder and Urethra
The ureters are small tubes that carry urine from the renal pelvis of the kidney to
the posterior inferior portion of the urinary bladder. The urinary bladder is a hollow
muscular container that lies in the pelvic cavity just posterior to the pubic symphysis. It
functions to store urine, and its size depends on the quantity of urine present. The
urinary bladder can hold from a few milliliters to a maximum of about 1000 mL of urine.
When the urinary bladder reaches a volume of a few hundred mL, a reflex is activated,
which causes the smooth muscle of the urinary bladder to contract and most of the
urine flows out of the urinary bladder through urethra. The urethra is a tube that exits
the urinary bladder inferiorly and anteriorly. The triangle-shaped portion of the urinary
bladder located between the opening of the ureters and the opening of the urethra is
called trigone. The urethra carries urine from the urinary bladder to the outside of the
body.
Renal Blood flow and Glomerular Filtration
The kidney receive 20% to 25% of the cardiac output under resting conditions,
averaging more than 1 L of arterial blood per minute. The renal arteries branch from the
abdominal aorta at the level of he second lumbar vertebra, enter the kidney, and
progressively branch into lobar arteries. Blood flows from the interlobular arteries
through the afferent arteriole, the glomerular capillaries, the efferent arteriole and the
peritubular capillaries. Some of the peritubular capillaries carry a small amount of blood
to the renal medulla in the vasa recta before entering the venous drainage. The blood
leaves the kidney in venous system closely corresponding to the arterial system:
interlobular veins, arcuate veins, interlobar veins, and the renal vein. The renal
circulation then empties into the inferior vena cava.
Physiology
Characteristics of Urine
Urine is a watery solution of nitrogenous waste an inorganic salts that are
removed from the plasma and eliminated by the kidneys. It is 5% water and 5%
dissolved solids and gases. The amount of these dissolved substances is indicated by it
specific gravity. The specific gravity of pure water, used as a standard is 1.000.
Because of the dissolved materials it contains, urine has a specific gravity that normally
varies from 1.010 to 1.040. When the kidneys are diseased, they lose the ability to
concentrate urine, and the specific gravity no longer varies as it does when the kidneys
function normally.
Urine formation
The chief function of the kidneys is to produce urine. Each part of the nephrons
performs a special function. There are three important processes by which urine is
formed. They are glomerular filtration, tubular reabsorption and tubular secretion.
What do the kidneys do?
The kidneys remove wastes and extra water from the blood to form urine. Urine flows
from the kidneys to the bladder through the ureters.
Your kidneys are bean-shaped organs, each about the size of your fist. They are
located near the middle of your back, just below the rib cage. The kidneys are
sophisticated reprocessing machines. Every day, your kidneys process about 200
quarts of blood to sift out about 2 quarts of waste products and extra water. The waste
and extra water become urine, which flows to your bladder through tubes called ureters.
Your bladder stores urine until you go to the bathroom.
The wastes in your blood come from the normal breakdown of active tissues and from
the food you eat. Your body uses food for energy and self-repair. After your body has
taken what it needs from the food, waste is sent to the blood. If your kidneys did not
remove these wastes, the wastes would build up in the blood and damage your body.
The actual filtering occurs in tiny units inside your kidneys called nephrons. Every
kidney has about a million nephrons. In the nephron, a glomeruluswhich is a tiny
blood vessel, or capillaryintertwines with a tiny urine-collecting tube called a tubule. A
complicated chemical exchange takes place, as waste materials and water leave your
blood and enter your urinary system.
At first, the tubules receive a combination of waste materials and chemicals that your
body can still use. Your kidneys measure out chemicals like sodium, phosphorus, and
potassium and release them back to the blood to return to the body. In this way, your
kidneys regulate the bodys level of these substances. The right balance is necessary
for life, but excess levels can be harmful.
The kidneys remove wastes and extra water from the blood to form urine. Urine flows
from the kidneys to the bladder through the ureters.
In addition to removing wastes, your
kidneys release three important hormones:
Erythropoietin (eh-RITH-ro-
POY-eh-tin), or EPO, which stimulates
the bone marrow to make red blood
cells
Renin (REE-nin), which
regulates blood pressure
Calcitriol (kal-suh-TRY-ul), the
active form of vitamin D, which helps
maintain calcium for bones and for
normal chemical balance in the body
What is renal function?
Your health care team may talk about the
work your kidneys do as renal function. If
you have two healthy kidneys, you have 100 percent of your renal function. This is more
renal function than you really need. Some people are born with only one kidney, and
these people are able to lead normal, healthy lives. Many people donate a kidney for
transplantation to a family member or friend. Small declines in renal function may not
cause a problem.
III. PATIENT AND HIS ILLNESS
A. Definition of the disease
Chronic or irreversible, renal failure is a progressive reduction of functioning renal
tissue such that the remaining kidney mass can no longer maintain the bodys
internal environment. Chronic Renal failure can develop insidiously over many years,
or it may result from an episode of acute renal failure from which the client has not
recovered.
Progressive loss of renal function over time; based on a gradual decline in the GFR and
creatinine clearance. The diagnosis of CKD requires the following:
1. Decline of kidney function for 3 months or more AND
2. Evidence of kidney damage (e.g. albuminuria or abnormal biopsy) OR
GFR <60 mL/min/1.73 m
2
Each patient is classified into one of the following 5 stages of CKD because
management and prognosis varies according to the progression of damage.
Stage 1: Kidney damage with normal or increased GFR (>90 mL/min/1.73 m
2
)
Stage 2: Mild reduction in GFR (60-89 mL/min/1.73 m
2
)
Stage 3: Moderate reduction in GFR (30-59 mL/min/1.73 m
2
)
Stage 4: Severe reduction in GFR (15-29 mL/min/1.73 m
2
)
Stage 5: Kidney failure (GFR <15 mL/min/1.73 m
2
or dialysis)
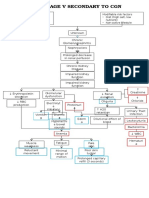
B. Precipitating Factors
Chronic glomerular disease such as glomerunephritis
Chronic infections such as chronic pyelonephritis or tuberculosis
Congenital anomalities such as polycystic
Vascular diseases, such as renal nephrosclerosis or hypertension
Hypertension
Glomerular and vascular changes:
o Elevated systemic blood pressures cause a hypertrophic response leading to
intimal thickening of the large and the small vasculature.
o The mechanisms are compensatory at first, but later lead to glomerular damage
Global sclerosis ischemic injury to the nephrons causes death
Focal segmental sclerosis glomerular enlargement for compensation of the
loss of nephrons in other areas of the kidney.
Interstitial nephritis:
o The vascular and glomerular disease lead to tubular atrophy and an intense
chronic interstitial nephritis
The intense chronic interstitial nephritis is thought be secondary to
immunologic processes against ischemia-mediated antigen changes on the
tubular epithelial cell surface.
Chronically these changes lead to tubular and glomerular loss causing nephrons
loss.
o With the death of some nephrons, less are available to maintain the GFR.
o Gradual decline in the GFR is noticed as the nephrons continue to die.
Obstructive processes such as calculi
nephrotoxic agents such as long-term aminoglycoside
endocrine diseases such as diabetic neuropathy
Such conditions gradually destroy the nephrons and eventually cause irreversible renal
failure. Similarly, acute renal failure that fails to respond to treatment becomes chronic
renal failure. Blockages
Scarring from infections or a malformed lower urinary tract system (birth defect)
can force urine to back up into the kidney and damage it. Blood clots or plaques of
cholesterol that block the kidneys blood vessels can reduce blood flow to the kidney
and cause damage. Repeated kidney stones can block the flow of urine from the kidney
and are another kind of obstruction that can damage the kidneys.
Overuse of Painkillers and Allergic Reactions to Antibiotics
Heavy use of painkillers containing ibuprofen (Advil, Motrin), naproxen (Aleve),
or acetaminophen (Tylenol) have been linked to interstitial nephritis, a kidney
inflammation that can lead to kidney failure. A new study suggests that ordinary use
of painkillers (e.g., one pill per day) is not harmful in men who are not at risk for
kidney disease. Allergic reactions toor side effects ofantibiotics like penicillin
and vancomycin may also cause nephritis and kidney damage.
Drug Abuse
Use of certain nonprescription drugs, such as heroin or cocaine, can damage the
kidneys, and may lead to kidney failure and the need for dialysis.
Inflammation
Certain illnesses, like glomerulonephritis (inflammation of the filtering units of the
kidneys), can damage the kidneys, sometimes enough to cause CKD. Some
glomerulonephritis is inherited, and some may be an immune response to infections like
strep throat.
C. Predisposing Factors
Sex- both sexes are affected by chronic renal failure. But in 1998, based on United
States Renal Data System, a higher total number of males with ESRD was found
Age- CRF can be found in people of any age, from infants to the very old. The
elderly population also is the most rapidly growing ESRD population in the United
States. Note that age 30 years progressive physiological glomerulosclerosis. Aging
also results in concomitant progressive physiological decrease in muscle mass such
that daily urinary creatinine excretion also decreases.
High risk groups for chronic kidney disease (CKD) include those with a family
history of kidney disease. One inherited disease, polycystic kidney disease, causes
large, fluid-filled cysts that eventually crowd out normal kidney tissue.
African Americans, Hispanics, Pacific Islanders, and Native Americans are also at
increased risk.
D. Clinical Manifestations
The clinical manifestations of CRF are present throughout the body. No organ system is
spared.
Electrolyte imbalances
Electrolyte balance may be upset by impaired excretion and utilization in
the kidney. Although many clients maintain normal serum sodium level, the salt-
wasting properties of some failing kidneys, in addition to vomiting and diarrhea,
may cause hyponatremia. Because the kidneys are efficient at excreting
potassium, potassium levels usually remain within normal limits until late in the
disease.
Several mechanisms contriburte to hypocalcemia. Conversion of 25-
hydroxycholecalciferol to 1,25-dihyroxycholecalciferol (necessary to absorb
calcium) is decreased, which results in reduced intestinal absorption of calcium.
At the same time, phosphate is not excreted, which causes hyperphosphatemia.
Because calcium and phosphate are inversely related, a high phosphate level
results in a reduced calcium level.
Metabolic changes
In advancing renal failure, BUN and serum creatinine rise as waste products
of protein metabolism accumulate in the blood. The serum creatinine level is the
most accurate measure of renal function. The proteinuria accompanying renal
disease and sometimes inadequate dietary intake of proteins cause
hypoproteinuria, which lowers the intravascular oncotic pressure. Metabolic
acidosis occurs because of the kidneys inability to excrete hydrogen ions.
Decrease reabsorption of sodium bicarbonate and decreased formation of
dihydrogen phosphate and ammonia contribute to this problem. Acidosis
accentuates hyperkalemia and the reabsorption of calcium from the bones.
Hematologic changes
The primary hematologic effect of renal failure is anemia, usually
normochromic and normocytic. It occurs because the kidneys are unable to produce
erythropoietin, a hormone necessary for red blood cell production. Frequently, the
fatigue, weakness, and cold intolerance accompanying the anemia lead to a
diagnosis of renal failure.
Gastrointestinal changes
The entire gastrointestinal system is affected. Transient anorexia, nausea,
vomiting are almost universal. Clients often experience a constant bitter , metallic, or
salty taste, and their breath commonly smells fetid, fishy or ammonia-like. Stomatitis,
parotitis and gingivitis are common problems because of poor oral hygiene and the
formation of ammonia from salivary urea. Accumulations of gastro may be a major
cause of ulcer disease. Esophagitis, gastritis, colitis, gastrointestinal bleeding, and
diarrhea may be present. Serum amylase level may be increased, although they do
not necessarily indicate pancreatitis.
Immunologic changes
Impairment of the immune system makes the client more susceptible to
infection. Several factors are involved, including depression of humoral antibody
formation, suppression of delayed hypersensitivity and decreased chemotactic
function of leukocytes. Immunosuppression is an important part of the medical
management of renal diseaes such as glomerulonephritis.
Cardiovascular changes
The most common clinical manifestation is hypertension, produced through:
mechanism of volume overload, stimulation of the renin-angiotensin system,
sympatheically mediated vasoconstriction, absence of prostaglandins.
Respiratory changes
Some of the respiratory effects such as pulmonary edema can be attributed to
fluid overload. Metabolic acidosis causes a compensatory increase in respiratory
rate as the lungs try to eliminate excess hydrogen ions.
Musculoskeletal changes
The etiologic mechanism involves the kidney-bone-parathyroid and calcium-
phosphate-vitamin D connections. As the GRF decreases, the phosphate excretion
decreases and calcium elimination increases. Abnormal levels of calcium and
phosphate stimulate the release of parathyroid hormone that mobilizes calcium from
the bones and facilitates phosphate excretion.
Integumentary changes
The skin is also often very dry because of atrophy of the sweat glands. Severe and
intractable pruritus may result from secondary hyperparathyroidism and calcium
deposits in the skin. The pallor of anemia is evident.
1. Changes in Urination
Because your kidneys are tasked with making urine, and thereby eliminating waste, any
changes in the frequency, color, or appearance of urine should be taken seriously.
Some common types of changes include:
Urinating more frequently during the night or in greater amounts
Urinating less often or in smaller amounts
Having foamy or bubbly urine or blood in your urine
Difficulty urinating
2. Swelling
If your kidneys are unable to remove extra fluid from your body, you will likely
experience swelling in your legs, ankles, feet, face, or hands. Water retention due to a
loss of GFR leading to sodium and fluid retention. Fluid moves into the extravascular
space, due to increased hydrostatic pressure, causing pitting edema in the lower
extremity (fluid movement could also be due to hypoalbuminemia, in some diseases,
leading to a low oncotic pressure).
3. Skin Rash / Itching
If your kidneys are unable to remove waste from the bloodstream, the buildup can
cause rashes and severe itching.
4. Leg, Back or Side Pain
Kidney problems can lead to pain in the back, side or even in the leg. Kidney cysts
(large, fluid-filled sacs) resulting from polycystic kidney disease that form on kidneys
and occasionally on the liver can also cause back and leg pain.
5. Metallic Taste in Mouth/Ammonia Breath
When waste builds up in the bloodstream, it can cause bad breath, a metallic taste in
the mouth, and affect how food tastes. You may also have a change in appetite that
results in weight loss.
6. Nausea and Vomiting
Waste buildup in the blood can also cause nausea and vomiting.
7. Feeling Cold
Healthy kidneys make the hormone known as erythropoietin, which prompts the body to
make oxygen-carrying red blood cells. Kidney disease can interrupt the healthy
production of this hormone and cause a decrease in red blood cells, a condition known
as anemia. Anemia and kidney disease can result in a variety of symptoms, including
constantly feeling cold and shortness of breath.
8. Shortness of Breath
Kidney disease can cause extra fluid to build up in the lungs, leading to shortness of
breath. Anemia, a common side-effect of kidney disease which starves your body of
oxygen, can also cause you to feel winded or short of breath. Fluid accumulation
causes pulmonary edema and loss of air space causing ventilation-perfusion mismatch.
This leaves less area for oxygen diffusion form the blood vessels.
9. Dizziness and Trouble Concentrating
When you suffer from anemia related to kidney failure, both your body and your brain
will be lacking the proper amount of oxygen. The result can be dizziness, trouble with
concentration, and memory-related issues.
10. Fatigue
When kidneys fail, and side effects like anemia set in, you may experience tired
muscles, weakness, and overall fatigue. Erythropoietin (EPO), the major erythropoiesis
stimulator, is released from the kidneys; with renal failure, there is loss of EPO release
V. MEDICAL MANAGEMENT
The goal of management is to maintain kidney function and homeostasis for as long as
possible. Because of the great deterioration of renal function, the duration of
management may vary from months to years. Nothing can be done to prevent or delay
the fatal outcome.
Control of urinary volume: fluids are forced since kidney has lessened ability
to concentrate solids. more fluids about 2litres is needed to excrete waste.
Sometimes frusemide may be required to increase urine production.
Control of nausea and vomiting: anorexia, nausea and vomiting tend to
develop when the cretinine clearance falls below 5ml/min. so reduction in protein
is required to improve nausea. Blood: 0.8-1.4 mg/dL is the normal. Due to
impaired kidney function, creatinine in the blood elevates.
Creatinine clearance rate was 10.g mg/dl on 4/2, 8.5 mg/dl on 068/4/6, 9.7mg/dl
on 068/4/9.
Antiseizure agents
Antihypertensive agents: hypertension is managed by intravascular volume
control and a variety of anti- hypertensive agents.
Control of hyperkalaemia will be treated with I/V glucose and insulin in a ratio of 3
gm Glucose to 1 unit soluble insulin.
Control of anemia: blood transfusion are frequently required.
Accurate record of input and output chart should be maintained
Other therapy: dialysis
It is usually initiated when the patient cannot maintain a reasonable
lifestyle with conservative treatment.
VI. Nursing Management:
Nursing care is directed toward assessing fluid status and identifying potential source of
imbalance
Implement a dietary program to ensure proper nutritional intake within the limits of the
treatment regimen.
Promote positive feelings by encouraging increased self care
Provide explanations and information to the patient and family concerning ESRD,
treatment options and potential complications
Nurse must be familiar with various drugs and their side effects
Provide emotional support to the patient and his family because of the numerous
changes experienced.
Cardiovascular disease (CVD)is the leading cause of death in patients with CKD.
o Reducing risk factors for development of CVD is beneficial.
E.g. treatment of hyperlipidemia, lifestyle and dietary changes
Tight blood pressure control:
o Reducing damage due to the end organ effects of hypertension on the kidney as
well as the heart.
o Angiotensin-converting enzyme inhibitors (ACEI) and angiotensin II
receptor blockers(ARBs) block the effects of angiotensin II on (i) sodium and
fluid retention, (ii) vasoconstriction, (iii) stimulating ADH release, (iv) stimulating
aldosterone release, and (v) inducing a sympathetic response.
ACEIs and ARBs also slow down progression of proteinuria in patients with
diabetic CKD.
Diabetes management:
o Tight glucose management slows the progression of vascular and heart disease.
Avoidance of IV contrast, NSAIDs, and nephrotoxic drugs:
o These agents can potentially induce an acute kidney injury (AKI) on the
underlying kidney disease and therefore exacerbate the baseline CKD.
Diet:
o Mixed evidence exists whether dietary protein restriction is beneficial in slowing
disease progression.
o Proteins affect the renal hemodynamics, raising the GFR, in hypothesized 2
ways.
Hormonal effects proteins cause secretion of glucagon, IGF-1 and kinins,
all of which have been shown to raise the GFR.
Tubuloglomerular effects high amino acid (AA) filtration leads to increased
AA and hence the sodium uptake in the proximal convoluted tubule. A
decreased sodium delivery to the distal convoluted tubule leads to the
rennin-angiotensin system activation via the macula densa and these work to
raise the GFR (mechanisms above)
o Controlling hyperphosphatemia: Protein restriction also limits phosphorus
consumption. Hyperphosphatemia plays a major role in the progression of renal
osteodystrophy. Phosphate binders are used to reduce phosphate absorption
through the GI tract.
VII. Surgical Management
Kidney transplantation: it involves transplanting a kidney from a living donor to a
recipient who has ESRD. The success rate increases if kidney transplantation from
a living donor is performed before dialysis is initiated.
VIII. REFERENCES
1. Coresh J, Selvin E, Stevens LA, et al. Prevalence of chronic kidney disease in
the United States. 2007.
2. Collins AJ, Foley RN, Chavers B, et al. U.S. renal data system 2011 annual data
report. Am J Kidney Dis. 2012.
3. Matsushita K, van der Velde M, Astor BC, et al. Association of estimated
glomerular filtration rate and albuminuria with all-cause and cardiovascular
mortality in general population cohorts: a collaborative meta-analysis. Lancet.
2010.
4. Rashidi A, Sehgal AR, Rahman M, O'Connor AS. The case for chronic kidney
disease, diabetes mellitus, and myocardial infarction being equivalent risk factors
for cardiovascular mortality inpatients older than 65 years. Am J Cardiol. 2008.
5. Rao MV, Qiu Y, Wang C, Bakris G. Hypertension and CKD: Kidney Early
Evaluation Program (KEEP) and National Health and Nutrition Examination
Survey (NHANES), 19992004. Am J Kidney Dis. 2008.
6. Botdorf J, Chaudhary K, Whaley-Connell A. Hypertension in cardiovascular and
kidney disease. Cardiorenal Med. 2011.
7. Segura J, Ruilope L. Hypertension in moderate-to-severe nondiabetic CKD
patients. Adv Chronic Kidney Dis. 2011.
8. Chobanian AV, Bakris GL, Black HR, et al. The seventh report of the Joint
National Committee on Prevention, Detection, Evaluation, and Treatment of High
Blood Pressure. 2003.
Chronic Kidney Disease. Retrieved from
http://www.medscape.com/viewarticle/766696_6.
Chronic Kidney Disease. Retrieved from http://www.nationalkidneycenter.org/chronic-
kidney-disease/symptoms/.
Chronic Kidney Disease. Retrieved from www.nationalkidneycenter.org/treatment-
options/kidney-dialysis/peritoneal-dialysis/.
TEN LEADING (10) CAUSES OF MORTALITY (2011). Retrieved from
http://www.doh.gov.ph/node/198.
Das könnte Ihnen auch gefallen
- A Case Study On Chronic Renal DiseaseDokument17 SeitenA Case Study On Chronic Renal Diseasematucojulio100% (1)
- Chronic Kidney Disease Case PresDokument32 SeitenChronic Kidney Disease Case Presnnaesor_1091Noch keine Bewertungen
- Chronic Kidney DiseaseDokument12 SeitenChronic Kidney DiseaseRoseben SomidoNoch keine Bewertungen
- My Case Study of Liver CirrhosisDokument13 SeitenMy Case Study of Liver Cirrhosisdysphile100% (1)
- End Stage Renal Disease Case StudyDokument8 SeitenEnd Stage Renal Disease Case StudyNikko Dela CruzNoch keine Bewertungen
- Case Study CKD DM Type 2Dokument7 SeitenCase Study CKD DM Type 2Brian Cornel0% (3)
- End Stage Renal DiseaseDokument62 SeitenEnd Stage Renal DiseaseMae Navidas DigdiganNoch keine Bewertungen
- ESRD Secondary To Diabetic Nephropathy CASE STUDY Docx 2Dokument42 SeitenESRD Secondary To Diabetic Nephropathy CASE STUDY Docx 2Eyerusalem100% (1)
- A Case Study On Chronic Kidney DiseaseDokument103 SeitenA Case Study On Chronic Kidney DiseaseLouella Mae CoraldeNoch keine Bewertungen
- Case Study On End Stage Renal FailureDokument19 SeitenCase Study On End Stage Renal Failurelenecarglbn100% (1)
- Chronic Renal FailureDokument1 SeiteChronic Renal Failurejj_cuttingedges100% (2)
- Case Study On Chronic Kidney DiseaseDokument101 SeitenCase Study On Chronic Kidney DiseaseZNEROL100% (6)
- CHF Case StudyDokument38 SeitenCHF Case StudyMelissa David100% (1)
- Chronic Kidney DiseaseDokument15 SeitenChronic Kidney Diseaseapi-270623039Noch keine Bewertungen
- Chronic Kidney DiseaseDokument33 SeitenChronic Kidney DiseasesexiiimammaNoch keine Bewertungen
- Liver CirrhosisDokument31 SeitenLiver CirrhosisAsniah Hadjiadatu Abdullah100% (1)
- Chronic Renal FailureDokument37 SeitenChronic Renal Failuredorkiebaby100% (10)
- CKD (F&e)Dokument110 SeitenCKD (F&e)Al-nazer Azer Al100% (1)
- Case Study On Chronic Kidney Disease Probably To Secondary HypertensionDokument18 SeitenCase Study On Chronic Kidney Disease Probably To Secondary Hypertensionkyeria77% (26)
- Case Study 18 CKDDokument7 SeitenCase Study 18 CKDapi-301049551Noch keine Bewertungen
- Case Study On Alcoholic Liver DiseaseDokument24 SeitenCase Study On Alcoholic Liver DiseaseKristine Alejandro100% (5)
- CaseStudy ChronicRenalFailureDokument29 SeitenCaseStudy ChronicRenalFailureCarlcedrick ManlapusNoch keine Bewertungen
- Pathophysiology of Alcoholic Liver DiseaseDokument4 SeitenPathophysiology of Alcoholic Liver Diseaseshailendra tripathiNoch keine Bewertungen
- Liver Cirrhosis: A Case Study OnDokument31 SeitenLiver Cirrhosis: A Case Study OnCharmaine del RosarioNoch keine Bewertungen
- Chronic Kidney Disease Case StudyDokument52 SeitenChronic Kidney Disease Case StudyGi100% (1)
- Acute Glomerulonephritis Case StudyDokument12 SeitenAcute Glomerulonephritis Case Study19lyon92100% (6)
- Acute Glomerulonephritis 42-mDokument27 SeitenAcute Glomerulonephritis 42-mcbanguisNoch keine Bewertungen
- Case Study - Chronic Kidney Disease Treated With DialysisDokument7 SeitenCase Study - Chronic Kidney Disease Treated With Dialysisapi-387604918100% (1)
- Acute Renal FailureDokument59 SeitenAcute Renal Failurepaul_v_44440% (1)
- Case Study 18Dokument4 SeitenCase Study 18api-271284613Noch keine Bewertungen
- Case Study - Septic ShockDokument16 SeitenCase Study - Septic ShockIrene Mae Villanueva Ariola100% (2)
- Case Study 10 Renal FailureDokument19 SeitenCase Study 10 Renal FailureAriadne Cordelette100% (2)
- End - Stage Renal DiseaseDokument59 SeitenEnd - Stage Renal DiseaseJonathan Diaz93% (15)
- Non-St Segment Elevation Myocardial Infarction (Nstemi)Dokument24 SeitenNon-St Segment Elevation Myocardial Infarction (Nstemi)MHIEMHOINoch keine Bewertungen
- Chronic Renal FailureDokument3 SeitenChronic Renal FailureIvana Yasmin Bulandres100% (2)
- Alcoholic Liver DiseaseDokument70 SeitenAlcoholic Liver Diseaseaannaass nNoch keine Bewertungen
- Pathophysiology of Chronic Kidney Disease: Predisposing Factors: Precipitating FactorsDokument1 SeitePathophysiology of Chronic Kidney Disease: Predisposing Factors: Precipitating FactorsReina Samson0% (1)
- Chronic Kidney Disease CompilationDokument33 SeitenChronic Kidney Disease CompilationGwen Stefanie Lagrimas ValloyasNoch keine Bewertungen
- Myocardial Infarction Case StudyDokument19 SeitenMyocardial Infarction Case Studyapi-312992151Noch keine Bewertungen
- Acute GlomerulonephritisDokument17 SeitenAcute GlomerulonephritisBayanSecond WardNoch keine Bewertungen
- Case Study of Chronic Kidney DiseaseDokument54 SeitenCase Study of Chronic Kidney DiseaseJomari Zapanta100% (4)
- Cholecystitis Case PresDokument103 SeitenCholecystitis Case PresAnton LaurencianaNoch keine Bewertungen
- CKDDokument35 SeitenCKDNATTAPAT SANGKAKULNoch keine Bewertungen
- Case Analysis FinalDokument29 SeitenCase Analysis FinalVeyNoch keine Bewertungen
- NCP Liver CirrhosisDokument7 SeitenNCP Liver CirrhosisIris Jimenez-BuanNoch keine Bewertungen
- Liver Cirrhosis: Review HepatologyDokument71 SeitenLiver Cirrhosis: Review HepatologyAstri Arri FebriantiNoch keine Bewertungen
- Acute Renal Failure Case StudyDokument18 SeitenAcute Renal Failure Case Studymanjeet3680% (5)
- Chronic Kidney DiseaseDokument9 SeitenChronic Kidney Diseaseluvgrace100% (1)
- Case StudyDokument37 SeitenCase StudyAnonymous t78m8ku100% (1)
- Pathophysiology CKD Secondary To CGNDokument1 SeitePathophysiology CKD Secondary To CGNNathan Vince CruzNoch keine Bewertungen
- Kidney Transplant PresentationDokument23 SeitenKidney Transplant PresentationApple Dela CruzNoch keine Bewertungen
- GlomerulonephritisDokument8 SeitenGlomerulonephritisMatthew Ryan100% (1)
- CHRONIC KIDNEY DISEASE Secondary To Chronic GlomerulonephritisDokument31 SeitenCHRONIC KIDNEY DISEASE Secondary To Chronic GlomerulonephritisJerwin Jade Bolor33% (3)
- 17 Urinary SystemDokument5 Seiten17 Urinary SystemOribello, Athenna Jae W.Noch keine Bewertungen
- Case Study ReportDokument16 SeitenCase Study ReportOluebube HerbertNoch keine Bewertungen
- ManuscriptDokument97 SeitenManuscriptAi RimandoNoch keine Bewertungen
- Chronic Renal FailureDokument46 SeitenChronic Renal Failurestepharry08100% (1)
- Case Study JatDokument45 SeitenCase Study JatHSEINNoch keine Bewertungen
- Mr. R.E.B. - CKDDokument61 SeitenMr. R.E.B. - CKDChristy Rose AgrisNoch keine Bewertungen
- CKD Case AnalysisDokument25 SeitenCKD Case Analysisしゃいな ふかみNoch keine Bewertungen
- Informed ConsentDokument4 SeitenInformed Consentnnaesor_1091Noch keine Bewertungen
- Impaired Skin Integrity Related To Surgical Removal of SkinDokument3 SeitenImpaired Skin Integrity Related To Surgical Removal of Skinnnaesor_10910% (2)
- Fire Works InjuryDokument39 SeitenFire Works Injurynnaesor_1091Noch keine Bewertungen
- Deductive Reasoning ReportDokument3 SeitenDeductive Reasoning Reportnnaesor_1091Noch keine Bewertungen
- Deductive Reasoning.Dokument13 SeitenDeductive Reasoning.nnaesor_1091Noch keine Bewertungen
- Some One Like You CordDokument2 SeitenSome One Like You Cordnnaesor_1091Noch keine Bewertungen
- The Lower Limb Tendinopathies Etiology, Biology and Treatment-Springer International (2016)Dokument202 SeitenThe Lower Limb Tendinopathies Etiology, Biology and Treatment-Springer International (2016)Tony Miguel Saba Saba100% (1)
- Learning Through PlayDokument2 SeitenLearning Through PlayThe American Occupational Therapy Association100% (1)
- A View On TB ControlDokument30 SeitenA View On TB ControlhonorinanuguidNoch keine Bewertungen
- Psychological Impact of Light and ColorDokument3 SeitenPsychological Impact of Light and ColorOwais MahmoodNoch keine Bewertungen
- Product CatalogDokument13 SeitenProduct Catalogkleos70Noch keine Bewertungen
- A Comparative Study of The Clinical Efficiency of Chemomechanical Caries Removal Using Carisolv® and Papacarie® - A Papain GelDokument8 SeitenA Comparative Study of The Clinical Efficiency of Chemomechanical Caries Removal Using Carisolv® and Papacarie® - A Papain GelA Aran PrastyoNoch keine Bewertungen
- Current Issues & Trends in Older: Persons Chronic CareDokument12 SeitenCurrent Issues & Trends in Older: Persons Chronic CareKeepItSecretNoch keine Bewertungen
- Indocollyre PDFDokument6 SeitenIndocollyre PDFUpik MoritaNoch keine Bewertungen
- Understanding HypokalemiaDokument4 SeitenUnderstanding HypokalemiaAudrey Leonar100% (1)
- Daniel J Carlat-The Psychiatric InterviewDokument391 SeitenDaniel J Carlat-The Psychiatric InterviewFrancielle Machado86% (7)
- NCP-DP NCM112LecDokument4 SeitenNCP-DP NCM112LecShane CabucosNoch keine Bewertungen
- Threatened AbortionDokument3 SeitenThreatened Abortionjay5ar5jamorabon5torNoch keine Bewertungen
- Advances and Challenges in Stroke RehabilitationDokument13 SeitenAdvances and Challenges in Stroke Rehabilitationarif 2006Noch keine Bewertungen
- Castlegar/Slocan Valley Pennywise November 21, 2017Dokument42 SeitenCastlegar/Slocan Valley Pennywise November 21, 2017Pennywise PublishingNoch keine Bewertungen
- Teresa Iacono 2014 What It Means To Have Complex Communication NeedsDokument6 SeitenTeresa Iacono 2014 What It Means To Have Complex Communication Needsapi-260603230Noch keine Bewertungen
- WarfarinDokument10 SeitenWarfarinMar Ordanza100% (1)
- Insulin IndexDokument13 SeitenInsulin IndexbookbookpdfNoch keine Bewertungen
- 3 Cultural GenogramDokument11 Seiten3 Cultural GenogramJohn Stanley100% (2)
- Assessing Apical PulseDokument5 SeitenAssessing Apical PulseMatthew Ryan100% (1)
- Lumbar Disc HerniationDokument8 SeitenLumbar Disc Herniationandra_scooterNoch keine Bewertungen
- Silver Hill Hospital Chronic Pain and Recovery CenterDokument8 SeitenSilver Hill Hospital Chronic Pain and Recovery CenterSilver Hill HospitalNoch keine Bewertungen
- The Art of Narrative PsychiatryDokument227 SeitenThe Art of Narrative Psychiatryroxyoancea100% (8)
- BiomekanikDokument474 SeitenBiomekanikRicaariani MyGeisha SmashblastNoch keine Bewertungen
- Montano NCP TbiDokument6 SeitenMontano NCP TbiKarl Angelo MontanoNoch keine Bewertungen
- European Union Herbal Monograph Mentha X Piperita L Aetheroleum Revision 1 enDokument12 SeitenEuropean Union Herbal Monograph Mentha X Piperita L Aetheroleum Revision 1 enTabsherah AnsariNoch keine Bewertungen
- How To Use BNF With ScenariosDokument6 SeitenHow To Use BNF With ScenariosLuxs23Noch keine Bewertungen
- Liver CleanseDokument84 SeitenLiver CleanseBrian Jones100% (7)
- Color - Enhancing Foods For Aquarium Fish: Sivaramakris Hnan.T, IvDokument18 SeitenColor - Enhancing Foods For Aquarium Fish: Sivaramakris Hnan.T, IvArun SudhagarNoch keine Bewertungen
- Acne RosaceaDokument28 SeitenAcne Rosaceanathy_soares100% (1)
- Phenoxymethyl Penicillin Potassium: PaciphenDokument2 SeitenPhenoxymethyl Penicillin Potassium: PaciphenKath CorralesNoch keine Bewertungen
- Secrets From the Eating Lab: The Science of Weight Loss, the Myth of Willpower, and Why You Should Never Diet AgainVon EverandSecrets From the Eating Lab: The Science of Weight Loss, the Myth of Willpower, and Why You Should Never Diet AgainBewertung: 3.5 von 5 Sternen3.5/5 (38)
- Body Love Every Day: Choose Your Life-Changing 21-Day Path to Food FreedomVon EverandBody Love Every Day: Choose Your Life-Changing 21-Day Path to Food FreedomBewertung: 4 von 5 Sternen4/5 (1)
- Eat & Run: My Unlikely Journey to Ultramarathon GreatnessVon EverandEat & Run: My Unlikely Journey to Ultramarathon GreatnessNoch keine Bewertungen
- The Obesity Code: Unlocking the Secrets of Weight LossVon EverandThe Obesity Code: Unlocking the Secrets of Weight LossBewertung: 4 von 5 Sternen4/5 (6)
- The Diabetes Code: Prevent and Reverse Type 2 Diabetes NaturallyVon EverandThe Diabetes Code: Prevent and Reverse Type 2 Diabetes NaturallyBewertung: 4.5 von 5 Sternen4.5/5 (4)
- Metabolism Revolution: Lose 14 Pounds in 14 Days and Keep It Off for LifeVon EverandMetabolism Revolution: Lose 14 Pounds in 14 Days and Keep It Off for LifeNoch keine Bewertungen
- Instant Loss On a Budget: Super-Affordable Recipes for the Health-Conscious CookVon EverandInstant Loss On a Budget: Super-Affordable Recipes for the Health-Conscious CookBewertung: 3.5 von 5 Sternen3.5/5 (2)
- The Complete Beck Diet for Life: The 5-Stage Program for Permanent Weight LossVon EverandThe Complete Beck Diet for Life: The 5-Stage Program for Permanent Weight LossBewertung: 3.5 von 5 Sternen3.5/5 (6)
- Glucose Revolution: The Life-Changing Power of Balancing Your Blood SugarVon EverandGlucose Revolution: The Life-Changing Power of Balancing Your Blood SugarBewertung: 5 von 5 Sternen5/5 (352)
- Glucose Goddess Method: A 4-Week Guide to Cutting Cravings, Getting Your Energy Back, and Feeling AmazingVon EverandGlucose Goddess Method: A 4-Week Guide to Cutting Cravings, Getting Your Energy Back, and Feeling AmazingBewertung: 5 von 5 Sternen5/5 (61)
- The Beck Diet Solution Weight Loss Workbook: The 6-Week Plan to Train Your Brain to Think Like a Thin PersonVon EverandThe Beck Diet Solution Weight Loss Workbook: The 6-Week Plan to Train Your Brain to Think Like a Thin PersonBewertung: 3.5 von 5 Sternen3.5/5 (33)
- The Diet Trap Solution: Train Your Brain to Lose Weight and Keep It Off for GoodVon EverandThe Diet Trap Solution: Train Your Brain to Lose Weight and Keep It Off for GoodNoch keine Bewertungen
- Eat Complete: The 21 Nutrients That Fuel Brainpower, Boost Weight Loss, and Transform Your HealthVon EverandEat Complete: The 21 Nutrients That Fuel Brainpower, Boost Weight Loss, and Transform Your HealthBewertung: 2 von 5 Sternen2/5 (1)
- The Stark Naked 21-Day Metabolic Reset: Effortless Weight Loss, Rejuvenating Sleep, Limitless Energy, More MojoVon EverandThe Stark Naked 21-Day Metabolic Reset: Effortless Weight Loss, Rejuvenating Sleep, Limitless Energy, More MojoNoch keine Bewertungen
- Keto Friendly Recipes: Easy Keto For Busy PeopleVon EverandKeto Friendly Recipes: Easy Keto For Busy PeopleBewertung: 3.5 von 5 Sternen3.5/5 (2)
- Rapid Weight Loss Hypnosis: Deep Sleep Your Way to Rapid Weight Loss, Healing Your Body and Self Esteem with Guided Meditations and Positive AffirmationsVon EverandRapid Weight Loss Hypnosis: Deep Sleep Your Way to Rapid Weight Loss, Healing Your Body and Self Esteem with Guided Meditations and Positive AffirmationsBewertung: 5 von 5 Sternen5/5 (7)
- Good Sugar Bad Sugar: Eat yourself free from sugar and carb addictionVon EverandGood Sugar Bad Sugar: Eat yourself free from sugar and carb addictionBewertung: 4.5 von 5 Sternen4.5/5 (29)
- Smarter Not Harder: The Biohacker's Guide to Getting the Body and Mind You WantVon EverandSmarter Not Harder: The Biohacker's Guide to Getting the Body and Mind You WantBewertung: 3.5 von 5 Sternen3.5/5 (2)
- Foods That Cause You to Lose Weight: The Negative Calorie EffectVon EverandFoods That Cause You to Lose Weight: The Negative Calorie EffectBewertung: 3 von 5 Sternen3/5 (5)
- Dr. Nowzaradan's Diet Plan: The Scales Don't Lie, People Do! The Only 1200 kcal Diet from Dr. NOW to Lose Weight Fast. 30-Day Diet PlanVon EverandDr. Nowzaradan's Diet Plan: The Scales Don't Lie, People Do! The Only 1200 kcal Diet from Dr. NOW to Lose Weight Fast. 30-Day Diet PlanNoch keine Bewertungen
- The Glucose Goddess Method: The 4-Week Guide to Cutting Cravings, Getting Your Energy Back, and Feeling AmazingVon EverandThe Glucose Goddess Method: The 4-Week Guide to Cutting Cravings, Getting Your Energy Back, and Feeling AmazingBewertung: 4.5 von 5 Sternen4.5/5 (4)
- Rapid Weight Loss Hypnosis for Women: Self-Hypnosis, Affirmations, and Guided Meditations to Burn Fat, Gastric Band, Eating Habits, Sugar Cravings, Mindfulness, and More.Von EverandRapid Weight Loss Hypnosis for Women: Self-Hypnosis, Affirmations, and Guided Meditations to Burn Fat, Gastric Band, Eating Habits, Sugar Cravings, Mindfulness, and More.Bewertung: 5 von 5 Sternen5/5 (36)
- The Whole Body Reset: Your Weight-Loss Plan for a Flat Belly, Optimum Health & a Body You'll Love at Midlife and BeyondVon EverandThe Whole Body Reset: Your Weight-Loss Plan for a Flat Belly, Optimum Health & a Body You'll Love at Midlife and BeyondBewertung: 4.5 von 5 Sternen4.5/5 (28)
- The Volumetrics Eating Plan: Techniques and Recipes for Feeling Full on Fewer CaloriesVon EverandThe Volumetrics Eating Plan: Techniques and Recipes for Feeling Full on Fewer CaloriesNoch keine Bewertungen
- The Carnivore Diet Bible: A Beginner’s Guide To Achieving Optimum Health, A Lean Body And Fast Fat LossVon EverandThe Carnivore Diet Bible: A Beginner’s Guide To Achieving Optimum Health, A Lean Body And Fast Fat LossBewertung: 5 von 5 Sternen5/5 (1)
- Extreme Weight Loss Hypnosis for Women: Powerful & Rapid Weight-Loss: Self-Hypnosis, Guided Meditations & Affirmations to Burn Fat, Look Amazing, Change Your Habits, Emotional Eating and More.Von EverandExtreme Weight Loss Hypnosis for Women: Powerful & Rapid Weight-Loss: Self-Hypnosis, Guided Meditations & Affirmations to Burn Fat, Look Amazing, Change Your Habits, Emotional Eating and More.Bewertung: 5 von 5 Sternen5/5 (28)
- Body Confidence: Venice Nutrition's 3 Step System That Unlocks Your Body's Full PotentialVon EverandBody Confidence: Venice Nutrition's 3 Step System That Unlocks Your Body's Full PotentialBewertung: 4 von 5 Sternen4/5 (2)
- Ultrametabolism: The Simple Plan for Automatic Weight LossVon EverandUltrametabolism: The Simple Plan for Automatic Weight LossBewertung: 4.5 von 5 Sternen4.5/5 (28)