Beruflich Dokumente
Kultur Dokumente
2 Cardio
Hochgeladen von
rashmi_harryOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
2 Cardio
Hochgeladen von
rashmi_harryCopyright:
Verfügbare Formate
Circulatory System
8/1/08
Human Biology 1 Circulatory System
A. Blood Vessels
1. Artery
- takes blood away from heart (may carry oxygenated or
deoxygenated blood)
- thick walls, connective tissue, withstand blood pressure
- middle layer of elastic muscle fibres expand to
accommodate rush of blood
- highest blood P
- ~120 70 mm Hg
2. Arteriole
- smaller than arteries, funnel blood to capillaries
- elastic tissue layer expands and contracts with rush of
blood
- sympathetic nervous control
- dilate or constrict diameter, which regulates blood
pressure
- from ~90 mm Hg down to ~40 mm Hg
3. Capillaries
- site of gas (and nutrient /waste) exchange
- site of immune inflammatory response
- lead off of arteriole network around tissues and
organs
- thin walls allow diffusion of nutrient, gases, and
wastes
- large surface area of network of capillaries allows for
greater exchange of nutrients and gases
- lowest velocity
- speed is inversely proportional to cross-sectional
area
- largest x-sec. area
- membrane contains lipoproteins which lower its
surface tension
- very narrow, forces RBC to move one abreast, and
therefore increase surface area for exchange
Text Diagram:
Capillary exchange
Where is the blood?
10% in the arteries
20% in the capillaries
70% in the veins
Relative Vessel Sizes:
Diameter/Wall Thickness
Aorta
2 cm bore /
2 mm thick
Artery
4 mm / 1 mm
Arteriole
50 20
Capillary
8 1
Venule
40 2
Vein
1.5 mm / 5
Vena Cava
3 cm / 1.5
(Source:
http://web.missouri.edu/~huxleyv/
Biophysics2000.html)
Relative Total Cross
Sectional Area (cm
2
)
~ 2.5 cm
2
- arteries
~ 40 cm
2
- arteriole
~2500 cm
2
- capillaries
~ 8 cm
2
- veins
(Source: Prov Exam, Aug., 2003)
Circulatory System
Human Biology 2 Circulatory System
- ~40 mm Hg arteriole end down to ~20 mm Hg
venule end
BP > Osmotic P
! fluid moves into the
ti ssues
BP < Osmotic P
! fluid moves into the
capill ary
4. Venule
- funnels blood from capillaries into veins
- very thin walls
- ~ 20 mm Hg decreasing to ~ 10 mm Hg
5. Veins
- takes blood back to heart from capillaries (to the
heart)
- valves in major veins, one way flow, prevent
backflow
Blood
Flow
Vein: Valve Mechanism
- veins act as a blood reservoir
- Lowest blood P
- ~10 mm Hg dropping to ~ 2mm Hg (or lower)
Text Diagram:
Vessel summary
Exemplar Q
How is the structure of an
arteriole related to its function?
(4 marks)
has thick walls that resist
blood pressure
has elastic fibres to allow
stretching and recoil
when the arteriole contracts,
this increases blood pressure
to the remainder of the body
endothelium layer provides
smooth surface (less friction)
for blood movement
has sphincters which control
blood flow to the capillary
beds
has smooth muscles which
control blood flow to the
capillary beds
any four for 1 mark each
(August 2006)
Circulatory System
Human Biology 3 Circulatory System
Source: http://web.missouri.edu/~huxleyv/Biophysics2000.html
Circulatory System
Human Biology 4 Circulatory System
B. Systems
System Artery Vein
Systemic
- refers to the body in
general
Oxygen-rich
(oxygenated)
CO
2
poor
CO
2
rich
(deoxygenated)
Pulmonary
- Refers to the vessels of the
lungs
CO
2
rich
(deoxygenated)
Oxygen-rich
(oxygenated)
CO
2
poor
Ftal
- Refers to the vessels of
the developing ftus
CO
2
rich
(deoxygenated)
Oxygen-rich
(oxygenated)
CO
2
poor
Source: www.medical-illustrator.co.uk/ fetal.html Copyright
Peter Gardiner 2001
X= Arteries (! arterioles)
Y= Capillaries
Z= (venules !) Veins
Circulatory System
Human Biology 5 Circulatory System
C. Major Vessels
Systemic
- Aorta
- Carotid artery, jugular vein
- Subclavian (artery and vein)
- Superior (anterior) vena cava (vein)
- Inferior (posterior) vena cava (vein)
- Hepatic vein
- Hepatic portal vein
- Mesenteric artery
- Renal (artery and vein)
- Iliac (artery and vein)
Pulmonary
- Pulmonary Trunk (artery)
- Pulmonary arteries
- Pulmonary veins
Coronary
- arteries and veins
D. Diseases of Vessels
Arteriosclerosis
- a generic term for number of diseases in which the
arterial wall thickens and loses elasticity
e.g.,
Atherosclersosis - assoc. with atheroma, a plaque
blockage
- cause: smoking, diet rich in low-density
lipoproteins (LDL the bad cholesterols) and poor
in high-density lipoproteins (HDL the good
cholesterols), lack of exercise, age
- Rx: preventative = diet, exercise, drug therapy to
lower cholesterol levels, surgery such as by-pass
and thromboplasty (vacuuming out the thrombosus
/ plaque)
Heart Attack
2/3 of all heart attacks are
caused by:
o high levels of bad
cholesterol and
o smoking.
The other top factors:
o High blood pressure
o Diabetes
o Abdominal obesity
o Stress
o Lack of daily fruits
and veges
o Lack of exercise
Text Diagram:
Arteriosclerosis
Text Diagram:
Major Vessels
Circulatory System
Human Biology 6 Circulatory System
E. The Heart
+ pericardial membrane
+ septum
1. Atrioventricular Valves (2)
- between atria and ventricles.
- tricuspid & mitral valves
- prevent blood leaking back into upper chambers of atria
2. Semi-lunar Valve (2)
- between the right ventricle and pulmonary artery, &
the left ventricle and the aorta
- pulmonary & aortic valve
- prevent backflow of blood into ventricles from the
pulmonary arteries and aorta
3. Coronary Arteries
- feed oxygen and nutrients to heart muscle.
- if they are blocked, the heart muscle will die from lack
of oxygen and nutrition (myocardial infarction)
4. Right Atria
- receives blood from head and abdomen low in oxygen
5. Left Atria
- receives oxygenated blood from the lungs via
pulmonary veins
6. Right Ventricle
- pumps blood low in oxygen through the pulmonary
trunk to the lungs
7. Left Ventricle
- pumps oxygenated blood out the aorta to the rest of the
body
- the major pump (4.5 L/min) of the heart, is the most
muscular chamber
8. Pulmonary Arteries
- attached to right ventricles
- blood low in oxygen flows through to lungs
Red Wine Myth
While there may be some
evidence to suggest older men
and post-menopausal women
may have some reduced risk
of cardiovascular disease from
light consumption (1 glass a
day), your still 40% more
likely to die of other
diseases, such as cirrhosis of
the liver, breast and other
cancers.
- Source: Am I Normal,
programme 5 - Alcohol,
http://www.bbc.co.uk/radio4/s
cience/am_i_normal_series_2.
shtml
Text Diagram:
Heart
Circulatory System
Human Biology 7 Circulatory System
9. Pulmonary Veins
- blood rich in oxygen flows through, from lungs to left
atrium
10. Chordae Tendineae
- holds valves in place, stops them from inverting
- valves between the atria and ventricles
- the heart strings
11. Septum
- wall between two sides of heart keeps oxygenated and
deoxygenated blood separated
The Heart Simplified
Pulmonary
Arteries
Pulmonary
valve
Aortic valve
r A
r V l V
Superior
Vena
Cava
Inferior
Vena
Cava
to lungs
from lungs (PV)
Pulmonary Veins
(from lungs)
Aorta
(to body)
Tricuspid
valve
Mitral
valve
Circulatory System
Human Biology 8 Circulatory System
F. Ftal Circulation
- in order (all terms refer to infant)
1. Umbilical Veins
- sends blood rich in oxygen and nutrients to the ductus
venosus in the liver of the infant from the placenta
2. Ductus Venosus (Venus Duct)
- takes blood rich in oxygen from umbilical vein and
moves it through the liver via the duct to the inferior
vena cava
3. Foramen Ovale (Oval Opening)
- opening between two atriums
- blood rich in oxygen from the mother is shunted from
right atrium to left atrium bypassing the lungs
4. Ductus Arteriosus (Arterial Duct)
- blood rich in oxygen from the pulmonary trunk (artery,
from right ventricle) moves blood across a bridge
called the ductus arteriosus to the aorta
Text Diagram:
Foetal Circulation
Circulatory System
Human Biology 9 Circulatory System
5. Umbilical Arteries
- takes blood low in oxygen from the infant to the mother
for exchange, back through the umbilical cord
Circulatory System
Human Biology 10 Circulatory System
G. The Beat goes on
- Sound
- lubb dupp or lub-dub
- Lub = blood passing through the atrioventricular
valves
- Dub = blood passing through the semi-lunar valves
- This sound comes from the valves opening and shutting on the
blood inside the heart.
- The first sound (the lub) happens when the blood hits the
mitral and tricuspid valves between the atria and ventricles.
- The next sound (the dub) happens when the blood hits the
aortic and pulmonic valves that close up after the blood has
been squeezed out of the heart and as the heart relaxes to fill
with blood for the next beat.
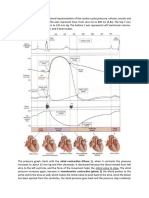
Cardiac Cycle
The events related to the
flow of blood that occur from
the beginning of one
heartbeat to the beginning of
the next.
- Wikipedia
Text Diagram:
Heart Beat
Circulatory System
Human Biology 11 Circulatory System
1. Sinoatrial Node (S-A Node)
- in dorsal wall of upper atrium
- called nodal tissues - muscular and nervous tissue
characteristics
- SA node is the pacemaker
- it initiates the heartbeat automatically
- sends impulses (as measured by an ECG /EKG) over
the atria muscle so they can contract
2. Atrioventricular Node (A-V Node)
- base of right atrium, near septum
- picks up impulse from SA node and delays it
momentarily (120 to 200 msec) to ensure the atria have
contracted fully and are about to relax,
- before the impulse is passed on thru the Bundle of
His to the purkinje fibres, and finally into the
ventricles
- the ventricles contract (systole)
3. Medulla Oblongata
- lower brain region
- control centre in brain for the heart
- connects with the autonomic nervous system and
sympathetic nervous system
- to speed heart up
- parasympathetic nervous system slows heart down
- Homoeostatic control of heart-rate
Source:
http://davidge2.umaryland.edu/~emig/ekgtu02.h
tml
This diagram correlates with
the heart drawing. The
initial inflection (purple)
corresponds to atrial
depolarization.
The large blue inflection
corresponds to ventricular
depolarization. The atrial
repolarization is buried in this
complex.
The green inflection
corresponds to ventricular
repolarization. This is a positive
inflection because the
repolarization begins at the
epicardial surface and
progresses through the
ventricular walls to the
endocardium.
Depolarization progresses from
endocardium to epicardium.
This combination of change in
direction and change in polarity
results in a double negative and
a positive inflection for
repolarization.
Circulatory System
Human Biology 12 Circulatory System
Summary of Cardiac Cycle:
When the SA node depolarizes, the action potential
(impulse) spreads throughout the atria, rapidly causing
atrial depolarization and contraction. The action potential
rapidly enters the AV node where it is delayed for 120 to
200 msec. The AV node conducts slowly because it
depends on slow inward calcium currents to depolarize
cells. The AV node also must conduct the action potential
through thin fibres which slow conduction. This delay is
deliberate and allows the ventricles time to fill following
atrial contraction.
The action potential spreads to the Bundle of His and then
to through the purkinje fibres. These rapidly depolarize
both ventricles. The left ventricle depolarizes slightly
before the right.
The cells repolarize following depolarization. Atrial
depolarization is not seen in an ECG because the higher
magnitude ventricular depolarization occurs
simultaneously. Ventricular repolarization is seen as the T
wave
Source: Introduction To EKGs
(http://davidge2.umaryland.edu/~emig/ekgtu01.html)
4. Sympathetic Nerves
Each inflection has a name and
signifies a stage in the Cardiac
(contraction) cycle.
P wave
SA node (atrial contraction)
QRS complex
Ventricular contraction
Ventricular depolarization
T wave
Ventricular filling
Ventricular repolarization
U wave
Represents final stage of
ventricular repolarization
Circulatory System
Human Biology 13 Circulatory System
- stress, speed up heart rate
- pupils dilate, blood P and respiration. incr.
- digestive activity decr.
- associated with fight or flight
5. Parasympathetic Nerves
- lowers beat rate (to normal rate)
[mnemonic: Paranormal]
H. Blood Pressure
- Pressure exerted by blood against blood vessel walls
- measured systolic pressure over diastolic pressure
Pulse
- expanding and recoiling of an arterial wall felt in any
artery that runs close to the surface of the skin, e.g.,
carotid, femoral
a. Systole
- highest arterial pressure, while heart is pumping
- ventricles are contracting to pump blood out into the
circulatory system
- systolic/diastolic (120/70 mm/Hg ave. for young male)
b. Diastole
- lowest arterial pressure
- ventricles are relaxed
- ! atrial contraction,
- the atria may contract at the same time but do
not influence BP
Circulatory System
Human Biology 14 Circulatory System
c. Normal blood pressure
- for an adult, a systole of between 110-150 is normal
- although it can be lower or higher, depending on the
individual
- an ave. of 120/70 to 140/90 is often given as a
norm (systole/diastole mm Hg)
- systolic will fluctuate with level of activity/stress
- diastolic will be 90 or lessbut should remain
constant for the individualextreme fluctuations
are danger signs
- e.g., at work: 122/80 (light exercise) to 180/80
(heavy exercise)
- e.g., at rest:114/80 (sitting) to 150/80 (playing
tennis)
Category Systolic (mm Hg) Diastolic (mm Hg)
Low (Hypotension) < 100 < 60
Normal (120/80) [120/70] < 130 < 85
High Normal 130 139 85-89
Mild Hypertension 140-159 (~145) 90-99
Moderate 160-179 (~165) 100-109
Severe 180-209 (~185) 110-119
Very Severe > 209 > 119
d. Hypertension
- high blood pressure
- mild: systole > 145
- severe: systole > 185
- causes include: hardening of arteries, diet, obesity,
hormone malfunction,
- Some Hormone examples that increase blood pressure
- ADH - release of antidiuretic hormone to increase
water reabsorption (also called vasopressin) from
the posterior pituitary gland will result in higher
blood pressure
- Adrenaline - from the adrenal medulla stimulates
flight or fight response of the sympathetic nervous
system
Circulatory System
Human Biology 15 Circulatory System
- Renin if blood sodium levels are low, renin is
released to ultimately stimulate the release of
aldosterone
- Aldosterone - from the adrenal cortex regulates
sodium level in blood, and therefore also blood
pressure, as more blood is pushed through the
kidney for reabsorpbtion of salt
- Autonomic nervous system - involuntary control
of heart glands
- Sympathetic = increase
- Incr. Heart rate = incr. BP
- Blood vessels contract = incr. BP
- Parasympathetic = decrease
- Inhibition of the sympathetic nervous
system may also raise BP
e. The Silent Killer
- 15% of adults have high blood P, and 25% of these
dont know it
f. Signs & Treatment
- morning headaches, felt at back of head; facial flushing,
ringing in ears (tinnitus), nose bleeding, shortness of
breath, frequent urination, smooth eye vessels become
inflamed
- untreated half of all cases will develop heart disease,
1/3 will die of stroke
- treatment: lifestyle (reduce stress, avoid smoking etc.),
diet (avoid excess salt, saturated fats), medication
g. Hypotension
- unusually low blood pressure (systole < 100) due to
weak pumping of the heart
I. Inflammatory Response
1. Overview
- bacteria invade tissue, toxins released attack cells
- mast cells release histamine, dilate vessel, increase
permeability of vessel
- fluid escapes the capillaries to site of invasion, area is
now inflamed
- neutrophils - enter site, squeezing through pores*,
then they phagocytize (engulf / eat) the invader
Text Diagram:
Inflammation
Text Extra readings:
Nonspecific & Specific
Defenses
Circulatory System
Human Biology 16 Circulatory System
- monocytes - arrive at site, swell into
macrophages, and engulf any bacteria
* prostaglandins are also involved here
J. The lymphatic system
- Lymph originates as blood plasma lost from the
circulatory system, which leaks out into the
surrounding tissues (interstitial spaces).
- The lymphatic system collects this interstitial
fluid by diffusion into lymph capillaries, filters it
of infection, and returns it to the circulatory system.
- preventing oedema swelling, which may
result in death as tissues are destroyed
- Once within the lymphatic system the interstitial
fluid is called lymph, and has almost the same
composition as the original interstitial fluid.
- Lymph fluid consists of a colourless, water solvent
containing amino acids, sugars, fatty acids,
coenzymes, hormones, neurotransmitters, salts, as
well as waste products from the cells while rich
in WBC (lymphocytes), both RBC and platelets are
absent (and ! colourless).
Reference: wikipedia and http://biology-pages.info
1. Overview
- Inflammation: recovers excess tissue fluid that
surrounds cells, and returns it to the main blood system
- Digestion: lacteals collect digested fat
- Immune: WBC fight infection at nodes (filters)
Extracellular Fluid
- all body fluid outside of
cells, either
o Interstitial fluid, which
bathes and surrounds the
cells, and makes up the
majority of extracellular
fluid, or
o Blood plasma, the
liquid component of
blood, in which the
WBC, RBC (and !
red), and platelets are
suspended.
Intracellular fluid
- is cytoplasm/cytosol
Text Diagram:
Lymph
Circulatory System
Human Biology 17 Circulatory System
- The lymphatic is an open system, unlike the blood
which flows within a closed loop. Muscles activity
throughout the body help to keep the lymph moving
forward (hence regular exercise = good immune
health)
a. lymph capillaries lie near capillaries to take up fluids
b. Lymph - fluid in lymph vessels
- a yellow-cream coloured fluid, rich in fat and WBC
c. lymph (vessels) veins merge to lymph ducts
- ultimately drain into subclavian vein ! superior vena
cava ! heart and back in to the blood system
d. lymph ducts have one-way valves to keep fluid moving
forward
e. lymph nodes along lymph vessels, composed of
lymphoid tissue
2. Lymph Organs
- Bone marrow
- formation of red blood cells and white blood cells
- Thymus gland is lymphoid tissue located just above
the heart, it gets smaller with age
All the lymph collected from
the entire left side of the body,
the digestive tract and the
right side of the lower part of
the body flows into a single
major lymph vessel, the
thoracic duct.
- The thoracic duct
empties about 100 ml of
lymph every hour into
the left subclavian vein.
The lymph in the right
side of the head, neck,
and chest is collected by
the right lymph duct and
empties into the right
subclavian vein.
- Source: http://biology-
pages.info
Circulatory System
Human Biology 18 Circulatory System
- functions in the maturation T-cells (lymphocyte)
- Lymph Nodes, e.g, tonsils, adenoids
- remove debris and purify lymph
- Spleen
- Node-like, but filled with blood instead of lymph
- Purifies the blood passing through (immune fcn)
K. Blood System
- total volume = 8-9% o f body mass,
- i.e., 100kg ! 8-9 kg = 8-9 L
- formation:
- red marrow
- spongy (cancellous) bone
- these are the flat bone and joints
- stem cells
1. White Cells (Leukocytes)
- produced in the red marrow of spongy bone
- larger than red blood cells
- fewer in number than reds
- lobed nucleus
- lifespan a few hours (18-36) to 14 days, but types
living 3-4 months
- amoeboid movement
- shape is amorphous
- colourless
a. Granulocytes - granules in cytoplasm and the mature
nucleus is segmented into 2-5 lobes, produced in the
red bone marrow
- phagocytic
Top: Neutrophil
Bottom: Lymphocyte
Text Diagram:
Blood Formation
Circulatory System
Human Biology 19 Circulatory System
- Neutrophils
- are important in the inflammatory process (as
phagocytes and mediators of inflammatory reactions).
- Basophils
- contain heparin and large amounts of histamine and are
active participants in hypersensitivityreactions.
- Eosinophils
- contains Major Basic Protein (MBP), known to be toxic
to several parasites (helminths, microfilariae;
schistomiasis), and some mammalian cells.
b. Agranulocytes - no granules in cytoplasm, circular or
indented nucleus, found in lymph tissue e.g. spleen
- Lymphocytes
- B-cells (antibody formation)
- T-cells (intiate, cytotoxic)
- Monocytes (macrophages)
- Phagocytes
2. Red Blood Cells (Erythrocytes)
- produced in the red marrow of spongy bone
- round and smaller than whites
- nucleus dissolves as they mature,
- hence the biconcave shape (as the cell collapses
inward)
- the nucleus is replaced by hemoglobin
- continuously produced in red bone marrow of long
bones, ends of long bones, skull and vertebrae
- carries oxygen (oxyhemoglobin HbO
2
)
- carries carbon dioxide (carbaminohemoglobin
HbCO
2
)
- buffers blood by taking up excess H
+
(reduced
hemoglobin - HHb)
- lifespan = ~3 months
- free floating
- red
3. Platelets (thrombocytes)
- v. small irregular cell fragments (of megakaryocytes,
in red bone marrow)
- fcn in blood clotting
Text Diagram:
Hemoglobin (Hb)
Erythropoietin
The kidneys make this
hormone, which stimulates
the bone (red) marrow to
make blood cells, in response
to low levels of O
2
in the
blood.
A drop of blood contains:
~5 million RBC
~10,000 WBC
~250,000 platelets
source: a student
Circulatory System
Human Biology 20 Circulatory System
4. Components of Blood
Plasma + Formed Elements (ratio) Blood =
1. Water
2. Proteins
3. Salts
4. Gases
5. Nutrients
6. Urea
7. Hormones, vitamins etc.
1. RBC (600)
2. WBC (1)
3. Platelets (40)
Text Diagram:
7
th
p 208, 8
th
p 236,
9
th
p 249, 11
th
p 227,
12
th
p 227
- Serum = plasma sans the protein fibrinogen
- Human blood is composed of 55% plasma and 45%
formed elements
- Plasma = 90% water.
- Solutes make up about 10% of the plasma volume
of which 7% are proteins.
- Albumin represents about 60% (about
40mg/ml) of the total plasma protein.
Albumin:
- A plasma protein very important in maintaining
fluid balance in the blood.
- Important in maintaining blood pressure,
regulating fatty acids, and hormone transport.
- synthesized in the liver.
Functions:
- Buffers pH
- Maintains Osmotic pressure
Circulatory System
Human Biology 21 Circulatory System
- Oncotic (colloidal osmotic) pressure in the
circulatory system is a form of osmotic pressure
exerted by proteins in blood plasma that
normally tends to pull water into the circulatory
system, i.e., oncotic pressure tends to pull
fluid into the capillaries. In conditions where
plasma proteins are reduced, e.g., from being
lost in the urine (proteinuria) or from
malnutrition, the result of low oncotic pressure
can be oedema excess fluid buildup in the
tissues.
- Transports thyroid hormones, e.g., Thyroxine
- Transports other hormones, particularly fat
soluble ones, e.g., cortisol
- Transports fatty acids ("free" fatty acids) to the
liver
- Transports unconjugated bilirubin
- RBC are destroyed in the spleen when they get
old or damaged. This releases hemoglobin,
which is broken down to heme, as the globin
parts are turned into amino acids. The heme is
then turned into unconjugated bilirubin in the
macrophages of the spleen. This unconjugated
bilirubin is not water soluble. It is then bound
to albumin and sent to the liver.
- In the liver it is conjugated with glucuronic
acid, making it soluble in water. Much of it
goes into the bile and thus out into the small
intestine.
- Transports many drugs, and serum albumin levels
can affect the half-life of drugs.
- Competitively binds calcium ions (Ca2+)
- 45% is protein bound, predominantly to
albumin, and is biologically inert
- Reference: Wikipedia
L. Blood Factors
Antigen: an agent that is foreign (i.e., non-self), and is
recognized by the immune system, often as foreign
surface-protein.
Antibody: a protein produced by lymphocytes (B-cells),
capable of identifying and binding to specific antigens
Albumin, basically is
- responsible for much of the
plasma colloidal osmotic
pressure and
- serves as a transport
protein carrying large
organic anions such as fatty
acids, bilirubin and many
drugs;
- also carries certain
hormones such as cortisol
and thyroxine when their
specific binding globulins
are saturated;
- and may act as a buffer.
Circulatory System
Human Biology 22 Circulatory System
1. Human Blood Types: ABO
- the A-B-O system is a means of classifying blood
according to the antigens located on the surface of the
erythrocytes (antigens are substance located on cells that
stimulate the production of antibodies)
TYPE: A
Antigen on RBC: A
Antibodies in Plasma: anti-B
Can get blood from: O, A
Can give blood to: A, AB
TYPE: B
Antigen on RBC: B
Antibodies in Plasma: anti-A
Can get blood from: O, B
Can give blood to: B, AB
TYPE: AB
Antigen on RBC: A & B on each RBC
Antibodies in Plasma: None
Can get blood from: O, A, B, AB
Can give blood to: AB
TYPE: O
Antigen on RBC: none
Antibodies in Plasma: anti-B, anti-A
Can get blood from: O
Can give blood to: O, A, B, AB
- Blood type O is a universal donor
- because O has no antigens attached to its surface for
the recipients antibodies to identify, therefore it can be
given to practically anyone
- AB is the universal acceptor
- because has A and B antigens but no antibodies, so can
receive all blood types
2. Rhesus factor
- the Rh factor is another type of blood antigen (antigen-
D). Eighty-five percent of the North American
population is Rh-positive (Rh
+
), meaning that they
Text Diagram:
ABO
Source:
http://anthro.palomar.edu/synt
hetic/synth_5.htm
Circulatory System
Human Biology 23 Circulatory System
have Rh antigens. A person without antigens in their
blood is Rh-negative (Rh
-
)
- if Rh
+
blood is given to an Rh
-
person, antibodies to
the Rh antigen will react with the antigen and
agglutination will occur
Rh Disease:
aka Erythroblastosis fetalis / Hemolytic disease
- when the mother is Rh
-
and father Rh
+
;
- the child may inherit Rh
+
allele; because mother and
child blood supplies are separate only a little mixing of
material occurs-usually at birth; subsequently the
mother develops antibodies to the Rh factor; if a
second Rh
+
child is conceived, serious damage may
occur as the mothers antibodies attack the childs
blooda condition called erythroblastosis fetalis
- ! is to give the Rh
-
mother anti-Rh antibodies,
these will destroy any Rh antigen in her blood
before her body produces any antibodies (Win-Rho
in Canada, and Rho-gram in the US)
- Doctor will discuss afore hand, as these drugs
may be associated with an increase risk of
cancer
3. Blood typing test
- look for agglutination to indicate type, e.g., if the blood
sample containing the anti-B compound (which mimics
antibody B in the blood) agglutinates then blood type is
B
- a second example: - only anti-Rh has agglutinated
anti-A anti-B anti-Rh
= blood type O
+
Text Diagram:
Hemolytic Disease
Text Diagram:
Blood Typing
Winnipeg, Manitoba1950s
- Bruce Chown (b-Winnipeg)
and John Bowman (b-
Winnipeg) developed
'WinRho', the serum that
prevents erythroblastosis
fetalis.
The mother is given
antibodies/immunoglobins
that mop up any Rh antigens,
before the mothers immune
system has time to produce
her own antibodies, thus she
never develops an immune
response, and may go on to
have more children if she so
desires.
Circulatory System
Human Biology 24 Circulatory System
M. Blood Clot
1. Overview
- clotting factors are always in the blood; platelets,
prothrombin (a globular protein) and fibrinogen
platelets clump at site of puncture
injured tissues release the enzyme (catalysis)
prothrombin activator (thromboplastin)
that converts prothrombin (a protein in the blood
plasma, which requires vitamin K to synthesize) to
thrombin (in the presence of Ca
2+
)
this in turn acts as an enzyme on fibrinogen (another
blood protein)
splitting it into long threads of fibrin
this serves as a framework to hold patch together
1. Platelets + Damaged cells " thromboplastin
2. thromboplastin + Prothrombin " thrombin
3. thrombin + Fibrinogen " fibrin
4. Fibrin + cells + dried serum = blood clot
- vitamin K (mostly produced by E. coli in the colon) is
necessary for the production of prothrombin (by the liver)
- absence of results in uncontrolled hemorrhage
N. Bloods a Rover
1. At the lungs
- oxygen diffuses out the alveoli to red blood cells
- oxygen combines with reduced hemoglobin to form
oxyhemoglobin and H
+
ions
A pO
2
of 100% = 4
molecules of O
2
per RBC/Hb
Text Diagram:
Clot
Student 3: Shows a positive
response of the control,
indicating that something is
wrong with this test it is
possibly contaminated, and
therefore the results are
unreadable, i.e., blood type is
unknown.
Students 1, 2, & 4: Show a
negative (nothing unexpected
has happened) response of
the control, indicating these
blood tests should be
accurate.
Circulatory System
Human Biology 25 Circulatory System
- freed H
+
combines with HCO
3
-
and forms H
2
O + CO
2
,
the carbon dioxide released from the bicarbonate ion
diffuses into the lungs
- H
+
not accumulated is released from HHb
(hemoglobin) and combines with the HCO
3
-
which
releases CO
2
- Hemoglobin is a carrier for O
2
, CO
2
, and H
+
.
2. At the tissues
- CO
2
produced in the cells of tissues diffuses into blood
- blood cells contain carbonic anhydrase to accelerate
reaction
- CO
2
combines with H
2
O, to form CO
2
, HCO
3
-
and
H
+
.
- H
+
taken up by Hb (hemoglobin sans H
+
)
- O
2
is released as a result
3. Carbonic Anhydrase
- enzyme within red blood cells, that facilitates the
conversion of CO
2
+ H
2
O to and from H
+
+ HCO
3
-
,
i.e.,
CO
2
+ H
2
O " H
2
CO
3
" H
+
+ HCO
3
-
at the tissues
(internal respiration)
H
+
+ HCO
3
-
" H
2
CO
3
" CO
2
+ H
2
O at the lungs
(external respiration)
- CO
2
transport:
- ~70% via HCO
3
-
- ~25% via Hemoglobin
- ~5% dissolved in the blood
4. Hydrogen Ions
- produced when hemoglobin binds with oxygen at the
lungs
- produced when carbon dioxide combines with water at
the tissues
5. Hemoglobin (Hb
-
)
- iron containing quaternary protein (globin)
- carries oxygen in blood, oxyhemoglobin (HbO
2
)
Circulatory System
Human Biology 26 Circulatory System
- buffer, picks up H
+
ions, reduced hemoglobin
(HHb)
- carries CO
2
, carbaminohemoglobin (HbCO
2
)
Das könnte Ihnen auch gefallen
- Human Circulatory SystemDokument114 SeitenHuman Circulatory Systempeterr1022100% (1)
- Human Body Book | Introduction to the Vascular System | Children's Anatomy & Physiology EditionVon EverandHuman Body Book | Introduction to the Vascular System | Children's Anatomy & Physiology EditionNoch keine Bewertungen
- CHP 05 (Blood and Circulation) DrRiyadAhmed PC 3Dokument69 SeitenCHP 05 (Blood and Circulation) DrRiyadAhmed PC 3Kamrun NaherNoch keine Bewertungen
- Human Body Book | Introduction to the Circulatory System | Children's Anatomy & Physiology EditionVon EverandHuman Body Book | Introduction to the Circulatory System | Children's Anatomy & Physiology EditionNoch keine Bewertungen
- Cardiovascular and Syrculation System, 2013Dokument92 SeitenCardiovascular and Syrculation System, 2013Santi Purnama SariNoch keine Bewertungen
- Cardiovascular System: Iii. Anatomy and PhysiologyDokument7 SeitenCardiovascular System: Iii. Anatomy and PhysiologyYam Bite-Size FabelloNoch keine Bewertungen
- Chapter 42 Reading GuideDokument5 SeitenChapter 42 Reading GuideCaleb SchantzNoch keine Bewertungen
- Pregnancy Induced HypertensionDokument7 SeitenPregnancy Induced HypertensionRalph Emerson RatonNoch keine Bewertungen
- Introduction To The CvsDokument43 SeitenIntroduction To The CvsParmesh PandeyNoch keine Bewertungen
- Cardiovascular System Lecture 1 2020 2021Dokument5 SeitenCardiovascular System Lecture 1 2020 2021olawandeilo123Noch keine Bewertungen
- 6th Lecture Human Anatomy and PhysiologyDokument8 Seiten6th Lecture Human Anatomy and PhysiologyDwnya S HasanNoch keine Bewertungen
- AcknowledgementDokument9 SeitenAcknowledgementJovin AshickNoch keine Bewertungen
- Cardiovascular System PPT FeDokument26 SeitenCardiovascular System PPT FeAngel Grace GaliasNoch keine Bewertungen
- Biology Form 5 Notes Chapter 1Dokument39 SeitenBiology Form 5 Notes Chapter 1Mayghen SelvanayagamNoch keine Bewertungen
- Science Form 3: Chapter 2 Blood Circulation and TransportDokument39 SeitenScience Form 3: Chapter 2 Blood Circulation and TransportNadzirah RedzuanNoch keine Bewertungen
- Pulmonary and Cardio SystemDokument7 SeitenPulmonary and Cardio SystemEduardo Niepes Jr.Noch keine Bewertungen
- Medical Science Part 2Dokument21 SeitenMedical Science Part 2Gauge FalkNoch keine Bewertungen
- Transport in AnimalsDokument12 SeitenTransport in AnimalsJedidiah DickNoch keine Bewertungen
- Pregnancy Induced HypertensionDokument9 SeitenPregnancy Induced HypertensionRiazell Antonio DungcaNoch keine Bewertungen
- Cardiovascularsystem 090820055728 Phpapp02Dokument75 SeitenCardiovascularsystem 090820055728 Phpapp02muhammad ijazNoch keine Bewertungen
- Circulatory System of MammalsDokument10 SeitenCirculatory System of Mammalsben-jNoch keine Bewertungen
- احلام 1 PDFDokument7 Seitenاحلام 1 PDFEhab Alaa Abd Al-AmeerNoch keine Bewertungen
- BloodDokument70 SeitenBloodTheophilus BaidooNoch keine Bewertungen
- Cardiovascular System BSN 1Dokument16 SeitenCardiovascular System BSN 1Arianne Jen GenotivaNoch keine Bewertungen
- Anatomy and PhysiologyDokument6 SeitenAnatomy and PhysiologyJulianne B. Dela CruzNoch keine Bewertungen
- Circulatory SystemDokument6 SeitenCirculatory SystemRatiram LilhareNoch keine Bewertungen
- Cardiovascular System: Presented by DR Aparna Ramachandran Mds 1 Dept of Public Health DentistryDokument73 SeitenCardiovascular System: Presented by DR Aparna Ramachandran Mds 1 Dept of Public Health DentistryAparna RamachandranNoch keine Bewertungen
- CardiovascularDokument92 SeitenCardiovascularRolinette DaneNoch keine Bewertungen
- Animals Part 1Dokument129 SeitenAnimals Part 1黄心怡Noch keine Bewertungen
- القلبDokument11 SeitenالقلبNajwa AbdualgaderNoch keine Bewertungen
- Chapter 14.1 - Cardiovascular System - Blood VesselsDokument56 SeitenChapter 14.1 - Cardiovascular System - Blood VesselsMichael PeraltaNoch keine Bewertungen
- About The Circulatry System 001Dokument46 SeitenAbout The Circulatry System 001gaboelgaNoch keine Bewertungen
- Circulatory System Vascular TissueDokument8 SeitenCirculatory System Vascular TissueDrSachin SrivastavaNoch keine Bewertungen
- Circulatory Word OfficeDokument6 SeitenCirculatory Word OfficeMaria Christina CaceresNoch keine Bewertungen
- Circulatory SystemDokument12 SeitenCirculatory SystemDipanshu JoshiNoch keine Bewertungen
- 2122 VesselsDokument70 Seiten2122 Vesselsapi-285078865Noch keine Bewertungen
- Circulation: Biology: Concepts & ConnectionsDokument66 SeitenCirculation: Biology: Concepts & ConnectionsGlen MangaliNoch keine Bewertungen
- NPTE CArdio NotesDokument27 SeitenNPTE CArdio NotesAubrey Vale SagunNoch keine Bewertungen
- SystemDokument63 SeitenSystemBeth Rubin RelatorNoch keine Bewertungen
- Cardio & LymphaticDokument13 SeitenCardio & LymphaticJoan GalarceNoch keine Bewertungen
- Bio Psychology Notes 2Dokument8 SeitenBio Psychology Notes 2Zubin Jammaa FulaniNoch keine Bewertungen
- Circulatory SysDokument10 SeitenCirculatory SysnaviNoch keine Bewertungen
- Cardiovascular SystemDokument12 SeitenCardiovascular Systemyousaf Murad khurramNoch keine Bewertungen
- Circulatory System Cardiovascular and LymphaticDokument60 SeitenCirculatory System Cardiovascular and LymphaticJJ AlmagroNoch keine Bewertungen
- Pregnancy Induced Hypertension (PIH) Is A Condition in WhichDokument9 SeitenPregnancy Induced Hypertension (PIH) Is A Condition in WhichmelwuaniehNoch keine Bewertungen
- Cardiovascular System F1Dokument56 SeitenCardiovascular System F1sunilNoch keine Bewertungen
- Circulatory SystemDokument111 SeitenCirculatory SystemYounas Bhatti100% (1)
- Blood CirculationDokument8 SeitenBlood CirculationnorafidaishakNoch keine Bewertungen
- Cardiovascular SystemDokument14 SeitenCardiovascular SystemAthena Huynh100% (1)
- Cardiovascular SystemDokument10 SeitenCardiovascular SystemDhea BugnaNoch keine Bewertungen
- Cardiovascular System - Kd13Dokument63 SeitenCardiovascular System - Kd13Alyssa Curry BroderickNoch keine Bewertungen
- Biology Chapter 10Dokument9 SeitenBiology Chapter 10wongchengen2006Noch keine Bewertungen
- Circulatory SystemDokument44 SeitenCirculatory SystemAdonai Jireh Dionne BaliteNoch keine Bewertungen
- Cardiovascular and Circulatory SystemDokument29 SeitenCardiovascular and Circulatory SystemfayeleechaiyapornkulNoch keine Bewertungen
- The Circulatory System: Agriscience 332 Animal Science #8646-A TEKS: (C) (2) (A) and (C) (2) (B)Dokument111 SeitenThe Circulatory System: Agriscience 332 Animal Science #8646-A TEKS: (C) (2) (A) and (C) (2) (B)brdaisyNoch keine Bewertungen
- Cardiovascular SystemDokument5 SeitenCardiovascular SystemDaniel PancuNoch keine Bewertungen
- Circulatory SystemDokument13 SeitenCirculatory System2015.562fatimazaherakhanumNoch keine Bewertungen
- Anatomy3 ParamedicalDokument34 SeitenAnatomy3 ParamedicalAtik YadavNoch keine Bewertungen
- Presidium Indirapuram Students Handout-3 Grade X (Biology) Chapter: Life Processes Topic: TransportationDokument8 SeitenPresidium Indirapuram Students Handout-3 Grade X (Biology) Chapter: Life Processes Topic: TransportationSaniya nebNoch keine Bewertungen
- Investigating Effect of Concentration On The Activity of TrypsinDokument4 SeitenInvestigating Effect of Concentration On The Activity of Trypsinrashmi_harryNoch keine Bewertungen
- Guidance Notes: in General You Should Be Able ToDokument3 SeitenGuidance Notes: in General You Should Be Able Torashmi_harryNoch keine Bewertungen
- Write-Up Rubric ChecklistDokument1 SeiteWrite-Up Rubric Checklistrashmi_harryNoch keine Bewertungen
- Enzymes: The Spit Lab: Teacher VersionDokument9 SeitenEnzymes: The Spit Lab: Teacher Versionrashmi_harryNoch keine Bewertungen
- ISC Specimen 2015 Biology Paper 2Dokument5 SeitenISC Specimen 2015 Biology Paper 2rashmi_harryNoch keine Bewertungen
- Lab 1: The Microscope (10 Points) : Exercise 1.1: Microscope Structure and FunctionDokument12 SeitenLab 1: The Microscope (10 Points) : Exercise 1.1: Microscope Structure and Functionrashmi_harryNoch keine Bewertungen
- Product Catalog EnglishDokument32 SeitenProduct Catalog Englishrashmi_harryNoch keine Bewertungen
- Food Tests: A. Benedict's Test For Reducing SugarsDokument3 SeitenFood Tests: A. Benedict's Test For Reducing Sugarsrashmi_harryNoch keine Bewertungen
- The Microscope: Summary of ExerciseDokument18 SeitenThe Microscope: Summary of Exerciserashmi_harryNoch keine Bewertungen
- Macromolecules LabDokument21 SeitenMacromolecules Labrashmi_harryNoch keine Bewertungen
- x4 Objective x10 Objective x40 Objective x100 ObjectiveDokument1 Seitex4 Objective x10 Objective x40 Objective x100 Objectiverashmi_harryNoch keine Bewertungen
- Soil ExperimentsDokument32 SeitenSoil Experimentsrashmi_harry100% (1)
- Nosepiece, Which Allow The Selection of Objectives of Different Magnifications. TheseDokument8 SeitenNosepiece, Which Allow The Selection of Objectives of Different Magnifications. Theserashmi_harryNoch keine Bewertungen
- Variables WorksheetDokument2 SeitenVariables Worksheetrashmi_harry0% (2)
- Student Record AS/A Level Biology Candidate NameDokument2 SeitenStudent Record AS/A Level Biology Candidate Namerashmi_harryNoch keine Bewertungen
- Practical Support 9: Size and ScaleDokument3 SeitenPractical Support 9: Size and Scalerashmi_harryNoch keine Bewertungen
- Investigating The Presence of Proteins, Carbohydrates and Fats in Different FoodsDokument4 SeitenInvestigating The Presence of Proteins, Carbohydrates and Fats in Different Foodsrashmi_harryNoch keine Bewertungen
- Bio NotesDokument71 SeitenBio Notesrashmi_harryNoch keine Bewertungen
- Cell Resp1 PaxsonDokument9 SeitenCell Resp1 Paxsonrashmi_harryNoch keine Bewertungen
- Biology Lab ReportDokument17 SeitenBiology Lab Reportrashmi_harryNoch keine Bewertungen
- 10 Acids and AlkalisDokument5 Seiten10 Acids and Alkalisrashmi_harry100% (1)
- 8 States of MatterDokument4 Seiten8 States of Matterrashmi_harryNoch keine Bewertungen
- 9 Properties of MatterDokument16 Seiten9 Properties of Matterrashmi_harryNoch keine Bewertungen
- Igcse Methodist High School Class Viii D Unit Test 3 Practical Chemistry (10) BIOLOGYDokument3 SeitenIgcse Methodist High School Class Viii D Unit Test 3 Practical Chemistry (10) BIOLOGYrashmi_harryNoch keine Bewertungen
- PH32 Exp-9qfrDokument2 SeitenPH32 Exp-9qfrMello DiaxNoch keine Bewertungen
- Operating Manual For TENSmed 911 & 931 by ENRAF NONIUSDokument39 SeitenOperating Manual For TENSmed 911 & 931 by ENRAF NONIUSJAY2222QNoch keine Bewertungen
- Healthy Juices: Carrot + Ginger + AppleDokument9 SeitenHealthy Juices: Carrot + Ginger + AppleGertrude QuaicoeNoch keine Bewertungen
- Cardiovascular SystemDokument26 SeitenCardiovascular SystemRismawatiNoch keine Bewertungen
- The Wiggers DiagramDokument2 SeitenThe Wiggers DiagramKuro ShiroNoch keine Bewertungen
- Ebook Electrocardiography For Healthcare Professionals Ise Paperback PDF Full Chapter PDFDokument67 SeitenEbook Electrocardiography For Healthcare Professionals Ise Paperback PDF Full Chapter PDFkenneth.bell482100% (26)
- Management of Patients With Special NeedsDokument4 SeitenManagement of Patients With Special NeedsSophia MolinaNoch keine Bewertungen
- Beyond Thrombocytopaenia, Haemorrhage and Shock: The Expanded Dengue SyndromeDokument11 SeitenBeyond Thrombocytopaenia, Haemorrhage and Shock: The Expanded Dengue SyndromePawan MishraNoch keine Bewertungen
- What Is The Ideal Cholesterol Level by Joel Fuhrman MDDokument4 SeitenWhat Is The Ideal Cholesterol Level by Joel Fuhrman MDDrRod SmithNoch keine Bewertungen
- Assessment of Pulmonary Edema: Principles and PracticeDokument14 SeitenAssessment of Pulmonary Edema: Principles and PracticeJeanPandieNoch keine Bewertungen
- Short Answer Questions in AnaesthesiaDokument134 SeitenShort Answer Questions in AnaesthesiaGlen Item92% (13)
- Types of Anesthesia and Your AnesthesiologistDokument3 SeitenTypes of Anesthesia and Your AnesthesiologistYamSomandarNoch keine Bewertungen
- English Speaking Material For Nursing StudentsDokument67 SeitenEnglish Speaking Material For Nursing StudentsJodi WijayaNoch keine Bewertungen
- 114 Final Brain Dump Part 2Dokument8 Seiten114 Final Brain Dump Part 2kelsey jacksonNoch keine Bewertungen
- Blood Is Thicker Than WaterDokument4 SeitenBlood Is Thicker Than WateraontreochNoch keine Bewertungen
- Tao of Balanced Diet: Regular Food Diet For Health and BeautyDokument26 SeitenTao of Balanced Diet: Regular Food Diet For Health and Beautycoquizzz100% (1)
- Circulatory System 1 QPDokument14 SeitenCirculatory System 1 QPlucyNoch keine Bewertungen
- Voice of Health FinalDokument80 SeitenVoice of Health FinalrajuhungudkarNoch keine Bewertungen
- Tachycardia PDFDokument2 SeitenTachycardia PDFubaidillah ubaiNoch keine Bewertungen
- Krok 2 2002-2003 TherapyDokument41 SeitenKrok 2 2002-2003 TherapyAli ZeeshanNoch keine Bewertungen
- Cardiovascular and Respiratory SystemDokument51 SeitenCardiovascular and Respiratory SystemAlexi Nicole CastaloneNoch keine Bewertungen
- Jurnal 4 Uji Jalan 6 MenitDokument10 SeitenJurnal 4 Uji Jalan 6 MenitSandy Tama Okvan YudhaNoch keine Bewertungen
- Course HeroDokument17 SeitenCourse HeroBalNoch keine Bewertungen
- Pericardial DX Endocarditis MyocarditisDokument63 SeitenPericardial DX Endocarditis MyocarditisIrfan Ners MaulanaNoch keine Bewertungen
- A Case Study On Hypertensive Urgency - Group 2 Section 3BDokument48 SeitenA Case Study On Hypertensive Urgency - Group 2 Section 3BhernandezmarianneroseNoch keine Bewertungen
- 004 LabsDiagnosticsManualDokument64 Seiten004 LabsDiagnosticsManualRaju Niraula100% (1)
- Conduct of Physical Examination RemindersDokument23 SeitenConduct of Physical Examination RemindersJazer DairoNoch keine Bewertungen
- CH17 Cardiac Surgery in The Adult 5th Edition 2018Dokument26 SeitenCH17 Cardiac Surgery in The Adult 5th Edition 2018ChengShiun ShiueNoch keine Bewertungen
- Hodder Science-Stage-6-answersDokument11 SeitenHodder Science-Stage-6-answersjean wongNoch keine Bewertungen
- Artificial HeartDokument108 SeitenArtificial HeartAlaa EmadNoch keine Bewertungen
- Return of the God Hypothesis: Three Scientific Discoveries That Reveal the Mind Behind the UniverseVon EverandReturn of the God Hypothesis: Three Scientific Discoveries That Reveal the Mind Behind the UniverseBewertung: 4.5 von 5 Sternen4.5/5 (52)
- The Rise and Fall of the Dinosaurs: A New History of a Lost WorldVon EverandThe Rise and Fall of the Dinosaurs: A New History of a Lost WorldBewertung: 4 von 5 Sternen4/5 (597)
- Why We Die: The New Science of Aging and the Quest for ImmortalityVon EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityBewertung: 4 von 5 Sternen4/5 (5)
- A Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsVon EverandA Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsBewertung: 4.5 von 5 Sternen4.5/5 (6)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisVon EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisBewertung: 3.5 von 5 Sternen3.5/5 (2)
- Gut: the new and revised Sunday Times bestsellerVon EverandGut: the new and revised Sunday Times bestsellerBewertung: 4 von 5 Sternen4/5 (393)
- Buddha's Brain: The Practical Neuroscience of Happiness, Love & WisdomVon EverandBuddha's Brain: The Practical Neuroscience of Happiness, Love & WisdomBewertung: 4 von 5 Sternen4/5 (216)
- 10% Human: How Your Body's Microbes Hold the Key to Health and HappinessVon Everand10% Human: How Your Body's Microbes Hold the Key to Health and HappinessBewertung: 4 von 5 Sternen4/5 (33)
- The Molecule of More: How a Single Chemical in Your Brain Drives Love, Sex, and Creativity--and Will Determine the Fate of the Human RaceVon EverandThe Molecule of More: How a Single Chemical in Your Brain Drives Love, Sex, and Creativity--and Will Determine the Fate of the Human RaceBewertung: 4.5 von 5 Sternen4.5/5 (517)
- Masterminds: Genius, DNA, and the Quest to Rewrite LifeVon EverandMasterminds: Genius, DNA, and the Quest to Rewrite LifeNoch keine Bewertungen
- Gut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)Von EverandGut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)Bewertung: 4 von 5 Sternen4/5 (411)
- Tales from Both Sides of the Brain: A Life in NeuroscienceVon EverandTales from Both Sides of the Brain: A Life in NeuroscienceBewertung: 3 von 5 Sternen3/5 (18)
- All That Remains: A Renowned Forensic Scientist on Death, Mortality, and Solving CrimesVon EverandAll That Remains: A Renowned Forensic Scientist on Death, Mortality, and Solving CrimesBewertung: 4.5 von 5 Sternen4.5/5 (397)
- Undeniable: How Biology Confirms Our Intuition That Life Is DesignedVon EverandUndeniable: How Biology Confirms Our Intuition That Life Is DesignedBewertung: 4 von 5 Sternen4/5 (11)
- Seven and a Half Lessons About the BrainVon EverandSeven and a Half Lessons About the BrainBewertung: 4 von 5 Sternen4/5 (110)
- The Ancestor's Tale: A Pilgrimage to the Dawn of EvolutionVon EverandThe Ancestor's Tale: A Pilgrimage to the Dawn of EvolutionBewertung: 4 von 5 Sternen4/5 (812)
- Who's in Charge?: Free Will and the Science of the BrainVon EverandWho's in Charge?: Free Will and the Science of the BrainBewertung: 4 von 5 Sternen4/5 (65)
- The Other Side of Normal: How Biology Is Providing the Clues to Unlock the Secrets of Normal and Abnormal BehaviorVon EverandThe Other Side of Normal: How Biology Is Providing the Clues to Unlock the Secrets of Normal and Abnormal BehaviorNoch keine Bewertungen
- Lymph & Longevity: The Untapped Secret to HealthVon EverandLymph & Longevity: The Untapped Secret to HealthBewertung: 4.5 von 5 Sternen4.5/5 (13)
- The Lives of Bees: The Untold Story of the Honey Bee in the WildVon EverandThe Lives of Bees: The Untold Story of the Honey Bee in the WildBewertung: 4.5 von 5 Sternen4.5/5 (44)
- The Consciousness Instinct: Unraveling the Mystery of How the Brain Makes the MindVon EverandThe Consciousness Instinct: Unraveling the Mystery of How the Brain Makes the MindBewertung: 4.5 von 5 Sternen4.5/5 (93)
- Moral Tribes: Emotion, Reason, and the Gap Between Us and ThemVon EverandMoral Tribes: Emotion, Reason, and the Gap Between Us and ThemBewertung: 4.5 von 5 Sternen4.5/5 (115)
- Why We Sleep: Unlocking the Power of Sleep and DreamsVon EverandWhy We Sleep: Unlocking the Power of Sleep and DreamsBewertung: 4.5 von 5 Sternen4.5/5 (2083)
- Good Without God: What a Billion Nonreligious People Do BelieveVon EverandGood Without God: What a Billion Nonreligious People Do BelieveBewertung: 4 von 5 Sternen4/5 (66)