Beruflich Dokumente
Kultur Dokumente
National Rural Health Mission (2005-2012)
Hochgeladen von
Alviro Cosseme0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
35 Ansichten39 Seitende
Originaltitel
nrhm_ap
Copyright
© © All Rights Reserved
Verfügbare Formate
PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldende
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
35 Ansichten39 SeitenNational Rural Health Mission (2005-2012)
Hochgeladen von
Alviro Cossemede
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 39
1
National Rural Health Mission
(2005-2012)
(Reaching affordable, quality health care to the
poorest households in the remotest regions)
2
About NHRM
Inaugurated on April 12, 2005
Correct the deficiencies of the health system
Increase spending on health from 0.9% of
GDP to 2-3% of GDP
Focus on 18 states northern and eastern
Good decentralized healthcare
Missionary approach
Intended for 2005 - 2012
3
Action Points
Provision of health activist in each village
Village health plan prepared through
panchayat involvement
Strengthening of rural hospitals
Integration of vertical health programs
(leprosy, TB, malarial programs, etc.) and
traditional medicine
Integration of plans at different levels
New health financing mechanisms
4
Major Stakeholders
Accredited Social Health Activist (ASHA)
Auxiliary Nurse Midwife and Anganwadi
worker
Panchayati Raj Institutions and NGOs
District Administration
State Governments
5
NRHM in Andhra Pradesh
Number of Sub-centres 12522
Number PHCs 1570
Number 24-hrs MCH Centres 800
Community Health Centres 167
District Hospital under APVVP 19
Area Hospital under APVVP 58
Teaching Hospitals 11
AP Profile
Estimated Population as on 1.10.2007 837.08 lakhs
0-5 years children 93.73 lakhs
Density of population ... 277 per sq km
Sex Ratio (Females/ 1000 males) ... 978
Literacy Rate
Total 60.47%
Male 73.32%
Female 50.43%
7
Health Profile
Rural area:
Number of Sub-centres 12522
Number PHCs 1570
Number 24-hrs MCH Centres 800
Urban area:
Post Partum Units 82
Urban Family Welfare Centres 131
Urban Health Centres 192
Community Health Centres 167
District Hospital under APVVP 23
Area Hospital under APVVP 57
Teaching Hospitals 11
8
Present Scenario
Andhra Pradesh is the fifth largest State in India
both in terms of geographical area and
population.
The State has a total population of 8.37 crores.
Since its formation in 1956, the State has made
considerable progress in various health indicators.
As a result of various health policies and National
Programs there has been considerable
improvement in the general health status of the
population
9
Achievements under
Achievements under
Key Indicators
Key Indicators
10
Infant Mortality Rate
77
64
56
0
10
20
30
40
50
60
70
80
SRS 1983 SRS 1993 SRS 2006
Infants Deaths / 1000 live births
11
Maternal Mortality Rate
417
341
195
0
50
100
150
200
250
300
350
400
450
1992-93 1998-99 2001-03
Per 1 lakh live births
1992-93 & 1998-99 Estimates by IIHFW
2001-03 SRS (2001-03)
12
Total Fertility Rate
3.2
2.5
2.0
0
0.5
1
1.5
2
2.5
3
3.5
SRS 1983 SRS 1993 SRS 2005
Children per women
13
Full Immunization
45
59
71.4
0
10
20
30
40
50
60
70
80
NFHS-1 (1992-93) NFHS-2 (1998-99) EC Survey 2003
%
14
Antenatal Care visits
75.3
80.2
86
65
70
75
80
85
90
NFHS-1 (1992-93) NFHS-2 (1998-99) NFHS-3 (2005-06)
Mothers who had at least 3 antenatal care visits for their last birth (%)
15
Institutional Deliveries
34.3
49.8
68.6
0
10
20
30
40
50
60
70
NFHS-1 (1992-93) NFHS-2 (1998-99) NFHS-3 (2005-06)
%
16
Sex Ratio
975
972
978
969
970
971
972
973
974
975
976
977
978
1981 1991 2001
Census
17
Life Expectancy at Birth
61.55
63.74
62.79
65
63.92
66.16
59
60
61
62
63
64
65
66
67
1996-2001 2001-2006 2006-2011
Male Female
(
I
n
Y
e
a
r
s
)
18
Expected outcomes
Indicator NRHM
by 2012
Present status AP
target
India AP
IMR (per 1000 live births) 30 57* 56* 30
MMR (per 1,00,000 live births) 100 301# 195# 100
TFR (children per women) 2.1 2.9** 2.0** 1.5
* SRS (2006) ** SRS (2005) # SRS (2001-03)
Achieve a cure rate (TB - DOTS) of 85% by 2012
Reduce prevalence rate of Leprosy to 0.43 per 10,000 by 2012
Increase Cataract operations to 6 lakhs per annum by 2012
(AP).
Reduce Malaria Mortality Rate to 60% by 2012 (No deaths
reported in 2006-07)
Reduce Filaria / Microfilaria rate to 80% by 2012.
19
Major Interventions
All 70,700 ASHA workers are placed.
Village Health & Sanitation Committees are formed in
all 21,916 Gram Pam of the state.
93.78% (1704 / 1817) of the Hospital Development
Committees registered and established.
12.36 lakh beneficiaries benefited through Janani
Suraksha Yoajana scheme since Nov-2005.
151 FRUs strengthened as CEMONC centres.
Out of 1570 PHCs, 50% of PHCs strengthened as
24-hrs MCH centres.
Rural Emergency Health Transport Scheme successfully
implemented through EMRI (108).
Health Information Help Line setup for information,
advise and guidance on any health emergency (104).
20
Accredited Social Health Activist (ASHA)
ASHA to act as health resource person-of-first-resort in all
maternal and child health matters, and to act as link-person
between the community and the service providers.
ASHA would act as a bridge between the ANM and the village
and be accountable to the Panchayat.
The ASHAs will receive performance-based incentives for
promoting universal immunization, referral and escort
services for Reproductive & Child Health and other healthcare
programmes, and construction of household toilets.
70,700 ASHAs identified and selected
All 70,700 ASHA workers are placed (55,400 in rural areas;
5,300 in urban areas & 10,000 in tribal areas)
Refresher training started for the trained ASHA workers.
Last Tuesday of every month being observed as ASHA day for
effective monitoring and ensuring timely payment of
incentives.
21
Janani Suraksha Yojana scheme
The Janani Suraksha Yojana (JSY) scheme launched on 1
st
Nov-2005
The JSY is a safe motherhood intervention under the National Rural
Health Mission.
The objective is to promote institutional deliveries and reduce
maternal and infant mortality.
2006-07 5.05 lakh beneficiaries are benifited
2007-08 5.63 lakh beneficiaries are benefited
Under the scheme, Rs.1000/- (Rs.700/- under JSY (GOI) + Rs.300/-
under Sukhibhava (State) scheme) is being paid to Rural BPL Woman
who delivers in any hospital (Govt. or Private) towards transport and
incidental expenses.
From 1
st
April 2006, JSY has been extended to BPL urban families
also and Rs.600/- cash assistance will be paid to such eligible
pregnant woman of urban areas who comes to Govt. Hospitals and
Private Health Institutions in Urban Areas for delivery Services.
22
JSY Eligible conditions
The following are the eligibility conditions for pregnant women
to be covered under the Scheme:
Belongs to a Rural/Urban BPL family.
She is above 19 years at the time of the delivery
The delivery is of the first child,
Or, it is the second or subsequent delivery, with the couple
having only one other living child;
Or, through in the current delivery three are twins, there is
only one only living child to that couple.
23
Interventions for Reducing MMR & IMR
Strengthening of First Referral Units with CEMONC
Services (Comprehensive Emergency Obstetric and
Neonatal Care)
151 CEMONC Centers have been set up with the
objective of providing life-saving emergency care to
mothers and children
Every CEMONC center is designed to have 4
obstetricians, 1 pediatrician, 1 anesthetist, blood
bank or blood storage center. Additional budget for
drugs & consumables for each case of delivery has
also been provided.
Contd..
24
Interventions for Reducing MMR & IMR
New Born Care Kit distribution
To prevent deaths from hypothermia and
infections, it is proposed to procure and supply
newborn Baby kits (A Hygienic Infant Wear) to all
SC / ST / BPL newborn babies and low birth weight
babies (delivered in Govt. Institutions) i.e. those
weighing less than 2000 grams.
The Newborn Care Kit consists of 2 Baby
Mattresses; 4 Baby Jackets; 3 Baby Caps; 3 pairs
of Gloves; 12 Baby Diapers and 8 Baby Blankets.
The Kit is sterile and would keep the baby warm
and prevent death from hypothermia and
infections.
1.20 lakhs New Born Care kits distributed.
25
Other interventions for promoting health
and medical facilities
24-hours MCH centre PHCs:
800 PHCs are being upgraded to provide 24-hrs
MCH services. Once in fortnight Specialist Service
Clinics i.e. Ob/Gyn are being provided for the
same.
2 Staff Nurses and three contingent part-time staff
are assisting in the 24-hrs MCH centre PHCs.
Budget for referral transport and additional
consumables are also being provided.
Contd..
26
Other interventions for promoting health
and medical facilities
Blood Banks & Blood Storage centres:
18 new Blood Banks and 89 Blood Storage centres
are being set up in the existing CEMONC centres and
Area Hospitals that do not have either a Blood Bank
or a Blood Storage Center;
Indian Red Cross Society has been identified as a
Nodal Agency to set-up & operate all these Blood
Banks & Blood Storage Centers.
In addition to the above, 40 Blood Storage Centres
have been sanctioned in the new CEMONC Centres.
Contd..
27
Other interventions for promoting health
and medical facilities
Hospital Development Societies
(Rogi Kalyana Samithi):
The constitution of HDS is to
improve service delivery and
management of public hospitals
through community participation.
This concept has been
internationally recognized as a very
successful model.
All District Hospitals registered
under the Societies Act were
given Rs.5.0 lakhs each per year
towards Hospital Development
Society.
PHC, CHCs and Area Hospitals
have been sanctioned Rs.1.0 lakh
each towards the same.
Contd..
Type Total Achieved %
CHCs 167 149 89.22
PHCs 1570 1487 94.71
Area
Hospitals
57 49 85.96
Dist.
Hospitals
23 19 82.61
Total 1817 1704 93.78
28
Other interventions for promoting health
and medical facilities
Village Health and Sanitation Committees
(Gram Panchayat Health Committee):
As per the guidelines of GOI, Village Health Sanitation
Committees (21,916) have been formed with the
objective of
ensuring optimal use of health services in the village;
improving participation of the village level health and
sanitation committees in maintaining quality health
services and;
preventing occurrence of epidemics in the villages.
Village Health & Sanitation Committees are formed with
Panchayat Sarpanch as Chairperson, and Ward Members,
AWWs and WHVs as members with the MPHAs (F) acting
as Member Convener.
An amount of Rs.2202.00 lakhs has been released to the
committees as per the population ratio.
29
Other interventions for promoting health
and medical facilities
Untied Funds for Sub-centres:
As part of the NRHM, it is proposed to provide each sub center
with Rs.10,000 as an untied fund to facilitate meeting urgent yet
discrete activities that need relatively small sums of money.
The fund shall be kept in a joint bank account of the ANM and the
Sarpanch
Untied Funds will be used only for the common good and not for
individual needs, except
In case of referral and transport in emergency situations.
Purchase of bleaching powder and disinfectants for use in
common areas of the village.
Payment/reward to ASHA for certain identified activities
Ad hoc payments for cleaning up sub center, especially after
childbirth.
Untied funds shall not be used for any salaries and recurring
expenditures or to meet the expenses of the Gram Panchayat.
Contd..
30
Other interventions for promoting health
and medical facilities
Untied Funds for PHCs :
Health sector reforms under the NRHM aims to increase
functional, administrative and financial resources and
autonomy to the field units under which every PHC will get
Rs.25,000/- p.a. as untied grant for local health action.
Similarly every PHC will get an Annual Maintenance Grant of
Rs.50,000/- for improvement and maintenance of physical
infrastructure.
Untied Funds will be used only for the common good and not
for individual needs, except
Provision of running water supply & electricity
Ad hoc payments for cleaning up the Center, especially after
childbirth.
Transport of emergencies to appropriate referral centers
Purchase of consumables such as bandages, bleaching powder and
disinfectants for use in common areas
Labour and supplies for environmental sanitation, such as clearing or
Larvicidal measures for stagnant water.
Payment/reward to ASHA for certain identified activities
Contd..
31
Other interventions for promoting health
and medical facilities
Untied Funds for CHCs:
Health sector reforms under the NRHM aims to increase
functional, administrative and financial resources and
autonomy to the field units under which every CHC will get
Rs.50,000/- p.a. as untied grant for local health action.
Untied Funds will be used only for the common good and not
for individual needs, except
Provision of running water supply & electricity
Ad hoc payments for cleaning up the Center, especially after
childbirth.
Transport of emergencies to appropriate referral centers
Purchase of consumables such as bandages, bleaching powder and
disinfectants for use in common areas
Labour and supplies for environmental sanitation, such as clearing or
Larvicidal measures for stagnant water.
Payment/reward to ASHA for certain identified activities
Contd..
32
Innovations
33
Rural Emergency Health Transport Scheme
Rural Emergency Health Transport Scheme
Govt. recognized EMRI as State Nodal Agency.
Emergencies with free-of-cost with toll free
number 108 on 24x7 basis.
Emergency health services in Govt. / Private
accredited hospitals.
Services through well trained people.
95% funding support from Govt. on direct
operational cost.
Attending average emergencies per day 4500.
Field Staff positioned 3,195.
34
20,165 Lives Saved
Advanced Life Saving Ambulance
35
Health Information Help Line (104)
Health Information Help Line (104)
It is a unique, innovative scheme implemented
for the first time in India.
The main objective of establishment of HIHL is to
assist the people particularly in rural & interior
areas who are facing difficulties in getting access
to a qualified doctor and also getting information
on any health problem.
Services round the clock through 104 toll free
number.
The facility was inaugurated on 21
st
Feb-2007 &
today it addresses 34000 calls per day.
36
Rural & Interior area Health Services
Rural & Interior area Health Services
(Fixed Day Health Service)
(Fixed Day Health Service)
Goal
Reduction of IMR & MMR
Access to integrated comprehensive primary
health care.
Objective
Services for identification, diagnosis, monitoring
& treatment, record keeping and referral of risk
cases in a habitation is possible through a
convergent, comprehensive, regular once-a-
month fixed day program.
Services will be provided through a mobile
health unit which will physically visit each
habitation.
37
Key Features
Implementation through PPP (HMRI).
Proposed to be launched from June-2008.
Initially to be implemented in 4 underserved
Districts viz. Srikakulam, Anantapur, Mahabubnagar
and Adilabad.
Health Services will be provided through Mobile
Health Units providing comprehensive clinical lab
diagnosis with treatment.
Each unit covering 3000 population per day and
475 units covering 4 crores population per month.
Target groups: pregnant women, infants, children
and people with chronic diseases.
Convergence with other stakeholders.
39
Das könnte Ihnen auch gefallen
- Khyber Pakhtunkhwa Health Sector Review: Hospital CareVon EverandKhyber Pakhtunkhwa Health Sector Review: Hospital CareNoch keine Bewertungen
- Using Casemix System for Hospital Reimbursement in Social Health Insurance Programme: Comparing Casemix System and Fee-For-Service as Provider Payment MethodVon EverandUsing Casemix System for Hospital Reimbursement in Social Health Insurance Programme: Comparing Casemix System and Fee-For-Service as Provider Payment MethodNoch keine Bewertungen
- Rural Health Care System in IndiaDokument22 SeitenRural Health Care System in IndiaSumit Singhal58% (12)
- Social Infrrastructure (Andhrapradesh)Dokument23 SeitenSocial Infrrastructure (Andhrapradesh)ramachanderbNoch keine Bewertungen
- National Health and FamilyDokument16 SeitenNational Health and FamilyshivaniNoch keine Bewertungen
- National Rural Health Mission NotesDokument3 SeitenNational Rural Health Mission NotesManish BaviskarNoch keine Bewertungen
- Health and Family Welfare-Writeup - 0Dokument11 SeitenHealth and Family Welfare-Writeup - 0Manpreet KaurNoch keine Bewertungen
- HCDSDokument35 SeitenHCDSKrishnaveni MurugeshNoch keine Bewertungen
- National Rural Health Mission: Dr. Rajeshwar Rao ADokument37 SeitenNational Rural Health Mission: Dr. Rajeshwar Rao Akuruvagadda sagarNoch keine Bewertungen
- Health: National Rural Health MissionDokument10 SeitenHealth: National Rural Health MissionsarthuNoch keine Bewertungen
- Rural Health Care System ProjectDokument25 SeitenRural Health Care System ProjectPragathi MittalNoch keine Bewertungen
- Health Care Delivery Concerns in IndiaDokument43 SeitenHealth Care Delivery Concerns in IndiaSaji Sadanandan50% (4)
- National Rural Health MissionDokument3 SeitenNational Rural Health MissionRenu R NairNoch keine Bewertungen
- Ayushman Bharat YojanaDokument28 SeitenAyushman Bharat YojanaParth VasaveNoch keine Bewertungen
- Health Infrastructure in IndiaDokument8 SeitenHealth Infrastructure in IndiaRahul GowlikarNoch keine Bewertungen
- Narayana Health Care - MainDokument19 SeitenNarayana Health Care - MainNeeraj GargNoch keine Bewertungen
- National Rural Health Mission AssignmentDokument12 SeitenNational Rural Health Mission AssignmentFaceless BubbiesNoch keine Bewertungen
- State Welfare Scheme UpdatedDokument16 SeitenState Welfare Scheme UpdatedWoke MillennialsNoch keine Bewertungen
- Schemes by GoIDokument41 SeitenSchemes by GoIMuraliNoch keine Bewertungen
- LDP AssignmentDokument12 SeitenLDP AssignmentSUBHASISH SAHOONoch keine Bewertungen
- Recent Advancement in HealthcareDokument14 SeitenRecent Advancement in HealthcareDeshraj VermaNoch keine Bewertungen
- Adilbad ReportDokument92 SeitenAdilbad ReportMohammed Rizwan AhmedNoch keine Bewertungen
- Infant and Maternal MortalityDokument7 SeitenInfant and Maternal MortalityGaurav PrabhakerNoch keine Bewertungen
- National Health Mission (NHM) : 2.2.1 AshaDokument14 SeitenNational Health Mission (NHM) : 2.2.1 AshaManisha MalikNoch keine Bewertungen
- RCH - IiDokument18 SeitenRCH - IiNeha ShalkarNoch keine Bewertungen
- Evaluation of Health Care SchemeDokument9 SeitenEvaluation of Health Care SchemeKimkimi TlauNoch keine Bewertungen
- JSSKDokument16 SeitenJSSKShivangi Gupta100% (1)
- Health Care Delivery System in IndiaDokument22 SeitenHealth Care Delivery System in IndiaSunija Selvam100% (2)
- Health Budgeting and Financing in Nepal - Policy PerspectivesDokument12 SeitenHealth Budgeting and Financing in Nepal - Policy PerspectivesSudeep UpretyNoch keine Bewertungen
- Excutive SummaryDokument11 SeitenExcutive Summaryratna lal sharmaNoch keine Bewertungen
- Annual Health Report 2012-13 NewDokument58 SeitenAnnual Health Report 2012-13 NewnitinNoch keine Bewertungen
- State Health SchemeDokument8 SeitenState Health SchemeWoke MillennialsNoch keine Bewertungen
- Health Schemes and Yojana IndiaDokument4 SeitenHealth Schemes and Yojana IndiaKailash Nagar100% (1)
- Challenges & Achievements of NRHMDokument3 SeitenChallenges & Achievements of NRHMRenu R NairNoch keine Bewertungen
- Health Family Welfare 3Dokument225 SeitenHealth Family Welfare 3Gopala Sundararaj SNoch keine Bewertungen
- National Rural Health MissionDokument3 SeitenNational Rural Health MissionAbhi PatelNoch keine Bewertungen
- National Rural Health MissionDokument3 SeitenNational Rural Health Missionbasha trimuNoch keine Bewertungen
- Shillong ProjectDokument27 SeitenShillong ProjectPranay JindalNoch keine Bewertungen
- Document 1Dokument3 SeitenDocument 1Kartavya TiwariNoch keine Bewertungen
- 2020 Health and Family WelfareDokument380 Seiten2020 Health and Family WelfaregowthamNoch keine Bewertungen
- Comparative Analysis of Health System of Nepal and India: Presented byDokument36 SeitenComparative Analysis of Health System of Nepal and India: Presented bySuvash RegmiNoch keine Bewertungen
- Guidelines For Distt Hospitals - Indian Public Health StandardsDokument124 SeitenGuidelines For Distt Hospitals - Indian Public Health StandardsTejinder SinghNoch keine Bewertungen
- Nurses in Implementation of National Rural Health Mission: Dr. Pratima Mittra Sr. Consultant, RCH - Ii / NRHM NihfwDokument32 SeitenNurses in Implementation of National Rural Health Mission: Dr. Pratima Mittra Sr. Consultant, RCH - Ii / NRHM NihfwPabhat KumarNoch keine Bewertungen
- Operational Guidelines 2012-13Dokument141 SeitenOperational Guidelines 2012-13Roy GoldenNoch keine Bewertungen
- Seminar Health Care DeliveryDokument39 SeitenSeminar Health Care DeliveryangayarkanniNoch keine Bewertungen
- Distt Health Action PlanDokument147 SeitenDistt Health Action PlanshailesjagtapNoch keine Bewertungen
- Time-Bound Goals For The Eleventh Five Year PlanDokument9 SeitenTime-Bound Goals For The Eleventh Five Year PlanAnand VakadeNoch keine Bewertungen
- DGHS IPHS CommunityHealthCentresDokument120 SeitenDGHS IPHS CommunityHealthCentresSargam MahendruNoch keine Bewertungen
- Reproductive Health, Including Family Planning Status Particularly of Vulnerable GroupsDokument9 SeitenReproductive Health, Including Family Planning Status Particularly of Vulnerable GroupsArifur RahmanNoch keine Bewertungen
- Piramal Swasthya ChallengeDokument9 SeitenPiramal Swasthya ChallengeShivran RoyNoch keine Bewertungen
- Health Sector SchemesDokument7 SeitenHealth Sector Schemesmathstar1Noch keine Bewertungen
- Unit Wise Question Will Come in Final Exam Unit 1: Q 2 ObjectivesDokument54 SeitenUnit Wise Question Will Come in Final Exam Unit 1: Q 2 ObjectivesPoonam Yadav roll no.53Noch keine Bewertungen
- Government SchemesDokument4 SeitenGovernment SchemessurajNoch keine Bewertungen
- National healthmission-NHMDokument52 SeitenNational healthmission-NHMNancy Singh100% (2)
- 5 Health 40 42Dokument3 Seiten5 Health 40 42sunit dasNoch keine Bewertungen
- Border District Cluster StrategyDokument2 SeitenBorder District Cluster StrategyRAJU100% (1)
- 101to 200 Baded HospitalDokument97 Seiten101to 200 Baded Hospitalar_danishNoch keine Bewertungen
- 13.1 Social Sectors Reforms (By Ayussh Sanghi)Dokument37 Seiten13.1 Social Sectors Reforms (By Ayussh Sanghi)harmless wolfNoch keine Bewertungen
- Millions Saved: New Cases of Proven Success in Global HealthVon EverandMillions Saved: New Cases of Proven Success in Global HealthBewertung: 5 von 5 Sternen5/5 (1)
- Doing the Right Thing: 'New' Building Zimbabwe's Health System: 'New' Building Zimbabwe's Health System: 'New Building: 'New Building' Zimbabwe's Health SystemVon EverandDoing the Right Thing: 'New' Building Zimbabwe's Health System: 'New' Building Zimbabwe's Health System: 'New Building: 'New Building' Zimbabwe's Health SystemNoch keine Bewertungen
- Carbohydrates Classification and ReactionsDokument31 SeitenCarbohydrates Classification and ReactionsAlviro CossemeNoch keine Bewertungen
- Site-Directed Mutagenesis - Wikipedia, The Free EncyclopediaDokument6 SeitenSite-Directed Mutagenesis - Wikipedia, The Free EncyclopediaAlviro CossemeNoch keine Bewertungen
- Dopt SpeechDokument4 SeitenDopt SpeechAlviro CossemeNoch keine Bewertungen
- The Fascinating World of Biotech: Back Education PlusDokument3 SeitenThe Fascinating World of Biotech: Back Education PlusAlviro CossemeNoch keine Bewertungen
- Free Microbiology BooksDokument3 SeitenFree Microbiology BooksAlviro CossemeNoch keine Bewertungen
- Literacy and Livelihood Through Self Help Groups in Urban Settings An Innovative Experiment in West Godavari District of Andhra PradeshDokument6 SeitenLiteracy and Livelihood Through Self Help Groups in Urban Settings An Innovative Experiment in West Godavari District of Andhra PradeshAlviro CossemeNoch keine Bewertungen
- Process of Seeking InformationDokument16 SeitenProcess of Seeking InformationAlviro CossemeNoch keine Bewertungen
- 12.sust Devp&Climate ChangeDokument15 Seiten12.sust Devp&Climate ChangeAlviro CossemeNoch keine Bewertungen
- Backward Regions Grant FundDokument20 SeitenBackward Regions Grant FundAlviro CossemeNoch keine Bewertungen
- Environmental Legislation: Module - 7Dokument16 SeitenEnvironmental Legislation: Module - 7Dinesh MehtaNoch keine Bewertungen
- 10.services SectorDokument19 Seiten10.services SectorAlviro CossemeNoch keine Bewertungen
- Energy, Infrastructure and Communications: Verview OF ErformanceDokument23 SeitenEnergy, Infrastructure and Communications: Verview OF ErformanceAlviro CossemeNoch keine Bewertungen
- BCIL ProcedureDokument4 SeitenBCIL ProcedureAlviro CossemeNoch keine Bewertungen
- PDF Manuals Restriction-Mapping-PlasmidDokument23 SeitenPDF Manuals Restriction-Mapping-PlasmidAlviro Cosseme0% (1)
- The Partition of India: August 14, 1947Dokument20 SeitenThe Partition of India: August 14, 1947Alviro CossemeNoch keine Bewertungen
- Non-Alcoholic Fatty Liver DiseaseDokument15 SeitenNon-Alcoholic Fatty Liver DiseaseKurnia pralisaNoch keine Bewertungen
- In-Patient Pharmacy Dispensing PersonnelDokument3 SeitenIn-Patient Pharmacy Dispensing Personneljanr123456Noch keine Bewertungen
- Nutrition in Pediatrics PDFDokument1.121 SeitenNutrition in Pediatrics PDFPutri Wulan Sukmawati100% (5)
- Final Letter To NLM Re - IJOEH Nov 2017Dokument35 SeitenFinal Letter To NLM Re - IJOEH Nov 2017Celeste MonfortonNoch keine Bewertungen
- Eye OintmentsDokument4 SeitenEye OintmentsAnke NemirovskyNoch keine Bewertungen
- Assessment of The Use of A Dental Mouth MirrorDokument7 SeitenAssessment of The Use of A Dental Mouth MirrorIOSRjournalNoch keine Bewertungen
- Exhibitor / Company Name Stall Name AreaDokument56 SeitenExhibitor / Company Name Stall Name AreaJyotsna PandeyNoch keine Bewertungen
- Case Files Pharmacology, 3rd Edition (2017!07!18 02-28-27 UTC)Dokument375 SeitenCase Files Pharmacology, 3rd Edition (2017!07!18 02-28-27 UTC)imperiouxx100% (2)
- Goris PDFDokument24 SeitenGoris PDFAndrew WongNoch keine Bewertungen
- 3 On Your Side Investigates: Jailed and AbusedDokument102 Seiten3 On Your Side Investigates: Jailed and AbusedShaCamree GowdyNoch keine Bewertungen
- Arixtra: (Fondaparinux Sodium) InjectionDokument26 SeitenArixtra: (Fondaparinux Sodium) InjectionTri Purma SariNoch keine Bewertungen
- Rational Use of The Drug (Rud) : Rovina Ruslami, DR., SPPD, PHDDokument31 SeitenRational Use of The Drug (Rud) : Rovina Ruslami, DR., SPPD, PHDamaliaramadhaniNoch keine Bewertungen
- KalanchoeDokument1 SeiteKalanchoeAnonymous iOYpj92Noch keine Bewertungen
- Iso 10555-1 2013Dokument30 SeitenIso 10555-1 2013Nick Ngo67% (3)
- Reading 9thDokument3 SeitenReading 9thicemangdNoch keine Bewertungen
- Faber TestDokument8 SeitenFaber TestHaura TsabitahNoch keine Bewertungen
- Nejme 2305752Dokument2 SeitenNejme 23057525fqkqkcdhtNoch keine Bewertungen
- Hizon, DrugsDokument4 SeitenHizon, DrugsDan HizonNoch keine Bewertungen
- Comparing Different Approaches To CounsellingDokument7 SeitenComparing Different Approaches To CounsellingTim RichardsonNoch keine Bewertungen
- Renal Cell Carcinoma - Nursing Considerations With The Use of Targeted TherapyDokument50 SeitenRenal Cell Carcinoma - Nursing Considerations With The Use of Targeted TherapyMarivic DianoNoch keine Bewertungen
- Mwalya Wambua Final ProjectDokument49 SeitenMwalya Wambua Final ProjectWILSON MACHARIANoch keine Bewertungen
- We Want The Airwaves - Star Amerasu PT 1Dokument9 SeitenWe Want The Airwaves - Star Amerasu PT 1Nia KingNoch keine Bewertungen
- ER Technician Competency ProfileDokument6 SeitenER Technician Competency Profileplanedude86Noch keine Bewertungen
- DyspneuDokument9 SeitenDyspneuAmy KochNoch keine Bewertungen
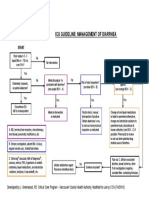
- Icu Guideline: Management of Diarrhea: StartDokument1 SeiteIcu Guideline: Management of Diarrhea: StartGracia VionaNoch keine Bewertungen
- Communication SkillsDokument6 SeitenCommunication SkillsImaneNoch keine Bewertungen
- Implant PanaceaDokument2 SeitenImplant PanaceaKarina OjedaNoch keine Bewertungen
- A Comparison of Free Weight Squat To Smith Machine Squat Using ElectromyographyDokument6 SeitenA Comparison of Free Weight Squat To Smith Machine Squat Using ElectromyographyJoão CasqueiroNoch keine Bewertungen
- Aki VS CKDDokument2 SeitenAki VS CKDKevin TranNoch keine Bewertungen
- ÁdadDokument24 SeitenÁdadFùq Tất ỨqNoch keine Bewertungen