Beruflich Dokumente
Kultur Dokumente
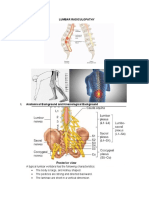
Lumbar Disk Herniation
Hochgeladen von
Syarifah Nadya ArfadOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Lumbar Disk Herniation
Hochgeladen von
Syarifah Nadya ArfadCopyright:
Verfügbare Formate
Herniation
Nuclear material that is displaced into the spinal canal is associated with a significant
inflammatory response, as has been demonstrated in animal studies. Disk injury results in an
increase in the proinflammatory molecules interleukin-1 (IL-1), IL-8, and tumor necrosis factor
(TNF) alpha. Macrophages respond to this displaced foreign material and seek to clear the spinal
canal. Subsequently, a significant scar is produced, even without surgery, and substance P, which
is associated with pain, is detected. Acute neural compression is responsible for dysfunction;
compression of a motor nerve results in weakness, and compression of a sensory nerve results in
numbness. Radicular pain is caused by inflammation of the nerve, which explains the lack of
correlation between the actual size of an intervertebral disk herniation or even the consequent
degree of neural compression and the associated clinical symptoms.
[17]
Furthermore, intervetebral disk degeneration may result in radial tears and leakage of the nuclear
material, which leads to neural toxicity. The subsequent inflammatory response often results in
neural irritation causing radiating pain without numbness, weakness, or loss of reflex, even when
neural compression is absent.
Several factors seem to influence the occurrence of herniated nucleus pulposus. Smoking is a
risk factor in the epidemiology of lumbar disk herniations and has been documented to decrease
the oxygen tension in the avascular disk dramatically, presumably by vasoconstrictive and
rheologic effects on blood. Lumbar disk herniation may result from chronic coughing and other
stresses on the disk. For example, sitting without lumbar support causes an increase in disk
pressures, and driving is also a risk factor because of the resonant coupling of 5-Hz vibrations
from the road to the spine. People who drive signifcant amounts have increased spinal problems;
truck drivers have the additional risk of spinal problems from lifting during loading and
unloading, which, unfortunately, is done after prolonged driving.
Studies have shown that peak stresses within a deteriorated intervertebral disk exceed those from
average loads on a normal disk, which is consistent with a pain mechanism. Further repetitive
stress at physiologic levels did not produce a herniation after prolonged testing, contradicting the
concept of injury accumulation with customary work activities. However, after a simulated
injury to the annulus (cutting), a lower mechanical stress did result in disk herniation, consistent
with intervertebral disk degeneration and with clinical experience on discography.
The presumed traumatic cause of disk herniations has been questioned scientifically in the
literature, particularly with the increased availability of genetic information.
[18, 19]
The pathologic state of a weakened annulus is a necessary condition for herniation to occur.
Many cases involve trivial trauma even in the presence of repetitive stress. An annular tear or
weak spot has not been demonstrated to result from repetitive normal stress from customary
activities or from physically stressful activities.
Mixter and Barr first recognized that the cartilaginous masses in the spinal canal of their patients
were not tumors or chondromas.
[13]
They proposed that herniation of the nucleus pulposus and
displacement of nuclear material caused neural irritation, inflammation, and pain. They showed
that excising a disk fragment was effective, but their recommendation to perform this procedure
with a fusion was necessitated by relatively aggressive laminectomy. This procedure has been
replaced by techniques that are less invasive, such as microdiscectomy.
Clinical Evaluation
Obtaining pertinent patient historical information should begin with an analysis of the chief
complaint. Does the patient's complaint concern dominant leg pain, dominant back pain, or a
mixture of significant problems with both? Next, is the onset acute, subacute, or chronic? Under
what circumstances does onset occur? What is the patient's prior history, particularly regarding
similar symptoms or treatment response?
Identify risk factors, obtain a pertinent medical history, and specifically exclude red flags, such
as nonmechanical pain, which causes pain at night without activities because pressure in the
pelvic veins may be increased upon reclining. Nonmechanical pain may be indicative of a tumor
or infection. A progressive neurologic deficit or cauda equina syndrome is considered a surgical
emergency because irreversible consequences may result if these are left untreated.
Obtaining a thorough history of activity intolerance requires some time and attention to the
details of specific examples and the positions or actions that cause problems. Also, it is helpful to
determine which activities the patient is unable or less able to perform and which activities
exacerbate or moderate the pain. An assessment of the physical demands of the patient's
occupation and daily activities provides the perspective for the described activity intolerance. A
pain drawing can be very helpful in assessing the pattern of pain, such as a dermatomal
distribution, or in assessing the organicity of the complaints.
Physical examination classically involves range-of-motion (ROM) testing of the lumbar and
cervical spine, but these findings may be more reflective of aging or deterioration in the
intervertebral disks and joints than any quantifiable assessment of impairment. The remainder of
the examination is essentially a neurologic assessment of weakness, dermatomal numbness,
reflex change, and, most important, sciatic or femoral nerve root tension in the lumbar spine.
Numerous examination maneuvers (eg, Lasegue classic test, Lasegue rebound sign, Lasegue
differential sign, Braggard sign, flip sign, Deyerle sign, Mendel-Bechterew sign, well leg test or
Fajersztajn sign, both-legs or Milgram test) are available but cloud the issue, because the sciatic
nerve root tension or straight-leg raising test is the basis for nearly all of them. They are
essentially modifications for subtle differences, but the provocation of radiating pain down the
leg is of a neural compressive lesion and compression of the sciatic nerve root, if it goes below
the knee. Furthermore, the provocation of radiating pain down the leg is the most sensitive test
for a lumbar disk herniation.
For a higher lumbar lesion, reverse straight-leg raising or hip extension that stretches the femoral
nerve is analogous to a straight-leg raising test. The Spurling test in the cervical spine is used to
detect foraminal stenosis (Kemp's test is used in the lumbar region) rather than specifically for
intervertebral disk herniation or nerve root tension. Careful hip, rectal, and genitourinary
examinations help exclude complications of those organ systems in the diagnosis of higher
lumbar lesions.
After obtaining plain radiographs, further imaging studies (eg, MRI, computed tomography [CT]
scanning, CT myelography) may be indicated to assess degenerative disk disease, loss of disk
height, and facet deterioration, such as sclerosis or hypertrophy. MRI clearly provides the most
information, perhaps too much, as it has a 25% false-positive rate (asymptomatic herniated
nucleus pulposus [HNP]). An HNP that is noted on imaging studies must be correlated with
objective examination findings; otherwise, it must be presumed to be an asymptomatic HNP if
there is no correlation between the imaging findings and pain or clinical symptoms. Therefore,
imaging studies should perhaps be reserved for cases in which positive physical findings have
been documented.
Other causes of significant back pain in the absence of neurologic findings should be considered.
Sciatic nerve irritation may result from sacroiliac dysfunction or degenerative joint disease
caused by the proximity of the sciatic notch to the sacroiliac joint or peripheral entrapment,
including piriformis syndrome. Careful examination with an adequate differential for the
diagnosis may prevent prolonged ineffective empirical care for presumed lumbar disk disease.
The facet syndrome has been controversial, but neurophysiologic studies have shown discharges
from the capsule consistent with pain, as well as inflammation and degenerative joint disease.
[20]
However, large numbers of patients have reported significant relief after facet joint injections for
nonspecific LBP; as a result, the facet syndrome has become more widely accepted. Clinically,
patients usually have pain only to the knee, not below, as would be expected from an HNP.
Conservative Treatment
Spontaneous improvement of low back discomfort has allowed ineffective treatments to
perpetuate, because benefits have been ascribed to them when they are prescribed while the
patient is still symptomatic but otherwise improving. Hippocrates expected improvement in
sciatica in 40 days, and the customary and contemporary guideline is 6 weeks. An often-quoted
study suggests near-resolution improvement of 90% of patients within 6 weeks, but this study
has been faulted because the criterion for patient recovery was failure to return to the observing
physician.
[21]
The prevalence of back problems is consistent with the failure of a subgroup of
patients to improve and to have periodic recurrent episodes of disability.
Analysis of the effectiveness of treatments and attempts to restrict treatment to those modalities
that have demonstrated efficacy are evidence-based medical practice. Bedrest has a long history
of use but has not been shown to be effective beyond the initial 1 or 2 days; after this period,
bedrest is counterproductive. All conservative treatments are essentially efforts to reduce
inflammation; therefore, only a very short period of rest is appropriate, anti-inflammatories are
of some benefit (because the pain is from inflammation of the nerve), and warm, moist heat or
modalities may be helpful. TNF decrease in preclinical
models.
[22]
Activities should be resumed as early as tolerated. Exercises and physical therapy
mobilize muscles and joints to facilitate the removal of edema and promote recovery. Muscle
relaxants mayoffersymptomatic relief of the acute muscle spasms but only in the early stages;
however, all are central acting, there is no direct relaxation of skeletal muscle, and they are also
sedating.
For back pain without radiculopathy, chiropractic care has high patient satisfaction when
performed within the first 6 weeks, and it has been shown to have good efficacy acutely from an
evidence-based standpoint.
[23]
Injections (eg, epidural) may be particularly helpful in patients
with radiculopathy by providing symptom relief, which allows the patient to increase activities
and helps facilitate rehabilitation.
[24, 25]
Any nuclear material that is herniated may shrink as the
proteoglycan deteriorates, loses its water-retaining ability, and turns from a grapelike object to a
raisinlike object.
Arbitrary time schedules for improvement are inappropriate in any patient who continues to
improve and whose function is relatively maintained. Traction in the acute setting may help
muscle spasms, but it does not reduce the HNP and has no good evidence of efficacy. The use of
traction does not justify hospital admission, as it is not cost-effective and can be administered on
an outpatient basis.
Long-term use of physical therapy modalities is no more effective than hot showers or hot packs
are at home. A transcutaneous electrical nerve stimulation (TENS) unit may be subjectively
helpful in some patients with chronic conditions. Encourage patients to essentially compensate
for intervertebral disk incompetence, as possible, by muscular stabilization, and to maintain
flexibility by initiating life-long exercise regimens, including aerobic conditioning, particularly
swimming, which allows gravity relief.
Assess the body mechanics of every patient who is disabled from work. Educate all patients
about body mechanics, and discuss the risk factors for faulty body mechanics, so that
applications can be incorporated into individual work settings, including appropriate seating (eg,
lumbar support). The lumbar facet joints are oriented relatively vertically, thus allowing forward
flexion, but the joints impact each other when a person bends and then rotates. Repetitive
bending and twisting have been noted to be epidemiologic problems in workers, and may be
associated with chronic pain and disability.
[26]
Attention to lifting techniques and ergonomic
modification at workstations may be very appropriate.
Surgical Intervention
The classic presentation of an herniated nucleus pulposus includes the complaint of sciatica, with
associated objective neurologic findings of weakness, reflex change, and dermatomal numbness.
Various surgical procedures have been reported and share the common goal of decompressing
the neural elements to relieve the leg pain. These procedures are most appropriate for patients
with minimal or tolerable back pain, with an essentially intact and clinically stable disk.
However, the hope of permanently relieving the back pain is a fantasy, a false hope.
The most common procedure for a herniated or ruptured intervertebral disk is a
microdiscectomy, in which a small incision is made, aided by an operating microscope, and a
hemilaminotomy is performed to remove the disk fragment that is impinging on the nerves.
Many patients who undergo microdiscectomy can be discharged with minimal soreness and
complete relief of leg pain after an overnight admission and observation. Same-day procedures
are in the process of cautious development; patients with dominant back pain have a different
problem, even if HNP is present, and would require stabilization by fusion if unresponsive to
well-managed appropriate therapy or arthroplasty (if there is an isolated level with good facet
joints).
Minimally invasive techniques have not replaced this standard microdiscectomy procedure but
can be summarized in 2 categories: central decompression of the disk and directed
fragmentectomy. Outpatient treatment has been reported.
[27]
Central decompression of the disk can be performed chemically or enzymatically with
chymopapain, by laser or plasma (ionized gas) ablation and vaporization, or mechanically by
aspiration and suction with a shaver such as the nucleotome or percutaneous lateral
decompression (arthroscopic microdiscectomy).
The Food and Drug Administration (FDA) initially released and then withheld chymopapain for
injection into lumbar disks because of adverse allergic reactions in patients; skin tests
subsequently were used to determine sensitivity. However, the procedure continued to induce
severe muscle spasms that could be far worse than those of an open operation and thus required
hospitalization and bedrest for up to 50% of patients.
[28]
This morbidity must be considered a
contradiction to the assertion by proponents that the enzyme is limited to the disk in the chemical
digestion of the nucleus pulposus, because the muscles are severely affected, which would not be
expected if the enzyme were contained. In addition, severe scarring in the spinal canal is noted
routinely after this procedure.
The nucleotome and laser central decompressions have been shown only to equal placebo in
effectiveness, and their use has declined. Superiority has not been demonstrated; patient selection
is crucial, with a steep learning curve.
[29]
Further development of alternatives, such as nucleoplasty, and efforts to reduce disk pressure
remain under study. The incidence of recurent herniation is small but may be irreducible. Efforts
to seal the annulus are under investigation.
Directed fragmentectomy is similar to an open microdiscectomy and has demonstrated greater
effectiveness than placebo. This procedure uses an arthroscopic approach and a probe that directs
a flexible pituitary rongeur from the center of the intervertebral disk toward the posterior
annulus. Endoscopic techniques to perform a directed fragmentectomy and to minimize
disruption of normal structures continue in development, but superiority has not been
demonstrated despite this minimally invasive approach.
Concerning the cervical spine, HNP customarily is treated anteriorly, because the pathology is
anterior and manipulation of the cervical cord is not tolerated by the patient. The posterior
approach is reserved for disk herniation that is confined to the foramen and for foraminal
stenosis. An alternative to the anterior cervical spine approach is minimal disk excision; clinical
stability following this procedure is dependent upon the residual disk, which is also true in cases
where there is lumbar spine involvement with back pain. Removal of neural compression
dramatically relieves radiculopathy; however, residual axial neck pain may result in significant
impairment.
Anterior cervical interbody fusion is another intervention. Proponents of discectomy alone assert
equivalent results, but the adequacy of follow-up in those case reports is a significant concern.
Patients with more severe disk degeneration, particularly myelopathy, would more uniformly
undergo fusion. Anterior instrumentation is being used more commonly, and interbody cages are
under consideration as a means of attaining more rapid rehabilitation and more consistent results.
Multilevel disc replacement has been suggested as at least similar to fusion.
[30]
Das könnte Ihnen auch gefallen
- Herniated Nucleus Pulposus TreatmentDokument19 SeitenHerniated Nucleus Pulposus Treatmentvicky174Noch keine Bewertungen
- Neck Pain and Lower Back Pain. Med Clin N Am. 2019.Dokument14 SeitenNeck Pain and Lower Back Pain. Med Clin N Am. 2019.Jose Fernando Diez100% (1)
- Detecting The Differences Radiculopathy, Myelopathy and Peripheral NeuropathyDokument70 SeitenDetecting The Differences Radiculopathy, Myelopathy and Peripheral Neuropathyapi-19502000100% (8)
- Diagnosis and Treatment of Sciatica: Data SupplementDokument12 SeitenDiagnosis and Treatment of Sciatica: Data SupplementAstie NomleniNoch keine Bewertungen
- Evaluationandtreatmentof Cervicalradiculopathy: Cayce A. Onks,, Gregory BillyDokument12 SeitenEvaluationandtreatmentof Cervicalradiculopathy: Cayce A. Onks,, Gregory BillyAndrés MardonesNoch keine Bewertungen
- Growth and Regeneration of Intervertebral Discs byDokument22 SeitenGrowth and Regeneration of Intervertebral Discs byenglish-exactlyNoch keine Bewertungen
- Whiplash Associated DisordersDokument12 SeitenWhiplash Associated DisorderspuchioNoch keine Bewertungen
- Bi Syndrome of The Knee Treated With Acupuncture With Patellofemoral Pain Syndrome As A CaseDokument4 SeitenBi Syndrome of The Knee Treated With Acupuncture With Patellofemoral Pain Syndrome As A CaseInfohoggNoch keine Bewertungen
- March2000 RCP MullerDokument5 SeitenMarch2000 RCP MullerMaría José Luengo SepúlvedaNoch keine Bewertungen
- Algoritmo de tratamiento para dolor secundario a sindrome de bertolotti 2024Dokument10 SeitenAlgoritmo de tratamiento para dolor secundario a sindrome de bertolotti 2024Oscar Cayetano Herrera RodríguezNoch keine Bewertungen
- Back Pain in Children: Causes and TreatmentDokument24 SeitenBack Pain in Children: Causes and TreatmentRin AinochanNoch keine Bewertungen
- Low Back Pain PDFDokument4 SeitenLow Back Pain PDFnetifarhatiiNoch keine Bewertungen
- Evidence-Based PT for Cervical RadiculopathyDokument9 SeitenEvidence-Based PT for Cervical RadiculopathyDr Abdallah BahaaNoch keine Bewertungen
- Lumbar Disc Disease: The Natural History: N G. B, M.DDokument4 SeitenLumbar Disc Disease: The Natural History: N G. B, M.DAfonsoAragãoNoch keine Bewertungen
- Persistent Low Back PainDokument8 SeitenPersistent Low Back PainAffan MsflNoch keine Bewertungen
- Kissing Spine SyndromeDokument4 SeitenKissing Spine SyndromeMarcel Quario OrinaNoch keine Bewertungen
- Cleveland Clinic Journal of Medicine 2007 Klineberg 905 13Dokument9 SeitenCleveland Clinic Journal of Medicine 2007 Klineberg 905 13Sohaib AliNoch keine Bewertungen
- BMJ Summary of Cervical Spondylosis and Neck Pain TreatmentsDokument5 SeitenBMJ Summary of Cervical Spondylosis and Neck Pain TreatmentsIsaac AlemanNoch keine Bewertungen
- Anesthesia Books 2019 Bonica's-4001-5000Dokument1.000 SeitenAnesthesia Books 2019 Bonica's-4001-5000rosangelaNoch keine Bewertungen
- Hard Work Never Hurt Anyone-Or Did It? A Review of Occupational Associations With Soft Tissue Musculoskeletal Disorders of The Neck and Upper LimbDokument6 SeitenHard Work Never Hurt Anyone-Or Did It? A Review of Occupational Associations With Soft Tissue Musculoskeletal Disorders of The Neck and Upper LimbpakemainmainNoch keine Bewertungen
- Alfedson and CookDokument6 SeitenAlfedson and CookppeterarmstrongNoch keine Bewertungen
- Cervical Radiculopathy: Sravisht Iyer Han Jo KimDokument8 SeitenCervical Radiculopathy: Sravisht Iyer Han Jo KimMatias ChandiaNoch keine Bewertungen
- fredericson2006Dokument10 Seitenfredericson2006allenshinigamixNoch keine Bewertungen
- Lumbar Disc HerniationDokument7 SeitenLumbar Disc HerniationkairalmurielNoch keine Bewertungen
- Types of Herniated Nucleus PulposusDokument6 SeitenTypes of Herniated Nucleus PulposusGayle BautistaNoch keine Bewertungen
- Managing Neuropathic PainDokument10 SeitenManaging Neuropathic PainAgusBhakti100% (1)
- Cervical Radiculopathy ReviewDokument8 SeitenCervical Radiculopathy ReviewE=MC2Noch keine Bewertungen
- Discogenic LBP Revised September 2017Dokument13 SeitenDiscogenic LBP Revised September 2017Clinton Franda Markus SitanggangNoch keine Bewertungen
- HDL Management ConservatorDokument8 SeitenHDL Management ConservatorCoLd AasdNoch keine Bewertungen
- Lumbar Degenerative Disk Disease - StatPearls - NCBI BookshelfDokument6 SeitenLumbar Degenerative Disk Disease - StatPearls - NCBI BookshelfAhmad SyahmiNoch keine Bewertungen
- Physiotherapy Management of SciaticaDokument6 SeitenPhysiotherapy Management of SciaticaMuly Arafah ZakariaNoch keine Bewertungen
- Herniated Lumbar Intervertebral DiskDokument10 SeitenHerniated Lumbar Intervertebral DiskRoberto López MataNoch keine Bewertungen
- Low BackDokument7 SeitenLow BackMuhammad FahmyNoch keine Bewertungen
- Shoulder Pain EvaluationDokument8 SeitenShoulder Pain EvaluationAnonymous 9lmlWQoDm8Noch keine Bewertungen
- Treatment of Lumbar Disc Herniation Evidence-Based PDFDokument6 SeitenTreatment of Lumbar Disc Herniation Evidence-Based PDFAnastasya FannyNoch keine Bewertungen
- Fast Facts: Perioperative Pain: Effective management has numerous benefitsVon EverandFast Facts: Perioperative Pain: Effective management has numerous benefitsNoch keine Bewertungen
- Management L Low Back PainDokument7 SeitenManagement L Low Back PainelsyamelindaNoch keine Bewertungen
- Ankylosing Spondylitis BMJ RevDokument5 SeitenAnkylosing Spondylitis BMJ RevsamarqandiNoch keine Bewertungen
- Cervical RadiculopathyDokument8 SeitenCervical RadiculopathyronnyNoch keine Bewertungen
- WEISSPNEDokument4 SeitenWEISSPNELauraNoch keine Bewertungen
- Durerea Vertebrogenă PUBMEDDokument4 SeitenDurerea Vertebrogenă PUBMEDIulia MoldovanNoch keine Bewertungen
- Chronic LumbagoDokument8 SeitenChronic LumbagoOscar FrizziNoch keine Bewertungen
- Entrapmentneuropathiesof Theupperextremity: Christopher T. Doughty,, Michael P. BowleyDokument14 SeitenEntrapmentneuropathiesof Theupperextremity: Christopher T. Doughty,, Michael P. BowleydwiNoch keine Bewertungen
- Subacromial Impingement Syndrome and Rotator Cuff Tendinopathy: The Dilemma of DiagnosisDokument4 SeitenSubacromial Impingement Syndrome and Rotator Cuff Tendinopathy: The Dilemma of DiagnosisTomBramboNoch keine Bewertungen
- Back PainDokument18 SeitenBack PainCabdiladif Ahmed McrfNoch keine Bewertungen
- Herniated Lumbar Intervertebral Disk: Epidemiology and Natural HistoryDokument6 SeitenHerniated Lumbar Intervertebral Disk: Epidemiology and Natural HistoryGeysel SuarezNoch keine Bewertungen
- Assessment and Management of Acute Low Back Pain - American Family PhysicianDokument9 SeitenAssessment and Management of Acute Low Back Pain - American Family PhysiciancaralivroNoch keine Bewertungen
- Jake PPDokument31 SeitenJake PPapi-323342594Noch keine Bewertungen
- Diare AnakDokument6 SeitenDiare AnakVictoria HusadaniNoch keine Bewertungen
- Back Pain Printable VersionDokument43 SeitenBack Pain Printable VersionSabin ParajuliNoch keine Bewertungen
- Lumbar Radiculopathy Medback Castillo Mendez EDITEDDokument12 SeitenLumbar Radiculopathy Medback Castillo Mendez EDITEDSteve ColbertNoch keine Bewertungen
- Original Paper: Lumbar Disk Herniations - Clinical Status, Diagnosis, Imaging, Surgical Treatment and Global OutcomeDokument6 SeitenOriginal Paper: Lumbar Disk Herniations - Clinical Status, Diagnosis, Imaging, Surgical Treatment and Global Outcomeasep budiyantoNoch keine Bewertungen
- 10, Pain Management of Spinalcord Injury-1Dokument23 Seiten10, Pain Management of Spinalcord Injury-1Zeeshan AhmadNoch keine Bewertungen
- Treatment of Chronic Lower Back Pain With Lumbar Extension and Whole-Body Vibration ExerciseDokument6 SeitenTreatment of Chronic Lower Back Pain With Lumbar Extension and Whole-Body Vibration ExerciseSuci NivlaharmyNoch keine Bewertungen
- Spinal Stenosis and Neurogenic Claudication - StatPearls - NCBI BookshelfDokument8 SeitenSpinal Stenosis and Neurogenic Claudication - StatPearls - NCBI BookshelfchhabraanNoch keine Bewertungen
- Dolor Sacro IliacoDokument6 SeitenDolor Sacro Iliacomaria antonieta0102Noch keine Bewertungen
- LBP 2Dokument12 SeitenLBP 2Attika DiniNoch keine Bewertungen
- Articol Unefs 2021Dokument12 SeitenArticol Unefs 2021Sclipcea DaniNoch keine Bewertungen
- New Perspectives On Neurogenic Thoracic Outlet SyndromeDokument10 SeitenNew Perspectives On Neurogenic Thoracic Outlet SyndromeMourning_WoodNoch keine Bewertungen
- Baobab MenuDokument4 SeitenBaobab Menuperseverence mahlamvanaNoch keine Bewertungen
- Three Comparison of Homoeopathic MedicinesDokument22 SeitenThree Comparison of Homoeopathic MedicinesSayeed AhmadNoch keine Bewertungen
- HVAC Master Validation PlanDokument51 SeitenHVAC Master Validation Plannavas197293% (30)
- Civil Service Exam Clerical Operations QuestionsDokument5 SeitenCivil Service Exam Clerical Operations QuestionsJeniGatelaGatillo100% (3)
- Bio310 Summary 1-5Dokument22 SeitenBio310 Summary 1-5Syafiqah ArdillaNoch keine Bewertungen
- Marshall Stability Test AnalysisDokument5 SeitenMarshall Stability Test AnalysisZick Zickry50% (2)
- Open Far CasesDokument8 SeitenOpen Far CasesGDoony8553Noch keine Bewertungen
- EA Linear RegressionDokument3 SeitenEA Linear RegressionJosh RamosNoch keine Bewertungen
- Human Rights Alert: Corrective Actions in Re: Litigation Involving Financial InstitutionsDokument3 SeitenHuman Rights Alert: Corrective Actions in Re: Litigation Involving Financial InstitutionsHuman Rights Alert - NGO (RA)Noch keine Bewertungen
- Mpu 2312Dokument15 SeitenMpu 2312Sherly TanNoch keine Bewertungen
- Bala Graha AfflictionDokument2 SeitenBala Graha AfflictionNeeraj VermaNoch keine Bewertungen
- Revision Worksheet - Matrices and DeterminantsDokument2 SeitenRevision Worksheet - Matrices and DeterminantsAryaNoch keine Bewertungen
- Ansible Playbook for BeginnersDokument101 SeitenAnsible Playbook for BeginnersFelix Andres Baquero Cubillos100% (1)
- Guide To Raising Capital From Angel Investors Ebook From The Startup Garage PDFDokument20 SeitenGuide To Raising Capital From Angel Investors Ebook From The Startup Garage PDFLars VonTurboNoch keine Bewertungen
- Employee Confidentiality and Non-Disclosure AgreementDokument5 SeitenEmployee Confidentiality and Non-Disclosure AgreementshamoojeeNoch keine Bewertungen
- Iphoneos 31Dokument159 SeitenIphoneos 31Ivan VeBoNoch keine Bewertungen
- Use Visual Control So No Problems Are Hidden.: TPS Principle - 7Dokument8 SeitenUse Visual Control So No Problems Are Hidden.: TPS Principle - 7Oscar PinillosNoch keine Bewertungen
- Mosfet 101Dokument15 SeitenMosfet 101Victor TolentinoNoch keine Bewertungen
- Worksheet 5 Communications and Privacy: Unit 6 CommunicationDokument3 SeitenWorksheet 5 Communications and Privacy: Unit 6 Communicationwh45w45hw54Noch keine Bewertungen
- Chromate Free CoatingsDokument16 SeitenChromate Free CoatingsbaanaadiNoch keine Bewertungen
- Product Data Sheet For CP 680-P and CP 680-M Cast-In Firestop Devices Technical Information ASSET DOC LOC 1540966Dokument1 SeiteProduct Data Sheet For CP 680-P and CP 680-M Cast-In Firestop Devices Technical Information ASSET DOC LOC 1540966shama093Noch keine Bewertungen
- Lewis Corporation Case 6-2 - Group 5Dokument8 SeitenLewis Corporation Case 6-2 - Group 5Om Prakash100% (1)
- CDI-AOS-CX 10.4 Switching Portfolio Launch - Lab V4.01Dokument152 SeitenCDI-AOS-CX 10.4 Switching Portfolio Launch - Lab V4.01Gilles DellaccioNoch keine Bewertungen
- Flowmon Ads Enterprise Userguide enDokument82 SeitenFlowmon Ads Enterprise Userguide ennagasatoNoch keine Bewertungen
- Unit 14 Ergonomics Design: AND ProductDokument24 SeitenUnit 14 Ergonomics Design: AND ProductRämêşh KątúřiNoch keine Bewertungen
- Basic Features of The Microcredit Regulatory Authority Act, 2006Dokument10 SeitenBasic Features of The Microcredit Regulatory Authority Act, 2006Asif Hasan DhimanNoch keine Bewertungen
- Gapped SentencesDokument8 SeitenGapped SentencesKianujillaNoch keine Bewertungen
- SolBridge Application 2012Dokument14 SeitenSolBridge Application 2012Corissa WandmacherNoch keine Bewertungen
- Service Manual: Precision SeriesDokument32 SeitenService Manual: Precision SeriesMoises ShenteNoch keine Bewertungen
- Composite Structures: A. Grimaldi, A. Sollo, M. Guida, F. MaruloDokument15 SeitenComposite Structures: A. Grimaldi, A. Sollo, M. Guida, F. MaruloSharan KharthikNoch keine Bewertungen