Beruflich Dokumente
Kultur Dokumente
5 Common Uts Diseases
Hochgeladen von
Jeremiah Nayosan0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
127 Ansichten9 Seitenhealth
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenhealth
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
127 Ansichten9 Seiten5 Common Uts Diseases
Hochgeladen von
Jeremiah Nayosanhealth
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 9
VESICOURETERAL REFLUX
What is vesicoureteral reflux (VUR)?
Vesicoureteral reflux occurs when urine dwelling in the bladder flows back into the ureters and often back into the
kidneys. The bladder is the hollow, muscular organ that stores urine before urination occurs. The bladder has three small
openings; two connect the ureters where urine is drained down from the kidneys, and one connects the bladder to the
urethra where urine exits the body.
The ureters are funnel-shaped tubes that carry urine from the kidneys. Ureters enter the bladder at a diagonal angle and
have a special one-way valve system that normally prevents urine from flowing back up the ureters in the direction of the
kidneys. When a child has vesicoureteral reflux, the mechanism that prevents the back-flow of urine does not work,
allowing urine to flow in both directions. This condition is most frequently diagnosed in infancy and childhood. A child
who has vesicoureteral reflux is at risk for developing recurrent kidney infections, which, over time, can cause damage
and scarring to the kidneys.
What causes vesicoureteral reflux?
There are many different reasons why a child may develop vesicoureteral reflux. Some of the more common causes
include:
VUR commonly occurs in children whose parents or siblings have the irregularity.
Children who are born with neural tube defects such as spina bifida may have VUR.
During infancy, the disease is more common among boys because as they urinate there is more pressure in their entire
urinary tract. In early childhood, the irregularity is more common in girls.
VUR can occur in children with other urinary tract abnormalities such as posterior urethral valves, ureterocele, or
ureter duplication.
VUR is more common in Caucasian children than in African-American children.
What are the symptoms of vesicoureteral reflux?
The following are the most common symptoms of vesicoureteral reflux. However, each child may experience symptoms
differently. Symptoms may include:
urinary tract infection (urinary tract infections are uncommon in children younger than 5 years and unlikely in boys at
any age, unless VUR is present)
trouble with urination including:
o urgency
o dribbling
o wetting pants
an abdominal mass may be detected from a swollen kidney
poor weight gain
high blood pressure
The symptoms of VUR may resemble other conditions or medical problems. Always consult your child's physician for a
diagnosis.
How is vesicoureteral reflux diagnosed?
VUR can often be detected by ultrasound before a child is born. If there is a family history of VUR, but your child has no
symptoms, your child's physician may elect to perform a diagnostic test to rule out VUR. Diagnostic procedures for VUR
may include:
voiding cystourethrogram (VCUG) - a specific x-ray that examines the urinary tract. A catheter (hollow tube) is
placed in the urethra (tube that drains urine from the bladder to the outside of the body) and the bladder is filled with a
liquid dye. X-ray images will be taken as the bladder fills and empties. The images will show if there is any reverse
flow of urine into the ureters and kidneys.
renal ultrasound - a non-invasive test in which a transducer is passed over the kidney producing sound waves which
bounce off the kidney, transmitting a picture of the organ on a video screen. The test is used to determine the size and
shape of the kidney, and to detect a mass, kidney stone, cyst, or other obstruction or abnormalities.
blood tests
Treatment for vesicoureteral reflux:
VUR can occur in varying degrees of severity. It can cause mild reflux, when urine backs up only a short distance in the
ureters. Or, it can cause severe reflux leading to kidney infection(s) and permanent kidney damage. Specific treatment for
VUR will be determined by your child's physician based on:
your child's age, overall health, and medical history
the extent of the condition
your child's tolerance for specific medications, procedures, or therapies
expectations for the course of the condition
your opinion or preference
Your child's physician may assign a grading system (ranging from 1 to 5) to indicate the degree of reflux your child has.
The higher the grade, the more severe the reflux.
Most children who have grade 1 through 3 VUR do not need any type of intense therapy. The reflux resolves on its own
over time, usually within five years. Children who develop frequent fevers or infections may require ongoing preventative
antibiotic therapy and periodic urine tests.
Children who have grade 4 and 5 reflux may require surgical intervention. During the procedure, the surgeon will create a
flap-valve apparatus for the ureter that will prevent reverse flow of urine into the kidney. In more severe cases, the scarred
kidney and ureter may need to be surgically removed.
New treatments are being introduced, in some cases, for vesicoureteral reflux. Consult your child's physician for more
information.
URINARY TRACT INFECTIONS (UTIS)
What are urinary tract infections (UTIs)?
Urinary tract infections are a serious, but common, health problem that affects millions of people each year. With the
reason remaining unclear, women are especially prone to urinary tract infections.
What causes urinary tract infections?
Normal urine is sterile and contains fluids, salts, and waste products. It is free of bacteria, viruses, and fungi. An infection
occurs when microorganisms, usually bacteria from the digestive tract, cling to the opening of the urethra, the hollow tube
that carries urine from the bladder to the outside of the body, and begin to multiply.
Most infections arise from Escherichia coli (E. coli) bacteria, which normally live in the colon.
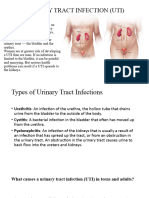
What are the different types of urinary tract infections?
A urinary tract infection may involve different sections of the urinary tract including the following:
urethritis - an infection of the urethra, the hollow tube that drains urine from the bladder to the outside of the body.
cystitis - a bacterial infection in the bladder that often has moved up from the urethra.
pyelonephritis - an infection of the kidneys that is usually a result of an infection that has spread up the tract, or from
an obstruction in the urinary tract. An obstruction in the urinary tract causes urine to back flow into the ureters and
kidneys.
What are the symptoms of a urinary tract infection?
The following are the most common symptoms of a urinary tract infection. However, each individual may experience
symptoms differently. Symptoms may include:
frequent urination
a painful, burning feeling during urination
fever
urine appears cloudy or reddish in color (blood may be present in the urine)
feeling pain even when not urinating
fatigue
pain in the back or side, below the ribs
nausea and/or vomiting
despite an intense urge to urinate, only a small amount of urine is passed
women may feel an uncomfortable pressure above the pubic bone
The symptoms of a urinary tract infection may resemble other conditions or medical problems. Always consult your
physician for a diagnosis.
How are UTIs diagnosed?
In addition to a complete medical history and physical examination, diagnostic tests and procedures may include the
following:
urinalysis - laboratory examination of urine for various cells and chemicals, such as red blood cells, white blood cells,
infection, or excessive protein.
intravenous pyelogram (IVP) - a series of x-rays of the kidney, ureters, and bladder with the injection of a contrast
dye into the vein - to detect tumors, abnormalities, kidney stones, or any obstructions, and to assess renal blood flow.
cystoscopy (Also called cystourethroscopy.) - an examination in which a scope, a flexible tube and viewing device,
is inserted through the urethra to examine the bladder and urinary tract for structural abnormalities or obstructions,
such as tumors or stones.
renal ultrasound - a non-invasive test in which a transducer is passed over the kidney producing sound waves which
bounce off of the kidney, transmitting a picture of the organ on a video screen. The test is used to determine the size
and shape of the kidney, and to detect a mass, kidney stone, cyst, or other obstruction or abnormalities.
Treatment for UTIs:
Specific treatment for UTIs will be determined by your physician based on:
your age, overall health, and medical history
extent of the disease
your tolerance for specific medications, procedures, or therapies
expectations for the course of the disease
your opinion or preference
Treatment may include:
antibacterial medications
other medications and/or a heating pad to relieve pain
behavior modifications, including the following:
o Drink plenty of water to help cleanse the urinary tract of bacteria.
o Avoid coffee, alcohol, and spicy foods.
o Quit smoking.
Preventing future urinary tract infections:
To reduce the likelihood of developing another UTI, a patient may consider the following:
Drink plenty of water every day.
Drink cranberry juice. Large amounts of vitamin C inhibit the growth of some bacteria by acidifying the urine.
Vitamin C supplements have the same effect.
Urinate when you feel the need and do not resist the urge to urinate.
Wipe from front to back to prevent bacteria around the anus from entering the vagina or urethra.
Take showers instead of tub baths.
Cleanse the genital area before/after sexual intercourse.
Avoid using feminine hygiene sprays and scented douches.
URINARY INCONTINENCE
What is urinary incontinence (UI)?
Urinary incontinence (UI) is the loss of urine control, or
the inability to hold your urine until you can reach a
restroom. More than 15 million men and women in the
United States experience incontinence. UI can strike at
any age. Women over age 50 are the most likely to
develop UI. Urinary incontinence may be a temporary
condition, resulting from an underlying medical condition.
It can range from the discomfort of slight losses of urine
to severe, frequent wetting.
What causes urinary incontinence?
Incontinence is not an inevitable result of aging, but is
particularly common in older people. It is often caused by
specific changes in body function that may result from
diseases, use of medications, and/or the onset of an
illness. Sometimes, it is the first and only symptom of a
urinary tract infection.
What are some of the different types of urinary
incontinence?
The following are some of the different types of urinary
incontinence:
urge incontinence - the inability to hold urine
long enough to reach a restroom. It is often found in
people who have conditions such as diabetes, stroke,
dementia, Parkinson's disease, and multiple sclerosis, but may be an indication of other diseases or conditions that
would also warrant medical attention.
stress incontinence - the most common type of incontinence that involves the leakage of urine during exercise,
coughing, sneezing, laughing, lifting heavy objects, or other body movements that put pressure on the bladder.
functional incontinence - leakage due to a difficulty reaching a restroom in time because of physical conditions such
as arthritis.
overflow incontinence - leakage that occurs when the quantity of urine produced exceeds the bladder's capacity to
hold it.
What are the symptoms of urinary incontinence?
The following are the most common symptoms of urinary incontinence. However, each individual may experience
symptoms differently. Symptoms may include:
inability to urinate
pain related to filling the bladder and/or pain related to urination without a proven bladder infection
progressive weakness of the urinary stream with or without a feeling of incomplete bladder emptying
an increased rate of urination without a proven bladder infection
needing to rush to the restroom and/or losing urine if you do not get to restroom in time
abnormal urination or changes in urination related to a nervous system
abnormality such as stroke, spinal cord injury, multiple sclerosis
leakage of urine that prevents activities
leakage of urine that began or continued after surgery
leakage of urine that causes embarrassment
frequent bladder infections
The symptoms of urinary incontinence may resemble other conditions or medical problems. Always consult your
physician for a diagnosis.
How is urinary incontinence diagnosed?
For people with urinary incontinence, it is important to consult a physician for a complete physical examination that
focuses on the urinary and nervous systems, reproductive organs, and urine samples. In many cases, patients will then be
referred to a urologist, a physician who specializes in diseases of the urinary tract.
Treatment for urinary incontinence:
Specific treatment for urinary incontinence will be determined by your physician based on:
your age, overall health, and medical history
extent of the disease
your tolerance for specific medications, procedures, or therapies
expectations for the course of the disease
your opinion or preference
Treatment may include:
certain behavioral techniques (including pelvic muscle exercises, biofeedback, and bladder training)
medications
surgery (if the incontinence is related to structural problems such as an abnormally positioned bladder or a blockage)
diet modifications (including eliminating caffeine in coffee, soda, and tea, and/or eliminating alcohol)
Managing urinary incontinence:
There are many products and devices available for managing urinary incontinence. Specifically designed absorbent
underclothing is available - which is no more bulky than normal underwear and can be worn easily under everyday
clothing. Other incontinence products include washable, adult cloth diapers or contoured cloth diapers with plastic covers.
In some cases, depending upon the type of incontinence and after other management methods have proven to be
ineffective, a catheter may be inserted into the urethra to collect the urine. Catheters may be used occasionally or on a
constant basis, in which case a tube connects to a bag that attaches to the leg. Men can use a type of external catheter,
condom catheter device, that is placed over the penis and connects to a bag that attaches to the leg.
Consult your physician with your questions regarding the management and treatment of urinary incontinence.
PEYRONIE'S DISEASE
What is Peyronie's disease?
Peyronie's disease is
characterized by a plaque, or
hard lump, that forms on the
erection tissue of the penis. The
plaque often begins as an
inflammation that may develop
into a fibrous tissue.
Peyronie's disease was first
described in 1743 by a French
surgeon, Franois de la Peyronie.
It was classified as a form of
impotence. However, now
impotence is recognized as one
factor associated with Peyronie's
disease, but is not always
present.
What causes Peyronie's
disease?
Some researchers believe Peyronie's disease develops following a trauma that causes bleeding inside the penis. This
trauma may explain acute cases of Peyronie's disease, but does not explain why most cases develop slowly, or what causes
the disease after no apparent traumatic event.
Generally, when the disease heals within a year or so, the plaque does not advance beyond an initial inflammatory phase.
However, when the disease lasts for years, the plaque often becomes a tough, fibrous tissue, and calcium deposits may
form.
What are the symptoms of Peyronie's disease?
The plaque in Peyronie's disease is benign, or non-cancerous. The following are the most common symptoms of
Peyronie's disease. However, each individual may experience symptoms differently. Symptoms may include:
Plaque on the top of the shaft, which is the most common condition, causes the penis to bend upward.
Plaque on the underside causes the penis to bend downward.
In cases where the plaque develops on both top and bottom, indentation and shortening of the penis may occur.
Pain, bending, and emotional distress can prohibit sexual intercourse.
Painful erections may occur.
The symptoms of Peyronie's disease may resemble other conditions or medical problems. Always consult your physician
for a diagnosis.
How is Peyronie's disease diagnosed?
A diagnosis of Peyronie's disease is usually made when men seek medical attention for painful erections and difficulty
with intercourse. In addition to a complete medical history and physical examination, diagnostic procedures for Peyronie's
disease may include the following:
ultrasound examination of the penis - a diagnostic technique which uses high-frequency sound waves to create an
image of the internal organs.
color Doppler examination - a type of ultrasound that uses sound waves to measure the flow of blood through a blood
vessel; waveforms of the blood flow are shown on the ultrasound screen (to evaluate erectile function, anatomy, and
blood flow).
Treatment for Peyronie's disease:
Specific treatment for Peyronie's disease will be determined by your physician based on:
your age, overall health, and medical history
extent of the disease
your tolerance for specific medications, procedures, or therapies
expectations for the course of the disease
your opinion or preference
In general, the goal of treatment is to keep the patient with Peyronie's disease sexually active. Providing education about
the disease and its course is often included in the treatment plan. In some cases, treatment is not necessary, as Peyronie's
disease often occurs in a mild form that heals without treatment in 6 to 15 months. Treatment may include:
prescribing or continuing palliative methods
surgery
vitamin E
Small studies have reported improvements with oral vitamin E prescribed by a physician; however, larger controlled
studies have not been completed to establish the effectiveness of this treatment.
injections of various chemical agents into the plaques
Injections of various chemical agents into the plaques have been utilized in a small number of patients, and, for this
reason, this intervention is considered unproven; unwanted side effects may occur.
radiation therapy
With this treatment approach, radiation is aimed at the plaque to reduce pain, but does not affect the plaque itself;
unwanted side effects or worsening of the disease may occur.
NEUROGENIC BLADDER
What is a neurogenic bladder?
The muscles and nerves of the urinary system
work together to hold urine in the bladder and
then release it at the appropriate time. Nerves
carry messages from the bladder to the brain and
from the brain to the muscles of the bladder
telling them either to tighten or release. In a
neurogenic bladder, the nerves that are supposed
to carry these messages do not work properly.
Complications of a neurogenic bladder:
The following problems are often associated with
a neurogenic bladder:
Urine Leakage
Urine leakage often occurs when the muscles
holding urine in do not get the right message.
Urine Retention
Urine retention often happens if the muscles holding urine in do not get the message that it is time to let go.
Damage To The Tiny Blood Vessels In The Kidney
Damage to the tiny blood vessels in the kidney often happens if the bladder becomes too full and urine backs up into
the kidneys, causing extra pressure.
Infection Of The Bladder Or Ureters
Infection of the bladder or ureters often results from urine that is held too long before being eliminated.
What causes neurogenic bladder?
The following are possible causes of neurogenic bladder:
diabetes
acute infections
accidents that cause trauma to the brain or spinal cord
genetic nerve problems
heavy metal poisoning
What are the symptoms of neurogenic bladder?
The following are the most common symptoms of neurogenic bladder. However, each individual may experience
symptoms differently. Symptoms may include:
urinary tract infection
kidney stones - these may be difficult to determine because you may not be able to feel pain associated with kidney
stones if you have spinal cord abnormalities. Symptoms of kidney stones include:
o chills
o shivering
o fever
urinary incontinence
small urine volume during voiding
urinary frequency and urgency
dribbling urine
loss of sensation of bladder fullness
The symptoms of neurogenic bladder may resemble other conditions and medical problems. Always consult your
physician for a diagnosis.
How is neurogenic bladder diagnosed?
When neurogenic bladder is suspected, both the nervous system (including the brain) and the bladder itself are examined.
In addition to a complete medical history and physical examination, diagnostic procedures for neurogenic bladder may
include the following:
x-rays of the skull and spine - a diagnostic test which uses invisible electromagnetic energy beams to produce images
of internal tissues, bones, and organs onto film.
electroencephalogram (EEG) - a procedure that records the brain's continuous, electrical activity by means of
electrodes attached to the scalp.
imaging tests of the bladder and ureters
tests that involve filling the bladder (to see how much it can hold and checking to see if the bladder empties
completely)
Treatment for neurogenic bladder:
Specific treatment for neurogenic bladder will be determined by your physician based on:
your age, overall health, and medical history
severity of symptoms
cause of the nerve damage
type of voiding dysfunction that results
your tolerance for specific medications, procedures, or therapies
expectations for the course of the condition
your opinion or preference
Treatment may include:
insertion of a catheter or hollow tube (to empty the bladder at regular intervals)
prophylactic (preventive) antibiotic therapy (to reduce the incidence of infection)
placement of an artificial sphincter - a procedure that involves placing an artificial cuff around the neck of the bladder
that can be inflated to prevent urinary incontinence and deflated when it is time to empty the bladder. You will still
require intermittent catheterization to completely empty the bladder.
surgery
Das könnte Ihnen auch gefallen
- UTI (Urinary Tract Infection)Dokument9 SeitenUTI (Urinary Tract Infection)Carson BirthNoch keine Bewertungen
- Urinary Tract InfectionsDokument4 SeitenUrinary Tract InfectionsRalph Patrick SamaniegoNoch keine Bewertungen
- Urinary Tract InfectionDokument10 SeitenUrinary Tract Infectionjaah diazNoch keine Bewertungen
- Readings: Acute PyelonephritisDokument6 SeitenReadings: Acute PyelonephritisMauriceNoch keine Bewertungen
- Urinary Tract Infection 1Dokument17 SeitenUrinary Tract Infection 1Annie Lou AbrahamNoch keine Bewertungen
- Urinary Tract InfectionsDokument17 SeitenUrinary Tract Infectionss.khan9211rediffmail.comNoch keine Bewertungen
- Urinary Tract Infection (UTI) : A Guide For WomenDokument2 SeitenUrinary Tract Infection (UTI) : A Guide For WomenBily ManNoch keine Bewertungen
- Urinary System by Carmelita ChavezDokument16 SeitenUrinary System by Carmelita ChaveztankmpNoch keine Bewertungen
- Urinary Tract Infection (UTI)Dokument9 SeitenUrinary Tract Infection (UTI)ogwal andrewictynetNoch keine Bewertungen
- Kidney InfectionDokument3 SeitenKidney InfectionMaxpein Zin Dell Valle-MoonNoch keine Bewertungen
- Urinary Tract Infection, Bladder and Bowel Dysfunction: 1) What Is A UTI?Dokument5 SeitenUrinary Tract Infection, Bladder and Bowel Dysfunction: 1) What Is A UTI?varssitha VNoch keine Bewertungen
- RLE Urinary Tract InfectionDokument13 SeitenRLE Urinary Tract InfectionAliza AlyyNoch keine Bewertungen
- Urinary Tract Infection (UTI)Dokument6 SeitenUrinary Tract Infection (UTI)Anonymous iG0DCOfNoch keine Bewertungen
- Pathophysiology of The Renal System For Pharmacy 2023Dokument86 SeitenPathophysiology of The Renal System For Pharmacy 2023Marlene NiyomuhozaNoch keine Bewertungen
- UTI in AdultsDokument4 SeitenUTI in Adultsjoan_padilla2000Noch keine Bewertungen
- Urinary Tract InfectionDokument30 SeitenUrinary Tract InfectionLeo Mar MakilanNoch keine Bewertungen
- Female Urinary System: Types of Urinary Tract InfectionDokument6 SeitenFemale Urinary System: Types of Urinary Tract InfectionCarmela BedanoNoch keine Bewertungen
- Urinary Tract InfectionDokument5 SeitenUrinary Tract InfectionDRANoch keine Bewertungen
- Understanding Urinary Incontinency: A Simplified GuideVon EverandUnderstanding Urinary Incontinency: A Simplified GuideNoch keine Bewertungen
- Elective 2 ReportDokument7 SeitenElective 2 ReportJem TellainNoch keine Bewertungen
- Posterior Urethral ValveDokument6 SeitenPosterior Urethral ValveMustafa AadanNoch keine Bewertungen
- Chapter 45 Urinary EliminationDokument29 SeitenChapter 45 Urinary EliminationKwenaNoch keine Bewertungen
- What Causes Urinary Retention?Dokument4 SeitenWhat Causes Urinary Retention?darkz_andreaslimNoch keine Bewertungen
- Pyelonephritis: Urinary Tract Infection Vesicoureteric RefluxDokument12 SeitenPyelonephritis: Urinary Tract Infection Vesicoureteric Reflux3ling3Noch keine Bewertungen
- Urinary IncontinenceDokument12 SeitenUrinary IncontinenceAmrit Preet KaurNoch keine Bewertungen
- Urinary Tract Infection UTI and Dementia FactsheetDokument10 SeitenUrinary Tract Infection UTI and Dementia FactsheettoobaziNoch keine Bewertungen
- Urinary Tract InfectionsDokument5 SeitenUrinary Tract InfectionsEben Leonel Albano MaiopueNoch keine Bewertungen
- Pediatric Urinary DisordersDokument27 SeitenPediatric Urinary DisordersKailash NagarNoch keine Bewertungen
- The Urinary System. The Urinary System Helps Maintain Proper Water and Salt Balance ThroughoutDokument4 SeitenThe Urinary System. The Urinary System Helps Maintain Proper Water and Salt Balance ThroughoutArjay EspañolNoch keine Bewertungen
- Vesico Ureteral RefluxDokument19 SeitenVesico Ureteral Refluxmadara ëNoch keine Bewertungen
- Intestinal Malrotation and VolvulusDokument14 SeitenIntestinal Malrotation and VolvulusSaf Tanggo Diampuan100% (1)
- Campoli 257 Renal CH 55Dokument26 SeitenCampoli 257 Renal CH 55FeliciaDorghamNoch keine Bewertungen
- Urinary Track Infection (Uti)Dokument8 SeitenUrinary Track Infection (Uti)Praise ToluwalaseNoch keine Bewertungen
- Uti 1Dokument75 SeitenUti 1Muwanga faizoNoch keine Bewertungen
- The Test Urine CultureDokument13 SeitenThe Test Urine CultureAnonymous 5aoV2RWWAwNoch keine Bewertungen
- Urinary Tract Infection (Maramag Eunice Laman Jenny Pearl)Dokument16 SeitenUrinary Tract Infection (Maramag Eunice Laman Jenny Pearl)Carlojay IniegoNoch keine Bewertungen
- Hematuria, (Blood in Urine) A Simple Guide to The Condition, Related Diseases And Use in Diagnosis of DiseasesVon EverandHematuria, (Blood in Urine) A Simple Guide to The Condition, Related Diseases And Use in Diagnosis of DiseasesBewertung: 5 von 5 Sternen5/5 (2)
- Swollen Kidney, (Hydronephrosis) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandSwollen Kidney, (Hydronephrosis) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Urinary RetentionDokument11 SeitenUrinary RetentionAngga PradianNoch keine Bewertungen
- Bladder & Bowel Elimination PDFDokument37 SeitenBladder & Bowel Elimination PDFSwarna JayarathnaNoch keine Bewertungen
- What Is Acute PyelonephritisDokument2 SeitenWhat Is Acute PyelonephritisAnnabel Dela CruzNoch keine Bewertungen
- Coli Bacterial Strains That Usually Inhabit The ColonDokument4 SeitenColi Bacterial Strains That Usually Inhabit The Colonemman122392Noch keine Bewertungen
- ####Bahan Kuliah ISK Blok 23 (Nov 2015)Dokument32 Seiten####Bahan Kuliah ISK Blok 23 (Nov 2015)ajengdmrNoch keine Bewertungen
- Urinary Disorders 2Dokument19 SeitenUrinary Disorders 2ula mdiNoch keine Bewertungen
- Urinary Tract Infection (UTI)Dokument39 SeitenUrinary Tract Infection (UTI)Sabita TripathiNoch keine Bewertungen
- Microbial Diseases of The Urinary System: Yemane Weldu (MSC., Assistant Professor)Dokument65 SeitenMicrobial Diseases of The Urinary System: Yemane Weldu (MSC., Assistant Professor)Lidiya TeshomeNoch keine Bewertungen
- Rinary Ract Nfections: Classification Pathophysiology Risk Factors Clinical Manifestation DiagnosticsDokument27 SeitenRinary Ract Nfections: Classification Pathophysiology Risk Factors Clinical Manifestation DiagnosticsDARYmagpantayNoch keine Bewertungen
- Female Urinary SystemDokument5 SeitenFemale Urinary SystemVikas SarkarNoch keine Bewertungen
- Uti Case StudyDokument7 SeitenUti Case StudyStephNoch keine Bewertungen
- Pyelonephritis 508Dokument8 SeitenPyelonephritis 508Dery ZhibharanyNoch keine Bewertungen
- Renal Notes Step 2ckDokument34 SeitenRenal Notes Step 2cksamreen100% (1)
- HYDRONEPHROSISDokument13 SeitenHYDRONEPHROSISAaroma BaghNoch keine Bewertungen
- Symptoms: For Bladder InfectionsDokument5 SeitenSymptoms: For Bladder InfectionsGene Ryuzaki SeseNoch keine Bewertungen
- Infection Urinary Tract Urine Bladder KidneyDokument18 SeitenInfection Urinary Tract Urine Bladder KidneygdquijanoNoch keine Bewertungen
- Urinary Tract InfectionsDokument15 SeitenUrinary Tract Infectionspreetie87Noch keine Bewertungen
- What Is The Urinary TractDokument1 SeiteWhat Is The Urinary TractAlou Dacuya CortezanoNoch keine Bewertungen
- Frequent Urination - What Causes A Frequent Urge To PeeDokument11 SeitenFrequent Urination - What Causes A Frequent Urge To PeeJimmy GillNoch keine Bewertungen
- What Is A Urinary Tract InfectionDokument3 SeitenWhat Is A Urinary Tract InfectionStepyn SalvadorNoch keine Bewertungen
- Uti PathoDokument15 SeitenUti PathoEden Astred ObilloNoch keine Bewertungen
- Slideshow For DadDokument25 SeitenSlideshow For DadJeremiah NayosanNoch keine Bewertungen
- Electrical TransformerDokument37 SeitenElectrical TransformerJeremiah NayosanNoch keine Bewertungen
- Classroom Program: Time No. of Minutes Learning AreasDokument4 SeitenClassroom Program: Time No. of Minutes Learning AreasJeremiah NayosanNoch keine Bewertungen
- Topic 16Dokument4 SeitenTopic 16Jeremiah NayosanNoch keine Bewertungen
- My ResumeDokument2 SeitenMy ResumeJeremiah NayosanNoch keine Bewertungen
- Basic Concepts of MovementDokument6 SeitenBasic Concepts of MovementJeremiah NayosanNoch keine Bewertungen
- Prof Ed SetDokument5 SeitenProf Ed SetIyen Dalisay100% (3)
- The Kalanguya TribeDokument3 SeitenThe Kalanguya TribeJeremiah Nayosan100% (1)
- K To 12 Basic Education CurriculumDokument7 SeitenK To 12 Basic Education CurriculumJeremiah NayosanNoch keine Bewertungen
- Test Questions. ShirineDokument6 SeitenTest Questions. ShirineJeremiah NayosanNoch keine Bewertungen
- Leadership Style of Mr222Dokument3 SeitenLeadership Style of Mr222Jeremiah NayosanNoch keine Bewertungen
- Evaluative Paragraph Municipality of KasibuDokument1 SeiteEvaluative Paragraph Municipality of KasibuJeremiah NayosanNoch keine Bewertungen
- Davies L. Luto: I Hereby Certify That The Above Information Is True and Correct To The Best of My Knowledge and BeliefDokument2 SeitenDavies L. Luto: I Hereby Certify That The Above Information Is True and Correct To The Best of My Knowledge and BeliefJeremiah Nayosan0% (1)
- The Nitrogen CycleDokument4 SeitenThe Nitrogen CycleJeremiah NayosanNoch keine Bewertungen
- Fundamentals of Criminal InvestigationDokument13 SeitenFundamentals of Criminal InvestigationJeremiah Nayosan100% (2)
- Detailed Lesson Plan in English V CarolineDokument5 SeitenDetailed Lesson Plan in English V CarolineJeremiah Nayosan100% (2)
- Ciminalistics Eteeap BeneficiaryDokument11 SeitenCiminalistics Eteeap BeneficiaryJeremiah Nayosan100% (3)
- Chapter 1Dokument8 SeitenChapter 1Jeremiah NayosanNoch keine Bewertungen
- How Government Corruptions Can Affect The Program of DevelopmentDokument5 SeitenHow Government Corruptions Can Affect The Program of DevelopmentJeremiah NayosanNoch keine Bewertungen
- Orayt Multi-Purpose CooperativeDokument1 SeiteOrayt Multi-Purpose CooperativeJeremiah NayosanNoch keine Bewertungen
- El Cid CompeadorDokument15 SeitenEl Cid CompeadorJeremiah NayosanNoch keine Bewertungen
- CASE STUDY HardDokument16 SeitenCASE STUDY HardJeremiah NayosanNoch keine Bewertungen
- How Does A Universal Motor WorkDokument3 SeitenHow Does A Universal Motor WorkJeremiah NayosanNoch keine Bewertungen
- Bambang HistoryDokument16 SeitenBambang HistoryJeremiah Nayosan75% (4)
- Test Statistics Fact SheetDokument4 SeitenTest Statistics Fact SheetIra CervoNoch keine Bewertungen
- Accountancy Department: Preliminary Examination in MANACO 1Dokument3 SeitenAccountancy Department: Preliminary Examination in MANACO 1Gracelle Mae Oraller0% (1)
- India: SupplyDokument6 SeitenIndia: SupplyHarish NathanNoch keine Bewertungen
- Rosenberg Et Al - Through Interpreters' Eyes, Comparing Roles of Professional and Family InterpretersDokument7 SeitenRosenberg Et Al - Through Interpreters' Eyes, Comparing Roles of Professional and Family InterpretersMaria AguilarNoch keine Bewertungen
- Chapter 9 - PPT (New)Dokument43 SeitenChapter 9 - PPT (New)Syarifah NourazlinNoch keine Bewertungen
- Lodge LeadershipDokument216 SeitenLodge LeadershipIoannis KanlisNoch keine Bewertungen
- HIS Unit COMBINES Two Birthdays:: George Washington's BirthdayDokument9 SeitenHIS Unit COMBINES Two Birthdays:: George Washington's BirthdayOscar Panez LizargaNoch keine Bewertungen
- Crime Scene Manual FullDokument19 SeitenCrime Scene Manual FullMuhammed MUZZAMMILNoch keine Bewertungen
- Easter in RomaniaDokument5 SeitenEaster in RomaniaDragos IonutNoch keine Bewertungen
- Trigonometry Primer Problem Set Solns PDFDokument80 SeitenTrigonometry Primer Problem Set Solns PDFderenz30Noch keine Bewertungen
- THE LAW OF - John Searl Solution PDFDokument50 SeitenTHE LAW OF - John Searl Solution PDFerehov1100% (1)
- Created By: Susan JonesDokument246 SeitenCreated By: Susan JonesdanitzavgNoch keine Bewertungen
- Literature Review On Catfish ProductionDokument5 SeitenLiterature Review On Catfish Productionafmzyodduapftb100% (1)
- Indus Valley Sites in IndiaDokument52 SeitenIndus Valley Sites in IndiaDurai IlasunNoch keine Bewertungen
- Google Automatically Generates HTML Versions of Documents As We Crawl The WebDokument2 SeitenGoogle Automatically Generates HTML Versions of Documents As We Crawl The Websuchi ravaliaNoch keine Bewertungen
- AdvacDokument13 SeitenAdvacAmie Jane MirandaNoch keine Bewertungen
- Chapter 12 NotesDokument4 SeitenChapter 12 NotesIvanTh3Great100% (6)
- Research PresentationDokument11 SeitenResearch PresentationTeano Jr. Carmelo C.Noch keine Bewertungen
- WHAT - IS - SOCIOLOGY (1) (Repaired)Dokument23 SeitenWHAT - IS - SOCIOLOGY (1) (Repaired)Sarthika Singhal Sarthika SinghalNoch keine Bewertungen
- Short-Term Load Forecasting by Artificial Intelligent Technologies PDFDokument446 SeitenShort-Term Load Forecasting by Artificial Intelligent Technologies PDFnssnitNoch keine Bewertungen
- Thesis Statement VampiresDokument6 SeitenThesis Statement Vampireslaurasmithdesmoines100% (2)
- Bagon-Taas Adventist Youth ConstitutionDokument11 SeitenBagon-Taas Adventist Youth ConstitutionJoseph Joshua A. PaLaparNoch keine Bewertungen
- Economic Value Added in ComDokument7 SeitenEconomic Value Added in Comhareshsoni21Noch keine Bewertungen
- Database Programming With SQL Section 2 QuizDokument6 SeitenDatabase Programming With SQL Section 2 QuizJosé Obeniel LópezNoch keine Bewertungen
- Configuration Steps - Settlement Management in S - 4 HANA - SAP BlogsDokument30 SeitenConfiguration Steps - Settlement Management in S - 4 HANA - SAP Blogsenza100% (4)
- De La Salle Araneta University Grading SystemDokument2 SeitenDe La Salle Araneta University Grading Systemnicolaus copernicus100% (2)
- MOA Agri BaseDokument6 SeitenMOA Agri BaseRodj Eli Mikael Viernes-IncognitoNoch keine Bewertungen
- Sentence Connectors: 1.contrast 1. A. Direct OppositionDokument8 SeitenSentence Connectors: 1.contrast 1. A. Direct OppositionCathy siganNoch keine Bewertungen
- SuperconductorDokument33 SeitenSuperconductorCrisanta GanadoNoch keine Bewertungen
- 1 Mark QuestionsDokument8 Seiten1 Mark QuestionsPhani Chintu100% (2)