Beruflich Dokumente
Kultur Dokumente
MC Versus LC
Hochgeladen von
M Iqbal Rahadyanto0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
24 Ansichten5 Seitenmini laparotomy journal
Copyright
© © All Rights Reserved
Verfügbare Formate
PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenmini laparotomy journal
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
24 Ansichten5 SeitenMC Versus LC
Hochgeladen von
M Iqbal Rahadyantomini laparotomy journal
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 5
Egyptian Journal of Surgery 214
Egyptian J ournal of Surgery Vol. 32, No. 3, J ul y 2013
ORIGINAL ARTICLE
M I N I LA P AR O TO M Y C H O LE C YS TE C TO M Y VE R S U S LAP A R O S C O P I C
C H O LE C YS TE C TO M Y: A P R O S P E C TI VE R AN D O M I Z E D S TU D Y
Mahmoud Abdelhameid Mahmoud,
1
Mohammed Korany,
2
Mohammed Khalil Elammary,
1
Hamdy M Hussein
1
1
General Surgery Department, Qena University Hospital, South Valley University,
2
General Surgery Department, Assiut
University Hospital, Assiut University, Egypt
Correspondence to: Mahmoud Abdelhameid Mahmoud, Email: mahmoud_abdelhameid@yahoo.com
Abstract
Background and Aim: Minilaparotomy cholecystectomy (MC) and laparoscopic cholecystectomy (LC) are
commonly applied surgical techniques in the management of non-complicated symptomatic gallstone disease.
We compared both MC and LC in a randomized trial.
Patients and Method: Forty three patients underwent LC were compared to forty five patients who
underwent MC (It is defined in this study as open cholecystectomy through incision less than 8 cm length).
The items of comparison were operative duration, operative and post-operative complications and success of
the procedure as one day surgery.
Results: Both groups were comparable as regarding age, sex, BMI and ASA status. The operation time was
statistically significant shorter for MC group when compared to LC group (P=0.001). In LC group; 2 patients
out of 43 patients (4.65%) were converted into the classic open method (one patient was due to massive
adhesion in the area of Calots triangle and the second patient was due to injury of CBD), while in MC group;
3 cases out of 45 cases (6.67%) required a more generous incision to use larger retractors to obtain a clearer
view of Calots triangle. The hospital stay for the LC group ranged between 12-24 hrs which is shorter than
the 1-2 days of the MC group. There were no significant late postoperative complications apart from 3 cases of
superficial surgical site infections among LC group and 2 cases among the MC group. LC
was successful as one day surgery in 40 patients out of 43 patients (the failure were due to; CBD injury and
patients couldn't tolerate oral fluid intake due to post-operative nausea and vomiting not respond
to the ordinary prokinetic drugs) while it was successful in 44 patients out of 45 patients among the MC
group (the failure was due to intolerable postoperative pain required 2 days admission for parenteral
analgesic).
Conclusion: MC was a better alternative to LC because of its shorter operative time, lower
complication rates and it didn't require learning curve or special instruments. LC had a faster post-operative
recovery.
Keywords: Minilaparotomy, laparoscopic cholecystectomy, one day surgery.
EJS, Vol. 32, No. 3, July 2013 215
INTRODUCTION
The first to describe cholecystectomy through a
minilaparotomy was probably Dubois, in 1982.
(1)
It
appears that the term "minicholecystectomy" (MC) was
coined by Goco and Chambers in 1983.
(2)
Minicholecystectomy refers to an operation performed
through a short right subcostal incision (4-10cm), offering
the currently much-spoken-about advantages of
minimally invasive surgery.
(3)
The benefits of this
procedure are well documented in a substantial number
of papers and abstracts published since.
(4-7)
Unfortunately, because of the "laparoscopic fever" which
has recently struck the international surgical community,
most surgeons feel compelled to adopt the
apparently more "glamorous" laparoscopic
cholecystectomy (LC). Consequently, MC remains at
present a relatively obscure and unpractised
procedure.
(4)
The aim of this study was to compare the results of the
laparoscopic (LC) and mini-laparotomy (MC) approach
to cholecystectomy, performed in Qena University
Hospital, South Valley University and in Assiut
University Hospital, Assiut University.
PATIENTS AND METHODS
All patients with gallstone disease were evaluated:
Clinical history and examination,
Abdominal US.
Preoperative respiratory function tests.
Routine investigations: CBC, Renal function tests,
Random blood sugar, Liver function tests, ECG, and
chest X ray.
Investigations may be required as MRCP.
Inclusion criteria:
Adults between 18 years and 50 years.
BMI: <30 kg/ m2.
ASA: I or II.
Normal pre-operative liver function tests.
No history of Jaundice.
Patients were assigned randomly in one of the 2
groups:
Group LC: patients were operated by the classic 4
ports laparoscopic cholecystectomy (12 mm port at
the umbilicus, 12 mm port at the epigastric region, 5
mm subcostal port at mid-clavicular line, 5 mm
subcostal port at anterior axillary line).
Group MC: patients were operated on through a
subcostal incision which in not more than 8 cm
length (Fig 1), medial retraction of rectus muscle was
required (without cutting of rectus muscle) in some
cases. Retrograde cholecystectomy "fundus down
technique" was performed if there was any difficulty
to identify safely the cystic duct or the artery by the
classic method.
Conversion was considered (for both groups) if the
operation was completed by the classic long subcostal
incision.
The following items were compared between the 2
groups:
Operative duration: from skin incision to skin
closure, including the time required to set up the
laparoscopic tubes, cables and instruments in LC
group.
Operative Complications: as bleeding, CBD injury
Hospitals stay (the number of nights in the hospital
after surgery plus nights during any readmission).
Short term follow up up to 6 months": for wound
infection, bile or blood collection, CBD stricture,
jaundice.
The criteria for discharge were strict. It included:
1. Stable vital data.
2. Tolerable pain.
3. No nausea, nor vomiting.
4. Tolerate light oral intake.
5. Self-care parameters: patient can walk to toilet
unsupported, can pull a sheet to cover himself.
Fund: The research was funded by the resources of Qena
University Hospital and Assiut University hospital.
Ethical Considerations: Written consent is signed by
each patient pre-operatively after complete simplified
clarification of the procedure to each one.
Statistical analysis: The results are expressed as the
mean SD& number (%). Statistical analysis was
performed with the software SPSS version 12, using
student T. test to determine significant for numeric
data, using Chi. square to determine sign for non-
parametric data. P value was determined as significant
(P<0.05).
Egyptian Journal of Surgery 216
Fig 1. Subcostal minilaparotomy incision.
RESULTS
Eighty eight patients were included in this study; 43
patients were included in LC group while the MC group
included 45 patients.
There were no statistical significant differences between
the two groups in terms of gender, age, body mass index
(BMI), or American Association of Anesthesiologist
(ASA) physical fitness classification. (Table 1).
Table 1. Data of the patients.
LC (43 pt.) MC (45 pt.) P value
Age (years) 20-61(36.2 ) 22-60 (37.2) .4
Sex (M:F) 5:38 5:40 .601
BMI range (mean) 20:29 (23.2) 19:30 (24) .45
ASA Status: I;II 22;21 22;23 .5
Conversion rate 2/ 43 (4.65 %) 3/ 45 (6.67 %) .52
Operating time (min) 35-160 (7527) 25-120 (5216) .001
Operative complications 1/ 43 0/ 45 .49
Hospital Stay (days) 12-24 hrs 1-2 days .376
Late complications 3/ 43 2/ 45 .47
In LC group; 2 patients out of 43 patients (4.65%) were
converted into the classic open method; one patient was
due to massive adhesion in the area of Calots triangle
while the second patient was due to injury of CBD which
required open surgery to repair the injury on T shaped
tube. In MC group; 3 cases out of 45 cases (6.67%)
EJS, Vol. 32, No. 3, July 2013 217
required a more generous incision to use larger retractors
to obtain a clearer view of Calots triangle.
The operating time for patients of LC group (7527 mins)
was significantly longer than the operating time for MC
group (5216 mins) (P value =0.001).
The hospital stay for the LC group ranged between 12- 24
hours which is shorter than the 1-2 days of the MC group
(we excluded the single case of LC which suffered CBD
injury and required 9 days of post-operative hospital
stay).
There were no significant late postoperative
complications apart from 3 cases of superficial surgical
site infections among LC group and 2 cases among the
MC group. They were treated by Antibiotics and
repeated dressings.
LC was successful as one day surgery in 40 patients out
of 43 patients (the failure were due to; CBD injury and
patients couldn't tolerate oral fluid intake due to post-
operative nausea and vomiting not respond to the
ordinary prokinetic drugs) while it was successful in 44
patients out of 45 patients among the MC group (the
failure was due to intolerable postoperative pain
required 2 days admission for parenteral analgesic).
DISCUSSION
During the past 15 years, LC has been established as a
dominant cholecystectomy procedure despite studies
showing MC to be very comparable.
(8-14)
There may be several reasons that favor laparoscopy
without firm scientific evidence. Companies that sell
laparoscopic instruments also may influence surgeons'
attitudes. Both patients and surgeons often have the
attitude that laparoscopy is a modern and more
advanced technique than open surgery, which may
influence patient recovery.
(8)
In earlier studies comparing LC and MC operations,
there was great variation in the MC technique, especially
concerning whether the rectus muscle was cut or not and
the maximum size of an incision. We believe that the
incision technique plays a major role in the MC
procedure. In our opinion, cutting the rectus muscle
means conversion to conventional laparotomy. The
variation in incision technique might explain the
differences in results between MC and LC studies.
(8)
In several earlier studies, the operating time from skin
incision to closure was shorter for the MC group than
for the LC group,
(10,13,15-17)
which also was seen in our
study. The operating time for the LC group was rather
long, may be because the time required for setting up
laparoscopic tubes, cables and instruments.
The postoperative hospital stay was slightly shorter for
the LC group in some studies,
(15,16,18)
but some studies
showed no difference in the postoperative hospital stay
between MC and LC.
(10,11,13,14)
In our study, the
postoperative hospital stay for LC group looked
prolonged when compared to MC group because one
case sustained CBD injury that needed a longer hospital
stay. This is an important result for health care
administrators because of limitations in health care
resources.
There are several reports in the literature that compare
complication and bile duct injury rates after LC and
Open Cholecystectomy (OC). Buanes and Mjaland.
(19)
in
a prospective comparative study between LC and OC,
reported significantly higher complication rates in the
open group (16% vs 9%). Similar results have been
reported by McIntyre et al. (20), who presented lower
morbidity after LC than after OC (3% vs 7%) and by
Williams et al.
(21)
who also reported lower complication
rates in the laparoscopic group (3.1% vs 7.5%), but in this
study fewer bile duct injuries occurred in the open
group.
However, McMahon et al.
(16)
and Ros et al.,
(17)
in
randomized trials that compared LC and MC, presented
similar rates of morbidity and bile duct injury between
the two groups. On the other hand, Targarona et al.,
(22)
in
a retrospective comparative study that focused on bile
duct injuries among 3,051 OCs and 1,630 LCs, reported
significantly higher rates of such complications in the
laparoscopic group. In our study, CBD injury rate was
significantly higher in the LC group.
As regarding to the minor complications, there were two
wound infections in the MC group as compared with
three in the LC group; the difference was not statistically
significant.
The instrumentation for the MC procedure is rather easy.
No disposable instruments are needed, whereas for the
LC procedure, disposable instruments often are used.
The cheaper instrumentation and the shorter operating
time combined with a similar recovery implies a cost
advantage for MC. The MC technique was a new
procedure compared with LC. However, it seems that
there is no remarkable learning curve for the MC
procedure.
In conclusion; Minilaparoscopic cholecystectomy is a
faster technique and has lower complication rates when
compared to laparoscopic cholecystectomy. Although LC
had a shorter post-operative hospital stay than MC, MC
may be performed as one day procedure in some
patients.
Egyptian Journal of Surgery 218
REFERENCES
1. Dubois F, Barthelot G. Cholecystectomie par
minilaparotomie. Nouv.Presse. Med. 1982;11:1139-41.
2. Goco I, Chambers L. "Mini-cholecystectomy" and
operative cholangiography. A mean of cost containment.
Am. Surg. 1983;49:143-5.
3. Cheslyn-Curtis S, Russell R. New trends in gallstone
management. Br. J. Surg. 1991;78:143-9.
4. Assalia A, Schein M, Kopelman D, Hashmonai M.
Minicholecystectomy vs. Conventional Cholecystectomy:
A Prospective Randomized Trial -Implications in the
Laparoscopic Era. W.J.S. 1993;17:755-9.
5. O'Dwyer P, Murphy J, O'Higgins N. Cholecystectomy
through a 5 cm subcostal incision. Br. J. Surg.
1990;77:1189-90.
6. O'Kelly T, Barr H, Malley W, Kettlewell M.
Cholecystectomy through a 5 cm subcostal incision. Br. J.
Surg. 1991;78:762.
7. Merrill J. Minimal trauma cholecystectomy (a "no
touch"procedure in a "well"). Am. Surg. 1988;54:256-61.
8. Harju J, Juvonen P, Eskelinen M, et al. Minilaparotomy
cholecystectomy versus laparoscopic cholecystectomy. A
randomized study with special reference to obesity. Surg
Endosc. 2006;20:5836.
9. Al-Tameem M. Minilaparotomy cholecystectomy. J R
Coll Surg Edinb. 1993;38:1547.
10. Majeed A, Troy G, Nicholl J, et al. Randomized,
prospective, single-blind comparison of laparoscopic
versus small-incision cholecystectomy. Lancet.
1996;347:98994.
11. Oyogoa S, Komenaka I, Ilkhani R. Minilaparotomy
cholecystectomy in the era of laparoscopic
cholecystectomy: A community-based hospital
perspective. Am. Surg. 2003;69:6047.
12. Squirrell D, Majeed A, Troy G, et al. A randomized,
prospective, blinded comparison of postoperative pain,
metabolic response, and perceived health after
laparoscopic and small incision cholecystectomy. Surgery.
1998;123:48595.
13. Syrakos T, Antonitsis P, Zacharakis E, et al. Small-incision
(minilaparotomy) versus laparoscopic cholecystectomy: a
retrospective study in a university hospital. Langenbecks
Arch Surg. 2004;389:1727.
14. Tyagi N, Meredith M, Lumb J, et al. A new minimal
invasive technique for cholecystectomy: subxiphoid
minimal stress triangle microceliotomy. Ann Surg.1994;
220: 617625.
15. McGinn F, Miles A, Uglow M, et al. Randomized trial of
laparoscopic and minicholecystectomy. Br J Surg.
1995;82:13747.
16. McMahon A, Russell I, Baxter J, et al. Laparoscopic versus
minilaparotomy cholecystectomy: a randomised trial.
Lancet. 1994;343:1358.
17. Ros A, Gustafsson L, Krook H, et al. Laparoscopic
cholecystectomy versus minilaparotomy cholecystectomy:
a prospective, randomized, single blind study. Ann Surg.
2001;234:7419.
18. Makinen A, Nordback I. Cholecystectomy:
comparison of minilaparotomy and laparoscopy. Int Surg.
1995;80:99101.
19. Buanes T, Mjaland O. Complications in laparoscopic and
open cholecystectomy: a prospective comparative trial.
Surg Laparosc Endosc. 1996;6:26672.
20. McIntyre R, Zoeter M, Weil K, Cohen M. A comparison
of outcome and cost of open vs. laparoscopic
cholecystectomy. J Laparoendosc Surg. 1992;2:1438.
21. Williams L, Chapman W, Bonau R, McGee E, et al.
Comparison of laparoscopic cholecystectomy with open
cholecystectomy in a single centre. Am. J. Surg.
1993;165:45965.
22. Targarona E, Marco C, Balague C, et al. How, when,
and why bile duct injury occurs. Surg Endosc.
1998;12:3226.
Das könnte Ihnen auch gefallen
- DAFTAR PUSTAKA BenarDokument2 SeitenDAFTAR PUSTAKA BenarM Iqbal RahadyantoNoch keine Bewertungen
- Connection StatusDokument2 SeitenConnection StatusM Iqbal RahadyantoNoch keine Bewertungen
- Sawaguchi Et Al-2012-Journal of Diabetes InvestigationDokument7 SeitenSawaguchi Et Al-2012-Journal of Diabetes InvestigationM Iqbal RahadyantoNoch keine Bewertungen
- DAFTAR PUSTAKA BenarDokument2 SeitenDAFTAR PUSTAKA BenarM Iqbal RahadyantoNoch keine Bewertungen
- Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) - Blood Clot Forming in A VeinDokument1 SeiteDeep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) - Blood Clot Forming in A VeinM Iqbal RahadyantoNoch keine Bewertungen
- Legal Information: System RequirementsDokument4 SeitenLegal Information: System RequirementsAlex BogdanNoch keine Bewertungen
- Attention To: HRD Manager PT Well Harvest Winning Alumina RefineryDokument1 SeiteAttention To: HRD Manager PT Well Harvest Winning Alumina RefineryM Iqbal RahadyantoNoch keine Bewertungen
- Ukuran Organ TubuhDokument1 SeiteUkuran Organ TubuhDiah Karomah PutriNoch keine Bewertungen
- Physical AdressDokument1 SeitePhysical AdressM Iqbal RahadyantoNoch keine Bewertungen
- Bayley ScalesDokument15 SeitenBayley ScalesM Iqbal RahadyantoNoch keine Bewertungen
- Saudi JAnaestesiaDokument5 SeitenSaudi JAnaestesiaM Iqbal RahadyantoNoch keine Bewertungen
- Physical AdressDokument1 SeitePhysical AdressM Iqbal RahadyantoNoch keine Bewertungen
- DAFTAR PUSTAKA BenarDokument2 SeitenDAFTAR PUSTAKA BenarM Iqbal RahadyantoNoch keine Bewertungen
- Oral Ivermectin Versus Malathion Lotion For Difficult-to-Treat Head LiceDokument10 SeitenOral Ivermectin Versus Malathion Lotion For Difficult-to-Treat Head LiceM Iqbal RahadyantoNoch keine Bewertungen
- URLListDokument3 SeitenURLListborman007Noch keine Bewertungen
- FilesDokument2 SeitenFilesFilip NedicNoch keine Bewertungen
- HLTV ReadmeDokument9 SeitenHLTV Readmewillquem16100% (4)
- Half-Life Version 1.1.1.1 Readme File 12/2/02Dokument18 SeitenHalf-Life Version 1.1.1.1 Readme File 12/2/02MemMinhNoch keine Bewertungen
- 52 HypoglycemiaDokument2 Seiten52 HypoglycemiaphobicmdNoch keine Bewertungen
- DAFTAR PUSTAKA BenarDokument2 SeitenDAFTAR PUSTAKA BenarM Iqbal RahadyantoNoch keine Bewertungen
- PCConsole TOCDokument1 SeitePCConsole TOCM Iqbal RahadyantoNoch keine Bewertungen
- Calende Event KasahfDokument4 SeitenCalende Event KasahfM Iqbal RahadyantoNoch keine Bewertungen
- Ê ÓÃË Ã÷Dokument2 SeitenÊ ÓÃË Ã÷FirmansyahAgilNoch keine Bewertungen
- 52 HypoglycemiaDokument2 Seiten52 HypoglycemiaphobicmdNoch keine Bewertungen
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5784)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (399)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (890)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (587)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (265)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (72)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2219)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (119)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- Maintenance of Gingival Form Following Implant PlacementDokument4 SeitenMaintenance of Gingival Form Following Implant PlacementRomina BitaNoch keine Bewertungen
- 0 1 The Pathophysiology of Shoulder Instability 2800953368Dokument8 Seiten0 1 The Pathophysiology of Shoulder Instability 2800953368César ArveláezNoch keine Bewertungen
- Case Log DefinitionsDokument6 SeitenCase Log DefinitionsSarah DNoch keine Bewertungen
- CRST1008 06Dokument4 SeitenCRST1008 06khairul ihsanNoch keine Bewertungen
- Nursing Process Care Plan: Assessment Analysis Planning Implementation EvaluationDokument2 SeitenNursing Process Care Plan: Assessment Analysis Planning Implementation EvaluationJamaila DomingoNoch keine Bewertungen
- Completion Lobectomy After WedgeDokument6 SeitenCompletion Lobectomy After WedgeAlin Ionut BurlacuNoch keine Bewertungen
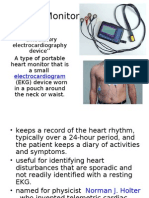
- Holter Monitor: 'Ambulatory Electrocardiography Device''Dokument22 SeitenHolter Monitor: 'Ambulatory Electrocardiography Device''Rachel PeredaNoch keine Bewertungen
- 1 PBDokument8 Seiten1 PBMahathir Harry PermanaNoch keine Bewertungen
- OT AssistantDokument9 SeitenOT AssistantIshfaq LoneNoch keine Bewertungen
- Broach TrialDokument1 SeiteBroach Trialjmhinos4833Noch keine Bewertungen
- Human Body Systems - Overview, Anatomy, Functions - KenhubDokument13 SeitenHuman Body Systems - Overview, Anatomy, Functions - Kenhubregina.rmsNoch keine Bewertungen
- Endoscopy and Microendoscopy of The Lacrimal Drainage SystemDokument60 SeitenEndoscopy and Microendoscopy of The Lacrimal Drainage SystemhwalijeeNoch keine Bewertungen
- FIRST PRENATAL VISIT CHECKLISTDokument8 SeitenFIRST PRENATAL VISIT CHECKLISTNadine BacalangcoNoch keine Bewertungen
- Avoiding Common Errors in The Emergency Department-1002-1280Dokument280 SeitenAvoiding Common Errors in The Emergency Department-1002-1280Hernando CastrillónNoch keine Bewertungen
- Managing Bone FracturesDokument2 SeitenManaging Bone FracturesMa. Ferimi Gleam BajadoNoch keine Bewertungen
- Advanced GI Nursing CareDokument13 SeitenAdvanced GI Nursing CareBobbi-MarieNoch keine Bewertungen
- A CT Scan or Computed Tomography ScanDokument7 SeitenA CT Scan or Computed Tomography ScanMonaysNoch keine Bewertungen
- Chapter 8 Self-Assessment Q&ADokument5 SeitenChapter 8 Self-Assessment Q&Apblinder1319Noch keine Bewertungen
- CCN CardioDokument5 SeitenCCN CardioSofia P. PanlilioNoch keine Bewertungen
- Zago - Essential US For Trauma - E-FASTDokument104 SeitenZago - Essential US For Trauma - E-FASTPetru Adăscăliţei100% (2)
- Femoral Hernia in MenDokument2 SeitenFemoral Hernia in MenSa FariNoch keine Bewertungen
- Diseases of Lacrimal ApparatusDokument46 SeitenDiseases of Lacrimal Apparatusসপ্নে ছোয়া মন100% (1)
- Periodontology 2000 - 2014 - Pjetursson - Sinus Floor Elevation Utilizing The Transalveolar ApproachDokument13 SeitenPeriodontology 2000 - 2014 - Pjetursson - Sinus Floor Elevation Utilizing The Transalveolar ApproachNourhan IbrahimNoch keine Bewertungen
- Pelvic Walls, Joints, Vessels & Nerves, Pelvic Organs PPT FinalDokument106 SeitenPelvic Walls, Joints, Vessels & Nerves, Pelvic Organs PPT Finalntege stuart100% (1)
- A Complicated Case of Incisional HerniaDokument29 SeitenA Complicated Case of Incisional Herniabheemrajy00Noch keine Bewertungen
- 1.15 ANATOMY - The LarynxDokument2 Seiten1.15 ANATOMY - The LarynxPaolo NaguitNoch keine Bewertungen
- Pds Price ListDokument8 SeitenPds Price ListRichard TaylorNoch keine Bewertungen
- (Board Review Series) Linda S. Costanzo - BRS Physiology, 5th Edition (Board Review Series) - Lippincott Williams & Wilkins (2010)Dokument7 Seiten(Board Review Series) Linda S. Costanzo - BRS Physiology, 5th Edition (Board Review Series) - Lippincott Williams & Wilkins (2010)Salifyanji SimpambaNoch keine Bewertungen
- 40th Annual Percivall Pott Scientific MeetingDokument26 Seiten40th Annual Percivall Pott Scientific MeetingAlex Mulligan100% (1)
- Surgical Anatomy of Nose and Maxilliary SinusDokument17 SeitenSurgical Anatomy of Nose and Maxilliary SinusAnish Kumar100% (1)