Beruflich Dokumente
Kultur Dokumente
Understanding Rheumatic Fever
Hochgeladen von
gitozsby0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
26 Ansichten7 SeitenRheumatic fever is a complication of untreated strep throat. It causes fever, muscle aches, swollen and painful joints. The greatest danger from the disease is the damage it can do to the heart.
Originalbeschreibung:
Originaltitel
Understanding Rheumatic Fever.docx
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenRheumatic fever is a complication of untreated strep throat. It causes fever, muscle aches, swollen and painful joints. The greatest danger from the disease is the damage it can do to the heart.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
26 Ansichten7 SeitenUnderstanding Rheumatic Fever
Hochgeladen von
gitozsbyRheumatic fever is a complication of untreated strep throat. It causes fever, muscle aches, swollen and painful joints. The greatest danger from the disease is the damage it can do to the heart.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 7
Understanding Rheumatic Fever
What Is Rheumatic Fever?
A rare but potentially life-threatening disease, rheumatic fever is a complication of untreated
strep throat caused by bacteria called group A streptococcus. The main symptoms -- fever,
muscle aches, swollen and painful joints, and in some cases, a red, lattice-like rash --
typically begin one to six weeks after a bout of strep. In some cases, though, the infection
may have been too mild to have been recognized.
Rheumatic fever can also cause a temporary nervous system disorder once known as St.
Vitus' dance. Today it is called chorea, or Sydenham's chorea. This is a nervous disorder --
characterized by rapid, jerky, involuntary movements of the body -- occurring chiefly in
childhood or during pregnancy and closely associated with rheumatic fever. People with mild
cases of chorea may find it difficult to concentrate or write. More severe cases can cause the
muscles of the arms, legs, or face to twitch uncontrollably.
The knees, ankles, elbows, and wrists are the joints most likely to become swollen from
rheumatic fever. The pain often migrates from one joint to another. However, the greatest
danger from the disease is the damage it can do to the heart. In more than half of all cases,
rheumatic fever scars the valves of the heart, forcing this vital organ to work harder to pump
blood. Over a period of months or even years -- particularly if the disease strikes again -- this
damage to the heart can lead to a serious condition known as rheumatic heart disease, which
can eventually cause the heart to fail.
Because of antibiotics, rheumatic fever is now rare in developed countries. In recent years,
though, it has begun to make a comeback in the U.S., particularly among children living in
poor, inner-city neighborhoods. The disease tends to strike most often in cool, damp weather
during the winter and early spring. In the U.S., it is most common in the northern states.
What Causes Rheumatic Fever?
Rheumatic fever results from an inflammatory reaction to certain group A
streptococcusbacteria. The body produces antibodies to fight the bacteria, but instead the
antibodies attack a different target: the body's own tissues. The antibodies begin with the
joints and often move on to the heart and surrounding tissues. Because only a small fraction
(fewer than 0.3%) of people with strep throat ever contract rheumatic fever, medical experts
say that other factors, such as a weakened immune system, must also be involved in the
development of the disease.
CAUTION! Monitor That Sore Throat
Pay attention to sore throats, especially in children. If your child has a severe sore throat
without other cold symptoms, accompanied by a fever higher than 101 degrees Fahrenheit, or
a milder sore throat that persists for more than two or three days, see a doctor. It may be strep
throat, which should be treated with antibiotics
Endocarditis
Endocarditis is inflammation of the inside lining of the heart chambers and heart valves
(endocardium).
Causes
Endocarditis can involve the heart muscle, heart valves, or lining of the heart. Most people
who develop endocarditis have a:
Birth defect of the heart
Damaged or abnormal heart valve
History of endocarditis
New heart valve after surgery
Endocarditis begins when different germs enter the bloodstream and then travel to the heart.
Bacterial infection is the most common cause of endocarditis.
Endocarditis can also be caused by fungi, such as Candida.
In some cases, no cause can be found.
Germs are most likely to enter the bloodstream during:
Central venous access lines
Injection drug use, from the use of unclean (unsterile) needles
Recent dental surgery
Other surgeries or minor procedures to the breathing tract, urinary tract, infected skin,
or bones and muscles
Symptoms
Symptoms of endocarditis may develop slowly or suddenly.
Fever, chills, and sweating are the classic symptoms. These sometimes can:
Be present for days before any other symptoms appear
Come and go, or be more noticeable at nighttime
Fatigue, weakness, and aches and pains in the muscles or joints may also be present.
Other symptoms can include:
Small areas of bleeding under the nails (splinter hemorrhages)
Red, painless skin spots on the palms and soles (Janeway lesions)
Red, painful nodes in the pads of the fingers and toes (Osler's nodes)
Shortness of breath with activity
Swelling of feet, legs, abdomen
Exams and Tests
The health care provider may detect a new heart murmur, or a change in a past heart murmur.
An eye exam may show bleeding in the retina and a central area of clearing. This is known as
Roth's spots. There may be small, pinpoint areas of bleeding on the surface of the eye or the
eyelids.
Tests that may be done include:
Blood culture -- helps identify the bacteria or fungus that is causing the infection
Complete blood count (CBC), C-reactive protein (CRP), or erythrocyte sedimentation
rate (ESR)
A routine echocardiogram or a transesophageal echocardiogram provides a closer
look at the heart valves
Treatment
You may need to be hospitalized at first to receive antibiotics through a vein (IV or
intravenously). Blood cultures and tests will help your health care provider choose the best
antibiotic.
You will then need long-term antibiotic therapy.
Patients usually need therapy for 4-6 weeks to fully remove all the bacteria from the
heart chambers and valves.
Antibiotic treatments that are started in the hospital will need to be continued at home.
Surgery to replace the heart valve is usually needed when:
The infection is breaking off in little pieces, resulting in strokes
The person develops heart failure as a result of damaged heart valves
There is evidence of more severe organ damage
Outlook (Prognosis)
Getting treatment for endocarditis right away improves the chances of a good outcome.
More serious problems that may develop include:
Brain abscess
Further damage to the heart valves, causing heart failure
Spread of the infection to other parts of the body
Stroke, caused by small clots or pieces of the infection breaking off and traveling to
the brain.
When to Contact a Medical Professional
Call your health care provider if you notice the following symptoms during or after treatment:
Blood in urine
Chest pain
Fatigue
Fever
Numbness
Weakness
Weight loss without change in diet
Prevention
The American Heart Association recommends preventive antibiotics for people at risk for
infectious endocarditis, such as those with:
Certain birth defects of the heart
Heart transplant and valve problems
Man-made (prosthetic) heart valves
Past history of endocarditis
These patients should receive antibiotics when they have:
Dental procedures that are likely to cause bleeding
Procedures involving the breathing tract
Procedures involving the urinary tract system
Procedures involving the digestive tract
Procedures on skin infections and soft tissue infections
Alternative Names
Valve infection; Staphylococcus aureus - endocarditis; Enterococcus - endocarditis;
Streptococcus viridans - endocarditis; Candida - endocarditis
Myocarditis
Email this page to a friend Share on facebook Share on twitter Bookmark & Share Printer-
friendly version
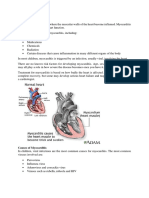
Myocarditis is inflammation of the heart muscle.
See also: Pediatric myocarditis
Causes
Myocarditis is an uncommon disorder that is usually caused by viral, bacterial, or fungal
infections that reach the heart.
Viral infections:
Coxsackie
Cytomegalovirus
Hepatitis C
Herpes
HIV
Parvovirus
Bacterial infections:
Chlamydia
Mycoplasma
Streptococcus
Treponema
Fungal infections:
Aspergillus
Candida
Coccidioides
Cryptococcus
Histoplasma
When you have an infection, your immune system produces special cells that release
chemicals to fight off disease. If the infection affects your heart, the disease-fighting cells
enter the heart. However, the chemicals produced by an immune response can damage the
heart muscle. As a result, the heart can become thick, swollen, and weak. This leads to
symptoms of heart failure.
Other causes of myocarditis may include:
Allergic reactions to certain medications or toxins (alcohol, cocaine, certain
chemotherapy drugs, heavy metals, and catecholamines)
Being around certain chemicals
Certain diseases that cause inflammation throughout the body (rheumatoid arthritis,
sarcoidosis)
Symptoms
There may be no symptoms. Symptoms may be similar to the flu. If symptoms occur, they
may include:
Abnormal heartbeat
Chest pain that may resemble a heart attack
Fatigue
Fever and other signs of infection including headache, muscle aches, sore throat,
diarrhea, or rashes
Joint pain or swelling
Leg swelling
Shortness of breath
Other symptoms that may occur with this disease:
Fainting, often related to irregular heart rhythms
Low urine output
Exams and Tests
A physical examination may show no abnormalities, or may reveal the following:
Abnormal heartbeat or heart sounds (murmurs, extra heart sounds)
Fever
Fluid in the lungs
Rapid heartbeat (tachycardia)
Swelling (edema) in the legs
Tests used to diagnosis myocarditis include:
Blood cultures for infection
Blood tests for antibodies against the heart muscle and the body itself
Chest x-ray
Electrocardiogram (ECG)
Heart muscle biopsy (endomyocardial biopsy)
Red blood cell count
Ultrasound of the heart (echocardiogram)
White blood cell count
Treatment
Treatment is aimed at the cause of the problem, and may involve:
Antibiotics
Anti-inflammatory medicines to reduce swelling
Diuretics to remove excess water from the body
Low-salt diet
Reduced activity
If the heart muscle is very weak, your health care provider will prescribe medicines to treat
heart failure. Abnormal heart rhythms may require the use of additional medications, a
pacemaker, or an implantable cardioverter-defibrillator. If a blood clot is in the heart
chamber, you will also receive blood thinning medicine.
Outlook (Prognosis)
How well you do depends on the cause of the problem and your overall health. The outlook
varies. Some people may recover completely. Others may have permanent heart failure.
Possible Complications
Cardiomyopathy
Heart failure
Pericarditis
When to Contact a Medical Professional
Call your health care provider if you have symptoms of myocarditis, especially after a recent
infection.
Seek immediate medical help if you have severe symptoms or have been diagnosed with
myocarditis and have increased:
Chest pain
Difficulty breathing
Swelling
Prevention
Promptly treating conditions that cause myocarditis may reduce the risk.
Alternative Names
Inflammation - heart muscle
Das könnte Ihnen auch gefallen
- Rheumatic FeverDokument3 SeitenRheumatic FeverKennette LimNoch keine Bewertungen
- Infective Endocarditis GuideDokument7 SeitenInfective Endocarditis GuideAkarsh RamNoch keine Bewertungen
- Causes of MyocarditisDokument3 SeitenCauses of MyocarditisTeresa CardinozaNoch keine Bewertungen
- Risk Factors Include Having: Congenital Heart DefectsDokument3 SeitenRisk Factors Include Having: Congenital Heart Defectspragna novaNoch keine Bewertungen
- Rheumatic Heart DiseaseDokument8 SeitenRheumatic Heart DiseaseJehannaMarEnggingAbdurahmanNoch keine Bewertungen
- Content Heart DiseaseDokument12 SeitenContent Heart Diseaseshifa23Noch keine Bewertungen
- Infectious EndocarditisDokument4 SeitenInfectious EndocarditisKhalid Mahmud Arifin100% (1)
- Rheumatic Heart DiseaseDokument10 SeitenRheumatic Heart DiseaseSuhas IngaleNoch keine Bewertungen
- What Is SepticemiaDokument3 SeitenWhat Is SepticemiaYhna Nesperos GelverioNoch keine Bewertungen
- Cardiovascular System ExplainedDokument18 SeitenCardiovascular System ExplainedJkiathlene JauganNoch keine Bewertungen
- Rheumatic Heart Disease Causes, Symptoms, and TreatmentDokument4 SeitenRheumatic Heart Disease Causes, Symptoms, and TreatmentJhen Jhen100% (1)
- Seminar On Rheumatic Fever UmeshDokument4 SeitenSeminar On Rheumatic Fever UmeshawasthiphothocopyNoch keine Bewertungen
- Endocarditis - Symptoms and Causes - Mayo ClinicDokument1 SeiteEndocarditis - Symptoms and Causes - Mayo ClinicBriandon CanlasNoch keine Bewertungen
- Xavier University Nursing Case Analysis on Infective EndocarditisDokument6 SeitenXavier University Nursing Case Analysis on Infective EndocarditisDudil GoatNoch keine Bewertungen
- Rheumatic FeverDokument3 SeitenRheumatic FeverPanji SaksonoNoch keine Bewertungen
- Report Pathopysiology (Endocarditis) 12Dokument7 SeitenReport Pathopysiology (Endocarditis) 12Ade Yulina Mursyidah Sa'adNoch keine Bewertungen
- A Very Lengthy AssignmentDokument7 SeitenA Very Lengthy AssignmentElmoi DoguilesNoch keine Bewertungen
- Rheumatic Fever Is AnDokument7 SeitenRheumatic Fever Is AnHamza SaeedNoch keine Bewertungen
- Critical Care in Cardiovascuiar DiseasesDokument42 SeitenCritical Care in Cardiovascuiar DiseasesSurbhi GujrathiNoch keine Bewertungen
- Dengue Hemorrhagic FeverDokument2 SeitenDengue Hemorrhagic FeverChristian TelmoNoch keine Bewertungen
- What Is Infective Endocarditis?Dokument5 SeitenWhat Is Infective Endocarditis?prasenjit_gayenNoch keine Bewertungen
- 2 - RH Fev, Inf EndoDokument37 Seiten2 - RH Fev, Inf EndoLobna ElkilanyNoch keine Bewertungen
- Micro - CVS InfectionsDokument55 SeitenMicro - CVS InfectionsMahmoud hilmyNoch keine Bewertungen
- Rheumatic Heart DiseaseDokument13 SeitenRheumatic Heart Diseasedy15Noch keine Bewertungen
- 8. Infections of the Cardiovascular System 2024Dokument46 Seiten8. Infections of the Cardiovascular System 2024aguilarjanicaNoch keine Bewertungen
- Cardiac Infections: (Outside To Inside)Dokument7 SeitenCardiac Infections: (Outside To Inside)Ashley MalsonNoch keine Bewertungen
- Endocarditis, Pericarditic, Myocarditis: TopicDokument104 SeitenEndocarditis, Pericarditic, Myocarditis: TopicOM VERMANoch keine Bewertungen
- MeningococcemiaDokument3 SeitenMeningococcemiaJoelius BoncodinNoch keine Bewertungen
- Rheumatic HeartDokument5 SeitenRheumatic HeartMariahnaSadjaluddinNoch keine Bewertungen
- By Mayo Clinic StaffDokument7 SeitenBy Mayo Clinic StaffKeith PerryNoch keine Bewertungen
- Causes and Treatment of Myocarditis in ChildrenDokument9 SeitenCauses and Treatment of Myocarditis in ChildrenMILENA SIERRANoch keine Bewertungen
- Rheumatic Heart DiseaseDokument14 SeitenRheumatic Heart Diseaseudaybujji100% (1)
- Infective EndocarditisDokument66 SeitenInfective Endocarditissanjivdas100% (4)
- Week 1Dokument7 SeitenWeek 1Balkess NajemNoch keine Bewertungen
- Care of patients with pericarditis, endocarditis, myocarditisDokument29 SeitenCare of patients with pericarditis, endocarditis, myocarditisDanial HassanNoch keine Bewertungen
- Seminar On Rhuematic Heart DiseaseDokument16 SeitenSeminar On Rhuematic Heart Diseasenaga maniNoch keine Bewertungen
- Adults Community Acquired PneumoniaDokument7 SeitenAdults Community Acquired PneumoniaDEth JU NafenNoch keine Bewertungen
- Infeksi Jantung: DR Elfiani, SP - PDDokument19 SeitenInfeksi Jantung: DR Elfiani, SP - PDjoniNoch keine Bewertungen
- Acquired Cardiac Disorders ExplainedDokument40 SeitenAcquired Cardiac Disorders ExplainedRajaNoch keine Bewertungen
- Case, HesedhDokument5 SeitenCase, HesedhHesedh TorresNoch keine Bewertungen
- Systemic Diseases: Learning ObjectivesDokument29 SeitenSystemic Diseases: Learning ObjectivesYuusuf MubarikNoch keine Bewertungen
- Rheumatic Heart DiseaseDokument23 SeitenRheumatic Heart DiseaseRashid Khaliff Enok Dignadice100% (3)
- Rheumatic Fever Symptoms, Causes & TreatmentDokument15 SeitenRheumatic Fever Symptoms, Causes & TreatmentEnas NeyazNoch keine Bewertungen
- Rheumatic Heart Disease: BackgroundDokument1 SeiteRheumatic Heart Disease: Backgroundadi govindNoch keine Bewertungen
- What Is Septic ShockDokument6 SeitenWhat Is Septic Shocksalome carpioNoch keine Bewertungen
- Infective EndocarditisDokument3 SeitenInfective Endocarditisdfgdfgdf123Noch keine Bewertungen
- Sem 11 Cardiovascular System & Dental ConsiderationsDokument143 SeitenSem 11 Cardiovascular System & Dental ConsiderationsJyoti Pol SherkhaneNoch keine Bewertungen
- Cardio InfectionDokument6 SeitenCardio InfectionCindy Mae de la TorreNoch keine Bewertungen
- Sam Mari DayananDokument3 SeitenSam Mari DayananRhea Mae Pindoy PagutaNoch keine Bewertungen
- Rheumtatic Fever 2018Dokument63 SeitenRheumtatic Fever 2018shapan biswaNoch keine Bewertungen
- Rheumatic Heart Disease and Fever ExplainedDokument2 SeitenRheumatic Heart Disease and Fever ExplainedDiaz RahmadiNoch keine Bewertungen
- Congenital Heart DiseaseDokument5 SeitenCongenital Heart DiseaseZAY EMNoch keine Bewertungen
- Rheumatic FeverDokument56 SeitenRheumatic Feveralmawang100% (1)
- Biochem QuizDokument2 SeitenBiochem QuizAiramel Shekina AlborNoch keine Bewertungen
- DengueDokument4 SeitenDengueAllysa Kyle AlfonsoNoch keine Bewertungen
- Англ - 2 курс, модульDokument19 SeitenАнгл - 2 курс, модульVoyage DanceNoch keine Bewertungen
- PericarditisDokument3 SeitenPericarditisKhalid Mahmud Arifin0% (1)
- PericarditisDokument52 SeitenPericarditissanjivdasNoch keine Bewertungen
- Inflamed Blood Vessels (Vasculitis), A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandInflamed Blood Vessels (Vasculitis), A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Vasculitis, A Simple Guide to the Condition, Treatment and Related DiseasesVon EverandVasculitis, A Simple Guide to the Condition, Treatment and Related DiseasesNoch keine Bewertungen
- Acs - Case StudyDokument2 SeitenAcs - Case StudyAubrie StellarNoch keine Bewertungen
- Cardiology census and patient detailsDokument9 SeitenCardiology census and patient detailsReda SoNoch keine Bewertungen
- EKG - Premature Ventricular Contractions (PVCS)Dokument8 SeitenEKG - Premature Ventricular Contractions (PVCS)SAM dabombdigNoch keine Bewertungen
- Mouse DissectionDokument6 SeitenMouse DissectionMauricio F. VillamarNoch keine Bewertungen
- A Case Study OnDokument176 SeitenA Case Study OnTasneem MamokanNoch keine Bewertungen
- PAW Print PAW Print PAW Print PAW Print: Principal's Column Principal's Column Principal's Column Principal's ColumnDokument6 SeitenPAW Print PAW Print PAW Print PAW Print: Principal's Column Principal's Column Principal's Column Principal's Columntica1118Noch keine Bewertungen
- Pathophysiology: Cardiovascular Diseases Coronary Artery Disease (CAD)Dokument5 SeitenPathophysiology: Cardiovascular Diseases Coronary Artery Disease (CAD)Grace Bernadine H. Ramos100% (1)
- Sony Hilal Wicaksono, MD Universitas Indonesia HospitalDokument14 SeitenSony Hilal Wicaksono, MD Universitas Indonesia HospitalSonyHilalWicaksonoNoch keine Bewertungen
- ACLS Megacode Testing ScenariosDokument12 SeitenACLS Megacode Testing Scenariosealm10100% (2)
- Crochet Anatomical Human Heart: by Kyla RaaymakersDokument7 SeitenCrochet Anatomical Human Heart: by Kyla RaaymakersJavier BejaranoNoch keine Bewertungen
- Listening 65Dokument8 SeitenListening 65Sunrise 2587Noch keine Bewertungen
- Edexcel International GCSE Biology Hard PPQDokument14 SeitenEdexcel International GCSE Biology Hard PPQTravel Unlimited100% (1)
- Cat Dissection ProjectDokument12 SeitenCat Dissection Projectapi-309363754Noch keine Bewertungen
- Igcse Biology Revision Finale!!Dokument143 SeitenIgcse Biology Revision Finale!!sohaila ibrahim100% (1)
- Nursing Responsibilities for MedicationsDokument5 SeitenNursing Responsibilities for Medicationsしゃいな ふかみNoch keine Bewertungen
- Facts About Coronary Heart DiseaseDokument3 SeitenFacts About Coronary Heart DiseaseHannalene DolorNoch keine Bewertungen
- Dr. RECKEWEGDokument73 SeitenDr. RECKEWEGtaichi767% (3)
- Thyroid StormDokument16 SeitenThyroid StormRaquid MariaNoch keine Bewertungen
- Form 3 Science Chapter 2Dokument9 SeitenForm 3 Science Chapter 2Mohamad Harith100% (5)
- Modern Management of Systolic Anterior Motion of The Mitral ValveDokument11 SeitenModern Management of Systolic Anterior Motion of The Mitral ValveRodri EspinNoch keine Bewertungen
- Mass Deliverance Manual (Revisi - Win WorleyDokument159 SeitenMass Deliverance Manual (Revisi - Win WorleyETHAN COLLEGE OF BIBLICAL STUDIESNoch keine Bewertungen
- Although Shock Has Been Recognised For Over 100 YearsDokument4 SeitenAlthough Shock Has Been Recognised For Over 100 YearsRusty HoganNoch keine Bewertungen
- AclsDokument13 SeitenAclsMohamed Kelany100% (1)
- Medical Abbreviation TermsDokument7 SeitenMedical Abbreviation TermsJmarie Brillantes PopiocoNoch keine Bewertungen
- The Physiology of Cardiopulmonary Resuscitation (CPR) - ECG & ECHODokument9 SeitenThe Physiology of Cardiopulmonary Resuscitation (CPR) - ECG & ECHOUrgencias La RazaNoch keine Bewertungen
- Iacta 2011 Janak Mehta Award Winning PresentationDokument56 SeitenIacta 2011 Janak Mehta Award Winning PresentationDr.Sandeep Kumar KarNoch keine Bewertungen
- Science 9Dokument3 SeitenScience 9Hezl Valerie ArzadonNoch keine Bewertungen
- LAHORE MEDICAL COLLEGE CHEMOTHERAPY EXAMDokument36 SeitenLAHORE MEDICAL COLLEGE CHEMOTHERAPY EXAMClinicalTraining0% (1)
- ATPL Human PerformanceDokument583 SeitenATPL Human PerformanceAmilton Morillas100% (1)
- ACLS Simulation ScenariosDokument14 SeitenACLS Simulation ScenariosVanessa HermioneNoch keine Bewertungen