Beruflich Dokumente
Kultur Dokumente
Evaluation of The Antiadhesion Potential of UV Cross-Linked Gelatin Films in A Rat Abdominal Model
Hochgeladen von
Loc Huynh0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
31 Ansichten8 Seitencontrolled-released formulation on pharmaceutics
Originaltitel
79e4150c06b9ba7c67
Copyright
© © All Rights Reserved
Verfügbare Formate
PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldencontrolled-released formulation on pharmaceutics
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
31 Ansichten8 SeitenEvaluation of The Antiadhesion Potential of UV Cross-Linked Gelatin Films in A Rat Abdominal Model
Hochgeladen von
Loc Huynhcontrolled-released formulation on pharmaceutics
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 8
Biomaterials 23 (2002) 29012908
Evaluation of the antiadhesion potential of UV cross-linked gelatin
lms in a rat abdominal model
Shojiro Matsuda
a,b
, Naomi Se
a,c
, Hiroo Iwata
a,
*, Yoshito Ikada
d
a
Institute for Frontier Medical Sciences, Kyoto University, Kawahara-cho 53, Shogoin, Sakyo-ku, Kyoto 606-8507, Japan
b
Research and Development Department, GUNZE Ltd., Natsumegaichi 46, Aono-cho, Ayabe, Kyoto 623-8513, Japan
c
JMS Company, Limited, Kako-machi 12-17, Naka-ku, Hiroshima 730-8652, Japan
d
Faculty of Medical Engineering, Suzuka University of Medical Science, Kataoka-cho 1001, Suzuka, Mie 510-0293, Japan
Received 27 November 2000; accepted 20 November 2001
Abstract
Among ve kinds of rat adhesion models tested, the following model was selected. The epigastric vein 2.5 cm from the midline of
the abdomen was cut by sharp scissors, and the lateral side of the cut epigastric vein was ligated using a 30 silk suture. This model
could be easily prepared and gave a rate of adhesion formation of 90%, which was useful for screening antiadhesive materials. For
the kinetic study of tissue adhesion in this model, an injured site was covered with a non-degradable poly(vinyl alcohol) (PVA) lm.
The incidence rate of adhesion was 18%, when the PVA lm covered the injured site for 2 days. This suggests that an antiadhesive
barrier should cover the injured site for at least 2 days. The antiadhesion efcacy of cross-linked gelatin lms were evaluated using
this adhesion model. The UV cross-linked gelatin lm which was designed to exist for 2 days but to disappear at day 3 in the rat
abdominal cavity showed the highest antiadhesion efcacy. r 2002 Elsevier Science Ltd. All rights reserved.
Keywords: Peritoneal adhesion; Rat; Antiadhesion; Gelatin lm
1. Introduction
Enormous efforts have been devoted to prevention of
tissue adhesion by improving surgical procedures and
using antiadhesion materials. However, tissue adhesion
continues to be a cause of post-surgical complications.
Placing a physical barrier between an injured site and
the adjacent tissues is a direct approach to prevent
adhesion. Various kinds of materials made of animal
tissues, biological materials and synthetic polymers have
been reported to be effective in reducing adhesion both
in animal models and in clinical practices [1]. Some have
been commercially and clinically used [25]. Non-
absorbable synthetic materials such as silicone and
polytetrauoroethylene sheets have been employed as
antiadhesive materials [6,7]. Although they can effec-
tively isolate an injured site from adjacent tissues and
prevent adhesion, because of their non-degradability
they may cause foreign body reactions, inducing strong
connective tissue formation which again evokes tissue
adhesion. Coating the injured surface with viscous
polymer solutions such as polyvinylpyrolidone, carboxy-
methylcellulose [8], dextran [9] and hyaluronic acid [10]
also have been reported to be effective. However, the
stay at the applied site depends on circumstances,
sometimes the polymer solutions may be readily washed
out before the injured surface becomes no longer
susceptible to adhesion formation. Sepralm
s
is a
hydrophilic lm composed of sodium hyaluronate and
carboxymethylcellulose. It is claimed that this lm
adheres to a wound surface and mechanically separates
the tissue during the post-operative healing phase. But,
some surgeons claimed difculty in handling because of
its brittleness and low mechanical properties. Interceed
s
is a knitted fabric composed of oxidized regenerated
cellulose and is reported to signicantly reduce adhesion
when blood contamination is avoided during applica-
tion [3,11]. As blood evacuation cannot always be done
effectively in a clinical situation, surgeons are not always
satised with Interceed
s
in the prevention of adhesion.
An antiadhesive material should be designed to stay
at the injured site during the post-operative wound
*Corresponding author. Tel.: +81-75-751-4119; fax: +81-75-751-
4144.
E-mail address: iwata@frontier.kyoto-u.ac.jp (H. Iwata).
0142-9612/02/$ - see front matter r 2002 Elsevier Science Ltd. All rights reserved.
PII: S 0 1 4 2 - 9 6 1 2 ( 0 1 ) 0 0 4 1 8 - 5
healing phase. The aims of the present study were (1) to
establish an animal model that can form adhesion with
high reproducibility, (2) to determine the critical time
when the injured surface no longer becomes susceptible
to adhesion formation in the model, (3) to design an
antiadhesive lm from gelatin on the basis of these
ndings, and (4) to examine its efcacy using the model.
2. Materials and methods
2.1. Materials
Six-week-old Wistar rats were purchased from Shi-
mizu Laboratory Animal Supply Co., Ltd. (Kyoto,
Japan). All animal procedures were in accordance with
institutional guidelines of Kyoto University on animal
experimentation. Gelatin, extracted using the alkaline
method from bovine bone (type I collagen), was donated
by Nitta Gelatin Co. Ltd. (Osaka, Japan). Antiadhesive
efcacy was determined for lms prepared from this. A
poly(vinyl alcohol) (PVA) hydrogel lm of 70 wt%
water content was prepared by low temperature crystal-
lization in a water/dimethyl sulfoxide mixed solvent [12]
and used for the kinetic study of tissue adhesion
formation.
To prepare gelatin lms, gelatin powder was dissolved
in distilled water to a concentration of 10 wt%. The
solution was cast on glass plates and allowed to dry in
air to obtain lms of 0.1 mm thickness. Cross-linking
was introduced by exposing both the sides of lms to
ultraviolet (UV) light in air 60 cm from an UV lamp
(Toshiba GL-15 (15 W)) for different time periods. The
lms were sterilized by ethyleneoxide gas for the animal
experiment.
2.2. Rat adhesion model
To set up an animal model to evaluate the efcacy of
antiadhesion materials, the adhesion incidence of ve
adhesion models were evaluated. In total, 52 rats were
used in this study. Rats were anesthetized by inhalation
of diethyl ether and their ventral hair was scraped using
a razor. Using the aseptic technique, a 3 cm incision was
made on the midline of the abdominal wall, and both
abdominal walls were reected and similar adhesion
models were made on each of the abdominal walls. One
site was excluded because of technical failure in
preparation of the adhesion model. A total of 103 sites
were used in this study. Five kinds of adhesion models
were prepared by varying the following factors, the
presence or absence of a 30 silk suture knot, location of
the injury (2.5 or 1.5 cm from the midline incision),
injury spot (on the epigastric vein or abdominal wall)
and cutting tissue by sharp scissors. The combinations
of these factors in the models are given in Table 1. After
preparing the models, the middle line incision was closed
using 30 silk suture. The animals were maintained
under free access to food and water. Seven days after
surgery, the incision was reopen to examine the injured
site for the incidence of adhesion by the naked eye.
Some of the model animals (e) were sacriced at 12 h, 1,
3 and 7 days after surgery to observe the adhesion
formation process at the injured site. The abdominal
wall of the injured site was removed and xed in 10 wt%
formalin solution. The tissues were processed by the
standard procedure for histological examinations and
their thin sections were examined after staining with
hematoxylineosin (HE).
2.3. Kinetic study on adhesion prevention
PVA lms with 2 3 cm
2
and 2 mm thickness were
sterilized with 70 vol% ethanol for 2 h and then swollen
in sterilized phosphate buffered saline at 251C for 1 h.
The adhesion models (e) were made on both sides of the
abdominal walls. A PVA hydrogel lm was applied and
xed with 50 nylon suture at four corners to cover the
injured site. In the preliminary experiments, the
existence of the nylon suture induced tissue reactions
Table 1
Incidence rates of adhesion formation 7 days after surgery in various rat abdominal adhesion models
Adhesion model Incidence of adhesion 7 days after surgery
Suture knot Injury location
from the midline (cm)
Injury spot Cutting No. of model sites Incidence rate (%)
Adhesion (+) Adhesion ()
(a) Removed 2.5 Vein Yes 4 16 20
b
(b) Present 1.5 Vein Yes 8 12 40
b
(c) Present 2.5 Wall Yes 13 7 65 NS
(d)
a
Present 2.5 Vein No 19 4 83 NS
(e) Present 2.5 Vein Yes 18 2 90
a
One site was excluded because of technical failure during preparation of the adhesion model.
b
Signicantly different from model (e) at the 0.1% level.
NS; not signicantly different from model (e) at the 5% level.
S. Matsuda et al. / Biomaterials 23 (2002) 29012908 2902
which spread over the injured model site. Therefore, to
reduce the effect of the nylon suture at the injured site,
relatively larger lms were applied in this kinetic study
than the lms used in the antiadhesion efcacy study. At
1, 2 and 3 days after closure, the abdomen was
reopened, and both the PVA lm and nylon sutures
were carefully removed not to disturb the injured model
surface, and the abdomen was closed again. One site at 2
days and all sites at 3 days were excluded, because the
adhesion formation had already occurred to the nylon
suture and PVA lm at the reopening. In total, 21 model
sites were evaluated. Seven days after the rst surgery,
all rats were sacriced for the assessment of adhesion by
the naked eye.
Some animals were sacriced at 12, 24, 36 and 48 h
after the lm application to observe the wound healing
process at the injured site histologically. The tissues were
processed by the standard procedure for histological
examinations and their thin sections were examined
after staining with hematoxylineosin (HE).
2.4. In vivo degradation of UV cross-linked gelatin lms
Cross-linked gelatin lms by UV irradiation for 5, 10,
20 and 40 h were used in the biodegradation study. In
total, 11 rats were used in this study. Each rat received
implantation of three pieces of lms with 1 1.5 cm
2
of
known dry weight intraperitoneally. At predetermined
times after implantation, the lms were explanted with
the surrounding tissue. This tissue was carefully
removed not to damage the lm. The lms were
completely dried under vacuum conditions and the dry
weights of the lms were measured. The extent of in vivo
degradation was expressed as the mean7SD of the
percentage of the remaining dry weight.
2.5. Antiadhesive efcacy evaluation
Forty-one rats were used in this study. Adhesion
models (e) were made on both sides of the abdominal
walls. Three sites were not used because of technical
failure in preparation of the adhesion model. In total, 79
model sites were used to evaluate the antiadhesive
efcacy of cross-linked gelatin. The animals were
divided into ve experimental groups. Group-1 (G-1)
consisted of animals that underwent the experimental
adhesion protocol of the model (e) without application
of an experimental antiadhesive sample. These animals
constituted the untreated control group. Group-2 (G-2)
was treated with the protocol with application of a non-
cross-linked gelatin lm as described later. Group-3 (G-
3), Group-4 (G-4) and Group-5 (G-5) were treated with
the same protocol, with application of UV 10, 20 and
40 h irradiated gelatin lm, respectively.
In G-2 to G-5, an antiadhesive sample of 1 1.5 cm
2
was placed on the injured site of the model (e) without
xation by suturing. The animals were maintained under
free access to food and water. Animals from the ve
groups were randomly operated by one surgeon. Two or
three animals from each group were operated per day.
The assessment of adhesion was examined 7 days after
the operation by the naked eye. When tissue adhesion
was observed at the model site, it was judged as the
occurrence of tissue adhesion regardless of adhesion
severity.
For the histological study, some rats were sacriced 1
day and 7 days after antiadhesive barrier application
and the model sites were removed and xed in 10 wt%
formalin solution. The tissue were processed by the
standard procedure for histological examinations
and their thin sections were examined after staining
with HE.
2.6. Statistical analysis
The chi-squared test, Yates correction and Fishers
exact test were employed to determine the signicant
differences of frequency between two groups. The
signicance which existed at Po0:05; Po0:01 and
Po0:001 was expressed by *, ** and ***, respectively.
3. Results
3.1. Adhesion model
Five kinds of adhesion models were prepared as given
in Table 1. The macroscopic appearances at the injured
site are shown in Fig. 1 for model (e) just after
preparation and 7 days after surgery. The greater
omentum adhered to the suture knot left on the
abdominal wall and spread over the surrounding tissue.
In most adhesions in all models, the greater omentum
was the principal tissue responsible for adhesion,
although the mesentery was also engaged in some
adhesions.
The incidence rates of adhesion are listed in Table 1
for each model. Adhesion depended on the location of
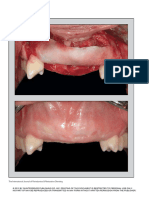
Fig. 1. Abdominal wall adhesion model (e) (see also Table 1). (A)
Immediately after surgery, arrow: silk suture knot, (B) 7 days after
surgery.
S. Matsuda et al. / Biomaterials 23 (2002) 29012908 2903
the surgical trauma and the existence of a suture knot.
A suture knot left on the site at 2.5 cm from the midline
of the abdomen caused adhesion at a rate >80% in
models (d) and (e). However, the incidence rate in model
(b), in which a suture knot was left on the site at 1.5 cm
from the midline, was signicantly lower than that of
model (e). This may be due to the movement of the
bowel facing the suture knot and the surgical trauma.
Although the location of the model site was an
important factor, the existence of a suture knot more
markedly affected the incidence of adhesion. Model (a),
in which the surgical trauma was made 2.5 cm from the
midline, but the suture knot was removed, demonstrated
the lowest incidence rate. The incidence rate of model (a)
was also signicantly lower than that of model (e). This
suggests that the existence of a suture knot was the main
factor in the incidence of adhesion. In model (e), the
epigastric vein was cut by sharp scissors and its distal
end was ligated using a 30 silk suture. A small amount
of blood exuded from the proximal end of the vein.
When the injury point was not on the epigastric point
(model (c)), or cutting by scissors was not done (model
(d)), the incidence rate was lower than that of model (e).
Since model (e) presented the highest adhesion inci-
dence, and might represent more realistic surgical events
than model (d), model (e) was employed in the following
experiments. However, no signicant difference was
found in the adhesion incidence rate between models (e)
vs. (c) and (e) vs. (d).
The tissues of model (e) were explanted at predeter-
mined time intervals. The photomicrographs of their
thin sections stained by HE are shown in Fig. 2. At 12 h
after surgery, the suture knot was partially covered with
an amorphous material. At day 1, the greater omentum
had already adhered to the suture knot, but the adhesion
was not strong, so that it could be released by weak
mechanical disturbance. At day 3, the population of
neutrophils decreased, but more monocytes and bro-
blasts inltrated into the area surrounding the suture,
and rm granulation tissue with neovascularization was
formed between the greater omentum and the abdom-
inal wall. At day 7, the granulation tissue became larger
and rmly covered the abdominal wall surrounding the
suture knot.
3.2. Kinetic study on adhesion prevention
The injured site of model (e) was covered with a PVA
lm xed by 50 nylon monolament suturing and then
the lm and the suture were removed at 1, 2 and 3 days
after the operation. The incident rates of adhesion
formation at day 7 after rst surgery are shown in Fig. 3.
The incidence rate of adhesion of the 1 day and 2 days
PVA covered model was signicantly lower than that of
the non-covered model. The incidence rate of the 2 days
PVA covered model was lower than that of 1 day, but
there was no signicant difference. Coverage of the
injured site with a hydrogel sheet for 3 days was
expected to drastically decrease the incidence of adhe-
sion, but this was not the case. At 3 days after coverage
by PVA lm, it was found that the greater omentum was
markedly adhered to the nylon suture, the surrounding
PVA lm and abdominal wall tissue. Removal of these
materials from the model site might be traumatic.
A kinetic study was not carried out beyond 3 days.
This suggests that the foreign materials might become
nuclei for new adhesion.
Fig. 2. Histological observation of the wound site of adhesion model
(e). Thin sections were stained with HE.
Fig. 3. Kinetic study of adhesion formation. A PVA lm was placed
on the wound part for various times after injury. After those periods,
the lm was removed. Seven days after the rst surgery, all rats were
sacriced for the assessment of adhesion by the naked eye. The
incidence rate of adhesion formation in the group without PVA lm
application was cited from that of model (e) in Table 1.
S. Matsuda et al. / Biomaterials 23 (2002) 29012908 2904
Microscopic examinations of the tissue healing
process of the model (e) are shown in Fig. 4. At 12 h
after PVA lm application, the suture knot was partially
covered with an amorphous substance and was almost
free from cell inltration. At 24 h after surgery,
neutrophils inltrated into the substance covering the
suture and the surrounding tissue, and a brin-like
exudate fully covered the suture. The tissue healing
continued under the PVA lm and granulation tissue
completely covered the suture knot 48 h after lm
application. These ndings indicate that antiadhesive
materials should cover the injured site for at least 48 h as
far as in this animal model.
3.3. Dependence of the biodegradation rate of gelatin
lms on UV irradiation time
Gelatin was employed as a material to prepare
antiadhesive lms, because it had been clinically used
as a biomaterial and is known to biodegrade after
implantation. Non-cross-linked gelatin lms were ra-
pidly swollen with water and dissolved into ascites
within several hours in the abdominal cavity. Therefore,
gelatin lms were cross-linked by UV irradiation to
retard their biodegradation. Fig. 5 shows that the
biodegradation of the gelatin lms treated with UV
light for different periods in the rat abdominal cavity.
The biodegradation rate decreased the longer the UV
irradiation time. Cross-linked gelatin lms adsorbed
ascites and became hydrogel after the implantation.
Films deformed but existed as a single piece, and its
volume decreased with increasing implantation periods.
Five hours UV irradiated gelatin lm was not found
after 1 day implantation. Similarly, 10 h UV irradiated
gelatin lm was not found after 3 days implantation. In
conjunction with the ndings of the kinetic studies with
PVA, 10 h irradiation appeared to be promising for
preparing antiadhesive lms.
3.4. Evaluation of the antiadhesion efcacy
The antiadhesion efcacy of gelatin was evaluated
using model (e). The materials were applied onto the
injured site of model (e) and left there without xation
by suturing. The incidence rates of adhesion are
summarized in Table 2 for each material. Among the
four antiadhesive application groups, only G-3 showed
a signicantly lower incidence rate of adhesion than the
control group (G-1). The incidence rates become higher
in the following order G-3, G-2, G-4 and G-5. This
suggests that the optimal UV irradiation time for the
lowest incidence rate of adhesion may exist between 0
and 20 h. G-5 showed a signicantly higher incidence
rate than G-3. Macroscopic views of the model site with
the 10 h UV irradiated gelatin lm just after application
and at day 7 are shown in Fig. 6(A) and (B),
respectively. The model site looked clear and smooth,
suggesting that it had been fully covered with regener-
ated tissue. Photomicrographs of the tissue sections are
shown in Fig. 6(C) and (D) for the gelatin lm irradiated
for 10 h at days 1 and 7 after application, respectively.
The gelatin lm could be clearly identied and the
amorphous tissue layer that was stained deeper than the
gelatin lm could be seen around the suture knot at day
1. Few neutrophils inltrated between the lm and the
abdominal wall. At day 7, the gelatin lm had already
been fully degraded and sparse granulation tissue
including monocytes and broblasts covered the suture.
The macroscopic and microscopic views of the model
site with the 40 h UV irradiated gelatin lm application
at day 7 are shown in Fig. 6(E) and (F), respectively.
Fig. 4. Histological observation of the wound site covered by the PVA
hydrogel lm. Thin sections were stained with HE.
Fig. 5. In vivo degradation of the cross-linked gelatin lms with
different UV irradiation times. Films irradiated for 5 and 10 h could
not be found by naked eye observation after 1 day and 3 days,
respectively. Irradiation time; J: 5 h, n: 10 h, &: 20 h and : 40 h.
Error bar indicates the standard deviation.
S. Matsuda et al. / Biomaterials 23 (2002) 29012908 2905
The lms were completely encapsulated by the granula-
tion tissue and the capsule tissue was covered by the
surrounding greater omentum.
4. Discussion
Various kinds of adhesion models have been devel-
oped using animals, but most have specic problems. As
discussed by Bakkum et al. [13], a reliable animal model
that can be reproduced and scored objectively, and that
possess clinical relevancy concerning the tissue involved
and pathogenesis of the adhesions, is sought. In the
present study, ve kinds of adhesion models were made
on the rat abdominal wall and compared to nd the
most suitable model that can be easily prepared and give
a high incidence rate of adhesion. Model (e) in which the
epigastric vein was cut 2.5 cm from the midline using
sharp scissors and the distal end of the epigastric vein
was ligated with a 30 silk suture gave a 90% incidence
rate of adhesion. This high incidence rate appears to be
because the model site involved a surgical trauma and a
foreign material (a suture knot). The ischemic area and
exuded blood have also been considered to induce
adhesion, but these factors did not exert signicant
effects on the adhesion incidence rates in the present
study. The present model could be easily prepared and
gave a high incidence rate, suggesting that this model is
useful for screening antiadhesive materials.
Fig. 7 shows the tissue reactions against the model site
with or without an antiadhesive material which were
elucidated from the ndings mentioned above. An
antiadhesive barrier should cover the injured site until
the site is no longer susceptible to adhesion and then the
barrier should quickly disappear from the site. Other-
wise, tissue adhesion would take place at the wound site,
accompanying foreign body reactions to the barrier
materials, which can cause another focus of adhesion.
For development of antiadhesive barriers, it is very
important to know the period of time that is required for
the injured tissue to change into a non-adherent surface
during the wound healing process.
By covering an injured site with a silicone lm for
predetermined periods, Rodeheaver et al. [14] deter-
mined the time period necessary for healing the injured
abdominal surface of rats, so that the tissue was no
longer susceptible to adhesion. They showed that a
material that remained on the injured surface for at least
36 h after injury was required for an effective reduction
in adhesion incidence. In the present study, a PVA lm
was employed to cover the model surface instead of the
silicone lm, because it was reported to induce less
granulation than silicone [15]. The PVA hydrogel was
Fig. 6. The macroscopic and microscopic view of the gelatin lm
applied abdominal wall adhesion model. (A) Immediately after
application of 10 h UV irradiated gelatin lm. (B) 1 week after
application of 10 h UV irradiated gelatin lm. (C) 1 day after
application of 10 h UV irradiated gelatin lm. (D) 1 week after
application of 10 h UV irradiated gelatin lm. (E) and (F) 1 week after
application of 40 h UV irradiated gelatin lm.
Table 2
Antiadhesive efcacy of gelatin lms
Group code Materials tested Incidence of adhesion 7 days after surgery
No. of model sites Incidence rate (%)
Adhesion (+) Adhesion ()
G-1
a
Without any agents 15 2
G-2 Gelatin lm without UV irradiation 10 6
G-3
a
Gelatin lm irradiated with UV for 10 h 8 11
G-4
a
Gelatin lm irradiated with UV for 20 h 10 3
G-5 Gelatin lm irradiated with UV for 40 h 13 1
a
One site of each group was excluded because of technical failure during preparation of the adhesion model.
**Signicantly different at the 1% level.
No mark; not signicantly different at the 5% level.
S. Matsuda et al. / Biomaterials 23 (2002) 29012908 2906
also reported to allow low molecular weight substances,
such as oxygen and nutrients, to freely pass through it
[16] and, thus, it is expected not to hinder the wound
healing process. In the present model, the incidence rate
of adhesion was 18%, when the PVA lm remained in
place for 2 days. When the PVA barrier remained in
place for a longer time, the nylon suture used to x the
PVA lm induced foreign body reactions and thus
allowed adhesion to take place at the periphery of the
lm. Both the ndings of Rodeheaver et al. [14] and the
present ones suggest that an antiadhesive barrier should
cover the injured site for at least 2 days to prevent the
adhesion of injured tissues.
In contrast to cross-linked gelatin lms, non-cross-
linked gelatin lm readily absorbs ascites, rapidly
dissolves at body temperature, and hence cannot stay
in place as a lm for more than several hours. As a
result, the antiadhesive effect of the non-cross-linked
gelatin lm was limited, although its incidence rate of
adhesion was lower than that of the controls. It has been
reported that the incidence of post-operative adhesion
can be effectively decreased by simple application of
viscous solutions of polysaccharides, such as carbox-
ymethylcellulose [8], dextran [9] or hyaluronic acid.
These viscous solutions will cover the injured surface for
a certain period of time. A similar benet may be
obtained when a non-cross-linked gelatin lm is applied.
A kinetic study using a PVA lm suggested that a
barrier should stay in place for at least 2 days. Gelatin
lms with various bioabsorption rates were prepared by
controlling the UV cross-link. It was expected at the
beginning of this study, that a lm that remained intact
for a longer time could more effectively prevent
adhesion. However, the gelatin lm prepared by 10 h
UV irradiation and absorbed within 3 days, could most
effectively prevent adhesion among the antiadhesive
barriers examined in the present study. The antiadhesive
efcacy of gelatin lms became less efcient as the UV
irradiation time became longer than 10 h. This is
probably because the prolonged existence of gelatin
lms at the injury site induced foreign body reactions
and resulted in adhesion.
As demonstrated above, the gelatin lm that was
designed to exist for 2 days but to disappear at day 3 in
the rat abdominal cavity showed a signicantly lower
incidence rate of adhesion than the controls. Although
longer periods of covering were expected to reduce the
incidence of adhesion, the lm that was not absorbed
within 3 days did not show better antiadhesion efcacy.
This may be explained in terms of foreign body
reactions induced by the antiadhesive material itself as
schematically shown in Fig. 7. In this antiadhesive
efcacy study, G-3 showed the highest antiadhesive
efcacy. However, the incidence rate of adhesion was
still 42%. For the development of an ideal antiadhesive
that can completely prevent adhesion, a bioabsorbable
material that has an optimal absorbability and that
induces little tissue reactions so as not to induce
adhesion formation by itself is required.
References
[1] Wiseman D. Polymers for the prevention of surgical adhesions.
In: Domb AJ, editor. Polymeric site-specic pharmacotherapy.
Arlington, TX: Wiley, 1994. p. 370421.
[2] Diamond MP, Linsky CB, Cunningham T, Constantine B,
diZerega GS, DeCherney AH. A model for sidewall adhesions
in the rabbit: reduction by an absorbable barrier. Microsurg
1987;8:197200.
[3] Interceed (TC7) Adhesion Barrier Study Group. Prevention of
postsurgical adhesions by Interceed (TC7), an absorbable adhe-
sion barrier: a prospective, randomized multicenter clinical study.
Fertil Steril 1989;51:9338.
[4] Diamond MP. The sepralm adhesion study group. Reduction of
adhesions after uterine myomectomy by Sepralm membrane
(HAL-F): a blinded, prospective, randomized, multicenter clinical
study. Fertil Steril 1996;66:90410.
[5] Becker JM, Dayton MT, Fazio VW, Beck DE, Stryker SJ,
Wexner SD, Wolff BG, Roberts PL, Smith LE, Sweeney SA,
Moore M. Prevention of postoperative abdominal adhesions
by a sodium hyaluronate-based bioresorbable membrane: a
Fig. 7. Schematic drawing of the tissue reactions against the model site with or without an antiadhesive material.
S. Matsuda et al. / Biomaterials 23 (2002) 29012908 2907
prospective, randomized, double-blind multicenter study. J Am
Coll Surg 1996;183:297306.
[6] Stark HH, Boyes JH, Johnson L, Ashworth CR. The use of
paratenon, polyethylene lm, or silastic sheeting to prevent
restricting adhesions to tendons in the hand. J Bone Jt Surg
1977;59:90813.
[7] Haney AF, Hesla J, Hurst BS, Kettel LM, Murphy AA, Rock JA,
Rowe G, Schlaff WD. Expanded polytetrauoroethylene (Gore-
Tex Surgical Membrane) is superior to oxidized regenerated
cellulose (Interceed TC7+) in preventing adhesions. Fertil Steril
1995;63:10216.
[8] Jaacobi Y, Israel AA, Goldberg EP. Prevention of postoperative
abdominal adhesions by tissue precoating with polymer solutions.
J Surg Res 1993;55:4226.
[9] Adhesion study group. Reduction of postoperative pelvic adhe-
sions with intraperitoneal 32% dextran 70: a prospective,
randomized clinical trial. Fertil Steril 1983;40:6129.
[10] Goldberg EP, Burns JW, Jaacobi Y. Prevention of postoperative
adhesions by precoating tissues with dilute sodium hyaluronate
solutions. In: Diamond MP, Reid RL, Di Zerega GS, Linsky CD,
editors. Gynecologic surgery and adhesion prevention. New
York: Wiley, 1993. p. 191204.
[11] Linsky CB, Diamond MP, DeCherney AH, diZerega GS,
Cunningham T. Effect of blood on the efcacy of barrier
adhesion reduction in the rabbit uterine horn model. Infertility
1988;1:27380.
[12] Cha WI, Hyon SH, Ikada Y. Transparent poly(vinyl alcohol)
hydrogel with high water content and high strength. Makromo-
lekulare Chemie 1992;193:191325.
[13] Bakkum EA, van Blitterswijk CA, Dalmeijer RAJ, Trimbos JB. A
semiquantitative rat model for intraperitoneal postoperative
adhesion formation. Gynecol Obstet Invest 1994;37:99105.
[14] Harris ES, Morgan RF, Rodeheaver GT. Analysis of the kinetics
of peritoneal adhesion formation in the rat and evaluation of
potential antiadhesive agents. Surgery 1995;117:6639.
[15] Inoue K, Fujisato T, Gu YJ, Burczak K, Sumi S, Kogire M, Tobe
T, Uchida K, Nakai I, Maetani S, Ikada Y. Experimental hybrid
islet transplantation: application of polyvinyl alcohol membrane
for entrapment of islets. Pancreas 1992;7:5628.
[16] Burczak K, Fujisato T, Hatada M, Ikada Y. Protein permeation
through poly(vinyl alcohol) hydrogel membranes. Biomaterials
1994;15:2318.
S. Matsuda et al. / Biomaterials 23 (2002) 29012908 2908
Das könnte Ihnen auch gefallen
- Scorpio PDFDokument3 SeitenScorpio PDFnimi2364010Noch keine Bewertungen
- Aeration PaperDokument11 SeitenAeration PapersehonoNoch keine Bewertungen
- Lab Assignment-1 1. Create Table Student (Rno, Name, DOB, Gender, Class, College, City, Marks)Dokument7 SeitenLab Assignment-1 1. Create Table Student (Rno, Name, DOB, Gender, Class, College, City, Marks)supreetNoch keine Bewertungen
- Broadway CafeDokument13 SeitenBroadway CafeIoana Taon100% (1)
- 2011 Article 9641Dokument11 Seiten2011 Article 9641hrnisaaNoch keine Bewertungen
- Fabrication, Characterization, and Biocompatibility Study of Gelatin-Blended Fibroin ScaffoldDokument10 SeitenFabrication, Characterization, and Biocompatibility Study of Gelatin-Blended Fibroin ScaffoldTrần Thị QuỳnhNoch keine Bewertungen
- Adhesionet TendinoreDokument7 SeitenAdhesionet TendinoreShkelzen DuciNoch keine Bewertungen
- 2008 in Vitro Cytotoxicity of Maxillofacial Silicone ElastomersDokument5 Seiten2008 in Vitro Cytotoxicity of Maxillofacial Silicone ElastomersNataliaNoch keine Bewertungen
- Suturing Principles in Dentoalveolar Surgery: W. Scott Jenkins, DMD, M. Todd Brandt, DDS, Jeffrey B. Dembo, DDS, MSDokument17 SeitenSuturing Principles in Dentoalveolar Surgery: W. Scott Jenkins, DMD, M. Todd Brandt, DDS, Jeffrey B. Dembo, DDS, MSKajal AhujaNoch keine Bewertungen
- Polymers 2022Dokument10 SeitenPolymers 2022Lab NanobiomaterialesNoch keine Bewertungen
- Wang Et Al-2017-Journal of Biomedical Materials Research Part ADokument29 SeitenWang Et Al-2017-Journal of Biomedical Materials Research Part AAbirame SivasNoch keine Bewertungen
- Clinical Potential of A Silk Sericin-Releasing Bioactive Wound Dressing For The Treatment of Split-Thickness Skin Graft Donor SitesDokument14 SeitenClinical Potential of A Silk Sericin-Releasing Bioactive Wound Dressing For The Treatment of Split-Thickness Skin Graft Donor SitesAgus DniNoch keine Bewertungen
- Regenerationof Periodontaltissues: Guidedtissue RegenerationDokument20 SeitenRegenerationof Periodontaltissues: Guidedtissue RegenerationPiyusha SharmaNoch keine Bewertungen
- Comparative Effectiveness of Cyanoacrylate Bioadhesives and Monofilamentsuture in Wound Healing A Histopathological and Physicoche 2157 7099 1000395Dokument8 SeitenComparative Effectiveness of Cyanoacrylate Bioadhesives and Monofilamentsuture in Wound Healing A Histopathological and Physicoche 2157 7099 1000395Kikilis AčiuvisNoch keine Bewertungen
- 1 s2.0 S0927775715000412 MainDokument8 Seiten1 s2.0 S0927775715000412 MainOana MariaNoch keine Bewertungen
- Is It Possible To Re-Use Mini-Implants For Orthodontic AnchorageDokument5 SeitenIs It Possible To Re-Use Mini-Implants For Orthodontic AnchorageMilton Castillo CaceresNoch keine Bewertungen
- Maxillo 4Dokument5 SeitenMaxillo 4Nirav RathodNoch keine Bewertungen
- Multi-Layer Dressing Made of Laminated Electrospun Nanowebs and Cellulose-Based Adhesive For Comprehensive Wound CareDokument16 SeitenMulti-Layer Dressing Made of Laminated Electrospun Nanowebs and Cellulose-Based Adhesive For Comprehensive Wound CareGading AuroraNoch keine Bewertungen
- Studies On Different Type of Sutures Using Aloe Vera Gel CoatingDokument6 SeitenStudies On Different Type of Sutures Using Aloe Vera Gel CoatingTJPRC PublicationsNoch keine Bewertungen
- Widening Keratinized Tissue Using Modified Free Gingival GraftDokument3 SeitenWidening Keratinized Tissue Using Modified Free Gingival GraftSebastián BernalNoch keine Bewertungen
- A Novel Multiparameter in Vitro ModelDokument9 SeitenA Novel Multiparameter in Vitro ModelthyNoch keine Bewertungen
- The Profile of Crosslinked Bovine Hydroxyapatite Gelatin Chitosan Scaffolds With 0.25% GlutaraldehydeDokument5 SeitenThe Profile of Crosslinked Bovine Hydroxyapatite Gelatin Chitosan Scaffolds With 0.25% GlutaraldehydenisaaNoch keine Bewertungen
- Skin Surface Model Material As A Substrate For Adhesion To Skin TestingDokument17 SeitenSkin Surface Model Material As A Substrate For Adhesion To Skin TestingAnakyn JaegerNoch keine Bewertungen
- Improved Edge Strength in A Facial Prosthesis by Incorporation of Tulle: A Clinical ReportDokument4 SeitenImproved Edge Strength in A Facial Prosthesis by Incorporation of Tulle: A Clinical ReportmadalinaNoch keine Bewertungen
- International Journal of Health Sciences and ResearchDokument6 SeitenInternational Journal of Health Sciences and ResearchDentist HereNoch keine Bewertungen
- Properties of Collagen/Chitosan Scaffolds For Skin Tissue EngineeringDokument10 SeitenProperties of Collagen/Chitosan Scaffolds For Skin Tissue EngineeringerinaapriliaNoch keine Bewertungen
- Surgical Therapy of Peri-ImplantitisDokument17 SeitenSurgical Therapy of Peri-Implantitiskaue francoNoch keine Bewertungen
- Effect of Chitosajournaln JournalDokument7 SeitenEffect of Chitosajournaln JournalSabrina Ceasy AnggraeniNoch keine Bewertungen
- Simion 2012)Dokument13 SeitenSimion 2012)SergioNoch keine Bewertungen
- Clinical Study: A Liquid Membrane As A Barrier Membrane For Guided Bone RegenerationDokument6 SeitenClinical Study: A Liquid Membrane As A Barrier Membrane For Guided Bone RegenerationStanislav ȘuiuNoch keine Bewertungen
- Effect of Freezing and Thawing On The Biomechanical Characteristics of Porcine Ocular TissuesDokument7 SeitenEffect of Freezing and Thawing On The Biomechanical Characteristics of Porcine Ocular TissuesMaher ElabdNoch keine Bewertungen
- Implant For Autologous Soft Tissue Reconstructio - 2018 - Journal of Plastic ReDokument11 SeitenImplant For Autologous Soft Tissue Reconstructio - 2018 - Journal of Plastic RePandhu HarlanNoch keine Bewertungen
- Wound-Healing Effects of Human Dermal Components With Gelatin DressingDokument10 SeitenWound-Healing Effects of Human Dermal Components With Gelatin Dressingsasibhushanarao poolaNoch keine Bewertungen
- البحث السادسDokument10 Seitenالبحث السادسMostafa Shaker El AasserNoch keine Bewertungen
- Long-Term Outcome of Allogeneic Cultivated Limbal Epithelial Transplantation For Symblepharon Caused by Severe Ocular BurnsDokument10 SeitenLong-Term Outcome of Allogeneic Cultivated Limbal Epithelial Transplantation For Symblepharon Caused by Severe Ocular BurnsAngelica SerbulNoch keine Bewertungen
- Jurnal Direct and Indirect Pulp CappingDokument9 SeitenJurnal Direct and Indirect Pulp Cappingninis anisaNoch keine Bewertungen
- Direct and Indirect Pulp Capping: A Brief History, Material Innovations, and Clinical Case ReportDokument9 SeitenDirect and Indirect Pulp Capping: A Brief History, Material Innovations, and Clinical Case ReportNaeimaNoch keine Bewertungen
- Assessment of Ionic and Anionic Surfactants Effect On Demineralized Osteochondral TissueDokument10 SeitenAssessment of Ionic and Anionic Surfactants Effect On Demineralized Osteochondral TissueVitalie CobzacNoch keine Bewertungen
- DentalDokument5 SeitenDentalStuartNoch keine Bewertungen
- Degradation Behaviour of Arrowroot Fibre (Maranta Arundinacea) Reinforced Arrowroot Starch Biocomposite FilmsDokument5 SeitenDegradation Behaviour of Arrowroot Fibre (Maranta Arundinacea) Reinforced Arrowroot Starch Biocomposite Filmsachmad nandangNoch keine Bewertungen
- (ARS Medica Tomitana 2017 ArticolDokument11 Seiten(ARS Medica Tomitana 2017 ArticolIon NegruNoch keine Bewertungen
- Bone Dust and Diced Cartilage Combined With Blood Glue: A Practical Technique For Dorsum EnhancementDokument5 SeitenBone Dust and Diced Cartilage Combined With Blood Glue: A Practical Technique For Dorsum EnhancementVLADIMIR RAMIREZ-BLANCOMDNoch keine Bewertungen
- 2016 Aparece en 2018Dokument9 Seiten2016 Aparece en 2018Fy ChsNoch keine Bewertungen
- Biopolymer Film Fabrication For Skin Mimetic Tissue Regenerative Wound Dressing ApplicationsDokument13 SeitenBiopolymer Film Fabrication For Skin Mimetic Tissue Regenerative Wound Dressing ApplicationsM R JYOTHINoch keine Bewertungen
- Coated Cotton Gauze With Ag/Zno/Chitosan Nanocomposite As A Modern Wound DressingDokument7 SeitenCoated Cotton Gauze With Ag/Zno/Chitosan Nanocomposite As A Modern Wound DressingRishi UpadhyayNoch keine Bewertungen
- Polymers 03 00509 v2Dokument18 SeitenPolymers 03 00509 v2Branko BabicNoch keine Bewertungen
- Setting Time Affects in Vitro Biological Properties of Root Canal SealersDokument4 SeitenSetting Time Affects in Vitro Biological Properties of Root Canal SealersNunoGonçalvesNoch keine Bewertungen
- J of Applied Polymer Sci - 2023 - Zhang - Advances in Wound Dressing Based On Electrospinning NanofibersDokument28 SeitenJ of Applied Polymer Sci - 2023 - Zhang - Advances in Wound Dressing Based On Electrospinning NanofibersSelvabala904260Noch keine Bewertungen
- Electrospun Eri Silk Fibroin Scaffold Coated With Hydroxyapatite For Bone Tissue Engineering ApplicationsDokument11 SeitenElectrospun Eri Silk Fibroin Scaffold Coated With Hydroxyapatite For Bone Tissue Engineering ApplicationsSenthil KumarNoch keine Bewertungen
- Study Relating To Biomedical SubjectsDokument8 SeitenStudy Relating To Biomedical Subjectsyisixo8693Noch keine Bewertungen
- Research ArticleDokument8 SeitenResearch ArticleGabriela SolanoNoch keine Bewertungen
- 88 JMSCRDokument4 Seiten88 JMSCRPradeep PradyNoch keine Bewertungen
- BF - 7 - 2 - 025003-Published PaperDokument10 SeitenBF - 7 - 2 - 025003-Published PaperJasonNoch keine Bewertungen
- A Comparative Study of The Cytotoxicity of Silver-Based Dressings in Monolayer Cell, Tissue Explant, and Animal ModelsDokument11 SeitenA Comparative Study of The Cytotoxicity of Silver-Based Dressings in Monolayer Cell, Tissue Explant, and Animal Modelsfranciscrick69Noch keine Bewertungen
- Ewing Dian Setyadi - Artikel Ilmiah - PpjpiDokument17 SeitenEwing Dian Setyadi - Artikel Ilmiah - PpjpiewingsetyadiNoch keine Bewertungen
- 1st Article - Vikas AggarwalDokument4 Seiten1st Article - Vikas AggarwalSai VyshuNoch keine Bewertungen
- Biological Prosthetics For Hernia Repair: EditorialDokument2 SeitenBiological Prosthetics For Hernia Repair: EditorialtexveerNoch keine Bewertungen
- MIT20 441JF09 Quiz3 SampleDokument4 SeitenMIT20 441JF09 Quiz3 SampleGuilherme HenriqueNoch keine Bewertungen
- Evaluation of The Effectiveness of Collagen Membrane in The Management of Oro Antral FistulaCommunication A Clinical StudyDokument8 SeitenEvaluation of The Effectiveness of Collagen Membrane in The Management of Oro Antral FistulaCommunication A Clinical StudyAthenaeum Scientific PublishersNoch keine Bewertungen
- Chitosan-Calcium Alginate Dressing Promotes Wound Healing - A Preliminary StudyDokument12 SeitenChitosan-Calcium Alginate Dressing Promotes Wound Healing - A Preliminary StudyPhạm Nhựt CườngNoch keine Bewertungen
- Thongchai2020 Article IntegrationOfCollagenIntoChitoDokument7 SeitenThongchai2020 Article IntegrationOfCollagenIntoChitoNelson SouzaNoch keine Bewertungen
- Cricchio 2009Dokument7 SeitenCricchio 2009elver galargaNoch keine Bewertungen
- Tissue Engineering and Wound Healing: A Short Case StudyVon EverandTissue Engineering and Wound Healing: A Short Case StudyBewertung: 5 von 5 Sternen5/5 (2)
- The Science of Superhydrophobicity: Enhancing Outdoor Electrical InsulatorsVon EverandThe Science of Superhydrophobicity: Enhancing Outdoor Electrical InsulatorsNoch keine Bewertungen
- Table of Content and PrefaceDokument5 SeitenTable of Content and PrefaceHaiderEbrahimNoch keine Bewertungen
- Rossmann Repair Training Guide - Google SlidesDokument167 SeitenRossmann Repair Training Guide - Google Slidesmirza baigNoch keine Bewertungen
- Hydraulics - MKM - DLX - Parts - Catalogue MAR 14 PDFDokument33 SeitenHydraulics - MKM - DLX - Parts - Catalogue MAR 14 PDFRS Rajib sarkerNoch keine Bewertungen
- By Beholding We Are ChangedDokument2 SeitenBy Beholding We Are ChangedAdrian EbensNoch keine Bewertungen
- 02-779 Requirements For 90-10 Copper - Nickel - Alloy Part-3 TubingDokument47 Seiten02-779 Requirements For 90-10 Copper - Nickel - Alloy Part-3 TubingHattar MNoch keine Bewertungen
- INERT-SIEX 200-300 IG-100: Design ManualDokument54 SeitenINERT-SIEX 200-300 IG-100: Design ManualSaleh Mohamed0% (1)
- SLC Past and Future Hustrulid KvapilDokument26 SeitenSLC Past and Future Hustrulid KvapilkinsaeyaNoch keine Bewertungen
- Q4 Lesson 3 Hinge Theorem and Its ConverseDokument36 SeitenQ4 Lesson 3 Hinge Theorem and Its ConverseZenn Tee100% (1)
- Bhsa Inggris'Dokument5 SeitenBhsa Inggris'Dwi NovianaNoch keine Bewertungen
- Chemical Bath DepositionDokument6 SeitenChemical Bath DepositionJune AlapaNoch keine Bewertungen
- Teiaiel - Visions of The FutureDokument2 SeitenTeiaiel - Visions of The FutureMarkosNoch keine Bewertungen
- OpenSeesPL 5ICEEDokument6 SeitenOpenSeesPL 5ICEEDaniel Hernandez AtencioNoch keine Bewertungen
- 12 Elements of Firearms TrainingDokument6 Seiten12 Elements of Firearms TraininglildigitNoch keine Bewertungen
- IES318 Series: DIN-Rail or Wall Mounting 8-Port 100M Unmanaged Industrial Ethernet SwitchDokument5 SeitenIES318 Series: DIN-Rail or Wall Mounting 8-Port 100M Unmanaged Industrial Ethernet SwitchSỹ TháiNoch keine Bewertungen
- Grundfosliterature SP A - SP LDokument104 SeitenGrundfosliterature SP A - SP LRizalino BrazilNoch keine Bewertungen
- Op Amp AssignmentDokument10 SeitenOp Amp AssignmentJuan-Wian CoetzerNoch keine Bewertungen
- SURELAM-380,540II (User Manual)Dokument25 SeitenSURELAM-380,540II (User Manual)kamran.sefyaliyevNoch keine Bewertungen
- Features and Highlights - : CapableDokument2 SeitenFeatures and Highlights - : CapableaarianNoch keine Bewertungen
- Derivation of Gravity Loads PDFDokument4 SeitenDerivation of Gravity Loads PDFHenry TuganoNoch keine Bewertungen
- Buongiorno - Etal - 2009 The Big Experimental CheckDokument15 SeitenBuongiorno - Etal - 2009 The Big Experimental CheckMikhail TarabrinNoch keine Bewertungen
- Chapter 1 - Physical Properties of Liquid PDFDokument43 SeitenChapter 1 - Physical Properties of Liquid PDFrohit sharmaNoch keine Bewertungen
- Dark Elves WarbandDokument9 SeitenDark Elves Warbanddueydueck100% (1)
- S01 Hydraulic and Eletric DiagramDokument18 SeitenS01 Hydraulic and Eletric DiagramgadeharogNoch keine Bewertungen
- 2019 MIPS Quality Historic BenchmarksDokument158 Seiten2019 MIPS Quality Historic BenchmarksJoe GellatlyNoch keine Bewertungen
- Modding For Ysflight - Scenery EditorDokument92 SeitenModding For Ysflight - Scenery Editordecaff_42Noch keine Bewertungen