Beruflich Dokumente
Kultur Dokumente
Course Objectives (Complete, L1-7)
Hochgeladen von
mrlucky098550 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
35 Ansichten56 SeitenCourse Objectives (Complete, L1-7)
Copyright
© © All Rights Reserved
Verfügbare Formate
PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCourse Objectives (Complete, L1-7)
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
35 Ansichten56 SeitenCourse Objectives (Complete, L1-7)
Hochgeladen von
mrlucky09855Course Objectives (Complete, L1-7)
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 56
Week 1 - History of Radiology:
(1) Know when and who invented radiology
Wilhelm Conrad Roentgen is recognized as the Father of Radiology/Roentgenology. In 1895,
Roentgen began experiments using electric current flow in a partially-evacuated glass tube,
known as a cathode-ray tube. He noticed that, whenever the tube was in operation, a piece of
barium platinocyanide in line with it gave off light.
Roentgen theorized that the interaction of electrons striking the tube's glass wall formed an
unknown radiation that caused the fluorescence. He called the mysterious phenomenon X-
radiation, or X-rays. Today, the cathode-ray tube is composed of tungsten, except in
mammography, where it is composed of molybdenum.
(2) Understand the concept of projection and how it affects image quality
The quality of a medical image is determined by the imaging method, the characteristics of the
equipment and the imaging variables selected by the operator. Image quality is not a single factor
but is a composite of at least 5 factors: contrast, blur, noise, artifacts and distortion.
(3) Understand the concept of how an image is formed
In projection imaging (radiography and fluoroscopy), images are formed by projecting an x-ray
beam through the patient's body and casting shadows onto an appropriate receptor that converts
the invisible x-ray image into a visible light image. The gamma camera records a projection
image that represents the distribution of radioactive material in the body. The primary advantage
of this type of image is that a large volume of the patient's body can be viewed with one image.
A disadvantage is that structures and objects are often superimposed so that the image of one
might interfere with the visibility of another. Projection imaging produces spatial distortion that
is generally not a major problem in most clinical applications.
Tomographic imaging, i.e., conventional tomography, computed tomography (CT), sonography,
single photon emission tomography (SPECT), positron emission tomography (PET), and MRI,
produces images of selected planes or slices of tissue in the patient's body. The general
advantage of a tomographic image is the increased visibility of objects within the imaged plane.
One factor that contributes to this is the absence of overlying objects. The major disadvantage is
that only a small slice of a patient's body can be visualized with one image. Therefore, most
tomographic procedures usually require many images to survey an entire organ system or body
cavity.
(4) Understand the amount of radiation exposure with different radiologic modalities
X-ray: most common imaging technique used today; the most common x-ray ordered is a chest
x-ray, and the musculoskeletal x-ray exam comes in second. An x-ray provides a 2-D image of
the 3-D interior of the body. A single x-ray passes through the body and exposes the film on a
radiograph (or fluorescent screen) placed on the opposite side.
CT: x-rays move as laser-like beam in an arch around the part of the body being observed. The
beam of x-rays passed through the region of the body imaged are collected by a detector that
converts the x-rays into electronic pulses, which produce readings of the tissue density into a
1cm slice of the body. From these readings, a computer can assemble a picture of the body,
called a CT scan, which can be viewed on a fluorescent screen, then photographed for later
examination. It obtains parts of the body that can't be seen on a standard x-ray with the help of
computer algorithms in conjunction with the enhanced x-ray technology.
MRI: uses the magnetic properties of the hydrogen nucleus, which is excited by radiofrequency
radiation transmitted by a coil, which surrounds by the body part being imaged. When placed in
strong magnetic fields, the nuclei of certain atoms absorb radiofrequencies beamed at them, and
then emit their own radio frequency waves. This process allows readers to see very clear pictures
of the inside of the body, including tissues, organs and blood vessels. MRI is a noninvasive
technique that does not use ionizing radiation. MRI has become one of the primary tools used to
image the brain, spinal cord, MSK (musculoskeletal) system, major blood vessels and several
key organs and extremities. The images can be produced in 3-D, which significantly enhances
the physician's ability to diagnose problems. MRI is also used to help view the process of surgery
in real time in 3-D, which assists with a whole host of surgical procedures.
Differences between CT scans and X-Ray's: CT scans are an advanced form of x-ray
technology used in detecting diseases in soft body tissues, and can actually provide images of
internal organs that are impossible to detect with standard x-ray techniques. X-rays are good at
finding bone fractures, and for being used as a contrasting agent for several types of exams;
however, CT provides greater detail and clarity. CT scans have additional advantages of being
able to produce imaging in virtually any orientation. It is a more technologically developed
version of an x-ray, which is used on specific parts of the body. It also provides better images for
bone structures, such as the inner ear as it can easily detect tumors in the auditory canal and
cochlea. CT scans help diagnose bone fractures, bone tumors, internal injuries and bleeding and
blood clots, and to monitor heart diseases and cancer.
Differences between CT scans & MRI's: MRI uses magnetic waves to produce images while
CT images are produced using x-rays. MRI provides moredetails of bony structures compared to
CT scans. CT scans cannot help much in seeing clearly, very fine, soft tissue details as in the
shoulder or knee compared to MRI. MRI scans are best for imaging soft tissue. CT scans are
much more costly and takes a longer time (30 minutes) to be completed compared to a MRI that
takes about 5 minutes to complete. People with surgical clips, metallic fragments, cardiac
monitors and pacemakers cannot have CT scans. Also, pregnant women should not have CT
scans, and they should be used with caution in children and young adults. MRI machines can
produce images in any plane without moving the patient. They also have the ability to change the
contrast of images, making them clearer than CT scans.
Table: American College of Radiology appropriateness criteria, relative radiation level
information
Relative radiation
level
Effective dose estimate
range
Example examinations
None 0 Ultrasound, MRI
Minimal <1 mSv Chest radiographs, hand radiographs
Low 15 mSv Head CT, lumbar spine radiographs
Medium 510 mSv Abdomen CT, barium enema, nuclear medicine
bone scan
High >10 mSv Abdomen CT without and with contrast, whole
body PET
Week 2 - Musculoskeletal:
(1) Understand fracture terminology
Displaced: loss of contact between fracture fragments
Dislocated: loss of contact between joint surfaces
Comminuted: bone fractures into 2+fragments
Impacted: bone fragments are driven into each other
Angulation: bone fragments are at angles to one another
Intra-articular: break crosses into joint surface; always result in some degree of cartilage damage.
Pathologic: abnormal bone; fracture through bone made weak by disease, such as a tumor.
Insufficiency: weak bone; fracture through weak bone, such as due to osteoporosis.
Occult: does not appear in x-rays, but bone shows new formation within 3-4 weeks of fracture.
Open vs. closed:
Closed/simple fracture: skin is still intact.
Open/compound fracture: involves wounds that communicate with the fracture.
Stress fracture: fracture through bone due to abnormal force; NOT an insufficiency fracture.
Greenstick / torus / buckle: typically occurs in a young, soft bone in which the bone bends
and partially breaks. It is due to mechanical failure on the tension side; that is, since the bone is
not as brittle as it would be in an adult, it does not completely fracture, but rather exhibits
bowing without complete disruption of the bone's cortex in the surface opposite the applied
force.
What do fractures look like?
- Loss of cortical integrtity
- Deformity
- Periosteal reaction (subactue): formation of new bone in response to injury or other stimuli of
the periosteum surrounding the bone
- Effusion
- Soft tissue swelling
- Bony lucency
- Invisible
(2) Be familiar with the cervical spine bone anatomy
Lateral view
P-A view
Contour lines/margins:
(3) Be able to identify the following plain films:
- Salter-Harris fracture: involves epiphyseal/growth plate of a bone; common injury in children.
Salter-Harris fracture
Normal epiphysis/growth plate
- Distal radius fracture
Colle's fracture: fracture of the distal radius with dorsal/posterior displacement of the
wrist and hand; it is aka "dinner fork" deformity. It is a dorsally-angulated fracture
because the fracture faces the dosrsal/posterior surface.
Smith's fracture (opposite of Colle's): fx of distal radius w/ volar/anterior/palmar
displacement of the wrist and hand.
Smiths fracture vs. Colles fracture:
Barton's fracture: comminuted (2+fragments), intra-articular fracture of the distal radius
with dislocation of the radiocarpal joint; palmar/volar is more common than
dorsal/posterior.
Boxers: transverse fracture through the neck of a metacarpal bone; more likely to occur from a
straight punch, hence the name. In this image, distal 5
th
metacarpal fracture.
- Simple vs. comminuted fracture: see above (Colles vs. Bartons)
- Dislocation vs. displacement
- Dislocation fracture (aka luxation): occurs when bones in a joint become displaced or
misaligned. It is often caused by a sudden impact to the joint. The ligaments always
become damaged as a result of a dislocation. A subluxation is a partial dislocation.
- Displaced fracture: fracture in which the 2 ends of the bone are separated from one
another, no longer in anatomical alignment.
- Hip Fracture (major kinds of femoral neck fractures)
- Greenstick fracture:
- Cervical spine fractures
CT: better for bone detail
MRI: better for soft tissue and joint detail
1. AA (atlanto-axial) dislocation
Hyperextension injury
Children>adults
Head slips forward on C1
Usually fatal
2. J efferson fracture of C1:
Fracture of the anterior and posterior arches of C1 (atlas vertebra), often appearing as
a 2-part or 3-part fracture.
Burst fracture; caused by compressive force
Bilateral breaks in anterior and posterior arches
Open mouth view shows bilateral offset of C1 on C2
Not associated with neurologic deficit
3. Hangmans fracture (traumatic spondylolisthesis) of C2:
Fracture of either both pedicles or pars interarticularis of C2 (axis vertebra).
Most common fracture of C2
Most common cervical spine fracture
Hyperextension/compression fracture
Fractures through pedicles of C2, with anterior slip of C2 on C3
Teardrop fracture of inferior aspect of C2 or C3 is clue to dx of Hangmans fracture
Not associated with neurologic deficit
4. Odontoid (Dens) fracture:
Fracture through the odontoid process (dens).
Hyperextension injury; generally associated with anterior of C1 subluxation on C2.
3 types:
Type I (tip of dens): extends through the tip of the dens; usually stable.
Type II (base of dens): extends through the base of the dens; most commonly
encountered fracture for this region of the axis, never stable.
Type III (sub-dentate / below dens): extends through vertebral body of the axis; can
be stable or unstable.
5. Flexion-teardrop fracture
Fracture of the antero-inferior aspect of a cervical vertebral body due to flexion of the
spine, along with vertical axial compression. It is usually associated with spinal cord
injury, often a result of displacement of the posterior portion of the vertebral body
into the central spinal canal.
Combination of flexion and compression, e.g. MVA (motor vehicle accident)
Teardrop fragment comes from antero-inferior aspect of vertebral body
Remainder of body displaced backward into spinal canal
Facet joint and interspinous distances usually widened
Disk space may be narrowed
70% have associated neurologic deficit
- Pathologic fracture: fracture through bone, made weak by disease, such as by a tumor
- Radial head (proximal radius) fracture: sails sign present =anterior and posterior fat pad
displacement/elevation/swelling surrounding the elbow joint
Week 3 - Abdomen Plain Films and Ultrasound
(1) Understand the diagnostic role of plain abdominal film
a. Abdominal X-ray has as much radiation as 30 chest xrays.
b. Good Reasons to order
i. Cheap, Fast, available, can be highly specific
c. Bad reasons to order
i. Cheap (get what you pay for), available (order because they can), can be
limited.
d. What it shows
i. Free fluid
ii. Air outside the bowel lumen
1. Intraperitoneal, retroperitoneal, abscess, pneumatosis
2. Cant see pneumoperitoneum in supine position (erect or lateral
decubitus is used)
iii. Air inside the bowel lumen
1. Ileus, Bowel obstruction, Volvulus
2. Small bowel vs colon air
a. Small bowel: Centrally located, valvulae conniventes
b. Colon: Peripherally located, haustral markings.
3. Too Much Gass Intestinal Dilation (3 cm in small bowel, 6-8 in
colon)
a. Think Obstruction or Ileus
i. Ileus think absent bowel sounds and think post-op
or possible meds that suppress bowel activity)
b. Next test for obstruction CT
4. Air fluid levels Look for associated signs of obstruction.
iv. Bowel wall thickening
v. Densities
1. Bones, appendicolith, stones, pancreatic calcification, AAA
vi. Organs.
Plain abdominal film:
- Normal plain abdominal film does not exclude ileus or other pathology, and may falsely
reassure the clinician
- Plain abdominal film has a limited value in the evaluation of abdominal pain
- Plain abdominal films are useful for detection of:
o Kidney stones
o Pneumoperitoneum
- All other indications: use CT or sonography/US (ultrasound)
(2) Understand the best test to order for gallbladder disease, appendicitis, kidney stones,
testicular pain, and ovarian/gyn issues
a. Gallbladder disease
vii. Ultrasound (Single best for cholecystitis)
1. Ultrasound is only 85% sensitive in detection of bile duct stones
(Still test of choice)
b. Pancreas
viii. CT
c. Appendicitis
ix. Ultrasound: for Peds, poor in adults.
x. MRI for Pregnant
xi. CT: Single Best test.
d. Kidney Stones
xii. Non-Con CT is more Sensitive
xiii. Ultrasound for Kidney masses (Cystic vs solid)
e. Testicular pain
xiv. Ultrasound (small parts imaging: testes, breast, thyroid)
f. OBGYN Issues
xv. Ultrasound
Gallbladder disease: ultrasound. Cholecystitis occurs when a calculus obstructs the cystic duct.
The trapped bile causes inflammation of the gallbladder wall. As gallstones are often occult on
CT, US is the preferred imaging method for the evaluation of cholecystitis, also allowing
assessment of the compressibility of the gallbladder.
Appendicitis: CT. According to a systematic review from UCSF comparing US vs. CT scans, CT
is more accurate than US for the diagnosis of appendicitis in adults and adolescents. CT has a
sensitivity of 94% and specificity of 95. US had an overall sensitivity of 86% and a specificity of
81%.
Kidney stones: CT without contrast. Ca
2+
-containing stones are relatively radiodense, and they
can often be detected by a traditional x-ray of the abdomen that includes the kidneys, ureters, and
bladder (KUB film). Where available, a non-contrast, helical CT scan is the diagnostic modality
of choice in the radiographic evaluation of suspected nephrolithiasis. All stones are detectable on
CT scans, except very rare stones composed of certain drug residues in the urine.
Testicular pain: ultrasound. Doppler ultrasonography in patients with testicular pain helps
distinguish torsion from other causes by assessing testicular blood flow. Radionuclide scanning
can also be used to image blood flow to the testes.
Ovary / gynecological issues: US can be used to determine the right treatment for an ovarian or
gynecologic issue by examining blood flow to the ovaries. Potential complications of
hysterectomy and other gynecologic and obstetric procedures are numerous. These complications
include ureteral obstruction or transection, bladder perforation, bowel perforation or obstruction,
fistula, bleeding, abscess, retention of surgical instruments or sponges, incisional hernia, and
tumor or endometriosis implants in surgical scars. The available imaging techniques are almost
as varied as the problems they investigate. CT, intravenous urography (IVU), ultrasonography,
MRI, gastrointestinal fluoroscopic studies, angiography and even scintigraphy can be used to
diagnose complications. Furthermore, each technique can be optimized to answer a particular
question. If the surgeon is looking for a specific complication, the technique should be adjusted
to answer that question. Typically, if cancer is being diagnostically investigated, then X-ray and
CT are not used due to radiation exposure.
SBO (small bowel obstruction) and/or perforated bowel: CT. CT is superior to conventional
radiography and barium studies in diagnosing SBO.
Pneumothorax: chest x-ray, P-A and lateral views. Traditionally a plain P-A chest x-rayhas been
the most appropriate first investigation. These are usually performed during maximal inspiration
(holding one's breath); no added information is gathered by obtaining a chest X-ray in expiration
(after exhaling). If the PA X-ray does not show a pneumothorax but there is a strong suspicion,
lateral X-rays may be performed, but this is not routine practice. CT can be useful in particular
situations, such as lung diseases like emphysema, and/or the identification of underlying lung
lesions. Ultrasound may be more sensitive than chest X-rays in the identification of
pneumothorax after blunt trauma to the chest.
CT: generally not used or used with caution for pregnant women, children and young adults
because of radiation exposure
(3) Be able to identify the following on a plain x-ray of the abdomen:
OBGYN Issues
Ultrasound
e. Small bowel obstruction
i. Dilation over 3cm. Look for valvulae conniventes
(thin circular folds of mucosa that span the entire
width)
ii. Causes: Adhesions, Ileus
f. Large bowel obstruction
i. Over 6-8 cm in diameter. Look for haustra.
ii. Peripherally located.
iii. Common cause: Colorectal carcinoma and
diverticular strictures, Hernias, Volvulus.
g. Constipation
i. Stool is Opaque white surrounded by black bowel gas
h. Free intraperitoneal air
i. Emergency (Bowel Perforation)
ii. Erect Position: Look for a crescent beneath the
diaphragm.
iii. (Below is same pt with free air highlighted in red)
i. Large kidney stones
- Small Bowel Obstruction
Key features of mechanical SBO:
- Dilated small bowel
- Fighting loops
- Little gas in colon, especially rectum
- Disproportionate dilatation of SB
- Large Bowel Obstruction
Key features of mechanical LBO:
Dilated colon until point of obstruction
Little or no air in sigmoid/rectum
Little or no gas in small bowel, if ileocecal valve remains competent
- Constipation
- Pneumoperitoneum (free intraperitoneal air)
Signs: air beneath diaphragm, both sides of bowel wall, falciform ligament sign
White arrow: evidence of free air between
the abdominal wall and the liver. Black
arrow: evidence of free fluid in the
peritoneum.
- Large Kidney Stones
Summary info from lecture (last 3 pages of text):
Hounsfield units (HU) relate the attenuation coefficients of tissue to that of water (HU =0)
Tissues with lower attenuation (fats) are negative (fats), those with higher attenuation
(bone/calcium) are positive
Windows adjust the gray scale to make visible different portions of the image
Metals can cause artifacts
Use water soluble oral contrast (if at all) when perforation is suspected. Other commonly used
contrast is barium.
IV contrast is I
-
(iodine) based; helps distinguish cystic from solid, as it helps to visualize
vasculature and viscera.
Contraindications of IV contrast include allergy (pre-treat with steroids) and renal insufficiency
(creatinine >2.0)
Sometimes IV contrast is not needed, e.g. renal stones or head trauma
CT should be used judiciously, especially in the young/children and pregnant women
CT plays a large role in the imaging of cancer, trauma, vascular pathology and abdominal
symptoms
Intra-abdominal fluid is a marker of pathology
Other important stuff:
Abdominal CT images, 2 axial:
Anterior
Posterior
Anterior
Posterior
What to look for:
Obstruction series Normal gas pattern Abnormal gas pattern Aunt Minnies (image
appearance so classic that, once you see it, you easily ID it) Extraluminal air Soft tissue
masses Calcifications
Normal gas patterns:
- Stomach: gas ALWAYS present
- Small bowel: gas in 23 loops of non-distended bowel
- Large bowel: gas almost always present in sigmoid or rectum
Normal fluid levels:
- - Stomach: fluid ALWAYS present, except in supine films
- Small bowel: few (23) levels of fluid possible
- Large bowel: no fluid should be present
Small bowel vs. Large bowel
- Small bowel:
-- Central
-- Valvulae extend across lumen
-- Maximal diameter of 2
- Large bowel:
-- Peripheral
-- Haustral markings do not extend from wall-to-wall
Week 4 - Chest: Part One:
(1) Understand X-ray densities and transmission of x-rays
Tissues having different densities show up as differing densities on the radiograph. There are 5
fundamental radiographic densities. This is how they may appear on the fluorescent screen: air
and gases appear black or radiolucent. Fat appears gray to black. Muscles and water appear grey.
Bones and calcium appear white, or radiopaque. Metal appears extremely white. A tissue that is
denser absorbs more x-rays than tissues that are less dense. Radiopaque (bone/calcium and
metal) is a very dense tissue, and a less dense tissue (fat) is said to be radiolucent.
(2) How does an x-ray create a visible image on a radiograph?
Beam from cathode tube fans out and increases in size the further away it is from the source
(cathode tube). Want the area being imaged closest to film (not x-ray source/tube) in order to
properly capture the area. The further away the film is to the area being imaged, the larger and
more fuzzy (i.e., less clear and focused) the organ/image will be.
X-ray radiation for medical imaging is typically produced by x-ray tubes, which operate through
bombarding the anode with high energy electrons emitted from a hot cathode. Image sharpness,
contrast, and patient dosage are important considerations in medical radiography and these
requirements determined the desired energies of the tube, the type of material used on the anode,
and the method in which the power is generated to drive the tube. The photons emitted come in
discrete bands of energy corresponding to the material of the anode, and the undesired bands are
removed. Choice of the anode and its emitted radiation energies depends on the application and
the tissues being imaged, for instance molybdenum is often used in mammography. Too high
radiation energies will result in poor pictures since the radiation cannot be readily attenuated,
however too low energies will increase the radiation dosage of the patient without improvements
in image quality.
Sharpness of a radiographic image is strongly determined by the size of the x-ray source. This is
determined by the area of the electron beam hitting the anode. A large photon source results in
more blurring in the final image and is worsened by an increase in image formation distance.
This blurring can be measured as a contribution to the modulation transfer function of the
imaging system.
(3) Describe the term that indicates when different densities may appear the same on a
radiograph, as well as being familiar with the major sources of artifact on chest x-rays.
Silhouette sign: produced when two fluid densities are contiguous and the individual outline
of each is lost. Commonly used in the evaluation of chest problems.
Loss of different densities when a film is too dark is due to OVER exposure, while a film that is
too white would be considered UNDER exposed could also explain different densities appearing
the same.
The silhouette sign refers to loss of normal border between structures, or an intra-thoracic radio-
opacity obscuring the border of the heart or aorta due to a contiguous structure.
In other words it
is difficult to make out the borders of a particular structure - normal or otherwise - because it is
next to another dense structure, both of which will come up as white on a standard X-ray. It may
occur, for example, in middle lobe disease, where the right heart margin is lost, and in right
lower lobe pneumonia, where the border of the diaphragm on the right side is obscured, while the
right heart margin remains distinct.
Most imaging methods can create image features that do not represent a body structure or object.
These are image artifacts. In many situations an artifact does not significantly affect object
visibility and diagnostic accuracy. But artifacts can obscure a part of an image or may be
interpreted as an anatomical feature. A variety of factors associated with each imaging method
can cause image artifacts.
Example of artifact caused by patients hair:
(4) Understand the technical approach to reading a chest x-ray
Check the image for - Inclusion, Projection, Rotation, Inspiration, Penetration and Artifact
Inclusion: A chest X-ray should include the entire thoracic cage. Look for First ribs,
costophrenic angles and the lateral edges of ribs.
Projection: PA projection is typical. X-rays pass from the posterior to the anterior of the
patient - hence Posterior-Anterior (PA) projection. The image is viewed as if looking at
the patient face-to-face.
Rotation: The spinous processes of the thoracic vertebrae are in the midline at the back
of the chest. They should form a vertical line that lies equidistant from the medial ends of
the clavicles, which are at the front of the chest. Rotation of the patient will lead to off-
setting of the spinous processes so they lie nearer one clavicle than the other. Find the
medial ends of the clavicles, Find the vertebral spinous processes, The spinous processes
should lie half way between the medial ends of the clavicles Assessing inspiration
Inspiration: To assess the degree of inspiration it is conventional to count ribs down to
the diaphragm. The diaphragm should be intersected by the 5th to 7th anterior ribs in the
mid-clavicular line. Less is a sign of incomplete inspiration.
Penetration: A well penetrated chest X-ray is one where the vertebrae are just visible
behind the heart. Although X-rays are still occasionally over or under exposed, a
discussion of penetration now best serves as a reminder to check behind the heart. The
left hemidiaphragm should be visible to the edge of the spine. Loss of the hemidiaphragm
contour or of the paravertebral tissue lines may be due to lung or mediastinal pathology.
Artifact: examples include rotation, incomplete inspiration and incorrect penetration.
Other radiographic artifact includes clothing or jewelry not removed. Other common
artifact to find is medical or surgical equiptment like NG tubes.
Mnemonic for reading a [normal] chest x-ray: ABCDEFGHI
A =Airway
B =Bone
C =Cardiac silhouette
D =Diaphragm
E =Edge of the heart
F =Field of lung
G =Gastric bubble
H =Hilum of lung
I =Impression (diagnosis)
14 steps (total):
1. Check the patient's name. Above all else, make sure you are looking at the correct chest
x-ray first.
2. Read the date of the chest radiograph. Make special note of the date when comparing
older radiographs (always look at older radiographs if available). The date the radiograph
is taken provides important context for interpreting any findings. For example, a mass
that has become bigger over 3 months is more significant than one that has become
bigger over 3 years.
3. Note the type of film (while this article assumes you are looking at a chest x-ray, practice
noting if it is a plain film, CT, angiogram, MRI, etc.) For chest x-ray, there are several
views as follows:
o The standard view of the chest is the posteroanterior radiograph, or "PA chest."
Posteroanterior refers to the direction of the x-ray traversing the patient from
posterior to anterior. This film is taken with the patient upright, in full inspiration
(breathed in all the way), and the x-ray beam radiating horizontally 6 feet away
from the film.
o The anteroposterior (AP) chest radiograph is obtained with the x-ray traversing
the patient from anterior to posterior, usually obtained with a portable x-ray
machine from very sick patients, those unable to stand, and infants. Because
portable x-ray units tend to be less powerful than regular units, AP radiographs
are generally taken at shorter distance from the film compared to PA radiographs.
The farther away the x-ray source is from the film, the sharper and less magnified
the image. (You can confirm this by placing your hand about 3 inches from a
desk, shining a lamp above it from various distances, and observing the shadow
cast. The shadow will appear sharper and less magnified if the lamp is farther
away.) Since AP radigraphs are taken from shorter distances, they appear more
magnified and less sharp compared to standard PA films.
o
Lateral chest x-ray.
The lateral chest radiograph is taken with the patient's left side of chest held
against the x-ray cassette (left instead of right to make the heart appear sharper
and less magnified, since the heart is closer to the left side). It is taken with the
beam at 6 feet away, as in the PA view.
o An oblique view is a rotated view in between the standard front view and the
lateral view. It is useful in localizing lesions and eliminating superimposed
structures.
o
Right lateral decubitus chest x-ray showing pleural effusion. The A arrow
indicates "fluid layering" in the right chest. The B arrow indicates the width of the
right lung. The volume of useful lung is reduced because of the collection of fluid
around the lung.
A lateral decubitus view is one taken with the patient lying down on the side. It
helps to determine whether suspected fluid (pleural effusion) will layer out to the
bottom, or suspected air (pneumothorax) will rise to the top. For example, if
pleural fluid is suspected in the left lung, check a left lateral decubitus view (to
allow the fluid to layer to the left side). If air is suspected in left lung, check a
right lateral decubitus view (to allow the air to rise to the left side).
4. Look for markers: 'L' for Left, 'R' for Right, 'PA' for posteroanterior, 'AP' for
anteroposterior, etc. Note the position of the patient: supine (lying flat), upright, lateral,
decubitus.
5. Note the technical quality of film.
o Exposure: Overexposed films look darker than normal, making fine details harder
to see; underexposed films look whiter than normal, and cause appearance of
areas of opacification. Look for intervertebral bodies in a properly penetrated
chest x-ray. An under-penetrated chest x-ray cannot differentiate the vertebral
bodies from the intervertebral spaces, while an over-penetrated film shows the
intervertebral spaces very distinctly.
To assess exposure, look at the vertebral column behind the heart on the
frontal view. If detailed spine and pulmonary vessels are seen behind the
heart, the exposure is correct. If only the spine is visible, but not the
pulmonary vessels, the film is too dark (overexposed). If the spine is not
visible, the film is too white (underexposed).
o Motion: Motion appears as blurred areas. It is hard to find a subtle pneumothorax
if there is significant motion.
o Rotation: Rotation means that the patient was not positioned flat on the x-ray film,
with one plane of the chest rotated compared to the plane of the film. It causes
distortion because it can make the lungs look asymmetrical and the cardiac
silhouette disoriented. Look for the right and left lung fields having nearly the
same diameter, and the heads of the ribs (end of the calcified section of each rib)
at the same location to the chest wall, which indicate absence of significant
rotation. If there is significant rotation, the side that has been lifted appears
narrower and denser (whiter) and the cardiac silhouette appears more in the
opposite lung field.
6.
Left tension pneumothorax. Note the large, well-demarcated area devoid of lung
markings, and deviation of the trachea (airway) and the heart away from the affected side.
The bright metallic spots are snaps for EKG readings.
Airway: Check to see if the airway is patent and midline. For example, in a tension
pneumothorax, the airway is deviated away from the affected side. Look for the carina,
where the trachea bifurcates (divides) into the right and left main stem bronchi.
7.
Fracture of the left clavicle.
Bones: Check the bones for any fractures, lesions, or defects. Note the overall size, shape,
and contour of each bone, density or mineralization (osteopenic bones look thin and less
opaque), cortical thickness in comparison to medullary cavity, trabecular pattern,
presence of any erosions, fractures, lytic or blastic areas. Look for lucent and sclerotic
lesions. A lucent bone lesion is an area of bone with a decreased density (appearing
darker); it may appear punched out compared to surrounding bone. A sclerotic bone
lesion is an area of bone with an increased density (appearing whiter). At joints, look for
joint spaces narrowing, widening, calcification in the cartilages, air in the joint space,
abnormal fat pads, etc.
8.
Enlarged cardiac silhouette in a case of aortic dissection (blood fills the mediastinum).
Note that the cardiac silhouette takes up more than half of the chest width. Characteristic
of aortic dissection here is the enlarged mediastinum (labeled 1) and aortic arched
(labeled 2).
Cardiac silhouette: Look at the size of the cardiac silhouette (white space representing the
heart, situated between the lungs). A normal cardiac silhouette occupies less than half the
chest width.
o Look for water-bottle-shaped heart on PA plain film, suggestive of pericardial
effusion. Get an ultrasound or chest Computed Tomagraphy (CT) to confirm.
9.
Left pleural effusion associated with left lower lobe pneumonia: note that the
costophrenic angle is blunted, and the left diaphragm is raised compared to the right.
Diaphragms: Look for a flat or raised diaphragm. A flattened diaphragm may indicate
emphysema. A raised diaphragm may indicate area of airspace consolidation (as in
pneumonia) making the lower lung field indistinguishable in tissue density compared to
the abdomen. The right diaphragm is normally higher than the left, due to the presence of
the liver below the right diaphragm. Also look at the costophrenic angle (which should be
sharp) for any blunting, which may indicate effusion (as fluid settles down). It takes
about 300-500 ml of fluid to blunt the costophrenic angle.
10.
A) Normal chest radiograph; B) Q fever pneumonia affecting the lower and middle lobes
of the right lung. Note the loss of the normal radiographic silhouette (contour) between
the affected lung and its right heart border as well as between the affected lung and its
right diaphragm border. This phenomenon is called the silhouette sign.
Edges of heart; External soft tissues: Check the edges of the heart for the silhouette sign:
a radioopacity obscuring the heart's border, in right middle lobe and left lingula
pneumonia, for example. Also, look at the external soft tissues for any abnormalities.
Note the lymph nodes, look for subcutaneous emphysema (air density below the skin),
and other lesions.
11.
Right lower lobe pneumonia. Note the prominent air-bronchogram sign: air visualized in
the peripheral intrapulmonary bronchi, due to an infiltrate or consolidation surrounding
the bronchi.
Fields of the lungs: Look for symmetry, vascularity, presence of any mass, nodules,
infiltration, fluid, bronchial cuffing, etc. If fluid, blood, mucous, or tumor, etc. fills the air
sacs, the lungs will appear radiodense (bright), with less visible interstitial markings.
12.
Gastric bubble: Look for the presence of a gastric bubble, just below the heart; note
whether it is obscured or absent. Assess the amount of gas and location of the gastric
bubble. Normal gas bubbles may also be seen in the hepatic and splenic flexures of the
colon.
13.
Enlarged lymph node in left hilum, in a case of carcinoid tumor.
Hila: Look for nodes and masses in the hila of both lungs. On the frontal view, most of
the hilar shadows represent the left and right pulmonary arteries. The left pulmonary
artery is always more superior than the right, making the left hilum higher. Look for
calcified lymph nodes in the hilar, which may be caused by an old tuberculosis infection.
14.
Breast implants.
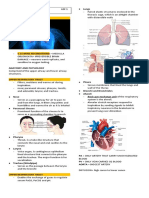
(5) When looking at a chest x-ray, be able to identify normal anatomic landmarks and
major disease patterns, such as:
- Right Atrium, Right Ventricle, Left Ventricle, Diaphragms, Ribs, Trachea,
Aortic Arch, Pulmonary Fissures, Costophrenic Angle (see below at chest x-ray anatomic
structures to check)
Pneumonia
CHF note enlarged heart
Cardiomegaly
Air Bronchogram
If an area of lung is consolidated it
becomes dense and white. If the
larger airways are spared, they are of
relatively low density (blacker). This
phenomenon is known as air
bronchogram and it is a
characteristic sign of consolidation.
Right Atrium, Right Ventricle,
Left Ventricle, Diaphragms, Ribs,
Trachea,
Aortic Arch, Pulmonary Fissures,
Costophrenic Angle
Pneumothorax
- Free Intraperitoneal Air
- Pneumonia: The x-ray findings of pneumonia are airspace opacity, lobar consolidation, or
interstitial opacities. There is usually considerable overlap. Again, pneumonias is a space
occupying lesion without volume loss. What differentiates it from a mass? Masses are generally
more well-defined. Pneumonia may have an associated parapneumonic effusion.
- Congestive Heart Failure: The earliest CXR finding of CHF is cardiomegaly, detected as an
increased cardiothoracic ratio (>50%). In the pulmonary vasculature of the normal chest, the
lower zone pulmonary veins are larger than the upper zone veins due to gravity. In a patient with
CHF, the pulmonary capillary wedge pressure rises to the 12-18 mmHg range and the upper zone
veins dilate and are equal in size or larger, termed cephalization. With increasing PCWP
(pulmonary capillary wedge pressure, 18-24 mmHg.), interstitial edema occurs with the
appearance of Kerley lines. Increased PCWP above this level is alveolar edema, often in a classic
peri-hilar bat wing pattern of density. Pleural effusions also often occur.
- Cardiomegaly: refers to excessive heart size in proportion to the diameter of the rib cage. Heart
size is usually estimated based on the cardiothoracic ratio, which compares the maximum width
of the cardiac silhouette on a frontal CXR, with the maximum internal diameter of the rib cage.
Cardiomegaly is usually present if the maximum width of the cardiac silhouette is >50% of the
maximum internal diameter of the rib cage.
- Air Bronchogram: sign in which branching radiolucent columns of air corresponding to bronchi
is seen, usually indicates air-space (alveolar) disease, as from blood, pus, mucus, cells, protein
surrounding the air bronchograms; this is often seen in RDS (respiratory distress syndrome),
specifically occurring due to infiltrates outlining larger air passageways. Air bronchograms occur
when there is pulmonary infiltration or edema in the tissues immediately adjacent to the bronchi.
Darker tubular densities can be seen when the inflammatory process involves the alveoli but has
not filled the bronchi with fluid, and therefore distinguishes this disease from cases of atelectasis
or pulmonary edema.
- Pneumothorax: The symptoms of pneumothorax can be vague and inconclusive, especially in
those with a small PSP, and confirmation with medical imaging is usually required. In contrast,
tension pneumothorax is a medical emergency and may be treated before imaging - especially if
there is severe hypoxia, very low blood pressure, or an impaired level of consciousness. In
tension pneumothorax, X-rays are sometimes required if there is doubt about the anatomical
location of the pneumothorax.
The lung is held close to chest wall because
of the negative pressure in the pleural space.
Once the negative pressure is lost the lung
tends to recoil due to elastic properties and
becomes atelectatic. This occurs in patients
with pneumothorax and pleural effusion.
- Pneumoperitoneum (free intraperitoneal air)
Signs: air beneath diaphragm, both sides of bowel wall, falciform ligament sign
White arrow: evidence of free air between the abdominal wall and the liver. Black arrow:
evidence of free fluid in the peritoneum.
Chest x-ray anatomic structures to check
1. Trachea/bronchi
2. Hilar structures
3. Lung zones
4. Pleura
5. Lung lobes/fissures
6. Costophrenic angles
7. Diaphragm
8. Heart
9. Mediastinum
10. Soft tissues
11. Bones
Week 5 - Chest: Part Two:
(1) Understand X-ray transmission and how that is related to CT scans
X-ray source and detectors rotate around patient
Amount of radiation transmitted though body at various angles is recorded
Creates density map of human tissue
Table carries patient past continuously rotating x ray tube =volumetric data
acquisition
CT scans are an advanced form of x-ray technology used in detecting diseases in soft body
tissues, and can actually provide images of internal organs that are impossible to detect with
standard x-ray techniques. X-rays are good at finding bone fractures, and for being used as a
contrasting agent for several types of exams; however, CT provides greater detail and clarity. CT
scans have additional advantages of being able to produce imaging in virtually any orientation. It
is a more technologically developed version of an x-ray, which is used on specific parts of the
body. It also provides better images for bone structures, such as the inner ear as it can easily
detect tumors in the auditory canal and cochlea. CT scans help diagnose bone fractures, bone
tumors, internal injuries and bleeding and blood clots, and to monitor heart diseases and cancer.
(2) Understand the resolution differences between chest x-ray and CT scans
An Xray produces a single image in which structures are overlaid on each other. In contract a CT
produces many slices of an image, essentially using many xrays at different angles to create
images of layers throughout the body.
There are several advantages that CT has over traditional 2D medical radiography (i.e. plain x-
ray films). First, CT completely eliminates the superimposition of images of structures outside
the area of interest. Second, because of the inherent high-contrast resolution of CT, differences
between tissues that differ in physical density by less than 1% can be distinguished. Finally, data
from a single CT imaging procedure consisting of either multiple contiguous or one helical scan
can be viewed as images in the axial, coronal, or sagittal planes, depending on the diagnostic
task. This is referred to as multi-planar reformatted imaging. CT scans use a high level of
ionizing radiation. Ionizing radiation has the capacity to break molecular bonds, and thus alter
the molecular structure of the irradiated molecules.
(3) Understand how IV contrast administration effects contrast
Intravenous contrast is used to highlight blood vessels and to enhance the structure of organs like
the brain, spine, liver, and kidney. Typically the contrast is contained in a special injector, which
injects the contrast through a small needle taped in place (usually on the back of the hand) during
a specific period in the CT exam. Once the contrast is injected into the bloodstream, it circulates
throughout the body. The CT's x-ray beam is weakened as it passes through the blood vessels
and organs that have "taken up" the contrast. These structures are enhanced by this process and
show up as white areas on the CT images. When the test is finished, the kidneys and liver
quickly eliminate the contrast from the body.
IV contrast is a substance that is opaque to x-rays. When administered, it brightens and allows
greater visualization of internal organs, arteries, veins and tissues as it courses through them. For
some exams it is essential and cannot be done properly without it, while with other exams it is
contraindicated, as it may cause anaphylaxis, nephropathy or negative / drug-drug interactions.
(4) When looking at CT scans, be able to identify normal landmarks:
- Heart (Here are 4 images: superior to inferior)
- Pulmonary Arteries
- Pulmonary Fissures
Right side:
major (oblique): separates upper from lower lobe
minor (horizontal): separates upper from middle lobe
Left side:
major (oblique): separates upper from lower lobe
The coronal CT image on the left shows the right minor (horizontal) fissure (white arrow), right
major fissure (yellow arrow), and left major (oblique) fissure. These structures are also seen on
the right lateral sagittal CT image on the right. The minor fissure separates the right superior lobe
from the right middle lobe. The right major fissure separates the right upper and middle lobes
from the inferior lobe. The left major fissure (middle CT image) separates the left upper and
lower lobes. These fissures are easy to see because this patient suffers significant pleural
effusions that fill the pleural space and partially separates the lobes.
Week 6 - Abdomen: CT & Sectional Anatomy
Italics are not part of objectives, but can help with understanding
Hounsfield Units: Relates attenuation coefficients of tissue to that of water. Low
attenuation (negative) blocks only a few exrays
o Air =-1000
o Fat =-50
o Water =0
o Tissue =40
o Calcium =100
o Bone =1000
Metals can cause artifacts
Use CT J udiciously especially in the youth
1. Know when to order a CT scan of the abdomen
a. CT is very usefull in the imaging of Cancer, Trauma, Vascular pathology, and
Abdominal Symptoms
b. Intraabdominal fluid is a marker of pathology.
2. Be able to determine when to use contrast and when to order a non-Con Abdominal
CT
a. Oral and IV Contrast (IV is Iodine based)
i. Water soluble Oral contrast if you suspect Perforation.
ii. IV Contrast helps with vasculature, Viscera and distinguishes cystic from
solid.
b. Risk for IV Contrast
i. Allergy (Pretreat with steroids)
ii. Renal insufficiency (Creatinine >2.0
c. No Contrast for Head Trauma and Renal Stones
3. Know how to diagnose the following conditions with an Abdominal CT
a. Kidney stones
i. History of Flank Pain
ii. (Left Ureteral Stone on image on the right)
b. Appendicitis
i. Worm like structure inferior to the cecum
ii. To find it, Find the ascending colon @ iliac crests and scroll down until
you reach the inferior cecum and find the worm.
c. Diverticulitis
i. Wall thickening and edema in the fat adjacent to the sigmoid colon (LLQ)
d. Abdominal aortic Aneurysm
i. Pt typically has hypotension and distended abdomen.
Week 7 - Neuroradiology: CT scan
(1) How are skull fractures characterized on a head CT (linear vs. depressed)
Linear: transverse full thickness of bone w/o being displaced downward
Depressed: comminuted fracture where bone is depressed inward, inc. pressure on brain
A skull fracture is most clinically significant if the paranasal sinus or skull base is involved.
- Distinguished from sutures
- Sutures have undulating margins both sutures
Linear skull fractures
This is the most common type of skull fracture. In a linear fracture, there is a break in the bone,
but it does not move the bone. These patients may be observed in the hospital for a brief amount
of time, and can usually resume normal activities in a few days. Usually, no interventions are
necessary.
Depressed skull fractures
This type of fracture may be seen with or without a cut in the scalp. In this fracture, part of the
skull is actually sunken in from the trauma. This type of skull fracture may require surgical
intervention, depending on the severity, to help correct the deformity.
Diastatic skull fractures
These are fractures that occur along the suture lines in the skull. The sutures are the areas
between the bones in the head that fuse when we are children. In this type of fracture, the normal
suture lines are widened. These fractures are more often seen in newborns and older infants.
Basilar skull fracture
This is the most serious type of skull fracture, and involves a break in the bone at the base of the
skull. Patients with this type of fracture frequently have bruises around their eyes and a bruise
behind their ear. They may also have clear fluid draining from their nose or ears due to a tear in
part of the covering of the brain. These patients usually require close observation in the hospital.
Intracranial hematoma (ICH)
There are several types of ICH, or blood clots, in or around the brain. The different types are
classified by their location in the brain. These can range from mild head injuries to quite serious
and potentially life-threatening injuries.
(2) Understand the most common clinical scenarios:
- Subdural, Subarachnoid, Intracerebral and Epidural Bleeds
- Subdural: rupture of bridging vein, usu. Due to deceleration and acceleration, or rotational
forces (atrophy predisposes, so common in elderly who fall)
- blood collects between arachnoid and dura matter, cant cross falx, tentorium
CT- Crescent shaped that crosses suture lines.
May contain hypodense foci due to serum, CSF or active bleeding (pic on right)
Subarachnoid:
- injury of small arteries or veins on the surface of the brain
- bleeds into space between pia and arachnoid matta
- Trauma is most common cause
- also due to rupture aneurysm
- worst H/A of life
- CT: Focal high density in sulci and fissures or linear hyperdensity in the cerebral sulci
Epidural Bleeds
-Usually associated with a skull fracture
-Lacerates a dural artery or a venous sinus (middle meningeal artery)
-The blood collects between the skull and dura
-On CT, a hyperdense biconvex mass
-Can cross the dural reflections unlike a subdural hematoma
-Usually does not cross suture lines where the dura tightly adheres to the adjacent skull
Intracerebral
The most common cause of non-traumatic intracerebral hematoma: hypertensive hemorrhage
Other causes include: Amyloid angiopathy
Ruptured vascular malformation
Coagulopathy
Hemorrhage into a tumor
Venous infarction
Drug abuse
Epidural hematoma
Epidural hematomas occur when a blood clot forms underneath the skull, but on top of
the dura, the tough covering that surrounds the brain. They usually come from a tear in an
artery that runs just under the skull called the middle meningeal artery. Epidural
hematomas are usually associated with a skull fracture.
Subdural hematoma
Subdural hematomas occur when a blood clot forms underneath the skull and underneath
the dura, but outside of the brain. These can form from a tear in the veins that go from the
brain to the dura, or from a cut on the brain itself. They are sometimes, but not always,
associated with a skull fracture.
Contusion or intracerebral hematoma
A contusion is a bruise to the brain itself. A contusion causes bleeding and swelling
inside of the brain around the area where the head was struck. Contusions may occur with
skull fractures or other blood clots such as a subdural or epidural hematoma. When
bleeding occurs inside the brain itself (also called "intraparenchymal hemmorage"), this
can sometimes occur spontaneously. When trauma is not the cause, the most common
causes are long-standing high blood pressure in older adults, bleeding disorders in either
children or adults, or the use of medications that cause blood thinning or certain drugs of
abuse.
Diffuse axonal injury (DAI)
These injuries are fairly common and are usually caused by shaking of the brain back and
forth, which can happen in car accidents, from falls or shaken baby syndrome. Diffuse
injuries can be mild, such as with a concussion, or may be very severe, as in diffuse
axonal injury (DAI). In DAI, the patient is usually in a coma for a prolonged period of
time, with injury to many different parts of the brain.
(3) Understand the most common cause of non-traumatic intracerebral bleeds
Hemorrhagic stroke, due to hypertensive hemorrhage
- 70-90% of non-traumatic primary intracerebral hemorrhages.
- Vasculopathy involving deep penetrating arteries of the brain.
- Thalamus, pons, cerebellum, and basal ganglia
Blood may extend into the ventricular system Associated with a poor prognosis
(4) Be familiar with the appearance of the following on a CT scan of the Head:
- Epidural Bleed
- Subdural Bleed
- Subarachnoid Bleed
- Intracerebral Bleed
- Hydrocephalus
- Skull Fracture
Hydrocephalus
- A problem with the ratio of production of CSF to its reabsorption
- Communicating hydrocephalus is the most common and is due to arachnoid villi and
subarachnoid space obstruction.
- Obstructive hydrocephalus is less common but may occur as a result of the following:
aqueductal stenosis or occlusion; trapped 4
th
ventricle; ependymitis
Hydrocephalus Normal
Normal (top) Hydrocephaus (bottom)
Week 8 - Interventional Radiology (FYI only)
1. Identify indications for common interventional radiology procedures
2. Introduce the student to the concepts of Interventional Radiology
Discuss various clinical conditions and integrate interventional radiographic procedures as it
applies to the clinical concepts
Das könnte Ihnen auch gefallen
- Etiology, Diagnosis, and Treatment of Primary AmenorrheaDokument19 SeitenEtiology, Diagnosis, and Treatment of Primary Amenorrheamrlucky09855Noch keine Bewertungen
- Family Medicine Clerkship Curriculum GuideDokument18 SeitenFamily Medicine Clerkship Curriculum Guidejb cookiesNoch keine Bewertungen
- OBDokument14 SeitenOBmrlucky09855Noch keine Bewertungen
- Key Pharm AssociationsDokument9 SeitenKey Pharm Associationsmrlucky09855Noch keine Bewertungen
- PCL ApplicationDokument11 SeitenPCL Applicationmrlucky09855Noch keine Bewertungen
- SurgeryDokument11 SeitenSurgerymrlucky09855Noch keine Bewertungen
- DiverticulosisDokument28 SeitenDiverticulosismrlucky09855Noch keine Bewertungen
- SPB CrimDokument19 SeitenSPB Crimmrlucky09855Noch keine Bewertungen
- ReadmeankiDokument1 SeiteReadmeankimrlucky09855Noch keine Bewertungen
- Bioremediation Boosts Diesel Cleanup in Suisun MarshDokument27 SeitenBioremediation Boosts Diesel Cleanup in Suisun Marshmrlucky09855Noch keine Bewertungen
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5783)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (119)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- Pfizer Adverse Event Report - Godspeed Everyone, GDokument22 SeitenPfizer Adverse Event Report - Godspeed Everyone, GChristopher CavallaroNoch keine Bewertungen
- MedFit Form (JAL)Dokument4 SeitenMedFit Form (JAL)FrancescoBarberoNoch keine Bewertungen
- N A S S: Modified Finnegan Neonatal Abstinence Score SheetDokument4 SeitenN A S S: Modified Finnegan Neonatal Abstinence Score SheetBob100% (1)
- Practical nursing jeopardy game questions and answersDokument29 SeitenPractical nursing jeopardy game questions and answersfairwoods80% (5)
- Frogdissectionpre LabDokument2 SeitenFrogdissectionpre Labapi-347112479Noch keine Bewertungen
- DLCO Vs KCODokument11 SeitenDLCO Vs KCOwongNoch keine Bewertungen
- Chama 13 MI SPIE Poster - Automated Lung Field Segmentation in CT Images Using Mean Shift Clustering and Geometrical FeaturesDokument1 SeiteChama 13 MI SPIE Poster - Automated Lung Field Segmentation in CT Images Using Mean Shift Clustering and Geometrical FeaturesChanukya Krishna ChamaNoch keine Bewertungen
- Science Class 7Dokument217 SeitenScience Class 7hafiza arishaNoch keine Bewertungen
- Human Anatomy and Body SystemsDokument28 SeitenHuman Anatomy and Body SystemsHolly May MontejoNoch keine Bewertungen
- NFSC 471-Case StudyDokument8 SeitenNFSC 471-Case Studyapi-242439244Noch keine Bewertungen
- Mine Rescue and Recovery WorkDokument48 SeitenMine Rescue and Recovery WorkPramod Kumar MaheshwariNoch keine Bewertungen
- BabyGym 1 Part 1 and PostersDokument18 SeitenBabyGym 1 Part 1 and PostersJavierNoch keine Bewertungen
- Presented By: Pramod Kumar MSC 1 Year RakconDokument37 SeitenPresented By: Pramod Kumar MSC 1 Year Rakconpramod kumawatNoch keine Bewertungen
- Lung Structure - BioNinjaDokument2 SeitenLung Structure - BioNinjaDaniel WalshNoch keine Bewertungen
- NCM 112 Lec 1 Sir Arnel Respiratory System: Basic Gas-Exchange Unit of The RespiratoryDokument5 SeitenNCM 112 Lec 1 Sir Arnel Respiratory System: Basic Gas-Exchange Unit of The RespiratoryJane BautistaNoch keine Bewertungen
- Antitussives and MucolyticsDokument1 SeiteAntitussives and MucolyticsArvin Bernardo QuejadaNoch keine Bewertungen
- Respiratory System ExplainedDokument5 SeitenRespiratory System ExplainedCynthia MelindaNoch keine Bewertungen
- Capnography - Self Study - GuideDokument22 SeitenCapnography - Self Study - GuideSuresh KumarNoch keine Bewertungen
- BreathingDokument5 SeitenBreathingvictory IsaacNoch keine Bewertungen
- Respiratory SystemDokument9 SeitenRespiratory SystemAtif JavaidNoch keine Bewertungen
- PneumoniaDokument48 SeitenPneumoniaSiti FatimahNoch keine Bewertungen
- Pretest New 2021 2022 Science 9Dokument4 SeitenPretest New 2021 2022 Science 9Aina jenine P ClaveriaNoch keine Bewertungen
- PsychiaDokument12 SeitenPsychiaLloyd Rafael EstabilloNoch keine Bewertungen
- Classification of Living OrganismsDokument37 SeitenClassification of Living OrganismsSweeetMimiNoch keine Bewertungen
- Pulmonary Edema Vs Pneumonia OrderDokument25 SeitenPulmonary Edema Vs Pneumonia OrderRizqon RohmatussadeliNoch keine Bewertungen
- Compre AnaphyDokument50 SeitenCompre AnaphyGEMMALYN BANGAYANNoch keine Bewertungen
- Respiratory Acidosis and Alkalosis ObjectivesDokument12 SeitenRespiratory Acidosis and Alkalosis Objectivesyayastoyz100% (1)
- DLL Science 9Dokument3 SeitenDLL Science 9RENE BOY VENTURILLONoch keine Bewertungen
- Assessment of The Chest and Lungs HandoutDokument2 SeitenAssessment of The Chest and Lungs Handoutkaren solibaNoch keine Bewertungen
- Grade 9 Science Respiratory System QuizDokument2 SeitenGrade 9 Science Respiratory System QuizBello Nelson67% (3)