Beruflich Dokumente
Kultur Dokumente
Repair of A Large Defect of The Upper Lip
Hochgeladen von
doctorban0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
48 Ansichten4 Seitenrepair
Originaltitel
Repair of a Large Defect of the Upper Lip
Copyright
© © All Rights Reserved
Verfügbare Formate
PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenrepair
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
48 Ansichten4 SeitenRepair of A Large Defect of The Upper Lip
Hochgeladen von
doctorbanrepair
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 4
RECONSTRUCTIVE CONUNDRUM
Repair of a Large Defect of the Upper Lip
PEDRO REDONDO, MD, PHD*
The author has indicated no signicant interest with commercial supporters.
A
77-year-old man with a history of nonmel-
anoma skin cancers of the forehead presented
for treatment of recurrent basal cell carcinoma of the
upper lip. The lesion had been operated on three
times previously and presented as a pathologic
induration upon palpation that affected the full
thickness of the lip.
Under local anesthesia, a pentagonal resection of the
lesion was performed with 0.5-cm lateral margins
and extending in depth as far as the submucosa. The
upper margin of the excision coincided with the ala
nasi and the lower margin with the vermilion. The
rst defect of skin and muscle was geometric,
measured 3 by 4 cm, and involved nearly one entire
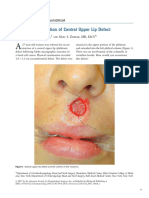
side of the upper lip (Figure 1). After the rst stage
of Mohs surgery, a positive margin was observed in
contact with submucosa of the bed, which meant
that a small en bloc excision had to be performed.
The patient requested a single-stage procedure for
the repair. How would you reconstruct this upper lip
defect?
Figure 1. Defect after Mohs excision with the planned ap marked.
*Department of Dermatology, University Clinic of Navarra, Pamplona, Spain
2013 by the American Society for Dermatologic Surgery, Inc. Published by Wiley Periodicals, Inc.
ISSN: 1076-0512 Dermatol Surg 2014;40:576579 DOI: 10.1111/dsu.12393
576
Reconstruction Options
The principles of an ideal upper lip reconstruction
include restoration of dynamic motion, sensation,
oral sphincter competence, and minimization of
distortion and disgurement. The distortion or
ablation of the melolabial fold and movement of
glabrous skin into the moustache area must be
avoided.
Reconstructive techniques of the upper lip include
simple closure along relaxed skin tension lines,
V-shaped excision, full-thickness skin grafting, sec-
ondary-intention healing, and tissue rearrangement.
If the defect is less than one-third of the upper lip, it
can usually be reconstructed by removing a V-
shaped wedge from the lip and closing the lip
primarily. Several options for closure of large
defects in this area exist, including melolabial
transposition ap, cheek advancement ap, and
tunnelled subcutaneous pedicle transposition ap.
The Procedure
The island pedicle ap is an excellent option for
closure of large and deep defects on the upper
cutaneous lip.
14
The reconstruction places incisions
at the junction of cosmetic units and uses an island
pedicle ap to replace resected tissue with similar
tissue, restoring the melolabial fold without
distorting surrounding functional and aesthetic
structures. This technique is cosmetically and func-
tionally successful, and the symmetry of the oral
commissure is maintained.
After tumor removal, the mobility of the surround-
ing tissue was determined. The closure lines were
planned so that they were located in the junctions of
cosmetic units without crossing the junctions. The
island pedicle ap has two lateral curvilinear inci-
sions tangential to the defect superiorly along the
melolabial fold and inferiorly along the vermilion
(Figure 1). The island ap is based on subcutaneous
fat lateral to orbicularis oris. The ap was under-
mined at the upper level of the subcutaneous fat,
mobilized and advanced medially, and gently pulled
into place with a hook.
A positive margin in contact with the submucosa of
the bed was observed after the rst stage of Mohs
surgery. As a result, we decided to excise the affected
area en bloc, including it in a small V-shaped
excision 1.5 cm wide (Figure 2). Lateral margins
were removed with margin control. This procedure
has the added advantage of making closure easier by
slightly reducing the necessary displacement of the
subcutaneous island pedicle advancement-ap.
The V-shaped excision was designed in such a way
that it extended over the complete height of the lip
from the vermilion to the base of the nose. A 30
chromic stitch was used to close the upper portion of
oral mucosa. The most important stitch was the
placement of a 60 silk stitch to align the vermilion
cutaneous junction (Figure 3).
The area around the secondary defect, from which
the ap was taken, was extensively undermined to
allow for appropriate mobility of the ap.
5
Once
sufcient mobility of the ap was achieved, the
anchoring stitch was placed. A small Burows
triangle superior to the lip defect was marked for
excision to enlarge the defect so that the border of
Figure 2. Final defect after V-shaped excision. The en bloc
excision was performed after the island pedicle ap was
incised.
REDONDO
40: 5: MAY 2014 577
the ap coincided with the ala nasi. Enlarging the
defect to facilitate positioning the border of the
island ap along an aesthetic boundary provided
maximum scar camouage. An absorbable 40
suture was used, avoiding vascular compromise of
the ap. Skin edges were approximated using 60
silk sutures. The ap donor site was closed in a V-Y
fashion (Figure 4). The patient was evaluated
4 months after the operation (Figure 5).
Discussion
Upper lip defects that are less than one-fourth of the
upper lip length can be closed directly. Primary
closure of larger defects often leads to asymmetry or
whistling deformity. The alar crescent advancement
ap technique has been widely used for repair of large
central (for varying-length partial- and full-thickness)
defects of the upper lip and base of the nose. This ap
can be conceptualized as a procedure that entails
removal of Burows triangles, followed by a cheek
advancement ap. Large central defects that involve
30% to 60% of the original width of the lip can be
reconstructed with transposition aps (AbbeEst-
lander ap) involving the use of lower lip tissue.
Defects more than two-thirds of the central upper lip
are best treated with rotation advancement aps that
recruit tissues from the lip and cheek regions.
Our patient lost the full thickness of the lip,
including the skin and muscle over almost half the
length of the lip. Vertical side-to-side closure or
wedge resection was not chosen owing to the length
of the defect, although a minimum V-shaped resec-
tion, which was necessary given local involvement,
aided nal closure. Melolabial subcutaneous tissue
island pedicle advancement aps have an excellent
blood supply, maintain the anatomy of the melola-
Figure 3. Suture of V-shaped excision and aligning the
vermilion junction.
Figure 4. Immediate postoperative result. The island pedi-
cle ap sutured in place after advancement.
Figure 5. The lip 4 months after surgery. Good aesthetic
and functional resultd. Only the median vertical scar of the
upper lip is still visible.
DEFECT OF THE UPPER LI P
DERMATOLOGI C SURGERY 578
bial fold, and do not disrupt follicular integrity,
allowing men to retain growth of moustache hair.
4
One potential complication of island pedicle ap is
trapdoor deformity. In this case, because we used the
ap for a deep defect that extended to the orbicularis
muscle, no thinning of the ap was necessary, and
this side effect was avoided. In the case of defects
that do not encompass the greater part of the upper
lip, surrounding tissue may be removed to the edges
of this cosmetic subunit to hide scars in the
melolabial crease and vermilion.
Conundrum Keys
Several goals must be considered in the reconstruc-
tive surgery of the upper lip:
(1) Try to hide the scars in the natural creases and
cosmetic units, particularly in the melolabial
groove and vermilion.
(2) Reconstruction with advancement island pedicle
ap preserves cosmetic boundaries and uses
similar, nonglabrous skin to preserve facial
hair in men.
(3) The key to achieving this degree of mobility is
extensive undermining in the subdermal plane in
the tissue surrounding the ap. The underlying
central vascular pedicle must be at least one-
third of the total surface area of the ap for the
overlying ap to remain viable.
(4) This simple and straightforward technique is a
single-stage procedure and provides good func-
tional and aesthetic results.
References
1. Li JH, Xing X, Liu HY, Li P, et al. Subcutaneous island pedicle
ap: variations and versatility for facial reconstruction. Ann Plast
Surg 2006;57:2559.
2. Tomich JM, Wentzell JM, Grande DJ. Subcutaneous island pedicle
laps. Arch Dermatol 1987;123:5148.
3. Dzubow LM. Subcutaneous island pedicle aps. J Dermatol Surg
Oncol 1986;12:5916.
4. Ray TL, Weinberger CH, Lee PK. Closure of large defects on the
cutaneous upper lip using an island pedicle ap. Dermatol Surg
2010;36:9314.
5. Chan STS. A technique of undermining a V-Y subcutaneous island
ap to maximize advancement. Br J Plast Surg 1988;41:627.
Address correspondence and reprint requests to: Pedro
Redondo, MD, PhD, Department of Dermatology,
University Clinic of Navarra, 31080 Pamplona, Spain, or
e-mail: predondo@unav.es
REDONDO
40: 5: MAY 2014 579
Das könnte Ihnen auch gefallen
- Lip Reconstruction: Learning ObjectivesDokument8 SeitenLip Reconstruction: Learning Objectivesalinutza_childNoch keine Bewertungen
- 2007 O To Z Reconstruction of Central Upper Lip DefectDokument5 Seiten2007 O To Z Reconstruction of Central Upper Lip DefectDimitris RodriguezNoch keine Bewertungen
- Surgical Incisions Balancing Surgical and Cosmetic Outcomes in Head and Neck OncosurgeryDokument4 SeitenSurgical Incisions Balancing Surgical and Cosmetic Outcomes in Head and Neck OncosurgeryDwarika Prasad BajgaiNoch keine Bewertungen
- 2010 Facial Degloving Approach To The MidfaceDokument4 Seiten2010 Facial Degloving Approach To The MidfaceAFJimenezONoch keine Bewertungen
- 10-16-02 Cleft Lip and Palate Part 2 TEKNIKDokument93 Seiten10-16-02 Cleft Lip and Palate Part 2 TEKNIKSulistyawati WrimunNoch keine Bewertungen
- Head and Neck Cancer - Reconstruction: HistoryDokument6 SeitenHead and Neck Cancer - Reconstruction: HistorySri MahyantiNoch keine Bewertungen
- Aesthetic Lip SplitsDokument4 SeitenAesthetic Lip Splitsrajtanniru100% (1)
- JC TopicDokument6 SeitenJC Topicवाधूलं कण्णन् कुमारस्वामिNoch keine Bewertungen
- MandibulectomiaDokument8 SeitenMandibulectomiaCarlos Eduardo BordaNoch keine Bewertungen
- One Stage Aesthetic and Functional Reconstruction of Major Lower Lip DefectsDokument5 SeitenOne Stage Aesthetic and Functional Reconstruction of Major Lower Lip DefectsDr. Hilder HernandezNoch keine Bewertungen
- Bilateral Cleft Lip and Whistling Deformity The X.43Dokument6 SeitenBilateral Cleft Lip and Whistling Deformity The X.43rupak979Noch keine Bewertungen
- Primary Bilateral Cleft Lip/Nose Repair Using A Modified Millard TechniqueDokument8 SeitenPrimary Bilateral Cleft Lip/Nose Repair Using A Modified Millard TechniqueJorge Antonio Espinoza YañezNoch keine Bewertungen
- Modified FAMMDokument4 SeitenModified FAMMSilverline TeamNoch keine Bewertungen
- Nasal Reconstruction 1Dokument11 SeitenNasal Reconstruction 1geoffrowley3Noch keine Bewertungen
- Cheek FlapDokument4 SeitenCheek FlapDae AhmadNoch keine Bewertungen
- Reconstruction of Intraoral Defects Using Facial Artery Musculomucosal FlapDokument6 SeitenReconstruction of Intraoral Defects Using Facial Artery Musculomucosal FlapRajan KarmakarNoch keine Bewertungen
- The Use of A Cutaneous Muscular Flap For Primary Naso Labial Repair With A Modified Tennison Randal TechniqueDokument4 SeitenThe Use of A Cutaneous Muscular Flap For Primary Naso Labial Repair With A Modified Tennison Randal TechniqueShaly MaduroNoch keine Bewertungen
- Skinflaps: Mary Tschoi,, Erik A. Hoy,, Mark S. GranickDokument16 SeitenSkinflaps: Mary Tschoi,, Erik A. Hoy,, Mark S. Granickdanico59Noch keine Bewertungen
- Lindsay 2010Dokument2 SeitenLindsay 2010Stelescu AndrasNoch keine Bewertungen
- 4 Oral Cavity ProceduresDokument10 Seiten4 Oral Cavity ProceduresAnne MarieNoch keine Bewertungen
- пожтяжка губ 4Dokument6 Seitenпожтяжка губ 4Alexey SorokinNoch keine Bewertungen
- Reconstruction of Defects of The Posterior Pinna.15Dokument4 SeitenReconstruction of Defects of The Posterior Pinna.15cliffwinskyNoch keine Bewertungen
- 15 JMSH 63 12Dokument4 Seiten15 JMSH 63 12shamsshanti999Noch keine Bewertungen
- An Alternative Alar Cinch Suture PDFDokument11 SeitenAn Alternative Alar Cinch Suture PDFmatias112Noch keine Bewertungen
- 38 Lip Reconstruction: Babak J.Mehrara, M.D., and Barry M.Zide, M.D., D.M.DDokument15 Seiten38 Lip Reconstruction: Babak J.Mehrara, M.D., and Barry M.Zide, M.D., D.M.Dandre andreNoch keine Bewertungen
- Use of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFDokument9 SeitenUse of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFJose Luis Granados SolerNoch keine Bewertungen
- Revision of An Upper Lip Scar Following - 2022 - Advances in Oral and MaxillofacDokument2 SeitenRevision of An Upper Lip Scar Following - 2022 - Advances in Oral and MaxillofacГне ДзжNoch keine Bewertungen
- The Early Secondary GingivoperiosteoplastyDokument11 SeitenThe Early Secondary GingivoperiosteoplastyAndrés Faúndez TeránNoch keine Bewertungen
- Gox 5 E1230Dokument6 SeitenGox 5 E1230Brînduşa CiobanuNoch keine Bewertungen
- Reconstruccion Parpado InferiorDokument6 SeitenReconstruccion Parpado InferiorLeonardCarreraDiazNoch keine Bewertungen
- Ann Burns and Fire Disasters 22 90Dokument7 SeitenAnn Burns and Fire Disasters 22 90alinutza_childNoch keine Bewertungen
- Secondary Deofrmities of Cleft Lip NoseDokument8 SeitenSecondary Deofrmities of Cleft Lip NoseahmedatefNoch keine Bewertungen
- Acquired Maxillary DefectsDokument19 SeitenAcquired Maxillary DefectstamersarwtsaadNoch keine Bewertungen
- Reconstrucción Defectos Nasales PDFDokument18 SeitenReconstrucción Defectos Nasales PDFSara OmNoch keine Bewertungen
- Zhao 2020Dokument2 SeitenZhao 2020miraraspopovic020Noch keine Bewertungen
- Lip Lowering SurgeryDokument15 SeitenLip Lowering SurgeryPrathik RaiNoch keine Bewertungen
- Facial ReconstructionDokument77 SeitenFacial ReconstructionDr-Mohammad Ali-Fayiz Al TamimiNoch keine Bewertungen
- The Bozola Flap in Oral Cavity Reconstruction PDFDokument4 SeitenThe Bozola Flap in Oral Cavity Reconstruction PDFPorcupine TreeNoch keine Bewertungen
- Simultaneous Reconstruction of The Secondary Bilateral Cleft Lip and Nasal Deformity: Abbé Flap RevisitedDokument9 SeitenSimultaneous Reconstruction of The Secondary Bilateral Cleft Lip and Nasal Deformity: Abbé Flap RevisitedwulanbrurrNoch keine Bewertungen
- BMS Flap ArticleDokument5 SeitenBMS Flap ArticleCynthia MelindaNoch keine Bewertungen
- 1 s2.0 S2667147622000103 MainDokument5 Seiten1 s2.0 S2667147622000103 MainWayan Sutresna YasaNoch keine Bewertungen
- Use of Retroauricular Temporal Flap For Large Post Oncosurgical Glabellar and Forehead DefectsDokument4 SeitenUse of Retroauricular Temporal Flap For Large Post Oncosurgical Glabellar and Forehead DefectsPalwasha Malik100% (1)
- Cleft 3Dokument6 SeitenCleft 3ASJADI SHEIKHNoch keine Bewertungen
- Ø Ø Ù - Ù - Ù - Ø Ù - Ø Ù - Ù - AlveolplastyDokument26 SeitenØ Ø Ù - Ù - Ù - Ø Ù - Ø Ù - Ù - AlveolplastyTasneem AbdNoch keine Bewertungen
- Treatment NASALDokument7 SeitenTreatment NASALRezaNoch keine Bewertungen
- Abbé - EstlanderDokument4 SeitenAbbé - EstlanderKoretta Esmeral AtehortúaNoch keine Bewertungen
- Modified Pontic Design For Ridge DefectsDokument11 SeitenModified Pontic Design For Ridge DefectsFaheemuddin MuhammadNoch keine Bewertungen
- Lip Nose DeformityDokument3 SeitenLip Nose DeformityBulfendri DoniNoch keine Bewertungen
- Nasal ReconstructionDokument14 SeitenNasal ReconstructionNovia Chrisnawati100% (1)
- Lip Reconstruction: Donald Baumann, M.D., and Geoffrey Robb, M.DDokument12 SeitenLip Reconstruction: Donald Baumann, M.D., and Geoffrey Robb, M.DBenedetta GuarinoNoch keine Bewertungen
- 10 16 02CleftLipandPalatePart2 PDFDokument93 Seiten10 16 02CleftLipandPalatePart2 PDFalinutza_childNoch keine Bewertungen
- Maxillectomy A ReviewDokument17 SeitenMaxillectomy A ReviewDr. T. Balasubramanian100% (3)
- Buccal Fat Pad ExtrusionDokument4 SeitenBuccal Fat Pad ExtrusionQuang BuiNoch keine Bewertungen
- Surgical Options in Oroantral Fistula TreatmentDokument5 SeitenSurgical Options in Oroantral Fistula TreatmentmartarayaniNoch keine Bewertungen
- Triangular Frenotomy A Novel Technique For Gummy Smile CorrectionDokument4 SeitenTriangular Frenotomy A Novel Technique For Gummy Smile CorrectionRAKERNAS PDGI XINoch keine Bewertungen
- Rhinoplasty WorkbookDokument21 SeitenRhinoplasty Workbookzena talibNoch keine Bewertungen
- Modified Rhomboid Flap For Facial ReconstructionDokument3 SeitenModified Rhomboid Flap For Facial ReconstructionahujasurajNoch keine Bewertungen
- Primary Cleft Lip and Palate Amit PapnejaDokument5 SeitenPrimary Cleft Lip and Palate Amit PapnejaAmit PapnejaNoch keine Bewertungen
- Nasal Septal PerforationDokument13 SeitenNasal Septal PerforationDr. T. Balasubramanian75% (4)
- Microfat Grafting in Nasal SurgeryDokument17 SeitenMicrofat Grafting in Nasal SurgerydoctorbanNoch keine Bewertungen
- Scar Treatment Variations by Skin TypeReview ArticleDokument10 SeitenScar Treatment Variations by Skin TypeReview ArticledoctorbanNoch keine Bewertungen
- Laser Skin Treatment in Non-Caucasian PatientsReview ArticleDokument8 SeitenLaser Skin Treatment in Non-Caucasian PatientsReview ArticledoctorbanNoch keine Bewertungen
- Scar Treatment Variations by Skin TypeReview ArticleDokument10 SeitenScar Treatment Variations by Skin TypeReview ArticledoctorbanNoch keine Bewertungen
- Aging BlepharoplastyDokument6 SeitenAging BlepharoplastydrbantmNoch keine Bewertungen
- Overlooked Complication ofDokument9 SeitenOverlooked Complication ofdoctorbanNoch keine Bewertungen
- The Open Brow LiftDokument8 SeitenThe Open Brow LiftdoctorbanNoch keine Bewertungen
- Laser-Assisted Patient Positioning A Straightforward Method To Ensure Consistent Head and Neck Aesthetic Photographs 8)Dokument3 SeitenLaser-Assisted Patient Positioning A Straightforward Method To Ensure Consistent Head and Neck Aesthetic Photographs 8)doctorbanNoch keine Bewertungen
- Non-Invasive, External Ultrasonic LipolysisDokument5 SeitenNon-Invasive, External Ultrasonic LipolysisdoctorbanNoch keine Bewertungen