Beruflich Dokumente
Kultur Dokumente
Case Study - Emphysema
Hochgeladen von
mackie_0419920 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
1K Ansichten6 Seitenknow more about emphysema
Originaltitel
Case Study- Emphysema
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenknow more about emphysema
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
1K Ansichten6 SeitenCase Study - Emphysema
Hochgeladen von
mackie_041992know more about emphysema
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 6
Saint Marys University
Bayombong, Nueva Vizcaya
Graduate School
In Partial Fulfillment of the Requirements in
Master of Science in Nursing- Adult Health Nursing 201
CASE STUDY: EMPHYSEMA
Submitted to:
Mrs. Hazel M. Valmores, RN, MSN, USRN
Instructor
Submitted by:
Mark Anthony T. Tabago, RN
1. Explain the pathophysiology of emphysema.
(See separate page for pathophysiology)
2. Are D.Z.s VS and Sa0
2
appropriate? If not, explain why?
Yes D.Z.s vital signs and oxygen saturation are appropriate to the
situation because he is in acute exacerbation meaning his condition gets worse;
thus, he will manifest tachypnea and tachycardia as compensatory mechanism;
and the oxygen saturation will be low. In the data, D.Z.s respiratory rate is 36
cpm, pulse rate is 124 bpm and oxygen saturation of 88%.
3. Identify three (3) nursing measures you could try to improve oxygenation.
The following are nursing interventions to improve oxygenation:
Place patient in Orthopneic position or high Fowlers position to maximize
lung expansion and to reduce respiratory effort
Teach effective breathing patterns such as pursed-lip breathing and
diaphragmatic breathing to improve ventilation in the alveoli by maintaining
intrathoracic pressure at the end of exhalation
Encourage patient to cough or huff every 1 to 2 hours, drink 10 glasses of
fluid a day if not contraindicated, and humidify inspired air to improve airway
clearance and remove mucus from airways allowing better ventilation
Administer supplementary oxygen at 2 Lpm to improve oxygenation/ tissue
perfusion
4. Explain the main purpose of the following classes of drugs: antibiotics,
bronchodilators, and corticosteroids.
Antibiotics are given to treat infections as most exacerbations are triggered by
bacterial infections; Antibiotics may be used to help fight respiratory infections
common in people with emphysema, such as acute bronchitis, pneumonia
and the flu
Bronchodilators are given to improve airflow; Bronchodilator medications may
help to relieve symptoms of emphysema by relaxing and opening the air
passages in the lungs
Corticosteroids are given to decrease inflammation if bronchodilators are not
sufficient; Corticosteroids can help relieve symptoms of emphysema
associated with asthma and bronchitis
5. What are the two most common side effects of bronchodilators?
Patients who have COPD are often prescribed medications called
bronchodilators. Bronchodilators work by relaxing and expanding the smooth
muscle of the airways making it easier to breath. Three types of bronchodilators
are commonly used for the treatment of emphysema: beta adrenergic agonists,
anticholinergics, and methylxanthines.
Common side effects of beta adrenergic agonists includes
Tachycardia
Palpitations
Premature ventricular contractions
Tremors
Hypokalemia
Common side effects of anticholinergics are
Dry mouth
Metallic taste
Common side effects of methylxanthines includes
Heart dysrhythmias
Convulsions
6. You deliver D.Z.s dietary tray, and he commends how hungry he is. As you
leave the room, he is rapidly consuming the mashed potatoes. When you
pick up the tray, you noticed that he hasnt touched anything else. When
you question him, he states, I dont understand it. I can be so hungry but
when I start to eat, I have trouble breathing and I have to stop. Explain this
phenomenon based on your knowledge of breakdown of carbohydrates
(CHO).
Carbohydrates tend to produce more carbon dioxide when broken down
which forces the lungs to work harder to expel the gas from our bodies. This
explains why D.Z. experience difficulty breathing when eating.
An important nutritional objective is to reduce the amount of carbon
dioxide being produced by the body. Carbohydrate is the macronutrient that
increases RQ (respiratory quotient) which is a measure of the ratio of the volume
of CO2 expired to the volume of oxygen consumed. By decreasing carbohydrate
in the diet, we are effectively decreasing the amount of CO2 produced, thereby
decreasing the burden of expiration on the patient. This also helps to decrease
respiratory infections and acidosis associated with emphysema. Therefore, the
prescribed diet is high in fat (as much as 55%) and protein and low in
carbohydrate.
7. Identify four (4) strategies that might improve his caloric intake
The following are strategies that improve caloric intake:
Eat meals when energy levels are at their highest, which is usually in the morning
Eat several small, nutrient-rich meals to avoid becoming breathless while eating
Eat slowly and chew foods thoroughly to avoid swallowing air while eating
Choose foods that are easy to chew. Modify food consistency if mastication
seems to increase fatigue while eating
Choose foods that are easy to prepare to conserve energy for eating
Limit salt. Consuming too much can cause the body to retain water and can
make breathing more difficult
Eat calcium- and vitamin D-rich foods to support bone health
Prepare meals that appear palatable and well presented
Avoid foods that cause gas or bloating. A full abdomen can make breathing
uncomfortable
Eat while sitting up to ease lung pressure
Drink liquids at the end of the meal to avoid feeling full while eating
Wear a cannula while eating if continuous oxygen is prescribed. Eating and
digestion require oxygen, so the body will need the extra oxygen
Limit caffeinated beverages, as caffeine can interfere with some medications and
cause nervousness or restlessness
Make the meal more enjoyable by engaging in social interaction while dining
Avoid aspiration by breathing carefully, swallowing, and sitting properly and with
good posture while eating
Rest before meals
8. Identify three (3) expected outcomes of D.Z.s treatment.
D.Z. will maintain patent airway as evidenced by decreased wheezes, decreased
tachypnea, decreased dyspnea, and arterial blood gas (ABG) within normal limit
D.Z.s breathing pattern will improve as evidenced by respiratory rate within
normal limit
D.Z. will demonstrate behavior/lifestyle changes to regain and/or maintain
appropriate weight as evidenced by increased in weight of 1 kg per week
9. You answer D.Z.s call light, and he asks for a carton of milk. You remind
him that milk causes an increased production of thick mucus. He replies
Yes, but you told me that I need lots of protein. How should you
respond?
If I were in that scenario, I would tell to D.Z. that there are other food
sources that are rich in protein aside from milk that he can take in because milk
increases mucus production thus, worsens his condition- provokes difficulty of
breathing due to increase mucus production. I would enumerate other sources of
protein like meat, egg, and the like.
10. You notice a box of dark chocolate on D.Z.s overbed table. He tells you
that he wakes at night and eats four or five pieces of chocolate. Several of
your COPD patients have identified craving for chocolates in the past. What
is the basis for this craving?
Breathing is very difficult for the COPD patient and tends to worsen as the
disease develops. Just breathing causes the person to consume approximately
1,000 calories more on a daily basis than people who dont have the disease.
Besides being delicious, chocolate provides more calories quicker than eating large
amounts of other foods. The caffeine in chocolate is a natural bronchodilator,
allowing the person to breathe easier after eating chocolate.
11. What would you do to address dietary and nutritional teaching needs with
D.Z. and his wife?
One of the best ways to address dietary and nutritional teaching needs with
D.Z. and his wife is to include them in the planning of care. Including the patient and
his significant others in planning of care will increase the patients compliance to
treatment regimen. How to do it? You should set an appointment with them and
have a lecture about proper diet and nutrition for patients with emphysema using
visual aids such as pamphlets or videos. Afterwards, allow them to ask clarificatory
questions with you; and if possible, ask them to state what they have learned.
12. List six educational topics that you need to explore with D.Z.
The following are educational topics to be explored with D.Z.:
Smoking Cessation Education (Ways on how to stop/quit smoking)
Exercise Regularly (Importance of exercise)
Influenza Vaccination (Avoiding respiratory infections)
Nutrition (Adequate and Proper Nutrition)
Medication Education (Compliance to Medical Treatment Regimen)
Lung Volume Reduction Surgery Education
13. What other health care professional would probably be involved in D.Z.s
treatments and how? What is the license/certification status of that
professions in the state in which you are practicing?
Physician- make the diagnosis
Nurse
Assessing the patient
Administering medications
Patient education
Dietitian- prepares food for the patient
Nutritionist- computes caloric intake of the patient
Physical Therapist- assist patient to find ways of increasing their strength and
activity tolerance
Respiratory Therapist
Assess patients cardio-respiratory system
Administer and interpret diagnostic breathing and blood test
Administer medical gases and medicated aerosol therapy to manage and
control breathing related abnormalities
Provide continuous invasive and non-invasive mechanical ventilation
therapy
Insert and maintain a variety of artificial airways
Assist the physician during flexible fiberoptic bronchoscopy services
14. How would you respond to her?
First of all, I will let the wife express all her concerns for me to assess and
prioritize it accordingly. By listening to her concerns I will be able to identify the
root or the cause why the wife is acting that way; and for that I would be able to
limit possible effects/complications that may arise by attending directly to the root
or cause of the problem. Secondly, I will be assessing her coping mechanism;
and I will offer/suggest other coping mechanisms that she may utilize since her
coping mechanism is no longer working for her. Third, I would explain to her the
condition of his husband that the weight loss she noticed was really expected for
COPD patients; and I will encourage her to lengthen her patience and
understanding for her husband because support mechanism is one factor that
may hasten the recovery of the patient.
Lastly, about her financial concerns, I will refer her to a social worker and
make an arrangement for both of them to discuss concerns about hospital bills/
financial bills.
Das könnte Ihnen auch gefallen
- Nurse Case StudyDokument25 SeitenNurse Case StudyAlreem Alhajry100% (1)
- Atelectasis, (Lung Collapse) A Simple Guide To The Condition, Diagnosis, Treatment And Related DiseasesVon EverandAtelectasis, (Lung Collapse) A Simple Guide To The Condition, Diagnosis, Treatment And Related DiseasesNoch keine Bewertungen
- Case Study COPDDokument16 SeitenCase Study COPDRegine Cimafranca Macalaguing100% (4)
- Asthma or Copd Case StudyDokument10 SeitenAsthma or Copd Case StudyMahendra ShrimaliNoch keine Bewertungen
- Review PharmacologyDokument137 SeitenReview PharmacologyGeronimo GonzalezNoch keine Bewertungen
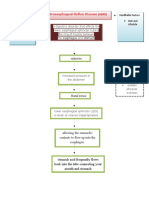
- Gastroesophageal Reflux Disease (GERD) : Non Modifiable Factors Age Pregnancy Modifiable Factors Diet and LifestyleDokument3 SeitenGastroesophageal Reflux Disease (GERD) : Non Modifiable Factors Age Pregnancy Modifiable Factors Diet and Lifestylejoyrena ochondraNoch keine Bewertungen
- Emphysema Case Study E3Dokument28 SeitenEmphysema Case Study E3scarletsky1975% (8)
- ATI Repiratory Questions - Answer KeyDokument11 SeitenATI Repiratory Questions - Answer KeyLeelee SheppardNoch keine Bewertungen
- Chronic Obstructive Bronchitis Is An Inflammation of The BronchiDokument9 SeitenChronic Obstructive Bronchitis Is An Inflammation of The Bronchiinamaliit100% (1)
- Nursing Care Plan For PneumoniaDokument2 SeitenNursing Care Plan For PneumoniaJonas Galeos100% (2)
- Pathophysiology of Meniere - FinalDokument1 SeitePathophysiology of Meniere - FinalMackie Pot PotNoch keine Bewertungen
- Buteyko Method - pdf1Dokument5 SeitenButeyko Method - pdf1fllexx66Noch keine Bewertungen
- Asthma Case StudyDokument4 SeitenAsthma Case StudyEver Green100% (2)
- Community Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandCommunity Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Copd CaseDokument36 SeitenCopd Casejho_Noch keine Bewertungen
- Velez College College of Nursing: Bascon, Karl Niño D. Calunsag, Hazel Kate C. Lague, Inah Krizia ODokument7 SeitenVelez College College of Nursing: Bascon, Karl Niño D. Calunsag, Hazel Kate C. Lague, Inah Krizia Oinah krizia lagueNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease: EmphysemaDokument11 SeitenChronic Obstructive Pulmonary Disease: EmphysemarielNoch keine Bewertungen
- Summer Training Guide For Pharmacy Students-1Dokument132 SeitenSummer Training Guide For Pharmacy Students-1Rania T. Sabri100% (2)
- Bronchial Asthma I. Objectives: A. U: - Espiratory InfectionsáDokument5 SeitenBronchial Asthma I. Objectives: A. U: - Espiratory InfectionsáEnah EvangelistaNoch keine Bewertungen
- Ards Cmap FinalDokument4 SeitenArds Cmap FinalPam Araune67% (3)
- Assessment Diagnosis Planning Intervention Rationale EvaluationDokument4 SeitenAssessment Diagnosis Planning Intervention Rationale EvaluationTrisha SuazoNoch keine Bewertungen
- Pathophysiology of EmphysemaDokument3 SeitenPathophysiology of EmphysemaApple Maiquez Garcia100% (1)
- Pathophysiology Copd-ChfDokument2 SeitenPathophysiology Copd-ChfZaira Batalo100% (2)
- Respiratory Failure, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandRespiratory Failure, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- PneumoniaDokument17 SeitenPneumoniajustin_saneNoch keine Bewertungen
- Nursing Diagnosis For AsthmaDokument6 SeitenNursing Diagnosis For AsthmaTINAIDA33% (3)
- (Patho) PTB COPDDokument1 Seite(Patho) PTB COPDKyle HannahNoch keine Bewertungen
- Pathophysiology of PneumoniaDokument2 SeitenPathophysiology of PneumoniaIrene Demegillo SalongaNoch keine Bewertungen
- Nursing DiagnosisDokument4 SeitenNursing DiagnosisKrizzia CarlosNoch keine Bewertungen
- 2 NCP Chronic Heart FailureDokument5 Seiten2 NCP Chronic Heart FailureLovely CacapitNoch keine Bewertungen
- Pneumonia PresentationDokument20 SeitenPneumonia PresentationsetanpikulanNoch keine Bewertungen
- ANURADHA M.pharm Final PPT 13-08-2018Dokument41 SeitenANURADHA M.pharm Final PPT 13-08-2018sharook abdul100% (1)
- Concept Map AsthmaDokument4 SeitenConcept Map AsthmaAstrid Moreno De LeonNoch keine Bewertungen
- NCP: Chronic Obstructive Pulmonary Disease and AsthmaDokument15 SeitenNCP: Chronic Obstructive Pulmonary Disease and AsthmaJavie100% (5)
- Nursing Process of PneumoniaDokument5 SeitenNursing Process of Pneumoniatin2x061275% (8)
- Causative Agents Causative Agents: Headache, Myalgia, & Nausea Are Added S/SX For Streptococcal PharyngitisDokument21 SeitenCausative Agents Causative Agents: Headache, Myalgia, & Nausea Are Added S/SX For Streptococcal PharyngitisDon Chiaw Manongdo100% (1)
- COPD Care PLAN PDFDokument2 SeitenCOPD Care PLAN PDFVanessaMUeller100% (1)
- Bronchial Asthma FinalDokument25 SeitenBronchial Asthma FinalRio Jane AsimanNoch keine Bewertungen
- EMPHYSEMADokument3 SeitenEMPHYSEMATryx N' Krix TrimorNoch keine Bewertungen
- Drug Study (Seretide)Dokument1 SeiteDrug Study (Seretide)Rene John Francisco100% (1)
- Nursing Practice III EdgeworthDokument8 SeitenNursing Practice III EdgeworthRichard Ines Valino100% (5)
- Case Study PnuemoniaDokument10 SeitenCase Study PnuemoniaKyle B. Nacionales Ü100% (1)
- Description: Chronic Bronchitis EmphysemaDokument16 SeitenDescription: Chronic Bronchitis EmphysemaJay-ar Zars0% (1)
- Copd Health TeachingDokument2 SeitenCopd Health TeachingMel Sevilla100% (1)
- COPD Case PresentationDokument50 SeitenCOPD Case PresentationSarah Ann Jamilla FaciolanNoch keine Bewertungen
- Electrolyte Imbalance 1Dokument3 SeitenElectrolyte Imbalance 1Marius Clifford BilledoNoch keine Bewertungen
- CopdDokument47 SeitenCopdNingshesil Ny HermantNoch keine Bewertungen
- Pneumonia Case StudyDokument5 SeitenPneumonia Case StudycrisolandNoch keine Bewertungen
- PT EducationDokument4 SeitenPT Educationapi-248017509Noch keine Bewertungen
- Discharge Planning PaperDokument5 SeitenDischarge Planning Paperapi-283173905Noch keine Bewertungen
- Medical Management For PneumoniaDokument2 SeitenMedical Management For PneumoniaSue Elaine100% (1)
- PHARYNGITISDokument8 SeitenPHARYNGITISWàrìs Ràfìqùé ßàlòçhNoch keine Bewertungen
- Asthma Nanda DiagnosesDokument4 SeitenAsthma Nanda DiagnosesZinya RobinsonNoch keine Bewertungen
- EmphysemaDokument3 SeitenEmphysemaKhalid Mahmud ArifinNoch keine Bewertungen
- Nursing Care PlanDokument2 SeitenNursing Care PlanAl RizkyNoch keine Bewertungen
- NCP For BreathingDokument17 SeitenNCP For BreathingCeleste Sin Yee100% (1)
- Case AnalysisDokument12 SeitenCase AnalysisFroilan TaracatacNoch keine Bewertungen
- NCP Copd4Dokument15 SeitenNCP Copd4Alessa Marie Crisostomo Salazar100% (1)
- Case Study of Pneumonia With Underlying Covid 19Dokument41 SeitenCase Study of Pneumonia With Underlying Covid 19Angel CauilanNoch keine Bewertungen
- Ineffective Airway ClearanceDokument2 SeitenIneffective Airway ClearanceMaria ArregoitiaNoch keine Bewertungen
- Nursing ManagementDokument16 SeitenNursing ManagementNica Marie LumbaNoch keine Bewertungen
- Acute BronchitisDokument7 SeitenAcute BronchitishqayqNoch keine Bewertungen
- Drug StudyDokument4 SeitenDrug StudyMelissa DavidNoch keine Bewertungen
- Medical Management: Pharmacologic TherapyDokument15 SeitenMedical Management: Pharmacologic TherapyDiana Jalaynie S. SambolawanNoch keine Bewertungen
- Australia GuidelinessDokument4 SeitenAustralia GuidelinessMaxend Arselino SilooyNoch keine Bewertungen
- Nursing DiagnosisDokument7 SeitenNursing DiagnosisMariya Mikaela Garcia SoledadNoch keine Bewertungen
- Copdcasestudy SinnDokument11 SeitenCopdcasestudy Sinnapi-342989632Noch keine Bewertungen
- Eating Well With COPDDokument16 SeitenEating Well With COPDDeep DakshaNoch keine Bewertungen
- Lewis COPD Case StudyDokument2 SeitenLewis COPD Case Studyatarisgurl08Noch keine Bewertungen
- Acls CertificateDokument1 SeiteAcls Certificatemackie_041992Noch keine Bewertungen
- Chapter 1 and 2Dokument17 SeitenChapter 1 and 2mackie_041992Noch keine Bewertungen
- Diversity and Cultural Competency Case StudiesDokument5 SeitenDiversity and Cultural Competency Case Studiesmackie_041992Noch keine Bewertungen
- Module Pharma TXDokument2 SeitenModule Pharma TXmackie_041992Noch keine Bewertungen
- Seretide: What Is in This LeafletDokument6 SeitenSeretide: What Is in This LeafletJazmaine Karyle ChuaNoch keine Bewertungen
- Nishant Respiratory SecondDokument10 SeitenNishant Respiratory SecondNishantNoch keine Bewertungen
- Copd HandoutDokument6 SeitenCopd Handoutapi-272951876Noch keine Bewertungen
- GOLD References 2014Dokument20 SeitenGOLD References 2014Septriawan Aenul RizkyNoch keine Bewertungen
- Asthma Copd 2Dokument27 SeitenAsthma Copd 2mj CanilangNoch keine Bewertungen
- Methacholine Challenge TestDokument8 SeitenMethacholine Challenge TestHafiz Hari NugrahaNoch keine Bewertungen
- Asthma Case StudyDokument4 SeitenAsthma Case Studymp1757Noch keine Bewertungen
- Respiratory SystemDokument104 SeitenRespiratory SystemKatisha JosephNoch keine Bewertungen
- Drug Study: Drug Classificati ON Mechanism of Action Rationale Common Side Effects Nursing ConsiderationDokument5 SeitenDrug Study: Drug Classificati ON Mechanism of Action Rationale Common Side Effects Nursing ConsiderationMaye ArugayNoch keine Bewertungen
- Drug StudyDokument7 SeitenDrug StudyMae Navidas DigdiganNoch keine Bewertungen
- Research Proposal PaperDokument16 SeitenResearch Proposal Paperapi-3124667550% (1)
- New Therapies in Asthma: by Suzanne G. Bollmeier, Pharm.D., BCPS, AE-CDokument31 SeitenNew Therapies in Asthma: by Suzanne G. Bollmeier, Pharm.D., BCPS, AE-CResky ShafaNoch keine Bewertungen
- Respiratory Questions by DR - OkashaDokument96 SeitenRespiratory Questions by DR - Okashamohammed okashaNoch keine Bewertungen
- Respiratory DrugsDokument6 SeitenRespiratory DrugsCurtney PedriaNoch keine Bewertungen
- Penyakit Paru Obstruktif Kronik (PPOK) : Fakultas Kedokteran Universitas Sultan Khairun (Unkhair)Dokument53 SeitenPenyakit Paru Obstruktif Kronik (PPOK) : Fakultas Kedokteran Universitas Sultan Khairun (Unkhair)WahyunitadotokaNoch keine Bewertungen
- Acefyl SPP - 03 Dec 2010Dokument54 SeitenAcefyl SPP - 03 Dec 2010maliakbar111Noch keine Bewertungen
- Pharmacology ReviewDokument28 SeitenPharmacology ReviewKathy Wollschleger100% (1)
- Drug StudyDokument28 SeitenDrug StudyJo Honey TimosaNoch keine Bewertungen
- Chronic Obstructive Pulmonary DiseaseDokument9 SeitenChronic Obstructive Pulmonary DiseaseKiara Denise TamayoNoch keine Bewertungen
- TheophyllineDokument27 SeitenTheophyllineAci LusianaNoch keine Bewertungen
- Drug Study Drug Name Mechanism of Action Dosage Indication Contraindication Side Effects Nursing InterventionsDokument5 SeitenDrug Study Drug Name Mechanism of Action Dosage Indication Contraindication Side Effects Nursing InterventionsYvonne AgathaNoch keine Bewertungen
- Frequently Prescribed DrugsDokument47 SeitenFrequently Prescribed DrugsMahogony ScottNoch keine Bewertungen