Beruflich Dokumente
Kultur Dokumente
Dyspnea Management in Early-Stage Lung Cancer: A Palliative Perspective
Hochgeladen von
Hanifa Nur AfifahOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Dyspnea Management in Early-Stage Lung Cancer: A Palliative Perspective
Hochgeladen von
Hanifa Nur AfifahCopyright:
Verfügbare Formate
Symptom Management Series
Dyspnea Management in
Early-Stage Lung Cancer
A Palliative Perspective
Anna Cathy Williams, BSN, PHN, RN Marcia Grant, DNSc, FAAN, RN
Brian Tiep, MD Jae Y. Kim, MD Jennifer Hayter, MA, OTR/L, SWC, CLT-LANA
A new cohort of lung cancer patient is on the horizon.
With rapidly evolving diagnostics and treatment
methodology, early-stage nonsmall cell lung cancer
patients are increasing in numbers. Although stage I-II
patients are deemed curable, there linger threats of
recurrence, new primaries, and existing or imposed
comorbidities due to the treatment itself. Consequently,
the outlook remains tenuous for this population. With
improving survival rates, it is imperative that patients
with early-stage nonsmall cell lung cancer be fully
assessed, aggressively managed, and followed up long
term, according to the National Comprehensive Cancer
Network guidelines. Dyspnea is one of the most
frightening of all symptoms, regardless of diagnosis
and stage of any disease. It accompanies feelings of
suffocating and even impending death. Given the
subjectivity of dyspnea, it is critical to assess the impact
it imposes on quality of life for each patient and their
loved ones. Cognizant of the abundance of care
involved in such cases, it is the palliative care nurse
who is the core advocate and coordinator of services.
Through a comprehensive care plan and interdisciplinary
effort, healthcare professionals may be able to offer
early-stage nonsmall cell lung cancer patients with
dyspnea stellar evidence-based intervention and
hopefully a greater chance of possessing a sense
of normalcy in their lifestyles.
KEY WORDS
dyspnea, early-stage lung cancer, quality of life
irtually unheard of before the last decade, earlystage nonsmall cell lung cancer (ES-NSCLC) survivors have become part of a growing population.
Currently comprising 15% of the 221,000 newly diagnosed
lung cancers in 2011, the National Cancer Institute cites
improved screening and increased public consciousness
in allowing the medical community to offer this group a
chance of curative intervention, something practically nonexistent in lung cancer.1,2 Approximately 32% of these individuals have a stage I or II disease, the focus population
for this article. Amounting to an approximately 50% 5-year
survival rate at stage IA-B, and averaging 30% for stages
V
332
www.jhpn.com
IIA-B,3-5 patients with newly diagnosed ES-NSCLC warrant
treatment methods that use an interdisciplinary approach.
It is only through comprehensive assessment, interdisciplinary management, and surveillance that the palliative
care team will demonstrate sound clinical strategies, enhancing the quality of life (QOL) for these patients and
their families.6
Often referred to as the sixth vital sign by leading
authorities, dyspnea is defined as respiratory demand exceeding the bodys ability to meet that need.2,3,7 It is a
subjective or perceived, sensory, varied, and yet common experience in lung cancer patients. It is associated
with a conscious sensation of uncomfortable breathing,
smothering or suffocating, difficult, or labored breathing;
inability to get enough air; or tightness in the chest.7,8 It
differs from tachypnea (increased respirations) or breathlessness, which can be a normal physiological response
as seen in exercise or a state of excitement.7 Dyspnea
varies in intensity, consisting of an interface among physiological, psychological, social, and environmental factors, inducing secondary responses.7,9 In the clinical
Anna Cathy Williams, BSN, PHN, RN, is Senior Research Specialist,
Division of Nursing Research & Education, Department of Cancer Control & Population Sciences, City of Hope, Duarte, California.
Marcia Grant, DNSc, FAAN, RN, is Director and Professor, Division of
Nursing Research & Education, Department of Cancer Control & Population Sciences, City of Hope, Duarte, California.
Brian Tiep, MD, is Staff Physician, Critical Care Medicine, Department
of Medical Specialists, City of Hope, Duarte, California.
Jae Y. Kim, MD, is Staff Surgeon, Division of Thoracic Surgery, Department of Surgery, City of Hope, Duarte, California.
Jennifer Hayter, MA, OTR/L, SWC, CLT-LANA, is Director, Expense
Rehabilitation Services, City of Hope, Duarte, California.
Address correspondence to Anna Cathy Williams, BSN, PHN, RN, Division of Nursing Research & Education, Department of Cancer Control
& Population Sciences, City of Hope, 1500 E Duarte Rd, Duarte, CA
91010 (acwilliams@coh.org).
The authors have no conflict of interest to disclose.
This work is supported by a grant from the National Cancer Institute (PO1
CA136396Palliative Care for Quality of Life and Symptom Concerns in
Lung Cancer; B. Ferrell, PI).
DOI: 10.1097/NJH.0b013e318258043a
Volume 14 & Number 5 & July 2012
Symptom Management Series
presentation chronic, labored breathing is one of the most
difficult symptoms to identify or manage, and once acquired, it promises to remain an ever-present condition.
Dyspnea possesses unique characteristics in that acute
episodes, such as asthma or bronchitis, are manageable
and tend to subside and resolve with uncomplicated or
minimal intervention of the underlying cause. Chronic
cases are persistent, linger, and have varied intensity, regardless of intervention. In chronic dyspnea, 85% of the
etiologies stem from cardiopulmonary and psychogenic causes.10 The American Thoracic Society suggests
the prevalence ranges from 55% to 87% in all stages of
lung cancer.
The sensation of breathlessness is frightening to patients and their caregivers (CGs), leading to a feeling of
suffocation and possible death. Not only is dyspnea an
alarming, multidimensional symptom, the impact on a
patients QOL is undeniable and often incessant.7,11,12
Cognizant of the needs of these individuals, it is the palliative care nurse, possessing a specialized skill set, who
is poised as the point person in coordinating care and
is a critical component of the interdisciplinary healthcare team.
Along with the diagnosis of ES-NSCLC, 60% of these
patients suffer comorbid conditions and symptoms, such
as chronic obstructive pulmonary disease (COPD) and
dyspnea.13 The plan of care should encompass pharmacological and nonpharmacological interventions for preexisting medical concerns, along with those issues imposed
by lung cancer or cancer treatments. Supportive and palliative care is an essential ingredient in ES-NSCLC patients
with dyspnea. The following discussion addresses the
etiology, assessment, management, and follow-up for the
symptom of dyspnea in ES-NSCLC patients.
CLINICAL CHARACTERISTICS AND
ETIOLOGY OF DYSPNEA IN
EARLY-STAGE LUNG CANCER
The most common symptom in all lung cancers, dyspnea
is one of the most unpleasant and is described subjectively
and according to the underlying cause. The etiology of
dyspnea can be direct or indirect (as seen in Table 1). A
direct cause of dyspnea involves cancer, or its effects,
such as tumor or lymphatic invasion, effusion, obstruction
of pulmonary tissue, or the complication of pulmonary
embolism.12,15,21 Indirect causes are numerous, such as
anemia, underlying cardiac or pulmonary disease, thoracic surgery, or cancer treatments such as chemotherapy,
biotherapy, and radiation.15,21
Dyspnea often displays similar characteristics but is
unique because of the underlying etiology and body system involved (ie, pulmonary or cardiac). It is frequently
Journal of Hospice & Palliative Nursing
classified by the severity, symptoms, type, duration, distress to the patient, and interference with activities of daily
living (ADLs).16,23 The pathophysiology is certainly poorly
understood,21,22 and etiologies are varied, as shown in
Table 1. Dyspnea stems from the mechanisms of increased ventilatory demand, impaired mechanical responses, or a blending of both.11 Variations exist in the
extent of dyspnea due to various afferent causes from the
brains autonomic center or the receptors in the airway,
lungs, and chest wall. Further contributors to the variability
of dyspnea are the type of provocation such as situation,
behavioral influence, and the patients ability to depict
the sensation.10,23
Breathlessness is unique in the sense that there are no
specialized dyspnea receptors, although more recently,
magnetic resonance imaging (MRI) studies have revealed
midbrain arenas exhibiting a perception of dyspnea.21
The reaction is likely a consequence of a complex interaction between chemoreceptor stimulation, mechanical
abnormalities in breathing, and the perception of the abnormalities by the central nervous system or neuromechanical uncoupling.21 Essentially, dyspnea results from the
cortex dominating the respiratory center, rousing chemoreceptors in the lung and respiratory muscles. Respiratory
effort intensifies, and there is a boost in the use of respiratory muscles. This amplifies ventilatory requirements and
can occur acutely, as in exercise or exertion, or chronically, as with COPD.2,24
QUALITY OF LIFE RELATED TO
DYSPNEA IN EARLY-STAGE
LUNG CANCER
A rapidly growing population of survivors brings with it
expectations of an enhanced QOL, along with a greater
emphasis on patient-centered issues. The goal of palliation is to improve patient care by managing symptoms in
the physical, psychological, social, and spiritual realms
associated with lung cancer and/or its treatment.17,25 Palliative intervention should be received concurrently with
treatment and continue as long as needed.
Current literature clearly demonstrates the impact of
dyspnea on surgical patients and their loved ones, before,
during, and after treatment,13,26 citing dyspnea as a common symptom in the years following surgical resection.
Additionally, the article reports that 65% of these patients
offered no complaint of preoperative dyspnea. In another
longitudinal study exploring QOL in patients with resected ES-NSCLC 2 years postoperatively, surgery was
found to have substantially reduced QOL across all domains except emotional functioning.13 The impact of dyspnea on QOL is undeniable. Physically, this symptom is
regarded as one of the most distressing, as the phenomenon
www.jhpn.com
333
Symptom Management Series
TABLE 1 Continued
TABLE 1 Etiology of Dyspnea
Known Cause
Possible Signs/
Symptoms
Accompanying
Dyspnea
Intervention
Direct cause
Tumor
Cough
Surgical
Lymph invasion
Difficulty
swallowing
Chemotherapy
Known Cause
Possible Signs/
Symptoms
Accompanying
Dyspnea
Intervention
MI
Cardiac enzymes
Cardiomyopathy
Diuretics and
monitor fluid
balance
Sepsis
Febrile
Cytology
Chills
Antibiotics
Patient reported
Treat underlying
cause
Grimace
Radiation
Obstruction/
restriction
Decreased oxygen
saturation
Controlled oxygen
COPD
Fremitus
Bronchodilators
Pulmonary
embolism
Clubbed fingers/
toes
Corticosteroids
Pain medications
as directed
Asthma
Cyanosis
Antibiotics
Distraction
technique
Confusion
Opioids
Anxiety
Tachypnea
Anxiolytics
Blood gases
Panic
Tachycardia
Teach coping
techniques
Diaphoresis
Psychology/CSW
referral
Pain
Sputum cytology
Pulmonary
rehabilitation
Effusion
Diminished breath
sounds
PleurX/pleurodesis
Tunneled catheter
Sedentary
lifestyle
Activity intolerance
Exercise program
Nutritional consult
Indirect cause
Cancer
treatments
Postoperative pain
Treat underlying
cause
Thoracic surgery
Loss of lung tissue
Pulmonary
rehabilitation
Chemotherapy/
biotherapy
Chemotherapyinduced nausea
and vomiting
(See Table 2)
Radiation
Cough
Anemia
Pallor
Transfusion
Erythropoietin
Nutritional
consult
Cardiac
pathology
Chest pain
ECG
CHF
Congestion
Echo
334
Remain with
pt during
exacerbation
Thoracentesis
www.jhpn.com
Abbreviations: CHF, congestive heart failure; COPD, chronic obstructive
pulmonary disease; CSW, clinical social work; ECG, electrocardiogram;
MI, myocardial infarction.
Adapted from References 6, 7, 10, 13, and 19-22.
of decreased oxygen lends to increased fatigue and breathlessness, and may be accompanied by discomfort, burning,
numbness, or a feeling of impending death.27,28 It impacts
ability to sleep, work, exercise, and experience intimacy.29
There is a multitude of psychological responses to dyspnea, that of fear, anxiety, and possibly guilt and depression, often exacerbating the dyspnea. From a social
standpoint, patients suffer all manner of upset. There is
observable role reversal, CG burden, loss of leisure activity, isolation, compromised sexuality, and frequently financial burden.27,30 Often overlooked is the spiritual
suffering involved, along with existential questions when
patients are faced with life-altering symptoms such as lung
cancer and dyspnea. Living often takes on new meaning
and purpose, even when patients are diagnosed at an
Volume 14 & Number 5 & July 2012
Symptom Management Series
TABLE 2 Methods of Pulmonary Rehabilitation
Prevention
Gas exchange/oxygen transport
(1) Smoking cessation
(1) Oxygen therapy
(2) Ensure immunizations
(2) Bronchial hygiene
(3) Prevent exacerbation
(3) Exercise program
(4) Optimize medical management
Self-management
(1) Medication training
(a) Metered dose inhaler
(b) Nebulizer
Exercise training
(1) Ambulation training
(2) Upper-extremity training
(3) Ventilatory muscle training
Functional training (ADLs)
(2) Bronchial hygiene
(1) Self-care
(3) Breathing retraining
(2) Care of the home
(4) Oxygen therapy
(3) Leisure pursuits
(5) Adequate nutrition
(4) Work (as appropriate)
(6) Family training
(5) Active lifestyle
(7) Reporting to physician
(6) Shopping
(8) Exacerbation protocol
(7) Sexual counseling
(a) Self-assessment
Team support
(b) Self-intervention
(1) Acceptance of disease
(c) Access physician
(2) Coping skills
Dyspnea relief
(3) Encouragement
(1) Exercise program
(4) Positive thinking
(2) Breathing retraining
(5) Self-esteem
(3) Bronchodilators
(6) QOL focus
(4) Bronchial hygiene
Advance directives
(5) Reduce anxiety, depression
(1) Advance directives
(6) Reduce fear, apprehension
(2) Continuing directives
(7) Improve confidence
Abbreviation: ADLs, activities of daily living.
Adapted from Tiep,14 Table 3.
early stage. There appears to be an abundance of uncertainty and loss of ones belief systems. It is imperative
that the nurses clinical assessment incorporates not only
diagnostic manifestations, but also provides a comprehensive examination into these all-encompassing QOL
dimensions.6
Journal of Hospice & Palliative Nursing
ASSESSMENT OF DYSPNEA IN
EARLY-STAGE LUNG CANCER
As dyspnea is a highly subjective symptom, evaluating
an individuals shortness of breath is an obscure circumstance at best, and severity may be associated with the
patients perception of what the dyspnea means.15 Along
www.jhpn.com
335
Symptom Management Series
TABLE 3 Assessment of Dyspnea in Early-Stage NonSmall Cell Lung Cancer Patients
Subjective
Objective
Self-reporting scales such as
History and physical examination
& Numeric rating scale
& Vital signs
0 = no problem, 10 = the worst
& Baseline Dyspnea Scale
& Systems review
& Respiratory assessment
Functional
Auscultation/percussion
Magnitude of task
Quality of breaths (pursed lip, puffing, blowing, flared nostrils)
Magnitude of effort
Dry or productive cough
& Respiratory Distress Observational Scale
Observational documentation
Sputum quantity and character
Use of accessory muscles
Ability to complete full sentence
Identify stable or unstable dyspnea and acute respiratory failure
& Skin color and temperature
& Dependent edema and abdominal girth
& Smoking and COPD screening
Symptoms and interference with ADLs
Pulmonary function testing
& Baseline, during treatment and exacerbations
& Pulse oximetry
& Onset (sudden or gradual), intensity, duration
& Spirometry
& What alleviates or aggravates dyspnea
Impact of symptoms on QOL
Laboratory testing
& Physical: difficulty breathing, decreased oxygen, compromised
activity, fatigue
& Complete blood count (anemia)
& Psychological: fear, depression, anxiety
& Chemistry
& Social: financial burden, isolation
& ABGs (blood gases)
& Spiritual: meaning and purpose in life, which is breathing
Assess
Imaging
& Inhaler/oxygen techniques
& Chest x-ray
& Medication administration and compliance
& CT
& Strategy for secretion clearance
& Echo
& Shuttle walking test
Education/evaluation as needed: (maintain symptoms diary)
Consultations and surveillance
& Alter perception of breathlessness
& Nutrition (healthy diet and maintenance)
Sit upright supported by pillow
& Pulmonary rehabilitation
Continued
336
www.jhpn.com
Volume 14 & Number 5 & July 2012
Symptom Management Series
TABLE 3 Continued
Subjective
Provide ambient air flow in environment (fan)
& Reduce respiratory demand
Objective
& CT every 6-12 mo, then annually
& Annual influence and pneumococcal vaccinations
Plan important activities first (energy conservation)
& Routine vital signs, pulse oximetry, and laboratory work
Teach pursed lip/diaphragmatic breathing
& Bone density as appropriate
Rest periods/relaxation and coping techniques
& Routine dental exams
Keep frequently used items within reach
& Regular physical activity
Walker or wheelchair as needed
Perform grooming sitting down
Wear clothing that is easy to put on
Avoid environmental irritants
Call medical doctor/nurse practitioner if
Febrile 9 100.5
Change in breathing, cough or sputum
Abbreviations: ABGs, arterial blood gases; ADLs, activities of daily living; COPD, chronic obstructive pulmonary disease; CT, computed tomography; QOL,
quality of life.
Adapted from references 6, 7, 10, 13, and 15-20.
with assessing dyspnea quality, specific descriptions
should be elicited according to the onset, duration, intensity, activity level, and psychological response before,
during, and after dyspnea experience.9,31,32 Upon the initial assessment, the nurse begins with the patients subjective (self-report) of dyspnea, which can involve a
quantitative scale (Table 3). Examples of scales available
are the Numeric Rating Scale (where 0 = the least problem and 10 = the worst), or visual analog scale, which
measures symptom intensity with a 100-mm line (vertical
or horizontal). Other commonly used measurements are
Baseline Dyspnea Index (which grades severity of dyspnea in 3 different categories; functional status, magnitude of task, and magnitude of effort, 0 = severe, 4 =
unimpaired) or Respiratory Distress Observational Scale,
which is survey-like with observational documentation.18,19,32 Collectively, all scales ask the patient to rate
dyspnea related to shortness of breath and impact on
ADLs and/or QOL.
Objective assessment involves a thorough history and
physical examination, providing invaluable information via
the actual interview, assessment scales, auscultation, and
percussion, and is diagnostic in at least one-half of patients.
The use of imaging yields discovery of common cardiopulmonary diseases, along with the diagnostics listed below.
Nursing assessment of dyspnea may assist in locating
the cause, in addition to establishing the most appropriJournal of Hospice & Palliative Nursing
ate interventions regarding symptom prevention, management, and follow-up. Table 3 presents an overview
of nursing appraisal components. Along with the oneto-one assessment, imaging, a complete blood count,
metabolic profile, arterial blood gases, echocardiogram/
electrocardiogram (echo/ECG), pulmonary function, and
sputum cytology should be completed. Consideration
should also be given to the possible adverse effects and
outcomes of the patient undergoing treatment intervention for their lung cancer, such as thoracic surgery, chemotherapy, or radiation.2,7,33
NURSING MANAGEMENT OF DYSPNEA
IN EARLY-STAGE LUNG CANCER
The goal of nursing in dyspnea is to obtain a full picture
of the patients experience and impact on ADLs and QOL
for both the patient and family. Nurses must also acknowledge and accept the patients self-report of dyspnea.32,33
Following a full assessment of all four domains in QOL
(physical, psychological, social, spiritual), as seen in
Table 3 it is of the utmost importance to achieve a thorough
understanding of the perceptions, fears, and uncertainties
surrounding the symptom of dyspnea. Nurses must be exceptionally skilled in assessing dyspnea in the ER-NSCLC
patient, along with implementing effectual interventions,
and improving outcomes for this population.
www.jhpn.com
337
Symptom Management Series
Once the medical and nursing assessment has taken
place, the underlying cause is addressed. Depending on
the chronicity of dyspnea, the nurse is able to provide support for disease management including the interdisciplinary
plan of care, promoting energy conservation, strict medication adherence, relaxation and coping techniques, nutritional evaluation, and pulmonary rehabilitation.34,35
Working collaboratively, the nurse ensures the highest QOL possible for the patient and family, rendering
education and referrals as needed. As an integral part
of follow-up, the nurse should advocate for chronic review of outcome and institute intervention refinement,
endorse organizational and policy strategies, and assess
program needs concerning services to facilitate adequate
surveillance, always embracing the patients QOL.36,37
MEDICAL MANAGEMENT OF PRIMARY
DISEASE EARLY-STAGE LUNG CANCER
Early-stage NSCLC patients with dyspnea undergo all nature of complex treatment, including, but not limited to,
surgery, radiotherapy, and chemotherapy or a combination thereof. Even with current, cutting-edge technologies, long-term survival remains somewhat elusive. After
initial, potentially curative treatment, long-term survival
without recurrence remains elusive, as many patients develop new primary lung malignancies. In addition, 21%
of ES-NSCLC patients enter into therapy with minimal or
no dyspnea, yet any number of curative interventions
may actually provoke dyspnea.38,39 After their potentially
restorative treatment, ES-NSCLC patients with dyspnea
require continued surveillance and follow-up care for dyspnea, other medical issues, and QOL concerns.
Clinical assessment and pretreatment evaluation for
stage IA may consist of pulmonary function, cardiopulmonary exercise testing, bronchoscopy, mediastinoscopy
and/or endobronchial ultrasound, and a positron emission
tomography (PET)/computed tomography (CT) scan. For
stage I-IIB, an MRI of the brain should also be performed.1,2,8
For early-stage disease, surgical resection is the standard of care, providing the best chance for cure. Surgical
procedures range from limited resections of wedge or
segmentectomy, to more extensive resections of a lobectomy, bilobectomy, or pneumonectomy. The surgery, if
offered as an intervention, is largely dependent on histology, the extent of disease, and comorbidities such
as cardiopulmonary status. Procedurally, surgery is performed with a posterolateral thoracotomy incision or that
of robotic or video-assisted thoracoscopic surgery (VATS).
The lesser invasive procedures may reduce pain and recovery time and perhaps lower morbidity.
For patients with wholly resected with stage I disease,
adjuvant chemotherapy or radiotherapy is not recommended. For stage I-IIB disease, chemotherapy and
338
www.jhpn.com
radiotherapy are most often instituted, according to histology, biomarkers, the tumor margins and location, and
lymph node sampling.2,4,7
At times, unique services may be available to the patient, such as pulmonary prerehabilitation/rehabilitation.
The definition of pulmonary rehabilitation is that it should
be evidence-based, multidisciplinary, and comprehensive intervention for patients with acute and chronic respiratory disease who are symptomatic and often have
decreased daily life activities.7 It is designed to reduce
symptoms, optimize function, increase participation, and
reduce healthcare costs through stabilizing or reversing
systemic manifestations of the disease.13,40,41 Indications
for referrals include dyspnea and comorbid lung diseases
such as COPD, asthma, and pulmonary fibrosis. Expectations would include a reduction in dyspnea, improved exercise capacity, sense of control regarding disease process,
and overall enhanced QOL.
In considering the potential for interdisciplinary roles, it
is best to consider who should be involved, the relevancy,
what the interventions might consist of, and how QOL outcomes are achieved. Most assuredly, thoracic surgeons or
medical oncologists perform important functions, providing appropriate treatment regimens, according to the patients medical requirements. Pulmonary rehabilitation
should be enlisted early on, pretreatment if possible. This
would help to establish a baseline, enhance pulmonary
function, and open the way for planning care during and
after therapy.12,39,40 Nutritional services should be provided to enhance the complex dietary needs of cancer
patients. Lastly, clinical social work and/or chaplaincy are
an indispensable support for any individual with a malignant process. Social work can also coordinate psychological, financial, or legal resources. It is only through such a
truly collaborative team that healing and progress can be
achieved throughout the lung cancer trajectory.1,2,5,12
Medical surveillance should consist of a regular history
and physical examination, along with a chest CT every
6 to 12 months for 2 years, then annually. The patient
should receive an annual influenza and pneumococcal
vaccination as appropriate, routine pulse oximetry, blood
pressure, cholesterol, and glucose monitoring. Additional
workup might consist of a bone density, routine dental examinations, and evaluation of diet and nutritional needs.
Regular physical activity should be encouraged.2,3
CASE PRESENTATION
Mr B. is a 67-year-old Asian American former athlete,
with a former 50-pack-year history of smoking. He presented with abnormal imaging, with presumed stage IIB
(ES-NSCLC). A PET/CT revealed uptake of a 5-cm mass
in the left upper lobe. There was also a small, slightly
spiculated density in the left lower lobe, along with an
Volume 14 & Number 5 & July 2012
Symptom Management Series
enlarged mediastinal lymph node. The patients comorbidities consisted of COPD, hypertension, and depression.
Along with a complete history and physical examination,
Mr B. underwent a preoperative education by the nurse.
Workup consisted of complete blood count and chemistry profile, pulmonary function, a brain MRI, bone scan,
and an echo/ECG. After it was noted that the brain MRI
and bone scan were negative, discussions related to treatment alternatives were conducted at a chest conference.
Upon dialog with the thoracic surgeon, Mr B. opted to undergo VATS consisting of a pneumonectomy and mediastinal lymph node sampling. He was cleared for surgery
and was later advised that the surgery went very well, and
tumor margins were clear. His case was presented at the interdisciplinary thoracic tumor board; since his biomarkers were positive for excision repair cross-complementing
group 1 and ribonucleotide reductase M1, the patient
decided on treatment defined by the National Comprehensive Cancer Network (NCCN) for stage IIB ES-NSCLC, per
the physicians recommendation. This consisted of adjuvant chemotherapy of taxotere and gemcitabine, giving
him the greatest chance for a curative effect. No radiation
was intended. The plan of care was thoroughly discussed
among the oncology team, the oncologist, and with the
family present.
Prior to his initial treatment, Mr B. was seen in pulmonary rehabilitation and nutrition and had a peripherally inserted central catheter line placed for ease of
obtaining blood specimens and chemotherapy administration. At his first chemotherapy appointment, with his
spouse present, he met with the oncologist and then
the chemo nurse. Teaching began with the patient
and CG concerning the treatment schedule and adverse
effects of the chemotherapy drugs, in concert with the
routine ancillary medications needed to complete regimen. Information was also provided on whom, when,
and where to call should issues arise. Symptom and
medication diaries were provided. They were to be filled
out and brought to clinic upon each return visit to evaluate for adverse events.
Mr B. did well postoperatively and with his chemo
treatment, yet suffered a great deal of dyspnea, due to
the surgical intervention. He was compliant in the pulmonary rehabilitation program, yet continued to become
more depressed over time at the loss of his athletic and
social capacities. He also admitted to fear of intimacy
and not being able to keep up with his spouse. He
was referred back to his local psychologist, who continues to work with Mr B. and his spouse on communication, role change, and intimacy concerns. At his last
clinic visit, 1 year after treatment, his spirits were up,
and he reported that his respiratory status had much improved. He cited his overall QOL as good. It was determined that he was in remission and would return for
Journal of Hospice & Palliative Nursing
follow-up according to guidelines established by the
NCCN (Table 3).
IMPLICATIONS FOR DYSPNEA IN
PALLIATIVE CARE
The intricacies of dyspnea are multifaceted and complex,
and challenges facing health professionals remain rigorous and challenging. Nursing management and education
of dyspnea in the ES-NSCLC patient are directed toward
prevention, expedient recognition, all-inclusive assessment, genuine interdisciplinary methodology, and thorough follow-up surveillance. Nurses must be aware of
the frequent and widespread etiologies of such cases and
institute chronic evaluation, coordination, and management of dyspnea, as these are all integral components in
the care of ES-NSCLC. Equipped with an understanding
of patients and families equating shortness of breath with
feelings of suffocation, helplessness, and isolation, the
nurse is cognizant that all aspects of care must be attended
to meticulously, from ADLs to the impact on QOL and rehabilitative referrals.
There is a continued need for further clinical research
in this arena. Although there are preliminary fundamental
guidelines and personalized care in place, clinicians and
nurse researchers must develop an empirical endeavor to
better understand the experience of dyspnea in ES-NSCLC
patients and their loved ones. With the increased numbers
of cancer survivors, healthcare must acknowledge the implications for establishing survivorship programs as an integral part of the cancer care trajectory.42
References
1. Movsas B, Khuri F, Kernstine K. Nonsmall cell lung cancer. In:
Padzur R, Coia L, Hoskins W, Wagman L, eds. Cancer Management: A Multidisciplinary Approach. 11th ed. London, UK:
CMP; 2008.
2. National Cancer Institute (NCI). Nonsmall cell lung cancer.
2011. http://www.cancer.gov/cancertopics/pdq/treatment/
nonsmall-cell-lung/healthprofessional. Accessed December
31, 2011.
3. American Cancer Society (ACS). Lung cancer: nonsmall cell.
2010. http://www.cancer.org. Accessed December 30, 2011.
4. Ost D, Goldberg J, Rolnitzky L, Rom WN. Survival after surgery
in stage IA and IB nonsmall cell lung cancer. Am J Respir Crit
Care Med. 2008;177(5):516-523.
5. Cancer: lung and bronchus. SEER; 2011. http://seer.cancer.gov/
statfacts/html/lungb.html. Accessed January 10, 2012.
6. Grant M, Economou D, Ferrell B, Bhatia S. Preparing professional staff to care for cancer survivors. J Cancer Survivor Res
Pract. 2007;1(1):98-106.
7. American Thoracic Society (ATS). Dyspnea. Am J Respir Crit
Care Med. 1999;159:321-340.
8. Colice GL, Shafazand S, Griffin JP, Keenan R, Bolliger CT.
Physiologic evaluation of the patient with lung cancer being
considered for resectional surgery: ACCP evidenced-based
clinical practice guidelines (2nd edition). Chest. 2007;132
(suppl 3):161S-177S.
www.jhpn.com
339
Symptom Management Series
9. Canty GR. Dyspnea. In: Newton S, Hickey M, Marrs J, eds.
Mosbys Oncology Nursing Advisor: A Comprehensive Guide
to Clinical Practice. St Louis, MO: Mosby; 2009:359-360.
10. Karnani NG, Reisfield GM, Wilson GR. Evaluation of chronic
dyspnea. Am Fam Physician. 2005;71(8):1529-1537.
11. Dudgeon D. Dyspnea, death rattle, and cough. In: Ferrell B,
Coyle N, eds. Oxford Textbook of Palliative Nursing. 3rd ed.
New York, NY: Oxford University Press; 2010:303-315.
12. Gaguski ME, Brandsema M, Gernalin L, Martinez E. Assessing
dyspnea in patients with nonsmall cell lung cancer in the acute
care setting. Clin J Oncol Nurs. 2010;14(4):509-513.
13. Feinstein MB, Krebs P, Coups EJ, et al. Current dyspnea among
long-term survivors of early-stage nonsmall cell lung cancer.
J Thorac Oncol. 2010;5(8):1221-1226.
14. Tiep BL. Disease management of COPD with pulmonary rehabilitation. Chest. 1997;112(6):1630-1656.
15. Thomas J, von Gunten CF. Dyspnea. In: Bruera E, Higginson I,
Ripamonti C, von Gunten C, eds. Textbook of Palliative Medicine. Great Britain: Hodder Arnold; 2006:655-662.
16. Boyars MC, Karmath BM, Mercado AC. Acute dyspnea: a sign
of underlying disease. Hosp Phys. 2004;40(7):23-27.
17. Gralla R, Edelman M, Detterbeck F, et al. Assessing quality of
life following neoadjuvant therapy for early stage nonsmall
cell lung cancer (NSCLC): results from a prospective analysis
using the Lung Cancer Symptom Scale (LCSS). Support Care
Cancer. 2009;17(3):307.
18. Mahler DA, Weinberg DH, Wells CK, Feinstein AR. The measurement of dyspnea. Contents, interobserver agreement, and
physiologic correlates of two new clinical indexes. Chest. 1984;
85(6):751-758.
19. Oncology Nursing Society (ONS). Tables of tools to measure
oncology nursing-sensitive patient outcomes: dyspnea. 2008.
http://ons.org/Research/PEP/Dyspnea. Accessed January 6, 2012.
20. National Comprehensive Cancer Network (NCCN). Nonsmall
cell lung cancer. Fort Washington, PA:NCCN; 2012.
21. Lechtzin N. Dyspnea: symptoms of pulmonary disorders. 2009.
http://merckmanuals.com/professional/print/pulmonary_
disorders/symptoms. Accessed January 3, 2012.
22. Smith CB, Nelson JE, Berman AR, et al. Lung cancer physicians
referral practices for palliative care consultation. Ann Oncol.
2012;23(2):382-387.
23. Thomas S, Bausewein C, Higginson I, Booth S. Breathlessness
in cancer patientsVimplications, management and challenges.
Eur J Oncol Nurs. 2011;15(5):459-469.
24. Inzeo D, Tyson L. Nursing assessment and management of
dyspneic patients with lung cancer. Clin J Oncol Nurs. 2003;7(3):
332-333.
25. Cooley ME. Quality of life in persons with nonsmall cell lung
cancer: a concept analysis. Cancer Nurs. 1998;21(3):151-161.
26. Houlihan NG, Tyson LB. Lung Cancer. 2nd ed: Oncology
Nursing Society; 2004.
27. Kamal AH, Maguire JM, Wheeler JL, Currow DC, Abernethy AP.
Dyspnea review for the palliative care professional: assessment,
burdens, and etiologies. J Palliat Med. 2011;14(10):1167-1172.
28. Smith EL, Hann DM, Ahles TA, et al. Dyspnea, anxiety, body
consciousness, and quality of life in patients with lung cancer.
J Pain Symptom Manage. 2001;21(4):323-329.
29. Hawkins Y, Ussher J, Gilbert E, Perz J, Sandoval M, Sundquist
K. Changes in sexuality and intimacy after the diagnosis and treatment of cancer: the experience of partners in a sexual relationship with a person with cancer. Cancer Nurs. 2009;32(4):
271-280.
30. Shell JA, Carolan M, Zhang Y, Meneses KD. The longitudinal
effects of cancer treatment on sexuality in individuals with
lung cancer. Oncol Nurs Forum. 2008;35(1):73-79.
31. Howell D. Dyspnea management: a biopsychosocial approach.
In: Hass ML, ed. Contemporary Issues in Lung Cancer: A
Nursing Perspective. 2nd ed. Sudbury, MA: Jones and Bartlett;
2010:195-216.
32. Registered Nurses Association of Ontario (RNAO). Nursing
care of dsypnea: practice recommendations. 2011. http://rnao
.org/pda/copd/practice_recommendations.html. Accessed
January 31, 2012.
33. Prigmore S. Assessment and nursing care of the patient with
dyspnea. 2005;101(14). http://www.nursingtimes.net. Accessed
February 14, 2012.
34. Breaden K. Recent advances in the management of breathlessness. Ind J Palliat Care. 2011;17(suppl):S29-S32.
35. Maxwell LA. Therapeutic nursing for managing breathlessness.
Nurs Times. 2007;103(22):28-29.
36. National Giudelines Clearinghouse (NGC). Nursing care of
dyspnea: the 6th vital sign. 2011. http://guideline.gov/popups/
printview.aspx?id=32419. Accessed January 31, 2012.
37. Oncology Nursing Society (ONS). Dyspnea: clinical practice
guidelines. 2008. http://ons.org/Research/PEP/Dyspnea. Accessed
January 6, 2012.
38. Cooley ME, Short TH, Moriarty HJ. Symptom prevalence, distress, and change over time in adults receiving treatment for
lung cancer. Psychooncology. 2003;12(7):694-708.
39. Sarna L, Cooley ME, Brown JK, Chernecky C, Elashoff D,
Kotlerman J. Symptom severity 1 to 4 months after thoracotomy
for lung cancer. Am J Crit Care. 2008;17(5):455-467; quiz 468.
40. National Guideline Clearinghouse (NGC). COPD: pulmonary
rehabilitation. 2010. http://www.guideline.gov/synthesis/syntheisi
.aspx?id=16423&search=dyspnea. Accessed January 31, 2012.
41. Smith IE, Pierga JY, Biganzoli L, et al. First-line bevacizumab
plus taxane-based chemotherapy for locally recurrent or metastatic breast cancer: safety and efficacy in an open-label study
in 2,251 patients. Ann Oncol. 2011;22(3):595-602.
42. Centers for Disease Control and Prevention. Cancer survivorship.
2012. http://www.cdc.gov/cancer/survivorship/. Accessed
February 3, 2012.
For more than 57 additional continuing education articles related to cancer, go to NursingCenter.com\CE.
340
www.jhpn.com
Volume 14 & Number 5 & July 2012
Das könnte Ihnen auch gefallen
- Laryngopharyngeal Reflux Disease: Integrative ApproachesVon EverandLaryngopharyngeal Reflux Disease: Integrative ApproachesNausheen JamalNoch keine Bewertungen
- The Role of A Nurse Specialist in A Modern Lung-CancerDokument12 SeitenThe Role of A Nurse Specialist in A Modern Lung-CancerM.Valent DiansyahNoch keine Bewertungen
- Allexander N. Hanania Radation Induced Lung InjuryDokument13 SeitenAllexander N. Hanania Radation Induced Lung InjuryAlejandro TurnerNoch keine Bewertungen
- Guia para El MedicoDokument6 SeitenGuia para El MedicoJuan Sebastian OrdoñezNoch keine Bewertungen
- Neuro-Oncology and Palliative Care: A Challenging InterfaceDokument5 SeitenNeuro-Oncology and Palliative Care: A Challenging InterfaceJiaNoch keine Bewertungen
- The Effect of Integrating Early Palliative Care Modalities On Patients With Lung Cancer-1Dokument9 SeitenThe Effect of Integrating Early Palliative Care Modalities On Patients With Lung Cancer-1api-396564080Noch keine Bewertungen
- What Are The Hidden Challenges of Lung CancerDokument5 SeitenWhat Are The Hidden Challenges of Lung CancerFarul HaizzatNoch keine Bewertungen
- Lung Cancer - 2021Dokument20 SeitenLung Cancer - 2021Gilbert LazarusNoch keine Bewertungen
- Primary Care For Cancers - Epidemiology, Causes, Prevention and Classification - A Narrative ReviewDokument7 SeitenPrimary Care For Cancers - Epidemiology, Causes, Prevention and Classification - A Narrative ReviewChew Boon HowNoch keine Bewertungen
- 19 TEP Tak2019Dokument12 Seiten19 TEP Tak2019Juan Carlos Uribe CaballeroNoch keine Bewertungen
- OutDokument10 SeitenOutErwinNoch keine Bewertungen
- Risk Factors For Short-Term Lung Cancer SurvivalDokument9 SeitenRisk Factors For Short-Term Lung Cancer SurvivalAhmad JunaidiNoch keine Bewertungen
- Strategies To Relieve Dyspnoea in Patients With Advanced Chronic Respiratory Diseases. A Narrative ReviewDokument10 SeitenStrategies To Relieve Dyspnoea in Patients With Advanced Chronic Respiratory Diseases. A Narrative ReviewChristine BelindaNoch keine Bewertungen
- Head NeckDokument8 SeitenHead NeckerandolphsavageNoch keine Bewertungen
- Ournal of Linical Ncology: PurposeDokument11 SeitenOurnal of Linical Ncology: PurposeRicky Cornelius TariganNoch keine Bewertungen
- Status Cancer PlamaniDokument10 SeitenStatus Cancer Plamanitenzi583Noch keine Bewertungen
- Objective: Breast Cancer Is The Most Common Type of Cancer Found in Women, in The United StatesDokument5 SeitenObjective: Breast Cancer Is The Most Common Type of Cancer Found in Women, in The United StatesdwiNoch keine Bewertungen
- SinopsisDokument7 SeitenSinopsisbee yournitaNoch keine Bewertungen
- Palliative Medicine in The ElderlyDokument13 SeitenPalliative Medicine in The ElderlyVerica JankelićNoch keine Bewertungen
- Managing Breathlessness: A Palliative Care Approach: Chloe Chin, Sara BoothDokument9 SeitenManaging Breathlessness: A Palliative Care Approach: Chloe Chin, Sara BoothRitu ShewaniNoch keine Bewertungen
- Therapy LeukemiaDokument11 SeitenTherapy LeukemiaGita RahmatikaNoch keine Bewertungen
- AML 10 Palliative NursingDokument5 SeitenAML 10 Palliative NursingutamiprakosoNoch keine Bewertungen
- Bronchoalveolar CarcinomaDokument5 SeitenBronchoalveolar CarcinomaFrancois Donatien De SadeNoch keine Bewertungen
- Enf Neuromus C y Pulmon 2012Dokument8 SeitenEnf Neuromus C y Pulmon 2012Christian Andrés CasasNoch keine Bewertungen
- DialoguesClinNeurosci 13 101Dokument8 SeitenDialoguesClinNeurosci 13 101Fira KhasanahNoch keine Bewertungen
- Non-Tuberculous Mycobacterial Pulmonary Infections: ReviewDokument12 SeitenNon-Tuberculous Mycobacterial Pulmonary Infections: Reviewmgoez077Noch keine Bewertungen
- Ada 2017Dokument11 SeitenAda 2017IvanCarrilloNoch keine Bewertungen
- Gheorghiu V Et Al 2017Dokument9 SeitenGheorghiu V Et Al 2017Margarida ReisNoch keine Bewertungen
- Asthma An Evidence Based Management UpdateDokument28 SeitenAsthma An Evidence Based Management UpdateYS NateNoch keine Bewertungen
- Der Kay 2018Dokument5 SeitenDer Kay 2018Giovanni HenryNoch keine Bewertungen
- DysphagiaDokument14 SeitenDysphagiaLisbeth TurraNoch keine Bewertungen
- RolqxcaplmonDokument8 SeitenRolqxcaplmonjesus armando mandujano barcenasNoch keine Bewertungen
- PIIS1556086416335158Dokument12 SeitenPIIS1556086416335158Gordana PuzovicNoch keine Bewertungen
- Chen 2015Dokument6 SeitenChen 2015nurminsyahNoch keine Bewertungen
- Treatment of CAP: Stratifying Care Based on SeverityDokument16 SeitenTreatment of CAP: Stratifying Care Based on SeverityditaNoch keine Bewertungen
- Pi Is 2058534917301993Dokument7 SeitenPi Is 2058534917301993hnzzn2bymdNoch keine Bewertungen
- ST Gallen 2021 A OncologyDokument20 SeitenST Gallen 2021 A OncologyJorge Apolo PinzaNoch keine Bewertungen
- EBR Format For StudentsDokument1 SeiteEBR Format For StudentsAPRIL GWEN DALAGANNoch keine Bewertungen
- MEHU130 U2 T74 Colorectal CancerDokument14 SeitenMEHU130 U2 T74 Colorectal CancerStefani AtlleNoch keine Bewertungen
- PHD Thesis On Lung CancerDokument8 SeitenPHD Thesis On Lung Cancerrebeccariveranewhaven100% (2)
- Research Paper PneumoniaDokument7 SeitenResearch Paper Pneumoniawkzcoprhf100% (1)
- Ebola and QuarantineDokument2 SeitenEbola and Quarantinem_rinaldi_sufri3298Noch keine Bewertungen
- Jurnal Perawatan PaliatifDokument16 SeitenJurnal Perawatan Paliatifnurwanda hamidaNoch keine Bewertungen
- Pulmonary Embolism in Children: Cme R ADokument11 SeitenPulmonary Embolism in Children: Cme R Azemenum temesgenNoch keine Bewertungen
- Lobel 2015Dokument5 SeitenLobel 2015Fabianto SantosoNoch keine Bewertungen
- LCTT 7 073Dokument10 SeitenLCTT 7 073Madalina ClivetNoch keine Bewertungen
- Sdra PDFDokument22 SeitenSdra PDFalfred1294Noch keine Bewertungen
- Pulmonary EmbolismDokument14 SeitenPulmonary EmbolismChrysi TsiouriNoch keine Bewertungen
- Necrotizing Pneumonia in Cancer Patients A.8Dokument4 SeitenNecrotizing Pneumonia in Cancer Patients A.8Manisha UppalNoch keine Bewertungen
- Treatment Considerations, and Nursing Implications: Cardiovascular Disease and HIV: PathophysiologyDokument12 SeitenTreatment Considerations, and Nursing Implications: Cardiovascular Disease and HIV: PathophysiologyRicardo Costa da SilvaNoch keine Bewertungen
- Philip C. Doyle - Clinical Care and Rehabilitation in Head and Neck Cancer-Springer International Publishing (2019)Dokument518 SeitenPhilip C. Doyle - Clinical Care and Rehabilitation in Head and Neck Cancer-Springer International Publishing (2019)劉恩齊Noch keine Bewertungen
- Hoffman 2000Dokument7 SeitenHoffman 2000jenny12Noch keine Bewertungen
- 3 The Risk of Second Primary Tumors in Head and Neck Cancer. A Systematic ReviewDokument11 Seiten3 The Risk of Second Primary Tumors in Head and Neck Cancer. A Systematic Review2211801733Noch keine Bewertungen
- Risk Factors For Drug-Resistant Streptococcus Pneumoniae and Antibiotic Prescribing Practices in Outpatient Community-Acquired PneumoniaDokument4 SeitenRisk Factors For Drug-Resistant Streptococcus Pneumoniae and Antibiotic Prescribing Practices in Outpatient Community-Acquired PneumoniakingkinresmytaNoch keine Bewertungen
- Dyspnea and Fatigue Trends Predict Heart Failure OutcomesDokument8 SeitenDyspnea and Fatigue Trends Predict Heart Failure Outcomesabraham rumayaraNoch keine Bewertungen
- Incidence and Risk Factors For Ventilator Associated Pneumon 2007 RespiratorDokument6 SeitenIncidence and Risk Factors For Ventilator Associated Pneumon 2007 RespiratorTomasNoch keine Bewertungen
- Asthma Exacerbations: Origin, Effect, and PreventionDokument10 SeitenAsthma Exacerbations: Origin, Effect, and PreventionGabriNoch keine Bewertungen
- Primer: Head and Neck Squamous Cell CarcinomaDokument22 SeitenPrimer: Head and Neck Squamous Cell CarcinomayohanasmjtNoch keine Bewertungen
- Primer: Head and Neck Squamous Cell CarcinomaDokument22 SeitenPrimer: Head and Neck Squamous Cell CarcinomaRashmeeta ThadhaniNoch keine Bewertungen
- HHS Public Access: Lung Cancer: Biology and Treatment OptionsDokument58 SeitenHHS Public Access: Lung Cancer: Biology and Treatment OptionsStéphanie DWNoch keine Bewertungen
- Current Status of Pain Management in ChildrenDokument7 SeitenCurrent Status of Pain Management in ChildrenHanifa Nur AfifahNoch keine Bewertungen
- Brunei Scholarship Application FormDokument15 SeitenBrunei Scholarship Application FormAbdul Khalik AssufiNoch keine Bewertungen
- Name: Vicky Dian Febriani NIM: I31110031Dokument3 SeitenName: Vicky Dian Febriani NIM: I31110031Hanifa Nur AfifahNoch keine Bewertungen
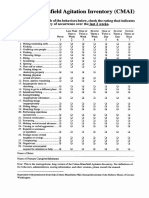
- 738 CMAI Scale5b25d PDFDokument1 Seite738 CMAI Scale5b25d PDFShes-Jap Te NdryshmeNoch keine Bewertungen
- Contoh Soal Uji Kompetensi Keperawatan KomunitasDokument39 SeitenContoh Soal Uji Kompetensi Keperawatan KomunitasUmairohSetengahTiga67% (3)
- Humor TherapyDokument9 SeitenHumor TherapyHanifa Nur AfifahNoch keine Bewertungen
- Skema Rantai Pemutus InfeksiDokument1 SeiteSkema Rantai Pemutus InfeksiHanifa Nur AfifahNoch keine Bewertungen
- Tugas Bing 2Dokument2 SeitenTugas Bing 2Hanifa Nur AfifahNoch keine Bewertungen
- KozierhDokument1 SeiteKozierhHanifa Nur AfifahNoch keine Bewertungen
- Hospital Anxiety and Depression Scale (HADS)Dokument5 SeitenHospital Anxiety and Depression Scale (HADS)BahRunNoch keine Bewertungen
- Emerging Concepts in The Diagnosis and Treatment of Patients With Undifferentiated AngioedemaDokument13 SeitenEmerging Concepts in The Diagnosis and Treatment of Patients With Undifferentiated AngioedemaHanifa Nur AfifahNoch keine Bewertungen
- Daftar PustakaDokument1 SeiteDaftar PustakaHanifa Nur AfifahNoch keine Bewertungen
- Dyspnea Management in Early-Stage Lung Cancer: A Palliative PerspectiveDokument9 SeitenDyspnea Management in Early-Stage Lung Cancer: A Palliative PerspectiveHanifa Nur AfifahNoch keine Bewertungen
- 1hDokument7 Seiten1hHanifa Nur AfifahNoch keine Bewertungen
- KozierhDokument1 SeiteKozierhHanifa Nur AfifahNoch keine Bewertungen
- KozierhDokument1 SeiteKozierhHanifa Nur AfifahNoch keine Bewertungen
- Patient Safety Incident Report Form SummaryDokument9 SeitenPatient Safety Incident Report Form SummaryJhun SantiagoNoch keine Bewertungen
- Myfortic ScripDokument31 SeitenMyfortic Scripjigyasha oarmarNoch keine Bewertungen
- Record Keeping A Pocket Guide 005 343Dokument6 SeitenRecord Keeping A Pocket Guide 005 343ryanbucoNoch keine Bewertungen
- Bahasa Inggris AskepDokument4 SeitenBahasa Inggris AskepMona Indah100% (2)
- Legal and Ethical Issues in Psychiatric NursingDokument38 SeitenLegal and Ethical Issues in Psychiatric NursingElizabeth McKee100% (2)
- Managing Hypertension Through Lifestyle ChangesDokument3 SeitenManaging Hypertension Through Lifestyle ChangespsychyzeNoch keine Bewertungen
- JumpSTART Training Presentation Instructor Course 2016 FinalDokument109 SeitenJumpSTART Training Presentation Instructor Course 2016 FinalvictorioNoch keine Bewertungen
- 0315 DVTDokument28 Seiten0315 DVTEloisa TardioNoch keine Bewertungen
- PHILIPPINES Asthma Consensus Guidelines 2009Dokument134 SeitenPHILIPPINES Asthma Consensus Guidelines 2009Sirias_black50% (2)
- Lower Gastrointestinal BleedingDokument18 SeitenLower Gastrointestinal Bleedingosama nawaysehNoch keine Bewertungen
- Mental Status ExamDokument24 SeitenMental Status ExamRemedios BandongNoch keine Bewertungen
- SOCIETY For ENDOCRINOLOGY ENDOCRINE EMERGENCY GUIDANCE - Emergency Management of Acute Adrenal Insufficiency (Adrenal Crisis) in Adult PatientsDokument3 SeitenSOCIETY For ENDOCRINOLOGY ENDOCRINE EMERGENCY GUIDANCE - Emergency Management of Acute Adrenal Insufficiency (Adrenal Crisis) in Adult PatientsMuhammad ReyhanNoch keine Bewertungen
- Core CompetencyDokument9 SeitenCore CompetencyCharm BarinosNoch keine Bewertungen
- Protooncogene Tyrosineprotein Kinase Srcrelated Mouth Pyogenic Granuloma An Investigation Involving 2 InstanceskermbDokument2 SeitenProtooncogene Tyrosineprotein Kinase Srcrelated Mouth Pyogenic Granuloma An Investigation Involving 2 Instanceskermbsaucebelief33Noch keine Bewertungen
- Blurred VisionDokument7 SeitenBlurred VisionRichi CiriacoNoch keine Bewertungen
- Nurs Fpx 4010 Assessment 3 Interdisciplinary Plan ProposalDokument5 SeitenNurs Fpx 4010 Assessment 3 Interdisciplinary Plan Proposalfarwaamjad771Noch keine Bewertungen
- Regulation For Optical Center and Optometry Services FinalDokument15 SeitenRegulation For Optical Center and Optometry Services FinalsafasayedNoch keine Bewertungen
- Management of Avn HipDokument13 SeitenManagement of Avn Hipterencedsza100% (1)
- TCA CrossDokument6 SeitenTCA CrosssalivaNoch keine Bewertungen
- Foreign and Local Literature Fatigue Among NursesDokument5 SeitenForeign and Local Literature Fatigue Among NursesMay Therese B. BoriborNoch keine Bewertungen
- Surgical Options in The Management of Inguinal Hernias: Mohammed Al-SaffarDokument61 SeitenSurgical Options in The Management of Inguinal Hernias: Mohammed Al-Saffarsgod34Noch keine Bewertungen
- Gastrointestinal Nursing Test BanksDokument2 SeitenGastrointestinal Nursing Test BanksNorhana Manas50% (6)
- Head To Toe Assessment GuideDokument3 SeitenHead To Toe Assessment GuideUmer Masood0% (1)
- Ethical Dilemma Essay 436 Benchmark RRDokument6 SeitenEthical Dilemma Essay 436 Benchmark RRapi-509517114Noch keine Bewertungen
- Vertical Control of Overbite in Mixed Dentition by Trainer SystemDokument7 SeitenVertical Control of Overbite in Mixed Dentition by Trainer SystemJUAN FONSECANoch keine Bewertungen
- Learning Objective: - Explain of Acute AbdomenDokument143 SeitenLearning Objective: - Explain of Acute AbdomenSamuel Sebastian SirapanjiNoch keine Bewertungen
- TB Screening in Pregnancy 1Dokument32 SeitenTB Screening in Pregnancy 1nurfitriwidiNoch keine Bewertungen
- Solved To Evaluate Whether Pre Surgery Patient Attitudes Affect Recovery and UltimateDokument1 SeiteSolved To Evaluate Whether Pre Surgery Patient Attitudes Affect Recovery and UltimateAnbu jaromiaNoch keine Bewertungen
- Universal Precautions PPT FinalDokument50 SeitenUniversal Precautions PPT Finalmarthinfp100% (1)
- Frontal Lobe Dysfunction DiagnosisDokument15 SeitenFrontal Lobe Dysfunction DiagnosisLetitia Claudia DobraniciNoch keine Bewertungen