Beruflich Dokumente
Kultur Dokumente
Ultrasonography in Effusion
Hochgeladen von
Rachmat AnsyoriOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Ultrasonography in Effusion
Hochgeladen von
Rachmat AnsyoriCopyright:
Verfügbare Formate
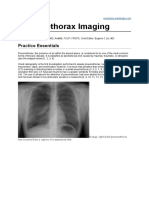
Plevral Grntleme
Ultrasonography in the Diagnosis
and Management of Pleural Diseases
Edwin F. Donnelly, M.D., Ph.D.
Vanderbilt University Medical Center Nashville, TN, USA
e-mail: edwin.donnelly@vanderbilt.edu
Introduction
The role of ultrasonography in the diagnosis and
management of different diseases is every changing because of changes not only ultrasound
technology, but also due to changes in technology in the competing modalities, such as computed tomography and magnetic resonance imaging. Due to the many advantages of ultrasonography, however, including its safety (1), portability, and real-time image display, this modality
continues to play an important and perhaps growing role in modern medicine.
The most common use of ultrasonography in the
thorax has been, and likely will continue to be,
the imaging of the heart. Traditionally, imaging of
the lungs has been limited, at best, because of
very poor transmission of the sound waves through air. However, it has long been recognized
that ultrasonography is quite suitable for imaging
the pleural space. Indeed the real-time response
of ultrasonography has made it the ideal modality
for not only imaging some pleural diseases, but
also for guiding interventions involving the pleural space.
Pleural Effusion
While the soft tissues of the thoracic wall demonstrate a complex pattern when reflecting sound waves, due to the numerous soft tissue interfaces within them, pure fluid such as that seen in a simple
transudative pleural effusion provides an ultrasound
image that is free of echoes and very easy to identify. For this reason, ultrasonography is perhaps the
ideal modality for imaging pleural effusions. Figure
1 illustrates the normal pleura. It can be seen as
bright white line. The lung, deeper to the pleura, is
not seen because the interface between the visceral
pleura and the air results in the reflection of nearly
all of the sound waves, leaving nothing but shadow
(white) visible in the lung. During real time viewing,
the gliding of the pleura can be seen (an important
sign for distinguishing normal lung from pneumothorax). Figure 2, however, demonstrates a large
| Cilt: 2 Say: 3 Yl 2008 |
81
Ultrasonography in the Diagnosis and Management of Pleural Diseases
Figure 2: Transudative pleural effusion. The effusion (eff)
Figure 1: Normal pleural. The transducer contacts the
skin at the point marked by the white arrowheads, and is
oriented to create a sagittal image, where the left side of
the image represents the superior direction. The normal
pleura is seen as a bright white line (black arrowheads).
Deep to the pleura there is only shadowing (bright lines)
from the aerated lung.
is anechoic (black and lacking internal echoes). The image
is oriented the same as in Figure 1. In this image, the diaphragm (arrows) is well outlined by the effusion. While transudative pleural effusions classically appear as anechoic on
ultrasonography, an exudative effusion can have this appearance as well.
transudative pleural effusion. The effusion is easily
seen as a large anechoic (black) area.
It is well-known that pleural effusions can be identified on plain radiography, ultrasonography,
computed tomography (CT) and magnetic resonance imaging (MRI). While CT and MRI may play
a role in the evaluation of some patients (2-4), routine pleural imaging has largely been with either
plain radiography or ultrasonography.
Plain radiography is well-known for its ability to
detect the presence of pleural effusions. And while it has long been established that an upright
chest film can detect as little as 25 cc of pleural
fluid5, or even less with a decubitus view (6), it
has also been long-established that ultrasonography is more sensitive and specific for the detection of pleural effusions, especially smaller effusions (7,8). Indeed, the paper by Colins, et al (5) found that up to 525 mL of pleural fluid could be
present without visible blunting of the costophrenic angle on an upright PA view of the chest. Fi-
82
| TTD Plevra Blteni |
Figure 3: Small pleural effusion. The effusion (eff) is
smaller than that of Figure 2, but otherwise has similar
imaging characteristics on ultrasonography. The diaphragm (arrow) is partially outlined by the effusion. This effusion was not visible on portable chest radiography.
gure 3 illustrates a small pleural effusion that was
detected by ultrasonography but not visible on a
supine chest radiograph.
Not only does ultrasound excel in the detection of
pleural fluid, but it is also superior to plain radiography in quantifying the amount of fluid present
in the pleural space (9) While not always of criti-
Edwin F. Donnelly, M.D., Ph.D.
cal importance, it is often useful to determine the
size of a pleural effusion because of its significance in determining etiology (10), prognosis (11) or
in guiding treatment (12-15).
Finally, ultrasonography can play a role in the
characterization of pleural effusions as transudates
or exudates. Typically, pleural effusions on ultrasonography can be classified into three groups;
1. Anechoic,
2. Complex, non-septated,
3. Septated. An anechoic pleural effusion appears
as homogeneously black. There is general agreement that both transudates and exudates may appear as anechoic fluid collections on ultrasonography (16,17). A complex, non-septated pleural
effusion shows some internal echoes. This pattern
can be seen in both transudates and exudates
(18). The final pattern, septated, however, is exclusively seen in exudates (16,17). Thus, the anechoic pleural effusion shown in Figure 2 could be
either a transudate or an exudate (though it was
shown by clinical history and chemical analysis to
be a transudate), the effusion shown in Figure 4
must be an exudate because of the presence of
prominent septations throughout it.
Figure 4: Septated pleural effusions. There are thick septations (arrows) in this pleural effusion. The presence of
septations is highly specific for exudative pleural effusion.
Thoracentesis
The work up or treatment of a pleural effusion often requires thoracentesis (19). Because of its portability and real-time imaging, ultrasonography
can be used for guidance during thoracentesis.
The use of ultrasonographic guidance has been
shown to be both safe (20-24) and effective
(25,26). While there is continued debate about
whether all thoracenteses should be performed
with ultrasonography, it is certainly preferred in
complicated cases (small or loculated pleural effusions, large body habitus or patients under mechanical ventilation) (22,23) and in cases where an
attempt without ultrasonographic guidance has
been made and failed (27,28).
In some cases, such as empyema, it may be necessary to place an indwelling percutaneous drainage catheter within the pleural space (29,30). While management by blind placement of a large-bore chest tube is often appropriate (30), ultrasound
guidance can be used for the accurate and safe
placement of small-bore drainage catheters (3133). Figure 5 illustrates an ultrasonographic ima-
Figure 5: Ultrasonographically-guided chest tube placement. The chest tube (arrows) is well seen within the pleural space. The visceral pleura (arrowhead) is visible just deep to the chest tube.
| Cilt: 2 Say: 3 Yl 2008 |
83
Ultrasonography in the Diagnosis and Management of Pleural Diseases
ge that confirms appropriate positioning of a
chest tube into the pleural space.
Pneumothorax
While the role of ultrasound in the diagnosis of
pneumothorax is not nearly as well-established as
for pleural effusion, it is known that ultrasound
can be used for accurate and rapid diagnosis of
pneumothorax (34). On a static image, the shadowing caused by air in the pleural space cannot
be distinguished from air in the lung parenchyma.
During real-time imaging, however, a pneumothorax can be diagnosed due to the absence of the
normally observed gliding between the two layers
of the pleura (35,36). While it is not suggested
that ultrasonography replace plain radiography
for the routine diagnosis of pneumothorax, there
will be many times when ultrasonography is already being performed for another indication, and
the additional scanning for the presence of a pneumothorax can be easily performed. Perhaps the
most-studied scenario is that of the trauma patient, where ultrasound may be utilized as a part of
the focused assessment with sonography for trauma (FAST) exam or a related protocol (37-39). As
ultrasonography is used more commonly for interventional procedures in the chest, such as central line placement and thoracentesis, it is possible that more attention will be placed on using the
ultrasonography machine already in the room to
make the immediate diagnosis of pneumothorax
when that complication occurs.
Pleural Masses
Both benign and malignant masses may arise in
the pleura. In addition, the pleura may be involved
secondarily by either direct extension or hematogenous spread of malignancy. In general, ultrasonography does not play a role in diagnosing the
different types of benign (lipoma, solitary fibrous
tumor of the pleura, and others) or malignant
(malignant mesothelioma and metastases) tumors, and ultrasonography generally cannot even
reliably distinguish benign tumors from malignant
ones (43). The role of ultrasonography in the evaluation of pleural masses is largely that of localization and guidance for percutaneous biopsy (44) Figure 6 shows a mass (Ewings sarcoma) that had
directly invaded into the pleural space.
Pleural Biopsy
Biopsy of the pleura may be necessary in cases
where thoracentesis fails to provide a diagnosis in
a suspected exudative effusion, or in cases of
pleural thickening or pleural masses where histology is required to make a diagnosis (45). While
both computed tomography and ultrasonog-
Pleural Thickening
Ultrasonography can be used to readily distinguish pleural fluid from pleural thickening (40,41).
The use of color Doppler ultrasound, which is sensitive to motion and renders pixels in color where
motion is detected but grayscale where no motion is detected, will demonstrate the motion of
pleural fluid during the cardiac and respiratory
cycles, but will reveal no motion (no color) in
pleural thickening (42).
84
| TTD Plevra Blteni |
Figure 6: Pleural mass. This Ewings sarcoma (mass) directly invaded the pleural space. There is an associated malignant pleural effusion (eff) visible adjacent to the mass.
The effusion also outlines the diaphragm (arrowheads).
Edwin F. Donnelly, M.D., Ph.D.
raphy can be used safely as image guidance for
pleural biopsies, (46-48) ultrasonography can be
particularly useful in guiding pleural biopsies
when there is a focal lesion that is well-seen with
that modality and in cases where real-time visualization of the biopsy needle is felt to be important.
Conclusion
Ultrasonography plays an important and growing
role in the diagnosis and management of pleural disease. Despite the increasing use of computed tomography, ultrasonographys ability to provide realtime images, its portability, low cost and unique basis of image contrast make it useful for a large number of both diagnostic and therapeutic scenarios.
REFERENCES
1.
Stewart HF, Stratmeyer ME, Center for Devices and
Radiological Health (US.). An Overview of ultrasound:
Theory, measurement, medical applications, and biological effects. US. Dept. of Health and Human Services Public Health Service Food and Drug Administration Center for Devices and Radiological Health: Rockville, Md; 1985.
2.
McLoud TC, Flower CD. Imaging the pleura: Sonography, CT, and MR imaging. AJR Am J Roentgenol
1991; 156: 1145-53.
3.
Evans AL, Gleeson FV. Radiology in pleural disease:
state of the art. Respirology 2004; 9: 300-12.
4.
Qureshi NR, Gleeson FV. Imaging of pleural disease.
Clin Chest Med 2006; 27: 193-213.
5.
Colins JD et al. Minimal detectable pleural effusions. A
roentgen pathology model. Radiology 1972; 105: 51-3.
6.
Moskowitz H, Platt RT, Schachar R, Mellins H. Roentgen
visualization of minute pleural effusion. An experimental
study to determine the minimum amount of pleural fluid visible on a radiograph. Radiology 1973; 109: 33-5.
10. Porcel JM, Vives M. Etiology and pleural fluid characteristics of large and massive effusions. Chest 2003;
124: 978-83.
11. Colice GL, et al. Medical and surgical treatment of parapneumonic effusions: An evidence-based guideline.
Chest 2000; 118: 1158-1171.
12. Light RW, George RB. Incidence and significance of
pleural effusion after abdominal surgery. Chest 1976;
69: 621-25.
13. Estenne M, Yernault JC, De Troyer A. Mechanism of
relief of dyspnea after thoracocentesis in patients with
large pleural effusions. Am J Med 1983; 74: 813-9.
14. Leslie WK, Kinasewitz GT. Clinical characteristics of
the patient with nonspecific pleuritis. Chest 1988; 94:
603-8.
15. Balik M, et al. Ultrasound estimation of volume of
pleural fluid in mechanically ventilated patients. Intensive Care Med 2006; 32: 318-21.
16. Yang PC et al. Value of sonography in determining the
nature of pleural effusion: Analysis of 320 cases. AJR
Am J Roentgenol 1992; 159: 29-33.
17. Sajadieh H, Afzali F, Sajadieh V, Sajadieh A. Ultrasound as an alternative to aspiration for determining
the nature of pleural effusion, especially in older people. Ann N Y Acad Sci 2004; 1019: 585-92.
18. Chen HJ et al. Sonographic appearances in transudative pleural effusions: Not always an anechoic pattern.
Ultrasound Med Biol 2008; 34: 362-9.
19. Bartter T, Santarelli R, Akers SM, Pratter MR. The evaluation of pleural effusion. Chest 1994; 106: 1209-14.
20. O'Moore PV, et al. Sonographic guidance in diagnostic and therapeutic interventions in the pleural space.
AJR Am J Roentgenol 1987; 149: 1-5.
21. Grogan DR, et al. Complications associated with thoracentesis. A prospective, randomized study comparing three different methods. Arch Intern Med 1990;
150: 873-7.
22. Jones PW, et al. Ultrasound-guided thoracentesis: is it
a safer method? Chest 2003; 123: 418-23.
7.
Gryminski J, Krakowka P, Lypacewicz G. The diagnosis of pleural effusion by ultrasonic and radiologic
techniques. Chest 1976; 70: 33-7.
23. Mayo PH, Goltz HR, Tafreshi M, Doelken P. Safety of
ultrasound-guided thoracentesis in patients receiving
mechanical ventilation. Chest 2004; 125: 1059-62.
8.
Emamian SA, Kaasbol MA, Olsen JF, Pedersen JF. Accuracy of the diagnosis of pleural effusion on supine
chest X-ray. Eur Radiol 1997; 7: 57-60.
24. Barnes TW, et al. Sonographically guided thoracentesis and rate of pneumothorax. J Clin Ultrasound 2005;
33: 442-446.
9.
Eibenberger KL, et al. Quantification of pleural effusions: sonography versus radiography. Radiology 1994;
191: 681-4.
25. Tsai TH, Yang PC. Ultrasound in the diagnosis and
management of pleural disease. Curr Opin Pulm Med
2003; 9: 282-90.
| Cilt: 2 Say: 3 Yl 2008 |
85
Ultrasonography in the Diagnosis and Management of Pleural Diseases
26. Diacon AH, Brutsche MH, Soler M. Accuracy of pleural
puncture sites: A prospective comparison of clinical
examination with ultrasound. Chest 2003; 123: 43641.
27. Hirsch JH, Rogers JV, Mack LA. Real-time sonography
of pleural opacities. AJR Am J Roentgenol 1981; 136:
297-301.
28. Weingardt JP, et al. Ultrasound findings following failed, clinically directed thoracenteses. J Clin Ultrasound
1994; 22: 419-26.
29. Sasse S, et al. The effects of early chest tube placement on empyema resolution. Chest 1997; 111:
1679-83.
30. Davies CW, Gleeson FV, Davies RJ. BTS guidelines for
the management of pleural infection. Thorax 2003;
58 (Suppl 2): 18-28.
31. Stavas J, vanSonnenberg E, Casola G, Wittich GR. Percutaneous drainage of infected and noninfected thoracic fluid collections. J Thorac Imaging 1987; 2: 80-7.
32. Silverman SG, et al. Thoracic empyema: Management
with image-guided catheter drainage. Radiology
1988; 169: 5-9.
33. Ulmer JL, Choplin RH, Reed JC. Image-guided catheter
drainage of the infected pleural space. J Thorac Imaging 1991; 6: 65-73.
34. Jaffer U, McAuley D. Best evidence topic report. Transthoracic ultrasonography to diagnose pneumothorax
in trauma. Emerg Med J 2005; 22: 504-5.
35 Targhetta R, et al. Ultrasonic signs of pneumothorax:
Preliminary work. J Clin Ultrasound 1993; 21: 24550.
36. Dulchavsky SA, et al. Prospective evaluation of thoracic ultrasound in the detection of pneumothorax. J
Trauma 2001; 50: 201-5.
37. Kirkpatrick AW, et al. Hand-held thoracic sonography
for detecting post-traumatic pneumothoraces: The Extended Focused Assessment with Sonography for
Trauma (EFAST). J Trauma 2004; 57: 288-95.
86
| TTD Plevra Blteni |
38. Knudtson JL, Dort JM, Helmer SD, Smith RS. Surgeonperformed ultrasound for pneumothorax in the trauma suite. J Trauma 2004; 56: 527-30.
39. Korner M, et al. Current Role of Emergency US in Patients with Major Trauma. Radiographics 2008; 28:
225-42.
40. Maskell NA, Butland RJ. BTS guidelines for the investigation of a unilateral pleural effusion in adults. Thorax 2003; 58 (Suppl 2): 8-17.
41. Wu RG, et al. Image comparison of real-time grayscale ultrasound and color Doppler ultrasound for use
in diagnosis of minimal pleural effusion. Am J Respir
Crit Care Med 1994; 150: 510-4.
42. Wu RG, Yang PC, Kuo SH, Luh KT. "Fluid color" sign:
A useful indicator for discrimination between pleural
thickening and pleural effusion. J Ultrasound Med
1995; 14: 767-9.
43. Mayo PH, Doelken P. Pleural ultrasonography. Clin
Chest Med 2006; 27: 215-27.
44. Bruns AS, Mastronarde JG. Imaging of pleural masses:
which to choose? Respir Med 2008; 102: 328-31.
45. Rahman NM, Gleeson FV. Image-guided pleural biopsy. Curr Opin Pulm Med 2008; 14: 331-6.
46. Chang DB, et al. Ultrasound-guided pleural biopsy
with Tru-Cut needle. Chest 1991; 100: 1328-33.
47. Adams RF, Gleeson FV. Percutaneous image-guided
cutting-needle biopsy of the pleura in the presence of
a suspected malignant effusion. Radiology 2001;
219: 510-4.
48. Benamore RE, Scott K, Richards CJ, Entwisle JJ. Imageguided pleural biopsy: Oiagnostic yield and complications. Clin Radiol 2006; 61: 700-5.
Das könnte Ihnen auch gefallen
- Thoracic Ultrasound and Integrated ImagingVon EverandThoracic Ultrasound and Integrated ImagingFrancesco FelettiNoch keine Bewertungen
- ABC of Pleural DiseasesVon EverandABC of Pleural DiseasesNajib M. RahmanNoch keine Bewertungen
- Guide To USDokument11 SeitenGuide To USAdel HamadaNoch keine Bewertungen
- Ultrasound diagnosis and management of pleural effusionDokument5 SeitenUltrasound diagnosis and management of pleural effusionegerpratamaNoch keine Bewertungen
- The V-Line: A Sonographic Aid For The Confirmation of Pleural FluidDokument4 SeitenThe V-Line: A Sonographic Aid For The Confirmation of Pleural FluidAlpi ApriansahNoch keine Bewertungen
- 1229 6490 1 PB PDFDokument10 Seiten1229 6490 1 PB PDFSitti_HazrinaNoch keine Bewertungen
- Ultrasound of The Thorax (Noncardiac)Dokument13 SeitenUltrasound of The Thorax (Noncardiac)ludiegues752Noch keine Bewertungen
- Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT FindingsDokument18 SeitenImaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT FindingsbagusNoch keine Bewertungen
- Author Section Editor Deputy Editor Contributor DisclosuresDokument10 SeitenAuthor Section Editor Deputy Editor Contributor DisclosuresannisNoch keine Bewertungen
- English Journal PetDokument51 SeitenEnglish Journal PetM. REZA RAMDHIKANoch keine Bewertungen
- 3.pleural Effusion Imaging - Overview, Radiography, Computed TomographyDokument32 Seiten3.pleural Effusion Imaging - Overview, Radiography, Computed TomographyAchmadRizaNoch keine Bewertungen
- Pneumothoraks Jurnal RadiologiDokument9 SeitenPneumothoraks Jurnal RadiologiRachmi MerrinaNoch keine Bewertungen
- Ecografia Toracica PDFDokument12 SeitenEcografia Toracica PDFCristinaLucanNoch keine Bewertungen
- PIIS0749070413000729Dokument25 SeitenPIIS0749070413000729Juan Carlos MezaNoch keine Bewertungen
- Blue Protocol. Lung Ultrasound in The Critically IllDokument12 SeitenBlue Protocol. Lung Ultrasound in The Critically IllRomina Alfonsina Decap CarrascoNoch keine Bewertungen
- Malignant Mesothelioma ImagingDokument22 SeitenMalignant Mesothelioma ImagingFatya WelinsaNoch keine Bewertungen
- Bedside Lung Ultrasound Versus Chest X-Ray Use in The Emergency DepartmentDokument3 SeitenBedside Lung Ultrasound Versus Chest X-Ray Use in The Emergency DepartmentharnellaNoch keine Bewertungen
- Content ServerDokument12 SeitenContent ServerIrvan Dwi FitraNoch keine Bewertungen
- Introduction To Ultrasound in Emergency Department: A&E Medical MeetingDokument24 SeitenIntroduction To Ultrasound in Emergency Department: A&E Medical MeetingdhanudgNoch keine Bewertungen
- Ultrasound Differentiation of Benign Versus Malignant Adnexal Masses - UpToDateDokument31 SeitenUltrasound Differentiation of Benign Versus Malignant Adnexal Masses - UpToDateRamackNoch keine Bewertungen
- 4.pneumothorax Imaging - Practice Essentials, Radiography, Computed TomographyDokument11 Seiten4.pneumothorax Imaging - Practice Essentials, Radiography, Computed TomographyAchmadRizaNoch keine Bewertungen
- POCUS NeumotoraxDokument20 SeitenPOCUS NeumotoraxRaydel ManuelNoch keine Bewertungen
- Pi Is 00960217166003657Dokument15 SeitenPi Is 00960217166003657Jesicca SNoch keine Bewertungen
- Rapid Diagnosis and Treatment of A Pleural Effusion in A 24-Year-Old ManDokument4 SeitenRapid Diagnosis and Treatment of A Pleural Effusion in A 24-Year-Old ManJonathan EdbertNoch keine Bewertungen
- Testicular Ultrasound: A Concise GuideDokument26 SeitenTesticular Ultrasound: A Concise GuideElshaer MohammedNoch keine Bewertungen
- Thesis Endobronchial UltrasoundDokument4 SeitenThesis Endobronchial Ultrasoundafknikfgd100% (2)
- Clinical Applications of Transthoracic UltrasoundDokument20 SeitenClinical Applications of Transthoracic UltrasoundFabiana Gonzalez da NóbregaNoch keine Bewertungen
- Jurnal 2Dokument0 SeitenJurnal 2Seftiana SaftariNoch keine Bewertungen
- Ultrasound A CL 2021Dokument17 SeitenUltrasound A CL 2021Alejandra SanchezNoch keine Bewertungen
- Thoracic ultrasound in horses: Evaluating the pleura and pulmonary parenchymaDokument8 SeitenThoracic ultrasound in horses: Evaluating the pleura and pulmonary parenchymaNatalia J. VidalNoch keine Bewertungen
- Signs in Chest ImagingDokument13 SeitenSigns in Chest ImagingSusuru AsepNoch keine Bewertungen
- Case 16797Dokument7 SeitenCase 16797eduardoNoch keine Bewertungen
- Imaging in Acute Respiratory Distress Syndrome: ReviewDokument13 SeitenImaging in Acute Respiratory Distress Syndrome: ReviewIva SeptianingsihNoch keine Bewertungen
- Review Article: The Spleen Revisited: An Overview On Magnetic Resonance ImagingDokument16 SeitenReview Article: The Spleen Revisited: An Overview On Magnetic Resonance ImagingrusselioNoch keine Bewertungen
- Usg PneumotoraksDokument7 SeitenUsg Pneumotoraksdicky wahyudiNoch keine Bewertungen
- Ultrasound For "Lung Monitoring" of Ventilated PatientsDokument11 SeitenUltrasound For "Lung Monitoring" of Ventilated PatientsCarlos FloresNoch keine Bewertungen
- Rambhia 2016Dokument24 SeitenRambhia 2016Heru SigitNoch keine Bewertungen
- NRes1 AssignmentDokument2 SeitenNRes1 AssignmentAinee MeuvinNoch keine Bewertungen
- Pleural Ultrasonography: A Useful Tool for Imaging Pleural DiseasesDokument13 SeitenPleural Ultrasonography: A Useful Tool for Imaging Pleural DiseasesmlannesNoch keine Bewertungen
- Advances in Trauma UltrasoundDokument12 SeitenAdvances in Trauma UltrasoundBruce Fredy Chino ChambillaNoch keine Bewertungen
- Thora CosDokument20 SeitenThora CosDani VélezNoch keine Bewertungen
- EJMCM - Volume 8 - Issue 4 - Pages 17-38Dokument22 SeitenEJMCM - Volume 8 - Issue 4 - Pages 17-38Munazzah MehakNoch keine Bewertungen
- Lungultrasoundfor Pulmonarycontusions: Samuel A. DickerDokument11 SeitenLungultrasoundfor Pulmonarycontusions: Samuel A. DickerCarlosfff1 QueirozNoch keine Bewertungen
- Pathognomonic Imaging Signs in Abdominal RadiologyDokument11 SeitenPathognomonic Imaging Signs in Abdominal RadiologyifzarNoch keine Bewertungen
- Imaging Small Pleural EffusionsDokument6 SeitenImaging Small Pleural EffusionsiiffaaffiiNoch keine Bewertungen
- UltrasoundTraumaCh02 Fast ExamDokument23 SeitenUltrasoundTraumaCh02 Fast Exam108dudleyNoch keine Bewertungen
- Differential Diagnosis of Pleural Effusion Syndrome GuideDokument26 SeitenDifferential Diagnosis of Pleural Effusion Syndrome GuideSriram Lakshmanan LNoch keine Bewertungen
- Routine Use of Point-of-Care Lung Ultrasound During The COVID-19 PandemicDokument4 SeitenRoutine Use of Point-of-Care Lung Ultrasound During The COVID-19 PandemicOswaldo MontesNoch keine Bewertungen
- Signs in Chest ImagingDokument13 SeitenSigns in Chest ImagingIulia DNoch keine Bewertungen
- Blue ProtocolDokument3 SeitenBlue ProtocolDorica GiurcaNoch keine Bewertungen
- Chapter 10 Sonographic Approach To Acute Abdominal PainDokument13 SeitenChapter 10 Sonographic Approach To Acute Abdominal PainSyed Shahrul Naz SyedNoch keine Bewertungen
- WSAVA Proceedings Highlights HRCT for Small Animal Lung ImagingDokument5 SeitenWSAVA Proceedings Highlights HRCT for Small Animal Lung ImagingKiki D. RestikaNoch keine Bewertungen
- Pneumotorax Syr06lDokument53 SeitenPneumotorax Syr06lflavia_craNoch keine Bewertungen
- Journal Radiologi 3Dokument14 SeitenJournal Radiologi 3WinayNayNoch keine Bewertungen
- Healthcare 09 01015Dokument20 SeitenHealthcare 09 01015Sori B. Requena C.Noch keine Bewertungen
- Ultrasound of The Pediatric Chest2019Dokument13 SeitenUltrasound of The Pediatric Chest2019JHONATAN MATA ARANDANoch keine Bewertungen
- Basic Radiographic PrinciplesDokument93 SeitenBasic Radiographic PrinciplesOdalis Lizeth Zamora100% (2)
- Lung Ultrasound: A New Tool For The CardiologistDokument9 SeitenLung Ultrasound: A New Tool For The CardiologistNag Mallesh RaoNoch keine Bewertungen
- Value of Chest Ultrasound in Diagnosis of Community Acquired PneumoniaDokument5 SeitenValue of Chest Ultrasound in Diagnosis of Community Acquired PneumoniaHarlan SiMarmutNoch keine Bewertungen
- Pulmonary Functional Imaging: Basics and Clinical ApplicationsVon EverandPulmonary Functional Imaging: Basics and Clinical ApplicationsYoshiharu OhnoNoch keine Bewertungen
- Bahan IKMDokument18 SeitenBahan IKMRifqiNoch keine Bewertungen
- Practice Guidelines 2001Dokument81 SeitenPractice Guidelines 2001Hamid Aizaz ChathaNoch keine Bewertungen
- Posterior Hipofisis DysfunctionDokument9 SeitenPosterior Hipofisis DysfunctionRachmat AnsyoriNoch keine Bewertungen
- UA Dan KardioDokument10 SeitenUA Dan KardioRachmat AnsyoriNoch keine Bewertungen
- Treatment of Burns in The First 24 HoursDokument10 SeitenTreatment of Burns in The First 24 HoursSurya Nirmala DewiNoch keine Bewertungen
- Gonorrhea MortalityDokument24 SeitenGonorrhea MortalityRachmat AnsyoriNoch keine Bewertungen
- A Guide To Diagnosis Iron Deficiency PDFDokument6 SeitenA Guide To Diagnosis Iron Deficiency PDFRachmat AnsyoriNoch keine Bewertungen
- Epidemiology of Liver Disease PDFDokument64 SeitenEpidemiology of Liver Disease PDFRachmat AnsyoriNoch keine Bewertungen
- Japanese Twins Growth ChartDokument10 SeitenJapanese Twins Growth ChartRachmat AnsyoriNoch keine Bewertungen
- Bleeding in Early and Late: PregnancyDokument31 SeitenBleeding in Early and Late: Pregnancysny007Noch keine Bewertungen
- Chart Pertumbuhan AnakDokument1 SeiteChart Pertumbuhan AnakWahyudi Pratama HarliNoch keine Bewertungen
- DyspepsiaDokument25 SeitenDyspepsiaCynthia StefanusNoch keine Bewertungen
- Values Patient CenteredDokument4 SeitenValues Patient CenteredRachmat AnsyoriNoch keine Bewertungen
- Normal Newborn Care: Advances in Maternal and Neonatal HealthDokument23 SeitenNormal Newborn Care: Advances in Maternal and Neonatal HealthRachmat AnsyoriNoch keine Bewertungen
- Wound Closure ManualDokument127 SeitenWound Closure ManualDougyStoffell100% (5)
- KDIGO AKI Guideline DownloadDokument141 SeitenKDIGO AKI Guideline DownloadSandi AuliaNoch keine Bewertungen
- Sulindac Vs Ibuprofen in SprainsDokument5 SeitenSulindac Vs Ibuprofen in SprainsRachmat AnsyoriNoch keine Bewertungen
- Itopride and DyspepsiaDokument9 SeitenItopride and DyspepsiaRachmat AnsyoriNoch keine Bewertungen
- Steroids As Adjuvant Treatment of Sore Throat in Acute Bacterial PharyngitisDokument3 SeitenSteroids As Adjuvant Treatment of Sore Throat in Acute Bacterial PharyngitisLucky PratamaNoch keine Bewertungen
- Cryotherapy in Ankle SprainsDokument7 SeitenCryotherapy in Ankle SprainsRachmat AnsyoriNoch keine Bewertungen
- Ankle Sprains ManagementDokument7 SeitenAnkle Sprains ManagementRachmat AnsyoriNoch keine Bewertungen
- Kolik AbdomenDokument7 SeitenKolik Abdomenuflah_Noch keine Bewertungen
- Introduction To Laboratory Tests Handout VersionDokument58 SeitenIntroduction To Laboratory Tests Handout VersionRachmat AnsyoriNoch keine Bewertungen
- Management of Endometriosis-Associated PainDokument10 SeitenManagement of Endometriosis-Associated PainRaul Garcia Salas CastilloNoch keine Bewertungen
- Chapter 3 NotesDokument10 SeitenChapter 3 Notesmjamie12345Noch keine Bewertungen
- Ethical Issues at The End of LifeDokument24 SeitenEthical Issues at The End of Lifeorderstuff36160100% (1)
- Stress Management ResourcesDokument58 SeitenStress Management ResourcesKomal JoshiNoch keine Bewertungen
- CBT For Depression in Young People Orygen 2018Dokument106 SeitenCBT For Depression in Young People Orygen 2018Surya MohanNoch keine Bewertungen
- Health Care Delivery System in IndiaDokument9 SeitenHealth Care Delivery System in IndiaPrabhjot Singh100% (4)
- Botox G Art 2016Dokument13 SeitenBotox G Art 2016Anamaria ZaccoloNoch keine Bewertungen
- Anal FissuresDokument2 SeitenAnal FissureskhadzxNoch keine Bewertungen
- Mayjune 07 WebDokument40 SeitenMayjune 07 WebDave100% (2)
- Dermnet NZ: MelasmaDokument5 SeitenDermnet NZ: MelasmaWin TheinNoch keine Bewertungen
- Dialog EFN2 Sudarmi 30140114040Dokument2 SeitenDialog EFN2 Sudarmi 30140114040sudarmiNoch keine Bewertungen
- Mental RetardationDokument34 SeitenMental RetardationJhon Cristian M. TolentinoNoch keine Bewertungen
- Mobility: How To Fix The 3 Most Common Mobility IssuesDokument32 SeitenMobility: How To Fix The 3 Most Common Mobility Issuespablo ito100% (4)
- Acute Intestinal Failure.11Dokument6 SeitenAcute Intestinal Failure.11albimar239512Noch keine Bewertungen
- Info-What Is Anger PDFDokument1 SeiteInfo-What Is Anger PDFClarisse MachadoNoch keine Bewertungen
- Peds PresentationDokument31 SeitenPeds Presentationapi-247218432Noch keine Bewertungen
- Blood CollectionDokument25 SeitenBlood Collectionطاهرة حربية AlcaldeNoch keine Bewertungen
- Epworth Richmond - Agency Staff Orientation Booklet MAY 2016Dokument33 SeitenEpworth Richmond - Agency Staff Orientation Booklet MAY 2016Anonymous BaD9jQNoch keine Bewertungen
- Traumatic Brain Injury and Cerebral ResuscitationDokument56 SeitenTraumatic Brain Injury and Cerebral ResuscitationsyahirNoch keine Bewertungen
- Rituparna ChatterjeeDokument2 SeitenRituparna ChatterjeeDRIVECURENoch keine Bewertungen
- Revista Chilena de Neuro-Psiquiatría: La Persona Del Terapeuta: Eje Fundamental de Todo Proceso TerapéuticoDokument13 SeitenRevista Chilena de Neuro-Psiquiatría: La Persona Del Terapeuta: Eje Fundamental de Todo Proceso TerapéuticocysagasNoch keine Bewertungen
- Jurnal Frozen PDFDokument27 SeitenJurnal Frozen PDFFahmi MiNoch keine Bewertungen
- Self-motivation quiz tipsDokument1 SeiteSelf-motivation quiz tipsRose D GuzmanNoch keine Bewertungen
- Endotracheal Tube ETT Insertion IntubationDokument3 SeitenEndotracheal Tube ETT Insertion IntubationmochkurniawanNoch keine Bewertungen
- Letty KuanDokument1 SeiteLetty KuanchrizthineeNoch keine Bewertungen
- Mindfulness Group Lesson PlansDokument3 SeitenMindfulness Group Lesson Plansapi-469144202Noch keine Bewertungen
- Camptodactyly: Christian Dumontier MD, PHD Centre de La Main Guadeloupe - FwiDokument49 SeitenCamptodactyly: Christian Dumontier MD, PHD Centre de La Main Guadeloupe - FwiProfesseur Christian Dumontier100% (1)
- Psycological EssayDokument2 SeitenPsycological Essayapi-431658211Noch keine Bewertungen
- Pengaruh Range of Motion (Rom) Aktif Dan Pasif Terhadap Rentang Gerak Pada Lansia Yang Mengalami Artitis Rematoid Di Kota BengkuluDokument11 SeitenPengaruh Range of Motion (Rom) Aktif Dan Pasif Terhadap Rentang Gerak Pada Lansia Yang Mengalami Artitis Rematoid Di Kota BengkuluNanda MaisyuriNoch keine Bewertungen
- Menopause and It's Effects On Your Sex Life in MarriageDokument27 SeitenMenopause and It's Effects On Your Sex Life in MarriageDebi WalterNoch keine Bewertungen