Beruflich Dokumente
Kultur Dokumente
Nurs0intravenous Insertion2d22 - 27
Hochgeladen von
Danecca Rubio Dela CruzOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Nurs0intravenous Insertion2d22 - 27
Hochgeladen von
Danecca Rubio Dela CruzCopyright:
Verfügbare Formate
Abu Dhabi NURSE
Revisiting Peripheral
Intravenous Cannula Insertion
By Nawal Ahmed, DipNsg
Nurse Educator, Mafraq Hospital
On completion of this article, you will be able to:
l
Apply venous system anatomy and physiology
to identify peripheral veins appropriate for peripheral intravenous insertion
Review peripheral intravenous insertion technique
Identify potential complications related to peripheral cannulation
NOTE: This article may be used for preparation
for a facility based competency based programme;
it is not intended to replace certification or competency assessments required in some facilities prior
to independent practice.
Introduction
Mastering peripheral intravenous (IV) insertion is a
challenging clinical skill. If you are like many nurses,
you may approach some IV insertion with apprehension. Inserting a peripheral IV catheter tests your
skills, takes time, and may be painful for your patient.
Your keys to successful IV insertion starts are assessing your patient's needs, distending the patient's
veins, and selecting an appropriate site and device.
This knowledge will assist the professional nurse to
make some important decisions as to where to site
the IV, what type of IV accessed is best used and
care for the patient receiving intravenous therapy.
Peripheral intravenous insertion
The first barrier to successful peripheral intravenous
insertion is the skin. The skin acts as a barrier between the outside environment and internal organs.
The risk for infection increases whenever the skin is
broken. An infusion access device perforates the skin,
interrupts the integrity of the barrier and increases
the risk for infection. Strict aseptic technique for peripheral intravenous insertion, care and maintenance
of the site is important. The skin itself serves multiple functions including; mechanical barrier to micro-organisms, regulation of sensation and temperature, as well as aiding in balance of the body's fluid
and electrolytes.
The skin consists of two main layers:
Epidermis: Composed of squamous cells that are less
sensitive than underlying structures, the epidermis
is the first line of defense against infection.
Dermis: Much thicker than and directly below the
epidermis, the dermis layer consists of blood vessels,
hair follicles, sweat glands, sebaceous glands, collagen and nerves. The dermis reacts quickly to painful stimuli as well as to temperature changes and
pressure sensation. The dermis is the most painful
layer during a peripheral intravenous inser- "Mastering peripheral
tion for the patient.
intravenous (IV) insertion
The fascia lies below the
dermis and epidermis is a challenging clinical
and provides a covering skill"
for blood vessels. The
vascular system is made up of blood vessels, which
include arteries, arterioles, capillaries and veins.
These vessels vary in size and function.
Arteries carry oxygenated blood away from the
heart. The aorta is the largest artery, emanating from
the heart. Arteries branch off the aorta. As they
branch off the aorta, they decrease in size and become
arterioles. Arterioles subdivide into capillaries.
Abu Dhabi NURSE
Veins carry deoxygenated blood back to the heart.
The deoxygenated venous blood is carried to the
right atrium through the superior vena cava. The
blood enters the right ventricle, exiting through the
pulmonary artery to the lungs, where it is oxygenated and carried to the left atrium through the pulmonary veins.
The pulmonary artery carries deoxygenated blood and the
pulmonary veins carry oxygenated blood; these are the only
exceptions to the rule that an artery contains oxygenated
and a vein deoxygenated blood.
Capillaries provide nutrients to the tissue and take
wastes away. Capillaries connect with venules, which
are the smallest veins. The
"Good documentation is venules connect with
crucial in order to record larger veins, eventually
your actions, the patient's leading to the vena cava,
is the largest vein
reaction, and clinical out- which
and connects directly to
comes"
the heart.
The vein, the second barrier to successful
peripheral intravenous insertion, consists of three
layers:
l Tunica adventitia--outer coating, is made of connective tissue, which is the support.
l
Tunica media--muscle and elastic tissues that
causes contraction and dilation.
Tunica intima--endothelial lining of the vein; a
single layer of smooth flat cells lying along the
length of the vein, allowing for smooth blood
flow; disruption of this layer exposes the basement membrane and the clotting process is immediately begun.
Also in the tunica intima layer are the semi-lunar
valves, which are directed toward the heart and prevent blood from flowing toward the extremities.
Therefore, the direction of the IV needle should always be toward the heart with the flow of the circulation.
Systemic veins are in two sets: deep and superficial.
Deep veins accompany the corresponding arteries
and are called venae comites or venae comitantes.
The superficial veins commence as a network of small
veins just under the skin. Superficial veins in the hand
and forearm are generally utilized for the initiation
of IV therapy; however, upper arm veins can be and
frequently are accessed as peripheral intravenous
insertion sites.
Table 1. Peripheral Intravenous Sites
Digital
Vein
Location
Catheter type
Comments
Lateral and dorsal segments of fingers
Use small flexible catheter
l
l
Difficult to access
Best to totally avoid
Metacarpal
Dorsum of hand, proximal to knuckles
Use flexible catheter or steel needle
l
Collapse sooner than central veins in cases of
shock
Requires splinting in confused and disorientated patients
Increase risk of complications if solutions are
hypertonic or irritant
Cephalic
Continuation of metacarpal vein of thumb
Parallels the radial bone
Use flexible catheter
l
Continues into antecubital fossa
Forearm provides natural splinting
Median antebrachial
Travels along ulnar side of inner forearm
Use small, flexible catheter
l
Easily visualised; painful insertion
Basilic
Travels along ulnar path on underside of fore
arm
Use flexible catheter
l
A large sized vein that can be used for larger
infusion devices
Median Cubital, Cephalic and Basilic Veins
Located inside the anticubital fossa
l
Very good for phlebotomy, NOT a preferable
site for IV insertion
(Adapted from Williams and Hadaway 2003)
When selecting a vein to perform a peripheral intravenous insertion, consider the following factors:
l
Patient's age--Infants have fewer accessible sites
than older children and adults. Hands, feet and
the antecubital region are generally the most accessible sites. The elderly may have fragile veins.
The tourniquet may need to be loose or not used
at all.
Patient's preference--Use the non-dominant side
whenever possible. Advise the patient of the optimal sites and ask which site they prefer.
Patient's activity-- Avoid lower extremities.
Consider allowing hands to be free, particularly
if the patient uses a walker, crutches or a wheel
chair.
Previous medical history--Avoid the affected
side, i.e., paralysis, mastectomy, burns, scars. Do
not place in close proximity to an infected wound
Presence of a shunt or graft--NEVER use the side
Abu Dhabi NURSE
the lower forearm. Do not administer continuous vesicant chemotherapy or parenteral nutrition via a peripheral IV.
that has a shunt or graft used for haemodialysis.
l
Time of therapy-When prolonged therapy is required, the distal portion of the vein should initially be used with subsequent re-sites above. If
possible, alternate arms and remember to begin
distally and work proximally.
Type of solution--Hypertonic solutions and various medications can be chemically irritating to
the vein. Consult with the pharmacist regarding
properties of the medication or solution. If the
solution is a known irritant, select a large vein in
Condition of vein-Previously used veins can become sensitive. If the vein has been recently used
for an infusion, is bruised, red, swollen, sore, or
is near a previously affected site; Do Not Use
The Vein.
Cannula size--The cannula should be as small
as possible and yet be able to effectively deliver
the therapy. (see table 2)
Table 2. Catheter Size
26 gauge
0.5mm
Neonatal
24 gauge
0.6mm
Neonatal - including blood products
Elderly, fragile veins
22 gauge
0.8mm
l
l
l
20 gauge
1mm
l
l
18 gauge
1.2mm
l
l
14 and 16 gauge
1.7 to 2mm
l
l
l
Paediatric standard
Neonatal blood components
Single dose
Adult standard
Paediatric blood components
Minor surgery
Adult blood components
Major surgery
Major trauma
Cardiac arrest
Vascular/ Cardiac Surgery
Note that the colours of the cannula have not been
mentioned in Table 2. Although there is an International Organisation for Standardization (ISO) proposal for standardisation of colours for peripheral
cannula, different manufacturing companies may
alter their colour codes, so know the size rather than
the colour a particular brand comes in.
Potential complications of peripheral intravenous access
The possibility that a patient may develop a complication from having a peripheral intravenous access
insitu increases proportionally with the time the access is required. Nurses must be aware of these complications (see table 3) to ensure prevention and early
detection if a complication arises.
Table 3. Reviewing Peripheral Line Complications
Symptom
Common Causes
Intervention:
Infiltration: the escape of nonvesicant solutions into the extravascular tissue.
l Coolness of skin around site
l Skin taut
l Slowing of infusion rate
l Oedema
l Sited over joint
l Insecurely taped
Discontinue IV, elevate the extremity based on patient comfort, and apply cold compresses.
Notify physician immediately if infiltrate toxic
Air Embolism: obstruction of blood vessel by air
l Pallor, cyanosis
l Dyspnea
l Cough
l Tachycardia
Abu Dhabi NURSE
l
l
l
l
l
l
l
l
l
Syncope
Shock
Cracked tubing
Air in administration set
Loose connections
Place patient on left side with head and shoulder lowered
Tighten all connections
Administer oxygen
Notify physician immediately
Phlebitis: inflammation of the vein, caused by mechanical and/or chemical injury.
l Site is red, warm and sore
l Possible red streak along vein
l Immune response
l Injury
l Mechanical Irritation
l Chemical Irritation
l Infection
Discontinue IV, apply warm, then cool compresses.
Draw blood cultures if ordered
Thrombophlebitis: inflammation caused by clot formation.
l Site is sore, hard, cordlike and warm; red line above site, oedema, and sluggish or stopped IV
l Malaise and or fever
Cannula not in use or flushed adequately
Discontinue IV, apply warm compresses.
Avoid massaging or palpating the area to prevent dislodgement of any embolus
Catheter embolism: free floating or dislodged fragment of catheter in the circulatory system.
Discomfort along the vein, decrease in blood pressure, weak rapid pulse, cyanosis and unconsciousness
Catheter is withdrawn before needle, or when the needle is rethreaded into the catheter.
Discontinue IV, apply a tourniquet above the site, take appropriate emergency measures, inspect catheter for rough edges that might indicate loss of fragments.
Obtain order for X-ray to determine if fragments are present.
Haematoma: blood outside the vessel into the extravascular system.
Discoloration of tissue at IV site, oedema
Cannula puncturing other vein wall
Discontinue IV, apply pressure for approximately 5 minutes.
Infection: caused by pathogenic organisms, may be local or systemic.
Site red and sore
Oedema and/or drainage may be present
l Use of unsterile equipment
l Non-aseptic procedures
l Inadequate skin preparation
Discontinue IV, culture any drainage, cleanse site with Povidone iodine and apply dressing. Culture tip
of catheter. Observe site; observe patient for signs and symptoms of systemic infection.
(Adapted from Williams and Hadaway 2003)
In order to prevent infection and complications it is
important to care for the cannula and the site:
Handle with care: don't contaminate equipment by
poor handling techniques
Inspect the site: the insertion site should be checked
regularly for any signs of infection or complications
Change the dressing: if a dressing is wet or soiled, it
should be changed
Securing the cannula: fixing the cannula securely
using a non-occlusive dressing
Signs of venous reactions: redness, tenderness or
swelling around the site indicates a localised reaction that requires the cannula to be re-sited
Change the cannula: change the cannula every 4872hrs (according to your facility policy). Don't forget the lines, every 24hrs for an intermittent infusion and every 48hrs for continuous therapy.
Check connections: all connections should be tight
Flush: Use an appropriate solution such as normal
saline 0.9% (in accordance with your facility policy),
to regularly flush a cannula
Abu Dhabi NURSE
Documenting the Procedure
Good documentation is crucial in order to record
your actions, the patient's reaction, and clinical outcomes. According to Millam and Hadaway (2003:10)
good documentation includes the following:
Type, length, and gauge size of the catheter inserted
Date and time of the procedure
Number of attempts made
Exact location of each attempt and the final successful site
Type of dressing applied
Patient's tolerance of the procedure, using actual
quotes of comments from the patient
Condition of the site
Specific types of fluids and medications infused
through the catheter, including the infusion rate,
dose, and diluent for all medication and any additives to the primary fluid.
Finally
Like any clinical nursing skill, mastering peripheral
intravenous (IV) insertion tests your skills, takes time,
Maybe it's a DVT?
Deep Vein Thrombosis (DVT) affects millions of people
every year. The development of a DVT in the leg isn't
necessarily life threatening, but if the clot moves to the
lungs, it can cause a pulmonary embolus. Pulmonary
Emboli may be so mild even the patient doesn't even
notice any symptoms, or severe enough for them to
have a cardiac arrest.
DVT's rarely occur in the absence of certain risk factors. Knowledge of them will assist your skills in identify patients who may be at risk and be focused when
performing a nursing physical examination. Can you
recognise them?
The risk factors for DVT are known as the 'Virchow's
triad':
1. Changes in blood coagulability
-
Traumatic, burn, and surgical injuries, because of tissue damage, release of tissue factors, and activation of the extrinsic pathway
of coagulation
Cancer, because fibrinolytic activity may be
reduced and because malignant tissue may
promote coagulation
2. Changes in the vessel wall
-
Atherosclerotic changes leading to rupture of
plaque on the vessel wall exposes thrombogenic material, activating platelets and the
coagulation cascade.
3. Changes in blood flow
-
Stasis related to prolonged immobility (such
as long flight), paralysis, varicose veins, or
heart failure
Increased blood viscosity
and may be painful for your patient. Assessing your
patient's needs, distending the patient's veins, and
selecting an appropriate site and device are the first
keys to a successful procedure.
References
Millam D.A. and Hadaway L.C. 2003. On the road
to successful I.V. starts. Nursing2003. May, Supplement. Vol 33 No 5, Pages 1 - 14
Terry J (Editor). 1995. Intravenous Therapy: Clinical
Principles and Practice. W.B. Saunders Co. Philadelphia
Williams, Penny and. Hadaway, Lynn C. 2003. Essentials of IV Therapy: MODULE 1: Peripheral IV Catheter Insertion, Care and Maintenance. Baxter Healthcare
Corporation. Accessed on the World Wide Web on
June 26th via http://www.baxter.com/doctors/
iv_therapies/education/iv_therapy_ce/basic_one/
basicone.html
Useful Website: Intravenous Nurses Society on
http://www.ins1.org
Special thanks, to Shaun Bowden for editing and Jeemol
Samual for assisting in the photographic procedure.
DVTs certainly cause vein inflammation, but
more than 50% of DVTs don't cause symptoms initially
as the thrombus doesn't completely occlude
the vein and the patient has adequate collateral circulation. The first hint of trouble for some patients is
the sudden onset of unexplained tachycardia,
tachypnea, anxiety, and hypoxia, indicating a
Pulmonary Embolus.
One of the most reliable physical findings in DVT is
unilateral oedema of the affected leg. Measure both legs
at midthigh and midcalf and compare the circumferences to each other and to earlier measurements. An
initial finding of a difference in circumference between
the left and right leg may not be significant, but any
increase in circumference should be reported and
documented. Other common physical signs of
DVT include warmth and erythema of the affected
extremity.
The patient may experience pain or tenderness in the
calf in response to movement or pressure or when they
stand. Homans' sign-increased resistance or pain that
occurs in the calf on forced dorsiflexion of the foot-has
been historically considered an indication of DVT, but
it's an unreliable diagnostic sign as calf pain from muscular injury will also elicit a Homans' sign. Because
many DVTs are difficult to detect clinically, diagnostic
studies may be indicated. One of the simplest is duplex venous ultrasonography or 'Doppler'; otherwise,
a venogram or possibly a Magnetic Resonance Image
(MRI) may have to be ordered.
Day, M.W. 2003 Recognizing and managing deep vein
thrombosis. Nursing2003, May. Vol 33 No 5,
pages 36 - 41
Abu Dhabi NURSE
Photographic Procedure for Peripheral
Intravenous Insertion
8.
1.
2.
3.
Wash hands thoroughly with antiseptic soap.
Wear protective gloves.
Select appropriate cannulation site (see table 1).
4.
Create an adequate venous filling by:
applying tourniquet
tap vein lightly
Instruct patient to clench or pump fest
Allow arm to hang over bedside
9.
Adjust cannula angle and advance cannula and
stylet a few millimetres further into the vein.
Withdraw the needle partially (about 5 mm.) to
avoid exit through the posterior vein wall. Advance the catheter off the needle into the vein.
Release the tourniquet.
The needle must never be reinserted while the
catheter is in the vein. This may sever the catheter.
10. Remove and discard stylet into sharp container
11. Check patency of cannula
5.
Clean the puncture site and the surrounding thoroughly with iodine or an alcohol and allow to dry.
6.
Stabilise skin and vein adequately and insert cannula (see table 2) into the vein at a low angle
12. Secure the cannula and apply dressing:
Tape the wings securely to the patient's skin
Protect the puncture site, use either sterile gauze
or sterile non-occlusive dressing as shown here.
13. Record date and time of insertion, and the name
of the operator.
14. Document procedure in accordance with hospital facility policy
7.
Check for blood return in the flash back
chamber.
15. Clear area and wash hands.
16. Educate patient and significant others about
complications and leave comfortable.
Das könnte Ihnen auch gefallen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5795)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- Coronary Artery DiseaseDokument110 SeitenCoronary Artery DiseaseMaesy Garcia LorenaNoch keine Bewertungen
- The Circulatory System - Test QuestionsDokument4 SeitenThe Circulatory System - Test Questionsflorin100% (1)
- MCQs in Intensive Care MedicineDokument288 SeitenMCQs in Intensive Care MedicineHiago Sousa90% (10)
- 1617 Biology o Level Top 60 QuestionsDokument39 Seiten1617 Biology o Level Top 60 QuestionsMeerab ShahNoch keine Bewertungen
- Anatomy and Physiology of Farm AnimalsDokument157 SeitenAnatomy and Physiology of Farm AnimalsOliver TalipNoch keine Bewertungen
- Soal Reading B.ing 22 Feb (Najhan)Dokument9 SeitenSoal Reading B.ing 22 Feb (Najhan)Green AlonsoNoch keine Bewertungen
- Human PhysiologyDokument257 SeitenHuman PhysiologyAyushNoch keine Bewertungen
- SS1 1ST Term Animal Husbandry E-NoteDokument29 SeitenSS1 1ST Term Animal Husbandry E-Notekanajoseph2009Noch keine Bewertungen
- Health & HygieneDokument5 SeitenHealth & Hygieneegy1971100% (2)
- Cambridge International AS & A Level: Biology 9700/12Dokument20 SeitenCambridge International AS & A Level: Biology 9700/12GiftElishaNdawalaNoch keine Bewertungen
- Biology 9700 FM23 Paper 2-SolvedDokument20 SeitenBiology 9700 FM23 Paper 2-Solvedrayedr602Noch keine Bewertungen
- Mark Scheme (Results) : January 2017Dokument23 SeitenMark Scheme (Results) : January 2017Raashed RamzanNoch keine Bewertungen
- CH 5 Blood and CirculationDokument9 SeitenCH 5 Blood and CirculationShokefun OlawaleNoch keine Bewertungen
- 5125 w10 Ms 4Dokument5 Seiten5125 w10 Ms 4mstudy123456Noch keine Bewertungen
- Case Report Buerger DiseaseDokument35 SeitenCase Report Buerger DiseaseIsyfaun NisaNoch keine Bewertungen
- Massage Therapies MT1 Cautions and ContraindicationsDokument21 SeitenMassage Therapies MT1 Cautions and ContraindicationsRobertDochertyNoch keine Bewertungen
- Red and White Blood Cell PostersDokument2 SeitenRed and White Blood Cell Postersapi-169639475Noch keine Bewertungen
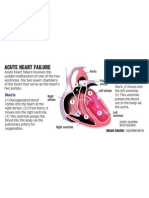
- Acute Heart FailureDokument1 SeiteAcute Heart FailureThe Press-Enterprise / pressenterprise.comNoch keine Bewertungen
- CA Sensation-Cs300 Brochure 0845-Rev-A EngDokument14 SeitenCA Sensation-Cs300 Brochure 0845-Rev-A Engjuancar90Noch keine Bewertungen
- What Were The Main Objectives of Clean Development MechanismDokument33 SeitenWhat Were The Main Objectives of Clean Development MechanismAleeza syedNoch keine Bewertungen
- Cardiovascular SystemDokument6 SeitenCardiovascular Systemtasneem8Noch keine Bewertungen
- Respiratory & Circulatory SystemDokument6 SeitenRespiratory & Circulatory SystemJanelleNoch keine Bewertungen
- (Journal) European Journal of Plastic Surgery 2003-2007Dokument1.936 Seiten(Journal) European Journal of Plastic Surgery 2003-2007yellowbieNoch keine Bewertungen
- BZYCT-135 English PDFDokument5 SeitenBZYCT-135 English PDFNeraj 32Noch keine Bewertungen
- November 2017 (v3) QP - Paper 2 CIE Biology IGCSEDokument20 SeitenNovember 2017 (v3) QP - Paper 2 CIE Biology IGCSEsansNoch keine Bewertungen
- NEB Biology Syllabus XI & XIIDokument26 SeitenNEB Biology Syllabus XI & XIIBhanu AryalNoch keine Bewertungen
- Breathing and Exchange of GasesDokument16 SeitenBreathing and Exchange of GasesVishal JoshiNoch keine Bewertungen
- Biology Paper 2 Marking SchemeDokument2 SeitenBiology Paper 2 Marking SchemeNyakweba DenisNoch keine Bewertungen
- Igcse Biology 4ed TR Eoc Test Answers 9Dokument2 SeitenIgcse Biology 4ed TR Eoc Test Answers 9pratham.0.kathuriaNoch keine Bewertungen
- Chemistry - Paper - Annual Exam - Xi - 2024Dokument5 SeitenChemistry - Paper - Annual Exam - Xi - 2024rajminnoob06Noch keine Bewertungen