Beruflich Dokumente
Kultur Dokumente
Predisponentes de Status Epileptico Mortalidad
Hochgeladen von
Ivan De La PeñaOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Predisponentes de Status Epileptico Mortalidad
Hochgeladen von
Ivan De La PeñaCopyright:
Verfügbare Formate
Brain & Development xxx (2014) xxxxxx
www.elsevier.com/locate/braindev
Original article
Early predictors of status epilepticus-associated mortality
and morbidity in children
Yoshihiro Maegaki a,, Youichi Kurozawa b, Akiko Tamasaki a, Masami Togawa c,
Akiko Tamura c, Masato Hirao d, Akihisa Nagao e, Takayuki Kouda f,
Takayoshi Okada g, Hiroshi Hayashibara h, Yuichiro Harada i, Makoto Urushibara j,
Chitose Sugiura k, Hitoshi Sejima l, Yuji Tanaka m, Hiroko Matsuda-Ohtahara n,
Takeshi Kasai o, Kazuko Kishi p, Syunsaku Kaji q, Mitsuo Toyoshima r,
Susumu Kanzaki s, Kousaku Ohno a, the Status Epilepticus Study Group1
b
a
Division of Child Neurology, Faculty of Medicine, Tottori University, Yonago, Japan
Division of Health Administration and Promotion, Faculty of Medicine, Tottori University, Yonago, Japan
c
Tottori Prefecture Central Hospital, Tottori, Japan
d
Tottori Red Cross Hospital, Tottori, Japan
e
Tottori Seikyo Hospital, Tottori, Japan
f
Tottori Municipal Hospital, Tottori, Japan
g
Tottori Prefecture Kousei Hospital, Kurayoshi, Japan
h
Yonago Medical Center, Yonago, Japan
i
Hakuai Hospital, Yonago, Japan
j
Tottori Prefecture Saiseikai Sakaiminato General Hospital, Sakaiminato, Japan
k
Tottori Prefectural Rehabilitation Center for Disabled Children, Yonago, Japan
l
Matsue Red Cross Hospital, Matsue, Japan
m
Matsue City Hospital, Matsue, Japan
n
Yasugi Municipal Hospital, Yasugi, Japan
o
Unnan City Hospital, Unnan, Japan
p
Shimane University School of Medicine, Izumo, Japan
q
Tsuyama Chuo Hospital, Tsuyama, Japan
r
Kagoshima University, Kagoshima, Japan
s
Division of Pediatrics and Perinatology, Faculty of Medicine, Tottori University, Yonago, Japan
Received 15 February 2014; received in revised form 21 June 2014; accepted 7 August 2014
Abstract
Background: Early predictors of status epilepticus (SE)-associated mortality and morbidity have not been systematically studied
in children, considerably impeding the identication of patients at risk. Objectives: To determine reliable early predictors of
SE-associated mortality and morbidity and identify the etiology of SE-associated sequelae in Japanese children. Methods: We
conducted a prospective multicenter study of clinical ndings and initial laboratory data acquired at SE onset, and assessed
Corresponding author. Address: Division of Child Neurology, Faculty of Medicine, Tottori University, 36-1 Nishi-cho, Yonago 683-8504, Japan.
Fax: +81 859 38 6779.
E-mail address: maegaki@med.tottori-u.ac.jp (Y. Maegaki).
1
Appendix 1
http://dx.doi.org/10.1016/j.braindev.2014.08.004
0387-7604/ 2014 The Japanese Society of Child Neurology. Published by Elsevier B.V. All rights reserved.
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Y. Maegaki et al. / Brain & Development xxx (2014) xxxxxx
outcomes at the last follow-up examination. In-hospital death during the acute period and neurological sequelae were classied as
poor outcomes. Results: Of the 201 children who experienced their rst SE episode, 16 exhibited poor outcome that was most commonly associated with acute encephalopathy. Univariate analysis revealed that the following were associated with poor outcomes:
young age (624 months); seizure duration >90 min; seizure intractability (failure of the second anticonvulsive drug); biphasic seizures; abnormal blood glucose levels (<61 or >250 mg/dL); serum aspartate aminotransferase (AST) P56 U/L; and C-reactive protein (CRP) levels >2.00 mg/dL. Multivariate analysis revealed that young age, seizure intractability, abnormal blood glucose levels,
and elevated AST and CRP levels were statistically signicant. Conclusions: Young age and seizure intractability were highly predictive of poor outcomes in pediatric SE. Moreover, abnormal blood glucose levels and elevated AST and CRP levels were predictors that might be closely associated with the etiology, especially acute encephalopathy and severe bacterial infection (sepsis and
meningitis) in Japanese children.
2014 The Japanese Society of Child Neurology. Published by Elsevier B.V. All rights reserved.
Keywords: Status epilepticus; Prognosis; Predictors; Acute encephalopathy
1. Introduction
2. Methods
The incidence, causes, and prognosis of pediatric status epilepticus (SE) vary worldwide because of distinct
environments, socioeconomic conditions, and genetic
susceptibility to acute neurological disorders; i.e., the
incidence of febrile seizures is much higher and that of
bacterial meningitis is lower in Japanese children than
in other children. SE predictors have been extensively
studied in adults; however, these studies might not provide reliable information for the prediction of pediatric
SE because the etiology in children is distinct from that
in adults. Early SE predictors have not been systematically studied in children, considerably impeding the
identication of patients at risk.
Inuenza-associated encephalopathy cases, in which
the initial presentation usually includes SE, have
increased markedly in Japan since the 19941995 inuenza epidemic; this prompted the Japanese Ministry of
Health, Labour and Welfare to initiate a national survey
of inuenza-associated encephalopathy in 1998. During
the 19981999 epidemic, 148 cases with a mortality of
31.8% and a morbidity of 27.7% were reported [1]. Such
acute encephalopathies are caused by pathogens other
than inuenza, and although they are a common cause
of acquired brain damage in Japanese children, the
pathophysiology remains unknown. These encephalopathies have been collectively termed as acute encephalopathy with inammation-mediated status epilepticus
(AEIMSE) [2]. Early diagnosis of AEIMSE is often difcult because laboratory results, including data from
cerebrospinal uid (CSF) analysis and neuroimaging,
are often unremarkable for several days after SE onset
[35]. Therefore, we initiated a prospective multicenter
status epilepticus study to determine the reliable early
predictors of SE-associated mortality and morbidity
and elucidate the etiology of SE-associated brain injury
in Japanese children.
2.1. Study design
The Status Epilepticus Study group includes
researchers belonging to 25 hospitals who have been
studying the etiology and prognosis of pediatric SE since
2005. The 25 hospitals included 7 intensive care units
and 18 local hospitals. Most pediatric SE patients in
Tottori prefecture, eastern Shimane prefecture, and
northern Okayama prefecture were referred to one of
these participating hospitals. Tottori Prefecture Central
Hospital serves severely ill pediatric patients living in the
north-western part of Hyogo prefecture and Tottori prefecture. Kagoshima University Hospital, which serves
severely ill pediatric patients in Kagoshima City, participated in this study. This group has been enrolling pediatric patients who suered seizures P20 min. Between
August 1, 2005 and March 31, 2010, over 250 patients
aged 1 month16 years were consecutively enrolled in
this study.
SE was dened as any seizure >30 min or a series of
recurrent seizures >30 min without complete recovery of
consciousness in this study. Patients with SE of any etiology were the participants of this study. The episodes
of rst SE during the study period were used for statistical analysis.
We used the modied version of the classication of
SE etiology proposed by Maytal et al. (Appendix 2)
[6]. Clinical ndings from each patient were used to
identify outcome predictors: these included demographic data, previous neurological conditions, factors
commonly associated with SE, SE characteristics, health
status at SE onset, and laboratory data. Prior neurological conditions included past seizures, comparative mental and motor development, and past neurological
insults. Factors associated with SE included pyrexia
and exposure to proconvulsant drugs (theophylline
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Y. Maegaki et al. / Brain & Development xxx (2014) xxxxxx
and antihistamines). SE characteristics included seizure
duration, type (generalized or focal), mode (continuous
or intermittent), intractability (failure of the second
anticonvulsive drug), and biphasic seizures (seizure
recurrence 26 days after SE onset). Initial laboratory
data, which were acquired at SE onset, were used for
analysis. They included white blood cell count, serum
sodium, aspartate aminotransferase (AST), alanine aminotransferase (ALT), creatine kinase, lactate dehydrogenase, C-reactive protein (CRP), and blood glucose
levels. CSF analysis, including bacterial and viral cultures, was performed when encephalitis, meningitis, or
AEIMSE was suspected. Virological tests included
CSF gene analysis for herpes simplex virus type 1 and
human herpesvirus 6, rapid inuenza or rotavirus antigen detection test, and serum viral antibodies. Cranial
computed tomography (CT) or magnetic resonance
imaging (MRI), and electroencephalography (EEG)
were performed to identify the cause of SE in patients
with suspected acute symptomatic etiology and in those
exhibiting neurological sequelae after SE. Additional
metabolites, including plasma and urine amino acids,
urine organic acids, and blood and CSF lactic acids,
were analyzed in patients who exhibited neurological
sequelae after SE as well. Clinical data using a uniform
chart were collected every 6 months from each hospital.
When necessary, additional information, including laboratory data, was obtained from medical records.
and bacterial culture of CSF samples; and (4) diuse
cerebral dysfunction and edema as indicated by symptoms, EEG ndings, and neuroimaging ndings.
AEIMSE subtypes such as hemorrhagic shock and
encephalopathy syndrome (HSES), acute necrotizing
encephalopathy (ANE), acute encephalopathy with
biphasic seizures and late reduced diusion (AESD),
and clinically mild encephalitis/encephalopathy with a
reversible splenial lesion (MERS) were classied according to previous reports [5,7]. Idiopathic hemiconvulsion
hemiplegia syndrome, characterized by long-lasting
febrile seizures followed by hemiplegia, has clinical and
imaging similarities to AESD [2,3,8]; therefore, it was
included in the AESD category as well.
This study was approved by the ethics committees of
Tottori University and each participating hospital.
2.3. Statistical analysis
Univariate analysis was performed for each candidate
variable, with poor outcome as the dependent variable.
Nonsignicant variables (P > 0.05) were excluded from
further analysis. Multivariate logistic regression analysis
was performed for those variables judged to be signicant in univariate analysis to identify independent predictors for poor outcome. The SPSS 15.0J software
(SPSS, Tokyo, Japan) was used for all the statistical
analysis. All the tests were two-tailed, and P value
<0.05 was considered to indicate statistical signicance.
2.2. Assessment
3. Results
Neurological status was initially assessed at discharge. When a patient had any developmental deterioration or neurological decit at discharge, follow-up
examinations were repeated by an experienced pediatrician or pediatric neurologist at each hospital. Neurological sequelae were assessed at the last follow-up
examination. Enjoji Scale of Infant Analytical
Development, TanakaBinet Intelligence Scale, or
Wechsler Intelligence Scale for Children was used to
determine the intellectual (IQ) or development quotient
(DQ). IQ/DQ < 70 or new-onset motor decit was
regarded as a sequela when a patient had no prior neurological or developmental decit. In addition, if a
patient exhibited a predisposing developmental or neurological problem, IQ/DQ decline >10 or new-onset
motor decit after SE, it was regarded as a sequela.
In-hospital death during the acute period and neurological sequelae were classied as poor outcomes.
AEIMSE was dened according to the following criteria [3,5,7]: (1) acute onset of impaired consciousness
accompanied by seizures during a febrile infection; (2)
exclusion of well-dened central nervous system (CNS)
inammation, head trauma, cerebrovascular disease,
toxic encephalopathy, and systemic and metabolic diseases; (3) normal cell count in CSF and negative viral
3.1. Prognosis of status epilepticus
Of the 230 patients who met the inclusion criteria, 29
patients were excluded because of insucient clinical or
laboratory data (poor outcomes, none); therefore, in
total, 201 patients were the subjects for the statistical
analysis. Two patients died in the hospital during the
acute period, and 1 of them had been diagnosed as having PraderWilli syndrome. One infant who had had
prior developmental delay (DQ, 67) due to bacterial
meningitis exhibited developmental deterioration at discharge. She was judged as poor outcome (DQ < 20) at
follow-up examination 1 month after SE and died unexpectedly thereafter. Fourteen patients without prior neurological or developmental problems who presented
developmental deterioration or new-onset neurological
decits at discharge were followed-up for at least
7 months (median, 45 months; range, 760 months). At
the last examination, 11 patients exhibited the following
neurological sequelae: vegetative state (n = 2), profound
mental retardation or developmental delay (IQ/
DQ < 20) with motor palsy (n = 1), severe mental retardation or developmental delay (IQ/DQ < 35; n = 2),
moderate mental retardation or developmental delay
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Y. Maegaki et al. / Brain & Development xxx (2014) xxxxxx
Table 1
Etiology of status epilepticus and prognosis.
Etiology of status epilepticus
No. of
patients
(%)
No. of
patients with
poor outcome
(in-hospital
deaths)
Cryptogenic
Febrile
Acute symptomatic
Acute encephalopathy with inammation- mediated status epilepticus
Acute encephalopathy with biphasic seizures and late reduced diusion
Hemorrhagic shock and encephalopathy syndrome
Clinically mild encephalitis/encephalopathy with a reversible splenial lesion
Acute necrotizing encephalopathy
Unclassied
Bacterial meningitis
Viral encephalitis
Cerebrovascular accident
Septic encephalopathy
Progressive encephalopathy
Remote symptomatic
Febrile on remote symptomatic
23 (11.4%)
93 (46.3%)
33 (16.4%)
21
0
0
16 (2)
13 (2)
(IQ/DQ < 50; n = 2; motor palsy in 1), and mild mental
retardation or developmental delay (IQ/DQ < 70; n = 4;
motor palsy in 1). On the other hand, 3 patients were
normalized at the follow-up examinations; DQs became
normal in 2, and hemiparesis improved in 1. The duration
from SE onset to normalization ranged from 6 to
12 months in the 3 patients. Further, 2 patients who
had had cerebral palsy (DQs, 38 and 67) exhibited
developmental deterioration at discharge. Their prognoses were profound developmental delay (DQ < 20) at
the follow-up periods of 16 and 42 months, respectively.
Thus, these 2 patients died in the hospital, and 14 patients
with neurological sequelae at the last follow-up examination were classied as poor outcome (8.0%, 16/201).
Of the 182 patients who did not reveal any developmental deterioration or new-onset neurological decit
at discharge, 165 (90.7%) were followed-up for at least
0.5 months (median, 22 months; range 0.565 months).
At the last clinical evaluation, they were all judged as
having no developmental deterioration and no
new-onset neurological decits.
3.2. Etiology of status epilepticus
The SE etiologies are listed in Table 1. In every case
with poor outcome at the time of the last follow-up
examination, including 13 patients with AEIMSE, 2
with septic encephalopathy, and 1 with bacterial meningitis, the etiology was acute symptomatic. Overall, there
were 21 patients with AEIMSE cases, and the 13
patients exhibiting poor outcomes included 2 fatalities
due to HSES (Table 1). Furthermore, 11 of the 21
patients with AEIMSE were also diagnosed as having
AESD, of which 7 exhibited poor outcomes.
11
3
3
1
3
4
3
3
2
1 (0.5%)
32 (15.9%)
19 (9.5%)
7
3(2)
0
1
2
1
0
0
2
0
0
0
In patients with febrile SE (93 patients), AEIMSE (21
patients), and febrile on remote symptomatic (19
patients), clinical diagnoses of acute infection were common cold in 74, inuenza virus infections in 18, viral
gastroenteritis in 12 (rotavirus infections in 5), exanthem
subitum in 12, viral bronchitis in 8, mycoplasma bronchopneumonia in 2, pneumonia in 1, chickenpox in 1,
hand-foot-and-mouth disease in 1, herpetic stomatitis
in 1, streptococcal pharyngitis in 2, and unknown in 1.
3.3. Early predictors of poor outcomes
Possible predictors were rst divided into 2 or more
categories. If the factors were rst divided into 3 or more
categories (e.g., age, seizure duration, and laboratory
date), they were rearranged into 2 categories before
being used for statistical analyses (Table 2). Poor outcome was higher in frequency in the 112- and 1324month age groups than in the 2548- and 49188-month
age groups. Therefore, age was categorized as 624 and
>24-months for statistical analysis. The rate of poor
outcome was similar between the patients with past febrile seizures and those with afebrile seizures; therefore,
past seizures were simply categorized as none and
present. With regard to seizure duration, poor outcome was higher in frequency in the 91120-min and
>120-min groups than in the <60-min and 6090-min
groups. Therefore, seizure duration was categorized as
690 and >90 min for statistical analysis. With regard
to serum sodium levels, the rate of poor outcome in
the patients with 131135 and <131 mmol/L was higher
compared with that in the patients with >135 mmol/L.
Therefore, serum sodium levels were categorized as
>135 and 6135 mmol/L. The rate of poor outcome in
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Y. Maegaki et al. / Brain & Development xxx (2014) xxxxxx
Table 2
Possible predictors that were rst divided into 3 or more categories.
SE, status epilepticus; AST, aspartate aminotransferase; CRP, C-reactive protein.
the patients with blood glucose levels of <61 or
>250 mg/dL was higher compared with that in the
patients with blood glucose levels of 61100 or 101
250 mg/dL. Therefore, blood glucose levels were categorized as 61250 and <61 or >250 mg/dL (<61/>250 mg/
dL). With regard to serum aspartate aminotransferase
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Possible predictor
Sex
Variable
Male
Female
Age at onset of SE (month)
>24
624
Motor or mental developmental delay
Past history of seizure
Pyrexia during SE (P38.0 C)
Proconvulsant drug
Seizure duration (>90 min)
Type of seizure
Generalized
Focal
Mode of seizure
Continuous
Intermittent
Intractability of seizure
Biphasic seizure
Serum sodium levels (mmol/L)
>135
6135
Blood glucose levels (mg/dL)
61250
<61/>250
Serum AST levels (U/L)
<56
P56
White blood cell count (cells/mm3) 615,500
>15,500
Serum CRP levels (mg/dL)
62.00
>2.00
All patients n = 201 (%)
Good outcome n = 185
(%)
Poor outcome n = 16 (%)
Odds ratio
105 (52.2)
96 (47.8)
124 (61.7)
77 (38.3)
42 (20.9)
80 (39.8)
134 (66.7)
15 (7.5)
37 (18.4)
131 (65.2)
70 (34.8)
175 (87.1)
26 (12.9)
36 (17.9)
13 (6.5)
116 (57.7)
85 (42.3)
179 (89.1)
22 (10.9)
177 (88.1)
24 (11.9)
146 (72.6)
55 (27.4)
167 (83.1)
34 (16.9)
95 (90.5)
90 (93.7)
123 (99.2)
62 (80.5)
36 (85.7)
77 (96.2)
120 (89.6)
12 (80)
31 (83.8)
120 (91.6)
65 (92.9)
163 (93.1)
22 (84.6)
29 (80.6)
8 (61.5)
109 (94.0)
76 (89.4)
170 (95.0)
15 (68.2)
171 (96.6)
14 (58.3)
135 (92.5)
50 (90.9)
158 (94.6)
27 (79.4)
10 (9.5)
6 (6.3)
1 (0.8)
15 (19.5)
6 (14.3)
3 (3.8)
14 (10.4)
3 (20)
6 (16.2)
11 (8.4)
5 (7.1)
12 (6.9)
4 (15.4)
7 (19.4)
5 (38.5)
7 (6.0)
9 (10.6)
9 (5.0)
7 (31.8)
6 (3.4)
10 (41.7)
11 (7.5)
5 (9.1)
9 (5.4)
7 (20.6)
1.000
0.633
1.000
29.758
2.483
0.324
3.792
3.327
2.981
1.000
0.839
1.000
2.47
4.184
10.057
1.000
1.844
1.000
8.815
1.000
20.357
1.000
1.227
1.000
4.551
SE, status epilepticus; AST, aspartate aminotransferase; CRP, C-reactive protein.
95% condence
interval
P value
0.2211.841
0.395
3.842230.495
0.8477.280
0.0891.175
0.83617.199
0.83313.291
1.0098.805
0.001*
0.097
0.086
0.084
0.089
0.048*
0.2802.519
0.755
0.7328.332
1.44312.128
2.81735.903
0.145
0.008*
0.000*
0.6585.166
0.244
2.87627.015
0.000*
6.44964.257
0.000*
0.4063.708
0.717
1.56313.252
0.005*
Y. Maegaki et al. / Brain & Development xxx (2014) xxxxxx
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Table 3
Univariate analysis of early predictors for poor outcome.
Y. Maegaki et al. / Brain & Development xxx (2014) xxxxxx
Table 4
Multivariate logistic regression analysis of early predictors for poor outcome.
Possible predictor
Odds ratio
95% condence interval
P value
Age at onset of SE 624 month
Seizure duration >90 min
Intractability of seizure
Biphasic seizure
Blood glucose level <61/>250 mg/dL
Serum AST levels P56 U/L
Serum CRP levels >2.00 mg/dL
17.714
4.412
4.940
3.319
7.101
9.905
7.261
1.808173.558
0.82623.567
1.01224.125
0.47223.357
1.11445.266
2.05547.729
1.31539.583
0.014*
0.083
0.048*
0.228
0.038*
0.004*
0.023*
SE, status epilepticus; AST, aspartate aminotransferase; CRP, C-reactive protein.
(AST) levels, the rate of poor outcome in the patients
with 56100 and >100 U/L was higher compared with
that in the patients with <56 U/L. Therefore, AST was
categorized as <56 and P56 U/L. With regard to white
blood cell (WBC) count, the rate of poor outcome was
variable in each group; therefore, WBC count was categorized as 615,500 and >15,500 cells/mm3. The rate of
poor outcome in the patients with C-reactive protein
(CRP) levels of <0.19 or 0.192.00 mg/dL was lower
compared with that in the patients with CRP levels of
2.014.00 or >4.00 mg/dL. Therefore, CRP levels were
categorized as 62.00 and >2.00 mg/dL.
Serum AST, ALT, creatine kinase, and lactate dehydrogenase levels were positively associated with each
other (e.g., the correlation coecient between AST
and ALT was 0.578, P < 0.01). Therefore, only AST levels were used as an independent factor for analysis.
Univariate analysis indicated that age 624 months,
seizure duration >90 min, intractability of seizure,
biphasic seizures, blood glucose levels <61 or
>250 mg/dL, AST levels P56 U/L, and CRP levels
>2.00 mg/dL were associated with poor outcome
(Table 3). Multivariate analysis revealed that young
age, seizure intractability, abnormal blood glucose levels, and elevated AST and CRP levels were statistically
signicant (Table 4).
4. Discussion
4.1. Predictors of poor outcome
In this prospective multicenter study of 201 children
presenting with SE, 16 exhibited poor outcomes (14 neurological sequelae; 2 in-hospital deaths). Age
624 months was an independent early predictor in this
study. Old age is an established risk factor for SE-associated mortality and morbidity in adults [9,10], primarily
owing to the age-dependence of the etiology, considering
that most SE episodes in the elderly are due to acute
CNS insults, which are generally associated with poor
outcomes. In contrast, studies on pediatric SE have indicated that young age is a risk factor for SE-associated
mortality and morbidity [6,1114]. In fact, 15 of the 16
patients with poor outcomes in our study were
624 months old, which was consistent with the nding
of another study [12] in which infants and young children were reported as more susceptible to acute systemic
or CNS insults, including bacterial meningitis, encephalitis, septic shock, and head trauma. One series reported
that AEIMSE onset was most common in infancy and
early childhood, with maximum incidence at the age of
1 year [7]. Therefore, it is possible that the poor
outcomes observed in young children with SE might
indicate increased susceptibility to a distinct set of
etiologies associated with an inherently poor outcome.
Seizure intractability was another independent early
predictor of poor outcome. It is not surprising that
seizure intractability was related to SE-associated
mortality and morbidity [10,14]. Lambrechtsen et al.
[14] studied refractory SE in children, which was
identical to seizure intractability (failure of the second
anticonvulsive drug) in this study, and reported that
in-hospital mortality and long-term morbidity were signicantly higher in refractory SE than in aborted SE.
They also found that predictors of poor outcome were
young age (<5 years), long seizure duration, and acute
symptomatic etiology [14]. On the other hand, long seizure duration (>90 min) was not signicantly associated
with poor outcome in this study. A positive association
between longer seizure duration and higher mortality/
morbidity has been reported as well [6,11,1416],
although not always conrmed [12]. It is still controversial whether long-lasting seizure activity directly contributes to brain injury because seizure duration is also
related to etiology.
In laboratory data acquired at SE onset, abnormal
blood glucose levels and elevated AST and CRP levels
were early predictors of SE-associated mortality and
morbidity in our multivariate analysis. High AST levels
could indicate SE etiology because they are usually high
in septic encephalopathy and some AEIMSE subtypes
with poor outcomes such as HSES and ANE. Furthermore, in a study of inuenza-associated encephalopathy,
high AST levels were identied as one of the mortality
predictors [17]. Serum CRP status is positive in bacterial
infections, including bacterial meningitis and septic
encephalopathy, which were the conditions associated
with the most severe outcomes in this series. Several
reports have examined the correlation between blood
glucose levels and outcomes in SE [13,1720]. In-hospi-
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Y. Maegaki et al. / Brain & Development xxx (2014) xxxxxx
tal death and neurological sequelae were associated with
hypoglycemia in the studies of pediatric SE [13,20]. In
the present study, in 2 of 3 patients with hypoglycemia,
1 was in septic shock and another had bacterial
meningitis, resulting in neurological sequelae in both.
Therefore, hypoglycemia could also be related to the etiology. On the contrary, poor outcomes were reported to
be associated with hyperglycemia in Japanese children
with inuenza-associated encephalopathy [17] and in
an adult SE series [18]. Hyperglycemia is common
in the early stage of SE and is caused by high
catecholamine drive. Mild hyperglycemia (blood glucose
level; 101250 mg/dL) was not related to prognosis in
the present study nor in the AESD study [19]. Hyperglycemia is known to be a risk factor for poor prognosis in
the cerebrovascular disease. The results of the present
study indicate that severe hyperglycemia (>250 mg/dL)
is also a risk factor for poor outcome in pediatric SE.
4.2. Etiology of poor outcome
The most important nding of this study is that the
etiology of SE-associated mortality and morbidity in
Japanese children was dierent from that identied in
other countries. AEIMSE was the major cause, whereas
other common disorders such as bacterial meningitis
infrequently induced SE-associated mortality and morbidity in Japanese children. AEIMSE accounted for
81.3% poor outcomes. The incidence of AEIMSE in
Japan is 302 cases per year, with complete recovery in
56.2%, mild to moderate sequelae in 22.1%, severe
sequelae in 13.5%, and death in 5.6% [7]. In other countries, SE-associated mortality and morbidity are usually
caused by bacterial meningitis, viral encephalitis, progressive encephalopathy, cerebrovascular disorders,
hypoxicischemic brain injury, or lung and cardiac complications [6,11,1315,21].
AEIMSE was rst described as acute encephalopathies
of obscure origin in infants and children by Lyon et al.
[22]. They reported 16 children, who after several days
of infectious disease, exhibited acute-onset disturbance
of consciousness, convulsions, and fever with no evidence
of CNS inammation. Since this rst description, the following 4 specic syndromes (subtypes) of AEIMSE have
been identied through clinical and pathological investigation: Reyes syndrome, HSES, ANE, and idiopathic
hemiconvulsionhemiplegia syndrome. With the development of advanced imaging techniques such as diusion-weighted MRI, new clinical AEIMSE subtypes
(AESD and MERS) have been recognized [35]. In this
study, the most common AEIMSE subtype was AESD,
which is characterized by convulsive SE at onset followed
by secondary seizures (biphasic seizures) from days 37,
resulted in mental deterioration in most patients.
AEIMSE can be distinguished from primary encephalitis on the basis of several characteristics. First, the
symptoms, clinical course, and imaging ndings of
AEIMSE, particularly AESD, MERS, and ANE, are
quite distinct from those of primary encephalitis irrespective of the pathogen [7]. Second, CSF results in
patients with AEIMSE are usually unremarkable
[1,23]. Third, viral and bacterial cultures are negative,
and viral DNA can seldom be isolated from CSF and
autopsied brain [1,23,24]. Fourth, inammatory changes
are usually not observed in the autopsied brain of
patients with AEIMSE [1,23,24].
Reyes syndrome and HSES have been reported
mainly from Europe and the United States of America,
whereas their occurrence is rare in Japan. Idiopathic
hemiconvulsionhemiplegia syndrome is reported
throughout the world. ANE is relatively common in
East Asia, but it has also been reported from Europe
and American countries. Although most studies on
AESD have been reported from Japan, a few have been
reported from outside Japan as well [25,26]. A recent
report demonstrated that East Asians and Japanese
might have a genetic susceptibility to AEIMSE [27,28].
We speculate, on the basis of the present study, that prolonged seizures during febrile infection and genetic susceptibility in young children greatly increase AEIMSE
risk.
4.3. Limitations
First, the early predictors of SE-associated mortality and morbidity observed in this study may not be
generalized because the underlying cause of SE in
Japanese children was dierent compared with that
in other countries. Second, this study was not population-based; therefore, milder SE cases might have
been missed. Third, patients who did not show any
developmental deterioration or new-onset neurological
decit at discharge were all judged as having no
sequelae at follow-up clinical evaluation. Subnormal
mentalities or minor developmental delays may have
been missed.
5. Conclusion
Our results yielded 2 valuable clinical conclusions.
First, younger pediatric patients presenting with seizure
intractability should be examined systematically to identify the etiology because they are at high risk of poor
outcomes. Second, pediatric patients with SE during
febrile illnesses accompanied by abnormal glucose level,
high serum AST, or CRP levels are at a higher risk of
severe bacterial infection or AEIMSE.
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Y. Maegaki et al. / Brain & Development xxx (2014) xxxxxx
Acknowledgements
This study was supported by Grant from MEXT
KAKENHI Grant Number 23591497.
The authors would like to thank Enago (http://
www.enago.jp) for the English language review.
Appendix A. Supplementary data
Supplementary data associated with this article can
be found, in the online version, at http://dx.doi.org/
10.1016/j.braindev.2014.08.004.
References
[1] Morishima T, Togashi T, Yokota S, Okuno Y, Miyazaki C,
Tashiro M, et al. Encephalitis and encephalopathy associated
with an inuenza epidemic in Japan. Clin Infect Dis 2002;35:
5127.
[2] Nabbout R, Vezzani A, Dulac O, Chiron C. Acute encephalopathy with inammation-mediated status epilepticus. Lancet Neurol 2011;10:99108.
[3] Maegaki Y, Kondo A, Okamoto R, Inoue T, Konishi K, Hayashi
A, et al. Clinical characteristics of acute encephalopathy of
obscure origin: a biphasic clinical course is a common feature.
Neuropediatrics 2006;37:26977.
[4] Takanashi J, Oba H, Barkovich AJ, Tada H, Tanabe H,
Yamanouchi H, et al. Diusion MRI abnormalities after
prolonged febrile seizures with encephalopathy. Neurology
2006;66:13049.
[5] Mizuguchi M, Yamanouchi H, Ichiyama T, Shiomi M. Acute
encephalopathy associated with inuenza and other viral infections. Acta Neurol Scand Suppl 2007;186:4556.
[6] Maytal J, Shinnar S, Moshe SL, Alvarez LA. Low morbidity and
mortality of status epilepticus in children. Pediatrics 1989;83:32331.
[7] Hoshino A, Saitoh M, Oka A, Okumura A, Kubota M, Saito Y,
et al. Epidemiology of acute encephalopathy in Japan, with
emphasis on the association of viruses and syndromes. Brain Dev
2012;34:33743.
[8] Okamoto R, Fujii S, Inoue T, Lei K, Kondo A, Hirata T, et al.
Biphasic clinical course and early white matter abnormalities may
be indicators of neurological sequela after status epilepticus in
children. Neuropediatrics 2006;37:3241.
[9] Rossetti AO, Hurwitz S, Logroscino G, Bromeld EB. Prognosis of
status epilepticus: role of aetiology, age, and consciousness
impairment at presentation. J Neurol Neurosurg Psychiatry 2006;
77:6115.
[10] Legriel S, Azoulay E, Resche-Rigon M, Lemiale V, Mourvillier B,
Kouatchet A, et al. Functional outcome after convulsive status
epilepticus. Crit Care Med 2010;38:2295303.
[11] Kravljanac R, Jovic N, Djuric M, Jankovic B, Pekmezovic T.
Outcome of status epilepticus in children treated in the intensive
care unit: a study of 302 cases. Epilepsia 2011;52:35863.
[12] Raspall-Chaure M, Chin RF, Neville BG, Scott RC. Outcome of
paediatric convulsive status epilepticus: a systematic review.
Lancet Neurol 2006;5:76979.
[13] Sadarangani M, Seaton C, Scott JA, Ogutu B, Edwards T, Prins
A, et al. Incidence and outcome of convulsive status epilepticus in
Kenyan children: a cohort study. Lancet Neurol 2008;7:14550.
[14] Lambrechtsen FA, Buchhalter JR. Aborted and refractory status
epilepticus in children: a comparative analysis. Epilepsia 2008;49:
61525.
[15] Dunn DW. Status epilepticus in children: etiology, clinical
features, and outcome. J Child Neurol 1988;3:16773.
[16] Maegaki Y, Kurozawa Y, Hanaki K, Ohno K. Risk factors for
fatality and neurological sequelae after status epilepticus in
children. Neuropediatrics 2005;36:18692.
[17] Nagao T, Morishima T, Kimura H, Yokota S, Yamashita N,
Ichiyama T, et al. Prognostic factors in inuenza-associated
encephalopathy. Pediatr Infect Dis J 2008;27:3849.
[18] Rathakrishnan R, Sidik NP, Huak CY, Wilder-Smith EP.
Generalised convulsive status epilepticus in Singapore: clinical
outcomes and potential prognostic markers. Seizure 2009;18:
2025.
[19] Hayashi N, Okumura A, Kubota T, Tsuji T, Kidokoro H,
Fukasawa T, et al. Prognostic factors in acute encephalopathy
with reduced subcortical diusion. Brain Dev 2012;34:6329.
[20] Loddenkemper T, Syed TU, Ramgopal S, Gulati D, Thanaviratananich S, Kothare SV, et al. Risk factors associated with death
in in-hospital pediatric convulsive status epilepticus. PLoS One
2012;7:e47474.
[21] Chin RF, Neville BG, Peckham C, Bedford H, Wade A, Scott
RC. Incidence, cause, and short-term outcome of convulsive
status epilepticus in childhood: prospective population-based
study. Lancet 2006;368:2229.
[22] Lyon G, Dodge PR, Adams RD. The acute encephalopathies of
obscure origin in infants and children. Brain 1961;84:680708.
[23] Sugaya N. Inuenza-associated encephalopathy in Japan. Semin
Pediatr Infect Dis 2002;13:7984.
[24] Nakai Y, Itoh M, Mizuguchi M, Ozawa H, Okazaki E,
Kobayashi Y, et al. Apoptosis and microglial activation in
inuenza encephalopathy. Acta Neuropathol 2003;105:2339.
[25] Jequier Gygax M, Deonna T, Maeder P, Mayor-Dubois C,
Roulet-Perez E. Acute infantile encephalopathy predominantly
aecting the frontal lobe (AIEF): a European case. Eur J Paediatr
Neurol 2011;15:15862.
[26] Raha S, Udani V. Acute infantile encephalopathy predominantly
aecting the frontal lobes (AIEF). Indian J Pediatr 2012;79:
16547.
[27] Chen Y, Mizuguchi H, Yao D, Ide M, Kuroda Y, Shigematsu Y,
et al. Thermolabile phenotype of carnitine palmitoyltransferase II
variations as a predisposing factor for inuenza-associated
encephalopathy. FEBS Lett 2005;579:20404.
[28] Shinohara M, Saitoh M, Nishizawa D, Ikeda K, Hirose S,
Takanashi J, et al. ADORA2A polymorphism predisposes
children to encephalopathy with febrile status epilepticus. Neurology 2013;80:15716.
Please cite this article in press as: Maegaki Y et al. Early predictors of status epilepticus-associated mortality and morbidity in children. Brain
Dev (2014), http://dx.doi.org/10.1016/j.braindev.2014.08.004
Das könnte Ihnen auch gefallen
- AAP UTI in InfantsDokument7 SeitenAAP UTI in InfantsGayl CordovaNoch keine Bewertungen
- Artículo 2 PDFDokument13 SeitenArtículo 2 PDFvitruvianxyzNoch keine Bewertungen
- Nephrotic SyndromeDokument14 SeitenNephrotic SyndromeKatia Rivera FabiánNoch keine Bewertungen
- Gold SpanishDokument41 SeitenGold Spanishdra.hadley100% (1)
- Gold SpanishDokument41 SeitenGold Spanishdra.hadley100% (1)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- D8045-16 Standard Test Method For Acid Number of Crude Oils and Petroleum Products by CatalyticDokument6 SeitenD8045-16 Standard Test Method For Acid Number of Crude Oils and Petroleum Products by CatalytichishamNoch keine Bewertungen
- Child Abuse Lesson PlanDokument7 SeitenChild Abuse Lesson PlanIrvie manalacNoch keine Bewertungen
- Budget Reform ProgramDokument31 SeitenBudget Reform ProgramSannyboy DatumanongNoch keine Bewertungen
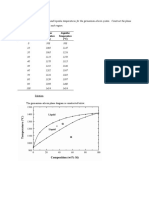
- Composition Solidus Temperature Liquidus Temperature: (WT% Si) (°C) (°C)Dokument7 SeitenComposition Solidus Temperature Liquidus Temperature: (WT% Si) (°C) (°C)Muhammad Ibkar YusranNoch keine Bewertungen
- Vocabulary June v22Dokument2 SeitenVocabulary June v22Wiston TonwisNoch keine Bewertungen
- Leonard Peikoff-Introduction To LogicDokument20 SeitenLeonard Peikoff-Introduction To Logicbursa07Noch keine Bewertungen
- Saep 1160Dokument12 SeitenSaep 1160JithuJohn100% (1)
- 432.01 Managing HSE in A Geophysical Nov 2017Dokument138 Seiten432.01 Managing HSE in A Geophysical Nov 2017Andrei Savu100% (1)
- 10 Major Sulfuric Acid Industrial Applications - WorldOfChemicalsDokument9 Seiten10 Major Sulfuric Acid Industrial Applications - WorldOfChemicalsFarhad MalikNoch keine Bewertungen
- Telecommunications GroundingDokument24 SeitenTelecommunications GroundingMike FordealsNoch keine Bewertungen
- Fulltext PDFDokument55 SeitenFulltext PDFManikandan VpNoch keine Bewertungen
- Modelling The Effects of Condensate Banking On High CGR ReservoirsDokument11 SeitenModelling The Effects of Condensate Banking On High CGR ReservoirslikpataNoch keine Bewertungen
- 493M GHC MG Mep WS L3 205 1B 00Dokument1 Seite493M GHC MG Mep WS L3 205 1B 00shehanNoch keine Bewertungen
- Flight School BundleDokument43 SeitenFlight School BundleyoyoNoch keine Bewertungen
- Ejercicio 1 Curso BRBDokument2 SeitenEjercicio 1 Curso BRBAlex MolinaNoch keine Bewertungen
- Standardization 1 PDFDokument7 SeitenStandardization 1 PDFmazharul HasanNoch keine Bewertungen
- Midterm2 KeyDokument6 SeitenMidterm2 KeyHungDoNoch keine Bewertungen
- How Hydraulic Valve Lifters WorkDokument1 SeiteHow Hydraulic Valve Lifters WorkSanket Sabale100% (1)
- Grades 4-10: Search Jobs in IndiaDokument2 SeitenGrades 4-10: Search Jobs in IndiaMD AKIL AHMEDNoch keine Bewertungen
- AssaultDokument12 SeitenAssaultEd Mundo100% (3)
- MSW TACSOP v.3.3Dokument59 SeitenMSW TACSOP v.3.3Mira BellaNoch keine Bewertungen
- K.golden Flower MeditationDokument6 SeitenK.golden Flower Meditationamjr1001Noch keine Bewertungen
- LaserDokument12 SeitenLasercabe79Noch keine Bewertungen
- Jurnal Kasus Etikolegal Dalam Praktik KebidananDokument13 SeitenJurnal Kasus Etikolegal Dalam Praktik KebidananErni AnggieNoch keine Bewertungen
- According To India International Coffee Festival in The TitledDokument4 SeitenAccording To India International Coffee Festival in The Titledsalman vavaNoch keine Bewertungen
- Financial Problems Are Commonly Faced by EveryoneDokument2 SeitenFinancial Problems Are Commonly Faced by EveryoneGrace Ann Mancao PototNoch keine Bewertungen
- Neicchi 270 ManualDokument33 SeitenNeicchi 270 Manualmits2004Noch keine Bewertungen
- Cell Division-Mitosis Notes: 2 New CellsDokument21 SeitenCell Division-Mitosis Notes: 2 New CellsCristina MariaNoch keine Bewertungen
- 01 05 Justin Capouch CBI PresentationDokument18 Seiten01 05 Justin Capouch CBI PresentationprabhuarunkumarNoch keine Bewertungen
- Total Parenteral NutritionDokument8 SeitenTotal Parenteral NutritionTemiloluwa AdeyemiNoch keine Bewertungen