Beruflich Dokumente
Kultur Dokumente
Article On Breast
Hochgeladen von
1234chocoOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Article On Breast
Hochgeladen von
1234chocoCopyright:
Verfügbare Formate
Breast series CLINICAL PRACTICE
Making sense of breast
pathology
Michael Bilous, MA, MBChB, FRCPA, is Clinical Associate Professor of Pathology, NSW Breast Cancer Institute,
University of Sydney, and Director of Tissue Pathology, Institute of Clinical Pathology and Medical Research,
Westmead Hospital, New South Wales.
Meagan Brennan, BMed, FRACGP, DFM, FASBP, is a breast physician, NSW Breast Cancer Institute,
Westmead Hospital, New South Wales. meaganb@bci.org.au
James French, MBBS, FRACS, is a breast and endocrine surgeon, NSW Breast Cancer Institute, Westmead Hospital,
New South Wales.
John Boyages, MBBS, FRANZCR, PhD, is Associate Professor and Executive Director, NSW Breast Cancer Institute,
Westmead Hospital, New South Wales.
An understanding of breast pathology is essential when caring for women with breast disease. Part five of this series discusses
the spectrum of common benign and malignant conditions including the distinction between invasive and noninvasive breast
cancer. It also aims to increase the general practitioners confidence in understanding breast pathology reports, arranging
appropriate referral for patients, and educating women about their disease.
here are three main categories of
breast disease:
Benign conditions these may require
treatment to relieve symptoms
Malignant conditions invasive carcinoma
requires multidisciplinary assessment
and treatment. Treatment may include
surgery, radiotherapy, and chemotherapy;
their use reflects the severity of disease
and its mortality rate. Similarly, the
pre-invasive form of breast carcinoma
ductal carcinoma in situ (DCIS) requires
treatment to ensure it does not directly
progress to invasive carcinoma
Conditions that identify the patient to
be at increased risk of future breast
carcinoma these include conditions such
as lobular neoplasia and atypical ductal
hyperplasia (ADH). Patients with these
conditions require close surveillance to
detect any onset of breast carcinoma at
an early stage, thereby maximising the
effectiveness of therapy.
The investigation of a breast abnormality
and the categorisation of any disease rely
on a combination of clinical, imaging and
biopsy techniques. These culminate in the
examination of a cell or tissue sample by a
pathologist.
Once the diagnosis of invasive breast
carcinoma has been made, the pathologist
is required to provide further information
including a range of prognostic and
predictive factors that help determine
appropriate therapy. A prognostic factor
is any measurement available at the time
of diagnosis associated with disease free
or overall survival such as tumour size or
nodal status. A predictive factor is any
measurement associated with response or
lack of response to a particular therapy such
as an oestrogen receptor positive tumour
responding to tamoxifen.
The pathologist is an important member
of the multidisciplinary team responsible
for the care of patients with breast disease.
For the patient with breast carcinoma,
tailoring therapy for the individual has
become the aim for all those involved. There
is increasing dependence on accurate and
reliable pathology reporting to reach this
goal.
Breast biopsy techniques
The pathologist may be presented with a
range of breast specimens. These may be
obtained by fine needle aspiration (FNA),
core biopsy, or open surgical biopsy.
Fine needle aspiration biopsy is a simple,
inexpensive, reliable and rapid technique
for obtaining cells from a targeted area of
breast tissue. It does however, depend
on the skill and experience of both the
aspirator providing the specimen and the
cytopathologist interpreting the cells.
A core biopsy involves obtaining single
or multiple tissue cores from the breast by
conventional or vacuum assisted means.
A vacuum assisted core biopsy (eg .
Mammotome ) results in a larger sample
and may in some cases allow complete
removal of the t arget abnormalit y in
Reprinted from Australian Family Physician Vol. 34, No. 7, July 2005 4 581
Clinical practice: Making sense of breast pathology
the breast.
If the lesion is impalpable, the surgeon
performing an open biopsy may require
imaging localisation of the target lesion
using mammography or ultrasound and
hook wire placement.
For these sampling techniques, it is
important that the pathologist receives
all relevant information concerning the
indication for biopsy and imaging findings.
Benign breast disease
In the past, benign breast changes were
often referred to collectively by terms
such as fibrocystic disease, mammary
dysplasia and benign mastopathy. These
terms were used to refer to a range of
benign breast changes, from cyclical clinical
nodularity to benign proliferative and
nonproliferative pathological changes seen
on biopsy. In the past 20 years, there has
been a move away from using these poorly
defined terms in favour of more specific
pathological terms. These specific terms
not only describe the particular lesion or
breast tissue change with greater accuracy,
but also provide an indication of the risk of
future breast carcinoma development.1
Table 1. Benign breast disease and invasive carcinoma risk2
No increased risk
Adenosis, other than sclerosing adenosis
Duct ectasia
Fibroadenoma lacking complex features
Fibrosis
Mastitis
Mild ductal hyperplasia of usual type without atypia
Cysts, gross or microscopic
Simple, apocrine metaplasia without associated hyperplasia or adenosis
Squamous metaplasia
Slightly increased risk (relative risk 1.52.0)
Complex fibroadenoma
Moderate or florid ductal hyperplasia of usual type without atypia
Sclerosing adenosis
Solitary papilloma without atypical hyperplasia
Moderately increased risk (relative risk 4.05.0)
Atypical ductal hyperplasia
Atypical lobular hyperplasia
Risk of carcinoma
There are several types of benign breast
disease shown to increase the risk of
developing breast carcinoma. The magnitude
of the risk appears to be dependent on the
degree of proliferative change and atypia
seen in the biopsy material (Table 1). 2
Much of the information used in this risk
assessment is derived from retrospective
r ev i ew s o f b r e a s t p a t h o l o g y. Th e s e
reviews are obtained from the biopsies
of thousands of women who continue to
be followed up, in some cases for more
than 20 years after the breast biopsy
was performed.3
Proliferative benign breast disease in the
form of ductal hyperplasia of moderate or
florid type can therefore be considered a
risk factor for developing invasive carcinoma
(Figure 1, 2). The magnitude of risk
is increased by other factors such as
Figure 1. Atypical ductal hyperplasia. The duct
shows a proliferation of atypical monomorphic cells
whose appearance closely resembles that of low
nuclear grade DCIS. The arrangement of the cells is
irregular in contrast to those seen in Figure 5
Epithelial
hyperplasia
Atypical ductal
hyperplasia
Figure 2. Florid ductal hyperplasia of usual type.
The two ducts are filled by a mixed population of cells
Ductal
carcinoma
in situ
Invasive
carcinoma
Figure 3. Continuum of change
family history of breast carcinoma and
nulliparity. It is important to note that this
associated increased risk of future invasive
carcinoma applies to both breasts, and
continues to be seen for 15 or more years
after diagnosis.3
582 3Reprinted from Australian Family Physician Vol. 34, No. 7, July 2005
Clinical implications
Common benign breast lesions include
fibroadenomas, cysts, and intraduct
papillomas. Breast lesions identified
as risk factors for subsequent invasive
breast carcinoma may require a different
management strategy (Table 2).
Clinical practice: Making sense of breast pathology
Table 2. Clinical implications of benign breast disease
Fibroadenoma
Carcinoma risk
no increased risk associated with fibroadenoma without hyperplasia
slightly increased risk of future breast carcinoma if hyperplasia, with or without atypia
Management implications
no special management needed for women with fibroadenoma without hyperplasia
women with a previous fibroadenoma with hyperplasia have a slightly increased risk of future breast carcinoma (usually no special
management is recommended as the increased risk is extremely small)
Cysts
Carcinoma risk
conflicting evidence as to whether cysts lead to increased risk (some studies show no increase in risk,4 others show a small
increase in risk5)
on balance there may be slight increase in risk, although not of clinical significance
Management implications
no special management is required
Intraduct papilloma
Carcinoma risk
a solitary intraduct papilloma results in a slightly increased risk
Diagnostic difficulty
intraduct papilloma may be difficult to distinguish from intraduct papillary carcinoma on percutaneous biopsy
Management implications
if a papilloma is suspected from FNA or core biopsy, surgical excision is recommended for full pathological assessment and to exclude
intraduct papillary carcinoma
Ductal hyperplasia of usual type (HUT) and ADH
Carcinoma risk
mild HUT without atypia carries no increased risk
ADH carries an increased risk (relative risk 45)
when associated with a family history of breast carcinoma in a first degree relative, ADH carries a 10 times increase in risk3
Diagnostic difficulty
pathological distinction between the two conditions is often extremely difficult and reproducibility of diagnosis between pathologists is poor
difficult to distinguish ADH from DCIS (carries an even higher risk of direct progression to invasive carcinoma)
Management implications
HUT needs no special management or surveillance
when ADH is suspected on FNA or core biopsy, excision of the lesion is recommended for further assessment as some will prove to be
DCIS, or may be adjacent to foci of DCIS6
if an open biopsy specimen shows ADH (without DCIS) there is no need for further management of the lesion, however given the
magnitude of risk, close surveillance by annual mammography and clinical breast examination is advisable
Atypical lobular hyperplasia (ALH)
Carcinoma risk
carries an increased risk similar to ADH
Diagnostic difficulty
some lesions displaying ALH on core biopsy are upgraded to carcinoma in situ or invasive carcinoma (usually ductal) after open biopsy7
Management implications
increasing trend to surgically excise lesions that show ALH on core biopsy
women with previous ALH on a core or excision biopsy should be monitored in the same way as women diagnosed with ADH
Reprinted from Australian Family Physician Vol. 34, No. 7, July 2005 4 583
Clinical practice: Making sense of breast pathology
The evolution of breast carcinoma
Invasive breast carcinoma has traditionally
been regarded as the final stage in a
continuum of proliferative changes in
the breast (Figure 3). The concept of a
continuum in the development of breast
carcinoma is now being questioned,
and classification of breast lesions is
being reconsidered.
It is likely that both genetics and
p a t h o l o g y w i l l c o n t r i b u t e t o f u tu r e
classifications of benign and malignant
breast lesions, and to our understanding
of the progression between the two. Some
benign proliferative lesions that show
atypia increase the risk of future breast
carcinoma. The lesions of DCIS and lobular
carcinoma in situ (LCIS) are considered
pre-invasive malignant lesions, which
are one step further along the spectrum
toward invasive breast carcinoma. The
management of these lesions is changing
with a trend toward more aggressive
management of proliferative and in situ
lesions (surgical excision).
Table 3. In situ breast carcinoma pathology report
Nuclear grade
high grade
intermediate grade
low grade
Lesion size
Pathological type/architecture
comedo, solid, cribriform, micropapillary
Margin status
margins involved with tumour, or
margins clear of tumour cells (measure clearance in mm)
Associated microcalcification
present or not
Presence of necrosis
present or not (presence is a poor prognostic feature)
Hormone receptors
can be tested (not routinely recommended)
the role of hormonal agents such as tamoxifen remains unclear in this setting
In situ breast carcinomas
In situ breast lesions include DCIS and
LCIS. In DCIS, the epithelial cells have
undergone malignant change, but the
malignant cells have not invaded through
the basement membrane of the duct or
acini to become invasive carcinoma. There
are several types of DCIS subclassified
by the pathologist into high, intermediate
and low nuclear grade, according to the
appearance of the cell nuclei (Figure 4, 5).
High nuclear grade DCIS has a high rate
of recurrence following treatment, and a
high proportion of these recurrences are as
invasive carcinoma (Figure 6). By contrast,
low nuclear grade DCIS has a lower rate of
recurrence and of progression to invasive
carcinoma. Intermediate nuclear grade
DCIS has an intermediate recurrence rate,
between that of high and low grade lesions.
However, low grade DCIS can recur at a
constant rate over many years. Although
the risks of local recurrence are lower at
5 years after initial treatment, the rates
Figure 4. High nuclear grade DCIS. The ducts
contain an increased number of large cells that
remain confined within the duct. The centres of
involved ducts contain necrotic cellular debris
Figure 6. Invasive duct carcinoma of no special type,
grade 3. Large pleomorphic carcinoma cells infiltrate
the breast in groups forming irregular tubules
Figure 5. Low nuclear grade DCIS. The duct is
expanded by a uniform population of cells forming
a cribriform or sieve-like pattern
Figure 7. Lobular carcinoma in situ. Small uniform
cells expand and fill the lobule
increase and approach that of high grade
DCIS 10 years after initial treatment.8
Treatment of DCIS is therefore dependent
to some extent on the classification of the
lesion on pathological examination. The
pattern of proliferation of the malignant cells
in DCIS affected ducts is recorded, although
the architecture of the lesion appears to
584 3Reprinted from Australian Family Physician Vol. 34, No. 7, July 2005
Clinical practice: Making sense of breast pathology
Table 4. DCIS and LCIS
Figure 8. Invasive lobular carcinoma, grade 1.
Carcinoma cells are small and uniform, and often
infiltrate the breast in single file columns
have very little correlation with the clinical
course of the disease All pathology reports
of an open biopsy of DCIS should include the
information listed in Table 3.
Lobular carcinoma in situ is currently
thought of as a marker of increased risk of
future invasive carcinoma, which may be
of ductal, lobular or other histological type
(Figure 7, 8). Lobular carcinoma in situ has
no specific clinical or imaging properties
and is usually diagnosed by the pathologist
as an incidental finding in a breast biopsy
performed for some other indication.
It is not defined as or treated as breast
cancer, however this thinking is changing.
Issues related to cancer risk, diagnosis
and management of DCIS and LCIS are
given in Table 4.
Invasive breast carcinoma
The pathology report
In recent years, breast carcinoma pathology
reports resulting from open breast biopsy,
breast conser vation and mastectomy
s p e c i m e n s h ave b e e n i n c r e a s i n g l y
standardised and expressed in summary or
synoptic format. Following the pathologists
description of the macroscopic appearance
of the specimen, there is usually a
summary of the critical features used to
make treatment decisions. Each report
should therefore contain all the important
prognostic and predictive information
required to guide prognosis and treatment.
The pathology report should include all the
information in Table 5.12,13
DCIS
Carcinoma risk
DCIS has the potential to develop into an invasive carcinoma (10 times risk)
after treatment DCIS can recur (may recur as invasive carcinoma rather than as
DCIS2)
future risk of in situ or invasive carcinoma elsewhere in the breast in women
who have had DCIS
Diagnostic difficulty
low nuclear grade DCIS can be extremely difficult to distinguish from ADH, and
small foci of invasive carcinoma may be missed in an excision specimen
DCIS diagnosed in a core biopsy may be found to be invasive carcinoma when
the lesion is excised (~15% of cases9)
Management implications
lesions diagnosed as DCIS on core biopsy require excision of the lesion for further
assessment in case invasive carcinoma is present
lesions confirmed to be DCIS on excision need to be managed as high risk
lesions, with all the principles of cancer management in mind (given that if the
lesion recurs, it may be invasive)
complete excision of the lesion is necessary with attention to margins
(mastectomy or wide local excision)
consider adjuvant treatment (radiotherapy) if a mastectomy has not been
performed. The role of tamoxifen remains unclear
consider treatment of the axilla (not currently recommended for pure DCIS, but
this is changing with the advent of sentinel lymph node biopsy and may be
recommended in the future for large areas of high nuclear grade DCIS)
women with previous DCIS need close monitoring (as for women with previous
invasive breast carcinoma) with the aim of detecting recurrence and new
carcinomas elsewhere in the breast
LCIS
Carcinoma risk
LCIS carries an increased risk of future breast carcinoma (either invasive ductal
or invasive lobular carcinoma)
risk is in the order of 12% for future breast carcinoma (higher in women with
previous LCIS than those with previous DCIS10)
future breast carcinoma may occur in either breast (not just original LCIS)
Diagnostic difficulty
the lesion may be underestimated on core biopsy and cannot be diagnosed on
FNA biopsy
there is emerging evidence that a significant number of lesions showing LCIS
on core biopsy are upgraded on excision biopsy to invasive carcinoma (either
ductal or lobular)11
Management implications
in the past, LCIS was considered to be a marker of future bilateral risk of
invasive carcinoma rather than a lesion requiring treatment in its own right this
thinking is changing
there is a trend to consider excising lesions that show LCIS on core biopsy
lesions confirmed to be LCIS on excision biopsy are usually managed with ongoing
close surveillance rather than further surgery
women with previous LCIS need close monitoring of both breasts as the risk of
future invasive carcinoma in either breast is high10
Reprinted from Australian Family Physician Vol. 34, No. 7, July 2005 4 585
Clinical practice: Making sense of breast pathology
Conclusion
References
1.
An understanding of breast pathology
is essential when caring for women with
breast disease. There are many benign breast
conditions that must be approached with
caution. They may reflect an undersampled
area of more serious breast pathology or
carry an increased risk of invasive carcinoma
in the future.
Conflict of interest: none declared.
2.
3.
4.
5.
Hutter RVP. Goodbye to fibrocystic disease. N
Engl J Med 1985;312:17981.
Rosen PP. Rosens breast pathology. 2nd ed.
Philadelphia: Lippincott, Williams & Wilkins, 2001.
Page DL, Dupont WD, Rogers LW, Rados MS.
Atypical hyperplastic lesions of the female breast. A
long term follow up study. Cancer 1985;55:2678708.
Dixon JM, McDonald C, Elton RA, Miller WR.
Risk of breast cancer in women with palpable
breast cysts: a prospective study. Edinburgh Breast
Group. Lancet 1999;353:17425.
Dixon JM. Cystic disease and fibroadenoma of the
breast: natural history and relation to breast cancer
risk. Br Med Bull 1991;47:25871.
Table 5. The invasive breast carcinoma pathology report
Tumour size
important prognostic factor
Histological type
invasive ductal carcinoma accounts for 80% of breast cancers
invasive lobular carcinoma accounts for 1015% of breast cancers
special types: tubular, cribriform, and mucinous carcinomas (particularly good
prognosis tumours12)
papillary, medullary and other uncommon histological types
Histological grade
important prognostic factor
grade 13 based on the combination of three pathological features: nuclear grade,
tubule formation, and mitotic rate
Accompanying DCIS
associated with local recurrence if extensive in patients treated for invasive
carcinoma by breast conservation surgery with close or positive margins 14
Lymph node involvement
important prognostic factor: the number of nodes dissected and the number
involved with metastatic carcinoma
Margins of excision
involvement of resection margins with invasive carcinoma or DCIS and margin
distance from cancer cells
these factors guide further treatment such as additional surgery or radiotherapy
may also predict risk, local recurrence
Lymphovascular invasion (LVI)
evidence of tumour cells invading into vessels
Presence of LVI is a poor prognostic factor
Changes in adjacent breast tissue
eg. DCIS, ADH, ALH, LCIS
Hormone and other receptors
predict response to adjuvant treatment
ER (oestrogen) and PR (progesterone) receptors
HER2 receptor overexpression is a marker of poor prognosis and also of response
of the carcinoma to Herceptin therapy. HER2 positive tumours may respond better
to anthracycline type chemotherapy and are generally less responsive to endocrine
therapy
586 3Reprinted from Australian Family Physician Vol. 34, No. 7, July 2005
6.
7.
8.
9.
10.
11.
12.
13.
14.
Harvey JM, Sterrett GF, Frost FA. Atypical ductal
hyperplasia and atypia of uncertain significance
in core biopsies from mammographically detected
lesions: correlation with excision diagnosis.
Pathology 2002;34:4106.
Irfan K, Brem RF. Surgical and mammographic
follow up of papillary lesions and atypical lobular
hyperplasia diagnosed with stereotactic vacuum
assisted biopsy. Breast J 2002;8:2303.
Boyages J, Delaney G, Taylor R. Predictors of local
recurrence after treatment of ductal carcinoma in
situ: a meta-analysis. Cancer 1999;85:61628.
Jackman RJ, Nowels KW, Rodriguez-Soto
J, Marzoni FA, Finkelstein SI, Shepard MJ.
Stereotactic, automated large core needle biopsy
of nonpalpable breast lesions: false-negative and
histologic underestimation rates after long term
follow up. Radiology 1999;210:799805.
Claus EB, Stowe M, Carter D, Holford T. The
risk of a contralateral breast cancer among women
diagnosed with ductal and lobular breast carcinoma
in situ: data from the Connecticut Tumor Registry.
Breast 2003;12:4516.
Jacobs TW, Connolly JL, Schnitt SJ. Nonmalignant
lesions in breast core needle biopsies: to excise or
not to excise? Am J Surg Pathol 2002;26:1095110.
Viale G. Histopathology of primary breast cancer
2003. Breast 2003;12:3916.
Australian Cancer Network Working Party. The
pathology reporting of breast cancer: a guide for
pathologists, surgeons, radiologists and oncologists.
2nd ed. Sydney, 2001.
Boyages J, Connolly JL, Schnitt SJ, Harris JR.
Definition of an extensive intraductal component.
In: The Pathology Reporting of Breast Cancer.
Australian Cancer Network. CAN Publication No.
2;6678.
AFP
Correspondence
Email: afp@racgp.org.au
Das könnte Ihnen auch gefallen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- ART THERAPY, Encyclopedia of Counseling. SAGE Publications. 7 Nov. 2008.Dokument2 SeitenART THERAPY, Encyclopedia of Counseling. SAGE Publications. 7 Nov. 2008.Amitranjan BasuNoch keine Bewertungen
- Assessment Test Descriptions PyDokument19 SeitenAssessment Test Descriptions PyDewa Ayu VeronicaNoch keine Bewertungen
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- MCQ PebcDokument7 SeitenMCQ Pebcshamram20050% (1)
- Healthy FoodDokument13 SeitenHealthy FoodKayden0% (1)
- Preoperative AssessmentDokument9 SeitenPreoperative Assessment1234chocoNoch keine Bewertungen
- Mapeh 9 4th Quarter ExamDokument6 SeitenMapeh 9 4th Quarter ExamAple Rigor100% (2)
- Mobilization of CabinDokument1 SeiteMobilization of CabinRashidi RahmanNoch keine Bewertungen
- Approach To The History and Evaluation of Vertigo and DizzinessDokument24 SeitenApproach To The History and Evaluation of Vertigo and DizzinessPAULA GABRIELA ABAD POLONoch keine Bewertungen
- Language of PreventionDokument9 SeitenLanguage of Prevention1234chocoNoch keine Bewertungen
- Fairy Tail - Main ThemeDokument3 SeitenFairy Tail - Main Theme1234chocoNoch keine Bewertungen
- Mbs Quick Guide: JULY 2020Dokument2 SeitenMbs Quick Guide: JULY 20201234chocoNoch keine Bewertungen
- Code Geass - StoriesDokument5 SeitenCode Geass - Stories1234chocoNoch keine Bewertungen
- Blue BirdDokument7 SeitenBlue Bird1234chocoNoch keine Bewertungen
- Doctor Talk: Communication Practice Role PlaysDokument6 SeitenDoctor Talk: Communication Practice Role Plays1234chocoNoch keine Bewertungen
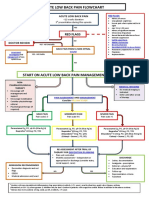
- Acute Low Back Pain Flowchart January 2017Dokument1 SeiteAcute Low Back Pain Flowchart January 20171234chocoNoch keine Bewertungen
- Topical Steroids (Sep 19) PDFDokument7 SeitenTopical Steroids (Sep 19) PDF1234chocoNoch keine Bewertungen
- Blue Card Declaration PDFDokument1 SeiteBlue Card Declaration PDF1234chocoNoch keine Bewertungen
- PBM Module1 MTP Template 0Dokument2 SeitenPBM Module1 MTP Template 01234chocoNoch keine Bewertungen
- Taking A Social and Cultural HistoryDokument3 SeitenTaking A Social and Cultural History1234chocoNoch keine Bewertungen
- Managing Mental Illness in Patients From CALD Backgrounds: PsychiatryDokument5 SeitenManaging Mental Illness in Patients From CALD Backgrounds: Psychiatry1234chocoNoch keine Bewertungen
- A Conceptual Framework For HealthDokument1 SeiteA Conceptual Framework For Health1234chocoNoch keine Bewertungen
- Acute Post-Op Pain ManagementDokument4 SeitenAcute Post-Op Pain Management1234chocoNoch keine Bewertungen
- Barrett's Esophagus: Identifying The Squamocolumnar (SC) and Gastroesophageal (GE) Junctions EndoscopicallyDokument10 SeitenBarrett's Esophagus: Identifying The Squamocolumnar (SC) and Gastroesophageal (GE) Junctions Endoscopically1234chocoNoch keine Bewertungen
- Prenatal Screening Test (AUS) PDFDokument24 SeitenPrenatal Screening Test (AUS) PDFshirley_ling_15Noch keine Bewertungen
- Mata Pelajaran: BAHASA INGGRIS Sat. Pendidikan: SMA Kelas / Program: XIDokument7 SeitenMata Pelajaran: BAHASA INGGRIS Sat. Pendidikan: SMA Kelas / Program: XICy FullNoch keine Bewertungen
- Surgery KGMU Proff Chapterwise by Arif Naseem 2009-2021Dokument4 SeitenSurgery KGMU Proff Chapterwise by Arif Naseem 2009-2021DR. PARDEEP SHARMANoch keine Bewertungen
- Updating Workplace First Aid KitsDokument2 SeitenUpdating Workplace First Aid KitsPANAMA GREEN BUILDING COUNCILNoch keine Bewertungen
- SwatiDokument11 SeitenSwatisd imNoch keine Bewertungen
- Epoch Elder Care Provides High Quality Assisted Living HomesDokument17 SeitenEpoch Elder Care Provides High Quality Assisted Living HomesMahesh MahtoliaNoch keine Bewertungen
- Pheochromocytoma Symptoms, Treatment, Diagnosis, TestDokument1 SeitePheochromocytoma Symptoms, Treatment, Diagnosis, TestIulian GherasimNoch keine Bewertungen
- UN Declaration of The Rights of The Child (1959)Dokument2 SeitenUN Declaration of The Rights of The Child (1959)bonalawNoch keine Bewertungen
- Albumin Administration in The Acutely Ill: What Is New and Where Next?Dokument10 SeitenAlbumin Administration in The Acutely Ill: What Is New and Where Next?Peter AgabaNoch keine Bewertungen
- Understanding COVID - 19 PandemicDokument10 SeitenUnderstanding COVID - 19 PandemicShyam KantNoch keine Bewertungen
- Lesson 1 Handwashing Powerpoint HSDokument38 SeitenLesson 1 Handwashing Powerpoint HSCharlene Fadrigon-OtazuNoch keine Bewertungen
- Practice Test - Mid TermDokument2 SeitenPractice Test - Mid Termngaanhc2ngtNoch keine Bewertungen
- Kernow LMC Newsletter - October 2019 Edition FINAL USE For WebsiteDokument14 SeitenKernow LMC Newsletter - October 2019 Edition FINAL USE For WebsiteCornwall and Isles of Scilly LMCNoch keine Bewertungen
- AAE Position On Vital Pulp Therapy July ProviderDokument8 SeitenAAE Position On Vital Pulp Therapy July ProviderSweet ToothNoch keine Bewertungen
- October 2023 PRC PLE Schedule and Reminders 2Dokument4 SeitenOctober 2023 PRC PLE Schedule and Reminders 2TrisNoch keine Bewertungen
- Liposuction: Immediately After SurgeryDokument1 SeiteLiposuction: Immediately After SurgeryScott J. Zevon, MD, FACSNoch keine Bewertungen
- Summary - Hyaline Membrane DiseaseDokument1 SeiteSummary - Hyaline Membrane DiseaseJet BautistaNoch keine Bewertungen
- Apixaban in Patients With Atrial FibrillationDokument12 SeitenApixaban in Patients With Atrial FibrillationthedancingseaNoch keine Bewertungen
- By Trevor Hiltbrand - Reviwed By: Free Shipping On Orders $150+ (U.S. Only.)Dokument4 SeitenBy Trevor Hiltbrand - Reviwed By: Free Shipping On Orders $150+ (U.S. Only.)Bruno ManestarNoch keine Bewertungen
- Hematemesis PDFDokument7 SeitenHematemesis PDFkevin_jawanNoch keine Bewertungen
- Drug Study: Phinma University of PangasinanDokument1 SeiteDrug Study: Phinma University of PangasinanVoid LessNoch keine Bewertungen
- A Prospective Study On The Practice of Conversion of Antibiotics From IV To Oral Route and The Barriers Affecting ItDokument3 SeitenA Prospective Study On The Practice of Conversion of Antibiotics From IV To Oral Route and The Barriers Affecting ItInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Caused by The .: Dengue Dengue Fever Is ADokument2 SeitenCaused by The .: Dengue Dengue Fever Is AEdrese AguirreNoch keine Bewertungen
- Suchita Srivastava & Anr Vs Chandigarh Administration On 28 August 2009Dokument11 SeitenSuchita Srivastava & Anr Vs Chandigarh Administration On 28 August 2009Disability Rights AllianceNoch keine Bewertungen