Beruflich Dokumente
Kultur Dokumente
Retinoblastoma Case Report Latest With Reference
Hochgeladen von
Masykur Ramadhan GaniCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Retinoblastoma Case Report Latest With Reference
Hochgeladen von
Masykur Ramadhan GaniCopyright:
Verfügbare Formate
1
Case report
RETINOBLASTOMA
Presenter : 1. Maskur Ramadhan S.Ked (100100083)
2. Muhammad Akbar Batubara S.Ked (100100321)
Supervisor : dr. Yazid Dimyati SpA (K)
Introduction
Retinoblastoma is an embroyonal malignancy of the retina and is the most
common intraocular tumor in children. Although the survival rate of children in the
USA and developed countries with retinoblastoma is extremely high, retinoblastoma
progresses to metastasis disease and death in over 50% of children worldwide.
Furthermore the associated loss of vision and the side effects of therapy are significant
problems that remain to be adressed.
Epidemiology
Approximately 250-350 new cases of retinoblastoma are diagnosed each year in
USA, with no know gender and or racial predilection. The cumulative lifetime
incidence of retinoblastoma is approximately 1:20000 live births, and the
retinoblastoma accounts for 4% of all pediatric malignancies. The median age of this
diagnosis is approximately 2 yr, and over 90% of cases are diagnosed in the children
under the age of 5. Overall about 2 thirds to 3 quarters of children with retinoblastoma
have unilateral tumors, with the remainder have bilateral retinoblastoma. Bilateral
retinoblastoma is more common in younger children, particularly in those diagnosed
under the age of 1 yr.
Retinoblastoma can be either her ditary or sporadic. Hereditary cases usually are
diagnosed at younger age and are multifocal and bilateral, while sporadic cases
usually diagnosed in older children who tend to have unilateral, unifocal involvement.
The hereditary form always associated with the loss of function of Retinoblastoma
gene (RB1) via gene mutation or gene deletion. ,The RB1 gene is located on
chromosome 13q14 and encodes the retinoblastoma protein (Rb), a tumor supressor
protein that controls cell cycle phase transition that has role in apoptosis and cell
differentiation. Many different causative mutation have been identified including
translocation, deletion, insertions, point mutations, and epigenetic modifications such
as gene methylation, The nature of predisposing mutation can affect the penetrane and
expressivity of retinoblastoma development.
According to Knudsons two hit model of oncogenesis, two mutational events are
required for retinoblastoma tumor development. In the hereditery form of
retinoblastoma the first mutation of RB1 gene is inherited through germinal cells and
the secong mutation occurs subsequently in somatic retinal cells. Second mutations
that lead to retinoblastoma often results in loss in normal allele and concomitant loss
of heterozygosity. Most children with hereditary retinoblastoma have spontaneous
new germinal mutations, and both parents have wild type retinoblastoma genes. In the
sporadic form, the two mutations occurs in somatic retinal cells. Heterozygous
carriers of oncogenic RB1 mutations demonstrate variable phenotypic expression.
Clinical manifestations
Retinoblastoma clasically presents with leukocoria, a white pupillary reflex,
white often is first noticedwhen a red reflex is not present at a routine newborn or well
child examination or in a flash phtograph of the child. Strabismus often is the initial
presenting complaint. Orbital inflammation, hyphema, and pupil irregularity can
occur with advancing disease. Pain can occur if secondary glaucoma is present. Only
about 10% of retinoblastoma cases are detected by routine ophthalmologic screening
in
the
context
of
positive
family
history.
Staging
The International Retinoblastoma Staging System (IRSS) may be used for
staging retinoblastoma.
There are several staging systems for retinoblastoma. The IRSS stages are based on
how much cancer remains after surgery to remove the tumor and whether the cancer
has spread.
Stage 0
The tumor is in the eye only. The eye has not been removed and the tumor was treated
without surgery.
Stage I
The tumor is in the eye only. The eye has been removed and no cancer cells remain.
Stage II
The tumor is in the eye only. The eye has been removed and there are cancer cells left
that can be seen only with a microscope.
Stage III
Stage III is divided into stages IIIa and IIIb:
In stage IIIa, cancer has spread from the eye to tissues around the eye socket.
In stage IIIb, cancer has spread from the eye to lymph nodes near the ear or in
the neck.
Stage IV
Stage IV is divided into stages IVa and IVb:
In stage IVa, cancer has spread to the blood but not to the brain or spinal cord.
One or moretumors may have spread to other parts of the body such as the
bone or liver.
In stage IVb, cancer has spread to the brain or spinal cord. It also may have
spread to other parts of the body.6
Diagnosis
Retinoblastomas are usually found when a child is brought to a doctor because he
or she has certain signs or symptoms. Most types of cancer can be found by physical
exam and imaging tests, but treatment is usually not begun until the diagnosis is
confirmed by a biopsy. During a biopsy, the doctor removes a sample from the tumor
and sends it to a lab to be looked at under a microscope. But biopsies are not usually
done to diagnose retinoblastoma for 2 reasons. First, taking a biopsy specimen from a
tumor in the eye cannot be done easily without harming the eye and risking spreading
cancer cells outside the eye. Second, retinoblastoma can be diagnosed accurately by
doctors who have experience with this disease, and it is unlikely to be confused
with other eye problems in children.3
Medical history and physical exam
If your child has signs or symptoms of retinoblastoma, the doctor will examine
your childs eyes and get a complete medical history. The doctor will ask about the
childs symptoms and may ask about any family history of retinoblastoma or other
cancers. This information is important when deciding if more tests and exams are
needed. Your family history is also useful for determining whether other relatives
could possibly pass this gene on to their children or develop this cancer themselves (if
they are young children) and might benefit from genetic counseling. If a
retinoblastoma is suspected, the doctor will refer you to an ophthalmologist (a doctor
who specializes in eye diseases), who will examine the eye closely to be more certain
about the diagnosis. The ophthalmologist will use special lights and magnifying
lenses
to
lookinside
the
eye.
Usually,
the
child
needs
to
be
under
generalanesthesia(asleep) during the exam so that the doctor can take a careful and
detailed look If a diagnosis of retinoblastoma seems likely based on the eye exam,
imaging tests will be
done to help confirm it and to find out how far it may have spread within the eye and
possibly to other parts of the body. Usually an ophthalmologist who specializes in
treating cancers of the eye (called an ocular oncologist) will make the final
determination. This doctor should also be part of the team of doctors treating the
cancer.
Imaging tests3
Imaging tests use x-rays, sound waves, magnetic fields, or radioactive substances to
create pictures of the inside of the body. Imaging tests may be done for a number of
reasons including:
To help tell if a tumor in the eye is likely to be a retinoblastoma
To determine how large the tumor is and how far it has spread
To help determine if treatment has been effective
Children with retinoblastoma may have one or more of these tests.
Ultrasound
Ultrasound uses sound waves to create images of tissues inside the body, such
as the inner parts of the eye. For this test, a small ultrasound probe is placed up
against the eyelid or eyeball. The probe gives off sound waves and detects the echoes
that bounce off the tissues inside and around the eye. The echoes are converted by a
computer into an image on a computer screen. Ultrasound is one of the most common
imaging tests for confirming the diagnosis of retinoblastoma. It is painless and does
not expose the child to radiation, but the child may need to be sedated (made sleepy)
so that the doctor can get a good look at the eye. This test can be very useful when
tumors in the eye are so large they prevent doctors from seeing inside the whole eye
because ultrasound can see through tissues. Optical coherence tomography (OCT)
is a similar type of test that uses light waves instead of sound waves to create very
detailed images of the back of the eye.
Magnetic resonance imaging (MRI) scan
MRI scans are often used for retinoblastomas because they provide very
detailed images of the eye and surrounding structures without using radiation. This
test is especially good at looking at the brain and spinal cord. Most children with
retinoblastoma will have at least one MRI scan. For children with bilateral
retinoblastomas (tumors in both eyes), many doctor continue to do MRI scans of the
brain for several years after treatment to look for tumors of the pineal gland
(sometimes called trilateral retinoblastoma). Unlike CT scans (described next), MRI
scans use radio waves and strong magnets to create images instead of x-rays. A
contrast material called gadolinium may be injected into a vein before the scan to see
details better. MRI scans may take up to an hour. Your child may have to lie inside a
narrow tube, which is confining and can be upsetting. Newer, more open MRI
machines can help with this, but the test still requires staying still for long periods of
time. The machines also make buzzing and clicking noises that may be disturbing.
Young children may be given medicine to help keep them calm or even asleep during
the test.3
Computed tomography (CT) scan
The CT scan is an x-ray test that produces detailed cross-sectional images of
parts of the body. CT scans can help determine the size of a retinoblastoma tumor and
how much it has spread within the eye and to nearby areas. Normally, either a CT or
an MRI scan is needed to do this, but usually not both. Because CT scans give off
radiation, which might raise a childs risk for other cancers in the future, most doctors
prefer to use MRI. However, a CT scan can show deposits of calcium inthe tumor
much better than an MRI, which can be very helpful when the diagnosis of
retinoblastoma is not clear. Instead of taking one picture, like a regular x-ray, a CT
scanner takes many pictures as it rotates around your child while he or she lies on a
table. A computer then combines these pictures into images of slices of the part of the
body being studied. Before the scan, your child may receive an IV (intravenous)
injection of a contrast dye that helps better outline structures in the body. The dye may
cause some flushing (a feeling of warmth, especially in the face). Some people are
allergic and get hives. Rarely, more serious reactions like trouble breathing or low
blood pressure can occur. Be sure to tell the doctor if your child has any allergies or
has ever had a reaction to any contrast material used for xrays. CT scans take longer
than regular x-rays, but not as long as MRI scans. A CT scanner with a narrow table in
the middle opening. Your child will need to lie still on the table while the scan is
being done. During the test, the table slides in and out of the scanner. Your child may
need to be sedated before the test to stay still and help make sure the pictures come
out well.3
Bone scan
A bone scan can help show if the retinoblastoma has spread to the skull or other
bones. Mostchildren with retinoblastoma do not need to have a bone scan. It is
normally used only whenthere is a strong reason to think retinoblastoma may have
spread beyond the eye.For this test, a small amount of low-level radioactive material
is injected into a vein(intravenously, or IV). (The amount of radioactivity used is very
low and will pass out of thebody within a day or so.) The material settles in areas of
damaged bone throughout the skeleton over the course of a couple of hours. Your
child then lies on a table for about 30minutes while a special camera detects the
radioactivity and creates a picture of the skeleton.Younger children may be given
medicine to help keep them calm or even asleep during the test.This test shows the
entire skeleton at once. Areas of active bone changes appear as hot spots on the
skeleton that is, they attract the radioactivity. These areas may suggest the
presence of cancer, but other bone diseases can also cause the same pattern. To help
tell these apart, other tests such as plain x-rays or MRI scans of the bone might be
needed. For more detailed information on imaging tests, see our document.3
Other tests
Some other types of tests are not commonly needed for retinoblastomas, but they may
be helpful in some situations.
Biopsy
For most cancers, a biopsy (removing a tissue sample from the tumor and
looking at it under a microscope) is needed to make a diagnosis. Trying to biopsy a
tumor at the back of the eye can often damage the eye and may spread tumor cells, so
this is almost never done to diagnose retinoblastoma. Instead, doctors make the
diagnosis based on eye exams and on imaging tests such as those listed above. This is
why it is very important that the diagnosis of retinoblastoma is made by experts.
Lumbar puncture (spinal tap)
Retinoblastoma may grow along the optic nerve, which connects the eye to the
brain. If the cancer has spread to the surface of the brain, this test can often find
cancer cells in samples of cerebrospinal fluid (the fluid that surrounds the brain and
spinal cord). Most children with retinoblastoma do not need to have a lumbar
puncture. It is normally used only when there is a reason to think retinoblastoma may
have spread into the brain. For this test, the doctor first numbs an area in the lower
part of the back over the spine. The child is typically given anesthesia so they will
sleep and not move during the procedure. This can help ensure the spinal tap is done
cleanly. A small, hollow needle is then placed between the bones of the spine to
withdraw a small amount of the fluid. The fluid is then looked at under a microscope
to check for cancer cells.3
Bone marrow aspiration and biopsy
These 2 tests may be done to see if the cancer has spread to the bone marrow,
the soft, inner part of certain bones. These tests are usually not needed unless the
retinoblastoma has spread to tissues next to the eye and doctors suspect that the cancer
may have also spread through the bloodstream to the bone marrow. The tests are
typically done at the same time. The samples are usually taken from the back of the
pelvic (hip) bone, but in some cases they may be taken from other bones. In bone
marrow aspiration, the skin over the hip and the surface of the bone may be numbed
with a local anesthetic. This test can be painful, so the child will probably be given
other medicines to reduce pain or even be asleep during the procedure. A thin, hollow
needle is then inserted into the bone, and a syringe is used to suck out (aspirate) a
small amount of liquid bone marrow. A bone marrow biopsy is usually done just after
the aspiration. A small piece of bone and marrow is removed with a slightly larger
needle that is pushed down into the bone. Once the biopsy is done, pressure is applied
to the site to help stop any bleeding.
The samples are then looked at under a microscope to see if tumor cells are
present.3
Hearing test.
Children with retinoblastoma taking certain chemotherapy drugs may have
their hearing tested (audiology test). In a young child, a normal newborn hearing
screen can serve as a baseline.7
Differential diagnosis5
Other causes of leukocoria
Persistent hyperplastic primary vitreous
Coats disease
Cataract
Endophthalmitis from Toxocaracanis
Choroidal coloboma
Retinopathy of prematurity
Treatment
Management of a child with retinoblastoma requires a multidisciplinary
approach. Ophthalmologists, pediatric oncologists, pediatric radiation oncologists,
pathologists, genetic counselors, social workers, nurses, and others play important
roles in the cure of the disease, salvage of vision, and support of the child with vision
loss and potential long-term sequelae. Many therapeutic options are available, and the
indications for a specific modality or a combination of modalities vary with each
patient. Furthermore, management varies for children with intraocular disease and
extraocular spread of the tumor. Most patients with unilateral disease present with
advanced intraocular disease and therefore usually undergo enucleation, which results
in a cure rate >95%. Children with involvement of both eyes at diagnosis usually
require multimodality therapy (chemotherapy, local therapies). Failure to control
disease in children with bilateral disease may lead to external beam radiation (EBR)
therapy. Enucleation is usually reserved for eyes with recurrent disease and no useful
vision.4
Management of Intraocular Disease
Staging of the disease has facilitated the assessment of treatments and
measurement of outcomes in oncology. The Reese-Ellsworth (R-E) classification for
intraocular retinoblastoma, developed in the 1960s, was used during the last 40 years
in assessing outcomes of therapy, and this classification facilitated the comparison of
10
results from various studies. The R-E classification was devised to predict prognosis
in eyes that were treated with EBR therapy. The classification scheme has five groups.
Eyes with disease consistent with the lower groups have a lower risk for enucleation
following EBR and group V eyes have the highest risk for enucleation. With the
advent of other therapies, including chemotherapy, which has increasingly replaced
EBR therapy in the treatment of intraocular disease, the usefulness of the R-E scheme
is less apparent. Several alternative schemes have been proposed recently by Shields
et al. and by Murphreeamong others. The classification proposed by Murphree is the
basis for several protocols for the treatment of intraocular retinoblastoma within the
Children's Oncology Group (COG). While the R-E classification and the classification
proposed by Murphree and others address intraocular disease, another classification
system has been proposed by Chantada et al to address extraocular disease and
microscopic disease following enucleation.4
Enucleation
Most children with unilateral retinoblastoma present with advanced disease, and
most of them require enucleation. Other indications for enucleation are for children
with bilateral disease where enucleation may be indicated for the eye with the most
advanced disease that does not respond to chemotherapy (rarely, enucleation is
indicated for both eyes), for the eye that has failed all known effective therapies, when
active tumor is present in an eye with no vision, when glaucoma is present as a result
of neovascularization of the iris or tumor invasion into the anterior chamber, and
when direct visualization of an active tumor is obstructed by conditions including
hemorrhage, corneal opacity, or cataract. Enucleation is curative in >95% of patients
with unilateral disease. Care should be taken to avoid perforation of the globe during
surgery and to obtain a long segment of the optic nerve in order to minimize the
chance of leaving tumor at the surgical margin. Orbital implants made of silicone,
plastic, hydroxyapatite, and MedPore are used at major treatment centers. By
connecting the implants to the orbital muscles, excellent cosmetic appearance can be
achieved. Complications such as wound dehiscence and conjunctival erosion,
although rare, may be seen with all types of implants.4
EBR Therapy
11
EBR therapy is an effective means of curing retinoblastoma. The most common
indication for EBR is for the eye in a young child with bilateral retinoblastoma who
has active or recurrent disease after completion of chemotherapy and local therapies.
Children with small tumors within the macula that do not respond to chemotherapy or
have recurrent disease following chemotherapy can benefit from EBR. With EBR
therapy, the entire tumor-bearing area of the globe is included along with at least 1 cm
of the optic nerve. The prescribed dose to the tumor ranges from 42 Gy to 46 Gy, with
the radiosensitive lens receiving significantly less. Preservation of the eye with
control of the disease using EBR therapy is in the range of 58%88%. Radiation
therapy has only a 50% local control rate in R-E groups IV and V disease, with a 95%
rate of preservation of the eye in R-E groups IIII. In a report of 63 R-E group Vb
eyes (tumors with vitreous seeds) that were irradiated at initial diagnosis, the ocular
survival rate was 53.4% at 10 years. However, the probability of developing a second
cancer following initial EBR therapy for group Vb disease in patients with bilateral
disease was 29.7% by 10 years after diagnosis.
Patients with hereditary disease who received EBR therapy are reported to have
a cumulative incidence of second cancers of 35%, compared with 6% for those who
did not receive EBR. Furthermore, patients who are <1 year of age and who receive
radiation therapy are several times more likely to develop second and subsequent
malignancies than those who are >12 months of age and receive radiation therapy. In
a cohort of patients with hereditary retinoblastoma, a strong relationship between
radiation dose and the development of soft tissue sarcomas was reported.
In subsequent follow-up of this cohort, significantly higher risks for melanoma,
cancers of the bone, nasal cavities, and brain, and soft tissue sarcomas (with an excess
of leiomyosarcoma) were documented. Cataracts, optic nerve damage, total retinal
vascular occlusion, vitreous hemorrhage, and facial and temporal bone hypoplasia are
other complications associated with EBR therapy. Proton beam radiation therapy
offers promise in reducing the significant long-term side effects associated with
conventional EBR therapy.4
Brachytherapy
12
Brachytherapy involves the placement of a radioactive implant (plaque), usually
on the sclera adjacent to the base of a tumor. Iodine-125 ( 125I), gold, and more recently
ruthenium have been used. The intention is to deliver a dose of 4,0004,500
cGytransclerally to the apex of the tumor over a period of 24 days. This treatment is
limited to tumors that are <16 mm in base and 8 mm in thickness, and can be used as
the primary treatment or, more frequently, in patients who had failed initial therapy
including previous EBR therapy. This modality can also be used when there is a
peripheral tumor with focal vitreous seeding around it. Relative contraindications
include larger tumors and those that involve the macula. Good tumor control has been
reported with this modalit. Side effects are less common than with EBR and include
optic neuropathy, radiation retinopathy, and cataract formation. Second malignancies
do not appear to be associated with this type of local therapy. An orbital implant
with 125I seeds was shown to be effective in treating patients who were at high risk for
orbital recurrence after enucleation.
Thermotherapy
Thermotherapy involves the application of heat directly to the tumor, usually in
the form of infrared radiation. A temperature between 45C and 60C is the goal of
this therapeutic approach and is below the coagulative threshold and therefore spares
the retinal vessels from coagulation. Thermotherapy alone can be used for small
retinoblastomas that are 3 mm in diameter without vitreous or subretinal seeds. In a
study of 91 tumors, 92% of the tumors that were <1.5 mm in diameter were controlled
with thermotherapy alone.4
Chemothermotherapy
Larger tumors or tumors with subretinal seeds are usually treated with a
combination of thermotherapy and chemotherapy. Tractional and vaso-occlusive
complications that can be seen with thermotherapy alone appear to be less frequent
when
thermotherapy
is
used
in
combination
with
chemotherapy
(chemothermotherapy). Chemotherapy and thermotherapy are delivered within hours
of each other. In one study of 188 retinoblastomas, tumor control was achieved in
86% of cases. The complications of chemothermotherapy included focal iris atrophy,
paraxial lens opacity, sector optic disk atrophy, retinal traction, optic disk edema,
13
retinal
vascular
occlusion,
retinal
detachment,
and
corneal
edema.
Chemothermotherapy may be especially useful for patients with small tumors
adjacent to the fovea and optic nerve, where radiation therapy or laser
photocoagulation may result in significant visual loss.4
Laser Photocoagulation
Laser photocoagulation is recommended only for small posterior tumors. The
treatment is delivered with an argon or diode laser or a xenon arc. The purpose of this
treatment is to coagulate all the blood supply to the tumor. Indirect ophthalmoscope
laser photocoagulation has significantly improved the delivery of photocoagulation.
Effective therapy usually requires 23 sessions at monthly intervals. Complications of
this treatment include retinal detachment, retinal vascular occlusion, retinal traction,
and preretinal fibrosis.
Cryotherapy
Cryotherapy induces tumor tissue to freeze rapidly, resulting in damage to the
vascular endothelium with secondary thrombosis and infarction of the tumor tissue.
Cryotherapy may be used as primary therapy for small peripheral tumors or for small
recurrent tumors previously treated with other modalities. Tumors are typically treated
three times per session, with one or two sessions at monthly intervals. Ninety percent
of tumors<3 mm in diameter are cured permanently, and complications are few and
rarely serious .Transient conjunctival edema and transient localized serous retinal
detachments can occur. Vitreous hemorrhage can be observed in large or previously
irradiated tumors.
Chemotherapy
Chemotherapy has been used to treat intraocular retinoblastoma since the early
1990s. Chemotherapy is used to reduce the size of the tumor to allow local
ophthalmological therapies, including cryotherapy and laser photocoagulation, or
thermotherapy, to eradicate the remaining disease. This combination of therapies has
been promoted to avoid EBR therapy and/or enucleation and thereby decrease the
potential for long-term side effects while salvaging some useful vision. The common
indications for chemotherapy for intraocular retinoblastoma include tumors that are
14
large and that cannot be treated with local therapies alone in children with bilateral
tumors. Chemotherapy can also be used in patients with unilateral disease when the
tumors are small but cannot be controlled with local therapies alone. Such patients
constitute only 10%15% of all patients with unilateral disease. Most patients with
unilateral disease are diagnosed with advanced intraocular disease and undergo
enucleation. Numerous studies have been published that show that chemotherapy is
very effective in eliminating the need for EBR/enucleation in R-E group IIII eyes,
while proving to be significantly less successful in eyes with group IV or V disease .
Selected patients with group IV disease have also had a very good response to
chemotherapy, and EBR and enucleation were avoided. The chemotherapy regimen
commonly used consists of carboplatin, vincristine, and etoposide. Cyclosporine has
been used in addition to these three agents in some institutions in order to try to
overcome drug resistance. Others have used carboplatin and vincristine without
etoposide and older studies used cyclophosphamide and doxorubicin. The
chemotherapy regimens from the different groups of investigators vary in the number
and frequency of chemotherapy cycles. All these regimens are well tolerated, with the
expected side effects of myelosuppression and its consequences, which include
invasive bacterial infections. Ototoxicity and renal toxicities are rare. There is also the
potential risk for second malignancies, especially when using etoposide (an
epipodophyllotoxin). The RE groups IIII and part of group IV correspond to group
B disease of the new international classification scheme that is a modification of the
one proposed by Murphree. Patients who have group B disease will be treated with
carboplatin and vincristine in the proposed COG trial, and their event-free survival
(EFS) at 2 years will be estimated, where an event is described as the need for
nonprotocol chemotherapy or EBR/enucleation.
Chemotherapy alone is not very effective in avoiding EBR/enucleation in
patients with R-E group V eyes, especially those with vitreous seeds. Friedman
etal.showed that only 53% of 30 group V (C, D, or E in the proposed classification)
eyes could be controlled with chemotherapy alone. Data from Chan et al. and
Villablanca et al. suggested that approximately 40% of group C and 70% of group D
eyes failed systemic chemotherapy alone. Based on these data, the trial proposed by
the COG involves systemic chemotherapy with carboplatin, vincristine, and etoposide
along with subtenon carboplatin for group C and D eyes .. Eyes with diffuse vitreous
15
seeding present a particularly difficult management problem and, as mentioned above,
rarely respond to chemotherapy alone. Although EBR therapy is modestly successful
in patients with vitreous seeds, new approaches are needed. A recent phase I study
using adenoviral vectors to deliver the herpes simplex thymidine kinase gene
followed by ganciclovir demonstrated durable clinical and histopathologic responses
in heavily pretreated patients with vitreous seeds .4
Management of Extraocular Disease
Patients with extraocular disease have a very poor prognosis with respect to
survival. Recently, there have been encouraging data to suggest that patients with
regional extraocular disease may benefit from a combination of conventional
chemotherapy and EBR and those with distant metastatic disease may benefit from
high-dose chemotherapy and EBR in conjunction with bone marrow stem cell
transplantation. Regional extraocular disease includes patients with orbital,
preauricular disease and patients with tumor found at the optic nerve surgical margin.
Chantada et al. reported a 5-year EFS rate of 84% in 15 patients with orbital or
preauricular disease treated with chemotherapy that included vincristine, doxorubicin,
and cyclophosphamide or vincristine, idarubicin, cyclophosphamide, carboplatin, and
etoposide. These patients also received EBR of 4,500 cGy administered to the optic
nerve chiasm for patients with orbital disease and to the involved nodes for those with
preauricular lymphadenopathy. A subsequent study showed that 12 patients with
positive optic nerve surgical margins were all event-free survivors following
chemotherapy as above and orbital radiation therapy of 4,0004,500 cGy. A similar
successful study was reported from Brazil.
Patients with metastatic extraocular disease have a poor prognosis when treated
with regimens of conventional doses of chemotherapy. There are several reports now
suggesting that high-dose chemotherapy with stem cell rescue combined with EBR
for areas of bulky disease at diagnosis is beneficial, with some long-term survivors
among patients with metastatic disease not involving the central nervous system
(CNS). It is rare for a patient with metastatic CNS involvement to survive using the
therapies described above. The proposed trial by the COG for patients with metastatic
16
disease involves conventional chemotherapy, stem cell harvest, high-dose
chemotherapy with stem cell rescue, and EBR of involved sites.4
PROGNOSIS
Approximately 95% of children with retinoblastoma are cured with modern
treatment in the USA. Current efforts using chemotherapy in combination with focal
therapy are intended to preserve useful vision and avoid external-beam radiation or
enucleation. Routine ophthalmologic examinations should continue until children are
over age 7 yr. Unfortunately the diagnosis of retinoblastoma in many children from
third-world countries is delayed, resulting in spread of the tumor outside of the orbit.
The prognosis for these children with retinoblastoma that has spread outside of the
eye is poor. Children with germ line RB1 mutations are at significant risk for
development of second malignancies, especially osteosarcoma and also soft tissue
sarcomas and malignant melanoma. The risk of second malignancies is further
increased by the use of radiation therapy. Other radiation-related late adverse effects
include cataracts, orbital growth deformities, lacrimal dysfunction, and late
retinal vascular injury.1
17
The aim of this paper is to report a case of retinoblastoma
CASE REPORT
Name
: MN
Age
: 3 years 11 months old
Sex
: Male
Date of Admission
: 02nd February 2015
Main Complaint
: Eye looks like a cat eye
History:
This main complaint is experienced by patients in 8 months ago, and had
brought to treatment within 4 months ago to the regional hospital of Banda Aceh.
History of red eye (+) experienced by patients within 5 months ago. Headache (+)
patients experienced since 1 month ago. at this point the patient is not in a state of
fever.
History of previous illness: Patients had previously been treated in regional hospitals
of Banda Aceh and was examined orbital CT scan with contrast, with the results of the
mass in the Vitreous Dextra with calcification.
History of drugs
: Nothing
Pregnant History
1st child in the family. Mother was 27 years old during pregnancy. There is no history
of fever, hypertension, diabetic mellitus, and herbal medicine consumption.
Birth History
Spontaneous; attended by nurses; BW 2100 gram; cyanotic (-). Abnormality at birth:
(-)
18
Immunization History
Till date all type of immunization completed
(BCG, Polio, Measles, Hep B, DPT)
Feeding History
From birth till 9th Months Old: Breast milk + formula milk
History of Growth and Development
-NILPhysical Examination
Generalized status
Body weight: 14 Kg, Body length: 94 cm
BW/age: z = < 0
BL/age : z = -2
BW/BL: z = 0
Interpretation : normal nutrition
Praesens status
Level of Consciousness: Compos Mentis, Blood pressure 110/60 mmHg, HR: 90
bpm, RR: 26 bpm, body temperature: 37 oC, body weight : 14 Kg, body length : 94
cm.
Anemic (-), Icteric (-), Cyanosis (-), Edema (-), Dyspnea (-).
Localized status
Head :
Eye: Right eye : light reflex (-), ciliary injection (+), conjuctiva injection (+), white
formation covering lower part of cornea.
Left eye : Light Reflex (+), Pupil 3mm
Conjuctiva palpebra inferior anaemic (-/-), sclera icteric (-/-).
Nose and ear: normal
Mouth: normal
19
Neck :
Lymph node enlargement (-).
Thorax:
Symmetrical fusiformis, Chest retraction(-), HR : 90 bpm, regular, murmur (-),
RR: 26 x/i, regular, ronkhi (-/-)
Abdomen:
Soepel, normoperistaltic. Liver, spleen and renal were unpalpable.
Extremities:
Pulse 90 bpm, regular, adequate pressure and volume, warm acral, Capillary Refill
Time < 3.
Urogenital:
Male, normal
Laboratory Findings on HAM Hospital ( 2nd February 2015), outgoing patient:
Table 1
Parameters
Complete Blood Count
Hemoglobin
Leucocyte
Trombocyte
Hematocrite
Eritrocyte
MCV
MCH
MCHC
RDW
PDW
MPV
Value
Normal Value
11,3 g %
9,36 x103 /mm3
425.000 /uL
33.7 %
4.48 mil/mm3
79.70 fl
26.70 pg
33,5 g/dl
12.70 %
9.2 fl
8.70 fl
13 18
4.000 11.000
150.000 450.000
39 54
4.50 6.50
82-100
24 30
28 32
14.9 18.7
10 18
7.2 10.0
Leucocytes Count :
Neutrophil
36.40
37 80
Lymphocyte
46.80
20 40
20
Monocyte
8.10
2-8
Eosinophil
6.50
16
Basophil
0.200
01
Neutrophil absolute
103/L
3.59
1.9-5.4
Lymphocyte absolute
103/L
4.36
3.7 10.7
Monocyte absolute
103/L
0.76
0.3 0.8
Eosinophil absolute
103/L
0.61
0.20 0.50
Basophil absolute
103/L
0.02
0 0.1
Table 2
Result
Normal
Liver
Bilirubin Total
0.28 mg/dL
<1
Bilirubin Direk
0,08 mg/dL
0-0.02
Fosatase alkali (ALP) 309U/L
<449
AST/SGOT
24U/L
<38
ALT/SGPT
13U/L
<41
Ureum
20.9 mg/dL
<50
Kreatinin
0.50 mg/dL
0.17-0.42
AsamUrat
4.7 mg/dL
<7,0
Renal
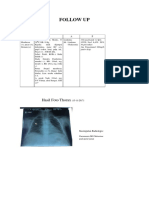
AP Chest Xray (02nd february 2015)
21
Cor tidak membesar
Sinuseas dan diafragma normal
Hilus normal
Corakan bronkovaskular normal
Tidak tampak bercak lunak
Result: Tidak tampak kardio megali, tidak tampak TB paru aktif
22
CT scan (18th October 2014)
Differential Diagnosis:
23
Working Diagnosis:
Retinoblastoma OD
Management:
Bed Rest
Diagnostic Planning:
Bone Marrow Puncture
Follow Up
02nd February 2015
S Red Eye (+), head pain (+)
O Sens: Compos Mentis, . Icteric (-). Edema (-). Cyanosis (-) Dyspnoe (-). Body Temperature :
370C . Body weight: 14 kg, Body length: 94 cm.
Head
Eye: Right eye : light reflex (-), ciliary injection (+), conjuctiva injection (+),
white formation covering lower part of cornea.
Left eye : Light Reflex (+), Pupil 3mm
Nose, Ear: normal
Neck
Thorax
Mouth: normal
Lymph node enlargement (-).
Symmetrical fusiformis, Chest retraction (-), HR : 96 bpm, regular, murmur (-),
RR: 24 bpm , regular, ronkhi (-/-).
Abdomen
Soepel. Normoperistaltic. Liver, spleen and renal unpalpable.
Extremities Blood pressure: 100/70 mmHg, Pulse 96 bpm, regular, adequate pressure and
volume, warm acral, Capillary Refill Time < 3,
Genital
male, within normal limit
A Retinoblastoma OD
P - Bed Rest
- Waiting for Laboratory Issue
Planning: Bone Marrow Puncture
3rd February 2015
S Red Eye (+), head pain (+)
O Sens: Compos Mentis, . Icteric (-). Edema (-). Cyanosis (-) Dyspnoe (-). Body Temperature :
370C . Body weight: 14 kg, Body length: 94 cm.
Head
Eye: Right eye : light reflex (-), ciliary injection (+), conjuctiva injection (+),
white formation covering lower part of cornea.
24
Left eye : Light Reflex (+), Pupil 3mm
Nose, Ear: normal
Neck
Thorax
Mouth: normal
Lymph node enlargement (-).
Symmetrical fusiformis, Chest retraction(-), HR : 92 bpm, regular, murmur (-),
RR: 22 bpm , regular, ronkhi (-/-).
Abdomen
Soepel. Normoperistaltic. Liver, spleen and renal unpalpable.
Extremities Blood pressure: 100/60 mmHg, Pulse 92 bpm, regular, adequate pressure and
volume, warm acral, Capillary Refill Time < 3,
Genital
male, within normal limit
A Retinoblastoma OD
P - Bed Rest
Planning:
- Take out the last laboratory issue (2/2/2015)
- Bone Marrow Puncture
4 February 2015
S Right Eye looks like cat eye, fever (-)
O Sens: Compos Mentis, . Icteric (-). Edema (-). Cyanosis (-) Dyspnoe (-). Body Temperature :
th
36,7o C . Body weight: 14 kg, Body length: 94 cm.
Head
Eye: Right eye : light reflex (-), ciliary injection (+), conjuctiva injection (+),
white formation covering lower part of cornea.
Left eye : Light Reflex (+), Pupil 3mm, conjunctiva palpebra Inferior pale (-)
Nose, Ear: normal
Neck
Thorax
Mouth: normal
Lymph node enlargement (-).
Symmetrical fusiformis, Chest retraction (-), HR : 96 bpm, regular, murmur (-),
RR: 24 bpm , regular, ronkhi (-/-).
Abdomen
Soepel. Normoperistaltic. Liver, spleen and renal unpalpable.
Extremities Blood pressure: 110/70 mmHg, Pulse 96 bpm, regular, adequate pressure and
volume, warm acral, Capillary Refill Time < 3,
Genital
male, within normal limit
A Retinoblastoma OD
P - Bed Rest
- Bone Marrow Puncture
- Waiting for Bone Marrow Puncture Result
- Plan for Chemotherapy
25
Discussions
Theory
The median age of this diagnosis is
Case
approximately 2 yr, and over 90% of
cases are diagnosed in the children under
the age of 5. Overall about 2 thirds to 3
quarters of children with retinoblastoma Patient is 3 years 11 months old, with
have
unilateral
tumors,
with
the unilateral retinoblastoma.
remainder have bilateral retinoblastoma.
Bilateral retinoblastoma is more common
in younger children, particularly in those
diagnosed under the age of 1 yr.
26
Retinoblastoma clasically presents with
leukocoria, a white pupillary reflex, white
often is first noticed when a red reflex is
not present at a routine newborn or well
child examination or in a flash phtograph
of the child. Strabismus often is the initial Patient had leukocoria ,
presenting
complaint.
inflammation,
hyphema,
Orbital Orbital inflamation (+)
and
pupil
irregularity can occur with advancing
disease. Pain can occur if secondary
glaucoma is present. Only about 10% of
retinoblastoma cases are detected by
routine ophthalmologic screening in the
context of of a positive family history.
Imaging
Ultrasonography, CT Scan, MRI, bone Ct scan had been done and shows
scan, lumbar puncture, biopsy, bone calcification on oculi dextra resulting
marrow aspiration and biopsy
Treatment
retinoblastoma
Management of intraocular disease
Enucleation
EBR therapy
brachytheraphy
chemotheraphy
thermal therapy
chemothermotheraphy
Chemotheraphy has been the therapy for
this patient
27
28
Conclusions
The conclusion of this paper is a boy, 3 year 11 months old, diagnosed with
Retinoblastoma OD, which is confirmed by the results of CT scan with contrast.
The patient received :
-
Bed Rest
Bone Marrow Puncture
Plan for Chemotherapy
29
References
1. Zage E. Peter and Herzog E. Cynthia, Retinoblastoma in Kliegman RM, Behrman
RE, Stanton BF, Schor NF, Geme III JWS, 2011. NelsonTextbook of Pediatrics,
19th Edition, Saunders Elsevier Inc, 1768-1769.
2. Hurwitz RL, Shields CL, Shields JA, et al. Retinoblastoma. In: Pizzo PA, Poplack
DG, eds. Principles and Practice of Pediatric Oncology. 6th ed. Philadelphia, Pa:
Lippincott Williams & Wilkins; 2011: 809837.
3. A Guide for parents for Retinoblastoma at St. Jude Children Research Hospital:
http://www.stjude.org/SJFile/a4522_what_is_retinoblastoma.pdf.
4. Murali C, Patricia C B, Evelyn A P, Sharon E P and Richard H; Retinoblastoma:
Review of Current Management: Society of translational Oncology, AlphaMed
press; http://theoncologist.alphamedpress.org/content/12/10/1237.full
5. Stephen V.L, Ben L, Retinoblastoma in Nepal: case report and review: Bujo Case
Reports,Vol II; 2014.
6. Staging
of
Retoinoblastoma;
National
Cancer
Institute;
http://www.cancer.gov/cancertopics/pdq/treatment/retinoblastoma/patient/page2
updated on 6th November 2014.
7. Ann-M L, MD, Kim E., MD, Kristin; Retinoblastoma, The Childrens Hospital of
Philadelphia: 2014.
Das könnte Ihnen auch gefallen
- RetinoblastomaDokument24 SeitenRetinoblastomaMiguel Carlos Navarro Tacderan100% (1)
- Problem-based Approach to Gastroenterology and HepatologyVon EverandProblem-based Approach to Gastroenterology and HepatologyJohn N. PlevrisNoch keine Bewertungen
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsVon EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsNoch keine Bewertungen
- Hemoblastosis in ChildrenDokument40 SeitenHemoblastosis in ChildrenAli Baker Algelane100% (3)
- Von Willebrand DiseaseDokument9 SeitenVon Willebrand DiseaserandyNoch keine Bewertungen
- Management of Tuberculosis: A guide for clinicians (eBook edition)Von EverandManagement of Tuberculosis: A guide for clinicians (eBook edition)Noch keine Bewertungen
- Chapter 14 - HematopathologyDokument66 SeitenChapter 14 - Hematopathologynigel farageNoch keine Bewertungen
- Congenital RubellaDokument15 SeitenCongenital RubellaShanaz AlvikhaNoch keine Bewertungen
- Neonatal Jaundice JCG0013 v3.1Dokument11 SeitenNeonatal Jaundice JCG0013 v3.1Alejandro Motolinía100% (1)
- The Abnormal PuerperiumDokument25 SeitenThe Abnormal PuerperiumMartijn JohanNoch keine Bewertungen
- Megaloblastic AnemiaDokument13 SeitenMegaloblastic AnemiaRoushanNoch keine Bewertungen
- Pyeloplasty (Anderson-Hynes)Dokument12 SeitenPyeloplasty (Anderson-Hynes)HardiTariqHammaNoch keine Bewertungen
- Chronic Suppurative Otitis MediaDokument6 SeitenChronic Suppurative Otitis MediaSuhas IngaleNoch keine Bewertungen
- The Bleeding Child OSCE HaemophiliaDokument3 SeitenThe Bleeding Child OSCE HaemophiliaJJ LimNoch keine Bewertungen
- New Guidelines For The Diagnosis of Paediatric Coeliac DiseaseDokument3 SeitenNew Guidelines For The Diagnosis of Paediatric Coeliac DiseaseDiana NicaNoch keine Bewertungen
- Molar Pregnancy: Capitol Medical Center CollegesDokument38 SeitenMolar Pregnancy: Capitol Medical Center CollegesDarlene Laude GoyaNoch keine Bewertungen
- DIC Case StudyDokument7 SeitenDIC Case StudyRobertNoch keine Bewertungen
- Gyne Case COCDokument37 SeitenGyne Case COCLian BaylosisNoch keine Bewertungen
- Chronic Otitis MediaDokument4 SeitenChronic Otitis MediaOvyanda Eka MItraNoch keine Bewertungen
- Scifed: PublishersDokument6 SeitenScifed: PublishersNadiarosmaliaNoch keine Bewertungen
- Trichiasis: Prepared By:pooja Adhikari Roll No.: 27 SMTCDokument27 SeitenTrichiasis: Prepared By:pooja Adhikari Roll No.: 27 SMTCsushma shresthaNoch keine Bewertungen
- Gyne LE 2: Stage IVA Is Characterized byDokument49 SeitenGyne LE 2: Stage IVA Is Characterized byĐinesh IlavarasanNoch keine Bewertungen
- MRCPCH Part Ii: Safdar Iqbal'sDokument5 SeitenMRCPCH Part Ii: Safdar Iqbal'sGalaleldin AliNoch keine Bewertungen
- AdenoidsDokument6 SeitenAdenoidsIfeanyichukwu OgbonnayaNoch keine Bewertungen
- Preterm Prelabour Rupture of MembranesDokument12 SeitenPreterm Prelabour Rupture of MembranesSeptiany Indahsari DjanNoch keine Bewertungen
- Hyperemesis GravidarumDokument5 SeitenHyperemesis GravidarumsalamredNoch keine Bewertungen
- Approach To FeverDokument80 SeitenApproach To FeverRaditia AbrahamNoch keine Bewertungen
- Session13 - Endometrial CaDokument27 SeitenSession13 - Endometrial CaCHALIE MEQUNoch keine Bewertungen
- Triple TestDokument2 SeitenTriple TestEva.lineNoch keine Bewertungen
- Child With HematuriaDokument42 SeitenChild With HematuriaalaaNoch keine Bewertungen
- Ultrasonography AssignmentDokument5 SeitenUltrasonography AssignmentAkshay VasishtaNoch keine Bewertungen
- Brain Abscess in Pediatric AgeDokument12 SeitenBrain Abscess in Pediatric AgeKatrina San GilNoch keine Bewertungen
- Diagnosis of MalariaDokument15 SeitenDiagnosis of MalariaSuranjan Pal100% (1)
- Acute Lymphoid LeukemiaDokument41 SeitenAcute Lymphoid Leukemiaummi ulfahNoch keine Bewertungen
- CholangitisDokument15 SeitenCholangitisFaye TanNoch keine Bewertungen
- Biopsy in Surgery RereDokument41 SeitenBiopsy in Surgery RereRererloluwa100% (1)
- BotulismDokument6 SeitenBotulismMarsiano QendroNoch keine Bewertungen
- Acute GlomerulonephritisDokument28 SeitenAcute GlomerulonephritisPaul SinsNoch keine Bewertungen
- Introduction To HematologyDokument61 SeitenIntroduction To HematologyThis is PonyNoch keine Bewertungen
- Interatitial Lung DiseaseDokument2 SeitenInteratitial Lung DiseaseIsabel CastilloNoch keine Bewertungen
- Manchester Anaemia GuideDokument13 SeitenManchester Anaemia Guidemubzy14Noch keine Bewertungen
- Discharge Summary PDFDokument2 SeitenDischarge Summary PDFbalab2311Noch keine Bewertungen
- Leukaemia: Definition: Leukemia Is A Malignant Disease of The Hematopoietic System (Blood Forming Cells)Dokument16 SeitenLeukaemia: Definition: Leukemia Is A Malignant Disease of The Hematopoietic System (Blood Forming Cells)Arnab Ghosh100% (1)
- The Complete Blood Count Is The Calculation of The Cellular (Formed Elements) of BloodDokument26 SeitenThe Complete Blood Count Is The Calculation of The Cellular (Formed Elements) of BloodNabard MhammadNoch keine Bewertungen
- Obs. InvestigationsDokument36 SeitenObs. InvestigationsSameena Rose AjmeriNoch keine Bewertungen
- Newborn NotesDokument44 SeitenNewborn NotesHaziq KamardinNoch keine Bewertungen
- Tuberculosis: Dr.V. Gangadharan Professor & Hod Department of Respiratory Medicine Saveetha Medical College HospitalDokument58 SeitenTuberculosis: Dr.V. Gangadharan Professor & Hod Department of Respiratory Medicine Saveetha Medical College HospitalJoanna RachelNoch keine Bewertungen
- Breast Cancer: Dr. Armando V. Tan AnatomyDokument9 SeitenBreast Cancer: Dr. Armando V. Tan AnatomyJennifer Dumaluan AtaNoch keine Bewertungen
- Hiv in Pregnancy FinalDokument73 SeitenHiv in Pregnancy Finalapi-3797079Noch keine Bewertungen
- A Case Study of Epidural HematomaDokument27 SeitenA Case Study of Epidural HematomaNeil GoNoch keine Bewertungen
- Clinical Features of Renal DiseaseDokument80 SeitenClinical Features of Renal DiseaseIdiAmadouNoch keine Bewertungen
- Chronic Suppurative Otitis MediaDokument16 SeitenChronic Suppurative Otitis MediaEmil P. MuhammadNoch keine Bewertungen
- RH IsoimmunizationDokument47 SeitenRH IsoimmunizationDuncan JacksonNoch keine Bewertungen
- LeprosyDokument26 SeitenLeprosyFamous manNoch keine Bewertungen
- Tropical Splenomegaly SyndromeDokument12 SeitenTropical Splenomegaly SyndromeSaidAandySaida100% (1)
- Nursing Pediatric Case StudyDokument9 SeitenNursing Pediatric Case StudyKJay Solijon100% (1)
- Case Presentation - Thanatophoric DysplasiaDokument20 SeitenCase Presentation - Thanatophoric Dysplasiaapi-390240132Noch keine Bewertungen
- The Effects of Music Therapy On Pain in Patients With Neuropathic PainDokument1 SeiteThe Effects of Music Therapy On Pain in Patients With Neuropathic PainMasykur Ramadhan GaniNoch keine Bewertungen
- Coffee Dictionary A-DDokument24 SeitenCoffee Dictionary A-DMasykur Ramadhan GaniNoch keine Bewertungen
- Follow UpDokument15 SeitenFollow UpMasykur Ramadhan GaniNoch keine Bewertungen
- Ghayat Al Hakim Book 1 PDFDokument94 SeitenGhayat Al Hakim Book 1 PDFMasykur Ramadhan GaniNoch keine Bewertungen
- ALS Drug SummaryDokument1 SeiteALS Drug SummaryPramod SharmaNoch keine Bewertungen
- Ascaris LumbricoidesDokument1 SeiteAscaris LumbricoidesMasykur Ramadhan GaniNoch keine Bewertungen
- PRESENTASI Retinoblastoma MaskurDokument39 SeitenPRESENTASI Retinoblastoma MaskurMasykur Ramadhan Gani100% (1)
- Retinoblastoma Case Report Latest With ReferenceDokument29 SeitenRetinoblastoma Case Report Latest With ReferenceMasykur Ramadhan GaniNoch keine Bewertungen
- Retinoblastoma Case Report Latest With ReferenceDokument29 SeitenRetinoblastoma Case Report Latest With ReferenceMasykur Ramadhan GaniNoch keine Bewertungen
- HPV Lung CancerDokument7 SeitenHPV Lung CancerAlina LazarNoch keine Bewertungen
- Vaksin HPVDokument14 SeitenVaksin HPVsutianiNoch keine Bewertungen
- List of Cervical Cancer Screening Centres in GhanaDokument15 SeitenList of Cervical Cancer Screening Centres in Ghanamyjoyonline.comNoch keine Bewertungen
- Skin Pathology: DR Shehu Abdullahi 19/01/2023Dokument23 SeitenSkin Pathology: DR Shehu Abdullahi 19/01/2023Mohammed HussainNoch keine Bewertungen
- დნმ-ის დაზიანების მექანიზმები კანცეროგენეზისა და კიბოს მკურნალობის დროსDokument1 Seiteდნმ-ის დაზიანების მექანიზმები კანცეროგენეზისა და კიბოს მკურნალობის დროსEMD GROUPNoch keine Bewertungen
- SGH Cervical Screening Colposcopy PathwaysDokument13 SeitenSGH Cervical Screening Colposcopy PathwaysAbraham ChiuNoch keine Bewertungen
- Ijms 20 01358Dokument24 SeitenIjms 20 01358CHETAN SOMUNoch keine Bewertungen
- High Dimensional Single Cell AnalysisDokument219 SeitenHigh Dimensional Single Cell AnalysisAndrew100% (1)
- Test Bank For The Biology of Cancer Second EditionDokument7 SeitenTest Bank For The Biology of Cancer Second EditionDale Passe100% (26)
- Ich Q5DDokument13 SeitenIch Q5DRatnam PrasadNoch keine Bewertungen
- MRCP NotesDokument33 SeitenMRCP NotesHemant DanielNoch keine Bewertungen
- Cancerul Si NeoplaziaDokument28 SeitenCancerul Si NeoplaziaBogdan SoltuzuNoch keine Bewertungen
- The Biology of CancerDokument21 SeitenThe Biology of CancerSarthak70% (47)
- Human Health and DiseasesDokument24 SeitenHuman Health and DiseasesAnujith AnuNoch keine Bewertungen
- TMP 610 CDokument6 SeitenTMP 610 CFrontiersNoch keine Bewertungen
- 4-Hyperplasia Part 2-1Dokument48 Seiten4-Hyperplasia Part 2-1Ali GamalNoch keine Bewertungen
- Cancer Karp 16Dokument5 SeitenCancer Karp 16Claudia Perez MestreNoch keine Bewertungen
- 11 PathologyDokument26 Seiten11 PathologyRocky BullNoch keine Bewertungen
- Adenoviruses - Medical Microbiology - NCBI Bookshelf PDFDokument9 SeitenAdenoviruses - Medical Microbiology - NCBI Bookshelf PDFNino MwansahNoch keine Bewertungen
- Felix Dietlein DissertationDokument6 SeitenFelix Dietlein DissertationBuySchoolPapersOnlineSingapore100% (1)
- Distant Metastases of Nasopharyngeal Carcinoma: Literature ReadingDokument33 SeitenDistant Metastases of Nasopharyngeal Carcinoma: Literature ReadingTeuku Muhammad Rizqi FadhlillahNoch keine Bewertungen
- Mouse Models For Gastric Cancer Matching Models ToDokument16 SeitenMouse Models For Gastric Cancer Matching Models ToUtami DewiNoch keine Bewertungen
- Hematology Topics 16-20Dokument20 SeitenHematology Topics 16-20Angelo Jude CobachaNoch keine Bewertungen
- Principles of Toxicology Third Edition 9781466503427 1466503424 - CompressDokument434 SeitenPrinciples of Toxicology Third Edition 9781466503427 1466503424 - CompressChristopher William LeeNoch keine Bewertungen
- Oncogene EtcDokument48 SeitenOncogene EtcInsyirah JohariNoch keine Bewertungen
- Basic Radiobiology (Slides) PDFDokument44 SeitenBasic Radiobiology (Slides) PDFSuhey07100% (2)
- Acquisition of A Hybrid E M State Is Essential For Tumorigenicity of Basal Breast Cancer CellsDokument12 SeitenAcquisition of A Hybrid E M State Is Essential For Tumorigenicity of Basal Breast Cancer CellsgangligonNoch keine Bewertungen
- NeoplasmDokument31 SeitenNeoplasmjpanay100% (1)
- Mechanisms of CarcinogenESIS PDFDokument37 SeitenMechanisms of CarcinogenESIS PDFJessenia ZuritaNoch keine Bewertungen
- Hallmarks of Cancer: New Dimensions: ReviewDokument17 SeitenHallmarks of Cancer: New Dimensions: ReviewVignesh RavichandranNoch keine Bewertungen