Beruflich Dokumente
Kultur Dokumente
S55
Hochgeladen von
Hery Saragih AndyCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
S55
Hochgeladen von
Hery Saragih AndyCopyright:
Verfügbare Formate
I
TELEMEDICAL EDUCATION:
TEACHING SPIROMETRY ON THE INTERNET
Esther H. Lum and Thomas J. Gross
Division of Pulmonary, Critical Care, and Occupational Medicine, Department of Internal Medicine,
University of Iowa Hospitals and Clinics, Iowa City, Iowa 52242
dvances in portable equipment have led to routine spirometry testing outside of
formal pulmonary function laboratories. Practitioners ordering these tests are not
formally trained in spirometry interpretation. Providing effective off-site training
can be challenging. Our objective was to develop a remotely accessible computer-based
tutorial for teaching spirometry interpretation to nonpulmonologists. We designed an
educational module that was accessible via the Internet and tested by 65 medical trainees
at a major university medical center. In addition, the module was posted within the
Virtual Hospital on the World Wide Web. Increases in spirometry interpretative skills
were assessed using pre- and post-tests submitted electronically. The spirometry module
significantly improved spirometry interpretation by nonspecialist trainees. This improvement included a broad increase in knowledge base and was observed independent of
training level and prior spirometry reading experience. We conclude that computerbased tutorials can effectively train off-site practitioners in spirometry interpretation.
This technology allows for the dissemination of educational material from a central site of
expertise and provides a valuable adjunct to limited teaching resources.
AM. J. PHYSIOL. 276 (ADV. PHYSIOL. EDUC. 21): S55S61, 1999.
Key words: pulmonary physiology; pulmonary function tests; Virtual Hospital; medical
education
The practitioners ordering these tests, however, may
not have had formal training in the performance or
interpretation of spirometry. Whereas automated interpretation programs are available, these rigid algorithms cannot, at present, fully replace an experienced reader (3). Educating primary caregivers in
spirometry interpretation could lead to more appropriate test acquisition, data utilization, and specialty
referral (4, 15, 16). Providing convenient, effective
educational opportunities for these off-site practitioners can be a daunting task. Increased personal and
institutional access to the information superhighway,
the Internet, offers new opportunities for the remote
delivery of computer-aided instruction (7).
Pulmonary function tests (PFT) are among the first
diagnostic studies employed in the evaluation of suspected lung disease. Indeed, the measurement of expired
airflow by simple spirometry is invaluable in many
clinical settings including the diagnosis and management of bronchial asthma, evaluation of chronic cough,
and quantification of disability impairment. Recent
innovations in PFT equipment have made portable
spirometry devices reliable and accurate (19). This has
allowed for the increasing use of simple spirometry in the
primary care setting. Thus spirograms can now be
performed routinely outside of traditional PFT laboratories in outpatient office practices, industrial clinics,
and community hospital emergency rooms (13, 19).
1043 - 4046 / 99 $5.00 COPYRIGHT r 1999 THE AMERICAN PHYSIOLOGICAL SOCIETY
VOLUME 21 : NUMBER 1 ADVANCES IN PHYSIOLOGY EDUCATION JUNE 1999
S55
The University of Iowa has developed and instituted
an electronic medical education forum, The Virtual
Hospital (11). This multimedia, integrated teaching
package is accessible through the Internet (http://
indy.radiology.uiowa.edu/) and is also available to
University of Iowa-affiliated clinical outreach centers
via a statewide telemedicine network (17). We have
developed a computer-based educational module to
test whether such a teaching network could be used
to effectively improve spirometry interpretation skills
for off-site nonpulmonologists.
grams. The spirograms and clinical identifiers were
used as stems for R-type multiple matching questions
using the same list of interpretations as possible
answers for each question (5). A lead-in instructed the
students to choose the single best interpretation and
stated that each answer could be used once, more
than once, or not at all. The spirograms and the
designated correct answers were reviewed by clinical
experts in PFT interpretation (see above). These
questions were grouped as a pre-test that was taken
before reading the educational module. The same
series of spirograms was relabeled with different
clinical vignettes, randomly reordered, and presented
with the same set of potential answers as a post-test
immediately on completion of the educational module. Completion of each test triggered submission of
the results to a dedicated electronic mailbox. Feedback on performance was provided via electronic mail
to those who requested it.
METHODS
Educational module. Using published American Thoracic Society (ATS) guidelines, we designed a computer-based tutorial on the interpretation of simple
spirometry (1). In addition to stressing recognition of
specific disease patterns, standards for assessing spirogram quality were also addressed (2). To ensure that
our recommendations were consistent with standard
practice, the guidelines were reviewed and approved
by the University of Iowa Hospitals and Clinics PFT
laboratory director as well as an outside expert
reviewer (Dr. William Eschenbacher, Baylor College
of Medicine, Houston). Textual content was composed on the authors personal computer and then
transferred by electronic mail to the Virtual Hospital
librarian for conversion into hypertext markup language (HTML) files. Representative spirometry tracings were obtained from clinical spirograms performed at the University of Iowa PFT laboratory.
These figures were scanned into Adobe Photoshop
v3.0 (Adobe Systems, San Jose, CA) using a HewlettPackard ScanJet IIc and inserted within the text
document. To aid reader visualization, a normal volunteer (E. H. Lum) performing spirometry and the
flow-volume loop accompanying this effort were video
recorded (Sony Handycam, 8 mm). These video images were digitized and inserted with hot text buttons
within the body of the spirometry module.
Subjects were recruited from among the medical
students, interns, and more senior house staff rotating
through the Department of Internal Medicine according to a protocol approved by the University of Iowa
Institutional Review Board. Subjects were diverted
from scheduled noon conferences to an educational
resource center complete with multiple personal
computer stations that provided Internet access with
bookmarks directing them to the Virtual Hospital.
After a brief introduction, participants were free to
complete the pre-test, module, and post-test at their
own pace with the option of submitting their test
scores under pseudonyms. Those who completed the
exercise were compensated with a free meal.
Remote distribution of spirometry module. A site
was created on the Virtual Hospital that contained the
pre-test, module, and post-test. This site was posted
within the Pulmonary Core Curriculum section without specific advertisement or promotion. Respondents to the module who submitted the pre-test
and/or post-test were asked to identify themselves by
level of training and/or health care occupation using a
drag-down menu. Those who provided electronic
mailing addresses were given their test results and
explanations of any incorrect answers.
Spirometry interpretation testing. A series of 12
spirograms representing the entire range of material
reviewed in the educational module was collected.
For each, a brief clinical scenario was composed
detailing a fictitious patients age and sex and the
reason for ordering the patients spirogram. A series of
nine possible interpretations accompanied the spiro-
Data analysis. Test scores were reported as the
number correct out of a possible score of 12. The time
VOLUME 21 : NUMBER 1 ADVANCES IN PHYSIOLOGY EDUCATION JUNE 1999
S56
are useful for both those in training as well as primary
caregivers in practice. Therefore, the change in preand post-test scores was examined for each trainee
subgroup to determine how previous knowledge base
influenced the effectiveness of the module. At all
levels of training, post-test scores increased significantly (Fig. 2). The greatest gain in scores was
observed among the medical students, who also
manifested the lowest average pre-test scores as expected on the basis of their limited experience with
the clinical use of spirometry (Fig. 2). Subgroups with
higher pre-test scores and, presumably, more experience with interpreting spirometry, still showed significant improvement in post-test scores (Fig. 2). Similarly, nearly all individuals improved their post-test
scores whether the pre-test score was above or below
the median for their respective trainee subgroup (Fig.
3). Thus spirometry interpretive performance improved
irrespective of training level or prior experience.
required to read the module and submit post-test
results was derived from log-on records and recorded
in whole minutes. Pre- and post-test scores were
analyzed using paired, two-tailed t-tests (Microsoft
Excel 5.0 for the Macintosh) with a P value of 0.05
considered a significant difference between population means. To limit the influence of outlying values,
data were also examined using median scores.
RESULTS
The spirometry module improved spirogram interpretation by trainees. The spirometry module was
administered to 65 participants, including 20 thirdyear medical students, 17 interns, and 28 senior house
staff. The test score results followed a normal distribution (Fig. 1) with scores improving from 6 0.3
(mean SE) on the pre-test to 8 0.3 correct answers
out of 12 on the post-test (P 0.001). Furthermore, the
median test score increased from 5 to 8 correct answers
out of a possible 12, demonstrating that the increase
in post-test mean score reflected overall group improvement and not simply individual high scores.
The spirometry interpretative skills improved
across a wide range of topics. The observed improvement in spirometry interpretation skills could
have resulted from learning a few novel facts or from a
more global educational enrichment. Analysis of individual test answers showed that for nearly every
question the percentage of correct responses increased (Fig. 4). The greatest gains appeared to
The spirometry module improves test performance at all levels of training. We are interested in
developing educational tools for off-site teaching that
FIG. 1.
The spirometry module improves spirogram interpretative skills. The spirometry module, with pre- and
post-test assessments, was administered to 65 participants. Test scores are distributed normally with improvement from 6 0.3 correct responses on the
pre-test (mean SE) to 8 0.3 correct responses out
of 12 total on the post-test (P F 0.001). Median score
also increased from 5 to 8 correct responses, confirming that improvement occurred across much of the
group.
FIG. 2.
Spirometry interpretation skills improve at all levels
of training. Test scores were subgrouped by participant training level. Data are displayed as median no.
of correct responses out of a possible 12; n no. of
participants. Note that the greatest improvement in
post-test scores was observed in the group with the
lowest pre-test values (medical students); however,
significant improvement was observed for all 3 subgroups (*P F .001, post-test vs. pre-test median).
VOLUME 21 : NUMBER 1 ADVANCES IN PHYSIOLOGY EDUCATION JUNE 1999
S57
involve learning the grading schema for airways obstruction, recognizing variable upper airway obstruction, and identifying uninterpretable tests. Overall,
participation in the module improved spirometry
interpretation across the entire range of disorders
tested.
The spirometry module was brief and simple to
use. To model the experience of a remote user, our
test group gained access to the spirometry module
using the University of Iowas Internet provider. The
time required to read the module and complete the
post-test ranged from 25 to 30 min; those participants
at advanced training levels required less time (medical
students 30 2 min, senior house staff 25 2 min).
During the test sessions, few problems were encountered using or accessing the module, and most participants did not require additional directions. Thus this
self-directed educational tool was effective, time efficient, and user friendly.
FIG. 3.
The spirometry module improved interpretive performance independent of prior experience. Pre- and
post-test scores are shown for intern subgroup as no.
of correct responses out of a possible 12, where AQ
indicate individual participants; arrowheads depict
pre- and post-test median scores for entire intern
group. All but 2 participants (A and C) had an improved post-test score after completing the spirometry module. Individual post-test scores improved
whether the associated pre-test score was initially
above or below the group median. Similar findings
were observed for other groups tested (data not
shown).
The spirometry module was effectively disseminated via the Internet. The spirometry module was
incorporated within the Pulmonary Core Curriculum
FIG. 4.
Computer-based tutorial produced broad improvement in spirometry
reading skills. Analysis of submitted answers for individual test questions
showed that the percentage of correct responses increased for nearly
every question tested. The largest increase in correct answers appeared to
involve the learning of classification schema for grading airways obstruction (questions 1, 4, 10, and 12), recognizing variable upper airway
obstruction (UAO; question 11), and identifying uninterpretable studies
(questions 2 and 9). mod, Moderate; r/o, rule out.
VOLUME 21 : NUMBER 1 ADVANCES IN PHYSIOLOGY EDUCATION JUNE 1999
S58
of the Virtual Hospital. The module was posted for 12
wk without specific advertisement. Despite this lack
of solicitation, the site received 4,000 hits representing the number of times the module was accessed. A pre-test was submitted by 122 participants
who identified themselves as medical students (53%),
house staff (12%), respiratory therapists (11%), and
others such as community physicians, nurses, and
non-health care workers. From those who offered
information up front and/or responded to follow-up
electronic mail, we were able to identify participants
from Canada, the United Kingdom, Italy, Malaysia,
Brazil, the Hawaiian Islands, and numerous sites
within the continental United States. We received 17
completed pairs of pre- and post-tests. All 17 respondents increased their scores, with a median improvement of 2 correct responses (range 1 to 4). Thus, with
the use of an existing electronic teaching network, the
spirometry module was internationally displayed and
accessed. For those motivated to submit pre- and
post-tests, use of the module improved spirometry
interpretation.
adhere to ATS guidelines (4). Thus there is an educational deficit among primary care providers in recognizing proper indications for and the correct interpretation of PFT that could negatively impact the delivery
of efficient, cost-effective health care.
In response to this educational need, we have designed a computer-based tutorial to teach spirometry
interpretation that is brief, effective, and widely accessible via the Internet. The criteria and guidelines set
forth by the ATS are emphasized in a user-friendly,
multimedia format. Our analysis demonstrates that the
spirometry module is educationally effective. Participants completing the module improved their ability to
correctly interpret spirograms (Fig. 1). This improved
performance was observed among all participants
independent of level of training or prior experience in
reading PFT (Figs. 2 and 3). Interpretative skills
improved across the range of patterns covered by the
module, demonstrating a broad-based increase in
knowledge beyond the acquisition of a few novel facts
(Fig. 4). Furthermore, the spirometry module can be
completed with minimal time commitment (30 min)
and little supplementary instruction, which will hopefully encourage additional sessions as needed.
DISCUSSION
As spirometry becomes more readily available outside
of traditional pulmonary function laboratories, it will
more frequently be ordered by caregivers who may
never have been formally trained in proper interpretation. This lack of instruction combined with an
emphasis on shifting diagnostic evaluations away from
specialized centers could lead to both misdiagnoses as
well as missed diagnoses. Indeed, the need for improved understanding of PFT indications and interpretation has been documented in other studies. A review
of PFT ordering patterns by primary care internists
and house staff at a community hospital found that up
to two-thirds of the studies requested were not fully
appropriate (16). Another study estimated that nonpulmonologists misinterpret spirometry up to one-third
of the time with errors in disease classification,
overreading of normal spirograms, and misreading of
abnormal studies that illustrated restrictive defects or
upper airway abnormalities (15). These authors suggest that standards for interpreting spirometry need to
be more readily available to primary care physicians
(15). Similarly, a recent Canadian study of PFT laboratories in British Columbia found marked interobserver
variability in interpretation of standard spirograms.
This variability was attributed primarily to failure to
The durability of the knowledge gained through
participation in the spirometry module was not assessed. The effectiveness of this computer-based tutorial was not directly compared with that of more
traditional printed texts or standard lectures on spirometry interpretation. Numerous other studies, however,
have confirmed the effectiveness of similar educational tools for teaching radiograph interpretation,
pulmonary auscultation, pediatric pulmonary diseases, and well-newborn care protocols (8, 1013).
Many of the participants in these studies preferred
computer-based techniques over more traditional devices with similar educational efficacy. We envision
computer-assisted learning serving as a welcome and
effective adjunct to more traditional curricula.
Certainly, computer-assisted learning has been integrated into the medical educational arena, and its
potential applications are seemingly limitless (7, 12,
14, 23). However, the real challenge lies in disseminating these educational opportunities to students and
practitioners who may not have immediate physical
VOLUME 21 : NUMBER 1 ADVANCES IN PHYSIOLOGY EDUCATION JUNE 1999
S59
ing medical education offering through the Virtual
Hospital (http://www.vh.org/Providers/Simulations/
Spirometry/SpirometryHome.html).
access to the training center. Since computers entered
the medical workplace, their use has become increasingly routine, in both the office and the hospital. After
the spirometry module was posted on-line within the
Virtual Hospital, off-site trainees and primary care
practitioners from various countries around the world
accessed the tutorial. Pre- and post-tests submitted via
electronic mail were received, processed, and responded to without further user costs above those for
Internet provider access. Thus an effective educational intervention was distributed internationally using technology that allows for central quality control
and updating, around-the-clock access, and, if automated, immediate feedback to the participant.
In summary, we used a computer-based educational
intervention to effectively teach spirometry interpretation to nonpulmonologists. With the use of the Virtual
Hospital as a central repository, this information was
distributed to trainees and primary caregivers all over
the world. This teaching service is now provided to
many off-campus referral centers and outreach clinics
as part of a University of Iowa information network.
Soon such tutorials may be linked to computerized
pulmonary function reports, facilitating combined
distribution of clinical data and relevant educational
materials. Our preliminary study is not intended to
prove that electronic educational tools are necessary
or superior to current teaching practices. However, as
time and resources for medical education continue to
shrink, computer-aided instruction via the Internet
offers promising, cost-effective adjuncts to traditional
modes of education. In the future, we anticipate
greater development and implementation of similar
educational interventions.
Our study highlights several areas of concern that
must be addressed for remotely accessible computerbased learning to realize its full potential. First, the
quality of presented material must be assured. Although we incorporated the central features of the
ATS recommendations for spirometry standardization
into the module, clinical interpretative skills are subject to personal biases of the teacher. To maintain the
quality of its material, the Virtual Hospital has initiated
a peer review system akin to that used by standard
published journals. All material is confidentially critiqued on-line and submitted by electronic mail to
minimize response time; reviews are repeated with
scheduled regularity to ensure that material remains
current (Dr. Michael Peterson, Virtual Hospital Editorial Board, personal communication). Second, we
received several comments noting great variability in
the quality of displayed graphics and response times
for viewing video images. Thus the usefulness of a
multimedia educational tool may be limited by the
equipment available to the end user. This limitation
stresses the importance of striving to find applications
that function across multiple-user platforms. Finally,
although we were pleased to receive nearly 4,000
visits at the spirometry module site, completed test
pairs represented 1% of the total audience. To fully
engage the target audience, additional carrot-and-stick
incentives such as continuing medical education credits or special certification may be required (6, 9, 22).
Toward this end, the spirometry module has recently
been incorporated into a medical student minicourse along with other similar modules on acidbase interpretation and respiratory pathophysiology.
In addition, the module is also available as a continu-
We thank Teresa Knutson-Choi, Nola Riley, and the Virtual Hospital
support staff for expert technical assistance.
This work was supported, in part, by the American Lung Association of Iowa and a grant from the National Library of Medicine.
Address for reprint requests and other correspondence: T. J. Gross,
Room C33-GH, Div. of Pulmonary, Critical Care, and Occupational
Medicine, Univ. of Iowa Hospitals and Clinics, Iowa City, IA 52242
(E-mail: thomas-gross@uiowa.edu).
Received 23 July 1998; accepted in final form 10 February 1999.
References
1. American Thoracic Society. Lung function testing: selection
of reference values and interpretative strategies. Am. Rev.
Respir. Dis. 144: 12021218, 1991.
2. American Thoracic Society. Standardization of spirometry,
1994 update. Am. J. Respir. Crit. Care Med. 152: 11071136,
1995.
3. Banks, D. E., M. L. Wang, L. McCabe, M. Billie, and J.
Hankinson. Improvement in lung function measurements
using a flow spirometer that emphasizes computer assessment
of test quality. J. Occup. Environ. Med. 38: 279283, 1996.
4. Broder, S. L., G. Copland, J. Berkowitz, and J. Road.
Inter-observer variability of pulmonary function test interpretation (Abstract). Am. J. Respir. Crit. Care Med. 155: A71, 1997.
5. Case, S. M., and D. B. Swanson. Constructing written test
questions for the basic and clinical sciences. [On-line] National
Board of Medical Examiners. http://www.nbme.org/new.version/item.htm [1999, Jan. 28]
VOLUME 21 : NUMBER 1 ADVANCES IN PHYSIOLOGY EDUCATION JUNE 1999
S60
6. Chao, J. Continuing medical education software: a comparative review. J. Fam. Pract. 34: 598604, 1992.
7. Chodorow, S. Educators must take the electronic revolution
seriously. Acad. Med. 71: 221226, 1996.
8. DAlessandro, M. P., J. R. Galvin, W. E. Erkonen, M. A.
Albanese, V. E. Michaelsen, J. S. Huntley, R. M. McBurney,
and G. Easley. The instructional effectiveness of a radiology
multimedia textbook (Hyperlung) versus a standard lecture.
Invest. Radiol. 28: 643648, 1993.
9. Davis, D. A., M. A. Thompson, A. D. Oxman, and B.
Haynes. Evidence for the effectiveness of CME. JAMA 268:
11111117, 1992.
10. Desch, L. W., M. T. Esquivel, and S. K. Anderson. Comparison of a computer tutorial with other methods for teaching
well-newborn care. Am. J. Dis. Child. 145: 12551258, 1991.
11. Galvin, J. R., M. P. DAlessandro, W. E. Erkonen, T. A.
Knutson, and D. L. Lacey. The Virtual Hospital: a new
paradigm for lifelong learning in radiology. Radiographics 14:
875879, 1994.
12. Glowniak, J. V. Medical resources on the Internet. Ann.
Intern. Med. 123: 123131, 1995.
13. Guntupalli, K. K., V. Bandi, C. Sirgi, C. Pope, A. Rios, and
W. Eschenbacher. Usefulness of flow-volume loops in emergency center and ICU settings. Chest 111: 481488, 1997.
14. Headrick, L., A. Kaufman, P. Stillman, L. Wilkerson, and
R. Wighton. Teaching and learning methods for new generalist
physicians. J. Gen. Intern. Med. 9: S42S49, 1994.
15. Hnatiuk, O., L. Moores, T. Loughney, and K. Torrington.
Evaluation of internists spirometric interpretations. J. Gen.
Intern. Med. 11: 204208, 1996.
16. Khatri, K., R. Kaufman, and W. Baigelman. Utilization of
pulmonary function tests by primary care internists in a
community hospital. Am. J. Med. Qual. 9: 4953, 1994.
17. Kienzle, M. G., D. Curry, J. Galvin, E. Hoffman, E. Holtum,
L. Shope, J. Torner, and D. Wakefield. Iowas national
laboratory for the study of rural telemedicine: a description of a
work in progress. Bull. Med. Libr. Assoc. 83: 3741, 1995.
18. Mangione, S., L. Z. Nieman, and E. J. Gracely. Comparison
of computer-based learning and seminar teaching of pulmonary
auscultation to first-year medical students. Acad. Med. 67:
S63S65, 1992.
19. Rebuck, D. A., N. A. Hanania, A. D. DUrzo, and K. R.
Chapman. The accuracy of a handheld portable spirometer.
Chest 109: 152157, 1996.
20. Santer, D. M., V. E. Michaelsen, W. E., Erkonen, R. J.
Winter, J. C. Woodhead, J. S. Gilmer, and M. P.
DAlessandro. A comparison of educational interventions:
multimedia textbook, standard lecture, and printed textbook.
Arch. Pediatr. Adolesc. Med. 149: 297302, 1995.
21. Sestini, P., E. Rensoni, M. Rossi, V. Beltrami, and M. Vagliasindi. Mulitmedia presentation of lung sounds as a learning aid for
medical students. Eur. Respir. J. 8: 783788, 1995.
22. Thompson, W. L., J. P. Dyke, and E. Buonocore. Using the
World-Wide Web to train and certify physicians in the safe use
of fluoroscopy. AJR Am. J. Roentgenol. 166: 12631264, 1996.
23. Weiler, R. M. Creating a virtual materials and resources index
for health education using the world wide web. J. Sch. Health
66: 205209, 1996.
VOLUME 21 : NUMBER 1 ADVANCES IN PHYSIOLOGY EDUCATION JUNE 1999
S61
Das könnte Ihnen auch gefallen
- Tfug 2005 02 Uc DavisDokument21 SeitenTfug 2005 02 Uc DavisHery Saragih AndyNoch keine Bewertungen
- Technical Writing-Technical ReportDokument3 SeitenTechnical Writing-Technical ReportHery Saragih Andy100% (1)
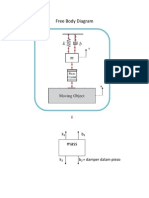
- Free Body DiagramDokument3 SeitenFree Body DiagramHery Saragih AndyNoch keine Bewertungen
- 2013 EuJRS 46 018 039 WicaksonoDokument22 Seiten2013 EuJRS 46 018 039 WicaksonoHery Saragih AndyNoch keine Bewertungen
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- CSEC Eng A Summary ExerciseDokument1 SeiteCSEC Eng A Summary ExerciseArisha NicholsNoch keine Bewertungen
- Google Automatically Generates HTML Versions of Documents As We Crawl The WebDokument2 SeitenGoogle Automatically Generates HTML Versions of Documents As We Crawl The Websuchi ravaliaNoch keine Bewertungen
- Speech by His Excellency The Governor of Vihiga County (Rev) Moses Akaranga During The Closing Ceremony of The Induction Course For The Sub-County and Ward Administrators.Dokument3 SeitenSpeech by His Excellency The Governor of Vihiga County (Rev) Moses Akaranga During The Closing Ceremony of The Induction Course For The Sub-County and Ward Administrators.Moses AkarangaNoch keine Bewertungen
- Accountancy Department: Preliminary Examination in MANACO 1Dokument3 SeitenAccountancy Department: Preliminary Examination in MANACO 1Gracelle Mae Oraller0% (1)
- Ergonomics For The BlindDokument8 SeitenErgonomics For The BlindShruthi PandulaNoch keine Bewertungen
- The Final Bible of Christian SatanismDokument309 SeitenThe Final Bible of Christian SatanismLucifer White100% (1)
- LittorinidaeDokument358 SeitenLittorinidaeSyarif Prasetyo AdyutaNoch keine Bewertungen
- Traps - 2008 12 30Dokument15 SeitenTraps - 2008 12 30smoothkat5Noch keine Bewertungen
- Grade 3Dokument4 SeitenGrade 3Shai HusseinNoch keine Bewertungen
- A Study On Investors Perception Towards Sharemarket in Sharekhan LTDDokument9 SeitenA Study On Investors Perception Towards Sharemarket in Sharekhan LTDEditor IJTSRDNoch keine Bewertungen
- 2022 Drik Panchang Hindu FestivalsDokument11 Seiten2022 Drik Panchang Hindu FestivalsBikash KumarNoch keine Bewertungen
- Coronally Advanced Flap With Connective Tissue GraDokument13 SeitenCoronally Advanced Flap With Connective Tissue GrasutriNoch keine Bewertungen
- Respiratory Examination OSCE GuideDokument33 SeitenRespiratory Examination OSCE GuideBasmah 7Noch keine Bewertungen
- "We Like": Rohit Kiran KeluskarDokument43 Seiten"We Like": Rohit Kiran Keluskarrohit keluskarNoch keine Bewertungen
- 800 Pharsal Verb Thong DungDokument34 Seiten800 Pharsal Verb Thong DungNguyễn Thu Huyền100% (2)
- CogAT 7 PlanningImplemGd v4.1 PDFDokument112 SeitenCogAT 7 PlanningImplemGd v4.1 PDFBahrouniNoch keine Bewertungen
- Popular Music Analysis and MusicologyDokument15 SeitenPopular Music Analysis and MusicologyAlexMartínVidal100% (3)
- Physics - TRIAL S1, STPM 2022 - CoverDokument1 SeitePhysics - TRIAL S1, STPM 2022 - CoverbenNoch keine Bewertungen
- Marcelo H Del PilarDokument8 SeitenMarcelo H Del PilarLee Antonino AtienzaNoch keine Bewertungen
- Ground Rules 2019Dokument3 SeitenGround Rules 2019Jeremiah Miko LepasanaNoch keine Bewertungen
- Some Problems in Determining The Origin of The Philippine Word Mutya' or Mutia'Dokument34 SeitenSome Problems in Determining The Origin of The Philippine Word Mutya' or Mutia'Irma ramosNoch keine Bewertungen
- Tugas 3Dokument20 SeitenTugas 3dellaayuNoch keine Bewertungen
- Simple Past TenselDokument3 SeitenSimple Past TenselPutra ViskellaNoch keine Bewertungen
- 2019 Ulverstone Show ResultsDokument10 Seiten2019 Ulverstone Show ResultsMegan PowellNoch keine Bewertungen
- The Gower Handbook of Project Management: Part 1: ProjectsDokument2 SeitenThe Gower Handbook of Project Management: Part 1: ProjectschineduNoch keine Bewertungen
- HG G5 Q1 Mod1 RTP PDFDokument11 SeitenHG G5 Q1 Mod1 RTP PDFKimberly Abilon-Carlos100% (1)
- The John Molson School of Business MBA 607 Final Exam June 2013 (100 MARKS)Dokument10 SeitenThe John Molson School of Business MBA 607 Final Exam June 2013 (100 MARKS)aicellNoch keine Bewertungen
- Administrator's Guide: SeriesDokument64 SeitenAdministrator's Guide: SeriesSunny SaahilNoch keine Bewertungen
- Drapeau Resume May09Dokument5 SeitenDrapeau Resume May09drmark212Noch keine Bewertungen
- Sysmex HemostasisDokument11 SeitenSysmex HemostasisElyza L. de GuzmanNoch keine Bewertungen