Beruflich Dokumente
Kultur Dokumente
Extrahepatic Biliary Duct Trauma: Spectrum
Hochgeladen von
ShandyfauzyOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Extrahepatic Biliary Duct Trauma: Spectrum
Hochgeladen von
ShandyfauzyCopyright:
Verfügbare Formate
THE WVESTERN
Journal of Medicine
Refer to: Burt TB, Nelson JA: Extrahepatic biliary duct traumaA spectrum of injuries. West J Med 134:283-289, Apr
1981
Extrahepatic Biliary Duct Trauma
A Spectrum of Injuries
TODD B. BURT, MD, and JAMES A. NELSON, MD, Salt Lake City
Blunt traumatic injury of the extrahepatic bile ducts (EBD) is uncommon.
Familiarity with the wide spectrum of possible EBD injuries is essential, however, because of the increasing number of nonpenetrating abdominal injuries
seen in modern society. These injuries include contusion with edema, hematoma and varying degrees of laceration. Edema and hematoma can result in
transient bile duct obstruction that clears spontaneously or cicatrizing inflammatory reaction resulting in stricture and obstruction. Common bile duct
stricture following blunt trauma is extremely rare, but is an unfortunate late
complication requiring biliary decompression to relieve progressive jaundice.
Laceration (partial or complete) can occur at any location in the EBD and
can be life-threatening if the diagnosis is overlooked. Hemobilia is an unusual
complication of laceration of the EBD. Failure to recognize the clinical manifestations of these uncommon injuries results in delayed and often incorrect
diagnoses. Percutaneous transhepatic cholangiography is a safe and accurate
procedure that is an important step in the workup of jaundice following blunt
trauma.
EXTRAHEPATIC BILE DUCT (EBD) injury from
blunt abdominal trauma (such as motor vehicle
accidents or acts of violence) is uncommon. Severe injuries, such as laceration or transection
require immediate surgical intervention to assure
patient survival. Injuries that are less obvious
clinically, including contusion with edema, hematoma from intramural and retroperitoneal hemorrhage and low-volume hemobilia, may be easily
overlooked particularly in patients suffering from
multiple trauma.
From the Department of Radiology, University of Utah College
of Medicine, Salt Lake City.
Submitted July 25, 1980.
Reprint requests to: Todd B. Burt, MD, Department of Radiology, University of Utah Medical Center, 50 North Medical
Drive, Salt Lake City, UT 84132.
Posttraumatic obstructive jaundice is an unfortunate sequela to EBD injuries. We report two
cases of jaundice resulting from obstruction of
the common bile duct following blunt trauma. In
one case obstruction was caused by duodenal
hematoma and edema which eventually cleared
spontaneously. In the other case retroperitoneal
and paraduodenal hematoma was followed by
fibrosis resulting in stricture that required surgical
bypass. Although upper gastrointestinal (GI) barium studies suggested the diagnosis and ultrasound testing showed bile duct dilatation, the site
and gross nature of the obstruction was best
demonstrated by thin-needle percutaneous transhepatic cholangiography (PTC). Our experience
THE WESTERN JOURNAL OF MEDICINE
283
EXTRAHEPATIC BILIARY DUCT TRAUMA
ABBREVIATIONS USED IN TEXT
EBD=extrahepatic bile ducts
GI = gastrointestinal
LD =lactate dehydrogenase
PTC = percutaneous transhepatic cholangiography
with these two unusual cases prompted this report
and a review of the literature.
Reports of Cases
CASE 1. A healthy 20-year-old woman sustained
blunt trauma to her right upper abdomen from
the steering wheel in a head-on auto accident.
Although the patient had considerable right upper
abdomen pain, there was no evidence of acute
abdomen or blood loss. Liver function test findings and amylase determinations were normal
except for mildly elevated levels of lactate dehydrogenase (LD). After a three-day stay in hospital the patient was discharged with only a complaint of mild pain of the right upper quadrant.
Two and one half weeks later, the patient returned, complaining of persistent right upper abdomen pain, nausea and the recent onset of
brownish-colored urine. She stated that she had
not been exposed to hepatitis, blood transfusion,
alcohol or intravenously given drugs. On physical
examination, yellowish discoloration of skin and
striking scleral icterus were noted. Findings of an
abdominal examination were normal except for
s.
Figure
1.-Upper
gastrointestinal barium
study showing narrow-
irregularity in
portion of
duodenum (arrow)
ing and
the second
the
that suggests hematoma or edema.
284
APRIL 1981
134
mild right upper quadrant tenderness. Significant
laboratory findings included the following: total
bilirubin 12.2 and direct bilirubin 9.6 mg per dl,
alkaline phosphatase 228 units, LD 222 units and
SGOT (serum aspartate aminotransferase; formerly
serum glutamic oxaloacetic transaminase) 131
units. Amylase, a complete blood count, prothrombin time and partial thromboplastin time
were within normal limits.
The patient was admitted to hospital and a
liver-spleen scan using technetium 99m sulphur colloid showed a liver and spleen withoutdefect. An upper GI study suggested an intraduodenal hematoma in the second portion of the
C-loop (Figure 1). An ultrasound test showed
mildly enlarged gallbladder and extrahepatic bile
ducts. PTC was done with a 23-gauge Chiba needle
on the third hospital day. This demonstrated a
normal intrahepatic biliary tree with obstruction
of the distal common bile duct by a persistent,
smooth-mass effect with failure to empty into the
duodenum. Follow-up films at one hour showed
persistent contrast in the biliary tree (Figure 2).
Figure 2.-One hour follow-up film after thin-needle
percutaneous transhepatic cholangiography. Tapered
distal common duct with meniscal obstruction (small
arrow) and no passage of contrast into duodenum.
Excretory urograms from contrast entering vascular
system from obstructed biliary system.
EXTRAHEPATIC BILIARY DUCT TRAUMA
Because of symptomatic improvement it was
elected to only observe the patient. Over the next
several months the patient's jaundice gradually
subsided without surgical intervention and all
symptoms resolved. Two years following the accident, the patient was asymptomatic with normal
findings on liver function tests.
CASE 2. A 22-year-old man sustained a crush
injury to the upper abdomen in a drilling accident.
An exploratory laparotomy was done immediately
because of grossly bloody peritoneal tap. During
the operation hematomas involving the second
and third portions of the duodenum, the retroperitoneal space and the posterior aspect of the
pancreas were found. The gallbladder was intact
and there was no evidence of bile duct laceration
or transection. The hematomas were drained and
the patient was later discharged with abdominal
wounds healing well and normal findings on liver
function tests except for mildly elevated LD levels.
The patient was readmitted approximately three
weeks later for persistent nausea, vomiting, a 25pound weight loss, and increasing malaise and
weakness. An upper GI study was done, which
showed compression of the duodenum by hematoma or fibrosis (Figure 3). Abdominal ultrasound testing demonstrated a normal pancreas,
and no dilated biliary ducts were seen. During
this hospital stay the patient was noted to have
scleral icterus. Laboratory results included total
bilirubin 5.2 mg per dl, alkaline phosphatase 504
units and SGOT 141 units. PTC was done with a
23-gauge Chiba needle, which showed dilated
hepatic and common bile ducts with complete
distal obstruction (Figure 4). No intraluminal
filling defects were present in the ducts or gallbladder. An operation was carried out immediately following the PTC and massive adhesions in
the area of the duodenum, gallbladder and liver
bed were discovered. Pronounced fibrosis and
thickening were present in the periampullary
region, but no residual hematomas were found.
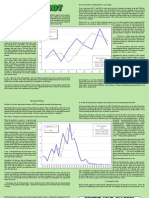
Figure 3.-Two views from upper gastrointestinal study showing irregularity and narrowing involving the second
and third portion of duodenum, which proved secondary to massive adhesions.
THE WESTERN JOURNAL OF MEDICINE
285
EXTRAHEPATIC BILIARY DUCT TRAUMA
Surgical decompression with T-tube drainage was
carried out and the patient's liver function gradually improved and symptoms slowly resolved.
However, because of persistent obstruction noted
on the follow-up T-tube cholangiograms, Rouxen-Y cholecystojejunostomy was done. The patient
tolerated this procedure well, and his post-
Figure 4.-PTC with injection into gall bladder shows
dilated extrahepatic biliary ducts and abrupt obstruction of the distal common bile duct. The obstruction
was secondary to pronounced fibrosis in the paraduodenal and retroperitoneal region (PTC = percutaneous
transhepatic cholangiography).
TABLE 1.-Causes of Jaundice Following
Blunt Abdominal Trauma
Trauma-related
Liver laceration
Liver hematoma
Liver abscess
Hepatic vascular accident
Budd-Chiari
Hemobilia
Acute pancreatitis
Posttraumatic hepatic dysfunction syndrome
Intrahepatic and extrahepatic duct damage
Posttraumatic cholecystitis
Surgery-related
latrogenic
Operative stress on preexisting liver disease
General anesthesia
Postoperative cholecystitis
Miscellaneous
Hemolysis (transfusions, resolving hematoma)
Viral hepatitis
Drug toxicity
286
APRIL 1981
* 134 * 4'
operative course was uncomplicated. During follow-up, findings of liver function tests returned
to normal and all symptoms resolved.
Discussion
Jaundice Following Trauma
Jaundice is often a perplexing complication that
develops following major abdominal traunma. Historical, clinical and laboratory data will often distinguish hemolytic, obstructive or hepatocellular
causes of jaundice. Following traumatic injuries,
however, many patients receive multiple blood
transfusions, may have preexisting liver disease,
and often undergo operations requiring general
anesthesia. In these cases, the differential diagnosis
may be difficult and easy differentiation becomes
impossible. Some important causes of jaundice
following blunt abdominal trauma are listed in
Table 1.
Liver lacerations, hematomas, abscesses and
vascular injuries may all result from blunt abdominal trauma and lead to jaundice.1 Rarely, as
illustrated in these two case reports, hematoma,
edema, or both, and fibrosis can compress the
distal common bile duct and result in temporary
or permanent obstruction. Recently, the posttraumatic hepatic dysfunction syndrome has been
described as a distinct clinicopathologic entity.2
This syndrome is considered to result from hepatic
ischemia caused by either hypoxia or hypotension
following resuscitation from major trauma.
In a traumatized patient who has undergone an
operation, mild hyperbilirubinemia in the first few
postoperative days may be viewed with interest
but without serious concern because many of these
patients are suspected of having hemolysis from
blood transfusions or from resorption of hematoma. If jaundice is persistent or progressive, however, iatrogenic surgical trauma to the biliary tree,
anesthetic toxicity and operative stress on preexisting liver disease should be considered as potential
causes.1 3'4 Acute acalculous cholecystitis must
also be considered because of its known occurrence in both traumatized and surgical patients.5'6
When obstructive jaundice is suspected, abdominal ultrasound testing and PTC are essential
to arrive at the correct diagnosis. Ultrasonography
is very helpful in demonstrating dilated biliary
ducts, gallbladder and common bile duct stones,
as well as abdominal hematomas, abscesses and
cysts. However, ultrasound testing alone cannot
diagnose an EBD laceration or indicate the site of
EXTRAHEPATIC BILIARY DUCT TRAUMA
TABLE 2.-EBD Rupture Due to
Blunt Abdominal Trauma
Type
No. of Cases NVo. of Deaths
Transected common duct .... 25
Lacerated common duct ..... 31
Transected hepatic duct ..... 2
Lacerated hepatic duct ...... 27
Lacerated cystic duct .....1..
Unknown site ............. 5
7
10
0
10
0
1
TOTAL .................. 91
EBD=extrahepatic bile duct
28
an obstruction.7 As illustrated in our case reports,
PTC is a fast, accurate and safe method for differentiating obstructive from nonobstructive jaundice and for defining the level of obstruction when
present. PTC may also show extravasation secondary to either a liver or biliary tree laceration,
intraluminal filling defects secondary to either
blood clots or stones, or deviation of the biliary
ducts from abscess or hematoma.
Pathophysiology of EBD Injuries
The exact nature of the force necessary to cause
injury to the EBD iS unknown, although the following have been postulated: (1) impingement
and compression of the ductal system on the vertebral column,8 (2) external compression of the
gallbladder with transmitted rise in intraductal
pressures resulting in "blowout of the duct"9 and
(3) laceration of the ductal system at the junction of its fixed and mobile portions.10"'1 The first
theory seems to explain best the duct injuries that
result in hematoma and edema, especially in the
periampullary and retroperitoneal region. Injuries
to the vessels supplying the EBD in this region
result from the crushing abdominal blow and result in hematoma and ischemia which may heal
with fibrosis. The last postulate best explains duct
laceration and is clinically supported in that rupture of the EBD is most frequently encountered
where the mobile common bile duct becomes fixed
as it enters the superior edge of the pancreas.'2
The blowout theory has not been confirmed in
animal models or in clinical situations.'3 Although
the exact pathophysiology still remains unclear,
it is likely that a combination of the mechanisms
proposed above is responsible for EBD injuries.
The rarity of injury to the portal vein and
hepatic artery has intrigued many writers. Dorton'4 suggested that the tortuous and elastic hepatic artery has no points of fixation near the area
of trauma, making it less susceptible to injury.
He also suggested that because the portal vein
has no valves, intraluminal pressure from a direct
blow is decompressed into the splenic reservoir,
dissipating the energy.
Extrahepatic Biliary Duct Injuries
Complete and partial laceration occurring in
all portions of the EBD have been previously described. A careful review of the literature from
1890 to 1970 by Rydell uncovered 91 cases of
EBD lacerations.'2 Table 2 tabulates the location
and degree of these ruptures. Since that time,
avulsion of the ampulla of Vater," "I as well as
several other reports of EBD ruptures,"-725 have
been added to the literature. The most common
location for duct disruption is the suprapancreatic
retroduodenal portion (superior border of the
pancreas."' 7'22 Laceration may be limited to a
single portion of the biliary tree'5 18,20,22,2" or may
be found in combination with other EBD injuries.2'
EBD injuries may also be isolated or may be found
in any combination with other abdominal visceral
injuries with the liver, duodenum, pancreas, and
spleen being the most common sites.2 When distal
common bile duct injuries occur, pancreatic and
duodenal injuries are commonly associated.'6
In severely injured patients, indications for
exploratory laparotomy are often clearly evident
and unsuspected biliary tract trauma may be
found during the operation. When the abdominal
injury is less severe or confined to the biliary tree,
however, indications for laparotomy may not be
present and a significant occult injury of the EBD
may remain undiagnosed. Walt and Grifka28 reported on 307 consecutive cases of blunt abdominal trauma and found that injuries to the
common bile duct were the least frequent injury
to result in exploratory laparotomy. To add to
the difficulty in differential diagnosis, a history
of trauma may not be given because the patient
may either feel that it was insignificant or fail
to recall it.
The clinical course of EBD lacerations has a
characteristic pattern20'22 as follows: (1) The initial injury may be followed by shock of varying
degree that usually lasts for only a few hours;
(2) this is often followed by a symptom-free
quiescent period of several days; (3) finally, progressive abdominal pain, nausea, vomiting, jaundice and, in some cases, abdominal distention
from bile ascites ensue. Acholic stools, fever,
rapid wasting of abdominal muscles and scleral
THE WESTERN JOURNAL OF MEDICINE
287
EXTRAHEPATIC BILIARY DUCT TRAUMA
icterus often develop as well. Although this sequence usually occurs over three to ten days,
symptoms may not become intense enough to
cause the patient to seek medical advice for weeks
to months. Abdominal paracentesis may yield bile,
at which time the diagnosis should be clear.27
Biliary duct obstruction resulting from edema
or hematoma in the duodenal, periampullary or.
retroperitoneal region is uncommon. During the
past 30 years more than 170 cases of intramural
and paraduodenal hematomas from blunt abdominal trauma have been reported. 2930 In only
four of these previously cited cases did the hematoma result in obstruction of the distal common
bile duct.733 To these, we add an additional
case, bringing the total to five. Of these cases,
three patients did not recall abdominal trauma,
one considered the traumatic episode minor and
one had significant blunt trauma to the abdomen.
This attests to the fact that a history of trauma is
not always obtained even when a serious duodenal
and retroperitoneal hematoma is present. In the
previously reported and currently presented cases
of biliary obstruction, one required decompression by cholecystojejunostomy,33 two resolved
after evacuation of the blood clot14,35 and the other
two resolved spontaneously (patients in reference
7 and in case 1). Jaundice developed as early as
three days,34 and as late as three weeks (case 1)
following the traumatic episode. Davis33 has suggested that the characteristic delay between injury
and jaundice is secondary to gradual increase in
the size of the hematoma. He postulates that as
the hematoma undergoes proteolysis, tissue fluid
is absorbed from the interstitial spaces by osmosis
and results in delayed obstruction of the distal
common bile duct.
Abdominal trauma may result in delayed obstruction of the common bile duct from fibrosis,
as illustrated in our second case. This is extremely
rare with only two other reported cases in the
English literature.37 These cases represent a more
subtle type of duct injury than rupture or complete division. A small tear with subsequent bile
leakage initially may not be evident clinically or
at laparotomy. This may result in a small area of
inflammation, followed by healing with fibrosis
that results in stricture or complete obstruction.
Another possibility is that paraduodenal hematoma may undergo organization with fibrosis and
subsequent common duct stricture. As noted both
in our case and a previously reported case, this
injury was not observed at initial laparotomy
despite mobilization of the head of the pancreas
and duodenum. In all cases the biliary tree required permnanent decompression by a Roux-en-Y
choledochojejunostomy.
Another important, albeit unusual, complication of EBD injury is hemobilia. Sandblom reviewed 355 cases of hemobilia and found that 55
percent were secondary to trauma.38 P53) If caused
by blunt trauma, the blow was usually extremely
violent and often resulted in damage to several
organs. He reported that most hemobilia resulted
from parenchymal rupturt of the liver and that
out of 80 patients with blunt abdominal trauma
Blunt Abdominal Trauma
ACUTE
Contusion and
+~~~~~
SUBACUTE Spontaneous <resolution
Laceratio
Periampullary and
edema
Compression
EBD
PeramullryandLaeraio
duodenal
EBD obstruction
CHRONIC
hematoma1a
I
-*-
-Hematoma
organization
Healing with
fibrosis
Partial transection
Spontaneous
resolution
Complete
Hemobilia
X transection
Inflammation
Bile
ascites
Intraluminal
clot
Gallstones
EBD stricture or
obstruction
Figure 5.-EBD injuries and sequelae secondary to blunt abdominal trauma (EBD=extrahepatic bile ducts).
288
APRIL 1981
134 * 4
EXTRAHEPATIC BILIARY DUCT TRAUMA
and hemobilia, only four originated from EBD
injuries.38(P)6 Hemobilia often develops following
trauma, with the classic triad of biliary colic,
jaundice and gastrointestinal bleeding. The pain,
produced by the distention of the bile ducts with
blood, precedes external evidence of bleeding, so
that a patient with recurrent episodes of bleeding
may be able to predict the onset of melana or
hematemesis. Arteriography is diagnostic when
hemorrhaging is actually occurring; intermittency
of bleeding, however, is characteristic of hemobilia. A related complication of theoretic interest
is the formation of gall stones from intraluminal
clots, which has been demonstrated by Sandblom.39 The incidence of this condition is unknown but is undoubtedly rare.
Surprisingly, no reports of posttraumatic EBD
fistulae or cysts were encountered in the literature. Bronchobiliary and pleurobiliary fistulae,
however, have been reported from intrahepatic
ducts to the chest after severe thoracic and abdominal trauma.40
Conclusion
Extrahepatic bile duct trauma may clearly result
in a wide spectrum of injuries as summarized in
Figure 5. Although these injuries are uncommon,
clinicians as well as radiologists must be thoroughly aware of their existence in order to provide
adequate care for these traumatized patients. Abdominal ultrasound and GI studies will often suggest an EBD injury, which can be safely and directly demonstrated by PTC. Treatment of EBD
laceration and transection is clearly surgical.22
When trauma results in edema or hematoma,
however, therapy must be based on the condition
of the individual patient and consideration of other
abdominal injuries.29
REFERENCES
1. Hardy JD: Postoperative jaundice, In Sabiston DC (Ed):
Textbook of Surgery, 11th Ed. Philadelphia, Saunders, 1977, pp
429-430
2. Champion HR, Jones RT, Trump BF, et al: Post-traumatic
hepatic dysfunction as a major etiology in post-traumatic jaundice.
J 'rrauma 16:650-657, 1976
3. Seror J, Schmitt JC, Pateras C, et al: Operative injuries to
the bile ducts. Int Surg 63:108-113, 1978
4. Hillis TM, Westbrook KC, Caldwell FT, et al: Surgical injury of the common bile duct. Am J Surg 134:712-716, 1977
5. Howard RJ, Velany JP: Postoperative cholecystitis. Am J
Dig Dis 17:213-218, 1972
6. Dupriest RW: Acute cholecystitis complicating trauma. Ann
Surg 189:84-89, 1979
7. Foley CL, Teele RL: Ultrasound of epigastric injuries after
blunt trauma. AJR 132:593-598, 1979
8. Lewis KM: Traumatic rupture of the bile duct. Ann Surg
108:237-241, 1938
9. Mason LB, Sidnury JB, Guiang S: Rupture of the extrahepatic ducts from non-penetrating trauma. Ann Surg 140:234241, 1954
10. Mohardt JH: Traumatic rupture of the common bile duct.
Q Bull NW Med Sch 30:16-20, 1956
11. Fish JC, Johnson GL: Rupture of the duodenum following
blunt trauma. Ann Surg 162:917-919, 1965
12. Rydell WB: Complete transection of the common bile duct
due to blunt abdominal trauma. Arch Surg 100:724-728, 1970
13. Fletcher WS, Mahnke DE, Dunphy JE: Complete division
of the common bile duct due to blunt abdominal trauma. J
Trauma 1:87-95, 1961
14. Darton HE: Complete division of the common bile duct
due to blunt abdominal trauma. Am Surg 31:331-335, 1965
15. Parkinson SW, Wisniewski ZS: Avulsion of the ampulla of
Vater: An isolated injury following blunt abdominal trauma. Aust
NZ J Surg 48:562-564, 1978
16. Balsano NA, Reynolds BM: Rupture of the common duct
and ampulla of Vater due to blunt trauma. Ann Surg 178:200203, 1973
17. Tonnesen P: Rupture of extra-hepatic biliary ducts from
blunt external trauma. Dan Med Bull 17:238-245, 1970
18. Janss G, Freimark L: Isolated transection of the common
duct. JACEP 8:161-163, 1979
19. Sinclair MC, Moore TC, Asch MJ, et al: Injury to hollow
abdominal viscera from blunt trauma in children and adolescents.
Am J Surg 128:693-698, 1974
20. Shorthouse AJ, Singh MP, Treasure T, et al: Isolated complete transection of the common bile duct by blunt abdominal
trauma. Br J Surg 65:543-545, 1978
21. Zollinger RM, Keller RT, Hubay CA: Traumatic rupture
of the right and left hepatic ducts. J Trauma 12:563-569, 1972
22. Turney WH, Lee JP, Raju S: Complete transection of the
common bile duct -due to blunt trauma. Ann Surg 179:440.444,
1974
23. Parkinson SW: Complete severance of the common bile
duct due to blunt trauma. Aust NZ J Surg 39:253-254, 1970
24. Caro AM, Losa JMO: Complete avulsion of the common
bile duct as a result of blunt abdominal trauma. J Pediatr Surg
5:60-62, 1970
25. Haynes CD, Given KS, Stone HH, et al: Nonsurgical
trauma to the extrahepatic ducts. South Med J 62:1323-1326, 1969
26. Moffat RC, Lucas RJ: Transection of the common bile duct
as an isolated injury following blunt trauma. Can J Surg 12:334335, 1969
27. Longmire WP, McArthur MS: Occult injuries of the liver,
bile duct, and pancreas after blunt abdominal trauma. Am J Surg
125:661-666, 1973
28. Walt AJ, Grifka TJ: Blunt abdominal injury, In Gurdjian
ES, Lange WA, Patrick LM, et al (Eds): Impact Injury and
Crash Protection. Springfield, IL, Charles C Thomas, 1970, pp
101-123
29. Fullen WD, Selle JG, Whitely DH, et al: Intramural duodenal hematoma. Ann Surg 179:549-555, 1974
30. Maull KI, Fallahzudeh H, Mays ET: Selective management
of posttraumatic obstructing intramural hematoma of the duodenum. Surg Gynecol Obstet 146:221-224, 1978
31. Izant RF, Drucker WR: Duodenal obstruction due to intramural hematoma in children. J Trauma 4:797-813, 1963
32. Resnicoff SA, Morton JH: Changing concepts concerning
intramural duodenal hematomas. J Trauma 9:561-576, 1969
33. Davis DR, Thomas CY: Intramural hematoma of the duodenum and jejunum. Ann Surg 153:394-398, 1961
34. Parrish RA, Edmondson HT, Moretz WH: Duodenal and
biliary obstruction secondary to intramural hematoma. Am J Surg
108:428-430, 1964
35. Ferguson IA, Goade WJ: Intramural hematoma of the duodenum. N Engl J Med 260:1176-1177, 1954
36. Felson B, Levin ET: Intramural hematoma of the duodenum: A diagnostic sign. Radiology 63:823-831, 1954
37. Skow JR, Longmire WP: Common duct stricture secondary
to blunt abdominal trauma. Ann Surg 40:576-578, 1974
38. Sandblom P: Hemobilia (Biliary Tract Hemorrhage), 1st
Ed. Springfield, IL, Charles C Thomas, 1972
39. Sandblom P, Mirkovitch U, Saegesser F: Formation and
fate of fibrin clots in the biliary tree. Ann Surg 185:356-366, 1977
40. Operal SS, Mandal AK: Traumatic thoracobiliary fistulae:
Clinical and review study. J Trauma 18:539-544, 1978
THE WESTERN JOURNAL OF MEDICINE
289
Das könnte Ihnen auch gefallen
- Ebook PDF The Phlebotomy Textbook 4th Edition PDFDokument41 SeitenEbook PDF The Phlebotomy Textbook 4th Edition PDFmelody.bowers405100% (29)
- Post LapChole Bile LeaksDokument41 SeitenPost LapChole Bile LeaksIfeanyichukwu OgbonnayaNoch keine Bewertungen
- Arteria MesentericaDokument3 SeitenArteria MesentericaJadilson BorgesNoch keine Bewertungen
- Diverticuloza DuodenalaDokument4 SeitenDiverticuloza Duodenalaraluca77Noch keine Bewertungen
- Management of Accessory Hepatic Ducts in Choledochal CystsDokument2 SeitenManagement of Accessory Hepatic Ducts in Choledochal CystsJosé MartínezNoch keine Bewertungen
- ABDOMINAL Assesory LiverDokument4 SeitenABDOMINAL Assesory Liverwelly_hartonoNoch keine Bewertungen
- Biloma After Laparoscopic Cholecystectomy: Case ReportDokument3 SeitenBiloma After Laparoscopic Cholecystectomy: Case ReportAlpriyando Rindy AgustinusNoch keine Bewertungen
- Small BowelDokument5 SeitenSmall BowelFachry MuhammadNoch keine Bewertungen
- Case 12192Dokument9 SeitenCase 12192Novi OktaviantiNoch keine Bewertungen
- Acute Gastric Dilation and Ischemia Secondary To Small Bowel ObstructionDokument4 SeitenAcute Gastric Dilation and Ischemia Secondary To Small Bowel ObstructionMudatsir N. MileNoch keine Bewertungen
- Recurrent Acute Pancreatitis and Massive Hemorrhagic Ascites Secondary To A Duodenal Duplication in A Child: A Case ReportDokument4 SeitenRecurrent Acute Pancreatitis and Massive Hemorrhagic Ascites Secondary To A Duodenal Duplication in A Child: A Case ReportHarnadi WonogiriNoch keine Bewertungen
- April 2009.caglayan GallstoneileusDokument4 SeitenApril 2009.caglayan GallstoneileusDaru KristiyonoNoch keine Bewertungen
- 19Dokument3 Seiten19Elizabeth ToapantaNoch keine Bewertungen
- July 10Dokument2 SeitenJuly 10junrey1990Noch keine Bewertungen
- 8874 33333 1 PBDokument3 Seiten8874 33333 1 PBRanga PereraNoch keine Bewertungen
- Kolangitis Case 1Dokument6 SeitenKolangitis Case 1Dhen Mas PrimanaNoch keine Bewertungen
- Case ReportDokument6 SeitenCase ReportArrizqi Ramadhani MuchtarNoch keine Bewertungen
- Jaundice: Presented by Dr. Pollock Prepared by Christopher Edwards Tintanalli Chapter 84, Pgs. 560-561 October 2005Dokument46 SeitenJaundice: Presented by Dr. Pollock Prepared by Christopher Edwards Tintanalli Chapter 84, Pgs. 560-561 October 2005Edwin Jose SNoch keine Bewertungen
- Steroid Induced Perforation of Gall Bladder-Report of A Rare Case and Review of LiteratureDokument2 SeitenSteroid Induced Perforation of Gall Bladder-Report of A Rare Case and Review of LiteratureIOSR Journal of PharmacyNoch keine Bewertungen
- EN Acute Pancreatitis As A Complication ofDokument5 SeitenEN Acute Pancreatitis As A Complication ofShandy JonnerNoch keine Bewertungen
- Jurnal Bedah 2Dokument5 SeitenJurnal Bedah 2nafamaulidinaNoch keine Bewertungen
- 201 203 AbdominalDokument3 Seiten201 203 AbdominalManal Salah DorghammNoch keine Bewertungen
- Kohler TIPSPortalveinthrombosis 10102015Dokument29 SeitenKohler TIPSPortalveinthrombosis 10102015sirrfsNoch keine Bewertungen
- Biliary Cast Syndrome in Portal Hypertensive Biliopathy: Direct Cholangioscopic Findings and Endoscopic Therapy With Metal StentDokument3 SeitenBiliary Cast Syndrome in Portal Hypertensive Biliopathy: Direct Cholangioscopic Findings and Endoscopic Therapy With Metal StentMarcelo CalossoNoch keine Bewertungen
- Raj KamalDokument5 SeitenRaj KamalBhavani Rao ReddiNoch keine Bewertungen
- Triple GallbladerDokument12 SeitenTriple GallbladerRudy Arindra WijayaNoch keine Bewertungen
- Cureus 0012 00000011460Dokument6 SeitenCureus 0012 00000011460AlixNoch keine Bewertungen
- Posttraumatic Hematuria With Pseudorenal Failure: A Diagnostic Lead For Diagnosing Intraperitoneal Bladder Rupture.Dokument4 SeitenPosttraumatic Hematuria With Pseudorenal Failure: A Diagnostic Lead For Diagnosing Intraperitoneal Bladder Rupture.Ketan VagholkarNoch keine Bewertungen
- Hepatobiliary and Pancreatic: AIDS CholangiopathyDokument2 SeitenHepatobiliary and Pancreatic: AIDS Cholangiopathykhan jeetNoch keine Bewertungen
- Cholecystitis: Causes and PathologyDokument12 SeitenCholecystitis: Causes and PathologySher KhanNoch keine Bewertungen
- Dr. Aisha Al-Zuhair General Surgery Kfhu - Khobar - Saudi Arabia Dec 16, 2009Dokument75 SeitenDr. Aisha Al-Zuhair General Surgery Kfhu - Khobar - Saudi Arabia Dec 16, 2009Bagus PattiwaelNoch keine Bewertungen
- Ausencia Congenita Del Conducto Cistico. Mini-Revision 2013Dokument6 SeitenAusencia Congenita Del Conducto Cistico. Mini-Revision 2013Bolivar IseaNoch keine Bewertungen
- A 45 - Year - Old Woman PresentingDokument19 SeitenA 45 - Year - Old Woman PresentingNicola4Noch keine Bewertungen
- Case StudyDokument18 SeitenCase Studyapi-259257079Noch keine Bewertungen
- s13304 011 0131 2 PDFDokument3 Seitens13304 011 0131 2 PDFRoderick Núñez JNoch keine Bewertungen
- What Is An Acute AbdomenDokument112 SeitenWhat Is An Acute AbdomenLavasa SharmaNoch keine Bewertungen
- Case ReportDokument5 SeitenCase ReportAmmar magdyNoch keine Bewertungen
- Orthotopic Liver TransplantationDokument5 SeitenOrthotopic Liver Transplantationsally satriaNoch keine Bewertungen
- Biliary Duct ImagingDokument7 SeitenBiliary Duct ImagingImam FahriNoch keine Bewertungen
- CT Mesenteroaxial GVDokument6 SeitenCT Mesenteroaxial GVkueputuNoch keine Bewertungen
- General Data: Chief Complain:: Case Protocol: Colon CaDokument8 SeitenGeneral Data: Chief Complain:: Case Protocol: Colon CaIC BNoch keine Bewertungen
- Background: Go ToDokument5 SeitenBackground: Go ToАлександр КравченкоNoch keine Bewertungen
- Intestinal Obstruction: By: Dr. Wasfi M SalaytaDokument16 SeitenIntestinal Obstruction: By: Dr. Wasfi M SalaytayayaNoch keine Bewertungen
- 3472-2. Manuscript - Word File-25886-1-10-20210921Dokument1 Seite3472-2. Manuscript - Word File-25886-1-10-20210921Patricia Peñaflor GrimaldoNoch keine Bewertungen
- Clinical Manifestations and Diagnosis of Urinary Tract Obstruction and Hydroneph PDFDokument32 SeitenClinical Manifestations and Diagnosis of Urinary Tract Obstruction and Hydroneph PDFAmjad Saud0% (1)
- Left-Sided Appendicitis with Intestinal MalrotationDokument10 SeitenLeft-Sided Appendicitis with Intestinal MalrotationpigzeniNoch keine Bewertungen
- Multilevel Duodenal Injury After Blunt TraumaDokument5 SeitenMultilevel Duodenal Injury After Blunt TraumaHanny RusliNoch keine Bewertungen
- Acute Mesenteric Ischemia in COVID19 Patient - NAT FixedDokument10 SeitenAcute Mesenteric Ischemia in COVID19 Patient - NAT FixedAde Tan RezaNoch keine Bewertungen
- Surgery CBL Module 4Dokument22 SeitenSurgery CBL Module 4A SNoch keine Bewertungen
- Gu Chart Note - EditedDokument1 SeiteGu Chart Note - Editedkm1021Noch keine Bewertungen
- GI Summer Review - Answers - Bosch (2013)Dokument16 SeitenGI Summer Review - Answers - Bosch (2013)Jessica MooreNoch keine Bewertungen
- 6 Imaging of Acute AbdomenDokument73 Seiten6 Imaging of Acute AbdomenAliyah Tofani PawelloiNoch keine Bewertungen
- Causes Symptoms Diagnosis Treatment CholecystitisDokument4 SeitenCauses Symptoms Diagnosis Treatment CholecystitisJu BuNoch keine Bewertungen
- Liver and BiliaryDokument15 SeitenLiver and Biliaryasmatmasoom5566Noch keine Bewertungen
- DR HK Leung Queen Elizabeth Hospital Joint Hospital Surgical Grand RoundDokument29 SeitenDR HK Leung Queen Elizabeth Hospital Joint Hospital Surgical Grand RoundNoy FaridaNoch keine Bewertungen
- KlatskinDokument24 SeitenKlatskinArian WawolumajaNoch keine Bewertungen
- Scintigraphicdetectionof Segmentalbile-Ductobstruction: Case ReportsDokument2 SeitenScintigraphicdetectionof Segmentalbile-Ductobstruction: Case ReportsMuzafar AhmedNoch keine Bewertungen
- Corrosive InjuryDokument6 SeitenCorrosive InjuryCristian O. Saavedra RodriguezNoch keine Bewertungen
- Intestinal ObstructionDokument52 SeitenIntestinal ObstructionAsfandyar Khan100% (2)
- Interventional Approaches Gallbladder DiseaseDokument9 SeitenInterventional Approaches Gallbladder DiseaseAntônio GoulartNoch keine Bewertungen
- PaperDokument9 SeitenPaperShandyfauzyNoch keine Bewertungen
- Wegener GranulomatosisDokument3 SeitenWegener GranulomatosisShandyfauzyNoch keine Bewertungen
- EDokument5 SeitenEShandyfauzyNoch keine Bewertungen
- Practice Makes Perfect Scalp RingwormDokument2 SeitenPractice Makes Perfect Scalp RingwormShandyfauzyNoch keine Bewertungen
- EDokument5 SeitenEShandyfauzyNoch keine Bewertungen
- Management of foreign body ingestion in childrenDokument5 SeitenManagement of foreign body ingestion in childrenShandyfauzyNoch keine Bewertungen
- Compartment SyndromeDokument3 SeitenCompartment SyndromeKoleksi Santek IIINoch keine Bewertungen
- MalariaDokument6 SeitenMalariaUm HamoOdNoch keine Bewertungen
- Wegeners Granulomatosis Diagnosis ManagementDokument22 SeitenWegeners Granulomatosis Diagnosis ManagementShandyfauzyNoch keine Bewertungen
- Hidranitis Kiko 2Dokument428 SeitenHidranitis Kiko 2ShandyfauzyNoch keine Bewertungen
- GiftasupDokument50 SeitenGiftasupFizza SiddiquiNoch keine Bewertungen
- Hemodynamic Regulation 1Dokument3 SeitenHemodynamic Regulation 1ShandyfauzyNoch keine Bewertungen
- CVD Info 11Dokument23 SeitenCVD Info 11Achmad FauzyNoch keine Bewertungen
- Fluid Therapy FinalDokument3 SeitenFluid Therapy FinalAngga Herlambang Nagarasit LiongNoch keine Bewertungen
- 1 Septicemia, & SepsisDokument14 Seiten1 Septicemia, & SepsisfgrNoch keine Bewertungen
- Sop For Periodic FitnessDokument6 SeitenSop For Periodic FitnessEkum EdunghuNoch keine Bewertungen
- Nanda Hematemesis MelenaDokument13 SeitenNanda Hematemesis MelenaLiya AnjelinaNoch keine Bewertungen
- Hesi Hints Part 4Dokument2 SeitenHesi Hints Part 4Sharon TanveerNoch keine Bewertungen
- Oral Myiasis PublicationDokument6 SeitenOral Myiasis PublicationAnkita GoklaniNoch keine Bewertungen
- Adjuvants - IntroductionDokument1 SeiteAdjuvants - Introductionsaranya INoch keine Bewertungen
- (English) About Your Heart Attack - Nucleus Health (DownSub - Com)Dokument2 Seiten(English) About Your Heart Attack - Nucleus Health (DownSub - Com)Ken Brian NasolNoch keine Bewertungen
- HSV 2 TreatmentDokument23 SeitenHSV 2 Treatmentbobhelp100% (1)
- STROKE-pathophysiology, Diagnosis, and Management, 4th EditionDokument3 SeitenSTROKE-pathophysiology, Diagnosis, and Management, 4th EditionNishi RuciNoch keine Bewertungen
- Somatic Cell Count and Type of Intramammary Infection Impacts Fertility in Vitro Produced Embryo TransferDokument6 SeitenSomatic Cell Count and Type of Intramammary Infection Impacts Fertility in Vitro Produced Embryo TransferalineNoch keine Bewertungen
- Electrochemical Methods For The Analysis of Clinically RelevantDokument90 SeitenElectrochemical Methods For The Analysis of Clinically Relevantch_ymyaaNoch keine Bewertungen
- Emergency drugs study guideDokument75 SeitenEmergency drugs study guideQuinonez Anna MarieNoch keine Bewertungen
- Solutions For Bronchoscopy Brochure 0001 v1 en 2012Dokument13 SeitenSolutions For Bronchoscopy Brochure 0001 v1 en 2012Monica PetreNoch keine Bewertungen
- EVD PosterDokument1 SeiteEVD PosterDwie 'keonk' UnisaspalaNoch keine Bewertungen
- Applied PalynologyDokument2 SeitenApplied PalynologySanjoy NingthoujamNoch keine Bewertungen
- Medical Image Computing (Cap 5937)Dokument44 SeitenMedical Image Computing (Cap 5937)Android ApplicationsNoch keine Bewertungen
- NCP JaundiceDokument3 SeitenNCP JaundiceCamille Joy BaliliNoch keine Bewertungen
- Nejm 2204556Dokument11 SeitenNejm 2204556tommy taylor084Noch keine Bewertungen
- The Nursing ProcessDokument152 SeitenThe Nursing ProcessHyacinth Jane Dela PeñaNoch keine Bewertungen
- The Truth Behind The Polio VaccineDokument28 SeitenThe Truth Behind The Polio VaccineFreedomFighter32100% (2)
- CSH Perspectives Rev - Apolipoprotein E and Apolipoprotein E Receptors - Normal Biology and Roles in ADDokument23 SeitenCSH Perspectives Rev - Apolipoprotein E and Apolipoprotein E Receptors - Normal Biology and Roles in ADGeneziz DiazNoch keine Bewertungen
- 2 4 Di Nitro Chloro BenzeneDokument9 Seiten2 4 Di Nitro Chloro BenzeneKannan NainarNoch keine Bewertungen
- Block Placement Report: Submitted To (Block Placement Coordinator) : MR Bhat IqbalDokument32 SeitenBlock Placement Report: Submitted To (Block Placement Coordinator) : MR Bhat IqbalSherry SherNoch keine Bewertungen
- Vermikompos and Gliocladium Effectiveness Against Fusarium WiltDokument8 SeitenVermikompos and Gliocladium Effectiveness Against Fusarium WiltJioWongMenengNoch keine Bewertungen
- E2870-13 Standard Test Method For Evaluating RelativDokument6 SeitenE2870-13 Standard Test Method For Evaluating RelativA MusaverNoch keine Bewertungen
- ASDAS CalculatorDokument4 SeitenASDAS CalculatorSthepany HuertasNoch keine Bewertungen
- Fundamentals of Epidemiology (EPID 610) Exercise 12 Screening Learning ObjectivesDokument4 SeitenFundamentals of Epidemiology (EPID 610) Exercise 12 Screening Learning Objectiveswelcome martin100% (1)
- SPD 200 RS Disability Comparison TemplateDokument18 SeitenSPD 200 RS Disability Comparison TemplateMUSYOKA KITUKUNoch keine Bewertungen