Beruflich Dokumente
Kultur Dokumente
Neurosyphilis Masquerading As An Acute Adie's Tonic Pupil: Report of A Case
Hochgeladen von
Olvaria MisfaOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Neurosyphilis Masquerading As An Acute Adie's Tonic Pupil: Report of A Case
Hochgeladen von
Olvaria MisfaCopyright:
Verfügbare Formate
Case Rep Ophthalmol 2011;2:205210
DOI: 10.1159/000329704
Published online:
June 28, 2011
2011 S. Karger AG, Basel
ISSN 16632699
www.karger.com/cop
This is an Open Access article licensed under the terms of the Creative Commons AttributionNonCommercial-NoDerivs 3.0 License (www.karger.com/OA-license), applicable to the online
version of the article only. Distribution for non-commercial purposes only.
Neurosyphilis Masquerading as
an Acute Adies Tonic Pupil:
Report of a Case
Gerardo D. Camorianoa, b Jacinthe Kassaba Amar Suchakb
Howard V. Gimbelac
a
c
Gimbel Eye Centre, and b University of Calgary, Calgary, Alta., Canada;
Loma Linda University, Loma Linda, Calif., USA
Key Words
Neurosyphilis Adies tonic pupil Anisocoria
Abstract
We describe the case of a male patient who presented with anisocoria, and was initially
diagnosed with an acute Adies tonic pupil. On subsequent laboratory testing, he was
found to have neurosyphilis. Magnetic resonance imaging demonstrated enhancement
of the right oculomotor nerve. This case underscores the importance of considering this
diagnosis in patients with acute onset internal ophthalmoplegia and hypersensitivity to
dilute pilocarpine, even in the absence of other oculomotor nerve findings.
Case Report
A 39-year-old man presented to our clinic with complaints of an enlarged right pupil of onset 10
days prior. He initially noted a difference in the pupil size while looking at his eyes in the mirror, and
complained of progressively worsening light sensitivity in the right eye. In addition, he described
blurred vision with reading and near work, which improved on covering his right eye. He denied a
recent history of headaches, diplopia, ptosis or blurred vision at distance. He also denied a previous
history of ocular trauma, use of scopolamine patches or recent upper respiratory infection symptoms.
His past medical history was significant only for genital herpes.
On examination, the best-corrected visual acuity was 20/20+2 in the right eye and 20/152 in the left
eye. Ocular motility was full bilaterally, and the patient was orthophoric in primary gaze. The visual
fields were full to confrontation, but on frequency doubling technology (FDT) visual field testing, he
was noted to have an inferior altitudinal defect in the left eye (fig. 1a). The intraocular pressures were 14
mm Hg in both eyes. Anisocoria was present, with the right pupil measuring 7.5 mm and the left pupil 4
mm in the light. In the dark, the right and left pupils measured 8 and 7.5 mm, respectively. Pupils were
also tested on convergence, and measured 6 mm in the right and 3 mm in the left. A sluggish response
was noted on redilation of the right pupil in going from near to distance vision. The patient also had a
small left relative afferent pupillary defect (RAPD) by the reverse RAPD technique. Slit lamp
examination of the anterior segment was within normal limits in both eyes. The anterior chamber was
Gerardo D. Camoriano
Gimbel Eye Centre
450, 493540 Avenue NW
Calgary, AB T3A 2N1 (Canada)
Tel. +1 403 286 3022, E-Mail davidcamoriano @ yahoo.com
205
Case Rep Ophthalmol 2011;2:205210
DOI: 10.1159/000329704
Published online:
June 28, 2011
2011 S. Karger AG, Basel
ISSN 16632699
www.karger.com/cop
deep and quiet bilaterally, and no iris sphincter tears or other signs of previous ocular trauma were
noted in the right eye. No vermiform movements were seen, but an atonic segment was present
inferotemporally in the iris collarette.
Given the clinical picture of anisocoria worse in the light and the tonicity noted in the right pupil on
distance fixation after convergence, pharmacological testing was undertaken with dilute pilocarpine
(fig. 2). A drop of dilute pilocarpine (0.125%) was instilled in each eye, and the pupil sizes were
measured at the same illumination at 5, 15, and 30 min intervals. Reversal of the anisocoria was noted
after 30 min, with the pupils measuring 2.5 and 4 mm in the right and left eyes, respectively. This was
consistent with denervation hypersensitivity of the right pupil and a diagnosis of an acute right Adies
tonic pupil. Homes-Adies syndrome was ruled out on testing of the peripheral reflexes, which were
within normal limits bilaterally.
On dilated fundus examination, superior optic disc pallor was noted in the left eye (fig. 1b). There
was slight cup-to-disc ratio asymmetry (0.3 mm in the right eye and 0.45 mm in the left eye), but the
pallor was out of proportion to the cupping. The disc margins were clear. Associated with this sectoral
disc pallor in the left eye, there was slight attenuation of the superior arcades. The vitreous, macula,
vessels, and periphery were within normal limits in the right eye. On red saturation test, the patient
volunteered having noticed decreased color intensity in the left eye for the last 2 years. However, on
Ishihara pseudoisochromatic plate testing, he was able to correctly identify all plates in both eyes. Based
on these findings in the left eye, an enhanced magnetic resonance imaging (MRI) brain and orbits study
was obtained, which revealed enhancement of the right oculomotor nerve, along its cisternal segment
into the oculomotor cistern of the superior right cavernous sinus (fig. 3). No orbital or intracranial mass
was seen, and there was no evidence of previous demyelinating disease.
Considering the unlikelihood of an Adies tonic pupil in a male patient, his previous history of
genital herpes, and the lack of a viral prodrome or any other cause to justify this diagnosis of exclusion,
rapid plasmin reagent (RPR), venereal disease research laboratory (VDRL), and fluorescent treponemal
antibody (FTA-Abs) tests were ordered. These tests were all positive and the patient was diagnosed with
probable neurosyphilis per Hooshmands criteria [1]. He was referred to the care of an infectious disease
specialist for treatment. A peripherally inserted central catheter was placed, and the patient was treated
with a 3-week course of procaine penicillin G.
Discussion
Our patients presentation was initially consistent with that of an acute Adies tonic
pupil given the decreased light and convergence responses, tonicity after accommodation,
hypersensitivity to dilute pilocarpine, and the inferotemporal atonic iris segment noted in
the right eye. In light of this unusual presentation, the patients right internal
ophthalmoplegia and left optic neuropathy were further investigated. Positive syphilis
serologies clinched the diagnosis, which was confirmed by enhancement of the right
preganglionic oculomotor nerve on MRI. Unfortunately, a lumbar puncture was not done
to confirm cerebrospinal fluid involvement. This was omitted by the infectious disease
specialist as it would not have altered the treatment of the patient. The differential
diagnosis of unilateral internal ophthalmoplegia in a young patient includes ocular or
orbital trauma, uveitis, acute viral illness, cycloplegic medication use, aneurysm (early
posterior communicating artery or internal carotid artery), direct or indirect (i.e. uncal
herniation) compressive oculomotor neuropathy secondary to an orbital or intracranial
mass, Nothnagel syndrome, Miller-Fisher syndrome, leptomeningeal disease, and Adies
tonic pupil. On physical examination, there were no signs of previous trauma or uveitis.
The patient had a left optic neuropathy, but denied a history of previous head trauma, and
no signs of optic nerve atrophy or healed fractures were seen on MRI. He was also asked
about a viral prodrome or history of previous eye infection, which he denied as well.
There was no corneal scarring to suggest previous herpetic ocular involvement. There was
206
Case Rep Ophthalmol 2011;2:205210
DOI: 10.1159/000329704
Published online:
June 28, 2011
2011 S. Karger AG, Basel
ISSN 16632699
www.karger.com/cop
likewise no history of mydriatic medication use, and this was ruled out on pupil
examination. Compression of the oculomotor nerve by an early aneurysm usually results
in subtle ocular motility deficits and/or ptosis, and the presence of an aneurysm was also
effectively ruled out on MRI. Fascicular involvement was not seen clinically or on MRI,
and on neurologic testing the patient did not exhibit ataxia or areflexia. Finally, the
patient did not have a history of malignancy and the right oculomotor nerve
enhancement on MRI was not typical of leptomeningeal disease.
True to its epithet as the great imitator, syphilis may affect almost any part of the eye
and present as an interstitial keratitis, scleritis, uveitis (anterior, intermediate, posterior or
panuveitis), retinal vasculitis, chorioretinitis, optic neuropathy or as a new-onset cranial
nerve palsy [2, 3]. In our case, the only positive findings were a right internal
ophthalmoplegia simulating an acute Adies tonic pupil and a chronic, subacute left optic
neuropathy. On review of the literature, there are several case reports of Adies tonic
pupils on patients with neurosyphilis, in most of which bilateral pupillary involvement
has been described [47]. To our knowledge, this is the second report of unilateral
internal ophthalmoplegia as a presenting sign of neurosyphilis [8]. We believe that only
one pupil was involved due to an early presentation of the disease, as our patient
manifested no other neurological symptoms aside from a mild visual disturbance
associated with a previous left optic neuropathy.
The patients left optic neuropathy may have been related to a self-limited treponemal
infection of the optic nerve or to another process. While retinal arteriolar attenuation has
been associated with syphilitic optic neuropathy, this usually results in a fast decline in
visual acuity [9]. However, other causes are less likely in this young patient, including
glaucoma (degree of cupping was out of proportion to the pallor and the extent of visual
field loss), previous optic neuritis (usually presents with a central or cecocentral scotoma,
and the patient did not have optic nerve enhancement or signs of demyelinating disease
on MRI), nutritional and/or toxic optic neuropathy (a bilateral, albeit asymmetrical
central or cecocentral visual field defect would have been expected), and Leber's
hereditary optic neuropathy (usually results in a fast decline in visual acuity in both eyes,
and diffuse optic disc pallor would have been expected). The patients left inferior
altitudinal visual field defect may have resulted from treponema-induced vasculitis of the
superior branch retinal arteries with subsequent atrophy of the nerve fiber layer in their
distribution.
This case underscores the importance of keeping neurosyphilis in the differential of
patients with unilateral ophthalmoplegia, particularly male patients in which a diagnosis
of an Adie's tonic pupil is three times less likely. A thorough sexual history in these cases
is helpful, but this may not be readily elicited. In these cases, a complete ophthalmic and
neurologic examination should be conducted to rule out other subtle coexisting
pathologies as in the case of our patient. In early cases of neurosyphilis, prompt diagnosis
affords the possibility of a cure, before the onset of the severe vascular, neurologic, and
psychiatric complications that may result in death [1].
Acknowledgements
The authors thank Rick Triebwasser (Gimbel Eye Centre, Calgary, Alta., Canada) and Jocelyn
Miskey (Rockyview Hospital Eye Clinic, Calgary, Alta., Canada) for providing the photographies.
207
Case Rep Ophthalmol 2011;2:205210
DOI: 10.1159/000329704
Published online:
June 28, 2011
2011 S. Karger AG, Basel
ISSN 16632699
www.karger.com/cop
Disclosure Statement
The authors have no proprietary or financial interest concerning products or instruments described.
Fig. 1. Initial FDT visual field and optic disc photographs. a FDT visual field at initial visit shows a left
inferior altitudinal defect. b Superior optic disc pallor in the left eye consistent with the visual field
defect.
208
Case Rep Ophthalmol 2011;2:205210
DOI: 10.1159/000329704
Published online:
June 28, 2011
2011 S. Karger AG, Basel
ISSN 16632699
www.karger.com/cop
Fig. 2. Anisocoria workup repeated 2 weeks after the initial diagnosis of an acute right Adies tonic
pupil. a Pupils in the light. b Pupils on convergence. c Reversal of anisocoria 30 min after instillation of
one drop of dilute pilocarpine (0.125%) in each eye. d Atonic inferotemporal segment of iris in the right
eye (arrows).
209
Case Rep Ophthalmol 2011;2:205210
DOI: 10.1159/000329704
Published online:
June 28, 2011
2011 S. Karger AG, Basel
ISSN 16632699
www.karger.com/cop
Fig. 3. MRI of the brain and orbits. a1a3 Three coronal post-gadolinium magnetization prepared
rapid acquisition gradient echo (MP-RAGE) sequence MR images reveal the abnormal enhancing right
oculomotor nerve between the right superior cerebellar artery and the P1 segment of the right posterior
cerebral artery. b Oblique sagittal view of the enhacing right oculomotor nerve.
References
1
Hooshmand H, Escobar M, Kopf S: Neurosyphilis. A study of 241 patients. JAMA 1972;219:726729.
Aldave AJ, King JA, Cunningham ET: Ocular syphilis. Curr Opin Ophthalmol 2001;12:433441.
Kiss S, Damico FM, Young LH: Ocular manifestations and treatment of syphilis. Semin Ophthalmol
2005;20:161167.
Englestein ES, Ruderman MI, Trojano RA, et al: Dilated tonic pupils in neurosyphilis. J Neurol Neurosurg
Psychiatry 1986;49:14551457.
Fletcher WA, Sharpe JA: Tonic pupils in neurosyphilis. Neurology 1986;36:188192.
Sakai T, Shikishima K, Mizobuci T, et al: Bilateral tonic pupils associated with neurosyphilis. Jpn J Ophthalmol
2003;47:368371.
Yakashi S, Ohshima J, Yonekura J, et al: A case of early syphilis presenting general paresis-like symptoms and
bilateral tonic pupils. Rinsho Shinkeigaku 1992;32:994999.
Zeligs MA, Joseph GF: Unilateral internal ophthalmoplegia: sole clinical sign in patient with syphilitic
meningitis. Arch Neurol Psychiatry 1945;54:389390.
Danesh-Meyer H, Kubis KC, Sergott RC: Not so slowly progressive vision loss. Surv Ophthalmol 1999;44:247
252.
210
Das könnte Ihnen auch gefallen
- Controversies in Neuro-Ophthalmic Management: An Evidence and Case-Based AppraisalVon EverandControversies in Neuro-Ophthalmic Management: An Evidence and Case-Based AppraisalAmanda D. HendersonNoch keine Bewertungen
- Orbital Apex Syndrome With Encephalitis A Rare and Serious Complication of Herpes Zoster Opthalmicus - Ludwig Melino Tjokrovonco 2Dokument12 SeitenOrbital Apex Syndrome With Encephalitis A Rare and Serious Complication of Herpes Zoster Opthalmicus - Ludwig Melino Tjokrovonco 2Handi KrisnaniNoch keine Bewertungen
- Orbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusDokument4 SeitenOrbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusYosiita KartinaaNoch keine Bewertungen
- Herpes Zoster OphthalmicusDokument12 SeitenHerpes Zoster OphthalmicusGio Vano NaihonamNoch keine Bewertungen
- Ni Hms 419332Dokument10 SeitenNi Hms 419332Monica Lauretta Sembiring IINoch keine Bewertungen
- Clinical Diagnosis and Management of Ocular Myasthenia GravisDokument11 SeitenClinical Diagnosis and Management of Ocular Myasthenia GravisAinul NurrahmahNoch keine Bewertungen
- Recurrent Optic Neuritis As A Clinical Manifestation in Multiple Sclerosis A Case Report - Anisa Feby ArifaniDokument11 SeitenRecurrent Optic Neuritis As A Clinical Manifestation in Multiple Sclerosis A Case Report - Anisa Feby Arifanidenny070111209Noch keine Bewertungen
- Atypical Presentation of Optic Neuritis in Multiple Sclerosis - Dian ParamitasariDokument15 SeitenAtypical Presentation of Optic Neuritis in Multiple Sclerosis - Dian ParamitasariGufront MustofaNoch keine Bewertungen
- Neuroretinitis Syphilis in Human Immunodeficiency Virus-Infected PatientDokument6 SeitenNeuroretinitis Syphilis in Human Immunodeficiency Virus-Infected PatientAnindya AgrasidiNoch keine Bewertungen
- Acute Multifocal Placoid Pigment EpitheliopathyDokument8 SeitenAcute Multifocal Placoid Pigment EpitheliopathyremotmNoch keine Bewertungen
- Laporan Kasus NeurooftalmologiDokument12 SeitenLaporan Kasus NeurooftalmologiPradistya Syifa YudiasariNoch keine Bewertungen
- Ocular Myasthenia Gravis in Children A Case Report - Muhammad Arief MunandarDokument10 SeitenOcular Myasthenia Gravis in Children A Case Report - Muhammad Arief Munandarirvan rahmanNoch keine Bewertungen
- HLA B-27 Associated Anterior Uveitis: American Academy of Optometry: Case Report #1Dokument22 SeitenHLA B-27 Associated Anterior Uveitis: American Academy of Optometry: Case Report #1Shabrina Amalia SuciNoch keine Bewertungen
- Esferofauia Aislada y GlaucomaDokument3 SeitenEsferofauia Aislada y GlaucomaManuel VasquezNoch keine Bewertungen
- Acute Retinal Necrosis Following Contralateral Herpes Zoster OphthalmicusDokument4 SeitenAcute Retinal Necrosis Following Contralateral Herpes Zoster Ophthalmicusnurul_sharaswatiNoch keine Bewertungen
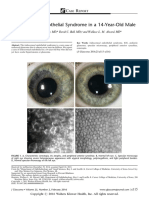
- Iridocorneal Endothelial Syndrome in A 14-Year-Old MaleDokument2 SeitenIridocorneal Endothelial Syndrome in A 14-Year-Old MaleCamiCasasNoch keine Bewertungen
- Clinical CasesDokument49 SeitenClinical Casesnorfitri hadeyNoch keine Bewertungen
- Case Report: Unilateral Optic Neuropathy and Acute Angle-Closure Glaucoma Following Snake EnvenomationDokument5 SeitenCase Report: Unilateral Optic Neuropathy and Acute Angle-Closure Glaucoma Following Snake EnvenomationErnesErlyanaSuryawijayaNoch keine Bewertungen
- American Journal of Ophthalmology Case ReportsDokument3 SeitenAmerican Journal of Ophthalmology Case ReportsElison Jaya PanggaloNoch keine Bewertungen
- Challenging Treatment of Bilateral Multiple Infection Panuveitis in HIV/AIDS PatientsDokument5 SeitenChallenging Treatment of Bilateral Multiple Infection Panuveitis in HIV/AIDS PatientsRosyid PrasetyoNoch keine Bewertungen
- Ophthal Notes PGDokument6 SeitenOphthal Notes PGSwati TyagiNoch keine Bewertungen
- A Case of Angle-Closure Glaucoma, Cataract, Nanophthalmos and Spherophakia in Oculo-Dento-Digital SyndromeDokument3 SeitenA Case of Angle-Closure Glaucoma, Cataract, Nanophthalmos and Spherophakia in Oculo-Dento-Digital SyndromeSriana K. LaliyoNoch keine Bewertungen
- 100255-Article Text-1482-2-10-20220311Dokument6 Seiten100255-Article Text-1482-2-10-20220311Fachry RahmanNoch keine Bewertungen
- Pi Is 0161642099901604Dokument3 SeitenPi Is 0161642099901604Wahyu SholekhuddinNoch keine Bewertungen
- Eye Movement Abnormalities in Stiff Person SyndromeDokument3 SeitenEye Movement Abnormalities in Stiff Person SyndromeEcaterina ChiriacNoch keine Bewertungen
- Goldenhar Syndrome An Ophthalmological Perspective: A Case SeriesDokument6 SeitenGoldenhar Syndrome An Ophthalmological Perspective: A Case SeriesInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Advanced Glaucoma As A Late Manifestation in Axenfeld-Rieger SyndromeDokument9 SeitenAdvanced Glaucoma As A Late Manifestation in Axenfeld-Rieger SyndromeollyNoch keine Bewertungen
- SOAL NO BaruDokument16 SeitenSOAL NO Barukautsar abiyogaNoch keine Bewertungen
- Advanced Glaukoma As A Late Manifestation in Axenfeld-Rieger SyndromeDokument8 SeitenAdvanced Glaukoma As A Late Manifestation in Axenfeld-Rieger SyndromeollyNoch keine Bewertungen
- Neuro-Ophthalmology: Introduction: James Goodwin, MD (Attending)Dokument4 SeitenNeuro-Ophthalmology: Introduction: James Goodwin, MD (Attending)Mariano FioreNoch keine Bewertungen
- Bilateral Atypical Optic Neuritis - Endi Pramudya LaksanaDokument12 SeitenBilateral Atypical Optic Neuritis - Endi Pramudya LaksanaGufront MustofaNoch keine Bewertungen
- Rehabilitative Optometric ManagementDokument5 SeitenRehabilitative Optometric ManagementirijoaNoch keine Bewertungen
- Opth 9 1041Dokument7 SeitenOpth 9 1041petrarizkyNoch keine Bewertungen
- Visual Evoked Potentials in Guillain-Barré Syndrome: MethodsDokument6 SeitenVisual Evoked Potentials in Guillain-Barré Syndrome: MethodsYulianti PurnamasariNoch keine Bewertungen
- Advanced Glaucoma As A Late Manifestation in Axenfeld-Rieger SyndromeDokument9 SeitenAdvanced Glaucoma As A Late Manifestation in Axenfeld-Rieger SyndromeollyNoch keine Bewertungen
- 100122-Article Text-1484-2-10-20220311Dokument11 Seiten100122-Article Text-1484-2-10-20220311muzakiNoch keine Bewertungen
- Ace SetiawanDokument11 SeitenAce SetiawanGlaucoma UnhasNoch keine Bewertungen
- August Morning Rounds HairDokument2 SeitenAugust Morning Rounds HairCristina DumitracheNoch keine Bewertungen
- Traumatic Hyphema: A Teaching Case Report: Priscilla Lenihan, OD Dorothy Hitchmoth, OD, FAAODokument9 SeitenTraumatic Hyphema: A Teaching Case Report: Priscilla Lenihan, OD Dorothy Hitchmoth, OD, FAAOMarshaNoch keine Bewertungen
- (10920684 - Neurosurgical Focus) Mechanisms of Visual Loss in PapilledemaDokument8 Seiten(10920684 - Neurosurgical Focus) Mechanisms of Visual Loss in PapilledemaYusuf BrilliantNoch keine Bewertungen
- Penatalaksanaan Pasien Dengan Sudut Tertutup Primer - DegianaDokument13 SeitenPenatalaksanaan Pasien Dengan Sudut Tertutup Primer - Degianacindy sweeteniaNoch keine Bewertungen
- A Case of Choroidal Neovascularization Secondary To Unilateral Retinal Pigment Epithelium DysgenesisDokument4 SeitenA Case of Choroidal Neovascularization Secondary To Unilateral Retinal Pigment Epithelium DysgenesisdedypurnamaNoch keine Bewertungen
- Secondary Acute Angle Closure Attack As An Initial Presentation of A Novel Type of Systemic Lupus ErythematosusDokument4 SeitenSecondary Acute Angle Closure Attack As An Initial Presentation of A Novel Type of Systemic Lupus ErythematosusPutri kartiniNoch keine Bewertungen
- Taiwan Journal of Ophthalmology: Hui-Chen Cheng, May-Yung Yen, An-Guor WangDokument3 SeitenTaiwan Journal of Ophthalmology: Hui-Chen Cheng, May-Yung Yen, An-Guor WangOmarAlbeshreiNoch keine Bewertungen
- Dong KimberlyDokument7 SeitenDong KimberlyalmaNoch keine Bewertungen
- Penatalaksanaan Glaukoma Sekunder Refrakter Pada Implantasi Lensa Intraokular Bilik Mata Depan - Pauline Meilisa SihiteDokument13 SeitenPenatalaksanaan Glaukoma Sekunder Refrakter Pada Implantasi Lensa Intraokular Bilik Mata Depan - Pauline Meilisa SihiteZikra Herlius14Noch keine Bewertungen
- American Journal of Emergency Medicine: Dietrich Jehle Mary Claire Lark, Clay O'BrienDokument3 SeitenAmerican Journal of Emergency Medicine: Dietrich Jehle Mary Claire Lark, Clay O'BrienGufront MustofaNoch keine Bewertungen
- Case Report: A Case of Type II Bilateral Sturge - Weber SyndromeDokument3 SeitenCase Report: A Case of Type II Bilateral Sturge - Weber SyndromeIOSRjournalNoch keine Bewertungen
- Acknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaDokument3 SeitenAcknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaNisrina FarihaNoch keine Bewertungen
- A Review of Optic NeuritisDokument5 SeitenA Review of Optic NeuritissatrianiNoch keine Bewertungen
- Jnnpsyc00477 0095aDokument1 SeiteJnnpsyc00477 0095aBorj de GuzmanNoch keine Bewertungen
- Abstract in English SWS Edit 3Dokument2 SeitenAbstract in English SWS Edit 3Vania MarissaNoch keine Bewertungen
- An Old Friend Revisited: Chloramphenicol Optic Neuropathy: Case ReportDokument3 SeitenAn Old Friend Revisited: Chloramphenicol Optic Neuropathy: Case ReportckeshavaNoch keine Bewertungen
- Casereport: Vishal Jain, MD, Anagha Deshmukh, MD, Stephen Gollomp, MDDokument4 SeitenCasereport: Vishal Jain, MD, Anagha Deshmukh, MD, Stephen Gollomp, MDlionkingNoch keine Bewertungen
- Panuveitis With Disc Edema After Dengue Fever: A Rare PresentationDokument3 SeitenPanuveitis With Disc Edema After Dengue Fever: A Rare PresentationRio AlexanderNoch keine Bewertungen
- tmp874C TMPDokument9 Seitentmp874C TMPFrontiersNoch keine Bewertungen
- The Nystagmus Blockage Syndrome: Congenital Nystagmus, Manifest Latent Nystagmus, or Doth?Dokument8 SeitenThe Nystagmus Blockage Syndrome: Congenital Nystagmus, Manifest Latent Nystagmus, or Doth?sosoNoch keine Bewertungen
- Jurnal StrabismusDokument3 SeitenJurnal StrabismusBonita AsyigahNoch keine Bewertungen
- Correlation of Visual Field Defects and Optical Coherence Tomography Finding in Migraine PatientsDokument5 SeitenCorrelation of Visual Field Defects and Optical Coherence Tomography Finding in Migraine Patientsmara 11Noch keine Bewertungen
- Clin Auton Res 2011 p55Dokument3 SeitenClin Auton Res 2011 p55Olvaria MisfaNoch keine Bewertungen
- AqqDokument1 SeiteAqqOlvaria MisfaNoch keine Bewertungen
- Tonic Pupil and Corneal Anesthesia After Vitrectomy and Encircling Band For Retinal Detachment in An Ex-Premature ChildDokument5 SeitenTonic Pupil and Corneal Anesthesia After Vitrectomy and Encircling Band For Retinal Detachment in An Ex-Premature ChildOlvaria MisfaNoch keine Bewertungen
- Conduction Block and Tonic Pupils in Charcot-Marie-Tooth Disease Caused by A Myelin Protein Zero p.Ile112Thr MutationDokument4 SeitenConduction Block and Tonic Pupils in Charcot-Marie-Tooth Disease Caused by A Myelin Protein Zero p.Ile112Thr MutationOlvaria MisfaNoch keine Bewertungen
- Rome III CriteriaDokument14 SeitenRome III CriteriaPutu Reza Sandhya PratamaNoch keine Bewertungen
- Effect of Controlled Photopigment On PupilDokument10 SeitenEffect of Controlled Photopigment On PupilOlvaria MisfaNoch keine Bewertungen
- EScholarship UC Item 7293c32tDokument1 SeiteEScholarship UC Item 7293c32tOlvaria MisfaNoch keine Bewertungen
- JDokument5 SeitenJOlvaria MisfaNoch keine Bewertungen
- Rome III CriteriaDokument14 SeitenRome III CriteriaPutu Reza Sandhya PratamaNoch keine Bewertungen
- Review Article: Neurological Disorders in Primary SJ Ogren's SyndromeDokument11 SeitenReview Article: Neurological Disorders in Primary SJ Ogren's SyndromeOlvaria MisfaNoch keine Bewertungen
- Effects of Some Ophthalmic Medications On Pupil Size: A Literature ReviewDokument5 SeitenEffects of Some Ophthalmic Medications On Pupil Size: A Literature ReviewOlvaria MisfaNoch keine Bewertungen
- Curr Opin Neurol 2008 p36Dokument7 SeitenCurr Opin Neurol 2008 p36Olvaria MisfaNoch keine Bewertungen
- Tonic Pupils: Andrew S. Gurwood, Od, Faao and Laura E. Lehn, OdDokument3 SeitenTonic Pupils: Andrew S. Gurwood, Od, Faao and Laura E. Lehn, OdOlvaria MisfaNoch keine Bewertungen
- PDF 29Dokument15 SeitenPDF 29Olvaria MisfaNoch keine Bewertungen
- Nishant Kumar - IEEE - SMC - 2009 - A Novel Approach To Video-Based Pupil TrackingDokument8 SeitenNishant Kumar - IEEE - SMC - 2009 - A Novel Approach To Video-Based Pupil TrackingOlvaria MisfaNoch keine Bewertungen
- Hulsman J Neuro Ophthalmol 2007 p308 PDFDokument2 SeitenHulsman J Neuro Ophthalmol 2007 p308 PDFOlvaria MisfaNoch keine Bewertungen
- Gilzenrat Nieuwenhuis Jepma CohenDokument18 SeitenGilzenrat Nieuwenhuis Jepma CohenOlvaria MisfaNoch keine Bewertungen
- Tonic Pupils: Andrew S. Gurwood, Od, Faao and Laura E. Lehn, OdDokument3 SeitenTonic Pupils: Andrew S. Gurwood, Od, Faao and Laura E. Lehn, OdOlvaria MisfaNoch keine Bewertungen
- Granhom Intro IJP Special IssueDokument14 SeitenGranhom Intro IJP Special IssueOlvaria MisfaNoch keine Bewertungen
- EScholarship UC Item 7293c32tDokument1 SeiteEScholarship UC Item 7293c32tOlvaria MisfaNoch keine Bewertungen
- EScholarship UC Item 7293c32tDokument1 SeiteEScholarship UC Item 7293c32tOlvaria MisfaNoch keine Bewertungen
- Controversies in Neuro OphthalmologyDokument23 SeitenControversies in Neuro OphthalmologyOlvaria MisfaNoch keine Bewertungen
- Joshi Et Al Bimj2010616568CRDokument4 SeitenJoshi Et Al Bimj2010616568CROlvaria MisfaNoch keine Bewertungen
- Goldinger Papesh CDPS 2012Dokument6 SeitenGoldinger Papesh CDPS 2012Olvaria MisfaNoch keine Bewertungen
- J Clin Neurol 2010 p38Dokument3 SeitenJ Clin Neurol 2010 p38Olvaria MisfaNoch keine Bewertungen
- Joshi Et Al Bimj2010616568CRDokument4 SeitenJoshi Et Al Bimj2010616568CROlvaria MisfaNoch keine Bewertungen
- Controversies in Neuro OphthalmologyDokument23 SeitenControversies in Neuro OphthalmologyOlvaria MisfaNoch keine Bewertungen
- Rome III CriteriaDokument14 SeitenRome III CriteriaPutu Reza Sandhya PratamaNoch keine Bewertungen
- BPJ58 IbsDokument12 SeitenBPJ58 IbsOlvaria MisfaNoch keine Bewertungen
- Deworming Latest FormDokument4 SeitenDeworming Latest FormMarianne GonzalesNoch keine Bewertungen
- Infectous DiseaseDokument9 SeitenInfectous DiseasejamikawasNoch keine Bewertungen
- Theories, Models, and FrameworksDokument24 SeitenTheories, Models, and FrameworksLemuel LinoNoch keine Bewertungen
- Locate Us Disclaimer: DSC ClinicDokument2 SeitenLocate Us Disclaimer: DSC ClinichanchiangNoch keine Bewertungen
- List of Medical Professionals-SPADokument8 SeitenList of Medical Professionals-SPANoemí GuzmartNoch keine Bewertungen
- Fractura e FalangsDokument16 SeitenFractura e FalangsJulio Cesar Guillen MoralesNoch keine Bewertungen
- Polymerase Chain ReactionDokument22 SeitenPolymerase Chain ReactionPoornaBasuri100% (1)
- Bear 1000Dokument2 SeitenBear 1000elabsNoch keine Bewertungen
- PsychologyDokument3 SeitenPsychologynylalNoch keine Bewertungen
- Stanley L. Erlandsen Jean E. Magney-Human Histology A Microfiche Atlas Volume 1 Cells and Tissues-University of Minnesota Press (1985)Dokument92 SeitenStanley L. Erlandsen Jean E. Magney-Human Histology A Microfiche Atlas Volume 1 Cells and Tissues-University of Minnesota Press (1985)Rashed HassounNoch keine Bewertungen
- TOC MillerDokument5 SeitenTOC MillerNikhil KumarNoch keine Bewertungen
- Extraction of Primary TeethDokument15 SeitenExtraction of Primary TeethDr. Abdulsalam Awas Dental CenterNoch keine Bewertungen
- 2020 Drug PricesDokument25 Seiten2020 Drug PricesChris-Goldie LorezoNoch keine Bewertungen
- Ki Breathing TranslationDokument52 SeitenKi Breathing TranslationNataly Kur100% (1)
- Medison - Sonoace 8000liveDokument6 SeitenMedison - Sonoace 8000liveJohnatan MonjesNoch keine Bewertungen
- Internal Medicine Case Write Up 1Dokument19 SeitenInternal Medicine Case Write Up 1Ariff Mahdzub100% (1)
- Surgical Sutures-10Dokument25 SeitenSurgical Sutures-10badar_aqNoch keine Bewertungen
- WebinabsDokument336 SeitenWebinabssacin99999Noch keine Bewertungen
- (Lecture) Approach To AscitesDokument48 Seiten(Lecture) Approach To AscitesJirayu Puthhai100% (1)
- Can Oral Sex Cause Throat CancerDokument4 SeitenCan Oral Sex Cause Throat CancerjyuldipNoch keine Bewertungen
- Errors in Cephalometry - WordDokument39 SeitenErrors in Cephalometry - WordSrinivasan BoovaraghavanNoch keine Bewertungen
- COUNSELLLIINNGGGGDokument6 SeitenCOUNSELLLIINNGGGGAnne GarciaNoch keine Bewertungen
- Pharmaceutical IndustryDokument15 SeitenPharmaceutical IndustrySri KanthNoch keine Bewertungen
- Anemia Flow ChartDokument1 SeiteAnemia Flow ChartCynthiaNoch keine Bewertungen
- Study of Lipid Profile in Coronary Heart Disease Patients in LibyaDokument9 SeitenStudy of Lipid Profile in Coronary Heart Disease Patients in LibyaInternational Medical PublisherNoch keine Bewertungen
- Topical Lotion Formulation PDFDokument45 SeitenTopical Lotion Formulation PDFMustafa ArarNoch keine Bewertungen
- Substance Abuse BrochureDokument2 SeitenSubstance Abuse Brochureapi-272566401Noch keine Bewertungen
- Shock Study Guide NursingDokument4 SeitenShock Study Guide NursingKory Christina100% (2)
- Sport InjuriesDokument31 SeitenSport InjuriesKartika Rizky LimNoch keine Bewertungen
- Chemistry in Everyday LifeDokument398 SeitenChemistry in Everyday LifeArsh DhawanNoch keine Bewertungen