Beruflich Dokumente
Kultur Dokumente
Presentasi Kasus GIST
Hochgeladen von
aribfarrasCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Presentasi Kasus GIST
Hochgeladen von
aribfarrasCopyright:
Verfügbare Formate
ARIB FARRAS WAHDAN
Case Presentation
I.
Identity
Name
Age
Gender
Tribe
Occupation
Address
In hospital since
II.
-
: NA
: 13 years old
: Women
: Javenese
:: Kedawung
: Mei 19th 2015
Anamnesis
Main Grievance
Additional Grievance
III.
: Lump in abdomen since 2 months
: Pain in abdomen, nausea
Historical of Present Disease
A girl with her mother came to the Arjawinangun hospital because she felt unwell in
her stomach. There is a lump in the abdomen since 2 months ago. The patient also
feel the pain at abdomen. The patient feels nauseous. The stool was black indicated
that there was blood in her stool. There was palpable mass in her abdomen. And She
had not historical of hipertension.
IV.
Historical of Past Disease
Hipertension (-)
V.
Historical of Family Disease
Hipertension (-)
VI.
Physical Examination
General Status
Present Status
General Condition
Awareness
Blood Pressure
Pulse
Breathing
Temperature
: Moderate
: Composmantis
: 110/70
: 84 x/minute
: 20 x/minute
: 37,5 C
Head
1
ARIB FARRAS WAHDAN
Form
Hair
Eye
: Normal, Simetrical
: Black Colour, No hair fall
: Anemic Conjungtival -/-, Icteric Schlera -/-, Light Refleks (+), Isocor
Ear
Nose
Mouth
pupil right = left
: Normal form, cerumen (-), tympani membrane intac
: Normal form, No septum deviation, epitaction -/: Normal
Neck
Enlargement lymph nodes (-)
Trachea in the middle
No mass
Thoraks
Lungs - pulmonary
Inspection
: The chest shape is symmetrical both of left and right
Palpation
: Fremitus tactile and vocal symmetrical right and left,
crepitus (-), tenderness (-), rebound tenderness (-)
: Sound of resonant in both lung fields
: Sound of vesicular and bronchial the entire lung field, ronkhi -/-,
Percussion
Auscultation
wheezing -/-
Abdomen
Inspection
Palpation
Percussion
Auscultation
Extremity
Upper
Lower
Genitalia
: Lump in abdomen
: Tenderness (-), rebound tenderness (-)
: There was a deaf/somber in abdomen
: Bowel (+)
: Muscle Tone : normal
Movement : aktif / aktif
Mass
:-/Strenght
: 5/5
Edema
:-/: Muscle Tone : normal
Movement : aktif / aktif
Mass
:-/Strenght
: 5/5
Edema
:-/: No abnormalities
Laboratory Examination
Routine Blood
2
ARIB FARRAS WAHDAN
Leukocytes
Hb
Platelets
Hematocrite
: 7790/mm3
: 8,8 gr/dL
: 253.000/mm3
: 25,1 %
Diagnosis
GIST
Differential Diagnosis
Two main differential diagnosis:
1. True gastric leimyoma or leimyosarkoma
2. Schwannoma
General differential diagnostic features of GIST reactive antibodies:
CD117 stains very few other spindled lesions but stains many carcinomas and
melanomas
CD34 stains many spindled lesions but stains almost no carcinomas or
melanomas
DOG1 stains very few spindled lesions or melanomas or carcinomas
Spindled, bland GIST DDx
Leiomyoma
Schwannoma
Fibromatosis
Sclerosing mesenteritis
Inflammatory fibroid polyp
Gastric plexiform fibromyxoma
Solitary fibrous tumor
Inflammatory myofibroblastic tumor
Endometrial stromal sarcoma
Calcifying fibrous pseudotumor
Spindled, malignant GIST DDx
Leiomyosarcoma
Malignant fibrous histiocytoma
Dedifferentiated liposarcoma
Epithelioid GIST
Poorly differentiated carcinoma
Melanoma/clear cell sarcoma
Glomus tumor
Gangliocytic paraganglioma
GI endocrine carcinoma
Extramedullary myeloid tumor
GI mucosal benign epithelioid nerve sheath tumo
Management
Operative
: Laparotomy, Omentectomy, Drainase
Prognosis
Quo ad vitam
: Ad bonam
3
ARIB FARRAS WAHDAN
Quo ad fungsionam
Quo ad sanationam
VII.
: Dubia ad bonam
: Ad Bonam
Literature Review
The Gastrointestinal System
The gastrointestinal (GI) system (or digestive system) processes food for energy and
rids the body of solid waste. After food is chewed and swallowed, it enters the
esophagus, a tube that carries food through the neck and chest to the stomach. The
esophagus joins the stomach just beneath the diaphragm (the thin band of muscle
below the lungs).
The stomach is a sac-like organ that holds food and helps the digestive process by
secreting gastric juice. The food and gastric juices are mixed into a thick fluid
called chyme that is then emptied into the small intestine. The small intestine
continues breaking down the food and absorbs most of the nutrients into the
bloodstream. This is the longest section of the GI tract, measuring more than 20 feet.
The small intestine joins the large intestine, the first part of which is the colon, a
muscular tube about 5 feet long. The colon absorbs water and mineral nutrients from
the remaining food matter. The waste left after this process goes into the rectum as
stool (feces), where it is stored until it passes out of the body through the anus.
Anatomy
Stomach
4
ARIB FARRAS WAHDAN
The stomach a thick walled organ that lies between the esophagus and the first part of
the small intestine (the duodenum). It is on the left side of the abdominal cavity; the
fundus of the stomach lying against the diaphragm. Lying beneath the stomach is the
pancreas. The greater omentum hangs from the greater curvature. A mucous
membrane lines the stomach which contains glands (with chief cells) that secrete
gastric juices, up to three quarts of this digestive fluid is produced daily. The gastric
glands begin secreting before food enters the stomach due to the parasympathetic
impulses of the vagus nerve, making the stomach also a storage vat for that acid. The
secretion of gastric juices occurs in three phases: cephalic, gastric, and intestinal. The
cephalic phase is activated by the smell and taste of food and swallowing. The gastric
phase is activated by the chemical effects of food and the distension of the stomach.
The intestinal phase blocks the effect of the cephalic and gastric phases.
Gastric juice also contains an enzyme named pepsin, which digests proteins,
hydrochloric acid and mucus. Hydrochloric acid causes the stomach to maintain a pH
of about 2, which helps kill off bacteria that comes into the digestive system via food.
The gastric juice is highly acidic with a pH of 1-3. It may cause or compound damage
to the stomach wall or its layer of mucus, causing a peptic ulcer. On the inside of the
stomach there are folds of skin call the gastric rugae. Gastric rugae make the stomach
very extendable, especially after a very big meal. The stomach is divided into four
sections, each of which has different cells and functions. The sections are: 1) Cardiac
region, where the contents of the esophagus empty into the stomach, 2) Fundus,
formed by the upper curvature of the organ, 3) Body, the main central region, and 4)
Pylorus or atrium, the lower section of the organ that facilitates emptying the contents
into the small intestine. Two smooth muscle valves, or sphincters, keep the contents of
the stomach contained. They are the: 1) Cardiac or esophageal sphincter, dividing the
tract above, and 2) Pyloric sphincter, dividing the stomach from the small intestine.
After receiving the bolus(chewed food) the process of peristalsis is started; mixed and
churned with gastric juices the bolus is transformed into a semi-liquid substance
called chyme.
Stomach muscles mix up the food with enzymes and acids to make smaller digestible
pieces. The pyloric sphincter, a walnut shaped muscular tube at the stomach outlet,
keeps chyme in the stomach until it reaches the right consistency to pass into the small
intestine. The food leaves the stomach in small squirts rather than all at once. Water,
alcohol, salt, and simple sugars can be absorbed directly through the stomach wall.
However, most substances in our food need a little more digestion and must travel
into the intestines before they can be absorbed. When the stomach is empty it is about
the size of one fifth of a cup of fluid. When stretched and expanded, it can hold up to
eight cups of food after a big meal.
Gastric Glands
There are many different gastric glands and they secret many different chemicals.
Parietal cells secrete hydrochloric acid; chief cells secrete pepsinogen; goblet cells
secrete mucus; argentaffin cells secrete serotonin and histamine; and G cells secrete
the hormone gastrin.
Vessels and nerves
ARIB FARRAS WAHDAN
Arteries: The arteries supplying the stomach are the left gastric, the right gastric and
right gastroepiploic branches of the hepatic, and the left gastroepiploic and short
gastric branches of the lineal. They supply the muscular coat, ramify in the
submucous coat, and are finally distributed to the mucous membrane.
Capillaries: The arteries break up at the base of the gastric tubules into a plexus of
fine capillaries, which run upward between the tubules, anatomizing with each other,
and ending in a plexus of larger capillaries, which surround the mouths of the tubes,
and also form hexagonal meshes around the ducts.
Veins: From these the veins arise, and pursue a straight course downward, between
the tubules, to the submucous tissue; they end either in the lineal and superior
mesenteric veins, or directly in the portal vein.
Lymphatics: The lymphatics are numerous: They consist of a superficial and a deep
set, and pass to the lymph glands found along the two curvatures of the organ. Nerves:
The nerves are the terminal branches of the right and left urethra and other parts, the
former being distributed upon the back, and the latter upon the front part of the organ.
A great number of branches from the celiac plexus of the sympathetic are also
distributed to it. Nerve plexuses are found in the submucous coat and between the
layers of the muscular coat as in the intestine. From these plexuses fibrils are
distributed to the muscular tissue and the mucous membrane.
Small Intestine
The small intestine is the site where most of the chemical and mechanical digestion is
carried out. Tiny projections called villi line the small intestine which absorbs
digested food into the capillaries. Most of the food absorption takes place in the
jejunum and the ileum. The functions of a small intestine is, the digestion of proteins
into peptides and amino acids principally occurs in the stomach but some also occurs
in the small intestine. Peptides are degraded into amino acids; lipids (fats) are
degraded into fatty acids and glycerol; and carbohydrates are degraded into simple
sugars. The three main sections of the small intestine is The Duodenum, The Jejunum,
The Ileum.
The Duodenum
In anatomy of the digestive system, the duodenum is a hollow jointed tube connecting
the stomach to the jejunum. It is the first and shortest part of the small intestine. It
begins with the duodenal bulb and ends at the ligament of Treitz. The duodenum is
almost entirely retro peritoneal. The duodenum is also where the bile and pancreatic
juices enter the intestine.
The Jejunum
The Jejunum is a part of the small bowel, located between the distal end of duodenum
and the proximal part of ileum. The jejunum and the ileum are suspended by an
extensive mesentery giving the bowel great mobility within the abdomen. The inner
surface of the jejunum, its mucous membrane, is covered in projections called villi,
which increase the surface area of tissue available to absorb nutrients from the gut
contents. It is different from the ileum due to fewer goblet cells and generally lacks
Preyer's patches.
ARIB FARRAS WAHDAN
The Ileum
Its function is to absorb vitamin B12 and bile salts. The wall itself is made up of folds,
each of which has many tiny finger-like projections known as villi, on its surface. In
turn, the epithelial cells which line these villi possess even larger numbers of micro
villi. The cells that line the ileum contain the protease and carbohydrate enzymes
responsible for the final stages of protein and carbohydrate digestion. These enzymes
are present in the cytoplasm of the epithelial cells. The villi contain large numbers of
capillaries which take the amino acids and glucose produced by digestion to the
hepatic portal vein and the liver. The terminal ileum continues to absorb bile salts, and
is also crucial in the absorption of fat-soluble vitamins (Vitamin A, D, E and K). For
fat-soluble vitamin absorption to occur, bile acids must be present.
Large Intestine
The large intestine (colon) extends from the end of the ileum to the anus. It is about 5
feet long, being one-fifth of the whole extent of the intestinal canal. It's caliber is
largest at the commencement at the cecum, and gradually diminishes as far as the
rectum, where there is a dilatation of considerable size just above the anal canal. It
differs from the small intestine in by the greater caliber, more fixed position,
sacculated form, and in possessing certain appendages to its external coat, the
appendices epiploic. Further, its longitudinal muscular fibers do not form a
continuous layer around the gut, but are arranged in three longitudinal bands or tni.
The large intestine is divided into the cecum, colon, rectum, and anal canal. In its
course, describes an arch which surrounds the convolutions of the small intestine. It
commences in the right iliac region, in a dilated part, the cecum. It ascends through
the right lumbar and hypochondriac regions to the under surface of the liver; here it
takes a bend, the right colic flexure, to the left and passes transversely across the
abdomen on the confines of the epigastric and umbilical regions, to the left
hypochondriac region; it then bends again, the left colic flexure, and descends through
the left lumbar and iliac regions to the pelvis, where it forms a bend called the
sigmoid flexure; from this it is continued along the posterior wall of the pelvis to the
anus.
There are trillions of bacteria, yeasts, and parasites living in our intestines, mostly in
the colon. Over 400 species of organisms live in the colon. Most of these are very
helpful to our health, while the minority are harmful. Helpful organisms synthesize
vitamins, like B12, biotin, and vitamin K. They breakdown toxins and stop
proliferation of harmful organisms. They stimulate the immune system and produce
short chain fatty acids (SCFAs) that are required for the health of colon cells and help
prevent colon cancer. There are many beneficial bacteria but some of the most
common and important are Lactobacillus Acidophilus and various species of
Bifidobacterium. These are available as "probiotics" from many sources.
Epidemiology
GISTs represent the most common mesenchymal neoplasms of the GIT. With an
annual incidence of 11-14 per 106 , they form 0.1%-3.0% of gastrointestinal
malignant tumors[5,6]. The median age at diagnosis is 60 years. There is usually no
predilection for either gender but some series suggest a slight male predominance.
7
ARIB FARRAS WAHDAN
GIST occurring in the familial form is autosomal dominant[5-7]. 5% of GISTs occur
in patients with neurofibromatosis type 1 syndrome, occurring mostly in the small
intestine and without KIT mutations. GIST also occurs as a part of Carney triad along
with paraganglioma and pulmonary chordoma in young females[6-9].
Etiology
The exact cause of GIST is unknown. However, 95% of patients with GIST have a
protein called Kit (CD 117) that has become abnormal, which then causes normal
cells to grow faster and become cancerous.
Pathophysiology
GISTs can develop anywhere along the GI tract from the esophagus to the rectum;
however, stomach (60%) and small intestine (30%) are the most common locations
for GIST. Only 10% of GISTs are found in the esophagus, mesentery, omentum, colon
or rectum. Up to 30% of GISTs exhibit high-risk (malignant) behavior such as
metastasis and infiltration[8,9,13,14]. The metastatic pattern is predominantly intraabdominal, with spread throughout the peritoneal cavity and to the liver. Lymph nodal
invasion is uncommon. GISTs with indolent (low-risk) behavior are typically found as
small submucosal lesions. True smooth muscle tumors/leiomyomas also occur
throughout the GI tract but are now thought to be rare in comparison to GISTs, except
in the esophagus where they are more common
Symptoms and Signs
Some patients have no symptoms and their tumors are found accidentally. For
example, some tumors may be found when having testing or surgery for another
reason. However, some people may experience symptoms such as abdominal pain
and/or bloating, bleeding from the bowel, decreased appetite, and/or tiredness.
Only 70% of the patients with GIST are symptomatic. While 20% are asymptomatic
and the tumors are detected incidentally, 10% of the lesions are detected only at
autopsy. Symptoms and signs are not disease specific, they are related more to the site
of the tumor[6,7,16]. Bleeding (30%-40%) comprises the most common symptom
after WJGO|www.wjgnet.com 104 June 15, 2013|Volume 5|Issue 6| vague abdominal
discomfort (60%-70%). Bleeding is attributed to the erosion into the GIT lumen.
Bleeding occurring into the peritoneal cavity due to a ruptured GIST can lead to acute
abdominal pain presenting as a surgical emergency.
Bleeding into the GI tract lumen, causing hematemesis, melena or anemia, is usually
more chronic on presentation. Most of the patients present with vague symptoms,
such as nausea, vomiting, abdominal discomfort, weight loss or early satiety.
Symptoms are usually site specific. These include dysphagia in the esophagus, biliary
8
ARIB FARRAS WAHDAN
obstruction around the ampulla of Vater or even intussusception of the small
bowel[6,7]. Lymph node metastases are uncommon in GIST. Distant metastases most
commonly occur in GISTs of the peritoneum, omentum, mesentery and the liver.
GISTs have a high tendency to seed and hence intraperitoneal or even scar metastases
are known to occur.
Diagnosis
No laboratory test can specifically confirm or rule out the presence of a GIST. The
following tests are generally ordered in the workup of patients who present with
nonspecific abdominal symptoms; abdominal pain; or complications of a GIST-like
hemorrhage, obstruction, or perforation:
Complete blood cell count
Coagulation profile
Serum chemistry studies
BUN and creatinine
Liver function tests, amylase and lipase values
Type, screen, and crossmatch
Serum albumin
Imaging studies
Plain abdominal radiography:
Nonspecific
May be part of an emergent workup
Abnormal gas patterns, including dilated loops of bowel or free extraluminal
air, may be seen with bowel obstruction or perforation
Barium and air (double-contrast) series:
Frequently provides only limited information
Can usually detect GISTs that have grown to a size sufficient to produce
symptoms
Barium swallow for patients with dysphagia
Barium enema for patients with constipation, decreased stool caliber, or
colonic manifestations
9
ARIB FARRAS WAHDAN
GISTs appear as an elevated, sharply demarcated filling defect [1]
The overlying mucosa typically has a smooth contour unless ulceration has
developed
Computed tomography scans of the abdomen and pelvis:
Important in the diagnosis and staging of GISTs
Provides comprehensive information regarding the size and location of the
tumor and its relationship to adjacent structures
Can also be used to detect the presence of multiple tumors and of metastatic spread.
CT characteristics of small GISTs (< 5 cm) are as follows :
Sharply demarcated
Homogeneous density
Mainly exhibit intraluminal growth patterns
CT characteristics of intermediate GISTs (5-10 cm) are as follows :
Irregular shape
Heterogeneous density
An intraluminal and extraluminal growth pattern
Signs of biological aggression, sometimes including adjacent organ infiltration
CT characteristics of large GISTs (>10 cm) are as follows :
Irregular margins
Heterogeneous densities
Locally aggressive behavior
Distant and peritoneal metastases
CT criteria associated with high-grade histology and increased mortality:
Tumor larger than 11.1 cm
Irregular surface contours
Indistinct margins
Adjacent organ invasion
Heterogeneous enhancement
10
ARIB FARRAS WAHDAN
Hepatic or peritoneal metastasis
Magnetic resonance imaging:
Like CT scanning, MRI can depict tumors and yield information about
surrounding structures
Can also be used to detect the presence of multiple tumors and metastases
Less well studied than CT for diagnosing GISTs, but appears equally sensitive
GISTs may appear hypointense on T2-weighted images
Positron emission tomography scanning with 2-[F-18]-fluoro-2-deoxy-D-glucose has
the following uses:
Detection of metastatic disease
Monitoring of response to adjuvant therapy (eg, imatinib mesylate)
Endoscopy:
Frequently performed early in the workup of patients with GI bleeding,
abdominal pain, or GI obstructive symptoms from GISTs
Endoscopic features of GISTs include the suggestion of a smooth submucosal
mass displacing the overlying mucosa
Ulceration or bleeding of the overlying mucosa from pressure necrosis may be
present
Problematic for biopsy specimen collection because of the submucosal
location of GISTs
Endoscopic biopsy results yield a diagnosis in less than 50% of cases
Obtaining a repeat biopsy in the same site as a prior biopsy may increase the
diagnostic yield
Endoscopic ultrasonography (EUS):
Allows localization of lesions and their characterization by ultrasonography
Fine-needle aspiration biopsy specimens may be obtained under sonographic
guidance
GISTs typically appear as a hypoechoic mass in the layer corresponding to the
muscularis propria
Complementary with CT
11
ARIB FARRAS WAHDAN
More accurate than CT in differentiating benign from malignant lesions
Allows a more comprehensive evaluation of the mass and the surrounding
structures than CT
EUS characteristics of malignant GISTs include the following:
Size larger than 4 cm (the only independent predictor)
Heterogeneous echogenicity
Internal cystic areas
Irregular borders on the extraluminal surfaces
EUS features that may help differentiate gastric GISTs from leiomyomas are as
follows:
Inhomogenicity
Hyperechogenic spots
A marginal halo
Higher echogenicity than the surrounding muscle layer
Aspects of EUS-guided biopsy are as follows:
Biopsy provides definitive diagnosis
Biopsy may be required when preoperative therapy is needed in cases where
the tumor is unresectable or only marginally resectable
Biopsy may not be necessary if the tumor is surgically resectable and
preoperative medical therapy is not required
Management
Surgery is the definitive therapy for patients with GISTs, as follows:
Radical and complete surgical extirpation offers the only chance for cure
Surgery is also indicated in symptomatic patients with locally advanced or
metastatic disease
Debulking large lesions is helpful when adjuvant therapy is contemplated
Laparoscopic resection has improved and is a more frequently considered
option
Imatinib mesylate is used in GIST as follows:
12
ARIB FARRAS WAHDAN
Adjuvant therapy post complete surgical resection in patients with high-risk
tumors
Neoadjuvant therapy with the goal of tumor shrinkage prior to surgical
resection
Other tyrosine kinase inhibitors are used when imatinib is not tolerated or is not
effective are as follows:
Sunitinib: Less specific than imatinib; approved as a second-line agent for
advanced GIST
Sorafenib: Investigational second-generation agent
Dasatinib: Investigational second-generation agent
Nilotinib: Investigational second-generation agent
Complication
GIST can complicate unusual locations such as colonic interposition and should be
kept in the differential diagnosis of such unusual presentations.
Prognosis
GIST can transform into malignant on 10 30 % cases. The manifestation of
malignant can be high selularity, local invansion, distant metastases, that normally on
liver and peritoneum. The metastases rarely happens on regional lymph node, lungs,
or bones.
Prognosis becomes worse if there is rupture on tumor, location in distal part, high
selularity, necrosis on tumor, an invansion or other organs metastases and c-kit gen
mutation.
13
ARIB FARRAS WAHDAN
REFFERENCE
American Cancer Society. 2014. Gastrointestinal Stromal Tumor (GIST). Retrieved
from
http://www.cancer.org/acs/groups/cid/documents/webcontent/003103pdf.pdf
Lumongga F. 2008. Gastro Intestinal Stromal Tumor. Departemen Patologi Anatomi
Universitas Sumatera Utara : Medan
Rammohan A., Sathyanesan J., Rajendran K., Pitchaimuthu A., Perumal S., Srinivasan
UP, Ramasamy R., Palaniappan R., Govindan M. A gist of gastrointestinal
stromal tumors: A review. World J Gastrointest Oncol, 5(6), 102-112
Robbins & Cotran. 2009. Dasar Patologis Penyakit edisi 7. EGC : Jakarta
Wengert A., Andybee, Atkin A., Angieatkin, Brentwaldrop, Lenford B., dkk. 2010.
Human Physiology/The gastrointestinal system.
14
Das könnte Ihnen auch gefallen
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- A Detailed Lesson Plan in Science 8: S8LT-Iva-13Dokument11 SeitenA Detailed Lesson Plan in Science 8: S8LT-Iva-13Kiesha Dame Eclipse SaliwanNoch keine Bewertungen
- Animal Structure Ruminant and MonogastricDokument23 SeitenAnimal Structure Ruminant and MonogastricQuinnee VallejosNoch keine Bewertungen
- Clinical Importance of Pittadhara KalaDokument61 SeitenClinical Importance of Pittadhara KalaSwanand Avinash JoshiNoch keine Bewertungen
- Cholel FinalDokument39 SeitenCholel FinalRizza DaleNoch keine Bewertungen
- Drug Absorption Gastrointestinal TractDokument23 SeitenDrug Absorption Gastrointestinal TractJose PerezNoch keine Bewertungen
- Colorectal CancerDokument50 SeitenColorectal CancerHans Chester Rirao Capinding100% (2)
- US of GIT of CattleDokument13 SeitenUS of GIT of CattlesangeetsamratNoch keine Bewertungen
- JejunumDokument3 SeitenJejunumspiraldaoNoch keine Bewertungen
- Anatomy of The Digestive Tube of Toco ToucanDokument11 SeitenAnatomy of The Digestive Tube of Toco ToucanYinneth SakuritaNoch keine Bewertungen
- GRADE 10 HSB End of Year ExamDokument14 SeitenGRADE 10 HSB End of Year ExamCHRISTOPHER SCALE100% (1)
- Profil Saluran PencernaanbroilerDokument9 SeitenProfil Saluran PencernaanbroilerAmalia Firdaus YantiNoch keine Bewertungen
- Liu2013-Influence White-Red SorghumDokument11 SeitenLiu2013-Influence White-Red SorghumOrang GoaNoch keine Bewertungen
- Histology Presentation: Roll Numbers 30-35Dokument25 SeitenHistology Presentation: Roll Numbers 30-35Hamza AhmedNoch keine Bewertungen
- First Week Nutrition For Broiler Chickens Effects-Wageningen University and Research 403639Dokument192 SeitenFirst Week Nutrition For Broiler Chickens Effects-Wageningen University and Research 403639Eduardo ViolaNoch keine Bewertungen
- Anatomy of Digestive SystemDokument20 SeitenAnatomy of Digestive Systemolive jollyNoch keine Bewertungen
- Histology of The Gastrointestinal TractDokument10 SeitenHistology of The Gastrointestinal TractDwi Rezky AmaliaNoch keine Bewertungen
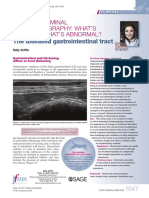
- Feline Abdominal Ultrasonography: What'S Normal? What'S Abnormal?Dokument14 SeitenFeline Abdominal Ultrasonography: What'S Normal? What'S Abnormal?Ветеринарная хирургия Dvm Тозлиян И. А.Noch keine Bewertungen
- Human Digestion PresentationDokument35 SeitenHuman Digestion PresentationYamyang Galay-BañoNoch keine Bewertungen
- The Stomach: Second Phase of Digestion, Following Mastication in The Mouth (Chewing) - It SecretesDokument9 SeitenThe Stomach: Second Phase of Digestion, Following Mastication in The Mouth (Chewing) - It Secretesمحمد العراقيNoch keine Bewertungen
- Promoter Terhadap Pertumbuhan Dan Ukuran Vili Usus Ayam BroilerDokument17 SeitenPromoter Terhadap Pertumbuhan Dan Ukuran Vili Usus Ayam BroilerLatifaNoch keine Bewertungen
- Small IntestineDokument28 SeitenSmall IntestineHusnainAhmedNoch keine Bewertungen
- Small IntestineDokument24 SeitenSmall IntestineMunawwar Mohd AdnanNoch keine Bewertungen
- Palm Kernel Expeller Meal On BroilersDokument8 SeitenPalm Kernel Expeller Meal On BroilersAnand KhandwekarNoch keine Bewertungen
- Structure and Function of The Stomach and IntestineDokument26 SeitenStructure and Function of The Stomach and IntestineMorris KariukiNoch keine Bewertungen
- Histology of Lower GITDokument27 SeitenHistology of Lower GITArwa100% (2)
- Volume 15, Number 2 February 2011Dokument154 SeitenVolume 15, Number 2 February 2011Nicolai BabaliciNoch keine Bewertungen
- Hookworm - Journal - 1 AchmadDokument8 SeitenHookworm - Journal - 1 AchmadFerry KusmalinggaNoch keine Bewertungen
- Intestinal Sodium Glucose Cotransporter 3 Expression Is Epithe - 2021 - Life SciDokument11 SeitenIntestinal Sodium Glucose Cotransporter 3 Expression Is Epithe - 2021 - Life SciPaoloMafaldoNoch keine Bewertungen
- Om Prakash Dinani, Et AlDokument2 SeitenOm Prakash Dinani, Et Alpyushgupta87Noch keine Bewertungen
- Gladwin 2014Dokument5 SeitenGladwin 2014CassiaNoch keine Bewertungen