Beruflich Dokumente
Kultur Dokumente
Clinical Evaluation of Scapular Dysfunction
Hochgeladen von
RudolfGerCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Clinical Evaluation of Scapular Dysfunction
Hochgeladen von
RudolfGerCopyright:
Verfügbare Formate
Clinical Evaluation of Scapular Dysfunction
ERIC L. SAUERS, PhD, ATC, CSCS AT. Still University
Clinical Evaluation
Ocapular dysfunction has been widely
implicated as a contributing factor to
shoulder pathology. Thus, evaluations of
scapular motion and strength have been
described as key components of a comprehensive shoulder examination. Some
methods for evaluating scapular function,
however, might not yield sufficient information from which to
make an informed clinKEY P O I N T S
ical decision regarding
Scapular evaluation should include repetiappropriate interventive loading of the scapula muscles.
tions. Traditional evaluation of the scapula
Soft-tissue mobility assessment of the
has often been limited
shoulder is an important aspect of scapular
to nothing more then
evaluation.
having patients raise
and lower their arms
Scapular special tests include the scapularfor several repetitions.
assistance test and the scapular-retraction
Unfortunately, observatest.
tion during unweighted
arm
elevation is often
Key Words: shoulder, dyskinesis, clasinsufficient to detect
sification
scapular dysfunction
because it fails to load and challenge the
scapulothoracic musculature.' Three-dimensional measurement of scapular kinematics
has provided a great deal of information
regarding normal and abnormal scapular
function, but these methods are not readily
available or practical in the clinical setting.
Determining appropriate clinical tests to
evaluate scapular dysfunction can be a
challenge. Therefore, the objective of this
article is to present methods for evaluating scapular dysfunction that will help
clinicians develop an appropriate course
of intervention.
Visualization
Evaluation of the scapula requires full visualization of the posterior thorax and both
scapulae. This can be achieved by having
male athletes remove their shirts and by
appropriately draping female athletes in
gowns tied at the neck and waist or having
them wear swimsuit tops or sport bras that
do not cover (thereby possibly stabilizing)
the scapula (Figure 1). Comprehensive evaluation of the scapula includes observation of
scapular motion to detect scapular dyskinesis
(aberrant scapular motion or winging).
I Weighted bilateral shoulder-flexion testing to
evaluate scapular motion.
Z006NumanKinetks-ATT 11(5). pp.l
10 1 SEPTEMBER 2 0 0 6
ATHLETIC THERAPY TODAY
Classification Protocols
Manual Muscle Testing
Several investigators''^ have reported on the development of scapular-assessment protocols that incorporate specific tests designed to load and challenge the
periscapular musculature in order to detect and classify movement dysfunction-Johnson et al.^ developed
a protocol that was later refined and used to evaluate
27 patients with active shoulder pathology (N = 32),'
Their data indicated that three simple clinical tests
should be performed to detect abnormal scapular
motion: (a) observation of bilateral scapular motion
during multiple repetitions (5-10) of unweighted
humeral elevation in the scapular plane to establish a
baseline of scapular movement, (b) observation of bilateral scapular motion during multiple repetitions (5-! 0)
of weighted (0.5-5 kg [I-10 lb]) shoulder flexion, and
(c) observation of scapular motion during performance
of resisted isometric external rotation with the arm at
the side in neutral rotation (scapular flip sign^). It is
important to note that an adequate amount of weight
should be chosen to load the scapular musculature but
not exacerbate shoulder pain.
Several scapular-classification protocols have
evolved from the work of Johnson et al.,^ and each
consists of similar test components that include
unweighted and weighted flexion and abduction and
the scapular flip sign.''^"*"^ Collectively these tests appear
to demonstrate acceptable intrarater' and interrater'-^'^
reliability and percentage agreement. '"'^ A positive test
for abnormal scapular motion with weighted flexion
has been shown to be a valid indicator of abnormal
scapular motion compared with three-dimensional
kinematic measures.'*
Of all of the tests reported, weighted shoulder
flexion has consistently been identified as the single
clinical test most highly associated with abnormal
scapular motion (Figure 1 ).''''^ Johnson etal.' reported
that weighted flexion and the scapular flip sign identified 100% of visible scapular-motion abnormalities.'
Gard et al.*' reported that weighted flexion identified the
most scapular-motion abnormalities (48/50), followed
by unweighted flexion (43/50). with lower values for
weighted (34/50) and unweighted abduction (29/50)
and resisted external rotation at neutral elevation
(scapular flip sign; 23/50). It is important to note that
the diagnostic value (accuracy, sensitivity, specificity,
and positive and negative predictive value) of these
tests in isolation, or as part of a classification protocol,
remains to be demonstrated.
In addition to scapular-motion assessment, a thorough
assessment of muscle strength should be performed
using graded manual muscle tests^ for the scapulastabilizing muscles including the serratus anterior,
rhomboids, and middle, upper, and lower trapezius.
These muscles are the primary scapular stabilizers,
and changes in their strength have been implicated in
altered scapular kinematics and subacromial impingement."*" Michener et al.'^ have demonstrated that a
single clinician can reliably assess these muscles using
a handiield dynamometer in patients with pain and
functional loss.
ATHLETIC THERAPY TODAY
Scapular Special Tests
The addition of scapular special tests including the
scapular-assistance test and scapular-retraction test
might prove useful in trying to determine whether
scapular-motion abnormalities are contributing to a
patient's symptoms. The scapular-assistance test is
performed by manually stabilizing the scapula on the
thorax and assisting the inferomedial border in rotating
in a stable and coordinated fashion while the patient
raises his or her arm (Figure 2),'^'"' A positive test is
when the patient reports a reduction of symptoms
I Scapular-assistance test.
SEPTEMBER 2006 I 11
while you are manually stabilizing and assisting the
scapula through a full range of motion.
The scapular-retraction test is another special test
that can be performed to assess the contribution of
the scapulothoracic articulation to impairments such
as pain and muscle weakness.'"^ The test is performed
by manual and patient-assisted retraction and stabilization of the scapula on the thorax (Figure 3). I prefer
to then have the patient move through a full range of
motion to assess any change in symptoms with manual
scapular stabilization. The scapular-retraction test has
been described as a test to assess the contribution of
scapular stability to muscle-force output. '^ The athlete
begins the test by performing a traditional empty-can
test with no scapular retraction or stabilization. The
scapula is then retracted and manually stabilized,
and the test is repeated. If the patient demonstrates
greater strength during retesting with the scapula in
the retracted and stabilized position, the test is considered positive.
The scapular-assistance and scapular-retraction
tests are both designed to stabilize and position the
scapula on the thorax. Diminished pain or increased
muscle strength during these tests suggests that abnormal scapular control is contributing to the patient's
symptoms, and rehabilitative interventions should be
implemented to restore scapular stability and motor
control. '* The diagnostic value of these tests, however,
remains to be demonstrated.
Soft-Tissue Mobility Assessment
Other useful adjuncts to clinical evaluation of the scapula include various tests of soft-tissue mobility about
the shoulder. Soft-tissue restrictions such as decreased
posterior shoulder mobility or increased pectoralisminor tightness can lead to alterations in scapular
kinematics, including reduced posterior tilting, upward
rotation, or external rotation during arm elevation.^''"'^
Posterior-capsuie or rotator-cuff tightness can be evaluated by measuring passive isolated glenohumeral-joint
internal rotation or cross-body horizontal adduction."*
Pectoraiis-minor tightness can be evaluated by measuring, with the patient supine, from the treatment
table to the posterior acromion. Wang et al.''' recently
determined that, with the patient supine on a treatment table, a linear distance between the posterior
acromion and the surface of the table of less than 2.5
cm is indicative of a short pectoralis minor.
Postural Assessment
Forward head posture, forward shoulder posture,
and thoracic kyphosis should be assessed as part of
any scapular evaluation.^'^^ Collectively, this triad of
impairments has been widely implicated in shoulder
dysfunction.^"^' Patients with spinal posture changes
indicative of forward head and shoulder posture and
thoracic kyphosis, such as increased cervical extension
and thoracic flexion, demonstrate altered scapular
kinematics consistent with subacromial impingement.^^" These postural malalignments are suspected
to inhibit scapular posterior tilt and external rotation
during arm elevation, thereby compromising the subacromial space. A quick and efficient postural screen
for forward head posture, forward shoulder posture,
and thoracic kyphosis can be accomplished using the
side-view plumb-line screen {Figure 4)."
Intervention Implications
figure 3 scapular-retraction test.
12 1 SEPTEMBER 2006
Patients with identifiable scapular impairments should
receive specific interventions to restore neuromuscular control, strength, and soft-tissue mobility and to
address postural malalignments. Treatment interventions for scapular dysfunction should be based on
specific clinical-examination findings. For instance,
two patients with subacromial-impingement syndrome
might have differing scapular contributions to their
pain and dysfunction that require different treatment
strategies. One patient might demonstrate scapular
ATHLETIC THERAPY TODAY
have been given higher priority based on the physical
examination.
Alterations in scapular kinematics in the presence
of shoulder pathology have been well demonstrated. "'^'*
Visible scapular-motion abnormalities might be more
common, however, in cases of long-standing or more
severe shoulder pathology' or in patients with nerve
injury.^^ Furthermore, the evidence suggests that visible
scapular-motion abnormalities are more prevalent in
patients with the specific diagnoses of shoulder instability and shoulder-impingement syndrome.'-^^
Proximal stability and neuromuscular control of
the scapula are critical to distal mobility and function
of the arm. A thorough and systematic evaluation of
the scapula to determine scapular-motion quantity and
quality, scapular-positioning contribution to pain and
strength, scapular-muscle strength, soft-tissue mobility,
and spinal posture should be central to every examination of the shoulder. This evaluation will help identify
specific impairments that might be contributing to
functional loss and disability and will serve to establish
clear priorities for treatment intervention. Nonetheless,
the prognostic value of scapular dysfunction in relation
to normal, pain-free shoulder function remains unclear.
More research is needed to evaluate the diagnostic and
prognostic value of scapular tests in specific patient
populations with well-defined shoulder pathology.
fiqure 4 postural assessment using the side-view plumb-line screen.
Clinical-Cvaluation Summary
dyskinesis and scapular-muscle weakness that are
leading to altered scapular kinematics (decreased
posterior tilt, external rotation, and upward rotation).
This patient would probably benefit most from a thorough scapular-stabilization and neuromuscular-control
rehabilitation program. The other patient might exhibit
coordinated and stable scapular motion but exhibit
significant pectoraiis-minor and posterior-capsule or
-cuff tightness in addition to forward shoulder posture
and thoracic kyphosis that are contributing to altered
scapular kinematics (decreased posterior tilt, external
rotation, and upward rotation). This patient would most
likely benefit from specific manual therapies aimed
at restoring soft-tissue mobility and thoracic extension coupled with strengthening exercises to promote
thoracic extension and scapular retraction. Patients
with negative scapular-examination findings should
still receive core scapular-stabilization exercises, but
these might be adjunctive to other interventions that
ATHLETIC THERAPY TODAY
1. The examiner must expose the posterior thorax
and scapulae by having male patients remove their
shirts or by draping female patients with a gown.
2. Visible observation of scapular-movement dysfunction usually requires that you repetitively challenge
the scapula under loaded conditions.
3. Clinical evaluation of the scapula should consist of
the following examination techniques:
a. Observation of bilateral scapular motion during
multiple repetitions (5-10) of unweighted shoulder flexion to determine a baseline.
b. Observation of bilateral scapular motion during
multiple repetitions (5-10) of weighted (0.5-5
kg [1-10 lb]) shoulder flexion.
c. Observation of scapular motion during performance of resisted isometric external rotation
SEPTEMBER 2006 I 13
with the arm at the side in neutral rotation
(scapular flip sign).
9. Kendall F, McCreary E, Provance P, Rodgers M, Romani W. Muscles:
Testing and Function With Posture and Pain. Baltimore, Md: Lippincott
Williams SWilkins: 2005
d. Manual muscle testing of the scapular-stabilizing muscles (serratus anterior, rhomboids, and
middle, upper, and lower trapezius).
10. LudewigPM, Cook TM. Alterations in shoulder kinematics and associated muscle activity in people with symptoms of shoulder impingement. Phys Ther. 2000;80(3):276-291.
e. Performance of the manual scapular-assistance
test and scapular-retraction test to determine the
contribution of scapular dysfunction to shoulder
symptoms.
f. Evaluation of specific soft-tissue mobility patterns such as posterior-capsule or rotator-cuff
hypomobility and pectoraiis-minor tightness.
g. Screening for forward head posture, forward
shoulder posture, and thoracic kyphosis using
a side-view plumb line.
4. A thorough clinical evaluation of the scapula that
demonstrates specific impairments (e.g., dyskinesis and hypomobility) should be used to determine
specific treatment interventions (e.g., strengthening and mobilization).
5. Further research into the diagnostic and prognostic
value of clinical tests to evaluate scapular dysfunction is needed. I
References
1. Johnson MP. van den Heuvel V, Sauers EL. Reliability of a classification protocol for the assessment of scapular motion in patients with
shoulder pathology. Paper presented at: 1st International Congress
of Shoulder and Elbow Therapists; 2004; Washington DC.
2. Johnson MP, Addesi S, Ebaugh DD. Development of a model to classify scapular motion: a pilot study Paper presented at: Meeting of the
Pennsylvania Physical Therapy Association; 2001: Harrisburg. Pa.
3. Kibier WB. Uhl TL. Maddux jWQ, Brooks PV, Zeller B. McMullen j .
Qualitative clinical evaluation of scapular dysfunction: a reliability
smdy. J Shoulder Elbow Surg. 2003; 11 (6):550-556.
4. T^te AR, McClure P, NeffN. Validation of a visual classification system
for scapular moiion dysfunction [abstract].y Orthop Sports Phys Ther.
2004;34|l) A42
5. Gard K, Ebaugh DD, Bilgin S, Sakaitis C. Interrater reliability of a
proposed scapular classification system [abstract]. _/ Orthop Sports
Phys Ther. 2005\35{\y.A7.
6. Gard K, FinocchiaroJ, Ebaugh DD, Interrater reliability of a proposed
scapular classification system [abstract]. J Orthop Sports Phys Ther.
2006;36(l):A10,
11. Tsai NT McClure PW, Karduna AR. Effects of muscle fatigue
on 3-dimensional scapular kinematics. Arch Phys Med Rehabil.
2003:84(7):1000-]005.
12. Michener LA, Boardman ND, Pidcoe PE, Frith AM. Scapular muscle
tests in subjects with shoulder pain and functional loss: reliability and
construct validity. Phys Ther. 2005;85(ll):li28-]138.
13 Kibler WB, Livingston B. Closed-chain rehabilitation for upper and
lower extremities. J ^ m Acad Orthop Surg. 2001 ;9(6):412-421.
14. Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder:
spectrum of pathology part III: the SICK scapula, scapular dyskinesis,
the kinetic chain, and rehabilitation. Arthroscopy. 2003;l9(6):64l661.
I 5. Kibier WB, McMullen J. Scapular dyskinesis and its relation to shoulder
pain. J Am Acad Orthop Surg. 2003; 11 (2): 142-151.
16. Borich M, Bright J, Loreilo D, Cieminski C, Buisman T. Ludewig PM.
Scapular motion alterations in cases of glenohumeral internal rotation
deficit [abstract].]Orthop Sports Phys Ther. 2006;36(l):A3l.
17. Borstad JD, Ludewig PM. The effect of long versus short pectoralis
minor resting length on scapular kinematics in healthy individuals.y
Orthop Sports Phys Ther. 2005;35(4):227-238.
18. Tyler TF, Roy T Nicholas SJ, Gleim GW Reliability and validity of a new
method of measuring posterior shoulder tightness, y Orthop Sports
Phys Ther. 1999;29(5):262-269, discussion 270-274.
19. Wang S, Trudell-Jackson E. Tossey L, Vo W, Theriault T Effectiveness
of two physical therapy interventions for increasing length in the pectoralis minor muscle [abstract] y Orthop Sports Phys Ther. 2006;36( I):
All.
20. Lewis JS, Green A, Wright C. Subacromial impingement syndrome:
the role of posture and muscle imbalance J Shoulder Elbow Surg.
2005;14(4):385-392.
21. Michener LA, McClure PW, Karduna AR. Anatomical and biomechanical mechanisms of subacromial impingement syndrome. Clin Biomech
(Bristol. Avon). 2003;i8(5):369-379.
22. Wang CH, McClure P, Pratt NE, Nobilini R. Stretching and strengthening exercises: their effect on three-dimensional scapular kinematics.
Arch Phys Med Rehabil. 1999;80(8):923-929
23. Finley MA, Lee RY. Effect of sitting posture on 3-dimensional scapular
kinematics measured by skin-mounted electromagnetic tracking sensors. Arch Phys Med Rehabil. 2003;84(4):563-568.
24. Lukasiewicz AC, McClure P, Michener L, Pratt N, SennettB. Comparison
of 3-dimensional scapular position and orientation between subjects
with and without shoulder impingement.y Orfftop Sports Phys Ther.
l999:29(10):574-583, discussion 584-586.
25. KuhnJE, PlancherKD, Hawkins RJ. Scapu]ar winging. J Am Acad Orthop
Surg. l995;3(6):319-325.
26. Warner JJ, Micheli LJ, Arslanian LE. Kennedy J, Kennedy R. Scapulothoracic motion in normal shoulders and shoulders with glenohumeral instability and impingement syndrome, a study using moire
topographic analysis. Ciin Orthop. 1992;285(199): 191 -199.
7. McClure PW. Tate AR. Egner MC, Greenberg EM, Yops RM, Neff NP
Development and interrater reliability testing of a system of classification for scapular dysfunction {absiraa]. J Orthop Sports Phys Ther.
2OO3;33(2):A23.
8. Kelly MJ, Brenneman SK. An examination sign to identify the presence
of a spinal accessory nerve palsy [abstract] .J Orthop Sports Phys Ther.
2000:30(1) A27,
14 1 SEPTEMBER 2006
Eric Sauers is an associate professor and director of the athletic training
program, as well as chair of the Department of Interdisciplinary Health
Sciences, at Arizona School of Health Sciences, A.T. Still University,
ATHLETIC THERAPY TODAY
Das könnte Ihnen auch gefallen
- Effect of Knee Position On Hip and Knee Torques During The Barbell SquatDokument5 SeitenEffect of Knee Position On Hip and Knee Torques During The Barbell SquatMattNoch keine Bewertungen
- 2 Biomechanics of The ShoulderDokument47 Seiten2 Biomechanics of The ShoulderDaniel PereiraNoch keine Bewertungen
- Overhead Throwing: Biomechanics and PathologyDokument7 SeitenOverhead Throwing: Biomechanics and Pathologyrapannika100% (1)
- The Role of Core StabilityDokument11 SeitenThe Role of Core StabilitykevintriyaNoch keine Bewertungen
- The Pain and Movement Reasoning ModelDokument7 SeitenThe Pain and Movement Reasoning ModelRamiro Avendaño Rebolledo100% (1)
- (OS 203) Basic Biomechanics of Musculoskeletal System PDFDokument3 Seiten(OS 203) Basic Biomechanics of Musculoskeletal System PDFSham David PTNoch keine Bewertungen
- A Kinetic Chain Approach For Shoulder RehabDokument9 SeitenA Kinetic Chain Approach For Shoulder RehabRicardo QuezadaNoch keine Bewertungen
- Kaltenborn 1993Dokument5 SeitenKaltenborn 1993hari vijayNoch keine Bewertungen
- Effects of Petrissage Massage On Fatigue and ExercDokument8 SeitenEffects of Petrissage Massage On Fatigue and ExercJGRBBKDVRNoch keine Bewertungen
- Phasic Activity of Intrinsic Muscles of The FootDokument14 SeitenPhasic Activity of Intrinsic Muscles of The FootpetcudanielNoch keine Bewertungen
- The Effects of Scapular Stabilization Based Exercise Therapy On PDFDokument15 SeitenThe Effects of Scapular Stabilization Based Exercise Therapy On PDFElisabete SilvaNoch keine Bewertungen
- MMT of CervicalDokument18 SeitenMMT of Cervicalsirms swatNoch keine Bewertungen
- 1.1 Musculoskeletal Care Modalities PDFDokument20 Seiten1.1 Musculoskeletal Care Modalities PDFDiana CalderonNoch keine Bewertungen
- The Convex Concave Rule and The Lever LawDokument4 SeitenThe Convex Concave Rule and The Lever LawOwais KhanNoch keine Bewertungen
- Sports Injuries Diagnosis and Management Fo PDFDokument2 SeitenSports Injuries Diagnosis and Management Fo PDFKahinyaNoch keine Bewertungen
- Ijspt-Biomechanics and Pathomechanics of The Patellofemoral JointDokument11 SeitenIjspt-Biomechanics and Pathomechanics of The Patellofemoral JointDevi MigiekaNoch keine Bewertungen
- BiomechanicsDokument17 SeitenBiomechanicss_chandrubioNoch keine Bewertungen
- Knee Injuries Part 1Dokument38 SeitenKnee Injuries Part 1meenoNoch keine Bewertungen
- Manual Muscle TestingDokument13 SeitenManual Muscle TestingPásztai ZoltánNoch keine Bewertungen
- Tendon Neuroplastic TrainingDokument9 SeitenTendon Neuroplastic TrainingLara VitorNoch keine Bewertungen
- Introduction To Theraputic ExerciseDokument27 SeitenIntroduction To Theraputic ExerciseArun Tamilvanan100% (2)
- Transverse Rotation of The Segments of The Lower Extremity in LocomotionDokument15 SeitenTransverse Rotation of The Segments of The Lower Extremity in Locomotionpetcudaniel100% (1)
- Bio Mechanics and Pathomechanics of Ankle JointDokument35 SeitenBio Mechanics and Pathomechanics of Ankle Joint56 Vignesh j 079Noch keine Bewertungen
- Knee Biomechanics: by Amrita..Dokument57 SeitenKnee Biomechanics: by Amrita..Chanda NathaniNoch keine Bewertungen
- Knee Biomechanics: Mark Arthur Martinez Trauma 1 April 5, 2018Dokument7 SeitenKnee Biomechanics: Mark Arthur Martinez Trauma 1 April 5, 2018Juan Alvaro EstradaNoch keine Bewertungen
- Functional Exercise ProgressionDokument6 SeitenFunctional Exercise ProgressionAnastasia Skamagki100% (1)
- Effectiveness of Mulligan's Mobilization Technique Versus Eccentric Exercises On Pain, Hand Grip Strength and Function in Subjects With Lateral EpicondylitisDokument8 SeitenEffectiveness of Mulligan's Mobilization Technique Versus Eccentric Exercises On Pain, Hand Grip Strength and Function in Subjects With Lateral EpicondylitisInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Rehabilitation of Scoliosis - Solo Final 6-10Dokument30 SeitenRehabilitation of Scoliosis - Solo Final 6-10Hanna RikaswaniNoch keine Bewertungen
- Distal Biceps Repair Rehabilitation Protocol by Tendayi MutsopotsiDokument5 SeitenDistal Biceps Repair Rehabilitation Protocol by Tendayi MutsopotsiPhysiotherapy Care SpecialistsNoch keine Bewertungen
- Staged Approach For Rehabilitation ClassificationDokument10 SeitenStaged Approach For Rehabilitation ClassificationCambriaChicoNoch keine Bewertungen
- Plug in GaitDokument70 SeitenPlug in GaitJobin VargheseNoch keine Bewertungen
- Basic of Geriatrics and Internal Medicine For PhysiotherapistDokument128 SeitenBasic of Geriatrics and Internal Medicine For PhysiotherapistDoha EbedNoch keine Bewertungen
- Mulligan Spinal Concept PDFDokument7 SeitenMulligan Spinal Concept PDFRabbeya AltafNoch keine Bewertungen
- Walking Aids KinesiologyDokument26 SeitenWalking Aids Kinesiologyfarwafurqan1Noch keine Bewertungen
- Appendix: Motor Control Training Intervention ManualDokument32 SeitenAppendix: Motor Control Training Intervention Manualgonchodiaz1703Noch keine Bewertungen
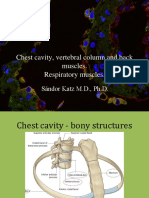
- Chest Cavity, Vertebral Column and Back Muscles. Respiratory MusclesDokument35 SeitenChest Cavity, Vertebral Column and Back Muscles. Respiratory MusclesOr100% (2)
- Shoulder Special TestsDokument36 SeitenShoulder Special TestsNidal HusseinNoch keine Bewertungen
- Musculosketal Imaging in Physical TherapyDokument14 SeitenMusculosketal Imaging in Physical TherapyWasemBhatNoch keine Bewertungen
- Biomechanics NotesDokument5 SeitenBiomechanics Notesjttizzle1995Noch keine Bewertungen
- Clinical Neurodynamics and Sports Medicine: Origins and DevelopmentDokument8 SeitenClinical Neurodynamics and Sports Medicine: Origins and DevelopmentWahid NasrudinNoch keine Bewertungen
- 14 Biomechanics of Normal Human Gait PDFDokument26 Seiten14 Biomechanics of Normal Human Gait PDFDiego A. MezaNoch keine Bewertungen
- PathomechanicsDokument8 SeitenPathomechanicsMike B AndersonNoch keine Bewertungen
- FroDokument5 SeitenFrochinmayghaisasNoch keine Bewertungen
- 52 Page PDF PF PPT Neurophysiological Effects of Spinal Manual Therapy in The Upper Extremity - ChuDokument52 Seiten52 Page PDF PF PPT Neurophysiological Effects of Spinal Manual Therapy in The Upper Extremity - ChuDenise MathreNoch keine Bewertungen
- Kibler Scapular DyskinesisDokument10 SeitenKibler Scapular Dyskinesisנתנאל מושקוביץ100% (5)
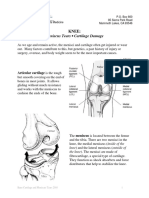
- Meniscus Tears - Cartilage Damage: KneeDokument9 SeitenMeniscus Tears - Cartilage Damage: KneedheenadayalanNoch keine Bewertungen
- Baseline Bubble Inclinometer User ManualDokument2 SeitenBaseline Bubble Inclinometer User Manualphcproducts100% (2)
- Godman - 1824 - Fascia of The Human BodyDokument27 SeitenGodman - 1824 - Fascia of The Human BodyDustin LimaNoch keine Bewertungen
- The Effect of Closed Kinetic Chain Exercises And.14Dokument7 SeitenThe Effect of Closed Kinetic Chain Exercises And.14fgomez235Noch keine Bewertungen
- Acl Rehab ProgrammeDokument8 SeitenAcl Rehab ProgrammePengintaiNoch keine Bewertungen
- Scientific Research Journal of India (SRJI) Vol - 2, Issue - 1, Year - 2013Dokument59 SeitenScientific Research Journal of India (SRJI) Vol - 2, Issue - 1, Year - 2013Dr. Krishna N. SharmaNoch keine Bewertungen
- Scapula DyskinesiaDokument5 SeitenScapula Dyskinesiamiguelax1Noch keine Bewertungen
- Bogduk 2009Dokument3 SeitenBogduk 2009Borys100% (1)
- Normal Biomechanics of Human Movement Sit To StandDokument4 SeitenNormal Biomechanics of Human Movement Sit To StandTafzz Sailo100% (1)
- Kinetic Control Cap1Dokument17 SeitenKinetic Control Cap1Yennifer Serna MoncadaNoch keine Bewertungen
- Subacromial Impingement Syndrome and Rotator Cuff Tendinopathy: The Dilemma of DiagnosisDokument4 SeitenSubacromial Impingement Syndrome and Rotator Cuff Tendinopathy: The Dilemma of DiagnosisTomBramboNoch keine Bewertungen
- Lumbar Stability PDFDokument9 SeitenLumbar Stability PDFPablo EstebanNoch keine Bewertungen
- VNG CB en Rev02 - HDDokument5 SeitenVNG CB en Rev02 - HDRudolfGerNoch keine Bewertungen
- Prevention & Early Outpatient Treatment Protocol For Covid-19Dokument3 SeitenPrevention & Early Outpatient Treatment Protocol For Covid-19jjoyner777Noch keine Bewertungen
- Effect of Spatial Orientation of The Horizontal Semicircular Canal On The Vestibulo-Ocular ReflexDokument8 SeitenEffect of Spatial Orientation of The Horizontal Semicircular Canal On The Vestibulo-Ocular ReflexRudolfGerNoch keine Bewertungen
- Analysis of Persistent Geotropic and Apogeotropic Positional Nystagmus of The Lateral Canal Benign Paroxysmal Positional VertigoDokument6 SeitenAnalysis of Persistent Geotropic and Apogeotropic Positional Nystagmus of The Lateral Canal Benign Paroxysmal Positional VertigoRudolfGerNoch keine Bewertungen
- Latest Statistics On England Mortality Data Suggest Systematic Mis-Categorisation of Vaccine Status and Uncertain Effectiveness of Covid-19Dokument24 SeitenLatest Statistics On England Mortality Data Suggest Systematic Mis-Categorisation of Vaccine Status and Uncertain Effectiveness of Covid-19RudolfGerNoch keine Bewertungen
- Severity of SARS-CoV-2 Reinfections As ComparedDokument3 SeitenSeverity of SARS-CoV-2 Reinfections As ComparedRudolfGerNoch keine Bewertungen
- Abnormal Cancellation of The Vestibulo-Ocular ReflexDokument4 SeitenAbnormal Cancellation of The Vestibulo-Ocular ReflexRudolfGerNoch keine Bewertungen
- A Simple Gain-Based Evaluation of The Video Head Impulse Test Reliably Detects Normal Vestibulo-Ocular Reflex Indicative of Stroke in Patients With Acute Vestibular SyndromeDokument8 SeitenA Simple Gain-Based Evaluation of The Video Head Impulse Test Reliably Detects Normal Vestibulo-Ocular Reflex Indicative of Stroke in Patients With Acute Vestibular SyndromeRudolfGerNoch keine Bewertungen
- COVID-19: Stigmatising The Unvaccinated Is Not JustifiedDokument1 SeiteCOVID-19: Stigmatising The Unvaccinated Is Not JustifiedVilag HelyzeteNoch keine Bewertungen
- COVID-19 and Compulsory Vaccination - AnDokument24 SeitenCOVID-19 and Compulsory Vaccination - AnRudolfGerNoch keine Bewertungen
- Early Estimates of SARS-CoV-2 Omicron Variant Severity Based On A Matched Cohort StudyDokument6 SeitenEarly Estimates of SARS-CoV-2 Omicron Variant Severity Based On A Matched Cohort StudyRudolfGerNoch keine Bewertungen
- Latest Statistics On England Mortality Data Suggest Systematic Mis-Categorisation of Vaccine Status and Uncertain Effectiveness of Covid-19Dokument24 SeitenLatest Statistics On England Mortality Data Suggest Systematic Mis-Categorisation of Vaccine Status and Uncertain Effectiveness of Covid-19RudolfGerNoch keine Bewertungen
- Autoimmune Hepatitis Developing After COVID 19 Vaccine PresumedDokument6 SeitenAutoimmune Hepatitis Developing After COVID 19 Vaccine PresumedRudolfGerNoch keine Bewertungen
- CMN Statement Final Version 5-10Dokument3 SeitenCMN Statement Final Version 5-10RudolfGerNoch keine Bewertungen
- Causes and Characteristics of Horizontal Positional NystagmusDokument9 SeitenCauses and Characteristics of Horizontal Positional NystagmusRudolfGerNoch keine Bewertungen
- A Practical Approach To Vertigo - A Synthesis of The Emerging EvidenceDokument14 SeitenA Practical Approach To Vertigo - A Synthesis of The Emerging EvidenceRudolfGerNoch keine Bewertungen
- Fall Prediction in Neurological Gait Disorders DifDokument15 SeitenFall Prediction in Neurological Gait Disorders DifRudolfGerNoch keine Bewertungen
- Head-Jolting Nystagmus Occlusion of The Horizontal Semicircular Canal Induced by Vigorous Head ShakingDokument4 SeitenHead-Jolting Nystagmus Occlusion of The Horizontal Semicircular Canal Induced by Vigorous Head ShakingRudolfGerNoch keine Bewertungen
- Janet G. Travell, MD: Historical PerspectivesDokument5 SeitenJanet G. Travell, MD: Historical PerspectivesRudolfGerNoch keine Bewertungen
- Benign Paroxysmal Positional Vertigo in ChildrenDokument5 SeitenBenign Paroxysmal Positional Vertigo in ChildrenRudolfGerNoch keine Bewertungen
- Cerebral Gray Matter Changes in Persistent Postural Perceptual DizzinessDokument8 SeitenCerebral Gray Matter Changes in Persistent Postural Perceptual DizzinessRudolfGerNoch keine Bewertungen
- A Randomized Controlled Trial Evaluating Integrative Psychotherapeutic Group Treatment Compared To Self-Help Groups in Functional VertigoDizzinessDokument17 SeitenA Randomized Controlled Trial Evaluating Integrative Psychotherapeutic Group Treatment Compared To Self-Help Groups in Functional VertigoDizzinessRudolfGerNoch keine Bewertungen
- Pelvic Pain With Sitting: Diagnostic Algorithm: A. Lee Dellon, MD, PHD, Johns Hopkins UniversityDokument1 SeitePelvic Pain With Sitting: Diagnostic Algorithm: A. Lee Dellon, MD, PHD, Johns Hopkins UniversityRudolfGerNoch keine Bewertungen
- Persistent Postural Perceptual Dizziness Is On A Spectrum in The General PopulationDokument11 SeitenPersistent Postural Perceptual Dizziness Is On A Spectrum in The General PopulationRudolfGerNoch keine Bewertungen
- The Spectrum of Vestibular MigraineDokument14 SeitenThe Spectrum of Vestibular MigraineRudolfGerNoch keine Bewertungen
- Benign Paroxysmal Positional Vertigo in ChildrenDokument5 SeitenBenign Paroxysmal Positional Vertigo in ChildrenRudolfGerNoch keine Bewertungen
- Projections From The Parabrachial Nucleus To The Vestibular Nuclei - Potential Substrates For Autonomic and Limbic Influences On Vestibular ResponsesDokument12 SeitenProjections From The Parabrachial Nucleus To The Vestibular Nuclei - Potential Substrates For Autonomic and Limbic Influences On Vestibular ResponsesRudolfGerNoch keine Bewertungen
- Fall Prediction in Neurological Gait Disorders DifDokument15 SeitenFall Prediction in Neurological Gait Disorders DifRudolfGerNoch keine Bewertungen
- Cerebral Gray Matter Changes in Persistent Postural Perceptual DizzinessDokument8 SeitenCerebral Gray Matter Changes in Persistent Postural Perceptual DizzinessRudolfGerNoch keine Bewertungen
- A Pilot Study To Evaluate Multi-Dimensional Effects of Dance For People With Parkinson's DiseaseDokument6 SeitenA Pilot Study To Evaluate Multi-Dimensional Effects of Dance For People With Parkinson's DiseaseRudolfGerNoch keine Bewertungen
- Lenoir Rhyne KickoffDokument34 SeitenLenoir Rhyne KickoffMike100% (1)
- Methods of Launching by LauncherDokument3 SeitenMethods of Launching by LauncherJahanzeb Khan50% (4)
- Star of BethlemDokument1 SeiteStar of BethlemDR PRABHAT TANDONNoch keine Bewertungen
- Acmc AnswersDokument21 SeitenAcmc AnswersAjay IyerNoch keine Bewertungen
- Flowchart Tort of NegligenceDokument3 SeitenFlowchart Tort of NegligenceYogita Hauradhun100% (8)
- Operator Manual: Generator SetDokument74 SeitenOperator Manual: Generator SetManoelNoch keine Bewertungen
- Instruction Manual: 109, 109 Happystart 111 115, 115 HDokument28 SeitenInstruction Manual: 109, 109 Happystart 111 115, 115 Hzeljko87Noch keine Bewertungen
- Judicial Affidavit HomicideDokument6 SeitenJudicial Affidavit HomicideDonnel BustamanteNoch keine Bewertungen
- Fetal Macrosomia ArtDokument14 SeitenFetal Macrosomia Artanyka2Noch keine Bewertungen
- Shoulder Biomechanics: Roberto Lugo, Peter Kung, C. Benjamin MaDokument11 SeitenShoulder Biomechanics: Roberto Lugo, Peter Kung, C. Benjamin MaAbyudya Rafif KurniawanNoch keine Bewertungen
- 2090 2697 2 108 PDFDokument5 Seiten2090 2697 2 108 PDFMuhammad Riza FahlawiNoch keine Bewertungen
- Ilyas S, Yulianti SR. Ilmu Penyakit Mata Edisi Ke Empat. Jakarta: FKUI Press 2012Dokument3 SeitenIlyas S, Yulianti SR. Ilmu Penyakit Mata Edisi Ke Empat. Jakarta: FKUI Press 2012Tompasobaru DuaNoch keine Bewertungen
- Skin Integrity and Wound CareDokument47 SeitenSkin Integrity and Wound CareCHALIE MEQUNoch keine Bewertungen
- Artifact 3Dokument4 SeitenArtifact 3api-414847385Noch keine Bewertungen
- JSA HEMP Well Services Pg36-40Dokument5 SeitenJSA HEMP Well Services Pg36-40Ashok SureshNoch keine Bewertungen
- Case Study of Hip FractureDokument2 SeitenCase Study of Hip FractureBernardete Freitas Barros100% (1)
- Slip-And-Fall Facts by Easter Law FirmDokument3 SeitenSlip-And-Fall Facts by Easter Law Firmjoe379Noch keine Bewertungen
- Crowe Classification by RanawatDokument10 SeitenCrowe Classification by RanawatShashank VermaNoch keine Bewertungen
- Fox Written RulingDokument62 SeitenFox Written RulingAnthony WarrenNoch keine Bewertungen
- OHSE Project HIRA - Fencing Work - R 01Dokument8 SeitenOHSE Project HIRA - Fencing Work - R 01Pankaj SinghNoch keine Bewertungen
- Neck MusclesDokument1 SeiteNeck MusclesAbdulla EL-ghalayiniNoch keine Bewertungen
- DR - Ramana Rao Pre-Hospital Services in Tamil NaduDokument73 SeitenDR - Ramana Rao Pre-Hospital Services in Tamil NaduBrunoNoch keine Bewertungen
- Alejandro v. Tankeh v. Development Bank of The PhilippinesDokument4 SeitenAlejandro v. Tankeh v. Development Bank of The PhilippinesJezenEstherB.PatiNoch keine Bewertungen
- Musculoskeletal Radiology NotesDokument62 SeitenMusculoskeletal Radiology Notesmeshmatic1234567100% (3)
- 19th Century Musket ManualDokument60 Seiten19th Century Musket Manualhwelch5792Noch keine Bewertungen
- The Skeletal and Musculatory System Word SearchDokument2 SeitenThe Skeletal and Musculatory System Word SearchdavybunyipNoch keine Bewertungen
- Jsa Radiography ActivitiesDokument4 SeitenJsa Radiography Activitiesnasar_mahsood80% (15)
- Gorean Treatments and ServesDokument3 SeitenGorean Treatments and ServesNishaNightFireNoch keine Bewertungen
- Boyd & Griffin Classification (1949)Dokument14 SeitenBoyd & Griffin Classification (1949)João Pedro ZenattoNoch keine Bewertungen
- Neuroimaging of Spinal Instability-Journal ReadingDokument18 SeitenNeuroimaging of Spinal Instability-Journal ReadingAmanda Aldilla MeutiadiNoch keine Bewertungen