Beruflich Dokumente
Kultur Dokumente
Nursing Care Plan of Pressure Ulcers
Hochgeladen von
Cyrus De Asis46%(13)46% fanden dieses Dokument nützlich (13 Abstimmungen)
115K Ansichten1 SeiteThe patient has an impaired skin integrity diagnosis related to age, immobility, and chronic disease. Symptoms include redness, blisters, and open lesions. Nursing interventions include introducing themselves, assessing risk factors, observing the skin and applying dressings, preventing moisture, using sterile technique, and encouraging hydration and nutrition. The goals are for the patient to receive treatment, show healing signs, and prevent future ulcers. Interventions aim to establish trust, identify risks, apply appropriate dressings, prevent infection, and promote healing through nutrition.
Originalbeschreibung:
nursing care plan pressure ulcers
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenThe patient has an impaired skin integrity diagnosis related to age, immobility, and chronic disease. Symptoms include redness, blisters, and open lesions. Nursing interventions include introducing themselves, assessing risk factors, observing the skin and applying dressings, preventing moisture, using sterile technique, and encouraging hydration and nutrition. The goals are for the patient to receive treatment, show healing signs, and prevent future ulcers. Interventions aim to establish trust, identify risks, apply appropriate dressings, prevent infection, and promote healing through nutrition.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
46%(13)46% fanden dieses Dokument nützlich (13 Abstimmungen)
115K Ansichten1 SeiteNursing Care Plan of Pressure Ulcers
Hochgeladen von
Cyrus De AsisThe patient has an impaired skin integrity diagnosis related to age, immobility, and chronic disease. Symptoms include redness, blisters, and open lesions. Nursing interventions include introducing themselves, assessing risk factors, observing the skin and applying dressings, preventing moisture, using sterile technique, and encouraging hydration and nutrition. The goals are for the patient to receive treatment, show healing signs, and prevent future ulcers. Interventions aim to establish trust, identify risks, apply appropriate dressings, prevent infection, and promote healing through nutrition.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 1
Nursing Diagnosis
Patient Outcomes
Nursing Interventions
Rationale
Evaluation
Impaired Skin Integrity
Related Factors:
1. Age
2. Immobility
3. Friction or shear
4. poor circulation
5. moisture
6. chronic disease
state
Evidenced by:
1. Redness
2. Blisters
3. Open lesion involving
the dermis
4. open lesion which
involves bones or
joint
5. drainage of pus
1. The patient will be
able to receive proper
medical attention
before it gets worse.
2. The patient will be
able to manifest signs
of healing and
reduction of pressure
ulcers.
3. The patient will be
able to prevent future
pressure ulcer
1. Introduce yourself at the start
of the nursing care.
1. This will establish trust in the
working phase.
2. Determine the risk factors
leading to pressure ulcer
formation:
age
disease
mobility
2. Elderly patients is less elastic and has
less moisture making it more prone to
skin impairment.
Please refer
to the Patient
Outcomes tab
3. Observe the skin integrity on
the bony prominences.
4. Apply prescribed dressing
such as hydrocolloid dressing.
5. Prevent over exposure to
moisture such as from urine or
perspiration.
6. Observe sterile technique in
doing procedures.
7. Hydrate the patient and
encourage intake of foods rich in
Vitamin C and protein.
3. The areas were the skin is stretched
are as follows: sacrum. Trochanters,
scapulae, elbows. These are the areas
were the highest skin breakdown are.
There is a possibility of skin ischemia
due compression of blood vessels.
4. This composition will prevent friction
or shear. Another way is to provide
emollient to skin to moisturize the skin.
5. This can prevent accumulation of
bacteria thereby keeping away from
infection.
6. Foreign body can also affect greatly
the capability of the skin to regenerate.
Keeping the area clean and free from
excessive moisture can lead to faster
healing process.
7. Collagen can come from Vitamin C,
eating lots of food rich in Vitamin C can
replace the lost collagen thereby leading
to faster healing process.
Das könnte Ihnen auch gefallen
- NCP Risk For Impaired Skin IntegrityDokument3 SeitenNCP Risk For Impaired Skin IntegrityAnne de Vera100% (11)
- NCP-Impaired Skin IntegrityDokument2 SeitenNCP-Impaired Skin IntegrityMikee Ann Valdez96% (26)
- NCP: Patient With A Pressure UlcerDokument2 SeitenNCP: Patient With A Pressure UlcerICa Marlina100% (1)
- Impaired Skin IntegrityDokument2 SeitenImpaired Skin IntegrityJerryson Justo100% (2)
- NCP Impaired Skin IntegrityDokument3 SeitenNCP Impaired Skin IntegrityFlauros Ryu Jabien83% (6)
- Impaired Skin IntegrityDokument7 SeitenImpaired Skin Integrityprickybiik100% (8)
- Nursing Care Plan For Pressure UlcerDokument4 SeitenNursing Care Plan For Pressure UlcerJobelle Acena67% (3)
- Impaired Urinary EliminationDokument2 SeitenImpaired Urinary EliminationHaon Anasu67% (3)
- Nursing Care Plan Impaired Skin IntegrityDokument2 SeitenNursing Care Plan Impaired Skin Integritycuicuita100% (3)
- NURSING CARE PLAN Problem Body Weakness Nursing Diagnosis Impaired PhysicalDokument1 SeiteNURSING CARE PLAN Problem Body Weakness Nursing Diagnosis Impaired Physicalmitchie riveraNoch keine Bewertungen
- Risk For Impaired Skin Integrity and Readiness For Enhanced PowerDokument3 SeitenRisk For Impaired Skin Integrity and Readiness For Enhanced PowerdanaNoch keine Bewertungen
- NURSING CARE PLAN On Impaired Skin IntegrityDokument2 SeitenNURSING CARE PLAN On Impaired Skin Integrityapi-371817493% (30)
- Impaired Skin IntegrityDokument2 SeitenImpaired Skin IntegritySharewin PulidoNoch keine Bewertungen
- Nursing Care Plan Assessment Nursing Diagnosis Inference Planning Intervention Rationale Evaluation SubjectiveDokument2 SeitenNursing Care Plan Assessment Nursing Diagnosis Inference Planning Intervention Rationale Evaluation SubjectiveGaurav Gaikwad100% (3)
- Impaired Skin Integrity Related To Surgical Removal of SkinDokument3 SeitenImpaired Skin Integrity Related To Surgical Removal of Skinnnaesor_10910% (2)
- NCPDokument7 SeitenNCPChris Denver BancaleNoch keine Bewertungen
- Nanda 11 Edi. P. 620-621Dokument3 SeitenNanda 11 Edi. P. 620-621Besael Baccol0% (1)
- NCP Acute Pain RT CancerDokument3 SeitenNCP Acute Pain RT CancerCharissa Magistrado De LeonNoch keine Bewertungen
- Betty Impaired Skin IntegrityDokument2 SeitenBetty Impaired Skin IntegrityBenjie DimayacyacNoch keine Bewertungen
- Nursing Care Plan: Cues and Data Nursing Diagnosis Analysis Goal and Objectives Interventions Rationale EvaluationDokument3 SeitenNursing Care Plan: Cues and Data Nursing Diagnosis Analysis Goal and Objectives Interventions Rationale EvaluationPaul Cubacub100% (1)
- Nursing Care Plan (Impaired Skin Integrity)Dokument4 SeitenNursing Care Plan (Impaired Skin Integrity)arlee marquez91% (161)
- Impaired Tissue Integrity Nursing Care PlanDokument2 SeitenImpaired Tissue Integrity Nursing Care PlanLynnette Adams Mayotte95% (20)
- NCP 2 Impaired Skin IntegrityDokument3 SeitenNCP 2 Impaired Skin IntegrityAela Maive MontenegroNoch keine Bewertungen
- NCP - Risk For Impaired Skin Integrity R/T Dry Skin and Behaviors That May Lead To Skin Integrity Impairment AEB Scratching of ScabsDokument1 SeiteNCP - Risk For Impaired Skin Integrity R/T Dry Skin and Behaviors That May Lead To Skin Integrity Impairment AEB Scratching of ScabsCarl Elexer Cuyugan Ano100% (4)
- Nursing Care PlanDokument3 SeitenNursing Care PlanInah Arcellana100% (2)
- Ineffective Tissue PerfusionDokument2 SeitenIneffective Tissue PerfusionDiane ReyNoch keine Bewertungen
- NCP Impaired Skin IntergrityDokument2 SeitenNCP Impaired Skin IntergrityLaura Sansonetti100% (6)
- Self Cre DeficitDokument3 SeitenSelf Cre DeficitSteph_Toinkz_240Noch keine Bewertungen
- Nursing Care Plan - Impaired Physical MobilityDokument2 SeitenNursing Care Plan - Impaired Physical MobilitySusan Croce57% (7)
- NCP Delayed Wound RecoveryDokument5 SeitenNCP Delayed Wound RecoveryDarkCeades100% (2)
- Nursing Care Plan Impaire Physical MobilityDokument2 SeitenNursing Care Plan Impaire Physical Mobilityderic90% (10)
- NCP FractureDokument2 SeitenNCP Fracturemawel50% (2)
- NCP Impaired Skin IntegrityDokument1 SeiteNCP Impaired Skin Integritysinister17Noch keine Bewertungen
- Nursing Care Plan: Acute PainDokument3 SeitenNursing Care Plan: Acute PainBakushido50% (6)
- Self Care DeficitDokument4 SeitenSelf Care DeficitEllaine RamirezNoch keine Bewertungen
- NCP - BedriddenDokument4 SeitenNCP - Bedriddenadelaigner_racho589475% (4)
- Mpaired Skin Integrity.Dokument8 SeitenMpaired Skin Integrity.Tamil VillardoNoch keine Bewertungen
- NCP - Impaired Skin IntegrityDokument1 SeiteNCP - Impaired Skin Integrityjanelee28240% (2)
- Test Bank For Essential Health Assessment 1st Edition Janice ThompsonDokument40 SeitenTest Bank For Essential Health Assessment 1st Edition Janice Thompsonharoldbrownorcnxeijgd100% (28)
- Possible Complications: Diabetes Fractures Kidney StonesDokument3 SeitenPossible Complications: Diabetes Fractures Kidney StonesMart TramNoch keine Bewertungen
- Objectives and EtiologyDokument2 SeitenObjectives and Etiologycataleya mesaNoch keine Bewertungen
- The Nurse Is Using Medical Asepsis When Providing Client Care. Which Action Did The Nurse Demonstrate?Dokument11 SeitenThe Nurse Is Using Medical Asepsis When Providing Client Care. Which Action Did The Nurse Demonstrate?clintyreee100% (1)
- Skin IntegrityDokument56 SeitenSkin IntegrityneehoshiNoch keine Bewertungen
- Skin Tear Prevention - Strategies For Preventing Skin Injury in At-Risk PopulationsDokument10 SeitenSkin Tear Prevention - Strategies For Preventing Skin Injury in At-Risk PopulationsCarolina RodriguezNoch keine Bewertungen
- Wound Dressings Update: Carolina Weller, Geoff SussmanDokument7 SeitenWound Dressings Update: Carolina Weller, Geoff SussmanyodinheimNoch keine Bewertungen
- Adult Nursing 2020/ Integumentary System Assist Lect /shelan Qahraman SkinDokument8 SeitenAdult Nursing 2020/ Integumentary System Assist Lect /shelan Qahraman Skinمحمد سعد طهNoch keine Bewertungen
- Pre-Reading For VIHDokument10 SeitenPre-Reading For VIHMaria ClaraNoch keine Bewertungen
- Merge-Davao (Multi - Educational Review Group Experts) : Physiological IntegrityDokument12 SeitenMerge-Davao (Multi - Educational Review Group Experts) : Physiological IntegrityNom NomNoch keine Bewertungen
- How Is A Wound Infection Treated?Dokument5 SeitenHow Is A Wound Infection Treated?Haider JulailiNoch keine Bewertungen
- How Is A Wound Infection Treated?Dokument5 SeitenHow Is A Wound Infection Treated?Haider JulailiNoch keine Bewertungen
- Test Bank For High Acuity Nursing 7th Edition WagnerDokument21 SeitenTest Bank For High Acuity Nursing 7th Edition WagnerDavidRobinsonfikq100% (41)
- NCLEX QuestionsDokument6 SeitenNCLEX QuestionsIRA MONIQUE CABADENNoch keine Bewertungen
- Actual Nursing Care Plan 2Dokument16 SeitenActual Nursing Care Plan 2Alyanna Evangelista100% (2)
- Nursing Assistant Educator: For Long Term CareDokument6 SeitenNursing Assistant Educator: For Long Term CareMarnelie Guerrero AbuanNoch keine Bewertungen
- Basic Skin Care and Prevention of Pressure UlcersDokument9 SeitenBasic Skin Care and Prevention of Pressure UlcersGeanieveve ElnasNoch keine Bewertungen
- Wound Care Case StudyDokument5 SeitenWound Care Case StudyJulia KennedyNoch keine Bewertungen
- Skin An Essential Organ-IIDokument30 SeitenSkin An Essential Organ-IIsameen tahirNoch keine Bewertungen
- CBT Material SDokument201 SeitenCBT Material Slucia0% (2)
- Aspirin: Assess The Overall Condition of The SkinDokument4 SeitenAspirin: Assess The Overall Condition of The SkinShaina Fe RabaneraNoch keine Bewertungen
- PERILIGHT EXPOSUREperinealcare Enema PDFDokument7 SeitenPERILIGHT EXPOSUREperinealcare Enema PDFDanna Uy100% (1)
- Cpdprogram Nursing 81718Dokument301 SeitenCpdprogram Nursing 81718PRC BoardNoch keine Bewertungen
- Schizophrenia Schematic DiagramDokument1 SeiteSchizophrenia Schematic DiagramCyrus De AsisNoch keine Bewertungen
- Coronary Artery Disease PathophysiologyDokument4 SeitenCoronary Artery Disease PathophysiologyCyrus De Asis89% (9)
- Cpdprovider Nursing 81718Dokument25 SeitenCpdprovider Nursing 81718PRC BoardNoch keine Bewertungen
- Cerebrovascular Accident Nursing Care PlanDokument4 SeitenCerebrovascular Accident Nursing Care PlanCyrus De Asis67% (12)
- Gestational Diabetes Mellitus PathophysiologyDokument1 SeiteGestational Diabetes Mellitus PathophysiologyCyrus De Asis100% (3)
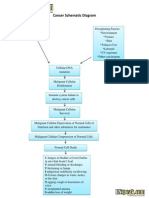
- Cancer Schematic DiagramDokument1 SeiteCancer Schematic DiagramCyrus De Asis100% (4)
- Liver Pathophysiology and Schematic DiagramDokument1 SeiteLiver Pathophysiology and Schematic DiagramCyrus De Asis100% (4)
- Pregnacy Induced Hypertension PhysiologyDokument1 SeitePregnacy Induced Hypertension PhysiologyCyrus De AsisNoch keine Bewertungen
- Preeclampsia Pathophysiology and Schematic DiagramDokument1 SeitePreeclampsia Pathophysiology and Schematic DiagramCyrus De Asis80% (10)
- Asthma Pathophysiology and DiagramDokument1 SeiteAsthma Pathophysiology and DiagramCyrus De Asis100% (1)
- Pregnacy Induced Hypertension - PIH - PathophysiologyDokument2 SeitenPregnacy Induced Hypertension - PIH - PathophysiologyCyrus De Asis100% (2)
- Ectopic Pregnancy PathophysiologyDokument1 SeiteEctopic Pregnancy PathophysiologyCyrus De Asis100% (2)
- Major Effects Hormones Pregnant MotherDokument1 SeiteMajor Effects Hormones Pregnant MotherCyrus De AsisNoch keine Bewertungen
- Burns Nursing Care Plan - NCP - Risk For InfectionDokument1 SeiteBurns Nursing Care Plan - NCP - Risk For InfectionCyrus De AsisNoch keine Bewertungen
- Anaphylactic Shock PathophysiologyDokument1 SeiteAnaphylactic Shock PathophysiologyCyrus De Asis100% (3)
- Geriatric Assessment Tool An Application of Core - Care and Cure ModelDokument1 SeiteGeriatric Assessment Tool An Application of Core - Care and Cure ModelCyrus De AsisNoch keine Bewertungen
- Diarrhea Nursing Care PlanDokument2 SeitenDiarrhea Nursing Care PlanCyrus De Asis87% (121)
- Hyperthyroidism Pathophysiology and Schematic DiagramDokument1 SeiteHyperthyroidism Pathophysiology and Schematic DiagramCyrus De Asis67% (9)
- Hypertension Nursing Care PlanDokument2 SeitenHypertension Nursing Care PlanCyrus De Asis93% (14)
- Iron Deficiency Anemia Schematic DiagramDokument2 SeitenIron Deficiency Anemia Schematic DiagramCyrus De Asis83% (12)
- Alzheimer's Disease Nursing Care PlanDokument2 SeitenAlzheimer's Disease Nursing Care PlanCyrus De Asis76% (17)
- Hiatal Hernia Pathophysiology - Schematic DiagramDokument1 SeiteHiatal Hernia Pathophysiology - Schematic DiagramCyrus De Asis100% (1)
- Nursing Care Plan Patient EndotrachealDokument2 SeitenNursing Care Plan Patient EndotrachealCyrus De Asis67% (6)
- Benign Prostatic Hyperplasia NCPDokument2 SeitenBenign Prostatic Hyperplasia NCPCyrus De Asis100% (2)
- Post-Throidectomy Nursing Care PlanDokument2 SeitenPost-Throidectomy Nursing Care PlanCyrus De AsisNoch keine Bewertungen
- Congestive Heart Failure Schematic DiagramDokument1 SeiteCongestive Heart Failure Schematic DiagramCyrus De Asis100% (1)
- Hydrocephalus PathophysiologyDokument1 SeiteHydrocephalus PathophysiologyCyrus De Asis100% (1)
- Schematic Diagram of Alcoholic CirrhosisDokument2 SeitenSchematic Diagram of Alcoholic CirrhosisCyrus De Asis0% (1)
- Bioptron Short BookDokument52 SeitenBioptron Short BookMonica100% (4)
- Prontosan Case StudiesDokument37 SeitenProntosan Case Studiesaldj2010Noch keine Bewertungen
- Clinical Experience With Surgical Debridement and Simultaneous Meshed Skin Grafts in Treating Biofilm-Associated Infection: An Exploratory Retrospective Pilot StudyDokument9 SeitenClinical Experience With Surgical Debridement and Simultaneous Meshed Skin Grafts in Treating Biofilm-Associated Infection: An Exploratory Retrospective Pilot StudyAsmat BurhanNoch keine Bewertungen
- 6.dabetic FootDokument81 Seiten6.dabetic FootArleen MatincaNoch keine Bewertungen
- A Textbook On Surgical Short Cases 4nbsped 8190568132 9788190568135 CompressDokument299 SeitenA Textbook On Surgical Short Cases 4nbsped 8190568132 9788190568135 CompressHamza Khan100% (1)
- MORINGO Plus and CellerikDokument38 SeitenMORINGO Plus and CellerikARIF PATEL100% (2)
- Impaired Skin IntegrityDokument3 SeitenImpaired Skin IntegrityGerardeanne Reposar100% (2)
- February 2007-Emergency Department Wound Management PDFDokument245 SeitenFebruary 2007-Emergency Department Wound Management PDFAndikaPurbaNoch keine Bewertungen
- Bedsore PDFDokument5 SeitenBedsore PDFIam BabuNoch keine Bewertungen
- Dokumen - Tips Ilmu Bedah FK Unsoed LibreDokument240 SeitenDokumen - Tips Ilmu Bedah FK Unsoed Libreyetti Trisna100% (1)
- Presentasi Traumatic Wound Management - A Comprehensive Wound Management Forum Discussion & Hands-On ModelsDokument57 SeitenPresentasi Traumatic Wound Management - A Comprehensive Wound Management Forum Discussion & Hands-On ModelsDadek PradnyanaNoch keine Bewertungen
- Effect of Custom-Made Footwear On Foot Ulcer Recurrence in DiabetesDokument8 SeitenEffect of Custom-Made Footwear On Foot Ulcer Recurrence in DiabetesJosé MorenoNoch keine Bewertungen
- Juan Carlos Vsim Prep 3Dokument5 SeitenJuan Carlos Vsim Prep 3Michelle Pinkhasova100% (3)
- Clinical Methods in ENT by P. T. WakodeDokument229 SeitenClinical Methods in ENT by P. T. WakodeQuranSunnat100% (1)
- Escuela Profesional de Enfermeria: CURSO: Inglés TécnicoDokument17 SeitenEscuela Profesional de Enfermeria: CURSO: Inglés TécnicoLeydi Rojas HuarcayaNoch keine Bewertungen
- CME Trunk, Abdomen, and Pressure Sore ReconstructionDokument15 SeitenCME Trunk, Abdomen, and Pressure Sore ReconstructionVeronica TomaselloNoch keine Bewertungen
- Skin Integrity and Wound CareDokument55 SeitenSkin Integrity and Wound Caremango47Noch keine Bewertungen
- Asuhan Keperawatan Pada Kerusakan Integritas KulitDokument19 SeitenAsuhan Keperawatan Pada Kerusakan Integritas KulitYuniar Valentine Putri PratiwiNoch keine Bewertungen
- Bioelectricity and Microcurrent TherapyDokument11 SeitenBioelectricity and Microcurrent TherapyGustavo Cabanas100% (2)
- Dermatology EssentialsDokument1.037 SeitenDermatology EssentialsViviana Malaver Yepes100% (10)
- Crohn DiseaseDokument2 SeitenCrohn DiseaseFiraFurqaniNoch keine Bewertungen
- Pressure Ulcer Assessment Chart & Body MapDokument2 SeitenPressure Ulcer Assessment Chart & Body MapWidfdsafdsaNoch keine Bewertungen
- Skin Grafting Surgical NursingDokument21 SeitenSkin Grafting Surgical NursingHEMMA100% (1)
- 2.4.2 Medorrhinum - AllenDokument49 Seiten2.4.2 Medorrhinum - AllenaldodiasNoch keine Bewertungen
- Burn Case Study - Saisankalp Shankar - 3A PathophysiologyDokument3 SeitenBurn Case Study - Saisankalp Shankar - 3A PathophysiologysaimarvelousNoch keine Bewertungen
- Monteiro Soares - Et - Al 2020 IWGDF Classification GuidelineDokument8 SeitenMonteiro Soares - Et - Al 2020 IWGDF Classification GuidelineDaoud AmineNoch keine Bewertungen
- TIME 2020 - ConsensoDokument28 SeitenTIME 2020 - ConsensoJacinta MontesNoch keine Bewertungen
- Complete Spanish Step by Step 2Nd Edition Barbara Bregstein Full ChapterDokument51 SeitenComplete Spanish Step by Step 2Nd Edition Barbara Bregstein Full Chapterolive.lieberman136100% (13)
- Case Record Form For ChildrenDokument32 SeitenCase Record Form For ChildrenPrasad javvajiNoch keine Bewertungen
- Incontinence Associated Dermatitis Made EasyDokument6 SeitenIncontinence Associated Dermatitis Made EasyRismaNoch keine Bewertungen