Beruflich Dokumente
Kultur Dokumente
HA, Fever, Pain
Hochgeladen von
Leonardo RanderOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
HA, Fever, Pain
Hochgeladen von
Leonardo RanderCopyright:
Verfügbare Formate
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
Headache, Fever, and Musculoskeletal Pain
Learning Objectives
1. Describe the basic pathophysiology behind various sources of pain and fever
2. List exclusions to self-treatment and know when to refer patients to a physician for
further assessment
3. Recommend appropriate non-pharmacologic and pharmacologic treatment options
4. Counsel patients on the selection and proper use of pain and fever products
Pain
1. Unpleasant sensory and/or emotional experience
a. Defined as an unpleasant sensation signaling actual or possible injury
b. Physical, affective, and learned components
2. Self-treatment is common in pain
a. $75+ million spent on OTC analgesics
b. Nearly half of patients dont read labeling
3. Acute or Chronic Pain
a. Acute pain: begins suddenly and usually does not last long
i. Symptoms:
b. Chronic pain: lasts for weeks or months; associated with a chronic disorder (such as
cancer, arthritis, diabetes, or fibromyalgia) or an injury that does not heal
i. Effects: depression, disturbed sleep, decreased energy, a poor appetite,
weight loss, decreased sex drive, and loss of interest in activities
ii. Breakthrough pain: pain that occurs during treatment for chronic pain
1. Begins suddenly, lasts up to 1 hour, and feels like the original pain but
more severe
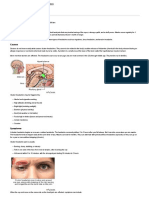
4. Pain Pathways
a. Pain due to injury begins at special pain
receptors
b. Transmit signals along nerves to the
spinal cord and then upward to the
brain
c. Signal sent backwards to original site of
pain, triggering muscles to contract
d. Pain signal also sent to the brain
e. Only when the brain processes the
signal and interprets it, do people
become conscious of the pain
Headaches
1. Classified as primary or secondary
a. Primary headaches: not associated with an underlying illness
1
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
i. Accounts for ~90% of headaches
ii. Examples: episodic and chronic tension-type headaches, migraine
headache with and without aura, cluster headaches, and medicationoveruse headaches
b. Secondary headaches: symptoms of an underlying condition such as head trauma,
stroke, substance abuse or withdrawal, bacterial and viral diseases, and disorders of
craniofacial structures
2. Pathophysiology of Headache
a. Sinus Headache:
b. Tension-type Headaches:
c. Migraine:
3. Clinical Presentation
a. Chronic tension-type headaches occurring 15 days/month for at least six months
may be a manifestation of psychological conflict, depression, or anxiety
i. May be associated with sleep disturbances, shortness of breath, constipation,
weight loss, fatigue, decreased sexual drive, palpitations, and menstrual
changes
Sinus Headache
Tension-type Headaches
Migraine
4. Treatment of Headache
a. Goals
i.
ii.
iii.
2
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
iv.
v.
b. Non-Pharmacologic Treatment
i. Avoidance of possible food triggers (nitrates, tyramine, phenylalanine,
caffeine, MSG
ii. Avoidance of hunger and low blood glucose
iii. Relaxation exercises, stress coping methods
iv. PT, acupuncture
v. Regular sleep and eating schedule
vi. Ice/cold packs
Exclusion Criteria for Self-Treatment
Primary Headaches
Symptoms > 10 days
Severe symptoms
3rd trimester
Children <8 years old
Symptoms of migraine without diagnosis
Diagnosed migraines with moderate to severe
symptoms
Secondary Headaches
High fever or sign of infection
Associated with a stiff neck and vomiting
Onset follows bending, lifting, or coughing
Sleep is disturbed
Headache is present upon awakening
Recent head or neck (e.g. whiplash) injury
Numbness, tingling, weakness of arms or legs
5. Self-Care of Headache
Asthma & nasal polyps, chronic/recurrent GI
ulcers, gout, coagulation disorders or
anticoagulant therapy, HBP, CHF, kidney
disease, or aspirin allergy?
Yes
Avoid salicylates & NSAIDS
No
Yes
< 12 years of age?
Avoid Naproxen
No
Yes
< 15 years of age?
No
Avoid salicylates if symptoms of
viral illness are present
For tension-type headaches, recommend
APAP, NSAID, or salicylate as appropriate.
For migraine, recommend NSAID or salicylate
as appropriate
Chronic Headache
Severe Headache
Episodic Headache
Severe Headache
Medical Referral
Follow up after 6-12 weeks
Follow up after 4-6 weeks
Follow up within 10 days
No
Adequate analgesia?
Yes
Intermittent use < 3x/week
3
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
6. Pharmacologic Treatments
Indication
Products
Mechanism of
Action
Non-Prescription Analgesic/Antipyretic Treatments
Salicylates
NSAIDs
Mild to moderate pain, fever,
Mild to moderate pain, fever,
inflammation
and inflammation
Acetylated: aspirin (ASA)
Non-acetylated: magnesium,
choline, sodium
Irreversibly inhibit prostaglandin
synthesis by inhibiting COX-1
and COX-2
Decrease prostaglandins =
decrease sensitivity to pain
Adverse Effects
Contraindications/P
recautions
Nausea, dyspepsia, heartburn,
bruising, prolonged bleeding
time, rash, angioedema (rare)
Pre-existing conditions: asthma,
nasal polyps, h/o ulcers or GI
bleeding, blood-clotting
disorders, gout, heart failure
Allergy: hypersensitivity to drug
Ibuprofen, Naproxen,
Ketoprofen
Reversible inhibition of
prostaglandin synthesis by
inhibiting COX-1 and COX-2
(peripheral sites)
Decrease prostaglandins =
decrease sensitivity to pain
Abdominal pain, heartburn,
nausea, vomiting, constipation,
flatulance
Asthma, allergy to ASA, ulcers,
gout, heart failure, high blood
pressure
APAP
Mild to moderate
pain, fever
No anti-inflammatory
effects
Tylenol
Central (CNS)
inhibition of
prostaglandins
Well tolerated
Skin rash, jaundice,
thrombocytopenia
Active Liver Disease
Alcoholics
Avoid in pregnancy (especially
3rd trimester)
Not recommended in children
with recent viral infection
(Reyes Syndrome)
Drug Interactions
Formulations
Avoid in pregnancy (especially
3rd trimester)
Valproic Acid
NSAIDs, including COX-2
inhibitors
Anticoagulants
Alcohol
Methotrexate
Sulfonylureas
Enteric Coated
Buffered
Effervescent
Sustained Release
Anticoagulants
Alcohol
Digoxin
Methotrexate
Sulfonylureas
Phenytoin (ibuprofen)
Alcohol
Warfarin
Ibuprofen: immediate-release,
chewable, capsules,
suspension, liquid drops
Naproxen: tablets
All forms
a. Recommended Dosages
Agent
Usual Adult Dose (Maximum Daily Dosage)
Pediatric Dosing
Dose by body weight (mg/kg)
Acetaminophen
Ibuprofen
Naproxen
Aspirin
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
b. Combination Products
i. ASA (250mg) +/- APAP (250mg) + Caffeine (30-65mg)
1. Synergistic analgesic effects-addition of caffeine causes
vasoconstriction of blood vessels in the brain
2. Indicated in mild to moderate pain, fever, and inflammation; often
used in migraines
7. Herbals and Supplements
Agent
Feverfew
Peppermint oil
Risks
Possible rebound headache
with chronic use; mouth
ulceration with direct contact
with leaves; possible
anticoagulation effect
Skin irritation, avoid during
pregnancy and lactation
Coenzyme Q10
Avoid during pregnancy and
lactation; minor GI disturbances
Magnesium
Diarrhea; GI upset
Use/Effectiveness
Treatment and prevention of migraine
headaches; mixed results from clinical trials
(difference in formulations?)
Topical treatment of tension headache;
preliminary evidence suggests peppermint oil
applied to forehead and temples may relieve
tension headaches
Prevention of migraine headaches; small, open
label trial demonstrated that 150mg/day
reduced frequency by 33%
Treatment and prevention of migraine
headache; mixed results for prevention
8. Patient Education
Tension-Type Headache
Migraine Headache
Precautions for Nonprescritpion Analgesics
Salicylates & NSAIDs
APAP
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
Musculoskeletal Pain
1. Musculoskeletal pain arises from the muscles, bones, joints, and connective tissue
a. Can be idiopathic, iatrogenic, or related to injury
b. Acute: result of minor injuries, strains, or sprains; self-limiting
c. Chronic: ongoing, persistent, or repetitive pain (arthritis, gout)
Types/Causes
Goals of Treatment
Myalgias: acute overuse of muscle
Tendonitis and bursitis: chronic overuse of
joint
Sprains, strains: twisting, excessive
stretching, tearing
Cramps: exercise-induced, menstrual
Lower back pain: muscle or disc
Joint pains: arthritis
2. Self-Care of Musculoskeletal Injuries and Disorders
Exclusions for Self-Treatment
Patient with complaint of pain
Pain duration > 10-14 days
Patient < 7 years old
High fever or other signs of infection
Nausea or severe vomiting
Weakness, numbness in any limb
Accompanied by redness, warmth,
swelling (joint/muscle)
Suspected fracture
Pelvic or abdominal pain (not
associated w/ menses)
Pregnancy or breast-feeding
Severe or worsening pain
Signs of neurological problems
Perform initial assessment
Yes
Exclusions for self-treatment?
No
Contraindications/
intolerances to OTC
analgesics?
Yes
Medical Referral
No
Pain from overexertion, or
muscle/joint injury?
No
Osteoarthritis?
No
Yes
Yes
Initiate nondrug
therapies & APAP.
F/U in 1 month
RICE therapy & oral or topical
analgesic. F/U in 7 days
Pain relief
satisfactory
or complete?
No
Maximize
therapy or
add topical.
F/U in 1 month
Yes
Pain improved or resolved?
No
Medical Referral
Yes
Continue therapy
PRN < 2 weeks. F/U to
assess for ADRs
Continue
therapy
Yes
Pain improved or resolved
No
6
Titrate dose to max dose.
Consider referral
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
3. Treatment Options
Non-Pharmacologic
a. Acute Therapies: use immediately (first 48-72
hours)
R
I
i. Systemic agents: APAP, ASA, NSAIDs
(see tables above for dosing
C
information)
E
b. Topical Agents: applied to intact skin to relieve
(REFERAL to health care provider/rehab)
pain
i. Analgesics/Anesthetics/Antipruritics
1. Inhibit cutaneous sensation of pain, burning, itching
ii. Counterirritants
1. Principle of paradoxical pain relief producing a less severe pain
counters a more intense one
a. Produce mild, local inflammatory effect thought to provide
relief at adjacent or underlying site
b. Many have analgesic/anesthetic properties as well
2. Applied not more than 3-4 times/day for up to 7 days
3. OK for use in children 2+ years old
Allyl isothicynate, ammonia
water, methyl salicylate,
turpentine oil
Menthol & camphor
Histamine dihydrochloride &
methyl nicotinate
Capsicum, capsicum
oleoresin, capsaicin
Rubefacients; promote redness & irritation via
capillary dilation
Promote cooling sensations, depress nerves
that perceive pain
Cause vasodilatation
Incite irritation without rubefacients (no
vasodilation)
c. Sub-acute & Chronic Therapies: use 72 hours after injury or long-term
i. Non-Pharmacological
1. Once inflammation resolved, replace ice with HEAT
a. 15-20 min intervals x 4 times/day
b. Promotes healing, minimizes muscle spasms
2. Reinstate exercise SLOWLY
Electronic heating pad
d. Complementary Therapies
-Pros: Reusable / Cons: $$$
i. Massage
Temporary heat products
-E.g.
Thermal
wraps, patches
ii. Acupuncture, acupressure
-Provide low-level heat for up to 12 hours
iii. Stress reduction
-Pros: Inexpensive / Cons: One-time use
iv. Physical therapy
1. Stretching, strengthening, range-of-motion exercises
v. Herbals/Supplements
1. Glucosamine + Chondroitin
a. MOA: anti-inflammatory properties, protect/rebuild cartilage
matrix & synovial fluid
7
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
2.
3.
4.
5.
b. Evidence grade A (strong) for osteoarthritis pain
i. Most evidence for knee joint
ii. Reduces subjective pain, NSAID dose
c. Glucosamine1500mg + Chondroitin 800-1200mg daily
d. Likely safe, well-tolerated
e. Cons:
i. $$$
ii. Slow onset of efficacy
Turmeric plenty of pain relief benefits
a. Evidence grade: C arthritis
Ginger relieves arthritis, headaches, menstrual cramps and
muscle soreness
a. Evidence grade: C dysmenorrhea, migraine, arthritis
Valerian Root natures tranquilizernatural pain reliever
a. Evidence grade: NOT studied for pain
Eucommia for your aching back and joints
a. Evidence grade: NO human studies available
Fever
1. Introduction
a. Body Temperature
i. Normal body temperature: 97.5-98.9F
ii. Regulated by a feedback system (physiological and behavioral adaptations
keep temperature in range)
1. Varies depending on: age, sex, ambient temperature, activity level
2. Time of day: 2am and 6am (lowest); 4pm and 10pm (highest)
b. Fever (pyrexia): regulated rise in body temperature in response to a pyrogen (sign of
increase in core set point)
i. Generally considered temp > 98.9F
ii. More common in children
iii. Majority self-limiting, nonthreatening; major reason for treating: alleviate
discomfort
iv. Causes: viral/bacterial pathogens, tissue damage, malignancy, CNS
inflammation, medications, idiopathic
c. Fever pathway
Release of
Pyrogens
Activation of
arachidonic
acid pathway
Release of
prostaglandin E2
FEVER
Body temp
reaches new set
point
Rise in set point
of hypothalamus
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
d. Types of fever
Hyperthermia
Hyperpyrexia
Unregulated increae incore
temperature without elevation of
hypothalamic set point
Temperature: 99.5-100.9F
Inadequate heat dissipation in response
to a warm enviornment (heat stroke)
Can be rapid and fatal
Antipyretic agents are ineffective
Temperature >106.7F
Extreme elevation of body temperature
(emergency situation)
Requires immediate and aggressive
body cooling
Usually associated with CNS
hemorrhage (thyroid storm, NMS,
kawasaki syndrome)
2. Signs/Symptoms and Complications
a. Fever itself is a symptom
i. Often accompanied by headache, diaphoresis, malaise, chills, arthralgia
b. Complications
i. Serious complications are rare: seizures, delirium, brain damage
ii. Increased risk of neural tube defects in pregnancy
iii. Febrile seizures
3. Detection of fever
a. When monitoring, always measure with same type of thermometer at same site
Body Site
Normal Range (F)
Fever
(F)
Thermometer
Comments
Rectal
Mercury, digital
Oral
Axillary
Tympanic
Mercury, digital
Mercury, digital
Infrared thermometer
Closest to core temp (Gold Standard)
1st line in infants/children
1st line in adults
Do not use for infants <6 mo
b. Thermometers
i. Mercury-in-glass: Rarely used in the US
1. ~5 minutes to obtain reading
2. Pros: Inexpensive, Compact size
3. Cons: breakable, slow, difficult to read, contents hazardous
ii. Digital electronic thermometer
1. 30-60 seconds to obtain reading
2. Pros: durable, easy to read, available in pen or pacifier shape, disposable
probe covers
3. Cons: require batteries, need to be calibrated
iii. Infrared: used for temporal & tympanic measurement
1. < 5 seconds to obtain reading
2. Detects heat from the arterial blood supply
3. Pros: fasting reading, relatively non-invasive
4. Cons: $$$, require batteries, require routine recalibration, inaccurate if
placed improperly
iv. Adhesive temperature strips: placed on forehead-changes color at various
temperature gradients
1. Pros: non-invasive
2. Cons: very inaccurate use NOT recommended; track trends in
temperature over time
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
4. Treatment
a. Goal: alleviate the discomfort by reducing temperature
Assess how temperature was
measured. Was it accurate?
No
Yes
Offer to take temp. Explain
proper methods. If fever
present go to next box
Obtain symptom
information, medical history,
allergy information
Exclusions for self-treatment?
Yes
Medical referral
No
Oral temp >101F or
equivalent?
Yes
No
Nondrug measures
antipyretic agent based on
patient factors
Exclusions for Self-Treatment
>6 mo. old with rectal temp
>104F
<6 mo. old with rectal temp
>100F
Severe symptoms of infection
that are not self-limiting
Risk for hyperthermia
Impaired oxygen utilization
Impaired immune function
CNS damage
Children with history of febrile
seizures or seizures
Child who develops spots or
rash
Child who refuses to drink fluids
Child who is very sleepy,
irritable, or hard to wake up
Child who is vomiting and
cannot keep down fluids
Nondrug measures
antipyretic agent if patient
has discomfort or if
patient/caregiver requests
Fever resolved after 3 days?
No
Medical referral
Yes
D/C therapy
b. Non-pharmacologic treatment
i. Adjunctive therapy if temp > 102
ii. Options: reduce clothing, remove blankets; keep room comfortably cool;
increase fluid intake; cold compress (armpits, groin, forehead)
c. Pharmacologic treatments
i. Antipyretics: aspirin, APAP, NSAIDs
1. Work to lower set point, NOT body temperature; bodys own adaptive
mechanisms facilitate drop in body temp
2. Dosing: see earlier charts
Pediatrics
Ibuprofen approved for use in children >6 mo.
APAP products do not have dosing listed for children <2
Alternating use of APAP and NSAIDs not recommended
Potential for overdose: risk dosing too frequently,
confusing with varying doseages/concentrations
No proof of increased efficacy
Pregnancy and Lactation
APAP is drug of choice
NSAIDs/ASA not recommended (especially in 3rd
trimester)
ASA not recommended during breast feeding
10
Amber Lanae Smith, PharmD, MS, BCPS
PHA 4010 Principles of Pharmacotherapy 1: Self-care and Alternative Health Care
5. Fever Phobia: displayed by parents with young children who present with fever
a. Characterized by:
i. Unnecessary or aggressive treatment of fever
ii. Checking temperature every hour
iii. Administering antipyretic agents for temperatures <100F
iv. Administering antipyretic agents more frequently than directed
v. Awakening children to administer antipyretic
b. Reassure parents
i. Educate on when to self-treat, appropriate dosing, how to monitor progress, and
when to call pediatrician
6. Counseling points
a. Generic vs. Brand name
b. Picking a specific product
c. Use caution with combination products
d. Importance of non-pharmacologic measures first
e. Reading labeling carefully before taking or administering
11
Das könnte Ihnen auch gefallen
- CTC 2020Dokument850 SeitenCTC 2020Mounira75% (4)
- 6 Foods To Avoid If You Have OsteoarthritisDokument12 Seiten6 Foods To Avoid If You Have OsteoarthritisPJ LedesmaNoch keine Bewertungen
- CTC2017 - Sample Chapter-Fibromyalgia PDFDokument13 SeitenCTC2017 - Sample Chapter-Fibromyalgia PDFMirandaNoch keine Bewertungen
- Fitness RX June IssueDokument34 SeitenFitness RX June Issuethepdfguy50% (2)
- Cluster Headache - MedlinePlus Medical EncyclopediaDokument3 SeitenCluster Headache - MedlinePlus Medical EncyclopediaUtpal KumarNoch keine Bewertungen
- Algoritma Neck PainDokument12 SeitenAlgoritma Neck PainAri SudarsonoNoch keine Bewertungen
- On Head AcheDokument27 SeitenOn Head Achesarath p rajuNoch keine Bewertungen
- Mental Health - PsychopharmacologyDokument4 SeitenMental Health - PsychopharmacologyRenetria DrakeNoch keine Bewertungen
- Headaches, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandHeadaches, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Minor AilmentsDokument37 SeitenMinor AilmentsNiamh Mone100% (3)
- HeadacheDokument41 SeitenHeadacheNatalia Khan100% (1)
- Medication Instructions Prior To SurgeryDokument11 SeitenMedication Instructions Prior To Surgeryhohj100% (1)
- Vitamins, Trace Minerals, and Other Micronutrients Mason JDokument10 SeitenVitamins, Trace Minerals, and Other Micronutrients Mason JLeonardo RanderNoch keine Bewertungen
- Tension Type HeadacheDokument30 SeitenTension Type HeadacheIndraYudhi100% (2)
- A Tension HeadacheDokument8 SeitenA Tension HeadachediesNoch keine Bewertungen
- Migraine LeafletDokument6 SeitenMigraine LeafletEliza SitinjakNoch keine Bewertungen
- Common DrugsDokument15 SeitenCommon DrugsKate Penelope DalidNoch keine Bewertungen
- Migraines: Migraine Treatment and Prevention Options: The most important information you need to improve your healthVon EverandMigraines: Migraine Treatment and Prevention Options: The most important information you need to improve your healthNoch keine Bewertungen
- Group 3 - Pharm 3DDokument3 SeitenGroup 3 - Pharm 3DAila Marie ArandillaNoch keine Bewertungen
- HeadacheDokument3 SeitenHeadachefoodpandaforeveryoneNoch keine Bewertungen
- Activity 56 Headache Zillah QuizolDokument6 SeitenActivity 56 Headache Zillah QuizolARAGON GEMMA LYNNoch keine Bewertungen
- Obesity1 02 Jul19 202301Dokument10 SeitenObesity1 02 Jul19 202301EDUARDO HUARTENoch keine Bewertungen
- Headaches Information For Patients Version 3Dokument4 SeitenHeadaches Information For Patients Version 3Renato KaindoyNoch keine Bewertungen
- HeadacheDokument16 SeitenHeadacheBagoes Ario BimoNoch keine Bewertungen
- Headache - A Quick TutorialDokument7 SeitenHeadache - A Quick TutorialLeilia FibrianasariNoch keine Bewertungen
- Headache 2Dokument21 SeitenHeadache 2geeeelzy07Noch keine Bewertungen
- MigraineDokument56 SeitenMigraineDivina AquinoNoch keine Bewertungen
- Ukdi Preparation I:: Neurogenic Pain Syndromes Peripheral Nerve DisordersDokument65 SeitenUkdi Preparation I:: Neurogenic Pain Syndromes Peripheral Nerve DisordersFelicia SutarliNoch keine Bewertungen
- (F1) Headache PDFDokument66 Seiten(F1) Headache PDFmdNoch keine Bewertungen
- HeadacheDokument42 SeitenHeadacheRaghoba GaonkarNoch keine Bewertungen
- Tension Type HeadacheDokument18 SeitenTension Type HeadacheRiris SihotangNoch keine Bewertungen
- 11 Types of Headaches - Causes, Symptoms, and TreatmentDokument27 Seiten11 Types of Headaches - Causes, Symptoms, and TreatmentCHIMA ONWUKA MONGNoch keine Bewertungen
- CCJM Relieving Migraine PainDokument12 SeitenCCJM Relieving Migraine PainBrian HarrisNoch keine Bewertungen
- Migraine Diagnosis: SupplementsDokument3 SeitenMigraine Diagnosis: Supplementsseema yadavNoch keine Bewertungen
- Advances in Migraine Prevention: Clinical Experience With TopiramateDokument64 SeitenAdvances in Migraine Prevention: Clinical Experience With TopiramateontabarkerNoch keine Bewertungen
- Health Teaching Plan For Pan CaDokument4 SeitenHealth Teaching Plan For Pan CaInah Floresta BesasNoch keine Bewertungen
- Pain Management For Medical StudentsDokument37 SeitenPain Management For Medical Studentsamq aloqiliNoch keine Bewertungen
- Cu7 - Pain 1Dokument18 SeitenCu7 - Pain 1FERMIL PASGALANoch keine Bewertungen
- Migraine and You: An Educational Guide For Migraine Headache SufferersDokument23 SeitenMigraine and You: An Educational Guide For Migraine Headache SufferersagelsantosNoch keine Bewertungen
- Guidelines For DoctorsDokument18 SeitenGuidelines For Doctorsmh125fizanNoch keine Bewertungen
- E-Therapeutics+ - Minor Ailments - Therapeutics - Central Nervous System Conditions - Vertigo and DizzinessDokument5 SeitenE-Therapeutics+ - Minor Ailments - Therapeutics - Central Nervous System Conditions - Vertigo and DizzinessSamMansuriNoch keine Bewertungen
- Naturopathic Medicine: A Short HistoryDokument3 SeitenNaturopathic Medicine: A Short HistoryRoseanne Legaspi CasayuranNoch keine Bewertungen
- Standard Medical CareDokument12 SeitenStandard Medical CareAbdul Moeed KhanNoch keine Bewertungen
- Journal Reading Syaraf-SuleDokument45 SeitenJournal Reading Syaraf-SuleDrosophila Meilani GasterNoch keine Bewertungen
- Physical Therapy II PresentationDokument2 SeitenPhysical Therapy II PresentationRaymondNoch keine Bewertungen
- AFP MigrañaDokument9 SeitenAFP MigrañaJuaan AvilaNoch keine Bewertungen
- Headache in Primary CareDokument32 SeitenHeadache in Primary CareSaif SinghNoch keine Bewertungen
- Lecture 8-Principles of Drug Use in Palliativ EcareDokument6 SeitenLecture 8-Principles of Drug Use in Palliativ EcareMachukiNoch keine Bewertungen
- 2019 Migraine Prevention and Treatment GuidelinesDokument14 Seiten2019 Migraine Prevention and Treatment Guidelinesshaik saifuddinNoch keine Bewertungen
- Sarah S. Taupan, RN, MN, DPADokument33 SeitenSarah S. Taupan, RN, MN, DPAKatri ArasaNoch keine Bewertungen
- Migraine Headache PDFDokument14 SeitenMigraine Headache PDFAl Hasyr SarminNoch keine Bewertungen
- Migraine: A Concise Presentation byDokument25 SeitenMigraine: A Concise Presentation bySaravan PramodNoch keine Bewertungen
- Headache and SeizuresDokument30 SeitenHeadache and Seizurestawfekmohamed03Noch keine Bewertungen
- Section 03 Concepts of Family MedicineDokument2 SeitenSection 03 Concepts of Family MedicineNikey LimNoch keine Bewertungen
- Headache: & Associated EmergenciesDokument63 SeitenHeadache: & Associated EmergenciesMahad IbrahemNoch keine Bewertungen
- Therapeutic Modalities: Therapeutic Modalities, Psychosocial Skills, and Nursing 1 Biophysical/ Somatic InterventionsDokument15 SeitenTherapeutic Modalities: Therapeutic Modalities, Psychosocial Skills, and Nursing 1 Biophysical/ Somatic InterventionsdaliaNoch keine Bewertungen
- Eng MigraineDokument5 SeitenEng MigrainedeepashajiNoch keine Bewertungen
- The Best Way To Prevent Migraine Is To Find Out What Triggers Your Attacks and Avoid or Limit These TriggersDokument3 SeitenThe Best Way To Prevent Migraine Is To Find Out What Triggers Your Attacks and Avoid or Limit These TriggersKARL PASCUANoch keine Bewertungen
- Migraine: Kementerian Kesehatan Republik Indonesia Politeknik Kesehatan Surakarta Jurusan Keperawatan Prodi Profesi NersDokument8 SeitenMigraine: Kementerian Kesehatan Republik Indonesia Politeknik Kesehatan Surakarta Jurusan Keperawatan Prodi Profesi NersTasya SyafhiraNoch keine Bewertungen
- Pharmaceutical Care Cases: Palliative Care PAIN and Constipation 2013 Notes DefinitionDokument5 SeitenPharmaceutical Care Cases: Palliative Care PAIN and Constipation 2013 Notes DefinitionLeyla MajundaNoch keine Bewertungen
- Hes 005 Session 12 SasDokument12 SeitenHes 005 Session 12 SasBread PartyNoch keine Bewertungen
- Hes 005 Session 12 SasDokument12 SeitenHes 005 Session 12 SasJose Melmar Autida AutenticoNoch keine Bewertungen
- Week 5 Portfolio QuestionsDokument4 SeitenWeek 5 Portfolio Questionsapi-479716004Noch keine Bewertungen
- Week 7 Category 3Dokument3 SeitenWeek 7 Category 3api-468093714Noch keine Bewertungen
- Headache 2Dokument11 SeitenHeadache 2khaled alahmadNoch keine Bewertungen
- Efns Guideline On The Treatment of Tension-Type Headache - Report of An Efns Task ForceDokument33 SeitenEfns Guideline On The Treatment of Tension-Type Headache - Report of An Efns Task ForcecindyNoch keine Bewertungen
- Remedies For Migraine: Medication, Treatments, Cures, And Home RemediesVon EverandRemedies For Migraine: Medication, Treatments, Cures, And Home RemediesNoch keine Bewertungen
- Redox Biology of Tuberculosis PathogenesisDokument62 SeitenRedox Biology of Tuberculosis PathogenesisLeonardo RanderNoch keine Bewertungen
- Free Radical Biology and MedicineDokument17 SeitenFree Radical Biology and MedicineLeonardo RanderNoch keine Bewertungen
- Beware of DockingDokument18 SeitenBeware of DockingLeonardo RanderNoch keine Bewertungen
- Steyn2012 PDFDokument14 SeitenSteyn2012 PDFLeonardo RanderNoch keine Bewertungen
- Onreplicating Ersistence of : Lawrence G. Wayne and Charles D. SohaskeyDokument27 SeitenOnreplicating Ersistence of : Lawrence G. Wayne and Charles D. SohaskeyLeonardo RanderNoch keine Bewertungen
- (Topics in Current Chemistry 239) Kenji Mori (Auth.), S. Schulz (Eds.) - The Chemistry of Pheromones and Other Semiochemicals I-Springer-Verlag Berlin Heidelberg (2004)Dokument217 Seiten(Topics in Current Chemistry 239) Kenji Mori (Auth.), S. Schulz (Eds.) - The Chemistry of Pheromones and Other Semiochemicals I-Springer-Verlag Berlin Heidelberg (2004)Leonardo RanderNoch keine Bewertungen
- Sign of The Cross: Downloaded FromDokument1 SeiteSign of The Cross: Downloaded FromLeonardo RanderNoch keine Bewertungen
- Cough, Cold and AllergiesDokument68 SeitenCough, Cold and AllergiesLeonardo RanderNoch keine Bewertungen
- Fever and PainDokument49 SeitenFever and PainLeonardo RanderNoch keine Bewertungen
- Legal and Regulatory Student Fall 2014Dokument33 SeitenLegal and Regulatory Student Fall 2014Leonardo RanderNoch keine Bewertungen
- CAM Self-Care Fall 2014 9.2.14Dokument51 SeitenCAM Self-Care Fall 2014 9.2.14Leonardo RanderNoch keine Bewertungen
- Phenothiazines Class Ethanolamines Class Tavist ® Dramamine ® Benadryl ® Unisom ® Nyquil ® Piperazine ClassDokument2 SeitenPhenothiazines Class Ethanolamines Class Tavist ® Dramamine ® Benadryl ® Unisom ® Nyquil ® Piperazine ClassLeonardo RanderNoch keine Bewertungen
- Insomnia and FatigueDokument5 SeitenInsomnia and FatigueLeonardo RanderNoch keine Bewertungen
- Calcium Pre-Reading Fall 2014Dokument10 SeitenCalcium Pre-Reading Fall 2014Leonardo RanderNoch keine Bewertungen
- Hometesting Devices Fall 2014Dokument50 SeitenHometesting Devices Fall 2014Leonardo RanderNoch keine Bewertungen
- Technical Description Bibliografic ReferencesDokument2 SeitenTechnical Description Bibliografic ReferencesLeonardo RanderNoch keine Bewertungen
- OTC Advisor - Fever, Cough, Cold, and Allergy FINAL PDFDokument33 SeitenOTC Advisor - Fever, Cough, Cold, and Allergy FINAL PDFmorsi0% (1)
- Naproxen-Eudragit Microspheres: Screening of Process and Formulation Variables For The Preparation of Extended Release TabletsDokument4 SeitenNaproxen-Eudragit Microspheres: Screening of Process and Formulation Variables For The Preparation of Extended Release TabletsDebby NovriozaNoch keine Bewertungen
- NaproxenDokument3 SeitenNaproxenAngel CatalanNoch keine Bewertungen
- Drug Study: Tabije, Arvie Jayselle P. Marbella, IvyDokument15 SeitenDrug Study: Tabije, Arvie Jayselle P. Marbella, IvyJaysellePuguonTabijeNoch keine Bewertungen
- Preoperative Assessment. Plauntz (2007)Dokument17 SeitenPreoperative Assessment. Plauntz (2007)Dario Cahuaza :VNoch keine Bewertungen
- Drug StudyDokument8 SeitenDrug StudymYiE23Noch keine Bewertungen
- XareltofinalDokument2 SeitenXareltofinalMuniba NasimNoch keine Bewertungen
- BioLiving in A High Tech WorldDokument103 SeitenBioLiving in A High Tech WorldAida BEkNoch keine Bewertungen
- Cozaar 25 MG: What Is Losartan (Cozaar) ?Dokument25 SeitenCozaar 25 MG: What Is Losartan (Cozaar) ?nyzgirl17Noch keine Bewertungen
- VaginoplastyDokument16 SeitenVaginoplastyAmanNoch keine Bewertungen
- Practice Advisory On The Appropriate Use of Nsaids in Primary CareDokument15 SeitenPractice Advisory On The Appropriate Use of Nsaids in Primary CareAsti IndriyaniNoch keine Bewertungen
- Che2060 Aspirin LabDokument22 SeitenChe2060 Aspirin Labbhavesh yadavNoch keine Bewertungen
- Medsurg Nursing Medications Cheat Sheet: by ViaDokument2 SeitenMedsurg Nursing Medications Cheat Sheet: by ViaABEGAIL SARASUANoch keine Bewertungen
- 22 23-Jabberwock-Handbook FillableDokument36 Seiten22 23-Jabberwock-Handbook Fillablesunain rizwanNoch keine Bewertungen
- Obat Dan Kehamilan, Drugs, Aman Untuk Ibu Hamil, FarmasiDokument13 SeitenObat Dan Kehamilan, Drugs, Aman Untuk Ibu Hamil, FarmasifrankysukwendyNoch keine Bewertungen
- MEFENAMIC-ACID-mefenamic Acid Caps Ule Sciele Pharma IncDokument14 SeitenMEFENAMIC-ACID-mefenamic Acid Caps Ule Sciele Pharma IncIrma DamayantiNoch keine Bewertungen
- Case 31 MerckDokument16 SeitenCase 31 MerckGaLb AbohaNoch keine Bewertungen
- Total Knee Replacement Manual and Therapy/Rehab Protocol: Dr. Edward Kelly, MD, MBADokument12 SeitenTotal Knee Replacement Manual and Therapy/Rehab Protocol: Dr. Edward Kelly, MD, MBAJasleen KaurNoch keine Bewertungen
- PHARMACEUTICAL CHEMISTRY (Analgesics Agents, Antipyretic Agents, Anti-Inflammatory Agents)Dokument34 SeitenPHARMACEUTICAL CHEMISTRY (Analgesics Agents, Antipyretic Agents, Anti-Inflammatory Agents)Dr. BABLI ROYNoch keine Bewertungen
- The 30-Day Guide To IVF Success: Diet, Chemicals, Sex, and MoreDokument14 SeitenThe 30-Day Guide To IVF Success: Diet, Chemicals, Sex, and MoreStacy Lactam SacopasoNoch keine Bewertungen
- Systemic Review On The Use of Diclofenacb Complex As An Antiinflammatorytreatment With Pain Relief Effect For Patients With Acute Lower Back Pain 2167 0846 1000216Dokument5 SeitenSystemic Review On The Use of Diclofenacb Complex As An Antiinflammatorytreatment With Pain Relief Effect For Patients With Acute Lower Back Pain 2167 0846 1000216Dhea Yulia LubisNoch keine Bewertungen
- Week 1Dokument14 SeitenWeek 1roxsan gNoch keine Bewertungen
- Pharmacology of MeloxicamDokument9 SeitenPharmacology of MeloxicamkwadwobrosNoch keine Bewertungen