Beruflich Dokumente
Kultur Dokumente
How U.S. Dental Care Became A National Emergency - Nisarg Patel
Hochgeladen von
selectiveraptur84Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
How U.S. Dental Care Became A National Emergency - Nisarg Patel
Hochgeladen von
selectiveraptur84Copyright:
Verfügbare Formate
How U.S.
Dental Care Became a National
Emergency | Nisarg Patel
Kyle Willis had a toothache. What he didn't have was a job -- or health and dental insurance. Willis,
who lived in Cincinnati, first visited a nearby dentist, where he was told one of his wisdom teeth had
to be pulled. However, as an unemployed, single father, he had no way to pay for the procedure and
decided to endure the pain. Just a few weeks later, Willis developed a headache and the side of his
face swelled like a balloon. He went to the Emergency Room, where he was prescribed painkillers,
which cost $3, and antibiotics, which cost $27. Unable to afford both, he bought only the painkillers.
While he was able to stop the pain over the next few days, the infection spread to his brain and
caused it to swell. He was rushed to the hospital, where he later died. Willis was 24.
This isn't a one-off tragedy. Like Willis, 130 million Americans -- over 40 percent of the population -do not have dental insurance. Over the last ten years, millions of patients have been showing up with
dental pain to hospital emergency departments (EDs) instead of dental practices, at the cost of
billions to hospitals, in hopes of receiving quick and affordable relief. ED physicians, however,
cannot do much to treat dental pain other than prescribe painkillers and antibiotics, and inform
patients upon discharge to visit a dentist. However, over 70 percent of patients who visit the ED for
dental-related conditions have no
http://abortion-support.com/blog/why-routine-dental-cleanings-are-so-vital/ form of dental coverage
and nearly one-fifth return to the ED with the same problem soon afterwards, signaling that a
significant number of people are having trouble accessing affordable dental care. The end result can
be fatal. 101 patients were found to have died due to dental-related problems in the ED in just a
three-year span.
This game of life or death is largely a political battle. While 44 states offer some capacity of dental
benefits to Medicaid-enrolled adults, only 28 offer coverage beyond emergency treatment, but still
fall short of the standard of care needed to maintain adequate oral health. Under the Affordable
Care Act, 30 states, including the District of Columbia, intend to expand Medicaid eligibility to
adults at up to 138 percent of the federal poverty level. Although the ACA mandates dental coverage
for individuals less than 18 years of age, adult dental coverage remains optional for insurers.
However, at least 22 of those Medicaid-expansion states intend to offer dental benefits to newly
eligible enrollees. 10 will offer extensive benefits, 7 will offer limited benefits, and 5 will offer
emergency benefits-services provided for the relief of pain and infection under defined emergency
situations-alone. Limited benefits include select diagnostic, preventative, and minor restorative
procedures. This covers less than 100 of the approximately 600 procedures recognized by the
American Dental Association's Code on Dental Procedures and Nomenclature. The per-person
annual expenditure is capped at $1,000. Extensive benefits, in contrast, covers at least 100 of the
approximately 600 procedures recognized by the American Dental Association's Code on Dental
Procedures and Nomenclature. The per-person annual expenditure is capped to at least $1,000, if
not more. To no surprise, states that opted out of providing dental coverage in their benefits
packages cited cost as their primary determining factor.
This trend is symptomatic of a larger structural and socioeconomic issue. The use of the emergency
department for dental problems serves as a marker for disparities in the quality of and access to
adequate dental care and health literacy. Over 70 percent of patients who come into the ED for
dental-related visits reside in low-income geographic areas. Medicaid enrollees often have trouble
finding the only 20 percent of dentists who accept Medicaid. Low reimbursement rates, high rates of
cancelled appointments, low compliance with treatment, and the administrative burden all
contribute to the scarcity in Medicaid-accepting dentists. Additionally, access to dental care is
limited not only by insurance coverage, but also an individual's discretionary income and
geographical location. As a result, low-income patients are at higher risk to forgo dental care
altogether, despite experiencing a greater burden of oral disease.
Although significant evidence links poor oral health to systemic diseases, particularly diabetes
mellitus and cardiovascular disease, most people are uneducated about the consequences of poor
oral hygiene and its role in overall health. Poor oral health literacy and compliance among families is
highly evident in the case of childhood tooth decay. Although it is virtually preventable, tooth decay
is the most common chronic illness among children. When ignored or untreated, it can cause severe
pain, tooth loss, systemic infection, and, in some cases, death. Despite this, nearly one in four
children in the U.S. have untreated tooth decay. For low-income children, it's every one in two.
The problem doesn't disappear with age either. The U.S. Centers for Disease Control and Prevention
estimate that nearly 50 percent of Americans over 30 suffer from periodontitis, which destroys the
gum tissue and bone that supports teeth and the jaw. In adults over 65, that number jumps to over
70 percent. In advanced cases, affecting nearly 9 percent of Americans, it can cause tooth loss,
pneumonia, poor pregnancy outcomes, and chronic inflammation, increasing the risk of diabetes,
cardiovascular disease, and stroke. Additional costs associated with these systemic health problems
as a result of poor oral health also contributes to otherwise preventable healthcare spending.
Chronic illness management costs the U.S. healthcare system nearly $300 billion annually.
Herein lies the economic incentive-in addition to improving the quality of U.S. healthcare-for
hospital administrators and policymakers to design and implement health system models to alleviate
disparities between access to dental care and medical care.
Local and state governments should expand dental clinics within Federally Qualified Health Centers
(FQHCs), of which the Affordable Care Act allotted $11 billion in new funds, and other community
health centers in low-income areas. Less than 60 percent of FQHCs offer dental services, and those
that do provide significantly limited adult dental care. While only about 2 percent of the dental
workforce provides care within FQHCs, the 2009 Children's Health Insurance Program
Reauthorization Act (CHIPRA) stipulated that FQHCs may contract with private dentists to provide
dental care to health center patients in private dental offices. Increasing the number of private
dentists who contract with federally supported health centers may increase dental coverage to
underserved populations and, given the increased patient pool, incentivizes dentists, particularly
recent graduates, to contract with FQHCs.
Finally, establishing literacy campaigns in conjunction with the expansion of FQHC dental coverage,
either through coordination with federal insurance programs, dental care companies, or media
partnerships, will be essential in improving oral health education and utilization of dental services
among newly eligible Medicaid beneficiaries, because no one deserves to lose their life to a
toothache.
http://www.huffingtonpost.com/nisarg-patel/a-killer-toothache-how-us-dental-care-became-a-national
-emergency_b_7835660.html
Das könnte Ihnen auch gefallen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Sarms 1 - The Ultimate Guide To SarmsDokument4 SeitenSarms 1 - The Ultimate Guide To SarmsHumbert Gym ColombinaNoch keine Bewertungen
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- Anticipatory Grief, Death, and BereavementDokument9 SeitenAnticipatory Grief, Death, and BereavementAdelina Rotaru100% (1)
- GMFMscoresheetDokument6 SeitenGMFMscoresheetAbdur RasyidNoch keine Bewertungen
- Psychology From Islamic Perspective (Amber)Dokument22 SeitenPsychology From Islamic Perspective (Amber)Rðbið HðqueNoch keine Bewertungen
- Methicillin-Resistant Staphylococcus Aureus PDFDokument23 SeitenMethicillin-Resistant Staphylococcus Aureus PDFGerardo N. Pabón Gallino100% (1)
- DewormingDokument48 SeitenDewormingJulie Ann Escartin80% (5)
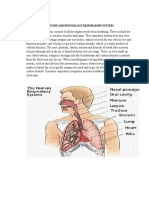
- Anatomy and Physiology Respiratory SystemDokument7 SeitenAnatomy and Physiology Respiratory Systemnoronisa talusobNoch keine Bewertungen
- Vocabulary Revision PhysiotherapyDokument4 SeitenVocabulary Revision PhysiotherapyHuong Giang100% (2)
- Degnala DiseaseDokument12 SeitenDegnala DiseaseSantosh Bhandari100% (1)
- Current Issues in Postoperative Pain Management PDFDokument12 SeitenCurrent Issues in Postoperative Pain Management PDFikm fkunissulaNoch keine Bewertungen
- Phenol First AidDokument7 SeitenPhenol First AidAnurag GhoshNoch keine Bewertungen
- Treatment of Oropharyngeal Dysphagia CarolMcKee (1) DPNS StudyDokument23 SeitenTreatment of Oropharyngeal Dysphagia CarolMcKee (1) DPNS Studyconstantineelia100% (1)
- Interns 2016 DistributionDokument13 SeitenInterns 2016 DistributionKashish ChawlaNoch keine Bewertungen
- Oculus Biom 5 Ophthalmoscope User ManualDokument36 SeitenOculus Biom 5 Ophthalmoscope User ManualRoberto FalconeNoch keine Bewertungen
- Leaflet of Bach Therapy PDFDokument2 SeitenLeaflet of Bach Therapy PDFPrakash VerekarNoch keine Bewertungen
- Guiding Principles For Best Practices in Geriatric PTDokument16 SeitenGuiding Principles For Best Practices in Geriatric PTPritesh KujurNoch keine Bewertungen
- National Guidelines On Management of Dengue Fever & Dengue Haemorrhagic Fever in Children and Adolescents - Sri LankaDokument53 SeitenNational Guidelines On Management of Dengue Fever & Dengue Haemorrhagic Fever in Children and Adolescents - Sri LankaNational Dengue Control Unit,Sri Lanka100% (1)
- Fitzgerald AnnInternMed 1999 130 70 Curiosity PDFDokument3 SeitenFitzgerald AnnInternMed 1999 130 70 Curiosity PDFPaulinaNoch keine Bewertungen
- Prospectus PDFDokument68 SeitenProspectus PDFPrince Digital ComputersNoch keine Bewertungen
- Moran CORE - How To Use The Direct OphthalmoscopeDokument1 SeiteMoran CORE - How To Use The Direct OphthalmoscopeSamsung M20APNoch keine Bewertungen
- Spray Bandage Strategy in Topical Drug DeliveryDokument9 SeitenSpray Bandage Strategy in Topical Drug DeliveryUday BaruahNoch keine Bewertungen
- Role, Prospects, and Limitation of HomoeopathyDokument43 SeitenRole, Prospects, and Limitation of HomoeopathyDr.bhagyaNoch keine Bewertungen
- David Blaine BiographyDokument7 SeitenDavid Blaine BiographyPunkaj YadavNoch keine Bewertungen
- Seroflo 250 Synchrobreathe - View Uses, Side Effects, Price and Substitutes - 1mgDokument10 SeitenSeroflo 250 Synchrobreathe - View Uses, Side Effects, Price and Substitutes - 1mgParteek SinglaNoch keine Bewertungen
- Egyptian Hospital Accreditation Program: Standards: Sixth Edition May 2005Dokument71 SeitenEgyptian Hospital Accreditation Program: Standards: Sixth Edition May 2005khayisamNoch keine Bewertungen
- 1 BarashDP - Paradigms Lost AbridgedDokument7 Seiten1 BarashDP - Paradigms Lost AbridgedFABIONoch keine Bewertungen
- Agenda Prac Draft Agenda Meeting 7 10 February 2022 - enDokument69 SeitenAgenda Prac Draft Agenda Meeting 7 10 February 2022 - ennegfbNoch keine Bewertungen
- Latihan Soal Procedure TextDokument2 SeitenLatihan Soal Procedure TextSuwari RisnawatiNoch keine Bewertungen
- Raja Nigantu IntroductionDokument8 SeitenRaja Nigantu IntroductionMedico PassNoch keine Bewertungen
- Informed ConsentDokument1 SeiteInformed Consentapi-107381417Noch keine Bewertungen