Beruflich Dokumente
Kultur Dokumente
Buccal Mucosa Cancer
Hochgeladen von
muhammad_ariefCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Buccal Mucosa Cancer
Hochgeladen von
muhammad_ariefCopyright:
Verfügbare Formate
11
Buccal Mucosa Cancer
Alain Gerbaulet
Introduction
In Europe and North America, buccal mucosa carcinoma represents 3 to 5% of oral-cavity cancer; it
is much more frequent in South Asia and Latin America. These differences are due to people
chewing arec and betel nuts, tobacco leaves and coca leaves mixed with lime, since these are
carcinogenic. In developed countries, tobacco contributes in one third of patients and alcohol in 20%
of them, but these aetiological factors are often underestimated. The proportion of females is higher
than in other head-and-neck cancers: the sex ratio is 3 : 1 (males/females).
Clinical symptoms are in decreasing order: simple discomfort, mass, pain, trismus, neck node. (3)
Primary tumours less than 40 mm in size, involving the anterior two thirds of the buccal mucosa,
without involvement of the gingiva and intermaxillary commissura, constitute an "ideal" indication for
brachytherapy.
External beam radiation alone or combined with brachytherapy is reserved for tumours larger than 40
mm or where radical surgery is contraindicated. (2)
Wide local excision with a safety margin of at least 5 mm is one of the treatments of choice for wellcircumscribed limited tumours. Radical surgery is indicated for tumours invading the intermaxillary
commissure or gingiva; this therapeutic approach is very invasive and must be followed by a
reconstructive procedure. (1,13)
Anatomical Topography
The buccal mucosa is bounded by the lower and upper gum sulcus; the lip commissure constitutes
its anterior limit; the posterior limit is the intermaxillary commissure. (8)
Lymphatic drainage is to submandibular nodes or directly to jugular nodes. (8,12)
Critical organs are the mandible, the gingiva and the teeth, but also, in the case of very infiltrating
tumours, soft tissues such as muscles and skin. (3,4)
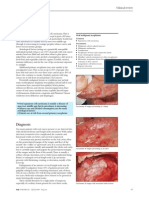
Fig 11.1: Primary squamous-cell cancer
of the buccal mucosa.
266 Buccal Mucosa Cancer
Pathology
Macroscopically, tumours may be exophytic, ulcerating, infiltrating or nodular or any combination.
The ease of brachytherapy depends on the exact position in the cheek.
Most tumours are squamous cell carcinomas. Other histopathological types are: glandular
carcinomas, lymphosarcomas, melanomas. Precancerous lesions are observed in one third of
patients. Nodal involvement is noted at the time of the initial diagnosis in about 40% of patients.
(2,12)
Work Up (see chapter on Head and Neck general aspects)
The work-up is comparable to other cancers of the oral cavity, but the particular carcinogenetic and
epidemiological factors must be evaluated. (12) Because of the frequent association of malignant
and premalignant tumours, the tumour site must be accurately described by diagrams, biopsies,
ultrasound and MRI. (1,13)
Indications, Contra-indications
Interstitial brachytherapy is strongly indicated for lesions of the anterior and central part of the buccal
mucosa. If there is deep involvement of the gingivobuccal sulcus, brachytherapy is contraindicated
as in floor of mouth carcinoma, because of the unacceptable risk of osteoradionecrosis to the
mandible. (3,4,7)
For the posterior third of the buccal mucosa, the indication for implant alone must be discussed case
by case. In fact, it is usually very difficult to evaluate tumour extension to the retromolar trigone
accurately and even more difficult to the intermaxillary commisure. (4,5)
Interstitial brachytherapy alone is indicated for small (< 40 mm), well-defined tumours, located in the
anterior two thirds of the buccal mucosa. This brachytherapy is followed, as for other oral-cavity
carcinomas, by a cervical node dissection in selected cases. (4,7)
For tumours larger than 40 mm, or tumours involving the posterior third of the buccal mucosa
(without involvement of the intermaxillary commissure), a combination of external-beam radiation and
brachytherapy boost is indicated.
When brachytherapy is contraindicated because of involvement of mandible, maxillary or
intramaxillary commissura and/or the tumour volume (>40 mm) external-beam radiotherapy is
indicated or in selected cases radical surgery with reconstruction. (1,13)
Target Volume
The target volume is defined by intraoral examination completed by a bidigital palpation of the
tumour; with one finger in the mouth and the other on the skin of the cheek. (4) The projection of the
gross tumour volume (GTV) should be drawn and the clinical target volume (CTV) mapped out on the
surface of the skin. The CTV comprises the GTV plus a safety margin of 10 mm at the anterior and
posterior parts of the tumour (GTV) and one of 5 to 10 mm at its upper and lower limits, according to
the position of the tumour in relation to the mandible and upper maxilla.
Buccal Mucosa Cancer 267
The drawing is completed by the projection of the different healthy structures, such as upper maxilla
and mandible. During this procedure, the mouth is alternatively open and closed.
If brachytherapy is used as a boost, the initial tumour volume must be known: its outer limits can be
marked with metallic clips, but these may move during the first phase of treatment and it is therefore
safer to draw the projection on to the skin, photograph the patient, and tattoo the peripheral
intrabuccal limits of the tumour differentiating as well as possible cancer and precancerous lesions.
(2)
CT-scan or preferably MRI can contribute to defining the tumour volume and consequently the target
volume more accurately. MRI is used at the time of diagnosis but also after the plastic tubes are
implanted to check the quality of the implant and to adjust the position of the radioactive sources.
Technique
Two implantation techniques are mainly used: guide gutters and plastic tubes according to the
tumour volume and site.
7.1
Superficial, well limited, anterior lesions, close to the lip commissure, smaller than 20 mm in
size are appropriate for the guide-gutter technique. (3,4) This implant can be performed under
local anaesthesia. The guide gutters are implanted parallel to the buccal mucosa in the
anteroposterior direction. The patient's mouth is open and an intraoral finger of the operator checks
the position of the guide gutter. In general, one double-guide gutter is sufficient, sometimes
completed by an extra single-guide gutter. After the replacement of the gutters by iridium hairpins,
the relative position of the suture around the bridge to the lip commissure is crucial to maintain the
radioactive material in position and be tolerated well by the patient.
7.2
The plastic-tube technique is indicated for all other lesions: the number of lines, distance
between the lines, number of planes and distance between the planes are established according to
the dimensions of the target volume.
Fig 11.2: Plastic-tube technique: the dimensions of the
tumour projected on the skin surface of the cheek are
checked according to the positioning of the metallic
needles.
Fig 11.3: Classical plastic tube implant: four lines
equidistant and parallel maintained in position by a
perforated catheter.
268 Buccal Mucosa Cancer
There are two ways of implanting a buccal mucosa carcinoma, taking into account the thickness of
the tumour and the anatomical characteristics of the cheek, whose thickness increases from the lip
commissure to the intermaxillary commissure.
7.2.1 With the first technique, the needles are implanted through the skin: first parallel to each
other, parallel to the oral mucosa and parallel to the horizontal branch of the mandible. Under digital
control, the lines are placed approximately 3-5 mm deep, under the buccal mucosa. They should
cover 10 mm of normal mucosa behind or in front of the lesion with a recommended spacing of 12 to
15 mm. Two or three plastic tubes are usually required to cover the target volume if the thickness of
the tumour does not exceed 5 mm. Plastic spacers at both ends keep the tubes parallel. Retention
buttons are fixed at both extremities (Fig 11.2,3).
If the lesion is thicker than 5 mm, a second plane of tubes is implanted between the first one and the
skin, with an interplane spacing equal to the intersource spacing in each plane.
With a single plane, the thickness of the target volume equals about 50% of the space between the
lines (i.e. distance 18 mm, treated thickness 9 mm). If the thickness to be treated is greater, 2 planes
are necessary or the second technique should be chosen (Fig 11.4).
Fig 11.4: Carinoma of the anterior part of
the buccal mucosa with extension to the
labial commissura. Two planes are necessary to
cover the posterior part of the CTV, one only for
the anterior part.
When the lesion is posterior, near the intermaxillary commissure, there is a risk of geographic miss at
the back with the parallel tubes, because isodose curves indent between the wires. In this case, we
recommend a posterior loop whose top is as close as possible to the intermaxillary commissure.
The two horizontal branches of this loop can be distanced 30 to 45 mm; one to two other lines are
implanted in-between. If four plastic tubes are implanted, they can form a double loop: a small
anterior one, close to the labial commissure, and a posterior one, close to intermaxillary commissure.
A loop forms a posterior barrier by linking the two outside parallel wires inside the cheek at 5 mm
from the bucco-alveolar sulcus in its upper and inferior parts. To perform the bridge
Buccal Mucosa Cancer 269
of the loop, the needles are implanted vertically through the skin into the mucosa or placed intraorally
under the buccal mucosa, with the help of a Reverdin needle (Pernot technique) (5,7) or a curved
hollow needle (Gerbaulet technique) (3,4) (see chapters on oropharynx, bladder) (Fig 11.5).
Fig 11.5: Radiograph with dummy sources (lead wires) showing a double loop procedure: anterior
loop/labial commissure, posterior loop/intermaxillary commissure.
Fig 11.6: Plastic tube technique : The plastic tubes are inserted, an anterior loop is performed close
to the labial commissural.
Fig 11.7: Plastic tube technique : the top of the anterior loop is loaded to well-irradiated labial
commissura, check radiograph of Iridium wires.
270 Buccal Mucosa Cancer
To improve the homogeneity of the dose, a median plastic tube is placed between the two parallel
branches, to obtain a spacing of 12 to 15 mm between each line. The posterior end of the median
radioactive wire must be about 7 mm from the bridge of the loop to avoid a hot spot. A customized
lead gutter is highly recommended to reduce the risk of osteoradionecrosis.
When the lesion is anterior, close to the commissure, the two outside parallel plastic tubes can be
replaced by a loop, using the same technique as that described above for posterior tumours (Fig
11.6,7).
7.2.2 A second technique, (Gerbaulet technique) used for very bulky infiltrating tumour is to
implant the needles perpendicularly to the skin of the cheek organized in several loops to cover the
target volume (Fig 11.8). (3)
Fig 11.8: Very bulky infiltrating tumour
extending from the buccal mucosa to the
muscles of the cheek. Five loops are
implanted perpendicular to the surface of the
cheek. The top of each loop is on the
surface of the buccal mucosa.
7.2.3 The loading is determined based on the target volume (CTV) according to the rules of the
Paris System. Whereas for other interstitial implants in head-and-neck carcinoma, radioactive
sources are perpendicular to the surface of the tumour, for buccal mucosa they are (except for the
second technique used in very bulky lesions) parallel to it, as it is usual for skin or lip cancers.
For all these different implants, the position of the lines must be checked not only when the mouth is
open but also closed, with the shielding device in place inside the oral cavity. In general, the
shielding system may reduce the thickness of the target volume by stretching the cheek and
squeezing the tumour so irradiation is better adapted. (3,5)
Buccal Mucosa Cancer 271
Dosimetry
Dosimetry is established from two orthogonal radiographs complemented by CT scan and/or MRI, to
determine as closely as possible both GTV and CTV. Different planes are chosen, perpendicular to
the radioactive lines: in the frontal plane when the lines are parallel to the buccal mucosa, in the
sagittal plane when the lines are perpendicular to the buccal mucosa. According to the Paris System
the central plane constitutes the reference plane. The reference dose is 85% of the basal dose rate.
(4)
Dose, Dose Rate, Fractionation
The total dose for LDR brachytherapy is 65 to 70 Gy for brachytherapy alone, 25 to 30 Gy when
brachytherapy is used as a boost after 45 to 50 Gy of external-beam irradiation. (3,4,5,7)
10
Monitoring
See chapter on head-and-neck general considerations.
11
Results
The largest multicentric study was done by the GEC (Groupe Europen de Curiethrapie) (Gerbaulet
and Pernot.) (2) Seven hundred forty-eight patients were treated for primary tumour with:
brachytherapy alone (31%) (A), combination of external beam irradiation + brachytherapy (11%) (B),
external beam irradiation alone (36%) (C), surgery often followed by radiation therapy (22%) (D).
These different therapeutic approaches were adapted to prognostic factors: tumour size, tumour site,
nodal status. (12) Five-year NED survival rate according to T stage was: T1 61%, T2 46%, T3 33%,
T4 10%. For the various treatments, the local failure rate (including all primary tumours) was: 19% for
brachytherapy alone, 35% for combination external beam irradiation + brachytherapy and for external
beam irradiation alone, 22% for surgery - external beam irradiation.
With the exception of the GEC multicentric trial, few other reports have been published of
brachytherapy in buccal-mucosa carcinoma (Table 11.1).
In these different studies, patients were treated with brachytherapy alone (A) or with combined
external-beam radiation and brachytherapy boost (B) in nearly 700 cases. When the two treatments
are compared, survival and local-control rates are better for brachytherapy 60% versus 35% and
75% versus 60%, respectively. Very few data have been published on complication rates. They are
estimated to be about 15 to 20% for brachytherapy alone (A) and 25 to 30% for combined irradiation
(B) (Fig 11.9,10).
272 Buccal Mucosa Cancer
Fig 11.9: Typical aspect of an exophytic tumour
of the buccal mucosa.
Fig 11.10: Result one year after treatment.
Table 11.1: Results for treatment of buccal mucosa cancer
Authors
Gerbaulet (2)
Pts
748
TNM
106 T1
210 T2
175 T3
257 T4
23 T1
33 T2
23 T3
6 Tx
T1-3 36
N0 35
Treatments
A 266
B 80
C 273
D 167
A
B
Brachy
LDR
Ra, Au, Ir
Gerbaulet (3,4)
84
Lapeyre Pernot (5 )
42
Plastic tubes:
parallel/loops
LDR Ir
Nair (6)
234
Stage I-IV
A, B, C, D
LDR Ra
Sakai (9)
55
T1-4
A, B, C, D
IBT
Mould
Shibuya (10)
45
T1 8
T2 30
T3 7
A, B
Perm Impl Au, Rn
LDR Ir
Legends:
Treatments :
.
A: brachytherapy alone
.
B: EBRT + brachytherapy
.
C: EBRT alone
.
D Surgery EBRT
.
IBT: interstitial brachytherapy
.
Perm Impl: Permanent implants
Results :
.
AS : Actuarial Survival OS: Overall Survival
DFS: Disease Free Survival
Survival %
A 64
B 41
C 26
D 66
A 60
B 31
Local Control %
A 81
B 65
C 45
D 78
A 74
B 52
OS 48
CSS 74
DFS 54
3yr-DFS
A 62
C 42
IBT 67
mould 48
C 27, D 61
AS 81
Parallel 58
Loops 91
IBT 94
mould 55
C 50, D 81
86
CSS: Cancer Specific Survival
Buccal Mucosa Cancer 273
12
References
1. Bloom ND, Spiro RH. Carcinoma of the cheek mucosa. A retrospective analysis. Am J Surg
1980; 140 (4): 556-9.
2. Gerbaulet A, Pernot M. Le carcinome epidermoide de la face interne de joue: propos de
748 malades. J Eur Radiother 1985; 6: 1-4.
3. Gerbaulet A, Haie-Meder C, Marsiglia H, et al. Role of brachytherapy in the treatment of
Head & Neck cancer. Ed: Mould RF, Battermann JJ, Martinez A, et al. In: Brachytherapy
from radium to optimisation 1994; 101-20.
4. Gerbaulet A, Maher M. Brachytherapy in the treatment of head and neck cancer. In Joslin
CAF, Flynn A, Hall EJ (eds.) Principles and practice of brachytherapy 2001; London: Arnold,
284-95.
5. Lapeyre M, Peiffert D, Malissard L, et al. An original technique of brachytherapy in the
treatment of epidermoid carcinoma of the buccal mucosa. Int J Radiat Oncol Biol Phys 1995;
33: 447-54.
6. Nair MK, Sankaranarayanan R, Padmanabhan TK. Evaluation of the role of radiotherapy in
the management of carcinoma of the buccal mucosa. Cancer 1988; 61: 1326-31.
7. Pernot M, Hoffstetter S, Peiffert D, Aletti P. Role of interstitial brachytherapy in oral and
oropharyngeal carcinoma: Reflection of a series of 1344 patients treated at the time of initial
presentation. Otolaryngol Head Neck Surg 1996; 115: 519-26.
8. Rice DH, Spiro HR. Current concepts in head and neck cancers. American Cancer Society
1989; 141.
9. Sakai M, Hatano K, Sekiya Y, et al. Radiotherapy for carcinoma of the buccal mucosa:
analysis of the prognostic factors. Nippon Igaku Hoshasen Gakkai Zasshi 1998; 98: 705-11.
10. Shibuya H, Takeda M, Matsumoto S, et al. Brachytherapy for non metastatic squamous cell
carcinoma of the buccal mucosa. An analysis of forty-five cases treated with permanent
implants. Acta Oncol 1993; 32: 327-30.
11. Takeda M, Shibuya H, Inoue T. The efficacy of gold-198 grain mould therapy for mucosal
carcinomas of the oral cavity. Acta Oncol 1996; 35 (4): 463-7.
12. Urist MM, OBrien CJ, Soong SJ, et al. Squamous cell carcinoma of the buccal mucosa:
analysis of prognostic factors. Am J Surg 1987; 154: 411-4.
13. Vegers JW, Snow GB, Van der Waal I. Squamous cell carcinoma of the buccal mucosa. A
review of 85 cases. Ann Otolaryngol 1979; 105: 192-5.
Das könnte Ihnen auch gefallen
- Lateral RhinotomyDokument11 SeitenLateral RhinotomyDiaz RandanilNoch keine Bewertungen
- LipCancer BrachyDokument10 SeitenLipCancer Brachyarungoel2Noch keine Bewertungen
- 13) Traitement Chirurgical Des Cancers de La Cavité BuccaleDokument6 Seiten13) Traitement Chirurgical Des Cancers de La Cavité BuccalebekkouchealiwalidNoch keine Bewertungen
- Surgical Treatment of Oral Cavity CancersDokument6 SeitenSurgical Treatment of Oral Cavity CancersbekkouchealiwalidNoch keine Bewertungen
- Floor of The Mouth Resection SprianoDokument10 SeitenFloor of The Mouth Resection SprianoMeni HolcbergNoch keine Bewertungen
- Figure 1A: Dr. William BruggeDokument5 SeitenFigure 1A: Dr. William BruggeAbrar SabawiNoch keine Bewertungen
- MastopexyDokument10 SeitenMastopexyMei WanNoch keine Bewertungen
- Transoral Laser Microsurgery in Carcinomas of The Oral Cavity, Pharynx, and LarynxDokument8 SeitenTransoral Laser Microsurgery in Carcinomas of The Oral Cavity, Pharynx, and LarynxKiana TehraniNoch keine Bewertungen
- ABC - Oral CancerDokument4 SeitenABC - Oral Cancerdewishinta12Noch keine Bewertungen
- Maxillectomy A ReviewDokument17 SeitenMaxillectomy A ReviewDr. T. Balasubramanian100% (3)
- Carcinoma Maxillary Sinus : of TheDokument6 SeitenCarcinoma Maxillary Sinus : of TheInesNoch keine Bewertungen
- Rinotomi LateralDokument5 SeitenRinotomi Lateralyunia chairunnisaNoch keine Bewertungen
- Parotidectomy For Benign Parotid Tumors: An Aesthetic ApproachDokument6 SeitenParotidectomy For Benign Parotid Tumors: An Aesthetic ApproachamelNoch keine Bewertungen
- Lateral Antrostomy For Max Sinus AugmentationDokument9 SeitenLateral Antrostomy For Max Sinus AugmentationsevattapillaiNoch keine Bewertungen
- Marsupialization of Keratocystic Odontogenic Tumors of The Mandible: Longitudinal Image Analysis of Tumor Size Via 3D Visualized CT ScansDokument14 SeitenMarsupialization of Keratocystic Odontogenic Tumors of The Mandible: Longitudinal Image Analysis of Tumor Size Via 3D Visualized CT ScansAndreas SimamoraNoch keine Bewertungen
- Journal: Nursing Leadership and ManagementDokument9 SeitenJournal: Nursing Leadership and ManagementdaliaNoch keine Bewertungen
- Oncological Safety of Prophylactic Breast Surgery: Skin-Sparing and Nipple-Sparing Versus Total MastectomyDokument9 SeitenOncological Safety of Prophylactic Breast Surgery: Skin-Sparing and Nipple-Sparing Versus Total MastectomynariecaNoch keine Bewertungen
- Maxilectomia TotalDokument18 SeitenMaxilectomia TotalmonitosmaxilosNoch keine Bewertungen
- Review Article: Intersphincteric Resection and Coloanal Anastomosis in Treatment of Distal Rectal CancerDokument10 SeitenReview Article: Intersphincteric Resection and Coloanal Anastomosis in Treatment of Distal Rectal CancerJaysonGarabilesEspejoNoch keine Bewertungen
- Early Breast Cancer TherapyDokument20 SeitenEarly Breast Cancer TherapyIpseet MishraNoch keine Bewertungen
- Imaging Features of Salivary Gland TumoursDokument11 SeitenImaging Features of Salivary Gland TumourskaryndpNoch keine Bewertungen
- Parasagittal MeningiomaDokument51 SeitenParasagittal MeningiomaAji Setia UtamaNoch keine Bewertungen
- 2016 Article 124Dokument7 Seiten2016 Article 124Debbie LanceroNoch keine Bewertungen
- PIIS027823911400576XDokument15 SeitenPIIS027823911400576XRudnapon AmornlaksananonNoch keine Bewertungen
- Healthcare 01 00084Dokument12 SeitenHealthcare 01 00084svrobertNoch keine Bewertungen
- Malignant Melanoma Beyond The Basics.42Dokument11 SeitenMalignant Melanoma Beyond The Basics.42andrew kilshawNoch keine Bewertungen
- Radioguided Sentinel Lymph Node Biopsy in Breast Cancer SurgeryDokument18 SeitenRadioguided Sentinel Lymph Node Biopsy in Breast Cancer Surgerybickxy_katiNoch keine Bewertungen
- 6 Neck DissectionDokument9 Seiten6 Neck DissectionAnne MarieNoch keine Bewertungen
- 6 The Paranasal SinusesDokument4 Seiten6 The Paranasal SinusesjorgeaznarNoch keine Bewertungen
- Principles Of Managing Soft Tissue SarcomasDokument33 SeitenPrinciples Of Managing Soft Tissue Sarcomasbashiruaminu100% (1)
- Wa0007.Dokument31 SeitenWa0007.hectordan.montes93Noch keine Bewertungen
- Article. Rectal Carcinoma-Imaging For Staging (2018)Dokument31 SeitenArticle. Rectal Carcinoma-Imaging For Staging (2018)Trí Cương NguyễnNoch keine Bewertungen
- Management of Cancer of The Retromolar Trigone: Eric M. Genden, Alfio Ferlito, Ashok R. Shaha, Alessandra RinaldoDokument5 SeitenManagement of Cancer of The Retromolar Trigone: Eric M. Genden, Alfio Ferlito, Ashok R. Shaha, Alessandra RinaldoGirish SubashNoch keine Bewertungen
- Articles Related To Submental FlapDokument8 SeitenArticles Related To Submental FlapDipti PatilNoch keine Bewertungen
- PIIS1064968921006942Dokument20 SeitenPIIS1064968921006942Monik AlamandaNoch keine Bewertungen
- Primary Vaginal Melanoma: About Two Cases Treated by RadiotherapyDokument5 SeitenPrimary Vaginal Melanoma: About Two Cases Treated by RadiotherapyIJAR JOURNALNoch keine Bewertungen
- Group 5 FinalDokument11 SeitenGroup 5 Finalapi-404851310Noch keine Bewertungen
- Compartmental Surgery in Tongue Tumours: Description of A New Surgical TechniqueDokument6 SeitenCompartmental Surgery in Tongue Tumours: Description of A New Surgical TechniqueDot DitNoch keine Bewertungen
- Debulking Surgery On Recurrent Dermal Neck Tumor Above Stoma After Total LaryngectomyDokument9 SeitenDebulking Surgery On Recurrent Dermal Neck Tumor Above Stoma After Total LaryngectomyTeuku Ahmad HasanyNoch keine Bewertungen
- Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, And Endodontology Volume 93 Issue 1 2002 [Doi 10.1067_moe.2002.119519] Norbert Jakse; Vedat Bankaoglu; Gernot Wimmer; Antranik Eskici; -- Primary WounDokument6 SeitenOral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, And Endodontology Volume 93 Issue 1 2002 [Doi 10.1067_moe.2002.119519] Norbert Jakse; Vedat Bankaoglu; Gernot Wimmer; Antranik Eskici; -- Primary WounMr-Ton DrgNoch keine Bewertungen
- Artigo 4Dokument6 SeitenArtigo 4gdaraujoNoch keine Bewertungen
- Eyelid Cancer by Skin Cancer FoundationDokument5 SeitenEyelid Cancer by Skin Cancer Foundationamrita90031Noch keine Bewertungen
- Clough K Oncoplasty BJSDokument7 SeitenClough K Oncoplasty BJSkomlanihou_890233161Noch keine Bewertungen
- Transcutaneous Transfacial Approaches To The Anterior Skull BaseDokument4 SeitenTranscutaneous Transfacial Approaches To The Anterior Skull Basequesti0neverythin9Noch keine Bewertungen
- Case Report: Modified and Grafted Coronectomy: A New Technique and A Case Report With Two-Year FollowupDokument7 SeitenCase Report: Modified and Grafted Coronectomy: A New Technique and A Case Report With Two-Year FollowupMuhammad ArifNoch keine Bewertungen
- 5.1 Treatment of Stage I and II (Early) Head and Neck Cancer - The Oral Cavity - UpToDateDokument30 Seiten5.1 Treatment of Stage I and II (Early) Head and Neck Cancer - The Oral Cavity - UpToDateMarco GornattiNoch keine Bewertungen
- Dsa510 PDFDokument22 SeitenDsa510 PDFkadinfathiaNoch keine Bewertungen
- Wide Field of Cancerization Case Report: February 2017Dokument5 SeitenWide Field of Cancerization Case Report: February 2017Mira AnggrianiNoch keine Bewertungen
- JC TopicDokument6 SeitenJC Topicवाधूलं कण्णन् कुमारस्वामिNoch keine Bewertungen
- Reporte de Casos de MixomaDokument8 SeitenReporte de Casos de Mixomacirugia.maxilo.melendezNoch keine Bewertungen
- Abdominal OperationDokument9 SeitenAbdominal OperationRaissaNoch keine Bewertungen
- Carcinoma Buccal Mucosa: Dr. Abhilash G JR-3Dokument47 SeitenCarcinoma Buccal Mucosa: Dr. Abhilash G JR-3LingeshNoch keine Bewertungen
- Ba So CelularDokument13 SeitenBa So CelularMihaela BubulacNoch keine Bewertungen
- Post-Burn Neck Reconstruction with Supraclavicular Artery Perforator FlapDokument6 SeitenPost-Burn Neck Reconstruction with Supraclavicular Artery Perforator Flapfabian hernandez medinaNoch keine Bewertungen
- Chapter 14A Pituitary Adenomas and CraniopharyngiomasDokument8 SeitenChapter 14A Pituitary Adenomas and CraniopharyngiomasMohammad Ali IsmailNoch keine Bewertungen
- Omentum OverlayDokument10 SeitenOmentum OverlayAlin MihetiuNoch keine Bewertungen
- The Use of Single Stapling Techniques Reduces Anastomotic Complications in Minimal Invasive Rectal SurgeryDokument9 SeitenThe Use of Single Stapling Techniques Reduces Anastomotic Complications in Minimal Invasive Rectal SurgeryHafidh HanifuddinNoch keine Bewertungen
- Reconstructive Rhinoplasty in Cases With Basal Cell Carcinoma of The NoseDokument6 SeitenReconstructive Rhinoplasty in Cases With Basal Cell Carcinoma of The NoseRaisa KhairuniNoch keine Bewertungen
- Assisted Laparoscopic Rectal Dissection Through Transanal Endoluminal VideoendoscopyDokument3 SeitenAssisted Laparoscopic Rectal Dissection Through Transanal Endoluminal VideoendoscopyPallavi SutarNoch keine Bewertungen
- Defenition and Classification of Cahexia Cancer PDFDokument7 SeitenDefenition and Classification of Cahexia Cancer PDFmuhammad_ariefNoch keine Bewertungen
- Data HIV KemenkesDokument5 SeitenData HIV Kemenkesmuhammad_ariefNoch keine Bewertungen
- Pi Is 0091674918312788Dokument31 SeitenPi Is 0091674918312788muhammad_ariefNoch keine Bewertungen
- Pneumonia Severity Index in Viral Community Acquired Pneumonia in AdultsDokument12 SeitenPneumonia Severity Index in Viral Community Acquired Pneumonia in Adultsmuhammad_ariefNoch keine Bewertungen
- Blood TransfusionDokument7 SeitenBlood Transfusionmuhammad_ariefNoch keine Bewertungen
- Diphtheria Guidelines FinalDokument47 SeitenDiphtheria Guidelines Finalmuhammad_ariefNoch keine Bewertungen
- Surgical Fixation of Rib Fractures 2013Dokument8 SeitenSurgical Fixation of Rib Fractures 2013muhammad_ariefNoch keine Bewertungen
- Impact of Intermittent Fasting On Health and Disease Processes PDFDokument13 SeitenImpact of Intermittent Fasting On Health and Disease Processes PDFmuhammad_ariefNoch keine Bewertungen
- Direct-acting antivirals do not increase HCC risk after HCV cureDokument25 SeitenDirect-acting antivirals do not increase HCC risk after HCV curemuhammad_ariefNoch keine Bewertungen
- CamScanner Scanned Document PagesDokument23 SeitenCamScanner Scanned Document Pagesmuhammad_ariefNoch keine Bewertungen
- Reducing Risks of Sudden Death in Epilepsy PatientsDokument13 SeitenReducing Risks of Sudden Death in Epilepsy Patientsmuhammad_ariefNoch keine Bewertungen
- Appi Ajp 2009 09070931Dokument10 SeitenAppi Ajp 2009 09070931muhammad_ariefNoch keine Bewertungen
- Contraceptive Methods 508Dokument1 SeiteContraceptive Methods 508Cynthia AyuPermatasariNoch keine Bewertungen
- Jurnal OMSKDokument23 SeitenJurnal OMSKmuhammad_ariefNoch keine Bewertungen
- Pebruari 2017Dokument5 SeitenPebruari 2017muhammad_ariefNoch keine Bewertungen
- Cough, Sputum HemoptisisDokument36 SeitenCough, Sputum Hemoptisismuhammad_ariefNoch keine Bewertungen
- CHF (Diagnosis, Patophysiology, Therapy, and Implication For Respiratory Care)Dokument10 SeitenCHF (Diagnosis, Patophysiology, Therapy, and Implication For Respiratory Care)blobfish_danboNoch keine Bewertungen
- Approach To InterpretationDokument164 SeitenApproach To Interpretationmuhammad_ariefNoch keine Bewertungen
- CHF (Diagnosis, Patophysiology, Therapy, and Implication For Respiratory Care)Dokument10 SeitenCHF (Diagnosis, Patophysiology, Therapy, and Implication For Respiratory Care)blobfish_danboNoch keine Bewertungen
- CHF (Diagnosis, Patophysiology, Therapy, and Implication For Respiratory Care)Dokument10 SeitenCHF (Diagnosis, Patophysiology, Therapy, and Implication For Respiratory Care)blobfish_danboNoch keine Bewertungen
- Sterilization and DisinfectionDokument41 SeitenSterilization and DisinfectionqiotenseiNoch keine Bewertungen
- Pehealth11 q2 Mod2of2 H.O.P.E v2Dokument26 SeitenPehealth11 q2 Mod2of2 H.O.P.E v2Avillz Mar LeeNoch keine Bewertungen
- DNV Publication ListDokument14 SeitenDNV Publication ListmohammadazraiNoch keine Bewertungen
- Lab Manual - General Chemistry (Spring 2019)Dokument83 SeitenLab Manual - General Chemistry (Spring 2019)jinri sandeulNoch keine Bewertungen
- LakesDokument14 SeitenLakesmanwartejam8Noch keine Bewertungen
- MR Safe Conditional PDFDokument4 SeitenMR Safe Conditional PDFAKSNoch keine Bewertungen
- Dentwiton Company Profile (En) 20221019-V2.1Dokument20 SeitenDentwiton Company Profile (En) 20221019-V2.1BRAIS FREIRÍA LORENZONoch keine Bewertungen
- Homework 1Dokument10 SeitenHomework 1Nam Anh KiraiNoch keine Bewertungen
- Brake Accumulator Test and ChargeDokument8 SeitenBrake Accumulator Test and ChargeBarzola Soto Omar100% (1)
- Presentation TranscriptDokument2 SeitenPresentation TranscriptHaile SilasieNoch keine Bewertungen
- 07a1bs07 Engineering ChemistryDokument7 Seiten07a1bs07 Engineering ChemistrychemistrymasterNoch keine Bewertungen
- Manual Reparatii Audi A2 1.6 FSI PDFDokument104 SeitenManual Reparatii Audi A2 1.6 FSI PDFferentz u100% (1)
- How To Make Waffles - Recipes - Waffle RecipeDokument5 SeitenHow To Make Waffles - Recipes - Waffle RecipeJug_HustlerNoch keine Bewertungen
- Foundations of Special and Inclusive EducationDokument24 SeitenFoundations of Special and Inclusive EducationStephanie Garciano94% (53)
- Bearing From Copper AlloyDokument7 SeitenBearing From Copper AlloyPhung Tuan AnhNoch keine Bewertungen
- Bams 1st Rachna Sharir Joints and Their Classification 16-05-2020Dokument15 SeitenBams 1st Rachna Sharir Joints and Their Classification 16-05-2020Sanjana SajjanarNoch keine Bewertungen
- Cell Membrane TransportDokument37 SeitenCell Membrane TransportMaya AwadNoch keine Bewertungen
- Ig2 of Bikas 00691520 x123Dokument20 SeitenIg2 of Bikas 00691520 x123Engr. Imran Hasan Pathan100% (4)
- Extent of Compliance on Waste Disposal PracticesDokument13 SeitenExtent of Compliance on Waste Disposal PracticesEzza Jean Paypa100% (3)
- Qhse Induction ModuleDokument20 SeitenQhse Induction Modulerahul kumarNoch keine Bewertungen
- Water Plant SOPDokument6 SeitenWater Plant SOPIndrie AgustinaNoch keine Bewertungen
- Endangered Species Lesson PlanDokument5 SeitenEndangered Species Lesson PlanIrena Stamenova100% (1)
- Term Paper Envl 4300 Ac 1Dokument18 SeitenTerm Paper Envl 4300 Ac 1api-693796798Noch keine Bewertungen
- Anaphylaxis and Epinephrine Auto-InjectorDokument7 SeitenAnaphylaxis and Epinephrine Auto-Injectorqueennita69Noch keine Bewertungen
- 17 Quarter 1 Module 17-ANAEROBICDokument20 Seiten17 Quarter 1 Module 17-ANAEROBICMah Jane DivinaNoch keine Bewertungen
- TRILOGY Product BrochureDokument8 SeitenTRILOGY Product BrochureMarina JankovicNoch keine Bewertungen
- Aafreen Project Report SIPDokument19 SeitenAafreen Project Report SIPshubham moonNoch keine Bewertungen
- Apartments in Trivandrum - Flats in Trivandrum - Heather HomesDokument6 SeitenApartments in Trivandrum - Flats in Trivandrum - Heather Homescresto indiaNoch keine Bewertungen
- Ficha Tecnica Sonometro Artisan SL2100PSDokument1 SeiteFicha Tecnica Sonometro Artisan SL2100PSJackson Steward Ríos SastoqueNoch keine Bewertungen
- 2018-06-21 Calvert County TimesDokument24 Seiten2018-06-21 Calvert County TimesSouthern Maryland OnlineNoch keine Bewertungen







































![Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, And Endodontology Volume 93 Issue 1 2002 [Doi 10.1067_moe.2002.119519] Norbert Jakse; Vedat Bankaoglu; Gernot Wimmer; Antranik Eskici; -- Primary Woun](https://imgv2-2-f.scribdassets.com/img/document/224676744/149x198/8c2fa96a30/1400316861?v=1)


































































