Beruflich Dokumente
Kultur Dokumente
BR J Ophthalmol 2001 Falkner 1324 7
Hochgeladen von
PrissilmaTaniaOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
BR J Ophthalmol 2001 Falkner 1324 7
Hochgeladen von
PrissilmaTaniaCopyright:
Verfügbare Formate
Downloaded from http://bjo.bmj.com/ on February 17, 2016 - Published by group.bmj.
com
1324
Br J Ophthalmol 2001;85:13241327
Outcome after silicone oil removal
Christiane I Falkner, Susanne Binder, Andreas Kruger
The Ludwig
Boltzmann Institute of
Retinology and
Biomicroscopic
Lasersurgery,
Department of
Ophthalmology, Rudolf
Foundation Clinic,
Juchgasse 25, A 1030
Vienna, Austria
C I Falkner
Department of
Ophthalmology, Rudolf
Foundation Clinic,
Juchgasse 25, A 1030
Vienna, Austria
S Binder
Department of
Ophthalmology,
Vienna General
Hospital,
Whringergrtel
1820, A 1090, Vienna,
Austria
A Kruger
Correspondence to:
Christiane I Falkner, MD
a9101872@unet.univie.ac.at
Accepted for publication
16 April 2001
Abstract
BackgroundCombined with vitreoretinal surgery, silicone oil injection has
become a standard technique and improves the prognosis of complex retinal
detachment. As silicone oil leads to long
term complications, removal of silicone
oil from the eye is recommended. To
evaluate the outcome after silicone oil
removal, retinal redetachment, visual
acuity, and complications were analysed.
MethodsThe authors analysed 115 consecutive cases of silicone oil removal (115
eyes), all operated by one surgeon. The
series consisted of retinal detachments
associated with proliferative vitreoretinopathy (103 eyes), proliferative diabetic
retinopathy (six eyes), or ocular trauma
(six eyes). The mean duration of intraocular silicone oil tamponade was 13.3
months, with a mean postoperative follow
up of 1.8 years.
ResultsAnatomic success after silicone
oil removal, defined as a complete retinal
attachment, was achieved in 95 of 115 eyes
(82.6%). Redetachment occurred in 20
eyes (17.4%), mostly within the first 6
months after silicone oil removal. Including the successfully reoperated eyes, the
authors present a final anatomic success
rate of 108 eyes (93.9%). Visual acuity
improved or remained unchanged in 93
eyes (80.9%).
ConclusionWhile reattachment and
complication rates were quite similar to
other studies, a better visual outcome was
achieved in these cases. The duration of
the silicone oil tamponade had no significant eVect on the reattachment rate. The
authors recommend not to apply standard
criteria for the timing of silicone oil
removal, but to decide individually, considering the underlying disease, as well as
the previous operations.
(Br J Ophthalmol 2001;85:13241327)
The use of silicone oil for the treatment of
otherwise inoperable retinal detachments was
first described by Cibis et al in 1962.1 Scott2
and Zivojnovic3 modified this technique, and
encouraging results were reported by many
other surgeons.48 Combined with vitreoretinal
surgery, silicone oil injection has become a
standard technique and improves the prognosis of complex retinal detachment associated
with proliferative vitreoretinopathy, giant retinal tears, proliferative diabetic retinopathy, or
ocular trauma. Compared with sulphur hexafluoride gas (SF6) as an intraocular tamponade for the management of retinal detachment,
eyes treated with silicone oil were more likely
www.bjophthalmol.com
to be successfully reattached, to achieve a better visual acuity, and to have fewer postoperative complications.911 However, silicone oil
leads to long term complications particularly
cataract, glaucoma, and keratopathy.5 7 12 13
Therefore several authors have recommended
the removal of silicone oil from the eye as soon
as a stable retinal situation is achieved.1417 Silicone oil removal is a procedure that carries a
definite risk of retinal redetachment, due to
reproliferation of epiretinal membranes and
increasing traction on the retina. In this report
we present the results of 115 eyes that
underwent modern pars plana vitrectomy and
silicone oil removal. Visual acuity, the incidence and development of complications like
cataract, hypertony or hypotony, keratopathy,
and retinal detachment were analysed to evaluate the outcome after silicone oil removal.
Patients and methods
We reviewed the records of 115 eyes of 115
consecutive patients who underwent silicone
oil removal between 1989 and 1999. All
surgery was performed by one surgeon (SB).
This series included 54 male patients (47%)
and 61 female patients (53%). The average age
of the patients at the time of surgery was 54.9
years, with the range between 13 and 83 years.
The indications for the use of silicone oil
were complex retinal detachments associated
with proliferative vitreoretinopathy (103 eyes,
89.2%), proliferative diabetic retinopathy (six
eyes, 5.4%) or ocular trauma (six eyes, 5.4%).
Cases with proliferative vitreoretinopathy
(PVR) showed various secondary diagnoses
(Fig 1). The PVR grading of our early cases
was done according to the Retina Society
classification of 1983.18 This group consisted of
66 eyes, with three eyes graded C3 and 63 eyes
graded D. The other 37 eyes were graded
according to the updated classification by
Machemer et al.19 In this group we found nine
cases graded C1, nine cases C2, and 19 cases
C3. All patients had previously undergone pars
plana vitrectomy combined with dissection of
epiretinal membranes, intraocular silicone oil
injection, and argon laser endophotocoagulation. In some cases additional perfluorocarbon
installation was performed. As a standard procedure in our clinic, aphakic eyes received inferior peripheral iridectomies to prevent pupillary block glaucoma. All eyes had been filled
with highly purified silicone oil with a viscosity
of 5000 centistokes. Many patients, particularly those with proliferative vitreoretinopathy,
had had other surgical procedures before the
silicone oil injection. Some of these procedures
were not administered in our clinic and therefore could not be reviewed. The duration of
intraocular silicone oil tamponade ranged from
1 month to 96 months, with a mean of 13.3
Downloaded from http://bjo.bmj.com/ on February 17, 2016 - Published by group.bmj.com
1325
Outcome after silicone oil removal
50
46
40
30
21
20
17
9
10
6
2
2
0
Pseudophakia
Figure 1
High
myopia
Giant
tears
Myopic
Glaucoma
macular holes
100
Others
Secondary diagnoses of the proliferative vitreoretinopathy cases.
120
110
Idiopathic
115
Total
Attached
103
95
86
90
80
70
60
50
40
30
20
10
0
Ocular trauma
3
PDR
PVR
All cases
Figure 2 Attachment rate after silicone oil removal (PDR = proliferative diabetic
retinopathy; PVR = proliferative vitreoretinopathy).
months. The criteria for silicone oil removal
were a complete and stable attached retina
within the encircling buckle and no active proliferative process or traction on the retina.
The oil was removed in vitrectomy technique via two sclerotomies under the binocular
ophthalmoscope and under fundus control. A
vacuum pump was used in all cases. In 11 cases
silicone oil removal was combined with cataract extraction and intraocular lens implantation. All patients had ocular examinations
before silicone oil removal, postoperatively and
at each follow up visit. These examinations
included best corrected visual acuity testing
using a Snellen eye chart, measurement of
intraocular pressure, slit lamp biomicroscopy,
and fundus control with direct (three mirror
contact lens) and indirect ophthalmoscopy.
There was a mean postoperative follow up
period of 1.8 years, ranging from 6 months to
3.5 years.
Results
Anatomic success after silicone oil removal,
defined as a flat retina with complete retinal
attachment anterior and posterior to the
buckle for a minimum of 6 months, was
achieved in 95 of 115 eyes (82.6%). Retinal
detachments anterior to the buckle stabilised
by laser coagulation were considered anatomic
failures. Retinal redetachment occurred in 20
eyes (17.4%). While no redetachment was seen
www.bjophthalmol.com
in the six eyes with primary ocular trauma, 17
of 103 eyes (16.5%) suVering from proliferative vitreoretinopathy (PVR), and three of six
eyes (50%) with proliferative diabetic retinopathy (PDR) presented retinal redetachment
(Fig 2). The mean duration of silicone oil tamponade in the attached group was 14.2 months
and in the redetached group 12.3 months.
Using the unpaired two tailed t test we found
no significant diVerence between the attached
group and the redetached group regarding the
duration of silicone oil tamponade (p =
0.82202).
We additionally compared two groups defined by the duration of silicone oil tamponade
(group 1: silicone oil tamponade for less than 6
months; group 2: silicone oil tamponade for
more than 6 months). Using the two tailed
Fishers exact test we found no significant difference (p = 0.70214) in the numbers of stable
and redetached cases in these two groups.
However, we discovered a diVerence between the attached and the redetached group
regarding the number of total operations.
Including the available data of previous operations we found a mean of 3.4 operations (range
26) in the redetached group and a mean of
1.8 operations (range 14) in the attached
group.
Redetachments occurred mainly within the
first 3 months. We found six redetachments
(30%) within the first postoperative month and
another eight (40%) within 3 months after silicone oil removal. Five patients (25%) developed a redetachment after 6 months and only
one patient (5%) after 16 months. All 20 eyes
were reoperated. In 15 eyes revision surgery
consisted of revitrectomy with replacement of
silicone oil. Revitrectomy with temporary
perfluorocarbon installation and intraocular
gas injection was successfully performed in
three eyes, cryotherapy and additional scleral
buckling in two cases. A stable reattached
retina was achieved in 13 of these 20 eyes
(65%), while seven eyes (35%) remained
uncured. Including the successfully reoperated
eyes, we present a final anatomic success rate of
93.9% (108 of 115 eyes).
Cataract formation was observed in 44 of 68
phakic eyes (64.7%), mostly within the first
postoperative year. In 34 eyes cataract extraction and implantation of a posterior chamber
lens was performed. In 11 of these patients
cataract surgery was combined with silicone oil
removal to improve the functional rehabilitation.
During silicone oil tamponade, elevated
intraocular pressure (IOP), higher than 21 mm
Hg, occurred in 54 eyes (46.9%). After silicone
oil removal, these temporary changes normalised in all but 14 patients (12.2%), who developed secondary glaucoma. Eight eyes were
treated successfully with antiglaucomatous
medication and six eyes needed a surgical procedure. A temporary hypotony with an IOP of
less than 8 mm Hg was seen in four patients
(3.5%).
Nine eyes (7.8%) demonstrated a postoperative keratopathy. In seven of these eyes, the
keratopathy disappeared within a few weeks,
Downloaded from http://bjo.bmj.com/ on February 17, 2016 - Published by group.bmj.com
1326
Falkner, Binder, Kruger
70
61
60
50
40
28
30
20
15
8
10
3
0
Figure 3
6/7
6/126/60
3/601/40
CF, HM
LP
Visual acuity at the last follow up examination (Snellen eye chart).
whereas the remaining two eyes required a
penetrating keratoplasty. Other complications
were intravitreal haemorrhage in five eyes
(4.3%), optic atrophy in four eyes (3.5%), and
phthisis in one eye (0.9%). No enucleation for
intractable chronic ocular pain was necessary.
To analyse the course of visual acuity (VA)
we compared the mean best corrected VA during silicone oil tamponade (6/60) with the
mean best corrected VA at the last follow up
visit (6/30). An increase of VA was combined
with continued improvement in retinal function after successful retinal reattachment, cataract extraction, and reduced optical eVects of
the silicone oil bubble after oil removal. Eyes
were only graded as improved or deteriorated
when VA changed two or more lines using the
Snellen eye chart. VA following silicone oil
removal, including eyes with retinal redetachment, improved in 62 cases (53.9%), remained
unchanged in 31 eyes (27%), and worsened in
22 eyes (19.1%). The visual loss was related to
the development of retinal redetachment, cataract, glaucoma, optic atrophy, keratopathy, vitreous haemorrhage, or a combination of two or
more of these complications. The final functional success rate with a minimum visual acuity of 1/40 was achieved in 92 patients (80%).
At the last follow up visit three patients (2.6%)
had a visual acuity of 6/7, 61 patients (53%) a
VA between 6/12 and 6/60, and 28 patients
(24.4%) showed a VA between 3/60 and 1/40.
In 15 patients (13%) the VA was counting fingers and hand movements and in eight patients
(7%) light perception (Fig 3).
Discussion
The reported incidence of redetachment varies
between 0% and 32%.48 12 1417 2025 This variation is most probably due to marked diVerences in the number of eyes studied, the duration of follow up after silicone oil removal, and
the underlying diseases. In our series retinal
redetachment after silicone oil removal occurred in 20 of 115 eyes (17.4%), while the
final anatomic failure rate was 6.1%. Other
authors report similar results6 21 25 or higher
failure rates.26 No conclusions can be drawn
from the high rate of redetachments in our
PDR group because of the small number of
cases.
www.bjophthalmol.com
Rates of anterior segment complications described in literature range from 34.5% to 100%
regarding cataract formation,57 12 14 15 17 22 26 27
and from 1.5% to 27.7% regarding elevated
IOP.47 1117 20 21 27 28 These results are comparable
with our findings (cataract 64.7%, elevated IOP
12.2%).
Rates of keratopathy were reported to
range from 4.5% to 63%48 12 1417 22 27 28 while
rates of hypotony vary between 5% and
51.4%.4 6 8 1416 21 22 27 Regarding these numbers, our rates definitely lie within the lower
segment (keratopathy 7.8%, hypotony 3.5%).
A better visual outcome was achieved in our
study. We had more patients with 6/60 or better postoperative VA than reported by others4 5 16 and more patients had an increased or
unchanged VA at the last follow up
visit.8 17 21 22 27 28 Stolba et al stated that a VA
between 6/60 and 6/20 is essential for total or
partial binocularity.29 This range of VA was
achieved in 63 of our 115 cases (54.8%). Cataract extraction and atraumatic surgery, paying
special attention to the foveal area, may be
reasons for the good functional outcome.
The optimal timing for the silicone oil
removal still remains unknown and recommendations range from 3 to 6 months of sustained
retinal attachment.15 16 In our series the duration of the silicone oil tamponade had no
significant eVect on the reattachment rate. We
have no fixed time limit for silicone oil removal.
We prefer to have the oil removed in all
patients, but we do not enforce removal if the
retina cannot be stabilised. We usually do not
remove the oil in unsuccessful cases with
detached retinas unless uncontrollable IOP as
a result of the silicone oil or other complications arises. A second silicone oil removal in
these eyes would be associated with an
increased risk of further redetachment, endless
surgical interventions, and a loss of quality of
life. We do not expect an improvement of VA
but a further loss of function.
Three to 6 months after silicone oil removal,
retinal redetachment generally becomes
unlikely.8 14 15 2124 This is important for scheduling re-examinations of the patients and we
therefore recommend close meshed controls
after silicone oil removalpostoperatively,
within the first week, every 2 weeks within the
first 3 months, every 36 weeks within the following 3 months, and afterwards every 6
months. This way, redetachments after silicone
oil removal can be discovered early and
brought under control in time. Incompletely
attached retinas can be stabilised without
silicone oil reinstillation by using extensive
laser photocoagulation, encircling bands, or
intraocular gas tamponade.
PVR, the major complication of retinal
detachment surgery, remains an unsolved
problem. The Daunomycin Study Group
examined the eYcacy of intraoperative application of daunorubicin in eyes with idiopathic
PVR. Daunorubicin is supposed to have a
positive eVect on the treatment of PVR by
reducing the number of reoperations and
increasing the reattachment rate.30 To improve
Downloaded from http://bjo.bmj.com/ on February 17, 2016 - Published by group.bmj.com
1327
Outcome after silicone oil removal
the outcome of complicated retinal redetachment in eyes with PVR, more studies and
research for drug combinations are necessary.
The success of silicone oil instillation seems
to depend on the number and quality of previous vitreoretinal surgical procedures, as seen in
our cases. Therefore, it is important to
carefully evaluate indications for all vitreoretinal procedures and to opt for definite treatment.
In conclusion, we recommend not to search
for standard criteria for the timing of silicone
oil removal but to evaluate each single case
individually. The underlying disease, as well as
the previous procedures determine the stability
of the retina. Close meshed and thorough
follow up examinations, especially in the first 3
months, are crucial to identify early signs of
reattachment. Although silicone oil tamponade
is the best yet available procedure for the treatment of complicated retinal detachment, we
hope that the pharmaceutical influence on
proliferative vitreoretinopathy will be further
evaluated.
1 Cibis PA, Becker B, Okun E, et al. The use of liquid silicone
in retinal detachment surgery. Arch Ophthalmol
1962;68:5909.
2 Scott JD. A rationale for the use of liquid silicone. Trans
Ophthalmol Soc UK 1977;97:2357.
3 Zivojnovic R, Mertens DA, Peperkamp E. Das flssige
Silikon in der Amotiochirurgie (II). Bericht ber 280
Flle-weitere Entwicklung der Technik. Klin Monatsbl
Augenheilkd 1982;181:44452.
4 McCuen BW, Landers MB, Machemer R. The use of
silicone oil following failed vitrectomy for retinal detachment with advanced proliferative vitreoretinopathy. Ophthalmology 1985;92:102934.
5 Dimopoulos ST, Heimann K. Sptkomplikationen nach
Silikonlinjektion. Langzeitbeobachtungen an 100 Fllen.
Klin Monatsbl Augenheilkd 1986;189:2237.
6 Luke K, Frster M, Laqua H. Langzeiterfahrungen mit
intraokularer Silikonl-Fllung. Fortschr Ophthalmol 1987;
84:968.
7 Federman JL, Schubert HD. Complications associated with
the use of silicone oil in 150 eyes after retina-vitreous surgery. Ophthalmology 1988;95:8706.
8 Azen SP, Scott IU, Flynn HW, et al. Silicone oil in the repair
of complex retinal detachments. A prospective observational multicenter study. Ophthalmology 1998;105:1587
97.
9 The Silicone Study Group. Vitrectomy with silicone oil or
sulfur hexaflouride gas in eyes with severe proliferative
vitreoretinopathy: results of randomized clinical trial:
Silicone Study Report 1. Arch Ophthalmol 1992;110:7709.
www.bjophthalmol.com
10 Abrams GW, Azen SP, McCuen BW, et al. Vitrectomy with
silicone oil or long acting gas in eyes with severe proliferative vitreoretinopathy: results of additional and long-term
follow-up. Silicone Study report 11. Arch Ophthalmol 1997;
115:33544.
11 Hammer M, Margo CE, Grizzard WS. Complex retinal
detachment treated with silicone oil or sulfur hexaflluoride
gas: a randomized clinical trial. Ophthalmic Surg Lasers
1997;28:92631.
12 Binder S, Velikay M, Zgner M, et al. Zum Sekundrglaukom nach Silikonlimplantation: Indikation, Technik und
Ergebnisse. Spektrum Augenheilkd 1988;2:2247.
13 Lucke K, Strobel B, Frster M, et al. Sekundrglaukome
nach Silikonlchirurgie. Klin Monatsbl Augenheilkd 1990;
196:2059.
14 Casswell AG, Gregor ZJ. Silicone oil removal. I. The eVect
on complications of silicone oil. Br J Ophthalmol 1987;71:
8937.
15 Casswell AG, Gregor ZJ. Silicone oil removal. II. Operative
and postoperative complications. Br J Ophthalmol 1987;71:
898902.
16 Zilis JD, McCuen BW, de Juan E, et al. Results of silicone oil
removal in advanced proliferative vitreoretinopathy. Am J
Ophthalmol 1989;108:1521.
17 Franks WA, Leaver PK. Removal of silicone oil-rewards and
penalties. Eye 1991;5:3337.
18 The Retina Society Terminology Committee. The classification of retinal detachment with proliferative vitreoretinopathy. Ophthalmology 1983;90:1215.
19 Machemer R, Aaberg TM, Freeman HM, et al. An updated
classification of retinal detachment with proliferative vitreoretinopathy. Am J Ophthalmol 1991;112:15965.
20 Pavlovic S, Dick B, Schmidt KG, et al. Langzeitergebnisse
nach Silikonlentfernung. Ophthalmologe 1995;92:6726.
21 Bodanowitz S, Hesse L, Poller S, et al. Management of retinal redetachment following silicone-oil removal. Ger J
Ophthalmol 1996;5:6772.
22 Scholda C, Egger S, Lakits A, et al. Silicone oil removal:
results, risks and complications. Acta Ophthalmol Scand
1997;75:6959.
23 Larkin GB, Flaxel CJ, Leaver PK. Phacoemulsification and
silicone oil removal through a single corneal incision. Ophthalmology 1998;105:20237.
24 Jonas JB, Budde WM, Knorr HL. Timing of retinal
redetachment after removal of intraocular silicone oil tamponade. Am J Ophthalmol 1999;128:62831.
25 Scholda C, Egger S, Lakits A, et al. Retinal redetachment
after silicone oil removal. Acta Ophthalmol Scand 2000;78:
1826.
26 Gonvers M. Temporary silicone oil tamponade in the treatment of complicated diabetic retinal detachments. Graefes
Arch Clin Exp Ophthalmol 1990;28:41522.
27 Hrle S, Schmidt J, Kroll P. Vitreoretinale Chirurgie bei
komplizierten Netzhautablsungen im Kindes- und Jugendalter. Ophtalmologe 2000;97:4826.
28 Wedrich A, Binder S, Velikay M, et al. Funktionelle und
anatomische Ergebnisse der Silikonlchirurgie bei proliferativer diabetischer Retinopathie. Spektrum Augenheilkd
1992;6:812.
29 Stolba U, Binder S, Krebs I, et al. Visual rehabilitation after
silicone oil removal. Poster presented at the Club Jules
Gonin 1998.
30 Wiedemann P, Hilgers RD, Bauer P, et al. Adjunctive
daunorubicin in the treatment of proliferative
vitreoretinopathy: results of a multicenter clinical trial.
Daunomycin Study Group. Am J Ophthalmol 1998;126:
5509.
Downloaded from http://bjo.bmj.com/ on February 17, 2016 - Published by group.bmj.com
Outcome after silicone oil removal
Christiane I Falkner, Susanne Binder and Andreas Kruger
Br J Ophthalmol 2001 85: 1324-1327
doi: 10.1136/bjo.85.11.1324
Updated information and services can be found at:
http://bjo.bmj.com/content/85/11/1324
These include:
References
Email alerting
service
Topic
Collections
This article cites 26 articles, 2 of which you can access for free at:
http://bjo.bmj.com/content/85/11/1324#BIBL
Receive free email alerts when new articles cite this article. Sign up in the
box at the top right corner of the online article.
Articles on similar topics can be found in the following collections
Retina (1546)
Vitreous (146)
Notes
To request permissions go to:
http://group.bmj.com/group/rights-licensing/permissions
To order reprints go to:
http://journals.bmj.com/cgi/reprintform
To subscribe to BMJ go to:
http://group.bmj.com/subscribe/
Das könnte Ihnen auch gefallen
- Practical Handbook for Small-Gauge Vitrectomy: A Step-By-Step Introduction to Surgical TechniquesVon EverandPractical Handbook for Small-Gauge Vitrectomy: A Step-By-Step Introduction to Surgical TechniquesNoch keine Bewertungen
- Ghora Ba 2016Dokument8 SeitenGhora Ba 2016marlon GarcíaNoch keine Bewertungen
- Silicone Preretinal Retraction. Results: Oil in The in 105Dokument6 SeitenSilicone Preretinal Retraction. Results: Oil in The in 105Thiago FerreiraNoch keine Bewertungen
- Silicone Oil and Intraocular Pressure: Unraveling The Post-Vitrectomy RelationshipDokument8 SeitenSilicone Oil and Intraocular Pressure: Unraveling The Post-Vitrectomy RelationshipInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Jurnal 1Dokument6 SeitenJurnal 1r_ayuNoch keine Bewertungen
- Vitrectomy Results in Proliferative Diabetic RetinopathyDokument3 SeitenVitrectomy Results in Proliferative Diabetic RetinopathyRohamonangan TheresiaNoch keine Bewertungen
- Clinical Study: Exclusive Use of Air As Gas Tamponade in Rhegmatogenous Retinal DetachmentDokument5 SeitenClinical Study: Exclusive Use of Air As Gas Tamponade in Rhegmatogenous Retinal DetachmentYunita Maharani BurhanNoch keine Bewertungen
- Original Article Incidence and Risk Factors For Intraocular Pressure Rise After Transconjunctival VitrectomyDokument6 SeitenOriginal Article Incidence and Risk Factors For Intraocular Pressure Rise After Transconjunctival VitrectomyNur Azizah Intan Putri IsmailNoch keine Bewertungen
- OJOph 2016062717483031Dokument8 SeitenOJOph 2016062717483031dechastraNoch keine Bewertungen
- Retina 2012 Sep 32 (Suppl 2) S225-31Dokument7 SeitenRetina 2012 Sep 32 (Suppl 2) S225-31roro207Noch keine Bewertungen
- Surgical Outcomes of Rhegmatogenous Retinal Detachment Associated With Ocular ToxoplasmosisDokument5 SeitenSurgical Outcomes of Rhegmatogenous Retinal Detachment Associated With Ocular Toxoplasmosisketrin capanemaNoch keine Bewertungen
- Incidence of Ocular Hypertension Following Silicone OilDokument3 SeitenIncidence of Ocular Hypertension Following Silicone OilarturocerpaNoch keine Bewertungen
- BMC OphthalmologyDokument7 SeitenBMC OphthalmologyRizki Yuniar WNoch keine Bewertungen
- Clinical StudyDokument6 SeitenClinical StudyKarina Mega WNoch keine Bewertungen
- Clinical StudyDokument7 SeitenClinical StudyAndre AzharNoch keine Bewertungen
- Therapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismDokument7 SeitenTherapeutic Effectiveness of Toric Implantable Collamer Lens in Treating Ultrahigh Myopic AstigmatismStephanie PfengNoch keine Bewertungen
- Shankar Ganvit END PDFDokument4 SeitenShankar Ganvit END PDFgyogi1989Noch keine Bewertungen
- Cuatro Tecnicas QuirurgicasDokument5 SeitenCuatro Tecnicas QuirurgicasmardocoftNoch keine Bewertungen
- Single-Step Transepithelial PHDokument9 SeitenSingle-Step Transepithelial PHlenniNoch keine Bewertungen
- Retinal Physician - Visualization in Vitrectomy - An UpdateDokument12 SeitenRetinal Physician - Visualization in Vitrectomy - An UpdateDr. M. Hannan JamilNoch keine Bewertungen
- Glaukoma TripleDokument5 SeitenGlaukoma TripleR.m. IrsanNoch keine Bewertungen
- The Effect of Trabeculectomy On Astigmatism .99150Dokument5 SeitenThe Effect of Trabeculectomy On Astigmatism .99150Yulias YoweiNoch keine Bewertungen
- Kag Rully (B.IG)Dokument7 SeitenKag Rully (B.IG)Rully Dwi SaputraNoch keine Bewertungen
- The Effectiveness of Laser Vitreolysis For Vitreous Floaters in Posterior Vitreous DetachmentDokument7 SeitenThe Effectiveness of Laser Vitreolysis For Vitreous Floaters in Posterior Vitreous Detachmentmistic0Noch keine Bewertungen
- Comparative Evaluation of Dry Eye Following Cataract Surgery: A Study From North IndiaDokument6 SeitenComparative Evaluation of Dry Eye Following Cataract Surgery: A Study From North IndiaInternational Organization of Scientific Research (IOSR)Noch keine Bewertungen
- Trabeculectomy With Mitomycin-C in Post-Traumatic Angle Recession Glaucoma in Phakic Eyes With No Prior Intraocular InterventionDokument7 SeitenTrabeculectomy With Mitomycin-C in Post-Traumatic Angle Recession Glaucoma in Phakic Eyes With No Prior Intraocular InterventionJennifer ChavezNoch keine Bewertungen
- The Course of Dry Eye After Phacoemulsification Surgery: Researcharticle Open AccessDokument5 SeitenThe Course of Dry Eye After Phacoemulsification Surgery: Researcharticle Open AccessDestia AnandaNoch keine Bewertungen
- Factor D Riesgo Glaucoma AfaquiaDokument6 SeitenFactor D Riesgo Glaucoma AfaquiaShirley M. Cerro RomeroNoch keine Bewertungen
- Effectiveness and Safety of The Clareon Monofocal Intraocular Lens: Outcomes From A 12-Month Single-Arm Clinical Study in A Large SampleDokument11 SeitenEffectiveness and Safety of The Clareon Monofocal Intraocular Lens: Outcomes From A 12-Month Single-Arm Clinical Study in A Large SampleHariom ShuklaNoch keine Bewertungen
- Long Term Outcome of Secondary Glaucoma Following Vitreoretinal SurgeryDokument3 SeitenLong Term Outcome of Secondary Glaucoma Following Vitreoretinal SurgeryNur Camelia PragnandaNoch keine Bewertungen
- Closed-Chamber Techniques For Iridodialysis Repair BMC 2018Dokument6 SeitenClosed-Chamber Techniques For Iridodialysis Repair BMC 2018Alexandre IshizakiNoch keine Bewertungen
- ABSTRACT - BOOK - 10th IcgsDokument135 SeitenABSTRACT - BOOK - 10th Icgsd_kourkoutasNoch keine Bewertungen
- Contact Lens and Anterior Eye: SciencedirectDokument4 SeitenContact Lens and Anterior Eye: SciencedirectMaricris Palacios VergaraNoch keine Bewertungen
- CMC - Tear Film StabilityDokument10 SeitenCMC - Tear Film StabilityTushar BatraNoch keine Bewertungen
- Timing of Quiescence and Uveitis Recurrences AfterDokument10 SeitenTiming of Quiescence and Uveitis Recurrences AfterFlor ArenasNoch keine Bewertungen
- Glaucoma After Lens-Sparing Vitrectomy For Advanced Retinopathy of PrematurityDokument6 SeitenGlaucoma After Lens-Sparing Vitrectomy For Advanced Retinopathy of PrematurityMariaCamilaPerezGuzmanNoch keine Bewertungen
- Jurnal 4Dokument8 SeitenJurnal 4Putri kartiniNoch keine Bewertungen
- Sulcus Implantation of A Single-Piece Foldable Acrylic Intraocular Lens After Posterior Capsular Rupture in Cataract SurgeryDokument6 SeitenSulcus Implantation of A Single-Piece Foldable Acrylic Intraocular Lens After Posterior Capsular Rupture in Cataract SurgeryPrizilia SaimimaNoch keine Bewertungen
- Translate Jurnal MataDokument5 SeitenTranslate Jurnal MataferryNoch keine Bewertungen
- BSN Reading (Scleral Buckling) RosalesDokument8 SeitenBSN Reading (Scleral Buckling) RosalesYvonnie RosalesNoch keine Bewertungen
- Persistent Corneal Edema After Collagen Cross-Linking For KeratoconusDokument6 SeitenPersistent Corneal Edema After Collagen Cross-Linking For KeratoconusRestu MegantaraNoch keine Bewertungen
- A Clinical Study On Visual Outcome and Complications of Penetrating KeratoplastyDokument12 SeitenA Clinical Study On Visual Outcome and Complications of Penetrating KeratoplastyIOSRjournalNoch keine Bewertungen
- Editorial: The Management of Retinal Detachment: Techniques and PerspectivesDokument3 SeitenEditorial: The Management of Retinal Detachment: Techniques and PerspectivesSarahNoch keine Bewertungen
- Ebn RugayDokument6 SeitenEbn RugayJeffrey Barcelon TanglaoNoch keine Bewertungen
- Jurding MataDokument7 SeitenJurding Matarandy_27995Noch keine Bewertungen
- Lasik 1 PDFDokument3 SeitenLasik 1 PDFJulie JohnsonNoch keine Bewertungen
- Trabekulektomi PD Glaukoma SekunderDokument6 SeitenTrabekulektomi PD Glaukoma SekundergcereiraaNoch keine Bewertungen
- 15 DaysDokument9 Seiten15 DayshersainaNoch keine Bewertungen
- Jurnal Cochrane 2Dokument7 SeitenJurnal Cochrane 2nova_nainaNoch keine Bewertungen
- Small Incision Lenticule ExtractionDokument5 SeitenSmall Incision Lenticule ExtractionvrlftrNoch keine Bewertungen
- Complications and Outcomes of Phacoemulsification Cataract Surgery Complicated by Anterior Capsule TearDokument7 SeitenComplications and Outcomes of Phacoemulsification Cataract Surgery Complicated by Anterior Capsule Teareder510Noch keine Bewertungen
- Trabeculectomy With Large Area Mitomycin-C Application As A First-Line Treatment in Advanced Glaucoma: Retrospective ReviewDokument6 SeitenTrabeculectomy With Large Area Mitomycin-C Application As A First-Line Treatment in Advanced Glaucoma: Retrospective ReviewMaria Angelina BunawanNoch keine Bewertungen
- Evaluation of The Safety and Efficacy of Therapeutic Bandage Contact Lenses On Post-Cataract Surgery PatientsDokument7 SeitenEvaluation of The Safety and Efficacy of Therapeutic Bandage Contact Lenses On Post-Cataract Surgery PatientsFitrian Hanif ZulkarnainNoch keine Bewertungen
- Eiger Moscovich2017Dokument6 SeitenEiger Moscovich2017evilelagNoch keine Bewertungen
- Glaukoma Setelah Operasi Katarak KongenitalDokument21 SeitenGlaukoma Setelah Operasi Katarak KongenitalAgustianeMawarniAlyNoch keine Bewertungen
- Corneal Edema Management With Ededay in Post CataractDokument12 SeitenCorneal Edema Management With Ededay in Post CataractRamon Andres SrNoch keine Bewertungen
- Cyclo-Cryotherapy For The Management of Absolute Glaucoma in Rural AreasDokument4 SeitenCyclo-Cryotherapy For The Management of Absolute Glaucoma in Rural AreasIvanalia Soli DeoNoch keine Bewertungen
- Scheimpflug Corneal Densitometry Changes After TrabeculectomyDokument7 SeitenScheimpflug Corneal Densitometry Changes After TrabeculectomyFernando MartínezNoch keine Bewertungen
- BR J Ophthalmol 2013 Dong Bjophthalmol 2013 303415Dokument8 SeitenBR J Ophthalmol 2013 Dong Bjophthalmol 2013 303415Icha NathaniaNoch keine Bewertungen
- Intraocular Pressure 1Dokument6 SeitenIntraocular Pressure 1Sher KhanNoch keine Bewertungen
- Gonioscopic AnatomyDokument30 SeitenGonioscopic AnatomymanognaaaaNoch keine Bewertungen
- Optimal Management of Pediatric Keratoconus: Challenges and SolutionsDokument9 SeitenOptimal Management of Pediatric Keratoconus: Challenges and SolutionsJesus Rodriguez NoriegaNoch keine Bewertungen
- Hyperopia & PresbyopiaDokument30 SeitenHyperopia & PresbyopiaTalha UR RehmanNoch keine Bewertungen
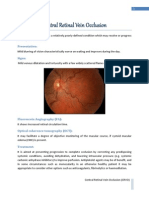
- Non-Ischemic Central Retinal Vein OcclusionDokument6 SeitenNon-Ischemic Central Retinal Vein OcclusionMahmoud Ahmed MahmoudNoch keine Bewertungen
- Diabetic Retinopathy: Clinical Findings and Management: Review ArticleDokument4 SeitenDiabetic Retinopathy: Clinical Findings and Management: Review ArticlewadejackNoch keine Bewertungen
- Herrero Vanrell2014Dokument17 SeitenHerrero Vanrell2014Fer RodriguezNoch keine Bewertungen
- Assignment 3: Units 2.1, 2.2 and 2.3 of Module 2 of The IACLE Contact Lens CourseDokument5 SeitenAssignment 3: Units 2.1, 2.2 and 2.3 of Module 2 of The IACLE Contact Lens CourseSumon SarkarNoch keine Bewertungen
- Congenital Cranial Dysinnervation Disorders (CCDDS) - Duane Syndrome Brown SyndromeDokument62 SeitenCongenital Cranial Dysinnervation Disorders (CCDDS) - Duane Syndrome Brown SyndromeGaurav shuklaNoch keine Bewertungen
- Common Eye Condition ManagementDokument24 SeitenCommon Eye Condition Managementexposus2003Noch keine Bewertungen
- Entoptic Phenomena, Photopsias, Phosphenes Entoptic Phenomena, Photopsias, Phosphenes Entoptični Pojavi, Fotopsije in FosfeniDokument11 SeitenEntoptic Phenomena, Photopsias, Phosphenes Entoptic Phenomena, Photopsias, Phosphenes Entoptični Pojavi, Fotopsije in FosfeniYahya YuusufNoch keine Bewertungen
- Ayurvedic: Exudative Age-Related Macular Degeneration and Its Management: A Case SeriesDokument36 SeitenAyurvedic: Exudative Age-Related Macular Degeneration and Its Management: A Case SeriesAravind KumarNoch keine Bewertungen
- OptHandbook2008 PDFDokument32 SeitenOptHandbook2008 PDFDan CocaliaNoch keine Bewertungen
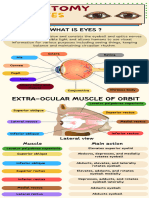
- Infographic of Eye AnatomyDokument2 SeitenInfographic of Eye AnatomyAshi RossNoch keine Bewertungen
- Write A Dialogue of at Least 150 Words Between A Nurse and A Patient Suffering of Earache/ An Eye ConditionDokument1 SeiteWrite A Dialogue of at Least 150 Words Between A Nurse and A Patient Suffering of Earache/ An Eye ConditionLaurusAdiaNoch keine Bewertungen
- Laser Technolas 217 - Excimer Laser SystemDokument34 SeitenLaser Technolas 217 - Excimer Laser Systemrubens.nascimento213Noch keine Bewertungen
- Chapter #9 Understanding Pathologic MyopiaDokument15 SeitenChapter #9 Understanding Pathologic MyopiavidulNoch keine Bewertungen
- IS Case Study DisabilitiesDokument5 SeitenIS Case Study DisabilitiesRuchiNoch keine Bewertungen
- Ms Shalakya TantraDokument40 SeitenMs Shalakya TantraIshwari Gaikwad100% (1)
- Cataract PPT JournalDokument18 SeitenCataract PPT JournalKulesh WaranNoch keine Bewertungen
- Daftar Harga BHP Alkes Mata 2021Dokument2 SeitenDaftar Harga BHP Alkes Mata 2021nadyaNoch keine Bewertungen
- Binocular Anomalies - GriffinDokument595 SeitenBinocular Anomalies - GriffinAdolph Grey75% (4)
- Diagnosis Banding KeratitisDokument7 SeitenDiagnosis Banding KeratitisNurwahidah Lakaming100% (2)
- The Human EyeDokument9 SeitenThe Human Eyegiana 4e100% (1)
- Amblyopia - Diagnosis and Treatment: Pamela J. Kutschke, BS, CoDokument6 SeitenAmblyopia - Diagnosis and Treatment: Pamela J. Kutschke, BS, CoKhushbu DedhiaNoch keine Bewertungen
- Refractive Mgmt/Intervention: Question 1 of 90Dokument39 SeitenRefractive Mgmt/Intervention: Question 1 of 90NoorNoch keine Bewertungen
- DistrictempanelledhospDokument14 SeitenDistrictempanelledhospSumit SinghalNoch keine Bewertungen
- Complicationts of Cataract Surgery (Other Anterior Segment Complications)Dokument30 SeitenComplicationts of Cataract Surgery (Other Anterior Segment Complications)Hikban FiqhiNoch keine Bewertungen
- Test Bank For Psychology 4th Edition Saundra K Ciccarelli J Noland WhiteDokument32 SeitenTest Bank For Psychology 4th Edition Saundra K Ciccarelli J Noland Whitepannageimban.81c15100% (40)
- Epiphora Etiology and Investigations: Moderator: DR Gururaj Wali Presenter: DR Shraddha SudarshanDokument53 SeitenEpiphora Etiology and Investigations: Moderator: DR Gururaj Wali Presenter: DR Shraddha Sudarshanshraddha sudarshanNoch keine Bewertungen
- George Asimellis - Visual Optics (Lectures in Optics, 4) 4 (2022, SPIE Press)Dokument722 SeitenGeorge Asimellis - Visual Optics (Lectures in Optics, 4) 4 (2022, SPIE Press)EUGEN100% (1)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Von EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Bewertung: 3 von 5 Sternen3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionVon EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionBewertung: 4 von 5 Sternen4/5 (404)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsVon EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNoch keine Bewertungen
- The Age of Magical Overthinking: Notes on Modern IrrationalityVon EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityBewertung: 4 von 5 Sternen4/5 (31)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisVon EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisBewertung: 4.5 von 5 Sternen4.5/5 (42)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDVon EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDBewertung: 5 von 5 Sternen5/5 (3)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeVon EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeBewertung: 2 von 5 Sternen2/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedVon EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedBewertung: 4.5 von 5 Sternen4.5/5 (82)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryVon EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryBewertung: 4 von 5 Sternen4/5 (46)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaVon EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsVon EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsBewertung: 4 von 5 Sternen4/5 (4)
- The Obesity Code: Unlocking the Secrets of Weight LossVon EverandThe Obesity Code: Unlocking the Secrets of Weight LossBewertung: 4 von 5 Sternen4/5 (6)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesVon EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesBewertung: 4.5 von 5 Sternen4.5/5 (1412)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsVon EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsBewertung: 5 von 5 Sternen5/5 (1)
- The Comfort of Crows: A Backyard YearVon EverandThe Comfort of Crows: A Backyard YearBewertung: 4.5 von 5 Sternen4.5/5 (23)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Von EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Bewertung: 4.5 von 5 Sternen4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityVon EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityBewertung: 4 von 5 Sternen4/5 (5)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsVon EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsBewertung: 4.5 von 5 Sternen4.5/5 (170)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisVon EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisBewertung: 5 von 5 Sternen5/5 (8)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisVon EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisBewertung: 3.5 von 5 Sternen3.5/5 (2)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessVon EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessBewertung: 4.5 von 5 Sternen4.5/5 (328)
- Troubled: A Memoir of Foster Care, Family, and Social ClassVon EverandTroubled: A Memoir of Foster Care, Family, and Social ClassBewertung: 4.5 von 5 Sternen4.5/5 (27)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingVon EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingBewertung: 4 von 5 Sternen4/5 (1138)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeVon EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeBewertung: 4.5 von 5 Sternen4.5/5 (253)