Beruflich Dokumente
Kultur Dokumente
5Rs GLAUKOMA
Hochgeladen von
Audy AndanaCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
5Rs GLAUKOMA
Hochgeladen von
Audy AndanaCopyright:
Verfügbare Formate
REVIEW ARTICLE
Five rules to evaluate the optic disc and
retinal nerve fiber layer for glaucoma
Murray Fingeret, O.D.,a,b Felipe A. Medeiros, M.D.,c Remo Susanna, Jr, M.D.,d and
Robert N. Weinreb, M.D.c
Department of Veterans Affairs, New York Harbor Health Care System, Brooklyn, New York; bState University of New York,
State College of Optometry, New York, New York; cHamilton Glaucoma Center and the Department of Ophthalmology,
University of California, San Diego, California; and dDepartment of Ophthalmology, University of So Paulo, So Paulo, Brazil
a
A systematic approach for the examination of the optic disc
and retinal nerve fiber layer is described that will aid in the
detection of glaucoma. This approach encompasses 5 rules:
evaluation of optic disc size, neuroretinal rim size and shape,
retinal nerve fiber layer, presence of parapapillary atrophy,
and presence of retinal or optic disc hemorrhages. A systematic process enhances the ability to detect glaucomatous
damage as well as the detection of progression, and facilitates appropriate management.
Key Words: Glaucoma, optic nerve, optic disc, retinal nerve
fiber layer, optic disc hemorrhages
he evaluation of the optic nerve and retinal nerve
fiber layer (RNFL) is essential to the recognition of
glaucomatous damage. An optic nerve or RNFL abnormality is often, but not always, the first sign of glaucomatous damage.1,2 In the earliest stages of the disease,
optic nerve and RNFL damage may be present, while
standard automated perimetry is still within normal limits.3-6 Early glaucomatous damage can be difficult to detect,
requiring careful observation of the optic nerve and RNFL.
Optic disc photography or optic nerve and RNFL imaging
should be performed at the initial visit and yearly thereafter to document the optic nerve and RNFL status. In
situations in which stability is in question, photography
and imaging may be done at earlier intervals.
Recent studies have found the difficulty clinicians have in
following guidelines proposed by professional organizations.7,8 These guidelines recommend documentation of the
optic disc appearance at the time of diagnosis and at periodic
intervals during followup. In one study utilizing a chart review, 193 primary open-angle glaucoma (POAG) patients
were followed up in 8 private practices in the Los Angeles
area for at least 2 years.8 Almost all patients had a photograph
or drawing at the initial examination, but, at the final followup visit, 33.2% had not had an optic nerve drawing or
photograph taken within the previous 2 years. Another 37.8%
had not had optic disc photography since the initial examination. A more recent chart review evaluated records from 395
POAG patients in 6 managed care plans.7 Only 53% had optic
disc photographs or drawings at the initial examination.
Fingeret M, Medeiros FA, Susanna Jr R, Weinreb RN. Five
rules to evaluate the optic disc and retinal nerve fiber layer for
glaucoma. Optometry 2005;76:661-8.
Although several textbooks and articles describe the characteristic signs of glaucomatous damage to the optic disc,
661
VOLUME 76 / NUMBER 11 / NOVEMBER 2005
OPTOMETRY
REVIEW ARTICLE
Figure 1
Figure 2
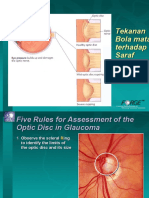
The first rule for the assessment of the optic disc is the
observation of the scleral ring and assessment of optic disc
size.
Figure 3
The optic disc size varies among individuals, with cup size
correlating with the size of the optic disc. These examples are
from 4 individuals with different optic disc sizes. The largest
is in the top left, followed by top right, lower left, and lower
right. Note how the cup size correlates with the disc size,
except for the picture in the lower left in which the person has
glaucoma with a wedge RNFL defect and large cup.
Figure 4
The optic disc size can be evaluated using the small spot of
light from the direct ophthalmoscope. In this example of an
average size disc, the spot approximates the size of the optic
disc.
The shape of the optic disc is oval, usually slightly greater
vertically than horizontally.
no systematic approach for optic disc examination in glaucoma has been widely disseminated.9,10 When examining a patient who either has
established glaucoma or is suspected of having
the disease, a systematic approach to optic disc
and RNFL examination is necessary so that glaucomatous optic neuropathy is not overlooked. A
thorough optic nerve examination should be
used along with perimetry to diagnose glaucoma
and to assess disease severity. Staging the disease and consideration of risk factors for glaucoma progression enables the clinician to establish a target intraocular pressure. The structural
assessment (optic nerve and RNFL) and functional evaluation (perimetry) are used together to
monitor for change over time as well restage the
patients condition.1
In this report, we describe a systematic approach
for the evaluation of the optic disc and RNFL in
glaucoma that can be incorporated easily into
clinical practice. This approach was conceived
originally by 3 of the authors and published as a
PowerPoint monograph entitled FORGE (Focusing Ophthalmology on Reframing Glaucoma
Evaluation) that was sponsored by Allergan, Inc.
Methodology
The five rules (5Rs) for the assessment of the
optic disc in glaucoma include:
1. Observe the scleral Ring to identify the
limits of the optic disc and evaluate its size.
662
OPTOMETRY
VOLUME 76 / NUMBER 11 / NOVEMBER 2005
REVIEW ARTICLE
Figure 5
Certain optic discs, such as those with high myopia, can be
difficult to evaluate.
Figure 6
In this example of a person with a tilted disk, the disc margin
is difficult to identify.
Figure 8
The ISNT rule states that in a healthy optic disc, the widest
rim tissue is found inferiorly, then superiorly, nasally, with the
temporal rim being the thinnest. This gives rise to a cup shape
that is often a horizontal oval.
Figure9
This example shows an optic disc in which the ISNT rule is not
obeyed, as seen by the thin rim inferiorly.
2. Identify the size of the Rim.
3. Examine the Retinal nerve fiber layer.
4. Examine the Region outside the optic disc
for parapapillary atrophy.
5. Watch for Retinal and optic disc hemorrhages.
Figure 7
The second rule for the assessment of the optic disc is to
identify the size of the neuroretinal rim.
Rule 1 recognizes that the first step in evaluating
the optic disc for glaucoma is evaluating its size
(see Figures 1 and 2). Optic discs vary considerably in size, with the size of the optic disc cup
correlating with the size of the optic disc.11,12 In
healthy subjects, a small disc (vertical disc diameter ! 1.5 mm) will have a small cup, whereas a
large disc (vertical disc diameter " 2.2 mm) will
have a large cup (see Figure 3). Therefore, large
663
VOLUME 76 / NUMBER 11 / NOVEMBER 2005
OPTOMETRY
REVIEW ARTICLE
Figure 10
Figure 11
The third rule for the assessment of the optic disc is to
examine the retinal nerve fiber layer. The normal RNFL has
bright striations in the superior temporal and inferior temporal regions of the optic disc; areas in which the RNFL is
thicker. As the RNFL is diffusely lost, the striations disappear, and the borders of small parapapillary retinal blood
vessels become more clearly visible.
A common way RNFL damage is identified is by the presence
of localized loss, as seen by a wedge-shape dark defect at 5
oclock.
optic discs in healthy individuals tend to have
large cups, which can lead to an erroneous diagnosis of glaucoma. However, small cups can be
glaucomatous in small discs.13,14 There are several methods to evaluate optic disc size. Sophisticated optic nerve imaging techniques such as
confocal scanning laser ophthalmoscopy and optical coherence tomography can provide precise
measurements. In clinical practice, however, the
clinician can assess the optic disc size by using a
direct ophthalmoscope or a slit lamp biomicroscope.15-17 With the direct ophthalmoscope, the
small light spot is utilized, which is 5 degrees in
size (approximately the size of the average optic
disc). For direct ophthalmoscopes with 2 spot
Figure12
Several small bands of RNFL dropout are seen between 7 and
9 oclock that extends back to the optic nerve.
Figure 13
The fourth rule for the assessment of the optic disc is to
examine the region adjacent to the optic disc for the
presence of parapapillary atrophy.
sizes, the smaller one is utilized. The middle spot
is used for those with 3 spot sizes. The spot is
aligned either over or adjacent to the optic disc
and the size of the optic disc is compared with
the size of the spot of light (see Figure 4). Another
method consists of using a slit lamp and a high
magnification fundus lens (e.g., 66 diopter [D],
78D, or 90D). A vertical slit is placed over the
optic disc and the beam adjusted until it approximates the vertical disc diameter. The measurement is then read off the calibrated knob on the
slit lamp. Correction factors are needed depending on the power of the fundus lens being used.
A #60D lens has a correction factor of x 1.0, 78D
lens x 1.1, and 90D x 1.3.18 The average vertical
optic disc diameter is 1.8 mm, and the average
horizontal diameter is 1.7 mm. Finally, there are
clinical situations such as in high myopia or
tilted optic discs in which it is difficult to evalu-
664
OPTOMETRY
VOLUME 76 / NUMBER 11 / NOVEMBER 2005
REVIEW ARTICLE
Figure14
Figure 15
Parapapillary atrophy can be divided into zones ! and ", with
zone " being present in many eyes with glaucoma. Zone "
is larger in this case and closer to the optic disc margin.
Figure 16
Optic disc hemorrhages take on many appearances, depending on how recently they have occurred. They tend to occur
in areas with rim tissue present.
Figure 17
The evaluation of the optic nerve in Example 1 is the
following: average disc size, ISNT rule not obeyed with the
inferior and superior rim being thin, a localized RNFL defect
is seen at 5 oclock, PPA is present between 3 and 5 oclock,
no hemorrhage, glaucoma is present.
The fifth rule for the assessment of the optic disc is to
observe for retinal and optic disc hemorrhages.
ate optic disc size because of the imprecise definition of the scleral ring and optic disc margins
(see Figures 5 and 6).
Rule 2 relates to the need to evaluate neuroretinal rim width (see Figure 7). Identification of the
neuroretinal rim width in all sectors of the optic
disc is of fundamental importance for detection
of diffuse and localized rim loss in glaucoma.
The rim width is the distance between the border of the optic disc and the position of blood
vessel bending. In healthy individuals, it is usually widest inferiorly, followed by superiorly,
nasally, and temporally (see Figure 8). The mnemonic ISNT helps one to remember this anatomic situation. This neuroretinal rim configuration gives rise to a cup shape that is either round
or horizontally oval in healthy subjects.14 When
the rim is thinner than expected and does not
obey the ISNT rule, glaucomatous damage must
be suspected (see Figure 9). Also, the color of the
rim needs to be evaluated. Pallor of the rim
increases the likelihood that a nonglaucomatous
optic neuropathy is present, especially when pallor is greater than cup size.
Rule 3 describes the examination of the RNFL
(see Figure 10). This is done either at the biomicroscope using a high magnification lens or by
inspecting fundus photographs. If using the slit
lamp and fundus lens, magnification is reduced
665
VOLUME 76 / NUMBER 11 / NOVEMBER 2005
OPTOMETRY
REVIEW ARTICLE
Figure 18
The evaluation of the optic nerve in Example 2 is the
following: average disc size; normal rim tissue, ISNT Rule is
obeyed; normal RNFL; no PPA; no hemorrhage; normal eye.
Figure 20
The evaluation of the optic nerve in Example 4 is the
following: disc size is large; ISNT rule obeyed, normal rim
tissue; RNFL normal; no significant PPA; only zone alpha
present; no hemorrhage; normal eye with large disc.
the superior and inferior poles when compared
with the temporal and nasal regions. Localized
RNFL loss appears as wedge-shaped dark areas
emanating from the optic disc (see Figure 11).
These defects follow an arcuate pattern as would
be expected from the normal RNFL anatomy (see
Figure 12). True RNFL defects are at least an
arteriole in width and extend back to the optic
disc compared with pseudodefects, which may
be thin or never extend to the optic nerve.
Figure 19
The evaluation of the optic nerve in Example 3 is the
following: large disc size, ISNT rule not obeyed, diffuse RNFL
loss, small PPA, no hemorrhage, glaucoma is present.
to 6 to 10x while using a 78D or 90D lens and
red-free or green light.19 RNFL defects may also
be visible in white light. In a healthy eye, bright
striations are visible, and the retina glistens in
the regions in which the RNFL is thickest, superior temporal and inferior temporal from the
disc.20-22 The examiner should observe the
brightness and striations of the RNFL as well as
the visibility of the parapapillary vessels. Typically, these vessels are indistinct but their borders become clearer as the RNFL is lost. RNFL
loss can occur in a diffuse, localized, or mixed
pattern.23 With diffuse loss, there is general reduction of the RNFL brightness, with reduction
of the difference normally occurring between
Rule 4 describes the examination of the parapapillary region, which is the area located just outside the optic disc (see Figure 13). Parapapillary
atrophy (PPA) refers to the thinning and degeneration of the chorioretinal tissue just outside of
the optic disc, which has an association with
development and progression of glaucoma.24-26
There are 2 forms of PPA, zone alpha (!) and
zone beta (") (see Figure 14). Zone ! is present in
most normal eyes as well as in eyes with glaucoma and is characterized by a region of irregular hypopigmentation and hyperpigmentation of
the retinal pigment epithelium (RPE).27,28 The
more important zone with regard to glaucoma is
zone ", which is caused by atrophy of the retinal
pigment epithelium (RPE) and choriocapillaris
leading to the large choroidal vessels and sclera
becoming visible.27,28 If both areas are present,
zone ! is always peripheral to the zone ". Zone "
is more common and extensive in eyes with
glaucoma than in healthy eyes. The area of PPA
is spatially correlated with the area of neuroreti-
666
OPTOMETRY
VOLUME 76 / NUMBER 11 / NOVEMBER 2005
REVIEW ARTICLE
nal rim loss, with the atrophy being largest in the
corresponding area of thinner neuroretinal
rim.27-29
Rule 5 refers to observation of retinal and optic
disc hemorrhages, which are indicative of glaucoma progression (see Figure 15).30-34 The hemorrhages draw their feathery shape from being
present in the nerve fiber layer (see Figure 16).
They are transient, lasting from 2 to 6 months,
but may recur.35 They may be either on the
retina, be just off the disc, or bisect the disc
margin and retina. They may also be located at
the level of the lamina cribrosa where they tend
to assume a round aspect. Sometimes the bleeding is minimal or occurs near blood vessels making detection difficult unless a meticulous examination is carried out. Hemorrhages most often
are located in the inferior temporal or superior
temporal regions, although they can occur in any
sector of the optic disc.36 Their color depends
upon how long they have been present. They
tend to be located in association with notching of
the neuroretinal rim or retinal nerve fiber layer
defects and may precede the later changes.37
Although more common in normal tension glaucoma, they can be present in all types and indicate that the condition is not stable and needs
further evaluation.
Several cases are provided to allow the reader to
go through the 5 Rs checklist and determine
whether glaucoma is present (see Figures 17, 18,
19, and 20). Each example illustrates a different
way glaucoma may present.
Conclusion
Optic disc and RNFL assessment can be performed according to 5 rules that include the
evaluation of optic disc size, rim shape and area,
presence of RNFL loss, PPA, and retinal or optic
disc hemorrhages. By following these 5 rules, a
thorough and systematic review of the optic disc
and RNFL will occur. This will improve the
ability to diagnosis and manage glaucoma.
Acknowledgments
The 5 Rs were developed by Robert N. Weinreb, M.D., and Felipe A.
Medeiros, M.D. from the Hamilton Glaucoma Center, University of California,
San Diego, and Remo Susanna, Jr., M.D. from the University of So Paulo. This
approach was first described in a PowerPoint monograph entitled FORGE
(Focusing Ophthalmology on Reframing Glaucoma Evaluation) distributed by
Allergan, Inc. Figures 1, 7, 10, 13, and 15 were originally published in the
FORGETM monograph distributed by Allergan, Inc.
References
1. Weinreb RN, Khaw PT. Primary open-angle glaucoma.
Lancet 2004;363:1711-20.
2. Medeiros FA, Weinreb RN. Medical backgrounders:
glaucoma. Drugs Today (Barc) 2002;38:563-70.
3. Quigley HA, Dunkelberger GR, Green WR. Retinal
ganglion cell atrophy correlated with automated perimetry in human eyes with glaucoma. Am J Ophthalmol
1989;107:453-64.
4. Sommer A, Katz J, Quigley HA, et al. Clinically detectable nerve fiber atrophy precedes the onset of glaucomatous field loss. Arch Ophthalmol 1991;109:77-83.
5. Harwerth RS, Carter-Dawson L, Smith EL 3rd, Barnes
G, Holt WF, Crawford ML. Neural losses correlated
with visual losses in clinical perimetry. Invest Ophthalmol Vis Sci 2004;45:3152-60.
6. Medeiros FA, Sample PA, Zangwill LM, Bowd C, Aihara
M, Weinreb RN. Corneal thickness as a risk factor for
visual field loss in patients with preperimetric glaucomatous optic neuropathy. Am J Ophthalmol 2003;136:
805-13.
7. Fremont AM, Lee PP, Mangione CM, et al. Patterns of
care for open-angle glaucoma in managed care. Arch
Ophthalmol 2003;121:777-83.
8. Hertzog LH, Albrecht KG, LaBree L, et al. Glaucoma
care and conformance with preferred practice patterns.
Examination of the private, community-based ophthalmologist. Ophthalmology 1996;103:1009-13.
9. Broadway DC, Nicolela MT, Drance SM, et al. Optic
disc appearance in primary open angle glaucoma. Surv
Ophthalmol 1999;43:223-43.
10. Tuulonen A, Airaksinen P. Initial glaucomatous optic
disc and retinal nerve fiber layer abnormalities and
their progression. Am J Ophthalmol 1991;111:485-90.
11. Healey PR, Mitchell P, Smith W, et al. Relationship
between cup-disc ratio and optic disc diameter: the Blue
Mountains Eye Study. Aust N Z J Ophthalmol 1997;25
Suppl 1:S99-101.
12. Jonas JB, Zach FM, Gusek GC, et al. Pseudoglaucomatous physiologic large cups. Am J Ophthalmol 1989;107:
137-44.
13. Garway-Heath DF, Ruben ST, Viswanathan A, et al.
Vertical cup/disc ratio in relation to optic disc size: its
value in the assessment of the glaucoma suspect. Br J
Ophthalmol 1998;82:1118-24.
14. Jonas JB, Gusek GC, Naumann GO. Optic disc, cup and
neuroretinal rim size, configuration and correlations in
normal eyes. Invest Ophthalmol Vis Sci 1988;29:1151-8.
15. Jonas JB, Papastathopoulos K. Ophthalmoscopic measurement of the optic disc. Ophthalmology 1995;102:
1102-6.
16. Garway-Heath DF, Rudnicka AR, Lowe T, et al. Measurement of optic disc size: equivalence of methods to
correct for ocular magnification. Br J Ophthalmol 1998;
82:643-9.
17. Lim CS, OBrien C, Bolton NM. A simple clinical
method to measure the optic disc size in glaucoma. J
Glaucoma 1996;5:241-5.
18. Ansari-Shahrezaei S, Maar N, Biowski R, et al. Biomicroscopic measurement of the optic disc with a highpower positive lens. Invest Ophthalmol Vis Sci 2001;42:
153-7.
667
VOLUME 76 / NUMBER 11 / NOVEMBER 2005
OPTOMETRY
REVIEW ARTICLE
19. Quigley HA, Sommer A. How to use nerve fiber layer
examination in the management of glaucoma. Trans Am
Ophthalmol Soc 1987;85:254-72.
20. Dichtl A, Jonas JB, Naumann GO. Retinal nerve fiber
layer thickness in human eyes. Graefes Arch Clin Exp
Ophthalmol 1999;237:474-9.
21. Jonas JB, Dichtl A. Evaluation of the retinal nerve fiber
layer. Surv Ophthalmol 1996;40:369-78.
22. Jonas JB, Nguyen NX, Naumann GO. The retinal nerve
fiber layer in normal eyes. Ophthalmology 1989;96:62732.
23. Jonas JB, Budde WM, Panda-Jonas S. Ophthalmoscopic
evaluation of the optic nerve head. Surv Ophthalmol
1999;43:293-320.
24. Jonas JB, Martus P, Horn FK, et al. Predictive factors of
the optic nerve head for development or progression of
glaucomatous visual field loss. Invest Ophthalmol Vis Sci
2004;45:2613-8.
25. Tezel G, Kolker AE, Wax MB, et al. Parapapillary chorioretinal atrophy in patients with ocular hypertension.
II. An evaluation of progressive changes. Arch Ophthalmol 1997;115:1509-14.
26. Tezel G, Kolker AE, Kass MA, et al. Parapapillary chorioretinal atrophy in patients with ocular hypertension.
I. An evaluation as a predictive factor for the development of glaucomatous damage. Arch Ophthalmol 1997;
115:1503-8.
27. Jonas JB, Naumann GO. Parapapillary chorioretinal atrophy in normal and glaucoma eyes. II. Correlations.
Invest Ophthalmol Vis Sci 1989;30:919-26.
28. Jonas JB, Nguyen XN, Gusek GC, et al. Parapapillary
chorioretinal atrophy in normal and glaucoma eyes. I.
Morphometric data. Invest Ophthalmol Vis Sci 1989;30:
908-18.
29. Tezel G, Kass MA, Kolker AE, et al. Comparative optic
disc analysis in normal pressure glaucoma, primary
open-angle glaucoma, and ocular hypertension. Ophthalmology 1996;103:2105-13.
30. Drance S, Anderson DR, Schulzer M. Risk factors for
progression of visual field abnormalities in normal-tension glaucoma. Am J Ophthalmol 2001;131:699-708.
31. Sonnsjo B, Dokmo Y, Krakau T. Disc haemorrhages,
precursors of open angle glaucoma. Prog Retin Eye Res
2002;21:35-56.
32. Ishida K, Yamamoto T, Sugiyama K, et al. Disk hemorrhage is a significantly negative prognostic factor in
normal-tension glaucoma. Am J Ophthalmol 2000;129:
707-14.
33. Rasker MT, van den Enden A, Bakker D, et al. Deterioration of visual fields in patients with glaucoma with
and without optic disc hemorrhages. Arch Ophthalmol
1997;115:1257-62.
34. Drance SM. Disc hemorrhages in the glaucomas. Surv
Ophthalmol 1989;33:331-7.
35. Kitazawa Y, Shirato S, Yamamoto T. Optic disc hemorrhage in low-tension glaucoma. Ophthalmology 1986;93:
853-7.
36. Jonas JB, Xu L. Optic disk hemorrhages in glaucoma.
Am J Ophthalmol 1994;118:1-8.
37. Sugiyama K, Uchida H, Tomita G, et al. Localized
wedge-shaped defects of retinal nerve fiber layer and
disc hemorrhage in glaucoma. Ophthalmology 1999;106:
1762-7.
Corresponding author:
Murray Fingeret, O.D.
Department of Veterans Affairs NYHHCS
Optometry Section
Linden Blvd and 179th Street
St. Albans, New York 11425
murray.fingeret@med.va.gov
668
OPTOMETRY
VOLUME 76 / NUMBER 11 / NOVEMBER 2005
Das könnte Ihnen auch gefallen
- Identification and Classification of Glaucoma Using Deep LearningDokument16 SeitenIdentification and Classification of Glaucoma Using Deep LearningNayan PathNoch keine Bewertungen
- s12886 017 0419 1Dokument8 Seitens12886 017 0419 1Madhu C KNoch keine Bewertungen
- A Hybrid Approach Based On R-CNN Resnet-50 Pre-Trained and Image Segmentation Algorithm To Detect Glaucoma Using Fundus ImageDokument14 SeitenA Hybrid Approach Based On R-CNN Resnet-50 Pre-Trained and Image Segmentation Algorithm To Detect Glaucoma Using Fundus ImageLuis Fernando ZhininNoch keine Bewertungen
- A Clinical Study To Correlate Visual Field Defects With Optic Disc Changes in 100 Patients With Primary Open Angle Glaucoma in A Tertiary Eye Care HospitalDokument3 SeitenA Clinical Study To Correlate Visual Field Defects With Optic Disc Changes in 100 Patients With Primary Open Angle Glaucoma in A Tertiary Eye Care HospitalIOSRjournalNoch keine Bewertungen
- A Hybrid Approach Based On R-CNN Resnet-50 Pre-Trained and Image Segmentation Algorithm To Detect Glaucoma Using Fundus ImageDokument14 SeitenA Hybrid Approach Based On R-CNN Resnet-50 Pre-Trained and Image Segmentation Algorithm To Detect Glaucoma Using Fundus ImageLuis Fernando ZhininNoch keine Bewertungen
- Optic Nerve Examination in Glaucoma (Edit)Dokument27 SeitenOptic Nerve Examination in Glaucoma (Edit)mazidahzulfa100% (1)
- Optic Disc Morphology in Primary Open Angle.42Dokument6 SeitenOptic Disc Morphology in Primary Open Angle.42syntacs skNoch keine Bewertungen
- FORGE II Presentation 2008 MSDokument99 SeitenFORGE II Presentation 2008 MSmdmmm100% (1)
- Comparacion Topografica de No Normal y MegalopapilaDokument5 SeitenComparacion Topografica de No Normal y MegalopapilaPatzy Yulissa Vasquez AlaniaNoch keine Bewertungen
- Correlation Between Retinal Nerve Fiber Layer Thickness by Optical Coherence Tomography and Perimetric Parameters in Optic Atrophy - PMCDokument6 SeitenCorrelation Between Retinal Nerve Fiber Layer Thickness by Optical Coherence Tomography and Perimetric Parameters in Optic Atrophy - PMCkagone walidNoch keine Bewertungen
- LTM SenseDokument6 SeitenLTM SenseNabilla MerdikaNoch keine Bewertungen
- 3 - Tuulonen1993Dokument12 Seiten3 - Tuulonen1993Eduardo HernandezNoch keine Bewertungen
- Key Papers On Optic Disc Evaluation in GDokument110 SeitenKey Papers On Optic Disc Evaluation in Gkhor hing sikNoch keine Bewertungen
- Optometry Department OPTO 374 The Synoptophore Dr. Safiah Mulla Name: Fatima Ahmad Abo-Qoaied ID: 426200452Dokument25 SeitenOptometry Department OPTO 374 The Synoptophore Dr. Safiah Mulla Name: Fatima Ahmad Abo-Qoaied ID: 426200452zecemariNoch keine Bewertungen
- Angelina Kristin Nikolas GlaukomaDokument16 SeitenAngelina Kristin Nikolas GlaukomaAngelina NikolasNoch keine Bewertungen
- Ocular Hypertension: An Approach To Assessment and ManagementDokument8 SeitenOcular Hypertension: An Approach To Assessment and ManagementimmanueldioNoch keine Bewertungen
- Development of Topographic Scoring System For Identifying Glaucoma in Myopic EyesDokument10 SeitenDevelopment of Topographic Scoring System For Identifying Glaucoma in Myopic EyesValentina Gracia ReyNoch keine Bewertungen
- TB GlaukomaDokument21 SeitenTB GlaukomaArdyNoch keine Bewertungen
- Predictive Diagnosis of GlaucomaDokument10 SeitenPredictive Diagnosis of GlaucomaEduardo HernandezNoch keine Bewertungen
- RNFL AsymmetryDokument24 SeitenRNFL Asymmetryhakimu10Noch keine Bewertungen
- Visual Field Loss in the Real World: A Book of Static Perimetry Test Targets for Eye Health ProfessionalsVon EverandVisual Field Loss in the Real World: A Book of Static Perimetry Test Targets for Eye Health ProfessionalsNoch keine Bewertungen
- Ocular Examination and Imaging TechniqueDokument33 SeitenOcular Examination and Imaging TechniqueluckyNoch keine Bewertungen
- (Cheng-2013) Superpixel Classification Based Optic Disc and Optic Cup Segmentation For Glaucoma ScreeningDokument14 Seiten(Cheng-2013) Superpixel Classification Based Optic Disc and Optic Cup Segmentation For Glaucoma Screening02f52a7241Noch keine Bewertungen
- Glaukoma Case ReportDokument9 SeitenGlaukoma Case ReportHIstoryNoch keine Bewertungen
- Glaucoma Case ReportDokument9 SeitenGlaucoma Case Reportsuci caraswatiNoch keine Bewertungen
- Increased Iris Thickness and Association With Primary Angle Closure GlaucomaDokument6 SeitenIncreased Iris Thickness and Association With Primary Angle Closure GlaucomaNinda AstariNoch keine Bewertungen
- The Value of Stereoscopic Optic Disc Photography: An Update On Imaging Techniques and ReliabilityDokument3 SeitenThe Value of Stereoscopic Optic Disc Photography: An Update On Imaging Techniques and Reliabilitypqwoeifjpakou134Noch keine Bewertungen
- GlaucomaDokument11 SeitenGlaucomaerkalemNoch keine Bewertungen
- Primary Retinal Detachment: Clinical PracticeDokument9 SeitenPrimary Retinal Detachment: Clinical PracticeAdita DitaNoch keine Bewertungen
- NIH Public Access: Author ManuscriptDokument19 SeitenNIH Public Access: Author ManuscriptSara GRNoch keine Bewertungen
- Practicalophthalmology Web 2Dokument104 SeitenPracticalophthalmology Web 2mohalbhm9Noch keine Bewertungen
- The Ocular Biometric and Corneal Topographic Characteristics of High-Anisometropic Adults in TaiwanDokument6 SeitenThe Ocular Biometric and Corneal Topographic Characteristics of High-Anisometropic Adults in TaiwanNurul Falah KalokoNoch keine Bewertungen
- Glaucoma Suspect: Diagnosis and Management: Risk FactorsDokument5 SeitenGlaucoma Suspect: Diagnosis and Management: Risk FactorsKrisno ParammanganNoch keine Bewertungen
- Diagnostic Ability of Retinal Ganglion Cell Complex, RetinalDokument7 SeitenDiagnostic Ability of Retinal Ganglion Cell Complex, RetinalYoselin Herrera GuzmánNoch keine Bewertungen
- FORGE I Full VersionDokument118 SeitenFORGE I Full VersionEhecatlNoch keine Bewertungen
- GlaucomaDokument16 SeitenGlaucomaSidhika GoenkaNoch keine Bewertungen
- High Myopia and Glaucoma Susceptibility The Beijing Eye StudyDokument5 SeitenHigh Myopia and Glaucoma Susceptibility The Beijing Eye StudyDickyStevanoZukhriNoch keine Bewertungen
- Primary Retinal DetachmentDokument9 SeitenPrimary Retinal DetachmentMarviane ThenNoch keine Bewertungen
- Cataract For Medical StudentsDokument7 SeitenCataract For Medical StudentsJustin Michal DassNoch keine Bewertungen
- VmsDokument92 SeitenVmsRohit Kumar S.SNoch keine Bewertungen
- Body Mass Index and Interocular Asymmetry of Retinal and Choroidal Thickness in Emmetropic and Ametropic SubjectsDokument13 SeitenBody Mass Index and Interocular Asymmetry of Retinal and Choroidal Thickness in Emmetropic and Ametropic SubjectsAthenaeum Scientific PublishersNoch keine Bewertungen
- Vitrectomy Results in Proliferative Diabetic RetinopathyDokument3 SeitenVitrectomy Results in Proliferative Diabetic RetinopathyRohamonangan TheresiaNoch keine Bewertungen
- Cryo RopDokument7 SeitenCryo RopJuan Pablo OlveraNoch keine Bewertungen
- Tekanan Bola Mata Terhadap Saraf OptikDokument35 SeitenTekanan Bola Mata Terhadap Saraf OptikArif Kusuma WardhanaNoch keine Bewertungen
- Ophthalmolog Y: Instruments & InvestigationDokument15 SeitenOphthalmolog Y: Instruments & Investigationhenry cazeNoch keine Bewertungen
- Rmo 97 40Dokument15 SeitenRmo 97 40JoseNoch keine Bewertungen
- AmblyopiaDokument10 SeitenAmblyopiaNoura RoseNoch keine Bewertungen
- Anterior Segment Examination: 15 Section II. Comprehensive Ophthalmic EvaluationDokument6 SeitenAnterior Segment Examination: 15 Section II. Comprehensive Ophthalmic EvaluationRaulLopezJaimeNoch keine Bewertungen
- The Glaucoma Handbook PDFDokument28 SeitenThe Glaucoma Handbook PDFLuis Miguel Salazar AmatureNoch keine Bewertungen
- Moon2019 PDFDokument7 SeitenMoon2019 PDFGusti Zidni FahmiNoch keine Bewertungen
- Dispensing NotesDokument103 SeitenDispensing Notesjancok100% (1)
- Fixation Stability SeedDokument6 SeitenFixation Stability SeedNaihtneNoch keine Bewertungen
- Primary Open-Angle Glaucoma: SeminarDokument10 SeitenPrimary Open-Angle Glaucoma: SeminarFebry LuthunananaNoch keine Bewertungen
- Retinal Nerve Fiber Loss in High-And Normal-Tension Glaucoma by Optical Coherence TomographyDokument4 SeitenRetinal Nerve Fiber Loss in High-And Normal-Tension Glaucoma by Optical Coherence TomographyRaditya BagusNoch keine Bewertungen
- Beck 1988Dokument3 SeitenBeck 1988Sebastian RiveroNoch keine Bewertungen
- Tinted Lens in Low VisionDokument10 SeitenTinted Lens in Low VisionAmrit PokharelNoch keine Bewertungen
- Endpd PDFDokument29 SeitenEndpd PDFNaveen AgrawalNoch keine Bewertungen
- Bjo08600238 PDFDokument5 SeitenBjo08600238 PDFSadhira GitaNoch keine Bewertungen
- Optical Coherence Tomography in Glaucoma: A Practical GuideVon EverandOptical Coherence Tomography in Glaucoma: A Practical GuideAhmet AkmanNoch keine Bewertungen
- PBR Table of ContentsDokument60 SeitenPBR Table of ContentsAli Sherazi100% (1)
- Concise CardiologyDokument354 SeitenConcise CardiologyAtish_Mathur_9874Noch keine Bewertungen
- Shoulder Dystocia ModuleDokument18 SeitenShoulder Dystocia Moduleapi-219741636100% (1)
- Filed Under: Multifocal Atrial TachycardiaDokument3 SeitenFiled Under: Multifocal Atrial TachycardiaBogdan TeoNoch keine Bewertungen
- Ethics in Pharmacy Practice: Under Supervision Of: DR Noha M SalehDokument24 SeitenEthics in Pharmacy Practice: Under Supervision Of: DR Noha M SalehEyad NabilNoch keine Bewertungen
- Certain Conditions Originating in The Perinatal PeriodDokument4 SeitenCertain Conditions Originating in The Perinatal PeriodOlivia KristiantiNoch keine Bewertungen
- Hooper 2015Dokument7 SeitenHooper 2015Jonathan JonesNoch keine Bewertungen
- Anesthetic Management of A Case of Congenital Diaphragmatic Hernia Delayed DiagnosisDokument3 SeitenAnesthetic Management of A Case of Congenital Diaphragmatic Hernia Delayed DiagnosisFhomensNoch keine Bewertungen
- Malaria Pregnancy RcogDokument29 SeitenMalaria Pregnancy RcogBonifacius Bayu Erlangga KusumaNoch keine Bewertungen
- Journey of The First 1000 Days 25 - 04 - 2018 For Web (Low Res) PDFDokument177 SeitenJourney of The First 1000 Days 25 - 04 - 2018 For Web (Low Res) PDFchandraprakash_shuklNoch keine Bewertungen
- Effect of Foot Massage To Decrease Physiological Lower Leg Oedema in Late Pregnancy: A Randomized Controlled Trial in TurkeyDokument7 SeitenEffect of Foot Massage To Decrease Physiological Lower Leg Oedema in Late Pregnancy: A Randomized Controlled Trial in TurkeyRichaanggrainiNoch keine Bewertungen
- Brochure IDC2017Dokument16 SeitenBrochure IDC2017Shahid ShaikhNoch keine Bewertungen
- DICOM Tags Used by Phoenix Modality WorklistDokument2 SeitenDICOM Tags Used by Phoenix Modality Worklistfgjruiz37Noch keine Bewertungen
- SEMINAR ON MULTIPLE PREGNANCY ContentDokument21 SeitenSEMINAR ON MULTIPLE PREGNANCY ContentMonika shankar0% (1)
- Mandelbaum 2020Dokument19 SeitenMandelbaum 2020Melati HasnailNoch keine Bewertungen
- EAACI - Food Allergy and Anaphylaxi PDFDokument294 SeitenEAACI - Food Allergy and Anaphylaxi PDFoci savitrieNoch keine Bewertungen
- Sample DictationsDokument9 SeitenSample DictationsPop NiceNoch keine Bewertungen
- Operative Obstetrics: Richard G. Moutvic, MD, FacogDokument58 SeitenOperative Obstetrics: Richard G. Moutvic, MD, FacogSdffNoch keine Bewertungen
- Steri-Lok RS 4p Bro EUDokument4 SeitenSteri-Lok RS 4p Bro EUandreirazorNoch keine Bewertungen
- Gynaecological Ultrasound in Clinical Practice PDFDokument247 SeitenGynaecological Ultrasound in Clinical Practice PDFyulb_1Noch keine Bewertungen
- Info DcsDokument9 SeitenInfo DcsKhei Laqui SNNoch keine Bewertungen
- Consultant General SurgeryDokument2 SeitenConsultant General SurgeryMohamed AbbasNoch keine Bewertungen
- Kunst Et Al-2014-Veterinary Radiology & UltrasoundDokument10 SeitenKunst Et Al-2014-Veterinary Radiology & Ultrasoundcristian9088Noch keine Bewertungen
- The Evolving Role of Midwives As Laborists: Original ReviewDokument8 SeitenThe Evolving Role of Midwives As Laborists: Original Reviewmnazri98Noch keine Bewertungen
- Principles of Endodontic SurgeryDokument29 SeitenPrinciples of Endodontic SurgeryCristina Ene100% (3)
- Research Proposal o NishaDokument14 SeitenResearch Proposal o NishaNishaThakuri100% (1)
- Hospitals That Offer ObservershipsDokument6 SeitenHospitals That Offer ObservershipsNisarg DaveNoch keine Bewertungen
- Clinical MedicineDokument18 SeitenClinical MedicineRishikesh AsthanaNoch keine Bewertungen
- Partially Dentate PatientDokument55 SeitenPartially Dentate PatientAhmed SamirNoch keine Bewertungen
- B.C. Masks LetterDokument4 SeitenB.C. Masks LetterCTV VancouverNoch keine Bewertungen