Beruflich Dokumente
Kultur Dokumente
SURGERY Lecture 1 - Small Intestine (Dr. Mendoza)
Hochgeladen von
Medisina101Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
SURGERY Lecture 1 - Small Intestine (Dr. Mendoza)
Hochgeladen von
Medisina101Copyright:
Verfügbare Formate
GENERAL SURGERY: SMALL INTESTINE
SURGERY BLOCK
2012
SURGERY
Small Intestine
Dr. Neil Mendoza
ANATOMY & PHYSIOLOGY
ANATOMY AND PHYSIOLOGY OF THE
Small Intestines
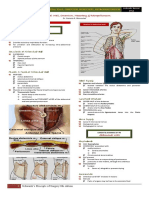
Small Intestine
One of the most important organs for immune defense
Largest endocrine organ of the body
Starts from the pylorus and ends at the cecum
3 parts:
Duodenum (20cm)
Jejunum (100 to 110cm)
Ileum (150 to 160 cm)
Has plicae circulares or valves of Kerkring
plicae circulares, the villi and the microvilli
increase the amount of surface area available for the
absorption of nutrients
Duodenum
Retro-peritoneal
Supplied by the Celiac artery & SMA
Brunners Gland
In submucosal layer
helps alkalinize contents
Paneth Cells & Goblet Cells
Epithelial layer
Jejunum
Suspended in a mobile mesentery
2/5 of whole intestinal length
Involved in adhesions
Occupies upper left of the abdomen
Thicker wall and wider lumen than the ileum
Mesentery has less fat and forms only 1-2 arcades
Has the most plica circulares and very long villi
Ileum
3/5 of whole intestinal length
Shorter villi
Occupies the lower right
has more fat and forms more arcades
Contains Payers patches
Ileum & jejunum is supplied by the SMA
Blood Supply
Proximal duodenum
Celiac Artery
Remainder of the small intestine & large intestines
Superior mesenteric artery
rd
Distal duodenum to proximal 2/3 of transverse
colon
Inferior Mesenteric Artery
rd
Distal 1/3 of transverse colon to proximal rectum
Layers of the Bowel Wall
TUNICA SEROSA
Outermost layer
Lined by Mesothelium
Loose collagenous CT
Covers the jejunum and ileum and anterior portion of the
duodenum
TUNICA MUSCULARIS
Composed of 2 smooth muscles layers
Thicker Inner Circular
Thinner outer longitudinal
Auerbachs plexus
Aka: Myenteric Plexus
Found b/w inner circular & outer longitudinal smooth
mm layer
Parasympathetic/ vagal innervation
Responsible for peristaltic movement
TUNICA SUBMUCOSA
Dense collagenous CT
Strongest layer of the bowel wall
Network of arterioles, lymphatics, venous plexuses, and
nerves crisscross through the submucosa
In a bowel anastomosis, submucosa is incorporated in the
suture
TUNICA MUCOSA
Innermost layer
3 sublayers
Lining Epithelial Layer
Contains epithelial cells with microvilli
Lamina Propia
Muscularis Mucosa
Meissners or Submucosal plexus is located
Contraction cause release of GI secretions
Characterized by villous structure
Plica Circulares or Valves of Kerkring
Amplifies potential absorptive surface area
twenty-fold.
Succus entericus
clear to pale yellow watery secretions from the glands
lining the small intestine walls
aka: Intestinal Juice
contains hormones, digestive enzymes, mucus,
substances to neutralize hydrochloric acid coming
from the stomach and Erepsin which further digests
polypeptides into amino acids, completing protein
digestion
ANATOMY AND PHYSIOLOGY OF THE
Small Intestines
Functions of Small Intestinal
PRIMARY FUNCTION
Digestion & absorption
All ingested food, fluid & secretion from the stomach,
liver, pancreas reach the small intestine
Most volume ingested, 9L/day, are absorbed in
the small intestine
1L/day absorbed in the colon
GENERAL SURGERY: SMALL INTESTINE
BARRIER FUNCTION
Epithelium selectively limits the permeation of potentially
harmful luminal substance.
Perturbed (disturbed) under a variety of pathological
conditions:
Clostridium difficile
Critical illness
DIGESTION AND ABSORPTION
Proximal small intestine
fat digestion and absorption occur.
diffuse into enterocytes by Micelles
formed by solubilized bile salts
reformed intracellularly as chylomicron
water & lipids
are absorbed by passive diffusion
Sodium Bicarbonate
is absorbed by active transport
Glucose & amino acid
absorbed by co-transport
Proximal Duodenum
food stuff are broken down by pancreatic proteases:
pancreatic lipase
trypsin
absorption of iron & calcium
Jejunum
Where majority of the food stuff is absorbed
Fructose
absorbed by facilitated diffusion
Distal Ileum
Where bile salts are reabsorbed into enterohepatic
circulation
Absorption of:
Vitamin B12
Vitamin B9
We can survive as long as ileocecal is intact.
SECRETION
Secretes isotonic fluid through active transcellular
transport of chloride
Diarrhea result when secretion exceeds colonic absorptive
capacity
Secretion > Colonic absorptive capacity = diarrhea
IMMUNE FUNCTION
Major source of IgA
Integrity of the GUT wall prevents bacterial translocation
into the wall of the intestine and abdominal cavity which
can lead to sepsis
Gut associated lymphoid tissue part of the immune
defense system which clears the abdominal cavity of
pathogenic bacteria found in Peyers patches
Found in Ileum
Lymphatic nodule
Lined by M-cells
Part of MPS
Important against toxic and pathogenic threats from
luminal environment
Lamina propria
contains plasma cells, mast cells and lymphocytes
Lymphocytes form Ig and Cytokine
NEUROENDOCRINE FUNCTION
Secretin
Release by enteroendocrine cells in the proximal
small bowel.
produced in the S cells of the duodenum in the
crypts of Lieberkhn
Stimulates
bicarbonate secretion
bile flow
Inhibit gastric acid secretion and GIT motility
Cholecystokinin
Released in response to luminal amino acids and
medium to long chain fatty acid.
synthesized by I-cells in the mucosal epithelium of
the small intestine and secreted in the duodenum
Targets the gallbladder contraction and the
Sphincter of Oddi relaxation to release bile
Also stimulates:
SURGERY BLOCK
2012
pancreatic enzyme secretion
cell growth in intestinal mucosa and pancreas
insulin release
GUT motility.
Note: Related to Fistula
Gastric Inhibitory Peptide
Aka: glucose-dependent insulinotropic peptide
induce insulin secretion
stimulated primarily by hyperosmolarity of
glucose in the duodenum
effects on fatty acid metabolism through stimulation
of lipoprotein lipase activity in adipocytes
Enteroglucagon
released following ingestion of a mixed meal, and
delays gastric emptying
secreted from mucosal cells primarily of the colon
and terminal ileum
Vasoactive Intestinal Peptide
smooth muscle relaxation: lower esophageal
sphincter, stomach, gallbladder
inhibition of gastric acid secretion and absorption
from the intestinal lumen.
Stimulates:
secretion of water and electrolytes in SI
secretion of water into pancreatic juice and bile
contraction of enteric smooth muscle
pancreatic bicarbonate secretion
dilating peripheral blood vessels
OVERALL EFFECTS: increase intestinal motility
Motilin
secreted by endocrine M cells in the crypts of the
small intestine, especially in the duodenum and
jejunum
increase the migrating myoelectric complex
component of gastrointestinal motility
stimulate the production of pepsin.
Aka: "Housekeeper of the gut"
improves peristalsis in the small intestine and clears
out the gut to prepare for the next meal
Bombesin
Together with cholecystokinin, it is the second major
source of negative feedback signals that stop eating
behavior
tumor marker for small cell carcinoma of lung,
gastric cancer, and neuroblastoma
Neurotensin
associated with colorectal cancer
Somatostatin
Inhibits intestinal, gastric, pancreatico-biliary
secretion and cell growth.
Aka: growth hormone-inhibiting hormone (GHIH) or
somatotropin release-inhibiting factor
Secreted in the stomach, intestine & delta cells of
the pancreas
Decrease rate of gastric emptying, and reduces
smooth muscle contractions and blood flow within
the intestine
Suppresses the release of pancreatic hormones
Inhibits insulin release when somatostatin is
released from delta cells of pancreas
Inhibits the release of glucagon
Suppresses the exocrine secretory action of pancreas
MOTILITY OF SMALL INTESTINE
Anterograde propulsion of luminal contents combined
with mixing action through segmentation.
Anterograde d/t longitudinal mm layer contraction
Mixing d/t circular mm layer contraction
Under positive control by local hormones:
Motilin
CCK
Initiated by pacesetter potential that originate in the
duodenum: Interstitial cells of Cajal
GENERAL SURGERY: SMALL INTESTINE
SURGERY BLOCK
2012
PATHOLOGY
DISEASES OF THE
SMALL INTESTINES
Mechanical Obstruction of the Small Intestines
OBSTRUCTION
Impairment in the normal flow of the luminal contents
Could either be extrinsic or intrinsic
Causes Of Intestinal Obstruction
NEONATE
INFANT
YOUNG ADULT
Atresia
Groin hernia
Adhesion
Midgut
volvulus
Intussusception
Groin hernia
Meconium
ileus
Meckels
diverticulum
CAUSES
SYMPTOMS
SIGNS
PLAIN FILMS
(initial dx
modality)
SBO vs COLONIC Obstruction
SBO
COLONIC
Adhesions
Cancer Inflammation
Groin hernias
Cramps
Cramps
Vomiting
Vomiting
-regular interval
-less frequent
Mid-moderate
Moderate-marked
distensions
distensions
Dilated air filled colon
Dilated loops with air fluid
with or without small
levels, paucity (few) distally.
bowel distention
EARLY DIAGNOSIS is the key to management
Mechanical blockage with failure of passage of bowel
contents.
CAUSES OF MECHANICAL OBSTRUCTION
Small Bowel Obstruction (80%)
20% of SURGICAL hospital admissions for ACUTE
ABDOMEN
TOP 3 Causes of SBO in WESTERN Society
Post-operative adhesion (50-75% overall)
Crohns disease (5% overall)
Primary & Metastatic Neoplasia (0-15% overall)
primary or extrinsic compression or invasion
Predominant cause in DEVELOPING countries
Hernias (8-15% overall)
External/Internal Hernia
OTHER CAUSES
Midgut volvulus
Superior mesenteric artery syndrome
compression of transverse duodenum
Intussusception
Hematoma
Gallstone
Bezoars
MIDGUT VOLVULUS
3
ADULT
Post-op
Adhesions
(70%)
Groin hernia
(10%)
- could
progress to
encarcerated
hernias
Cancer
(5%)
PATHOPHYSIOLOGY
According to Anatomical Relationship to the Intestinal Wall
EXTRALUMINAL or EXTRINSIC
Adhesions
60%, especially after pelvic surgery.
MAIN CAUSE of SBO in adults
Majority is POST-operative
Minority d/t PERITONITIS
Diagnosis of SBO d/t adhesion if primarily
one of exclusion
Adhesive bands not seen on conventional
CT
Only abrupt change in caliber of the bowel
is seen without any associated mass lesion,
significant inflammation, or bowel wall
thickening at the transition point
HISTORY is important for correlation
Neoplastic
20%, majority are metastatic that have
peritoneal implants.
Can compress adjacent tissues
Carcinomatosis
widespread dissemination of cancer
throughout the body
Hernias
10% of cases
MOST COMMON cause of SBO in
DEVELOPING countries
Classified according to ANATOMIC location
of the orifice through w/c the bowel
protrudes
EXTERNAL Hernias
most common
ventral or inguinal
DIAGNOSIS
Obvious
on
clinical
examination in most cases
INTERNAL Hernias
less common
occurs when there is protrusion of
the
viscera
through
the
peritoneum or mesentery & into a
compartment w/in the abdominal
cavity
DIAGNOSIS
Almost always RADIOLOGIC
Abscesses
Abscesses Forms a fibrous bands
Constrict and obstruct lumen
Endometriosis
Affects 5% of women of reproductive age
Exact prevalence of bowel endometriosis is
UNKNOWN
GENERAL SURGERY: SMALL INTESTINE
INTRAMURAL or INTRINSIC
Neoplasms
Primary neoplastic cause of SBO are rare
Intrinsic neoplasms <2% pf gastrointestinal
malignancies
Adenocarcinoma
50 %
distal duodenum and proximal
jejunum
cause hemorrhage or ulceration.
SBO d/t aSB adenocarcinoma indicates
an advanced state & shows
pronounces, asymmetric, & irregular
mural thickening
Lymphomas
20%
non-Hodgkins
Ileum> Jejunum> Duodenum.
Occasionally obstruct.
Carcinoid
>50% in distal ileum
Most asymptomatic.
Leiomyosarcoma
> 5 cm in diameter.
Obstruction, bleeding, perforation is
common.
Gastrointestinal Stromal Tumor (GIST)
Inflammatory
Crohns:
Acute inflammation, edema or
stricture
Bowel
luminal
narrowing
d/t
transmural
acute
inflammatory
process
CICATRICAL Stenosis of affected
segments
Manifestation of long standing
disease
CAUSES
Adhesions
incisional hernias
exacerbation
of
the
inflammatory condition
postoperative strictures in
patients
who
have
undergone
previous
intestinal surgery
Infectious
Congenital
Mesenteric defect can occur even after
surgery.
CONGENITAL DEFECT in the mesentery
Hole
Small Intestines
Herniate Into Defect
SURGERY BLOCK
2012
Hematomas
May occur secondary to
anticoagulant therapy
iatrogenic intervention
trauma
Radiation Enteritis
Obstruction in the late phase 1 year after
radiation therapy, usually to the pelvis
Ileal loops
Most affected part of SB
Causes SBO primarily by
producing adhesive & fibrotic changes
in the mesentery
luminal narrowing & dysmotility
induced by Radiation Serositis
Vascular Causes
Occlusion of the mesenteric arterial or
venous vascular supply ISCHEMIA wall
thickening SBO
CT Scan
FINDINGS
thrombosis or occlusion of the
mesenteric vessels
thickening of the bowel wall
PNEUMATOSIS & air in the
PORTAL System seen in bowel
infarction
INTRALUMINAL (with in the lumen)
Gallstones
resulting to gallstone ileus
rare complication of GB stone through a
biliary-intestinal fistula with subsequent
impaction in the small bowel
CT findings are pathognomonic:
TRIAD
Pneumobilia
Ectopic gallstone
SBO
Enterolithiasis
mineral concretion or calculus formed
anywhere in the gastrointestinal system.
Bezoars
balls of undigested materials, insoluble
fiber, and undissolved medicines that resist
the action of digestive enzymes in the
stomach.
Foreign Body
CLINICAL PRESENTATION
Colicky abdominal pain
Abdominal distention
Obstipation
Nausea and Vomiting
Vomiting
more common in proximal obstruction,
small bowel more than large bowel
Feculent vomiting
distal or late obstruction
do immediate surgery
INTERNAL HERNIA
MECHANICAL OBSTRUCTION
Malrotation, duplication, congenital bands
Bands
fibrous tissue that kink the area of the
small bowel.
Intussusception
Relatively rare in adults
<5% of SBOs
Only
LEAD-POINT
intussusceptions
secondary to neoplasms, adhesion, or
foreign bodies are a/w SBO
Diarrhea
In both partial and complete obstruction, it may be
present in the early in the course because of
increased motility and contractile activity of the
GENERAL SURGERY: SMALL INTESTINE
bowel in order to propel luminal contents beyond the
obstruction.
Increased or decreased bowel sounds:
Increased in early, may see peristaltic waves
Decreased in late, because of bowel exhaustion.
Note interval, frequency, audible rushes of
bowel sounds.
Overflow diarrhea
only liquid can pass the obstruction.
Hypotension and Shock
Can be d/t Bacteremia Sepsis Septic Shock
Bowel dilates with accumulation of water and
electrolytes in the lumen and within the wall of the
bowel (third space) leading to dehydration and
hypotension Third Space Loss
Accumulation of
H2O & E+/- in
Lumen & 3rd space
Dilatation of the
bowel
HYPOTENSION
DEHYDRATION
Bacteremia
Bacterial translocation:
E. coli
Strep faecalis
Klebsiella
Small intestinal lumen contents translocate in the
systemic circulation leading to bacteremia
Compromised ventilation
d/t:
Increased abdominal pressure
decreased venous return
elevation of diaphragm
Fever
Inflammatory response
Strangulated bowel
Closed loop obstruction
has increased intraluminal pressure with
decrease mucosal blood flow.
Ischemia more pronounced in closed loop
obstruction like volvulus
suspect if patient is with persistent fever.
more pronounce in both end strangulation.
IL-1 (fever)
IL-2 (recruitment of macrophage)
LABORATORY FINDINGS
Hemoconcentration
represented by Hct
increased concentration of cells and solids in the
blood usually resulting from loss of fluid to the tissues
indicative of dehydration
Early signs of dehydration:
tongue dryness: 1-1.5L fluid loss.
Late signs of dehydration
Sunken eyeballs: >2L fluid loss
Leukocytosis
Guaiac positive:
Fecal Occult Blood Test for presence of blood in the
feces that is not visibly apparent
Malignancy (Colorectal CA), Intussusception or
infarction, intestinal ischemia, TB enteritis.
Electrolyte imbalance
Proximal obstruction
Hypokalemic-Hypochloremic Alkalosis
Distal obstruction- less dramatic
STRANGULATED OBSTRUCTION
Example:
Volvulus
Closed loop obstruction a/w intestinal ischemia
Approximately 10% of patients with SBO due to delay in
diagnosis and surgical treatment
High mortality rate
FEATURES
tachycardia
localized abdominal tenderness
fever
marked leukocytosis
acidosis
laboratory findings:
elevated serum amylase, lipase, LDH,
phosphate and potassium
CT Scan
has a detection rate of 63%-100%
Findings: suggestive but not specific
Thickening and increased attenuation of the
affected bowel wall
A halo or target sign
Pneumatosis intestinalis
Gas in the portal vein
DIAGNOSIS
Goals
distinguish between mechanical obstruction from
ileus
NON Mechanical Differential Diagnosis
Adynamic Ileus d/t
Post Laparotomy
Pancreatitis
Peritonitis
Mesenteric Ischemia
Neuroleptics
Opiates
Where is the site of Obstruction?
Small Bowel
Large Bowel
whether it is partial or complete obstruction
differentiate between simple and strangulating
obstruction
Simple Obstruction
Wall Viability NOT compromise
Strangulated Obstruction
Compromised blood supply Intestinal
Ischemia
URGENT
surgery
vs
conservative management
determine the etiology
Clinical History & P.E.
RADIOLOGY
Plain Film
ADVANTAGES
Diagnostic in 50-60% of cases
look for small bowel distention, multiple
air-fluid levels, decreased colonic gas and
stool.
Widely available and low cost
TRIAD of small bowel obstruction
dilated small bowel (>3cm )
air-fluid levels seen in upright
paucity of air in the colon
DISADVANTAGES
NON-diagnostic & misleading in ~ 50%
Poor predictor of site or cause of
obstruction
Frequently fails to demonstrate findings of
ischemia or infarction
Upright Film
Look for air, fluid, bowel pattern, and
pneumothorax
Pneumothorax is an indication for surgery
because it can lead to perforation then
spillage of the intestinal content in the
peritoneum causing peritonitis.
Look for air under the diaphragm
Alternatives:
Chest x-ray if diaphragm is visible
Since no fluid
exchange or the
fluid remain in the
lumen & 3rd space
SURGERY BLOCK
2012
GENERAL SURGERY: SMALL INTESTINE
Left Lateral Decubitus if patient cant
sit or stand
Check air on lateral abdominal
wall area
Supine Film
Colonic gas seen in supine film
Pre-sacral (pelvic area)
(+) radiolucent, affected is the rectum
and may indicate a partial obstruction.
Shadow in the pre-sacral area
Air
radiolucent (dark)
Normal inside the bowel and lungs
Tissue
White hazy
Radiodense
Small intestine
see plicae circulares or valves of
Kerkring
Colon
See haustra
Air-Fluid Level:
Gas
due to swallowed air
Fluid
swallowed fluid
gastrointestinal secretion
increase
epithelial
water
secretion
More than 3 air-fluid level clinically
significant
Bowel distention
Obstruction elevated intramural
pressure ischemia necrosis
Presentation
for
strangulated
obstruction
Barium swallow and/or enema
ANTEGRADE CONTRAST study
DISADVANTAGE
Not useful in high grade obstruction
Water-soluble contrast usually diluted by
fluids in the bowel poor mucosal detail.
Slow transit time
Prolonged retention of barium
Not done in patient with complete
obstruction due to pressure.
Small Bowell Follow Through
Specific barium enema test for SI
Not done in complete obstruction d/t
pressure & risk of perforation
Enteroclysis
fluoroscopic X-ray of the small intestine
SURGERY BLOCK
2012
Radiocontrast is infused through a tube inserted
through the nose to the duodenum
images are taken in real time as the contrast
moves through aided by administration of
methyl cellulose
Sequential infusion promotes anterograde flow
beyond the point of obstruction
Positive predictive value 100%
Level of obstruction in 89%
Causes of obstruction in 86%
CT Scan
ADVANTAGE
High grade obstruction 81% sensitivity, 63%
with all grades.
Able to show cause of obstruction in 9395% of cases
Provides information regarding state of
bowel wall
Strangulation
closed loop obstruction
ischemia and infarction.
Findings of small bowel obstruction:
Discrete transition zone
Intra-luminal contrast unable to pass
beyond the transition zone
Colon containing little gas or fluid
Strangulation is suggested:
Thickening of the bowel wall
Pneumatosis intestinalis
gas cysts in the bowel wall
ominous finding in ischemia
Portal venous gas
Mesentery haziness
Poor uptake of intravenous contrast into
the wall of the affected bowel
Limitation: unable to detect partial intestinal
obstruction (<50% sensitivity)
IMPORTANT QUESTIONS TO ASK REGARDING SBO
Simple or Strangulated Obstruction?
Simple Strangulation
Considered when the bowel is only occluded at
one or several points along its course
Proximal part of the bowel is variably distended,
depends on the severity & duration
Strangulated Obstruction
10% of SBO
Most are closed loop
Diagnosed when a bowel loop of variable
length is occluded at 2 adjacent points
along its course
Occlusion can be partial or complete
Is ischemia present?
Venous mesenteric blood flow gets compromised first
vascular pressure & vessel engorgement w/
continuing arterial influx
Hemorrhage into bowel wall & lumen can occur &
finally arterial supply ceases d/t arterial spasms
following vascular resistance
TREATMENT
Points to Consider
Correct fluid & electrolyte imbalance:
Isotonic fluid
Monitor resuscitation (foley catheter/CVP)
NPO / TPN
Broad spectrum antibiotic (due to bacterial
translocation)
Placed NGT to decompress the stomach and decrease
nausea, distention and risk of aspiration
Expeditious celiotomy (to minimize risk of
strangulation).
Type of operation based on operative finding causing
intestinal obstruction
Non-operative Cases:
60-85% resolution
NG tube decompression, fluid resuscitation, bowel
rest
Serial exams and electrolyte management
GENERAL SURGERY: SMALL INTESTINE
IFC
Broad spectrum antibiotics
Conservative management is done when within 24-48
hours patients condition improved, meaning:
(-) fever
(+) bowel sounds
WBC
Conservative management preferred d/t no. of
surgery risk of adhesion
Indications:
Post-op Adhesions
Uncomplicated Bowel obstruction
REMEMBER the 6 Ns
NPO
NGT decompression
aNtacids (proton pump inhibitor) for ulcer
(NPO,NGT)
NSS Isotonic IV
aNtibiotics for bacterial growth
iNput and output (monitor urine )
Operative:
Complete obstruction that does not resolve
Incidence of strangulation increase significantly after
12-24 hours, manifested by
Fever
Tachycardia
Focal tenderness ( localized)
Leukocytosis (indicate disease progression)
Operative treatment depends on the etiology
lysis of adhesions
small bowel resection ( for strangulation)
Pathophysiology of Post-operative small bowel obstruction
Adhesions
Internal herniation
Inflammation
Preventive treatment of Post-operative small bowel
obstruction
NG tube
Gastrograffin challenge
100 cc of Gastrograffin is placed through the
NGT and then it is clamped for 2 hours, then get
a simple abdominal film
Decision to operate
Postoperative Ileus
Impaired intestinal motility
Most common cause of delayed discharge following
abdominal operations
Temporary and reversible
Resolve spontaneously & only require non-op mx
Aka: Pseudo-Obstruction
Defined as the prolonged inhibition of coordinated movements
of the GIT
Possible indicators:
N&V
Distention
Pain
Absence of the stool and flatus
ILEUS
7
SURGERY BLOCK
2012
ETIOLOGY
Abdominal surgery
Infection & inflammation (sepsis/peritonitis)
Electrolyte imbalance (Hypo K, Mg & Na)
Drugs (anticholinergic, opiates)
Visceral myopathies (degeneration/fibrosis of smooth
muscle)
Visceral neuropathies (degenerative disorders of
Myenteric & submucosal plexuses)
SYMPTOMS
Inability to tolerate solid & liquid by mouth
Nausea/vomiting
Lack of flatus & bowel movements
Diminished or absent bowel sound
Abdominal pain and distention
DIAGNOSIS
History of recent abdominal surgery
Discontinue opiates
Serum electrolyte determination
CT scan better than FPA in postoperative setting to
exclude presence of abscess or mechanical obstruction
PATHOPHYSIOLOGY
Accdg to Silo, et al:
Extensive inflammatory response within the intestinal
muscularis after bowel surgery.
Accdg to Behrendt, et al:
Direct relation between the inflammatory reaction
and the macrophages of the intestinal muscularis that
participate and functional
smooth muscle
impairment.
Accdg to Schwartz, et al:
Found an induction of cyclooxygenase-2 mRna and
protein in resident macrophages that decrease the
jejunal circular muscle contractility through the
prostaglandins
PREVENTION & TREATMENT
NPO, if prolong TPN is required
NGT to decompress the stomach
Correct fluid & electrolyte imbalance
Give ketorolac and reduce the dose of opioids
Cerulide, Erythromycin, Metoclopramide, Somatostatin
have all been studied as treatment for post-operative ileus
with no conclusive results.
Demonstrated
a
relationship
between
patient
expectations after surgery and outcome ( Disbrow, et al)
Showed benefits of chewing gums on postoperative bowel
motility believed to the be related to sham feeding (Asa0,
et al)
Multiple studies have demonstrated that patient will often
tolerate feeding within 24 hour after surgery.
Postoperative small bowel obstruction
Temporary return of bowel function followed by distention and
obstipation within 4 weeks of laparotomy
Principal indicators:
abdominal pain
vomiting
distension
obstipation
radiographic confirmation of postoperative small bowel
obstruction (Frank and Phillips)
Defined as crampy abdominal pain, vomiting and radiographic
findings consistent with intestinal obstruction after an initial
return of bowel function within 30 days after surgery (Ellozy, et
al)
Order of Return of normal bowel function
Small intestine
Stomach
Colon
DDx
Ileus is a differential diagnosis for obstruction
Ileus resolves spontaneously and may proceed to
obstruction.
Common cause of ileus:
Electrolyte imbalance
Potassium paralyzes the small bowel
Hypokalemia= hypoactive bowel
GENERAL SURGERY: SMALL INTESTINE
Special Forms of Obstruction
Stricture (narrowing)
CAUSES
Crohns
NSAIDS
Radiation therapy- increasing cause of adhesion
Mesenteric ischemia
DECREASED BLOOD FLOW
ISCHEMIA
ISCHEMIA
STRICTURE
FORMATION
TREATMENT
Resect and Restore normal bowel.
If chronic and progressive: resection is the best
approach
Internal hernias
Abnormalities related to prior surgeries
Congenital defects
Surgical repair of the defect with resection of nonviable bowel
If gangrenous, resect if not reduce.
Gallstone ileus
1-2% of intestinal obstruction affecting patients 60 years
and above
Stones >2.5 cm, enters the GIT by ulceration and
fistulization into the distal duodenum
Choledoduodenal fistula most common site of entry
Causes distal ileal obstruction
Presents with intestinal obstruction and aerobilia
Aerobilia
air in the biliary tree which is not normal
may cause perforation and fistula formation.
SURGICAL TREATMENT:
One stage procedure
recommended if patients condition is good and
anatomy is well-delineated.
three different procedures are conducted
simultaneously
Enterolithotomy (cutting the border of the
bowel longitudinally to remove gallstones)
Cholecystectomy (gallbladder removal)
Fistula repair (closing of the fistula).
Mirizzi's syndrome
rare cause of acquired jaundice
a/w large gallstones that compress the common
hepatic duct
obstructive jaundice can be caused by direct extrinsic
compression by the stone or from fibrosis caused by
chronic cholecystitis inflammation.
cholecystocholedochal fistula can occur.
How can gallstone get into the bowel?
GALLBLADDER STONE
EXCERT PRESSURE ON GALLBLADDER WALL
CREATES ADHESION B/W GALLBLADDER & DUODENUM
FISTULA FORMATION
SURGERY BLOCK
2012
Enterocutaneous Fistula
Abnormal communications linking two epithelialized surfaces.
abnormal communication between hollow viscera and skin.
Serious and dreaded complication of GI diseases and their
treatments, such as surgery.
Etiology:
Spontaneous 15% to 25%:
Radiation
IBD
Diverticular disease
Ischemic bowel
Appendicitis
Perforated duodenal ulcers
Malignancies
Post-operative 75% to 85%:
Anastomotic breakdown
Unrecognized bowel injuries during dissection or
abdominal closure.
Operations for cancer, IBD and lysis of adhesions are
most at risk
CLASSIFICATION
Output:
Low: 200 ml/24 hour
Moderate: 200 to 500 ml/24 hour
High: 500 ml/24 hour (poorer prognosis)
Anatomic Location in the GI tract:
Unfavorable: stomach, lateral duodenum, ligament of
Treitz, and ileum.
Favorable:
Esophagus,
duodenal
stump,
pancreaticobiliary, jejunum.
Anatomic features UNFAVORABLE for spontaneous
closure:
Foreign body
Radiation
Inflammation/Infection:
adjacent abscess or diseased bowel
Epithelialization of the fistula tract
Neoplasm
Distal obstruction
Fistula tract <2 cm length and enteral defects >1 cm.
Clinical Presentation:
Fever
Elevated WBC
Increased abdominal tenderness
Prolonged ileus
Signs of wound infection
th
th
Sepsis b/w the 5 and 10 postoperative days.
Drainage of enteric content (from the surgical wound)
either spontaneously or upon reopening of the wound.
RADIOLOGIC STUDIES
Plain radiography
GI contrast studies
Fistulograms
Ultrasonography
CT scan
Main role is to aid in the anatomic localization of the
fistula.
MANAGEMENT
Diagnosis and recognition
Stabilization and investigation
Control complications within 24 to 48 hours of recognition
of fistula.
MAIN GOAL is reduction of fistula output
Definitive care
Usually occurs if the fistula fails to respond to medical
treatment after 4 to 6 weeks.
Non-Op Management:
NPO
NG tube
H2 antagonist or PPIs
Protection
Drainage of abscess
Correction of fluid, electrolytes, and nutritional imbalances
Malnutrition is present in 55-90% of patient in ECF
responsible for most morbidity & mortality
should be considered if there is:
GENERAL SURGERY: SMALL INTESTINE
body weight loss of at least 10%
hypoproteinemia.
42% Mortality with serum albumin
<2.5 g/dl
Use of TPN is associated with spontaneous closure
Broad spectrum closure
Somatostatin: inhibit gastric, pancreatic, biliary, and
enteric secretions.
Octreotide
Somatostatins synthetic analogue
Definitive care:
Usually occurs if the fistula fails to respond to medical
treatment after 4 to 6 weeks.
Operative interventions:
Oversewing of the fistula
Resection of the diseased segment with primary
anastamosis.
Exteriorization
Serosal patch with either jejunum or
defunctionalized Roux
Laparotomy should be delayed to allow resolution of
intrabdominal adhesions for patients in the early
post-operative phase.
Major abdominal surgery results in a dense peritoneal
rd
th
reaction that is maximum from the 3 to the 10
postoperative week.
Surgery within this window may result in a more
difficult dissection and risks compounding technical
problems encountered.
During this period:
surgery is generally only undertaken if theres:
gangrene
peritonitis
bleeding
surgery is only limited to:
proximal defunctioning stoma formation
control of sepsis.
ECF closure can also be promoted by the use of :
vacuum-assisted closure systems
fibrin glue.
Small Bowel Neoplasm
SI General considerations
Rapid transit
Lower luminal bacterial load
Enhanced capacity to metabolize dietary carcinogens
Increase amount of lymphoid tissue
Clinical presentations
Intestinal obstruction
occult GIT hemorrhage
Growth, adhesion, kinking
Majority are benign
10% of all GI tumors (benign or malignant)
Rare d/t
Rapid transit time
Local immune system of the small bowel mucosa (IgA)
Alkaline pH
Relatively low concentration of bacteria; low
concentration of carcinogenic products of bacterial
metabolism.
Presence of mucosal enzymes (hydrolases) that destroy
certain carcinogens
Efficient epithelial cellular apoptotic mechanisms that
serve to eliminate clones harboring genetic mutation
50 60 y/o
Risk factors:
Red meat
Ingestion of smoked or cured foods
Crohns disease
Celiac sprue
Hereditary nonpolyposis colorectal cancer (HNPCC)
Familial adenomatous polyposis (FAD) 100% to develop
duodenal CA
Peutz-Jeghers syndrome
SURGERY BLOCK
2012
Symptoms:
Most are asymptomatic
Symptoms:
Vague abdominal pain
epigastric discomfort, N/V, abdominal pain,
diarrhea
Bleeding
hematochezia or hematemesis
Obstruction
intussuception, circumferential growth, kinking
of the bowel, intramural growth
MOST COMMON PRESENTATION:
crampy abdominal pain, distention, N&V
Hemorrhage
usually indolent
nd
2 common mode of presentation
Pathology and Differential diagnosis
Benign
Adenoma
Gardners syndrome and Familial Polyposis coli
predispose to small bowel adenoma
Leiomyoma
Fibroma
Hamartoma:
tissue elements normally found at that site, but
which are growing in a disorganized mass
Hamartomatous polyps occur as part of PeutzJeghers syndrome
Lipoma
Malignant
Adenocarcinoma
Crohns disease of small bowel and Celiac
disease predispose to adenocarcinoma, small
bowel lymphoma
Lymphoma
Carcinoid
DIAGNOSIS
More commonly located in the proximal small bowel
For most are asymptomatic it is rarely diagnosed
preoperatively
Serological examination
Serum 5-hydroxyindole acetic acid (HIAA) for
carcinoid.
CEA a/w small intestinal adenocarcinoma but only if
w/ liver metastasis
upper GI endoscopy or Upper GI series
Ancillary Tests
Radiological examination:
Enteroclysis
TEST OF CHOICE 90% sensitivity
UGIS w/ intestinal follow through
Small bowel follow through
CT scan
Angiography / RBC scan --> bleeding lesions
Endoscopy:
EGD (esophagus, gastric, and duodenum)
Colonoscopy
Push endoscopy
Extended small bowel enteroscopy
BENIGN NEOPLASM
Majority cause no symptoms and are discovered
incidentally
Adenomas are the most common
Adenoma
GENERAL SURGERY: SMALL INTESTINE
SURGERY BLOCK
2012
Leiomyomas are the most common that cause symptoms.
Surgical excision is indicated
TYPES OF BENIGN TUMORS
Adenomatous Polyps
Tubular/True adenoma
Often asymptomatic
May bleed or cause obstruction
Low malignant potential
Usually seen in the ileum
Villous adenoma
Greater malignant potential
30% harbor malignant foci on detailed
microscopic evaluation
Most common in the duodenum
In brunners gland
soap bubble appearance on contrast
radiography
No report of secretory diarrhea
Endoscopic polypectomy or submucosal
resection if non-invasive vs segmental
resection.
Brunners gland adenoma
Represent hyperplasia of the exocrine
glands of the duodenum
Little malignant potential
Mimic PUD
Lipoma
Leiomyoma
10
Leiomyoma and other stromal tumor
Most common symptomatic benign lesion
Associated w/ bleeding
Diagnosed by angiography
Jejunum most common location
May reach considerable size before diagnosis
May present as palpable, movable abdominal
mass
Obstruction, pain, bleeding
2 growth pattern:
Intramurally obstruction
Both intramural and extramural
Dumbbell shaped
Majority are asymptomatic
Segmental resection is the recommended
treatment.
Tumor grade, based on mitotic activity and size
correlate with prognosis
<5 cm almost always benign
>5 cm behave malignant, 50% dead within 3
years of recurrent disease.
Lipoma
Most commonly in the ileum
No malignant potential
do not require removal unless symptomatic
May form lead point intussusception
Distinguishable by CT because of low attenuated
appearance.
Peutz-Jeghers Syndrome
Hamartomatous Polyps
Inherited syndrome of:
Mucocutaneous melatonin pigmentation:
face, buccal mucosa, palm, sole,
perianal area
Gastrointestinal polyp
enteric jejunum and ileum are most
frequent part of GIT followed by
colon, rectum and stomach
Symptoms:
colicky abdominal pain
due to intermittent intussuception
Hemorrhage
Treatment:
Segmental resection of the bowel causing
obstruction or bleeding.
Cure IMPOSSIBLE due to widespread
intestinal involvement
Fibromas
Hemangiomas
Neurofibromas
CLINICAL PRESENTATION
Bowel Obstruction
can be d/t lead point intussuseption
Chronic Anemia
d/t chronic blood loss
(+) fecal occult blood
Acute Anemia
Melena
DIAGNOSIS
Barium follow through
Abdominal CT
Endoscopic Videocapsule for nonobstructing lesions
TREATMENT
Bowel resection w/ end to end anastomosis
MALIGNANT NEOPLASM
General consideration:
Obstruction and occult bleeding
Delay in diagnosis is common
Surgical resection seldom curative
th
th
6 to 7 decade of life
Adenocarcinoma most common, then carcinoid,
lymphoma and leiomyosarcoma
Palliation with bypass if non-resectable
Tumor Type
ADENOCA
CARCINOID
LYMPHOMA
GIST
MALIGNANT NEOPLASMS OF SMALL BOWEL
Cell of Origin
Frequency
Predominant Site
Epithelial Cell
35-50%
Duodenum
Enterochromaffin
20-40%
Ileum
Cells
Lymphocytes
10-15%
Ileum
Interstitial Cell of
10-15%
Cajal
TYPES OF MALIGNANT NEOPLASM
Adenocarcinoma
Most common CA of small bowel
About half of all small bowel malignancies
2x more common in MEN
Commonly WELL DIFFERENTIATED mucussecreting tumors
Presents with
weight loss
bleeding
anemia
GENERAL SURGERY: SMALL INTESTINE
11
obstruction
jaundice.
Most lesions located in proximal bowel
Most common in duodenum and proximal
jejunum
Half involve the ampulla of Vater.
Spreads to
Lymph nodes
Liver
Peritoneal serosa
MANAGEMENT
Resection
best treatment
Chemo/Radio:
INEFFECTIVE
PROGNOSIS
Patients w/ resectable tumors
5 year survival: 25%
Leiomyosarcoma
10-20% of all malignant small bowel tumors
Spread by:
direct extension
hematogenous route to liver, lungs or bone
Treatment:
wide en-bloc resection with associated
mesentery
Extended lymphadenectomy NOT INDICATED.
5 yr survival 10-50%
Low grade lesions 80% survival in 5 years
High grade lesions median survival of less
than 18 months.
Chemo/radio: INEFFECTIVE
Lymphoma
10-20% of malignant small bowel tumors
Ileum is most commonly involved
Primary small bowel lymphoma
most common extranodal form of
lymphoma.
Presents with fatigue, weight loss and abdominal
pain.
Treatment: primarily surgical
Adjuvant therapy RECOMMENDED with positive
margins
Carcinoid tumors
EPIDIMIOLOGY
20-40% of primary small intestinal
malignancies.
Most common tumor found in Meckels
diverticulum
th
Highest incidence in the 6 decade.
Multicentric 30%
Derived from ENTEROCROMAFFIN CELLS
Associated with secretion of neurohormonal
substances
Serotonin
substance P
LOCATIONS
50% located in the appendix
50% located in distal 3 feet of ileum
rectum
MORPHOLOGY
firm submucosal nodules with a yellow, tan
or gray cut surface
Follow as indolent course, with median duration
of 2 years of symptoms before diagnosis
METASTASIS
Metastatic disease present in 60% of cases
time of diagnosis.
Based on Location
3% metastatis from appendiceal and
rectal carcinoid
35% metastasis from ileal carcinoids.
Based on SIZE
Tumors 1-2 cm metastasize in about
50%
2 cm metastasize up to 90%
SURGERY BLOCK
2012
Metastasis to the liver may produce the
malignant carcinoid syndrome:
episodic diarrhea
flushing
abdominal cramps
later:
R-sided valvular heart disease
Asthma
Bronchoconstriction caused by
SEROTONIN & other vasoactive
substances secreted by tumor
Treatment:
Wide segmental resection
Resection of primary & metastatic tumor
Usually associated with primary tumors of the
foregut or midgut and rarely the hindgut
DIAGNOSIS
Elevated levels of serotonin
increases intestinal peristalsis
invokes intestinal fluid and electrolytes
secretion
Confirmed with 5HIAA (5
hydorxyindolacetic acid) urinary levels
inactive breakdown product of
5HT
I-meraio-dibenzylguanidine
scintigraphy
(MIBG)
occasionally be useful to localize midgut carcinoid tumors.
PROGNOSIS
3-year median survival with liver metastasis
versus 5 years in patient with nonresectable tumors without metastasis.
Overall 5-year survival 30-50%
GIST
Most common sarcoma of the GI tract
Clinical presentation is variable:
Tumors are often asymptomatic
Patients may have common, nonspecific
symptoms, resulting in underdiagnosis or
misdiagnosis
All GIST have the potential to become malignant
Risk is based on size and mitotic index at
presentation
Manifestations r/t location & size of tumor
Vague GI pain or discomfort
GI hemorrhage
Anemia
Anorexia
Weight loss
Nausea
Fatigue
Acute
Intraperitoneal
bleeding
or
perforation
15% Other (rectum,
esophagus, mesentery,
retroperitoneum)
25% Small intestine
50% Stomach
10% Colon
SITES of Growth
Stomach
MC site, 50%
Small Intestine 25%
Others: 15%
Rectum
Mesentery
Esophagus
Retroperitoneum
GENERAL SURGERY: SMALL INTESTINE
DIAGNOSIS
CT Scan of Abdomen & Pelvis w/ oral/IV
contrast
18FDG-PET
GIST are highly metabolic
Endoscopic Ultrasound
Liver Function Test
CBC
SURGICAL assessment
Resectable vs nonresectable
Primary tumor only vs metabolic
MANAGEMENT
Surgery
remains the PRINCIPAL treatment for
resectable primary GIST
Standard sarcoma chemotherapy
Ineffective
Limited response rate 5%
Median time to progression 3-4
months
No impact on survival
Surgical Consideration
goal of resection
Complete gross resection with the
intact pseudocapsule
GIST tend to displace, not invade,
surrounding organs
Negative microscopic margins are
desirable
Lymphadenectomy coz GIST rarely
metastasize to the regional lymph
nodes
Recurrence is common
CLINICAL PRESENTATION
Lower GIB Occult blood or Melena
Diarrhea
Perforation Peritonitis
Bowel Obstruction
DIAGNOSIS
Contrast Follow through
CT for elective cases
Plain Film Abdomen for acute cases
TREATMENT
Segmental Bowel Resection
Diverticular Disease of the Small Bowel
MECKELs DIVERTICULUM
TRUE congenital diverticulum
a small bulge in the small intestine present at birth.
Meckels Diverticulum
12
It is a vestigial remnant of the omphalomesenteric duct
Aka: vitelline duct or yolk stalk
most frequent malformation or congenital anomaly of
the gastrointestinal tract
Occurs 0.3-2.5% of the population
Usually between 3 and 5 cm long
Around 10-150 cm from ileocecal valve
60% presence of heterotrophic
mucosa has been
described including that of the gastric, duodenal, colonic
or pancreatic nature
Gastric mucosa (60%)
Pancreatic acini
Brunners gland
SURGERY BLOCK
2012
Pancreatic islets
Colonic mucosa
Endometriosis
Hepatobiliary tissues
RULES OF TWOS:
2% prevalence
2:1 female predominance
Location 2 feet (~ 40cm) proximal to the ileocecal
valve in adults.
Half of those are asymptomatic are younger than 2
years of age
Complications:
Ulceration
presents as hemorrhage or perforation
Perforation
intraluminal pressure from foreign body
Diverticulitis
virtually impossible to differentiate from
appendicitis
Obstruction
Volvulus of the intestine
Entrapment of intestine by the mesodiverticular
band
Intussuception
Stricture due to diverticulitis
Littres hernia
Meckels diverticulum within an inguinal
hernial sac or femoral hernia sac.
Can produce intussusception, volvulus or adhesive
band
Complication rates
Hemorrhage- 31%
Inflammation-25%
Bowel obsruction-16%
Intusussception-11%
Hernial involvement-11%
Fistula-4%
Tumors-2%
Chances of having complication
4.2%- children
3%-adults
0%-elderly
Clinical Manifestations
Asymptomatic
4% symptomatic due to complication
50% are younger than 10y/o
Symptomatic (Bleeding > obstruction >
diverticulitis)
Bleeding
50% in children and pt younger 18y/o
rare in pt older than 30y/o
intestinal obstruction most common in
adult
diverticulitis is indistinguishable to
appendicitis
Neoplasm seen: CARCINOID
Radionucleic scan (Meckels scan)
Diagnostic studies
Rarely demonstrated in Barium studies
Fistulogram in cases of umbilical fistula
For asymptomatic usually discovered as an
incidental findings in radiographic imaging,
endoscopy, or intraoperatively.
Enteroclysis
75% accuracy but not applicable during acute
cases.
Meckels scan
Radionuclide scans (99m Tc-pertechnate)
for ectopic gastric mucosa or in active bleeding
detects gastric mucosa; 90% accurate
Angiography to localize site of bleeder
Surgical treatment
Resection w/ enterorrhapy
if symptomatic or has complications
If
morbidity
approach
zero,
incidental
diverticulectomy should be performed
GENERAL SURGERY: SMALL INTESTINE
Diverticulectomy:
diverticulitis
obstruction w/ removal of associated band
Segmental resection for:
Bleeding
If with tumor
ACQUIRED SMALL BOWEL DIVERTICULA
FALSE diverticula
Epidemiology
Increases w/ age; seldom seen < 40y/o (50-70y/o)
DUODENUM DEVIERTICULA
Most common; usually adjacent to ampulla
90% are aymptomatic
75% arise in the medial wall
Periampullary regions
Causes
Cholangitis
Pancreatitis
CBD stones
AKA: periampullary, juxtapapillary, or periVaterian diverticula
JEJUNOILEAL DIVERTICULA
RARE
May cause obstruction
80% - jejunum (tends to be large and multiple)
15% - ileum (tends to be small and solitary)
5% - both ileum and jejunum
COMPLICATION w/ diverticulum
Bleeding
Perforation
Bacterial overgrowth
Pathophysiology:
Abnormalities of intestinal smooth muscle or
dysregulated motility leading to herniation.
Associated w/:
Bacterial overgrowth vit B12 deficiency,
megaloblastic anemia, malabsorption &
steatorrhea
Periampullary duodenal diverticula:
Obstructive jaundice
Pancreatitis
Intestinal obstruction due to compression of
adjacent bowel
Diagnosis:
Best diagnosed w/ ENTEROCLYSIS
Treatment:
Asymptomatic ---> left alone
Bacterial overgrowth --> antibiotics
Bleeding and obstruction ---> segmental resection
for jejunoileal diverticula
Diverticulectomy if located in the duodenum
For medial duodenal diverticula ---> do lateral
duodenotomy and oversewing of the bleeder
May invaginate the diverticula into the
duodenal lumen then excised
If related to the ampulla ---> extended
sphincterotoplasty
If perforated ----> excised and closed w/
omental patch;
if inflammed ---> placed gastrojejunostomy
Short Bowel Syndrome
General considerations:
Normal adult tolerated resection because of excess GUT
mucosa
Duodenum:
Iron and Calcium absorption
Distal ileum
Vit. B12 and Bile salts
Up to 40% of the small bowel can be removed with
moderate sequelae
50%- significant sequelae
>70%-survival threatened
Etiology:
Massive resection of small bowel due to
13
SURGERY BLOCK
2012
thrombosis or embolus
Volvulus with massive resection in children
Small Bowel Neoplasm
Trauma
Chrons Disease
Mesenteric Infarction
Radiation Enteritis
Multiple Fistulas
Encountered in patients with jejuno-ileal by-pass for morbid
obesity
SHORT GUT SYNDROME
Resection of more than half of the small bowel length
serious malabsorption
Residual small bowel length of <2m diminished work
capacity
Residual small bowel length of <1m require home
parenteral nutrition on an indefinite basis
Ileal resections are less well tolerated than jejunal
resections
Complications
Loss of terminal ileum results in impairment of conjugated
bile salts and fat absorption
Survival threatened if less than two feet beyond
duodenum.
Limited ileal resection increases bile salt load to colon
resulting in mucosal injury and diarrhea
>100 cm ileal resection results in loss or total bile salt
pool leading to steatorrhea
Adaptive Responses
Mucosal hyperplasia
Increase in caliber of remaining small intestine.
Treatment
Initial therapy aimed at maintenance of fluid and
electrolyte balance
TPN
often indicated, sometimes throughout the lifetime
the patient.
Necessary for MASSIVE small bowel resection
Regimen must provide 40 Kcal/Kg body weight
Enteral nutrition enhance adaptive response
In 1m small bowel, TPN discontinued with time
d/t small bowel will hypertrophy
Intensive medical management:
High fiber diet
growth hormone
glutamine: essential aa
Oral nutrition is based on an elemental diet
Antiperistaltic agents should be given, vitamins, B12
parenteral
Surgical Approach
Intestinal lengthening procedures
<60 cm, intestinal transplantation
Chronic Idiopathic Inflammatory Disease of the
Bowel
CHRONs DISEASE
Regional, transmural, granulomatous enteritis.
Chronic, idiopathic inflammatory dse
Ethnic groups: East Europe (Ashkenazi Jew)
Female predominance, 2x higher smokers
st
Familial association: 30x in siblings, 13x in 1 degree
relatives).
Higher socioeconomic status
Breast feeding is protective
ETIOLOGY
Unknown
Hypothesis:
Infectious:
Chlamydia
Pseudomonas
Mycobacterium paratuberculosis
Listeria monocytogenesis
Measles
Yersinia enterocolitica
GENERAL SURGERY: SMALL INTESTINE
SURGERY BLOCK
2012
ChronS Disease
14
Immunologic abnormalities:
Humeral & cell-mediated immune reactions
against gut cells.
Genetic factors:
Chromosome 16 (IBD1 --> NOD2)
PATHOLOGY
Affect any portion of GIT:
Small bowel alone (30%)
Ileocolitis (55%)
Colon alone (15%)
HALLMARK: focal, transmural inflammation of the
intestine
EARLIEST SIGN:
aphthous ulcers
surrounded by halo erythema over a noncaseating granuloma
enlarge and coalesce transversely forming
cobblestone appearance.
Advanced dse: transmural inflammation.
COMPLICATIONS
adhesions to adjacent bowel,
stricture formation (fibrosis),
intra-abdominal abscesses,
fistula or free perforation (peritonitis)
Skip lesions and w/ fat wrapping
encroachment of mesenteric fat onto the serosal
surface
PATHOGNOMONIC for Crohns.
CLINICAL MANIFESTATIONS
Most common symptom:
Abdominal pain
Diarrhea
Weight loss
Other symptoms depends on type of complications:
obstruction (fibrosis)
perforation (peritonitis, fistula, intraabdominal
abscess)
toxic megacolon
marked colonic dilatation
abdominal tenderness
fever & leukocytosis)
cancer (6x greater/more advanced):
POOR PROGNOSIS
perianal dse (fissure, fistula, stricture or abscess)
Extra-intestinal manifestation:
erythema nodosum & peripheral arthritis are
correlated w/ severity of intestinal inflammation
DIAGNOSIS
Endoscopy
esophagogastroduodenoscopy (EGD)
colonoscopy
w/ biopsy.
Barium enema / intestinal series
Enteroclysis (small bowel)
MORE ACCURATE
CT scan to reveal intra-abd. abscesses
TREATMENT
Medical:
Intravenous fluids
NGT to rest GIT (elemental diet/TPN)
Medications:
to relieve diarrhea
relieve pain
control infection (antibiotic)
Anti-inflammatory
Aminosalicylates
Corticosteroid
immunomodulators
azathioprine 6-mercaptopurine
cyclosporine
SURGICAL
Indicated if:
with complications
Types:
Segmental resection w/ primary anastomosis:
Microscopic evidence of the dse at the resection
margin does not compromise a safe anastomosis,
hence, a frozen section is unnecessary.
Stricturoplasty
Bypass procedures (gastrojejunostomy)
TUBERCULOUS ENTERITIS
In developing and under develop countries
Resurgence in develop countries due to:
AIDS epidemic
Influx of Asian migrants
Use of immunosuppressive agents
Forms:
Primary infection:
caused by M. tuberculosis bovine from ingested
milk
Secondary infection
swallowing bacilli from active pulmonary TB
Tuberculous Enteritis
Patterns:
Hypertrophic causes stenosis or obstruction
Ulcerative diarrhea and bleeding
Ulcero-hypertrophic
Indication for surgery: Obstruction
Common in ileocecal area
Differential diagnosis ileocecal CA
Treatment:
Right hemicolectomy
if ileum and cecum are part of the disease colon
for perforation, obstruction, hemorrhage
Chemotherapy (given 2 wks prior to surgery up to 1
yr).
Rifampicin
Isoniazid
Ethambutol
TYPHOID ENTERITIS
Caused by Salmonella typhi
Diagnosis
Culture from blood or feces
Agglutinins against O and H antigen
Medical management
Chloramphenicol
trimethropin-sulfamethoxazole
amoxicillin
quinolones
Absolute indication for surgery
Perforation
Hemorrhage
GENERAL SURGERY: SMALL INTESTINE
Segmental resection (w/ primary anastomosis or
ileostomy)
DO RESECTION If patient is hemodynamically unstable
despite of transfusion
Mesenteric Ischemia
Clinical Syndrome:
ACUTE MESENTERIC ISCHEMIA
Pathophysiology
Arterial embolus:
most common: 50% from the heart
usually lodge distal to origin of the middle
colic artery
Arterial thrombosis:
occlusion occurs at proximal near its origin.
Vasospasm
Aka: Nonocclusive Mesenteric Ischemia
(NOMI)
usually in critically-ill pt. receiving
vasopressors.
Venous thrombosis:
5-15%
95% SMV
Primary:
no etiologic factor identified
Secondary:
heritable or acquired coagulation
disorder
CHRONIC MESENTERIC ISCHEMIA
Develops insidiously allows for collateral circulation
to develop
Rarely leads to infarction.
Usually due to arteriosclerosis
Usually two mesenteric arteries are involved
Manifestation:
ACUTE MESENTERIC ISCHEMIA
Severe abdominal pain out of proportion to the
degree of abd. Tenderness: HALLMARK
Colicky at the mid-abdomen.
Nausea / vomiting, diarrhea
abd. Distention
peritonitis
passage bloody stool
CHRONIC MESENTERIC ISCHEMIA
Postprandial abd. pain food-fear
most common
No laboratory test sensitive for the detection of acute
mesenteric ischemia prior to the onset of intestinal infarction
The presence of its hallmark sign is an indication for immediate
CELIOTOMY
DIAGNOSTIC TOOLS
Angiography
most reliable: 74 100% sensitivity and 100%
specificity
It is GOLD STANDARD for the diagnosis of arterial
mesenteric ischemia
CT scanning is used to:
Disorder other than abdominal condition causing
abdominal pain
Evidence of occlusion or stenosis of mesenteric
vasculature.
Evidence of ischemia in the intestine & mesentery
TEST OF CHOICE for acute mesenteric venous
thrombosis
Treatment:
w/ signs of peritonitis --> celiotomy
check for viability of the bowel:
Necrotic ----> segmental resection
Questionable viability ----> second look laparotomies
Surgical revascularization (embolectomy / thrombectomy
/ mesenteric bypass).
Not done if:
segment is necrotic
patient too unstable
Done if pt diagnosed w/ emboli or thrombus-induced
acute mesenteric ischemia w/o signs of peritonitis.
15
SURGERY BLOCK
2012
May give thrombolysis
Thrombolytic agents:
Streptokinase
Urokinase
recombinant tissue plasminogen activator
Useful only in partially occluded vessels
given w/in 12 hrs. after onset of symptoms.
EVALUATION
EVALUATION OF
Small Intestines Disorders
Radiology
PAF
Upright & Supine Position
Assess obstruction & perforation
SIGNS of Obstruction
Air fluid level
Absence of pre-sacral gas
pneumoperitoneum
Patient with acute abdominal pain, distention, nausea, vomiting &
obstipation
PLAIN ABDOMINAL RADIOGRAPHY
Complete or high grade
partial SBO
Surgical
Mgt.
Normal equivocal low grade
partial SBO
Cross sectional
imaging
-Sonography*
-MDCT: start at the end!
1.Confirm the diagnosis
2.Characterize the severity of obstruction
3.Identify the transition pt.
4.Identify the cause of obstruction
5.Look for complication
SBFT or
Enteroclysis/CT
enteroclysis
Mgt:
Conservative
Surgery
*useful primarily when CT is unavailable
Small Bowel Follow Through
Establish investigation to outline the small bowel
Assess
Tumors
Chrons Disease
Fistula
Polyps
Esophagus, stomach, duodenum are easily occluded in detail
Small bowel is then radiographed at periodic intervals &
fluoroscopically taken
Enteroclysis
minimally invasive radiographic procedure of the small
intestine
require the introduction of a catheter
INDICATIONS
Suspected/Known small bowel obstruction
Neoplasm (cancer)
Inflammatory bowel disease
Unexplained GI bleeding
DISADVANTAGES
Uncomfortable to the patient
Higher dose of radiation
GENERAL SURGERY: SMALL INTESTINE
16
ADVANTAGES
much quicker than a routine single contrast small bowel
follow through exam
luminal distention will straighten the circular walls & will
determine the thickness
INVESTIGATIONS
Selective Splanchnic Angiography
reliable method for detection of angioplastic lesions
bleeding can be located if the patient is bleeding
actively at the time of investigation
>1cc
Isotope Labeled Red Cells
occult GI bleeding
at least 0.5 cc for 24 hr period
SURGERY BLOCK
2012
Das könnte Ihnen auch gefallen
- Bowel AnastomosisDokument30 SeitenBowel AnastomosismrashaiedehNoch keine Bewertungen
- Absite CH 32 BilliaryDokument14 SeitenAbsite CH 32 BilliaryJames JosephNoch keine Bewertungen
- Bile Duct InjuryDokument62 SeitenBile Duct InjuryShashidhara Puttaraj100% (1)
- Atlas of Surgery Cameron Volume II. 2ndDokument6 SeitenAtlas of Surgery Cameron Volume II. 2ndAlberto RamírezNoch keine Bewertungen
- Preparing Severely Jaundiced Patient For SurgeryDokument2 SeitenPreparing Severely Jaundiced Patient For Surgerylentini@maltanet.netNoch keine Bewertungen
- Dr. E. J. Arteen F.R.C.S General & Colorectal Consultant Surgeon European-Gaza HospitalDokument83 SeitenDr. E. J. Arteen F.R.C.S General & Colorectal Consultant Surgeon European-Gaza Hospitalpt.mahmoudNoch keine Bewertungen
- Penetrating Abdominal TraumaDokument3 SeitenPenetrating Abdominal TraumaamrulNoch keine Bewertungen
- Rectal Cancer PPT 2.1Dokument131 SeitenRectal Cancer PPT 2.1Usmle GuyNoch keine Bewertungen
- Management of Anastomotic Complications of Colorectal SurgeryDokument13 SeitenManagement of Anastomotic Complications of Colorectal Surgerydadupipa100% (1)
- In Service Exam For Breast DR Paul BalisiDokument11 SeitenIn Service Exam For Breast DR Paul BalisiAmiel Francisco ReyesNoch keine Bewertungen
- Basic Science Questions: ND RD TH THDokument42 SeitenBasic Science Questions: ND RD TH THShaira Aquino VerzosaNoch keine Bewertungen
- Operative Surgery ManualDokument273 SeitenOperative Surgery Manualvikeshramkelawon8422100% (1)
- Surgery II - Pancreas 2014Dokument20 SeitenSurgery II - Pancreas 2014Medisina101Noch keine Bewertungen
- Absite Review QuestionsDokument81 SeitenAbsite Review QuestionsJames JosephNoch keine Bewertungen
- Pancreatic Cancer: Early Detection Offers Best Chance of CureDokument18 SeitenPancreatic Cancer: Early Detection Offers Best Chance of Curemywifenoor1983Noch keine Bewertungen
- Safe CholecystectomyDokument60 SeitenSafe CholecystectomyCarlos Reyes100% (1)
- Pancreatic and Duodenal Injuries UpdateDokument59 SeitenPancreatic and Duodenal Injuries UpdateAndrie KundrieNoch keine Bewertungen
- Updated review of diagnosis and treatment of cystic hepatic lesionsDokument8 SeitenUpdated review of diagnosis and treatment of cystic hepatic lesionsMayerlin CalvacheNoch keine Bewertungen
- Oncoplastic and Reconstructive BreastDokument14 SeitenOncoplastic and Reconstructive BreastYefry Onil Santana Marte100% (1)
- Subtotal Cholecystectomy-''Fenestrating'' Vs ''Reconstituting'' Subtypes and The Prevention of Bile Duct Injury - Definition of The Optimal Procedure In  Difficult Operative ConditionsDokument8 SeitenSubtotal Cholecystectomy-''Fenestrating'' Vs ''Reconstituting'' Subtypes and The Prevention of Bile Duct Injury - Definition of The Optimal Procedure In  Difficult Operative ConditionsBolivar Isea100% (1)
- Blunt Adominal TraumaDokument14 SeitenBlunt Adominal TraumaMuhammad Bima AkbarNoch keine Bewertungen
- Duodenal Stump LeakageDokument14 SeitenDuodenal Stump LeakageCosmin NicolescuNoch keine Bewertungen
- General Surgery (Must Know)Dokument93 SeitenGeneral Surgery (Must Know)Binit BharatiNoch keine Bewertungen
- Internal Hernias Diagnosis and TypesDokument26 SeitenInternal Hernias Diagnosis and TypesIslam MagdyNoch keine Bewertungen
- Dr. Asif Mian Ansari DNB Resident Dept. of General Surgery Max Hospital, MohaliDokument25 SeitenDr. Asif Mian Ansari DNB Resident Dept. of General Surgery Max Hospital, MohaliKarem Maali100% (1)
- ABSITEDokument38 SeitenABSITEVik SharNoch keine Bewertungen
- ABSITE Review of Surgery QuestionsDokument40 SeitenABSITE Review of Surgery QuestionsPoppip PipNoch keine Bewertungen
- Surgery TacticsDokument154 SeitenSurgery TacticsAiman Arifin0% (1)
- NEET SS January 2022 MCh GI Surgery RecallDokument58 SeitenNEET SS January 2022 MCh GI Surgery RecallRajhan 410Noch keine Bewertungen
- Bowel Anastomosis TechniquesDokument43 SeitenBowel Anastomosis Techniquesprabowoaji12100% (1)
- Duodenal InjuryDokument54 SeitenDuodenal InjuryTony HardianNoch keine Bewertungen
- ABSITE CH 10 Nutrition PDFDokument8 SeitenABSITE CH 10 Nutrition PDFJames JosephNoch keine Bewertungen
- Prof - Amer Eltwati Ben Irhuma Consultant Surgeon Sebha Medical CollegeDokument79 SeitenProf - Amer Eltwati Ben Irhuma Consultant Surgeon Sebha Medical Collegeckyew64100% (1)
- Breast Absite QuestionsDokument18 SeitenBreast Absite QuestionsGeshabelle ApuraNoch keine Bewertungen
- Principles of Laparoscopic & Robotic Surgery: Aaquila Sherin Bismi J J Blessy OommanDokument46 SeitenPrinciples of Laparoscopic & Robotic Surgery: Aaquila Sherin Bismi J J Blessy OommanAsif AbbasNoch keine Bewertungen
- Gall Stone Disease: DR M.farhad General SurgeonDokument56 SeitenGall Stone Disease: DR M.farhad General SurgeondrelvNoch keine Bewertungen
- Beck, David E. - Kann, Brian R. - Margolin, David A. - Vargas, H. David - Whitlow, Charles B - Improving Outcomes in Colon and Rectal Surgery (2019, CRC Press - Taylor & Francis Group)Dokument441 SeitenBeck, David E. - Kann, Brian R. - Margolin, David A. - Vargas, H. David - Whitlow, Charles B - Improving Outcomes in Colon and Rectal Surgery (2019, CRC Press - Taylor & Francis Group)Daniel StaniloaieNoch keine Bewertungen
- 7 Liver - Spleen TraumaDokument34 Seiten7 Liver - Spleen Traumabagus75% (4)
- Git DisturbancesDokument119 SeitenGit DisturbancesPeterpan NguyenNoch keine Bewertungen
- Chapter 5 ATLSDokument27 SeitenChapter 5 ATLSUlfaa MutiaaNoch keine Bewertungen
- Management of The Pancreatic Remnant During Whipple OperationDokument4 SeitenManagement of The Pancreatic Remnant During Whipple OperationYacine Tarik Aizel100% (1)
- 5B Surgery 1st-2nd SE #28-32 #17-18Dokument3 Seiten5B Surgery 1st-2nd SE #28-32 #17-18Liza SoberkaayoNoch keine Bewertungen
- NEET-SS GI SurgeryDokument72 SeitenNEET-SS GI SurgeryadiNoch keine Bewertungen
- Manual of Surgery Volume FirstDokument538 SeitenManual of Surgery Volume Firstmiky1320100% (2)
- Hemicolectomy 1Dokument40 SeitenHemicolectomy 1Preethi GudipalliNoch keine Bewertungen
- Endoscopic SurgeryDokument152 SeitenEndoscopic SurgeryiciNoch keine Bewertungen
- Acute Abdominal Pain MS LectureDokument63 SeitenAcute Abdominal Pain MS Lectureheka_amrongNoch keine Bewertungen
- Abdominal Surgery All in OneDokument50 SeitenAbdominal Surgery All in OneAnne ChoyNoch keine Bewertungen
- Atlas of Surgical Techniques For Colon, Rectum and AnusDokument414 SeitenAtlas of Surgical Techniques For Colon, Rectum and AnusjenniferjebamaniNoch keine Bewertungen
- INGUINAL-SCROTAL SWELLINGS GUIDEDokument23 SeitenINGUINAL-SCROTAL SWELLINGS GUIDEAzmyza Azmy100% (1)
- Artery First Approach To Pancreatic Cancer Resection A Review of The Evidence For BenefitDokument3 SeitenArtery First Approach To Pancreatic Cancer Resection A Review of The Evidence For BenefitFlaviu Ionuț FaurNoch keine Bewertungen
- All You Need To Know About Vascular SurgeryDokument33 SeitenAll You Need To Know About Vascular SurgeryDr. Vinicius MajdalaniNoch keine Bewertungen
- Nir Hus Absite Review Q10Dokument11 SeitenNir Hus Absite Review Q10nir4846Noch keine Bewertungen
- Anatomy of OesophagusDokument25 SeitenAnatomy of OesophagusRabi SyedNoch keine Bewertungen
- Recent Advances in SurgeryDokument42 SeitenRecent Advances in SurgerymohanNoch keine Bewertungen
- Pouchitis and Ileal Pouch Disorders: A Multidisciplinary Approach for Diagnosis and ManagementVon EverandPouchitis and Ileal Pouch Disorders: A Multidisciplinary Approach for Diagnosis and ManagementNoch keine Bewertungen
- The Surgical Oncology Review: For the Absite and BoardsVon EverandThe Surgical Oncology Review: For the Absite and BoardsNoch keine Bewertungen
- The Guide to Breast Reconstruction: Step-By-Step from Mastectomy Through ReconstructionVon EverandThe Guide to Breast Reconstruction: Step-By-Step from Mastectomy Through ReconstructionBewertung: 4 von 5 Sternen4/5 (1)
- Congestive Heart Failure - Dra. DeduyoDokument10 SeitenCongestive Heart Failure - Dra. DeduyoMedisina101Noch keine Bewertungen
- Acute Coronary Syndrome - Dra. Deduyo PDFDokument6 SeitenAcute Coronary Syndrome - Dra. Deduyo PDFMedisina101Noch keine Bewertungen
- Infective Endocarditis - Dr. Payawal PDFDokument6 SeitenInfective Endocarditis - Dr. Payawal PDFMedisina101Noch keine Bewertungen
- Deep Vein Thrombosis - Dr. Deduyo PDFDokument17 SeitenDeep Vein Thrombosis - Dr. Deduyo PDFMedisina101Noch keine Bewertungen
- Aortic Stenosis Symptoms and Physical Exam FindingsDokument9 SeitenAortic Stenosis Symptoms and Physical Exam FindingsMedisina101Noch keine Bewertungen
- Coronary Artery Disease - Dra. Deduyo PDFDokument7 SeitenCoronary Artery Disease - Dra. Deduyo PDFMedisina101Noch keine Bewertungen
- Detecting Abnormal Cardiac RhythmsDokument10 SeitenDetecting Abnormal Cardiac RhythmsMedisina101100% (1)
- Arrythmia Part 2 - Dr. Payawal PDFDokument8 SeitenArrythmia Part 2 - Dr. Payawal PDFMedisina101Noch keine Bewertungen
- ECG Part 1 - Dr. Payawal PDFDokument10 SeitenECG Part 1 - Dr. Payawal PDFMedisina101Noch keine Bewertungen
- ECG Part 2 - Dr. Payawal PDFDokument4 SeitenECG Part 2 - Dr. Payawal PDFMedisina101Noch keine Bewertungen
- Peripheral Vascular Medicine - Dr. Deduyo PDFDokument14 SeitenPeripheral Vascular Medicine - Dr. Deduyo PDFMedisina101Noch keine Bewertungen
- Diseases of the Aorta: Causes and Types of Aortic AneurysmsDokument11 SeitenDiseases of the Aorta: Causes and Types of Aortic AneurysmsMedisina101Noch keine Bewertungen
- Pedia Pulmo I 10.4.16Dokument129 SeitenPedia Pulmo I 10.4.16Medisina101Noch keine Bewertungen
- Diagnosing Chest Pain CausesDokument8 SeitenDiagnosing Chest Pain CausesMedisina101Noch keine Bewertungen
- Valvular Heart Diseases Part 1 - Dr. BartolomeDokument18 SeitenValvular Heart Diseases Part 1 - Dr. BartolomeMedisina101Noch keine Bewertungen
- External Abdominal Hernias GuideDokument12 SeitenExternal Abdominal Hernias GuideMedisina101100% (1)
- Congenital Heart Diseases - Dr. BartolomeDokument12 SeitenCongenital Heart Diseases - Dr. BartolomeMedisina101Noch keine Bewertungen
- Cardiac Tumors Slides - Dr. BartolomeDokument81 SeitenCardiac Tumors Slides - Dr. BartolomeMedisina101Noch keine Bewertungen
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Dokument13 SeitenSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101Noch keine Bewertungen
- Pedia Pulmo 3 11.03.16Dokument49 SeitenPedia Pulmo 3 11.03.16Medisina101Noch keine Bewertungen
- Acquired Heart DiseaseDokument44 SeitenAcquired Heart DiseaseMedisina101Noch keine Bewertungen
- Cardiac Tumors - Dr. BartolomeDokument12 SeitenCardiac Tumors - Dr. BartolomeMedisina101Noch keine Bewertungen
- Pedia Pulmo 2 10.18.16Dokument73 SeitenPedia Pulmo 2 10.18.16Medisina101Noch keine Bewertungen
- SURGERY Lecture 4 - Breast (Dra. Fernandez)Dokument15 SeitenSURGERY Lecture 4 - Breast (Dra. Fernandez)Medisina101100% (1)
- PEDIA - Cardio (Esguerra) PDFDokument9 SeitenPEDIA - Cardio (Esguerra) PDFMedisina101Noch keine Bewertungen
- SURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Dokument19 SeitenSURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Medisina101100% (1)
- Pediatric Cardiology II Lecture SummaryDokument5 SeitenPediatric Cardiology II Lecture SummaryMedisina101Noch keine Bewertungen
- Surgery II - Pancreas 2014Dokument20 SeitenSurgery II - Pancreas 2014Medisina101Noch keine Bewertungen
- Head and Neck SurgeryDokument15 SeitenHead and Neck SurgeryMedisina101100% (1)
- Digestive Anatomy LabDokument124 SeitenDigestive Anatomy LabMary Beth DawsonNoch keine Bewertungen
- Brain & Organ FunctionsDokument5 SeitenBrain & Organ FunctionsaysiiNoch keine Bewertungen
- Morbid Obesity Case StudyDokument12 SeitenMorbid Obesity Case Studyapi-437064053Noch keine Bewertungen
- Digesti Dan AbsorpsiDokument57 SeitenDigesti Dan AbsorpsisariNoch keine Bewertungen
- Digestive System Label MeDokument13 SeitenDigestive System Label MeMuhammad AdibNoch keine Bewertungen
- How Drugs Work - Basic Pharmacology For Healthcare ProfessionalsDokument19 SeitenHow Drugs Work - Basic Pharmacology For Healthcare ProfessionalsSebastián Pérez GuerraNoch keine Bewertungen
- Module 1 Foods 7tve ExploratoryDokument20 SeitenModule 1 Foods 7tve ExploratoryPoseidon NipNoch keine Bewertungen
- BIOCHEM DigestionDokument53 SeitenBIOCHEM DigestionAngelika Perez CunanNoch keine Bewertungen
- (BIO) Chapter 4 - Nutrition in HumanDokument21 Seiten(BIO) Chapter 4 - Nutrition in Humantaco ghoulNoch keine Bewertungen
- Drugs Acting On Blood and Blood Forming AgentsDokument29 SeitenDrugs Acting On Blood and Blood Forming AgentsSri RamNoch keine Bewertungen
- DigestiveDokument6 SeitenDigestiveanon_783012033Noch keine Bewertungen
- Effect of Fatty Acids or Calcium Soaps On Rumen and Total Nutrient DigestibilityDokument9 SeitenEffect of Fatty Acids or Calcium Soaps On Rumen and Total Nutrient DigestibilityBruno DamiãoNoch keine Bewertungen
- 2018 Year 11 Human Biology ATAR Course OutlineDokument21 Seiten2018 Year 11 Human Biology ATAR Course OutlineNessrynNoch keine Bewertungen
- Lesson Plan Digestive System DETAILEDDokument14 SeitenLesson Plan Digestive System DETAILEDElezalde Labadan MacasNoch keine Bewertungen
- Secretion of Small IntestineDokument18 SeitenSecretion of Small IntestineMaliha MumtazNoch keine Bewertungen
- Frog Dissection ADokument7 SeitenFrog Dissection AFrances AguinaldoNoch keine Bewertungen
- Photosynthesis and Digestion ProcessesDokument4 SeitenPhotosynthesis and Digestion ProcessesRajender Kumar SharmaNoch keine Bewertungen
- 5 stages nutrition processDokument52 Seiten5 stages nutrition processhueymeyNoch keine Bewertungen
- CSEC Biology DigestionDokument53 SeitenCSEC Biology DigestionKemoy FrancisNoch keine Bewertungen
- Digestive System: MouthDokument5 SeitenDigestive System: MouthSTEPHEN OTEDANoch keine Bewertungen
- NMAT Biology ReviewerDokument27 SeitenNMAT Biology Reviewermarin kitagawaNoch keine Bewertungen
- Foods For Your Thoughts On Nutrition and Functional FoodsDokument40 SeitenFoods For Your Thoughts On Nutrition and Functional FoodsĐặng Nhật100% (1)
- The Human Digestive SystemDokument12 SeitenThe Human Digestive SystemmarwaNoch keine Bewertungen
- Digestive SystemDokument20 SeitenDigestive SystemCyrie sheene bilocuraNoch keine Bewertungen
- Test Bank For Fundamentals of Sectional Anatomy 2nd Edition by LazoDokument22 SeitenTest Bank For Fundamentals of Sectional Anatomy 2nd Edition by Lazojuliehayespdsgyfbjom100% (18)
- DLL q4 w1Dokument13 SeitenDLL q4 w1Mayolita NavalloNoch keine Bewertungen
- Vigorous Males Ensure Fertile FL OcksDokument3 SeitenVigorous Males Ensure Fertile FL OcksmahmudNoch keine Bewertungen
- Function of The Small IntestineDokument4 SeitenFunction of The Small Intestine139315Noch keine Bewertungen
- Blood Vessels and PressureDokument2 SeitenBlood Vessels and PressureAIMEE MARGARET FLORESNoch keine Bewertungen
- Nutrition in AnimalsDokument11 SeitenNutrition in Animalsvicky virratNoch keine Bewertungen