Beruflich Dokumente
Kultur Dokumente
Final Burst Abdomen in Pregnancy
Hochgeladen von
saryindrianyCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Final Burst Abdomen in Pregnancy
Hochgeladen von
saryindrianyCopyright:
Verfügbare Formate
Case report
Burst abdomen in pregnancy: A proposed management algorithm
Amalachukwu M. Okpala1, Samuel A. Debrah2 and Mohammed Mouhajer3
Ghana Med J 2016; 50(2): 115-118 DOI: http://dx.doi.org/10.4314/gmj.v50i2.10
1
Department of Plastic Surgery, Leeds General Infirmary, Leeds, United Kingdom 2Department of Surgery,
School of Medical Sciences, University of Cape Coast, Cape Coast, Ghana 3Department of Obstetrics and
Gynaecology, Korle Bu Teaching Hospital, Accra, Ghana
Corresponding author: Amalachukwu M. Okpala
E-mail: drmaluski@yahoo.com
Conflict of interest: None declared
SUMMARY
Management of the burst abdomen is complex due to the co-morbidities associated with it. When coupled with intraabdominal sepsis and pregnancy, it becomes even more difficult due to the ethical issues that have to be considered
when managing both mother and child. Due to the paucity of literature on this subject, a management algorithm has
been proposed which aims at tackling this delicate issue. However, the major consideration in the management of
these cases is that decisions are to be made based on optimization of the condition of the mother.
Keywords: Burst abdomen, pregnancy, management, algorithm, intra-abdominal sepsis
INTRODUCTION
Acute abdomen in pregnancy, and thus management of
its complications, remains one of the most challenging
diagnostic and therapeutic dilemmas of today despite
advancements in medical technology.1 Wound dehiscence following intra - abdominal sepsis in pregnancy is
rare, and the management of such a complex case is a
conundrum to both the surgeon and the obstetrician.
Whether to close or not to close the abdomen, or when
and how to deliver the fetus depends on both maternal
and fetal factors which must be considered to have the
most optimal outcome.
Case report
Eighteen-year-old Miss CN was referred from a hospital
in the district to the Central Regional Hospital as a case
of intestinal obstruction post laparotomy for typhoid
perforation in pregnancy at 23 weeks gestation. Patient
had undergone surgery 3 days prior to referral, and intra
operative findings were faeculent peritoneal fluid, and a
single large ileal perforation 15 cm from the ileo-caecal
junction. A simple closure had been done. Three days
post operatively, abdominal distension was noticed,
associated with bilious vomiting, hence the referral from
the district hospital.
On initial assessment at the emergency unit, a young,
very ill looking female with marked pallor and a temperature of 38.o C was noted. She was tachypnoeic and
tachycardic, with a blood pressure of 100/64 mmHg.
115
Her abdomen was distended, with pus oozing out from a
sub-umbilical midline incision, which was held, together by non-absorbable sutures. Obstetric examination
(abdomino-pelvic ultrasound) revealed a viable fetus at
23 weeks gestation.
Laboratory investigations showed a haemoglobin level
of 6.6 g/dl and a white cell count of 14.6 x 10 9 /L. A
diagnosis of deep surgical site infection post laparotomy
with severe anaemia was made. Patient was admitted
and resuscitated with intravenous fluids, intravenous
antibiotics and blood transfusions. A wound swab was
taken for culture and sensitivity. Skin sutures were removed to facilitate drainage of pus, and patient was
managed on a high protein/calorie enteral diet. On the
tenth day of admission, the patient developed a burst
abdomen. A Bogota bag was provided for closure of the
abdomen due to the finding of a septic hostile abdomen
in an anaemic malnourished patient.
The surgical wound granulated over rapidly, and the
foetus was monitored regularly via abdominal ultrasound and daily foetal kick counts. Seven weeks after
admission (gestational age 31 weeks) and after a course
of steroids to promote foetal lung maturation, patient
went into preterm labour and delivered a live male infant via spontaneous vaginal delivery. The neonate was
taken to the neonatal intensive care unit for further monitoring.
www.ghanamedj.org Volume 50 Number 2 June 2016
Case report
Management algorithm for burst abdomen in pregnancy
Burst abdomen in pregnancy (post laparotomy; post incisional hernia etc)
-----------------------------------------------------------------------------------------------
<24 weeks
> 24 weeks
Intra-abdominal sepsis
Intra-abdominal sepsis
Yes ------------------------------------------- No
No ------------------------------------------------------ Yes
Foetus alive
Foetus alive
Yes --------------------------------------------------------- No
Foetus alive
Foetus alive
Yes --------------------------------No
SM
SM
NPWT/BB
C/S
TOP
CS/SVD with
1o mesh repair
NPWT/BB + EHR
Mesh repair
NPWT/BB
SVD/CS when possible
EHR
Yes ------- --------- No
NPWT/BB
Mesh repair
No -----------------
SM
C/S
NPWT/BB
EHR
--------------------Yes
SM
NPWT/BB
SVD/CS when possible
EHR
SVD Spontaneous Vaginal Delivery; NPWT Negative Pressure Wound Therapy; CS Caesarean Section;
TOP Termination of pregnancy
SM -Surgical management involves laparotomy and peritoneal lavage if required; BB Bogota bag;
EHR Elective hernia repair
Patient was discharged with a healthy neonate to be
reviewed on an outpatient basis. The wound subsequently healed with secondary intention, with future consideration of incisional hernia repair.
DISCUSSION
Typhoid fever is a distinctive acute systemic febrile
infection caused by several serotypes of the Gramnegative bacillus Salmonella (primarily Salmonella
choleraesuis serotypes typhi and paratyphi).2 A study
carried out in a hospital in Pakistan showed that nonpregnant women with typhoid fever were more likely to
develop complications as compared to the pregnant
women.2 The authors of that study also derived the hypothesis that disease complications in typhoid fever are
related to host immunity and less likely to occur with
the immunological changes associated with pregnancy.2
Having said this, when complications due to typhoid
perforation do occur, the lives of the mother and the
foetus are at stake.
116
TOP + 10 mesh repair
CS/SVD
Fetal losses, especially when typhoid perforation occurs
during the first and second trimester, are high .3 Maternal mortality rate is also high and this is probably due to
the physiological changes in pregnancy coupled with
the stress of typhoid infection and intra-abdominal sepsis.3
Surgery is the gold standard for the treatment of typhoid
perforation after adequate resuscitation, correction of
electrolyte imbalance and commencement of appropriate antibiotic therapy.2 Multiple local, regional, and systemic factors can contribute to post-laparotomy wound
dehiscence as occurred in our case.4 The patient had
wound infection with ongoing intra-abdominal sepsis
due the gross peritoneal contamination; bowel distension due to a combination of bowel edema, paralytic
ileus and a gravid uterus; and severe anaemia with malnutrition.
www.ghanamedj.org Volume 50 Number 2 June 2016
Case report
There are different modalities available for the management of wound dehiscence post laparotomy, which
range from primary repair with sutures/mesh reinforcement, to entero-atmospheric treatment.5 However, in the
presence of intra-abdominal sepsis and a gradually enlarging uterus, the management option with the best
outcome for both mother and foetus becomes more difficult to choose due to fewer viable options. An online
search for the management of similar cases revealed 3
cases of burst abdomen during pregnancy, 2 due to incisional hernias, and the third due to surgical site infection
post laparotomy.6,7,8 The first case had a burst abdomen
due to an incisional hernia at a gestational age of 28
weeks which was initially managed with a mesh hernia
repair and tension sutures. The baby was subsequently
delivered by Caesarean section at 34 weeks with a concurrent surgical repair of the hernia.6 The second case of
burst abdomen due to an incisional hernia occurred at
35 weeks gestation, and underwent a Caesarean section
with concurrent hernia repair without a mesh.7 These
cases had no overt on-going intra-abdominal sepsis,
hence the choice of management. The third case developed an intra-abdominal abscess with wound failure at a
gestational age of 27 weeks post small bowel resection,
and was managed on Negative Pressure Wound Therapy
(NPWT). The wound was healed in 4 weeks, and the
baby was delivered vaginally at 39 weeks.
The advantage of NPWT post wound dehiscence is well
documented in literature.4There is no evidence of randomized controlled trials involving use of NPWT in
gravid patients. This may be due to the rarity of such
cases. However, the two cases in which NPWT were
used in gravid patients reported excellent outcomes for
both mother and baby.8,10
Due to the paucity of literature on the management of
wound dehiscence due to intra-abdominal sepsis in
pregnant patients, the authors have suggested a management algorithm (Figure 1). It takes a broad look at
the management of the burst abdomen in pregnancy
according to the presence of intra-abdominal sepsis and
the gestational age of viability which is 24 weeks according to WHO guidelines.9 Those who present with
intra-abdominal sepsis usually undergo an elective incisional hernia repair after management of the pregnancy
and the sepsis.
2.
Important points to consider are:
1. The availability of neonatal intensive care units
for resuscitation and management of preterm
deliveries.
2. Management decisions must be made based on
the health of the mother, not of the foetus.
3. Gestational age of viability differs among different countries, depending on the quality of
their neonatal intensive care units. The suggested algorithm can be adapted to suit the selected gestational age of viability for whichever health care system it is implemented in.
117
CONCLUSION
Management of the acute abdomen, and the sequelae of
complications that may arise in pregnancy is a challenge
even for the best equipped facilities. There is a paucity
of literature on the management of wound dehiscence in
pregnancy with/without intra-abdominal sepsis. A management algorithm for such cases has been suggested.
Although no adverse effects have been reported in the
cases in which NPWT was used in the gravid patient,
randomized controlled trials and long term follow up
would be necessary to confirm its overall safety in
pregnancy and absence of long term effects on the foetus. Decisions on management of these cases must be
made based on the health of the mother.
REFERENCES
1.
3.
4.
5.
6.
7.
8.
Goran Augustin, Mate Majerovic. Non-obstetric
acute abdomen during pregnancy. Eur J Obstet Gynecol Reprod Biol 2007; 131: 4 12.
Sulaiman K, Sarwari AR; Culture-confirmed typhoid fever and pregnancy. Int J Infect Dis 2007;
11:337 341.
Naaya HU, Eni UE, Chama CM. Typhoid Perforation in Maiduguri, Nigeria. Ann Afr Med 2004;
3(2): 69 -72.
Heller L, Levin S, Butler C. Management of abdominal wound dehiscence using vacuum assisted
closure in patients with compromised healing. Am J
Surg 2006; 191(2): 165 172.
Lopez-Cano M, Pereira J, Armengol-Carrasco M.
Acute postoperative open abdominal wall: Nosological concept and treatment implications. World J
Gastrointest Surg 2013; 5(12):314 -320.
Kumar R, Sonika A, Kaberi B, Sunesh K, Charu C.
Gravid Uterus in an incisional hernia leading to
burst abdomen. The Internet Journal of Gynecology
and Obstetrics 2004; 5 (1).
Dubey C, Gupta N, Gupta C, Arora R, Sachdeva P.
Successful pregnancy outcome in a case of gravid
uterus in an incisional hernia leading to burst abdomen. The Internet Journal of Gynecology and
Obstetrics 2009; 13 (1).
Shapiro S, Mumme D. Use of Negative Pressure
Wound Therapy in the Management of Wound De-
www.ghanamedj.org Volume 50 Number 2 June 2016
Case report
9.
118
hiscence in a Pregnant Patient. Wounds 2008; 20
(2):46 48.
Ikechebelu JI, Eleje GU, Ugochukwu EF, Edokwe
ES. Should we re-define age of Fetal Viability in
Nigeria? A Case Report of Newborn Survival from
pre-viable pre-labor rupture of membranes. J Womens Health Issues Care 2014; 3:3.
10. Asukai K, Kashiwazaki M, Koizumi K, Nobunaga
T, Yano H. A case report of a 19-week gravid patient with a dehisced abdominal wound and treated
with V.A.C. ATS Therapy System. Int Wound J
2014; doi:10.1111/iwj.12352
www.ghanamedj.org Volume 50 Number 2 June 2016
Das könnte Ihnen auch gefallen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5795)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1091)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- FCS (SA) Intermediate Paper 2 Blueprints 20-10-2019Dokument7 SeitenFCS (SA) Intermediate Paper 2 Blueprints 20-10-2019Kishan NaiduNoch keine Bewertungen
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- Types of Hernia and Its ManagementDokument80 SeitenTypes of Hernia and Its ManagementVisaagan Kalaithasan50% (2)
- 3881825Dokument30 Seiten3881825saryindrianyNoch keine Bewertungen
- Male Genitalia AbnormalitiesDokument25 SeitenMale Genitalia AbnormalitiesClaudette Kyle CornelioNoch keine Bewertungen
- Nakshatra & DiseaseDokument4 SeitenNakshatra & DiseaseMauricio Avila100% (1)
- EMQs and MCQs For Medical Finals (PDFDrive)Dokument337 SeitenEMQs and MCQs For Medical Finals (PDFDrive)Samuel TanNoch keine Bewertungen
- Hernia Repair Sequelae (2010) (UnitedVRG) PDFDokument544 SeitenHernia Repair Sequelae (2010) (UnitedVRG) PDFPhilip Manalu100% (1)
- Acute Fatty Liver of Pregnancy: Letter To EditorDokument2 SeitenAcute Fatty Liver of Pregnancy: Letter To EditorsaryindrianyNoch keine Bewertungen
- Acute Fatty Liver of Pregnancy: Better Understanding of Pathogenesis and Earlier Clinical Recognition Results in Improved Maternal OutcomesDokument8 SeitenAcute Fatty Liver of Pregnancy: Better Understanding of Pathogenesis and Earlier Clinical Recognition Results in Improved Maternal OutcomessaryindrianyNoch keine Bewertungen
- Nelson2013 Ajog PDFDokument7 SeitenNelson2013 Ajog PDFsaryindrianyNoch keine Bewertungen
- Pregnancy-Related Liver Disorders: Seminar Journal of Clinical and Experimental HepatologyDokument12 SeitenPregnancy-Related Liver Disorders: Seminar Journal of Clinical and Experimental HepatologysaryindrianyNoch keine Bewertungen
- ACG Clinical Guideline: Liver Disease and Pregnancy: Practice GuidelinesDokument19 SeitenACG Clinical Guideline: Liver Disease and Pregnancy: Practice GuidelinessaryindrianyNoch keine Bewertungen
- Causes and Management of Surgical Wound Dehiscence: Department of General SurgeryDokument10 SeitenCauses and Management of Surgical Wound Dehiscence: Department of General SurgerysaryindrianyNoch keine Bewertungen
- Birth After Previous Caesarean Section (C Obs 38) Re Write July 2015 1Dokument27 SeitenBirth After Previous Caesarean Section (C Obs 38) Re Write July 2015 1saryindrianyNoch keine Bewertungen
- 1 s2.0 S0889854515001163Dokument18 Seiten1 s2.0 S0889854515001163saryindrianyNoch keine Bewertungen
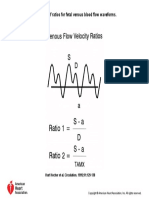
- Calculation of Ratios For Fetal Venous Blood Flow WaveformsDokument1 SeiteCalculation of Ratios For Fetal Venous Blood Flow WaveformssaryindrianyNoch keine Bewertungen
- Technical Series 2 Using PartographDokument5 SeitenTechnical Series 2 Using PartographsaryindrianyNoch keine Bewertungen
- Rupture of Membranes Guideline For The Management of Preterm PrelabourDokument10 SeitenRupture of Membranes Guideline For The Management of Preterm PrelaboursaryindrianyNoch keine Bewertungen
- Post Caesarean Surgical Site Infections 2Dokument6 SeitenPost Caesarean Surgical Site Infections 2saryindrianyNoch keine Bewertungen
- Risk Factors For Wound Dehiscence After Laparotomy - Clinical Control TrialDokument9 SeitenRisk Factors For Wound Dehiscence After Laparotomy - Clinical Control TrialsaryindrianyNoch keine Bewertungen
- Common Surgical ProceduresDokument4 SeitenCommon Surgical ProceduresKim Glaidyl BontuyanNoch keine Bewertungen
- Questions and Answers About HerniasDokument2 SeitenQuestions and Answers About HerniasmysarasjNoch keine Bewertungen
- 2 Hiatal Hernia ManuscriptDokument4 Seiten2 Hiatal Hernia Manuscriptkint manlangitNoch keine Bewertungen
- Hernias Case PresentationDokument46 SeitenHernias Case Presentationraxym17Noch keine Bewertungen
- Mcqs Mock Exams For General Surgery Board ExamDokument5 SeitenMcqs Mock Exams For General Surgery Board ExamMoiz AhmedNoch keine Bewertungen
- Hernia Inguinal 1, Anatomia, SCNA 2018Dokument15 SeitenHernia Inguinal 1, Anatomia, SCNA 2018Angie Cristina Hoyos EcheverriNoch keine Bewertungen
- Examination of AbdomenDokument67 SeitenExamination of Abdomenvikram kumarNoch keine Bewertungen
- Gastro-Intestinal System Diagnostic TestsDokument11 SeitenGastro-Intestinal System Diagnostic TestsFev BanataoNoch keine Bewertungen
- 06 Inguinal Hernia SrsDokument10 Seiten06 Inguinal Hernia SrslowhillNoch keine Bewertungen
- Is It Psychological, Physical, or Both?: Sue M. Mcdonnell, PHD, CaabDokument8 SeitenIs It Psychological, Physical, or Both?: Sue M. Mcdonnell, PHD, CaabSarai Snchz PrietoNoch keine Bewertungen
- USAT MONTSERRAT COLLEGE OF MEDICINE Surgery General ProgrammeDokument37 SeitenUSAT MONTSERRAT COLLEGE OF MEDICINE Surgery General ProgrammeUSATPGANoch keine Bewertungen
- Abrahamson 1989Dokument1 SeiteAbrahamson 1989CRISTIAN MEDRANONoch keine Bewertungen
- Cases Elog BookDokument13 SeitenCases Elog BookFaryal UfaqNoch keine Bewertungen
- Abnormalities of The Penis: PhimosisDokument4 SeitenAbnormalities of The Penis: PhimosisShun Reigh SumilangNoch keine Bewertungen
- Examination of Gastrointestinal SystemDokument37 SeitenExamination of Gastrointestinal SystemayushiNoch keine Bewertungen
- Examination of A StomaDokument3 SeitenExamination of A StomaChloe100% (1)
- Teaching Files: Detailed Newborn ExaminationDokument51 SeitenTeaching Files: Detailed Newborn ExaminationcorinadumitruNoch keine Bewertungen
- Hiatus Hernia - Chinese Herbs, Chinese Medicine, AcupunctureDokument6 SeitenHiatus Hernia - Chinese Herbs, Chinese Medicine, AcupunctureCarlCordNoch keine Bewertungen
- Hiatus Hernia CheckedDokument34 SeitenHiatus Hernia CheckedPiyali SahaNoch keine Bewertungen
- Hernia+scrotal MassDokument82 SeitenHernia+scrotal MassJJ JirapathNoch keine Bewertungen
- Hernia Surgical Mesh Implants: What Is A Hernia?Dokument3 SeitenHernia Surgical Mesh Implants: What Is A Hernia?Vishnu KumarNoch keine Bewertungen
- Meta-Analysis of Closure of The Fascial Defect During Laparoscopic Incisional and Ventral Hernia RepairDokument10 SeitenMeta-Analysis of Closure of The Fascial Defect During Laparoscopic Incisional and Ventral Hernia RepairUday PrabhuNoch keine Bewertungen
- Modul Digestive Blok 9Dokument25 SeitenModul Digestive Blok 9prabuNoch keine Bewertungen
- Case Report Relaparotomy Two Years After Incisional Hernia Repair Using A Free Fascia Lata GraftDokument4 SeitenCase Report Relaparotomy Two Years After Incisional Hernia Repair Using A Free Fascia Lata GraftDeddy WidjajaNoch keine Bewertungen