Beruflich Dokumente
Kultur Dokumente
Hypertensive Crisis
Hochgeladen von
Abdul Hannan AliCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Hypertensive Crisis
Hochgeladen von
Abdul Hannan AliCopyright:
Verfügbare Formate
CME
EARN CATEGORY I CME CREDIT by reading this article and the article beginning on page 20 and successfully
completing the posttest on page 50. Successful completion is dened as a cumulative score of at least 70%
correct. This material has been reviewed and is approved for 1 hour of clinical Category I (Preapproved) CME
credit by the AAPA. The term of approval is for 1 year from the publication date of August 2010.
LEARNING OBJECTIVES
Understand the distinction between hypertensive emergency and urgency
Describe the pathogenesis of hypertensive crisis and hypertensive encephalopathy
Discuss the clinical manifestations and initial evaluation of a patient in a hypertensive crisis
Identify the conditions associated with hypertensive emergency and urgency
Emergency or urgency? Effective
management of hypertensive crises
PAs need to identify the patients condition in order to select the most appropriate
intervention while avoiding overaggressive treatment of the nonemergent patient.
Kishore Kuppasani, MS, MPA, PA-C;
Alluru S. Reddi, MD, PhD
ypertensive crisis is a significant increase in
BP, usually to levels higher than 180/110
mm Hg. Hypertensive crises are classified
as emergency or urgency. Depending on the
type of crisis, BP should be reduced gradually or must be reduced immediately to prevent target organ
damage. Recognition of the type of manifest hypertensive
crisis is paramount to successful management and treatment
of the at-risk patient.
stress, thus limiting further dissection of the aorta. On the
other hand, a previously nonadherent hypertensive patient
who presents to the ED for a reason other than hypertension
but has a BP of 220/130 mm Hg and is otherwise asymptomatic does not require immediate BP reduction. The distinction between emergency and urgency should always be made
in the ED to prevent overaggressive treatment (Table 1).
PREVALENCE AND INCIDENCE
An estimated 1% of all hypertensive patients will experience
a hypertensive crisis during their lifetimes.1 However, the per-
of BPusually 220/130 mm Hg or higherwith acute and
ongoing target organ damage to the kidneys, heart, vascular system, brain, or eyes. Hypertensive emergency requires
the initiation of BP reduction within minutes to hours to
prevent further progression of target organ damage. BP
should not be lowered to less than 140/90 mm Hg, except
in patients with aortic dissection or eclampsia.
Hypertensive urgency is defined as an elevation of
BPusually 180/110 mm Hg or higherwithout target
organ damage. BP should be lowered gradually over
12 to 24 hours, but not to a normal level (target level,
approximately 160/110 mm Hg).
The clinical status of the patient, not the degree of BP elevation, defines an emergency in certain cases. For example,
in a patient with acute aortic dissection who presents to the
emergency department (ED) with a BP of 160/110 mm Hg,
the systolic BP (SBP) must be lowered to less than 120 mm
Hg within 20 minutes. The rapid reduction reduces shear
44 JAAPA AUGUST 2010 23(8) www.jaapa.com
ISM / Phototake
TYPES OF HYPERTENSIVE CRISES
Hypertensive emergency is defined as a severe elevation
A fundus view of hypertensive retinopathy in the right eye shows
hemorrhages and exudates caused by hypertension.
centage of patients who present to an ED with hypertensive
crisis is not known. A 1-year study reported that hypertensive crises accounted for 27.5% of all ED visits for medical
urgenciesemergencies;2 of those, 20.8% were for hypertensive urgencies and 6.4% were hypertensive emergencies. The
prevalence of hypertensive crisis in this study was 3%.
Little is known about what factors can precipitate a hypertensive crisis. However, a previous diagnosis of hypertension,
nonadherence to antihypertensive medication regimens, and
elevated BP that is not adequately controlled were found to
increase a patients risk for hypertensive crisis.3
PATHOPHYSIOLOGY
The pathophysiology of hypertensive crisis is poorly understood. A sudden increase in BP seems to further accentuate
shear stress in the vessel wall, which leads to additional endothelial damage, further activation of the neurohormonal
(renin-angiotensin II-aldosterone, sympathetic nervous system,
and vasopressin) system, induction of oxidative stress, and
inflammatory cytokines. The coagulation cascade is also activated by the resultant platelet aggregation and fibrin deposition. These changes lead to vasoconstriction, thrombosis, and
fibrinoid necrosis and result in hypoperfusion and ischemia.3-8
Cerebral edema and hypertensive encephalopathy
may result from impaired autoregulation of the brain. A
sudden increase in BP causes forced vasodilation of the
cerebral vessel to accommodate hyperperfusion. This
vasodilation is initially segmental, giving the appearance
of a sausage-string pattern on magnetic resonance angiography or conventional angiography, but soon becomes
diffuse. The endothelium becomes more dysfunctional
than before, allowing plasma components to diffuse into
the surrounding interstitium, leading to cerebral edema
and, finally, hypertensive encephalopathy.
Hypertensive patients in an emergency state present with
target organ damage, and patients in an urgency state do
not have target organ damage. Table 2 lists conditions associated with hypertensive emergency and urgency. The
frequency of target organ damage is not uniform. Target
organ damage reported in one study included cerebral infarction (24.5%), intracerebral or subarachnoid hemorrhage
(4.5%), hypertensive encephalopathy (16.3%), acute pulmonary edema (22.5%), acute heart failure (14.3%), acute
MI or unstable angina (12%), aortic dissection (4.5%), and
eclampsia (2%).2
SYMPTOMS AND EVALUATION
In a hypertensive emergency, the patient presents with
severe headache, nausea, vomiting, chest pain, dyspnea,
neurologic deficit, and vertigo.2 In a hypertensive urgency,
the patient may present with severe headache, dyspnea,
epistaxis, or severe anxiety. These symptoms may overlap
in patients in both types of crisis.
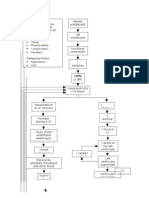
Early triage is an important part of the initial evaluation and establishes the appropriate therapeutic strategies
to improve morbidity and mortality (Figure 1). Patient
TABLE 1. Characteristics of hypertensive emergency
and urgency
Hypertensive
emergency
Hypertensive
urgency
Signs and symptomsa
More
frequent
Less frequent
or minimal
Acute severe increase in BP
Yes
Yes
Acute target organ damage
Yes
No
Acute BP reduction needed
Yes
No
IV medications needed
Yes
No
Hospitalization
Admit to
ICU and
monitor BP
Discharge from
ED with followup in 2-4 d
Characteristic
Key: ED, emergency department.
a
Signs and symptoms seen in a hypertensive emergency include severe headache,
nausea, vomiting, chest pain, dyspnea, neurologic decit, and vertigo. Signs and
symptoms seen in a hypertensive urgency include severe headache, dyspnea,
epistaxis, or severe anxiety. These may overlap in patients in both types of crisis.
TABLE 2. Conditions associated with hypertensive crisis
Hypertensive emergency
(symptomatic and with target organ damage)
Acute aortic dissection
Acute left ventricular failure with pulmonary edema
Acute MI
Acute renal failure
Adrenergic crisis (pheochromocytoma crisis, cocaine ingestion,
clonidine or beta-blocker withdrawal, amphetamine overdose)
Eclampsia
Hypertensive encephalopathy
Ischemic and hemorrhagic stroke
Hypertensive urgency
(asymptomatic and without target organ damage)
Epistaxis
Postoperative hypertension
Renovascular hypertension
Scleroderma crisis
Severe hypertension
Severe hypertension associated with burns or organ transplantation
Severe hypertension with coronary artery disease
www.jaapa.com AUGUST 2010 23(8) JAAPA
45
CME Hypertensive crisis
HYPERTENSIVE CRISIS
BP >220/130 mm Hg
Symptomatic
Acute target organ
damage
BP ~180/110 mm Hg
Asymptomatic
No target organ
damage
urinalysis. Laboratory studies for serum renin, aldosterone,
catecholamines, or urine metanephrines should be ordered if
secondary hypertension is suspected. Urine toxicology may be
indicated in select cases. An ECG may suggest ischemia and/
or left ventricular hypertrophy. Chest radiography is needed
to evaluate heart size and lungs. A widened mediastinum on
chest radiography is suggestive of aortic dissection and can be
confirmed with CT or MRI. Both CT and MRI are helpful
in the evaluation of cerebral or abdominal pathology. Table:
Hypertensive crisis evaluation and differential diagnosis (in
the online version of this article) lists the possible diagnoses
indicated by the initial findings.
TREATMENT
Hypertensive
emergency
Hypertensive
urgency
IV medications
Monitor patient in
ICU
Oral medications
Follow-up in 2-4 d
FIGURE 1. Triage of patients in hypertensive crisis
history should focus on signs and symptoms, such as
headache, dyspnea, seizures, nausea, vomiting, epistaxis,
mental status, previous history of hypertension, and
medications. Physical examination should include brief
fundoscopic, cardiac, lung, and neurologic examinations.
Establishing the patients volume status is essential because heart failure and acute glomerulonephritis may
manifest with volume overload. Pheochromocytoma and,
at times, renovascular hypertension may manifest with
volume depletion.
Eye examination may reveal papilledema or other grades of
retinopathy. Laboratory studies include a CBC with peripheral smear, serum electrolytes, creatinine, BUN, glucose, and
Management of a specific hypertensive crisis depends on
the signs and symptoms as well as the target organ damage.
Drug therapy should be individualized (Table 3).
Hypertensive emergency The patient should be admitted to the ICU for continuous BP monitoring. Once a
hypertensive emergency is identified, IV administration
of an appropriate drug should be started in the ED. The
initial goal is to lower BP by 25% of the mean arterial
BP within minutes to 1 hour and stabilize BP to approximately 160/100 to 110 mm Hg over the next 2 to 6 hours.9
Rapid BP reduction below this level may precipitate renal,
coronary, or cerebral ischemia. If the patient is stable and
tolerates a BP of 160/100 to 110 mm Hg, further reduction to near normal can be attempted over 24 to 48 hours.
However, normal BP levels should not be achieved in
the patient with ischemic stroke. SBP should be lowered
to less than 120 mm Hg in the patient with aortic dissection.9 Table 4 describes the signs and symptoms, preferred
agent(s), and agents to be avoided when treating a patient
in a hypertensive emergency. Suggested target BP levels
are also listed.
Hypertensive urgency Patients will not have sustained
target organ damage; therefore, their BP can be followed
and treated with short-acting oral agents after eliminating
any triggering factors, such as pain. If the patient does not
have any triggering factors and severe hypertension persists, the patient is considered to have chronic hypertension.
Parenteral drugs are not needed, nor is a rapid reduction
of BP, as there is no evidence to suggest that these patients
KEY POINTS
Depending on the type of crisis (emergency or urgency), BP should be reduced gradually or must be reduced immediately to prevent
target organ damage. Recognition of the type of manifest hypertensive crisis is paramount to successful management and treatment
of the at-risk patient.
Hypertensive emergency is dened as a severe elevation of BPusually 220/130 mm Hg or higherwith acute and ongoing target
organ damage to the kidneys, heart, vascular system, brain, or eyes. Hypertensive urgency is dened as an elevation of BPusually
180/110 mm Hg or higherwithout target organ damage.
The most important task for the ED clinician is to identify whether the patients condition is a hypertensive emergency or urgency.
The goal is to avoid overaggressive treatment of the nonemergent patient while initiating the most appropriate treatment.
46 JAAPA AUGUST 2010 23(8) www.jaapa.com
TABLE 3. Commonly used drugs in hypertensive crises3-9,13
Drug
Dosage
Onset
Duration
Adverse effects
PARENTERAL DRUGS USED IN HYPERTENSIVE EMERGENCIES
ADRENERGIC INHIBITORS
Esmolol (Brevibloc, generics)
250-500 mcg/kg/min,
then 50-100 mcg/kg/min;
may repeat bolus after
5 min or increase to 300
mcg/kg/min
1-2 min
10-30 min
Asthma First-degree heart block
Heart failure Hypotension
Nausea
Labetalol (generics)
20-80 mg bolus q10min
5-10 min
2-6 h
Bronchospasm Heart block
Nausea Scalp tingling Vomiting
Phentolamine (Oraverse, Regitine)
5-10 mg/min
1-2 min
10-30 min
Flushing Headache Tachycardia
20-40 mg in 5 min
5-15 min
2-3 h
Hypokalemia Volume depletion
Enalaprilat (generics)
1.25-5 mg q6h
15-30 min
4-6 h
Angioedema Hypotension
Renal failure
Fenoldopam (Corlopam, generics)
0.1-0.3 mcg/kg/min
5-10 min
30 min
Headache Nausea Tachycardia
Hydralazine (generics)
10-20 mg bolus
10-20 min
1-4 h
Flushing Headache Tachycardia
Vomiting
Nicardipine (Cardene, generics)
5-15 mg/h
5-10 min
2-4 h
Headache Flushing
Reex tachycardia
Nitroglycerin (generics)
5-100 mcg/min
1-3 min
5-10 min
Headache Hypotension Vomiting
Sodium nitroprusside (Nitropress)
0.25-10 mcg/kg/min
Immediate
1-2 min
Cyanate toxicity Hypotension
Nausea Vomiting
DIURETICS
Furosemide (generics), used with
other agents
VASODILATORS
ORAL DRUGS FOR HYPERTENSIVE URGENCIES
Amlodipine (Norvasc, generics)
5-10 mg
30-50 min
18-24 h
Headache Flushing
Peripheral edema Tachycardia
Captopril (Capoten, generics)
12.5-25 mg
15-60 min
4-6 h
Cough
Renal failure with bilateral renal
artery stenosis
Clonidine (Catapres, Jenloga,
generics)
0.2 mg
30-120 min
8-12 h
Dry mouth Hypotension
Sedation
Furosemide (Lasix, generics)
20-40 mg
30-60 min
4-5 h
Hypokalemia Volume depletion
Labetalol (Trandate, generics)
200-400 mg
20-120 min
8-12 h
Bronchospasm
Decreased myocardial contractility
Heart block
Nicardipine (Cardene, generics)
20-30 mg
30-120 min
6-8 h
Headache Tachycardia
www.jaapa.com AUGUST 2010 23(8) JAAPA
47
CME Hypertensive crisis
TABLE 4. Preferred IV therapy in hypertensive emergency
Emergency
Signs and symptoms
Drug(s) of choice
Drug(s) to be avoided
Target BP
Acute MI
Chest pain Dyspnea
Esmolol Labetalol
Nitroglycerine
Hydralazine (may
increase heart rate and
O2 consumption)
Gradual reduction
to 5%-10% of MAP
Acute renal failure
and hematuria
No specic signs or
symptoms unless
uremia or HF is present
Fenoldopam
Nicardipine
Nitroprusside (rapid
BP reduction causes
further alteration in
autoregulation)
Gradual reduction to 10%
of MAP over several hours
Aortic dissection
Chest pain
(intrascapular region)
Headache Syncope
Esmolol
Labetalol plus
nitroprusside
Hydralazine (may
increase mechanical
stress)
SBP <120 mm Hg within
20 min
Cocaine withdrawal
Agitation AMS
Phentolamine
Propranolol (complete
beta blockade and
increases BP)
10%-15% reduction
of MAP
Eclampsia
Headache Seizures
Hydralazine Labetalol
MgSO4 Nicardipine
Nifedipinea
ACE inhibitors (fetal
abnormalities)
Nitroprusside (cyanate
toxicity)
DBP <90 mm Hg gradually
(<1 h)
Hypertensive
encephalopathy
Headache AMS
Papilledema
(common but not
always present)
Fenoldopam Labetalol
Nicardipine
Clonidine (sedation)
Nitroglycerine
Nitroprusside
(increases ICP)
25% reduction of MAP
over 2-3 h
Intracerebral
hemorrhage
AMS
Headache
Neurologic (focal)
decit
SBP >200 mm Hg or
MAP >150 mm Hg:
Esmolol
Labetalol
Nicardipine
Hydralazine
(increases ICP)
Nitroglycerine
Nitroprusside
High ICP: Maintain MAP
<130 mm Hg or SBP <180
mm Hg for the rst 24 h
Normal ICP: Maintain MAP
<110 mm Hg or SBP <160
mm Hg for rst 24 h
Ischemic stroke
AMS
Headache
Neurologic (focal)
decit
BP >180/120 mm Hg or
MAP >140 mm Hg:
Labetalol
Nicardipine
Clonidine (sedation)
15% reduction of MAP
BP <140/90 mm Hg
should be avoided
Maintain a BP of
<180/105 mm Hg for
24 h after thrombolysis
Left ventricular
failure and
pulmonary edema
Chest pain
Dyspnea
ACE inhibitors
Furosemide
Nitroglycerine
Nitroprusside
Hydralazine
Labetalol (may
worsen HF)
10%-15% reduction of MAP
Pheochromocytoma
Headache
Sweating
Labetalol
Phentolamine
Diuretics (volume
depletion)
Nitroprusside
(hypotension)
Gradual reduction until
symptoms improve
Subarachnoid
hemorrhage
AMS
Headache
Neurologic
(focal decit)
MAP >130 mm Hg:
Esmolol
Labetalol
Nicardipine
Oral nimodipineb
Hydralazine
(increases ICP)
Nitroglycerine
Nitroprusside
Maintain SBP <160 mm Hg
(MAP >130 or <70 mm Hg
carries poor prognosis)
Key: AMS, altered mental status; DBP, diastolic BP; ICP, intracranial pressure; HF, heart failure; MAP, mean arterial pressure; MgSO4, magnesium sulfate; SBP, systolic BP.
a
Only long-acting nifedipine is used.
b
Oral nimodipine has a hypotensive effect but is not used to treat hypertension. It is used to prevent delayed ischemic neurologic decit.
48 JAAPA AUGUST 2010 23(8) www.jaapa.com
experience immediate (from hours to a few days) target
organ damage if left untreated. BP will fall by 6% within 1
hour even before antihypertensive drugs are started.8 Thus,
parenteral use of antihypertensive agents should be avoided
in the uncomplicated patient with severe hypertension.
Some clinicians hesitate to treat hypertensive urgency
in the ED. Oral agents should be considered if the patients BP is higher than 180/110 mm Hg and are indicated when the patients BP is higher than 220/120 mm
Hg.10,11 BP should be reduced to approximately 160/110
mm Hg over a period of 12 to 24 hours after triggering
factors are corrected to avoid myocardial, cerebral, and
renal ischemia.
Follow-up within 2 to 4 days after the ED visit is extremely
important. Patients should be instructed to schedule a followup appointment with a primary care physician or an outpatient clinic as soon as possible.
Prognosis Patient prognosis after a hypertensive crisis is
poor. A 30-year follow-up of 315 patients with hypertensive
emergency showed a 5-year survival of 74%.12 The most
common causes of death were renal failure (40%), stroke
(24%), MI (11%), and heart failure (10%).
CONCLUSION
The most important task for the ED clinician is to identify whether the patients condition is a hypertensive
emergency or urgency. The goal is to avoid overaggressive treatment of the nonemergent patient while initiating
the most appropriate treatment. Effective management
of hypertensive crises improves both morbidity and
mortality. JAAPA
ONLINE EXTRAS AT
www.jaapa.com
Table: Hypertensive crisis evaluation and
differential diagnosis
Kishore Kuppasani is a hospitalist PA at the University Hospital, UMDNJ,
Newark, New Jersey. Alluru Reddi is professor of medicine, Department of
Medicine, Division of Nephrology and Hypertension, UMDNJ-New Jersey
Medical School, Newark. The authors have indicated no relationships to
disclose relating to the content of this article.
REFERENCES
1. Kinkaid-Smith P, McMichael J, Murphy EA. The clinical course and pathology of hypertension
with papilloedema (malignant hypertension). Quart J Med. 1958;27(105):117-153.
2. Zampaglione B, Pascale C, Marchisio M, Cavallo-Perin P. Hypertensive urgencies and emergencies: prevalence and clinical presentation. Hypertension. 1996;27(1):144-147.
3. Patel HP, Mitsnefes M. Advances in the pathogenesis and management of hypertensive crisis.
Curr Opin Pediatr. 2005;17(2):210-214.
4. Kitiyakara C, Guzman NJ. Malignant hypertension and hypertensive emergencies. J Am Soc
Nephrol. 1998;9(1):133-142.
5. Vaughan CJ, Delanty N. Hypertensive emergencies. Lancet. 2000;356(9227):411-417.
6. Aggarwal M, Khan IA. Hypertensive crisis: hypertensive emergencies and urgencies. Cardiol
Clin. 2006;24(1):135-146.
7. Marik PE, Varon J. Hypertensive crises: challenges and management. Chest. 2007;131(6):1949-1962.
8. Nolan CR, Linas SL. Malignant hypertension and other hypertensive crises. In: Schrier RW, ed.
Diseases of the Kidney & Urinary Tract. 8th ed. Philadelphia, PA: Wolters Kluwer/Lippincott,
Williams & Wilkins; 2007:1370-1436.
9. Chobanian AV, Bakris GL, Black HR, Cushman WC, et al. Seventh report of the Joint National
Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension. 2003;42(6):1206-1252.
10. Shayne P. Against routine initiation of antihypertensive therapy in the emergency department.
Ann Emerg Med. 2009;54(6):792-793.
11. Slovis CM, Reddi AS. Increased blood pressure without evidence of acute end organ damage.
Ann Emerg Med. 2008;51(3S):S7-S9.
12. Lip GY, Beevers M, Beevers DG. Complications and survival of 315 patients with malignant-phase
hypertension. J Hypertens. 1995;13(8):915-924.
13. Rosei EA, Salvetti M, Farsang C. European Society of Hypertension Scientic Newsletter: treatment of hypertensive urgencies and emergencies. J Hypertens. 2006;24(12):2482-2485.
www.jaapa.com AUGUST 2010 23(8) JAAPA
49
TABLE. Hypertensive crisis evaluation and differential diagnosis
Assessment and/or ndings
Differential diagnosis
HISTORY
Chest pain radiates to left arm and back
Acute MI Aortic dissection
Dyspnea, pulmonary edema
Left ventricular failure
Headache, nausea, vomiting, altered mental status, seizures,
focal neurologic decit
Stroke
Hematuria, red blood cell casts
Acute glomerulonephritis Vasculitis
Illicit drug use
Cocaine ingestion
Nonadherence to previous antihypertensive therapy
Clonidine or beta-blocker withdrawal
IMAGING STUDIES
Chest CT (false or double lumen of aorta)
Aortic dissection
Chest MRI (intramural hematoma appearing as crescentic
thickening around aortic wall)
Aortic dissection
Chest radiography
Rib notching caused by dilated intercostal arteries
Widening of mediastinum
Aortic dissection
Coarctation of aorta
ECG
Deep T-wave inversions in the absence of MI
Q waves, ST-T abnormalities
Subarachnoid hemorrhage
Acute MI
Head CT or MRI (ischemia or hemorrhage)
Stroke
Transesophageal echocardiography (intimal ap, double lumen)
Aortic dissection
LABORATORY STUDIES
CBC (anemia) and schistocytes on peripheral blood smear
Microangiopathic hemolytic anemia
Serum potassium (low) and serum bicarbonate (high)
Metabolic alkalosis associated with renovascular hypertension
Primary aldosteronism
Serum creatinine and BUN (elevated)
Renal failure
Serum glucose
Elevated
Low
Diabetes mellitus Pheochromocytoma
Precipitates hypertensive encephalopathy
Serum renin (low) and serum aldosterone (high)
Primary aldosteronism
Plasma catecholamines and urine metanephrine (elevated)
Pheochromocytoma
Urinalysis (red blood cells, red blood casts)
Acute glomerulonephritis Vasculitis
Urine toxicology
Cocaine ingestion
Pregnancy test (positive)
<20 weeks
>20 weeks with seizures
>20 weeks without seizures
Acute or chronic hypertension
Preeclampsia
Eclampsia
PHYSICAL EXAMINATION
Systolic BP
High in arms and low in legs
Difference >20 mm Hg in arms, pulse decit, weak pulses
Coarctation of aorta
Aortic dissection
Orthostatic BP and pulse changes
Pheochromocytoma Volume depletion
Eyes
Grade 2 retinopathy (arteriovenous nicking, narrowing)
Grades 3 (hemorrhages, exudates) and 4 (papilledema) retinopathy
Chronic hypertension
Target organ damage (previously called malignant hypertension)
Neck (jugular vein distension)
Left ventricular failure
Heart (S3 sound)
Left ventricular failure
Lungs (crackles, congestion)
Left ventricular failure
Abdomen
Bruits
Gravid uterus
Aneurysms Renal artery stenosis
Preeclampsia-eclampsia
Peripheral edema
Left ventricular failure
Neurologic decit with seizures
Eclampsia Hypertensive encephalopathy Stroke
Das könnte Ihnen auch gefallen
- Hypertensive CrisisDokument13 SeitenHypertensive Crisis.Katherine CalderonNoch keine Bewertungen
- Hypertensive EmergencyDokument4 SeitenHypertensive EmergencyRara MuuztmuuztmuccuNoch keine Bewertungen
- Hypertensive CrisesDokument42 SeitenHypertensive Crisescabinetuldeigiena0% (2)
- Hypertensive CrisisDokument7 SeitenHypertensive Crisisalul847474Noch keine Bewertungen
- Cardiomyopathy Dilated CardiomyopathyDokument5 SeitenCardiomyopathy Dilated Cardiomyopathym3d1k100% (1)
- Stroke: Hypertensive UrgencyDokument4 SeitenStroke: Hypertensive UrgencyMaricar TaboraNoch keine Bewertungen
- Upper Gastrointestinal Bleeding: Anthony Alexander University of The West Indies at MonaDokument40 SeitenUpper Gastrointestinal Bleeding: Anthony Alexander University of The West Indies at MonaAy Alex0% (1)
- Hypertensive CrisisDokument30 SeitenHypertensive CrisisAfraDewitaNoch keine Bewertungen
- Stevens Johnson Syndrome CASEDokument53 SeitenStevens Johnson Syndrome CASEKathrina CraveNoch keine Bewertungen
- CHF Case Study (Dokument35 SeitenCHF Case Study (EzraManzanoNoch keine Bewertungen
- HypothyroidismDokument59 SeitenHypothyroidismAmir Mahmoud100% (1)
- HCVDDokument5 SeitenHCVDkhrizaleehNoch keine Bewertungen
- Hypertensive Cardiovascular Disease Also Known As Hypertensive Heart Disease Occurs Due To The Complication of Hypertension or High Blood PressureDokument3 SeitenHypertensive Cardiovascular Disease Also Known As Hypertensive Heart Disease Occurs Due To The Complication of Hypertension or High Blood Pressurejoanneceline16Noch keine Bewertungen
- Ineffective Cerebral Tissue Perfusion Related ToDokument7 SeitenIneffective Cerebral Tissue Perfusion Related TohannahNoch keine Bewertungen
- Nephrolithiasis - Drug StudyDokument5 SeitenNephrolithiasis - Drug StudyAia JavierNoch keine Bewertungen
- TAHBSO ReportDokument4 SeitenTAHBSO ReportsachiiMeNoch keine Bewertungen
- Cor Pulmonale: Dr. Gerrard UyDokument13 SeitenCor Pulmonale: Dr. Gerrard Uyfaridah azzah sariNoch keine Bewertungen
- CHF PathophysiologyDokument12 SeitenCHF PathophysiologyprofgambhirNoch keine Bewertungen
- Clinical Manifestations and Treatment of HypokalemiaDokument16 SeitenClinical Manifestations and Treatment of Hypokalemiagerontogeria100% (2)
- Kawasaki DiseaseDokument38 SeitenKawasaki DiseaseJayson CabarceNoch keine Bewertungen
- SIADH (Syndrome of Inapproperiate Antidiuretic Hormone Secretion)Dokument11 SeitenSIADH (Syndrome of Inapproperiate Antidiuretic Hormone Secretion)itsmesubu100% (2)
- Post-op-Case-Conference-DM FootDokument44 SeitenPost-op-Case-Conference-DM FootShereen DS Lucman100% (1)
- Decrease Cardiac OutputDokument6 SeitenDecrease Cardiac OutputGerardeanne ReposarNoch keine Bewertungen
- Heart Failure COncept MapDokument2 SeitenHeart Failure COncept MapJrBong SemaneroNoch keine Bewertungen
- Angina PectorisDokument25 SeitenAngina PectorisPC NNoch keine Bewertungen
- Addison'sDokument4 SeitenAddison'sKoRnflakesNoch keine Bewertungen
- Pathophysiology Diagram of Congestive Heart FailureDokument3 SeitenPathophysiology Diagram of Congestive Heart FailureLeng Royo BrionesNoch keine Bewertungen
- NCP UgibDokument4 SeitenNCP UgibErnest Brian FernandezNoch keine Bewertungen
- PathophysiologyDokument2 SeitenPathophysiologyKarla Karina Dela CruzNoch keine Bewertungen
- Hypovolemic Shock 05Dokument50 SeitenHypovolemic Shock 05Chary JaztineNoch keine Bewertungen
- Intra Abdominal HypertensionDokument22 SeitenIntra Abdominal HypertensionFernando MorenoNoch keine Bewertungen
- NCP DMDokument21 SeitenNCP DMKate ManalastasNoch keine Bewertungen
- Acute Coronary Syndrome - CSDokument91 SeitenAcute Coronary Syndrome - CSMASII89% (9)
- Myocardial InfarctionDokument28 SeitenMyocardial Infarctionshaitabligan100% (1)
- Case Study Pleural EffusionDokument4 SeitenCase Study Pleural EffusionKhristine Anne FabayNoch keine Bewertungen
- Patofisiologi Septic-ShockDokument35 SeitenPatofisiologi Septic-ShockAmiroh Kurniati50% (2)
- Sepsis, Septic Shock, MODSDokument19 SeitenSepsis, Septic Shock, MODSPaul Zantua80% (5)
- Hemodialysis: Carina Joane Villareal-Barroso, R.N.,M.NDokument108 SeitenHemodialysis: Carina Joane Villareal-Barroso, R.N.,M.NJune BarsNoch keine Bewertungen
- HypocalcemiaDokument24 SeitenHypocalcemiaกรคุง ภิญโญพจนารถ100% (3)
- Decreased Cardiac Output FinalDokument2 SeitenDecreased Cardiac Output FinalSandraDeeNoch keine Bewertungen
- A Case Study About Upper GastroIntestinal BleedingDokument46 SeitenA Case Study About Upper GastroIntestinal BleedingChristal Mae VillaminNoch keine Bewertungen
- Mary Cris Canon CHF For or Case Study.Dokument12 SeitenMary Cris Canon CHF For or Case Study.Mary Cris CanonNoch keine Bewertungen
- 403 Full PDFDokument10 Seiten403 Full PDFKuroto YoshikiNoch keine Bewertungen
- CholangitisDokument4 SeitenCholangitisNarianne Mae Solis Bedoy100% (1)
- Hemorrhagic Cerebro Vascular DiseaseDokument37 SeitenHemorrhagic Cerebro Vascular Diseasejbvaldez100% (1)
- Acute Kidney InjuryDokument16 SeitenAcute Kidney InjuryPutrii Rahayu Sriikandi100% (1)
- Pneumothorax+Case+Study+ 1Dokument2 SeitenPneumothorax+Case+Study+ 1Anonymous iOpPt7sIoNoch keine Bewertungen
- Pathophysiology of CholangitisDokument4 SeitenPathophysiology of CholangitisAmni 'Pam' Zulkifar100% (1)
- Anatomy and Physiology PneumoniaDokument4 SeitenAnatomy and Physiology PneumoniaJohnson MallibagoNoch keine Bewertungen
- Acute Post-Streptococcal GlomerulonephritisDokument15 SeitenAcute Post-Streptococcal GlomerulonephritisJeanne Marie ValesNoch keine Bewertungen
- Pleural EffusionDokument12 SeitenPleural EffusionWan HafizNoch keine Bewertungen
- Hemorrhagic StrokeDokument27 SeitenHemorrhagic StrokeMuhammad FarhanNoch keine Bewertungen
- PELVIOLITHIASISDokument45 SeitenPELVIOLITHIASISAriane VidalNoch keine Bewertungen
- Acetaminophen ToxicityDokument14 SeitenAcetaminophen ToxicityJam MajNoch keine Bewertungen
- Left-Sided Heart FailureDokument3 SeitenLeft-Sided Heart FailureKhalid Mahmud ArifinNoch keine Bewertungen
- Hypovolemic ShockDokument13 SeitenHypovolemic ShockJed ProwellNoch keine Bewertungen
- HA-RLE-WS # 8 Assessing CultureDokument5 SeitenHA-RLE-WS # 8 Assessing CultureJULIE ANNE CORTEZNoch keine Bewertungen
- Hypertensive Emergencies in The Emergency DepartmentDokument13 SeitenHypertensive Emergencies in The Emergency DepartmentLuis Lopez RevelesNoch keine Bewertungen
- Hypertensive CrisisDokument60 SeitenHypertensive CrisisDzikrul Haq KarimullahNoch keine Bewertungen
- Uncontrolled Blood PressureDokument6 SeitenUncontrolled Blood PressureFika SilviaNoch keine Bewertungen
- Therapy of Acute Respiratory Infections in Children: NoveltiesDokument11 SeitenTherapy of Acute Respiratory Infections in Children: NoveltiesrizkaNoch keine Bewertungen
- Valvular Heart DiseaseDokument73 SeitenValvular Heart Diseaseindia2puppy100% (4)
- Case 4-2021: A 70-Year-Old Woman With Dyspnea On Exertion and Abnormal Findings On Chest ImagingDokument12 SeitenCase 4-2021: A 70-Year-Old Woman With Dyspnea On Exertion and Abnormal Findings On Chest ImagingBruno ConteNoch keine Bewertungen
- Esophageal Diverticula - AMBOSSDokument1 SeiteEsophageal Diverticula - AMBOSSRazan Al-ZataryNoch keine Bewertungen
- Kawasaki Disease Case ReportDokument17 SeitenKawasaki Disease Case ReportAlvaro Villarejo PérezNoch keine Bewertungen
- Treatment of Portal HypertensionDokument10 SeitenTreatment of Portal HypertensionLourianne NcNoch keine Bewertungen
- Neuro Trauma: Nathan Mcsorley Speciality Trainee Neurosurgery 23B Ninewells HospitalDokument35 SeitenNeuro Trauma: Nathan Mcsorley Speciality Trainee Neurosurgery 23B Ninewells HospitalnathanNoch keine Bewertungen
- Rheumatoid Arthritis Drug StudyDokument2 SeitenRheumatoid Arthritis Drug StudyChristaNoch keine Bewertungen
- Nursing Care Plan: University of Tabuk Faculty of Applied Medical Science Department of NursingDokument3 SeitenNursing Care Plan: University of Tabuk Faculty of Applied Medical Science Department of NursingZedoo AlmaroaaneNoch keine Bewertungen
- World Rabies DayDokument6 SeitenWorld Rabies DayZETTYNoch keine Bewertungen
- Mi (Case # 1) : 1. How Would You Classify Mr. Smith's Chest Pain?Dokument11 SeitenMi (Case # 1) : 1. How Would You Classify Mr. Smith's Chest Pain?Faizan MazharNoch keine Bewertungen
- Land of NodDokument7 SeitenLand of NodMaltesers1976Noch keine Bewertungen
- Magic Surgery NotesDokument54 SeitenMagic Surgery NotesChimwemwe TemboNoch keine Bewertungen
- Learning Area Grade Level Quarter Date: English 9 4Dokument4 SeitenLearning Area Grade Level Quarter Date: English 9 4Kim So-Hyun100% (1)
- Neonatal Respiratory DistressDokument59 SeitenNeonatal Respiratory DistressMohamad Saleh100% (7)
- QRP Neurology Part 2Dokument245 SeitenQRP Neurology Part 2lakshminivas PingaliNoch keine Bewertungen
- Brief Description Down Syndrome A. DescriptionDokument4 SeitenBrief Description Down Syndrome A. DescriptionJohn Rey AbadNoch keine Bewertungen
- Aleukemic LeukemiaDokument3 SeitenAleukemic LeukemialilisNoch keine Bewertungen
- Cleansing and DetoxificationDokument1 SeiteCleansing and DetoxificationerosNoch keine Bewertungen
- Drug Name Gemcitabine: Synonym (S) : Common Trade Name (S) : ClassificationDokument8 SeitenDrug Name Gemcitabine: Synonym (S) : Common Trade Name (S) : ClassificationOka Robi MuhammadNoch keine Bewertungen
- Homeopathy Cases by KadwaDokument179 SeitenHomeopathy Cases by Kadwaabckadwa100% (3)
- Jabeen & TahirDokument12 SeitenJabeen & TahirSanaNoch keine Bewertungen
- Osce RadioDokument74 SeitenOsce Radioberhanu nathanielNoch keine Bewertungen
- NCM 104 RLE Module 3 FinalsDokument22 SeitenNCM 104 RLE Module 3 FinalsAlexander DontonNoch keine Bewertungen
- Pass The MRCS HistoryDokument115 SeitenPass The MRCS HistoryMariajanNoch keine Bewertungen
- Rickettsia eDokument10 SeitenRickettsia eDeep Iyaz100% (1)
- Epidemiological and Clinical Features of Pediatric COVID-19: Researcharticle Open AccessDokument7 SeitenEpidemiological and Clinical Features of Pediatric COVID-19: Researcharticle Open AccessAditha Fitrina AndianiNoch keine Bewertungen
- De Quervains TendonitisDokument2 SeitenDe Quervains TendonitisisnainiNoch keine Bewertungen
- 1 InfectionDokument41 Seiten1 InfectionIMA MSN TNNoch keine Bewertungen