Beruflich Dokumente
Kultur Dokumente
Pediatric Surgery Dr. A. Igama
Hochgeladen von
Marco Paulo Reyes NaoeOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Pediatric Surgery Dr. A. Igama
Hochgeladen von
Marco Paulo Reyes NaoeCopyright:
Verfügbare Formate
PEDIATRIC
SURGERY
Neonate
-
Air
distends
GIT,
splinting
diaphragm
-
Gastric
fluid
refluxes
into
lungs
-
Saliva
pools
in
pouch
&
aspirated
Recognition
Prenatal
-
Ultrasound
Polyhydraminos
No gastric bubble
Dr. Alfredo Igama
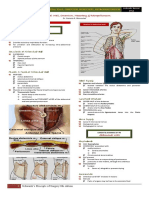
NEONATAL RESPIRATORY DISTRESS
Objectives
To be able to recognize 3 surgical conditions as possible
causes of respiratory distress in neonates, namely:
(1) Esophageal Atresia
(2) Diaphragmatic hernia
(3) Eventration of the diaphragm
To be able to explain the pathophysiology involved in the
above conditions
To be able to provide the appropriate initial management
in such cases
To be familiar with the basic surgical therapy for such
cases
Neonate
-
Clinical
Excessive drooling
Choking when fed
Progressive respiratory distress
-
ESOPHAGEAL ATRESIA / TRACHEO-ESOPHAGEAL FISTULA
Etiology:
Intraembryonic pressure
Epithelial closure
Vascular accident
Factors affecting rate and timing of cell proliferation &
differentiation in region of trachea & lung bud before 4
weeks AOG
Radiologic
Tip of catheter confirms level of pouch
Contrast instillation seldom needed
Contrast actually contraindicated:
barium toxic to lungs
Also
confirms:
Distal
TEF
Duodenal
atresia
Incidence:
1 in 2,500 live births
Most common type is esophageal atresia with distal
tracheoesophageal fistula
There is a slight male preponderance
Chromosomal anomalies frequent (6.6% of infants)
trisomy 13 and 18
Types:
80-90%
5-8%
2-4%
1%
1%
Isolated EA
With gas in abdomen
Gas in stomach only or
double bubble
Gasless abdomen
Prediction of Survival (Spitz Classification)
Group Rate (%)
Birth weight > 1,500g w/o major Congenital Heart
1.
Disease
Birth weight < 1,500 g or a major Congenital Heart
2.
Disease
Birth weight < 1,500 g and a major Congenital Heart
3.
Disease
Pre-operative Preparations:
Limit stress
Keep warm
Hydration
NPO, suction upper pouch
Upper body elevated (if with TEF)
Check for other anomalies
EA
with
distal
TEF
Isolated
EA
Isolated
TEF
EA
with
proximal
TEF
EA
with
proximal
&
distal
TEF
Survival
97
59
22
Positioning of Patient & EA Pouch Decompression
Associated
Anomalies:
1. Cardiovascular
anomalies
11-49%
2. GUT
24%
3. GIT
24%
4. Skeletal
13%
5. Neural
tube
defects
23%
6. Hydrocephalus
5.2%
Pathophysiology:
In
utero
-
Upper
pouch
distends,
compressing
trachea
&
causing
tracheomalacia
-
Amniotic
fluid
in
airways
drain
to
GIT
(through
fistula),
with
decreased
stenting
of
alveoli
Determine other associated congenital anomalies
-
VACTERL syndrome
Surgical
Options:
Immediate Primary Repair
-
Early correction of all anomalies
-
May not be tolerated by patients in poor medical
condition
Page 1 of 6
DR. ALFREDO IGAMA MAY 18-19, 2015
Delayed Primary Repair
-
Improve patients condition over a few days before
definitive surgery
-
Requires dedicated supportive care
Staged
Procedure
-
Several
successive
surgeries
as
the
patients
condition
permits
-
Supportive
care
not
too
demanding
Surgical Procedures:
Staging
Procedures
-
Gastrostomy
-
Medium-
to
long-term
vascular
access
-
Cervical
esophagostomy
-
TEF
occlusion
or
ligation
(w/o
esophageal
anastomosis)
-
Esophageal
lengthening
-
Esophageal
replacement
Primary
Correction
-
Trans0thoracic
ligation
of
TEF
with
esophageal
anastomosis
-
Throacoscopic
approach
recent
development
Complications:
Anastomotic leak
Stricture
Recurrent TEF
Gastroesophageal reflux
Tracheomalacia
Diagnosis:
Prenatal ultrasound 25 weeks
-
Bowel loops within chest
-
Polyhydramnios
-
Absent or intrathoracic gas bubble
-
Mediastinal
-
Fetal hydrops
Amniocentesis
Chromosomal analysis
Maternal Serum AFP
Chest
X-ray
air
and
fluid
loops
within
the
left
hemithorax
-
Mediastinal
shift
-
Minimal
gas
within
abdomen
Management:
1. Prenatal
Care
-
Support
the
fetus
and
bring
to
term
-
Refer
to
the
appropriate
tertiary
perinatal
center
2.
Preoperative
care
-
Conventional
mechanical
ventilation
Avoid
mask
-
Endotracheal
intubation
-
Control
pul,onary
HPN
-
Neuromuscular
blockade
-
NGT
-
Echocardiography
-
Surfactant
replacement
therapy
-
Nitric
oxide
-
Extracorporeal
membrane
oxygenation
(ECMO)
3.
Surgical
Management
-
Timing
delayed
until
there
is
evidence
that
the
pulmonary
hypertension
has
been
resolved
-
Technique
repair
of
defect
primarily
or
with
prosthesis
Types:
CONGENITAL DIAPHRAGMATIC HERNIA
Herniation of abdominal organs into the thoracic cavity
through a defect in the diaphrag
1 in 2,000-5,000 live births
2x in females
Questions on CDH
30-60% overall mortality
will from Dr.
Tecsons lecture
Bochdalek
85-90%
-
Posterolateral
-
Left-sided
80-90%
Morgagni
2.6%
-
Retrosternal
Pentalogy
of
Cantrell
1. Omphalocoel
2. Inferior
sternal
cleft
3. Severe
cardiac
defect
ectopia
cordis
4. Pericardial
defects
5. Hiatal
hernia
Defects:
Pulmonary
hypoplasia
-
Decreased
pulmonary
mass
and
weight
-
Decreased
branchial
divisions
-
Reduction
in
the
number
of
alveoli
and
bronchioles
Increase muscularization of pulmonary arterioles
Persistent pulmonary HPN
Surfactant deficiency
Associated
anomalies
Clinical
Presentation:
Respiratory
distress
-
Tachypnea,
grunting
respiration,
chest
retraction,
pallor
cyanosis
-
Hypoxia,
hypercarbia,
acidosis
Scaphoid
abdomen
Increased
chest
diameter
Mediastinal
shift
Bowel
sounds
in
the
chest
Decreased
breath
sounds
EVENTRATION OF THE DIAPHRAGM
Abnormal elevation of the diaphragm
Paradoxical motion of respiration
Incomplete development of muscles and central tendon
Mostly left-side
Clinical Manifestations:
Respiratory distress
Tachypnea
Pallor
Decreased breath sounds
Mediastinal shift
DR. ALFREDO IGAMA MAY 18-19, 2015
Chest Radiology:
Elevated
hemidiaphragm
Fluoroscopy
or
Ultrasound:
Paradoxic motion diaphragm
Mediastinal
shift
Treatment:
Plication
of
the
diaphragm
Page
2
of
6
Vomiting
Normal vomiting
Abnormal
vomiting
-
Medical
vs.
Surgical
-
Color
(bilious
=
surgical)
-
Timing
-
Manner
of
vomiting
Diagnostics:
Ultrasound
-
Doughnut
sign
-
Target
bulls
eye
sign
-
3-4
mm
muscle
thickness
(normal
1-2
mm)
UGIS
-
String
sign
-
Shoulder
sign
Electrolyte disturbance
Hypochloremic hypokalemic metabolic alkalosis
Management
Correct electrolyte imbalance normal saline
Ramstedts
pyloromyotomy
Intestinal Obstruction in the Newborn
Bilious emesis cardinal symptom
Prompt recognition & treatment
Classification
Bilious
vomiting
w/
minimal
abdominal
distention
(a) Proximal
obstruction
Paucity
of
gas
No
distal
air
(b) Distal
Bilious
emesis
and
abdominal
obstruction
distention
DUODENAL
OBSTRUCTION
Duodenal
atresia
Duodenal
web
Duodenal
stenosis
Annular
pancreas
Duodenal
duplication
Malrotation
w/
midgut
volvulus
Duodenal Atresia
Failure of recanalization of the duodenal lumen from its
solid cord stage
Classification of Duodenal Atresia
Description
Mucosal diaphragmatic membrane
Most common
Short fibrous cord connecting the two sides
Complete separation of two ends
Abdominal calcification meconium peritonitis
Pneumatosis / free abdominal air NEC
Plain abdominal x-ray
Ba Enema
-
Microcolon or to identify small vs. large colon
HYPERTROPHIC PYLORIC STENOSIS
Most common cause of gastric outlet obstruction in children
Type
I
II
III
Clinical Presentation and Diagnosis
-
Hx of polyhydramnios (30-50%)
-
Associated Downs syndrome
-
Bilious vomiting
-
Full epigastrium
-
Abdominal distention not observed
-
NGT > 30 mL of bile-stained gastric fluid
-
Double-bubble sign
Management:
-
Fluid
and
electrolyte
correction
-
OGT
-
Duodenoduodenostomy
Associated
Anomalies:
-
Annular
pancreas
-
Malrotation
-
Anterior
portal
vein
-
Downs
syndrome
Incidence:
1-3 in every 1,000 live births
M-F
=
4:1
Associated Anomalies:
Intestinal malrotation
Obstructive uropathy
Esophageal atresia
Etiology:
Gastric hyperacidity leading to muscle spasm and
hypertrophy
Abnormal pyloric innervation
Abnormal motility secondary to pacemaker cells
Clinical Presentation:
Nonbilious, projectile vomiting shortly after feeding
between 3 and 6 weeks old
Blood-streaked or coffee-ground vomitus
Infant constantly hungry
History of frequent formula changes
Palpable olive-shaped mass in the RUQ
Differential Diagnosis:
Overfeeding
GER
Elevated ICP
Pylorospasm with delayed gastric emptying
Antral web
Gastric neoplasm
Gastric duplication
Extrinsic gastric compression
JEJUNOILEAL
ATRESIA
Etiology:
Vascular occlusion
Mesenteric vascular accidents
Incidence:
1 of 400 to 1 of 5,000 live births
Type
I
II
IIIa
Classification of Jejunoileal Atresia
Description
Membranous atresia with intact mesentery
19%
Blind ends of the bowel with intact mesentery
31%
Blind with defect in the mesentery
46%
Page 3 of 6
DR. ALFREDO IGAMA MAY 18-19, 2015
GIT: SURGICAL CAUSES OF VOMITING
Topic Guide:
1.
Hypertrophic Pyloric Stenosis
2.
Duodenal Obstruction
3.
Jejunoileal Atresia
4.
Malrotation and Volvulus
5.
Intussusception
6.
Hirschprungs Disease
Diagnosis:
History of maternal polyhydramnios (> 2,000 mL)
Bilious vomiting
Abdominal distention
Failure to pass normal amounts of meconium
st
-
1 24 hours of life
-
250 grams passed rectally
Baby gram supine, upright, lateral
Ladds bands obstructing the duodenum
Narrow mesenteric pedicle
Volvulus obstructing the jejunum at its blood supply
Management:
Fluid and electrolyte correction
Maintain appropriate body temperature
NGT
Antibiotics
Surgical
Management
-
Upper
abdominal
distention
-
Reestablish
intestinal
continuity
-
Preserve
bowel
length
and
normal
anatomy
-
End-to-oblique
anastomosis
Nutritional
support
Morbidity:
Pneumonia
Peritonitis
Sepsis
MALROTATION
AND
VOLVULUS
Congenital
abnormal
positioning
of
midgut
Elongation
Rotation
Fixation
Clinical
Presentation:
st
Seen in the 1 few weeks of life
Bile-stained vomitus due to obstruction of the upper third
of the duodenum
Abdominal distention
Pain and irritability
Passage of blood per rectum
Failure to thrive older infants
Erythema and edema of the abdominal wall
Intestinal
Development
6
weeks
rapid
growth
of
intestines
10-12
weeks
midgut
returns
to
abdominal
cavity
o
270
counter-clockwise
rotation
around
the
superior
mesentery
C-loop
duodenum
fixed
retroperitoneally
at
the
right
upper
quadrant
Cecum
fixed
to
the
lateral
abdominal
wall
at
the
right
lower
quadrant
Radiologic Diagnosis:
Plain abdominal X-ray
-
Paucity of intestinal gas
-
Few scattered air-fluid levels
-
Distended gastric and duodenum
Normal Intestinal Rotation
Incomplete Rotation:
Results from non-fixation of the ascending and descending
portion of the colon to the retroperitoneum and a
redundant small mesentery
Cecum remains in the epigastrium
UGIS
-
Preferred
diagnostic
study
-
Corkscrew-like
deformity
of
the
duodenum
-
Duodenum
and
jejunum
is
in
the
right
upper
(normally
wala
sa
right)
-
Dilated
stomach
and
airless
abdomen
Barium
enema
is
only
suggestive
of
Management:
OGT
IVF resuscitation
Antibiotics
Surgery should be done within 4-8 hours because of the
threat of volvulus
-
Counter-clockwise derotation of the volvulus
Page 4 of 6
DR. ALFREDO IGAMA MAY 18-19, 2015
Paucity of intestinal gas on X-ray
Clinical Presentation:
Well nourished male infant about 8 months of age
suddenly awakens from sleep with colicky abdominal pain.
Pain may pass and the child may go back to sleep, only to
be awakened shortly with a similar picture that does not
remit. Pain is followed by several bouts of vomiting that
may become bilious and then the passage of blood mucus
rectally, which has the appearance of currant jelly.
Robust, healthy infant with abdominal colic
Stools normal then dark redmucoid stools like currant
jelly 95%
Vomitus undigested bilious 80%
Lethargic and somnolent between attacks
Sausage-shaped abdominal mass
Pathology:
Idiopathic
intussusception
-
Less
than
1-year-old
-
During
attacks
of
upper
respiratory
tract
infections
and
diarrhea
-
Adenovirus,
rotavirus,
rheovirus,
echovirus
-
Hypertrophy
of
Peyers
patches
Intussusception in older age group secondary to
anatomical lead point Meckels diverticulum, appendix,
polyp, tumors, foreign bodies
Starts with venous compression from the invagination fo
the bowel and its
Diagnostic Studies:
CBC, serum electrolytes
Plain abdominal x-ray not diagnostic
-
Abdominal mass
-
Mabnormal distribution of gas and fecal contents
-
Sparse large bowel gas
-
Air-fluid levels in the presence of bowel obstruction
Abdominal
ultrasound
-
Target
lesion
-
Pseudokidney
sign
-
-
-
-
Antibiotics
BT
Hydrostatic
barium
enema
or
saline
reduction
Pneumatic
reduction
Surgical
-
When
non-operative
management
fails
-
Manual
reduction
anastomosis
if
gangrenous
-
Appendectomy
HIRSCHPRUNGS
DISEASE
Congenital
absence
of
parasympathetic
ganglia
cells
in
the
wall
of
the
GT
tract
Bowel
unable
to
relax
and
without
peristalsis
Involves
rectum
extending
proximally
75%
rectosigmoid
Incidence:
1 in 5,000 live births
M-F ratio 4:1
Total aganglionosis reverse
30% of patients have relatives afflicted with disease
Clinical Presentation:
Newborn
-
Non-passage
or
delayed
passage
of
meconium
-
Abdominal
distention
-
Bilious
vomiting
-
Visible
bowel
loops
-
Rectal
exam
Rectal vault empty
Increased sphincteric tone
Explosive stools on removal of examining finger
Infants and older children
-
History of obstipation and constipation
-
Failure to thrive
-
History of delayed passage of meconium
-
Abdominal distention
-
Bouts of diarrhea and vomiting (enterocolitis)
-
Foul-smelling stools
Diagnosis:
Plain abdominal X-rays
-
Air-fluid levels
-
Distended bowels
-
No presacral air
Barium
enema
-
Spasm
and
a
narrowed
lumen
-
Transition
zone
Tissue confirmation: Auerbach plexus in muscular layer
-
Biopsy specimens
Seromuscular biopsy of bowel wall
Full thickness transrectal biopsy
-
Suction biopsy Meissners plexus in submucosal
layer
Management:
Non-operative no signs or peritonitis, perforation,
sepsis, and gangrene
-
NGT
-
IVF
Page
5
of
6
DR. ALFREDO IGAMA MAY 18-19, 2015
Malrotation:
Ladds
Procedure
-
Straightening
of
Duodenbum
-
Widening
of
Mesentery
-
Small
bowel
at
the
right
hemiabdomen;
large
bowel
at
the
left
-
Appendectomy
(optional)
INTUSSUSCEPTION
Invagination
of
a
portion
of
the
intestine
into
itself,
producing
vascular
compromise
Majority are ileocolic and
without lead point
Seen in infants between
5-10 months old
Adenovirus and rotavirus
infection prior to
intussusception
Trans-anal Rectal Biopsy:
Definitive diagnosis for Hirschsprungs disease
-
Open
-
Suction
Differential Diagnosis:
Premature infant
Sepsis
NEC
Meconium plug syndrome
Intestinal dysmotility syndrome
Functional
constipation
Preoperative Management
Colonic / rectal decompression with warm saline
Gastric decompression
Treat enterocolitis
Colostomy normal segment
Nutrition
Operative Management:
Usually performed between 4 months and 1 year of age
and weight of 12-20 lbs
Goal:
-
Resection
of
the
involved
segment
-
Re-establishment
of
functional
and
continent
anus
Definitive
procedures:
-
Swenson
procedure
-
Duhamel
procedure
-
Scott
Boleys
endorectal
pullthrough
Pull-Through Procedures:
Soave-Boley technique
Swensons
technique
AJB J Medicine Batch 2016
Page 6 of 6
DR. ALFREDO IGAMA MAY 18-19, 2015
Das könnte Ihnen auch gefallen
- Case Study On SyphillisDokument18 SeitenCase Study On Syphillisdia_pee100% (1)
- 5 6057345046456304562Dokument490 Seiten5 6057345046456304562DK DeepakNoch keine Bewertungen
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Dokument13 SeitenSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101Noch keine Bewertungen
- Pharma Super TableDokument56 SeitenPharma Super TableMarco Paulo Reyes NaoeNoch keine Bewertungen
- 008 Plain X-Ray AbdomenDokument7 Seiten008 Plain X-Ray AbdomenAthul GurudasNoch keine Bewertungen
- A System of Operative Surgery, Volume IV (of 4)Von EverandA System of Operative Surgery, Volume IV (of 4)Bewertung: 4 von 5 Sternen4/5 (1)
- Microscopic Examination of UrineDokument89 SeitenMicroscopic Examination of UrineLucia SurduNoch keine Bewertungen
- Florist ContractDokument1 SeiteFlorist ContractMarco Paulo Reyes NaoeNoch keine Bewertungen
- Congenital AnomaliesDokument69 SeitenCongenital AnomaliesArnella Hutagalung100% (1)
- Budwig Cancer GuideDokument101 SeitenBudwig Cancer Guidedora.oreiro9920Noch keine Bewertungen
- Pediatric Surgery 2 (Respiratory and Gastrointestinal Conditions) PDFDokument12 SeitenPediatric Surgery 2 (Respiratory and Gastrointestinal Conditions) PDFRenatoCosmeGalvanJunior100% (1)
- Systemic Surgery NuggetsDokument17 SeitenSystemic Surgery NuggetsAhmad UsmanNoch keine Bewertungen
- A Disease Study On: AppendectomyDokument8 SeitenA Disease Study On: Appendectomybryan leguiabNoch keine Bewertungen
- Anal ProblemsDokument35 SeitenAnal ProblemsSandip VaghelaNoch keine Bewertungen
- The Spleen - A Surgical Perspective: by Col. Abrar Hussain ZaidiDokument43 SeitenThe Spleen - A Surgical Perspective: by Col. Abrar Hussain Zaidiabrar_zaidiNoch keine Bewertungen
- PEDTRIC SURGERY Dr. Isabedra - PDF Notes - 201702082201Dokument25 SeitenPEDTRIC SURGERY Dr. Isabedra - PDF Notes - 201702082201deevonc100% (1)
- SURGERY 2 Decury Notes Pediatric SurgeryDokument3 SeitenSURGERY 2 Decury Notes Pediatric SurgeryDasha VeeNoch keine Bewertungen
- Surgery TacticsDokument154 SeitenSurgery TacticsAiman Arifin0% (1)
- Vascular InjuryDokument85 SeitenVascular InjuryWildaNoch keine Bewertungen
- Selective Serotonin Reuptake Inhibitors: Naoe, Marco Paulo RDokument38 SeitenSelective Serotonin Reuptake Inhibitors: Naoe, Marco Paulo RMarco Paulo Reyes NaoeNoch keine Bewertungen
- Surgery Oral Exam TopicsDokument115 SeitenSurgery Oral Exam Topicsmange24Noch keine Bewertungen
- Basic Emergency Skills in Trauma Part 3 - Penetrating Abdoninal Injury - Dr. Oliver BelarmaDokument3 SeitenBasic Emergency Skills in Trauma Part 3 - Penetrating Abdoninal Injury - Dr. Oliver BelarmaRaquel ReyesNoch keine Bewertungen
- 1 Inguinal Hernia EditedDokument34 Seiten1 Inguinal Hernia EditedNadhirah ZulkifliNoch keine Bewertungen
- Assessment of Back Pain-BMJDokument30 SeitenAssessment of Back Pain-BMJMarco Paulo Reyes NaoeNoch keine Bewertungen
- Inguinal Scrotal SwellingsDokument23 SeitenInguinal Scrotal SwellingsAzmyza Azmy100% (1)
- Pediatric Surgical Handbook PDFDokument139 SeitenPediatric Surgical Handbook PDFNia LahidaNoch keine Bewertungen
- General Principles of Fracture ManagmentDokument55 SeitenGeneral Principles of Fracture ManagmentkylieverNoch keine Bewertungen
- Paediatric Surgery - Common ProblemsDokument32 SeitenPaediatric Surgery - Common ProblemsPhaniraj RamachandrulaNoch keine Bewertungen
- eMRCS Pathology 326 MCQsDokument101 SeiteneMRCS Pathology 326 MCQsSaad KhanNoch keine Bewertungen
- Applied Anatomy of Upper Limb Part OneDokument66 SeitenApplied Anatomy of Upper Limb Part Oneprinceej100% (3)
- Osteomyelitis: Acute & ChronicDokument35 SeitenOsteomyelitis: Acute & ChronicrainakenovNoch keine Bewertungen
- Head & Neck: Most CommonDokument6 SeitenHead & Neck: Most CommonJüdith Marie Reyes BauntoNoch keine Bewertungen
- Surgery CaseDokument43 SeitenSurgery CaseAvni GuptaNoch keine Bewertungen
- Abdominal Surgery All in OneDokument50 SeitenAbdominal Surgery All in OneAnne ChoyNoch keine Bewertungen
- Schwartz 9th Ed: Chapter Outline: The SpleenDokument22 SeitenSchwartz 9th Ed: Chapter Outline: The SpleenKathryn Reunilla100% (1)
- PSGS Review 2015Dokument230 SeitenPSGS Review 2015yassercarlomanNoch keine Bewertungen
- Help Pedsurgeryafricavolume01 PDFDokument413 SeitenHelp Pedsurgeryafricavolume01 PDFEbuwa AmadasunNoch keine Bewertungen
- Hernia Examination OSCE GuideDokument7 SeitenHernia Examination OSCE GuideEssa AfridiNoch keine Bewertungen
- Medicine CPC ScriptDokument4 SeitenMedicine CPC ScriptMarco Paulo Reyes NaoeNoch keine Bewertungen
- Medicine Palliative CareDokument5 SeitenMedicine Palliative CareMarco Paulo Reyes NaoeNoch keine Bewertungen
- Preoperative Evaluation: Mary Diane Z. IsmaelDokument44 SeitenPreoperative Evaluation: Mary Diane Z. IsmaelDiane IsmaelNoch keine Bewertungen
- ABSITE CH 37 Anal and Rectal PDFDokument13 SeitenABSITE CH 37 Anal and Rectal PDFJames JosephNoch keine Bewertungen
- 4 PEDIA 8 - Bleeding DisordersDokument5 Seiten4 PEDIA 8 - Bleeding DisordersRainy Liony DuhNoch keine Bewertungen
- BreastDokument49 SeitenBreastcryphonexyNoch keine Bewertungen
- Goc Marina Reviewer PDFDokument57 SeitenGoc Marina Reviewer PDFAl Jhem Geronimo60% (5)
- 2018.surgery Intestinal Obstruction in Infants and ChildrenDokument11 Seiten2018.surgery Intestinal Obstruction in Infants and ChildrenFranz SalazarNoch keine Bewertungen
- Emergency Pediatric SurgeryDokument27 SeitenEmergency Pediatric SurgerysoftmailNoch keine Bewertungen
- Essentials for Practice of Medicine in the Frontline: From Tropical Africa; Pleasantly Different Volume 2Von EverandEssentials for Practice of Medicine in the Frontline: From Tropical Africa; Pleasantly Different Volume 2Noch keine Bewertungen
- Anatomy of OesophagusDokument25 SeitenAnatomy of OesophagusRabi SyedNoch keine Bewertungen
- Surgery - Pediatric GIT, Abdominal Wall, Neoplasms - 2014ADokument14 SeitenSurgery - Pediatric GIT, Abdominal Wall, Neoplasms - 2014ATwinkle SalongaNoch keine Bewertungen
- Anatomic Defects of The Abdominal WallDokument4 SeitenAnatomic Defects of The Abdominal WallKristen MontejoNoch keine Bewertungen
- QC1 Prelims 2019 HandoutsDokument202 SeitenQC1 Prelims 2019 HandoutsFrances Salud40% (5)
- Phyllodes TumorDokument20 SeitenPhyllodes TumorManuela KarinaaNoch keine Bewertungen
- TableDokument6 SeitenTablemanuNoch keine Bewertungen
- Examination of Head and Neck SwellingsDokument22 SeitenExamination of Head and Neck SwellingsObehi EromoseleNoch keine Bewertungen
- Abdominal Access TechniquesDokument7 SeitenAbdominal Access TechniquesdrmarcsNoch keine Bewertungen
- Operative Surgery ManualDokument273 SeitenOperative Surgery Manualvikeshramkelawon8422100% (1)
- PATHology Questions MGR Medical UniversityDokument40 SeitenPATHology Questions MGR Medical UniversityPONNUSAMY P50% (2)
- test1 محولDokument85 Seitentest1 محولTojan Faisal Alzoubi100% (1)
- 40 Phimosis 1Dokument8 Seiten40 Phimosis 1Navis Naldo AndreanNoch keine Bewertungen
- Case Protocol SampleDokument1 SeiteCase Protocol SampleMarco Paulo Reyes NaoeNoch keine Bewertungen
- Tutorials in Surgery For 4th Medical StudentsDokument180 SeitenTutorials in Surgery For 4th Medical StudentsAnonymous jSTkQVC27bNoch keine Bewertungen
- ThesisDokument140 SeitenThesisPrem LathaNoch keine Bewertungen
- Percutaneous Surgery of the Upper Urinary Tract: Handbook of EndourologyVon EverandPercutaneous Surgery of the Upper Urinary Tract: Handbook of EndourologyPetrisor Aurelian GeavleteBewertung: 5 von 5 Sternen5/5 (1)
- 3rd and 4th Stage of LaborDokument8 Seiten3rd and 4th Stage of LaborMarco Paulo Reyes NaoeNoch keine Bewertungen
- Intra Abdominal 2009Dokument8 SeitenIntra Abdominal 2009Shinta Dwi Septiani Putri WibowoNoch keine Bewertungen
- Carcinoma Penis Management: Dr. Lilamani Rajthala MS Resident Moderator: Dr. Samir ShresthaDokument63 SeitenCarcinoma Penis Management: Dr. Lilamani Rajthala MS Resident Moderator: Dr. Samir ShresthaBibek GhimireNoch keine Bewertungen
- Surgery Notes PDFDokument7 SeitenSurgery Notes PDFhassan_5953Noch keine Bewertungen
- Laparoscopic Repair of Inguinal HerniaDokument12 SeitenLaparoscopic Repair of Inguinal Herniawadhe omara100% (1)
- C 1+ 2 Surgicl Pathology of OesophagusDokument91 SeitenC 1+ 2 Surgicl Pathology of OesophagusSayuridark5Noch keine Bewertungen
- Fast HugDokument41 SeitenFast HugBharti NaraNoch keine Bewertungen
- (Surg2) 5.3 Urology Part 2 - Dr. YusiDokument19 Seiten(Surg2) 5.3 Urology Part 2 - Dr. YusiAlloiBialbaNoch keine Bewertungen
- PeritonitisDokument34 SeitenPeritonitisabrar_zaidiNoch keine Bewertungen
- Pouchitis and Ileal Pouch Disorders: A Multidisciplinary Approach for Diagnosis and ManagementVon EverandPouchitis and Ileal Pouch Disorders: A Multidisciplinary Approach for Diagnosis and ManagementNoch keine Bewertungen
- Ob-Gyn Post Graduate Interns May-June 2017-2018Dokument1 SeiteOb-Gyn Post Graduate Interns May-June 2017-2018Marco Paulo Reyes NaoeNoch keine Bewertungen
- Table of Contents Williams Endocrinology 13th EditionDokument4 SeitenTable of Contents Williams Endocrinology 13th EditionMarco Paulo Reyes NaoeNoch keine Bewertungen
- Fever and HyperthermiaDokument6 SeitenFever and HyperthermiaMarco Paulo Reyes NaoeNoch keine Bewertungen
- Williams Endocrinology Large CoverDokument1 SeiteWilliams Endocrinology Large CoverMarco Paulo Reyes Naoe33% (9)
- APRIL 2017: Aurora Hill and Engineer's Hill Health CentersDokument2 SeitenAPRIL 2017: Aurora Hill and Engineer's Hill Health CentersMarco Paulo Reyes NaoeNoch keine Bewertungen
- Special Awards - ListDokument7 SeitenSpecial Awards - ListMarco Paulo Reyes NaoeNoch keine Bewertungen
- Gastroenterology-Liver, Pancreas and Gall Bladder LecturesDokument7 SeitenGastroenterology-Liver, Pancreas and Gall Bladder LecturesMarco Paulo Reyes NaoeNoch keine Bewertungen
- Acute Nephritic SyndromeDokument1 SeiteAcute Nephritic SyndromeMarco Paulo Reyes NaoeNoch keine Bewertungen
- Adrenal Glands: I. Historical BackgroundDokument7 SeitenAdrenal Glands: I. Historical BackgroundMarco Paulo Reyes NaoeNoch keine Bewertungen
- Diseases of The Muscle - MEDISINA 2017Dokument9 SeitenDiseases of The Muscle - MEDISINA 2017Marco Paulo Reyes NaoeNoch keine Bewertungen
- Physiology of The Pleural SpaceDokument78 SeitenPhysiology of The Pleural SpaceAhmad RafiqiNoch keine Bewertungen
- Urinary System-WPS OfficeDokument21 SeitenUrinary System-WPS OfficeMario Sr. SumpoNoch keine Bewertungen
- Overview He Most As IsDokument20 SeitenOverview He Most As IsManushi ChauhanNoch keine Bewertungen
- Chin Chong MinDokument3 SeitenChin Chong MinSHine PukurNoch keine Bewertungen
- Nursing Care Plan Myocardia InfarctionDokument3 SeitenNursing Care Plan Myocardia Infarctionaldrin1920Noch keine Bewertungen
- Wikipedia Names ClearDokument127 SeitenWikipedia Names ClearJassim AlblooshiNoch keine Bewertungen
- Physical Capabilities of Instructors at The End of Hot Fire Training (0305) (158529)Dokument42 SeitenPhysical Capabilities of Instructors at The End of Hot Fire Training (0305) (158529)Onion PapaNoch keine Bewertungen
- Contents (Continued) : Chapter 5. Nondestructive Inspection (Ndi)Dokument3 SeitenContents (Continued) : Chapter 5. Nondestructive Inspection (Ndi)blackhawkNoch keine Bewertungen
- Agenda Prac Draft Agenda Meeting 7 10 February 2022 - enDokument69 SeitenAgenda Prac Draft Agenda Meeting 7 10 February 2022 - ennegfbNoch keine Bewertungen
- Tushar FinalDokument29 SeitenTushar FinalRaj Prixit RathoreNoch keine Bewertungen
- MPUshtrimet 20162017 Verore FDokument98 SeitenMPUshtrimet 20162017 Verore FJeronim H'gharNoch keine Bewertungen
- Vasoactive Agents in Shock.2Dokument8 SeitenVasoactive Agents in Shock.2Linamaria LozanoNoch keine Bewertungen
- Postmenopausal OSTEOPOROSIS GuidelinesDokument42 SeitenPostmenopausal OSTEOPOROSIS GuidelinesAbelNoch keine Bewertungen
- V Jttu/: Prices ChangeDokument179 SeitenV Jttu/: Prices ChangeKarpincho3Noch keine Bewertungen
- Craniospinal Irradiation AssignmentDokument8 SeitenCraniospinal Irradiation Assignmentapi-269666683Noch keine Bewertungen
- Farm ChemicalsDokument16 SeitenFarm ChemicalsHasrul RosliNoch keine Bewertungen
- Stock Per 2 Nov 20 HargaDokument13 SeitenStock Per 2 Nov 20 HargaLutfi QamariNoch keine Bewertungen
- Montana Polst FormDokument2 SeitenMontana Polst FormitargetingNoch keine Bewertungen
- Kosmetik BatalDokument5 SeitenKosmetik BatalNurul AtikNoch keine Bewertungen
- WarfarinDokument2 SeitenWarfarinWAHYU NOFANDARI HERDIYANTINoch keine Bewertungen
- Vocabulary Revision PhysiotherapyDokument4 SeitenVocabulary Revision PhysiotherapyHuong Giang100% (2)
- Avascular Necrosis - Causes, Symptoms, Prevention & TreatmentDokument26 SeitenAvascular Necrosis - Causes, Symptoms, Prevention & TreatmentSatrio Bangun NegoroNoch keine Bewertungen