Beruflich Dokumente
Kultur Dokumente
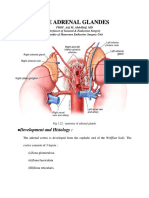
Adrenal Glands: I. Historical Background
Hochgeladen von
Marco Paulo Reyes NaoeOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Adrenal Glands: I. Historical Background
Hochgeladen von
Marco Paulo Reyes NaoeCopyright:
Verfügbare Formate
Topic
Guide:
I.
II.
III.
IV.
V.
VI.
VII.
VIII.
Historical
Background
Anatomy
Adrenal
Physiology
Disorders
of
the
Adrenal
Cortex
Disorders
of
the
Adrenal
Medulla
The
Adrenal
Incidentaloma
Adrenal
Insufficieny
Adrenal
Surgery
I. HISTORICAL
BACKGROUND
Bartolomeo
Provided
the
first
accurate
anatomic
account
of
Eustachus:
1563
the
adrenals
Baron
James
Cuvier:
1805
Described the anatomic division of the adrenals
into cortex and medulla
Thomas
Addison:
1855
Described the features of adrenal insufficiency,
which still bears his name
DeCreccio: 1865
Provided the first description of congenital
adrenal hyperplasia (CAH) occurring in a female
pseudohermaphrodite in 1865
Felix
Frankel:
1885
First identified pheochromocytomas but they
were not named as such until Ludwick Pick
(1912)
Ludwick
Pick:
1912
Term
pheochromocytoma
Noted
the
characteristic
chromaffin
reaction
of
the
tumor
cells
Adrenaline:
1897
Agent from the adrenal medulla that elevated
blood pressure in dogs
Subsequently named epinephrine in 1897
Cesar
Roux:
1926
Performed the first successful adrenalectomies
for pheochromocytoma in Switzerland
Charles
Mayo:
1927
Performed one of the first successful
adrenalectomies for pheochromocytoma in the
United States
Harvey
Cushing:
1932
Described 11 patients who had moon facies,
truncal obesity, hypertension, and other
features of the syndrome that now bears his
name
Kendall
First synthesized cortisone
Aldosterone:
1952
First identified in 1952
Jerome
Conn:
1955
Described the syndrome resulting from
excessive secretion of Aldosterone
Knowsley-
Thornton:
1889
First successful adrenalectomy
Removed a large, 20-pound, adrenal tumor with
the left kidney in a 36-year-old woman in 1889
Perry
Sargent:
1914
Performed the first planned adrenalectomy
Flank Approach
Used by Charles Mayo in 1927, he performed
adrenalectomies for pheochromocytoma; and
Roux in Switzerland
Michael
Gagner:
1992
Described the first laparoscopic procedure for
the adrenal gland
Since then, laparoscopic adrenalectomy became
standard of care approach for majority of benign
adrenal tumors
Martin Walz
Developed and modernized laparoscopic
posterior retroperitoneal adrenalectomy
II.
ANATOMY
Anatomy
The
adrenal
glands
are
paired,
retroperitoneal
organs
located
superior
and
medial
to
the
kidneys
at
the
level
of
the
eleventh
ribs.
The
normal
adrenal
gland
measures
5
3
1
cm
and
weighs
4
to
5
g.
The
right
gland
is
pyramidal
shaped
and
lies
in
close
proximity
to
the
right
hemidiaphragm,
liver,
and
infe-
rior
vena
cava
(IVC).
The
left
adrenal
is
closely
associated
with
the
aorta,
spleen,
and
tail
of
the
pancreas.
Histology
A. Cortex
-
Appears
yellow
due
to
high
lipid
content
-
Accounts
for
about
80
to
90%
of
the
glands
volume.
-
Histologically
divided
into
3
zones:
(1) Zona
Glomerulosa
(2) Zona
Fasciculata
(3) Zona
Reticularis
Outer
are
consists
of
small
cells
Zona
Site
of
production
of
mineralocorticoid
Glomerulosa
aldosterone
Made
up
of
larger
Site
of
production
of
cells
that
often
glucocorticoids
and
Zona
appear
foamy
due
adrenal
androgens
Fasciculata
to
multiple
lipid
inclusions
Cells
are
smaller
Zona
compared
to
Zona
Reticularis
fasciculata
B. Medulla
-
10-15%
of
adrenal
gland
volume
-
Reddish-brown
-
Produces
catecholamines
(epinephrine
&
norepinephrine)
-
Cells
are
polyhedral
arranged
in
cords
Referred as chromaffin cells because they stain
specifically with chromium salts
ADRENAL GLANDS Page 1 of 7
DR. BANNY C. BAY GENUINO APRIL 30, 2015
ADRENAL
GLANDS
Dr.
Banny
Bay
C.
Genuino
III. PHYSIOLOGY
IV. DISORDERS OF THE ADRENAL CORTEX
Hyperaldosteronism
Primary (Conns Syndrome)
-
Adenoma (70%)
-
Idiopathic Bilateral Hyperplasia (30%)
-
Adrenocortical carcinoma and glucocorticoid-
suppressible hyperaldosteronism (<1%)
Seconadary
S/Sx: hypertension, hypochalemia
Dxcs:
-
Biochemical
-
Imaging:
CT
scan/MRI
Aldosterone functions mainly to increase sodium
reabsorption and potassium and hydrogen ion excretion at
the level of the renal distal convoluted tubule.
Once
the
biochemical
diagnosis
is
confirmed,
further
evaluation
should
be
directed
at
determining
which
patients
have
a
unilateral
aldosteronoma
vs.
bilateral
hyperplasia,
because
surgery
is
almost
always
curative
for
the
former,
but
usually
not
the
latter.
Only
20%
to
30%
of
patients
with
hyperaldosteronism
secondary
to
bilateral
adrenal
hyperplasia
benefit
from
surgery,
and
as
described,
selective
venous
catheterization
is
useful
to
predict
which
patients
will
respond.
For
the
other
patients,
medical
therapy
with
spironolactone,
amiloride,
or
triamterene
is
the
mainstay
of
management.
Glucocorticoid-suppressible
hyperaldosteronism
is
treated
by
administering
exogenous
dexamethasone
at
doses
of
0.5
to
1
mg
daily.
Treatment
with
spironolactone
may
help
decrease
glucocorticoid
requirements
in
this
condition
and
avoid
symptoms
of
Cushings
syndrome.
Postoperatively,
some
patients
experience
transient
hypoaldosteronism
requiring
mineralocorticoids
for
up
to
3
months.
Rarely,
acute
Addisons
disease
may
occur
2
to
3
days
after
adrenalectomy.
Adrenalectomy
is
>90%
successful
in
improving
hypokalemia
and
about
70%
successful
in
correcting
hypertension.
ADRENAL
GLANDS
Page
2
of
7
DR. BANNY C. BAY GENUINO APRIL 30, 2015
Cushings
syndrome
-
Symptoms
and
signs
resulting
from
hypersecretion
of
cortisol
regardless
of
etiology
Cushings
disease
-
Pituitary tumor (adenoma) bilateral adrenal
hyperplasia and hypercortisolism
Etiology of Cushings Syndrome
ACTH-dependent (70%)
Pituitary adenoma or Cushings disease (~70%)
Ectopic ACTH production* (~10%)
Ectopic CRH production (<1%)
ACTH-independent (20%-30%)
Adrenal adenoma (10%-15%)
Adrenam carcinoma (5%-10%)
Adrenal hyperplasia pigmentedmicronodular cortical
hyperplasia or gastric inhibitory peptide-sensitive
macronodular hyperplasia (5%)
Other
Pseudo-Cushings Syndrome
Iatrogenic exogenous administration of steroids
*From small cell lung tumors, pancreatic islet cell tumors, medullar
thryoid cancers, pheochromoctyomas, and carcinoid tumors of the
lung, thymus, gut, pancreas, and ovary
ACTH = adrenocorticotropic hormone; CRH = corticotrophin-
releasing hormone
Most common cause of Cushings syndrome
EXOGENOUS
Most common cause of endogenous Cushings syndrome
PITUITARY ADENOMA (90%)
Features of Cushings Syndrome
SYSTEM
MANIFESTATION
Weight gain central obesity, buffalo hump,
General
supraclavicular fat pads
Hirsutism, plethora, purple striae, acne
Integumentary
ecchymosis
Cardiovascular
Hypertension
Musculoskeletal Generalized weakness, osteopenia
Neuropsychiatric Emotional lability, psychosis, depression
Metabolic
Diabetes or glucose intolerance, hyperlipidemia
Renal
Polyuria, renal stones
Impotence, decreased libido, mentsrual
Gonadal
irregularities
ADRENAL GLANDS Page 3 of 7
DR. BANNY C. BAY GENUINO APRIL 30, 2015
Hypercotisolism
Cushing described patients with a peculiar fat deposition,
amenorrhea, impotence (in men), hirsutism, purple striae,
hypertension, diabetes, and other features that constitute
the syndrome
Diagnostic studies for confirming Cushings syndrome:
-
OVERNIGHT DST
-
24-HOUR URINARY FREE CORTISOL
-
11:00 PM SALIVARY CORTISOL
Laparoscopic adrenalectomy: adrenal adenomas
Open adrenalectomy: large tumors (6 cm) or
adrenocortical cancers
Bilateral adrenalectomy: primary adrenal hyperplasia
Cushings
disease:
-
Transsphenoidal
excision
of
the
pituitary
adenoma:
successful
in
80%
of
patients
-
Pituitary
irradiation:
Persistent or recurrent disease after surgery
Associated with a high rate of
panhypopituitarism
Some patients develop visual deficits
-
Stereotactic radiosurgery
Uses CT guidance
Deliver high doses of radiotherapy to the tumor
(photon or gamma knife) and also bilateral
laparoscopic adrenalectomy
Medical adrenalectomy: (patients who fail to respond to
treatment)
-
KETOCONAZOLE
-
METYRAPONE
-
AMINOGLUTETHIMIDE
Ectopic ACTH production
-
Treating the primary tumor
-
Medical or bilateral laparoscopic adrenalectomy
Palliate patients with unresectable disease
Ectopic ACTH-secreting tumor cannot be
localized
Adrenocortical Cancer
Rare neoplasms: 2 per 1 million worldwide incidence
th
th
Bi-modal age distribution: children and adults (4 and 5
decades of life)
Majority are sporadic
Associated with germline mutations of:
-
p53 (LI-FRAUMENI SYNDROME)
-
MENIN (MULTIPLE ENDOCRINE NEOPLASIA TYPE 1)
Nonfunctioning (50%) Patients with functioning tumors
often present with the rapid
Cortisol-secreting
onset
of
Cushings
syndrome
(30%)
accompanied
by
virilizing
Androgens
(20%)
features.
Nonfunctioning
tumors
Estrogens
(10%)
more
commonly
present
with
an
Aldosterone
(2%)
enlarging
abdominal
mass
and
Multiple
hormones
abdominal
or
back
pain.
Rarely,
(35%)
weight
loss,
anorexia,
and
nausea
may
be
present.
What is the most common functioning adrenocortical
cancer = CORTISOL-SECRETING
What is the least common functioning adrenocortical
cancer = ALDOSTERONE
Diagnostics
-
Serum
electrolyte
levels
-
Urinary
catecholamines
-
Dexamethasone
suppression
test
-
24-hour
urine
collection
for
cortisol
-
CT
and
MRI
scans:
SIZE of the adrenal mass on imaging studies is
the single most important criterion to help
diagnose malignancy
The most important predictor of survival in patients with
adrenal cancer is the ADEQUACY OF RESECTION!
Adjuvant setting?
Surgical
debulking
Sex
Steroid
Excess
Virilizing
syndromes
-
PLASMA
DHEA
-
URINE
17-KETO-STEROIDS
-
GLUCOCORTICOIDS
Feminizing adrenal tumors
-
ESTROGEN LEVEL
-
URINE 17-KETO-STEROIDS
Virilizing tumors produce excessive amounts of the androgen
precursor, DHEA, which can be measured in plasma or urine as 17-
ketosteroids. Patients with feminizing tumors also have elevated
urinary 17-ketosteroids in addition to increased estrogen levels.
Androgen-producing tumors often are associated with production of
other hormones such as glucocorticoids.
Treatment: adrenalectomy
Adrenolytic
drugs
-
MITOTANE
-
AMINOGLUTETHIMIDE
-
KETOCONAZOLE
ADRENAL
GLANDS
Page
4
of
7
DR. BANNY C. BAY GENUINO APRIL 30, 2015
Sudden death may occur in patients with
undiagnosed tumors who undergo other surgeries or
biopsy.
-
Symptoms such as anxiety, tremulousness,
paresthesias, flushing, chest pain, shortness of
breath, abdominal pain, nausea, vomiting, and others
are and may be episodic in nature
Dxcs:
-
Biochemical studies (24-hour urine samples for
catecholamines and their metabolites, as well as by
determining plasma metanephrine levels)
Urinary metanephrines
VMA
measurements
-
Radiologic
studies
CT scan
MRI
MIBG (metaiodobenzylguanidine) specific for
pheochromocytoma
Treatment:
-
Medical
Blood pressure control
o -blockers such as phenoxybenzamine
o -Blockers such as propranolol
Volume
repletion
-
Surgical
Adrenalectomy is the treatment of choice for
patients with pheochromocytoma. The chief goal
of surgery is to resect the tumor completely with
minimal tumor manipulation or rupture of the
tumor capsule.
Hereditary
Pheochromocytomas
Multiple and bilateral
Unilateral adrenalectomy
Cortical-sparing subtotal adrenalectomy
Laparoscopic subtotal adrenalectomy
Recurrent pheochromocytoma
Autotransplantation of adrenocortical tissue
However, most pheochromocytomas <5 cm in diameter can be
safely resected laparoscopically.
Malignant Pheochromocytomas
12% to 29% of pheochromocytomas
Decreased survival
No definitive histologic criteria defining malignant
pheochromocytomas
-
Malignancy usually is diagnosed when there is
evidence of invasion into surrounding structures or
distant metastases
-
Most common sites: bone, liver, regional lymph
nodes, lung, and peritoneum
Brain, pleura, skin, and muscles may also
occasionally be involved
Pleomorphism, nuclear atypia, and abundant mitotic
figures are seen in benign tumors. Capsular and vascular
invasion may be seen in benign lesions as well.
ADRENAL GLANDS Page 5 of 7
DR. BANNY C. BAY GENUINO APRIL 30, 2015
Congenital Adrenal Hyperplasia
A group of disorders that result from deficiencies or
complete absence of enzymes involved in adrenal
steroidogenesis
CONGENITAL ADRENAL LIPOID HYPERPLASIA
-
Most severe form of CAH
-
CHOLESTEROL DESMOLASE DEFICIENCY
-
Disruption of all steroid biosynthetic pathways
fatal salt-wasting syndrome in phenotypic female
patients
21 -HYDROXYLASE most common enzyme deficiency
nd
11 -HYDROXYLASE 2 most common enzyme
deficiency
Dxcs:
-
Karyotype
analysis
-
Measurement
of
plasma
and
urinary
steroids
Imaging:
-
CT
-
MRI
-
NP-59
Treatment:
-
Medically:
Traditionally
Cortisol and mineralocorticoid replacement to
suppress the hypothalamic-pituitary-adrenal axis
The doses of steroids required often are
supraphysiologic and lead to iatrogenic
hypercortisolism
-
Bilateral laparoscopic adrenalectomy
Recently has been proposed as an alternative
treatment
Has been successfully performed in a limited
number of patients for various forms of CAH
V. DISORDERS OF THE ADRENAL MEDULLA
Pheochromocytoma
The 10 percent tumor
-
10% are BILATERAL
-
10% are MALIGNANT
-
10% OCCUR IN PEDIATERIC PATIENTS
-
10% are EXTRA-ADRENAL
-
10% are FAMILIAL
Functional
Paraganglioma:
-
Extra-adrenal
tumors
-
At
sites
of
sympathetic
ganglia
in
the
ORGAN
OF
ZUCKERKANDL,
NECK,
MEDIASTINUM,
ABDOMEN,
AND
PELVIS
S/Sx:
-
The
classic
triad:
Headache,
palpitations,
and
diaphoresis
-
Nonspecific
-
Cardiovascular
complications
-
Exercise,
micturition,
defecation
precipitating
factors
-
Hypertension:
most
common
clinical
sign;
can
be
Paroxysmal with intervening normotension
Sustained with paroxysms
Sustained hypertension alone.
VI. THE ADRENAL INCIDENTALOMA
Incidentalomas
-
Lesions discovered during imaging performed for
unrelated reasons
-
Excludes tumors discovered on imaging studies
performed for evaluating symptoms of hormone
hypersecretion or staging patients with known cancer
-
Incidence: 0.4% to 4.4%.
MEMORIZE!
VII. ADRENAL INSUFFICIENCY
Etiology of Adrenal Insufficiency
PRIMARY
SECONDARY
Autoimmune (autoimmune polyglandular
disease type I and II)
Exogenous
Infectious TB, fungi, CMV, HIV
glucocorticoid
Hemorrhage spontaneous
therapy
(Waterhouse-Friderichsen syndrome)
Bilateral
and secondary to stress, trauma,
adrenalectomy
infections, coagulopathy, or
Pituitary or
anticoagulants
hypothalamic tumors
Metastases
Pituitary hemorrhage
Infiltrative disorders amyloidosis,
(postpartum
hemochromatosis
Sheehans syndrome)
Adrenoleukodystrophy
Transsphenoidal
Congenital adrenal hyperplasia
resection of pituitary
Drugs ketoconazole, metyrapone,
tumor
aminoglutethimide, mitotane
Most common cause of insufficiency = EXOGENOUS
S/Sx:
-
Stressed
patients
with
any
of
the
relevant
risk
factors
-
May
mimic
sepsis,
myocardial
infarction,
or
pulmonary
embolus
-
Presents
with
fever,
weakness,
confusion,
nausea,
vomiting,
lethargy,
abdominal
pain,
or
severe
hypotension.
Chronic Adrenal Insufficiency
-
Patients with metastatic tumors, may be more subtle
-
Fatigue, salt craving, weight loss, nausea, vomiting,
and abdominal pain
-
Patients may appear hyperpigmented from increased
secretion of CRH and ACTH, with increased -
melanocyte-stimulating hormone side-products.
Diagnostic
Studies
-
Laboratory
findings:
hyponatremia,
hyperkalemia,
eosinophilia,
mild
azotemia,
and
fasting
or
reactive
hypoglycemia.
-
PBS:
may
demonstrate
eosinophilia
in
approximately
20%
of
patient
-
ACTH
stimulation
test
ACTH is infused intravenously, and cortisol levels
are measured at 0, 30, and 60 minutes. Peak
cortisol levels <20 g/dL suggest adrenal
insufficiency.
HIGH ACTH LEVELS WITH LOW PLASMA
CORTISOL levels are diagnostic of primary
adrenal insufficiency.
Hydrocortisone interferes with ACTH which is
used in diagnosis of insufficiency
Management:
-
Volume
resuscitation
-
Dexamethasone
(4
mg)
should
be
administered
intravenously.
Hydrocortisone
(100
mg
intravenously
every
8
hours)
also
may
be
used,
but
it
interferes
with
testing
of
cortisol
levels.
-
Infection
should
be
sought,
identified,
and
treated.
The
ACTH
stimulation
test
should
be
performed
to
confirm
the
diagnosis
-
Mineralocorticoids
(fludrocortisone
0.050.1
mg
daily)
may
be
required
once
the
saline
infusions
are
discontinued.
ADRENAL GLANDS Page 6 of 7
DR. BANNY C. BAY GENUINO APRIL 30, 2015
ADRENAL
GLANDS
Page
7
of
7
DR. BANNY C. BAY GENUINO APRIL 30, 2015
VIII. ADRENAL SURGERY
Open
MIS
Anterior approach
Transabdominal (anterior and
Posterior approach
lateral)
Lateral approach
Retroperitoneal (lateral or
posterior) approach)
Laparoscopic adrenalectomy has rapidly become the
standard procedure of choice for the excision of most benign-
appearing adrenal lesions <6 cm in diameter. The role of
laparoscopic adrenalectomy in the management of adrenocortical
cancers is controversial.
Complications of Adrenal Surgery
Cushings
syndrome:
-
Prone
to
infectious
-
Thrombotic
complications
Creation of pneumoperitoneum
Excessive retraction and dissection
Postoperative hemodynamic instability
-
Pheochromocytomas
Adrenal insufficiency after bilateral adrenalectomy and
sometimes after unilat- eral adrenalectomy
Long-term morbidity: NELSONS SYNDROME
-
Nelsons Syndrome = enlargement of pituitary gland
after you remove the adrenals
-
This leads to increased ACTH levels,
hyperpigmentation, visual field defects, headaches,
and extraocular muscle palsies. Transsphenoidal
pituitary resection is the ini- tial mode of therapy, and
external-beam radiotherapy is used in patients with
residual tumor or extrasellar invasion.
Das könnte Ihnen auch gefallen
- The Adrenal GlandesDokument19 SeitenThe Adrenal GlandesamrsameerNoch keine Bewertungen
- AdrenalDokument19 SeitenAdrenalRumela Ganguly ChakrabortyNoch keine Bewertungen
- Adrenal Insufficiency and Cushing's Disease-1Dokument34 SeitenAdrenal Insufficiency and Cushing's Disease-1Mwanja MosesNoch keine Bewertungen
- Cushing's SyndromeDokument35 SeitenCushing's SyndromeYoga KarsendaNoch keine Bewertungen
- Adrenal DisordersDokument57 SeitenAdrenal Disordersnashadmohammed99Noch keine Bewertungen
- Cushing's SyndromeDokument35 SeitenCushing's SyndromeShankara Pillai100% (3)
- Case Report: Grace Y. Kim, MD Helen Anaedo, MD Sahar Nozad, MD Tipu Nazeer, MD Hassan Shawa, MDDokument6 SeitenCase Report: Grace Y. Kim, MD Helen Anaedo, MD Sahar Nozad, MD Tipu Nazeer, MD Hassan Shawa, MDPedro Gómez RNoch keine Bewertungen
- Adrenal Gland Disorders ExplainedDokument73 SeitenAdrenal Gland Disorders ExplainedReunita ConstantiaNoch keine Bewertungen
- Disorders of The Adrenal Glands: Adrenal Cortical Adenoma and CarcinomaDokument9 SeitenDisorders of The Adrenal Glands: Adrenal Cortical Adenoma and Carcinomahussain AltaherNoch keine Bewertungen
- Absite CH 21 AdrenalDokument10 SeitenAbsite CH 21 AdrenalJames JosephNoch keine Bewertungen
- Adrenal Gland Disorders: Cushing's, Primary Aldosteronism & MoreDokument9 SeitenAdrenal Gland Disorders: Cushing's, Primary Aldosteronism & Morehussain AltaherNoch keine Bewertungen
- New Advances in Diagnosis and Treatment of Cushing SyndromeDokument12 SeitenNew Advances in Diagnosis and Treatment of Cushing SyndromeIka AnisaNoch keine Bewertungen
- Liyon - Endocrine GlandDokument26 SeitenLiyon - Endocrine GlandLiyon BasnetNoch keine Bewertungen
- Cancer - June 1979 - Diasio - Adenocarcinoma of The Pancreas Associated With Hypoglycemia Case Report and Review of TheDokument8 SeitenCancer - June 1979 - Diasio - Adenocarcinoma of The Pancreas Associated With Hypoglycemia Case Report and Review of Theabdullah shamshirNoch keine Bewertungen
- Cushing's - Syndrome - Nov 2010Dokument35 SeitenCushing's - Syndrome - Nov 2010Jim Jose AntonyNoch keine Bewertungen
- Uro2008, Vol.35, Issues 3, Minimally Invasive Genitourinary ProceduresDokument180 SeitenUro2008, Vol.35, Issues 3, Minimally Invasive Genitourinary ProcedureschuvanlaiNoch keine Bewertungen
- P Wave T Waves QRS ComplexDokument16 SeitenP Wave T Waves QRS ComplexYousef Al-AmeenNoch keine Bewertungen
- Recurrence of Cushing's Disease After Bilateral Adrenalectomy: A Myth or Reality?Dokument4 SeitenRecurrence of Cushing's Disease After Bilateral Adrenalectomy: A Myth or Reality?Gordana PuzovicNoch keine Bewertungen
- Definition - Cushing's Syndrome Is The Combination of Symptoms and SignsDokument4 SeitenDefinition - Cushing's Syndrome Is The Combination of Symptoms and SignsSuhas IngaleNoch keine Bewertungen
- Internal medicine שחזוריםDokument66 SeitenInternal medicine שחזוריםLaith Bajis NassarNoch keine Bewertungen
- Endocrine Pancreas: Dr. Hasan Manzoor Ahmed MBBS, MS General and Hepatobiliary SurgeryDokument54 SeitenEndocrine Pancreas: Dr. Hasan Manzoor Ahmed MBBS, MS General and Hepatobiliary SurgeryMEHJABINHAQNoch keine Bewertungen
- ENDOCRINE DISORDERS (Autosaved)Dokument81 SeitenENDOCRINE DISORDERS (Autosaved)Princewill SeiyefaNoch keine Bewertungen
- Table of Content: S.No. Topic NumberDokument10 SeitenTable of Content: S.No. Topic NumbercharanNoch keine Bewertungen
- Endocrine PBL Trigger 3Dokument6 SeitenEndocrine PBL Trigger 3Ho Yong WaiNoch keine Bewertungen
- Pathology of Adrenal Glands.Dokument41 SeitenPathology of Adrenal Glands.Sukma Eka PratiwiNoch keine Bewertungen
- AdrenalDokument47 SeitenAdrenalamrsameerNoch keine Bewertungen
- AdrenalDokument9 SeitenAdrenalNada MuchNoch keine Bewertungen
- Adrenal Gland DisordersDokument24 SeitenAdrenal Gland Disorderssimona mariana dutuNoch keine Bewertungen
- Thyroid Nodule WorkupDokument39 SeitenThyroid Nodule WorkupRumana IslamNoch keine Bewertungen
- Renal Cancers - Shalom - 2Dokument30 SeitenRenal Cancers - Shalom - 2Bryan FjbNoch keine Bewertungen
- Adrenalectomy: Dr. Subbaiah. M.P.TDokument27 SeitenAdrenalectomy: Dr. Subbaiah. M.P.Tvicentiu2003Noch keine Bewertungen
- Cushing Syndrome: M.Sc. (N) 1 YearDokument30 SeitenCushing Syndrome: M.Sc. (N) 1 YearRanjana SharmaNoch keine Bewertungen
- Imaging of the Adrenal GlandsDokument140 SeitenImaging of the Adrenal GlandsSahana RNoch keine Bewertungen
- Mediastinal Mass in A Dog With Syncope and Abdominal DistensionDokument3 SeitenMediastinal Mass in A Dog With Syncope and Abdominal DistensionIoana SanduNoch keine Bewertungen
- Common Pediatric Malignancies: Wilms Tumor and NeuroblastomaDokument34 SeitenCommon Pediatric Malignancies: Wilms Tumor and NeuroblastomanazymalfikryNoch keine Bewertungen
- General Pathology 2nd BM Neoplasia Blood Vessel Cardiovascular Pathology Pulmonary PathologyDokument64 SeitenGeneral Pathology 2nd BM Neoplasia Blood Vessel Cardiovascular Pathology Pulmonary PathologyCherry RahimaNoch keine Bewertungen
- Pediatric Imaging 2020Dokument84 SeitenPediatric Imaging 2020shellers24Noch keine Bewertungen
- Disorders of The Adrenal Glands: Adrenal Cortical Adenoma and CarcinomaDokument9 SeitenDisorders of The Adrenal Glands: Adrenal Cortical Adenoma and Carcinomahussain AltaherNoch keine Bewertungen
- 2-Adrenal Path.Dokument72 Seiten2-Adrenal Path.Lea MonzerNoch keine Bewertungen
- Aortic Dissection Associated With Aortic Aneurysms and Posterior Paresis in A DogDokument7 SeitenAortic Dissection Associated With Aortic Aneurysms and Posterior Paresis in A DogMuhamad Abdul MubdiNoch keine Bewertungen
- Archives of Renal Diseases and ManagementDokument3 SeitenArchives of Renal Diseases and ManagementPeertechz Publications Inc.Noch keine Bewertungen
- Addison+conn+cush+feo+adr IncidentalomaDokument65 SeitenAddison+conn+cush+feo+adr IncidentalomaMjn BausatNoch keine Bewertungen
- Ep171905 CRDokument6 SeitenEp171905 CRTantri SyahtiraNoch keine Bewertungen
- SurgeryDokument30 SeitenSurgeryLuai Tuma KhouryNoch keine Bewertungen
- T5 Pancreas PDFDokument19 SeitenT5 Pancreas PDFAmin ZahariNoch keine Bewertungen
- CUSHING'S SyndromeDokument9 SeitenCUSHING'S SyndromeTheavuthyNoch keine Bewertungen
- Discussion: Meigs' Syndrome and Pseudo-Meigs' SyndromeDokument3 SeitenDiscussion: Meigs' Syndrome and Pseudo-Meigs' SyndromeFlapianne SimenceriauNoch keine Bewertungen
- Diseases of Rectum and Anal CanalDokument68 SeitenDiseases of Rectum and Anal CanalKoridor Falua Sakti Halawa 21000063Noch keine Bewertungen
- Necrotizing Enterocolitis (Sultn Aiman NeazyDokument59 SeitenNecrotizing Enterocolitis (Sultn Aiman NeazyMohammed ElhashimiNoch keine Bewertungen
- 005 - Cushing SyndromeDokument51 Seiten005 - Cushing SyndromeLucas Victor AlmeidaNoch keine Bewertungen
- Anaesthesia in Emergency Laparotomy: Speaker:P.Shravani Moderator:Dr.K.Vinay Assistant ProfessorDokument52 SeitenAnaesthesia in Emergency Laparotomy: Speaker:P.Shravani Moderator:Dr.K.Vinay Assistant ProfessorSanthi Swetha PudhotaNoch keine Bewertungen
- Surgery and Post OpDokument96 SeitenSurgery and Post OpNguyễn Nhật HoàngNoch keine Bewertungen
- Symptomatic Lymphangioma of The Adrenal Gland: A Case ReportDokument3 SeitenSymptomatic Lymphangioma of The Adrenal Gland: A Case Reportjulio perezNoch keine Bewertungen
- Fat Emboli in LiposuctionDokument34 SeitenFat Emboli in LiposuctionRicky Herdianto100% (1)
- TiroidektomyDokument80 SeitenTiroidektomyGideon Ardhya TrinoviantoNoch keine Bewertungen
- Acute Mesenteric Ischemia: A Challenging Diagnostic Disease-Four Cases Reports and Literature Review (AMI)Dokument10 SeitenAcute Mesenteric Ischemia: A Challenging Diagnostic Disease-Four Cases Reports and Literature Review (AMI)rahmatobineNoch keine Bewertungen
- Adrenal Disorders: Dr. Anil Dhakal Lecturer, Internal MedicineDokument53 SeitenAdrenal Disorders: Dr. Anil Dhakal Lecturer, Internal MedicineBi PinNoch keine Bewertungen
- Systemic Vasculitis Clinical ApproachDokument65 SeitenSystemic Vasculitis Clinical ApproachLydwiNa Jc100% (1)
- Cushings Addisons and Acromegaly EdDokument45 SeitenCushings Addisons and Acromegaly Edsamehseef100% (1)
- The Newer Physiology in Surgical and General PracticeVon EverandThe Newer Physiology in Surgical and General PracticeNoch keine Bewertungen
- Fever and HyperthermiaDokument6 SeitenFever and HyperthermiaMarco Paulo Reyes NaoeNoch keine Bewertungen
- Physiology Index CardsDokument30 SeitenPhysiology Index CardsMarco Paulo Reyes NaoeNoch keine Bewertungen
- Williams Endocrinology Large CoverDokument1 SeiteWilliams Endocrinology Large CoverMarco Paulo Reyes Naoe33% (9)
- Electronic Chapter Harrison's 19th EditionDokument1 SeiteElectronic Chapter Harrison's 19th EditionMarco Paulo Reyes Naoe0% (1)
- CPC NarrationDokument5 SeitenCPC NarrationMarco Paulo Reyes NaoeNoch keine Bewertungen
- Alcoholic Liver DiseaseDokument22 SeitenAlcoholic Liver DiseaseVikramjeet SinghNoch keine Bewertungen
- Pharma Super TableDokument56 SeitenPharma Super TableMarco Paulo Reyes NaoeNoch keine Bewertungen
- Ob-Gyn Post Graduate Interns May-June 2017-2018Dokument1 SeiteOb-Gyn Post Graduate Interns May-June 2017-2018Marco Paulo Reyes NaoeNoch keine Bewertungen
- Table of Contents Williams Endocrinology 13th EditionDokument4 SeitenTable of Contents Williams Endocrinology 13th EditionMarco Paulo Reyes NaoeNoch keine Bewertungen
- Gradeschool ReviewerDokument7 SeitenGradeschool ReviewerMarco Paulo Reyes NaoeNoch keine Bewertungen
- Price List For PVC Single Loop Wire From OREZADokument1 SeitePrice List For PVC Single Loop Wire From OREZAMarco Paulo Reyes NaoeNoch keine Bewertungen
- Approach to Leg Edema DiagnosisDokument4 SeitenApproach to Leg Edema DiagnosisMarco Paulo Reyes NaoeNoch keine Bewertungen
- Assessment of Back Pain-BMJDokument30 SeitenAssessment of Back Pain-BMJMarco Paulo Reyes NaoeNoch keine Bewertungen
- SEIZURE CASE PROTOCOLDokument1 SeiteSEIZURE CASE PROTOCOLMarco Paulo Reyes NaoeNoch keine Bewertungen
- APRIL 2017: Aurora Hill and Engineer's Hill Health CentersDokument2 SeitenAPRIL 2017: Aurora Hill and Engineer's Hill Health CentersMarco Paulo Reyes NaoeNoch keine Bewertungen
- Florist ContractDokument1 SeiteFlorist ContractMarco Paulo Reyes NaoeNoch keine Bewertungen
- Gastroenterology-Liver, Pancreas and Gall Bladder LecturesDokument7 SeitenGastroenterology-Liver, Pancreas and Gall Bladder LecturesMarco Paulo Reyes NaoeNoch keine Bewertungen
- Special Awards - ListDokument7 SeitenSpecial Awards - ListMarco Paulo Reyes NaoeNoch keine Bewertungen
- Liver Cirrhosis2 LectureDokument104 SeitenLiver Cirrhosis2 LectureMarco Paulo Reyes NaoeNoch keine Bewertungen
- Admiting Conference - Acute GastroenteritisDokument38 SeitenAdmiting Conference - Acute GastroenteritisMarco Paulo Reyes NaoeNoch keine Bewertungen
- Pharma AntidiarrhealDokument3 SeitenPharma AntidiarrhealMarco Paulo Reyes NaoeNoch keine Bewertungen
- Selective Serotonin Reuptake Inhibitors: Naoe, Marco Paulo RDokument38 SeitenSelective Serotonin Reuptake Inhibitors: Naoe, Marco Paulo RMarco Paulo Reyes NaoeNoch keine Bewertungen
- Cancer Drugs MRSDokument12 SeitenCancer Drugs MRSMarco Paulo Reyes NaoeNoch keine Bewertungen
- Pharma AntidiarrhealDokument3 SeitenPharma AntidiarrhealMarco Paulo Reyes NaoeNoch keine Bewertungen
- Consent in Emergency CasesDokument10 SeitenConsent in Emergency CasesMarco Paulo Reyes NaoeNoch keine Bewertungen
- The ParturientDokument22 SeitenThe ParturientMarco Paulo Reyes NaoeNoch keine Bewertungen
- CPC SCRIPT SemifinalDokument5 SeitenCPC SCRIPT SemifinalMarco Paulo Reyes NaoeNoch keine Bewertungen
- Acute Nephritic SyndromeDokument1 SeiteAcute Nephritic SyndromeMarco Paulo Reyes NaoeNoch keine Bewertungen
- 3rd and 4th Stage of Labor Dr. BaduaDokument8 Seiten3rd and 4th Stage of Labor Dr. BaduaMarco Paulo Reyes NaoeNoch keine Bewertungen
- Ventilater CareDokument6 SeitenVentilater CarehelenfreedaeqdNoch keine Bewertungen
- Chest RadiologyDokument129 SeitenChest RadiologyNadiya SafitriNoch keine Bewertungen
- Therapeutic Communication TechniquesDokument10 SeitenTherapeutic Communication TechniquesJohn Eric Contreras VillegasNoch keine Bewertungen
- Med J Malaysia Vol 64 No 4 Dec 2009Dokument55 SeitenMed J Malaysia Vol 64 No 4 Dec 2009Musthafa Afif WardhanaNoch keine Bewertungen
- IV Therapy 2 PDFDokument132 SeitenIV Therapy 2 PDFJulie May SuganobNoch keine Bewertungen
- Mono 114Dokument511 SeitenMono 114Jose Angel AbadíaNoch keine Bewertungen
- ENT and Head & Neck CT Imaging ExamplesDokument84 SeitenENT and Head & Neck CT Imaging Examplesdrqazi777Noch keine Bewertungen
- Dental Product CatalogDokument193 SeitenDental Product CatalogJeanBrinzaNoch keine Bewertungen
- A Rat Model For Oral Mucositis Induced byDokument7 SeitenA Rat Model For Oral Mucositis Induced byYanski DarmantoNoch keine Bewertungen
- 1 5053054235202027721Dokument175 Seiten1 5053054235202027721andifa aziz satriawanNoch keine Bewertungen
- Verb Surgical - Surgery in The Digital AgeDokument15 SeitenVerb Surgical - Surgery in The Digital AgemedtechyNoch keine Bewertungen
- KaoshikiiDokument24 SeitenKaoshikiiapi-238078813Noch keine Bewertungen
- Portofolio FatmaDokument12 SeitenPortofolio FatmafitriaokNoch keine Bewertungen
- Three in A Row A Case Series of Cervical TuberculosisDokument6 SeitenThree in A Row A Case Series of Cervical TuberculosisJonelle baloloyNoch keine Bewertungen
- Nursing Fundamental Q&ADokument26 SeitenNursing Fundamental Q&ALinjumol T GNoch keine Bewertungen
- Clavicle Fracture RehabDokument7 SeitenClavicle Fracture Rehabnmmathew mathewNoch keine Bewertungen
- Useful Plants - Medicines: at LeastDokument8 SeitenUseful Plants - Medicines: at LeastJavier Yaguareté100% (1)
- A New Validated Stability-Indicating RP-HPLC Method For The Estimation of Pitavastatin in Tablet Dosage FormsDokument8 SeitenA New Validated Stability-Indicating RP-HPLC Method For The Estimation of Pitavastatin in Tablet Dosage FormsSriram NagarajanNoch keine Bewertungen
- 2024-02-08 St. Mary's County TimesDokument32 Seiten2024-02-08 St. Mary's County TimesSouthern Maryland OnlineNoch keine Bewertungen
- Social Skills and Autism Spectrum Disorders Application ListDokument82 SeitenSocial Skills and Autism Spectrum Disorders Application ListAl OyNoch keine Bewertungen
- Perioperative NursingDokument26 SeitenPerioperative NursingTine Guibao100% (1)
- HSB Pneumonia Antibiotic AlgorithmDokument4 SeitenHSB Pneumonia Antibiotic AlgorithmDr.Senthil KumarNoch keine Bewertungen
- Benjamin A. Root Understanding Panic and Other Anxiety Disorders 2000Dokument122 SeitenBenjamin A. Root Understanding Panic and Other Anxiety Disorders 2000StefanNoch keine Bewertungen
- The Cowards of WarDokument9 SeitenThe Cowards of WarJess Willox100% (1)
- Davey Cord - MSDSDokument4 SeitenDavey Cord - MSDSTara VergitaNoch keine Bewertungen
- 0 The Mega BrainDokument388 Seiten0 The Mega Brainhwzeee100% (14)
- Closure of Midline Diastema by Multidisciplinary Approach - A Case ReportDokument5 SeitenClosure of Midline Diastema by Multidisciplinary Approach - A Case ReportAnonymous izrFWiQNoch keine Bewertungen
- COVID 19 Bharat India Report November09 2022 DailyCases 1116 Deaths 5 Based 781 DaysAnalysis Fbclid IwAR2orDokument225 SeitenCOVID 19 Bharat India Report November09 2022 DailyCases 1116 Deaths 5 Based 781 DaysAnalysis Fbclid IwAR2orP Eng Suraj SinghNoch keine Bewertungen
- Memorandum of UnderstandingDokument3 SeitenMemorandum of UnderstandingLionel MsuNoch keine Bewertungen
- Flare Ups in Endodontics - 1 Etiological FactorsDokument6 SeitenFlare Ups in Endodontics - 1 Etiological FactorsdrshravyaNoch keine Bewertungen